Abstract
Aims
Chronic kidney disease (CKD) is a common complication after liver transplantation (LT). The etiology of CKD is broad and may only be assessed accurately by renal histology. The current study aimed to analyze the safety of renal biopsy in daily clinical practice as well as its usefulness regarding management of CKD after LT.
Methods
We performed a retrospective analysis of clinical data and renal biopsies obtained from patients with severe renal impairment (overt proteinuria, progressive deterioration of renal function) after LT with respect to safety, etiology of renal disease, and therapeutic consequences.
Results
Renal biopsies were obtained from 14 patients at median (minimum–maximum) 3 (0.2–12) years after LT. No major complications associated with renal biopsy were observed. Histomorphological alterations were varied (nephrosclerosis, n = 5; IgA-glomerulonephritis, n = 4; tenofovir-associated nephropathy, membranoproliferative glomerulonephritis type 1, membranous glomerulonephritis, amyloid A amyloidosis, and calcineurin inhibitor nephropathy, n = 1, respectively). The diagnosis of specific renal diseases other than calcineurin-inhibitor nephrotoxicity facilitated specific treaments and avoided unnecessary modification of immunosuppression in the majority of patients.
Conclusions
Renal biopsy in patients with CKD after LT seems safe and may offer specific therapeutic options. Furthermore, unnecessary changes of immunosuppression can be avoided in a considerable number of patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic kidney disease (CKD) is common after liver transplantation (LT) and the mortality rate correlates with severity of renal impairment [1,2,3]. Early renal dysfunction after LT has been associated with the use of the calcineurin inhibitors (CNI) cyclosporine A (CsA) and tacrolimus (TAC) [4]. Notably, all approved immunosuppression regimens to prevent liver graft rejection contain either CsA or TAC. Nevertheless, the etiology of CKD after LT may be multifactorial and even independent from CNI nephrotoxicity as independent risk factors for CKD such as arterial hypertension and diabetes mellitus are common after LT [3, 5, 6]. Remarkably, the majority of studies addressing therapeutic interventions in patients with renal failure after LT focus on modification of immunosuppression without prior histological proof of CNI nephrotoxicity [7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26]. The sum of patients investigated in these studies, mainly without renal biopsy, markedly outnumbers the reported histological-based analyses of renal disease after LT [27,28,29,30].
Although improvement of kidney function in patients with CKD after LT has been observed following CNI withdrawal or reduction in general, the effect was of only doubtful clinical significance in some studies, and was more pronounced the earlier the immunosuppression was commenced after LT modification [13,14,15,16,17,18,19,20,21,22,23,24,25]. On the other hand, low exposure to CNI as well as conversion from a CNI to a mammalian target of rapamycin (mTOR) inhibitor has recently been associated with antibody-mediated liver graft rejection [31]. Therefore, modification of immunosuppression without histological confirmation of CNI nephropathy could harm the patient and, moreover, the existence of concurrent specific renal diseases and thereby the chance to administer specific treatment options may be missed. Thus, renal biopsy could guide further therapeutic approaches with regard to preservation or improvement of renal function, but it is performed only infrequently both in daily clinical practice and clinical studies, presumably because of its invasive nature and uncertainty of the clinical consequences.
Exact determination of CKD may be of special importance in patients with rapid and severe deterioration of renal function, and renal biopsy may be justified particularly under these conditions. The aim of the present study was therefore to focus on patients with progressive and severe CKD after LT and evaluate whether renal biopsy in liver graft recipients is a safe procedure in daily clinical practice and whether the histological results are of importance for further treatment of renal disease.
Methods
Study design
Renal biopsy in general is indicated in patients with clinically significant renal disease and presumable therapeutic consequences [32]. The present retrospective study was performed between 2011 and 2015 in liver graft recipients attending the LT follow-up clinic at a German tertiary center. Renal function was assessed by use of the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) formula in ml/min/1.73 m2 [33]. According to our center’s protocol, all patients with new onset of overt proteinuria or progressive renal failure defined by a persistent (at least 3 months) decline of estimated glomerular filtration rate (eGFR) of at least 30 ml/min/1.73 m2, or both, were considered for a renal biopsy.
Study approval was obtained by the local Ethics Committees for Medical Research in accordance with the 1975 Declaration of Helsinki. Main exclusion criteria were prior kidney transplantation or age < 18 years. Medical history, clinical, and biochemical data as well as immunosuppressant trough levels were assessed at the time of renal biopsy, as well as 6 and 12 months after renal biopsy. Concomittant risk factors for CKD such as arterial hypertension, diabetes mellitus, dyslipoproteinemia, and nicotine consumption were recorded. All patients received optimized treatment of comorbidities with a known influence on renal function, e.g. arterial hypertension, diabetes mellitus, and dyslipidemia, independently of the renal biopsy according to current international guidelines [34,35,36].
Immunosuppression
The standard immunosuppression protocol at our center during the study phase included intraoperative induction therapy with the interleukin (IL)-2 receptor antagonist basiliximab and 500 mg methylprednisolone i.v. A second dosage of basiliximab was applied on day 4 after LT. Initial immunosuppression consisted of mycophenolate mofetil at a daily dose of 2 g, and CNIs were not introduced before day 3 after LT. All but one patient included in the current study were transplanted at our center. Maintenance immunosuppression contained CNI alone or in combination with mycophenolate mofetil and occationally prednisolone. An mTor containing regime was possible to be chosen in individual cases.
Renal biopsy
Preparation of renal biopsy included physical and ultrasound examination, a biochemical profile, blood and platelet count, prothrombin time, partial thromboplastin time and in-vitro bleeding time. Per protocol renal biopsy was done only as an inpatient procedure. Percutaneous renal biopsy itself was performed in the prone position under local anesthesia with a 14 gauge spring-loaded needle (CR Bard GmbH, Karlsruhe, Germany) under real-time ultrasonic guidance into the lower pole of the left kidney. Post-biopsy patients had to remain at bed rest overnight. To detect bleeding and other complications, vital functions such as heart rhythm and blood pressure were monitored for at least 24 h. Additionally, urine analysis, complete blood count as well as ultrasound examinations were obtained at least 4 and 16 h post intervention.
Histological assessment of kidney biopsies
Histology of kidney biopsies was read by specialized pathologists as described previously [37]. All renal biopsy specimens were submitted for diagnostic purposes (light microscopy, immune histology, electron microscopy) and processed using a standardized routine protocol. For most renal diseases and classification schemes, an adequate biopsy has to contain at least ten glomeruli. In the current study, adequacy of sample size was determined by the specialized renal pathologist. Briefly, formalin-fixed and paraffin-embedded kidney biopsy specimens were sectioned into 2 µm thick paraffin sections with at least 8 serial sections stained either by periodic acid-Schiff (PAS) or hematoxylin–eosin (HE) stainings. Additionally, a Congo red staining as well as immunohistochemical stainings with antisera specific for immunoglobulin (Ig)A (1:150,000), IgG (1:100,000), IgM (1:75,000), C1q (1:75,000) and C3c (1:75,000, all polyclonal rabbit antisera, Dako Cytomation, Hamburg, Germany) were performed in all cases. In Congo red positive cases, additional stainings with antibodies specific for the kappa (1:50,000) and lambda (1:100,000) light chains (both polyclonal rabbit antisera, Dako) and for amyloid A (1:500, monoclonal, mouse, clone mc-1, Dako) for differentiation of the amyloid deposits were initiated.
Biopsy serial sections were evaluated according to standard nephropathological protocols, which includes (1) analysis of percentage of cortical and medullary tissue, (2) quantitative and qualitative glomeruli assessment with special respect to globally or segmentally sclerosis, and (3) reporting of any intra- or extracapillary proliferation. Within the tubulointerstitium acute or chronic damage, interstitial fibrosis and inflammation were reported and quantified if possible. Intrarenal arteries and arterioles were evaluated in terms of wall thickening, hyalinosis, inflammation as well as acute or chronic thrombosis. In electron micropscopy, glomerular ultrastructure was analyzed with respect to changes of the glomerular basement membrane, podocyte foot process effacement, endothelial cell damage, and osmiophilic or fibrillary deposits.
A special focus was placed on signs of acute and chronic CNI nephrotoxicity. Acute CNI effects are considered mostly hemodynamically-mediated and may comprise any morphological lesion. The corresponding histopathological lesions comprise acute tubular damage with characteristic isovolumetric vacuolisation of the cytoplasm of tubular epithelial cells being the most common morphological feature. In contrast, chronic CNI-nephrotoxicity comprises patchy or striped tubular atrophy and fibrosis, tubular microcalcification and most typically a nodular type of arteriolar hyalinosis [38].
Statistical analyses
Clinical and biochemical characteristics of patients were expressed as mean ± standard deviation (SD) or median [minimum (min.)–maximum (max.)] as appropriate. Correlations between two variables were calculated by the Friedman test. Unless indicated otherwise, all tests were two tailed and p values < 0.05 were considered significant.
Results
Patients’ characteristics
Overall, 102/221 (46%) liver graft recipients attending the post LT surveillance program had impaired renal function. Criteria for renal biopsy were fulfilled in 14 patients within the respective study period. The median (range) age at time of renal biopsy was 53 (32–63) years, and renal biopsy was performed at a median (range) interval after LT of 3 (0.2–12) years. Detailed patients’ characteristics at renal biopsy are reported in Table 1. At the time of renal biopsy, 12/14 patients were receiving a CNI-based immunosuppression protocol, while the other two patients were on an mTOR-inhibitor and a mycophenolate mofetil mono-immunosuppression regimen, respectively. Co-medication with mycophenolate mofetil or low dose prednisolone was administered in ten and three patients, respectively. No patient received a CNI/mTOR inhibitor combination protocol at the time point of renal biopsy (Table 2).
Assessment of risk factors and histological changes of kidney disease
Detailed information on risk factors of renal disease, immunosuppression, and histological assessment of renal biopsies is presented in Table 2. In particular, diabetes mellitus and arterial hypertension were present in 6/14 and 11/14 patients, respectively. Pre- and post-transplant dialysis was documented in 2 and 5 patients. Histological assessment of CKD showed a broad spectrum of underlying diseases with nephrosclerosis (n = 5) and mesangioproliferative IgA-glomerulonephritis (n = 4) being the most frequent forms. Tubular atrophy and interstitial fibrosis was present in all patients ranging from 5 to 70%. Of note, CNI pathognomonic changes, such as isometric vacuolization of proximal tubular cells, arteriolar hyalinosis with medial/peripheral nodules and striped pattern of tubular atrophy/interstitial fibrosis, were found in only 1 of 14 patients (Table 2).
Assessment of complications after renal biopsy, therapeutic consequences of kidney histology, and clinical course
Renal biopsy was a safe procedure in our cohort as no major complication was observed. A peri-renal hematoma without subsequent interventions was documented in 4/14 (29%) patients by routine ultrasound 1 day after biopsy, whereas a complete uncomplicated course was observed in the remaining 10 patients.
In one patient with histological features of CNI nephrotoxicity, immunosuppression was changed from TAC to everolimus (EVR). However, renal function did not improve significantly, and TAC was reinitiated because of planned surgery. Of note, this patient received hemodialysis peri-transplant, and renal biopsy also demonstrated signs of diabetic nephropathy as the predominant underlying chronic renal disease. In the remaining 13 patients, modification of immunosuppression was not done in the knowledge of respective histological changes, whereas antiviral medication to target hepatitis B virus was changed in one patient with tenofovir nephropathy. In the remaining patients, CNI-independent nephropathy was treated according to specific nephrologic recommendations.
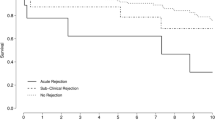
To further determine dynamics of renal function, eGFR was assessed 6 and 12 months after renal biopsy. Follow-up data were available in 13/14 patients after 24 weeks and after median (range) 361 (303–381) days, respectively. Dynamics of eGFR estimated by CKD-EPI formula are given in Fig. 1. In detail, mean ± SD eGFR was 39.49 ± 16.88 ml/min/1.73 m2 at renal biopsy, and 38.17 ± 15.16 ml/min/1.73 m2 12 months thereafter (p = n.s.), while mean ± SD TAC trough levels were comparable between time point of biopsy (5.26 ± 1.03 ng/ml) and follow-up after 12 months (4.81 ± 2.08, p = n.s.).
Fig. 1 shows renal function at liver transplantation in comparison to renal function at time point of kidney biopsy and follow-up at 6 and 12 months thereafter, given as mean ± SD eGFR assessed by the CKD-EPI formula
Discussion
Determination of correct diagnosis and optimal treatment of renal impairment after LT is challenging. The etiological spectrum is broad and the clinical course ranges from mild and stable CKD to rapid deterioration of renal function [2, 3]. Although renal biopsy is considered indicated in patients with clinically significant renal disease and presumable therapeutic consequences based on the histological finding in general [32], data about histological changes in patients with CKD after LT are scarce [27,28,29,30]. In this study, we analyzed whether renal biopsy is safe after LT under daily clinical conditions and justified by the therapeutic consequences.
Our current data strongly encourage to perform kidney biopsies more frequently in patients with CKD after LT. The procedure was found to be safe and histological assessment revealed etiologies of CKD which would not have been established otherwise. Thus, results of renal biopsies enabled specific nephrologic treatment and helped to avoid unnecessary modification of immunosuppression. According to current data, kidney biopsy is a safe procedure [39]. In line with this study, we observed no severe complications in our case series of renal biopsy in liver transplant recipients. Thus, we suggest that renal biopsy may be considered more often in liver graft recipients developing renal impairment, including patients with preserved renal function and before development of proteinuria. Moreover, histologically-proven CNI nephrotoxicity was rare in our study, although the majority of patients received a CNI-based immunosuppression. In general, CNI-associated histomorphological changes are considered irreversible despite occasional reports of reversibility [40, 41]. However, it cannot be excluded that CNI nephrotoxicity contributed at least in part to the nephrosclerotic alterations observed in our study. Bearing this in mind, our data, although based on a limited number of patients, nevertheless indicate that CNI nephrotoxicity may not play the etiologic key role for CKD in long-term liver graft recipients as suggested by the high numbers of studies investigating reduction of CNI exposure to improve renal function after LT [13,14,15,16,17,18,19,20,21,22,23,24,25]. As low exposure to CNI has been associated with rejection and an unfavorable course after LT [31], CNI reduction or withdrawal without histologically-proven CNI nephropathy may not be recommended in patients with CKD after LT in general.
The results of our study must not be misinterpreted as implying that CNI nephrotoxicity is to be neglected as an important cause of CKD after LT. Of note, improvement or preservation of renal function has been shown in studies investigating CNI minimizing or avoiding strategies in the early period after LT [8,9,10,11,12, 26]. Histologically, CNI nephrotoxicity has been attributed to putative irreversible renal vessels injury, tubular atrophy and interstitial fibrosis [38]. However, the CNI target trough level in current immunosuppression regimens after LT is lower even in the first year after LT in comparison to the time shortly after introducing CNI in transplantation medicine, and this may have also influenced severity and verifiability of CNI nephrotoxicity over a longer time period. It has to be stressed that studies investigating modification of immunosuppression in patients with established CKD after LT predominantly did not provide histological data to characterize CKD [7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26]. Clinically significant improvement of renal function after CNI reduction or withdrawal was not shown convincing and conclusive in all the respective studies in liver graft recipients with established CKD [7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26]. This could be explained by irreversible CNI-associated renal damage as well as concurrent etiologies. Given the low percentage of histologically-proven CNI in patients with CKD after LT in our and other studies [27,28,29,30], it seems reasonable that further interventional trials on this topic may use renal biopsy as an inclusion criterion.
Finally, it should be stressed that the results of our study must be taken with caution. The number of patients with renal biopsy was limited. This, however, is a common problem in studies investigating renal biopsy after LT [27,28,29,30]. Lee et al., for example, reported histological data in 10 of 544 liver graft recipients with CKD. Nevertheless, our results are reliable as the histological patterns found in our study are in line even with other studies investigating histologic alterations in patients with CKD after LT [27,28,29,30]. Furthermore, the spectrum of underlying renal diseases observed in the current study may have been influenced by the biopsy selection criteria. Although the criteria used seem reasonable because in these constellations the putative consequences can be considered to outweigh putative risks of the invasive procedure, it is likely that the results of the biopsies are not representive of the complete etiological spectrum of CKD after LT.
In conclusion, the findings of the current study indicate that renal biopsy after LT is safe and that the etiology of CKD after LT is varied including rare renal diseases. Without renal biopsy, the appropriate specific nephrological treatment could be missed. Thus, we suggest that patients with renal impairment after LT should be offered a thorough nephrological diagnostic workup including renal biopsy to explore other diagnoses than CNI toxicity with potential for specific treatment options.
Abbreviations
- ALT:
-
Alanine transaminase
- AST:
-
Aspartate transaminase
- CKD-EPI:
-
Chronic Kidney Disease Epidemiology Collaboration
- CKD:
-
Chronic kidney disease
- CMV:
-
Cytomegalovirus
- CNI:
-
Calcineurin inhibitor(s)
- CsA:
-
Cyclosporine A
- DN:
-
Diabetic nephropathy
- eGFR:
-
Estimated glomerular filtration rate
- HBV:
-
Hepatitis B virus
- HCC:
-
Hepatocellular carcinoma
- HCV:
-
Hepatitis C virus
- Maximum:
-
Max.
- MELD:
-
Model of end stage liver disease
- Minimum:
-
Min.
- MMF:
-
Mycophenolate mofetil
- mTOR:
-
Mechanistic target of rapamycine
- LT:
-
Liver transplantation
- SIR:
-
Sirolimus
- SD:
-
Standard deviation
- sec:
-
Seconds
- TAC:
-
Tacrolimus
- ULN:
-
Upper limit of normal
References
Ojo AO, Held PJ, Port FK, Wolfe RA, Leichtman AB, Young EW et al (2003) Chronic renal failure after transplantation of a nonrenal organ. N Engl J Med 349(10):931–940
Allen AM, Kim WR, Therneau TM, Larson JJ, Heimbach JK, Rule AD (2014) Chronic kidney disease and associated mortality after liver transplantation—a time-dependent analysis using measured glomerular filtration rate. J Hepatol 61(2):286–292
Moreno JM, Cuervas-Mons V, Rubio E, Pons F, Herreros de TA, Turrión VS et al (2003) Chronic renal dysfunction after liver transplantation in adult patients: prevalence, risk factors, and impact on mortality. Transpl Proc 35(5):1907–1908
Ziolkowski J, Paczek L, Senatorski G, Niewczas M, Oldakowska-Jedynak U, Wyzgal J et al (2003) Renal function after liver transplantation: calcineurin inhibitor nephrotoxicity. Transpl Proc 35(6):2307–2309
Kim J-Y, Akalin E, Dikman S, Gagliardi R, Schiano T, Bromberg J et al (2010) The variable pathology of kidney disease after liver transplantation. Transplantation 89(2):215–221
Giusto M, Berenguer M, Merkel C, Aguilera V, Rubin A, Ginanni Corradini S et al (2013) Chronic kidney disease after liver transplantation: pretransplantation risk factors and predictors during follow-up. Transplantation 95(9):1148–1153
Boudjema K, Camus C, Saliba F, Calmus Y, Salamé E, Pageaux G et al (2011) Reduced-dose tacrolimus with mycophenolate mofetil vs. standard-dose tacrolimus in liver transplantation: a randomized study. Am J Transpl 11(5):965–976
Neuberger JM, Mamelok RD, Neuhaus P, Pirenne J, Samuel D, Isoniemi H et al (2009) Delayed introduction of reduced-dose tacrolimus, and renal function in liver transplantation: the “ReSpECT” study. Am J Transpl 9(2):327–336
TruneČka P, Klempnauer J, Bechstein WO, Pirenne J, Friman S, Zhao A et al (2015) Renal Function in de novo liver transplant recipients receiving different prolonged-release tacrolimus regimens—the DIAMOND study. Am J Transpl 15(7):1843–1845
De Simone P, Nevens F, De Carlis L, Metselaar HJ, Beckebaum S, Saliba F et al (2012) Everolimus with reduced tacrolimus improves renal function in de novo liver transplant recipients: a randomized controlled trial. Am J Transpl 12(11):3008–3020
Sterneck M, Kaiser GM, Heyne N, Richter N, Rauchfuss F, Pascher A et al (2014) Everolimus and early calcineurin inhibitor withdrawal: 3-year results from a randomized trial in liver transplantation. Am J Transpl 14(3):701–710
Masetti M, Montalti R, Rompianesi G, Codeluppi M, Gerring R, Romano A et al (2010) Early withdrawal of calcineurin inhibitors and everolimus monotherapy in de novo liver transplant recipients preserves renal function. Am J Transpl 10(10):2252–2262
Kornberg A, Küpper B, Thrum K, Krause B, Büchler P, Kornberg J et al (2011) Sustained renal response to mycophenolate mofetil and CNI taper promotes survival in liver transplant patients with CNI-related renal dysfunction. Dig Dis Sci 56(1):244–251
Teperman L, Moonka D, Sebastian A, Sher L, Marotta P, Marsh C et al (2013) Calcineurin inhibitor-free mycophenolate mofetil/sirolimus maintenance in liver transplantation: the randomized spare-the-nephron trial. Liver Transpl 19(7):675–689
Cicinnati VR, Yu Z, Klein CG, Sotiropoulos GC, Saner F, Malagó M et al (2007) Clinical trial: switch to combined mycophenolate mofetil and minimal dose calcineurin inhibitor in stable liver transplant patients—assessment of renal and allograft function, cardiovascular risk factors and immune monitoring. Aliment Pharmacol Ther 26(9):1195–1208
Créput C, Blandin F, Deroure B, Roche B, Saliba F, Charpentier B et al (2007) Long-term effects of calcineurin inhibitor conversion to mycophenolate mofetil on renal function after liver transplantation. Liver Tanspl 13(7):1004–1010
Ponton C, Vizcaíno L, Tomé S, Otero E, Molina E, Castroagudín JF et al (2010) Improvement of renal function after conversion to mycophenolate mofetil combined with low-level calcineurin inhibitor in liver transplant recipients with chronic renal dysfunction. Transpl Proc 42(2):656–659
Kong Y, Wang D, Shang Y, Liang W, Ling X, Guo Z et al (2011) Calcineurin-inhibitor minimization in liver transplant patients with calcineurin-inhibitor-related renal dysfunction: a meta-analysis. PLoS One 6(9):e24387
Reich DJ, Clavien PA, Hodge EE (2005) Mycophenolate mofetil for renal dysfunction in liver transplant recipients on cyclosporine or tacrolimus: randomized, prospective, multicenter pilot study results. Transplantation 80(1):18–25
Pageaux G-P, Rostaing L, Calmus Y, Duvoux C, Vanlemmens C, Hardgwissen J et al (2006) Mycophenolate mofetil in combination with reduction of calcineurin inhibitors for chronic renal dysfunction after liver transplantation. Liver Tanspl 12(12):1755–1760
Watson CJE, Gimson AES, Alexander GJ, Allison MED, Gibbs P, Smith JC et al (2007) A randomized controlled trial of late conversion from calcineurin inhibitor (CNI)-based to sirolimus-based immunosuppression in liver transplant recipients with impaired renal function. Liver Tanspl 13(12):1694–1702
De Simone P, Carrai P, Precisi A, Petruccelli S, Baldoni L, Balzano E et al (2009) Conversion to everolimus monotherapy in maintenance liver transplantation: feasibility, safety, and impact on renal function. Transpl Int 22(3):279–286
Gerhardt T, Terjung B, Knipper P, Palmedo H, Woitas RP, Kalff J et al (2009) Renal impairment after liver transplantation—a pilot trial of calcineurin inhibitor-free vs. calcineurin inhibitor sparing immunosuppression in patients with mildly impaired renal function after liver transplantation. Eur J Med Res 14(5):210–215
Beckebaum S, Klein CG, Sotiropoulos GC, Saner FH, Gerken G, Paul A et al (2009) Combined mycophenolate mofetil and minimal dose calcineurin inhibitor therapy in liver transplant patients: clinical results of a prospective randomized study. Transpl Proc 41(6):2567–2569
Herlenius G, Felldin M, Nordén G, Olausson M, Bäckman L, Gustafsson B et al (2010) Conversion from calcineurin inhibitor to either mycophenolate mofetil or sirolimus improves renal function in liver transplant recipients with chronic kidney disease: results of a prospective randomized trial. Transpl Proc 42(10):4441–4448
Schnitzbauer AA, Sothmann J, Baier L, Bein T, Geissler EK, Scherer MN et al (2015) Calcineurin inhibitor free de novo immunosuppression in liver transplant recipients with pretransplant renal impairment: results of a pilot study (PATRON07). Transplantation 99(12):2565–2575
Fujinaga K, Usui M, Yamamoto N, Ishikawa E, Nakatani A, Kishiwada M et al (2014) Hypertension and hepatitis C virus infection are strong risk factors for developing late renal dysfunction after living donor liver transplantation: significance of renal biopsy. Transpl Proc 46(3):804–810
Lee JH, Cho YH, Ryu SJ, Kim SS, Lee YH, Jang I-A et al (2013) Clinical usefulness of kidney biopsy in liver transplant recipients with renal impairment. Kidney Res Clin Pr 32(4):153–157
Pillebout E, Nochy D, Hill G, Conti F, Antoine C, Calmus Y et al (2005) Renal histopathological lesions after orthotopic liver transplantation (OLT). Am J Transpl 5(5):1120–1129
Pichler RH, Huskey J, Kowalewska J, Moiz A, Perkins J, Davis CL et al (2016) Kidney biopsies may help predict renal function after liver transplantation. Transplantation 100(10):2122–2128
Del Bello A, Congy-Jolivet N, Danjoux M, Muscari F, Lavayssière L, Esposito L et al (2015) De novo donor-specific anti-HLA antibodies mediated rejection in liver-transplant patients. Transpl Int 28(12):1371–1382
Fuiano G, Mazza G, Comi N, Caglioti A, De Nicola L, Iodice C et al (2000) Current indications for renal biopsy: a questionnaire-based survey. Am J Kidney Dis 35(3):448–457
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF, Feldman HI et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Kidney Disease: Improving Global Outcomes (KDIGO) Blood Pressure Work Group (2012) KDIGO clinical practice guideline for the management of blood pressure in chronic kidney disease. Kidney Int S2(5):337–341
Kidney Disease: Improving Global Outcomes (KDIGO) Lipid Work Group (2013) KDIGO clinical practice guideline for lipid management in chronic kidney disease. Kidney Int S3(3):259–305
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group (2013) KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int S3(1):1–150
Jung O, Haack HS, Buettner M, Betz C, Stephan C, Gruetzmacher P et al (2012) Renal AA-amyloidosis in intravenous drug users—a role for HIV-infection? BMC Nephrol 13:151
Naesens M, Kuypers DRJ, Sarwal M (2009) Calcineurin inhibitor nephrotoxicity. Clin J Am Soc Nephrol 4(2):481–508
Esposito V, Mazzon G, Baiardi P, Torreggiani M, Semeraro L, Catucci D et al (2018) Safety and adequacy of percutaneous kidney biopsy performed by nephrology trainees. BMC Nephrol 19(1):14
Collins BS, Davis CL, Marsh CL, McVicar JP, Perkins JD, Alpers CE (1992) Reversible cyclosporine arteriolopathy. Transplantation 54(4):732–734
Morozumi K, Thiel G, Albert FW, Banfi G, Gudat F, Mihatsch MJ (1992) Studies on morphological outcome of cyclosporine-associated arteriolopathy after discontinuation of cyclosporine in renal allografts. Clin Nephrol 38(1):1–8
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Martin-Walter Welker, Consultancies/speaker’s fees: AbbVie, Amgen, Bayer, BMS, Gilead, Novartis, Roche, Sequana Medical. Travel Support: AbbVie, Astellas, Bayer, BMS, Novartis, Janssen, Roche. Nina Weiler, Consultancies/speaker´s bureau for Astellas, Novartis. Wolf Otto Bechstein, Consultancies/speaker’s fees: Astellas, Celgene, Gilead, Integra, Medupdate, MerckSerono, Novartis, Teva. Eva Herrmann, nothing to report. Christoph Betz, noting to report. Mark Schöffauer, nothing to report. Stefan Zeuzem, Consultancies/speaker’s bureau for Abbvie, BMS, Gilead, Janssen, Merck. Christoph Sarrazin, Consultancies/Advisory boards: Abbott, BMS, Gilead, Janssen, Merck/MSD, Roche. Research support: Abbott, Gilead, Janssen, Siemens. Speaker: Abbott, BMS, Gilead, Janssen, Merck/MSD, Qiagen, Roche, Siemens. Kerstin Amann, Speaker/Advisory boards: Alexion, Böhringer Ingelheim. Oliver Jung, nothing to report. On behalf of the remaining authors, no financial, personal, or professional interests that could be construed to have influenced the paper have to be reported.
Ethical statement
Study approval was obtained by the local Ethics Committee for Medical Research in accordance with the 1975 Declaration of Helsinki.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Welker, MW., Weiler, N., Bechstein, W.O. et al. Key role of renal biopsy in management of progressive chronic kidney disease in liver graft recipients. J Nephrol 32, 129–137 (2019). https://doi.org/10.1007/s40620-018-0506-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-018-0506-2