Abstract
Objectives
Growing research indicates that self-compassion is associated with key physical health outcomes in non-clinical adult populations. This systematic review was designed to characterize the mediators linking self-compassion to physical health outcomes, evaluate study quality and theoretical evidence, compare findings to the mental health literature, and provide directions for future research.
Methods
We searched Embase, Medline, APA PsycInfo, Scopus, AMED, and Web of Science for relevant articles (including the inclusion of formal statistical mediation tests) from 2003 to February 2022. Study quality was assessed with Downs and Black Checklist for Measuring Quality and Mediation Quality Checklist tools.
Results
We screened 6439 articles for title and abstracts, assessed 101 full texts for eligibility, and included 20 relevant articles. A range of mediators were categorized as testing psychological or behavioral factors. Perceived stress (n = 5), emotion regulation (n = 5), negative affect (n = 3), and coping strategies (n = 3) were the most frequently assessed mediators. In general, self-compassion had a significant indirect effect on physical health via negative affect and perceived stress (in the absence of overlapping affective mediators). Findings for emotion regulation and coping strategies were mixed.
Conclusions
The mediational evidence linking self-compassion to physical health via psychological and behavioral factors remains underdeveloped and focused on the measures of affect and emotion regulation. Future studies need to broaden the scope of mediators to include other self-regulatory factors indicated by theory (e.g., motivational and physiological indices) and implement designs other than cross-sectional/correlational.
Protocol Registration
PROSPERO CRD42021241915.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
A growing body of evidence suggests that self-compassion is associated with better mental health and psychosocial well-being (e.g., Zessin et al., 2015). While there are multiple definitions and measures of self-compassion (Mascaro et al., 2020), for the purposes of this systematic review, self-compassion is defined as a way of responding to the self in times of suffering, characterized by self-kindness versus self-judgment, common humanity versus isolation, and mindfulness versus over-identification or avoidance (detailed descriptions of each component can be found in Neff, 2003). Meta-analyses have found that greater self-compassion was associated with greater overall and psychological well-being (Zessin et al., 2015) and lower mental health symptoms such as stress, anxiety, and depression (MacBeth & Gumley, 2012; Marsh et al., 2018). These findings were largely consistent with self-compassion interventional data (Ferrari et al., 2019; Kirby et al., 2017). Taken together, the evidence from cross-sectional and interventional studies suggests that the development of self-compassion has benefits for psychosocial and mental health outcomes.
Although less intensively researched, studies have indicated that self-compassion may predict key physical health outcomes and health behaviors (Phillips & Hine, 2019; Sirois et al., 2015). For example, self-compassion has been associated with health-promoting behaviors (Gedik, 2019; Li et al., 2020; Sirois, 2015) such as medical adherence (Sirois & Hirsch, 2019), seeking medical care (Terry et al., 2013), healthy eating (Adams & Leary, 2007; Schoenefeld & Webb, 2013), and exercise (Magnus et al., 2010). Other studies have linked self-compassion with key physical health indices, including good sleep quality (Brown et al., 2020), reports of fewer physical symptoms (i.e., fatigue, headaches, shortness of breath; Dunne et al., 2018; Hall et al., 2013; Terry et al., 2013), and lower physiological responses to stress (Arch et al., 2014; Breines et al., 2014).
However, despite increasing evidence for the benefits of self-compassion, the mechanisms behind it remain unclear. Both as a trait characteristic and in terms of how self-compassion is reflected in the content of interventions, self-compassion is a complicated, multi-component construct. One systematic review has suggested that emotion regulation strategies underpin the links between self-compassion and mental health (Inwood & Ferrari, 2018). Other studies of potential pathways in mental health have tested a range of possible psychosocial mediators, predominantly in cross-sectional, correlational designs. Mediators thought to link self-compassion to mental health and psychosocial outcomes include aspects of rumination and worry (Arimitsu & Hofmann, 2015; Fresnics & Borders, 2017; Hodgetts et al., 2020; Johnson & O'Brien, 2013; Raes, 2010; Tandler et al., 2020), emotion regulation (Chishima et al., 2018; Meyer & Leppma, 2019), coping (Hamrick & Owens, 2019; Li et al., 2021), perceived stress (Luo et al., 2019), positive and negative affect (Schmidt et al., 2019), subjective happiness (Booker & Dunsmore, 2019), gratitude (Nguyen et al., 2020), and depressive symptoms (Kelliher Rabon et al., 2018).
In contrast to this rapid expansion of evidence and debate regarding the key mediators in mental health research, evidence regarding possible mediators in physical health contexts remains less well-developed. As noted, self-compassion is a complex construct and it is possible that self-compassion may influence physical health outcomes via similar, different, or multiple pathways (Homan & Sirois, 2017). Indeed, it is unclear whether the same mediators and pattern of findings seen between self-compassion and mental health will explain the pathways between self-compassion and physical health outcomes.
To date, theoretical discussion of the putative mechanisms behind self-compassion has predominantly occurred in the context of mental health. Several theories have been offered, focusing on possible roles for cognitive processes, for example, reductions in automatic thinking, cognitive fusion, cognitive appraisal (Arimitsu & Hofmann, 2015; Basharpoor et al., 2021; Chishima et al., 2018), and ruminative depression (Fresnics & Borders, 2017; Fresnics et al., 2019). In such views, because self-compassionate individuals are less self-critical or judgemental, they are less likely to experience negative affect (or perceived stress) following challenging events or ruminate less about the possible negative implications.
However, perhaps the broadest theoretical framework used to understand self-compassion’s effects (and the most overtly relevant to physical health) is found in theories of self-regulation (Baumeister & Heatherton, 1996; Homan & Sirois, 2017; Sirois et al., 2015, 2019). Approaches in the line, such as the self-regulation resource model (SRRM; Sirois et al., 2015), suggest that self-compassion may “free up” the individuals’ resources for self-regulation by reducing engagement with negative affect while generating positive affect to support healthy self-regulation and promote good health.
In this light, the aims of the current review were threefold. Firstly, it was designed to systematically review and characterize the range of mediators that have been empirically assessed in physical health contexts. Summarizing the frequency with which different types of mediators have been assessed is important in terms of identifying areas of focus and omission in this field. Secondly, we evaluated study quality and risk of bias, and assessed the quality of the mediational approaches currently being used. Lastly, we evaluated the extent to which the mediators assessed to date are (a) similar or different to the mediators evaluated in mental health contexts and (b) are reflective of the mediators hypothesized to be important in theories of self-compassion.
Methods
This systematic review was conducted according to the PRISMA guidelines (Liberati et al., 2009; Rethlefsen et al., 2021). The search for articles was conducted using six online databases including Embase, Medline, APA PsycInfo, Scopus, AMED, and Web of Science from 2003 to February 2022.
In the interests of transparency, it is worth noting that the initial PROSPERO registration (CRD42021241915) was amended to change the search focus from “psychosocial health” to “physical health,” approximately one-month after the initial pre-registration but prior to data extraction. In brief, this change was implemented because initial psychosocial health searches led to a near-exclusive capturing of psychological mediators, impairing our ability to address questions regarding different types of mediators.
Search Strategy
An initial search strategy was developed and reviewed by a subject librarian on 11th November 2020, as well as drawing from the search terms employed in prior systematic reviews in related areas (Inwood & Ferrari, 2018; Wilson et al., 2019). Given the limited number of studies around mediators of self-compassion, only the synonyms and keywords relating to self-compassion were searched. This approach was adopted as restricting the number of elements in a search strategy optimizes recall and minimizes the chance of missing relevant references (Bramer et al., 2018). As a result, the strategy included selfcompassion* or self compassion* or compassion* adj3 self* and, based on the search strategy used in a systematic review and meta-analysis on self-compassion (Wilson et al., 2019), the terms self-kindness or self kindness were also included. Reference checks and forward citation searches for the selected studies were conducted.
Definition of Terms
Due to the limited number of studies evaluating the mediators linking self-compassion with physical health outcomes, a broad criterion of “physical health” was used. The broad criterion ranged from commonly evaluated key physical health outcomes and health behaviors in the self-compassion literature (Dunne et al., 2018; Sirois et al., 2015; Terry & Leary, 2011) including sleep quality, stress, physical symptoms, health-promoting behaviors, and substance-related problems. We did not include certain eating-related outcomes (e.g., disordered eating or intuitive eating), given the close psychological overlap between those variables and mental health factors. Given the purpose of this review, we did not impose any restrictions on the type of mediators evaluated.
Inclusion Criteria
We included studies that met the following criteria: studies published in English, original peer-reviewed articles published in an academic journal, published in or after 2003 (the publication of the first standardized measure of self-compassion; Neff, 2003) quantitative studies (self- or other-report), observational studies (cross-sectional or longitudinal), experimental or randomized controlled trials, individuals aged 18 + years, subjective and/or objective measures of physical health as reported outcomes, and analyses of the total self-compassion score (either state or trait; Neff, 2003).
While ongoing discussions around the conceptualization and measurement of self-compassion are clearly important (e.g., Ferrari et al., 2022; Khoury, 2019; Muris & Otgaar, 2020; Neff, 2022), our pre-registered inclusion criteria only captured studies using the total Self-Compassion Scale (SCS) score; including the full SCS (Neff, 2003) and the SCS short-form (Raes et al., 2011). Given the heterogeneity in both mediators and outcome types, maintaining consistency in the indices of self-compassion was critical to facilitating interpretation and synthesis. Therefore, we elected to focus on the best-established and most widely used measure, only including studies representing this specific conceptualization and measurement of self-compassion. Using omega index estimates, Neff (2016) found that the overall self-compassion score accounted for at least 90% of reliable variance across all populations. In more recent findings, Neff (2022) suggested that the total self-compassion score most comprehensively represents the self-compassionate approach to suffering. It is thus possible that future works evaluating broader or different conceptualizations of self-compassion will produce distinct mediators.
Given our focus on mediators, we only included studies including a formal statistical test of mediation in which studies had to demonstrate an indirect effect — mediated a*b pathway (Hayes, 2013). Mediation analyses could be conducted using well-established methods, including multiple regression and structural equation modelling. Tests of indirect effects could include a range of established methods such as bootstrap confidence interval and Monte Carlo methods.
Although some argue that intervention studies such as randomized controlled trials (RCT) or other prospective designs are more valid designs to test mediation (Kraemer et al., 2002), the underdeveloped nature of this research area meant that most studies were cross-sectional. However, mediation analysis can be conducted even where causality cannot be established due to design limitations (Hayes, 2013); theory and solid arguments can form the initial basis for subsequent causal claims. We did not distinguish between complete and partial mediation, as recent works have suggested this distinction is not meaningful (Hayes, 2013; Rucker et al., 2011). Finally, while we included studies that evaluated self-compassion both as a predictor and mediator in different models, we only reported and interpreted the results of the mediation models that included self-compassion as the predictor.
Exclusion Criteria
Studies were excluded if they comprised reports of qualitative designs, systematic reviews, meta-analyses, letters, commentaries, thesis manuscripts, editorials, corrections, errata, reviews, editorials, abstracts-only, conference abstracts or book chapters. Studies administering or testing subscale measures of self-compassion were excluded based on concerns described in the inclusion criteria. Studies with participants aged under 18 years were excluded, as were studies of those meeting the diagnostic criteria (current or within the last 5 years) for a mental health disorder (according to DSM-5) and/or a chronic illness diagnosis (according to ICD-11). We focused on non-clinical adult samples (including student samples and young adults over 18) as there are marked differences between clinical and non-clinical samples in self-compassion-related constructs, such as self-criticism and fears of compassion, particularly in their association with mental health outcomes such as depression (Gilbert et al., 2014). Given the strong links between mental and physical health (Nabi et al., 2008; Surtees et al., 2008), other confounding factors may exist in clinical populations. Disentangling the mediators of self-compassion that are specific to the non-clinical population, in the absence of other co-morbid and confounding variables that are common in clinical populations, could help elucidate the actual associations between self-compassion and physical health.
Study Selection
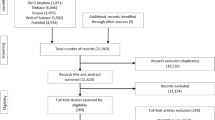
Initially, 19 eligible papers were identified from 6439 papers (see Fig. 1 for a schematic of the selection process) by two researchers (first author JC and reviewer AB). Of the 101 articles assessed for full-text screening, the majority (80%) were excluded based on various reasons, but not assessing a physical health outcome was the most common exclusion criterion (70%). Two additional papers were identified by JC and AB from reference checks and forward citation searches, resulting in 21 papers, although one additional study was subsequently excluded due to including a clinical population.
Overall, 20 papers (articles with more than one mediation studies were counted as separate studies) meeting all inclusion criteria were identified, and the following information was extracted by JC and AB for summary tables: sample characteristics, study design, self-compassion measurement, mediator variables and measures, physical health outcomes and measures, quality ratings for Downs and Black (Downs & Black, 1998), test of mediation, correlations, results of mediational analyses, co-variates (if reported), and mediation checklist (Rhodes & Pfaeffli, 2010). Although we did not observe any specific patterns, the two researchers (JC and AB) were inconsistent in approximately 3% of the decisions regarding article selection. All inconsistencies were resolved by mutual consent or by consulting a senior researcher (NC).
Study Methodological and Mediation Quality Rating Assessments
In line with our aim of assessing studies’ risk of bias and the quality of mediational approaches, 20 identified papers were evaluated for methodological and mediation quality using the Checklist for Measuring Quality (Downs & Black, 1998) and an adapted version of the Mediation study quality checklist (Rhodes & Pfaeffli, 2010). The Checklist for Measuring Quality has high internal consistency, good inter-rater and test re-test reliability (Downs & Black, 1998), and can be applied across designs (Malik et al., 2015). Importantly for this review, Downs and Black’s (1998) tool has been applied to both cross-sectional and longitudinal designs. Various adapted versions have been used from the original 27 items. For our review, we used the original, 27-item checklist for intervention studies and an adapted 15-item checklist (Irving et al., 2006) for non-intervention studies (e.g., cross-sectional and longitudinal). The additional 12 items asked for intervention studies were 4, 8, 9, 13, 14, 15, 17, 19, 23, 24, 26, and 27. Given the variation in the number of quality evaluation items relevant to different study types, a percentage score was used to present and compare the overall quality assessment results across intervention and non-intervention designs. Consistent with prior systematic review and meta-analysis using the Downs and Black tool (Munn et al., 2010), study quality was scored as follows: > 75% as high, 60–74% as moderate, and < 60% as low.
In addition, a mediation quality checklist tool initially developed by Lubans et al. (2008), and later adapted by Cerin et al. (2009) and Rhodes and Pfaeffli (2010), was adapted for the current review. The updated mediation checklist tool contains 11 items (three additional items from the original 8-item checklist by Lubans et al. (2008)). Items assess the quality of mediation studies in scale reliability, mediation analysis methods, and assessment of change in mediators preceding change in the outcome (for intervention studies). For the current review, all 11 items were used but some of the item wordings were adapted (e.g., from physical activity to physical health outcomes). Each item was scored in a yes (1) or no (0) format and a total score was generated by summing up all items. We used the criteria by Cerin et al. (2009) in which studies scoring 0–3 were deemed low-quality, 4–6 as medium-quality, and 7–9 as high-quality studies. Both quality checks were conducted independently by JC and AB. Similarly, while there were no specific questions or sections resulting in inconsistent ratings, there was disagreement in approximately 6% in risk of bias and mediation quality checklist assessments. All disagreements were resolved by mutual consent or by consulting the senior researcher (NC) to reach 100% agreement.
Results
Overview of Studies
Table 1 presents a summary of study characteristics included in the current review. All studies used quantitative designs and normative samples (n = 20/20). Nine involved university student samples, others employed community (n = 4/20) or Amazon Mechanical Turk (MTurk) samples (n = 2/20). One study combined university and community samples and others consisted of mothers with young children, employees, educators, and psychologists. Of the studies that reported gender proportions, apart from two studies reporting only 45% female samples, most studies had over 50% women (55 to 100%). The largest number of included articles was from Canada (n = 10/20), two studies originated from Germany and the UK, and single studies originated from the UK, the USA, Australia, and China. Three studies did not report the country where the study was conducted. Sample sizes ranged from 68 to 646 participants and the mean age of included study participants ranged from 20 to 42 years.
All studies used either the full 26-item Self-Compassion Scale (Neff, 2003) or the 12-item Self-Compassion Scale Short Form (Raes et al., 2011), as per our inclusion criteria. A range of physical health outcomes were assessed. Most studies used validated self-report measures to assess outcomes: sleep quality (n = 8/20) was assessed by Insomnia Severity Index (Bastien et al., 2001), sleep quality index (Jenkins et al., 1988), and the Pittsburgh Sleep Quality Index (Buysse et al., 1989). Physical symptoms (n = 1/20) were assessed by the Symptoms of Illness Checklist (SIC; Stowell et al., 2009), stress (n = 1/20) by the Depression and Anxiety Scale (Lovibond & Lovibond, 1995), and physical health (n = 1/20) by the RAND 36-Item Health Survey (Hays & Morales, 2001).
The measurement of health-promoting behaviors (n = 3/20) was more varied. Eating behavior was measured by the three items according to the Chinese Dietary Guidelines (Wang et al., 2016). Other health-promoting behaviors, including intentions, were measured by the Wellness Behavior Inventory (Sirois, 2001). Bedtime procrastination (n = 2/20) was measured by the Bedtime Procrastination Scale (Kroese et al., 2014). Lastly, drinking to cope with anxiety/depression, coping-motivated marijuana use, and alcohol/marijuana-related problems (n = 4/20) were assessed. Drinking to cope with depression and anxiety was measured by the Modified Drinking Motives Questionnaire–Revised (MDM-R; Blackwell & Conrod, 2003), coping motivated marijuana use was measured by Marijuana Motives Measure questionnaire (MMM; Simons et al., 1998), alcohol-related problems were measured by the Young Adult Alcohol Consequences Questionnaire (YAACQ; Read et al., 2006), and marijuana-related problems were measured by the Brief Marijuana Consequences Questionnaire (BMCQ; Simons et al., 2012).
The primary purpose of the current review was to quantify and characterize the factors tested as possible mediators of the relationships between self-compassion and physical health. A range of mediators were evaluated via self-report measures. Most studies used validated scales, but some measures had lower content validity and internal consistency due to selecting specific items from the full-scale (not subscales), using measures from manuals but not journal publications, and reporting internal reliability (α-value) from another study but not from the specific sample. However, some of these limitations were captured by methodological and mediation quality check assessments (refer to Tables 1 and 2).
In addressing another aim of this review, the most frequently assessed mediators were perceived stress (n = 5/20) and (aspects of) emotion regulation (n = 5/20). Studies evaluating stress used the Perceived Stress Scale (Cohen et al., 1983), although one used the Short Form Perceived Stress Scale (PSS-4; Leung et al., 2010), and one study used the stress subscale from the Depression Anxiety Stress Scales (DASS-21; Lovibond & Lovibond, 1995). Emotion regulation (and/or emotion regulation difficulties) was typically assessed using the Difficulties in Emotion Regulation Scale (DERS; Gratz & Roemer, 2004). Two studies used all six dimensions (non-acceptance, goal direction, impulse control, awareness, strategies, clarity), whereas one study only used five dimensions, omitting the awareness dimension (Bardeen et al., 2012). One study used the cognitive reappraisal subscale of the Emotion Regulation Questionnaire (ERQ; Gross & John, 2003), and one study used the Cognitive Emotional Regulation Questionnaire (Garnefski et al., 2001).
In addition to stress and emotion regulation, positive and negative affect (n = 3/20) and various maladaptive coping strategies (n = 3/20) were also commonly evaluated mediators. Affect was typically assessed with the Positive and Negative Affect Schedule (PANAS; Watson et al., 1988), with one study using the short 10-item version of the PANAS-X (Watson & Clark, 1999). For maladaptive coping strategies, drinking to cope with anxiety and depression was measured by the 28-item MDM-R (Blackwell & Conrod, 2003) and coping motivated marijuana use was measured by MMM (Simons et al., 1998; previously used as an outcome measure by Wisener & Khoury, 2020; Study 2).
Other prospective mediators included rumination (n = 2/20), health-promoting behaviors (n = 2/20), health self-efficacy (n = 1/20), proactive health focus (n = 1/20), burnout (n = 1/20), mother guilt (n = 1/20), anxiety about sleep (n = 1/20), and poor sleep hygiene (n = 1/20). Rumination was measured by a shortened version of the Rumination Response Scale (Nolen-Hoeksema & Morrow, 1991) and a modified version of the Ruminative Responses Scale (Treynor et al., 2003). Health-promoting behaviors were measured by the 10-item Wellness Behaviors Inventory (WBI; Sirois, 2001) and Health Promoting Lifestyle Profile II (HPLPII; Walker et al., 1995). Health self-efficacy was measured by the Control Beliefs Inventory (CBI; Sirois, 2002), and proactive health focus was measured by the Proactive Health Focus scale (PHF; Terry et al., 2013). Burnout was measured by the Professional Quality of Life (ProQOL-5) scale (Stamm, 2009), and mother guilt was measured by the State Shame and Guilt Scale (SSGS; Marschall et al., 1994). Lastly, anxiety about sleep was measured by the Anxiety and Preoccupation about Sleep Questionnaire (APSQ; Tang & Harvey, 2004) and sleep hygiene was measured by the Sleep Hygiene Index (SHI; Mastin et al., 2006).
Quality Ratings (Downs and Black Checklist and Mediation Checklist)
Recall that the current review assessed the quality of the included studies, including risk of bias and the quality of the mediational approaches. Across the 20 included studies, quality ratings for Downs and Black (1998) ranged from 40% (low-quality) to 73% (moderate quality). Six studies scored within the low rating range of 40–53% (Butz & Stahlberg, 2018; Hwang et al., 2019; Li et al., 2020; Sirois et al., 2019; Vaillancourt & Wasylkiw, 2019; Wisener & Khoury, 2021) and 14 scored within the moderate quality, 60–73%, range (Butz & Stahlberg, 2018; Dunne et al., 2018; Finlay-Jones et al., 2015; Homan & Sirois, 2017; Hu et al., 2018; Miller & Strachan, 2020; Rakhimov et al., 2022; Semenchuk et al., 2021; Sirois et al., 2015, 2019; Wisener & Khoury, 2020, 2021). More specific study ratings can be found in Table 1.
Mediation checklist ratings ranged from low to high quality with scores ranging from 2 to 8 (out of 11). One study scored 8 with high quality (Study 2; Butz & Stahlberg, 2018), 12 studies scored within the moderate quality ratings within the range of 4–5 (Butz & Stahlberg, 2018; Finlay-Jones et al., 2015; Homan & Sirois, 2017; Hwang et al., 2019; Rakhimov et al., 2022; Semenchuk et al., 2021; Sirois et al., 2015, 2019; Wisener & Khoury, 2021), and seven scored within the low quality range of 2–3 (Dunne et al., 2018; Hu et al., 2018; Li et al., 2020; Miller & Strachan, 2020; Vaillancourt & Wasylkiw, 2019; Wisener & Khoury, 2020).
Associations Between Target Variables (Self-Compassion, Mediators, and Physical Health Outcomes)
To facilitate interpretations regarding the types of mediators investigated thus far, mediators were grouped into (1) psychological and (2) behavioral factors. Given that most mediators were psychological, we further subcategorized psychological mediators into (1a) emotional and affective, and (1b) social-cognitive processes. These groupings were made conjointly by the first author (JC) in consultation with the senior researcher (NC). Such decisions were based on whether the mediators reflected theoretically similar constructs on the basis of face validity considerations of the self-regulation theory (Baumeister & Heatherton, 1996), basic psychological theories of emotions and affect, social-cognitive processes, and broad conceptualizations of behavioral theories. The purpose of the grouping was to assist in the current review’s aim of quantifying the types and frequency of mediators tested for enabling us to identify the types of constructs most in need of further evaluation.
Below, the findings from the review are presented under these groupings. First, correlations among the target variables and the mediational findings are summarized and the presence/absence of an indirect effect noted. Given that co-variation between the predictor and outcome variables is no longer a requirement for testing for cause and effect (Hayes, 2013), only the correlations between (i) putative mediators and self-compassion and (ii) mediators and outcomes are discussed. Note, however, that correlations between self-compassion and outcomes can be found in Table 2.
Secondly, we report findings of indirect effects of various mediators linking self-compassion to physical health. Out of the 20 studies, nine used simple mediation models (Butz & Stahlberg, 2018; Dunne et al., 2018; Hu et al., 2018; Hwang et al., 2019; Miller & Strachan, 2020; Semenchuk et al., 2021; Sirois et al., 2019; Vaillancourt & Wasylkiw, 2019) and eight used multiple parallel mediation models (Finlay-Jones et al., 2015; Semenchuk et al., 2021; Sirois et al., 2015, 2019; Wisener & Khoury, 2020, 2021). Of the remaining three studies, one used a serial mediation model (Homan & Sirois, 2017), one used a multilevel mediation model (Li et al., 2020), and the remaining one used both multiple and sequential mediation in the same model using SEM (Rakhimov et al., 2022). However, given the current review’s aim of quantifying and characterizing the mediators, we report various indirect effects under the appropriate mediator groupings. Table 2 presents a summary of results including correlations, mediation indirect effects, and quality ratings.
Self-Compassion, Behavioral Mediators, and Physical Health Outcomes
Three out of 20 included studies evaluated behavioral factors (more specifically, health-promoting behaviors and poor sleep hygiene) as possible mediators of the association between self-compassion and physical health outcomes. One study did not report correlations (Dunne et al., 2018), and another study found a moderate, positive correlation between health behaviors and self-compassion (r = 0.49, p < 0.001) and a moderate, positive correlation between health behaviors and physical health outcomes (r = 0.40, p < 0.001) (Homan & Sirois, 2017). Finally, one study showed that poor sleep hygiene had a negative, moderate correlation with self-compassion (r = − 0.33, p < 0.001), and a positive, moderate correlation with poor sleep quality (r = 0.41, p < 0.001).
For mediation effects, self-compassion had an indirect effect on physical health outcomes, physical symptoms (Dunne et al., 2018), and physical health (Homan & Sirois, 2017) via health behavioral mediators. Additionally, while self-compassion did not have an indirect effect on poor sleep quality via poor sleep hygiene (in a multiple mediation model), sequential mediation showed that self-compassion did have an indirect effect on poor sleep quality via (1) perceived stress then poor sleep hygiene and via (2) anxiety about sleep, perceived stress, then poor sleep hygiene.
Self-Compassion, Psychological Mediators (Emotional and Affective Factors), and Physical Health Outcomes
Five possible psychological mediators were evaluated: emotion regulation, positive affect, negative affect, perceived stress, and anxiety about sleep. Five studies evaluated (difficulties or aspects of) emotion regulation as a possible mediator between self-compassion and physical health outcomes. These studies showed negative correlations between difficulties in emotion regulation and self-compassion (from r = −.29 to −.73, p <.01) and between emotion regulation and outcomes (from r = .21 to .60, p <.01) including stress (Finlay-Jones et al., 2015) and maladaptive coping strategies (Wisener & Khoury, 2020, 2021). One study assessing cognitive reappraisal as a possible mediator reported a moderate, positive correlation with self-compassion (r = .49, p <.001) and a weak, negative correlation with bedtime procrastination (r = −.17, p <.001) (Study 2; Sirois et al., 2019). The other study assessing Cognitive Emotional Regulation (CERQ) (Study 2; Semenchuk et al., 2021) as a mediator found positive correlations between self-compassion and CERQ subscales except for the acceptance subscale (ranging from r = .19 to .46, p <.001). The correlations between CERQ subscales and poor sleep quality showed mixed findings: some were non-significant (self-blame, acceptance, putting into perspective, catastrophizing, and other blame) and others had weak, positive correlations (rumination, positive refocusing, refocus on planning, and catastrophizing; ranging from r = .15 to .17, p <.01, and r = .19, p <.001).
The findings for mediation analyses were also mixed. One study found that self-compassion had an indirect effect on physical health (stress) via emotion regulation difficulties (measured by five facets of DERS; Finlay-Jones et al., 2015) while another found that self-compassion had an indirect effect on physical health (bedtime procrastination) via cognitive reappraisal and negative affect (Sirois et al., 2019). Two studies found that self-compassion only had an indirect effect on outcome via specific facets of the DERS. One found that self-compassion had an indirect effect on drinking to cope with depression via limited access to emotion regulation strategies (Study 1; Wisener & Khoury, 2021) and another found that self-compassion had an indirect effect on coping motivated marijuana use via non-acceptance of emotions (Study 2; Wisener & Khoury, 2021). No other DERS facets had significant indirect effects in both studies. One study found that self-compassion had an indirect effect on poor sleep quality via self-blame but not via other cognitive emotion regulation strategies (Study 2; Semenchuk et al., 2021).
Two studies evaluated both negative and positive affect as mediators and one additional study evaluated negative affect alone. For negative affect, studies showed moderate, negative correlations with self-compassion (ranging from r = − 0.30 to − 0.48, p < 0.01) (Sirois et al., 2015) and weak, positive correlations with bedtime procrastination (Sirois et al., 2019) (ranging from r = − 0.26 to − 0.28, p < 0.01). A single study with health behavior intention as the outcome (Sirois et al., 2015) showed a weak, negative correlation with negative affect (r = − 0.15, p < 0.01). Studies of positive affect showed moderate, positive correlations with self-compassion (ranging from r = 0.43 to 0.44, p < 0.01), a weak, negative correlation with bedtime procrastination (r = − 0.20, p < 0.001), and a moderate, positive correlation with health behavior intentions (r = 0.36, p < 0.01) (Sirois et al., 2015, 2019). Mediational analyses showed an indirect effect for self-compassion on health outcomes via negative effect (Sirois et al., 2015). However, no significant indirect effects were observed for positive affect (Sirois et al., 2015, 2019).
Five out of 20 studies that included perceived stress as the mediator found strong, negative correlations with self-compassion (ranging from r = − 0.53 to − 0.80, p < 0.01) and moderate to strong correlations in the expected direction with physical health outcomes. In other words, moderate, positive correlations were observed between stress and poorer physical health (ranging from r = 0.34 to 0.43, p < 0.01) (Homan & Sirois, 2017; Hu et al., 2018; Hwang et al., 2019; Li et al., 2020; Rakhimov et al., 2022). Conversely, moderate to large negative correlations were observed between stress and indices of good physical health (ranging from r = − 0.41 to − 0.60, p < 0.001). For mediation analyses, four studies showed that self-compassion had an indirect effect on physical health via perceived stress (Homan & Sirois, 2017; Hu et al., 2018; Hwang et al., 2019; Li et al., 2020). One study showed that self-compassion did not have an indirect effect on poor sleep quality via perceived stress (in a multiple model with anxiety about sleep and poor sleep hygiene). However, for sequential mediation, self-compassion had an indirect effect on poor sleep quality via (1) perceived stress then poor sleep hygiene and via (2) anxiety about sleep, perceived stress, then poor sleep hygiene. The strong positive association between perceived stress and anxiety about sleep (r = 0.57, p < 0.001) suggests high overlap between the two variables may account for the null finding (i.e., non-significant indirect effect) for perceived stress (Rakhimov et al., 2022). Lastly, one study assessing anxiety about sleep showed a negative, weak correlation with self-compassion (r = − 0.28, p < 0.001), and a positive, strong correlation with poor sleep quality (r = 0.55, p < 0.001). Mediation analysis showed that self-compassion had an indirect effect on poor sleep quality via anxiety about sleep (Rakhimov et al., 2022).
Self-Compassion, Psychological Mediators (Social-Cognitive Processes), and Physical Health Outcomes
Mediational studies have tested several social-cognitive processes: self-efficacy, guilt, burnout, rumination, maladaptive coping, and proactive health focus. Self-efficacy had a positive, moderate correlation with self-compassion (r = 0.40, p < 0.01), and a strong, positive correlation with health behavior intentions (r = 0.56, p < 0.01) (Sirois et al., 2015). Mediation analysis found that self-compassion had an indirect effect on health behavior intentions via self-efficacy as well as negative affect (but not positive affect) in the same multiple mediation model. Proactive health focus had a moderate, positive correlation with self-compassion (r = 0.30, p < 0.001), and a weak, negative correlation with poor sleep quality (r = − 0.00, p < 0.001). Mediation analysis found that self-compassion did not have an indirect effect on sleep quality via proactive health focus (Semenchuk et al., 2021).
Correlations were not reported in the study that evaluated guilt as a possible mediator, but the study found an indirect effect of self-compassion on health-promoting behavior via mother guilt (Miller & Strachan, 2020). One study evaluating burnout had a strong, negative correlation with self-compassion (r = − 0.67, p < 0.01) and a moderate, negative correlation with sleep quality (r = − 0.46, p < 0.01). Mediation analysis showed that self-compassion had an indirect effect on sleep quality via burnout (Vaillancourt & Wasylkiw, 2019). However, this finding needs to be interpreted with caution as the study showed low quality ratings on the mediation checklist. Similarly, for rumination as the mediator, analyses showed moderate to large, negative correlations with self-compassion (ranging from r = − 0.31 to − 0.62, p < 0.01) and sleep quality (ranging from r = − 0.47 to − 0.59, p < 0.01). Mediation analyses showed that self-compassion had an indirect effect on sleep quality via rumination for both cross-sectional and intervention study designs (Study 1 and 2; Butz & Stahlberg, 2018).
Several maladaptive coping strategies (drinking to cope with anxiety, drinking to cope with depression, coping motivated marijuana use) were evaluated as potential mediators between self-compassion, alcohol, and marijuana-related problems (Wisener & Khoury, 2020). Such mediators (drinking to cope with anxiety, drinking to cope with depression, and coping motivated marijuana use) had weak-to-moderate negative correlations with self-compassion (ranging from r = − 0.25 to − 0.41, p < 0.01). Additionally, the same set of mediators had moderate, positive correlations with various substance-related outcomes (e.g., alcohol, marijuana-related problems, drinking to cope with depression, anxiety, and coping motivated marijuana use, ranging from r = 0.40 to 0.44, p < 0.01). Mediation analysis showed that self-compassion had an indirect effect on marijuana-related problems via coping motivated marijuana use (Study 2; Wisener & Khoury, 2020). Furthermore, parallel mediation analyses showed that self-compassion had an indirect effect on alcohol-related problems via drinking to cope with anxiety but not via drinking to cope with depression (Study 1; Wisener & Khoury, 2020).
In summary, while the magnitude of correlations among target variables ranged from weak to strong, most studies found significant indirect effects between self-compassion and health outcomes via the proposed psychological (affective/emotional and social-cognitive) mediators, behavioral mediators. However, positive affect (n = 2/20), some DERS and CERQ facets (n = 3/20), drinking to cope with depression (n = 1/20), and proactive health focus (n = 1/20) did not mediate the associations between self-compassion and the specific physical health outcomes measured in various studies (Semenchuk et al., 2021; Sirois, 2015; Sirois et al., 2019; Wisener & Khoury, 2020, 2021).
Discussion
The primary aim of this review was to quantify and characterize the mediators thought to link self-compassion to physical health outcomes in non-clinical adult populations. To date, mediational studies in this domain have focused on testing psychological mediators that are broadly similar to those seen in mental health research (e.g., perceived stress, negative affect, and emotion regulation). Although a few behavioral mediators were also evaluated, the extent to which mediators are theoretically relevant remains unclear. In terms of quality assessment, evaluation tended to suggest low to moderate quality for risk of bias, and predominantly low to moderate for the mediation checklist. Improvements for future mediation studies are needed both in methodology and in implementing better mediation analysis practice. Interpretatively, most included studies tended to use the self-regulation theory (Baumeister & Heatherton, 1996) as their general theoretical framework. Below, these findings are considered more fully, with specific attention given to summarizing the evidence and considering study and mediational quality.
Additionally, the implications for which the current data may have on evaluating the pathways in which self-compassion may impact physical health outcomes will be considered. Directions for future studies are also given.
Mediator Types and Frequency in Linking Self-Compassion to Physical Health
In summarizing the frequency with which the different types of mediators have been assessed in evaluating links between self-compassion and physical health, the current review found an ongoing focus on psychological mediators, notably affective and social-cognitive factors (n = 15/20). Perceived stress (n = 5/20) and emotion regulation (n = 5/20) were the most frequently evaluated mediators. However, despite (a) physical health outcomes being distinct from mental health and (b) health being more directly impacted by behavior, only three studies examined possible behavioral mediators (Dunne et al., 2018; Homan & Sirois, 2017; Rakhimov et al., 2022).
In testing the different mediator types, preliminary evidence shows that psychological mediators predominate but mediation effects remain somewhat mixed. We observed consistent significant indirect effects for negative affect and perceived stress (in the absence of overlapping affective mediator — anxiety about sleep) (Rakhimov et al., 2022) but not for positive affect (Sirois et al., 2015, 2019). Additionally, we found mixed significant and non-significant indirect effects for emotion regulation (Finlay-Jones et al., 2015; Sirois et al., 2019; Wisener & Khoury, 2021).
Behavioral factors linking self-compassion to physical health outcomes were less commonly studied. In summary, health-promoting behaviors tend to be significant mediators but sleep-hygiene only had an indirect effect in sequential mediating pathways when the effects of anxiety about sleep and perceived stress had been accounted for. While the limited number of studies of behavioral factors makes it challenging to derive a pattern, initial evidence suggested that “negative” psychological constructs (e.g., negative affect) were more relevant to physical health outcomes than positive ones (e.g., positive affect).
Mediation Methods and Study Methodological Quality
A second aim of the current review was to assess study and mediational method quality — seeking to identify areas of relative strength and weakness in the ways research has sought to identify self-compassion’s potential mediators in physical health contexts. Broadly, the evaluation presented here suggested that in terms of both study and mediational quality, ongoing concerns remain. For risk of bias, although most studies scored within the acceptable, moderate range, six studies scored within the low range, indicating more serious limitations. Methodologically, the most common issues regarded limitations of external validity (notably generalizability) and internal validity (regarding internal consistency, confounding and selection bias). Future studies seeking to evaluate clinical or patient populations should further consider the issue of external validity as it is likely to have greater importance in health care evaluation and change in clinical practice. Regarding internal validity, most studies did not consider confounders and some studies did not report internal consistency (α-value) for the self-reported scales. In future work, we highly recommend identifying and evaluating confounders and reporting internal consistencies for all scales representative of the specific study sample.
Likewise, for the mediation checklist, most studies showed some concerns. Most issues were found in the study designs (e.g., cross-sectional and correlational), not having conducted an appropriate power analysis for mediation analyses, not addressing and controlling for confounds and covariates, and not conducting a sensitivity analysis. Despite the importance of addressing and controlling for confounds (Valente et al., 2017) and covariates (Hayes & Rockwood, 2017) in mediational testing, only a few studies identified and controlled for potential confounders and covariates. Furthermore, while sensitivity analyses assessing the influence of unmeasured confounders are often recommended (VanderWeele, 2019), such analyses were not evident in any included studies. Hence, possible confounders and covariates together with a possible impact from unmeasured factors may be explaining alternative pathways.
Although not captured by the mediation checklist, an important factor to consider in current mediation analyses is the types of indirect effects used by researchers. Various methods are used to test for indirect effects, but bootstrapping confidence interval techniques are strongly recommended (Hayes, 2013; Preacher & Hayes, 2004, 2008). Previous methods such as the causal steps approach by Baron and Kenny (1986) have been criticized on multiple grounds, notably regarding issues with power (Fritz & MacKinnon, 2007; MacKinnon et al., 2002). Likewise, Sobel’s test (Sobel, 1982) has also been criticized for being low in power mainly due to the assumption of normality for the sampling distribution of the indirect pathway (Hayes & Rockwood, 2017). Of the studies included in this review, two used path analysis (Hwang et al., 2019; Sirois et al., 2019), one used Sobel’s test (Finlay-Jones et al., 2015), and another study used Monte Carlo methods (Li et al., 2020). The remainder used the recommended bootstrap confidence interval methods using PROCESS (Hayes, 2013). In summary, most studies used the recommended methods of indirect testing, which avoids making false assumptions about the mediators of interest. However, future mediation studies need to identify and control for possible confounds and should conduct a power analysis suited to intended mediational analyses.
Interpretation of Findings in Relation to Existing Empirical Data
Our review showed a heavy concentration of psychological mediators linking self-compassion to health outcomes together with a few potential behavioral mechanisms being unique to physical health outcomes. This pattern raises two general points worth considering. Firstly, the mediators assessed in physical health largely overlap with those assessed in mental health (mainly psychological factors), when in fact, this “mediator set” may not be entirely suitable. Secondly, other types of mediators (behavioral, motivational, and social constructs), which may be more relevant to physical health outcomes, were notably absent in current mediation works.
Despite broad similarities and overlap in terms of the types of mediators examined thus far across physical and mental health areas of study (e.g., positive and negative affect, emotion regulation), the data from this review also suggest we must be careful in assuming that the same mediators will operate in all contexts. For example, a previous systematic review evaluating emotion regulation as the mechanism of change found consistent support for emotion regulation as the mediator between self-compassion and mental health outcomes (Inwood & Ferrari, 2018). However, findings were mixed in this review; some found significant (Finlay-Jones et al., 2015; Sirois et al., 2019) and others non-significant (Wisener & Khoury, 2021) indirect effects of emotion regulation linking self-compassion to physical health.
There are a number of possible reasons that emotion regulation might be a less consistent mediator in physical versus mental health contexts. For example, the mixed findings could be due to measurement issues with the Difficulties in Emotion Regulation Scale (DERS; Gratz & Roemer, 2004). In our review, some studies employed all six DERS facets (Wisener & Khoury, 2021), whereas some only employed five facets without the Awareness subscale (Finlay-Jones et al., 2015). A previous study has suggested problems with the Awareness subscale as it may not represent the same higher-order emotion regulation construct as the other five dimensions (Bardeen et al., 2012). In support of this notion, subsequent factor analytic work suggested that DERS had good internal consistency with a robust bifactor latent structure without the Awareness subscale (Hallion et al., 2018). Hence, it is possible that the mixed findings are reflecting issues with varied factor structures of DERS rather than differences in associations between target variables. However, it is also possible that similar measurement issues also exist in mental health contexts.
A more likely explanation for the irregularity of emotion regulation is due to the heterogeneity in physical health outcomes studied so far. The current review focused on physical health outcomes, but nonetheless included studies that evaluated emotion regulation as mediators on outcomes ranging from stress (Finlay-Jones et al., 2015) to bedtime procrastination (Sirois et al., 2019) and drinking to cope with depression/anxiety and coping motivated marijuana use (Wisener & Khoury, 2021). Given ongoing debate regarding the direction of the links between self-compassion and physical health (e.g., higher self-compassion predicting better physical health or better physical health influencing higher self-compassion levels) (Hall et al., 2013; Raque-Bogdan et al., 2011), mixed results may reflect the different types of physical health outcomes and their measurements. Nonetheless, these findings highlight the possibility that the psychological mediators thought to link self-compassion to mental health outcomes may not be suitable for investigations in other contexts, such as in physical health (which are more heterogeneous in nature).
An important final comment reflects the need for future work to assess positive affect using measures that include indices of low arousal positive emotions. The current review found that positive affect did not mediate the links between self-compassion and health outcomes (health behavior intentions, bedtime procrastination; Sirois et al., 2015; Sirois et al., 2019), suggesting that reductions in negative affect may be more important. However, studies to date have indexed positive affect via the Positive and Negative Affect Scale (PANAS; Watson et al., 1988) which does not assess low arousal states such as acceptance, calm, or equanimity that appear more consonant with self-compassion theory (Neff, 2003). Evidence from related studies in mindfulness suggests a link between meditation and greater lower arousal positive states (Jones et al., 2018) and incorporating such measures seems likely to return interesting findings.
Interpretation of Findings in Relation to Theoretical Evidence
In considering how we might expand our investigation of the types of mediators to encompass those suited to physical health, theories of self-regulation (Baumeister & Heatherton, 1996), the adaptive regulation of emotions (Gratz & Roemer, 2004), and stress and coping (Lazarus, 1966) appear the most viable theoretical bases for current mediators. Theoretically, self-compassionate individuals are more likely to respond to health-related failures with acceptance rather than self-criticism or judgment (self-kindness), view their setbacks as part of the wider human experience (common humanity), and with less rumination (mindfulness; Adams & Leary, 2007). In theory, this way of managing failures might enhance physical health by freeing up the resources needed for more effective behavioral self-regulation (Sirois et al., 2015). This view is consistent with the limited strength model of self-regulation (Baumeister & Heatherton, 1996; Baumeister et al., 2007), which suggests that individuals have a limited supply of “willpower” for acts of self-control. When this general resource gets depleted, we are more likely to experience failures in self-control.
The included studies showed some support for the self-regulation resource model (SRRM) (Sirois et al., 2015) in which self-compassion enhances physical health via reductions in negative affect. Interestingly, we did not find supporting evidence for an increase in positive affect (Sirois et al., 2015, 2019). Conceptually, there are logical reasons to expect that negative affect might have a stronger effect than positive affect. For example, as self-compassion is apparent in times of suffering (Neff, 2003), it is possible that self-compassion may interrupt individuals’ tendency for self-critical thoughts or responses to negative or “failed” health goals (e.g., failing to exercise three times a week), thereby reducing the negative affect associated with activation of threat systems (i.e., experience less set-back). Reductions in negative affect may, in turn, require fewer regulatory resources to protect the self thus freeing up self-regulatory capacity for future health-promoting practices and behaviors.
In summary, while there is some indirect evidence suggesting that self-compassion may “free up” resources and prevent depletion (as indexed via reductions in negative affect) thus resulting in better physical health, more direct empirical examinations are warranted. Most studies treat differences in the affective or emotional aspects of self-regulation as if they indexed this process, while other aspects of self-regulation (which may be as important in physical health outcomes, notably in relation to behavioral change such as motivation, goals, and values) have not yet been evaluated. Previous work has suggested that understanding an individual’s core values and goals in relation to self-compassion may be important (McGehee et al., 2017) as do influential approaches such as the theory of planned behavior (Ajzen, 1991). Future studies offering direct tests of the hypothesized self-regulatory mediational pathways (e.g., motivational factors and goal orientation) are clearly needed.
Limitations, Implications, and Future Directions
There are a few limitations to consider in the current review. Recall that the primary aim of the current review was to quantify and characterize the mediators linking self-compassion and physical health. However, in all initial stages of mediation reviews, temporal precedence posits a challenge in determining the true indirect effects. While some studies tested alternative models (e.g., Wisener & Khoury, 2021) and used different types of mediation models to test various associations (e.g., using multiple or serial mediation), few studies with homogenous mediator and outcome types limited our ability to make reliable comparisons across different findings.
Additionally, most of the studies included here were cross-sectional, correlational designs, effectively precluding clarity regarding the directionality of the relationships among self-compassion, proposed mediators, and outcomes. For example, it is possible that the onset of physical health issues may reduce individual’s self-compassion (e.g., by increasing feelings of isolation and reducing a sense of common humanity; Casati et al., 2000). Equally, previous studies suggest that the links between mechanisms and health outcomes may be reciprocal and mutually reinforcing (Sirois et al., 2019). Given such complex, dynamic associations, prospective studies will likely prove useful in understanding the temporal links between self-compassion and physical health outcomes.
The samples in most included studies were predominantly female. Of those included studies reporting ethnicity, most participants self-identified as Caucasian or White, limiting generalizability to other samples (including clinical populations). Prior work such as that by Koopmann-Holm and Tsai (2017) delineated important cultural variation in the perception, experience, and expression of compassion and other studies suggested that the concept of self-compassion varies depending on contextual (cultural) values (Montero-Marin et al., 2018). Given that individuals think and behave in ways that are consistent with their culturally shared values (Hofstede et al., 2005), more work considering how cultural characteristics may influence mediational tests is needed.
More broadly, our findings may also be influenced by publication bias. Although a few published studies have reported non-significant indirect effects, it is possible that our review overestimated the likelihood of certain mediators simply because “positive” mediational findings are more likely to be published. Equally, in the absence of pre-registration, it is possible that published studies evaluated other mediators in initial analyses but did not (or could not) publish them due to non-significant indirect effects. While the significant indirect effects for various mediators tended to be consistent across multiple studies for the most part, publication bias needs to be carefully considered when interpreting the results.
Finally, the limitations associated with measurement issues should be noted. All studies relied on self-report measures which are prone to a number of biases including issues with recall, self- and other-presentation, and aggregation (Podsakoff et al., 2012). Prior work shows that self-compassion is associated with lower hypochondriasis (Raque-Bogdan et al., 2011), meaning differences in reporting may be influential. Incorporating objective measures is one obvious solution for future studies. Perhaps more importantly, included studies all relied on a specific conceptualization of self-compassion, measuring this construct via either the full Self-Compassion Scale (Neff, 2003) or the SCS short-form (Raes et al., 2011). While this focus enhanced homogeneity in the predictor variables, it also means that our findings may or may not generalize to studies using different measurement approaches (e.g., in which self-compassion was examined via compassionate self-responding and uncompassionate self-responding; Muris & Otgaar, 2020). While plurality in theory and measurement is critical to the development of self-compassion research, the mediational literature based on more recent approaches was insufficiently developed to permit synthesis and would have required deviation from the pre-registered criteria. However, detailed discussions of the ongoing self-compassion measurement and conceptualization debate can be found in Ferrari et al. (2022), Khoury (2019), Muris and Otgaar (2020), and Neff (2022).
Additionally, alternative conceptualizations, influenced by particular theoretical traditions and other views, such as Gilbert (2014) model based on mammalian caring systems, may be of benefit in future studies (Kirby, 2017). Thus, future studies might also benefit from measuring self-compassion from a broader range of perspectives (Gilbert, 2014) notably those emphasizing biosocial goals/motives and physiology (Kirby, 2017), and the evolved physiological systems for caring (e.g., oxytocin, the myelinated parasympathetic system, vagal tone, and heart rate; Kirby et al., 2017).
Overall, this is the first systematic review to characterize the range and summarize the mediators that have been empirically assessed in linking self-compassion and physical health. Notably, both study methodology and mediation quality need to be improved in future mediation studies. A range of mediators broadly reflective of psychological (emotional and affective, and social-cognitive processes) and behavioral factors have been tested. Among the more commonly assessed mediators, negative affect, and stress (when not concurrently modelled with overlapping affective mediators such as anxiety) consistently mediated links between self-compassion and physical health outcomes but findings regarding emotion regulation were mixed. More generally, although physical health outcomes differ from mental health outcomes in important ways, the current mediators evaluated similar prospective mediators observed in mental health research.
There is a notable absence of studies testing behavioral, motivational, and social pathways or testing measures reflective of different conceptualizations of self-compassion. Cross-sectional study designs predominate, creating key limitations; experimental, interventional, and prospective designs are needed, as are studies with pre-registered analytic plans. Despite such limitations, self-compassion remains a promising target for interventional work in physical health. Ongoing attention to mediational considerations will benefit and facilitate our theoretical understanding of the construct as well as self-compassion interventions and treatments that can optimize physical health and well-being.
References
All references marked with an * are included in the review.
Adams, C. E., & Leary, M. R. (2007). Promoting self-compassionate attitudes toward eating among restrictive and guilty eaters. Journal of Social and Clinical Psychology, 26(10), 1120–1144. https://doi.org/10.1521/jscp.2007.26.10.1120
Ajzen, I. (1991). The theory of planned behavior. Organizational Behavior and Human Decision Processes, 50(2), 179–211. https://doi.org/10.1016/0749-5978(91)90020-T
Arch, J. J., Brown, K. W., Dean, D. J., Landy, L. N., Brown, K. D., & Laudenslager, M. L. (2014). Self-compassion training modulates alpha-amylase, heart rate variability, and subjective responses to social evaluative threat in women. Psychoneuroendocrinology, 42, 49–58. https://doi.org/10.1016/j.psyneuen.2013.12.018
Arimitsu, K., & Hofmann, S. G. (2015). Cognitions as mediators in the relationship between self-compassion and affect. Personality & Individual Differences, 74, 41–48. https://doi.org/10.1016/j.paid.2014.10.008
Bardeen, J. R., Fergus, T. A., & Orcutt, H. K. (2012). An examination of the latent structure of the Difficulties in Emotion Regulation Scale. Journal of Psychopathology and Behavioral Assessment, 34(3), 382–392. https://doi.org/10.1007/s10862-012-9280-y
Baron, R. M., & Kenny, D. A. (1986). The moderator–mediator variable distinction in social psychological research: Conceptual, strategic, and statistical considerations. Journal of Personality Social Psychology, 51(6), 1173. https://doi.org/10.1037//0022-3514.51.6.1173
Basharpoor, S., Mowlaie, M., & Sarafrazi, L. (2021). The relationships of distress tolerance, self-compassion to posttraumatic growth, the mediating role of cognitive fusion. Journal of Aggression, Maltreatment & Trauma, 30(1), 70–81. https://doi.org/10.1080/10926771.2019.1711279
Bastien, C. H., Vallières, A., & Morin, C. M. (2001). Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Medicine, 2(4), 297–307. https://doi.org/10.1016/S1389-9457(00)00065-4
Baumeister, R. F., Schmeichel, B. J., & Vohs, K. D. (2007). Self-regulation and the executive function: The self as controlling agent. In A. W. Kruglanski & E. T. Higgins (Eds.), Social psychology: Handbook of basic principles (2nd ed., pp. 516–539). Guilford Press.
Baumeister, R. F., & Heatherton, T. F. (1996). Self-regulation failure: An overview. Psychological Inquiry, 7(1), 1–15. https://doi.org/10.1207/s15327965pli0701_1
Blackwell, E., & Conrod, P. J. (2003). A five-dimensional measure of drinking motives [Unpublished manuscript]. Department of Psychology, University of British Columbia.
Booker, J. A., & Dunsmore, J. C. (2019). Testing direct and indirect ties of self-compassion with subjective well-being. Journal of Happiness Studies: An Interdisciplinary Forum on Subjective Well-Being, 20(5), 1563–1585. https://doi.org/10.1007/s10902-018-0011-2
Bramer, W. M., de Jonge, G. B., Rethlefsen, M. L., Mast, F., & Kleijnen, J. (2018). A systematic approach to searching: An efficient and complete method to develop literature searches. Journal of the Medical Library Association, 106(4), 531. https://doi.org/10.5195/jmla.2018.283
Breines, J., Toole, A., Tu, C., & Chen, S. (2014). Self-compassion, body image, and self-reported disordered eating. Self and Identity, 13(4), 432–448. https://doi.org/10.1080/15298868.2013.838992
Brown, L., Houston, E. E., Amonoo, H. L., & Bryant, C. (2020). Is self-compassion associated with sleep quality? A meta-analysis.Mindfulness, 82–91.https://doi.org/10.1007/s12671-020-01498-0
*Butz, S., & Stahlberg, D. (2018). Can self-compassion improve sleep quality via reduced rumination? Self and Identity, 17(6), 666–686.https://doi.org/10.1080/15298868.2018.1456482
Buysse, D. J., Reynolds, C. F., III., Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Research, 28(2), 193–213. https://doi.org/10.1016/0165-1781(89)90047-4
Casati, J., Toner, B. B., De Rooy, E. C., Drossman, D. A., & Maunder, R. G. (2000). Concerns of patients with inflammatory bowel disease. Digestive Diseases and Sciences, 45(1), 26–31. https://doi.org/10.1111/j.1572-0241.2001.03877.x
Cerin, E., Barnett, A., & Baranowski, T. (2009). Testing theories of dietary behavior change in youth using the mediating variable model with intervention programs. Journal of Nutrition Education Behavior, 41(5), 309–318. https://doi.org/10.1016/j.jneb.2009.03.129
Chishima, Y., Mizuno, M., Sugawara, D., & Miyagawa, Y. (2018). The influence of self-compassion on cognitive appraisals and coping with stressful events. Mindfulness, 9(6), 1907–1915. https://doi.org/10.1007/s12671-018-0933-0
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). Perceived stress scale (PSS). Journal of Health and Social Behavior, 24, 285. https://doi.org/10.1037/t02889-000
Downs, S. H., & Black, N. (1998). The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. Journal of Epidemiology & Community Health, 52(6), 377–384. https://doi.org/10.1136/jech.52.6.377
*Dunne, S., Sheffield, D., & Chilcot, J. (2018). Brief report: Self-compassion, physical health and the mediating role of health-promoting behaviours. Journal of Health Psychology, 23(7), 993–999. https://doi.org/10.1177/1359105316643377
Ferrari, M., Hunt, C., Harrysunker, A., Abbott, M. J., Beath, A. P., & Einstein, D. A. (2019). Self-compassion interventions and psychosocial outcomes: A meta-analysis of RCTs. Mindfulness, 10(8), 1455–1473. https://doi.org/10.1007/s12671-019-01134-6
Ferrari, M., Ciarrochi, J., Yap, K., Sahdra, B., Hayes, S. C. (2022). Embracing the complexity of our inner worlds: Understanding the dynamics of self-compassion and self-criticism. Mindfulness. https://doi.org/10.1007/s12671-022-01897-5
*Finlay-Jones, A. L., Rees, C. S., & Kane, R. T. (2015). Self-compassion, emotion regulation and stress among australian psychologists: Testing an emotion regulation model of self-compassion using structural equation modeling. PLoS ONE, 10 (7) e133481. https://doi.org/10.1371/journal.pone.0133481
Fresnics, A., & Borders, A. (2017). Angry rumination mediates the unique associations between self-compassion and anger and aggression. Mindfulness, 8(3), 554–564. https://doi.org/10.1007/s12671-016-0629-2
Fresnics, A. A., Wang, S. B., & Borders, A. (2019). The unique associations between self-compassion and eating disorder psychopathology and the mediating role of rumination. Psychiatry Research, 274, 91–97. https://doi.org/10.1016/j.psychres.2019.02.019
Fritz, M. S., & MacKinnon, D. P. (2007). Required sample size to detect the mediated effect. Psychological Science, 18(3), 233–239. https://doi.org/10.1111/j.1467-9280.2007.01882.x
Garnefski, N., Kraaij, V., & Spinhoven, P. (2001). Negative life events, cognitive emotion regulation and emotional problems. Personality and Individual Differences, 30(8), 1311–1327. https://doi.org/10.1016/S0191-8869(00)00113-6
Gedik, Z. (2019). Self-compassion and health-promoting lifestyle behaviors in college students. Psychology, Health & Medicine, 24(1), 108–114. https://doi.org/10.1080/13548506.2018.1503692
Gilbert, P. (2014). The origins and nature of compassion focused therapy. British Journal of Clinical Psychology, 53(1), 6–41. https://doi.org/10.1111/bjc.12043
Gilbert, P., McEwan, K., Catarino, F., & Baião, R. (2014). Fears of compassion in a depressed population: Implication for psychotherapy. Journal of Depression and Anxiety. https://doi.org/10.4172/2167-1044.S2-003
Gratz, K. L., & Roemer, L. (2004). Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment, 26(1), 41–54. https://doi.org/10.1023/B:JOBA.0000007455.08539.94
Gross, J. J., & John, O. P. (2003). Individual differences in two emotion regulation processes: Implications for affect, relationships, and well-being. Journal of Personality and Social Psychology, 85(2), 348. https://doi.org/10.1037/0022-3514.85.2.348
Hall, C. W., Row, K. A., Wuensch, K. L., & Godley, K. R. (2013). The role of self-compassion in physical and psychological well-being. Journal of Psychology: Interdisciplinary and Applied, 147(4), 311–323. https://doi.org/10.1080/00223980.2012.693138
Hallion, L. S., Steinman, S. A., Tolin, D. F., & Diefenbach, G. J. (2018). Psychometric properties of the Difficulties in Emotion Regulation Scale (DERS) and its short forms in adults with emotional disorders. Frontiers in Psychology, 9, 539. https://doi.org/10.3389/fpsyg.2018.00539
Hamrick, L. A., & Owens, G. P. (2019). Exploring the mediating role of self-blame and coping in the relationships between self-compassion and distress in females following the sexual assault. Journal of Clinical Psychology, 75(4), 766–779. https://doi.org/10.1002/jclp.22730
Hayes, A. F., & Rockwood, N. J. (2017). Regression-based statistical mediation and moderation analysis in clinical research: Observations, recommendations, and implementation. Behaviour Research Therapy, 98, 39–57. https://doi.org/10.1016/j.brat.2016.11.001
Hayes, A., F. (2013). Introduction to mediation, moderation, and conditional process analysis: A regression-based approach. Guilford Press.
Hays, R. D., & Morales, L. S. (2001). The RAND-36 measure of health-related quality of life. Annals of Medicine, 33(5), 350–357. https://doi.org/10.3109/07853890109002089
Hodgetts, J., McLaren, S., Bice, B., & Trezise, A. (2021). The relationships between self compassion, rumination, and depressive symptoms among older adults: the moderating role of gender. Aging & Mental Health, 25(12), 2337–2346. https://doi.org/10.1080/13607863.2020.1824207
Hofstede, G., Hofstede, G. J., & Minkov, M. (2005). Cultures and organizations: Software of the mind (Vol. 2). New York: Mcgraw-hill.
*Homan, K. J., & Sirois, F. M. (2017). Self-compassion and physical health: Exploring the roles of perceived stress and health-promoting behaviors. Health Psychology Open, 4(2), 2055102917729542. https://doi.org/10.1177/2055102917729542
*Hu, Y., Wang, Y., Sun, Y., Arteta-Garcia, J., & Purol, S. (2018). Diary study: The protective role of self-compassion on stress-related poor sleep quality. Mindfulness, 9(6), 1931–1940. https://doi.org/10.1007/s12671-018-0939-7
*Hwang, Y.-S., Medvedev, O. N., Krageloh, C., Hand, K., Noh, J.-E., & Singh, N. N. (2019). The role of dispositional mindfulness and self-compassion in educator stress. Mindfulness, 10(8), 1692–1702. https://doi.org/10.1007/s12671-019-01183-x
Inwood, E., & Ferrari, M. (2018). Mechanisms of change in the relationship between self-compassion, emotion regulation, and mental health: A systematic review. Applied Psychology Health Well Being, 10(2), 215–235. https://doi.org/10.1111/aphw.12127
Irving, D. B., Cook, J. L., & Menz, H. B. (2006). Factors associated with chronic plantar heel pain: A systematic review. Journal of Science and Medicine in Sport, 9(1–2), 11–22. https://doi.org/10.1016/j.jsams.2006.02.004
Jenkins, C. D., Stanton, B.-A., Niemcryk, S. J., & Rose, R. M. (1988). A scale for the estimation of sleep problems in clinical research. Journal of Clinical Epidemiology, 41(4), 313–321. https://doi.org/10.1016/0895-4356(88)90138-2
Johnson, E. A., & O’Brien, K. A. (2013). Self-compassion soothes the savage ego-threat system: Effects on negative affect, shame, rumination, and depressive symptoms. Journal of Social and Clinical Psychology, 32(9), 939–963. https://doi.org/10.1521/jscp.2013.32.9.939
Jones, D. R., Graham-Engeland, J. E., Smyth, J. M., & Lehman, B. J. (2018). Clarifying the associations between mindfulness meditation and emotion: Daily high-and low-arousal emotions and emotional variability. Applied Psychology: Health and Well-Being, 10(3), 504–523. https://doi.org/10.1111/aphw.12135
Kelliher Rabon, J., Sirois, F. M., & Hirsch, J. K. (2018). Self-compassion and suicidal behavior in college students: Serial indirect effects via depression and wellness behaviors. Journal of American College Health, 66(2), 114–122. https://doi.org/10.1080/07448481.2017.1382498
Khoury, B. (2019). Compassion: Embodied and embedded. Mindfulness, 10(11), 2363–2374. https://doi.org/10.1007/s12671-019-01211-w
Kirby, J. (2017). Compassion interventions: The programmes, the evidence, and implications for research and practice. Psychology and Psychotherapy, 90(3), 432–455. https://doi.org/10.1111/papt.12104
Kirby, J. N., Tellegen, C. L., & Steindl, S. R. (2017). A meta-analysis of compassion-based interventions: Current state of knowledge and future directions. Behavior Therapy, 48(6), 778–792. https://doi.org/10.1016/j.beth.2017.06.003
Koopmann-Holm, B., Tsai, J. L. (2017). The cultural shaping of compassion. In E. M. Seppälä, E. Simon-Thomas, S. L. Brown, M. C. Worline, C. D. Cameron, & J. R. Doty (Eds.), Oxford handbook of compassion science (pp. 273–285). Oxford University Press.
Kraemer, H. C., Wilson, G. T., Fairburn, C. G., & Agras, W. S. (2002). Mediators and moderators of treatment effects in randomized clinical trials. Archives of General Psychiatry, 59(10), 877–883. https://doi.org/10.1001/archpsyc.59.10.877
Kroese, F. M., De Ridder, D. T., Evers, C., & Adriaanse, M. A. (2014). Bedtime procrastination: Introducing a new area of procrastination. Frontiers in Psychology, 5, 611. https://doi.org/10.3389/fpsyg.2014.00611
Lazarus, R. S. (1966). Psychological stress and the coping process. McGraw-Hill.
Leung, D. Y., Lam, T.-H., & Chan, S. S. (2010). Three versions of Perceived Stress Scale: Validation in a sample of Chinese cardiac patients who smoke. BMC Public Health, 10(1), 1–7. https://doi.org/10.1186/1471-2458-10-513
Li, A., Wang, S., Cai, M., Sun, R., & Liu, X. (2021). Self-compassion and life-satisfaction among Chinese self-quarantined residents during COVID-19 pandemic: A moderated mediation model of positive coping and gender. Personality & Individual Differences, 170, 110457. https://doi.org/10.1016/j.paid.2020.110457
*Li, Y., Deng, J., Lou, X., Wang, H., & Wang, Y. (2020). A daily diary study of the relationships among daily self-compassion, perceived stress and health-promoting behaviours. International Journal of Psychology, 55(3), 364–372. https://doi.org/10.1002/ijop.12610
Liberati, A., Altman, D. G., Tetzlaff, J., Mulrow, C., Gøtzsche, P. C., Ioannidis, J. P., . . . Moher, D. (2009). The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Journal of Clinical Epidemiology, 62(10), e1–e34. https://doi.org/10.1136/bmj.b2700
Lovibond, P. F., & Lovibond, S. H. (1995). The structure of negative emotional states: Comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behaviour Research and Therapy, 33(3), 335–343. https://doi.org/10.1016/0005-7967(94)00075-U
Lubans, D. R., Foster, C., & Biddle, S. J. (2008). A review of mediators of behavior in interventions to promote physical activity among children and adolescents. Preventive Medicine, 47(5), 463–470. https://doi.org/10.1016/j.ypmed.2008.07.011
Luo, Y., Meng, R., Li, J., Liu, B., Cao, X., & Ge, W. (2019). Self-compassion may reduce anxiety and depression in nursing students: A pathway through perceived stress. Public Health, 174, 1–10. https://doi.org/10.1016/j.puhe.2019.05.015
MacBeth, A., & Gumley, A. (2012). Exploring compassion: A meta-analysis of the association between self-compassion and psychopathology. Clinical Psychology Review, 32(6), 545–552. https://doi.org/10.1016/j.cpr.2012.06.003
MacKinnon, D. P., Lockwood, C. M., Hoffman, J. M., West, S. G., & Sheets, V. (2002). A comparison of methods to test mediation and other intervening variable effects. Psychological Methods, 7(1), 83. https://doi.org/10.1037/1082-989x.7.1.83
Magnus, C. M., Kowalski, K. C., & McHugh, T.-L.F. (2010). The role of self-compassion in women’s self-determined motives to exercise and exercise-related outcomes. Self and Identity, 9(4), 363–382. https://doi.org/10.1080/15298860903135073
Malik, S., Wells, A., & Wittkowski, A. (2015). Emotion regulation as a mediator in the relationship between attachment and depressive symptomatology: A systematic review. Journal of Affective Disorders, 172, 428–444. https://doi.org/10.1016/j.jad.2014.10.007
Marschall, D., Sanftner, J., & Tangney, J. P. (1994). The state shame and guilt scale [Unpublished work]. VA, George Mason University.
Marsh, I. C., Chan, S. W., & MacBeth, A. (2018). Self-compassion and psychological distress in adolescents—A meta-analysis. Mindfulness, 9(4), 1011–1027. https://doi.org/10.1007/s12671-017-0850-7
Mascaro, J. S., Florian, M. P., Ash, M. J., Palmer, P. K., Frazier, T., Condon, P., & Raison, C. (2020). Ways of knowing compassion: How do we come to know, understand, and measure compassion when we see it? Frontiers in Psychology, 11, 2467. https://doi.org/10.3389/fpsyg.2020.547241
Mastin, D. F., Bryson, J., & Corwyn, R. (2006). Assessment of sleep hygiene using the Sleep Hygiene Index. Journal of Behavioral Medicine, 29(3), 223–227. https://doi.org/10.1007/s10865-006-9047-6
McGehee, P., Germer, C., & Neff, K. (2017). Core values in mindful self-compassion. In L. Monteiro, J. Compson, & F. Musten (Eds.), Practitioner’s guide to ethics and mindfulness-based interventions (pp. 279–293). Springer.
Meyer, L. P., & Leppma, M. (2019). The role of mindfulness, self-compassion, and emotion regulation in eating disorder symptoms among college students. Journal of College Counseling, 22(3), 211–224. https://doi.org/10.1002/jocc.12138
*Miller, C. L., & Strachan, S. M. (2020). Understanding the role of mother guilt and self-compassion in health behaviors in mothers with young children. Women & Health, 60(7), 763–775. https://doi.org/10.1080/03630242.2020.1713966
Montero-Marin, J., Kuyken, W., Crane, C., Gu, J., Baer, R., Al-Awamleh, A. A., . . . Garcia-Campayo, J. (2018). Self-compassion and cultural values: A cross-cultural study of self-compassion using a multitrait-multimethod (MTMM) analytical procedure. Frontiers in Psychology, 9, 2638. https://doi.org/10.3389/fpsyg.2018.02638
Munn, J., Sullivan, S. J., & Schneiders, A. G. (2010). Evidence of sensorimotor deficits in functional ankle instability: A systematic review with meta-analysis. Journal of Science Medicine in Sport, 13(1), 2–12. https://doi.org/10.1016/j.jsams.2009.03.004
Muris, P., & Otgaar, H. (2020). The process of science: A critical evaluation of more than 15 years of research on self-compassion with the Self-Compassion Scale. Mindfulness, 11(6), 1469–1482. https://doi.org/10.1007/s12671-020-01363-0
Nabi, H., Kivimaki, M., De Vogli, R., Marmot, M. G., & Singh-Manoux, A. (2008). Positive and negative affect and risk of coronary heart disease: Whitehall II prospective cohort study. British Medical Journal, 337, 32–36. https://doi.org/10.1136/bmj.a118
Neff, K. (2003). The development and validation of a scale to measure self-compassion. Self and Identity, 2(3), 223–250. https://doi.org/10.1080/15298860309027
Neff, K. D. (2016). The Self-Compassion Scale is a valid and theoretically coherent measure of self-compassion. Mindfulness, 7(4), 1009–1009. https://doi.org/10.1007/s12671-016-0560-6
Neff, K. D. (2022). The differential effects fallacy in the study of self-compassion: Misunderstanding the nature of bipolar continuums. Mindfulness, 13(3), 572–576. https://doi.org/10.1007/s12671-022-01832-8
Nguyen, T. M., Bui, T. T. H., Xiao, X., & Le, V. H. (2020). The influence of self-compassion on mindful parenting: A mediation model of gratitude. The Family Journal, 28(4), 455–462. https://doi.org/10.1177/1066480720950421
Nolen-Hoeksema, S., & Morrow, J. (1991). A prospective study of depression and posttraumatic stress symptoms after a natural disaster: The 1989 Loma Prieta Earthquake. Journal of Personality and Social Psychology, 61(1), 115. https://doi.org/10.1037/0022-3514.61.1.115
Phillips, W. J., & Hine, D. W. (2019). Self-compassion, physical health, and health behaviour: A meta-analysis. Health Psychology Review, 15(1), 113–139. https://doi.org/10.1080/17437199.2019.1705872
Podsakoff, P. M., MacKenzie, S. B., & Podsakoff, N. P. (2012). Sources of method bias in social science research and recommendations on how to control it. Annual Review of Psychology, 63, 539–569. https://doi.org/10.1146/annurev-psych-120710-100452
Preacher, K. J., & Hayes, A. F. (2004). SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behavior Research Methods, Instruments, Computers, 36(4), 717–731. https://doi.org/10.3758/BF03206553
Preacher, K. J., & Hayes, A. F. (2008). Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behavior Research Methods, 40(3), 879–891. https://doi.org/10.3758/BRM.40.3.879
Raes, F. (2010). Rumination and worry as mediators of the relationship between self-compassion and depression and anxiety. Personality and Individual Differences, 48(6), 757–761. https://doi.org/10.1016/j.paid.2010.01.023
Raes, F., Pommier, E., Neff, K. D., & Van Gucht, D. (2011). Construction and factorial validation of a short form of the Self-Compassion Scale. Clinical Psychology & Psychotherapy, 18(3), 250–255. https://doi.org/10.1002/cpp.702
*Rakhimov, A., Ong, J., Realo, A., & Tang, N. K. (2022). Being kind to self is being kind to sleep? A structural equation modelling approach evaluating the direct and indirect associations of self-compassion with sleep quality, emotional distress and mental well-being.Current Psychology, 1–14. https://doi.org/10.1007/s12144-021-02661-z
Raque-Bogdan, T. L., Ericson, S. K., Jackson, J., Martin, H. M., & Bryan, N. A. (2011). Attachment and mental and physical health: Self-compassion and mattering as mediators. Journal of Counseling Psychology, 58(2), 272. https://doi.org/10.1037/a0023041
Read, J. P., Kahler, C. W., Strong, D. R., & Colder, C. R. (2006). Development and preliminary validation of the young adult alcohol consequences questionnaire. Journal of Studies on Alcohol, 67(1), 169–177. https://doi.org/10.15288/jsa.2006.67.169
Rethlefsen, M. L., Kirtley, S., Waffenschmidt, S., Ayala, A. P., Moher, D., Page, M. J., & Koffel, J. B. (2021). PRISMA-S: An extension to the PRISMA statement for reporting literature searches in systematic reviews. Systematic Reviews, 10(1), 1–19. https://doi.org/10.1186/s13643-020-01542-z
Rhodes, R. E., & Pfaeffli, L. A. (2010). Mediators of physical activity behaviour change among adult non-clinical populations: A review update. International Journal of Behavioral Nutrition and Physical Activity, 7(1), 1–11. https://doi.org/10.1186/1479-5868-7-37
Rucker, D. D., Preacher, K. J., Tormala, Z. L., & Petty, R. E. (2011). Mediation analysis in social psychology: Current practices and new recommendations. Social Personality Psychology Compass, 5(6), 359–371. https://doi.org/10.1111/j.1751-9004.2011.00355.x
Schmidt, C. K., Raque-Bogdan, T. L., & Hollern, E. A. (2019). Self-compassion, affect, and body image in college women. Journal of College Counseling, 22(2), 152–163. https://doi.org/10.1002/jocc.12127
Schoenefeld, S. J., & Webb, J. B. (2013). Self-compassion and intuitive eating in college women: Examining the contributions of distress tolerance and body image acceptance and action. Eating Behaviors, 14(4), 493–496. https://doi.org/10.1016/j.eatbeh.2013.09.001
*Semenchuk, B. N., Onchulenko, S., & Strachan, S. M. (2021). Self-compassion and sleep quality: Examining the mediating role of taking a proactive health focus and cognitive emotional regulation strategies. Journal of Health Psychology, 13591053211047148. https://doi.org/10.1177/13591053211047148
Simons, J., Correia, C. J., Carey, K. B., & Borsari, B. E. (1998). Validating a five-factor marijuana motives measure: Relations with use, problems, and alcohol motives. Journal of Counseling Psychology, 45(3), 265. https://doi.org/10.1037/0022-0167.45.3.265
Simons, J. S., Dvorak, R. D., Merrill, J. E., & Read, J. P. (2012). Dimensions and severity of marijuana consequences: Development and validation of the Marijuana Consequences Questionnaire (MACQ). Addictive Behaviors, 37(5), 613–621. https://doi.org/10.1016/j.addbeh.2012.01.008
*Sirois, F. M. (2015). A self-regulation resource model of self-compassion and health behavior intentions in emerging adults. Preventive Medicine Reports, 2, 218–222. https://doi.org/10.1016/j.pmedr.2015.03.006
Sirois, F. M., & Hirsch, J. K. (2019). Self-compassion and adherence in five medical samples: The role of stress. Mindfulness, 10(1), 46–54. https://doi.org/10.1007/s12671-018-0945-9
Sirois, F. M., Kitner, R., & Hirsch, J. K. (2015). Self-compassion, affect, and health-promoting behaviors. Health Psychology, 34(6), 661–669. https://doi.org/10.1037/hea0000158
*Sirois, F. M., Nauts, S., & Molnar, D. S. (2019). Self-compassion and bedtime procrastination: An emotion regulation perspective. Mindfulness, 10(3), 434–445. https://doi.org/10.1007/s12671-018-0983-3
Sirois, F. (2001). The Wellness Behaviors Inventory [Unpublished manual]. Carleton University.
Sirois, F. (2002). The Control Beliefs Inventory [Unpublished manual]. Carleton University.
Sobel, M. E. (1982). Asymptotic confidence intervals for indirect effects in structural equation models. Sociological Methodology, 13, 290–312. https://doi.org/10.2307/270723
Stamm, B. H. (2009). Professional quality of life measure: Compassion, satisfaction, and fatigue version V (ProQOL). https://proqol.org/ProQol_Test.html
Stowell, J. R., Hedges, D. W., Ghambaryan, A., Key, C., & Bloch, G. J. (2009). Validation of the symptoms of illness checklist (SIC) as a tool for health psychology research. Journal of Health Psychology, 14(1), 68–77. https://doi.org/10.1177/1359105308097947
Surtees, P., Wainwright, N., Luben, R., Wareham, N., Bingham, S., & Khaw, K.-T. (2008). Psychological distress, major depressive disorder, and risk of stroke. Neurology, 70(10), 788–794. https://doi.org/10.1212/01.wnl.0000304109.18563.81
Tandler, N., Kruger, M., & Petersen, L.-E. (2020). Better battles by a self-compassionate partner? The mediating role of personal conflict resolution styles in the association between self-compassion and satisfaction in romantic relationships. Journal of Individual Differences. https://doi.org/10.1027/1614-0001/a000333
Tang, N. K., & Harvey, A. G. (2004). Correcting distorted perception of sleep in insomnia: A novel behavioural experiment? Behaviour Research and Therapy, 42(1), 27–39. https://doi.org/10.1016/S0005-7967(03)00068-8
Terry, M. L., & Leary, M. R. (2011). Self-compassion, self-regulation, and health. Self and Identity, 10(3), 352–362. https://doi.org/10.1080/15298868.2011.558404
Terry, M. L., Leary, M. R., Mehta, S., & Henderson, K. (2013). Self-compassionate reactions to health threats. Personality and Social Psychology Bulletin, 39(7), 911–926. https://doi.org/10.1177/0146167213488213
Treynor, W., Gonzalez, R., & Nolen-Hoeksema, S. (2003). Rumination reconsidered: A psychometric analysis. Cognitive Therapy and Research, 27(3), 247–259. https://doi.org/10.1023/A:1023910315561
*Vaillancourt, E. S., & Wasylkiw, L. (2019). The intermediary role of burnout in the relationship between self-compassion and job satisfaction among nurses. The Canadian journal of nursing research = Revue canadienne de recherche en sciences infirmieres. https://doi.org/10.1177/0844562119846274
Valente, M. J., Pelham, W. E., III., Smyth, H., & MacKinnon, D. P. (2017). Confounding in statistical mediation analysis: What it is and how to address it. Journal of Counseling Psychology, 64(6), 659. https://doi.org/10.1037/cou0000242
VanderWeele, T. J. (2019). Principles of confounder selection. European Journal of Epidemiology, 34(3), 211–219. https://doi.org/10.1007/s10654-019-00494-6
Walker, S. N., Sechrist, K. R., & Pender, N. J. (1995). Health promotion model-instruments to measure health promoting lifestyle: Health-promoting lifestyle profile [HPLP II](Adult version). https://deepblue.lib.umich.edu/bitstream/handle/2027.42/85349/HPLP_II-background_and_permission.pdf?sequence=1&isallowed=y
Wang, S. S., Lay, S., Yu, H. N., & Shen, S. R. (2016). Dietary guidelines for Chinese residents (2016): Comments and comparisons. Journal of Zhejiang University-SCIENCE B, 17(9), 649–656. https://doi.org/10.1631/jzus.B1600341
Watson, D., Clark, L. A., & Tellegen, A. (1988). Development and validation of brief measures of positive and negative affect: The PANAS scales. Journal of Personality and Social Psychology, 54(6), 1063. https://doi.org/10.1037//0022-3514.54.6.1063
Watson, D., & Clark, L. A. (1999). The PANAS-X: Manual for the positive and negative affect schedule-expanded form [Unpublished manuscript]. University of Iowa.
Wilson, A. C., Mackintosh, K., Power, K., & Chan, S. W. (2019). Effectiveness of self-compassion related therapies: A systematic review and meta-analysis. Mindfulness, 10(6), 979–995. https://doi.org/10.1007/s12671-018-1037-6
*Wisener, M., & Khoury, B. (2020). Is self-compassion negatively associated with alcohol and marijuana-related problems via coping motives? Addictive Behaviors, 111(106554). https://doi.org/10.1016/j.addbeh.2020.106554
*Wisener, M., & Khoury, B. (2021). Specific emotion-regulation processes explain the relationship between mindfulness and self-compassion with coping-motivated alcohol and marijuana use. Addictive Behaviors, 112(106590). https://doi.org/10.1016/j.addbeh.2020.106590
Zessin, U., Dickhäuser, O., & Garbade, S. (2015). The relationship between self-compassion and well-being: A meta-analysis. Applied Psychology: Health and Well-Being, 7(3), 340–364. https://doi.org/10.1111/aphw.12051
Acknowledgements
Many thanks to Anne Wilson, the Subject Librarian, for her assistance in formulating search terms and strategies.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Contributions
JC came up with the conception and structure of the review, conducted the search and study quality assessment, wrote the manuscript, and contributed to all manuscript revisions. AB collaborated in conducting the search and study quality assessment. AS, AC, and JK assisted in reviewing various parts of the manuscript. NC collaborated in conceptualizing and structuring the review, writing the manuscript, and contributed to all manuscript revisions. All authors collaborated in reviewing and editing the final manuscript and approved it for submission.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cha, J.E., Boggiss, A.L., Serlachius, A.S. et al. A Systematic Review on Mediation Studies of Self-Compassion and Physical Health Outcomes in Non-Clinical Adult Populations. Mindfulness 13, 1876–1900 (2022). https://doi.org/10.1007/s12671-022-01935-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-022-01935-2