Abstract
Background
Miconazole is an imidazole antifungal agent that has amply been used in the treatment of superficial mycosis. Preliminary data indicate that miconazole may also induce anticancer effects. As yet, however, little is known about the therapeutic efficacy of miconazole on cancer and the putative mechanism(s) involved. Here, we show that miconazole suppresses hypoxia inducible factor-1α (HIF-1α) protein translation in different cancer-derived cells.
Methods
The effect of miconazole on HIF-1α expression was examined by Western blotting and reverse transcriptase polymerase chain reaction assays in human U87MG and MCF-7 glioma and breast cancer-derived cell lines, respectively. The transcriptional activity of the HIF-1 complex was confirmed using a luciferase assay. To assess whether angiogenic factors are increased under hypoxic conditions in these cells, vascular endothelial growth factor (VEGF) levels were measured by ELISA. Metabolic labeling was performed to examine HIF-1α protein translation and global protein synthesis. The role of the mammalian target of rapamycin (mTOR) signaling pathway was examined to determine translation regulation of HIF-1α after miconazole treatment.
Results
Miconazole was found to suppress HIF-1α protein expression through post-transcriptional regulation in U87MG and MCF-7 cells. The suppressive effect of HIF-1α protein synthesis was found to be due to inhibition of mTOR. Miconazole significantly inhibited the transcriptional activity of the HIF-1 complex and the expression of its target VEGF. Moreover, miconazole was found to suppress global protein synthesis by inducing phosphorylation of the translation initiation factor 2α (eIF2α).
Conclusion
Our data indicate that miconazole plays a role in translational suppression of HIF-1α. We suggest that miconazole may represent a novel therapeutic option for the treatment of cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Hypoxia inducible factor-1 (HIF-1), a critical modulator of the transcriptional response to changes in tissue oxygenation, is a heterodimeric molecule consisting of HIF-1α and HIF-1β. HIF-1 is over-expressed under many pathophysiological conditions, including myocardial infarction, inflammation, and brain, lung, prostate, breast and gynecological cancers [1, 2]. HIF-1α, a transcription factor, is known to regulate various genes involved in metastasis and angiogenesis [3]. Under normoxic conditions, HIF-1α is hydroxylated and subsequently bound to the von Hippel-Lindau (VHL) tumor suppressor protein, leading to its degradation via the ubiquitin-proteasome pathway. Under hypoxic conditions, HIF-1α accumulates and moves to the nucleus where it dimerizes with HIF-1β and activates target genes [4, 5]. HIF-1 activates the expression of several known hypoxia-responsive genes, including VEGF, which encodes vascular endothelial growth factor, a key regulator of angiogenesis [6], GLUT1, which encodes glucose transporter 1 [7], BNIP3, which encodes BCL2/adenovirus E1B 19 kDa protein-interacting protein 3, the expression of which has been shown to be increased in hypoxic regions of human tumors [8], and PFKFB3, which encodes 6-Phosphofructo-2-kinase/fructose-2,6-bisphosphatase-3, a master regulator of glycolysis [9].
Miconazole represents an important antifungal agent of the imidazole derivatives. It has been used worldwide in the treatment of superficial skin fungal infections. The effect of miconazole was previously shown to be attributed to inhibition of the fungal cytochrome P-450 complex, including the 14α-lanosterol demethylase enzyme, which regulates ergosterol biosynthesis essential for fungal cell membrane formation [10]. In addition to ergosterol biosynthesis inhibition in fungal cells, miconazole has also been reported to reduce human osteosarcoma cell viability through Ca2+ mobilization, suppression of steroidogenesis and blocking of Ca2+ activated K+ channels [11].
Recent investigations have shown that miconazole may induce anticancer effects in various human solid tumors, including bone, brain, and colon tumors in animal models [11–13], and that miconazole may dose dependently arrest the cell cycle of tumor cells at the G0/G1 phase [13]. In human osteosarcoma cells, miconazole may increase Ca2+ levels via induction of Ca2+ release from the endoplasmic reticulum, thereby inhibiting the proliferation of these tumor cells. In addition, it has been reported that miconazole is able to induce a reduction in angiogenesis and tumor size in glial tumors in xenograft animal models [12, 13]. To gain further insight into the putative therapeutic efficacy of miconazole on cancer cells, we examined its effects on HIF-1α and the mTOR signaling pathway in U87MG glioma cells and MCF-7 breast cancer cells.
2 Materials and methods
2.1 Cell culture and reagents
U87MG and MCF-7 cells were cultured in Dulbecco’s modified Eagle’s medium, supplemented with 10 % v/v fetal bovine serum (Hyclone), 100 U/ml penicillin and 100 μg/ml streptomycin, at 37 °C in a humidified atmosphere containing 5 % CO2. Hypoxic conditions were induced by incubating cells in a chamber containing 1 % oxygen, 5 % CO2 and 94 % nitrogen at 37 °C. Miconazole, cycloheximide (CHX) and trichloroacetic acid (TCA) were purchased from Sigma. MG132 was purchased from Calbiochem. N-(methoxyoxoacetyl)-glycin methyl ester (DMOG), an inhibitor of prolyl hydroxylase, was obtained from Cayman Chemical. The luciferase assay kit was obtained from Promega, Madison, WI. Lipofectamine 2000 reagent was purchased from Invitrogen. Antibodies against HIF-1α were obtained from BD Bioscience and antibodies against HIF-1β were obtained from Santa Cruz Biotechnology. Antibodies against 4EBP1, p70S6K, RPS6, eIF2α, phospho-p70S6K (Thr421/Ser424), phospho-RPS6, phospho-4EBP1 (Thr37/46), and phospho-eIF2α were purchased from Cell Signaling Technology. Anti-β-actin antibodies were purchased from Sigma.
2.2 Immunoblotting
Cells, resuspended in RIPA lysis buffer (50 mM Tris–HCl, pH 7.4, 150 mM NaCl, 0.1 % SDS, 0.25 % sodium deoxycholate, 1 mM EDTA, 1 mM EGTA, 0.1 % NP-40, plus proteinase inhibitors), were incubated in ice for 10 min, after which non-soluble material was eliminated by centrifugation. Total protein concentrations were determined using the Bradford assay. The samples were then subjected to SDS-PAGE and the proteins were transferred to nitrocellulose membranes as described previously [14]. Non-specific binding was blocked with 5 % skimmed milk for 1 h, after which the membranes were incubated with primary antibodies (1:2000) overnight at 4 °C. Next, the membranes were incubated with secondary antibodies (1:2000) for 90 min at room temperature, and protein bands were visualized using a chemiluminescent reagent (Amersham Bioscience) and exposure to X-ray films or analyzed with LAS 3000 (Fujifilm Co.) using MultiGauge software.
2.3 Reverse transcription polymerase chain reaction (RT-PCR)
Total RNA was extracted from cells using Trizol reagent (Invitrogen). RT-PCR reactions were performed as described previously [15]. The primers used in this study were as follows: (forward primer) 5′-CTCAAAGTCGGACAGCCTCA-3′ and (reverse primer) 5′-CCCTGCAGTAGGTTTCTGCT-3′ for HIF-1α, and (forward primer) 5′-CGTCTTCACCACCATGGAGA-3′ and (reverse primer) 5′-CGGCCATCACGCCACAGTTT-3′ for GAPDH. The PCR products were examined using agarose gel electrophoresis containing ethidium bromide under ultraviolet transillumination.
2.4 Transient transfection and luciferase assays
The hypoxia response element (HRE)-driving firefly luciferase reporter plasmid pGL2-TK-HRE (kindly provided by Dr. Giovanni Melillo) [16] was used to assess luciferase activity. One day before transfection, U87MG and MCF-7 cells were seeded (5 × 104 and 8 × 104, respectively) on 35-mm culture dishes. pGL2-TK-HRE and a renilla luciferase expression plasmid pRL-TK (Promega) were mixed together with Lipofectamine 2000 and transiently co-transfected into cells according to the manufacturer’s instructions. The transfections were allowed to proceed for 16 h, followed by incubation with miconazole for another 4 h. Firefly luciferase and renilla luciferase activities in cell lysates were determined using the Dual-Glo luciferase assay system (Promega), according to the manufacturer’s instructions. The relative luciferase activity was calculated as the ratio of firefly/renilla luciferase activity.
2.5 Quantification of VEGF production
U87MG and MCF-7 cells were cultured in 6-well culture plates at a density of 2 × 105/well. Media were collected after overnight culture and centrifuged at 800 rpm for 4 min at 4 °C to remove cell debris. Culture supernatants were assayed for VEGF using the Quantikine human VEGF ELISA kit from R&D Systems according to the manufacturer’s instructions.
2.6 Metabolic labeling, immunoprecipitation and TCA precipitation
Before metabolic labeling, U87MG and MCF-7 cells were cultured in 60 mm culture dishes at a density of 4.5 × 105 and 1 × 106 cells/dish, respectively. Cells were washed with PBS, starved for methionine/cysteine for 3 h, and treated with miconazole in methionine/cysteine-free DMEM for 21 h. DMOG at a final concentration of 5 mM was then added and cells were incubated for another 30 min. Subsequent labeling was carried out with 35S-methionine/cysteine (GE Healthcare life Science) at a final concentration of 100 μCi/ml in culture medium and cells were incubated for 2 h, washed once with PBS and lysed in RIPA lysis buffer containing protease inhibitors. The resulting lysates were then centrifuged at 13,000 rpm for 15 min at 4 °C. Equal concentrations of 35S-labeled proteins were immunoprecipitated with anti-HIF-1α antibody. The immunoprecipitated proteins were washed and resolved on SDS-PAGE, after which the gels were dried and exposed to X-ray films. Overall protein synthesis was assessed after treatment of cells with indicated concentrations of miconazole, followed by labeling with 35S-methionine/cysteine for 1 h. Next, cell lysates were washed once with PBS and precipitated with 10 % trichloroacetic acid (TCA) for 30 min at 4 °C, after which radioactivity in the cell lysates was examined using a liquid scintillation analyzer (Packard instrument Co). Alternatively, cell lysates were resolved by SDS-PAGE and exposed to X-ray film.
2.7 Statistical analyses
All values were expressed as mean ± SD from three independent experiments. Comparison of results between different groups was performed by student t-test. A P-value ≤ 0.05 was considered to be statistically significant.
3 Results
3.1 Miconazole decreases HIF-1α expression
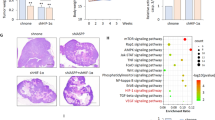
Previously, it has been found that HIF-1α is over-expressed in different cancers, including glioblastoma and breast cancer [17–19]. Based on this information, we selected the glioblastoma and breast cancer cell lines U87MG and MCF-7, respectively, to examine the expression of HIF-1α after miconazole treatment. To assess the effect of miconazole on HIF-1α protein expression, U87MG and MCF-7 cells were treated with various concentrations of miconazole under normoxic and hypoxic conditions. As shown in Fig. 1a, miconazole induced a dose-dependent inhibition of HIF-1α expression, both under normoxic and hypoxic conditions in U87MG cells. A similar effect was observed in MCF-7 cells. The effect of miconazole on HIF-1α appears to be specific, because HIF-1β protein levels did not change after miconazole treatment. Since miconazole at 20 μM concentration resulted in a significant decrease in HIF-1α expression, we treated the cells with 20 μM miconazole and assessed the effect on HIF-1α at different time points. As shown in Fig. 1b, a significant inhibition of HIF-1α expression in both cell lines was observed after 2 h of treatment, and this effect was more pronounced after longer periods of miconazole treatment. This HIF-1α inhibition was observed under both normoxic and hypoxic conditions. Together, these results indicate that miconazole reduces HIF-1α protein expression in a dose- and time-dependent manner. To ascertain whether the observed reductions in HIF-1α protein levels could result from transcriptional inhibition, we performed RT-PCR. This analysis did not reveal any significant changes in HIF-1α mRNA levels in miconazole treated U87MG and MCF-7 cells under both hypoxic and normoxic conditions (Fig. 1c). These latter results suggest that miconazole suppresses HIF-1α protein expression through posttranscriptional regulation.
Miconazole reduces HIF-1α protein expression. a U87MG and MCF-7 cells were cultured in DMEM for 24 h before treatment with indicated concentrations of miconazole for 8 h under normoxic and hypoxic conditions. Protein lysates were assayed by Western blotting and β-actin was used as a loading control. b U87MG and MCF-7 cells were treated with 20 μM miconazole for indicated time points. The cell lysates were subjected to Western blot analysis. c U87MG and MCF-7 cells were treated with miconazole for 20 h under hypoxic conditions. Total RNA was isolated and the mRNA expression level of HIF-1α was determined by RT-PCR
3.2 Miconazole inhibits HIF-1 transcriptional activity
In order to address the question whether the observed suppressed expression of HIF-1α reduces the transcriptional activity of the HIF-1 complex, we next performed a HIF-1 reporter assay. To this end, we treated cells with miconazole under normoxic and hypoxic conditions and, subsequently, assessed the transcriptional activity of HIF-1. As shown in Fig. 2a, miconazole treatment significantly inhibited basal and hypoxia-induced promoter activities in a dose-dependent manner. This effect was seen in both cancer cell lines. Next, we investigated the expression level of VEGF, a target of HIF-1, in U87MG and MCF-7 cells. We found that VEGF protein levels in the culture media were increased under hypoxic conditions, but that these levels were decreased after treatment of the cells with miconazole (Fig. 2b). These results suggest that miconazole can suppress the transcription of HIF-1 downstream genes, such as the angiogenic factor VEGF, through the reduction of HIF-1α protein expression.
Miconazole inhibits the transcriptional activity of HIF-1 and the expression of VEGF. a U87MG and MCF-7 cells were transiently transfected with pGL2-TK-HRE and pRL-TK plasmids, and treated with vehicle or indicated concentrations of miconazole under normoxic and hypoxic conditions. Luciferase activity was assessed 20 h after transfection using Dual-Glo luciferase assay systems. Relative luciferase activity of the HIF-1 target promoter was determined by the ratio of firefly/renilla luciferase activity and normalized to the activity of the control vector. * indicates a significant difference from the vehicle-treated group under normoxic conditions (p < 0.05). # indicates a significant difference from the vehicle-treated group under hypoxic conditions (p < 0.05). b U87MG and MCF-7 cells were treated with miconazole for 8 h under hypoxic conditions. VEGF levels in culture medium were assessed by ELISA. # indicates a significant difference from the vehicle-treated group under hypoxic conditions (p < 0.05)
3.3 Miconazole reduces HIF-1α protein translation
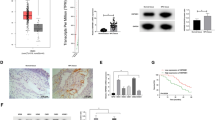
Since we found that miconazole causes inhibition of HIF-1α protein expression, we hypothesized that this effect might be due to reduced HIF-1α protein translation. To test this hypothesis, we assessed the accumulation rate of HIF-1α protein in the presence of miconazole. To this end, U87MG and MCF-7 cells were pretreated with miconazole for 24 h followed by incubation with MG132, a proteasome inhibitor, to block HIF-1α protein degradation. By doing so, we found that miconazole treatment significantly reduces the accumulation rate of HIF-1α in both cell lines (Fig. 3a). As a control, cells only treated with MG132 showed an accumulation of HIF-1α protein in a time-dependent manner. These results suggest that miconazole inhibits HIF-1α protein translation. We next carried out a metabolic labeling assay to substantiate the effect of miconazole on the translation of HIF-1α protein. To this end, U87MG and MCF-7 cells were pretreated with vehicle (control) or 20 μM miconazole and labeled with 35S-methionine/cysteine for 2 h. The metabolic labeling assay was performed in the presence of MG132 to block the degradation of newly synthesized HIF-1α protein. The results show that miconazole significantly inhibits the accumulation of newly synthesized HIF-1α protein (Fig. 3b). Together with the data presented in Fig. 3a, these results suggest that the reduction of HIF-1α expression induced by miconazole is associated with the inhibition of HIF-1α protein translation.
Miconazole inhibits HIF-1α protein translation. a U87MG and MCF-7 cells were pretreated with 20 μM miconazole followed by treatment with proteasomal inhibitor MG132 for 30, 60, 90, and 120 min. Cells were lysed and Western blotting was performed for HIF-1α. Blots were probed with anti-β-actin antibody for equal loading. Lower panels show the quantification of HIF-1α signal intensities by LAS 3000 image analyzer following normalization to β-actin. HIF-1α levels from miconazole untreated cells are considered as 100 %, and the effect of miconazole co-treated with MG132 is represented as relative change. The linear trend from the vehicle treated group is indicated by a solid line. The linear trend from the miconazole treated group is indicated by a dotted line. b Cells were treated with 20 μM miconazole for 24 h under normoxic conditions before the addition of 35S-labeled methionine/cysteine. MG132 was applied simultaneously with 35S-methionine/cysteine to the indicated samples. The lower panel shows the quantification of signal intensities in each lane. c Cells were pretreated with miconazole or vehicle for 24 h, and cycloheximide (CHX) was added for the indicated time periods. Protein extracts were analyzed for the expression of HIF-1α by immunoblot assay. The lower panel shows the quantification of the HIF-1α signal intensities using the same method as under Fig. 3a
It has been reported that HIF-1α protein expression levels are largely determined by a balance between protein synthesis and degradation [20]. We, therefore, tested whether miconazole may affect HIF-1α protein stability in addition to protein synthesis. To this end, U87MG and MCF-7 cells were treated with protein translation inhibitor cycloheximide (CHX) alone or in combination with miconazole. CHX was used to block protein synthesis and, thus, to enable the assessment the half-life of the HIF-1α protein. As shown in Fig. 3c, treatment of miconazole did not induce any significant changes in the half-life of the HIF-1α protein. These results suggest that miconazole inhibits HIF-1α protein expression in U87MG and MCF-7 cells through the inhibition of HIF-1α protein synthesis rather than through the enhancement of its degradation.
3.4 Miconazole inhibits global protein translation
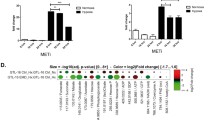
Next, we hypothesized that the inhibitory effect of miconazole on HIF-1α protein translation could be associated with an overall reduction in protein translation. To test this hypothesis, we assessed the effect of miconazole on overall protein synthesis. First, we examined this effect using a TCA precipitation assay. After treatment of miconazole, 35S-methionine/cysteine labeled cell lysates were prepared and the incorporated radioactivity was measured after TCA precipitation. By doing so, a decrease in 35S-methionine/cysteine incorporation was observed in miconazole treated cells (Fig. 4a). Next, 35S-methionine/cysteine incorporated whole cell lysates were subjected to SDS-PAGE. The resulting data again showed that miconazole was able to inhibit overall protein synthesis (Fig. 4b). Taken together, these data suggest that the observed miconazole-mediated decrease in HIF-1α protein translation is associated with an inhibitory effect of miconazole on overall protein translation.
Miconazole suppresses global protein synthesis and inhibits the mTOR signaling pathway. a Cells were pretreated with the indicated concentrations of miconazole for 24 h. Next, 35S-methionine/cysteine was added and the cells were incubated for 1 h. Cells were harvested and proteins from the lysates were precipitated by 10 % trichloroacetic acid (TCA). The level of protein synthesis is shown as a percentage of the value obtained in the absence of miconazole. * indicates a significant difference from the vehicle-treated group. b 35S-labeled methionine/cysteine cells were pretreated with miconazole and harvested. Next, cell lysates were electrophoresed in SDS-PAGE and radioactivity-incorporated material was detected by autoradiography. The right panel shows the quantification of signal intensities in each lane. c Cells were treated with indicated concentrations of miconazole for 20 h under normoxic and hypoxic conditions and, subsequently, cell lysates were subjected to SDS-PAGE and blotted. Membranes were incubated with different antibodies as indicated
The mammalian target of rapamycin (mTOR) is a central regulator of protein translation, cell growth, angiogenesis and metabolism [21]. Activation of mTOR complex 1 (mTORC1) results in phosphorylation of its substrates, such as p70S6 kinase 1 (p70S6K1) and eukaryotic initiation factor 4E-binding protein 1 (4EBP1) [22]. We, therefore, set out to investigate the effect of miconazole treatment on these downstream mTOR signaling targets. By doing so, we found that miconazole treatment causes a dose-dependent decrease in phosphorylation of p70S6K and 4EBP1 (Fig. 4c), which parallels the reduction of HIF-1α protein levels (Fig. 1a). Upon immunoblotting, 4EBP1 is detected as three distinct bands, commonly designated as α (lower), β (middle) and γ (upper). α and β represent the hypophosphorylated forms, whereas γ represents the hyperphosphorylated form [23]. We also found that the downstream target of p70S6K, ribosomal protein S6 (RPS6), was dephosphorylated. These data suggest that miconazole-induced reduction of protein synthesis occurs at the level of translation initiation, and is related to the inhibition of mTOR signaling. A well-known mechanism underlying the inhibition of protein synthesis is the phosphorylation of eIF2α, i.e., phosphorylated eIF2α leads to a global inhibition of mRNA translation initiation [24]. We, therefore, examined whether miconazole may induce the phosphorylation of eIF2α. We indeed found that treatment of miconazole causes an increase in eIF2α phosphorylation in a dose-dependent manner (Fig. 4c), suggesting that miconazole inhibits general protein translation through eIF2α phosphorylation in addition to mTOR inhibition. Collectively, these data suggest that miconazole inhibits global protein translation by modulating the mTOR and eIF2α signaling pathways.
4 Discussion
Miconazole has been shown to affect tumorigenesis through an inhibitory effect on the G0/G1 phase of the cell cycle in various human cancer cells [13, 25]. Although miconazole has been extensively studied as an antifungal agent in cancer patients [26–28], its exact role in the treatment of cancer is largely unknown. Recent reports have increasingly provided evidence for an anticancer effect of miconazole. Miconazole has e.g. been found to cause a dose-dependent increase in tumor latency, a decrease in final tumor incidence and a decrease in tumor multiplicity in animal models [29]. Also, in glial tumors miconazole has been found to significantly inhibit capillary tube formation and tumor size [12]. Here, we show for the first time that miconazole inhibits HIF-1α protein translation and, thereby, inhibits the angiogenic factor VEGF in U87MG and MCF-7 cancer cells.
HIF-1α has been found to be up-regulated in various types of cancer, and to mediate downstream hypoxic and non-hypoxic signaling pathways. Over-expression of HIF-1α is an indicator of poor prognosis in a variety of cancers [30–33]. Our study has uncovered a distinct role of miconazole in the inhibition of HIF-1α and the regulation of signaling pathways involved in the transcription of pro-angiogenic genes. In various cancers, HIF-1α has been found to be expressed at early stages of tumorigenesis and to correlate with the vascular densities of the lesions. Thus, HIF-1 activity may contribute to the angiogenic switch that is associated with the production of pro-angiogenic factors such as VEGF in tumors, leading to high aggressiveness [34]. When HIF-1α synthesis is inhibited, it may hamper angiogenesis and tumor growth. Here, we found that miconazole can inhibit HIF-1α protein translation. Thus, it is reasonable to assume that angiogenesis and tumor growth may be reduced by miconazole-mediated HIF-1α inhibition.
Angiogenesis supports tumor cell proliferation, and inhibition of angiogenesis is considered to be a potent strategy to treat cancer [35]. Several proteins have been identified as angiogenic activators, including VEGF, angiogenin, transforming growth factor (TGF)-α and -β, hepatocyte growth factor (HGF) and epidermal growth factor (EGF) [36]. Among these, VEGF is considered to be the most potent angiogenic factor in cancerous tissues. VEGF activates endothelial cells that produce matrix metalloproteinases (MMPs). These MMPs break down the extracellular matrix and promote the migration of endothelial cells into the surrounding tissues to initiate angiogenesis [37]. Our data indicate that miconazole suppresses VEGF levels and, thus, indicate that miconazole may serve as a novel treatment option for cancer. As of yet, however, the involvement of other angiogenic factors cannot be ignored. This latter notion is in agreement with a report by Rundhang et al. [38] showing that miconazole as an inhibitor of epoxygenase may inhibit angiogenesis under hypoxic conditions. P450 2C11 epoxygenase (CYP epoxygenase) catalyzes epoxyeicosatrienoic acids (EETs) from arachidonic acids. Miconazole has been found to block the formation of EETs by inhibiting epoxygenase and to decrease endothelial tube formation in co-cultures of astrocytes and capillary endothelial cells [12, 39, 40].
HIF-1α levels may be disturbed when its rates of synthesis and/or degradation are altered. The observed increase in the accumulation of HIF-1α after application of the proteasome inhibitor (MG132) indicates that HIF-1α proteins are continuously degraded by the proteasomal system. However, the reduced accumulation of HIF-1α after miconazole treatment supports the notion that miconazole may inhibit the level of HIF-1α by reducing protein translation rather than by increasing HIF-1α protein degradation. HIF-1α translation inhibition may affect the mTOR signaling pathway which, in turn, controls tumor cell growth [41]. Previous work by others has shown that protein synthesis may be inhibited by hypoxia-induced changes in mRNA translation, and that this process is mediated by the mTOR signaling pathway [42, 43]. mTOR is known to act through two different complexes, mTORC1 and mTORC2. The mTORC1 complex regulates protein synthesis through its downstream targets 4EBP1 and S6K. The mTOR effector molecules 4EBP1 and p70S6K are required for tumor growth and angiogenesis through HIF-1 mediated activation and, ultimately, VEGF expression up-regulation [44, 45]. These data are in conformity with our observation that miconazole may inhibit protein translation through dephosphorylation of p70S6K, 4EBP1 and RPS6. Translation inhibition by miconazole may be the major factor in inhibiting HIF-1α protein synthesis. Our findings are in agreement with a previous study showing that mTOR inhibition may lead to a profound attenuation of HIF-1α [46].
It is well-known that eIF2α controls the regulation of eukaryotic protein synthesis at the level of translation initiation. HIF-1α translation regulation is mediated by phosphorylation of eIF2 [47], which forms a ternary complex with GTP and the initiator (Met)-tRNA. During protein synthesis, a transition of eIF2α-GDP to eIF2α-GTP is required for the reformation of ternary translation initiation complexes [48]. Phosphorylation of eIF2α causes a global inhibition of protein synthesis. Our work shows that miconazole inhibits protein synthesis through eIF2α phosphorylation. This observation indicates that under hypoxic conditions miconazole affects gene expression at the level of translation through the eIF2α phosphorylation pathway [14]. We conclude that our results suggest that miconazole initiates translational suppression of HIF-1α through the inhibition of mTOR phosphorylation and the induction of eIF2α phosphorylation.
References
J.J. Lou, Y.L. Chua, E.H. Chew, J. Gao, M. Bushell, T. Hagen, Inhibition of hypoxia-inducible factor-1 alpha (HIF-1alpha) protein synthesis by DNA damage inducing agents. PLoS One 5, e10522 (2010)
A.J. Majmundar, W.J. Wong, M.C. Simon, Hypoxia-inducible factors and the response to hypoxic stress. Mol. Cell 40, 294–309 (2010)
G.L. Semenza, Targeting HIF-1 for cancer therapy. Nat. Rev. Cancer 3, 721–732 (2003)
W.G. Kaelin Jr., The von Hippel-Lindau tumour suppressor protein: O2sensing and cancer. Nat. Rev. Cancer 8, 865–873 (2008)
N. Masson, C. Willam, P.H. Maxwell, C.W. Pugh, P.J. Ratcliffe, Independent function of two destruction domains in hypoxia-inducible factor-alpha chains activated by prolyl hydroxylation. EMBO J. 20, 5197–5206 (2001)
D.J. Manalo, A. Rowan, T. Lavoie, L. Natarajan, B.D. Kelly, S.Q. Ye, J.G. Garcia, G.L. Semenza, Transcriptional regulation of vascular endothelial cell responses to hypoxia by HIF-1. Blood 105, 659–669 (2005)
C.D. Young, A.S. Lewis, M.C. Rudolph, M.D. Ruehle, M.R. Jackman, U.J. Yun, O. Ilkun, R. Pereira, E.D. Abel, S.M. Anderson, Modulation of glucose transporter 1 (GLUT1) expression levels alters mouse mammary tumor cell growth in vitro and in vivo. PLoS One 6, e23205 (2011)
N. Shaida, R. Launchbury, J.L. Boddy, C. Jones, L. Campo, H. Turley, S. Kanga, A.H. Banham, P.R. Malone, A.L. Harris, S.B. Fox, Expression of BNIP3 correlates with hypoxia-inducible factor (HIF)-1alpha, HIF-2alpha and the androgen receptor in prostate cancer and is regulated directly by hypoxia but not androgens in cell lines. Prostate 68, 336–343 (2008)
H. Bando, T. Atsumi, T. Nishio, H. Niwa, S. Mishima, C. Shimizu, N. Yoshioka, R. Bucala, T. Koike, Phosphorylation of the 6-phosphofructo-2-kinase/fructose 2,6-bisphosphatase/PFKFB3 family of glycolytic regulators in human cancer. Clin. Cancer Res. 11, 5784–5792 (2005)
G.E. Piérard, T. Hermanns-Lê, P. Delvenne, C. Piérard-Franchimont, Miconazole, a pharmacological barrier to skin fungal infections. Expert. Opin. Pharmacother. 13, 1187–1194 (2012)
H.T. Chang, W.C. Chen, J.S. Chen, Y.C. Lu, S.S. Hsu, J.L. Wang, H.H. Cheng, J.S. Cheng, B.P. Jiann, A.J. Chiang, J.K. Huang, C.R. Jan, Effect of miconazole on intracellular Ca2+ levels and proliferation in human osteosarcoma cells. Life Sci. 76, 2091–2101 (2005)
D. Zagorac, D. Jakovcevic, D. Gebremedhin, D.R. Harder, Antiangiogenic effect of inhibitors of cytochrome P450 on rats with glioblastoma multiforme. J. Cereb. Blood Flow Metab. 28, 1431–1439 (2008)
C.H. Wu, J.H. Jeng, Y.J. Wang, C.J. Tseng, Y.C. Liang, C.H. Chen, H.M. Lee, J.K. Lin, C.H. Lin, S.Y. Lin, C.P. Li, Y.S. Ho, Antitumor effects of miconazole on human colon carcinoma xenografts in nude mice through induction of apoptosis and G0/G1 cell cycle arrest. Toxicol. Appl. Pharmacol. 180, 22–35 (2002)
M. Bi, C. Naczki, M. Koritzinsky, D. Fels, J. Blais, N. Hu, H. Harding, I. Novoa, M. Varia, J. Raleigh, D. Scheuner, R.J. Kaufman, J. Bell, D. Ron, B.G. Wouters, C. Koumenis, ER stress-regulated translation increases tolerance to extreme hypoxia and promotes tumor growth. EMBO J. 24, 3470–3481 (2005)
H.J. Jung, S.I. Suh, M.H. Suh, W.K. Baek, J.W. Park, Pentamidine reduces expression of hypoxia-inducible factor-1α in DU145 and MDA-MB-231 cancer cells. Cancer Lett. 303, 39–46 (2011)
A. Rapisarda, B. Uranchimeg, D.A. Scudiero, M. Selby, E.A. Sausville, R.H. Shoemaker, G. Melillo, Identification of small molecule inhibitors of hypoxia-inducible factor 1 transcriptional activation pathway. Cancer Res. 62, 4316–4324 (2002)
K.L. Talks, H. Turley, K.C. Gatter, P.H. Maxwell, C.W. Pugh, P.J. Ratcliffe, A.L. Harris, The expression and distribution of the hypoxia-inducible factors HIF-1alpha and HIF-2alpha in normal human tissues, cancers, and tumor-associated macrophages. Am. J. Pathol. 157, 411–421 (2000)
J. Du, R. Xu, Z. Hu, Y. Tian, Y. Zhu, L. Gu, L. Zhou, PI3K and ERK-induced Rac1 activation mediates hypoxia-induced HIF-1α expression in MCF-7 breast cancer cells. PLoS One 6, e25213 (2011)
C. Ercan, J.F. Vermeulen, L. Hoefnagel, P. Bult, P. van der Groep, E. van der Wall, P.J. van Diest, HIF-1α and NOTCH signaling in ductal and lobular carcinomas of the breast. Cell. Oncol. 35, 435–442 (2012)
M. Yee Koh, T.R. Spivak-Kroizman, G. Powis, HIF-1 regulation: not so easy come, easy go. Trends Biochem. Sci. 33, 526–534 (2008)
D.B. Shackelford, D.S. Vasquez, J. Corbeil, S. Wu, M. Leblanc, C.L. Wu, D.R. Vera, R.J. Shaw, mTOR and HIF-1alpha-mediated tumor metabolism in an LKB1 mouse model of Peutz-Jeghers syndrome. Proc. Natl. Acad. Sci. U. S. A. 106, 11137–11142 (2009)
D.C. Fingar, C.J. Richardson, A.R. Tee, L. Cheatham, C. Tsou, J. Blenis, mTOR controls cell cycle progression through its cell growth effectors S6K1 and 4E-BP1/eukaryotic translation initiation factor 4E. Mol. Cell. Biol. 24, 200–216 (2004)
F.H. Pham, P.H. Sugden, A. Clerk, Regulation of protein kinase B and 4E-BP1 by oxidative stress in cardiac myocytes. Circ. Res. 86, 1252–1258 (2000)
R.C. Wek, H.Y. Jiang, T.G. Anthony, Coping with stress: eIF2 kinases and translational control. Biochem. Soc. Trans. 34, 7–11 (2006)
A.D. Rodrigues, D.F. Lewis, C. Ioannides, D.V. Parke, Spectral and kinetic studies of the interaction of imidazole anti-fungal agents with microsomal cytochromes P-450. Xenobiotica 17, 1315–1327 (1987)
M.R. Moody, V.M. Young, M.J. Morris, S.C. Schimpff, In vitro activities of miconazole, miconazole nitrate, and ketoconazole alone and combined with rifampin against Candida spp. and Torulopsis glabrata recovered from cancer patients. Antimicrob. Agents Chemother. 17, 871–875 (1980)
W.M. Jordan, G.P. Bodey, V. Rodriguez, S.J. Ketchel, J. Henney, Miconazole therapy for treatment of fungal infections in cancer patients. Antimicrob. Agents Chemother. 16, 792–797 (1979)
F. Meunier-Carpentier, M. Cruciani, J. Klastersky, Oral prophylaxis with miconazole or ketoconazole of invasive fungal disease in neutropenic cancer patients. Eur. J. Cancer Clin. Oncol. 19, 43–48 (1983)
R.A. Lubet, V.E. Steele, I. Eto, M.M. Juliana, G.J. Kelloff, C.J. Grubbs, Chemopreventive efficacy of anethole trithione, N-acetyl-L-cysteine, miconazole and phenethylisothiocyanate in the DMBA-induced rat mammary cancer model. Int. J. Cancer 72, 95–101 (1997)
H. Zhong, A.M. De Marzo, E. Laughner, M. Lim, D.A. Hilton, D. Zagzag, P. Buechler, W.B. Isaacs, G.L. Semenza, J.W. Simons, Overexpression of hypoxia-inducible factor 1alpha in common human cancers and their metastases. Cancer Res. 59, 5830–5835 (1999)
T. Shibaji, M. Nagao, N. Ikeda, H. Kanehiro, M. Hisanaga, S. Ko, A. Fukumoto, Y. Nakajima, Prognostic significance of HIF-1 alpha overexpression in human pancreatic cancer. Anticancer Res. 23, 4721–4727 (2003)
B. Bachtiary, M. Schindl, R. Potter, B. Dreier, T.H. Knocke, J.A. Hainfellner, R. Horvat, P. Birner, Overexpression of hypoxia-inducible factor 1alpha indicates diminished response to radiotherapy and unfavorable prognosis in patients receiving radical radiotherapy for cervical cancer. Clin. Cancer Res. 9, 2234–2240 (2003)
R. Bos, P. van der Groep, A.E. Greijer, A. Shvarts, S. Meijer, H.M. Pinedo, G.L. Semenza, P.J. van Diest, E. van der Wall, Levels of hypoxia-inducible factor-1alpha independently predict prognosis in patients with lymph node negative breast carcinoma. Cancer 97, 1573–1581 (2003)
G. Powis, L. Kirkpatrick, Hypoxia inducible factor-1alpha as a cancer drug target. Mol. Cancer Ther. 3, 647–654 (2004)
M. Malecki, P. Kolsut, R. Proczka, Angiogenic and antiangiogenic gene therapy. Gene Ther. 12(Suppl 1), S159–S169 (2005)
N. Nishida, H. Yano, T. Nishida, T. Kamura, M. Kojiro, Angiogenesis in cancer. Vasc. Health Risk Manag. 2, 213–219 (2006)
J.E. Rundhaug, Matrix metalloproteinases, angiogenesis, and cancer. Clin. Cancer Res. 9, 551–554 (2003)
M. Medhora, J. Daniels, K. Mundey, B. Fisslthaler, R. Busse, E.R. Jacobs, D.R. Harder, Epoxygenase-driven angiogenesis in human lung microvascular endothelial cells. Am. J. Physiol. Heart Circ. Physiol. 284, H215–H224 (2003)
C. Zhang, D.R. Harder, Cerebral capillary endothelial cell mitogenesis and morphogenesis induced by astrocytic epoxyeicosatrienoic acid. Stroke 33, 2957–2964 (2002)
D.H. Munzenmaier, D.R. Harder, Cerebral microvascular endothelial cell tube formation: role of astrocytic epoxyeicosatrienoic acid release. Am. J. Physiol. Heart Circ. Physiol. 278, H1163–H1167 (2000)
R.J. Shaw, L.C. Cantley, Ras, PI(3)K and mTOR signalling controls tumour cell growth. Nature 441, 424–430 (2006)
A. Rapisarda, G. Melillo, UVC inhibits HIF-1alpha protein translation by a DNA damage- and topoisomerase I-independent pathway. Oncogene 26, 6875–6884 (2007)
E. Connolly, S. Braunstein, S. Formenti, R.J. Schneider, Hypoxia inhibits protein synthesis through a 4E-BP1 and elongation factor 2 kinase pathway controlled by mTOR and uncoupled in breast cancer cells. Mol. Cell. Biol. 26, 3955–3965 (2006)
C.X. Bian, Z. Shi, Q. Meng, Y. Jiang, L.Z. Liu, B.H. Jiang, P70S6K 1 regulation of angiogenesis through VEGF and HIF-1alpha expression. Biochem. Biophys. Res. Commun. 398, 395–399 (2010)
D.A. Guertin, D.M. Sabatini, Defining the role of mTOR in cancer. Cancer Cell 12, 9–22 (2007)
K.X. Knaup, K. Jozefowski, R. Schmidt, W.M. Bernhardt, A. Weidemann, J.S. Juergensen, C. Warnecke, K.U. Eckardt, M.S. Wiesener, Mutual regulation of hypoxia-inducible factor and mammalian target of rapamycin as a function of oxygen availability. Mol. Cancer Res. 7, 88–98 (2009)
K. Zhu, W. Chan, J. Heymach, M. Wilkinson, D.J. McConkey, Control of HIF-1alpha expression by eIF2 alpha phosphorylation-mediated translational repression. Cancer Res. 69, 1836–1843 (2009)
C. Koumenis, C. Naczki, M. Koritzinsky, S. Rastani, A. Diehl, N. Sonenberg, A. Koromilas, B.G. Wouters, Regulation of protein synthesis by hypoxia via activation of the endoplasmic reticulum kinase PERK and phosphorylation of the translation initiation factor eIF2alpha. Mol. Cell. Biol. 22, 7405–7416 (2002)
Acknowledgments
We would like to thank Dr. Giovanni Melillo (National Cancer Institute, Frederick, MD, USA) for providing the pGL2-TK-HRE plasmid. This research was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF), funded by the Ministry of Education, Science and Technology (NRF-2011-0013913).
Conflict of interest
All authors of this manuscript declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Jee-Young Park and Hui-Jung Jung contributed equally to this work.
Rights and permissions
About this article
Cite this article
Park, JY., Jung, HJ., Seo, I. et al. Translational suppression of HIF-1α by miconazole through the mTOR signaling pathway. Cell Oncol. 37, 269–279 (2014). https://doi.org/10.1007/s13402-014-0182-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-014-0182-8