Abstract
Background
Muscle wasting is common and insidious in end-stage renal disease (ESRD). Loss of muscle quantity and quality reduces quality of life and increases mortality in ESRD patients. Additionally, secondary hyperparathyroidism (SHPT) causes muscle atrophy. Meanwhile, vitamin D, which is used for SHPT treatment, plays an essential role in muscle growth.
Objectives
We prospectively investigated the effect of active vitamin D administration on muscle mass.
Methods
We measured muscle mass based on bioelectrical impedance analysis in 68 hemodialysis patients. Patients were divided into a control group (without active vitamin D administration) and a VitD group (with active vitamin D administration). We compared muscle mass at the beginning of treatment and 1 year later. We also investigated health-related quality of life (HR-QOL) using the Medical Outcome Study Short Form-36 (SF-36).
Results
The VitD group experienced a significant increase in the amount of change in total muscle mass and muscle mass percentage in men (p = 0.025) but not in women (p = 0.945). By multivariable logistic regression analysis, active vitamin D administration was independently associated with increased muscle mass percentage in men only. In the SF-36, the physical functioning (PF) scores were significantly decreased at the end of the study in the patients without active vitamin D treatment, especially in women.
Conclusion
Our results suggested that active vitamin D treatment was associated with increased muscle mass in men, and it might have a favorable effect on maintaining PF in HR-QOL in hemodialysis patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Skeletal muscle wasting is common and insidious in end-stage renal disease (ESRD) [1, 2]. Previous literature demonstrated that factors including acidosis, protein-energy malnutrition, co-morbid illnesses, aging, oxidative stress, inflammation [3], anemia, water and electrolyte disturbances, carnitine deficiency [4], hyperparathyroidism [5–7], and very low levels of physical activity contribute markedly to muscle fiber loss and atrophy [1, 3–10]. This loss of muscle quantity and quality is associated with metabolic and functional deficits and reduced quality of life in hemodialysis patients [11]. Furthermore, muscle wasting is recognized as a strong predictor of mortality in ESRD [12].
Secondary hyperparathyroidism (SHPT) develops in ESRD in response to disruptions in the homeostatic control of parathyroid hormone (PTH) secretion related to alterations in serum phosphorous, calcium, and declining 1,25 dihydroxy vitamin D (1,25(OH)2D) levels, which occur with deterioration in renal function [13]. As a major action, PTH regulates serum calcium by acting mainly on bone and kidney and stimulating calcium reabsorption and bone resorption in low serum calcium level situations [14]. In addition, increased PTH causes wasting, weight loss, weakness, muscle atrophy, and negative nitrogen balance in patients with primary and secondary hyperparathyroidism [5–7].
Vitamin D plays an essential role in muscle growth and development [15] and in regulating muscle contractility [16]. 1,25(OH)2D is the biologically active metabolite and the form of vitamin D that binds to receptors on human muscle tissue [17]. Numerous animal and human studies have demonstrated that vitamin D deficiency is associated with decreased muscle size [18–20] and strength [21, 22], and with reduced physical function, and increased falls and non-vertebral fractures in the elderly [13, 23]. Conversely, vitamin D supplementation improves muscle strength, walking distance, and functional ability in vitamin D-deficient elderly people [23]. In ESRD patients, the 1,25(OH)2D level usually decreases with a decline in renal function. Thus, vitamin D deficiency may contribute to the significant muscle atrophy, weakness, and widespread disability experienced by not only elderly people but also ESRD patients. However, the current focus of vitamin D treatment is mainly the control of SHPT and its effects on bone metabolism and tissue calcification, as outlined in the current Kidney Disease Outcomes Quality Initiative (K/DOQI) guidelines [13]. In fact, a few studies have examined the effects of vitamin D treatment on muscle function in patients with ESRD [24, 25].
Hence, we prospectively investigated the effect of active vitamin D administration on muscle mass and health-related quality of life (HR-QOL) in hemodialysis patients.
2 Methods
2.1 Study Subjects
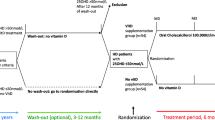
This was a prospective study of data from a single medical center (Shinzato Clinic, Nagasaki, Japan). In total, 184 patients who received hemodialysis between April 2007 and April 2008 were eligible for this study. Kindaly AF-2P® and AF-3P® (Fuso Pharmaceutical Industries Ltd., Osaka, Japan) were mixed in equal proportions and used as dialysate. The final electrolyte concentrations after preparation of the dialysate were as follows: Na+ 140 mEq/L; K+ 2.0 mEq/L; Ca2+ 2.75 mEq/L; Mg2+ 1.0 mEq/L; Cl− 112.25 mEq/L; CH3COO− 8 mEq/L; HCO3 − 27.5 mEq/L; and C6H12O6 125 mg/dL. The dialysate was not changed during the study period. Exclusion criteria were patients who resumed dialysis after renal graft failure and in whom we could not measure precise muscle mass because of amputation and astasia. We excluded 116 participants based on the aforementioned exclusion criteria. Finally, 68 patients (28 men and 40 women) were included for further analysis. These patients were divided into two groups: (1) the subjects without active vitamin D administration, defined as the control group; and (2) the subjects with active vitamin D administration for more than 9 months of the year, defined as the VitD group. Active vitamin D includes alfacalcidol, calcitriol, and maxacalcitol, regardless of the route of administration. All subjects gave informed consent for study participation. This study was approved by the Ethics Committee of Nagasaki University Hospital (authorization number 12052801) and performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
2.2 Clinical Measurements and Health-Related Quality of Life (HR-QOL) Evaluation
Sociodemographic characteristics, ESRD etiology, medical history, prescription, and details of the hemodialysis treatment modality were obtained from medical records. Height and body weight (BW) before dialysis at the beginning of the week were recorded in the clinic. Body mass index (BMI) was calculated as weight in kg divided by the square of height in meters. Routine laboratory examination was performed before dialysis at the beginning of the week fortnightly, and levels of hemoglobin, serum calcium and phosphorus, serum albumin, intact PTH (iPTH), creatinine, total cholesterol (TC), C-reactive protein (CRP), and HCO3 − were determined. The level of corrected calcium (cCa) was calculated using albumin. The adequacy of dialysis was assessed by Kt/V (amount of dialysis delivered: K = clearance of urea, t = time on dialysis, V = estimated total body water) [26]. The normalized protein catabolic rate (n-PCR) was calculated using a single-compartment model [26]. All data were measured at the beginning of the study and again 1 year later. In addition, we investigated HR-QOL using the Medical Outcome Study Short Form-36 (SF-36 version 2, iHope International, Tokyo, Japan) for patients at the beginning and 1 year after the beginning of the study. This instrument has been used extensively in populations of patients with renal disease [27].
2.3 Muscle Mass Measurement
We measured muscle mass based on bioelectrical impedance analysis (BIA) by using body composition meter dual-frequency DC-320 (Tanita Corporation, Tokyo, Japan) before dialysis at the beginning of the week. We measured muscle mass at the beginning and 1 year after the beginning of the study.
2.4 Statistical Analysis
Results are expressed as mean ± standard deviation (SD). Differences in laboratory values between the control group and VitD group were evaluated using the t test. Multiple logistic linear regression analysis was performed to determine the correlation between the rate of change in muscle mass and the other variables measured at the beginning of study. Probability values <0.05 were indicative of statistical significance. All statistical analyses were performed using SPSS® version 11.0 software (SPSS Japan, Tokyo, Japan).
3 Results
3.1 Baseline Characteristics of Study Patients
Baseline characteristics of the two groups are shown in Table 1. Mean age ± SD was 58.9 ± 13.6 years. The mean dialysis period ± SD was 133.2 ± 96.4 months, mean BW ± SD was 53.0 ± 8.9 kg, and mean BMI ± SD was 22.0 ± 3.4 kg/m2. The primary ESRD etiologies were as follows: 41 patients had chronic glomerulonephritis, nine had diabetic nephropathy, five had nephrosclerosis, and 13 had other diseases. The mean percentage of muscle mass ± SD in BW (muscle mass/BW × 100) was 37.8 ± 5.8 % in all participants. The mean size of dialyzer membrane ± SD was 1.80 ± 0.26 m2, and the mean time of dialysis treatment ± SD was 3.93 ± 0.47 h. The mean Kt/V ± SD was 1.27 ± 0.24, and the mean n-PCR ± SD was 0.90 ± 0.13 g/kg/day. During the study period, 26 patients never received vitamin D therapy (control group), and 42 patients received active vitamin D therapy for >9 months (VitD group). There were no significant differences in age, primary ESRD etiology, dialysis period, the condition of dialysis, BW, and BMI between the two groups at the beginning of the study. In addition, there was also no significant difference in mean muscle mass percentage ± SD between the control group and VitD group at baseline status (37.4 ± 5.3 vs. 38.0 ± 6.1 %; p = 0.662). At the beginning of the study, the VitD group showed significantly higher levels of serum cCa and iPTH and lower levels of TC than the control group. However, no significant difference in hemoglobin, phosphorus, albumin, creatinine, CRP, HCO3 −, Kt/V, or n-PCR levels was noted between groups (Table 1).
3.2 Clinical Parameters of All Patients and Each Group After 1 Year
One year later, there were similar differences between cCa, iPTH, and TC. We observed significantly higher levels of phosphorus in the VitD group than in the control group at the end of the study. Although Kt/V and n-PCR showed an increasing trend in both groups, no significant difference in these levels was noted between the control and VitD groups at the end of the study period (Table 2). As to the amount of change in total muscle mass and muscle mass percentage between the beginning and end of the study, there were no significant differences between the control group and VitD group (Fig. 1).
Change in total muscle mass percentage (a) and total muscle mass (b) from the beginning to the end of the study in all subjects (control and VitD groups). There were no significant differences between the control and VitD groups. The values in the figure show mean ± standard deviation. ALL all participants, Control subjects without active vitamin D administration, Vitamin D subjects with active vitamin D administration for >9 months in a year, VitD vitamin D group
3.3 Baseline Characteristics by Sex
Next, we analyzed these parameters in subgroups by sex. Baseline characteristics of men and women in the two groups are shown in Table 3. The men in the VitD group showed significantly higher iPTH levels and lower TC levels than those in the control group at the beginning of the study. After active vitamin D treatment, the mean cCa ± SD level increased (9.1 ± 1.1 to 9.8 ± 1.2 mg/dL; p = 0.017). Similarly, women in the VitD group showed higher cCa and iPTH levels than those in the control group at the beginning of the study. However, in women, active vitamin D treatment had no effect on the cCa level at the end of the study (Table 4). The dosage and type of vitamin D administered are shown in Table 5.
3.4 Amounts of Change in Muscle Mass in Men and Women in Each Group
Active vitamin D administration significantly increased the amount of change in total muscle mass and mean muscle mass percentage ± SD in men (control group, −0.90 ± 1.6 % vs. VitD group, 0.63 ± 1.26 %; p = 0.025) but not in women (control group, −0.2 ± 1.00 % vs. VitD group, −0.2 ± 1.40 %; p = 0.945) (Fig. 2). In multivariable logistic regression analysis adjusted for confounding factors such as sex, age, dialysis period, height, BW, iPTH, and muscle mass percentage at baseline, active vitamin D administration was independently associated with the increased muscle mass percentage in men but not in women (Table 6).
Change in total muscle mass percentage (a) and total muscle mass (b) from the beginning to the end of the study in men and women in each group (control and VitD groups). The amount of change in total muscle mass and muscle mass percentage significantly increased in men but not in women in the VitD group compared with the control group. The black bars represent the mean ± SD in the control group (subjects without active vitamin D administration). The white bars show the mean ± SD in the vitamin D group (subjects with active vitamin D administration for >9 months in a year). SD standard deviation, VitD vitamin D group
3.5 Effect of Active Vitamin D Administration on HR-QOL
We analyzed the effect of active vitamin D administration on HR-QOL using the SF-36. In the control group, a significant decrease of scores in physical functioning (PF) was found at the end of the study compared with the beginning of the study (p = 0.013) (Fig. 3a). However, in the VitD group, there was no difference in the scores of all SF-36 components before and after the study (Fig. 3b). Next, we analyzed the SF-36 scores for men and women. For the men in the VitD group, mental health scores at the end of the study significantly decreased compared with scores at the beginning (p = 0.016) [Fig. 3d]. Meanwhile, in women, we observed a significant decrease in PF scores only in the control group (p = .010) [Fig. 3e].
The results of the SF-36 score between the beginning and end of the study in the control group (a all participants; c men; e women) and VitD group (b all participants; d men; f women). In the control group, a significant decrease of scores in physical functioning was found at the end of the study compared with the beginning of the study (a). However, in all participants of the VitD group (b) and in the men of the control group (c), there was no difference in the scores of all SF-36 components before and after the study. In the men of the VitD group, mental health scores at the end of the study significantly decreased compared with those at the beginning of the study (d). Meanwhile, in women, we observed a significant decrease of physical functioning scores in the control group (e) but not in the VitD group (f). The black bars represent the mean SF-36 scores ± SD at the beginning of the study. The white bars show the mean SF-36 scores ± SD at the end of the study. BP bodily pain, GH general health, MCS mental component summary, MH mental health, PCS physical component summary, PF physical functioning, pre the SF-36 scores investigated at the beginning of the study, post the SF-36 scores investigated at the end of the study, RCS role/social component summary, RE role emotional, RP role physical, SD standard deviation, SF social functioning, SF-36 Medical Outcome Study Short Form-36, VitD vitamin D group, VT vitality
4 Discussion
In this study, we investigated the association between active vitamin D administration and the amount of change in muscle mass in hemodialysis patients. In consideration of the effects of age, dialysis period, height, BW, iPTH, and muscle mass percentage at the beginning of the study, we found a significant correlation between active vitamin D administration and increased muscle mass in men only. Meanwhile, active vitamin D administration in women prevented a decrease in PF scores independent of the effect on muscle mass.
Vitamin D supplementation has beneficial effects on muscle strength and balance in elderly people [28]. However, a few studies have examined the effects of vitamin D treatment on muscle and muscle function in patients with ESRD [24, 25, 29–31]. To our knowledge, our study is the first report on the association between active vitamin D and the amount of change in muscle mass assessed by BIA and HRQOL simultaneously. BIA is well-known to be an easily reproducible, inexpensive, and non-invasive method to measure body composition, such as body fluid volume, muscle mass, and fat mass [32–34], compared with the conventional methods, dual-energy X-ray absorptiometry, and whole-body magnetic resonance imaging [33, 35]. Therefore, we consider BIA to be a useful method to assess muscle mass in the clinical condition.
We considered several mechanisms by which active vitamin D administration increased muscle mass. Active vitamin D binding to the nuclear and membrane-associated vitamin D receptor (VDR) of skeletal muscle cells triggers genomic and non-genomic effects shown to positively affect muscle [36]. The activation of nuclear VDR increases the synthesis of muscle skeletal proteins important for muscle function [37–40] and phosphate metabolism, resulting in positive effects on muscle contraction [37]. Furthermore, active vitamin D plays a role in the regulation of muscle cell proliferation and differentiation [40, 41]. Thus, active vitamin D itself might exert positive effects on muscle mass directly via these mechanisms. Furthermore, we observed a significant association between active vitamin D administration and increased muscle mass in men but not in women. The reasons for differences between the sexes are uncertain, yet potential explanations may involve differences in baseline lean body mass, muscle strength, physical activity, and circulating levels of testosterone, a hormone that is anabolic to muscle [42, 43].
In the present study, we also investigated the association between active vitamin D and HR-QOL. As a result, although the PF scores were significantly decreased at the end of the study in the patients without active vitamin D treatment, especially in women, the VitD group showed no significant change in PF scores before and after the study. These results suggest that active vitamin D administration might prevent the decline of PF associated with aging or other factors, independent of the change in muscle mass. Although we did not assess muscle strength or muscle function in the present study, there might be a significant association with these parameters and HR-QOL. On the other hand, for the men in the VitD group, mental health scores at the end of the study were significantly decreased compared with those at the beginning. Although the reason for this is uncertain, men treated with active vitamin D tended to show an increased level of serum calcium within the normal range. Because Tanaka et al. [44] previously reported that hypercalcemia is associated with poor mental health in dialysis patients, the increased serum calcium level may influence mental health in the men of the VitD group.
There are several limitations to this study. First, this study is a retrospective analysis in which follow-up and treatment protocols were not standardized. In addition, the total number of participants was only 68 patients, which is a relatively small sample size, and the patients showed a low prevalence of diabetes mellitus. Second, we could not examine the difference among drugs, dose, or active vitamin D administration route because of the small sample size. In addition, we did not check the physical activity levels or exercise frequency in daily life, and we could not examine the effect of history of active vitamin D administration. Therefore, these factors might affect our results. Third, we could not investigate the effect of acidosis on muscle mass, which is reported to enhance amino acid degradation and increase muscle proteolysis [45] because data on HCO3 − after 1 year were lacking. However, since there was no difference in HCO3 − levels before dialysis, and the adequacy of dialysis throughout the study period was the same between groups, we believe that muscle mass was not affected by acidosis in this study. Last, our study period was limited to 1 year. Therefore, the long-term effect of active vitamin D is unclear.
5 Conclusion
Our results suggested that active vitamin D treatment was associated with increased muscle mass in men, and it might have a favorable effect on maintaining PF in HR-QOL. Hence, we hope for a prospective large-scale study to confirm our results and to investigate the long-term effects of active vitamin D on falls, fractures, HR-QOL, or mortality, which are attributed to decreased muscle mass.
References
Kouidi E, Albani M, Natsis K, et al. The effects of exercise training on muscle atrophy in haemodialysis patients. Nephrol Dial Transplant. 1998;13:685–99.
Lim PS, Cheng YM, Wei YH. Large-scale mitochondrial DNA deletions in skeletal muscle of patients with end-stage renal disease. Free Radic Biol Med. 2000;29:454–63.
McElroy A, Silver M, Morrow L, Heafner BK. Proximal and distal muscle weakness in patients receiving hemodialysis for chronic uremia. Phys Ther. 1970;50:1467–81.
Fahal IH, Bell GM, Bone JM, Edwards RH. Physiological abnormalities of skeletal muscle in dialysis patients. Nephrol Dial Transplant. 1997;12:119–27.
Frame B, Heinze EG Jr, Block MA, Manson GA. Myopathy in primary hyperparathyroidism. Observations in three patients. Ann Intern Med. 1968;68:1022–7.
Kopple JD, Cianciaruso B, Massry SG. Does parathyroid hormone cause protein wasting? Contrib Nephrol. 1980;20:138–48.
Patten BM, Bilezikian JP, Mallette LE, et al. Neuromuscular disease in primary hyperparathyroidism. Ann Intern Med. 1974;80:182–93.
Caso G, Garlick PJ. Control of muscle protein kinetics by acid-base balance. Curr Opin Clin Nutr Metab Care. 2005;8:73–6.
Diesel W, Emms M, Knight BK, et al. Morphologic features of the myopathy associated with chronic renal failure. Am J Kidney Dis. 1993;22:677–84.
Stannard SR, Johnson NA. Energy well spent fighting the diabetes epidemic. Diabetes Metab Res Rev. 2006;22:11–9.
Johansen KL, Shubert T, Doyle J, et al. Muscle atrophy in patients receiving hemodialysis: effects on muscle strength, muscle quality, and physical function. Kidney Int. 2003;63:291–7.
Desmeules S, Lévesque R, Jaussent I, et al. Creatinine index and lean body mass are excellent predictors of long-term survival in haemodiafiltration patients. Nephrol Dial Transplant. 2004;19:1182–9.
National Kidney Foundation. K/DOQI clinical practice guidelines for bone metabolism and disease in chronic kidney disease. Am J Kidney Dis. 2003;42(4 Suppl):S1–201.
Komrakova M, Krischek C, Wicke M, et al. Influence of intermittent administration of parathyroid hormone on muscle tissue and bone healing in orchiectomized rats or controls. J Endocrinol. 2011;209:9–19.
Endo I, Inoue D, Mitsui T, et al. Deletion of vitamin D receptor gene in mice results in abnormal skeletal muscle development with deregulated expression of myoregulatory transcription factors. Endocrinology. 2003;144:5138–44.
Vazquez G, de Boland AR, Boland R. Stimulation of Ca2+ release-activated Ca2+ channels as a potential mechanism involved in non-genomic 1,25(OH)2-vitamin D3-induced Ca2+ entry in skeletal muscle cells. Biochem Biophys Res Commun. 1997;239:562–5.
Marantes I, Achenbach SJ, Atkinson EJ, et al. Is vitamin D a determinant of muscle mass and strength? J Bone Miner Res. 2011;26:2860–71.
Holick MF. Environmental factors that influence the cutaneous production of vitamin D. Am J Clin Nutr. 1995;61(3 Suppl):638S–45S.
McKenna MJ. Differences in vitamin D status between countries in young adults and the elderly. Am J Med. 1992;93:69–77.
van der Wielen RP, Löwik MR, van den Berg H, et al. Serum vitamin D concentrations among elderly people in Europe. Lancet. 1995;346:207–10.
Mingrone G, Greco AV, Castagneto M, Gasbarrini G. A woman who left her wheelchair. Lancet. 1999;353:806.
Prabhala A, Garg R, Dandona P. Severe myopathy associated with vitamin D deficiency in western New York. Arch Intern Med. 2000;160:1199–203.
Janssen HC, Samson MM, Verhaar HJ. Vitamin D deficiency, muscle function, and falls in elderly people. Am J Clin Nutr. 2002;75:611–5.
Wanic-Kossowska M, Grzegorzewska A, Plotast H, Bombicki K. Does calcitriol therapy improve muscle function in uremic patients. Perit Dial Int. 1996;16(Suppl 1):S305–8.
Henderson RG, Russell RG, Ledingham JG, et al. Effects of 1,25-dihydroxycholecalciferol on calcium absorption, muscle weakness, and bone disease in chronic renal failure. Lancet. 1974;1:379–84.
Shinzato T, Nakai S, Fujita Y, et al. Determination of Kt/V and protein catabolic rate using pre- and post-dialysis blood urea nitrogen concentrations. Nephron. 1994;67:280–90.
Diamant MJ, Harwood L, Movva S, et al. A comparison of quality of life and travel-related factors between in-center and satellite-based hemodialysis patients. Clin J Am Soc Nephrol. 2010;5:268–74.
Muir SW, Montero-Odasso M. Effect of vitamin D supplementation on muscle strength, gait and balance in older adults: a systematic review and meta-analysis. J Am Geriatr Soc. 2011;59:2291–300.
Gordon PL, Sakkas GK, Doyle JW, Shubert T, Johansen KL. Relationship between vitamin D and muscle size and strength in patients on hemodialysis. J Ren Nutr. 2007;17:397–407.
Bertoli M, Luisetto G, Arcuti V, Urso M. Uremic myopathy and calcitriol therapy in CAPD patients. ASAIO Trans. 1991;37:M397–8.
Gómez-Fernández P. Sánchez Agudo L, Calatrava JM. [Chronic kidney insufficiency and respiratory muscle function. Changes induced by treatment with 1,25(OH)2D3]. Med Clin (Barc). 1990;94:204–7.
Kraemer M. A new model for the determination of fluid status and body composition from bioimpedance measurements. Physiol Meas. 2006;27:901–19.
Tengvall M, Ellegård L, Malmros V, et al. Body composition in the elderly: reference values and bioelectrical impedance spectroscopy to predict total body skeletal muscle mass. Clin Nutr. 2009;28:52–8.
Pietiläinen KH, Kaye S, Karmi A, et al. Agreement of bioelectrical impedance with dual-energy x-ray absorptiometry and MRI to estimate changes in body fat, skeletal muscle and visceral fat during a 12-month weight loss intervention. Br J Nutr. 2013;109:1910–6.
Basile C, Vernaglione L, Di Iorio B, et al. Development and validation of bioimpedance analysis prediction equations for dry weight in hemodialysis patients. Clin J Am Soc Nephrol. 2007;2:675–80.
Hazell TJ, DeGuire JR, Weiler HA. Vitamin D: an overview of its role in skeletal muscle physiology in children and adolescents. Nutr Rev. 2012;70:520–33.
Boland R, de Boland AR, Marinissen MJ, et al. Avian muscle cells as targets for the secosteroid hormone 1,25-dihydroxy-vitamin D3. Mol Cell Endocrinol. 1995;114:1–8.
Zanello SB, Boland RL, Norman AW. cDNA sequence identity of a vitamin D-dependent calcium-binding protein in the chick to calbindin D-9K. Endocrinology. 1995;136:2784–7.
Barton-Davis ER, Shoturma DI, Musaro A, Rosenthal N, Sweeney HL. Viral mediated expression of insulin-like growth factor I blocks the aging-related loss of skeletal muscle function. Proc Natl Acad Sci U S A. 1998;95:15603–7.
Brunner A, de Boland AR. 1,25-Dihydroxyvitamin D3 affects the synthesis, phosphorylation and in vitro calmodulin binding of myoblast cytoskeletal proteins. Z Naturforsch C. 1990;45:1156–60.
Drittanti L, de Boland AR, Boland R. Modulation of DNA synthesis in cultured muscle cells by 1,25-dihydroxyvitamin D-3. Biochim Biophys Acta. 1989;1014:112–9.
Araujo AB, Travison TG, Bhasin S, et al. Association between testosterone and estradiol and age-related decline in physical function in a diverse sample of men. J Am Geriatr Soc. 2008;56:2000–8.
Giannoulis MG, Sonksen PH, Umpleby M, et al. The effects of growth hormone and/or testosterone in healthy elderly men: a randomized controlled trial. J Clin Endocrinol Metab. 2006;91:477–84.
Tanaka M, Yamazaki S, Hayashino Y, et al. Hypercalcaemia is associated with poor mental health in haemodialysis patients: results from Japan DOPPS. Nephrol Dial Transplant. 2007;22:1658–64.
Dumler F, Falla P, Butler R, et al. Impact of dialysis modality and acidosis on nutritional status. ASAIO J. 1999;45:413–7.
Acknowledgments
This work was supported by research grant from the Japan Dialysis Outcome Research Group. All authors have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mori, A., Nishino, T., Obata, Y. et al. The Effect of Active Vitamin D Administration on Muscle Mass in Hemodialysis Patients. Clin Drug Investig 33, 837–846 (2013). https://doi.org/10.1007/s40261-013-0132-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40261-013-0132-7