Key summary points
Is IgA/IgG reactivity against neural tissue epitopes associated with delirium severity and activation of the immune response system?
AbstractSection FindingsIgA antibody levels against neurofilament protein, glial fibrillary acidic protein, myelin basic protein, metabotropic glutamate receptors 1 and 5, N-Methyl-D-Aspartate receptor GLU1 (NR1) and GLU2 (NR2), and heat shock protein 60 strongly predict severity of delirium and are associated with activation of the cytokine network.
AbstractSection MessagePolyreactive antibody-associated breakdown of immune tolerance, cytokine network activation and neuronal injuries are involved in delirium.
Abstract
Objectives
Activation of the immune–inflammatory response system (IRS) and a deficiency in the compensatory immunoregulatory system (CIRS), neuronal injuries, and alterations in the glutamate receptor (GlutaR), aquaporin-4 (AQP4) and heat shock protein 60 (HSP60) are involved in delirium. Increased serum levels of neurofilament protein (NFP), glial fibrillary acidic protein (GFAP) and myelin basic protein (MBP) are biomarkers of neuronal injury. This investigation delineates whether elevated IgA/IgG reactivity against those self-antigens is associated with delirium severity and IRS activation.
Methods
We measured peak Delirium Rating Scale (DRS) scores on days 2 and 3 following surgery in 59 hip fractured older adults, and IgA and IgG antibody levels against MBP, NFP, GFAP and myelin oligodendrocyte glycoprotein (MOG), metabotropic glutamate receptors mGluRs 1 and 5, N-Methyl-D-Aspartate receptor (NMDAR) GLU1 (NR1) and GLU2 (NR2), APQ4 and HSP60.
Results
The IgA antibody levels against those self-antigens, especially GFAP, MBP and HSP60, strongly predict peak DRS scores on days 2 and 3 post-surgery. IgA reactivity against NMDAR and baseline DRS scores explained 40.6% of the variance in peak DRS scores, while IgA against NMDAR, IgG against MBP and age explained 29.1% of the variance in the IRS/CIRS ratio. There was no correlation between DRS scores and IgG directed against other self-antigens.
Conclusions
Increased IgA levels against neuronal self-antigens, AQP4 and HSP60 are risk factors for delirium. Polyreactive antibody-associated breakdown of immune tolerance, IRS activation and injuries in the neuronal cytoskeleton, oligodendrocytes, astrocytes, glial cells, and myelin sheath are involved in the pathophysiology of delirium.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Delirium is a neuropsychiatric syndrome characterized by impairments in neurocognitive functions, awareness, psychomotor functions and circadian rhythms and is common in hospitalized older adults following hip fracture surgery [1, 2]. The prevalence of this condition in the post-operative period is 16.9–24% [3, 4]. A significant proportion of older adults who develop delirium are at increased risk of prolonged intensive care unit stay, increased medical comorbidities, and increased morbidity and mortality [5,6,7]. Risk factors for delirium comprise age, the aging brain, dysfunctions in neurotransmitters (serotonin, dopamine, glutamate, acetylcholine) and neuronal circuits, disorders in circadian rhythms, endocrine disorders, previous medical disorders including depression, stroke, and dementia [1, 2, 8,9,10] and duration of surgery and blood loss during surgery [2, 4, 11].
There is now evidence that delirium in older adults after surgery for hip fracture is associated with activation of immune–inflammatory pathways. Previous research has linked increases in peripheral C-reactive protein (CRP), interleukin-6 (IL-6), CXCL8 (IL-8) and tumor necrosis factor (TNF)-α to the onset of post-operative delirium [2]. These results indicate that activation of M1 macrophages and an acute phase (or inflammatory) response are associated with delirium. Another study found higher levels of IL-2, a T helper-1 (Th-1) cytokine, in delirium, along with higher levels of IL-1 and IL-6, but not higher levels of TNF-α, CXCL8, or CRP [2, 12]. Moreover, different studies showed an increased neutrophil/lymphocyte ratio (NLR) in patients with delirium [11, 13,14,15], indicating activation of immune–inflammatory pathways [2].
Recently, we established that post-surgery delirium due to hip fracture is characterized by an increased activity of the immune–inflammatory response system (IRS) and a relative decrease in the activity of the compensatory immunoregulatory system (CIRS) as indicated by an increased IRS/CIRS ratio [2]. The IRS response comprises activation of the M1 phenotype (with increased levels of IL-6, CXCL8, and TNF-α), Th-1 phenotype (based on assays of IL-2, IL-12 ad interferon-γ (IFN-γ)), as well as the Th-17 phenotype (including IL-6 and IL-17) [2, 16]. The CIRS is the aggregate of different negative immunoregulatory factors, including Th-2 (e.g., IL-4), T regulatory (Treg) (e.g., IL-10) and cytokine receptors, e.g., the IL-1 receptor antagonist (sIL-1RA) which have anti-inflammatory properties thereby preventing hyperinflammation [2, 16]. In delirium, the IRS/CIRS ratio is increased, indicating that CIRS activities (particularly IL-4 and sIL-1RA) are insufficient to regulate and attenuate the IRS [2].
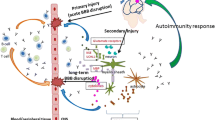
Such findings suggest that delirium following hip fracture surgery is caused by an immune–inflammatory process initiated by hip tissue trauma and the release of damage-associated molecular patterns (DAMPs), which initiate a cascade of early inflammatory mechanisms ranging from local tissue injury to inflammatory cell activation to a peripheral IRS and neuroinflammation, and that these pathways are more pronounced in subjects with lower CIRS functions [2]. Nevertheless, there are no reports on the type of DAMPS that could be involved as, for example, heat shock proteins (HSP) which may act as DAMPS or perhaps “DAMPERs” [17, 18].
Furthermore, there is some evidence that dysfunctions in the neuroaxis and neuronal injuries are risk factors for acute brain failure [1, 10]. Hepatic failure, alcohol withdrawal and ischemia, for example, can all cause glutamate excitotoxicity, resulting in acute brain failure. Anti-NMDA receptor (NMDAR) encephalitis (AMDARE) may cause psychomotor agitation, disinhibition, manic delirium and catatonia [19], while lowering glutamate excitotoxicity reduces catatonia [20]. Another risk factor for delirium is neurofilament light, an indicator of neuronal injury, which is linked to neurodegenerative processes in the brain and delirium severity independently of inflammatory biomarkers [21, 22]. In addition, plasma glial fibrillary acid protein (GFAP), which is expressed in astrocytes and is involved in cell communication, is another putative biomarker of post-surgery cognitive impairments and neuronal injury [23]. In another investigation, immunological responses to brain damage markers such as myelin basic protein (MBP) were studied in alcohol withdrawal delirium [24]. Three days following the onset of delirium, antibodies to MBP were higher in patients than in controls, according to the latter investigation. Human aquaporin 4 (AQP4) water channels are detected in endothelial cells, the blood–brain barrier (BBB) and astrocytes, and upregulation of AQP4 is related to dehydration and cerebral edema, both of which are risk factors for delirium [25, 26].
Following BBB and neuronal injuries, proteins such as AQP4, MBP and myelin oligodendrocyte glycoprotein (MOG), a transmembrane protein that regulates myelination and is expressed only by oligodendrocytes, may translocate to the bloodstream and mount immunoglobin (Ig) IgA/IgG antibody production against these antigens [24]. Moreover, polyreactive antibodies (PABs), including IgA PABs, may have homeostatic and immunoregulatory effects, but can be accompanied by breakdown of immune tolerance and PAB-related disorders [27]. In spite of this, there is no evidence that IgA/IgG reactivity against HSP60, the metabotropic glutamate receptors mGluRs 1 and 5 (GlutaR), N-Methyl-D-aspartate receptors GLU1 (NR1) and GLU2 (NR2) (NMDAR), MBP, NFP, GFAP, MOG, or AQP4 is linked with the onset or severity of delirium or the elevated IRS/CIRS ratio in delirium.
Hence, the present study was conducted to examine whether IgA/IgG to HSP60, GlutaR, NMDAR, MBP, MOG, NFP, AFAP and AQP4 are associated with the onset and severity of delirium and enhancement of the IRS (increased IRS/CIRS ratio) in older adults with hip fracture surgery. According to our a priori hypothesis, delirium severity and the IRS response during delirium are characterized by increased IgA/IgG to HSP60 and neuronal self-antigens, implying that these indicators of immune and neuronal injuries are other risk factors for delirium.
Methods
Participants
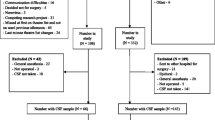
Between June 2019 and February 2020, we recruited 59 older adults with hip fractures who were admitted to the Hip Fracture Pathway Inpatient Care at King Chulalongkorn Memorial Hospital in Bangkok, Thailand. The study included patients aged 65 and older who had a low energy impact hip fracture, underwent a hip fracture operation and were postoperatively transferred to the surgery intensive care unit (SICU) or orthopedic units. Exclusion criteria included: coma, major psychiatric illness (such as psycho-organic disorders, schizophrenia, bipolar disorders), a life-time history of (neuro)-inflammatory and/or neurodegenerative disease (including Parkinson's disease, Alzheimer's disease, multiple sclerosis), (auto)immune disorders (including inflammatory bowel disease, psoriasis, rheumatoid arthritis, systemic lupus erythematosus), a high energy impact hip fracture, intracranial vascular lesions, pre-fracture dementia, metastatic fractures, traumatic brain injury from falling. Patients with previously diagnosed major depression, patients with mild stroke who were remitted one year after their acute stroke and subjects with mild cognitive impairment (MCI) could be included.
Clinical assessments
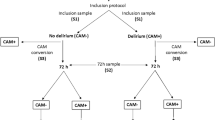
Initially, demographic and clinical data from the research participants' electronic medical records and bedside interviews were extracted. Within 24 h after surgery, the baseline cognitive status and delirium scores were assessed. The cognitive status, delirium severity and diagnosis were then re-assessed daily for three consecutive days postoperatively. The Delirium Rating Scale, Revised-98-Thai version (DRS-R-98) was used at the bedside to assess the presentation and severity of delirium on the evening of day 0 (pre-operative day) and twice a day for three days following surgery [28, 29]. The DRS-R-98-T has high sensitivity, specificity for delirium and shows adequate inter-rater reliability [28, 29]. Prior to hospitalization, we recorded the use of anticholinergic medications, benzodiazepines, opiates, and psychotropic drugs, as well as relevant peri-/post-operative clinical data such as operative time, blood loss and the need for restraint due to psychomotor agitation. Post-surgery cardiovascular complications were registered, including severe hypertensive states, atrial fibrillation, other arrhythmias and acute coronary events. The body mass index (BMI) was computed as body weight (in kg) divided by height (in meter) squared.
The study protocol was reviewed and approved by the Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand (registration number 528/61), institutional review board in accordance with the International Guideline for the Protection of Human Subjects, as required by the Declaration of Helsinki, The Belmont Report, CIOMS Guideline and International Conference on Harmonization in Good Clinical Practice (ICH-GCP). All patients and their guardians (first degree family members) signed an informed consent form.
Assays
Along with the clinical evaluation, venous blood samples were collected at 7 a.m., day 0. Blood samples were sent to the laboratory for IgA/IgG and cytokine/chemokine assays and frozen at – 80 ℃ until thawed. IgA and IgG to diverse neuronal epitopes and HSP60 were assayed employing ELISA techniques; MBP was purchased from Sigma-Aldrich® (St. Louis, MO, USA), and AQP4, MOG, NFP, GFAP, NMDA receptors GLU1 (NR1) and GLU2 (NR2) (labeled as NMDAR), metabotropic glutamate receptor or mGluRs 1 & 5 (labeled as GlutaR), and HSP60 were synthesized by Bio-Synthesis® (Lewisville, TX, USA). Alkaline phosphatase-conjugated affinity pure goat anti-human IgA (α) and anti-human IgG, FCγ, were purchased from Jackson-Immuno Research® (West Grove, PA USA). Stock solution of 1 mg/mL was prepared from all antigens. From optimal dilution of 1:100–1:200, 100 µL of each antigen was prepared in 0.01 M carbonate buffer pH 7.6, added to different wells of microtiter plates and incubated overnight at 4 °C. Plates were washed, and 200 µL of 2% bovine serum albumin (BSA) in 0.01 M PBS pH 7.4 was added to all wells in order to saturate the non-coated sites. After repeated washing, 100 µL of patients’ serum, calibrators and controls, at a dilution of 1:100 in 0.01 M PBS pH 7.4 containing 2% BSA and 0.05% Tween 20, were added to different duplicate wells and incubated for one hour at room temperature. Several wells containing all reagents, but not serum, were used for measurement of the reaction background or blank. During the incubation, sera antibodies bind strongly to antigen-coated microwells. Following washing and removal of unbound serum proteins, alkaline phosphatase-labeled anti-human IgA at dilution 1:400, or anti-human IgG at dilution 1:800 was added to different sets of microwell plates, which were then incubated again for one hour. After a repeat of the washing step, addition of substrate para-nitrophenylphosphate concentration of 1 mg/ml and incubation for 30 min at room temperature, a yellow color was developed in proportion to the concentration of antibody in the samples. Then, 60 µL of 2 N NaOH was added to stop the reaction and produce the endpoint color, which was measured by an ELISA reader at 405 nm. Antibody indices were measured using the following formula: antibody index = (OD of the sample – OD blank)/(OD of calibrator – OD of blank). We developed these antibody assays for our research by applying highly pure antigens to ELISA plates. Following completion of the many steps required for ELISA and the inclusion of calibrators, negative and positive controls, the indices were calculated. All tests were performed in duplicate, and variations between the two wells were less than 6%. All assays were performed on sera that were obtained in blind fashion. Consequently, we computed two composite scores reflecting Gluta and NMDA receptor status and neuronal injuries as Ig responses to z GlutaR + z NMDAR (dubbed GlutaNMDAR) and z MBP + z MOG + z NFP + z AFAP (dubbed neuronal). As such, we entered 4 primary input variables in the analyses, namely GlutaNMDAR, neuronal, AQP4 and HSP60.
As previously described [2], the Bio-Plex ProTM Human Chemokine Assays (Bio-Rad Laboratories, Inc. USA) were used to assay cytokines/chemokines, and samples were read with the Bio-Plex® 200 System (BioRad, Carlsbad, California, USA). The intra-assay CV for all analytes was 11.0%. We used fluorescence intensities, blank analyte subtracted, in the data analysis because fluorescence intensities are a better option than concentrations, especially when using multiple plates [2]. Because more than 20% of the measured concentrations of IL-2, IL-10, IL-12 and IL-13 were below the detection limit, these cytokines/growth factors were excluded from the analyses of single cytokines/growth factors. Nonetheless, these values were considered when creating immune profiles because detectable levels of those cytokines/growth factors may contribute to IRS/CIRS responses. The IRS and CIRS immune profiles, as well as the IRS/CIRS ratio, were the primary immune outcome variables in this study. The latter ratio was calculated as z (z IL-1 + z IL-6 + zTNF-α + z CXCL8 + z CCL3 + z sIL-RA + z IL-2 + z IL-12 + z IFN-γ + z IL-17) – z (z IL-4 + z IL-9 + zIL-13 + z IL-10) [2, 16].
Statistics
Analysis of variance (ANOVA) was used to evaluate between-group differences in scale variables, while the Chi-square test was employed to determine connections between sets of categorical variables. The key outcome measures are the quantitative DRS-R-98 scale scores at days 2 and 3 being predicted by the biomarkers measured two days earlier. Moreover, we also extracted the first principal component (PC) of both DRS measurements (dubbed DRS2 + 3) to estimate the severity of delirium symptoms averaged over days 2 and 3. Moreover, we dichotomized the DRS2 + 3 scores using a cut-off value of 0.223 yielding a group with lower PC DRS2 + 3 and one with higher scores. The association between the IgA against self-antigens (input variables) and the dichotomized DRS2 + 3 scores (output variables) was examined using automatic logistic regression analysis. We computed the Odds ratio (OR) with 95% confidence intervals (CI) as well as parameter estimates (B with SE values) and used Nagelkerke values as pseudo-R2 effect sizes. We used generalized estimating equations (GEE) to examine the associations between DRS on days 2 and 3 (or the IRS/CIRS ratio at days 1 and 2) and the IgA-against self-antigens on day 0 while allowing for the intervening effects of baseline DRS, sex, age, previous neurological diseases, BMI, duration of surgery, time to surgery, estimated blood loss during surgery and use of deliriogenic medications. Multiple associations between input and output variables were corrected using False Discovery Rate (FDR) p correction. The associations between the IgA reactivity to self-antigens and day 2 and 3 DRS scores, DRS day2 + 3 and the IRS/CIRS data on day 2 were computed using Pearson’s product moment correlation coefficients. Using the IgA/IgG values (and allowing for the effects of socio-demographic and clinical data) as input variables, multivariate regression analysis was used to predict dependent variables (DRS-R-98 scores on days 2 and 3 and DRS2 + 3), while examining R2 changes, multivariate normality (Cook's distance and leverage), multicollinearity (using tolerance and VIF), homoscedasticity (using White and modified Breusch–Pagan tests for homoscedasticity) and different residual plots. We also utilized an automatic step-up procedure with a p-to-enter of 0.05 and a p-to-remove of 0.06. As a result, only significant predictors are included in the final multiple regression model. All these regression analyses were always bootstrapped using 5000 samples, and these results are displayed if the findings did not agree. IBM SPSS Windows version 28 version 2022 was used for statistical analysis, and a significance level of 0.05 was used (two tailed tests). Given an effect size of 0.30, alpha of 0.05, power of 0.80, with five predictors, the a priori determined sample size for a multiple regression analysis is approximately 49 using G power analysis. The effect size was set at Cohen’s f2 = 0.3, namely a medium effect size corresponding to a coefficient of determination of 0.23. The sample size for a repeated measurement design ANOVA should be around n = 60 when the effect size is 0.3, alpha is 0.05 and power is 0.80, with two groups and two repeated measurements (the biomarkers).
Results
Socio-demographic data
Table 1 shows the socio-demographic, clinical and immune data in older adults divided into those with lower and higher peak DRS values. Figure 1 shows the DRS values on day 0, day 1 and peak DRS scores in both patients with high and low peak DRS values. Repeated measurement ANOVA (age and CNS disease adjusted) showed a significant effect of time × group interaction (F = 30.51, df = 1/55, p < 0.001), and time (F = 6.78, df = 1/55, p = 0.012), and significant differences in DSR scores between both groups (F = 17.75, df = 1/55, p < 0.001). People with higher peak DRS values were significantly older than the other subjects. There were no significant differences in sex, BMI, education, blood loss during surgery, time lag between fall and hospital admission and, length of stay in hospital until surgery between both groups. The total length of stay in the hospital was larger in patients with high peak DRS values. The IRS and IRS/CIRS composite scores were significantly higher in subjects with a higher DRS2 + 3 score. Electronic Supplementary File (ESF) Fig. 1 shows the measurement of the DRS score from day 0 to day 3 (adjusted for age and T2DM).
Delirium Rating Scale, Revised-98-Thai version (DRS) scores on the surgery day (day 0) and 1, 2 and 3 days after surgery for hip fracture in patients with and without increased peak (day 2 and 3) DRS scores. In the latter, there is a significant effect of time (p < 0.01), whilst no significant effect is established in the other patient group. The differences between both groups are significant on days 1 and 2 + 3 (p < 0.01)
Differences in IgA/IgG responses among DRS groups
Table 2 shows the results of logistic regression analysis with the IgA antibody levels as input variable and the high DRS2 + 3 groups as dependent variable. We found that IgA neuronal, IgA GlutaNMDAR, IgA against AQP4 and HSP60 were significantly and positively associated with the high DRS2 + 3 group. These differences remained significant after FDR p-correction. Binary logistic regression analysis showed that IgA antibody levels to MPB (p = 0.010), MOG (p = 0.014), NFP (p = 0.020), AFAP (p = 0.016), GlutaR (p = 0.023) and NMDAR (p = 0.006) were significantly higher in the group with increased peak DRS scores. These differences remained significant after FDR p-correction. Figure 2 shows the differences in the IgA values between both DRS groups. All differences were significant using ANOVA. Electronic file Fig. 1 shows the mean IgG values to the same self-antigens, indicating that not one of those measurements was significantly associated with the DRS groups.
Clustered bar graph showing the IgA antibody levels to different neuronal tissue antigens and heat shock protein 60 (HSP60) in post-surgery patients with hip fracture with and without increased peak (day 2 and 3) Delirium Rating Scale, Revised-98-Thai version (DRS) scores. All IgA values are significantly different between both groups (p < 0.01). MBP myelin basic protein, MOG myelin oligodendrocyte glycoprotein, NFP neurofilament protein, GFAP glial fibrillary acidic protein, GlutaR glutamate receptor, NMDAR N-methyl-D-aspartate receptor, IgA Neuronal z composite score based on MBP, MOG, NFP and GFAP IgA values, IgA GlutaNMDAR z composite score combining IgA responses to GlutaR and NMDAR
Associations between IgA/IgG values and the DRS scale scores
Table 2 shows the results of GEE analysis with the DRS scores on day 2 and the peak DRS scores as repeated measures and the IgA values as explanatory variables. The results show that the DRS scores from day 0 to 2–3 days later were significantly associated with the IgA levels to neuronal and GlutaNMDAR antigens HSP60, and AQP4. These differences remained significant after p correction. The solitary IgA levels to neuronal and GlutaNMDAR antigens were all significant and the strongest effects were found on HSP60 and GFAP.
Table 3 shows the correlations between the 4 primary biomarker variables and the DRS scores on day 1, peak DRS2 + 3 scores and the actual changes in peak DRS2 + 3 scores after partialling out the effects of DRS day 0 (dubbed the residualized DRS2 + 3). There were no significant associations between the IgA values and DRS scores on day 1. There were significant associations between all IgA, and these correlations remained significant after p correction.
There were no significant correlations between the IgA and IgG values and age, sex, drug status, blood loss during surgery, smoking and alcohol use (even without p correction). There were no significant correlations between the IgA and IgG values to the same self-antigen (even without p correction). We found (see Table 2) that the cardio-vascular complications of surgery were in part predicted by the combined effects of IgA and IgG reactivity levels to self-antigens (entered a z unit-based composites based on the 8 self-antigens).
Associations between immune data, DRS scores and IgA values
Table 2 shows the results of GEE analysis with the day 1 and peak DRS2 + 3 scores (repeated measurements) as dependent variables and the IgA antibody levels or IRS/CIRS data as predictors. Table 2 shows that the IRS and IRS/CIRS ratio, but not CIRS, significantly predicted the DRS scores from day 0 to days 2–3. Table 3 shows that the 4 key IgA values were all correlated with the IRS and IRS/CIRS, but not CIRS data.
Results of multiple regression analysis
Table 4 shows the results of multivariate regression analyses with the peak DRS2 + 3 values as dependent or outcome variable, and the separate IgA/IgG values as primary explanatory variables, whilst allowing for the effects of age, sex, CNS disease (MCI + previous mild stroke), length of hospital stay, T2DM, use of medications (including SSRIs) and DRS day 0 (to partial out the effects of baseline values). Regression #1 shows that 40.6% of the variance in the peak DRS2 + 3 scores was explained by the regression on IgA to NMDAR and DRS day 0, indicating that the actual changes in DRS from baseline to 2–3 days later are associated with the IgA values. Figure 3 shows the partial regression of the peak DRS2 + 3 score on IgA to NMDAR after adjusting for basal DRS values. We have rerun the same regression without the DRS day 0 values. Regression #2 shows that 36.0% of the variance in the peak DRS2 + 3 score was explained by the regression on IgA NMDAR age and CNS disease (all positively associated). Regression #3 shows that 25.9% of the variance in peak DRS2 + 3 scores was explained by age and use of selective serotonin reuptake inhibitors. The same table also shows the results of three regressions with the IRS/CIRS ratio as dependent variable. Regression #4 shows that 19.5% of the variance in the IRS/CIRS ratio on day 1 was explained by the regression on IgA MBP and CNS disease (all positively). We found (regression #5) that 29.1% of the variance in the IRS/CIRS ratio was explained by the combined effects of IgA to NMDAR, IgG to MBP and age (all positively associated). Figure 4 shows the partial regression of the IRS/CIRS ratio on IgG MBP. Regression #6 shows that 23.1% of the variance in the IRS/CIRS ratio was explained by IgG-to MBP and age combined. There was a significant association between T2DM and increased composite IgA values with a low effect size (Table 4). Length of stay in hospital was best predicted by the combined effects of CNS disease and peak DRS2 + 3 values. Post hoc G*Power analysis shows that, for all regressions shown in Table 4, except regression #7, the obtained Cohen’ f2 effect sizes range between 0.24 and 0.68 and that the obtained power ranges between 0.925 and 0.999.
Discussion
Increased IgA reactivity to neuronal antigens and HSP60 are associated with delirium
The first major finding of this study is that the IgA antibody reactivities to neuronal self-antigens, AQP4 and HSP60 strongly predict the severity of delirium symptoms a few days later. This is the first study to demonstrate such alterations in delirium, although a few publications have indicated elevated serum/plasma concentrations of NFP, GFAP and MBP [21,22,23,24]. Previously, abnormalities in AQP4 expression were linked to cerebral edema and dehydration, both of which can produce delirium [26, 27]. Other results indicated that glutamate and the NMDAR system are linked to acute brain failure, including disinhibition and manic delirium [19, 20].
Our findings support the hypothesis that neuronal damage and abnormalities in the neuroaxis, AQP4, HSP90 and the glutamate/NMDAR system may contribute to the pathogenesis of delirium. Thus, elevated GFAP, MBP and NFP levels are possible indicators of brain tissue and neuronal damage in brain trauma and neurological disorders [21,22,23]. For instance, people with traumatic brain injury, brain tumors, infections, stroke and multiple sclerosis have elevated MBP levels [30,31,32]. MBP is an essential component of myelin sheaths and plays a crucial function in myelin formation; hence, it is referred to as the “executive protein of the myelin sheath" [33]. Following brain injury, MBP dissociates from the plasma membrane and is secreted into the extracellular matrix, where it functions as an antigen to activate immune–inflammatory pathways [33]. In addition, MBP may bind to the external surface of neuronal plasma membranes, causing neurotoxicity by disrupting lipid bilayers and increasing membrane permeability. As a result, MBP may have a role in demyelination following brain injury, as well as its repercussions, which include inflammatory reactions and cell death [33].
NFP is found in the cytoplasm of neurons, where it, in conjunction with microfilaments and microtubules, forms the cytoskeleton and modulates cell shape, axonal projections and transport [34, 35]. NFPs are affected by neuronal trauma and neurodegeneration and may therefore be used as biomarkers of neuronal structural integrity and axonal fiber track damage [36]. Following brain trauma, NFP levels rise in CSF and plasma/serum and are detected in a variety of diseases, such as Alzheimer's, Huntington's, and Parkinson's disease, multiple sclerosis and toxic neuropathies [36]. In addition, the buildup of NFPs may trigger neurodegenerative processes, such as those observed in Alzheimer's and Parkinson's disease, amyotrophic lateral sclerosis and diabetic neuropathy [37].
GFAP is an intermediate filament in the cytoskeleton of astrocytes and non-myelinating Schwann cells, and its expression is elevated during reactive astrogliosis in response to various CNS traumata [38, 39]. Following brain trauma, GFAP is released into the plasma via BBB breakdown, and elevated levels may therefore serve as biomarkers for acute CNS injuries, glial cell injury and neurotoxicity [39]. Importantly, GFAP also serves as an autoantigen that provokes immune responses causing autoimmune responses in the CNS [39].
MOGs are an essential component of oligodendrocyte surface membranes and function as surface receptors, govern the integrity of oligodendrocyte microtubules and play a crucial role in the formation and maintenance of myelin sheaths [40]. Upon translocation to the peripheral blood compartment, MOG may induce autoimmune reactions. Anti-MOG antibodies are found in multiple sclerosis and optic neuritis; however, it is unclear whether elevated antibody levels are part of an immune–inflammatory response or are pathogenic [41]. AQP4 may regulate osmotic water transport through epithelial cell and astrocyte membranes [42, 43]. AQP4-mediated water transport also promotes neuroexcitation and cell growth [44]. Antibodies to AQP4 may be generated as for example in atypical multiple sclerosis and MOG antibody-associated disease (MOGAD), which is an immune–inflammatory CNS disorder characterized by demyelination [41, 45].
The GlutaR and NMDAR are involved in the pathophysiology of acute brain failure for example during alcohol withdrawal, a lack of inhibition of NMDAR that may cause delirium [46], while also increased glutamate activity is involved in the pathophysiology of delirium [47, 48]. Moreover, a significant association between delirium tremens and a functional polymorphism of the glutamatergic kainate receptor subunit GlurR7 was observed in patients with alcohol dependence [49]. Anti-glutamate receptor and anti-NMDAR antibodies are observed in serum in various conditions such as epilepsia, systemic lupus erythematosus, ataxia, encephalitis, stroke, trauma and neuropsychiatric disorders including schizophrenia [50,51,52]. Moreover, these antibodies may bind GlutaR and change glutamate-induced signaling and cause damage to brain neurons possibly leading to cell death and behavioral and cognitive impairments [50].
HSPs have protective activities against cell damage and are released into the blood under conditions of stress [53,54,55,56,57]. In several medical conditions, such as inflammatory illnesses, multiple sclerosis, trauma, cardiovascular disorders, diabetes mellitus and sepsis, elevated levels of HSP have been found to damage the endothelium cells, leading to atherosclerosis [56,57,58]. Antibodies to HSP60 are linked to an increased risk of cardiovascular disease in older persons [55].
The IgA and IgG responses are associated with IRS activation
The second major finding of this study is that the IgG to MBP and IgA to neuronal self-antigens and HSP60 were substantially linked with IRS activation (a combination of M1, Th-1, and Th-17 profiles), but not with the CIRS composite index (computed as a composite of Th-2 and Treg functions). Anti-MBP IgG antibodies have hydrolytic, proteolytic or antibody enzyme (abzyme) activity against MBP, thus leading to myelin sheath degradation and immune–inflammatory reactions [59, 60]. Moreover, IgA in general may also have pro-inflammatory effects, such as the breakdown of immune tolerance, the formation of complexed IgA or the IgA-Fc alpha Receptor I axis [27, 61,62,63]. As a result, these IgG and IgA responses may enhance the immune–inflammatory response and inflammation, thereby increasing the risk of delirium in older adults [2]. Moreover, both the IgG and IgA levels to neuronal tissue antigens and HSP60 predict cardio-vascular complications after surgery again suggesting that their pro-inflammatory properties may be involved.
Interpretation of the results
The detection of IgA to MBP, GFAP, NFP, MOG, AQP4 and GlutaR in delirium may suggest that dysfunctions or injuries in the neuronal cytoskeleton, axons, astrocytes, oligodendrocytes, glial cells and myelin sheath are associated with an increased risk of delirium. Notably, delirium was not associated with elevated IgG levels directed to the same self-epitopes. Nevertheless, natural PABs may be protective because they are a first-line defense against microbial invasion and have immunoregulatory, immune surveillance and homeostatic effects, and induce and maintain immune tolerance [27, 63, 64]. However, various conditions, such as toxic chemicals, mycotoxins, bacterial antigens, molds and food antigens, can subvert their protective mechanisms, resulting in immune and B cell tolerance breakdown and PAB-related disorders [27, 63]. Importantly, PABs may elicit inflammatory responses thereby contributing to autoimmunity [27, 63]. In animal models, administration of such PABs to the brain may cause neuronal damage [65]. Such low-affinity natural PABs may act as precursors for the more pathogenic and high affinity Abs [66]. The data imply that elevations in IgA reactivity to a variety of neuronal tissue and HSP60 are risk factors for delirium [27], which along with the effects of the trauma and surgery, and the enhancement of the IRS contribute to the development of delirium symptoms in older adults.
It was previously hypothesized that delirium is associated with CNS neuroinflammation, with increased expression of inflammatory mediators that may cause neurotoxicity and neuronal dysfunction [67]. Neuroinflammation and delirium are associated with peripheral endothelial activation and BBB breakdown because of peripheral immune activation [68,69,70,71]. Furthermore, peripherally generated autoreactive autoantibodies may cross a leaky BBB alongside T effector cells and pro-inflammatory mediators and circumvent the BBB [71]. Autoantibodies may bind to the neuronal cell surface and then internalize to bind to intracellular components, explaining why autoimmunity in the brain plays a role in many CNS diseases [72]. Interestingly, previous research has found links between serum antineuronal antibodies, a leaky BBB, brain reactive autoantibodies and neuropsychiatric symptoms [70, 71, 73].
Limitations
The present study’s findings should be interpreted in light of its limitations. First, the study was conducted on a smaller study group, and therefore, our results deserve replication. Second, the results would have been more interesting if we had also assayed the IgM responses to the same and other self-antigens, including oxidatively specific epitopes [67]. The latter have strong housekeeping and negative immunoregulatory effects [67], and their assays should shed further light on the mechanisms leading to delirium.
Conclusions
IgA responses to MBP, MOG, NFP, GFAP, GlutaR, NMDAR, APQ4 and HSP60 strongly predict peak DRS scores at 2- and 3-days post-surgery. We discovered that IgA to NMDAR and baseline DRS scores explained 40.6% of the variance in peak DRS scores on days 2 and 3, and IgA to NMDAR, IgG to MBP, and age explained 29.1% of the IRS/CIRS ratio variance. Increased IgA to neuronal tissue antigens, AQP4, and HSP60 are risk factors for delirium. PAB-associated immune tolerance breakdown, as well as dysfunctions or injuries in the neuronal cytoskeleton, oligodendrocytes, glial cells, and myelin sheath, coupled with IRS enhancement and lowered CIRS protection, can explain the onset of delirium at least partially.
Availability of data and materials
The dataset generated during and/or analyzed during the current study will be available from Prof. Dr. Michael Maes upon reasonable request and once the dataset has been fully exploited by the authors.
References
Maldonado JR (2018) Delirium pathophysiology: an updated hypothesis of the etiology of acute brain failure. Int J Geriatr Psychiatry 33(11):1428–1457. https://doi.org/10.1002/gps.4823
Thisayakorn P, Thipakorn Y, Tantavisut S, Sirivichayakul S, Maes M (2022) Delirium due to hip fracture is associated with activated immune-inflammatory pathways and a reduction in negative immunoregulatory mechanisms. BMC Psychiatry 22(1):369. https://doi.org/10.1186/s12888-022-04021-y.PMID:35641947;PMCID:PMC9158285
Yang Y, Zhao X, Dong T, Yang Z, Zhang Q, Zhang Y (2017) Risk factors for postoperative delirium following hip fracture repair in elderly patients: a systematic review and meta-analysis. Aging Clin Exp Res 29(2):115–126
Wu J, Yin Y, Jin M, Li B (2021) The risk factors for postoperative delirium in adult patients after hip fracture surgery: a systematic review and meta-analysis. Int J Geriatr Psychiatry 36(1):3–14
Arshi A, Lai WC, Chen JB, Bukata SV, Stavrakis AI, Zeegen EN (2018) Predictors and sequelae of postoperative delirium in geriatric hip fracture patients. Geriatric Orthop Surg & Rehabilit 9:2151459318814823
Brauer CA, Coca-Perraillon M, Cutler DM, Rosen AB (2009) Incidence and mortality of hip fractures in the United States. JAMA 302(14):1573–1579
Lee HB, Oldham MA, Sieber FE, Oh ES (2017) Impact of delirium after hip fracture surgery on one-year mortality in patients with or without dementia: a case of effect modification. Am J Geriatr Psychiatry 25(3):308–315
Maldonado JR (2008) Delirium in the acute care setting: characteristics, diagnosis and treatment. Critical Care Clin 24(4):657–722, vii
Hshieh TT, Inouye SK, Oh ES (2020) Delirium in the elderly. Clin Geriatr Med 36(2):183–199
Marcantonio ER, Rudolph JL, Culley D, Crosby G, Alsop D, Inouye SK (2006) Serum biomarkers for delirium. J Gerontol A Biol Sci Med Sci 61(12):1281–1286. https://doi.org/10.1093/gerona/61.12.1281
Thisayakorn P, Tangwongchai S, Tantavisut S, Thipakorn Y, Sukhanonsawat S, Wongwarawipat T, Sirivichayakul S, Maes M (2021) Immune, blood cell, and blood gas biomarkers of delirium in elderly individuals with hip fracture surgery. Dement Geriatr Cogn Disord 50(2):161–169. https://doi.org/10.1159/000517510
Dugan, K, Patel, BK, Pohlman, A, Hall, JB, Kress, JP, Wolfe, KS (2019) Prevalence of Delirium Correlates with Pro-Inflammatory Cytokines in Patients with Septic Shock. D50 CRITICAL CARE: THE METAMORPHOSIS—PAIN, SEDATION, DELIRIUM, ICU-ACQUIRED WEAKNESS, AND PALLIATIVE CARE. Am Thoracic Soc Int Conf Abstracts: Am Thoracic Soc. pp. A6671.
Egberts A, Mattace-Raso FU (2017) Increased neutrophil-lymphocyte ratio in delirium: a pilot study. Clin Interv Aging 12:1115–1121
Kotfis K, Ślozowska J, Safranow K, Szylińska A, Listewnik M (2019) The practical use of white cell inflammatory biomarkers in prediction of postoperative delirium after cardiac surgery. Brain Sci 9(11):308
He R, Wang F, Shen H, Zeng Y, Zhang L (2020) Association between increased neutrophil-to-lymphocyte ratio and postoperative delirium in elderly patients with total hip arthroplasty for hip fracture. BMC Psychiatry 20(1):496
Maes M (2018) Carvalho AF (2018) the compensatory immune-regulatory reflex system (CIRS) in depression and bipolar disorder. Mol Neurobiol 55(12):8885–8903. https://doi.org/10.1007/s12035-018-1016-x
van Eden W, Spiering R, Broere F, van der Zee R (2012) A case of mistaken identity: HSPs are no DAMPs but DAMPERs. Cell Stress Chaperones 17(3):281–292. https://doi.org/10.1007/s12192-011-0311-5
Broere F, van der Zee R, van Eden W (2011) Heat shock proteins are no DAMPs, rather “DAMPERs.” Nat Rev Immunol 11(8):565. https://doi.org/10.1038/nri2873-c1
Restrepo-Martínez M, López-Hernández JC, Espinola-Nadurille M, Bayliss L, Medina-Rioja R, Martínez-Ángeles V, Galnares-Olalde J, Téllez-Martínez JA (2021) Ramírez-Bermúdez J (2021) Psicosis autoinmune [Autoinmune psychosis]. Rev Alerg Mex 68(4):276–290. https://doi.org/10.29262/ram.v68i4.981
Bittner D (2017) NMDA Antagonists for Treatment of Catatonia with Delirium. May 21, NMDA Antagonists for Treatment of Catatonia with Delirium (hcplive.com)
Casey CP, Lindroth H, Mohanty R, Farahbakhsh Z, Ballweg T, Twadell S, Miller S, Krause B, Prabhakaran V, Blennow K, Zetterberg H, Sanders RD (2020) Postoperative delirium is associated with increased plasma neurofilament light. Brain 143(1):47–54. https://doi.org/10.1093/brain/awz354. (Erratum.In:Brain.2020Mar1;143(3):e24)
Ballweg T, White M, Parker M, Casey C, Bo A, Farahbakhsh Z, Kayser A, Blair A, Lindroth H, Pearce RA, Blennow K, Zetterberg H, Lennertz R, Sanders RD (2021) Association between plasma tau and postoperative delirium incidence and severity: a prospective observational study. Br J Anaesth 126(2):458–466. https://doi.org/10.1016/j.bja.2020.08.061
Rappold T, Laflam A, Hori D, Brown C, Brandt J, Mintz CD, Sieber F, Gottschalk A, Yenokyan G, Everett A, Hogue CW (2016) Evidence of an association between brain cellular injury and cognitive decline after non-cardiac surgery. Br J Anaesth 116(1):83–89. https://doi.org/10.1093/bja/aev415.
Volkova YV, Dubivska SS, Omelchenko-Seliukova AV, Biletskyi OV (2021) Dynamics of neurospecific autoimmune disorders and cognitive functions in patients with polytrauma and alcohol withdrawal syndrome complicated by alcohol delirium. Rep Vinnytsia Nation Med Univ. https://doi.org/10.31393/reports-vnmedical-2021-25(4)-16
Vojdani A, Mukherjee PS, Berookhim J, Kharrazian D (2015) Detection of antibodies against human and plant aquaporins in patients with multiple sclerosis. Autoimmune Dis 2015:905208. https://doi.org/10.1155/2015/905208
Sfera A, Osorio C (2014) Water for thought: is there a role for aquaporin channels in delirium? Front Psychiatry 5:57. https://doi.org/10.3389/fpsyt.2014.00057
Vojdani A, Vojdani E (2019) Food-Associate Autoimmunities. When food turns your immune system against you. Chapter 12 The role of polyreactive antibodies in health and disease. A&G Wilshire LLC, Beverly Hills, pp 1–23 (ISBN-10: 0578499770)
Pipanmekaporn T, Wongpakaran N, Mueankwan S, Dendumrongkul P, Chittawatanarat K, Khongpheng N et al (2014) Validity and reliability of the Thai version of the Confusion Assessment Method for the Intensive Care Unit (CAM-ICU). Clin Interv Aging 9:879–885
Bangphichet A (2008) Reliability and validity of the Thai version of the Delirium Rating Scale-Revised-98 (DRS-R-98).
de Vries J, Thijssen WA, Snels SE, Menovsky T, Peer NG, Lamers KJ (2001) Intraoperative values of S-100 protein, myelin basic protein, lactate, and albumin in the CSF and serum of neurosurgical patients. J Neurol Neurosurg Psychiatry 71(5):671–674. https://doi.org/10.1136/jnnp.71.5.671.
Lamers KJ, van Engelen BG, Gabreëls FJ, Hommes OR, Borm GF, Wevers RA (1995) Cerebrospinal neuron-specific enolase, S-100 and myelin basic protein in neurological disorders. Acta Neurol Scand 92(3):247–251. https://doi.org/10.1111/j.1600-0404.1995.tb01696.x
Nakagawa H, Yamada M, Kanayama T, Tsuruzono K, Miyawaki Y, Tokiyoshi K, Hagiwara Y, Hayakawa T (1994) Myelin basic protein in the cerebrospinal fluid of patients with brain tumors. Neurosurgery 34(5):825–833. https://doi.org/10.1227/00006123-199405000-00006. (Discussion 833)
Zhang J, Sun X, Zheng S, Liu X, Jin J, Ren Y, Luo J (2014) Myelin basic protein induces neuron-specific toxicity by directly damaging the neuronal plasma membrane. PLoS ONE 19(9):e108646. https://doi.org/10.1371/journal.pone.0108646.
Yuan A, Rao MV, Veeranna Nixon RA (2012) Neurofilaments at a glance. J Cell Sci 125(14):3257–3263. https://doi.org/10.1242/jcs.104729
Hoffman PN, Lasek RJ (1975) The slow component of axonal transport Identification of major structural polypeptides of the axon and their generality among mammalian neurons. J Cell Biol 66(2):351–366. https://doi.org/10.1083/jcb.66.2.351
Yuan A, Nixon RA (2021) Neurofilament proteins as biomarkers to monitor neurological diseases and the efficacy of therapies. Front Neurosci 15:689938. https://doi.org/10.3389/fnins.2021.689938.
Didonna A, Opal P (2019) The role of neurofilament aggregation in neurodegeneration: lessons from rare inherited neurological disorders. Mol Neurodegener 14(1):19. https://doi.org/10.1186/s13024-019-0318-4.
Hol EM, Pekny M (2015) Glial fibrillary acidic protein (GFAP) and the astrocyte intermediate filament system in diseases of the central nervous system. Curr Opin Cell Biol 32:121–130. https://doi.org/10.1016/j.ceb.2015.02.004
Yang Z, Wang KK (2015) Glial fibrillary acidic protein: from intermediate filament assembly and gliosis to neurobiomarker. Trends Neurosci 38(6):364–374. https://doi.org/10.1016/j.tins.2015.04.003
Ambrosius W, Michalak S, Kozubski W, Kalinowska A (2020) Myelin oligodendrocyte glycoprotein antibody-associated disease: current insights into the disease pathophysiology, diagnosis and management. Int J Mol Sci 22(1):100. https://doi.org/10.3390/ijms22010100
Peschl P, Schanda K, Zeka B, Given K, Böhm D, Ruprecht K, Saiz A, Lutterotti A, Rostásy K, Höftberger R, Berger T, Macklin W, Lassmann H, Bradl M, Bennett JL, Reindl M (2017) Human antibodies against the myelin oligodendrocyte glycoprotein can cause complement-dependent demyelination. J Neuroinflammation 14(1):208. https://doi.org/10.1186/s12974-017-0984-5.
Salman MM, Kitchen P, Halsey A, Wang MX, Törnroth-Horsefield S, Conner AC, Badaut J, Iliff JJ, Bill RM (2022) Emerging roles for dynamic aquaporin-4 subcellular relocalization in CNS water homeostasis. Brain 145(1):64–75. https://doi.org/10.1093/brain/awab311.PMID:34499128;PMCID:PMC9088512
Vella J, Zammit C, Di Giovanni G, Muscat R, Valentino M (2015) The central role of aquaporins in the pathophysiology of ischemic stroke. Front Cell Neurosci 9:108. https://doi.org/10.3389/fncel.2015.00108.
Verkman AS, Rossi A, Crane JM (2012) Live-cell imaging of aquaporin-4 supramolecular assembly and diffusion. Methods Enzymol 504:341–354. https://doi.org/10.1016/B978-0-12-391857-4.00017-3.
Redenbaugh V, Flanagan EP (2022) Monoclonal antibody therapies beyond complement for NMOSD and MOGAD. Neurotherapeutics. https://doi.org/10.1007/s13311-022-01206-x
Burns MJ (2022) What is the role of alcohol withdrawal in the pathogenesis of delirium tremens (DTs)? MedScape June 23, 2022. What is the role of alcohol withdrawal in the pathogenesis of delirium tremens (DTs)? (medscape.com)
Caplan J (2012) Delirium, sigma-1 receptors, dopamine, and glutamate. How does haloperidol keep the genie in the bottle? Crit Care Med 40(3):982–983
Flacker JM, Lipsitz LA (1999) Neural mechanisms of delirium: current hypotheses and evolving concepts. J Gerontol A Biol Sci Med Sci 54(6):B239–B246. https://doi.org/10.1093/gerona/54.6.b239. (Erratum in: J Gerontol A Biol Sci Med Sci 1999;54(7):B275)
Preuss UW, Zill P, Koller G, Bondy B, Hesselbrock V, Soyka M (2006) Ionotropic glutamate receptor gene GRIK3 SER310ALA functional polymorphism is related to delirium tremens in alcoholics. Pharmacogenomics J 6(1):34–41. https://doi.org/10.1038/sj.tpj.6500343
Levite M (2014) Glutamate receptor antibodies in neurological diseases. J Neural Transm (Vienna) 121(8):1029–1075. https://doi.org/10.1007/s00702-014-1193-3
Hanly JG, Robichaud J, Fisk JD (2006) Anti-NR2 glutamate receptor antibodies and cognitive function in systemic lupus erythematosus. J Rheumatol 33(8):1553–1558
Coesmans M, Smitt PA, Linden DJ, Shigemoto R, Hirano T, Yamakawa Y, van Alphen AM, Luo C, van der Geest JN, Kros JM, Gaillard CA, Frens MA, de Zeeuw CI (2003) Mechanisms underlying cerebellar motor deficits due to mGluR1-autoantibodies. Ann Neurol 53(3):325–336. https://doi.org/10.1002/ana.10451
Delogu G, Signore M, Mechelli A, Famularo G (2002) Heat shock proteins and their role in heart injury. Curr Opin Crit Care 8(5):411–416. https://doi.org/10.1097/00075198-200210000-00007
Niizeki T, Takeishi Y, Watanabe T, Nitobe J, Miyashita T, Miyamoto T, Kitahara T, Suzuki S, Sasaki T, Bilim O, Ishino M, Kubota I (2008) Relation of serum heat shock protein 60 level to severity and prognosis in chronic heart failure secondary to ischemic or idiopathic dilated cardiomyopathy. Am J Cardiol 102(5):606–610. https://doi.org/10.1016/j.amjcard.2008.04.030
Martine P, Rébé C (2019) Heat shock proteins and inflammasomes. Int J Mol Sci 20(18):4508. https://doi.org/10.3390/ijms20184508
de Lima Filho JB, Freire L, Nahas EAP, Orsatti FL, Orsatti CL (2020) Heat shock protein 60 antibodies are associated with a risk factor for cardiovascular disease in bedridden elderly patients. Front Mol Biosci 7:103. https://doi.org/10.3389/fmolb.2020.00103.
Shamaei-Tousi A, Stephens JW, Bin R, Cooper JA, Steptoe A, Coates AR, Henderson B, Humphries SE (2006) Association between plasma levels of heat shock protein 60 and cardiovascular disease in patients with diabetes mellitus. Eur Heart J 27(13):1565–1570. https://doi.org/10.1093/eurheartj/ehl081
Canul-Euan AA, Zúñiga-González G, Palacios-Luna JE, Maida-Claros R, Díaz NF, Saltigeral-Tigeral P, Karina García-May P, Díaz-Ruiz O, Flores-Herrera H (2021) Increased levels of plasma extracellular heat-shock proteins 60 and 70 kDa characterized early-onset neonatal sepsis. Front Pediatr 9:740274. https://doi.org/10.3389/fped.2021.740274
Ponomarenko NA, Durova OM, Vorobiev II, Belogurov AA, Telegin GB, Suchkov SV, Misikov VK, Morse HC 3rd, Gabibov AG (2006) Catalytic activity of autoantibodies toward myelin basic protein correlates with the scores on the multiple sclerosis expanded disability status scale. Immunol Lett 103(1):45–50. https://doi.org/10.1016/j.imlet.2005.10.006
Warren KG, Catz I (1999) An extensive search for autoantibodies to myelin basic protein in cerebrospinal fluid of non-multiple-sclerosis patients: implications for the pathogenesis of multiple sclerosis. Eur Neurol 42(2):95–104. https://doi.org/10.1159/000069418
Hansen IS, Baeten DLP, den Dunnen J (2019) The inflammatory function of human IgA. Cell Mol Life Sci 76(6):1041–1055. https://doi.org/10.1007/s00018-018-2976-8
van Gool MMJ, van Egmond M (2021) IgA and FcαRI versatile players in homeostasis, infection, and autoimmunity. Immunotargets Ther 9:351–372. https://doi.org/10.2147/ITT.S266242
Dimitrov JD, Planchais C, Roumenina LT, Vassilev TL, Kaveri SV, Lacroix-Desmazes S (2013) Antibody polyreactivity in health and disease: statu variabilis. J Immunol 191(3):993–999. https://doi.org/10.4049/jimmunol.1300880
Reyneveld GI, Savelkoul HFJ, Parmentier HK (2020) Current understanding of natural antibodies and exploring the possibilities of modulation using veterinary models. A review. Front Immunol 11:2139. https://doi.org/10.3389/fimmu.2020.02139.
Zhang J, Jacobi AM, Wang T, Berlin R, Volpe BT, Diamond B (2009) Polyreactive autoantibodies in systemic lupus erythematosus have pathogenic potential. J Autoimmun 33(3–4):270–274. https://doi.org/10.1016/j.jaut.2009.03.011
Zhou ZH, Tzioufas AG, Notkins AL (2007) Properties and function of polyreactive antibodies and polyreactive antigen-binding B cells. J Autoimmun 29(4):219–228. https://doi.org/10.1016/j.jaut.2007.07.015
Cerejeira J, Firmino H, Vaz-Serra A, Mukaetova-Ladinska EB (2010) The neuroinflammatory hypothesis of delirium. Acta Neuropathol 119(6):737–754. https://doi.org/10.1007/s00401-010-0674-1
Hughes CG, Pandharipande PP, Thompson JL, Chandrasekhar R, Ware LB, Ely EW, Girard TD (2016) Endothelial activation and blood-brain barrier injury as risk factors for delirium in critically ill patients. Crit Care Med 44(9):e809–e817. https://doi.org/10.1097/CCM.0000000000001739.
Taylor J, Parker M, Casey CP, Tanabe S, Kunkel D, Rivera C, Zetterberg H, Blennow K, Pearce RA, Lennertz RC, Sanders RD (2022) Postoperative delirium and changes in the blood-brain barrier, neuroinflammation, and cerebrospinal fluid lactate: a prospective cohort study. Br J Anaesth 129(2):219–230. https://doi.org/10.1016/j.bja.2022.01.005
Zameer A, Hoffman SA (2001) Immunoglobulin binding to brain in autoimmune mice. J Neuroimmunol 120(1–2):10–18. https://doi.org/10.1016/s0165-5728(01)00412-x
Platt MP, Agalliu D, Cutforth T (2017) Hello from the other side: how autoantibodies circumvent the blood-brain barrier in autoimmune encephalitis. Front Immunol 8:442. https://doi.org/10.3389/fimmu.2017.00442.
Kapadia M, Sakic B (2011) Autoimmune and inflammatory mechanisms of CNS damage. Prog Neurobiol 95(3):301–333. https://doi.org/10.1016/j.pneurobio.2011.08.008
Maes M, Sirivichayakul S, Kanchanatawan B, Vodjani A (2019) Breakdown of the paracellular tight and adherens junctions in the gut and blood brain barrier and damage to the vascular barrier in patients with deficit schizophrenia. Neurotox Res 36(2):306–322. https://doi.org/10.1007/s12640-019-00054-6
Morris G, Puri BK, Olive L, Carvalho AF, Berk M, Maes M (2019) Emerging role of innate B1 cells in the pathophysiology of autoimmune and neuroimmune diseases: association with inflammation, oxidative and nitrosative stress and autoimmune responses. Pharmacol Res 148:104408. https://doi.org/10.1016/j.phrs.2019.104408
Acknowledgements
We gratefully acknowledge the help of all psychiatry/orthopedic/anesthesiology nursing staff and residents involved in the execution of this study.
Funding
This study was supported by a Ratchadapisek Sompoch Endowment Fund of the Faculty of Medicine, Chulalongkorn University (RA62/014).
Author information
Authors and Affiliations
Contributions
PT: designed the conception, planned, and collected the data, provided a delirium care, interpreted the results, drafted and revised the manuscript. YT: planned and collected the data, provided a delirium care, revised the manuscript. ST: planned and collected the data, provided an orthopedic care, revised the manuscript. SS: prepared, analyzed, and interpreted the laboratory specimens, revised the manuscript. MM: designed the conception, analyzed, and interpreted the data, drafted and revised the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval and consent to participate
Approval for the study was obtained from the Institutional Review Board of the Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand (registration number 528/61), in compliance with the International Guideline for Human Research protection, as required by the Declaration of Helsinki, conducted according to Thai and international ethics and privacy laws. Written informed consent was obtained before the study from the patients or their guardians (first-degree family members).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Maes, M., Thisayakorn, P., Thipakorn, Y. et al. Reactivity to neural tissue epitopes, aquaporin 4 and heat shock protein 60 is associated with activated immune–inflammatory pathways and the onset of delirium following hip fracture surgery. Eur Geriatr Med 14, 99–112 (2023). https://doi.org/10.1007/s41999-022-00729-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-022-00729-y