Abstract
Recent years have seen increased engagement amongst health economists with the capability approach developed by Amartya Sen and others. This paper focuses on the capability approach in relation to the evaluative space used for analysis within health economics. It considers the opportunities that the capability approach offers in extending this space, but also the methodological challenges associated with moving from the theoretical concepts to practical empirical applications. The paper then examines three ‘families’ of measures, Oxford Capability instruments (OxCap), Adult Social Care Outcome Toolkit (ASCOT) and ICEpop CAPability (ICECAP), in terms of the methodological choices made in each case. The paper concludes by discussing some of the broader issues involved in making use of the capability approach in health economics. It also suggests that continued exploration of the impact of different methodological choices will be important in moving forward.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Capability well-being offers a broader evaluative space to decision makers both in its multi-dimensional nature and its concern with freedoms to achieve |
Methodological choices have to be made in shifting from the conceptual framework of Sen’s capability approach to empirical applications within health economics |
Measures are starting to become available for use in practice, with the OxCap, ASCOT and ICECAP measures being furthest in development |
Current applications in decision making remain at a relatively early stage of development but the approach offers promise for the future |
1 Introduction
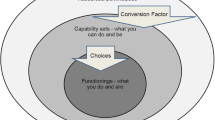
The capability approach is associated with a large body of work generated by Amartya Sen and others. [1–6] that aims to change the focus of evaluation from utility (happiness) to functionings and capabilities [2]. These functionings and capabilities are seen as a person’s ability to be and to do things that they have reason to value [2]. A concern with capabilities can be used both in advocating and evaluating social policies. The approach has generated work on health justice [7], evaluating health interventions [8, 9] and capturing patient experience [10]. This paper, however, is restricted to the application of the approach within health economics.
Health economics has long made use, albeit restricted, of the capability approach [11, 12]. Justifications for adopting the, now standard, extra-welfarist approach were clearly influenced by Sen’s critique of welfarism [12–14]. The extra-welfarist approach allows the inclusion of non-utility information (i.e. going beyond preferences/happiness/satisfaction) through characteristics of people [14], which in practice has meant focusing on health-related functionings [11] operationalised generally through quality-adjusted life-years (QALYs) that combine information on length and health status.
Some health economists have, however, argued for greater use of the capability approach [11, 15–18], in part because it can, potentially, “provide a richer evaluative space enabling improved evaluation of many interventions” (Coast et al [19], p. 667). This paper focuses on the development of capability measures for use in economic evaluation and health economics more generally. The paper continues by exploring the opportunities for generating this richer evaluative space, the methodological challenges involved and the progress that has been made. The discussion outlines some broader challenges that remain in applying the capability approach within health economics.
2 Opportunities
Although some work has attempted to justify the QALY as a full interpretation of Sen’s work [20, 21], this misses a potential advantage of the approach in its extension of the informational or evaluative space used in determining whether one intervention or policy is more beneficial than another [19]. Relative to current practice in health economics, this extension of the evaluative space can be seen as extending it beyond utility (if compared with the standard welfarist approach, as in most of Sen’s writings [2]) or as extending it beyond health (if compared with the usual interpretation of the extra-welfarist approach [11]). The capability approach potentially alters the focus in two ways.
First, the intrinsically multi-dimensional nature of the capability approach [2] shifts the concern towards a broader set of outcomes. This is important for many evaluations that fall under the ‘health’ banner in policy terms but where outputs are not solely health related. Public health interventions provide a good example, where health may be one concern but others might include impacts on anti-social behaviour (e.g. alcohol-reduction schemes) or on the ability to pursue educational objectives (e.g. policies to reduce teenage pregnancy). Social care interventions, too, may lead to changes in how a person can live their lives, but do not directly impact on health (e.g. the provision of a wheelchair to those with impaired mobility may significantly enhance capability without improving health); again, a broader focus may better capture benefits from interventions.
Second, the capability approach shifts the focus away from achieved functionings towards the freedom that a person has in their lives to achieve different aspects of well-being. This is important because a person’s ability to be or do something in life may be of value even if they choose not to take up that capability. A focus on capability also avoids misinterpreting measured lack of functionings as a poor outcome when that level of functioning is chosen by an individual for whom a higher level of functioning is possible. For example one person at the end of life may be better able to alleviate pain by going into a hospice but may choose to remain at home with family; because of the lack of availability of such care in some locations another individual may not have this capability to be free of pain.
There is some institutional acknowledgement of the opportunities inherent in this approach in the UK in the current stances of both the National Institute for Health and Care Excellence and the Social Care Institute for Excellence. Both of these organisations recommend for social care the possibility of using two of the three capability measures that will be examined in detail in this paper [22, 23].
3 Challenges
There is no single way in which to operationalise the capability approach [2, 24] and Sen’s view is that different ways of both measuring and valuing capability and/or functioning can be consistent with the broad framework [2]. Whilst some have seen this as a hindrance [24] (in part because of the lack of ‘user friendliness’ of the approach [4, 6]), others view it as an advantage, and perhaps Sen’s stance on this issue should not be seen as surprising; after all, there have been many interpretations of utility over the years [25, 26]. Nevertheless, a key challenge for applying the approach in health economics relates to how it could and/or should be interpreted and used for enhancing resource allocation decisions. Crucial questions relate to both the measurement and valuation of capabilities.
3.1 Methodological Challenges in Measurement
Although there is openness to different means of identifying capabilities, researchers clearly need to defend their choice of method and ensure that the process of capability selection is rigorous and transparent. Choices need to be justified in a number of areas.
3.1.1 Capabilities or Functionings?
Within the general capability approach there is a distinction between capability (what I am able to do or be) and achieved functioning (what I actually do or am) [2]. The question of how best to capture capability, however, is still uncertain. The main method that has been used to date has been to “preface questions about functionings with terms such as ‘can’ and ‘are able to’” (Coast et al [19], p. 668), but there has been little research as yet on the extent that people pay attention to the terminology and thus whether this wording produces anything materially different from asking about functionings. Some qualitative work, however, provides evidence that some people distinguish between the two [27, 28].
3.1.2 Participatory Methods or a Definitive List of Capabilities?
There has been disagreement within the capability approach about how capabilities should be specified: whether there should be a single capability list for use in all contexts or whether each context requires a different list. Nussbaum has argued that Sen should endorse a definitive list of capabilities [3] and has developed her own list of central capabilities as a theory of social justice, at a highly abstract level. Others have sided with Sen in opposing a definitive list [4, 6, 29]; even with context-specific lists there are some who have focused on expert-led approaches [30] and others who have recommended more participatory approaches [31] that involve finding out from the relevant communities about important capabilities.
There are arguments for and against both expert-led and participatory approaches. Expert-led approaches guard against bias stemming from adaptation. (Adaptation is considered important by Sen in critiquing the utility approach, as those who have adapted to a particular state, for example of poverty, may overestimate the value of their current state and thus underestimate the value of an improvement in that state.). Expert-led approaches avoid the problem of people not being able to envisage themselves as having the opportunity to achieve a valuable functioning and thus not reporting it as something to strive for. Expert-led approaches are, however, open to the charge of paternalism. Standpoint theory asserts that those who are marginalised or suppressed are privileged with the greatest understanding of their experience [32]. Participatory techniques that develop an understanding of the population group may ensure greater relevance and meaningfulness of attributes to respondents [33]. An alternative option is to try to combine expert-led and participatory approaches to obtain the best of both approaches [34].
3.1.3 Truly ‘Objective’ or Perceived Capabilities?
The capability approach focuses on objective capabilities in the sense that they should be determined through impartial assessment [35] in part to avoid problems associated with adaptation [36]. The possibility of measuring complex capabilities (e.g. around relationships or self-respect) objectively is unknown, however, given that impartial observers may not have sufficient knowledge to fully judge a person’s capability and that ‘impartiality’ may be difficult to achieve. If a person does assess their own capability or, indeed, if others are to assess it for them, it is important to use terminology that is meaningful to those completing the assessment.
3.2 Methodological Choices in Valuation
Valuation choices also need to be explored and justified within the capability approach, particularly given the vagueness of the theoretical framework in this respect.
3.2.1 Methods for Obtaining Social Values
There are still considerable uncertainties about the best methods for valuation within the capability approach. Sen acknowledges that as the capability approach is applied in different contexts there will be different choices about how, and what, weights (values) are attached to different capabilities [37]. At the conceptual level, he stresses that valuing is not the same thing as desiring or experiencing happiness [38]; in terms of actual guidance on valuation, Sen merely asserts that values should be arrived at through “reasoned consensus” (Sen 1999 [38], pp 78–79). It is not at all clear, however, how this might be achieved in practice.
An alternative approach draws on Cookson’s re-interpretation of the QALY methodology as a form of capability; he highlights the possibility of using aggregations of individual societal valuations to arrive at a social value, which could then be examined in the light of deliberation and debate [20]. A second alternative is to value all capabilities equally or through simple averaged weights. An example of such an approach is the Human Development Index, which presents results as a single index with simple averaged weights [39]. A further alternative is not to attempt any combining across dimensions, although this may make a measure less useful for decision making.
3.2.2 Anchoring of Values
Much resource allocation in health economics has to contemplate issues of length of life as well as health or well-being. If capability measures are to assist in resource allocation decisions, this issue needs consideration. One option is to avoid combining these values; within a list such as Nussbaum’s [3], for example, Life would be one amongst a number of dimensions to be considered by decision makers. A second approach is to estimate society’s willingness to trade between capability well-being and death, as done with the QALY approach (there between health and death), and to anchor a capability well-being measure at full capability and death. A third approach is to anchor capability well-being at full capability and no capability, and to assume that, with death, a person has no capability.
4 Progress
There has been rapid progress over the last 10 years in moving forward on capability measurement within health economics although much remains to be achieved. This section focuses on three of the most developed and used groups of measures: OxCap [34, 40, 41], ASCOT [42, 43] and ICECAP [44–47]. Attributes for these measures are shown in Table 1.
The Oxford Capability instruments (OxCap) approach to capability measurement began in work by Anand et al. [40] which used secondary data from household and panel surveys to develop a 64 item questionnaire. To make the measure practical for evaluating public health interventions, Lorgelly et al. [34] used focus groups, factor analysis, pilot questionnaires and interviews to reduce the number of questions to 18 (OCAP-18). A more recent adjustment to Anand et al.’s work by Simon et al. [41] aimed to make the questionnaire suitable for evaluating capabilities in mental health interventions, although the resulting OxCap-MH is similar to OCAP-18.
The Adult Social Care Outcome Toolkit (ASCOT) was developed with the aim of capturing capability specifically in relation to social care. The ASCOT instrument began as the Older People’s Utility Scale (OPUS) [43] and has evolved through four versions, with Sen’s capability theory appearing only relatively late in its development [42, 48].
The ICEpop CAPability (ICECAP) measures began with work by Grewal et al. [44], who aimed initially to develop a measure of quality of life for older people that could cross health and social care. They found through qualitative analysis that it was the capability to achieve important functionings that was of particular relevance for older people within the UK and went on to develop a capability well-being measure with five attributes [44]. Subsequent work developed the five-attribute ICECAP-A measure for the adult population [46] and the seven-attribute ICECAP-SCM, a supportive care measure for use with people at the end of life [49]. For each measure, the developers started from first principles rather than adjusting existing measures.
The measures have varied in how they treat the question of capabilities versus functionings. Whilst Anand et al.’s [40] work originally focused on achieved functionings, both OCAP-18 and OxCap-MH questions were re-worded so that the capability of an individual and not their functioning levels was captured [34, 41]. All the ICECAP measures are also worded as capabilities rather than functionings. ASCOT works somewhat differently, with the highest level of each attribute emphasising capability and the remaining three levels reflecting levels of basic functioning [42].
The measures also vary in the basis for the capabilities evaluated. Whilst the identification of attributes for the OxCap has been expert led, the ICECAP and ASCOT instruments were developed through participatory methods (in-depth qualitative work with representatives of the relevant populations). Guided by and aligning to Nussbaum’s central capabilities [3], Anand et al. [40] drew on existing questions from the British Household Panel Survey to assess capability well-being, with later OxCap versions evolving from that initial list. In contrast, both ASCOT and ICECAP started from the need to go beyond health in evaluation, with the move to capability coming later; ICECAP, in particular, drew on themes from the qualitative work to make the link with the capability approach [44]. The participatory approach used within ICECAP also shows the differences that are obtained by focusing on particular groups in the population; although ICECAP-A and ICECAP-O are similar in many ways, they show differences particularly around the ‘achievement’ (ICECAP-A) and ‘role’ (ICECAP-O) attributes [44, 46], with some evidence that the older population struggle with the ‘achievement’ attribute of ICECAP-A because of associations with employment [27].
All three approaches to capability measurement focused on measuring perceived capabilities, although the ASCOT measure has versions for use with proxies. For the ICECAP-SCM, current work is exploring completion of the measure by different groups [50], aiming to understand issues of adaptation and develop means of enhancing ‘objectivity’.
There are further differences between the measures in terms of valuation although none has used deliberative approaches, which focus on democratic discussion and informed debate. ICECAP and ASCOT both used best-worst scaling (BWS) [51] to obtain aggregate social values, whilst OxCap assumed equal values for each capability indicator on the measure, albeit calculated with different numerical methods across the different versions [41]. Simon et al. argue that a core motivation for using the capability approach is its multi-dimensional nature and hence generating a single score for capability well-being, reflecting population preferences, is “conceptually in tension with the original capability approach” (Simon et al. [41], p 195). They view this as potentially restricting the opportunities that the capability approach offers in terms of policy making and instead aim to provide additional multi-dimensional information to decision makers, to enhance a process that would otherwise rely solely on QALYs. There is a risk, however, that given relatively complex unweighted information offered alongside a more precisely and technically packaged QALY result, decision makers will tend to rely on the latter. Possibly for this reason, developers of the other two measures generated weights for the different capabilities within their measures, ASCOT from both social care and general populations [42], and ICECAP from the general population [45, 47]. Coast et al. [45] have argued that BWS is appropriate for the capability approach as it represents values rather than preference, given there is no trade-off between capabilities with BWS.
Given the lack of weighting within the OxCap measures, the question of anchoring has not arisen. For ASCOT and ICECAP this issue has been approached differently, with ASCOT anchoring (using a time trade-off method) values at ideal social care-related quality of life and death (with values from −0.19 to 1) [42], and the ICECAP measures anchoring between full and no capability [45, 47].
5 Discussion
This paper has considered the application of the capability approach within health economics. It briefly outlined the approach and considered the opportunities that it provides within health economics, before examining the measurement challenges associated with using the approach in practice. The paper also explored current progress as well as distinctions between the available approaches.
All current approaches remain at a relatively early stage of development but there is increasing use of the measures both in research generally [52, 53] and specifically in assessments of cost effectiveness [54–57]. Whilst there are now a number of measures offering potential for use in exploring the impact of interventions on capability, there remain important areas for future research. First, further research around the implications of using different approaches to the generation of both measurement systems and their valuation will be important in ensuring that the eventual application of the capability approach does not just latch onto the first viable measure and stifle further development [58].
Second, although there is increasing evidence of validity for some capability instruments [48, 53, 59–69], there is still very little evidence about sensitivity to change and the limited information is mixed [70–72]. Given that generic capability measures cover a greater informational space—the entirety of a person’s life (rather than just their health, for example)—it may be more difficult for such measures to show sensitivity to change. Such information is fundamental in ensuring that measures are able to distinguish between different interventions and thus help in decision making, although it is also important that the change that is noted is important to people. It is possible for measures to be sensitive to change without that change being valued. Information about the validity of measures does not seem to have been of concern within the more general capability literature, but it deserves more consideration. Certainly, for capability assessment to influence health and social care decision making, validity information is vital.
Third, research into how to use the capability approach in decision making has lagged behind work on generating measures. This is a clear area for future research that can build on work in a number of areas both from within health economics and outside. These include research into individual preferences for different equity considerations that has been conducted in relation to health and the QALY [73–78], research into community preferences that has attempted to guide principles for priority setting [79–81] and work on multi-dimensional poverty from within the economic development literature [82]. Whilst some researchers use capability measures in approaches that are almost identical to the standard extra-welfarist QALY approach [54, 55, 57], research looking at alternatives that are more focused on equity/achieving minimum thresholds is also starting to appear [7, 8, 83]. This now includes the practical development of empirical methods for assessing sufficient capability (using the ICECAP measures and based on a minimum threshold) in an evaluative framework [83], as well as purely conceptual work related to considering equality in terms of the extent to which health capability falls short of average or target levels [84]. Considerably more research of this type is, however, required.
The capability approach is intended to be a flexible framework and this is both its great strength and its great weakness. Any application of the approach will inevitably represent compromises between the philosophy and the practicalities of application. Each of the measures discussed above represents the totality of a number of different choices. The extent to which they remain faithful to the underlying philosophy will always be a matter for debate and some have disparaged these attempts as providing little in the way of conceptual advance [8]. It is our contention, however, that only by attempting to use the theory will we develop a better understanding of the advantages and disadvantages of different choices. One aspect that all these approaches have in common is that they do not hide behind an abstract conceptual paradigm and refuse to go further, and in that sense they all provide advances to the general thinking around the capability approach in health economics. Much exploration is still required, however, and cooperation and informed debate will help to advance the practical application of the capability approach as a distinct alternative in evaluation and to determine how the theory is most applicable in the context of health economics.
References
Sen A. Inequality reexamined. New York: Russell Sage Foundation; 1992.
Sen A. Capability and well-being. In: Nussbaum MC, editor. The quality of life. Oxford: Clarendon Press; 1993.
Nussbaum MC. Capabilities as fundamental entitlements: Sen and social justice. Fem Econ. 2003;9(2–3):33–59.
Alkire S. Why the capability approach? J Hum Dev. 2005;6:115–33.
Robeyns I. The capability approach: a theoretical survey. J Hum Dev. 2005;6:93–114.
Robeyns I. The capability approach in practice. J Polit Philos. 2006;14:351–76.
Venkatapurum S. Health justice: an argument from the capabilities approach. Cambridge: Polity Press; 2011.
Ruger JP. Health capability: conceptualization and operationalization. Am J Public Health. 2010;100:41–9.
Ruger JP. Health and social justice. Lancet. 2004;364:1075–80.
Entwistle VA, Watt IS. Treating patients as persons: a capabilities approach to support delivery of person-centred care. Am J Bioeth. 2013;13(8):29–39.
Coast J, Smith RD, Lorgelly P. Welfarism, extra-welfarism and capability: the spread of ideas in health economics. Soc Sci Med. 2008;67:1190–8.
Culyer AJ. Commodities, characteristics of commodities, characteristics of people, utilities, and the quality of life. In: Baldwin S, editor. Quality of life: perspectives and policies. London: Routledge; 1990. p. 9–27.
Culyer AJ. The normative economics of health care finance and provision. Oxford Rev Econ Pol. 1989;5(1):34–56.
Brouwer WBF, Culyer AJ, van Exel NJA, Rutten FFH. Welfarism vs. extra-welfarism. J Health Econ. 2008;27:325–38.
Anand P, Dolan P. Equity, capabilities and health. Soc Sci Med. 2005;60:219–22.
Anand P. Capabilities and health. J Med Eth 2005;31:299–303.
Anand P. Introduction. Soc Indic Res. 2005;74:1–8.
Lorgelly PK, Lawson KD, Fenwick EAL, Briggs AH. Outcome measurement in economic evaluation of public health interventions: a role for the capability approach? Int J Envir Res Public Health. 2010;7:2274–89.
Coast J, Smith RD, Lorgelly P. Should the capability approach be applied in health economics? Health Econ. 2008;17:667–70.
Cookson R. QALYs and the capability approach. Health Econ. 2005;14:817–29.
Bleichrodt H, Quiggin J. Capabilities as menus: a non-welfarist basis for QALY evaluation. J Health Econ. 2013;32:128–37.
National Institute for Health and Care Excellence. The social care guidance manual. London: National Institute for Health and Care Excellence; 2013.
Francis J, Byford S. SCIE’s approach to economic evaluation in social care. London: Social Care Institute for Excellence; 2011.
Sugden R. Welfare, resources and capabilities: a review of inequality reexamined by Amartya Sen. J Econ Lit. 1993;31:1947–62.
Blaug M. Economic theory in retrospect. 5th ed. Cambridge: Cambridge University Press; 1996.
Roncaglia A. The wealth of ideas: a history of economic thought. Cambridge: Cambridge University Press; 2005.
Al-Janabi H, Keeley T, Mitchell P, Coast J. Can capabilities be self-reported? A think aloud study. Soc Sci Med. 2013;87:116–22.
Horwood J, Sutton E, Coast J. Evaluating the face validity of the ICECAP-O capabilities measure: a ‘think aloud’ study with hip and knee arthroplasty patients. Appl Res Qual Life. 2014. doi:10.1007/s11482-013-9264-4.
Alkire S. Using the capability approach: prospective and evaluative analyses. In: Comin F, Qizilbash M, Alkire S, editors. The capability approach: concepts, measures and applications. New York: Cambridge University Press; 2008.
Robeyns I. Sen’s capability approach and gender inequality: selecting relevant capabilities. Fem Econ. 2003;9(2–3):61–92.
Burchardt T, Vizard P. ‘Operationalizing’ the capability approach as a basis for equality and human rights monitoring in twenty-first century Britain. J Hum Dev Capab. 2011;12:91–119.
Wylie A. Why standpoint matters. In: Figueroa R, Harding S, editors. Science and other cultures: issues in philosophies of science and technology. London: Routledge; 2003.
Kinghorn P, Robinson A, Smith RD. Developing a capability-based questionnaire for assessing well-being in patients with chronic pain. Soc Indic Res 2014. doi:10.1007/s11205-014-0625-7.
Lorgelly PK, Lorimer K, Fenwick EA, Briggs AH. The capability appraoch: developing an instrument for evaluating public health interventions: final report. University of Glasgow: Glasgow Centre for Population Health; 2008.
Sen A. Reason, freedom and well-being. Utilitas. 2006;18:80–96.
Sen A. Health: perception versus observation. BMJ. 2002;324:860–1.
Sen A. The idea of justice. London: Allen Lane; 2009.
Sen A. Commodities and capabilities. New Delhi: Oxford University Press; 1999.
Puri J, Gaye A, Kurukulasuriya S, Scott T. Measuring human development: a primer. New York: UNDP; 2007.
Anand P, Hunter G, Carter I, Dowding K, Francesco G, van Hees M. The development of capability indicators. J Hum Dev Capab. 2009;10(1):125–52.
Simon J, Anand P, Gray A, Rugkasa J, Yeeles K, Burns T. Operationalising the capability approach for outcome measurement in mental health research. Soc Sci Med. 2013;98:187–96.
Netten A, Burge P, Malley J, et al. Outcomes of social care for adults: developing a preference-weighted measure. Heath Technol Assess 2012;16(16).
Netten A, Ryan M, Smith P. The development of a measure of social care outcome for older people. Report No. 1690/2. Kent: PSSRU; 2002.
Grewal I, Lewis J, Flynn TN, Brown J, Bond J, Coast J. Developing attributes for a generic quality of life measure for older people: preferences or capabilities? Soc Sci Med. 2006;62:1891–901.
Coast J, Flynn TN, Natarajan L, et al. Valuing the ICECAP capability index for older people. Soc Sci Med. 2008;67:874–82.
Al-Janabi H, Flynn TN, Coast J. Development of a self-report measure of capability wellbeing for adults: the ICECAP-A. Qual Life Res. 2012;21:167–76.
Flynn TN, Huynh E, Peters TJ, et al. Scoring the ICECAP-A capability instrument: estimation of a UK general population tariff. Health Econ 2014. doi:10.1002/hec.3014
Forder JE, Caiels J. Measuring the outcomes of long term care. Soc Sci Med. 2011;73(12):1766–74.
Sutton E, Coast J. Development of a supportive care measure for economic evaluation of end-of-life care, using qualitative methods. Palliat Med. 2014;28:151–7.
Bailey CJ, Orlando R, Kinghorn P, Armour K, Perry R, Coast J. Measuring quality of end of life using ICECAP-SCM: feasibility and acceptability. BMJ Support Palliat Care. 2014;4:112.
Flynn TN, Louviere J, Peters T, Coast J. Best-worst scaling: what it can do for health care research and how to do it. J Health Econ. 2007;26:171–89.
Visser VS, Comans TA, Scuffham PA. Evaluation of the effectiveness of a community-based crisis intervention program for people bereaved by suicide. J Commun Psychol. 2014;42(1):19–28.
Flynn TN, Chan P, Coast J, Peters TJ. Assessing quality of life among British older people using the ICECAP-O capability measure. Appl Health Econ Health Policy. 2011;9:317–29.
Henderson C, Knapp M, Fernandez J-L, et al. Cost effectiveness of telehealth for patients with long term conditions (Whole Systems Demonstrator telehealth questionnaire study): nested economic evaluation in a pragmatic, cluster randomised controlled trial. BMJ. 2013;346.
Makai P, Looman W, Adang E, Melis R, Stolk E, Fabbricotti I. Cost-effectiveness of integrated care in frail elderly using the ICECAP-O and EQ-5D: does choice of instrument matter? Eur J Health Econ. 2014. doi:10.1007/s10198-014-0583-7.
Forder J, Malley J, Towers A-M, Netten A. Using cost-effectiveness estimates from survey data to guide commissioning: an application to home care. Health Econ. 2013. doi: 10.1002/hec.2973.
Jones K, Forder J, Caiels J, Welch E, Glendinning C, Windle C. Personalization in the health care system: do personal health budgets have an impact on outcomes and cost? J Health Serv Res Pol. 2013;18(Suppl 2):59–67.
Smith RD, Lorgelly P, Al-Janabi H, Venkatapurum S, Coast J. The capability approach: an alternative paradigm for health economics? In: Jones A, editor. Elgar companion to health economics. Cheltenham: Edward Elgar Publishing; 2012.
Coast J, Peters TJ, Natarajan L, Sproston K, Flynn TN. An assessment of the construct validity of the descriptive system for the ICECAP capability measure for older people. Qual Life Res. 2008;17:967–76.
Makai P, Brouwer WBF, Koopmanschap MA, Nieboer AP. Capabilities and quality of life in Dutch psycho-geriatric nursing homes: an exploratory study using a proxy version of the ICECAP-O. Qual Life Res. 2012;21:801–12.
Makai P, Koopmanschap MA, Brouwer WBF, Nieboer AA. A validation of the ICECAP-O in a population of post-hospitalized older people in the Netherlands. Health Qual Life Outcomes 2013;11(57):1–11.
Davis JC, Liu-Ambrose T, Richardson CG, Bryan S. A comparison of the ICECAP-O with EQ-5D in a falls prevention clinical setting: are they complements or substitutes? Qual Life Res 2012.
Davis JC, Bryan S, McLeod R, Rogers J, Khan K, Liu-Ambrose T. Exploration of the association between quality of life, assessed by EQ-5D and ICECAP-O, and falls risk, cognitive function and daily function, in older adults with mobility impairments. BMC Geriatr. 2012;12(1):65.
Couzner L, Ratcliffe J, Crotty M. The relationship between quality of life, health and care transition: an empirical comparison in an older post-acute population. Health Qual Life Outcomes. 2012;10:1–9.
Couzner L, Ratcliffe J, Lester L, Flynn TN, Crotty M. Measuring and valuing quality of life for public health research: application of the ICECAP-O capability index in the Australian general population. Int J Public Health. 2012.
Al-Janabi H, Peters TJ, Brazier J, et al. An investigation of the construct validity of the ICECAP-A capability measure. Qual Life Res. 2013;22:1831–40.
Malley JN, Towers A-M, Netten AP, Brazier JE, Forder JE, Flynn T. An assessment of the construct validity of the ASCOT measure of social care-related quality of life with older people. Health Qual Life Outcomes. 2012;10(21):1–14.
Makai P, Beckebans F, van Exel J, Brouwer WBF. Quality of life of nursing home residents with dementia: validation of the German version of the ICECAP-O. PLoS ONE. 2014;9(3):e92016.
Callaghan L, Towers A-M. Feeling in control: comparing older people’s experiences in different care settings. Ageing Soc. 2014;1–25. doi:10.1017/S0144686X13000184.
Comans TA, Peel NM, Gray LC, Scuffham PA. Quality of life of older frail persons receiving a post-discharge program. Health Qual Life Outcomes. 2013;11(1):58.
Parsons N, Griffin XL, Achten J, Costa ML. Outcome assessment after hip fracture. Is EQ-5D the answer? Bone Joint Res 2014;3:69–75.
Flynn TN, Huynh E, Dieppe P, Coast J, Pollard B. Change in capability-related quality of life resulting frorm hip or knee replacement: results from a cohort study using the ICECAP-O instrument: WP13_003. Adelaide: Institute for Choice; 2013.
Dolan P, Shaw R, Tsuchiya A, Williams A. QALY maximisation and people’s preferences: a methodological review of the literature. Health Econ. 2005;14:197–208.
Tsuchiya A, Dolan P, Shaw R. Measuring people’s preferences regarding ageism in health: some methodological issues and some fresh evidence. Soc Sci Med. 2003;57:687–96.
Tsuchiya A, Williams A. A “fair innings” between the sexes: are men being treated inequitably? Soc Sci Med. 2005;60:277–86.
Tsuchiya A, Dolan P. Do NHS clinicians and members of the public share the same views about reducing inequalities in health? Soc Sci Med. 2007;64:2499–503.
Tsuchiya A, Dolan P. Equality of what in health? Distinguishing between outcome egalitarianism and gain egalitarianism. Health Econ. 2009;18:147–59.
Donaldson C, Baker R, Mason H, et al. The social value of a QALY: raising the bar or barring the raise? BMC Health Serv Res. 2011;11(8):1–8.
Mooney G. ‘Communitarian claims’ as an ethical basis for allocating health care resources. Soc Sci Med. 1998;47:1171–80.
Mooney G. Communitarian claims and community capabilities: furthering priority setting? Soc Sci Med. 2004;60:247–55.
Wiseman V. Inclusiveness in the value base for health care resource allocation. Social Sci Med. 2014;2014:98–106.
Alkire S, Foster J. Counting and multidimensional poverty measurement. J Public Econ. 2011;95:476–87.
Mitchell PM, Roberts TE, Barton PM, Coast J. Applying the sufficient capability approach in health economic evaluations. Paper presented to the Health Economists’ Study Group meeting, Exeter. 2013.
Ruger JP. Ethics and goverance of global health inequalities. J Epid Comm Health. 2006;60:998–1003.
Acknowledgements
An EU-funded ERC Starting Grant (261098 EconEndLife) funds Joanna Coast and Philip Kinghorn to conduct research into the allocation of resources in end-of-life care using a capability framework. At the time this work was conduced, Paul Mitchell was funded through NIHR core funding to the Health Economics Unit, University of Birmingham.
Contributions
Each author initially drafted one section: JC Opportunities; PK Challenges; and PM Progress. Sections were drawn together into a complete first draft and edited by JC. All authors then commented on that first complete draft and on subsequent versions, and agreed on the final version of the paper. JC acts as guarantor for the paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Coast, J., Kinghorn, P. & Mitchell, P. The Development of Capability Measures in Health Economics: Opportunities, Challenges and Progress. Patient 8, 119–126 (2015). https://doi.org/10.1007/s40271-014-0080-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40271-014-0080-1