Abstract
We hypothesized that a part of therapeutic effects of endurance training on insulin resistance is mediated by increase in cardiac and skeletal muscle mitochondrial lactate transporter, monocarboxylate transporter 1 (MCT1). Therefore, we examined the effect of 7 weeks endurance training on the mRNA and protein expression of MCT1 and MCT4 and their chaperon, CD147, on both sarcolemmal and mitochondrial membrane, separately, in healthy and type 2 diabetic rats. Diabetes was induced by injection of low dose of streptozotocin and feeding with high-fat diet. Insulin resistance was confirmed by homeostasis model assessment-estimated insulin resistance index and accuracy of two membranes separation was confirmed by negative control markers (glucose transporter 1 and cytochrome c oxidase. Real-time PCR and western blotting were used for mRNA and protein expression, respectively. Diabetes dramatically reduced MCT1 and MCT4 mRNA and their expression on sarcolemmal membrane whereas the reduction in MCT1 expression was less in mitochondrial membrane. Training increased the MCT1 mRNA and protein expression in both membranes and decreased insulin resistance as an adaptive consequence. In both tissues increase in CD147 mRNA was only parallel to MCT1 expression. The response of MCT1 on sarcolemmal and mitochondrial membranes was different between cardiac and skeletal muscles which indicate that intracellular lactate kinetic is tissue specific that allows a tissue to coordinate whole organism metabolism.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Insulin resistance—the decreased ability of insulin to regulate glucose utilization by tissue—is a major feature of noninsulin-dependent diabetes mellitus (NIDDM) [12]. The pathophysiological mechanism of insulin resistance in type 2 diabetic patients is multifactorial [4]. Substrate availability and substrate competition between lactate, free fatty acids, and glucose for oxidation have been suggested as two mechanisms to exacerbate muscle insulin resistance and glucose intolerance [12]. An increase in blood lactate is often seen in type 2 diabetic patients, ranging from 0.6 mmol/l in lean subjects to 0.8 and 1.1 mmol/l in obese and NIDDM patients, respectively [14]. This hyperlactatemia is also present in skeletal muscle that suppresses the uptake and intracellular metabolism of glucose by impairment in insulin signaling pathways [11].
The lactate concentration in muscle is a result of its flux into and out of the muscle cells. Transport of lactate across the plasma membrane is performed in a pH-dependent manner and mediated by a family of proton-coupled monocarboxylate transporters (MCTs) [1, 5]. The two most common isoforms found in cardiac and skeletal muscles are MCT1 and MCT4, and their distribution is tissue specific [1, 7]. MCT1 is highly expressed in oxidative tissue and facilitates lactate uptake at both the sarcolemmal and mitochondrial membranes [5]; whereas, MCT4 is found predominantly in glycolytic fibers and its putative role is lactate extrusion [5]. MCTs expressions are regulated by variety of stimuli. Contractile activity [6], exercise [15], and hypoxia [35] increase their expression while denervation [30], hind limb suspension [16], and hyperlactatemia have a negative effect [23].
The latter have been reported in type 2 diabetic patients in both plasma [31] and skeletal muscle [33], and disturbance in whole body lactate turnover appears to be important in the development on insulin resistance. The increased plasma lactate level accelerates hepatic gluconeogenesis and elevates fasting plasma glucose as a consequence [31]. On the other hand, elevated concentration on lactate in skeletal muscle can compete with glucose for aerobic oxidation in peripheral tissue [12].
It has been suggested that diabetic hyperlactatemia found in type 2 diabetes could be more related to a decreased in lactate uptake [17] and the decrease in MCT1 and MCT4 expressions in cardiac and skeletal muscles as the major consumers of lactate [17]. Coexpression studies in cultured cells suggest that CD147, a ubiquitous type I single-span transmembrane glycoprotein of the Ig superfamily [13], is required for normal expression of MCT1 and MCT4 [13]. A previous study showed that CD147 play an important role for delivery of MCT1 and MCT4 to the plasma membrane [24] and CD147 knockout mice fail to express MCT1, MCT3, and MCT4 in retinal cells, even when their mRNAs are present [36]. However, there is little information about the CD147 expression in type 2 diabetes, and the role of CD147 in the regulation of MCT1 and MCT4 expressions in type 2 diabetes remains elusive. Therefore, the aim of this study is to investigate (1) the MCT1, MCT4, and their chaperon CD147 expression in heart and skeletal muscle of type 2 diabetic rats and (2) the effects of endurance training on MCT1 and MCT4 expressions in both sarcolemmal and mitochondrial membranes as rate-limiting sites for lactate uptake and oxidation, respectively and their consequences on plasma and muscle lactate concentration and insulin resistance.
Method
Animals
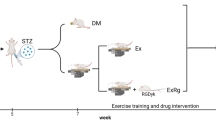
Male Wistar rat (5 weeks old) were purchased from Pastor Institute (Tehran) and housed in an air-conditioned room (temperature, 22 ± 3 °C) on a 12-h light–12-h dark cycle. All rats were fed rat chow for 2 weeks ad libitum, and their body weights were measured daily. After an acclimation period of 2 weeks, the animals were assigned randomly into four groups, according to their body weight: control (C; n = 10), trained (T; n = 10), diabetic control (DC; n = 15), and trained diabetic (TD; n = 15). Four animals—three and one from DC and TD, respectively—were died during the experiment and nine rats from each group were used for final measurements. Ethical approval for experimental protocol was obtained from the ethical Committees on Animal Care at the endocrinology and metabolism research center of Tehran University.
Diabetes induction procedure
At the onset of 8 weeks of age, the rats from diabetic groups were fed high-fat diet (Table 1) for 2 weeks and then diabetes was induced by intraperitoneal injection of streptozotocin (STZ; 35 mg/kg, ip) in a 0.1-M citrate buffer (pH 4.5) [43]; 48 h after the STZ injection, nonfasting glucose concentrations were determined via blood sample that were taken from the orbital sinus. Blood collected via heparinized tube and plasma separation was performed by centrifugation at 3,000×g for 10 min at 4 °C. Plasma glucose concentration was determined by glucose oxidase method [48], and the animal showing FBG of ≥300 mg/dl were considered as type 2 diabetic [43]. Feeding high-fat diet was continued for 7 weeks for diabetic groups; whereas, the animals of the C and T groups were given standard pellet diet.
Training intervention
Endurance training was started at 10 weeks of age and performed every day for 7 weeks. Initially, the TD and T groups were familiarized with a motor-driven treadmill running at low speeds (15–20 m/min) for 20 min/day for the first 5 days. Thereafter, the speed and duration were increased progressively over the 7-week period until the animals were running at 30 m/min for 35 min for the last 2 weeks. The control and sedentary diabetic animals remained sedentary in their cages for the duration of the 7-week training program.
Collection of blood and tissue samples
After the end of experimental protocol, all the animals were fasted overnight but allowed free access to water. The following morning, animals were anesthetized (ketamin (90 mg/kg) and xylazin (10 mg/kg), ip), and the soleus, extensor digitorumlongus (EDL) muscles, and heart were excised rapidly, frozen in liquid nitrogen, and stored at −80 °C for subsequent analysis. Blood sample was withdrawn by heart puncture, plasma separated as above, and stored at −80 °C. These samples were used for measurement of FBG, fasting plasma insulin, fasting serum lactate concentration, and plasma lipid profile.
Insulin resistance confirmation
Two following conditions were considered for selection of insulin resistance type 2 diabetes rats:
-
1.
Fasting plasma insulin concentration above 60 pmol/l
-
2.
homeostasis model assessment-estimated insulin resistance (HOMA-IR) index of >2.5 [29]. HOMA-IR values were estimated using the following formula:
$$ \mathrm{HOMA}-\mathrm{IR}\ \mathrm{index}=\mathrm{fasting}\ \mathrm{plasma}\ \mathrm{insulin}\ \left(\upmu \mathrm{U}/\mathrm{ml}\right)\times \mathrm{fasting}\ \mathrm{plasma}\ \mathrm{glucose}\ \left(\mathrm{mmol}/\mathrm{l}\right)/22.5 $$Normal if <2.5, marker of insulin resistance if ≥2.5 [29]
Biochemical measurement
Plasma glucose was determined by the glucose oxidase method [48]. Plasma insulin concentration was measured by ELISA technique (mouse/rat insulin ELISA kit, cat. No. EZRMI-13K). The sensitivity of the assay was 0.1 ng/ml and the intra- and inter-assay coefficients were lower than 10 %. Total cholesterol and triglycerides were determined by the clinical lab of our research center. Plasma and muscle lactate concentrations were determined by lactate assay kit (cat. No. K607-100, Biovision) as follows: 50 μl of serum sample aliquot was mixed with 200 μl of ice-cold 7 % perchloric acid and muscle lactate content was determined from perchloric acid extracts. Approximately 50 mg of muscle samples were powdered and incubated for 10 min in 8 vol. of ice-cold 6 % perchloric and centrifuged at 1,500×g for 10 min at 4 °C [21]. The supernatant was removed and then lactate concentration was measured according to manufacturer’s instructions for both muscle and serum samples.
Western blotting
Approximately 150–200 mg from each tissue was powdered with cold mortar and pestle in liquid nitrogen and sarcolemmal fractions (SL) and mitochondrial fractions (MI) were isolated as previously described [10]. Briefly, tissue were homogenized in ice-cold solution A (210 mM sucrose, 2 mM EGTA, 40 mM NaCl, and 30 mM HEPES, pH 7.4). The homogenate was centrifuged at 1,000×g for 10 min at 4 °C to eliminate erythrocyte material. Pellet was removed and centrifuged at 10,000×g for 20 min at 4 °C. The pellet was washed in 1 ml of buffer B (1 mM EDTA and 10 mM Tris, pH 7.4) and then resuspended in 100 μl of buffer C and 33 μl of 16 % SDS and centrifuged at room temperature for 20 min to remove any insoluble materials. This sample was considered as MI fraction. Supernatant was diluted with 0.75 ml of buffer C (1.167 M KCl and 58.3 mM Na4P2O7·10H2O, pH 7.4) and centrifuged in a Beckman ultracentrifuge at 230,000×g for 120 min at 4 °C to remove contractile proteins. The pellet was washed in 1 ml of buffer B and resuspended in 100 μl of buffer C and 33 μl of 16 % SDS and centrifuged at room temperature for 20 min to remove any insoluble materials. Supernatants containing SL were aliquoted and stored at −80 °C for subsequent analysis. Total protein was determined via Bradford technique using bovine serum albumin as a standard; 20 μg total protein of each sample was loaded and separated on 12 % SDS-PAGE and transferred by electroblotting onto polyvinylidenedifluoride membranes (Amersham). Membranes were incubated for 1 h at room temperature on an orbital shaker in 10 % blocking buffer (150 mM NaCl, 0.1 % Tween 20, and 50 mM Tris; pH 7.5 (TTBS)), 5 % skimmed milk and incubated in primary antibody overnight at 4 °C (in Tris-buffered saline). Membranes were washed once for 15 min and then twice for 5 min in TTBS and then incubated for 90 min at room temperature with secondary antibody in Tris-buffered saline. Membranes were washed as above, and protein expression was then detected by enhanced chemiluminescence according to manufacture instructions. Autoradiographic film were exposed to membranes and developed. Molecular weight standards were used to identify appropriate antibody binding. Band densities were determined with ImageJ densitometer software. Rat erythrocyte ghost was used as a positive control and to fix an arbitrary unit to allow comparison between experiments (1 equals the MCT1 signal generated by 5 μg of rat erythrocyte ghost).
Rat erythrocyte ghost preparation
Fresh blood from a rat was mixed with 7 vol. of acid-citrate-dextrose buffer (75 mM sodium citrate, 38 mM citric acid, and 138 mM d-glucose) and centrifuged at 16,000×g. The supernatant and buffy coat are removed and pellet washed thrice in 66 mM NACL. The sedimented cell was diluted in 66 mM NaCl for 25 % cell suspension. Cell suspension mixed with hemolyzed buffer (1 mM EDTA, 9.64 mM NaCl, 3.61 mM Na2HPO4, and 1.2 mM KH2PO4; pH 7.2) in 1:7 volume ratio and placed on ice for 20 min. The solution was centrifuged at 20,000×g for 15 min at 4 °C, and pellet diluted with ten times volume of buffer containing 9.6 mM Tris-HCl, 20 mM NaCl; pH 7.2) and washed once in this buffer and again in buffer containing 4.8 mM Tris-HCl and 10 mM NaCl. Pellet washed once in 100 mM KCl and two times in water and diluted in CO2-free water [41].
Real-time PCR
Tissue was powdered with cold mortar and pestle and total RNA was isolated using Isol RNA-Lysis reagent. Approximately 50 mg of powdered tissue was added to 1 ml ice-cold Isol and homogenized. Homogenates were centrifuged at 12,000×g for 10 min at 4 °C to remove pellet. Chloroform (200 μl) was added to the supernatant fraction and shaken vigorously for 15 s. The organic and aqueous phases were separated by centrifugation at 12,000×g for 15 min. The aqueous phase was removed, 600 μl isopropanol was added, and RNA was isolated according to the manufacturer’s instructions. RNA concentration and purity was estimated by OD 260/280.
cDNA synthesis was performed with 1 μg RNA in a total reaction volume of 20 μl using random hexamer oligonucleotides. Reverse transcriptase reactions were performed according to the manufacturer’s instructions. Quantitative real-time PCR was performed using a 7300 Real-Time PCR System (Applied Biosystems, Step One, Germany). The PCR reaction was carried out using SYBR Green II, and ROX was used as a reference dye. The thermocycling conditions were: 10 min at 95 °C, followed by 40 cycles of 95 °C for 15 s and 60 °C for 60 s. The primer sequences used are listed in Table 2.
Gene expressions were expressed relative to the expression of the 18S housekeeping gene. To avoid detection of nonspecific PCR products, the purity of each amplified product was confirmed using a melting curve analysis. Data quantification was carried out using the 2−∆∆CT method [26]. Primer amplification efficiencies were determined using serial cDNA dilutions and should be approximately equal [26].
Statistical analysis
Data are expressed as means ± SE. The difference between variables calculated using one-way ANOVA completed with Tukey’s post hoc test. In all comparisons, the significant level was set at α = 0.05.
Results
Body weight
At the start of the study, there were no differences in body weight between the four groups of animals. Increase in the body weights of the diabetic groups slightly decreased in the first few days after the onset of diabetes, and then body weight continue to increase normally. After 3 weeks, the difference in body weight between the DC group and others was significant (P < 0.05) and did not return to a nonsignificant level up to the end of the study.
Plasma glucose and insulin concentration and HOMA-IR index
The plasma glucose, insulin, TG, total cholesterol, and HOMA-IR index values in four groups are shown in Table 3. As expected, at the end of the study, in the DC and TD groups, plasma glucose concentrations were higher than both C and T groups (P < 0.01; Table 3). Compared with the DC, endurance training significantly reduced plasma glucose concentrations in the TD, but the difference was still significant between the TD and both C and T groups. Plasma insulin and HOMA-IR index, measured at the end of the 7-week study were significantly higher in the DC and TD groups, in comparison to sedentary and trained animals (P < 0.01; Table 3). However, with training, both plasma insulin and HOMA-IR index at rest were significantly decreased in the TD group than DC animals (P < 0.05; Table 3). The difference was still significant between the TD and both C and T groups (P < 0.01; Table 3).
Plasma and lactate concentration
Blood lactate concentrations, measured at rest at the onset of the study did not significantly differ among four groups although higher values were found in diabetic groups in comparison to healthy animals (Table 4). In contrast, at the end of the 7-week study in the DC animals, the resting plasma lactate concentration was significantly higher than the T and C groups (P < 0.01; Table 4). Endurance training decreased plasma lactate concentrations in the TD but the difference was not significant with DC.
At the end of the study, soleus lactate concentration in the DC was significantly higher than the T and C (P < 0.01; Table 4) and TD groups (P < 0.05). However, with training, the soleus lactate concentration at rest was lowered to the levels observed in the C animals where no significant difference was observed (Table 4). Similar results were found for EDL muscle.
In cardiac, no significant difference was observed between DC and C groups and endurance training significantly decreased the cardiac lactate concentration in the T groups in comparison to the TD and DC (P < 0.01; Table 4) and C groups (P < 0.05).
MCT1 and MCT4 expressions
Diabetes-induced changes on MCT1 expression
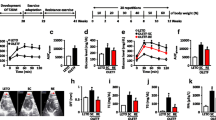
In SL fraction, after 7 weeks of type 2 diabetes induction, the MCT1 expression of the soleus (P < 0.01), EDL (P < 0.01), and heart (P < 0.01) were significantly less in the DC in comparison to the C group (Fig. 1). No difference was observed among MCT1 expression in MI fractions in any of the above tissues in DC than C group.
MCT1 expression of EDL, soleus, and heart at both SL and MI fractions at the end of the study relative to control: MCT1 signal generated by 5 μg of rat erythrocyte ghost. Values are means ± SD, C (n = 9), T (n = 9), DC (n = 9), and TD (n = 9). *P < 0.05; **P < 0.01, significant difference between groups
Effects of training on MCT1 expression
After 7 weeks of endurance training, the MCT1 expression in SL fractions of the soleus (P < 0.05), EDL (P < 0.01), and heart (P < 0.01) were significantly higher in T in comparison to DC group. Also in MI fractions, significant differences, soleus (P < 0.01), EDL (P < 0.01), and heart (P < 0.01), were found between DT and CD.
There were also training-induced increases in MCT1 expression in SL fractions of the soleus (P < 0.01) and EDL (P < 0.05) in the T group in comparison to C. The significant differences soleus (P < 0.05), EDL (P < 0.01), and heart (P < 0.01) were also observed between these groups (P < 0.01; Fig. 1).
Diabetes-induced changes on MCT4 expression
After 7 weeks of type 2 diabetes induction, the MCT4 expression of the soleus (P < 0.01) and EDL (P < 0.05) were significantly less in the DC in comparison to the C group (Fig. 2).
Effects of training on MCT4 expression
After 7 weeks of endurance training, the MCT4 expression in the soleus (P < 0.05) and EDL (P < 0.01) were significantly higher in the T in comparison to DC group. Also, significant differences in MCT4 expression only observed in the EDL (P < 0.01) between T and C groups (P < 0.05).
MCT1 and MCT4 mRNA
mRNA content was determined among tissue, and for below analyses, the data in the C control group have been set to 100 % for each tissue. After 7 weeks of type 2 diabetes induction, the MCT1 mRNA content of soleus (P < 0.01), EDL (P < 0.01), and heart (P < 0.05) decreased in DC as compared with the C group (Fig. 3).
Effects of training on MCT1 mRNA
After 7 weeks of endurance training, the MCT1 mRNA content of soleus (P < 0.05), EDL (P < 0.01), and heart (P < 0.01) were significantly higher in the T than DC group (Fig. 3). Significant difference was also found for the MCT1 mRNA in EDL (P < 0.01) in the T and TD.
After 7 weeks of type 2 diabetes induction, the MCT4 mRNA content of soleus (P < 0.01) and EDL (P < 0.05) decreased in the DC as compared with the C group (Fig. 4) and after 7 weeks of endurance training, significant increase in MCT4 mRNA was observed in soleus (P < 0.01) and EDL (P < 0.05) in the T than DC (Fig. 4). Significant increase (P < 0.01) was also found after 7 weeks of endurance training in the TD than TC (Fig. 4).
CD147 mRNA
After the end of the experiment, the CD147 mRNA content of soleus (P < 0.01) and heart (P < 0.01) were significantly decreased in the DC than T group (Fig. 5).
Membranes cross-contamination control
To assess cross contamination of the membrane fractions, we used cytochrome c oxidase (COX) as a marker of the mitochondrial membrane and as markers of the SL fraction. Contamination of the SL fraction by mitochondrial remnants was negligible because of the relatively lower amount of COX measured in the SL fraction, as suggested by the low ratios of COX in the SL fraction to COX in the MI fraction. On the other hand, the abundance of glucose transporter (GLUT)-1 in the SL fraction confirms that plasma membrane proteins were concentrated in that fraction (Fig. 6).
Discussion
We have examined the effects of type 2 diabetes on MCT1 and MCT4 mRNA and protein expression and their chaperone CD147 in rat cardiac and skeletal muscles. The novel results in this study are as follows: (1) type 2 diabetes markedly decreases MCTs and their chaperone CD147 expression at both transcriptional and translational level in cardiac and skeletal muscle in a fiber type-specific manner, (2) exercise-induced increase in cardiac and skeletal muscles mitochondrial MCT1 attenuate their resting lactate concentration and decrease insulin resistance as a consequence, and (3) exercise-induced alterations in MCT1 expression on sarcolemmal and mitochondrial membrane are tissue specific.
In the present study, diabetes was induced by consumption of high-fat diet and low-dose injection of STZ. The fat used in our experiment was tallow which mainly consists of saturated (43 %), monounsaturated fatty acids (50 %), and polyunsaturated fatty acids (5 %). So in our experiment, the unwanted changes in oxidative stress resulting from polyunsaturated fatty acids consumption could be negligible. Induction of type 2 diabetes was confirmed by the very high concentrations of glucose and occurrence of insulin resistance was established by the high values of HOMA-IR index, plasma fasting insulin concentration [42, 50]. High-fat diet in combination of low-dose STZ injection influenced the blood level of glucose, triglyceride, and cholesterol, as was indicated in animals of the C group. Due to substrate competition among fatty acids and glucose metabolic-related production, hyperglycemia increased the lipid level in blood [37], and the triglycerides and glucose level increased in sedentary diabetic animal. Since the incessant existence of hyperglycemia and hypertriglyceridemia would confuse the metabolic pathways of other lipids [37] and the blood cholesterol level increased in sedentary diabetic animals. During the course of this study, the nondiabetic animals gained weight at a normal rate, as reported elsewhere [17], whereas the DC animals gained weight at a faster rate, as has been shown previously [38, 43, 50]. Thus, the feeding of HFD for a period of 9 weeks produced rats with insulin resistance syndrome as was characterized by the increased body weight (obesity), hyperglycemia, hypertriglyceridemia, hypercholesterolemia, and compensatory hyperinsulinemia which can confirm the development of type 2 diabetes in this study.
In the other hand, 7 weeks of endurance training decreased fasting plasma glucose concentration in TD animals. Endurance training can decrease the plasma glucose concentration via increase in insulin sensitivity [2, 20], GLUT-4 expression in skeletal muscle sarcolema membrane [25], and its translocation to plasma membrane [25]. Also at the end of study, plasma insulin concentration decreased in TD animals. This exercise-induced reduction can occur via increase in IRS-2 expression [34], PI3P pathway activity [19], and MAPK [19], all together these changes can lead to improve insulin signaling pathway and decrease resting blood insulin concentration as a consequence.
Diabetes induction increased the resting plasma lactate concentrations in both diabetic groups where the values were significantly higher than healthy groups. This result has been reported and confirmed by previous studies [17, 33]. Surprisingly, we did not find any significant decrease in plasma lactate concentration in TD in comparison to CD, despite a tendency to decrease with training. As we found the significant increase in sarcolemmal MCT1 expression, it can be speculated that factors other than the decrease in lactate uptake contribute to hyperlactatemia in NIDDM. In fact, adipose tissues have been shown to release abnormal amounts of lactate in obesity [33]. Therefore, we also measured MCT1 gene expression in adipocytes and found that MCT1 mRNA was significantly higher in diabetic groups (unreported data). As we did not observe significant difference in MCT1 expression in adipocytes between CD and TD, we can hypothesize that this tissue did not benefit from endurance training to the same extent as muscle and still released lactate into the circulation. According to literature, in this cell type MCT1 may be the predominant isoform and it has been reported that under certain condition such as hypoxia MCT1 can export lactic acid into the circulation [35]. This could partially explain why we did not find a significant decrease of plasma lactate level after training. Also, the elevation of plasma lactate concentration in diabetic animals might be a consequence of increase in fat mass in these groups. Although we did not determine the fat mass, more weight gain occurred in DC animals, and possible expanded fat mass in this group can also partially explain the increased plasma lactate concentration.
However, skeletal muscle lactate concentration was significantly decreased following training. This can be explained by the increase in muscle oxidative activity, reflected by an increase in cytochrome oxidase content (unreported data), which could have led to an increased skeletal muscle lactate clearance. Also, we observed the significant increase in mitochondrial MCT1 expression in both heart and skeletal muscle that lead to increase of lactate uptake by mitochondria and its oxidation as a consequence. This exercise-induced reduction in skeletal muscle has physiological implications as elevated muscle lactate has been implicated in the development of insulin resistance. Indeed, lactate infusion in animals has been shown to induce insulin resistance in skeletal muscle, decreasing glucose utilization [47] and impairing insulin signaling [11]. Moreover, competition between glucose and FFA was introduced by Randle, and a similar competitive effect has also been shown between glucose and lactate [28]. In skeletal muscle, lactate can be converted to pyruvate and added to the glucose-derived pyruvate and both may be further oxidized in the tricarboxylic acid cycle. From a point of view based on energy, lactate appears to be a more efficient substrate compared with glucose and can be directly oxidized via the PDH complex [28] which leads to a decrease in the glucose uptake promoting insulin resistance as a consequence.
This study showed that MCT1 and MCT4 belonged to a class of metabolic genes that are responsible to exercise training. However, the decrease in MCT1 and MCT4 expressions in the DC animals also indicate that other factors such as endocrine (hyperinsulinemia) or metabolic changes may be involved in their expression. The former was shown in the study by Bonen et al. where the injection of testosterone for 1 week changed the MCT1 and MCT4 expressions in skeletal muscle [18].
In this study, the effects of diabetes and exercise occurred at both transcriptional and translational level but vary in a different way between MCT1 and MCT4. MCT4 was more affected by transcriptional mechanisms than MCT1. The very long 3′ untranslated region of MCT1 (1.6 kb) may be involved in the translational repression [32]. However, exercise training lead to increase in the MCT1 and MCT4 mRNA. It has been shown that exercise training can increase the expression of MCT1 by upregulating PGC1-α expression. The upregulation of PGC1-α was reported previously in other studies by contractile activity [3] or exercise training in rat [44] and human [39]. The release of Ca2+ by exercise training can promote Ca2+-activated pathway and lead to an increase in PGC1-α expression by phosphorylation and activation of ATF-2 by p38 MAPK signaling pathway [49].
Also, exercise can upregulate several metabolic genes via hypoxia through HIF-1α-dependent mechanism (hypoxia-induced factor 1α). Other studies have shown an increase in both MCT4 protein and mRNA expression in response to hypoxia and demonstrated that the promoter is activated by hypoxia [45].This contraction/exercise-induced upregulation of MCT4 appears to be attributable to increase HIF-1α that binds the identified HRE sites on MCT4 promoter and stimulates MCT4 promoter activity [45].
As it has been reported that mitochondrial membrane has MCT1 [11, 15, 22, 46] which can highly be correlated to the mitochondrial oxidative function [8, 10], we separated an MI and a SL fraction from whole muscle homogenate by using differential centrifugation as previously described by Brooks et al. [10]. Cross contamination of the membrane fractions was controlled using negative control markers. COX was used as a marker of the mitochondrial membrane and GLUT-1 as marker of the SL fraction. The high COX content in the MI fraction along with the absence of any GLUT-1 confirmed the mitochondrial origin of the MI fraction. Despite the dramatic effect of diabetes on sarcholemmal MCT1, mitochondrial MCT1 was not affected by diabetes because no significant difference was found between the DC and C groups. This result again suggests that MCTs expression is regulated by different mechanisms. Both the mitochondrial and sarcholemmal MCT1 increased in response to endurance training, but the responses were different and increase of the mitochondrial MCT1 was higher in comparison to sarcholemmal. These exercise-induced changes can lead to an increase lactate gradient from cytosolic to mitochondria and promote lactate oxidation as a consequence that partially explain the decrease of muscle lactate concentration after adaptation to exercise. The sensitivity and different response of mitochondrial MCT1 to endurance training can confirm its role in cell–cell lactate shuttle.
Surprisingly, the response of the mitochondrial MCT1 was tissue specific. In cardiac muscle, the amount of increase in MCT1 expression on both mitochondrial and sarcholemmal membranes were almost alike whereas different in skeletal muscle. The properties of tissue can partially modulate the expression of mitochondrial MCT1. On the basis of the high oxidative capacity of cardiac tissue, this is a net lactate consumer whereas skeletal muscle can simultaneously produce, consume, and oxidize lactate that has been explained by the lactate shuttle mechanism [9]. Lactate production in one cell compartment and its removal in another can change cell redox that increases transcription of some genes through redox-dependent transcription regulation [27]. As mitochondria has a capacity of direct lactate oxidation [9] and this organelle do not produce this substrate, the oxidation of lactate in mitochondria can lead to less change in redox state in comparison to skeletal muscle where the production of lactate from pyruvate can occur. These findings all together can help us in introducing the intracellular lactate kinetic hypothesis in which the extent of lactate kinetic in each tissue can cause the specific changes in a positive manner. However, more well-designed studies focusing exactly on lactate kinetic in metabolically heterogeneous tissues are needed to confirm this hypothesis.
CD147 and MCTs belonged to a class of heteromeric membrane proteins being assembled in the endoplasmic reticulum prior to further transportation to the membrane via the Golgi complex. CD147 is an ancillary protein required for the expression of MCTs and the interaction between CD147 and MCT1 or MCT4 may be required for their translocation and correct localization to plasma membrane [40]. In addition, MCT1 and MCT4 have been demonstrated to be required for glycosylation and cell surface expression of CD147. For the first time, in the current study, it has been shown that diabetes decreases the CD147 expression in cardiac and skeletal muscles. This can partially explain the reduction in MCT1 and MCT4 expressions seen in type 2 diabetes. Surprisingly, the effect of diabetes and training-induced effects were more predominant in the oxidative tissue in comparison to glycolytic fibers which is possibly due to their high oxidative capacity. It is likely that suppression of mitochondria biogenesis be related to the decrease in CD147 expression; however, more studies are needed to clear it.
In summary, our results showed that MCT1 and MCT4 expressions have a dramatic reduction in type 2 diabetes, and endurance training can alleviate this reduction to normal levels via transcriptional and translational modifications. In addition, the decrease in CD147 expression that has occurred in type 2 diabetes can partially explain the reduction in MCT1 and MCT4 expressions.
References
Andrew PH, Nigel TP (1999) The proton-linked monocarboxylate transporter (MCT) family: structure, function and regulation. Biochem J 343:281–299
Becker-immermann K, Berger M, Berchtold P, Gries FA, Herberg L, Schewenen M (1982) Treadmill training improves intravenous glucose tolerance and insulin sensitivity in fatty Zuckerrats. Diabetologia 22:468–474
Benton CR, Yoshida Y, Lally J, Han XX, Hatta H, Bonen A (2008) PGC-1α increases skeletal muscle lactate uptake by increasing the expression of MCT1 but not MCT2 or MCT4. Physiol Genomics 35:45–54
Bloomgarden MD (2005) Concepts of Insulin Resistance. Metab Syndr Relat Disord 3:284–293
Bonen A (2001) The expression of lactate transporters (MCT1 and MCT4) in heart and muscle. Eur J Appl Physiol 86:6–11
Bonen A, Mio T, Dragana M, Catherine H, John JH, Andrew P (2000) Isoform-specific regulation of the lactate transporters MCT1 and MCT4 by contractile activity. Am J Physiol Endocrinol Metab 279:E1131–E1138
Brooks GA (2009) Cell-cell and intracellular lactate shuttles. J Physiol 23:5591–5600
Brooks GA, Dubouchaud H, Brown M, Sicurello JP, Butz CE (1999) Role of mitochondrial lactate dehydrogenase and lactate oxidation in the intracellular lactate shuttle. J Physiol 96:1129–1134
Brooks GA, Brown MA, Butz CE, Sicurello JP, Dubouchaud H (1999) Cardiac and skeletal muscle mitochondria have a monocarboxylate transporter MCT1. J Appl Physiol 87(5):1713–1718
Butz CE, McClelland GB, Brooks GA (2004) MCT1 confirmed in rat striated muscle mitochondria. J Appl Physiol 97:1059–1066
Choi CS, Kim YB, LeeFN ZJM, Kahn BB, Youn JH (2002) Lactate induces insulin resistance in skeletal muscle by suppressing glycolysis and impairing insulin signaling. Am J Physiol Endocrinol Metab 283:E233–E240
Defronzo RA, Simonson D, Ferrannini E (1982) Hepatic and peripheral insulin resistance: a common feature of type 2 (non-insulin dependent) and type 1 (insulin dependent) diabetes mellitus. Diabetologia 23:313–319
Deora AA, Philp N, Hu J, Bok D, Rodriguez-Boulan E (2005) Mechanisms regulating tissue-specific polarity of monocarboxylate transporters and their chaperone CD147 in kidney and retinal epithelia. PNAS 45:16245–16250
DiGirolamo M, Newby FD, Lovejoy J (1992) Lactate production in adipose tissue: a regulated function with extraadipose implications. FASEB J 6:2405–2412
Dubouchaud H, Butterfield GE, Wolfel EE, Bergman BC, Brooks GA (2000) Endurance training, expression and physiology of LDH, MCT1 and MCT4 in skeletal muscle. Am J Physiol Endocrinol Metab 278:E571–E579
Dubouchaud H, Granier P, Mercier J, Le Peuch C, Prefaut C (1996) Lactate uptake by skeletal muscle sarcolemmal vesicles decreases after 4 wk of hindlimb unweighting in rats. J Appl Physiol 80:416–421
Enoki T, Yoshida Y, Hatta H, Bonen A (2003) Exercise training alleviates MCT1 and MCT4 reductions in heart and skeletal muscles of STZ induced diabetic rats. J Appl Physiol 94:2433–2438
Enoki T, Yoshida Y, Lally J, Hatta H, Bonen A (2006) Testosterone increases lactate transport, monocarboxylate transporter MCT1 and MCT4 in rat skeletal muscle. J Physiol 1:433–443
Frøsig C, Rose AJ, Treebak JT, Kiens B, Richter EA, Wojtaszewski JF (2007) Effects of endurance exercise training on insulin signaling in human skeletal muscle: interactions at the level of PI3-K, Akt and AS160. Diabetes 56:2093–2102
Goodyear LJ, Hirshman MF, Knutson SM, Horton ED, Horton ES (1974) Effect of exercise training on glucose homeostasis in normal and insulin-deficient diabetic rats. J Appl Physiol 65:844–851
Gutmann L, Wahlefeld AW (1974) l-lactate determination with lactate dehydrogenase and NAD. Meth Enzym Anal 1464–1472
Hashimoto T, Hussien R, Cho HS, Kaufer D, Brooks GA (2008) Evidence for the mitochondrial lactate oxidation complex in rat neurons: demonstration of an essential component of brain lactate shuttles. PLoS One 3(8):e2915
Kelley KM, Hamann JJ, Navarre C, Gladden LB (2002) Lactate metabolism in resting and contracting canine skeletal muscle with elevated lactate concentration. J Appl Physiol 93:865–872
Kirk P, Wilson MC, Heddle C, Brown MH, Barclay AN, Halestrap AP (2000) CD147 is tightly associated with lactate transporters MCT1 and MCT4 and facilitates their cell surface expression. EMBO J 19(15):3896–904
Kraniou GN, Cameron-Smith D, Hargreaves M (2006) Acute exercise and GLUT4 expression in human skeletal muscle: influence of exercise intensity. J Appl Physiol 101:934–937
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2−Delta Delta C(T). Method 25:402–408
Liu H, Colavitti R, Rovira II, Finkel T (2005) Redox-dependent transcriptional regulation. Circ Res 97:967–974
Lombardi AM, Fabris R, Bassetto F, SerrR LA, Federspil G, Girard J, Vettor R (1999) Hyperlactatemia reduces muscle glucose uptake and GLUT-4 mRNA while increasing (E1a)PDH gene expression in rat. Am J Physiol Endocrinol Metab 39:E922–E929
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
McCullagh KJ, Bonen A (1995) Reduced lactate transport in denervated rat skeletal muscle. Am J Physiol Regul Integr Comp Physiol 268:R884–R888
Metz L, Sirvent P, Py G, Brun JF, Fédou C, Raynaud E, Mercier J (2005) Relationship between blood lactate concentration and substrate utilization during exercise in type 2 diabetic postmenopausal women metabolism. Clin Exp 54:1102–1107
Miyamoto S, Chiorini JA, Urcelay E, Safer B (1996) Regulation of gene expression for translation initiation factor eIF-2 alpha: importance of the 3′ untranslatedregion. Biochem J 315:791–798
Mondon CE, Jones IR, Azhar S, Hollenbeck CB, Reaven GM (1992) Lactate production and pyruvate dehydrogenase activity in fat and skeletal muscle from diabetic rats. Diabetes 41:1547–1554
O’Gorman DJ, Karlsson HK, McQuaid S, Yousif O, Rahman Y, Gasparro D, Glund S, Chibalin AV, Zierath JR, Nolan JJ (2006) Exercise training increases insulin-stimulated glucose disposal and GLUT4 (SLC2A4) protein content in patients with type 2 diabetes. Diabetologia 49:2983–2992
Pérez de Heredia F, Wood IS, Trayhurn P (2010) Hypoxia stimulates lactate release and modulates monocarboxylate transporter (MCT1, MCT2, and MCT4) expression in human adipocytes. Pflugers Arch-Eur J Physiol 459:509–518
Philp NJ, Ochrietor JD, Rudoy C, Muramatsu T, Linser PJ (2003) Loss of MCT1, MCT3, and MCT4 expression in the retinal pigment epithelium and neural retina of the 5A11/basigin-null mouse. Invest Ophthalmol Vis Sci 44:1305–1311
Randle PJ, Garland PB, Hales CN, Newsholme EA (1963) The glucose fatty-acid cycle. Its role in insulin sensitivity and the metabolic disturbances of diabetes mellitus. Lancet 1:785–789
Reed MJ, Meszaros K, Entes LJ, Claypool MD, Pinkett JG, Gadbois TM, Reaven GM (2000) A new rat model of type 2 diabetes: the fat-fed, streptozotocin-treated rat. Metabolism 49:1390–1394
Russell AP, Feilchenfeldt J, Schreiber S, Praz M, Crettenand A, Gobelet C, Meier CA, Bell DR, Kralli A, Giacobino JP, Deriaz O (2003) Endurance training in humans leads to fiber type-specific increases in levels of peroxisome proliferator-activated receptor-gamma coactivator-1 and peroxisome proliferator-activated receptor-alpha in skeletal muscle. Diabetes 52:2874–2881
Schneiderhan W, Scheler M, Holzmann KH, Marx M, Gschwend JE, Bucholz M, Gress TM, Seufferlein T, Adler G, Oswald F (2009) CD147 silencing inhibits lactate transport and reduces malignant potential of pancreatic cancer cells in in vivo and in vitro models. Gut 58:1391–1398
Schwoch C, Pasoow H (1984) preparation and properties of human erythrocyte ghosts. Mol Cell Biochem 152(2):197–218
Sharma AK, Srinivasan BP (2009) Triple verses glimepiride plus metformin therapy on cardiovascular risk biomarkers and diabetic cardiomyopathy in insulin resistance type 2 diabetes mellitus rats. Eur J Pharm Sci 38:433–444
Srinivasan K, Viswanad B, Asrat L, Kaul CL, Ramarao P (2005) Combination of high-fat diet-fed and low-dose streptozotocin-treated rat: a model for type 2 diabetes and pharmacological screening Srinivasan. Pharmacol Res 52:313–320
Terada S, Tabata I (2004) Effects of acute bouts of running and swimming exercise on PGC-1alpha protein expression in rat epitrochlearis and soleus muscle. Am J Physiol Endocrinol Metab 286:E208–E216
Ullah MS, Davies AJ, Halestrap AP (2006) The plasma membrane lactate transporter MCT4, but not MCT1, is up-regulated by hypoxia through a HIF-1-dependent mechanism. J Biol Chem 281:9030–9037
Valenti D, de Bari L, Atlante A, Passarella S (2002) l-lactate transport into rat heart mitochondria and reconstruction of the l-lactate/pyruvate shuttle. Biochem J 364:101–104
Vettor R, Lombardi AM, Fabris R, Pagano C, Cusin I, Rohner JF, Federspil G, Jeanrenaud B (1997) Lactate Infusion in anesthetized rats produces insulin resistance in heart and skeletal muscles. Metabolism 46:684–690
Wincey C, Marks V (1961) A micro-method for measuring glucose using the autoanalyzer and glucose-oxidase. J Clin Pathol 14:558–559
Wright DC, Geiger PC, Han DH, Jones TE, Holloszy JO (2007) Calcium induces increases in peroxisome proliferator-activated receptor gamma coactivator-1alpha and mitochondrial biogenesis by a pathway leading to p38 mitogen activated protein kinase activation. J Biol Chem 82:18793–18799
Zhang F, Ye C, Li G, Ding W, Zhou W, Zhu H, Chen G, Luo T, Guang M, Liu Y, Zhang D, Zheng S, Yang J, Gu Y, Xie X, Luo M (2003) The rat model of type 2 diabetic mellitus and its glycometabolism character. Exp Anim 52(5):401–407
Acknowledgments
This study was supported by a Centre grant from the Endocrinology and Metabolism Research Center of Tehran University of Medical Sciences. We also acknowledge all our collaborators.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nikooie, R., Rajabi, H., Gharakhanlu, R. et al. Exercise-induced changes of MCT1 in cardiac and skeletal muscles of diabetic rats induced by high-fat diet and STZ. J Physiol Biochem 69, 865–877 (2013). https://doi.org/10.1007/s13105-013-0263-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-013-0263-6