Abstract
Recurrent implantation failure (RIF) is characterized by repeated embryo transfers without pregnancy. To date, the etiology of RIF remains poorly understood. Accumulating evidence indicates a beneficial role of endometrial extracellular vesicles (EVs) during the implantation by delivering signaling molecules to embryos, especially miRNAs. However, whether EVs secreted by RIF patients’ endometria have a similar miRNA expression profile of endometrial EVs of fertile women has not been investigated. Therefore, in this study, we compared the miRNA expression profiles between the endometrial EVs of RIF patients (RIF-EVs) and fertile women (FER-EVs). Endometrial tissues from fifteen RIF patients and nine fertile women were collected and digested to cells for culture. Endometrial cells were modulated by estrogen and progesterone to mimic the secretory phase, and the conditioned medium was collected for EV isolation. EVs were determined by western blotting, nanoparticle tracking analysis, and transmission electronic microscopy (TEM). Three pairs of EV samples from two groups were used for miRNA sequencing, and twelve RIF-EV samples and six FER-EV samples were used for validation using quantitative reverse transcription polymerase chain reaction (qRT-PCR). Results showed that a total of 11 miRNAs were differently expressed in the RIF-EVs. Besides, four of the differently expressed miRNAs were validated using qRT-PCR. Target genes of the differently expressed miRNAs were predicted, and the functional analysis was performed. Besides, we proved that the most significantly different miRNA, 6131, inhibited the growth and invasion of HTR8/SVneo cells. Our study suggested that the altered miRNAs in the RIF-EVs might be involved in the pathogenesis of RIF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The impressive advances of assisted reproductive technology (ART) have allowed numerous infertile couples to achieve clinical pregnancy [1]. However, a new challenge has emerged: recurrent implantation failure (RIF). RIF refers to a condition in which women experience repeated implantation failures after transferring good-quality embryos [2, 3]. Although a universal definition of RIF has not been established, it is widely accepted that three or more consecutive implantation failures meet the criteria [4]. The incidence of RIF is difficult to predict as definition and populations vary, with figures up to 10% being reported [5]. Clarifying the pathogenesis of RIF, which may provide benefits to treatments, is in great demand.
A successful implantation depends on the synchronized interactions between a receptive endometrium and functional embryos [6, 7]. Among these two factors, the endometrium is considered to be more important, since endometrial factors are responsible for approximately two-thirds of implantation failures [7, 8]. Therefore, many studies have aimed to characterize the differences between the endometria of RIF patients and fertile women to investigate the possible mechanisms. They demonstrated that the RNA and protein profiles in the endometria of RIF patients were altered [9,10,11]. Moreover, several embryonic implantation–related pathways, including Wnt and cellular adhesion pathways, were greatly affected [9]. These findings confirmed the aberrant nature of RIF patients’ endometria. However, the detailed mechanisms, by which such distorted endometria interfered with implantation, have not been clarified.
Extracellular vesicles (EVs) are nanometer-sized, membrane-enclosed vesicles, acting as mediators of intercellular communication [12,13,14]. EVs can be secreted from almost all cell types [15], whereas they display compositional heterogeneity according to their original cell type and of its status [16]. Given the altered molecular repertoires in the RIF patients’ endometria, it is legitimate to speculate that the contents in the endometrial EVs of RIF patients are different compared to those of fertile women.
Recent evidence indicated that EVs played an important role in the embryonic implantation. Previous studies have identified a significant role of embryonic-derived EVs in the implantation [17]. For example, embryo-derived EVs could be internalized by maternal endometrial cells [18]. Moreover, peri-implantation embryos secreted specific miRNAs regulating the migration of endometrial stromal cells, which might promote the success of implantation [19]. Meanwhile, endometrium also transferred EVs to peri-implantation embryos [20]. Moreover, the signaling molecules packaged in the EVs could be transferred to embryonic cells, modulating implantation. The contents in the EVs are various, including proteins, mRNAs, and non-coding RNAs [21]. Among all these components, microRNA (miRNA) has been intensively studied, not only for its abundance in the EVs but also for the potent modulating capacity in the recipient cells [22, 23]. Studies identified several specific miRNAs in the endometrial EVs functional in the embryos. For example, miR-21 in the endometrial EVs facilitated the growth of murine fertilized embryos [24]. Moreover, EVs from secretory endometrium enhanced the adhesive capacity of pre-implantation embryos via miR-30d [20]. These studies emphasized a crucial role of miRNAs in the endometrial EVs. However, the miRNA expression and its functions in the EVs secreted by the endometria of RIF patients have not been investigated.
Therefore, in this study, we aimed to compare the miRNA profiles between endometrial EVs of RIF patients and fertile women. High-throughput sequencing was used to investigate the miRNA profiles in the endometrial EVs. The functions of differently expressed miRNAs were annotated. HTR8/SVneo cells, which are derived from the first trimester villous explant, are widely accepted as an ideal cell line to investigate the invasion capacity of embryos during implantation [25]. Therefore, we transfected the most significantly different miRNA, 6131, into HTR8/SVneo cells and investigated the role of miR-6131 on the growth and invasion of embryonic cells.
Materials and Methods
Patients
A total of 24 women were recruited in this study. All participants were under 40 years of age and had regular menstrual cycles. The clinical characteristics of the two groups are summarized in Table 1. Women who experienced consecutive three or more implantation failures after transferring good-quality embryos (both cleavage embryos and blastocysts) were included in the RIF group (n = 15). The quality of cleavage embryos and blastocysts was determined morphologically, and the detailed grading methods were described in the previously published literature [26, 27]. The good-quality cleavage embryos were defined as having the correct number of cells corresponding to the day of its development, evenness of cell division, and less than 20% fragmentation by volume. Besides, the quality of blastocysts was assessed using a previously published grading system [26], and embryos graded at 4AA, 4AB, 4BA, and 4BB were considered good-quality embryos. In this study, RIF patients asked for assisted reproductive technology therapy because of unexplained infertility or tubal factors. Meanwhile, women who conceived naturally and delivered a live birth in the previous 2 years via cesarean section without associated comorbidities were considered fertile (n = 9). Besides, these women also had their fallopian tubes ligated during the cesarean section. They intended to have another child with the help of assisted reproductive technology. Some clinicians suggested that hysteroscopy and endometrial scratching prior to IVF-ET treatments might be beneficial to the pregnancy outcomes [28, 29]. Therefore, patients who consented and intended to accept hysteroscopy and endometrial sampling were recruited in the study. The exclusion criteria were uterine abnormalities, endocrinological disorders (including diabetes, impaired glucose tolerance, insulin resistance, thyroid diseases, polycystic ovarian syndrome, hyperprolactinemia, diminished ovarian reserve, and premature ovarian failure), antiphospholipid antibody syndrome, and karyotype anomalies. Besides, the endometrial tissues were examined histologically. Women presented with endometritis or endometrial polyps were also excluded. Endometrial tissues were obtained during hysteroscopy on days 9–11 of the menstrual cycle. The endometrial samples were conserved in cold sterile phosphate-buffered saline (PBS) and transferred to the laboratory immediately. Written informed consent was obtained from all participants. This study was approved by the Institutional Review Board of Tongji Hospital (TJ-IRB20190420).
Cell Culture
Endometrial tissues were washed thrice in PBS to remove the blood. Tissues were minced and digested in 1 mg/mL IV collagenase at 37 °C for 20 min. Cell suspension was filtered through a 70-μm aperture sieve to remove the debris. During the window of implantation (WOI), both endometrial epithelial cells and stromal cells underwent hormone modulation and endometrial proliferation-differentiation switching to prepare a receptive status [30, 31]. Given the importance of epithelial cells and stromal cells during WOI, therefore, endometrial tissues were digested to endometrial cells to imitate the in vivo environment, and both cell types were included in this study. Endometrial cells were cultured in Dulbecco’s modified Eagle’s medium (DMEM)/F12 (Boster, Wuhan, China) supplemented with 10% fetal bovine serum (FBS, Sijiqing, Hangzhou, China). Since the endometrial tissues were obtained at the proliferation phase, to mimic the secretory phase, cells were modulated by 10−8 M estrogen and 10−7 M progesterone following a protocol as previously reported [32, 33]. When cells reached 80% confluence, the culture medium was discarded, and the confluent cells were washed thrice in PBS to remove the remaining FBS. Then, cells were replenished with serum-free DMEM/F12 and primed with 10−8 mol/L estrogen and 10−7 mol/L progesterone. Cells were treated for 2 days, and the conditioned medium was collected every 24 h to isolate EVs.
EV Isolation
EVs secreted by endometrial cells of RIF patients (RIF-EVs) and fertile women (FER-EVs) were isolated from the conditioned medium by ultra-centrifugation as previously described [34]. Briefly, the conditioned medium was centrifuged at 2000g for 20 min at 4 °C followed by centrifugation at 10,000g for 30 min at 4 °C to remove debris. The suspension was centrifuged at 120,000g for 80 min at 4 °C to precipitate the vesicles. The precipitant was resuspended in PBS and ultra-centrifuged again at 120,000g for 80 min to pelleted EVs. EV-enriched pellets were resuspended with 30–50 μL of PBS and stored at − 80 °C.
Western Blotting
EV or cell samples were lysed by the mixture of radioimmunoprecipitation assay (RIPA) and proteinase inhibitor cocktail (Servicebio, Wuhan, China) at 4 °C for 30 min. Then, the lysates were centrifuged at 12,000g for 20 min at 4 °C. The protein concentration of the supernatant was detected using a BCA assay Kit (Boster, Wuhan, China) according to the manufacturer’s protocols. Proteins were mixed with loading buffer and incubated in the boiling water for 10 min to prepare the loading samples. Each sample (5 μg protein) was separated by sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE) gel and transferred to polyvinylidene difluoride (PVDF) membranes. The membranes were blocked with 5% skim milk and incubated with the following primary antibodies at 4 °C overnight: CD9 (AF5139, affinity, 1:1000); calnexin (#2433, CST, 1:1000); Alix (DF9027, affinity, 1:1000); and TSG101 (A2216, Abclonal, 1:1000). Then, the membranes were incubated with secondary antibodies (anti-rabbit immunoglobulin G (IgG), horseradish peroxidase (HRP)–linked antibody, 7074S, CST, 1:1000) at 37 °C for 1 h. After that, membranes were immersed in electrochemiluminescence (ECL) substrate (abs920, Absin, Shanghai, China), and the signals were captured using a chemiluminescence imaging system (Gene Gnome XRQ; Syngene, Frederick, MD, USA).
Transmission Electronic Microscopy
An aliquot of EV sample was placed on the surface of a carbon-coated copper grid for 5 min, and the extra liquid was removed. The attached EVs were negatively stained using 2% phosphotungstic acid and air-dried. EV-containing grids were observed using a transmission electron microscope (HT7700, HITACHI, Tokyo, Japan).
Nanoparticle Tracking Analysis
The size and distribution of EVs were analyzed using ZetaView (PMX110-S, Meerbusch, Germany) according to the manufacturer’s instructions. All EV samples were diluted at a ratio of 1:500 to 1:2000 with distilled water to meet the concentration recommended by the instrument. All nanoparticle tracking analysis (NTA) measurements were performed with a ZetaView sensitivity of 70 and a shutter value of 70. Each experiment was performed in triplicate.
RNA Extraction and miRNA Sequencing
Three RIF-EV samples and three FER-EV samples were used for miRNA sequencing. Total RNAs of EVs were extracted using Qiagen exoRNeasy Maxi Kit (77,164, Qiagen, Hilden, Germany) according to the manufacturer’s instructions. The quality and purity of RNAs were determined using Nanodrop 2000 spectrophotometer, standard denaturing agarose gel electrophoresis, and RNA Labchip. miRNA library of each sample was constructed by polyadenylation, cDNA synthesis, and polymerase chain reaction (PCR) amplification. The libraries were gel-purified and quantified by quantitative real-time PCR. The quality of libraries was accessed on the Qsep100 system, and miRNA sequencing was performed on Illumina HiSeq Nova. Based on the sequencing data, differentially expressed miRNAs, defined as (log2 |fold change|) > 1 and p value < 0.05, were identified using the DESeq2 R package. Volcano plots were created on the R platform.
The total RNAs of cells were extracted using RNA-easy Isolation Reagent (R701-02-AA, Vazyme, Nanjing, China) following the manufacturer’s instructions.
Target Gene Prediction and Pathway Analysis
Target genes of miRNA were predicted by four online databases, including miRanda, TargetScan, miRDB, and Starbase. Target genes overlapped in 3 or more databases were calculated and analyzed. Gene ontology (GO) and Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment analysis of these target genes was annotated.
Quantitative Real-Time Polymerase Chain Reaction
Another twelve RIF-EV and six FER-EV samples were used to validate the differently expressed miRNAs. A total of 100 ng RNA extracted from each EV sample was converted to cDNA immediately. The synthesis of cDNA and quantitative real-time polymerase chain reaction (qRT-PCR) were performed using the All-in-one miRNA qRT-PCR Detection Kit (QP015, GeneCopoeia, Guangzhou, China) according to the manufacturer’s instructions. The relative expression of miRNA was calculated by the 2–ΔΔCt method and normalized to miR-16 as previous literature recommended [35, 36]. Each sample was detected in triplicate.
Cell Transfection
HTR8/SVneo cells were purchased from American Type Culture Collection (ATCC). HTR8/SVneo cells were suspended in DMEM/F12 supplemented with 10% FBS and plated in the 6-well plates at a density of 100,000 cells per well at 37 °C for 12 h. Then, cells were transfected with miR-6131-mimics or miR-scramble (relative control) using a PepMute transfection kit (SignaGen Laboratories, Frederick, MD, USA) following the manufacturer’s instructions. The transfected cells were then subjected to RNA extraction or functional assays.
Cell Counting Kit-8 (CCK-8) Assays
HTR8/SVneo cells were suspended in FBS-free DMEM/F12 and cultured in 96-well plates at a density of 2000 cells per well for 12 h. Then, cell viability was assessed using CCK-8 assays (Beyotime, Shanghai, China) following the manufacturer’s instructions. The absorbance was measured at 450 nm by a microplate reader (Bio-Tek Instruments, Inc., Winooski, VT, USA).
Transwell Invasion Assays
The invasive capacity of HTR8/SVneo cells was evaluated using a transwell invasion assay. Cultrex Basement Membrane Extract (BME; 3533-005-02; R&D Systems, Minneapolis, MN, USA) was diluted with serum-free DMEM/F12 at a ratio of 1:2, and every transwell insert (8-μm pores and 24-well plates) was pre-coated with 55 μL of the diluted BME. HTR8/SVneo cells were suspended in serum-free DMEM/F12 and loaded on the BME pre-coated inserts of 24-well plates at a density of 10,000 cells per insert. The lower chamber was filled with 400 μL DMEM/F12 containing 10% FBS. RIF-EVs or FER-EVs were co-cultured with HTR8/SVneo cells for 24 h at 37 °C. Following co-culture, the upper side of the inserts was erased by cotton swabs to remove the non-invaded cells. Then, the inserts were fixed in 4% paraformaldehyde and stained with crystal violet. Photos of the inserts were captured using a microscope (Axio Observer A1; Carl Zeiss) and its associated software. Finally, cell numbers were counted in five random fields.
Statistical Analysis
The clinical characteristics of all women were presented as mean ± standard deviation (SD), and statistical differences were calculated by Student’s t test using SPSS 24.0 (IBM, Chicago, IL, USA). The experimental data (including qRT-PCR, CCK-8 assays, and transwell invasion assays) were expressed as mean ± standard error of mean (SEM). Data were analyzed by the Mann-Whitney test (qRT-PCR) or Student’s t test (CCK-8 and transwell invasion assays) using GraphPad Prism 5.0 (GraphPad Software, La Jolla, CA, USA). Statistical significance was set at p < 0.05.
Results
Clinical Characteristics
A total of fifteen RIF patients and nine fertile women were recruited in this study. The clinical characteristics of the study groups are shown in Table 1. No differences were found in age, BMI, length of the menstrual cycle, and hormonal levels on day 3 of the menstrual cycle between the two groups.
Characterization of EVs
The classic protein markers of EVs, including Alix, CD9, and TSG101, were detected in the RIF-EVs and FER-EVs, and endometrial cells from RIF patients (RIF ECs) or fertile women (FER ECs) served as controls. The results showed that CD9, TSG101, and Alix were enriched in RIF-EVs and FER-EVs. Meanwhile, the endoplasmic reticulum–specific protein calnexin, which was enriched in the cell samples (RIF ECs and FER ECs), was undetectable in the EV samples (Fig. 1a). The morphology of RIF-EVs and FER-EVs (Fig. 1b) was captured using TEM. Both of them were presented as bilayered membrane vesicles.
Characterization of RIF-EVs and FER-EVs. The expression of EV protein markers was detected in the RIF-EVs and FER-EVs, and endometrial cells from RIF patients and fertile women served as controls. Western blotting showed that both RIF-EVs and FER-EVs expressed Alix, TSG101, and CD9. While the endoplasmic reticulum–specific protein calnexin, which was positive in the cells, was undetectable in the EV samples (a). The representative TEM images of RIF-EVs and FER-EVs were displayed (b). The size of EVs was evaluated using NTA. The number of EVs (c) and the mean size of EVs (d) were compared between the two groups. The representative NTA images of RIF-EVs (e) and FER-EVs (f) were shown. EVs, extracellular vesicles; RIF, recurrent implantation failure; FER, fertile; EC, endometrial cells; NTA, nanoparticle tracking analysis; TEM, transmission electronic microscopy
The size and distribution of RIF-EVs (n = 6) and FER-EVs (n = 6) were evaluated using NTA. The representative NTA images of RIF-EVs (Fig. 1e) and FER-EVs (Fig. 1f) were shown. The results showed that the number of vesicles was decreased in the RIF-EVs group; however, no significance was found (Fig. 1c). Besides, the mean size of RIF-EVs and FER-EVs was similar and around 100–200 nm (Fig. 1d).
Different miRNA Profiles in RIF-EVs and FER-EVs
Three RIF-EV samples and three FER-EV samples were used to analyze the miRNA profiles using high-throughput sequencing. All miRNAs detected in each sample were exhibited in Supplemental Table 1. After the raw data was normalized, the differential miRNAs were analyzed using DEseq2 with the criteria of p value < 0.05 and (log2 |fold change|) > 1. We found that 11 miRNAs were differently expressed in the RIF-EVs compared to those in the FER-EVs (Fig. 2a). Among the differently expressed miRNAs, ten of them were upregulated, and one of them, miR-27a-5p, was downregulated (Table 2).
The different miRNA expression profiles in RIF-EVs. The differently expressed miRNAs were visualized in a volcano plot (a). Red and blue dots represented the significantly upregulated miRNAs and downregulated miRNAs, respectively. The relative expression of miRNAs was detected in another 12 RIF-EV samples and 6 FER-EV samples (b). The relative fold change was normalized to miR-16. Data were expressed as mean ± standard error of mean (SEM). *p value < 0.05; **p value < 0.01. EVs, extracellular vesicles; RIF, recurrent implantation failure; FER, fertile
MiRNA Validation
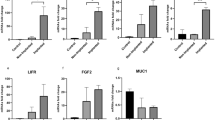
We validated the expression of miR-6131, miR-1246, miR-218-5p, and miR-433-3p in 12 RIF-EV samples and 6 FER-EV samples using qRT-PCR. Relative fold change of the differently expressed miRNAs was normalized to miR-16. As shown in Fig. 2b, miR-6131, miR-1246, and miR-218-5p were significantly increased in the RIF-EV samples, while the expression of miR-433-3p was similar between the two groups. The detailed qRT-PCR data are displayed in Table 3.
Target and Functional Analysis of the Differently Expressed miRNAs
The target genes of the 11 differently expressed miRNAs were predicted by 4 online databases (TargetScan, miRanda, miRDB, and Starbase) simultaneously. To reveal the function of these differently expressed miRNAs, GO and KEGG pathway analyses were performed on their target genes, which overlapped in at least three databases. GO terms consisted of three domains, biological process, cellular component, and molecular function. For the biological process of predicted target genes of the different miRNAs in RIF-EVs, the rhythmic process and cell-cell junction organization were the most associated (Supplemental Fig. 1). For the cell component, postsynaptic density and protein phosphatase type 2A complex were the most significantly enriched terms (Supplemental Fig. 2). As for the molecular function, transcription cofactor binding and RNA polymerase II core promoter proximal region sequencing–specific DNA binding were the most associated (Supplemental Fig. 3). KEGG pathway analysis showed the top 15 pathways that the predicted genes were involved in, and the PI3K-Akt pathway and MAPK pathway were the most associated pathways (Fig. 3).
KEGG pathway analysis of the target genes of the altered miRNAs in RIF-EVs. The target genes of the differently expressed miRNAs were predicted and their functions were annotated by KEGG pathway analysis. The top 15 pathways that were enriched were shown. The size of dots represented the number of target genes that were involved. p values of pathways were indicated by the color of dots
MiR-6131 Inhibited the Proliferation and Invasion of Embryonic Cells
After transfection, the expression of miR-6131 was significantly increased in the miR-6131-mimics group compared to the miR-scramble group (Fig. 4a). Besides, the viability and invasion were compared between two groups using CCK-8 assays and transwell invasion assays, respectively. The results showed that cellular viability was significantly decreased in the miR-6131-mimics group compared to that in the miR-scramble group (Fig. 4b). Moreover, the invasion capacity was also decreased in the miR-6131-mimics group (Fig. 4e). The representative images of invaded cells were shown (Fig. 4c, d).
miR-6131 overexpression inhibited the proliferation and invasion of HTR8/SVneo cells. HTR8/SVneo cells were transfected miR-6131-mimics or miR-scramble (served as relative control). The expression of miR-6131 was significantly increased in the miR-6131-mimics transfected cells (a). Cell viability was compared between the two groups using CCK-8 assays (b). The invasion capacity was determined using transwell invasion assays. The representative images of the two groups were displayed (c, d). Scale bar = 50 μm. The number of invaded cells was significantly decreased in the miR-6131-mimics group
Discussion
EVs are emerging as important messengers between embryos and maternal endometrium [37]. Previous literature reported that embryos secreted EVs in the culture medium [38]. Besides, embryo-derived EVs could be internalized by endometrium [18]. Meanwhile, accumulating evidence recognizes the role of endometrial EVs in the regulation of implantation [20]. Studies indicate that endometrial EVs promote the growth and implantation of embryos, and several specific molecules, especially miRNAs, have been reported to be functional during the implantation process [20, 24]. However, whether EVs secreted by the endometria of RIF patients exhibit similar miRNA repertoires that present in the normal condition has not been clarified. Therefore, in this study, we compared the miRNA expression profiles between endometrial EVs from RIF patients and fertile women.
In the current study, EVs were isolated from the conditioned medium of endometrial cells, treated with hormones to imitate the receptive status as previously documented [33]. Via modulation in vitro, the discrepancies in hormonal profiles between different individuals may be avoided. The characterization of RIF-EVs and FER-EVs was determined. Data showed that both RIF-EVs and FER-EVs were positive for classic EV markers and negative for calnexin, which confirmed the purity of EVs and excluded the possibility that cells and their debris contaminated EV samples. The size and distribution of RIF-EVs and FER-EVs were detected using NTA. Data showed that the sizes of RIF-EVs and FER-EVs were around 100–200 nm, which was in accordance with previous literature [39]. Besides, the mean size and number of vesicles were similar between RIF-EVs and FER-EVs. Moreover, the morphology of RIF-EVs and FER-EVs was visualized by TEM, and our data suggested that both types of EVs presented with the classic bilayer-membrane structure (Fig. 1b).
We found that eleven miRNAs were differently expressed in RIF-EVs; of these, ten miRNAs were upregulated, and one was downregulated. Although no previous study has identified miRNA expression in the endometrial EVs of RIF patients, several studies have reported the miRNA profiles of RIF patients’ endometria [10, 40]. By comparing our data with miRNA expression in the endometria, we found several miRNAs, including miR-6131, miR-1290, and miR-218-5p, which were highly enriched in the RIF patients’ endometria, were also upregulated in the RIF-EVs [40]. It has been postulated that EVs could function as tools to maintain cellular homeostasis by delivering the aberrantly upregulated molecules [41]. In this regard, several specific molecules, which were highly enriched in the RIF patients’ endometria, might also display an increased expression pattern in the endometrial EVs. Based on this hypothesis, the similar miRNA expression pattern in the endometria and endometrial EVs was reasonable. Our data showed that miR-1246 and miR-1290 were also enriched in the RIF-EVs. These two miRNAs have been reported to be negatively correlated with endometrial receptivity [42]. According to the abovementioned hypothesis, the increased level of miR-1246 and miR-1290 in the RIF-EVs may indicate the inadequate endometrial receptivity of RIF patients.
However, not all the miRNAs exhibited the same expression pattern in the RIF-EVs as they presented in the endometria. We speculated that two possibilities might be responsible for this discrepancy. On the one hand, women with RIF showed great discrepancies among themselves since the inclusion criteria of RIF and fertile women varied in different researches due to the lack of universal definition. Even similar studies on endometrial miRNA profiles of RIF patients did not meet a common result [10, 40, 43]. On the other hand, some miRNAs might be specific to EVs. Instead of secreting miRNAs randomly, recent evidence indicates that EVs package miRNAs following a selective mechanism [44, 45]. Though EVs are derived from endometrial cells, the miRNA expression profiles may differ from those of the originating cells [14, 41, 46]. Therefore, although some miRNAs were not overexpressed in the endometria of RIF patients, their high abundance in RIF-EVs was reasonable.
Among the upregulated miRNAs, several of them, such as miR-423-5p, miR-433-3p, and miR-409-3p, were reported to inhibit tumor cell proliferation and invasive capacity [47, 48]. It is widely accepted that trophoblast cells and cancer cells share similar biological behaviors, including proliferation, migration, and invasion [49]. In this regard, it is legitimate to hypothesize that the abovementioned miRNAs might be transferred to embryonic cells via EVs and impede the invasion and proliferation of trophoblast cells, which might be involved in the pathogenesis of implantation failure. This hypothesis has been supported by previous literature, demonstrating that the endometrial EVs of RIF patients attenuated the growth and invasion of embryos [34].
We validated the expression of several significantly dysregulated miRNAs 6131, 1246, 218-5p, and 433-3p, on a larger set of RIF-EV samples using qRT-PCR. Data showed the expressions of miR-6131, miR-218-5p, and miR-1246 were significantly increased in the RIF-EVs, which was in accordance with the sequencing results. The target genes of the altered miRNAs were predicted, and their functions were analyzed using the Go and KEGG pathway enrichment analysis. Results showed that the most relevant pathways were PI3K-Akt and MAPK pathways, which were of great importance to the survival of embryos and the implantation process [50]. Based on the above discussion, we speculated that the differently expressed miRNAs in the RIF-EVs might affect embryonic development and implantation by targeting the MAPK and PI3K-Akt pathways.
Besides, according to KEGG analysis, several other pathways, including actin cytoskeleton and focal adhesion pathways were also regulated by the differently expressed miRNAs. The cytoskeleton mainly consisted of microtubules, intermediate filaments, and microfilaments, which play enormously important roles in embryonic implantation and embryogenesis [51]. Cytoskeletal reorganization and remodeling allow the symmetric cell divisions and cellular polarization in the peri-implantation embryos [51]. In addition, focal adhesion is one of the cell communication mechanisms essential for cell motility, migration, proliferation, and survival [52]. During implantation, focal adhesion pathways play a vital role by promoting blastocyst invasion [53]. Given the importance of cytoskeleton and focal adhesion pathways in the embryos, it is legitimate to postulate that the dysregulated miRNAs might interfere with embryonic implantation. To further validate our hypothesis, we selected the most significantly different miRNA, miR-6131, and investigated its role in the embryonic cells. The results showed that the upregulation of miR-6131 significantly inhibited cellular viability and invasion, supporting our hypothesis stated above.
The mechanisms for implantation failure have been intensively studied. A number of researches have considered that embryos might be an active player and investigated their roles in the implantation [54]. They found that embryos regulated the endometrial function in the implantation via paracrine actions [18, 55]. For example, it has been reported that miRNAs identified in the embryo culture medium regulated the endometrial functions [19]. Besides, the secreted miRNAs in the embryo culture medium strongly correlated with the pregnancy outcomes [56]. Moreover, embryonic cells secreted EVs that regulated the proliferation of endometrial cells [57]. Researchers have recently recognized that endometrium is no longer a passive factor in the implantation [58]. Moreover, several literatures have proposed that endometria could sense the quality of embryos and even modulate embryonic growth [59]. Previous research found that endometria of RIF patients attenuated embryonic growth and invasion via the EV pathways [34]. Given the altered miRNAs in the RIF-EVs and their related functions, our study might provide possible mechanisms for the attenuated embryos treated by endometrial EVs of RIF patients.
However, the present study was limited by being based on in vitro experiments. Endometrial EVs isolated from the conditioned medium might exhibit subtle differences compared to those secreted in the intrauterine environment. Besides, in the current study, women who conceived naturally and had a live birth history without IVF treatments were considered relative controls. Although this inclusion criterion has been widely accepted in similar studies [60, 61], it is still limited since the endocrinological environment might be affected by the controlled ovarian stimulation during IVF treatment [62]. In this regard, naturally conceived women might present with different endocrine profiles compared to RIF patients. Therefore, further studies with better control groups will be required.
Conclusions
In the current study, we identified the different miRNA expression profiles in the endometrial EVs of RIF patients. By comparing with previous studies, we speculated that these dysregulated miRNAs might interfere with embryonic implantation by being transferred to embryonic cells via EVs, which may provide novel insights to understand the pathogenesis of RIF.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Bashiri A, Halper KI, Orvieto R. Recurrent implantation failure-update overview on etiology, diagnosis, treatment and future directions. Reprod Biol Endocrinol. 2018;16(1):121.
Hashimoto T, Koizumi M, Doshida M, Toya M, Sagara E, Oka N, et al. Efficacy of the endometrial receptivity array for repeated implantation failure in Japan: a retrospective, two-centers study. Reprod Med Biol. 2017;16(3):290–6.
Sheikhansari G, Soltani-Zangbar MS, Pourmoghadam Z, Kamrani A, Azizi R, Aghebati-Maleki L, et al. Oxidative stress, inflammatory settings, and microRNA regulation in the recurrent implantation failure patients with metabolic syndrome. Am J Reprod Immunol. 2019;82(4):e13170.
Sebastian-Leon P, Garrido N, Remohi J, Pellicer A, Diaz-Gimeno P. Asynchronous and pathological windows of implantation: two causes of recurrent implantation failure. Hum Reprod. 2018;33(4):626–35.
Koot YEM, Hviid Saxtorph M, Goddijn M, de Bever S, Eijkemans MJC, Wely MV, et al. What is the prognosis for a live birth after unexplained recurrent implantation failure following IVF/ICSI? Hum Reprod. 2019;34(10):2044–52.
Kong S, Zhou C, Bao H, Ni Z, Liu M, He B, et al. Epigenetic control of embryo-uterine crosstalk at peri-implantation. Cell Mol Life Sci. 2019;76(24):4813–28.
Achache H, Revel A. Endometrial receptivity markers, the journey to successful embryo implantation. Hum Reprod Update. 2006;12(6):731–46.
Zhao S, Qi W, Zheng J, Tian Y, Qi X, Kong D, et al. Exosomes derived from adipose mesenchymal stem cells restore functional endometrium in a rat model of intrauterine adhesions. Reprod Sci. 2020;27(6):1266–75.
Koler M, Achache H, Tsafrir A, Smith Y, Revel A, Reich R. Disrupted gene pattern in patients with repeated in vitro fertilization (IVF) failure. Hum Reprod. 2009;24(10):2541–8.
Revel A, Achache H, Stevens J, Smith Y, Reich R. MicroRNAs are associated with human embryo implantation defects. Hum Reprod. 2011;26(10):2830–40.
Bielfeld AP, Pour SJ, Poschmann G, Stuhler K, Krussel JS, Baston-Bust DM. A proteome approach reveals differences between fertile women and patients with repeated implantation failure on endometrial level−does hCG render the endometrium of RIF patients? Int J Mol Sci. 2019;20(2):425.
Ratajczak J, Wysoczynski M, Hayek F, Janowska-Wieczorek A, Ratajczak MZ. Membrane-derived microvesicles: important and underappreciated mediators of cell-to-cell communication. Leukemia. 2006;20(9):1487–95.
Zhu Z, Zhang Y, Zhang Y, Zhang H, Liu W, Zhang N, et al. Exosomes derived from human umbilical cord mesenchymal stem cells accelerate growth of VK2 vaginal epithelial cells through microRNAs in vitro. Hum Reprod. 2019;34(2):248–60.
Colombo M, Raposo G, Thery C. Biogenesis, secretion, and intercellular interactions of exosomes and other extracellular vesicles. Annu Rev Cell Dev Biol. 2014;30:255–89.
Ha D, Yang N, Nadithe V. Exosomes as therapeutic drug carriers and delivery vehicles across biological membranes: current perspectives and future challenges. Acta Pharm Sin B. 2016;6(4):287–96.
Properzi F, Logozzi M, Fais S. Exosomes: the future of biomarkers in medicine. Biomark Med. 2013;7(5):769–78.
Vyas P, Balakier H, Librach CL. Ultrastructural identification of CD9 positive extracellular vesicles released from human embryos and transported through the zona pellucida. Syst Biol Reprod Med. 2019;65(4):273–80.
Giacomini E, Vago R, Sanchez AM, Podini P, Zarovni N, Murdica V, et al. Secretome of in vitro cultured human embryos contains extracellular vesicles that are uptaken by the maternal side. Sci Rep. 2017;7(1):210. https://doi.org/10.1038/s41598-017-05549-w.
Berkhout RP, Keijser R, Repping S, Lambalk CB, Afink GB, Mastenbroek S, et al. High-quality human preimplantation embryos stimulate endometrial stromal cell migration via secretion of microRNA hsa-miR-320a. Hum Reprod. 2020;35(8):1797–807.
Vilella F, Moreno-Moya JM, Balaguer N, Grasso A, Herrero M, Martinez S, et al. Hsa-miR-30d, secreted by the human endometrium, is taken up by the pre-implantation embryo and might modify its transcriptome. Development. 2015;142(18):3210–21.
Shah R, Patel T, Freedman JE. Circulating extracellular vesicles in human disease. N Engl J Med. 2018;379(10):958–66.
Asgari S. RNA as a means of inter-species communication and manipulation: progresses and shortfalls. RNA Biol. 2017;14(4):389–90.
Griffiths-Jones S. miRBase: microRNA sequences and annotation. Curr Protoc Bioinformatics. 2010;Chapter 12:Unit 12.9.1–0.
Lv C, Yu WX, Wang Y, Yi DJ, Zeng MH, Xiao HM. MiR-21 in extracellular vesicles contributes to the growth of fertilized eggs and embryo development in mice. Biosci Rep. 2018;38(4):BSR20180036. https://doi.org/10.1042/BSR20180036.
Hannan NJ, Paiva P, Dimitriadis E, Salamonsen LA. Models for study of human embryo implantation: choice of cell lines? Biol Reprod. 2010;82(2):235–45.
Cutting R, Morroll D, Roberts SA, Pickering S, Rutherford A, Bfs, et al. Elective single embryo transfer: guidelines for practice British Fertility Society and Association of Clinical Embryologists. Hum Fertil (Camb). 2008;11(3):131–46.
Stephenson EL, Braude PR, Mason C. International community consensus standard for reporting derivation of human embryonic stem cell lines. Regen Med. 2007;2(4):349–62.
Lensen S, Venetis C, Ng EHY, Young SL, Vitagliano A, Macklon NS, et al. Should we stop offering endometrial scratching prior to in vitro fertilization? Fertil Steril. 2019;111(6):1094–101.
Barash A. Local injury to the endometrium doubles the incidence of successful pregnancies in patients undergoing in vitro fertilization. Fertil Steril. 2003;79(6):1317–22.
Haraguchi H, Saito-Fujita T, Hirota Y, Egashira M, Matsumoto L, Matsuo M, et al. MicroRNA-200a locally attenuates progesterone signaling in the cervix, preventing embryo implantation. Mol Endocrinol. 2014;28(7):1108–17.
Fukui Y, Hirota Y, Matsuo M, Gebril M, Akaeda S, Hiraoka T, et al. Uterine receptivity, embryo attachment, and embryo invasion: multistep processes in embryo implantation. Reprod Med Biol. 2019;18(3):234–40.
Greening DW, Nguyen HP, Evans J, Simpson RJ, Salamonsen LA. Modulating the endometrial epithelial proteome and secretome in preparation for pregnancy: the role of ovarian steroid and pregnancy hormones. J Proteome. 2016;144:99–112.
Greening DW, Nguyen HP, Elgass K, Simpson RJ, Salamonsen LA. Human endometrial exosomes contain hormone-specific cargo modulating trophoblast adhesive capacity: insights into endometrial-embryo interactions. Biol Reprod. 2016;94(2):38.
Liu C, Yao W, Yao J, Li L, Yang L, Zhang H, et al. Endometrial extracellular vesicles from women with recurrent implantation failure attenuate the growth and invasion of embryos. Fertil Steril. 2020;114(2):416–25.
Mo LJ, Song M, Huang QH, Guan H, Liu XD, Xie DF, et al. Exosome-packaged miR-1246 contributes to bystander DNA damage by targeting LIG4. Br J Cancer. 2018;119(4):492–502.
Occhipinti G, Giulietti M, Principato G, Piva F. The choice of endogenous controls in exosomal microRNA assessments from biofluids. Tumour Biol. 2016;37(9):11657–65.
Burnett LA, Nowak RA. Exosomes mediate embryo and maternal interactions at implantation and during pregnancy. Front Biosci. 2016;8:79–96.
Marin D, Scott RT Jr. Extracellular vesicles: a promising tool for assessment of embryonic competence. Curr Opin Obstet Gynecol. 2018;30(3):171–8.
Evans J, Rai A, Nguyen HPT, Poh QH, Elglass K, Simpson RJ, et al. In vitro human implantation model reveals a role for endometrial extracellular vesicles in embryo implantation: reprogramming the cellular and secreted proteome landscapes for bidirectional fetal-maternal communication. Proteomics. 2019:e1800423.
Shi C, Shen H, Fan LJ, Guan J, Zheng XB, Chen X, et al. Endometrial microRNA signature during the window of implantation changed in patients with repeated implantation failure. Chin Med J. 2017;130(5):566–73.
Kim KM, Abdelmohsen K, Mustapic M, Kapogiannis D, Gorospe M. RNA in extracellular vesicles. Wiley Interdiscip Rev RNA. 2017;8(4). https://doi.org/10.1002/wrna.1413.
Ponsuksili S, Tesfaye D, Schellander K, Hoelker M, Hadlich F, Schwerin M, et al. Differential expression of miRNAs and their target mRNAs in endometria prior to maternal recognition of pregnancy associates with endometrial receptivity for in vivo- and in vitro-produced bovine embryos. Biol Reprod. 2014;91(6):135.
Choi Y, Kim HR, Lim EJ, Park M, Yoon JA, Kim YS, et al. Integrative analyses of uterine transcriptome and microRNAome reveal compromised LIF-STAT3 signaling and progesterone response in the endometrium of patients with recurrent/repeated implantation failure (RIF). PLoS One. 2016;11(6):e0157696.
Villarroya-Beltri C, Gutierrez-Vazquez C, Sanchez-Cabo F, Perez-Hernandez D, Vazquez J, Martin-Cofreces N, et al. Sumoylated hnRNPA2B1 controls the sorting of miRNAs into exosomes through binding to specific motifs. Nat Commun. 2013;4:2980.
Balaguer N, Moreno I, Herrero M, Gonzalez M, Simon C, Vilella F. Heterogeneous nuclear ribonucleoprotein C1 may control miR-30d levels in endometrial exosomes affecting early embryo implantation. Mol Hum Reprod. 2018;24(8):411–25.
Valadi H, Ekstrom K, Bossios A, Sjostrand M, Lee JJ, Lotvall JO. Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat Cell Biol. 2007;9(6):654–9.
Wu L, Zhang Y, Huang Z, Gu H, Zhou K, Yin X, et al. MiR-409-3p inhibits cell proliferation and invasion of osteosarcoma by targeting zinc-finger E-box-binding Homeobox-1. Front Pharmacol. 2019;10:137.
Sun S, Wang X, Xu X, Di H, Du J, Xu B, et al. MiR-433-3p suppresses cell growth and enhances chemosensitivity by targeting CREB in human glioma. Oncotarget. 2017;8(3):5057–68.
Ferretti C, Bruni L, Dangles-Marie V, Pecking AP, Bellet D. Molecular circuits shared by placental and cancer cells, and their implications in the proliferative, invasive and migratory capacities of trophoblasts. Hum Reprod Update. 2006;13(2):121–41.
O'Neill C, Li Y, Jin XL. Survival signaling in the preimplantation embryo. Theriogenology. 2012;77(4):773–84.
Schatten H, Sun QY. Posttranslationally modified tubulins and other cytoskeletal proteins: their role in gametogenesis, oocyte maturation, fertilization and pre-implantation embryo development. Adv Exp Med Biol. 2014;759:57–87.
Saeed-Zidane M, Tesfaye D, Mohammed Shaker Y, Tholen E, Neuhoff C, Rings F, et al. Hyaluronic acid and epidermal growth factor improved the bovine embryo quality by regulating the DNA methylation and expression patterns of the focal adhesion pathway. PLoS One. 2019;14(10):e0223753.
Kaneko Y, Lecce L, Day ML, Murphy CR. Focal adhesion kinase localizes to sites of cell-to-cell contact in vivo and increases apically in rat uterine luminal epithelium and the blastocyst at the time of implantation. J Morphol. 2012;273(6):639–50.
Zohni KM, Gat I, Librach C. Recurrent implantation failure: a comprehensive review. Minerva Ginecol. 2016;68(6):653–67.
Alminana C, Bauersachs S. Extracellular vesicles: multi-signal messengers in the gametes/embryo-oviduct cross-talk. Theriogenology. 2020;150:59–69.
Rosenbluth EM, Shelton DN, Wells LM, Sparks AE, Van Voorhis BJ. Human embryos secrete microRNAs into culture media--a potential biomarker for implantation. Fertil Steril. 2014;101(5):1493–500.
Bidarimath M, Khalaj K, Kridli RT, Kan FW, Koti M, Tayade C. Extracellular vesicle mediated intercellular communication at the porcine maternal-fetal interface: a new paradigm for conceptus-endometrial cross-talk. Sci Rep. 2017;7:40476.
Bastu E, Demiral I, Gunel T, Ulgen E, Gumusoglu E, Hosseini MK, et al. Potential marker pathways in the endometrium that may cause recurrent implantation failure. Reprod Sci. 2019;26(7):879–90.
Macklon NS, Brosens JJ. The human endometrium as a sensor of embryo quality. Biol Reprod. 2014;91(4):98.
Martinez-Zamora MA, Tassies D, Reverter JC, Creus M, Casals G, Civico S, et al. Increased circulating cell-derived microparticle count is associated with recurrent implantation failure after IVF and embryo transfer. Reprod BioMed Online. 2016;33(2):168–73.
Kasvandik S, Saarma M, Kaart T, Rooda I, Velthut-Meikas A, Ehrenberg A, et al. Uterine fluid proteins for minimally invasive assessment of endometrial receptivity. J Clin Endocrinol Metab. 2020;105(1):dgz019. https://doi.org/10.1210/clinem/dgz019.
Ullah K, Rahman TU, Pan HT, Guo MX, Dong XY, Liu J, et al. Serum estradiol levels in controlled ovarian stimulation directly affect the endometrium. J Mol Endocrinol. 2017;59(2):105–19.
Funding
This study was supported by the National Natural Science Foundation of China (NSFC 81771582, NFSC 81901561, and NSFC 81701450).
Author information
Authors and Affiliations
Contributions
C.L. designed the experiments. C.L. collected the endometrial samples. C.L. and M.W. performed the experiments. C.L. wrote the manuscript, which was revised by H.Z. and C.S.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that there are no conflicts of interest.
Ethics Approval
This study was approved by the Institutional Review Board of Tongji Hospital (TJ-IRB20190420).
Consent to Participate
Not applicable.
Consent to Publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary Figure 1
(PNG 123 kb).
Supplementary Figure 2
(PNG 101 kb).
Supplementary Figure 3
(PNG 156 kb).
ESM 1
(PDF 2285 kb).
Rights and permissions
About this article
Cite this article
Liu, C., Wang, M., Zhang, H. et al. Altered microRNA Profiles of Extracellular Vesicles Secreted by Endometrial Cells from Women with Recurrent Implantation Failure. Reprod. Sci. 28, 1945–1955 (2021). https://doi.org/10.1007/s43032-020-00440-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-020-00440-y