Abstract
In tumour cells, the tetramer/dimer ratio of the pyruvate kinase isoenzyme type M2 (M2-PK) determines whether glucose carbons are degraded to lactate with production of energy (tetrameric form) or are channelled into synthetic processes (dimeric form). The influence of different tumour microenvironment conditions on the tetramer/dimer ratio of M2-PK and cell doublings were investigated in a non-metastatic and metastatic pancreatic cancer cell line. The metastatic Colo357 cells contained about fourfold more M2-PK protein and about 3.5-fold more dimeric M2-PK than the non-metastatic Panc-1 cells. In Colo357 cells hypoxia, glucose starvation as well as acidification induced an increase of the dimeric form of M2-PK, whereas in Panc-1 cells no effect on M2-PK was observed. Under hypoxia in Colo357 cells, the dimerization and inactivation of M2-PK results in an inhibition of cell proliferation, whereas under glucose starvation and acidification the dimerization of M2-PK allowed further cell doublings. M2-PK expression and the quaternary structure of M2-PK are influenced by the tumour metastatic potential. The quaternary structure of M2-PK may be differently affected by hypoxia, glucose starvation and acidification with severe consequences on cell doublings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tumour development is associated with major metabolic changes. Otto Warburg noted in 1920 that tumour cells have high glucose consumption and lactate production even in the presence of oxygen (aerobic glycolysis) [1]. Since then, intensive work has been invested to explain the phenomenon of aerobic glycolysis in tumour cells. Although metabolic characteristics of tumour cells have been identified, the reason why tumour cells have high aerobic glycolysis has not been fully established [2]. It has been proposed that the glycolytic phenotype may initially arise as an adaptation response to local hypoxia but that persistent or cyclical hypoxia subsequently exerts selection pressures that lead to constitutive upregulation of glycolysis, even in the presence of oxygen [2].
A consistent metabolic alteration during tumour formation is an increase in glycolytic enzyme activities as well as changes in the glycolytic isoenzymes [3, 4]. One of the glycolytic enzymes which is consistently altered during tumourogenesis is pyruvate kinase (E.C. 2.7.1.40), the last enzyme within the glycolytic chain responsible for glycolytic energy production. Dependent upon the metabolic characteristics of the tissues, different isoenzymes of pyruvate kinase are expressed which differ widely in their kinetic characteristics and metabolic regulation mechanisms [4]. All normal proliferating cells, express the pyruvate kinase isoenzyme type M2 (M2-PK) including embryonic cells and adult stem cells but it is particularly expressed in tumour cells. During tumour formation, the tissue-specific isoenzymes of pyruvate kinase disappear and M2-PK is expressed [4]. Knockdown of M2-PK expression with short hairpin RNAi and replacement of M2-PK with M1-PK, which is the characteristic isoenzyme of muscle and brain, reduced the ability of human tumour cell lines to form tumours in nude mouse xenografts [5]. M2-PK plays a bi-functional role in tumour metabolism. In contrast to the three other pyruvate kinase isoenzymes which always consist of four subunits, M2-PK may occur in a tetrameric form with high affinity to its substrate phosphoenolepyruvate (PEP) and in a dimeric form with a low PEP affinity. The tetrameric form is highly active under physiological conditions and favours the energy regenerating conversion of PEP to pyruvate [4]. The dimeric form of M2-PK is nearly inactive under physiological conditions resulting in an accumulation of the glycolytic intermediates above PK and increased channelling of glucose carbons into synthetic processes, i.e., nucleic acid, amino acid and phospholipid synthesis. In tumour cells, M2-PK is mainly dimeric due to direct interaction with different oncogenes [4]. The dimeric form of M2-PK (Tumour M2-PK) is released from tumours into the blood and stool and may be used for diagnostic purposes [6-11].
The tetramer/dimer ratio of M2-PK is not a stationary value and varies depending upon the concentrations of key metabolites. High fructose 1,6-P2 levels, for example, induces a re-association of the dimeric form of M2-PK to the tetrameric form. Conversely, when the fructose 1,6-P2 levels decrease below a certain value, the tetrameric form dissociates to the dimeric form again. The metabolite-regulated oscillation of M2-PK between the highly active tetrameric and nearly inactive dimeric form imparts the possibility of a sensitive adaption of tumour metabolism to different metabolic conditions [4, 5, 12].
Alteration in the tumour microenvironment in the form of inadequate oxygen and nutrient supply and lactate release results in tumour tissue hypoxia, nutrient deprivation and acidification which may lead to cell cycle arrest, apoptosis and necrosis [13, 14]. However, hypoxic and acidic tumours are more resistant to treatment and have high malignant potential [14]. Hypoxia induces cancer progression through proteomic and genomic changes activating angiogenesis, anaerobic metabolism and other processes that enable tumour cells to survive in an oxygen- and nutrient-deficient environment [14]. A key regulator for the adaption of metabolism to hypoxic conditions is the cytoplasmic hypoxia-inducible factor alpha [15]. Glucose starvation was found to induce the dissociation of the tetrameric form of M2-PK due to a rapid lowering of fructose 1,6-P2 levels [12].
Pancreatic cancers are highly aggressive and carry a poor prognosis. They are characterised by being hypovascular [16]. Clinical studies have demonstrated that pancreatic tumours release Tumour M2-PK (dimeric form of M2-PK) which can be detected in the plasma with the levels correlating with tumour stage [6-9, 11]. The influence of the tumour microenvironment on levels of tumour M2PK has not been adequately investigated. In the present study, we compared the effect of hypoxia, glucose deprivation and acidification on the growth of a non-metastatic and a metastatic pancreatic cancer cell line and compared this with M2-PK expression and levels of Tumour M2-PK.
Material and methods
Cell culture
The human pancreatic cancer cell-line Panc-1, the normal proliferating cell-line human microvascular endothelial cells (HMEC-1) and the human breast cancer cell-line MCF-7 were obtained from the European Collection of Cell Culture. The human pancreatic cancer cell-line Colo357 was gifted by Prof N R Lemoine, Centre for Molecular Oncology and Imaging, The Royal London School of Medicine and Dentistry, London, UK. Under control conditions HMEC-1, Panc-1, and Colo357 cell lines were cultured in Dulbeco’s modified eagle’s medium (DMEM; Gibco, UK) which contained 4,500 mg/l glucose. MCF-7 cells were cultivated in Earl’s minimum essential medium (EMEM; Gibco, UK) which contained 1,000 mg/l glucose. Both media were supplemented with penicillin/streptomycin solution (1%) and 10% foetal bovine serum (FBS). Furthermore, DMEM was supplemented with 2 mM glutamine. EMEM already contained glutamine in a concentration of 2 mM.
Acidic medium was prepared by addition of 1 mM of 2-N-Morpholinoethanesulfonic acid and 25 mM of 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid (Sigma-Aldrich, UK) to DMEM which contained no bicarbonate buffer [17]. The final pH value of the medium was adjusted to 6.5 using 1 mM NaOH or HCl. For glucose-deprived cultivation DMEM (GIBCO, U.K) without glucose and with 10% FBS supplementation was used. Glucose-deprived condition was defined as <50 mg/dl glucose concentration in the culture media as described before [18].
For hypoxic conditions, cells were placed in a hypoxia chamber (Innova CO-48, New Brunswick Scientific, New Jersey, USA) with 1% O2, 5% CO2 and 94% Nitrogen. Under control conditions, the cell lines were cultivated at 21% O2 and 5% CO2.
Cell viability and proliferation rate assessment
Two million cells were plated on a 75 cm2 flask with 15 ml culture medium and cultured for 24, 48, 72 and 96 h, respectively, without changing the culture medium. For the experiments involving altered culture conditions, cells were initially grown in normal conditions for 2 days. Thereafter, the medium was changed and the cells were grown within the new culture conditions without further changes to the medium. For cell counting non-adherent cells floating in the culture medium were sedimented by low centrifugation. Adherent cells were removed from the flask using 0.25% Trypsin ethylenediaminetetraacetic acid (Gibco, UK) and were added to the non-adherent cells. Cell viability was assessed at the different time points by trypan blue exclusion and the viable cells were counted under an inverted phase contrast microscope (Nikon TMS-F, Japan) in a haemocytometer (Bright Line™ Haemocytometer Z359629, Sigma, UK). The proliferation rate was estimated as number of cell-doublings within 96 cultivation hours according to the following equation:
whereby, F = cell density after 96 h, I initial cell number/dish
Sample preparation
After counting, cells were washed three times with cold phosphate buffered saline and pelleted by centrifuging at 800 rpm. Cell pellets were stored at−80 ˚C. The frozen cell pellets were each resuspended in 1 ml of ice cold homogenisation buffer (10 mM Tris, 1 mM NaF and 1 mM Mercaptoethanol, pH 7.4) and homogenised using a Dounce tissue grinder (Wheaton Science products, USA). The homogenised cells were then centrifuged at 40,000×g (Optima™ TLX Ultracentrifuge, Beckman Coutler™, USA) for 20 min and the supernatants of the cell homogenates were used for western blotting and Tumour M2-PK measurements.
M2-PK western blot
The protein content in the cell homogenate supernatant was measured by Bradford assay. For immunoblotting, 20 µg of cell homogenate supernatant protein was separated on 10% sodium dodecyl sulfate polyacrylamide gel (Invitrogen, Paisley, UK). After electrophoresis, the proteins were transferred to polyvinylidene fluoride membranes (Biorad, Hemel Hempstead, UK) by wet electroblotting and incubated overnight with anti-M2-PK monoclonal mouse antibody (DF-4, ScheBo Biotech AG, Giessen, Germany). The secondary antibody used was peroxidase-conjugated anti-mouse goat polyclonal antibody (Pierce Biotechnology, Perbio Science, Cramlington, UK). Immunoreactive proteins were detected using an enhanced chemiluminescence system (SuperSignal West Dura Extended Duration Substrate, Pierce Biotechnology, Perbio Science, Cramlington, UK) on an X-ray film (Fuji Super Rx, Fuji Photo Film (UK) Ltd). Density of each band was measured by densitometry. Actin was used as loading control and detected using anti-actin polyclonal sheep antibody (Sigma-Aldrich, Dorset, UK) as primary and anti-sheep rabbit polyclonal antibody (Pierce Biotechnology, Perbio Science, Cramlington, UK) as secondary antibody.
Tumour M2-PK assay
Tumour M2-PK was measured using an enzyme-linked immunosorbent assay (ELISA) kit (ScheBo® Tumour M2-PK™). The assay is a sandwich-type ELISA based on two monoclonal antibodies specific for the dimeric form of M2-PK with no cross-reactivity with the tetrameric or other isoforms of pyruvate kinase. Tumour M2-PK concentration in the cell homogenate supernatants was expressed in milli-units/milligram protein whereby the protein content of the samples was measured using the Bradford method.
Statistical analysis
For comparison of the Tumour M2-PK levels between the different cell lines in different cultivation conditions, a one-way analysis of covariance was performed using the statistical program package BMDP1V [19]. Tumour M2-PK values were adjusted to cell density to describe the adjusted means. Since the statistical distribution of the Tumour M2-PK values was skewed to the right, a logarithmic transformation of the data was performed and the results were presented as geometric mean and dispersion factor (\( {\overline x_{\rm{g}}} \times {\hbox{D}}{{\hbox{F}}^{\pm 1}} \)). This is the delogarithmic form of the arithmetic mean and standard deviation of the previously logarithmically transformed data. A non-linear regression was calculated to analyse the correlation between Tumour M2-PK levels and cell density using SPSS version 13 (SPSS Inc., Chicago, IL, USA).
The mean value and standard error of the mean of the total M2-PK by western blot in each condition was compared using one-way analysis of variance.
Results
M2-PK expression in HMEC-1, MCF-7, Panc-1 and Colo357 cells
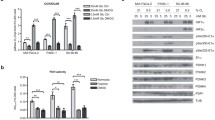
In order to compare M2-PK expression in the different cell lines western blot analysis was performed using a monoclonal anti-M2-PK antibody. Due to the denaturating conditions, western blots do not discriminate between the tetrameric and dimeric form of M2-PK and represents total M2-PK protein. As shown in Fig. 1, all four cell lines expressed the pyruvate kinase isoenzyme type M2. M2-PK expression was highest in the metastatic Colo357 cell line, whereby the amount of M2-PK calculated by densitometry was about fourfold higher than in Panc-1 (p < 0.01), fivefold higher than in MCF-7 (p < 0.01) and ninefold higher than in HMEC-1 (p < 0.01). The lowest amount of M2-PK protein was detected in the normal proliferating cell line HMEC-1.
Western blot analysis of M2-PK expression in HMEC-1, MCF-7, Panc-1 and Colo357 cells. About 2 million cells were seeded per dish for each cell line. After three cultivation days when cell density was about 10 million cells/dish for each cell line a cell homogenate supernatant equivalent to 20 µg protein (BioRad method) was loaded into each slot. Actin was used as a loading control. The bars represent mean ± SEM of three different experiments; **p < 0.01
Tumour M2-PK contents in HMEC-1, MCF-7, Panc-1 and Colo357
In different cell lines, Tumour M2-PK levels, the concentration of the dimeric form of M2-PK, were measured using a sandwich ELISA which specifically quantifies the dimeric form but does not detect the tetrameric form of M2-PK. The mean inter assay coefficient of variance (CV) was 20.8% (11.9-30.15%) and the mean intra assay CV was 4.3% (0.18-16.6%). As shown in Fig. 2, tumour M2-PK decreased with increasing cell density.
Dependency of Tumour M2-PK values from cell density in HMEC-1, MCF-7, Colo357 and Panc-1 cells. Non-linear regression was used to establish correlation between Tumour M2-PK and cell density and the best fitting curve was drawn using the equation: Y = a + b*e−c*x, whereby Y-tumour M2-PK (m Units/mg protein), X-cell density (millions) and a, b and c are the best fit values from the non-linear regression analysis. HMEC-1 (r 2: 0.47, p < 0.05), MCF-7 (r 2: 0.514, p < 0.001), Panc-1 (r 2: 0.25, p < 0.05) and Colo 357 (r 2: 0.44, p < 0.01)
In order to consider further possible dependency of Tumour M2-PK on cell density a one-way analysis of covariance with cell density as covariable was performed. The mean values represent adjusted mean values that have been adjusted to negate the influence of cell density. Tumour M2-PK levels were lowest in HMEC-1 and highest in Colo357 cells (Table 1). When the Tumour M2-PK values were normalised with total M2-PK protein as determined by western blotting (relative Tumour M2-PK) the normal proliferating cell line HMEC-1 still contained the lowest relative amount of Tumour M2-PK. In the metastatic Colo357 cells, relative Tumour M2-PK was equal to that of MCF-7 cells and about 3.5-fold higher than that in Panc-1 cells, which derive from a primary pancreatic tumour.
Alteration to the tumour micro-environment and M2-PK expression
M2PK levels were measured under condition of (a) hypoxia, (b) glucose deprivation and (c) acidic pH.
-
(a)
Effect of hypoxia on cell proliferation, M2-PK expression and Tumour M2-PK content in Panc-1 and Colo357 cells
Hypoxia had significant impact on the cell proliferation of Colo357 and led to a decrease in cell doublings to 1/5 of that of control cells within 96 h (p < 0.001). In contrast, hypoxia did not significantly affect the growth of Panc-1 cells (Table 2). Hypoxia did not change the M2-PK expression in either cell line (Fig. 3). However, in Colo357 cells Tumour M2-PK levels significantly increased about fourfold when cultivated at low oxygen supply (p < 0.001) (Table 3). Since the total M2-PK protein contents remained unchanged, the increase in Tumour M2-PK levels indicates a dimerization of M2-PK in hypoxic Colo357 cells. In Panc-1 cells, Tumour M2-PK levels increased slightly but this was not significant.
Total content of M2-PK protein of Colo357 and Panc-1 cells cultivated under different conditions. Cells were cultivated for 2 days under control conditions until cell density was about 3-4 million cells/dish. Thereafter, the cultivation medium was changed as indicated and the cells were cultivated for 24, 48, 72, and 96 h, respectively, without further changes of the culture medium. For each cell line and each cultivation time point cell homogenate supernatants equivalent to 20 µg protein (BioRad method) were loaded into each slot. Actin was used as a loading control. The bars in a denote the summarised mean Optical Density (ODu) of M2-PK bands at 24, 48, 72 and 96 h from three different experiments. b Denotes a representative M2-PK western blot plate from one of the three experiments
-
(b)
Effect of glucose deprivation on cell proliferation, M2-PK expression and Tumour M2-PK content in Panc-1 and Colo357 cells
In Colo-357 cells at low glucose supply, the number of cell doublings within 96 h significantly decreased versus controls (p < 0.05) while in Panc-1 cell doublings were not significantly affected (Table 2). In both cell lines, glucose deprivation did not affect M2-PK expression (Fig. 3). However, a significant three- to fourfold increase in tumour M2-PK levels was measured in Colo357 cells (p < 0.001). Since total M2-PK protein was not affected at low glucose supply the increase in Tumour M2-PK levels point to a dimerization of M2-PK in glucose deprived Colo357 cells. In Panc-1 cells, a slight increase was measured. However, this increase was not significant (Table 3).
-
(c)
Effect of acidic pH on cell proliferation, M2-PK expression and Tumour M2-PK content in Panc-1 and Colo357 cells
The pH value in acidic condition was stable over a 96 cultivation hours for Colo357 (6.70 ± 0.2; n = 40) and Panc-1 cells (6.45 ± 0.5; n = 40). The pH value of the control medium was also unchanged throughout 96 h of cultivation (7.4 ± 0.5; n = 40). Whereas in Colo357 cells, acidification had no effect on the cell doubling rates, in Panc-1 cells cell proliferation was nearly totally suppressed (p < 0.05; Table 2).
On exposure to acidic pH (6.5), neither in Colo357 nor in Panc-1 cells M2-PK expression was significantly affected (Fig. 3). However, in Colo-357 cells cultivated at pH 6.5 Tumour M2-PK levels were about sixfold higher than their counterparts at normal pH (Table 3). Since the amount of total M2-PK protein was not affected by low pH, the sixfold increase in Tumour M2-PK value indicate a strong dimerization of M2-PK in Colo357 cells at acidic pH. In Panc-1 cells, Tumour M2-PK values were not significantly affected by the acidification of the medium (Table 3).
Discussion
This study has compared M2-PK expression and tumour M2-PK levels in a non-metastatic and a metastatic human pancreatic cancer cell line with control cell lines and evaluated the effect of changes in the pancreatic tumour microenvironment on M2PK levels. Panc-1 is an epithelioid cell line derived from a primary human pancreatic carcinoma of ductal cell origin [20] whereas, Colo357 originated from a lymph node metastasis of a pancreatic adenocarcinoma [21]. Previous immunohistological studies have demonstrated that M2-PK expression in primary tumours is usually heterogeneous whereas metastases have a homogeneous expression [4]. In accordance with the immunohistological results, in the current study, the metastatic Colo357 cells contained about fourfold more M2-PK protein and about 3.5-fold more dimeric M2-PK than the Panc-1 cells which derived from a primary tumour. Elevated levels and activities of M2-PK have also been found in other cancer cell lines with high metastatic potential such as MHCC97 (human hepatocellular carcinoma) and H.Ep.2 (human laryngeal carcinoma) [3, 22]. The amount of M2-PK protein in Panc-1 cells was similar to that in MCF-7 cells, a cell line derived from a human breast cancer [23]. However, in MCF-7 cells Tumour M2-PK levels normalised against M2-PK protein were about threefold higher than that in Panc-1 cells which indicates that in MCF-7 cells the tetramer/dimer ratio of M2-PK was more shifted towards the dimeric form than in Panc-1 cells. In comparison to the tumour cell lines Colo357, MCF-7 and Panc-1, non-tumour cell line HMEC-1 contained the lowest amount of total M2-PK protein as well as the lowest amount of dimeric M2-PK, which is in accordance with the finding that normal proliferating cells are characterised by a higher amount of the tetrameric form whereas in tumour cells the tetramer/dimer ratio is shifted towards the dimeric [4]. The dimerization of M2-PK in tumour cells is caused by interaction with different oncoproteins, i.e., pp60v-src, HPV-16 E7, A-Raf [4].
In all four cell lines, Tumour M2-PK levels decreased with increasing cell density. Dependencies upon cell density have also been found for other enzymes and cell lines and also for intracellular metabolites and metabolic flux rates [24]. In contrast to tumour M2-PK the total M2-PK expression did not show any dependency upon cell density. The microenvironment of solid tumours is characterised by varying oxygen and glucose supply and low pH values due to the release of acidic metabolic products such as lactate [13, 14]. In the present study, we simulated different nutrient supply conditions in solid tumours by culturing the two pancreatic cancer cells lines (Colo357 and Panc-1) under hypoxia, glucose deprivation and low pH value, respectively. As shown by western blot analysis, the different cultivation conditions had no effect on the overall content of M2-PK protein. However, different effects were found on the Tumour M2-PK levels and cell doublings. In Colo357 cells, a fourfold increase of Tumour M2-PK under hypoxia, a threefold increase under glucose deprivation and about 6.5-fold increase at low pH value were found. Since total M2-PK values were not changed under the different cultivations conditions, the increase of Tumour M2-PK values points to a dimerization of M2-PK under all three cultivation conditions. In contrast to Colo357 cells, mean levels of Tumour M2-PK in Panc-1 cells were slightly but not significantly increased under hypoxia and glucose deprivation and slightly but not significantly decreased at low pH. Acidification of tumour cell environment is a consequence of upregulated aerobic glycolysis with increased lactate, H+ and CO2 production. The intracellular pH value in tumour cells is usually in the range between 7.0 and 7.2 [25]. Intracellular H+ ions and lactic acid are transported out of the cells by membrane bound Na+/H+ exchangers (NHE-1) and H+/lactic acid co-transporters while CO2 diffuses rapidly across the plasma membrane and is converted to carbonic acid by membrane-bound ectoenzyme carbonic anhydrase [26]. The uptake of the weak base HCO −3 via a member of the Na+-dependent and Na+-independent Cl−/HCO −3 exchangers contributes to an intracellular alkalinisation [26]. The resulting extracellular pH in most solid tumours is usually acidic (5.8-7.2) [27]. The pH value used for acidic condition in our study was within this range. An extracellular acidic environment helps in tumour invasion by killing of normal cells and allowing clonal selection of tumour cells by caspase mediated activation of p53 dependent apoptosis [28, 29].
The dimerization of M2-PK observed in Colo357 cells at low pH value may reduce the amount of lactate released from tumour cells into their environment thereby preventing further acidification. This may explain why Colo357 cell doubling was not affected by low pH whereas in Panc-1 cells which were unable to increase the dimeric form of M2-PK suppression of cell proliferation took place. The dimerization of M2-PK observed in glucose-deprived Colo357 cells is presumably caused by a decrease of the key M2-PK regulator fructose 1,6-P2 as previously described by Ashizawa et al [12]. Under glucose deprivation, a high amount of the dimeric M2-PK favours the channelling of the reduced glucose carbons available into synthetic processes. When glutaminolysis provides an alternative source for energy generation, the dimerization of M2-PK may enable tumour cells to proliferate even under low glucose supply. In our glucose-deprived experiments, oxygen was not limited. Therefore, oxygen-dependent glutaminolysis was available as alternative source for energy generation [4, 30]. Thus, in glucose deprived Colo357 cells proliferation was slightly reduced but not completely suppressed.
Under hypoxia, mitochondrial respiration and glutaminolysis fail as energy sources since both pathways depend on oxygen supply. In both cell lines under hypoxia, the total content of M2-PK protein was not changed which may indicate that although the M-gene which encodes for the pyruvate kinase isoenzyme type M2 has hypoxia responsive site [31], hypoxia may not necessarily upregulate M2-PK levels.
In Colo357 cells, the fourfold increase of the dimeric form of M2-PK under hypoxic conditions suggests that the Colo357 cells may be unable to shift to glycolytic energy regeneration at low oxygen supply. The dimerization of M2-PK together with the inhibition of the oxygen-dependent energy regeneration by mitochondrial respiration and glutaminolysis may explain the strong inhibition of cell proliferation in Colo357 cells. In Panc-1 cells, which did not show a significant effect of hypoxia on Tumour M2-PK, cell population doubling was not significantly affected.
In conclusion, we have demonstrated that neither in the non-metastatic Panc-1 cell line nor in the metastatic Colo357 cell line the level of M2PK enzyme was affected by hypoxia, glucose deprivation or acidic pH. However, the changes to the tumour environment had a major effect on tumour cell proliferation and the level of the tumour associated dimeric M2-PK. The dimerization of M2-PK under adverse tumour conditions may have a role in clonal selection and tumour progression, which requires further investigation.
References
Warburg O, Poesener K, Negelein E. Über den Stoffwechsel der Tumoren. Biochem Z. 1924;152:319–44.
Gatenby RA, Gillies RJ. Why do cancers have high aerobic glycolysis? Nat Rev Cancer. 2004;4:891–9.
Board M, Humm S, Newsholme EA. Maximum activities of key enzymes of glycolysis, glutaminolysis, pentose phosphate pathway and tricarboxylic acid cycle in normal, neoplastic and suppressed cells. Biochem J. 1990;265:503–9.
Mazurek S, Boschek CB, Hugo F, Eigenbrodt E. Pyruvate kinase type M2 and its role in tumor growth and spreading. Semin Cancer Biol. 2005;15:300–8.
Christofk HR, Vander Heiden MG, Harris MH, Ramanathan A, Gerszten RE, Wei R, et al. The M2 splice isoform of pyruvate kinase is important for cancer metabolism and tumour growth. Nature. 2008;452:230–33.
Cerwenka H, Aigner R, Bacher H, Werkgartner G, el Shabrawi A, Quehenberger F, et al. TUM2-PK (pyruvate kinase type tumor M2), CA19-9 and CEA in patients with benign, malignant and metastasizing pancreatic lesions. Anticancer Res. 1999;19:849–51.
Kumar Y, Gurusamy K, Pamecha V, Davidson BR. Tumor M2-pyruvate kinase as tumor marker in exocrine pancreatic cancer a meta-analysis. Pancreas. 2007;35:114–9.
Novotny I, Dite P, Dastych M, Zakova A, Trna J, Novotna H, et al. Tumor marker M2-pyruvate-kinase in differential diagnosis of chronic pancreatitis and pancreatic cancer. Hepatogastroenterology. 2008;55:1475–7.
Ventrucci M, Cipolla A, Racchini C, Casadei R, Simoni P, Gullo L. Tumor M2-pyruvate kinase, a new metabolic marker for pancreatic cancer. Dig Dis Sci. 2004;49:1149–55.
Mazurek S, Luftner D, Wechsel HW, Schneider J, Eigenbrodt E. Tumour M2-PK: a marker of the tumour metabolome. In: Diamandis E, Fritsche H, Lilja H, Chan DW, Schwartz M, editors. Tumour markers: physiology,pathobiology, technology and clinical applications. Washington DC: AACC Press; 2002. p. 471–5.
Kumar Y, Tapuria N, Kirmani N, Davidson BR. Tumour M2-pyruvate kinase: a gastrointestinal cancer marker. Eur J Gastroenterol Hepatol. 2007;19:265–76.
Ashizawa K, Willingham MC, Liang CM, Cheng SY. In vivo regulation of monomer-tetramer conversion of pyruvate kinase subtype M2 by glucose is mediated via fructose 1, 6-bisphosphate. J Biol Chem. 1991;266:16842–6.
Gottfried E, Kunz-Schughart LA, Ebner S, Mueller-Klieser WF, Hoves S, Andreesen R. Tumor-derived lactic acid modulates dendritic cell activation and antigen expression. Blood 2006 Mar 1;107:2013-21.
Vaupel P, Kallinowski F, Okunieff P. Blood flow, oxygen and nutrient supply, and metabolic microenvironment of human tumors: a review. Cancer Res. 1989;49:6449–65.
Maxwell PH, Ratcliffe PJ. Oxygen sensors and angiogenesis. Semin Cell Dev Biol. 2002;13:29–37.
Ranniger K, Saldino RM. Arteriographic diagnosis of pancreatic lesions. Radiology. 1966;86:470–4.
Cuvier C, Jang A, Hill RP. Exposure to hypoxia, glucose starvation and acidosis: effect on invasive capacity of murine tumor cells and correlation with cathepsin (L + B) secretion. Clin Exp Metastasis. 1997;15:19–25.
Cui H, Darmanin S, Natsuisaka M, Kondo T, Asaka M, Shindoh M, et al. Enhanced expression of asparagine synthetase under glucose-deprived conditions protects pancreatic cancer cells from apoptosis induced by glucose deprivation and cisplatin. Cancer Res. 2007;67:3345–55.
Dixon WJ, editor. BMDP Statistical software manual. Berkeley, Los Angeles: Oxford University of California Press; 1992.
Lieber M, Mazzetta J, Nelson-Rees W, Kaplan M, Todaro G. Establishment of a continuous tumor-cell line (panc-1) from a human carcinoma of the exocrine pancreas. Int J Cancer. 1975;15:741–7.
Morgan RT, Woods LK, Moore GE, Quinn LA, McGavran L, Gordon SG. Human cell line (COLO 357) of metastatic pancreatic adenocarcinoma. Int J Cancer. 1980;25:591–8.
Ding SJ, Li Y, Shao XX, Zhou H, Zeng R, Tang ZY, et al. Proteome analysis of hepatocellular carcinoma cell strains, MHCC97-H and MHCC97-L, with different metastasis potentials. Proteomics. 2004;4:982–94.
Dickson RB, Bates SE, McManaway ME, Lippman ME. Characterization of estrogen responsive transforming activity in human breast cancer cell lines. Cancer Res. 1986;46:1707–13.
Mazurek S, Michel A, Eigenbrodt E. Effect of extracellular AMP on cell proliferation and metabolism of breast cancer cell lines with high and low glycolytic rates. J Biol Chem. 1997;272:4941–52.
Webb SD, Sherratt JA, Fish RG. Mathematical modelling of tumour acidity: regulation of intracellular pH. J Theor Biol. 1999;196:237–50.
Pouyssegur J, Dayan F, Mazure NM. Hypoxia signalling in cancer and approaches to enforce tumour regression. Nature. 2006;441:437–43.
Wike-Hooley JL, van den Berg AP, van der ZJ, Reinhold HS. Human tumour pH and its variation. Eur J Cancer Clin Oncol. 1985;21:785–91.
Park HJ, Lyons JC, Ohtsubo T, Song CW. Acidic environment causes apoptosis by increasing caspase activity. Br J Cancer. 1999;80:1892–7.
Williams AC, Collard TJ, Paraskeva C. An acidic environment leads to p53 dependent induction of apoptosis in human adenoma and carcinoma cell lines: implications for clonal selection during colorectal carcinogenesis. Oncogene. 1999;18:3199–204.
Rossignol R, Gilkerson R, Aggeler R, Yamagata K, Remington SJ, Capaldi RA. Energy substrate modulates mitochondrial structure and oxidative capacity in cancer cells. Cancer Res. 2004;64:985–93.
Shimizu T, Uehara T, Nomura Y. Possible involvement of pyruvate kinase in acquisition of tolerance to hypoxic stress in glial cells. J Neurochem. 2004;91:167–75.
Acknowledgements
The authors are thankful to ScheBo Biotech, Giessen, Germany for their partial support for the research work done.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kumar, Y., Mazurek, S., Yang, S. et al. In vivo factors influencing tumour M2-pyruvate kinase level in human pancreatic cancer cell lines. Tumor Biol. 31, 69–77 (2010). https://doi.org/10.1007/s13277-009-0010-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-009-0010-3