Abstract
Paraquat (PQ), a widely characterized neurotoxicant, has been generally accepted as one of the environmental factors in the etiology of Parkinson’s disease (PD). Despite the direct evidence that PQ could induce inflammatory responses in central nervous system, the putative adverse effects of PQ on the neuroimmune interactions have rarely been investigated. High-mobility group box 1 (HMGB1) has been proven to be relevant to the neuroinflammation involved in PD; however, whether and how HMGB1 exerts modulatory effects in nervous system upon PQ exposure remain elusive. Therefore, the present study investigated the underlying association between HMGB1 and PQ exposure in SH-SY5Y cells, which is a well-established in vitro model for PD research. We observed that HMGB1 was markedly increased in a concentration and time-dependent manner upon PQ exposure, and the elevated HMGB1 could be translocated into cytosol and then released to the extracellular milieu of SH-SY5Y cells. Knockdown of HMGB1 inhibited the activation of RAGE-P38-NF-κB signaling pathway and the expression of inflammation cytokines such as TNF-α and IL-6. These results suggested that HMGB1 is involved in the PQ-induced neuron death via activating RAGE signaling pathways and promoting neuroinflammatory responses.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a typical progressive neurodegenerative disorder characterized by selective loss of dopaminergic neurons (Bertram and Tanzi 2005; Brichta and Greengard 2014; Mamelak 2018). Except for familial inheritance, genetic susceptibility, aging, and environmental chemical exposure have been reported to be involved in the multifactorial pathogenesis of PD (Ball et al. 2019; Chen and Ritz 2018). Paraquat (1, 1′-dimethyl-4, 4′-bipyridinium, PQ) is a widely used nonselective herbicide; its neurotoxicity associated with PD has been generally accepted (Lou et al. 2016; Tanner et al. 2011). Despite most of the current mechanisms underlying PQ-induced PD were mainly focused on oxidative stress, mitochondrial dysfunction, as well as α-synuclein aggregation (Brichta and Greengard 2014; Chang et al. 2013; Lou et al. 2012), mounting interests in studying neuroimmune interactions considered neuroinflammation as a crucial mediator in understanding the pathogenesis of PD (Barcia 2013). However, the adverse effects of PQ on the neuroimmune interactions and how they contribute to PD pathogenesis have rarely been reported yet.
High-mobility group box 1 (HMGB1) is a highly conserved nonhistone DNA-binding protein and serves as a structural component to facilitate the assembly of nucleoprotein complexes (Sims et al. 2010). HMGB1 could be actively secreted from inflammatory cells or passively released from apoptotic or necrotic cells and function as a cytokine to initiate inflammatory responses (Bell et al. 2006). This mechanism might be particularly relevant to PD as increased levels of HMGB1 were detected in human postmortem substantia nigra specimens as well as in the cerebrospinal fluid and serum of PD patients (Santoro et al. 2016).
Both in vitro and in vivo evidence showed that HMGB1 are affected by those neurotoxins that could induce PD. HMGB1 expression level was found to be altered by pesticide rotenone and could interact with α-synuclein and perturb the autophagy process to induce dopaminergic neuron death (Huang et al. 2017). MPTP, a classical PD-related toxicant, could upregulate HMGB1 mRNA and protein levels in mouse models (Santoro et al. 2016). Furthermore, HMGB1 translocation was observed in dopaminergic neurons in 6-OHDA-treated rat models (Sasaki et al. 2016). Notably, systemic administration of neutralizing antibodies to HMGB1 could relieve dopaminergic neuron death in PD models via inhibition of microglial activation and subsequent neuroinflammation (Santoro et al. 2016; Sasaki et al. 2016). Previous research also reported that HMGB1 could activate TLR4-IL23-IL17A to promote inflammatory responses in PQ-induced acute lung injury (Yan et al. 2017). All these evidences suggested that HMGB1 might play a vital role in the pathogenesis of PD, and PQ exposure probably induce certain alterations in the concentration or location of HMGB1, thereby contributing to the pathogenesis of PD. Thus in the present study, the human neuroblastoma cells (SH-SY5Y) were applied to understand whether and how HMGB1 was affected upon PQ exposure. We first detected HMGB1 expression after PQ treatment and observed that HMGB1 could translocate into cytosol and then release to extracellular environment. We also found that HMGB1 could activate RAGE signaling pathway to promote the neuroinflammatory responses. Moreover, the interaction between HMGB1 and RAGE signaling pathway was confirmed by knocking down HMGB1 in SH-SY5Y cells with or without PQ exposure. Our results demonstrated that HMGB1 mediates the neuroinflammatory responses via disrupting RAGE signaling pathway in PQ-treated SH-SY5Y cells.
Materials and Methods
Chemicals and Reagents
Paraquat dichloride (molecular weight 257.16 g/mol, analytical standard, PQ) (#36541, Sigma-Aldrich, St. Louis, MO, USA) was purchased from Sigma-Aldrich. Dosing solutions were prepared by dissolving the calculated amount of PQ in cell culture medium, following the approved standard operating procedures for handling toxic agents. All other reagents were obtained from commercial sources and were of the highest available grade.
Cell Culture and Treatments
SH-SY5Y cells were purchased from Chinese Academy of Sciences Cell Bank in Kunming. Frozen cells were thawed and expanded in DMEM/F12 medium (#11320082, Gibco Life Technologies Corporation, Carlsbad, CA, USA) supplemented with 10% fetal bovine serum (FBS) (#04–001-1A, Biological Industries, Israel Beit), 100 units/ml penicillin and100 μg/ml streptomycin (#P1400, Beijing Solarbio Science & Technology Co., Ltd., China), 4.5 g/l glucose, 3.7 g/l NaHCO3, and 4 mM L-glutamine. Cells were incubated in a humidified atmosphere with 5% CO2 at 37 °C and then passaged by 0.25% trypsin (#25200056, Gibco Life Technologies Corporation, Carlsbad, CA, USA) at about 80% confluence.
Cell Viability Measurement by Trypan Bule Staining
Cell viability was first measured with trypan blue (#C0040, Beijing Solarbio Science & Technology Co., Ltd., China) staining. SH-SY5Y cells growing at exponential phase were seeded in 96-well plates with a density of 105 cells/mL. After treated with various dosages of PQ (0, 75, 150, 300, 600 μmol/L) for 24 h or 150 μmol/L PQ for different durations (0, 12, 24, 48, 72, 96 h), cells were harvested and resuspended. By mixing with 0.4% trypan blue solution, viable and dead cells were counted manually using a hematocytometer. Cell survival rate in each treatment group was calculated as a percentage of viable cells. Relative cell viability was obtained as a percentage of the cell survival rate in the control groups.
Cell Viability Measurement by MTT Assay
Cell viability was determined by MTT assay. SH-SY5Y cells growing at exponential phase were seeded in 96-well plates with a density of 105 cells/mL. After treated with various dosages of PQ (0, 75, 150, 300, 600 μmol/L) for 24 h or 150 μmol/L PQ for different durations (0, 12, 24, 48, 72, 96 h), 50 μl MTT solution was added to each well and incubated for another 4 h. Remove the supernatant from each well, add 150 μl DMSO (#D2650, Sigma-Aldrich, St. Louis, MO, USA), and mix well. Absorbance was then detected at 490 nm using a spectrophotometer. Each treatment group has five replicates. Cell viability was obtained as a percentage of the value of survival cells in the control groups.
Measurement of HMGB1 Level in the Cell Culture Medium by ELISA
SH-SY5Y cells were plated in 10 cm dishes at a density of 5x106 cells/mL and treated with different doses of PQ (0, 75, 150, 300 μmol/L) for 24 h or treated with150μmol/L PQ for different durations (0, 12, 24, 36, 48 h). The supernatants were collected and stored at − 80 °C until assay for HMGB1 was performed. HMGB1 levels were determined by human ELISA kits (#SEA399Hu, CLOUD-CLONE CORP., CCC, USA) according to the procedures provided by the manufacturers.
Western Blotting Assay
SH-SY5Y cells with different treatments were washed with ice-cold PBS (#32194, HyClone, USA) and then were incubated with lysis buffer on ice for 10 min. The cell lysates were centrifuged at 12000 x g for 5 min at 4 °C. Protein concentrations were determined by BCA method (#KGPBCA, KeyGEN BioTECH, Nanjing, China). Nuclear and cytoplasmic extracts (#BB31122, Shanghai BestBio Science, China) and whole cell lysis (#KGP2100, KeyGEN BioTECH, Nanjing, China) were separated by sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) and transferred to PVDF membranes. The membranes were probed with HMGB1 (1:1000, #ab79823, Abcam, USA), RAGE (1:500, #16346–1-AP, Wuhan Proteintech, China), p38 MAPK (P38, 1:500, #14064–1-AP, Wuhan Proteintech, China), p-p38 MAPK (p-P38, 1:500, #AF4001, Affinity Biosciences, OH, USA), TNF-α (1:1000, #60291–1-Ig, Wuhan Progeintech, China), IL-6 (1:1000, #21865–1-AP, Wuhan Proteintech, China), NF-κB/p65 (1:1000, #10745–1-AP, Wuhan Progeintech, China), p-ΙκBα (1:1000,, #ab133462, Abcam, MA, USA), ΙκBα (1:1000, #10268–1-AP, Wuhan Proteintech, China), and β-actin (1:10000, #TA-09, Beijing ZSGB-BIO, China) antibodies at 4 °C overnight. After washing with TBST (#P25133, Shanghai Double-helix biotech CO. Ltd., China) for 1 h, membranes were incubated with alkaline phosphatase goat anti-rabbit IgG (1:2000, #ZB-2308, Beijing ZSGB-BIO, China) or peroxidase-conjugated goat anti-mouse IgG (1:2000, #ZB-2305, Beijing ZSGB-BIO, China)and then imaged using New Super ESL Assay (#KGP1128, KeyGEN BioTECH, Nanjing, China) on Thermo Fisher iBright Imaging System. Quantification of the band density was determined by densitometric analysis.
HMGB1 Protein Expression Detected by Immunofluorescence Assay
SH-SY5Y cells were plated in 24-well plates at a density of 5x105 cells/mL and incubated overnight. After treated with 150 μmol/L PQ for different durations (0, 12, 24, 36 h), cells were then fixed with 4% paraformaldehyde (#Top0382, Beijing Biotoppted Science & Technology Co., Ltd., China) for 15 min, blocked with 5% BSA (#A6010, Beijing Biotoppted Science & Technology Co., Ltd., China) for 1 h, incubated with anti-HMGB1 antibody (1:250, #66525–1-Ig, Wuhan Proteintech, China) at 4 °C overnight, and then incubated with rhodamine (TRITC)-conjugated goat anti-mouse IgG (1:50, #SA00007–1, Wuhan Proteintech, China) for 1 h. Finally, cover slips were then incubated with DAPI (#C0065, Beijing Solarbio Science & Technology Co., Ltd., China) for double staining and then mounted on glass slides. The fluorescence intensity was detected by using an inverted fluorescent microscope (IX-81, Olympus).
HMGB1-shRNA Design and Cell Transfection
shRNA targeting HMGB1 mRNA (shHMGB1) (GGACAAGGCCCGTTATGAAAG) or negative control mRNA sequence (shNC) (TTCTCCGAACGTGTCACGT) were designed and synthesized by using pGMLV-SC5 RNAi lentiviral vector. Synthesized oligonucleotides were annealed and ligated to the BamHI/EcoRI sites of pGMLV-eGFP to produce pGMLV-eGFP-shHMGB1 or pGMLV-eGFP-shNC. eGFP expression was used to detect the transfection of lentivirus. SH-SY5Y cells were plated in 6-well plates at a density of 5x104 cells/mL and incubated overnight. The other day, cells were cultured in complete culture medium (control group), complete culture medium containing shHMGB1 diluent (HMGB1 shRNA group), or complete culture medium containing shNC diluent (NC shRNA group), respectively. After transfected for 12 h, the culture medium was replaced with complete culture medium, and cells were incubated for 72 h and screened in media containing 2 mg/l puromycin (#P8230, Beijing Solarbio Science & Technology Co., Ltd., China). Since pGMLV-SC5 RNAi lentiviral vector contains eGFP and anti-puromycin gene, the SH-SY5Y cells transfected with lentiviral vector can be observed with green fluorescent. Cells were harvested to determine the HMGB1 protein level by western blotting assay. After successful transfection, cells in these three groups were further treated with different concentrations of PQ (0, 75, 150, 300 μmol/L) for 24 h.
Statistical Analysis
Data were shown by the means ± SE of at least three independent experiments. Statistical differences between experimental groups were determined by ANOVA followed by Tukey post hoc test. Significance level was set at p < 0.05.
Results
Effects of PQ Exposure on SH-SY5Y Cell Viability
The effects of PQ on the viability of SH-SY5Y cells were determined by both Trypan blue staining and MTT assay. Cell viability upon PQ treatment was expressed as the percentage of viability from control group. There was no significant change in cell survival rate when treated with 75 μmol/L PQ for 24 h. After treated with 150 μmol/L PQ for 24 h, cell viability was significantly reduced (p < 0.05). With the increase of PQ concentration, the reduction of cell viability became more severe, showing a dose-dependent manner (r = −0.909) (Fig. 1A and C).
We further observed the time-course effects of PQ exposure on SH-SY5Y cell viability. Upon treatment with 150 μmol/L PQ for 24 h, cell viability was significantly decreased (p < 0.05). With prolonged exposure, cell viability was dramatically reduced, indicating a time-dependent manner (r = −0.937) (Fig. 1B and D).
Alteration of Extracellular HMGB1 Level in PQ-Treated SH-SY5Y Cells
To investigate the effects of PQ exposure on HMGB1 release in SH-SY5Y cells, we treated cells with different doses of PQ (0, 75, 150, 300 μmol/L) for 24 h and determined the extracellular HMGB1 level in the cell culture supernatants by using ELISA. These results showed that HMGB1 level was significantly increased upon treatment with 150 μmol/L or higher concentration of PQ (Fig. 2), indicating that PQ to some extent stimulates SH-SY5Y cells to release HMGB1 outside the cells.
Alteration of extracellular HMGB1 level in PQ-treated SH-SY5Y cells. SH-SY5Y cells were treated with different doses of PQ (0, 75, 150, 300 μmol/L) for 24 h, and then cell culture supernatants were collected. Levels of HMGB1in cell culture media were determined by ELISA. Data are presented as mean ± SE (n = 5). * p < 0.05, vehicle control versus PQ treatment
Massive HMGB1 Release Following PQ Exposure in SH-SY5Y Cells
To further explore the dynamic impacts of PQ exposure on HMGB1 release in SH-SY5Y cells, we treated cells with 150 μmol/L PQ and determined the HMGB1 levels in different locations at multiple time points (0, 12, 24, 36, 48, 60 h). Specifically, HMGB1 protein levels in nucleus and cytoplasm were detected by both western blotting and ELISA, whereas HMGB1 protein levels in the cell culture media were detected by ELISA.
We observed that HMGB1 protein levels in nucleus first increased and then decreased during the PQ exposure (Fig. 3A and B). HMGB1 accumulated to a high level after 12 h exposure and dramatically decreased afterward. Interestingly, HMGB1 protein levels in cytoplasm also showed a first-increase-then-decrease pattern. However, in cytoplasm, HMGB1 increased to the highest level until 24 h exposure and then start to decrease afterward (Fig. 3C and D). In addition, HMGB1 protein levels in the cell culture supernatants were found to be continuously increased until 48 h exposure (Fig. 3E). These results indicated that HMGB1 was rapidly released from nucleus to cytoplasm and finally accumulated in extracellular culture media after PQ-induced cell impairment.
Massive release of HMGB1 from nucleus to cytoplasm and its accumulation in PQ-treated SH-SY5Y cell culture medium. SH-SY5Y cells were treated with 150 μmol/L PQ and harvested at multiple time points (0, 12, 24, 36, 48, 60 h). Levels of HMGB1 in cell nucleus (A) and cytoplasm (C) were determined by western blotting with anti-HMGB1 at various time points after PQ exposure. Lamin B1 and β-actin were used as the internal control for normalization of nucleus and cytoplasm, respectively. Histogram showed the quantitative evaluation of HMGB1 bands in nucleus (B) and cytoplasm (D) by densitometry. (E) Levels of HMGB1 in nucleus/cytoplasm/cell culture media were determined by ELISA. Data are presented as mean ± SE (n = 5). * p < 0.05, vehicle control versus PQ treatment
Translocation of HMGB1 from SH-SY5Y Nuclei to Cytoplasm Following PQ Exposure
Translocation of HMGB1 from nucleus to cytoplasm and its subsequent extracellular release were further confirmed by using immunofluorescence method. Under normal conditions, HMGB1 was exclusively located in the nuclei of SH-SY5Y cells (Fig. 4A and C). A significant increase of the fluorescence intensity of HMGB1 was observed at 12 h after PQ treatment (Fig. 4D). In the meantime, some HMGB1was also found in the cytoplasm (Fig. 4F), suggesting that PQ induced a massive production of HMGB1 in SH-SY5Y nucleus and some of them start translocating to the cytoplasm.
PQ-induced translocation of HMGB1 from nucleus to cytoplasm in SH-SY5Y cells. SH-SY5Y cells were treated with 150 μmol/L PQ and harvested at multiple time points (0, 12, 24, 36, 48, 60 h). (A–L) HMGB1 localizations in cells were visualized by immunostaining with anti-HMGB1 (red), and nuclei were visualized by staining with DAPI (blue). Scale bar = 100 μm. (M–N) Quantification of the HMGB1 fluorescence intensity in different time points after PQ exposure. Data are presented as mean ± SE (n = 3). * p < 0.05, vehicle control versus PQ treatment
After 24 h of PQ exposure, the fluorescence intensity of HMGB1 in the nuclei is reduced, whereas the fluorescence intensity of HMGB1 in the cytoplasm increased (Fig. 4G and I), indicating that HMGB1 produced in nucleus induced by PQ is continuously translocated to cytoplasm.
After 36 h of PQ exposure, intracellular (either in nuclei or in cytoplasm) HMGB1 immunoreactivity appeared to be much weaker than earlier time points (Fig. 4J and L), suggesting that most of the HMGB1 induced by PQ has been released to the outside of SH-SY5Y cells at this moment.
PQ-Activated RAGE Signaling Pathway in SH-SY5Y Cells
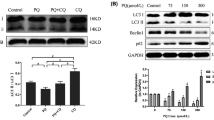
HMGB1 can be associated with cellular biological processes through the differential engagement of multiple surface receptors including TLR and RAGE ligands (Sims et al. 2010). Since RAGE activation has been implicated in sterile inflammation and neurological diseases (Chen et al. 2007), we would like to clarify whether PQ-induced HMGB1 release initiate the activation of RAGE signaling pathway in SH-SY5Y cells. We explored the effects of different concentrations of PQ (0, 75, 150, 300 μmol/L) on SH-SY5Y cells for 24 h by western blotting assay. Our results showed that the expression level of RAGE protein was significantly increased after PQ treatment (Fig. 5A and B). In addition, PQ treatment significantly increased the levels of RAS protein and phosphorylated P38 protein (p-P38) (Fig. 5A, C, and D). These results indicated that accumulated extracellular HMGB1 induced by PQ bind to the cell surface receptor RAGE and activate the RAGE signaling pathway. With the increase dosage of PQ exposure, the increase of these molecular expressions became more obvious, showing a dose-dependent manner.
Effects of PQ on RAGE signaling pathway in SH-SY5Y cells. Cells were treated with different doses of PQ (0, 75, 150, 300 μmol/L) or 500 μmol/L of MPP+ for 24 h. (A) Total protein lysates were evaluated by western blot analysis for the expression levels of RAGE, RAS, P38, and p-P38 protein. β-actin was used as the internal control for normalization. (B–D) Histogram showed the quantitative evaluation of each protein band by densitometry. The data are presented as mean ± SE. * p < 0.05, compared with the vehicle control. MPP+, known to affect RAGE signaling pathways, was used as a positive control
Lentivirus-Mediated shRNA Downregulated HMGB1 in SH-SY5Y Cells
Western blot was used to evaluate the efficiency of HMGB1 knockdown by lentivirus-mediated shRNA. The results showed that the expression of HMGB1 protein was significantly suppressed in HMGB1 shRNA group when compared with control group (Fig. 6). In contrast, the HMGB1 protein level in NC shRNA group exhibited no significant difference when compared with control group, confirming the role of scrambled shRNA as a negative control (Fig. 6).
Knockdown of HMGB1 by lentivirus-mediated shRNA in SH-SY5Y cells. Cells were transfected with HMGB1 shRNA or NC shRNA. (A) Total protein lysate was evaluated by western blot analysis for the expression level of HMGB1 protein in each group. β-actin was used as the internal control for normalization. (B) Histogram showed the quantitative evaluation of protein band by densitometry. The data are presented as mean ± SE. * p < 0.05, compared with the vehicle control
Knockdown of HMGB1 Reduces PQ Toxicity on SH-SY5Y Cells
We next investigated whether the knockdown of HMGB1 has any protective effects on PQ-treated SH-SY5Y cells. The viability of SH-SY5Y cells in different groups were determined by MTT assay and were expressed as the percentage of viability from control group. Figure 7 showed that transfection with scrambled shRNA or HMGB1-shRNA has no obvious effects on cell viability (NC shRNA and HMGB1 shRNA in Fig. 7). After treated with 150 μmol/L PQ for 24 h, the viability of SH-SY5Y cells was significantly reduced by ~ 22.6% (PQ in Fig. 7) when compared with the control group (control in Fig. 7). However, knockdown of HMGB1 attenuated the reduction of cell viability in SH-SY5Y cells after PQ exposure (HMGB1 shRNA + PQ in Fig. 7) when compared with PQ-treated cells without HMGB1 knockdown (NC shRNA + PQ in Fig. 7).
Knockdown of HMGB1 rescues SH-SY5Y cells from PQ toxicity. SH-SY5Y cells transfected with HMGB1 shRNA or NC shRNA were treated with 150 μmol/L PQ for 24 h. Cell viability was demonstrated as percentage in viability from the negative control. Columns, mean (n = 3); bars, ±SE; * p < 0.05, compared with the vehicle control; #: p < 0.05, compared with the NC shRNA + PQ group
Knockdown of HMGB1-Inhibited RAGE Signaling Pathway in PQ-Treated SH-SY5Y Cells
To further illustrate the relationship between HMGB1 and RAGE signaling pathway, we first knockdown the HMGB1 in SH-SY5Y cells and treated them with 150 μmol/L PQ for 24 h. By checking the HMGB1 protein expression by western blot assay, we confirmed that lentivirus-mediated HMGB1 shRNA dramatically attenuated the increase of HMGB1 protein induced by PQ exposure (Fig. 8A and B). It is worth mentioning that our preliminary data showed that there was no significant difference between cells treated with PQ (PQ group) and scrambled shRNA-transfected cells treated with PQ (NC shRNA + PQ group), so we can confirm that there is no obvious interaction between PQ and scrambled shRNA. Thus, in this manuscript, we did not present data from NC shRNA + PQ group, as they are the same with PQ group.
Knockdown of HMGB1-inhibited RAGE signaling pathway in PQ-treated SH-SY5Y. SH-SY5Y cells transfected with HMGB1 shRNA or NC shRNA were treated with 150 μmol/L PQ for 24 h. (A) Total protein lysates were evaluated by western blot analysis for the expression level of HMGB1, RAGE, RAS, p-P38, and P38 protein. β-actin was used as the internal control for normalization. (B–E) Histogram showed the quantitative evaluation of protein band by densitometry. The data are presented as mean ± SE. * p < 0.05, compared with the vehicle control. ap < 0.05, compared with the vehicle control; bp < 0.05, compared with the PQ treatment group
Subsequently, the expression levels of PQ-activated key molecules along RAGE signaling pathway like RAGE and RAS were both inhibited by HMGB1 knockdown (Fig. 8A, C, and D). In addition, PQ-increased phosphorylated P38 protein expression was also attenuated by HMGB1 knockdown (Fig. 8A and E). These results revealed that HMGB1 plays a vital role in the process of activating RAGE signaling pathway in SH-SY5Y cells treated by PQ. Upon PQ exposure, SH-SY5Y cells released large amount of HMGB1 which accumulated in extracellular environment. By knockdown of HMGB1, PQ exposure was not able to produce enough extracellular HMBG1 to bind the cell surface receptor RAGE, thereby inhibiting the RAGE signaling pathway.
Knockdown of HMGB1 Alleviates NF-κB p65 Expression and the Intensity of Inflammation in PQ-Treated SH-SY5Y Cells
To further illustrate the role of HMGB1 in NF-κB signaling and related inflammation responses, validation of activation or inhibition of protein expression level after PQ treatment in SH-SY5Y cells (both wild type and HMGB1 knockdown) was performed by using western blotting. As shown in Fig. 9, NF-κB p65 subunit expression was significantly increased after PQ exposure. However, knockdown of HMGB1 reduced the level of NF-κB p65 after being exposed to PQ when compared with PQ-treated cells without HMGB1 knockdown. NF-κB p65 elevation is always accompanied by the phosphorylation of ΙκBα (p-ΙκBα), which could dissociate itself from NF-κB in cytoplasm, thereby releasing the NF-κB p65 subunit. Here we also confirmed that the expression level of p-ΙκBα was also markedly increased after PQ treatment, and this increase was significantly attenuated by HMGB1 knockdown. The protein expression of pro-inflammatory cytokines (TNF-α, IL-6), which was significantly increased upon PQ exposure, was decreased significantly in the presence of HMGB1 shRNA. These results indicated that knockdown of HMGB1 could alleviate the upregulated NF-κB signaling and inflammatory responses in SH-SY5Y cells treated with PQ.
Knockdown of HMGB1 alleviates NF-κB p65 expression and the intensity of inflammation in PQ-treated SH-SY5Y cells. SH-SY5Y cells transfected with HMGB1 shRNA or NC shRNA were treated with 150 μmol/L PQ for 24 h. (A) Total protein lysates were evaluated by western blot analysis for the expression level of NF-κB/p65, ΙκBα, p-ΙκBα, TNF-α, and IL-6 protein. β-actin was used as the internal control for normalization. (B–E) Histogram showed the quantitative evaluation of protein band by densitometry. The data are presented as mean ± SE. ap < 0.05, compared with the vehicle control; bp < 0.05, compared with the PQ treatment group
Discussion
Paraquat (1, 1′-dimethyl-4, 4′-bipyridinium, PQ) is a widely characterized neurotoxicant capable of inducing a series of nervous system disorders, including neurobehavioral defects and neurodegenerative diseases such as Parkinson’s disease (Lou et al. 2016; Tanner et al. 2011). Neuroinflammation has been considered to be a crucial mediator between progressive neural degeneration and neurotoxicant exposures (Barcia 2013; Gagne and Power 2010). However, the adverse effects of PQ on the neuroimmune interactions and how they contribute to pathogenesis and progression of PD have rarely been reported so far.
HMGB1, a highly conserved nonhistone DNA-binding protein, could be actively released to cytosol and extracellular environment and function as a cytokine to initiate inflammatory responses (Bell et al. 2006; Sims et al. 2010). Recent studies have demonstrated that HMGB1 is associated with several neurodegenerative disorders such as amyotrophic lateral sclerosis (ALS), Alzheimer’s disease (AD), and PD (Hwang et al. 2013; Jang et al. 2013; Lo Coco et al. 2007; Santoro et al. 2016; Sasaki et al. 2016). For example, HMGB1 was proven to be able to promote ALS progression by inducing neuroinflammation and damaging motor neurons in mice (Lo Coco et al. 2007). In AD animal models, HMGB1 secretion was induced by β-amyloid peptide (Aβ) and could accelerate neuronal cell death (Jang et al. 2013). HMGB1 might be particularly relevant to PD as elevated cerebrospinal fluid and serum HMGB1 were detected in PD patients (Santoro et al. 2016). In addition, HMGB1 alterations were found in both in vivo and in vitro PD models, suggesting that HMGB1 plays an important role in the pathogenesis of PD (Guan et al. 2018; Huang et al. 2017; Santoro et al. 2016; Sasaki et al. 2016).
Previous research has reported that acute PQ exposure could increase the level of HMGB1 in bronchoalveolar lavage fluid, thus activating TLR4 signaling pathway to promote lung injury. Reactive oxygen species (ROS) production induced by PQ exposure is also involved in HMGB1 release. HMGB1 released from apoptosis cells is oxidized on Cys106 in a process that requires reactive oxygen species (ROS), which play as a primary trigger in affecting the HMGB1 accumulation (Kazama et al. 2008). However, whether and how HMGB1 exert modulatory effects upon lower-dose PQ exposure in nervous system still remain to be illustrated. Thus, in the present study, we selected the human neuroblastoma cell line (SH-SY5Y), a widely used in vitro model for PD research to investigate the underlying association between HMGB1 and PQ neurotoxicity (Xicoy et al. 2017).
Dose-dependent impacts of PQ on SH-SY5Y cells were initially explored. When SH-SY5Y cells were treated with PQ (≥ 150 μmol/L) for longer than 24 h, cell viability markedly decreased compared to untreated cells. As expected, extracellular HMGB1 content was significantly increased upon treatment with 150 μmol/L or higher concentration of PQ. These results confirmed that a certain concentration of PQ (≥ 150 μmol/L) could stimulate SH-SY5Y cells to release HMGB1 to extracellular environment, which is somehow relevant to the reduced cell viability. Since HMGB1 is predominantly located in the nucleus, we further investigated the impacts of PQ exposure on the dynamic translocation process of HMGB1. Our results revealed that HMGB1 protein level in nucleus first increased to the peak level after 12 h exposure and dramatically decreased afterward. Similarly, HMGB1 in cytoplasm accumulated to a peak level after 24 h exposure and hereafter start to decrease. In contrast, extracellular HMGB1 continuously increased during the first 48 h exposure. It has been reported that both neurons and astrocytes could secrete HMGB1 under several pathological circumstances, such as cerebral ischemia or subarachnoid hemorrhage (Qiu et al. 2008; Sun et al. 2014; Zhang et al. 2011). Sasaki et al. observed HMGB1 translocation in dopaminergic neurons in PD rat models (Sasaki et al. 2016). These findings supported our hypothesis that PQ exposure induced a massive production of HMGB1 in nucleus whereas HMGB1 rapidly translocated from nucleus to cytoplasm and is thus continuously released to the outside of SH-SY5Y cells.
To further illustrate the role of HMGB1 in PQ-induced neurotoxic effects, we knock down HMGB1 in SH-SY5Y cells by using lentivirus-mediated RNA interference technique. Our results showed that the deleterious effects induced by PQ can be inhibited by knockdown of HMGB1, demonstrating a role of HMGB1 in causing damage to the SH-SY5Y cells upon PQ treatment. In consistent with our findings, recent studies reported that systemic administration of neutralizing antibodies to HMGB1 could relieve dopaminergic neuron death in PD models (Santoro et al. 2016; Sasaki et al. 2016).
HMGB1 has been reported to be associated with cellular biological processes through the differential engagement of multiple surface receptors including TLRs (TLR2, TLR4) and RAGE (receptor for advanced glycation end products) ligands (Sims et al. 2010). Although interactions between HMGB1 and TLRs may also be important, we found that the effects of HMGB1 were, at least partially, exerted through activation of the multiligand receptor RAGE. RAGE has been described to bind to a diverse array of damage-associated molecular patterns (DAMPs) such as HMGB1 (Sims et al. 2010). Knockdown of HMGB1 in the PQ-treated SH-SY5Y cells led to reduced expression of RAGE in combination with reduced cell death, indicating that the downstream signaling cascades of RAGE contribute to the damaging effects of HMGB1. HMGB1-RAGE interaction has been shown to be pathogenic in models of ischemic injury and Alzheimer’s disease (Kim et al. 2006; Mazarati et al. 2011). Previous studies have revealed that HMGB1 exposure upregulated RAGE (Andersson and Tracey 2011; Schmidt et al. 2001), supporting our findings that knockdown of HMGB1 is the possible reason for the reduced expression of RAGE. Our investigation on further downstream cascade known to be activated upon RAGE-ligand interaction revealed that the expression levels of RAS, P38, and NF-κB P65 protein are increased after PQ treatment, which could be suppressed by HMGB1 knockdown (Bierhaus et al. 2005; Downs et al. 2015; Xu et al. 2010). NF-κB activation triggered by engagement of Aβ and RAGE via MAPK pathway was also observed in AD models (Kierdorf and Fritz 2013). In primary neuronal cell culture, activation of RAGE leads to the production of MAPK pathway and Ras (Huttunen et al. 1999). In addition, p38 MAPK signaling pathway is involved in PQ-induced neuron death and lung injury (Niso-Santano et al. 2006; Pei et al. 2014). Together with these evidences, we confirmed that RAGE-P38-NF-κB signaling pathways are likely to contribute to the HMGB1-mediated effects upon PQ exposure.
In addition, our results also demonstrated the involvement of significant upregulation of TNF-α and IL-6 in the neuroinflammation upon PQ exposure. In characterizing pro-inflammatory effects of HMGB1, we showed that knockdown of HMGB1 suppressed the increase of TNF-α and IL-6 in SH-SY5Ycells after PQ treatment. Multiple studies have reported that HMGB1 could elicit the upregulation of pro-inflammation cytokines. Sasaki et al. found that anti-HMGB1 mAb suppresses the increase of IL-6 and IL-1β in the striatum in rat model of PD (Sasaki et al. 2016). Santoro et al. found that neutralization of HMGB1 lowers TNF-α level in MPTP-treated mice (Santoro et al. 2016). These findings provided further evidence that HMGB1 may be a key molecule in the neuroinflammatory responses induced by PQ exposure.
It is worth noting that mechanisms beyond RAGE receptor activation may contribute to the HMGB1-mediated neurotoxic effects of PQ. NF-κB pathway could be activated by multiple upstream signals. ROS produced by PQ exposure may behave as an intrinsic signal transduction molecule and modulate NF-κB activity (Lambeth 2004; Wang et al. 2014). On the other hand, Mac1, an adhesion molecule broadly expressed on microglia, can also react to DAMPs in neuronal tissues (Block and Hong 2007; Floden et al. 2005). Binding of HMGB1 to microglial Mac1 could activate NF-κB pathway to induce neuroinflammation in microglia, which form a vicious cycle to drive chronic, progressive neurodegeneration (Gao et al. 2011). Meanwhile, HMGB1 may also act on neuron Mac1 to mediate chronic neuroinflammation in neurons themselves.
Taken together, our study found that HMGB1 was markedly increased in a concentration or time-dependent manner upon PQ exposure and the elevated HMGB1 could be translocated into cytosol and then released to the extracellular milieu of SH-SY5Y cells. Moreover, we demonstrated that HMGB1 plays a major role in PQ-induced neuroinflammation and that the RAGE-P38-NF-κB signaling pathways contribute to the HMGB1-mediated effects upon PQ exposure.
Conclusions
The results in the present study showed that paraquat (PQ) exposure could induce a massive translocation of HMGB1 protein from nuclei to the extracellular milieu of SH-SY5Y cells. We also demonstrated that HMGB1 contributes to the neurotoxicity of PQ by activating RAGE-P38-NF-κB signaling pathways and promoting the secretion of pro-inflammatory cytokines.
References
Andersson U, Tracey KJ (2011) HMGB1 is a therapeutic target for sterile inflammation and infection. Annu Rev Immunol 29:139–162. https://doi.org/10.1146/annurev-immunol-030409-101323
Ball N, Teo WP, Chandra S, Chapman J (2019) Parkinson's disease and the environment. Front Neurol 10:218. https://doi.org/10.3389/fneur.2019.00218
Barcia C (2013) Glial-mediated inflammation underlying parkinsonism. Scientifica (Cairo) 2013:357805. https://doi.org/10.1155/2013/357805
Bell CW, Jiang W, Reich CF 3rd, Pisetsky DS (2006) The extracellular release of HMGB1 during apoptotic cell death. Am J Physiol Cell Physiol 291:C1318–C1325. https://doi.org/10.1152/ajpcell.00616.2005
Bertram L, Tanzi RE (2005) The genetic epidemiology of neurodegenerative disease. J Clin Invest 115:1449–1457. https://doi.org/10.1172/JCI24761
Bierhaus A et al (2005) Understanding RAGE, the receptor for advanced glycation end products. J Mol Med 83:876–886. https://doi.org/10.1007/s00109-005-0688-7
Block ML, Hong JS (2007) Chronic microglial activation and progressive dopaminergic neurotoxicity. Biochem Soc Trans 35:1127–1132. https://doi.org/10.1042/BST0351127
Brichta L, Greengard P (2014) Molecular determinants of selective dopaminergic vulnerability in Parkinson's disease: an update. Front Neuroanat 8:152. https://doi.org/10.3389/fnana.2014.00152
Chang X, Lu W, Dou T, Wang X, Lou D, Sun X, Zhou Z (2013) Paraquat inhibits cell viability via enhanced oxidative stress and apoptosis in human neural progenitor cells Chem Biol Interact 206:248–255. https://doi.org/10.1016/j.cbi.2013.09.010
Chen H, Ritz B (2018) The search for environmental causes of Parkinson's disease: moving forward. J Parkinson's Dis 8:S9–S17. https://doi.org/10.3233/JPD-181493
Chen X, Walker DG, Schmidt AM, Arancio O, Lue LF, Yan SD (2007) RAGE: a potential target for Abeta-mediated cellular perturbation in Alzheimer's disease. Curr Mol Med 7:735–742. https://doi.org/10.2174/156652407783220741
Downs CA, Kreiner LH, Johnson NM, Brown LA, Helms MN (2015) Receptor for advanced glycation end-products regulates lung fluid balance via protein kinase C-gp91(phox) signaling to epithelial sodium channels. American journal of respiratory cell and molecular biology 52:75–87. https://doi.org/10.1165/rcmb.2014-0002OC
Floden AM, Li S, Combs CK (2005) Beta-amyloid-stimulated microglia induce neuron death via synergistic stimulation of tumor necrosis factor alpha and NMDA receptors. J Neurosci 25:2566–2575. https://doi.org/10.1523/JNEUROSCI.4998-04.2005
Gagne JJ, Power MC (2010) Anti-inflammatory drugs and risk of Parkinson disease: a meta-analysis. Neurology 74:995–1002. https://doi.org/10.1212/WNL.0b013e3181d5a4a3
Gao HM, Zhou H, Zhang F, Wilson BC, Kam W, Hong JS (2011) HMGB1 acts on microglia Mac1 to mediate chronic neuroinflammation that drives progressive neurodegeneration. J Neurosci 31:1081–1092. https://doi.org/10.1523/JNEUROSCI.3732-10.2011
Guan Y, Li Y, Zhao G, Li Y (2018) HMGB1 promotes the starvation-induced autophagic degradation of alpha-synuclein in SH-SY5Y cells Atg 5-dependently life Sci 202:1-10. https://doi.org/10.1016/j.lfs.2018.03.031
Huang J et al (2017) HMGB1 mediates autophagy dysfunction via perturbing Beclin1-Vps34 complex in dopaminergic cell model. Front Mol Neurosci 10:13. https://doi.org/10.3389/fnmol.2017.00013
Huttunen HJ, Fages C, Rauvala H (1999) Receptor for advanced glycation end products (RAGE)-mediated neurite outgrowth and activation of NF-kappaB require the cytoplasmic domain of the receptor but different downstream signaling pathways. J Biol Chem 274:19919–19924. https://doi.org/10.1074/jbc.274.28.19919
Hwang CS, Liu GT, Chang MD, Liao IL, Chang HT (2013) Elevated serum autoantibody against high mobility group box 1 as a potent surrogate biomarker for amyotrophic lateral sclerosis. Neurobiol Dis 58:13–18. https://doi.org/10.1016/j.nbd.2013.04.013
Jang A et al (2013) p35 deficiency accelerates HMGB-1-mediated neuronal death in the early stages of an Alzheimer's disease mouse model. Curr Alzheimer Res 10:829–843
Kazama H, Ricci JE, Herndon JM, Hoppe G, Green DR, Ferguson TA (2008) Induction of immunological tolerance by apoptotic cells requires caspase-dependent oxidation of high-mobility group box-1 protein. Immunity 29:21–32. https://doi.org/10.1016/j.immuni.2008.05.013
Kierdorf K, Fritz G (2013) RAGE regulation and signaling in inflammation and beyond. J Leukoc Biol 94:55–68. https://doi.org/10.1189/jlb.1012519
Kim JB et al (2006) HMGB1, a novel cytokine-like mediator linking acute neuronal death and delayed neuroinflammation in the postischemic brain. J Neurosci 26:6413–6421. https://doi.org/10.1523/JNEUROSCI.3815-05.2006
Lambeth JD (2004) NOX enzymes and the biology of reactive oxygen. Nat Rev Immunol 4:181–189. https://doi.org/10.1038/nri1312
Lo Coco D, Veglianese P, Allievi E, Bendotti C (2007) Distribution and cellular localization of high mobility group box protein 1 (HMGB1) in the spinal cord of a transgenic mouse model of ALS. Neuroscience letters 412:73–77. https://doi.org/10.1016/j.neulet.2006.10.063
Lou D, Chang X, Li W, Zhao Q, Wang Y, Zhou Z (2012) Paraquat affects the homeostasis of dopaminergic system in PC12 cells. Pesticide biochemistry and physiology 103:81–86. https://doi.org/10.1016/j.pestbp.2012.04.001
Lou D, Wang Q, Huang M, Zhou Z (2016) Does age matter? Comparison of neurobehavioral effects of paraquat exposure on postnatal and adult C57BL/6 mice. Toxicol Mech Methods 26:667–673. https://doi.org/10.1080/15376516.2016.1223241
Mamelak M (2018) Parkinson's disease, the dopaminergic neuron and Gammahydroxybutyrate. Neurol Ther 7:5–11. https://doi.org/10.1007/s40120-018-0091-2
Mazarati A, Maroso M, Iori V, Vezzani A, Carli M (2011) High-mobility group box-1 impairs memory in mice through both toll-like receptor 4 and receptor for advanced glycation end products. Experimental neurology 232:143–148. https://doi.org/10.1016/j.expneurol.2011.08.012
Niso-Santano M, Moran JM, Garcia-Rubio L, Gomez-Martin A, Gonzalez-Polo RA, Soler G, Fuentes JM (2006) Low concentrations of paraquat induces early activation of extracellular signal-regulated kinase 1/2, protein kinase B, and c-Jun N-terminal kinase 1/2 pathways: role of c-Jun N-terminal kinase in paraquat-induced cell death. Toxicol Sci 92:507–515. https://doi.org/10.1093/toxsci/kfl013
Pei YH, Cai XM, Chen J, Sun BD, Sun ZR, Wang X, Qian XM (2014) The role of p38 MAPK in acute paraquat-induced lung injury in rats. Inhal Toxicol 26:880–884. https://doi.org/10.3109/08958378.2014.970784
Qiu J et al (2008) Early release of HMGB-1 from neurons after the onset of brain ischemia. Journal of cerebral blood flow and metabolism : official journal of the International Society of Cerebral Blood Flow and Metabolism 28:927–938. https://doi.org/10.1038/sj.jcbfm.9600582
Santoro M et al (2016) In-vivo evidence that high mobility group box 1 exerts deleterious effects in the 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine model and Parkinson's disease which can be attenuated by glycyrrhizin. Neurobiol Dis 91:59–68. https://doi.org/10.1016/j.nbd.2016.02.018
Sasaki T et al (2016) Anti-high mobility group box 1 antibody exerts neuroprotection in a rat model of Parkinson's disease. Exp Neurol 275(Pt 1):220–231. https://doi.org/10.1016/j.expneurol.2015.11.003
Schmidt AM, Yan SD, Yan SF, Stern DM (2001) The multiligand receptor RAGE as a progression factor amplifying immune and inflammatory responses. The Journal of clinical investigation 108:949–955. https://doi.org/10.1172/JCI14002
Sims GP, Rowe DC, Rietdijk ST, Herbst R, Coyle AJ (2010) HMGB1 and RAGE in inflammation and cancer. Annu Rev Immunol 28:367–388. https://doi.org/10.1146/annurev.immunol.021908.132603
Sun Q et al (2014) Early release of high-mobility group box 1 (HMGB1) from neurons in experimental subarachnoid hemorrhage in vivo and in vitro. Journal of neuroinflammation 11:106. https://doi.org/10.1186/1742-2094-11-106
Tanner CM et al (2011) Rotenone, paraquat, and Parkinson's disease. Environmental health perspectives 119:866–872. https://doi.org/10.1289/ehp.1002839
Wang X, Luo F, Zhao H (2014) Paraquat-induced reactive oxygen species inhibit neutrophil apoptosis via a p38 MAPK/NF-kappaB-IL-6/TNF-alpha positive-feedback circuit. PLoS one 9:e93837. https://doi.org/10.1371/journal.pone.0093837
Xicoy H, Wieringa B, Martens GJ (2017) The SH-SY5Y cell line in Parkinson's disease research: a systematic review. Mol Neurodegener 12:10. https://doi.org/10.1186/s13024-017-0149-0
Xu Y, Wang S, Feng L, Zhu Q, Xiang P, He B (2010) Blockade of PKC-beta protects HUVEC from advanced glycation end products induced inflammation. Int Immunopharmacol 10:1552–1559. https://doi.org/10.1016/j.intimp.2010.09.006
Yan B, Chen F, Xu L, Xing J, Wang X (2017) HMGB1-TLR4-IL23-IL17A axis promotes paraquat-induced acute lung injury by mediating neutrophil infiltration in mice. Sci Rep 7:597. https://doi.org/10.1038/s41598-017-00721-8
Zhang J et al (2011) Anti-high mobility group box-1 monoclonal antibody protects the blood-brain barrier from ischemia-induced disruption in rats. Stroke 42:1420–1428. https://doi.org/10.1161/STROKEAHA.110.598334
Funding
The present study was supported by the National Natural Science Foundation of China (81560538), Natural Science Foundation of Ningxia (NZ17055), and Project for Developing Top Western Disciplines in University (Public health and Preventive Medicine) (NXYLXK2017B08).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict(s) of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Huang, M., Guo, M., Wang, K. et al. HMGB1 Mediates Paraquat-Induced Neuroinflammatory Responses via Activating RAGE Signaling Pathway. Neurotox Res 37, 913–925 (2020). https://doi.org/10.1007/s12640-019-00148-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-019-00148-1