Abstract
In this study, we investigated the effects of DDR1 on the invasion and metastasis in gastric cancer (GC) via epithelial-mesenchymal transition (EMT). Immunohistochemistry analysis was used to detect DDR1, E-cadherin, and Vimentin expression in GC tissues as well as DDR1 expression in GC cell lines and normal gastric epithelial cells. The relationship between DDR1 expression and EMT in GC cell lines was explored by down and upregulating DDR1 and examining corresponding changes in the expression of EMT-related proteins and in biological characteristics. Furthermore, a nude mice model with a transplantation tumor generating from stably transfected GC cells with DDR1 overexpression was established and performed to further reveal the effects of DDR1 expression on cellular morphology and growth of GC. Our results showed that DDR1 was highly expressed in GC tissues and cell lines compared with adjacent tissues and normal cell line, and its expression was significantly higher in GC having poor differentiation (p < 0.01), advanced depth of wall invasion (p = 0.020), lymph node metastasis (p = 0.0001), liver metastasis (p < 0.01), and high TNM stage (p < 0.01). Western blot analyses revealed that DDR1 overexpression resulted in a significant decrease in the expression of E-cadherin (p < 0.01) and an increase in the expression of Vimentin and Snail (p < 0.01), while knockdown of DDR1 led to opposite outcomes. We further demonstrated that DDR1 overexpression promoted GC cell proliferation (p < 0.05), migration (p < 0.01), and invasion (p < 0.01), and accelerated the growth (p < 0.05) as well as the microvessel formation (p < 0.01) of transplantation tumor in nude mice. Our study establishes that DDR1 enhances invasion and metastasis of gastric cancer via EMT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gastric cancer (GC) is one of the most common malignant tumors of the alimentary tract and is characterized by low early diagnostic rate, high degree of malignance, and early metastasis. Although diagnosis and treatment have significantly improved in recent years [1] and mortality caused by GC notably decreased in past decades [2], it is still a leading cause of cancer mortality in the world [3] and approximately 50 % of the patients recrudesce and develop distant metastasis after treatment [1]. Therefore, the underlying mechanism of the invasion and metastasis of GC has been one of the focus in recent GC research.
DDR1 is one member of discoidin domain receptors (DDRs), which constitute a unique subfamily of non-integrin collagen receptors and are receptor tyrosine kinases containing a discoidin homology region in their N-terminal domain [4]. DDRs are comprised of DDR1 and DDR2. DDR1 has at least five isoforms generated through alternative splicing of the kinase domain of the human DDR1 gene [4, 5]. Growing evidence suggests that it is highly expressed in certain kinds of tumors [6–10], especially in highly invasive tumors and is involved in cellular adhesion and morphogenesis, differentiation, migration and invasion, ECM remodeling, proliferation and apoptosis, and poor prognosis [6, 11–15]. In highly invasive non-small cell lung cancer, DDR1 was significantly correlated with lymph node metastasis and shorter survival, and overexpression of DDR1 enhanced cell mobility and invasion [6, 14]. In lung cancer bone metastasis, inhibition of DDR1 reduced cell survival, homing, and colonization [16], indicating its involvement in cell migration and invasion in lung cancer. Moreover, DDR1 was found to be associated with cellular migration and invasion in hepatocellular carcinoma (HCC) [17] as well as HCC recurrence [9] and was also identified to be a potential biomarker for serous ovarian cancer [10]. Our previous study showed that DDR1 was overexpressed in GC tissues [18], suggesting its potential involvement in the progression of the cancer.
Epithelial-mesenchymal transition (EMT) is a unique process where epithelial cells undergo remarkable morphological changes, at the core of which is a transition from an epithelial cobblestone to an elongated mesenchymal phenotype, leading to increased mobility and invasion [19, 20]. EMT progression is featured by the loss of proteins involved in cell junctions such as E-cadherin and the expression of mesenchymal markers such as Vimentin and Snail [19, 20]. It is an important process in the metastasis of various kinds of solid tumors [21, 22], including gastric carcinomas [23, 24]. Kim et al. demonstrated that the expression of EMT-related genes such as E-cadherin, Vimentin, N-cadherin, and Snail was associated with poor prognosis of GC [25]. In esophageal cancer cells, enhanced EMT through Interleukin-23 via Wnt/β-catenin pathway increased cell proliferation, migration, and invasion [26]. In ovarian serous adenocarcinoma, the growth of tumor was suppressed by DYRK2 regulating EMT through Snail degradation [27]. Recently, Miao et al. reported that DDR1 could promote cellular invasion via EMT in non-small cell lung cancer [6]. In addition, prior studies have documented Snail as a regulator of EMT and a mediator for cancer progression and metastasis. Specifically, Snail was reported to control EMT by suppressing E-cadherin expression [28, 29], to affect tumor growth and metastasis of ovarian carcinoma [30] as well as the overall survival of ovarian cancer patients [31], and to accelerate the lymph node and distant metastasis of tumors via suppressing EMT induced by E-cadherin [32, 33]. Moreover, Snail played a part in cell proliferation and protection against cell death, which is indispensable to tumor metastasis [33]. Despite these findings, the relationships between DDR1 expression, clinicopathological characteristics, and EMT in GC are still largely unknown.
Although DDR1 has been verified to play a role in the initiation and development of tumors and its overexpression generally signals poor prognosis [34–36], the mechanism by which DDR1 affects cell proliferation and metastasis in GC is poorly understood to date. In this study, we examined the expression levels of DDR1 and EMT-associated proteins E-cadherin and Vimentin in GC tissues in order to explore their correlations with tumor invasion and clinicopathologic parameters of GC patients. We also investigated the relationship between DDR1 expression and EMT by down and upregulating DDR1 expression levels in GC cell lines and detecting corresponding changes in the expression of E-cadherin, Vimentin, and Snail, and the changes in biological characteristics. Additionally, a model of nude mice with a transplantation tumor generating from stably transfected GC cells with DDR1 overexpression was established and performed to further reveal the effects of DDR1 expression on cellular morphology and growth of GC.
Materials and methods
Patients and tissue samples
A consecutive series of 160 tissue samples was collected from patients with GC who were treated with subtotal or total resection by gastrectomy at Lanzhou University Second Hospital between January 2009 and December 2012. There was no local or systemic treatment conducted on these patients before the operation. Written informed consent was obtained from all patients before sample collection, and the study was approved by the institutional Review Board of Lanzhou University Second Hospital. The patients comprised 122 males and 38 females with a mean age of 62 (24–90). Age and gender of the patients, tumor size, cell differentiation, depth of wall invasion, status of lymph node metastasis, vascular invasion, and lymphatic invasion were obtained from histopathology records and summarized in Table 1. The stage of GC was determined according to the 1997 tumor-node-metastasis (TNM) classification of malignant tumors of the American Joint Committee on cancer. The tissue specimens were formalin-fixed and paraffin-embedded, stained with hematoxylin-eosin (HE), and classified by a pathologist. HE results were compared to histopathology records from Lanzhou University Second Hospital.
Cell lines and culture conditions
The GC cell lines SGC7901, MKN45, and BGC823 were purchased from the Institute of Biochemistry and Cell Biology of the Chinese Academy of Sciences (Shanghai, China). GES1, a SV40-transformed immortal human gastric epithelial cell line, was established at Peking University Cancer Hospital. Cells were cultured in RPMI 1640 Medium (Hyclone, USA) with 10 % fetal bovine serum (FBS, Hyclone, USA) at 37 °C in a humidified atmosphere containing 5 % CO2.
Immunohistochemistry
Immunohistochemical staining for DDR1, E-cadherin, and Vimentin was conducted on formalin-fixed and paraffin-embedded tissue sections. All antibodies were purchased from Santa Cruz, USA. Immunohistochemical staining was performed as described previously [37]. Immunohistochemistry for GC cells and GES1 were conducted on cell climbing slice fixed with 4 % paraformaldehyde (Solarbio, Beijing, China) without antigen retrieval. Results of immunostaining were scored according to a previous report [38].
Western blot
Cells were lysed in RIPA buffer supplemented with PMSF (RIPA:PMSF = 99:1, Solarbio, Beijing, China), incubated on ice for 30 min, and then centrifuged at 12,000 rpm for 15 min at 4 °C. The protein lysates were subjected to 10 % SDS-PAGE and transferred to PVDF membranes (Millipore, USA) at 250 mA for 0.5 to 1 h. After blocking with 5 % non-fat milk (BD, USA) at room temperature for 1 h, the membranes were incubated with the following primary antibodies: DDR1 (rabbit anti-human monoclonal antibody, 1:200, Santa Cruz, USA), Vimentin (rabbit anti-human monoclonal antibody, 1:500, Santa Cruz, USA), E-Cadherin (rabbit anti-human monoclonal antibody, 1:500, Cell Signaling Technology, USA), Snail (rabbit anti-human monoclonal antibody, 1:500, Cell Signaling Technology, USA), and β-actin (mouse anti-human polyclonal antibody, 1:1000, ZSGB-BIO, Beijing, China) overnight at 4 °C. After incubation with sheep anti-rabbit or sheep anti-mouse IgG secondary antibodies (1:5000, LI-COR, USA) at room temperature for 1 h, the fluorescence intensity was detected by Odyssey Infrared fluorescence imaging system (LI-COR, USA).
Knockdown transfection
DDR1-targeted small interfering RNA (siRNA) was designed using BLOCK-iT™ RNAi Designer and synthesized by GenePharma (Shanghai, China). The target sequences of DDR1 siRNA were sense 5′-CCACCAACUUCAGCAGCUUdTdT-3′ and antisense 5′-AAGCUGCUGAAGUUGGUGGdTdT-3′. The negative control sequences of siRNA (NC) were sense 5′-UUCUCCGAACGUGUCACGUTT-3′ and antisense 5′-ACGUGACACGUUCGGAGAATT-3′, obtained from GenePharma (Shanghai, China). MKN45 cells were transiently transfected with the DDR1 targeted siRNA using FuGENE HD (Promega, USA) according to instructions from the manufacturer. The cells were then incubated with complete growth medium for 6 h at 37 °C. Seventy-two hours after transfection, the cells were harvested for relevant assays.
Overexpression transfection
DDR1 cDNA was synthesized and a recombinant plasmid (pGL4.17, Promega, USA) was created by BGI (Beijing, China). PCR-amplification, enzyme digestion, and electrophoresis were performed sequentially to obtain DDR1 from the recombinant plasmid, which was then cloned to the lentiviral vector (Lentivirus-NC, GenePharma, Shanghai, China) carrying green fluorescent protein (GFP) and anti-puromycin gene. After plasmid amplification, identification, and sequencing, HEK293T was transfected with the recombinant lentiviral vector (Lentivirus-DDR1) to collect virus supernatant, with which BGC823 were infected in the presence of 5 μg/mL polybrene (Sigma, USA). BGC823 cells with stable expression of DDR1 were selected using puromycin (Sigma, USA) at a concentration of 0.6 μg/mL, which was tested as the optimal lethal concentration, and then were used in this study. BGC823 cells transfected with the control lentiviral vector (Lentivirus-NC, GenePharma, Shanghai, China) were used as the negative control.
Cell proliferation assay
MTT was used to examine the effects of DDR1 knockdown or DDR1 overexpression on cell proliferation of GC. GC cells were seeded at a density of 2 × 103 cells/100 μL medium in 96-well plates and treated with 20 μL MTT at 24, 48, or 72 h, respectively. After incubation with MTT for 4 h, 100 μL 10 % SDS was added to each well and the plates were placed overnight at room temperature. Optical density (OD) values at 570 nm were measured by Microplate Reader (Omega Bio-Tek, USA).
Colony formation assay
BGC823 cells (100 cells/well) with and without upregulated DDR1 expression were seeded in 6-well plates, respectively. After 15 days, the medium was removed and cells were fixed with 4 % paraformaldehyde (Solarbio, Beijing, China) for 15 min and stained with 0.1 % crystal violet. After washing with distilled water and air drying, single cell colonies (>50) were counted.
Migration assay
Cells at logarithmic phase were harvested and made to be single cell suspension (5 × 106 cells/mL). Transwell chambers (Minipore, USA) were placed in a 24-well plate with 100 μL cell suspension containing 1 % FBS added into the upper chambers and 600 μL medium containing 10 % FBS into lower chambers as the attractant. After 24-h incubation in a 5 % CO2 atmosphere, the suspension and medium were removed and non-migratory cells in the upper chambers were wiped with wet cotton swabs. Cells in the lower chambers were fixed and stained with crystal violet for counting under an optical microscope.
Invasion assay
Transwell chambers (Minipore, USA) were placed in a 24-well plate and the upper chambers were first added with 100 μL Matrigel (BD, USA). Two hours later, 100 μL cell suspension (1 × 107 cells/mL) and 600 μL medium were added into the upper and lower chambers, respectively. Similar to migration assay described above, cells and the Matrigel in the upper chambers were wiped off whereas cells in the lower side were fixed and stained for counting.
In vivo assays
Female BALB/c nude mice (6–8 weeks old, 18–22 g), purchased from Vital River Laboratory Animal Technology Co. Ltd. (Beijing, China), were fed under specific pathogen-free conditions. The mice were randomly divided into two groups (n = 6 per group) and were subcutaneously inoculated with 2 × 106 BGC823 cells with (BGC-DDR1) or without (BGC-NC) DDR1 overexpression, respectively. Small animal in vivo imaging (SAIVI) was conducted on the nude mice at 1, 3, 5, and 7 weeks, respectively, after the inoculation, and the fluorescence intensity of transplanted tumor in nude mice at each time point was detected and quantified as an indirect measure for the size of transplantation tumor by the SAIVI system. The mice were sacrificed after 7 weeks, and the tumor was taken to study its tissue morphology by HE staining and the expression of angiogenesis-associated protein CD34 by immunohistochemistry. The experiments were approved by the Ethics Committee of Lanzhou University Second Hospital.
Statistical analysis
All of the statistical analyses were performed using the SPSS 21.0 software (SPSS, China). The χ 2 test or Fisher’s exact test was used to analyze the association between DDR1, E-cadherin, and Vimentin expression and clinicopathologic parameters of the patients. The significance of differences between groups was determined by Student’s t test or analysis of variance (ANOVA). Data were presented as mean ± standard deviation (SD). All reported p values were two-sided and considered statistically significant when p < 0.05.
Results
Correlation of DDR1, E-cadherin, and Vimentin expression with clinicopathological features in GC
Table 1 shows the clinicopathological data and DDR1, E-cadherin, and Vimentin expression of 160 GC patients. As revealed by the χ 2 test, DDR1 expression was significantly higher in GC having poor differentiation (p < 0.01), advanced depth of wall invasion (p = 0.020), lymph node metastasis (p = 0.0001), liver metastasis (p < 0.01), and high TNM stage (p < 0.01) but was not correlated with age, gender, tumor size, lymphatic invasion, or vascular invasion. The expression of E-cadherin was significantly correlated with vascular invasion (p = 0.012) and lymphatic invasion (p = 0.015) while that of Vimentin was higher in GC having poor differentiation (p = 0.006), lymph node metastasis (p < 0.01), vascular (p < 0.01) and lymphatic invasion (p = 0.002), and high TNM stage (p < 0.01).
Correlation between DDR1, E-cadherin, and Vimentin expression in GC tissues
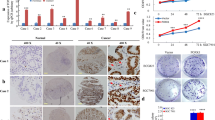
To further explore the expression pattern between DDR1, E-cadherin, and Vimentin, immunohistochemical analyses were conducted on GC and adjacent normal tissues. Figure 1a presents representative images of DDR1, E-cadherin, and Vimentin expression in GC tissues and adjacent normal gastric tissues. Immunostaining scores showed that DDR1 was expressed in the membrane of gastric cancer cells and the expression rate reached 80 % (128/160), while those of E-cadherin and Vimentin were 38.75 % (62/160) and 71.25 % (114/160), respectively (Table 2). In comparison, the expression rates of DDR1, E-cadherin, and Vimentin in adjacent normal gastric tissue were 5 % (1/20), 100 % (20/20), and 10 % (2/20), respectively. Unreported χ 2 test showed that the expression rates of DDR1 and Vimentin were remarkably higher in GC tissues than in adjacent gastric normal tissues (p < 0.0001) while that of E-cadherin was considerably lower in GC tissues (p < 0.0001). The χ 2 test further revealed DDR1 expression in GC tissues to be significantly correlated with the expression of E-cadherin and Vimentin (p < 0.01; Table 2). Specifically, of 160 specimens, 36 (22.5 %) were positive for both DDR1 and E-cadherin, and 106 (66.25 %) were positive for both DDR1 and Vimentin (Table 2).
Expression of DDR1 and EMT-associated proteins E-cadherin and Vimentin in GC and normal tissues and cells. a Representative images with a ×400 magnification of DDR1, E-cadherin, and Vimentin expression in GC tissues and in adjacent normal gastric tissues. DDR1 and Vimentin were higher expressed in GC tissues than in adjacent normal gastric tissues while E-cadherin expression was lower in GC tissues than in adjacent normal gastric tissues. b Representative images with a ×400 magnification of DDR1 expression in the normal gastric epithelial cells and three GC cell lines. DDR1 expression was positive for all three GC cell lines but negative for the normal gastric epithelial cells. Expression levels were assessed and scored by immunohistochemistry analysis
Expression analysis of DDR1 in GC cell lines and normal gastric epithelial cells
To investigate whether DDR1 expression is associated with GC, immunohistochemistry analysis was employed to detect DDR1 expression in both GC cell lines and normal gastric epithelial cells. Figure 1b exhibits representative images of DDR1 expression in a normal gastric cell line and three GC cell lines. Immunostaining scores showed that DDR1 was expressed in all three GC cell lines, namely, MKN45, SGC7901, and BGC823, in a descending order of expression level. In contrast, DDR1 expression in GES1, which is a normal gastric epithelial cell line, was negative (−). These results indicate that DDR1 expression may be involved in the initiation and development of GC.
Effects of DDR1 on the expression of E-cadherin, Vimentin, and Snail in GC cell lines
To identify the relationship between expression of DDR1 and EMT-associated proteins in GC cell lines, DDR1 expression was downregulated in DDR1 high-expressing cell line MKN45 and upregulated in DDR1 low-expressing cell line BGC823. The resulting changes in the expression of DDR1 and EMT-associated proteins were detected by western blot analysis.
As shown in Fig. 2a, b, DDR1 expression was significantly lower in MKN45, 72 h after transfection with DDR1-siRNA (Fig. 2a, b, left; *p < 0.05), and was remarkably higher in BGC823 after stable transfection with DDR1 recombinant lentivirus (Fig. 2a, b, right; **p < 0.01). Furthermore, western blot analysis showed that inhibition of DDR1 expression in MKN45 resulted in a significant increase in the expression of E-cadherin (Fig. 2a, b, left; **p < 0.01), and a decrease in the expression of Vimentin and Snail (Fig. 2a, b, left; *p < 0.05). In contrast, overexpression of DDR1 in BGC823 resulted in opposite outcomes in terms of the expression levels of the abovementioned proteins (Fig. 2a, b, right; **p < 0.01). These results indicate that inhibition of DDR1 suppresses EMT whereas DDR1 overexpression promotes it.
Effects of DDR1 on the expression of E-cadherin, Vimentin, and Snail and on the GC cell proliferation. a Left, western blot analysis of the changes in expression of DDR1, E-cadherin, Vimentin, and Snail in MKN45 before and after transfection with DDR1-siRNA; right, western blot analysis of the changes in expression of DDR1, E-cadherin, Vimentin, and Snail in BGC823 before and after stable transfection with DDR1 recombinant lentiviral vector. b Graphical representation of Fig. 2a. c Left and middle, MTT assay was used to examine GC cell proliferation at 24, 48, and 72 h respectively, consistently showing that DDR1 knockdown in MKN45 inhibited cell proliferation whereas DDR1 overexpression promoted the proliferation of BGC823; right, colony formation assay further revealed that DDR1-overexpressed BGC823 cells possessed higher monoclonal forming ability. *p < 0.05; **p < 0.01
Effects of DDR1 on cell proliferation
MTT assay was used to examine the changes in cell proliferation of GC cells. Compared with negative control, inhibition of DDR1 expression in MKN45 significantly suppressed cell proliferation (Fig. 2c, left, MKN-SI vs MKN-NC, *p < 0.05, **p < 0.01), while the cell proliferation was markedly increased in BGC823 cells with DDR1 overexpression as compared with control cells (Fig. 2c, middle, BGC-DDR1 vs BGC-NC, *p < 0.05, **p < 0.01). Moreover, the colony formation assay confirmed that DDR1-overexpressed BGC823 cells had a significantly higher monoclonal forming ability compared with negative control (Fig. 2c, right, BGC-DDR1 vs BGC-NC, *p < 0.05).
In addition, the investigation on cell cycle and apoptosis showed that neither inhibition of DDR1 in MKN45 nor DDR1 overexpression in BGC823 had considerable effects on the cell cycle and apoptosis of GC cells. The results are not reported here and provided upon request.
Effects of DDR1 on cell migration and invasion
The effects of DDR1 expression on cell migration and invasion were explored using Transwell migration and invasion assay. The results showed that inhibition of DDR1 expression in MKN45 resulted in a significantly reduced number of migratory and invasive cells (Fig. 3a, b, MKN-SI vs MKN-NC, **p < 0.01). It was also showed that DDR1 overexpression in BGC823 remarkably increased the number of cells across the membrane (Fig. 3c, d, BGC-DDR1 vs BGC-NC, **p < 0.01). These results suggest that DDR1 promotes GC cell migration and invasion.
Effects of DDR1 on GC cell migration and invasion. a Representative images with a ×100 magnification of migratory and invasive MKN45 cells with (MKN-SI) and without (MKN-NC) DDR1 knockdown. b Knockdown of DDR1 in MKN45 resulted in a significantly reduced number of migratory or invasive cells. c Representative images with a ×100 magnification of migratory and invasive BGC823 cells with (BGC-DDR1) and without (BGC-NC) DDR1 overexpression. d DDR1 overexpression resulted in a significantly increased number of migratory or invasive BGC823 cells. **p < 0.01
Effects of DDR1 on transplantation tumor in nude mice
We further established a nude mice model with transplantation tumor to better understand the effects of DDR1 on tumor growth and cellular morphology in vivo. Figure 4a shows representative images of nude mice with transplantation tumor under SAIVI. Quantification of the fluorescence intensity of the transplanted tumor, as presented in Fig. 4b, confirmed that DDR1 overexpression significantly accelerated the growth of BGC823 cells in the subcutaneous transplantation tumor in nude mice as compared with control group (Fig. 4b, *p < 0.05, **p < 0.01). In addition, the immunohistochemical staining of tumor tissues showed that CD34 expression was significantly increased in DDR1 over-expressing group (Fig. 4d, e, **p < 0.01), indicating that DDR1 overexpression promoted the microvessel formation of the transplantation tumor.
Effects of DDR1 on transplantation tumor in nude mice. a Female nude mice were subcutaneously inoculated with BGC823 cells with (BGC-DDR1) and without (BGC-NC) DDR1 overexpression. Small animal in vivo imaging (SAIVI) was conducted on the nude mice at 1, 3, 5, and 7 weeks, respectively, after the inoculation. b The fluorescence intensity of transplanted tumor in nude mice at each time point was detected and quantified by the SAIVI system. Compared to those inoculated with negative control BGC823 cells, mice with DDR1-overexpressed BGC823 cells had higher growth in transplantation tumor. c Representative images of hematoxylin-eosin (HE) staining of tumor tissues with the magnification of ×200 and ×400, respectively. d Representative images of immunohistochemical staining of CD34 with a magnification of ×400 and the arrows indicate where there is microvascular formation. e Microvessel density was measured, showing that CD34 expression was significantly higher in DDR1 over-expressing group. *p < 0.05; **p < 0.01
Discussion
As one member of DDRs, DDR1 has become a potential biomarker [10], prognostic predictor [6, 9], and therapeutic target for tumors [8, 39]. Targeting to DDR1, several agents have been developed and tested [39–41]. While prior research has documented significant functional roles of DDR1 in various cancers, little information is available on its expression and involvement in gastric cancer. This study investigated the effects of DDR1 on the invasion and metastasis in GC. Our results showed that DDR1 was highly expressed in GC tissues and cell lines compared with adjacent tissues and normal cell line, confirming our previous report [18] and indicating that DDR1 overexpression may contribute to GC progression. We further demonstrated that DDR1 overexpression enhanced GC cell proliferation, migration, and invasiveness, and accelerated the growth of transplantation tumor.
Our study also provided useful insights to the mechanism underlying functional effects of DDR1 in GC. First of all, our results indicated that EMT could be the underlying mechanism by which DDR1 affects GC progression. A bunch of studies showed that EMT was involved in the invasion and metastasis of GC and reversing EMT has become a potential therapeutic strategy [42–44]. Maeyama et al. observed switching in discoid domain receptor expressions in SLUG-induced EMT [45]. Furthermore, DDR1 regulated the stabilization of cell surface E-cadherin and E-cadherin-mediated cell aggregation [46] and triggered epithelial cell differentiation by promoting cell adhesion through stabilization of E-cadherin [47]. DDR1/E-cadherin complex regulated the activation of DDR1 and cell spreading [48]. A recent study showed that DDR1 was associated with poor prognosis of non-small cell lung cancer and promoted cell invasion via EMT [6]. This study demonstrated that downregulation of DDR1 suppressed EMT while its overexpression promoted EMT, suggesting that DDR1 enhanced proliferative, migratory, and invasive abilities of GC cells through EMT.
While DDR1 may exert a kinase-independent function on EMT, this study suggested another possibility that DDR1 affects EMT through Snail. Snail signaling is intimately associated with EMT. For instance, Snail was reported to mediate ovarian tumor neovascularization, growth, and metastasis via regulating EMT [49]. It was also shown that through inhibition of E-cadherin expression, Snail/HDAC1/HDAC2 complex facilitated EMT and thereby the metastasis of pancreatic cancer [50]. Our results revealed a significant correlation between DDR1, EMT, and Snail, offering a possibility that the promotion of EMT by DDR1 in GC cells may be induced by Snail signaling. Furthermore, Zhou et al. showed that GSK-3β binds to and phosphorylates Snail, thereby regulating the function of Snail in inducing EMT [51]. It is thus plausible yet speculative that the functional effects of DDR1 in GC progression and metastasis documented in this study might be realized by DDR1-mediated phosphorylation that affects EMT through Snail. Further investigations examining the binding between Snail and DDR1 or exploring the effects of Snail knockdown on DDR1 cancer-related functions are of great necessity to elucidate the mechanisms.
CD34 is a distinguishing feature of vascular endothelial cells and microvessel density (MVD) is considered one of the important measures for tumor proliferation and growth. The expression level of CD34 evaluated by immunohistochemistry represents a measure for MVD. It was testified that MVD in tumor tissues was correlated with malignancy and prognosis of tumor. For instance, MVD in prostate malignant tumors was positively linked with pathological classification and prognosis [52–54]. As an important vascular marker, CD34 rendered great values in the evaluation and diagnosis for prognosis of patients with liver cancer [55, 56]. In ovarian cancer, a high expression level of CD34, or equivalently of MVD, signalled poor prognosis and high mortality [57]. Moreover, CD34 expression and MVD in GC tissues were correlated with malignancy and metastasis of GC [58]. Our results showed that DDR1 overexpression remarkably accelerated the growth of transplantation tumor and increased the level of MVD in vivo, indicating that DDR1 increases the growth of tumor at least partly by promoting microvessel formation yet the exact mechanism entails further analysis.
In conclusion, this study provides evidence that DDR1 enhances the invasion and metastasis of GC cells by promoting EMT and accelerates the growth of transplantation tumor as well as the microvessel formation of the tumor. However, further studies are needed to identify the precise molecular mechanisms underlying the functional effects of DDR1 in GC invasion and metastasis.
References
Feng Q, Pei W, Zheng ZX, Bi JJ, Yuan XH. Clinicopathologic characteristics and prognostic factors of 63 gastric cancer patients with metachronous ovarian metastasis. Cancer Biol Med. 2013;10(2):86–91.
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Michael J. Cancer statistics, 2009. CA Cancer J Clin. 2009;59:225–49.
Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics, 2002. CA Cancer J Clin. 2005;55:74–108.
Alves F, Vogel W, Mossie K, Millauer B, Hofler H, Ullrich A. Distinct structural characteristics of discoidin I subfamily receptor tyrosine kinases and complementary expression in human cancer. Oncogene. 1995;10(3):609–18.
Alves F, Saupe S, Ledwon M, Schaub F, Hiddemann W, Vogel WF. Identification of two novel, kinase-deficient variants of discoidin domain receptor 1: differential expression in human colon cancer cell lines. FASEB J. 2001;15:1321–3.
Miao L, Zhu S, Wang Y, Li Y, Ding J, Dai J, et al. Discoidin domain receptor 1 is associated with poor prognosis of non-small cell lung cancer and promotes cell invasion via epithelial-to-mesenchymal transition. Med Oncol. 2013;30(3):626.
Johnson JD, Edman JC, Rutter WJ. A receptor tyrosine kinase found in breast carcinoma cells has an extracellular discoidin I-like domain. Proc Natl Acad Sci U S A. 1993;90(22):10891.
Shimada K, Nakamura M, Ishida E, Higuchi T, Yamamoto H, Tsujikawa K, et al. Prostate cancer antigen-1 contributes to cell survival and invasion though discoidin receptor 1 in human prostate cancer. Cancer Sci. 2008;99(1):39–45.
Jian ZX, Sun J, Chen W, Jin HS, Zheng JH, Wu YL. Involvement of discoidin domain 1 receptor in recurrence of hepatocellular carcinoma by genome-wide analysis. Med Oncol. 2012;29:3077–82.
Quan J, Yahata T, Adachi S, Yoshihara K, Tanaka K. Identification of receptor tyrosine kinase, discoidin domain receptor 1 (DDR1a), as a potential biomarker for serous ovarian cancer. Int J Mol Sci. 2011;12(2):971–82.
Medici D, Nawshad A. Type I collagen promotes epithelial-mesenchymal transition through ILK-dependent activation of NFkappaB and LEF-1. Matrix Biol. 2010;29(3):161–5.
Ongusaha PP, Kim JI, Fang L, Wong TW, Yancopoulos GD, Aaronson SA, et al. p53 induction and activation of DDR1a kinase counteract p53-mediated apoptosis and influence p53 regulation through a positive feedback loop. EMBO J. 2003;22(6):1289–301.
Ford CE, Lau SK, Zhu CQ, Andersson T, Tsao MS, Vogel WF. Expression and mutation analysis of the discoidin domain receptors 1 and 2 in non-small cell lung carcinoma. Br J Cancer. 2007;96(5):808–14.
Yang SH, Baek HA, Lee HJ, Park HS, Jang KY, Kang MJ, et al. Discoidin domain receptor 1 is associated with poor prognosis of non-small cell lung carcinomas. Oncol Rep. 2010;24:311–9.
Shen Q, Cicinnati VR, Zhang X, Iacob S, Weber F, Sotiropoulos GC, et al. Role of microRNA-199a-5p and discoidin domain receptor 1 in human hepatocellular carcinoma invasion. Mol Cancer. 2010;9:227. doi:10.1186/1476-4598-9-227.
Valencia K, Ormazábal C, Zandueta C, Luis-Ravelo D, Antón I, Pajares MJ, et al. Inhibition of collagen receptor discoidin domain receptor-1 (DDR1) reduces cell survival, homing, and colonization in lung cancer bone metastasis. Clin Cancer Res. 2012;18(4):969–80.
Park HS, Kim KR, Lee HJ, Choi HN, Kim DK, Kim BT, et al. Overexpression of discoidin domain receptor 1 increases the migration and invasion of hepatocellular carcinoma cells in association with matrix metalloproteinase. Oncol Rep. 2007;18(6):1435–41.
Yu JJ, Wei LN, Dong C, Fan H, Yu Y, Feng YH, et al. Expression of DDR1a and its clinical significance in gastric carcinoma. Chin J Cancer Prev Treat. 2012;19(14):1074–7.
Kim HP, Han SW, Song SH, Jeong EG, Lee MY, Hwang D, et al. Testican-1-mediated epithelial-mesenchymal transition signaling confers acquired resistance to lapatinib in HER2-positive gastric cancer. Oncogene. 2014;33(25):3334–41.
Bonnomet A, Brysse A, Tachsidis A, Waltham M, Thompson EW, Polette M, et al. Epithelial-to-mesenchymal transitions and circulating tumor cells. J Mammary Gland Biol Neoplasia. 2010;15:261–73.
Zavadil J, Haley J, Kalluri R, Muthuswamy SK, Thompson E. Epithelial-mesenchymal transition. Cancer Res. 2008;68:9574–7.
Thiery JP, Acloque H, Huang RY, Nieto MA. Epithelial–mesenchymal transitions in development and disease. Cell. 2009;139871–890.
Katoh M. Epithelial-mesenchymal transition in gastric cancer. Int J Oncol. 2005;27(6):1677–83.
Zheng HX, Cai YD, Wang YD, Cui XB, Xie TT, Li WJ, et al. Fas signaling promotes motility and metastasis through epithelial-mesenchymal transition in gastrointestinal cancer. Oncogene. 2013;32(9):1183–92.
Kim MA, Lee HS, Lee HE, Kim JH, Yong HK, Kim WH. Prognostic importance of epithelial–mesenchymal transition-related protein expression in gastric carcinoma. Histopathology. 2009;54:442–51.
Chen D, Li W, Liu S, Su Y, Han G, Xu C, et al. Interleukin-23 promotes the epithelial-mesenchymal transition of oesophageal carcinoma cells via the Wnt/β-catenin pathway. Sci Rep-UK. 2015;5:8604.
Yamaguchi N, Mimoto R, Yanaihara N, Imawari Y, Hirooka S, Okamoto A, et al. DYRK2 regulates epithelial-mesenchymal- transition and chemosensitivity through Snail degradation in ovarian serous adenocarcinoma. Tumor Biol. 2015;1–11.
Batlle E, Sancho E, Francí C, Domínguez D, Monfar M, Baulida J, et al. (2000). The transcription factor snail is a repressor of E-cadherin gene expression in epithelial tumour cells. Nat Cell Biol. 2000;2(2):84–9.
Cano A, Pérez-Moreno MA, Rodrigo I, Locascio A, Blanco MJ, del Barrio MG, et al. The transcription factor snail controls epithelial–mesenchymal transitions by repressing E-cadherin expression. Nat Cell Biol. 2000;2(2):76–83.
Jin H, Yu Y, Zhang T, Zhou X, Zhou J, Jia L, et al. Snail is critical for tumor growth and metastasis of ovarian carcinoma. Int J Cancer. 2010;126(9):2102–11.
Blechschmidt K, Sassen S, Schmalfeldt B, Schuster T, Höfler H, Becker KF. The E-cadherin repressor Snail is associated with lower overall survival of ovarian cancer patients. Brit J Cancer. 2008;98(2):489–95.
Shields MA, Krantz SB, Bentrem DJ, Dangi-Garimella S, Munshi HG. Interplay between β1-integrin and Rho signaling regulates differential scattering and motility of pancreatic cancer cells by snail and Slug proteins. J Biol Chem. 2012;287(9):6218–29.
Kudo-Saito C, Shirako H, Takeuchi T, Kawakami Y. Cancer metastasis is accelerated through immunosuppression during Snail-induced EMT of cancer cells. Cancer Cell. 2009;15(3):195–206.
Green D, Ponce DL, Leon-Rodriguez E, Sosa-Sanchez R. Adenocarcinoma of the stomach: univariate and multivariate analysis of factors associated with survival. Am J Clin Oncol. 2002;25:84–9.
Steeg PS. Tumor metastasis: mechanistic insights and clinical challenge. Nat Med. 2006;12:895–904.
Hwang TL, Lee LY, Wang CC, Liang Y, Huang SF, Wu CM. Claudin-4 expression is associated with tumor invasion, MMP-2 and MMP-9 expression in gastric cancer. Exp Ther Med. 2010;1(5):789–97.
Matsuyama W, Hashiguchi T, Umehara F, Matsuura E, Kawabata M, Arimura K, et al. Expression of vascular endothelial growth factor in tuberculous meningitis. J Neurol Sci. 2001;186:75–9.
Fromowitz FB, Viola MV, Chao S, Oravez S, Mishriki Y, Finkel G, et al. Ras p21 expression in the progression of breast cancer. Hum Pathol. 1987;18(12):1268–75.
Gao M, Duan L, Luo J, Zhang L, Lu X, Zhang Y, et al. Discovery and optimization of 3-(2-(Pyrazolo [1, 5-a] pyrimidin-6-yl) ethynyl) benzamides as novel selective and orally bioavailable discoidin domain receptor 1 (DDR1a) inhibitors. J Med Chem. 2013;56(8):3281–95.
Kim HG, Tan L, Weisberg EL, Liu F, Canning P, Choi HG, et al. Discovery of a potent and selective DDR1 receptor tyrosine kinase inhibitor. ACS Chem Biol. 2013;8(10):2145–50.
Yan SB, Peek VL, Ajamie R, Buchanan SG, Graff JR, Heidler SA, et al. LY2801653 is an orally bioavailable multi-kinase inhibitor with potent activity against MET, MST1R, and other oncoproteins, and displays anti-tumor activities in mouse xenograft models. Invest New Drugs. 2013;31(4):833–44.
Wang SH, Li X, Zhou LS, Cao ZW, Shi C, Zhou CZ, et al. microRNA-148a suppresses human gastric cancer cell metastasis by reversing epithelial-to-mesenchymal transition. Tumor Biol. 2013;34(6):3705–12.
Shi Z, Zhang J, Qian X, Han L, Zhang K, Chen L, et al. AC1MMYR2, an inhibitor of dicer-mediated biogenesis of oncomir miR-21, reverses epithelial–mesenchymal transition and suppresses tumor growth and progression. Cancer Res. 2013;73(17):5519–31.
Voon DC, Wang H, Koo JK, Nguyen TA, Hor YT, Chu YS, et al. Runx3 protects gastric epithelial cells against epithelial-mesenchymal transition-induced cellular plasticity and tumorigenicity. Stem Cells. 2012;30(10):2088–99.
Maeyama M, Koga H, Selvendiran K, Yanagimoto C, Hanada S, Taniguchi E, et al. Switching in discoid domain receptor expressions in SLUG-induced epithelial-mesenchymal transition. Cancer. 2008;113(10):2823–31.
Eswaramoorthy R, Wang CK, Chen WC, Tang MJ, Ho ML, Hwang CC, et al. DDR1a regulates the stabilization of cell surface E-cadherin and E-cadherin-mediated cell aggregation. J Cell Physiol. 2010;224(2):387–97.
Yeh YC, Wu CC, Wang YK, Tang MJ. DDR1a triggers epithelial cell differentiation by promoting cell adhesion through stabilization of E-cadherin. Mol Biol Cell. 2011;22(7):940–53.
Wang CZ, Yeh YC, Tang MJ. DDR1a/E-cadherin complex regulates the activation of DDR1a and cell spreading. Am J Physiol Cell Physiol. 2009;297(2):C419–29.
Abdulkhalek S, Geen OD, Brodhagen L, Haxho F, Alghamdi F, Allison S, et al. Transcriptional factor snail controls tumor neovascularization, growth and metastasis in mouse model of human ovarian carcinoma. Clin Transl Med. 2014;3(1):1–16.
von Burstin J, Eser S, Paul MC, Seidler B, Brandl M, Messer M, et al. E-cadherin regulates metastasis of pancreatic cancer in vivo and is suppressed by a SNAIL/HDAC1/HDAC2 repressor complex. Gastroenterology. 2009;137(1):361–71.
Zhou BP, Deng J, Xia W, Xu J, Li YM, Gunduz M, et al. Dual regulation of Snail by GSK-3β-mediated phosphorylation in control of epithelial–mesenchymal transition. Nat Cell Biol. 2004;6(10):931–40.
Bettencourt MC, Bauer JJ, Sesterhenn IA, Connelly RR, Moul JW. CD34 immunohistochemical assessment of angiogenesis as a prognostic marker for prostate cancer recurrence after radical prostatectomy. J Urol. 1998;160(2):459–65.
Erbersdobler A, Isbarn H, Dix K, Steiner I, Schlomm T, Mirlacher M, et al. Prognostic value of microvessel density in prostate cancer: a tissue microarray study. World J Urol. 2010;28(6):687–92.
Miyata Y, Ohba K, Matsuo T, Watanabe SI, Hayashi T, Sakai H, et al. Tumor-associated stromal cells expressing E-prostanoid 2 or 3 receptors in prostate cancer: correlation with tumor aggressiveness and outcome by angiogenesis and lymphangiogenesis. Urology. 2013;81(1):136–42.
Ho JW, Poon RT, Sun CK, Xue WC, Fan ST. Clinicopathological and prognostic implications of endoglin (CD105) expression in hepatocellular carcinoma and its adjacent non-tumorous liver. World J Gastroentero. 2005;11(2):176–81.
Yao Y, Pan Y, Chen J, Sun X, Qiu Y, Ding Y. Endoglin (CD105) expression in angiogenesis of primary hepatocellular carcinomas: analysis using tissue microarrays and comparisons with CD34 and VEGF. Ann Clin Lab Sci. 2007;37(1):39–48.
He L, Wang Q, Zhao X. Microvessel density as a prognostic factor in ovarian cancer: a systematic review and meta-analysis. Asian Pac J Cancer P. 2015;16(3):869–74.
Bădescu A, Georgescu CV, Vere CC, Crăiţoiu S, Grigore D. Correlations between Her2 oncoprotein, VEGF expression, MVD and clinicopathological parameters in gastric cancer. Rom J Morphol Embryo. 2012;53(4):997–1005.
Acknowledgments
This work was funded by the Health Bureau of Gansu Province (No. GSWST2011-08), the National Natural Science Foundation of China (No. 81272661), and the Lanzhou University Second Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Written informed consent was obtained from all patients before sample collection, and the study was approved by the institutional Review Board of Lanzhou University Second Hospital.
The experiments were approved by the Ethics Committee of Lanzhou University Second Hospital.
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Xie, R., Wang, X., Qi, G. et al. DDR1 enhances invasion and metastasis of gastric cancer via epithelial-mesenchymal transition. Tumor Biol. 37, 12049–12059 (2016). https://doi.org/10.1007/s13277-016-5070-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-016-5070-6