Abstract
Combination treatment may target different pathophysiological events following cerebral ischemia thus enhancing the efficacy of treatment in thromboembolic stroke. Taurine confers a neuroprotective effect in the mechanical stroke model. This effect has not been assessed in an embolic stroke model. Here, we sought to evaluate the neuroprotective effect of taurine alone and in combination with thrombolytic therapy to investigate whether combined administration would extend the therapeutic time window without increasing the hemorrhagic transformation in a rat embolic stroke model. Rats were subjected to right embolic middle cerebral artery occlusion and then randomly assigned to the following groups: saline treatment alone at 4 h, urokinase, taurine treatment alone at 4, 6, or 8 h, and the combination of taurine and urokinase at 4, 6, or 8 h after the insult. Brain infarct volume, neurobehavioral outcome, regional cerebral blood flow, intracranial hemorrhage incidence were observed and evaluated. Posttreatment with taurine at 4 or 6 h, urokinase at 4 h or in combination at 4, 6, or 8 h significantly reduced infarct volume and improved neurobehavioral outcome. The combination treatment had better neurobehavioral outcome and smaller infarction volume than urokinase or taurine treatment alone. The clinical outcome correlated well with infarct volume. Together, the present study suggests that administration of taurine after stroke is neuroprotective, seemingly because it reduces the reperfusion damage of urokinase, leading to widen the therapeutic window for the thrombolytic effect of urokinase to 8 h. Thrombolysis can also enhance the neuroprotective effect of taurine. The reduction of inflammatory response, neuron death and inhibition of blood brain barrier (BBB) disruption may underlie the beneficial effects of combination of taurine and urokinase in the treatment of embolic stroke.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
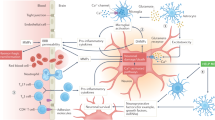
There are two major strategies currently being evaluated for ischemic stroke. One is to restore cerebral blood flow through the use of thrombolysis. The other is to minimize postischemic reperfusion injury and salvage ischemic brain tissue through the use of neuroprotective agents. Intravenous thrombolysis with tissue-type plasminogen activator (IV rt-PA) can be beneficial to some patients when given within 4.5 h of stroke onset [1]. But IV rt-PA has limitations in both efficacy and application for some patients. Accumulating evidence shows that IV therapy is less effective in the patients with carotid territory or vertebrobasilar artery occlusion [2–4]. In addition, the use of IV rt-PA is limited by low recanalization rates which have been shown to be associated with poorer outcome [5]. Recanalization rates are especially low with IV rt-PA in patients with proximal, large-vessel occlusions [6–9]. Compared with IV rt-PA, intra-arterial (IA) thrombolysis has the advantage of being site specific, which doubles the chances of recanalization and will likely improve the patient outcome [10]. Prolyse in acute cerebral thromboembolism I and II reported that local and IA thrombolytic therapy with pro-urokinase could improve the outcome for ischemic stroke patients if used within 6 h of symptom onset [11, 12]. However, increased risk of intracranial hemorrhage and narrow time window limit the use of the thrombolysis. Compared with thrombolysis, neuroprotective agents and strategies have been studied for years and appear to be effective in a variety of preclinical stroke models (Figs. 1 and 2). So far none of the drugs have proven conclusively to be effective in humans. One of the main reasons of failure in clinical trials may be that the drugs could not efficaciously access the ischemic target tissue because of the ischemic low reperfusion.
Evaluation of stroke model. a Regional cerebral blood flow measured using LDF in the ipsilateral parietal cortex prior to and 2 h after embolization (n = 7). b a Latex perfusion. b Evans blue staining. c Prepared Chinese ink perfusion. d TTC staining. e Coronal sections of Evans blue staining. f Coronal section of black ink perfusion
In order to achieve the greatest chance of success, new neuroprotective strategies need to be explored. Combination treatment with thrombolysis and neuroprotective agents directs at both the vascular and cellular mechanisms of ischemic brain injury that are likely to have the greatest impact upon stroke disability. Animal studies have already confirmed that combination treatment can act synergistically to extend the time window for thrombolysis and increase the efficacy of neuroprotectant agents [13] and may serve as a future strategy for stroke therapy in humans.
Our previous studies have already proven that exogenous administration of taurine can significantly decrease the infarct volume and improve the neurological outcome in the mechanical stroke model of rat [14]. In the present study, we test the hypothesis that intravenous administration of taurine in combination with intra-arterial administration of urokinase enhances efficacy of thrombolysis and neuroprotection, in addition, extends the therapeutic window of stroke in a rat model of embolic stroke.
Material and Methods
All experimental procedures were approved by the Ethics Committee for Experimental Animals of Beijing Neurosurgical Institute that is in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals. The experiments were designed to use the smallest number of animals and to minimize their suffering.
Animal Model
Male Sprague–Dawley rats (Military institute of medical science, China) weighing 280–350 g were subjected to embolic middle cerebral artery occlusion (MCAO) [15]. Briefly, single-intact, fibrin-rich, 24-h-old, 5-cm-long homologous clot was positioned at the origin of the middle cerebral artery (MCA) via a 15-mm length of modified PE-50 catheter. Continous laser Doppler flowmetry (LDF; USA) was used to monitor regional cerebral blood flow (rCBF) in order to ensure adequacy of embolic occlusion. For placement of the LDF probe, a burr hole 2–3 mm in diameter was created in the right parietal bone (2 mm posterior and 5 mm lateral to bregma) [16]. LDF values of rCBF were recorded at various time points beginning 10 min prior to clot injection and ending 20 min after thrombolysis. LDF measurement were used to ensure that rCBF in all rats were reduced to <30% of pre-ischemic baseline after clot injection. Rats were anesthetized with chloral hydrate (400 mg/kg IP) and allowed to breathe spontaneously. Rectal temperature was maintained at 37 ± 0.5°C throughout the surgical procedure using a feedback-regulated heating system.
Evaluation of Embolic Stroke Model
We also further evaluated reproducibility and consistency of the model from the following aspects: (1) To visualize artery perfusion territory which the embolus blocked, one rat was perfused with prepared Chinese black ink through the left ventricle immediately after clot injection. (2) To visualize the final lodgment of the embolus within the cerebral vasculature, one rat was perfused with heparin saline followed by injection with blue latex through the left ventricle immediately after clot injection. (3) Evans blue was used as BBB permeability marker to reveal the BBB disruption territory where evans blue dye leaks from cerebral vasculature into brain parenchyma. One rat was injected with 3% evans (2 ml/kg, IV) at 3 h after clot injection, let it equilibrium for 3 h, then perfused with heparin saline to show the staining territory. (4) 2,3,5-triphenyltetrazolium chloride (TTC; Sigma) staining to visualize the brain tissue necrosis territory.
Treatment Protocols
Taurine (Shanghai Chemical Reagents Company, dissolved in sterile 0.9% saline) was intravenously infused at a dose of 50 mg−1 kg−1 ml−1 (high dose) or 2.5 mg−1 kg−1 ml−1 (low dose) on the basis of previous research [14]. Urokinase (Shanghai Biochemical Reagents Company, dissolved in sterile 0.9% saline) was infused into the internal carotid artery at a dose of 5,000 U/kg over 5 min through the catheter used for clot administration. Dose of urokinase was used on the basis of previously published studies on rats [17, 18]. After embolization, animals were randomly divided into the following groups:(1)To examine the effect of taurine alone on ischemia, high-dose taurine was administered to ischemic rats at 4 or 6 h after MCAO, low-dose taurine was administered to ischemic rats at 6 or 8 h after MCAO; (2) to examine the effect of urokinase alone on ischemia, urokinase was administered to ischemic rats at 4, 6, or 8 h after MCAO; (3) to examine the effect of combination therapy of urokinase and taurine on ischemia, high-dose taurine and urokinase were administered at 4 or 6 h after MCAO, low-dose taurine and urokinase were administered at 6 or 8 h after MCAO. The control group consisted of ischemic rats administered the same volume of 0.9% of saline at 4 h after MCAO (Fig. 1).
Neurological Deficit Evaluation
Neurological deficits were examined at 3 and 24 h, respectively, after MCAO. A five-point neurological score was used [19]: 0, no observable deficit; 1, forelimb flexion; 2, forelimb flexion and decreased resistance to lateral push; 3, forelimb flexion, decreased resistance to lateral push, and unilateral circling in three successive trials; 4, signs of grades 3 plus a decrease in consciousness.
Measurement of Infarct Volume, Hemorrhage
Twenty-four hours after MCAO, infarct volume was measured on six TTC-stained coronal sections, as described previously [20]. Gross hemorrhage, defined as blood evident on the coronal sections, was evaluated on six coronal sections for each animal at 24 h after MCAO. Evidence of gross hemorrhage on any section was considered to show the presence of hemorrhage in that animal.
Standard Zymography
Twenty-four hours after embolic ischemia, metalloproteinase extraction from brain was performed according to a previously described method [21]. Zymographies were performed using a published method [22] with minor modification. Elevations in matrix metalloproteinases (MMPs) were expressed as the ratio of the ischemic and the nonischemic hemispheric integrated density values, both corrected for protein.
Histological Evaluation
Five-micrometer-thick paraffin-embedded coronal sections from the center of the ischemic lesion at the level of the anterior commissure were glass mounted for histological staining. To evaluate the inflammatory cells within the brain, a polyclonal antibody against human myeloperoxidase (MPO; 1:200 dilution; DAKO Carpineria, CA, USA) was used [19, 23]. Only morphologically intact MPO-immunoreactive cells were included in the counts. To measure the number of apoptotic cells, terminal deoxynucleotidyl transferase-mediated dUTP nick end labeling (TUNEL) was performed using the Apoptosis Detection Kit (ApopTag; Chemicon International, CA, USA) according to the manufacturer’s protocol. The number of MPO-positive or TUNEL-positive cells were counted in ten randomly chosen fields (×400) of the penumbra of the cortex or striatum. Five microscopic fields per penumbra region per section were analyzed. Data are presented as the average of the number obtained from striatum and cortex penumbras.
Data Expression and Statistical Analysis
All data in this study were presented as mean ± standard error (SEM). We first evaluated normality of each measure of interest. Nonparametric Kruskal–Wallis test would be considered if the data were ill behaved. One-way ANOVA followed by Fisher’s least significant difference multiple comparison test was used to compare the difference of ordinal data between groups. Fisher’s exact test was used to compare the difference of intracranial hemorrhagic complications among the groups. Spearman’s rank-order correlation test was used for ranked pairs. Values of P < 0.05 were considered as significant.
Results
Embolic Stroke Model
After clot injection, rCBF immediately dropped to <25% of pre-ischemic baselines and was sustained at least for 2 h after clot injection. Latex perfusion visualized the final lodgment of the embolus located in the origin of the MCA, part of the clot extended into the MCA main trunk. Black ink perfusion showed the clot completely stop the blood flow to the MCA territory and Evans blue staining showed obvious BBB disruption in the MCA perfusion territory. TTC staining showed the tissue necrosis located in the MCA perfusion territory (Fig. 2).
Infarct Volume
Animals receiving treatment with high-dose taurine at 4 or 6 h after ischemia significantly (P < 0.01) reduced infarct volume compared with the control group. Likewise animals treated with urokinase at 4 or 6 h but not at 8 h after ischemia significantly (P < 0.01) reduced infarct volume compared with the control group. Rats treated with taurine and urokinase at 4, 6, or 8 h had infarct volume significantly lower than that of the control 24 h after MCAO (P < 0.01). Addition of high-dose taurine to urokinase at 6 h after ischemia further reduced infarct volume compared with urokinase-treatment-alone group (P < 0.05). Addition of low-dose taurine to urokinase at 8 h after ischemia further augmented the effect of taurine in reduction of the neuron damage (P < 0.05), which achieved better neuroprotection than any single-drug-treated groups (P < 0.05) (Fig. 3).
Effects of taurine treatment alone and in combination treatment with urokinase on infarct volume assessed in each group 24 h after MCAO. UK urokinase, H-Tau high-dose taurine (50 mg/kg/ml), L-Tau low-dose taurine(2.5 mg/kg/ml). a Four-hour high-dose taurine combination treatment groups. b Six-hour high-dose taurine combination treatment groups. c Six-hour low-dose taurine combination treatment groups. d Eight-hour low-dose taurine combination treatment groups. e Urokinase-treatment-alone groups. f Photographs showing representative brain lesion after TTC Staining of coronal brain slices from different groups. Values are mean ± SEM. *P < 0.05; **P < 0.01 vs control group; #P < 0.05; ##P < 0.01 vs. combination treatment group (n = 11)
Neurological Assessment
Three hours after MCAO, there was no significant difference among the groups. Treatment with high-dose taurine at 4 or 6 h after MCAO significantly (P < 0.01) improved neurobehavioral outcome 24 h after ischemia compared with control animals. Likewise, animals treated with urokinase at 4 h after MCAO exhibited a significant (P < 0.01) reduction in neurobehavioral scores from the control group 24 h after ischemia. Rats treated with taurine and urokinase at 4, 6, or 8 h had neurobehavioral outcome significantly higher than that of the control 24 h after MCAO (P < 0.01). Furthermore, high-dose combination treatment at 6 h after the insult had the better neurobehavioral outcome than 6-h urokinase treatment alone (P < 0.05), or low-dose combination treatment at 8 h after the insult had the better neurobehavioral outcome than 8-h urokinase treatment alone (P < 0.05) (Fig. 4).
Effects of taurine treatment alone and in combination treatment with urokinase on neurobehavioral scores assessed in each group after 3 or 24 h after MCAO. UK urokinase, H-Tau high-dose taurine (50 mg/kg/ml), L-Tau low-dose taurine (2.5 mg/kg/ml). a Four-hour high-dose taurine combination treatment groups. b Six-hour high-dose taurine combination treatment groups. c Six-hour low-dose taurine combination treatment groups. d Eight-hour low-dose taurine combination treatment groups. e Urokinase-treatment-alone groups. Values are mean ± SEM.*P < 0.05; **P < 0.01 vs control group; #P < 0.05; ##P < 0.01 vs combinaion treatment group (n = 11)
Cerebral Hemorrhage
Treatment with taurine alone or combined with urokinase did not significantly increase the incidence of hemorrhage in the 24 h after MCAO compared with the control group (P > 0.05) (Table 1).
Correlations between Clinical Outcome and Neuropathologic Damage
The total infarct volume for the animals surviving 24 h was highly correlated with the neurologic scores on day 1 (n = 98; r = 0.353; P < 0.01; Spearman’s), the rCBF on day 1(n = 98, r = −0.302; P < 0.01; Spearman’s). In other words, animals with smaller infarcts fared better functionally and higher regional cerebral blood flow.
MMP Standard Zymography
Zymograms revealed only inactive pro-form of MMP-2 (72 kDa) and MMP-9 (dimmer 210 kDa, pro-form 92 kDa, and cleaved-form 88 kDa). Compared with control animals, the hemispheric cleaved-MMP-9 ratio after treatment with taurine (high dose), urokinase alone or in combination was not increased (P > 0.05). However, treatment with urokinase alone at 6 h after MCAO significantly increased the MMP-2 ratio compared with the control group (P < 0.05), and the MMP-2 ratio in the combination treatment was also significantly lower than that of the urokinase treatment alone (P < 0.01). Treatment with taurine alone and in combination with urokinase at 4 h after MCAO significantly decreased the pro-MMP-9 ratio (P < 0.05) compared with the control group. In addition, the pro-MMP-9 ratio in combination treatment was also significantly lower than that of urokinase treatment alone (P < 0.01). Treatment with urokinase alone at 6 h after MCAO significantly increased the pro-MMP-9 and dimmer-MMP-9 ratio compared with the control group (P < 0.05), treatment with urokinase alone at 4 h after MCAO only increased the dimmer-MMP-9 ratio compared with the control group (P < 0.05) (Fig. 5).
Representive gelatin zymogram showing the effects of urokinase or taurine alone and in combination treatment on MMP-9 and MMP-2 assessed in each group after 24 h after MCAO. Mw indicates molecular weight standards; std indicates zymography standards. MMP indicates matrix metalloproteinase. a Ischemic brain tissue a control group; b, e UK 4- and 6-h treatment group; c, f H-Tau 4- and 6-h treatment group; d, g UK + H-Tau 4- and 6-h treatment group. b Nonischemic brain tissue. a’ Control group; b’, e’ UK 4- and 6-h treatment group; c’, f’ H-Tau 4- and 6-h treatment group; and d’, g’ UK + H-Tau-4- and 6-h treatment group. Protein marker and the corresponding molecular weights (kDa) are shown on the left. c, d Standard densitometry technique was used to quantify these changes as fold increase versus nonischemic baselines (mean ± SEM) *P < 0.05 vs control group, ##P < 0.01 vs combination treatment group (n = 9)
Myeloperoxidase-Immunoreactive Cells
Treatment with taurine (high dose) alone at 4 h after ischemia and in combination with urokinase at 4 or 6 h after ischemia significantly reduced the number of the MPO-immunoreactive-positive cells compared with the control group (P < 0.05 or P < 0.01), treatment with urokinase alone at 6 h after ischemia significantly increased the number of the MPO-immunoreactive-positive cells compared with the control group (P < 0.01). In addition, the number of MPO-immunoreactive-positive cells of combination treatment group at 4 and 6 h after MCAO was significantly lower than that of urokinase alone treatment group (P < 0.01) (Fig. 6).
Myeloperoxidase-immunoreactive cells. a The position of MCA, slices being analyzed and distribution of neuronal damage in coronal slices at 24 h after MCAO in the rat brain are schematically indicated over the picture of the rat brain. I ischemic hemisphere, N nonischemic hemisphere, AC anterior commissure. 1, 2 Ischemic core. 3, 4 Ischemic penumbra. b Photomicrographs show myeloperoxidase-immunoreactive cells from a representative rat in the control (vehicle treatment) group (a), UK 4- and UK 6-h treatment group (b, c), H-Tau 4- and 6-h treatment group (d, e), UK + H-Tau 4- and 6-h treatment group (f, g), and sham group (h). c, d Quantitative analysis of myeloperoxidase-immunoreactive cells shows the effects of taurine treatment alone and in combination with urokinase on the density of myeloperoxidase (MPO)-immunoreactive cells. *P < 0.05; **P < 0.01 vs control group; ##P < 0.01 vs combination treatment group (n = 6). All images were taken at the same magnification of ×400
Terminal Deoxynucleotidyl Transferase-Mediated dUTP Nick End Labeling
Treatment with taurine alone at 4 h after MCAO and combination treatment with urokinase at 4 or 6 h after MCAO significantly reduced the number of TUNEL-positive cells in the ipsilateral hemisphere compared with the control group (P < 0.05) (Fig. 7).
Terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end labeling (TUNEL)-positive cells. a Photomicrographs show TUNEL-positive cells from a representative rat in the control (vehicle treatment) group (a), UK 4- and 6-h treatment group (b, c), H-Tau 4- and 6-h treatment group (d, e), UK + H-Tau 4- and 6-h treatment group (f, g), and sham group (h). b, c Quantitative analysis of TUNEL-positive cells shows the effects of taurine combination with urokinase on the density of TUNEL-positive cells. *P < 0.05; **P < 0.01 vs control group (n = 6). All images were taken at the same magnification of ×400
Discussion
In this animal model, a fibrin-rich clot reliably occluded the origin of MCA, stably decreased rCBF and produced a reproducible and consistent infarction volume. The stroke model was most closely resembling human embolic stroke and suitable for investigation of the synergistic effects of thrombolytic drugs with potential neuroprotective agent.
Taurine (2-aminoethanosulfonic acid) is an important inhibitory neurotransmitter that is available in abundance in the central nervous system. It plays an essential role in both brain development and regeneration, and it also promotes the survival and proliferation of neurons [24]. Taurine-containing neurons are fairly resistant to cerebral ischemia induced by the four-vessel occlusion [25, 26]. Taurine is also an endogenous neuroprotectant. The main mechanisms of taurine for its neuroprotection include osmoregulation, antiexcitotoxicity, membrane stabilization, neuromodulation and regulation of calcium homeostasis which provide a pharmacological basis of the treatment against ischemia/reperfusion damage.
It is one of our aims in this study to evaluate the neuroprotective effect of taurine treatment alone in a thromboembolic stroke model of rats. Our previous study revealed that taurine treatment at 1 h after ischemia improved neurological outcome and decreased infarct volume in a dose-dependent manner in the focal cerebral ischemic model prepared by the intra-luminal filament technique. Taurine at the dose of 5, 15, or 50 mg/kg had marked protection, and 50 mg/kg of taurine is most effective. However, taurine at the dose of 1 or 2.5 mg/kg only had tendency to reduce ischemic damage [14]. Thus, in the present study, the neuroprotective effect of taurine treatment alone at the dose of 50 mg/kg (optimal dose) or 2.5 mg/kg (suboptimal dose) was investigated in the focal embolic stroke model. Our results showed that intravenous administration of taurine at the dose of 50 mg/kg even at 6 h after ischemic injury had neuroprotective effect. However, administration of taurine at the dose of 2.5 mg/kg only exhibited a trend to attenuate ischemic damage in the focal embolic stroke model. These results were more consistent with our previous results, which provided further evidence to confirm the neurprotective effect of taurine against focal cerebral ischemia. In contrast to our data, it has been reported that intraperineal administration of taurine at the dose of 100 mg/kg at the onset of focal ischemia reveals a trend towards protection; however, it does not reach statistical significance [27]. The somewhat difference compared with our results might be due to the different doses to be used and the biphasic action of taurine [14, 28, 29]. Further studies are necessary to better understand the potential for taurine as a neuroprotective agent in cerebral ischemia.
However, the primary aim of the study was to evaluate the synergistic effect of taurine and urokinase. Our data demonstrated that combination treatment of taurine and urokinase, administered at 4, 6, and even 8 h after the onset of MCAO, reduced infarct volume and improved the neurological outcome without increasing the risk of hemorrhagic transformation in an embolic stroke model of rats. Furthermore, the effect of combination treatment was better than each monotherapy with urokinase or taurine. Single low dose of taurine (2.5 mg/kg) alone did not ameliorate the embolic infarction at 6 or 8 h after the onset, but it would salvage or “freeze” the penumbra, allowing a longer time window for administration of thrombolysis. Combination treatment was conducive to taurine entering into ischemic tissue and enhancing its protective effect as a consequence. Treatment with urokinase alone was effective in reducing infarct volume at 4, 6 h but not 8 h after ischemia, incidence of hemorrhagic transformation were increased along with delayed thrombolysis treatment. When perfusion was recovered after administration of urokinase, it made taurine more easily access to ischemic tissue, the entering taurine could attenuate inflammatory reaction, oxidative stress, disruption of brain blood barrier and apoptosis [14, 30–34], finally extended the therapeutic window until to 8 h after the onset, which would lead to an increased number of patients being eligible for thrombolytic therapy.
In order to clarify the mechanism of combination treatment of taurine and urokinase, the effect of the combination treatment on MMPs expression, the numbers of MPO and TUNEL immunoreactive positive cells in ischemic brain tissue were investigated.
MMPs are zinc-endopeptidases with multifactorial actions in central nervous system physiology and pathology. Accumulating data suggest that MMPs have a deleterious role in the acute phase of stroke. By degrading neurovascular matrix, MMP-9 promotes BBB disruption, edema formation, hemorrhagic transformation, inflammation. By disrupting cell-matrix signaling and microenvironment homeostasis, MMP-9 triggers neuron apoptosis/necrosis [35]. Reperfusion after focal stroke further leads to the release and activation of MMP-9 from neutrophils that are recruited to the postischemic brain, this neutrophil-derived MMP-9 exhibits self-amplifying proinflammatory effects that trigger further neutrophil-endothelial adherence, neutrophil plugging of capillaries, and diapedesis into brain parenchyma [36]. Taken together, MMP-9, inflammatory response and apoptosis interact with each other to enhance the brain damage. On the other hand, neutrophils play an important role in the development of ischemic/reperfusion injury and the increase in brain MPO activity after focal cerebral ischemia virtually reflects the neutrophil infiltration [37].Thus, estimation of MPO immunoreactivity is used as an effective maker to evaluate the degree of inflammation and ischemic/reperfusion injury.
In the present study, combination treatment with taurine and urokinase at 4 or 6 h after stroke onset significantly reduce the density of MPO-immunoreactive cells, TUNEL-positive cells and MMP activity without increasing hemorrhagic transformation and the inhibitory effects of combination treatment were superior to that of each treatment with taurine or urokinase alone, suggesting that the neuroprotective mechanism of combination treatment might be partially related to reduction of inflammatory response, inhibition of BBB disruption and neuronal apoptosis.
More investigators have recently reported that IA thrombolysis with urokinase is safe and efficacy for the treatment of stroke patients [38–41]. In addition, urokinase is more economical than rt-PA, which could significantly reduce medical costs for stroke patients and also means that more patients might benefit from thrombolysis therapy. Therefore, IA thrombolysis using urokinase may provide an alternative to IV thrombolysis with rt-PA in selected patients with acute ischemic stroke. In the current study, we found that the combination of taurine with IA urokinase markedly improved the neuroprotective effect and extended the therapeutic time window in experimental stroke, which represents a promising strategy for the treatment of stroke, especially for patients with large artery occlusion. Because of catheter techniques and skilled facilities, IA thrombolysis needs to be performed in experienced stroke centers. With more interventionist teams develop the required skilled for IA thrombolysis, more patients would benefit from this therapy approach.
Our study has several potential weaknesses. The occurrence of intracranial hemorrhage is a major concern after administration of thrombolytic therapy. In the present study, we only evaluated the incidence of visible hemorrhage. Although it is clinically relevant, quantitative analysis of brain hemorrhage volume might better reflect the severity of hemorrhagic transformation. Moreover, brain samples were collected at 24 h after stroke onset in this study, more samples collected at earlier time points after onset might better address the causality concern between infarction volume and biochemical analysis. Finally, only short term functional outcome were evaluated in this study. For the sake of future translational significance, long-term safety and efficacy of combination therapy on embolic stroke is to be evaluated in the future.
Conclusions
Our data demonstrates that treatment of embolic stroke with taurine alone at a dose of 50 mg/kg at even 6 h after ischemic onset exerts significantly neuroprotective effect, combination treatment of taurine and urokinase may yield additional benefit and extend the therapeutic window of thrombolysis to 8 h after stroke, suggesting that combination treatment with taurine and urokinase may provide a novel strategy for treatment of acute stroke and implies its translational significance. The reduction of inflammatory response, neuron apoptosis and attenuation of BBB disruption may underlie the beneficial effects of taurine and combination of taurine and urokinase in the treatment of embolic stroke.
References
Hacke W, Kaste M, Bluhmki E, Brozman M, Dávalos A, Guidetti D, et al. Thrombolysis with alteplase 3 to 4.5 h after acute ischemic stroke. N Engl J Med. 2008;359:1317–29.
Macleod MR, Davis SM, Mitchell PJ, Gerraty RP, Fitt G, Hankey GJ, et al. Results of a multicentre, randomised controlled trial of intra-arterial urokinase in the treatment of acute posterior circulation ischaemic stroke. Cerebrovasc Dis. 2005;20:12–7.
Agarwal P, Kumar S, Hariharan S, Eshkar N, Verro P, Cohen B, et al. Hyperdense middle cerebral artery sign: can it be used to select intra-arterial versus intravenous thrombolysis in acute ischemic stroke? Cerebrovasc Dis. 2004;17:182–90.
Qureshi AI, Ezzeddine MA, Nasar A, Suri MF, Kirmani JF, Janjua N, et al. Is IV tissue plasminogen activator beneficial in patients with hyperdense artery sign? Neurology. 2006;66(8):1171–4.
Labiche LA, Al-Senani F. WojnerAW, et al. Is the benefit of early recanalization sustained at 3 months? A prospective cohort study. Stroke. 2003;34:695–8.
Alexandrov AV, Molina CA, Grotta JC, et al. Ultrasound enhanced systemic thrombolysis for acute ischemic stroke. N Engl J Med. 2004;351:2170–8.
Brott TG, Haley Jr EC, Levy DE, et al. Urgent therapy for stroke. Part 1. Pilot study of tissue plasminogen activator administered within 90 minutes. Stroke. 1992;23:632–40.
Von Krummer R, Hacke W. Safety and efficacy of intravenous tissue plasminogen activator and heparin in acute middle cerebral artery stroke. Stroke. 1992;23:646–52.
Trouillas P, Nighoghossian N, Getenet JC, et al. Open trial of intravenous tissue plasminogen activator in acute carotid territory stroke: correlations of outcome with clinical and radiological data. Stroke. 1996;27:882–90.
Mattle HP. Intravenous or intra-arterial thrombolysis? It’s time to find the right approach for the right patient. Stroke. 2007;38:2038–40.
Del Zoppo GJ, Higashida RT, Furlan AJ, et al. PROACT: a phase II randomized trial of recombinant pro-urokinase by direct arterial delivery in acute middle cerebral artery stroke. Stroke. 1998;29:4–11.
Furlan A, Higashida R, Wechsler L, et al. Intra-arterial pro-urokinase for acute ischemic stroke: the PROACT II study: a randomized controlled trial. JAMA. 1999;282:2003–11.
Zhang L, Zhang ZG, Zhang CL, Zhang RL, Chopp M. Intravenous administration of a GPIIb/IIIa receptor antagonist extends the therapeutic window of intra-arterial tenecteplase-tissue plasminogen activator in a rat stroke model. Stroke. 2004;35:2890–095.
Sun M, Xu C. Neuroprotective mechanism of taurine due to up-regulating calpastatin and down-regulating calpain and caspase-3 during focal cerebral ischemia cellular and molecular neurobiology. Cell Mol Neurobiol. 2008;28:593–611.
Asahi M, Asahi K, Wang XY, Lo EH. Reduction of tissue plasminogen activator-induced hemorrhage and brain injury by free radical spin trapping after embolic focal cerebral ischemia in rats. J Cereb Blood Flow Metab. 2000;20:452–7.
Paxinos G, Watson C. The Rat Brain Stereotaxic Coordinates. 2nd ed. Orlando: Academic Press; 1986.
Shuaib A, Yang Y, Siddiqui M, Kalra J. Intraarterial urokinase produces significant attenuation of infarction volume in an embolic focal ischemia model. Exp Neurol. 1998;154:330–5.
Yang Y, Li Q, Shuaib A. Enhanced neuroprotection and reduced hemorrhagic incidence in focal cerebral ischemia of rat by low dose combination therapy of urokinase and topiramate. Neuropharmacology. 2000;39:881–8.
Bederson JB, Pitts LH, Tsuji M, Nishimura MC, Davis RL, Bartkowski H. Rat middle cerebral artery occlusion: evaluation of the model and development of a neurologic examination. Stroke. 1986;17:472–6.
Lin TN, He YY, Wu G, Khan M, Hsu CY. Effects of brain edema on infarct volume in a focal cerebral ischemia model in rats. Stroke. 1993;24:117–21.
Zhang JW, Gottschall PE. Zymographic measurement of gelatinase activity in brain tissue after detergent extraction and affinity-support purification. J Neurosci Methods. 1997;76:15–20.
Kleiner DE, Stetler-Stevenson WG. Quantitative zymography: detection of pictogram quantities of gelatinase. Anal Biochem. 1994;218:325–9.
Zhang ZG, Chopp M. Measurement of myeloperoxidase immunoreactive cells in ischemic brain after transient middle cerebral artery occlusion in the rat. Neurosci Res Comm. 1997;20:85–91.
Lima L, Obregon F, Cubillos S, Fazzino F, Jaimes I. Taurine as a micronutrient in development and regeneration of the central nervous system. Nutr Neurosci. 2001;4:439–43.
Matsumoto K, Ueda S, Hashimoto T, Kuriyama K. Ischemic neuronal injury in the rat hippocampus following transient forebrain ischemia: evaluation using in vivo microdialysis. Brain Res. 1991;543:236–42.
Wu JY, Lin CT, Johanssen FF, Liu JW. Taurine neurons in rat hippocampal formation are relatively inert to cerebral ischemia. Adv Exp Med Biol. 1994;359:289–98.
Shuaib A. The role of taurine in cerebral ischemia: studies in transient forebrain ischemia and embolic focal ischemia in rodents. Adv Exp Med Biol. 2003;526:421–31.
Sanberg PR, Willow M. Dose-dependent effects of taurine on convulsions induced by hypoxia in the rat. Neurosci Lett. 1980;16:297–300.
Schurr A, Tseng MT, West CA, Rigor BM. Taurine improves the recovery of neuronal function following cerebral hypoxia: an in vitro study. Life Sci. 1987;40:2059–66.
Schuller-Levis GB, Park E. Taurine and its chloramine: modulators of immunity. Neurochem Res. 2004;29:117–26.
Guz G, Oz E, Lortlar N, Ulusu NN, Demirogullari B, Omeroglu S, et al. The effect of taurine on renal ischemia/reperfusion injury. Amino Acids. 2007;32:405–11.
Raschke P, Massoudy P, Becker BF. Taurine protects the heart from neutrophil-induced reperfusion injury. Free Radic Biol Med. 1995;19:461–71.
Giriş M, Depboylu B, Doğru-Abbasoğlu S, Erbil Y, Olgaç V, Aliş H, et al. Effect of taurine on oxidative stress and apoptosis-related protein expression in trinitrobenzene sulphonic acid-induced colitis. Clin Exp Immunol. 2008;152:102–10.
Marcinkiewicz J, Kurnyta M, Biedroń R, Bobek M, Kontny E, Maśliński W. Anti-inflammatory effects of taurine derivatives (taurine chloramine, taurine bromamine, and taurolidine) are mediated by different mechanisms. Adv Exp Med Biol. 2006;583:481–92.
Zhao RZ, Wang S, Kim HY, Storrie H, Rosen BR, Mooney DJ, et al. Role of matrix metalloproteinases in delayed cortical responses after stroke. Nat Med. 2006;12:441–5.
Gidday JM, Gasche YG, Copin JC, Shah AR, Perez RS, Shapiro SD, et al. Leukocyte-derived matrix metalloproteinase-9 mediates blood-brain barrier breakdown and is proinflammatory after transient focal cerebral ischemia. Am J Physiol Heart Circ Physiol. 2005;289:H558–68.
Matsuo Y, Onodera H, Shiga Y, Nakamura M, Ninomiya M, Kihara T, et al. Correlation between myeloperoxidase-quantified neutrophil accumulation and ischemic brain injury in the rat. Effects of neutrophil depletion. Stroke. 1994;25:1469–75.
Ogawa A, Mori E, Minematsu K, Taki W, Takahashi A, Nemoto S, et al. Randomized trial of intraarterial infusion of urokinase within 6 hours of middle cerebral artery stroke: the middle cerebral artery embolism local fibrinolytic intervention trial (MELT) Japan. Stroke. 2007;38(10):2633–9.
Lee DH, Jo KD, Kim HG, Choi SJ, Jung SM, Ryu DS, et al. Local intraarterial urokinase thrombolysis of acute ischemic stroke with or without intravenous abciximab: a pilot study. J Vasc Interv Radiol. 2002;13(8):769–74.
Yu YY, Niu L, Gao L, Zhao ZW, Deng JP, Qu YZ, et al. Intraarterial thrombolysis and stent placement for acute basilar artery occlusion. J Vasc Interv Radiol. 2010;21(9):1359–63.
Arnold M, Fischer U, Schroth G, Nedeltchev K, Isenegger J, Remonda L, et al. Intra-arterial thrombolysis of acute iatrogenic intracranial arterial occlusion attributable to neuroendovascular procedures or coronary angiography. Stroke. 2008;39(5):1491–5.
Sources of funding
This work was supported by the Beijing Natural Science Foundation of China, NO: 7052018.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guan, W., Zhao, Y. & Xu, C. A Combined Treatment with Taurine and Intra-arterial Thrombolysis in an Embolic Model of Stroke in Rats: Increased Neuroprotective Efficacy and Extended Therapeutic Time Window. Transl. Stroke Res. 2, 80–91 (2011). https://doi.org/10.1007/s12975-010-0050-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-010-0050-4