Abstract
The rapid advancement in the area of microRNAs (miRNAs) from discovery to their translation into therapeutic moieties reflects their significance as important regulators in the management of disease pathology. The miRNAs can potentially be a new class of drugs in the near future for the treatment of various lung diseases, but it lacks the current knowledge how these identified therapeutic moieties can be designed into an effective, patient complaint and targeted drug delivery system. miRNAs have characteristic features like small size and low molecular weight which makes them easily translated into an effective drug delivery system. In this review, we have summarised the concept of miRNAs and different approaches which can be employed to deliver miRNAs effectively and safely to the target cells including the challenges associated with their development in particular emphasis on pulmonary diseases. Such approaches will be of interest for both the biological and formulation scientists to understand and explore the new vistas in the area of miRNA delivery for pulmonary inflammatory diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
MicroRNAs (miRNAs) are short non-coding RNAs which control gene expression post-transcriptionally by directly blocking translation of their target messenger RNAs (mRNAs) or by repressing protein production via mRNA destabilisation [1]. miRNAs have been identified in contributing an integral role in the post-transcriptional regulation of gene expression, which are generated by endogenous sources of nucleic acids. They regulate various biological processes (cell differentiation and growth, metabolism, cell signalling, apoptosis) related to cancer and inflammation [2]. miRNAs are the novel potential candidates for targeted therapeutic approaches and also employed as biomarkers for various diseases like cancer and chronic inflammatory diseases [3–5].
Biogenesis of miRNAs
The miRNA biogenesis commences with the (1) transcription of the miRNAs by RNA polymerase II to generate (2) Pri-miRNAs, the stem loop structures which are fragmented by RNase III enzyme Drosha and double-stranded RNA-binding domain (dsRBD) protein DGCR8/Pasha converting into hairpin precursor pre-miRNA. (3) The excised pre-miRNA is transported to the cytoplasm by Exportin −5 via Ran-GTP-dependant mechanism, where its (4) cleaving occurs by Dicer protein which generates miRNA duplex containing mature miRNA strand and various accessory protein assemblies. This duplex is incorporated in RNA-induced silencing complex (RISC) (2) to engage the post-transcriptional regulation of target mRNA translation [6–16] (Fig. 1) (adapted from reference 18)
.
There are various miRNAs which are already in the therapeutic development process [17]. Some of them are miR-122 for hepatitis C virus, which is phase 2 clinical trials along with miR-208/499 and miR-34 for chronic heart failure and cancer, respectively, which are under the pre-clinical development phase.
miRNAs in lung diseases
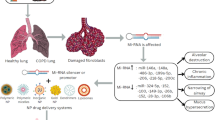
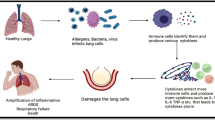
The various signalling pathways which are activated during the advancement of the inflammation in lungs involve miRNAs, and its role involving the innate and adaptive immunity depicts its potential function in regulating the inflammatory diseases such as asthma and COPD [18]. So far, only some miRNAs have been identified which are associated with specific inflammatory diseases and their underlying mechanisms; however, their molecular targets are yet to be identified. The various miRNAs which are involved in the inflammatory airway diseases are shown in Table 1.
The various experimentally verified targets for different miRNAs associated with the chronic lung diseases include IL-6 [38], IFNB1 [39], TLR4 [40], TGF-β pathway [41–43], phosphoinositide 3-kinase (PI3K)/Akt pathway [44], IL-10 [45], IL-13 [46], IL-12A [47], glycogen synthase kinase 3 beta (GSK3B) [19] and IL-10 [21, 25].
Rats exposed to the cigarette smoke have shown downregulation of 24 miRNA expressions (especially let-7 family, miR-10, miR-26, miR-30, miR-34, miR-99, miR-122, miR-123, miR-124, miR-125, miR-140, miR-145, miR-146, miR-191, miR-192, miR-219, miR-222 and miR-223) in comparison to control group. miR-294, inhibitor of transcriptional repressor genes, was the only upregulated in smoke-exposed rats [48]. In a different study with bronchial airway, epithelial cells have shown the downregulation of miRNAs in smokers especially miR-218, miR-15a, miR-199b, miR-125a/b and miR-294 as compared to non-smokers. Similar results were obtained (downregulation of miR-218) with lung squamous cell carcinoma [49].
Many pre-clinical and clinical trials have been up and running so as to investigate the capacity of miRNAs in improving disease pathophysiology. These attempts have thus produced adequate mechanistic data which shows that miRNAs play a critical role in regulating disease-related pathways.
Various miRNAs are already in the therapeutic development phase (pre-clinical), which include let-7 for lung cancer, miR-34 for lung cancer and prostate cancer, miR-29 for cardiac fibrosis and miR-122 for hepatitis C virus [50–54].
miRNA mimics including Let-7 [19, 20] and miR-34 [52, 64] have been demonstrated efficacious in wide variety of solid tumours in mice models of cancer. The therapeutic efficacy was assessed based on the effect of miRNA on proliferation and apoptosis of tumour cells, as well as a specific repression of oncogenes.
In contrast, miRNA antagonist approach (antagomirs) for miR-208, miR-499 and miR-195 has been shown to be beneficial in chronic heart diseases, where administration of these antagomirs ameliorated the disease features such as cardiomyocyte hypertrophy, fibrosis and stress-induced expression of β-myosin heavy chain (β-MHC) and hypothyroidism in respective mouse models. The various identified miRNAs with their therapeutic indication and clinical trial status are shown in Table 2.
The inclusion of miRNAs in lung cancer has already been shown; however, the role of miRNAs in inflammatory airway disease is still unknown and under investigations. Despite that, there are various literature available showing the therapeutic potential of miRNAs in the treatment of inflammatory airway diseases, but very limited literature is available with the potential drug delivery systems that can be employed as a carrier to administer the miRNAs effectively to the patients. Some of the published in vivo delivery strategies for cancer therapy are shown in Table 3.
Despite that, number of miRNAs been identified in various diseases to target in order to control the disease features; the main hindrance is the translation of these identified biological moieties into an effective drug delivery. This mini review enlists identified miRNAs in the treatment of pulmonary diseases, approaches which have been employed to deliver miRNAs effectively and safely to the target cells along with the challenges associated with their development. MiRNAs have characteristic features like small size and low molecular weight, which makes them easily translated into an effective drug delivery system.
Methods to manipulate the use of miRNAs in treatment of disease pathology
There are two main approaches been used to modulate the miRNAs in various diseases. One approach is focussed on inhibiting the elevated microRNA involved in the pathogenesis of disease using miRNA antagonists such as synthetic anti-miRNAs, which are also known as locked nucleic acids (LNAs), and the another approach include the use of miRNA sponges (miR-SP), which are employed to sequester the mis-expressed miRNAs. The second approach is primarily used for miRNAs involved with various targets [65].
Challenges associated with miRNA delivery
There are various challenges associated with the miRNA delivery, which includes [66] poor permeation of miRNAs into tumour tissues due to mechanical and biological barriers, unmodified mircoRNA antagonists and microRNA mimics are quickly degraded and cleared in the blood circulation; potential to induce immunotoxicity and neurotoxicity, poor intracellular delivery and aggregation within the endosomes of naked miRNAs result in inefficient gene silencing; and various off-target effects and insufficient and saturated microRNA processing enzymes lead to dysfunction of therapeutic miRNAs. In order to design an optimised, stable and effective pulmonary drug delivery system containing miRNA, it requires the following three important aspects: lung biology, drug delivery mode or device and nature of therapeutic moiety or drug. All three parameters are interdependent.
Approaches to overcome the barriers associated with delivery of miRNAs
There are various biological and physico-chemical factors associated, which minimise the effective delivery of miRNAs (Fig. 2) to the target cells [67]. The important associated hindrances and their solution includes
-
1.
Degradation and elimination of miRNAs by nuclease, renal clearance and phagocytic immune cells can be minimised by optimising the particle size, surface charge and chemical modification of the miRNAs or by delivering the miRNAs locally.
-
2.
Poor permeation of miRNAs through tissues and cells can be achieved by employing various targeting ligands and cell-penetrating moieties.
-
3.
Intracellular disposition of the miRNAs can be avoided by using fusogenic peptides.
In vivo delivery of miRNAs
miRNA-based therapeutics with various anti-cancer drugs have been already investigated [66], employing different vehicles like local delivery which includes intratumoral injection of miRNA vectors to the nanoparticle formulation, systemic delivery, modified miRNAs antagonist and miRNA mimics, the 2′OH group modification, LNA modification, the passenger and strand modifications, viral (using viruses such as lentiviruses, adenoviruses and adeno-associated viruses (AAVs) and non-viral delivery, inorganic (gold, carbon and silica) nanoparticles, polymer (poly (lactic-co-glycolic acid) or PLGA and PEI) based delivery such as nanoparticles and lipid based such as liposomes and solid-lipid nanoparticles (SLNs) (Fig. 3).
The basic principle involved in the delivery of miRNAs includes the association of the particulated nanocarrier [lipid vesicles (liposomes), polymeric nanoparticles, gold nanoparticles, dendrimers and micelle] with the identified miRNA, which ultimately forms a complex as a multifunctional nanocarrier. This nanocarrier will deliver the miRNA to the target tissue (Fig. 4).
The above listed approaches are already being successful with various drugs employed for the treatment of respiratory diseases. There are various drug delivery systems which can easily be used for miRNA delivery. Some of the published reports with drug delivery systems employed for the drugs associated to respiratory diseases are listed below.
Rifampicin-encapsulated liposome suspensions were formulated and converted them into dry powders by freeze-drying. These liposomes were non-toxic to bronchial epithelial cells, small airway epithelial and alveolar macrophages (AMs). Also, the liposomes did not activate alveolar macrophages (AMs) to produce interleukin-1β, tumour necrosis factor-α and nitric oxide at a level that would cascade to other inflammatory effects [68].
Similar effects were also observed with the prepared proliposome powders containing isoniazid (INH) [69], levofloxacin (LEV) [70] and pyrazinamide (PZA) [71] in a dry powder aerosol form using spray drying method with an aim of having INH and LEV-proliposomes as an alternative for pulmonary tuberculosis treatment to be delivered to the lower airways.
Furthermore, another derivative of pyrazinamide, pyrazinamide (PZA)-L-leucine, was also formulated as nanospray in the form of dry powders for the pulmonary tuberculosis treatment [72].
Also, for the treatment of multidrug-resistant tuberculosis, a dimple-shaped chitosan carrier was developed to deliver ethambutol dihydrochloride (EDH) using nanospray drying, which reveals that these chitosan carriers can effectively be used in a dry powder inhaler which can minimise the possible side effects associated with pure EDH [73].
Amphotericin B (AmB) is considered as a gold standard for therapy against invasive fungal diseases; an attempt has been made to prepare its dry powder inhalers using a new excipient sodium deoxycholate sulphate (SDS) in order to enhance its solubility and ultimately its bioavailability. The prepared SDS–lipid-based nanoparticles of AmB were having significantly reduced toxicity to alveolar macrophage cells as compared to pure AmB. These SDS–lipid-based nanoparticles had the potential to be used as an alternative option to FungizoneR for an AmB formulation for inhalation [74].
Another attempt with AmB is development of AmB-lipid formulations, a lyophilised system using freeze-drying. The prepared formulations have also shown lesser toxicity to the kidney cells by the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay along with less production of nitric oxide as compared to pure AmB. Permeation studies revealed twofold to fivefold higher permeation with the prepared formulations sue to presence of lipid bilayer as compared to pure AmB. The prepared formulation may be a potential approach for the treatment of invasive pulmonary aspergillosis by targeting alveolar macrophages [75].
Lung cancer treatment was studied by formulating nanoparticles using gelatin type A (GA) and gelatin type b (GB) releasing cordycepin, which is an effective and non-invasive material for the treatment of lung cancer cells. The higher amount of the cordycepin release was observed with prepared GA nanoparticles due to large surface area of small size nanoparticles as compared to GB. Nanoparticles in turn have shown higher anti-proliferative and anti-migratory effects on A549 lung cancer cells [76].
Despite that, ipratropium bromide and fenoterol hydrobromide inhaler formulations are available in the market, but still, the factors affecting stability of these drugs together in a single formulation are not clear. Taking into consideration this fact, pressurised metered micronised ipratropium bromide and micronised fenoterol hydrobromide pressurised metered dose inhalers were prepared and tested for their stability and performance by evaluating their various factors such as vapour pressure and dielectric constants of the propellant and cosolvent mixture so as the drugs can get aerosolised properly, physical stability and dose uniformity. All the prepared formulations have demonstrated good physico-chemical properties and stability profile [77].
Another recent advancement in the drug delivery for pulmonary administration includes the development of triggered-release lipid nanocapsules (LNCs), which are the semi-rigid spherical capsules with a triglyceride core, which is a good site to trap pulmonary drugs which have poor aqueous solubility. LNCs were prepared using phase-inversion temperature method, where their main aim was to investigate the kinetics of the LNCs following administration into mouse lungs in presence and absence of bacterial lipopolysaccharide (LPS) and where they have shown that the lung clearance of LNCs was unaffected by the presence of acute lung inflammation [78, 79].
Recent advancements in pulmonary drug delivery: therapeutic implications of pulmonary nanoformulations
In order to further improve the mechanism of the pulmonary absorption of the drug through nanoparticles as drug delivery various studies have been carried out, one of the recent published literature have shown that nanoparticles when inhaled normally deposit in the lungs, which they have to transit through respiratory tract lining fluid (RTLF), where the nanoparticles have interaction with the RTLF, where they have identified the biomolecular corona formation in RTLF which is necessary to be considered for an optimised design of inhalers containing nanomedicines in order to have acceptable safety and tailored clearance profiles (Fig. 5) [80, 81].
The corona normally contains a substantial contribution from various innate immunity proteins like surfactant protein A, napsin A and complement (C1q and C3) proteins. The formation of corona around the drug carriers is not considered with positive prospective, but the recent studies have shown that the developed corona can be employed as a “sponge” in order to load the drugs to achieve targeted effects. One of a such study includes the loading of anti-cancer drugs doxorubicin and meloxicam that have shown improved anti-proliferative effect on MG-63 cells when they were loaded into the corona formed around silica nanoparticles [82]. Such advancements have open new vistas in the area of pulmonary drug delivery.
Another important biological component which might influence the disposition of inhaled drugs is P-glycoprotein (P-gp) in the respiratory epithelium. It is still unclear and under investigation. One of a study with pulmonary absorption of digoxin in mdr1a-deficient and mdr1a-competent mice have shown that no difference in the rate of absorption was observed between these two mice, which shows that P-gp have little effect on the disposition of digoxin [83].
By understanding the phenomenon such as biomolecular corona, P-glycoprotein, etc., which are involved in absorption of drugs from various novel drug delivery systems (nanoparticles and polymeric advanced drug delivery systems), can have a great biological and therapeutic implications in designing stable and effective pulmonary drug delivery systems.
Also, with advancement in the in vitro techniques using various human respiratory epithelial cell cultures like 16HBE14o- and Calu-3, and primary cultured human alveolar type I-like cells (hAEpC) aids in having better understanding of in vitro-in vivo correlation of pulmonary absorption of drugs in order to understand the formulation behaviour and to design an effective and targeted drug delivery system [84].
Ciprofloxacin liposomal formulations were formulated with an objective to improve lung residence time, improved patient compliance and avoiding multiple daily administration of inhaled anti-microbial therapy. The drug release from the liposomal formulations was observed using membrane diffusion, air interface Calu-3 cells and isolated perfused rat lungs as in vitro and ex vivo methods. The drug release was quite consistent with all the methods and easily correlated with in vivo profiles [85]. Another example includes the drug permeability testing of 10 low-molecular-weight compounds in 16HBE14o- airway cell layers, which is correlated with the isolated perfused rat lung [86]. The application of such in vitro and ex vivo methods is the robust approach to understand the mechanism and in vivo pharmacokinetics of drug delivery systems in lesser time.
Also, another approach for the targeted drug delivery comprises of cationic lipoplexes for the lung cancer treatment by encapsulating microRNA-29b in the lipoproteins, which were tested on the murine model and demonstrated that the lipoplexes accumulate on the tumour site showing its targeted efficiency [87].
Another recent development which is still under investigation includes microvesicles and exosomes. These are the cell-derived membrane vesicles (CMVs) which are endogenous carriers and can help in transporting proteins and nucleic acids. They play an important role in the treatment of various inflammatory diseases, where the delivery of the biological moiety to the site of action is crucial. Both exosomes and microvesicles have various advantages over the other drug delivery systems. Further investigations are required unpinning the tissue homing of the CMVs so as to discover the components required for the organ- and cell-specific targeting behaviour along with its long circulation, reduce nonspecific uptake, release inside the cells and low immunogenicity. Unrevealing these features can help in designing artificial CMV-inspired, nanosized drug delivery systems [88, 89].
Other published targeted drug delivery of various miRNAs
Various studies have already been carried out on the miRNAs targeted delivery using different novel drug delivery systems which can be employed as a platform for the pulmonary drug delivery. One of the recent attempts to deliver anti-sense microRNA-21 using PLGA nanoparticles for cancer treatment was made in order to enhance the effects of temozolomide (TMZ) on glioblastoma cells which exhibit high IC50 value for TMZ. These PLGA nanoparticles as a cotherapeutic strategy carrying anti-sense mir-21 were found to be effective for intracellular delivery and sustained release of anti-sense miR-21 in knocking down the increased levels of miR-21 prior to TMZ treatment [90].
Another attempt has been made using anti-sense-miR-21-PS (as anti-apoptosis inducer) and anti-sense-miR-10b-PS (metastasis inducer) loaded in polymer nanoparticles for the triple-negative breast cancer, where the targeted delivery has been achieved showing substantial reduction in the tumour growth at a very low dose of 0.15 mg/kg as compared to the control/placebo nanoparticles showing the importance of this drug delivery as a potential for the treatment of triple-negative breast cancer [91].
Similarly, the systemic delivery of anti-sense peptide, anti-miR-155, in a unique polymer nanoparticle system have shown reduction in the levels of increased miR-155 controlling in vivo the growth of “addicted” pre-B cell tumours, which conclude a promising drug delivery system for the treatment of lymphoma/leukaemia [92].
MicroRNA-29b drug delivery system for the targeted drug delivery in the form of transferrin-conjugated anionic lipopolyplex nanoparticles was prepared as a novel treatment for acute myeloid leukaemia. The prepared nanoparticles have shown more than 200-fold increase of mature miR-29b in comparison to free miR-29b, which were efficient than the non-transferrin-conjugated NP-miR-29b [93].
All the above-cited attempts can be used as platforms in translating the miRNA-based drug delivery systems for various pulmonary diseases. Apart from miRNAs, small interfering RNA (siRNA) are also gaining popularity in the treatment of various lung diseases, for which the similar drug delivery systems (lipid vesicles and nanoparticles) have been employed, which are successfully in clinical trials. Such evidences show that these vehicles can also be employed successfully for the delivery of miRNAs to control the disease pathology [94, 95].
Various siRNAs which are under clinical trials include Atu027, TKM-ApoB, TKM-PLK1, ALN-VSP02 and ALN-TTR01 as lipid nanoparticles and siG12D LODER as biodegradable polymer matrix [96, 97].
microRNA-responsive drug delivery systems
Keeping the ideal characteristics like zero premature release, targeted recognition and controlled release which are expected from a drug delivery system to deliver biologicals, Zhang et al. [98] have developed and reported traceable and aptamer-targeted drug nanocarrier containing doxorubicin (Dox) by capping mesoporous silica-coated quantum dots with a programmable DNA hybrid by forming 12 base pairs between parts of anti-miR-21 and the anchor DNA on the nanoparticles to form a DNA gate to prevent leaking of Dox, and the release of drug was controlled by microRNA. When the nanocarrier was delivered to the HeLa cells by the processes like endocytosis and aptamer-mediated recognition, it gets unlocked by the overexpressed miR-21 by competitive hybridisation leading to the sustained lethality of HeLa cells (Fig. 6). This approach is very novel in various inflammatory conditions, where some miRNAs overexpressed, and this overexpression can be employed as mechanism by using blend of chemotherapy and gene therapy for a targeted treatment for inflammatory diseases with maximal therapeutic efficacy and lesser side effects.
In nutshell, miRNAs are novel potential candidates for targeted therapeutic approaches and also employed as biomarkers for various diseases like cancer and chronic inflammatory diseases. They have been identified to regulate various biological processes like cell differentiation and growth, metabolism, cell signalling, apoptosis in different cancers and inflammatory diseases, one of which is pulmonary diseases. Attempts are currently in progress to identify miRNAs for the treatment of pulmonary diseases along with strategies focussing on their safe and effective delivery to the target cells in vivo. Some of the delivery approaches that are gaining attention include nanoparticles, liposomes, nanocapsules, gold nanoparticles, dendrimers and micelle, microvesicles and exosomes; however, the development of suitable miRNA formulation is still a challenge.
Despite the advancements observed in pharmaceutical and medical biotechnologies, the understanding in context to the in vivo delivery of miRNA is still very limited. It requires further thorough investigations so as to design an optimised, stable and effective pulmonary drug delivery system containing miRNA. Fundamentally, three important interdependent features that play a critical role in formulating an optimised, effective in vivo miRNA drug delivery system include lung biology, drug delivery mode or device and nature of therapeutic moiety or drug. This review article will be beneficial to the researchers involved/getting involved in miRNA research, a platform to understand the importance of miRNAs as drug delivery; the challenges associated in order to select the best drug delivery mode so as to achieve maximal targeting and efficacy.
Conclusions and prospects
miRNA-based therapy provides a promising platform for the treatment of various pulmonary diseases. Pulmonary drug delivery has various associated advantages like non-invasive, locally restricted (targeted drug delivery) and better patient compliance as it can be administered by the patient itself. Also, anti-miRNA therapy, where the anti-miR oligonucleotide is chemically modified, is a potential therapy which can be delivered without delivery vectors for different miRNAs, which are already in the clinical trial phases.
The main limitation is the translation of identified therapeutic miRNAs into the clinic is due to the absence of appropriate formulation delivery systems. With the recent advancements and technology, various novel drug delivery systems such as nanoparticles, liposomes, niosomes, dendrimers and micelles can be effectively and safely used as a vehicle for the miRNA delivery. Also, the recent discoveries like triggered-release lipid nanocapsules, sponges and biomolecular corona further advance the horizons and understanding of advanced drug delivery for miRNAs.
These novel approaches of drug delivery may open new vistas for potential miRNAs in the pulmonary clinic by designing various advanced drug delivery systems, which can have improved clinical outcome.
References
Greene CM, Gaughan KP. miRNAs in asthma: potential therapeutic targets. Curr Opin Pulm Med. 2013;19:66–72.
Schickel R, Boyerinas B, Park SM, Peter ME. MiRNAs: key players in the immune system, differentiation, tumorigenesis and cell death. Oncogene. 2008;27:5959–74.
Griffiths-Jones S. The microRNA registry. Nucleic Acids Res. 2004;32:D109–11.
Griffiths-Jones S, Grocock RJ, van Dongen S, Bateman A, Enright AJ. miRBase: microRNA sequences, targets and gene nomenclature. Nucleic Acids Res. 2006;34:D140–4.
Weiland M, Gao XH, Zhou L, Mi QS. Small RNAs have a large impact: circulating miRNAs as biomarkers for human diseases. RNA Biol. 2012;9:850–9.
Borchert GM, Lanier W, Davidson BL. RNA polymerase III transcribes human miRNAs. Nat Struct Mol Biol. 2006;13:1097–101.
Chen CZ, Li L, Lodish HF, Bartel DP. MiRNAs modulate hematopoietic lineage differentiation. Science. 2004;303:83–6.
Cullen BR. Transcription and processing of human microRNA precursors. Mol Cell. 2004;16:861–5.
Lee Y, Ahn C, et al. The nuclear RNase III Drosha initiates microRNA processing. Nature. 2003;425:415–9.
Landthaler M, Yalcin A, Tuschl T. The human DiGeorge syndrome critical region gene 8 and its D. melanogaster homolog are required for miRNA biogenesis. Curr Biol. 2004;14:2162–7.
Yi R, Qin Y, Macara IG, Cullen BR. Exportin-5 mediates the nuclear export of pre-miRNAs and short hairpin RNAs. Genes Dev. 2003;17:3011–6.
Bohnsack MT, Czaplinski K, Gorlich D. Exportin 5 is a RanGTP-dependent dsRNA-binding protein that mediates nuclear export of pre-miRNAs. RNA. 2004;10:185–91.
Lund E, Guttinger S, Calado A, Dahlberg JE, Kutay U. Nuclear export of microRNA precursors. Science. 2004;303:95–8.
Grishok A et al. Genes and mechanisms related to RNA interference regulate expression of the small temporal RNAs that control C. elegans developmental timing. Cell. 2001;106:23–34.
Hutvagner G, McLachlan J, Pasquinelli AE, Balint E, Tuschl T, Zamore PD. A cellular function for the RNA interference enzyme dicer in the maturation of the let-7 small temporal RNA. Science. 2001;293:834–8.
Zhang H, Kolb FA, Brondani V, Billy E, Filipowicz W. Human dicer preferentially cleaves dsRNAs at their termini without a requirement for ATP. EMBO J. 2002;21:5875–85.
Andrew GB, Paul L, The therapeutic potential of miRNAs, Innovations in Pharmaceutical Technology, 52–55
Plank M, Maltby S, Mattes J, Foster PS. Targeting translational control as a novel way to treat inflammatory disease: the emerging role of MiRNAs. Cli Exp All. 2013;43:981–99.
Polikepahad S et al. Proinflammatory role forlet-7 miRNAs in experimental asthma. J Biol Chem. 2010;285:30139–49.
Kumar M et al. Let-7 microRNA-mediated regulation of IL-13 and allergic airway inflammation. J Allergy Clin Immunol. 2011;128:1077–85.
Lu TX, Munitz A, Rothenberg ME. MicroRNA-21 is up-regulated in allergic airway inflammation and regulates IL-12p35 expression. J Immunol. 2009;182:4994–5002.
Lu TX, Hartner J, Lim EJ, et al. MicroRNA-21 limits in vivo immune response mediated activation of the IL-12/ IFN-gamma pathway, Th1 polarization, and the severity of delayed-type hypersensitivity. J Immunol. 2011;187:3362–73.
Liu G, Friggeri A, Yang Y, et al. miR-21 mediates fibrogenic activation of pulmonary fibroblasts and lung fibrosis. J Exp Med. 2010;142:663–72.
Kuhn AR, Schlauch K, Lao R, Halayko AJ, Gerthoffer WT, Singer CA. MicroRNA expression in human airway smooth muscle cells: role of miR-25 in regulation of airway smooth muscle phenotype. Am J Respir Cell Mol Biol. 2009;42:506–13.
Mohamed JS, Lopez MA, Boriek AM. Mechanical stretch up-regulates microRNA-26a and induces human airway smooth muscle hypertrophy by suppressing glycogen synthase kinase-3beta. J Biol Chem. 2010;285:29336–47.
Sharma A et al. Antagonism of mmu-mir-106a attenuates asthma features in allergic murine model. J Appl Physiol. 2012;113:459–64.
Mattes J, Collison A, Plank M, Phipps S, Foster PS. Antagonism of microRNA- suppresses the effector function of TH2 cells and the development of allergic airways disease. Proc Natl Acad Sci U S A. 2009;106:18704–9.
Collison A, Herbert C, Siegle JS, Mattes J, Foster PS, Kumar RK. Altered expression of microRNA in the airway wall in chronic asthma: miR-126 as a potential therapeutic target. BMC Pulm Med. 2011;11:29.
Oglesby IK, Bray IM, Chotirmall SH, et al. miR-126 is downregulated in cystic fibrosis airway epithelial cells and regulates TOM1 expression. J Immunol. 2010;184:1702–9.
Xie T, Liang J, Liu N, et al. MicroRNA-127 inhibits lung inflammation by targeting IgG Fc gamma receptor I. J Immunol. 2012;188:2437–44.
Chiba Y, Tanabe M, Goto K, Sakai H, Misawa M. Down-regulation of miR-133a contributes to up-regulation of Rhoa in bronchial smooth muscle cells. Am J Respir Crit Care Med. 2009;180:713–9.
Collison A, Mattes J, Plank M, Foster PS. Inhibition of house dust mite-induced allergic airways disease by antagonism of microRNA-145 is comparable to glucocorticoid treatment. J Allergy Clin Immunol. 2011;128:160–7.
Sato T, Liu X, Nelson A, et al. Reduced MiR-146a increases prostaglandin E2 in chronic obstructive pulmonary disease fibroblasts. Am J Respir Crit Care Med. 2010;182:1020–9.
Larner-Svensson HM et al. Pharmacological studies of the mechanism and function of interleukin-1beta-induced miRNA-146a expression in primary human airway smooth muscle. Respir Res. 2010;11:68.
Yamamoto M et al. Decreased miR-192 expression in peripheral blood of asthmatic individuals undergoing an allergen inhalation challenge. BMC Genomics. 2012;13:655.
Mizuno S et al. MicroRNA-199a-5p is associated with hypoxia-inducible factor-1alpha expression in lungs from patients with COPD. Chest. 2012;142:663–72.
Liu F, Qin HB, Xu B, Zhou H, Zhao DY. Profiling of miRNAs in pediatric asthma: upregulation of miRNA-221 and miRNA-485-3p. Mol Med Report. 2012;6:1178–82.
Qin HB et al. Inhibition of miRNA-221 suppresses the airway inflammation in asthma. Inflammation. 2012;35:1595–9.
Iliopoulos D, Hirsch HA, Struhl K. An epigenetic switch involving NF-kappaB, Lin28, let-7 microRNA, and IL6 links inflammation to cell transformation. Cell. 2009;139:693–706.
Witwer KW, Sisk JM, Gama L, Clements JE. MicroRNA regulation of IFN-beta protein expression: rapid and sensitive modulation of the innate immune response. J Immunol. 2010;184:2369–76.
Androulidaki A et al. The kinase Akt1 controls macrophage response to lipopolysaccharide by regulating miRNAs. Immunity. 2009;31:220–31.
Lu Z, Liu M, Stribinskis V, et al. MicroRNA-21 promotes cell transformation by targeting the programmed cell death 4 gene. Oncogene. 2008;27:4373–9.
Kim YJ, Hwang SJ, Bae YC, Jung JS. MiR-21 regulates adipogenic differentiation through the modulation of TGF-beta signaling in mesenchymal stem cells derived from human adipose tissue. Stem Cells. 2009;27:3093–102.
Petrocca F, Vecchione A, Croce CM. Emerging role of miR-106b-25/miR-17-92 clusters in the control of transforming growth factor beta signaling. Cancer Res. 2008;68:8191–4.
Di Leva G, Gasparini P, Piovan C, et al. MicroRNA cluster 221-222 and estrogen receptor alpha interactions in breast cancer. J Natl Cancer Inst. 2010;102:706–21.
Guan H, Fan D, Mrelashvili D, et al. MicroRNA let-7e is associated with the pathogenesis of experimental autoimmune encephalomyelitis. EurJ Immunol. 2012;43:104–14.
Zwiers A, Kraal L, van de Pouw Kraan TC, Wurdinger T, Bouma G, Kraal G. Cutting edge: a variant of the IL-23R gene associated with inflammatory bowel disease induces loss of microRNA regulation and enhanced protein production. J Immunol. 2011;188:1573–7.
Schembri F et al. MiRNAs as modulators of smoking induced gene expression changes in human airway epithelium. Proc Natl Acad Sci U S A. 2009;106:2319–24.
Davidson MR, Larsen JE, Yang IA, Hayward NK, Clarke BE, Duhig EE, et al. MicroRNA-218 is deleted and down regulated in lung squamous cell carcinoma. PLoS One. 2010;5:e12560.
Trang P, Medina PP, Wiggins JF, Ruffino L, Kelnar K, Omotola M, Homer R, Brown D, Bader AG, Weidhaas JB, et al. Regression of murine lung tumors by the let-7 microRNA. Oncogene. 2010;29:1580–7.
Wiggins JF, Ruffino L, Kelnar K, Omotola M, Patrawala L, Brown D, Bader AG. Development of a lung cancer therapeutic based on the tumor suppressor microRNA-34. Cancer Res. 2010;70:5923–30.
Liu C, Kelnar K, Liu B, Chen X, Calhoun-Davis T, Li H, Patrawala L, Yan H, Jeter C, Honorio S, et al. The microRNA miR-34a inhibits prostate cancer stem cells and metastasis by directly repressing CD44. Nat Med. 2011;17:211–5.
Van Rooij E, Sutherland LB, Thatcher JE, DiMaio JM, Naseem RH, Marshall WS, Hill JA, Olson EN. Dysregulation of miRNAs after myocardial infarction reveals a role of miR-29 in cardiac fibrosis. Proc Natl Acad Sci U S A. 2008;105:13027–32.
Lanford RE, Hildebrandt-Eriksen ES, Petri A, Persson R, Lindow M, Munk ME, Kauppinen S, Orum H. Therapeutic silencing of microRNA-122 in primates with chronic hepatitis C virus infection. Science. 2010;327:198–201.
He XX, Chang Y, Meng FY, Wang MY, Xie QH, Tang F, Li PY, Song YH, Lin JS. MicroRNA-375 targets AEG-1 in hepatocellular carcinoma and suppresses liver cancer cell growth in vitro and in vivo. Oncogene. 2012;31:3357–69.
Trang P, Medina PP, Wiggins JF, Ruffino L, Kelnar K, Omotola M, Homer R, Brown D, Bader AG, Weidhaas JB, Slack FJ. Regression of murine lung tumors by the let-7microRNA. Oncogene. 2010;29:1580–7.
Ibrahim AF, Weirauch U, Thomas M, Grunweller A, Hartmann RK, Aigner A. MicroRNA replacement therapy for miR-145 and miR-33a is efficacious in a model of colon carcinoma. Cancer Res. 2011;71:5214–24.
Obad S, dos Santos CO, Petri A, Heidenblad M, Broom O, Ruse C, Fu C, Lindow M, Stenvang J, Straarup EM, Hansen HF, Koch T, Pappin D, Hannon GJ, Kauppinen S. Silencing of microRNA families by seed-targeting tiny LNAs. Nat Genet. 2011;43:371–8.
R. Paulmurugan, N.M. Sekar, T.V. Sekar, Biodegradable polymer nanocarriers for therapeutic antisense microRNA delivery in living animals, SPIE BiOS, International Society for Optics and Photonics, 2012, 823208–823213
Akao Y, Nakagawa Y, Hirata I, Iio A, Itoh T, Kojima K, Nakashima R, Kitade Y, Naoe T. Role of anti-oncomirs miR-143 and -145 in human colorectal tumors. Cancer Gene Ther. 2010;17:398–408.
Kasar S, Salerno E, Yuan Y, Underbayev C, Vollenweider D, Laurindo MF, Fernandes H, Bonci D, Addario A, Mazzella F, Raveche E. Systemic in vivo lentiviral delivery of miR-15a/16 reduces malignancy in the NZB de novo mouse model of chronic lymphocytic leukemia. Genes Immun. 2012;13:109–19.
Tivnan A, Orr WS, Gubala V, Nooney R, Williams DE, McDonagh C, Prenter S, Harvey H, Domingo-Fernandez R, Bray IM, Piskareva O, Ng CY, Lode HN, Davidoff AM, Stallings RL. Inhibition of neuroblastoma tumor growth by targeted delivery of microRNA-34a using anti-disialoganglioside GD2 coated nanoparticles. PLoS One. 2012;7:e38129.
Wu Y, Crawford M, Yu B, Mao Y, Nana-Sinkam SP, Lee LJ. MicroRNA delivery by cationic lipoplexes for lung cancer therapy. Mol Pharm. 2011;8:1381–9.
Trang P, Wiggins JF, Daige CL, Cho C, Omotola M, Brown D, Weidhaas JB, Bader AG, Slack FJ. Systemic delivery of tumor suppressor microRNA mimics using a neutral lipidemulsion inhibits lung tumors in mice. Mol Ther. 2011;19:1116–22.
Broderick JA, Zamore PD. MicroRNA therapeutics. Gene Ther. 2011;18:1104–10.
Chen Y, Gao D-Y, Huang L. In vivo delivery of miRNAs for cancer therapy: challenges and strategies. Adv Drug Deliv Rev. 2015;81:128–41.
Huiyuan W, Yifan J, Huige P, Yingzhi C, Peizhi Z, Yongzhuo H. Recent progress in microRNA delivery for cancer therapy by non-viral synthetic vectors. Adv Drug Deliv Rev. 2015;81:142–60.
Narumon C, Athip N, Pethchawan P, Teerapol S. Monitoring safety of liposomes containing rifampicin on respiratory cell lines and in vitro efficacy against Mycobacterium bovis in alveolar macrophages. J Drug Target. 2009;17(10):751–76.
Rojanarat W, Changsan N, Tawithong E, Pinsuwan S, Chan H-K, Srichana T. Isoniazid proliposome powders for inhalation—preparation, characterization and cell culture studies. Int J Mol Sci. 2011;12:4414–34.
Rojanarat W, Nakpheng T, Thawithong E, Yanyium N, Srichana T. Levofloxacin-proliposomes: opportunities for use in lung tuberculosis. Pharmaceutics. 2012;4:385–412.
Rojanarat W, Nakpheng T, Thawithong E. Niracha Yanyium, and Teerapol Srichana inhaled pyrazinamide proliposome for targeting alveolar macrophages. Drug Delivery. 2012;19(7):334–45.
Kaewjan K, Srichana T. Nano spray-dried pyrazinamide-L-leucine dry powders, physical properties and feasibility used as dry powder aerosols. Pharm Dev Technol. 2016;21(1):68–75.
Ahmad MI, Ungphaiboon S, Srichana T. The development of dimple-shaped chitosan carrier for ethambutol dihydrochloride dry powder inhaler. Drug Dev Ind Pharm. 2015;41(5):791–800.
Gangadhar KN, Adhikari K, Srichana T. Synthesis and evaluation of sodium deoxycholate sulfate as a lipid drug carrier to enhance the solubility, stability and safety of an amphotericin B inhalation formulation. Int J Pharm. 2014;471:430–8.
Adhikari K, Buatong W, Thawithong E, Suwandecha T, Srichana T. Factors affecting enhanced permeation of amphotericin B across cell membranes and safety of formulation. AAPS PharmSciTech. 2016;17(4):820–8.
Aramwit P, Porasuphatana S, Srichana T, Nakpheng T. Toxicity evaluation of cordycepin and its delivery system for sustained in vitro anti-lung cancer activity. Nanoscale Res Lett. 2015;10:152. doi:10.1186/s11671-015-0851-1.
Ninbovor J, Sawatdee S, and Srichana T, Factors affecting the stability and performance of ipratropium bromide; fenoterol hydrobromide pressurized-metered dose inhalers, AAPS PharmSciTech 2013; vol. 14, No. 4
Patel A, Woods A, Riffo-Vasquez Y, Babin-Morgan A, Jones M-C, Jones S, Sunassee K, Clark S, de Rosales RTM, Page C, Spina D, Forbes B, Dailey LA. Lung inflammation does not affect the clearance kinetics of lipid nanocapsules following pulmonary administration. J Control Release. 2016;235:24–33.
Chana J, Forbes B, Jones SA. Triggered-release nanocapsules for drug delivery to the lungs. Nanomedicine. 2015;11(1):89–97.
Kumar A, Bicer EM, Morgan AB, Pfeffer PE, Monopoli M, Dawsond KA, Eriksson J, Edwards K, Lynham S, Arno M, Behndig AF, Blomberg A, Somers G, Hassall D, Dailey LA, Forbes B, Mudway IS. Enrichment of immunoregulatory proteins in the biomolecular corona of nanoparticles within human respiratory tract lining fluid. Nanomedicine: Nanotechnology, Biology, and Medicine. 2016;12:1033–43.
Kumar A, Forbes B, Mudway I, Bicer EM, Dailey LA. What are the biological and therapeutic implications of biomolecule corona formation on the surface of inhaled nanomedicines? Nanomedicine (Lond). 2015;10(3):343–5.
Shahabi S, Treccani L, Dringen R, Rezwan K. Utilizing the protein corona around silica nanoparticles for dual drug loading and release. Nanoscale. 2015;7:16251–65.
Manford F, Riffo-Vasquez Y, Spina D, Page CP, Hutt AJ, Moore V, Johansson F, Forbes B. Lack of difference in pulmonary absorption of digoxin, a P-glycoprotein substrate, in mdr1a-deficient and mdr1a-competent mice. J Pharm Pharmacol. 2008;60(10):1305–10.
Forbes B, Ehrhardt C. Human respiratory epithelial cell culture for drug delivery applications. Eur J Pharm Biopharm. 2005;60:193–205.
Ong HX, Benaouda F, Traini D, Cipolla D, Gonda I, Bebawy M, Forbes B, Young PM. In vitro and ex vivo methods predict the enhanced lung residence time of liposomal ciprofloxacin formulations for nebulisation. Eur J Pharm Biopharm. 2014;86(1):83–9.
Manford F, Tronde A, Jeppsson AB, Patel N, Johansson F, Forbes B. Drug permeability in 16HBE14o- airway cell layers correlates with absorption from the isolated perfused rat lung. Eur J Pharm Sci. 2005;26(5):414–20.
Wu Y. Melissa Crawford, Yicheng Mao, Robert J lee, Ian C Davis, Terry S Elton, L James lee and Serge P Nana-Sinkam, Therapeutic delivery of microRNA-29b by cationic lipoplexes for lung cancer. Molecular Therapy Nucleic Acids. 2013;2:e84.
van Dommelen SM, Vader P, Lakhal S, Kooijmans SAA, van Solinge WW, Wood MJA, Schiffeler RM. Microvesicles and exosomes: opportunities for cell-derived membrane vesicles in drug delivery. J Control Release. 2012;161:635–44.
Kooijmans SAA, Vader P, van Dommelen SM, van Solinge WW, Schiffelers RM. Exosome mimetics: a novel class of drug delivery systems. Int J Nanomedicine. 2012;7:1525–41.
Ananta JS, Paulmurugan R, Massoud TF. Nanoparticle-delivered antisense MicroRNA-21 enhances the effects of temozolomide on glioblastoma cells. Mol Pharm. 2015;12(12):4509–17.
Devulapally R, Sekar NM, Sekar TV, Foygel K, Massoud TF, Willmann JK, Paulmurugan R. Polymer nanoparticles mediated codelivery of antimiR-10b and antimiR-21 for achieving triple negative breast cancer therapy. ACS Nano. 2015;9(3):2290–302.
Babar IA, Cheng CJ, Booth CJ, Liang X, Weidhaas JB, Saltzman WM, Slack FJ. Nanoparticle-based therapy in an in vivo microRNA-155 (miR-155)-dependent mouse model of lymphoma. Proc Natl Acad Sci U S A. 2012;109(26):E1695–704.
Huang X, Schwind S, Yu B, Santhanam R, Wang H, Hoellerbauer P, Mims A, Klisovic R, Walker AR, Chan KK, Blum W, Perrotti D, Byrd JC, Bloomfield CD, Caligiuri MA, Lee RJ, Garzon R, Muthusamy N, Lee LJ, Marcucci G. Targeted delivery of microRNA-29b by transferrin-conjugated anionic lipopolyplex nanoparticles: a novel therapeutic strategy in acute myeloid leukemia. Clin Cancer Res. 2013;19(9):2355–67.
Yu Z, Wang Z, Gemeinhart RA. Progress in microRNA delivery. J Control Release. 2013;172:962–74.
Muthiah M, Park I-K, Cho C-S. Nanoparticle-mediated delivery of therapeutic genes: focus on miRNA therapeutics. Expert Opinion on Drug Delivery. 2013;10(9):1259–73.
Yu F, Takeshita F, Kuwano K, Ochiya T. RNAi therapeutic platforms for lung diseases. Pharmaceuticals. 2013;6:223–50.
Kong YW, Ferland-McCollough D, Jackson TJ, Bushell M. MiRNAs in cancer management. Lancet Oncol. 2012;13:249–58.
Zhang P, Cheng F, Zhou R, Cao J, Li J, Burda C. Qianhao Min and Jun-Jie Zhu DNA-hybrid-gated multifunctional mesoporous silica nanocarriers for dual-targeted and microRNA-responsive controlled drug delivery. Angew Chem Int Ed. 2014;53:2371–5.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Dua, K., Hansbro, N.G., Foster, P.S. et al. MicroRNAs as therapeutics for future drug delivery systems in treatment of lung diseases. Drug Deliv. and Transl. Res. 7, 168–178 (2017). https://doi.org/10.1007/s13346-016-0343-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-016-0343-6