Abstract
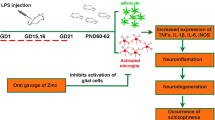
In the present study, we examined the effect of perinatal Escherichia coli lipopolysaccharide (LPS) exposure on the developing rat cerebellum and tested the hypothesis that maternal infections impact brain structure and function by mechanisms involving increase in oxidative stress and changes in brain type 2 iodothyronine deiodinase (D2)- and thyroid hormone (TH)-responsive genes. Spontaneously hypertensive rat (SHR) and Sprague–Dawley (SD) rat dams were challenged with LPS (200 μg/kg body weight) exposure during pregnancy (G10–G15) and lactation (P5–P10), the time periods corresponding, respectively, to the first/second and the third trimesters of human pregnancy. LPS exposure resulted in a significantly decreased motor learning in SD male (29.8 %) and in female (55.0 %) pups (p < 0.05); changes in rollover and startle response showed only a trend. The LPS challenge also resulted in a trend (p = 0.09) toward increased cerebellar levels of the oxidative stress marker 3-nitrotyrosine (3-NT) in SD male (16.2 %) and female (21.2 %) neonates, while 3-NT levels were significantly decreased (p < 0.05) in SHR female pups. D2 activity, responsible for local intra-brain conversion of thyroxine (T4) to the active hormone, 3′,3,5-triiodothyronine (T3), was significantly (p < 0.05) decreased in LPS-challenged SHR male (40.3 %) and SD female (47.4 %) pups. Several genes were affected by LPS. Notably, D2 (DIO2) and brain-derived neurotrophic factor (BDNF) were significantly elevated in SHR females, while transthyretin (TTR) expression was decreased in both SD males and females (P < 0.05). In vitro chronic exposure of cerebellar cultures to LPS resulted in decreased arborization of Purkinje cells while D2 was only increased transiently. Our data demonstrate that perinatal LPS exposure impacts the developing cerebellum in strain- and sex-dependent manner via complex mechanisms that involve changes in oxidative stress, enzymes involved in maintaining local TH homeostasis, and downstream gene expression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Clinical and epidemiological data suggest that maternal infection during pregnancy and nursing increases the probability of neonatal brain injury and may have a long-lasting impact on brain functions. Maternal infection during pregnancy has been linked to neurological and neurobehavioral disorders in humans such as cerebral palsy [1, 2], neonatal strokes [3], schizophrenia [4, 5], and affective disorders [4]. Animal studies implicate bacterial infection in the pathology of Parkinson’s disease [6] and, notably, schizophrenia and autism [7].
Bacterial infection triggers a response that involves production of inflammatory mediators - cytokines. The triggering signals are delivered by the endotoxins lipopolysaccharides (LPS), major components of the outer membrane of Gram-negative bacteria. Such responses can be elicited in animals by a direct exposure to LPS, thus modeling infection. LPS administered to the pregnant mother are transferred to the fetus through the placenta [8] and result in increased cytokines levels in amniotic fluid [9, 10] and the fetal brain [9]. Bacterial infection of the lactating mother also results in increased levels of cytokines in the milk [11].
LPS also triggers increased oxidative stress [12–14]. Experimental evidence suggests that cellular injury during the inflammatory response is mediated by reactive oxygen species [15] and that endotoxin-induced excessive free radical production damages and opens the blood–brain barrier [16]. Further, LPS is not only a potent trigger of oxidative stress [12, 16] but also a disruptor of antioxidant defenses [12]. The combined effect of high levels of free radicals and low levels of scavengers leads to oxidative stress [17] that promotes injury in the developing brain. Further, in vitro addition of LPS to glial cultures increases the production of free radicals [18], although this effect has been recently reassigned to the response of microglial cells [19].
LPS also regulates expression of the type 2 iodothyronine deiodinase (D2), an enzyme that converts the pro-hormone thyroxine (T4) to the active hormone, 3′,3,5-triiodothyronine (T3), and is responsible for most of the T3 supply within the brain [20]. D2 activity is increased in the mediobasal hypothalamus, anterior pituitary, and cerebral cortex after LPS administration [21]. Furthermore, D2 activity and mRNA are both increased by LPS exposure in astrocyte culture in vitro [22]. Furthermore, the induction of D2 activity by cAMP in in vitro cultures is inhibited by oxidative stress [23]. LPS-mediated increase in D2 in glial cultures has been shown to be associated with elevated T3-dependent gene expression in co-cultured neurons [24], suggesting that LPS-induced changes in D2 or oxidative stress could impact the developing CNS.
Interestingly, LPS exerts a sex-dependent response [25] and LPS-induced cytokine expression exhibits a sexually dimorphic profile [26, 27]. LPS stimulates the production of the cytokine TNF-α in vivo and in vitro [28], while the regulation of nitric oxide (NO) synthesis and apoptosis by TNF-α is estrogen dependent [29]. Further, the actions of the cytokine IL-1β, which is implicated in cerebrovascular brain injury, can be modified by estrogen [30]. These observations underscore the importance of measuring the effects of LPS treatment separately in both sexes.
The present study was undertaken to address the hypothesis that maternal infection during pregnancy, as modeled by LPS exposure, could lead to increased oxidative stress which in turn would inhibit cerebellar D2 activity and result in an altered pattern of thyroid hormone-dependent gene expression that would impair cerebellar development and function. To test this supposition, we examined the effects of maternal challenge with LPS in two strains of rats with different thresholds to oxidative stress, spontaneously hypertensive rats (SHR) and Sprague–Dawley (SD) rats, to test for genetically dependent sensitivity to inflammation, and in the male and in female neonates, to test for the sex-dependent nature of these effects. Neurodevelopment was assessed in terms of milestones such as roll over time and auditory function, and motor learning. The neurodevelopmental findings were correlated with cerebellar levels of the oxidative stress marker 3-nitrotyrosine (3-NT) and D2 activity. We further examined the expression of several thyroid hormone (TH)-dependent genes and genes implicated in cerebellar development. We find that maternal challenge with LPS during the perinatal period leads to deficiencies in motor learning, which are manifested in a strain- and sex-dependent manner. These changes are accompanied by a selective increase in oxidative stress, decreased D2 activity, and altered expression of cerebellar genes. Furthermore, chronic exposure of primary cerebellar cultures to LPS in vitro resulted in abnormal Purkinje cell arborization. While LPS-exposed cultures showed an initial increase in D2, this increase was transient and was not observed at later time following LPS exposure. Using these models, we begin to unravel the mechanism of LPS-triggered effects on Purkinje cells and their link to neurodevelopmental changes.
Materials and Methods
Animals and Treatment
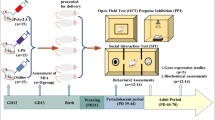
The animal experimentation protocols were approved by the Institutional Animal and Use Committee at Harvard Medical School and by the Animal Care and Experimentation Committee, Gunma University, Japan. For all in vitro experiments, timed pregnant SHR or SD rat dams purchased from Charles River Breeding Laboratories (Germantown, NY) on gestational day 7 (G7) (G1 defined as the first day after co-housing of males and females on which the female is found to have either a sperm plug or a sperm-positive vaginal smear) were individually housed under standard vivarium conditions (12:12 h light cycle, at 21–24 °C). Standard laboratory chow and water were available ad libitum. Following a period of recovery from the stress of shipment, selected SHR dams (n = 3) and SD dams (n = 6) were challenged with lipopolysaccharides (LPS; Sigma-Aldrich, St Louis, MO) at a dose of 200 μg/kg body weight (BW) via subcutaneous injections from G10 through G15 and then again from postnatal day 5 (P5) through P10; control SHR dams (n = 3) and SD dams (n = 3) received an equal volume of saline solution injections (Fig. 1).
Schematic representation of LPS exposure and neurobehavioral testing. Timed pregnant SHR or SD rats received LPS at a dose of 200 μg/kg body weight via subcutaneous injections from G10–G15 and P5–P10; control SHR and SD dams received an equal volume of saline. Rollover time (RO) was measured on P3–P5; startle response (ST) and eye opening (EO) were observed on P12–P14. Male and female pups were tested on a rotarod (RT) either on P20 to measure spontaneous motor function in untrained group (ROTAROD UNTR), or daily between P12 and P20 to assess the learned motor function in trained pups (ROTAROD TR). Animals were euthanized on P21 and cerebella dissected out for biochemical analysis
Maternal mass was monitored daily during pregnancy in both control and treatment groups. Neonates were counted, sexed, and weighed on P1/P2, and their mass was monitored daily until euthanasia on P21. The pups in LPS-challenged and control groups were tested for neurodevelopment milestones and auditory and motor functions between birth and P20. Cerebellar tissue derived from these animals on P21 was analyzed for oxidative stress, D2 activity, and gene expression.
Neurodevelopmental Milestones
Neurodevelopmental milestones were assessed between birth and P21 (weaning) separately in male and female offspring derived from LPS-challenged and control dams. Assessments included testing their righting response (rollover time), auditory (startle) response, and eye opening. Righting response was measured on P3–P5 as the time required for a rat pup to right itself when placed in a supine position. Onset of the startle response - a sign of acquiring hearing ability - was measured on P12–P14 in terms of head movement response to the sound of pen tapped against a glass surface performed consistently by a single experimenter. Eye opening was recorded between P12 and P14.
Motor Functions
Motor functions were measured using a rotarod. Selected male and female neonates were tested daily starting on P12 on a rotarod with an accelerating speed setting through P20 according to the procedure described earlier [31, 32]. Using this paradigm, motor learning was measured by increasing the speed of rotation and evaluating the same neonates over time; the pups tested on a rotarod from P12 through P20 represented “trained pups.” The “trained group” included 7 control SHR pups from 3 separate litters (3 males, 4 females), 12 control SD pups from 3 litters (6 males, 6 females), 6 LPS-challenged SHR pups from 3 litters (3 males, 3 females) and 23 LPS-challenged SD pups from 6 litters (11 males, 12 females). Each neonate was subjected to one trial on a rotarod rotating at incremental speeds in the range of 2–20 rpm during 5-min intervals. The length of time the animal remained on the rotarod and the rotational speed were recorded. If all animals were able to remain on the rotarod during a 5-min interval, the speed of rotation was increased. Remaining pups from each exposure group were kept as rotarod-naïve until P20 and were then tested on a rotarod set at a maximum speed of 20 rev/5 min. The pups tested for the first time represented “untrained pups.” The “untrained group” included 12 control SHR pups from 3 litters (5 males, 7 females), 23 control SD pups from 3 litters (12 males, 11 females), 15 LPS-challenged SHR pups from 3 litters (9 males, 6 females) and 44 LPS-challenged SD pups from 6 litters (24 males, 20 females).
Cerebellar Tissue
On P21, all pups were euthanized by decapitation. The cerebella, from the pups tested on the rotarod only on P20, including the cerebellum, were rapidly dissected, frozen on dry ice, and stored at −80 °C for further analysis.
Analysis of Cerebellar 3-Nitrotyrosine [3-NT] Levels
The 3-NT levels were measured in the cerebellar homogenates prepared from frozen tissue according to the procedure previously described [33]. Briefly, the cerebella were homogenized in a phosphate buffer containing detergents and protease inhibitors. The supernatants were collected by centrifugation at 16,000×g for 30 min at 4 °C. 3-NT in the supernatants was measured using aliquots derived from ∼25 mg tissue and a commercially available 3-NT enzyme-linked immunosorbent assay (ELISA) kit (Percipio Biosciences, Inc.; Foster City, CA). The ELISA plates were read at 450 nM. Data on 3-NT levels are expressed in picomoles per gram of tissue.
Analysis of Cerebellar D2 Activity
D2 activity in the cerebellum was measured by quantifying 125I-release from a 125I-labeled T4 tracer (5,700 mCi/mg; Perkin Elmer Life Sciences, Boston, MA) as described previously [34]. For the assays, 50 μg of protein was incubated for 4 h at 37 °C with 1 nM T4, 1 mM propylthiouracil (PTU), and 20 mM dithiothreitol (DTT). Background levels of deiodination were determined under identical conditions using 100 nM unlabeled T4.
Analysis of the Effect of LPS on Cerebellar TH-Dependent Gene Expression
Cerebellar mRNA was isolated using Trizol (Invitrogen, Carlsbad, CA) following the manufacturer’s instructions. Quantitative real-time PCR (qRT PCR) was used to measure gene expression levels and was performed as described previously [34] with the following modifications: SuperScript VILO (Invitrogen, Carlsbad, CA) was used for cDNA synthesis following the manufacturer’s instructions. Using qRT PCR, we have analyzed the expression of the following TH-dependent genes: suppressor-of-white-apricot-1 (SWAP-1 [60]), outer dense fiber of sperm tails 4 (Odf4), type 2 iodothyronine deiodinase (DIO2), cold-inducible RNA binding protein (Cirbp), and transthyretin (TTR). We also analyzed genes critically involved in cerebellar development: Purkinje cell protein 2 (Pcp2), type 3 iodothyronine deiodinase (DIO3), brain-derived neurotrophic factor 1 (BDNF-1), reelin (RELN), and Forkhead box protein 4 (FoxP4); cyclophilin A (CycloA) gene was used as a housekeeper gene for normalization. The primers for each of the genes are presented in Table 1.
Primary Cerebellar Culture
Timed pregnant Wistar rats were purchased from Japan SLC, Inc (Hamamatsu, Japan). Rat pups were decapitated under diethyl ether anesthesia on P1. Cerebellar cultures were prepared according to the procedure previously published [35] with some modification. To be brief, cerebellar tissue was digested with 0.2 U/mL papain (Worthington. Lakewood, NJ, USA) and filtered through 70-μm cell strainer (BD Biosciences, USA). Dissociated cells were suspended in a DMEM/F12 medium (1 % penicillin–streptomycin, 100 μg/ml transferrin, 10 μg/ml insulin, 30 nM sodium selenite, and 10 % FBS) and plated at a density of 3.0 × 105 cells/mL in poly-l-lysine-coated wells of chamber slides (NUNC Lab-Tek, Nalge Nunc International, Rochester, NY, USA). On the following day, cells were treated with different concentration of LPS for 24 h (acute exposure) or continuously from P2 to P17 (chronic exposure); half of the medium was replaced with fresh medium every 3 days, and cells were cultured for 17 days.
D2 Activity in Cerebellar Cultures
To measure D2 activity in cerebellar cultures, cells were plated in 6-well plates. At harvesting, the culture medium was aspirated and cells were rinsed with 2 ml ice-cold PBS and stored at −80 °C for later analysis. For assay, cells were collected by scraping in lysis buffer (0.1 M phosphate and 1 mM EDTA at pH 6.9 with 10 mM dithiothreitol and 0.25 M sucrose). After sonication, 50 μg protein of each sample was used for D2 assay as described above [34]. Samples were incubated in a reaction buffer (1 nM T4, 20 mM DTT, 1 mM PTU) with 125I-labeled T4 at 37 °C for 2 h. The reaction was stopped by TCA precipitation, with 100 μl of horse serum as the carrier protein, and free 125I in the supernatant was measured by gamma counting.
Immunocytochemical Analysis of Purkinje Cells
Immunocytochemical analysis of cultured cells was performed as described previously [35]. Briefly, cells were stained with a mouse monoclonal α-calbindin–28K antibody (1:1,000; McAB 300; Swant, Bellinzona, Switzerland) and fluorescein isothiocyanate (FITC)-labeled donkey anti-mouse antibody (1:200; Molecular Probes, Eugene, OR, USA). The morphological changes were examined under a laser confocal scanning microscope (FV1000D spectral-type inverted IX81 microscope; Olympus, Tokyo, Japan). To quantify dendrite arborization, the images were captured and the outline of the cell and dendritic branches of randomly selected Purkinje cells from each experiment was traced manually; the area was computed using NIH Image software (Image J). Data shown represent mean ± SE of one experiment; a total of three independent experiments were performed to confirm consistency of the results.
Statistical Analysis
The data presented here are derived from at least three litters per treatment group; the number of litters and male and female pups per groups is presented in the context of each analysis. When applicable, a two-way ANOVA was run to determine the relationship between treatment and sex. If a statistically significant interaction was found, a two-sample t test was carried out. All values are reported as a mean ± the standard error of the mean (SEM). For all statistical tests, p < 0.05 level of confidence was considered significant; 0.05 < p < 0.1 was considered a trend toward significance [36].
Results
Effect of LPS Challenge During Pregnancy on Gain in Maternal Body Mass
For perinatal exposure, pregnant and lactating dams received 12 subcutaneous injections (Fig. 1) for a cumulative dose of LPS of ∼500 μg/dam. Exposure to LPS during G10-G15 corresponds to the period of cerebellar Purkinje cell birth and simulates infection in pregnant women during the beginning of the second trimester of pregnancy [37]. Challenge with LPS during P5–P10 corresponds to the period of granule cells proliferation, a critical period of brain development; LPS administration during that time simulates infection during the second and the third trimester of pregnancy in humans [37, 38].
There were no overt signs of LPS toxicity in dams of either rat strain challenged during pregnancy (G10–G15). The relative gain in maternal body mass did not differ significantly between the LPS challenged and control dams (data not shown).
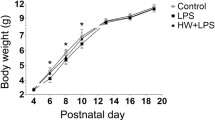
Perinatal LPS Challenge Has Little Effect on Neonatal Mass Gain in SHR and None in SD Strain
SHR pups were much smaller than SD pups at birth (Table 2), and in general, we observed a much greater mortality in SHR neonates that was further increased upon LPS treatment (data not shown). As shown in Table 2, on P2, the mass of LPS-challenged SHR neonates was slightly increased in both male (4.9 % increase) and female pups (5.3 % increase), but this difference was not found to be significant. The growth rate of LPS-challenged SHR pups appeared to be decreased, and on P21, the mass of LPS-challenged pups was slightly lower in both males and females, but this decrease was again not found to be significant.
In SD neonates, neonatal mass on P2 was not affected by LPS challenge in either males or females (Table 2). Furthermore, the growth rate of LPS-challenged SD pups was not affected, and there was no difference in mass between the LPS-challenged and control male or female pups on P21.
LPS Exposure Affects Cerebellar Mass in a Strain-Dependent Manner
LPS challenge resulted in no significant change in cerebellar mass in SHR pups (Table 2). Similarly, there was no significant change in cerebellar mass in SD pups (Table 2).
Effect of LPS Challenge on Rollover Time
The rollover time on P4 appeared to be increased in LPS-challenged SHR male pups (15.5 %) and in females (51.3 %; Table 3); however, this effect was not significant. In the SD strain, average rollover time was slightly increased in LPS-challenged male (10.4 %) but decreased in female (18.8 %; Table 2) pups, but again the differences were not found to be statistically significant.
The Effect of LPS Challenge on the Onset of the Auditory Response
The maturation of auditory function was tested by startle response. The percent of the responding male and female pups per litter was recorded and the mean per litter calculated (Table 3). In the SHR pups challenged with LPS the startle response, measured in terms of a decrease in percent of responders per litter on P14, showed no significant change (Table 3). In the SD strain, LPS-challenged male pups were not affected, while the startle response was decreased in female pups by 23.1 % (Table 3), although this was not statistically significant.
Effect of LPS Challenge on Spontaneous Motor Function on P20
To assess spontaneous motor behavior, a subset of rotarod “naïve” rats was tested on P20 on a rotarod set to a maximum setting of 20 rpm/5 min; this subset is referred to as “untrained pups” (Fig. 2). LPS challenge did not affect falling latency in untrained SHR male (Fig. 2a) or female pups (Fig. 2b). Similarly, LPS challenge did not affect falling latency in untrained SD male (Fig. 2c) or SD female pups (Fig. 2d).
LPS exposure impairs motor learning in a strain-dependent manner. Motor performance is presented as falling latency on the rotarod apparatus (seconds). Data are expressed as mean ± SEM. To assess the spontaneous motor behavior, a subset of rotarod “naïve” rats was tested on P20 on a rotarod set to a maximum setting of 20 rpm/5 min; this subset is referred to as “untrained pups” (P20-UNTR). The untrained pups are represented by: a C, 3 litters, 3 males; LPS, 3 litters, 3 males. b C, 3 litters, 3 females; LPS, 3 litters, 3 females. c C, 3 litters, 12 males; LPS, 6 litters, 30 males. d C, 3 litters, 10 females; LPS, 6 litters, 24 females. Perinatal LPS exposure did not affect spontaneous falling latency in SHR males (a) or female pups (b). Similarly, perinatal LPS exposure did not affect spontaneous falling latency in SD male (c) or SD female pups (d). To assess the effect of LPS on motor learning, selected male and female neonates from each litter were tested on a rotarod daily commencing on P12 neonates and continued until P20 (P20-TR). The trained pups are represented by: a C, 3 litters, 3 males; LPS, 3 litters, 3 males. b C, 3 litters, 4 females; LPS, 3 litters, 3 females. c C, 3 litters, 18 males; LPS, 6 litters, 41 males. d C, 3 litters, 16 females; LPS, 6 litters, 36 females. The mean “learned” falling latency in SHR was not affected in LPS-exposed male or female. The mean falling latency in LPS-exposed SD male pups was 60.1 % of that observed in control male pups (c; *p < 0.05), and in LPS-exposed SD female pups, it was by 54.0 % of that observed in control female pups (d; *p < 0.05)
Effect of LPS Challenge on Motor Learning Is Strain Dependent
To assess the effect of LPS challenge on motor learning, selected male and female neonates from each litter were tested on a rotarod daily commencing on P12 and continuing until P20; this subset is referred to as “trained pups” (Fig. 2).
Overall, SHR pups showed improvement in rotarod performance with age, but their falling latency was shorter than that observed in SD pups at P20. Further, SHR showed little improvement in rotarod performance with training (Fig. 2). The LPS challenge did not affect learned motor behavior (measured in terms of falling latency) in SHR male or female pups (Fig. 2a, b).
On the other hand, SD pups showed improvement in their rotarod performance with both age and training. Notably, the LPS challenge induced significant impairment in motor learning in SD pups of both sexes. The mean falling latency in LPS-challenged male pups was 60.1 % of that observed in control male pups (p < 0.05; Fig. 2c), while in LPS-challenged female pups it was 54.0 % of that observed in control female pups (p < 0.05; Fig. 2d).
LPS Challenge Alters Cerebellar Levels of Oxidative Stress Marker, 3-Nitrotyrosine (3-NT) in a Strain- and Sex-Dependent Manner
The levels of the oxidative stress marker 3-NT were quantified in cerebellar tissue obtained from LPS-challenged male and female SHR and SD rat pups on P21 (Fig. 3). The levels of 3NT were significantly (p < 0.05) decreased only in females (Fig. 3b) SHR pups challenged with LPS, while there was no change in 3-NT levels in male pups. In contrast, the challenge with LPS in SD rats resulted in increased 3-NT levels in both male (16.2 %; Fig. 3c) and in female (21.2 %; Fig. 3d) pups, but the difference was not found to be statistically significant.
LPS exposure results in altered cerebellar 3-NT levels. Cerebellar 3-NT levels are presented as picomoles per gram of tissue. a C, 3 litters, 6 males; LPS 3 litters, 14 males. b C, 3 litters, 7 females; LPS, 3 litters, 7 females. c C, 3 litters, 7 males; LPS, 6 litters, 16 males. d C, 3 litters, 6 females; LPS, 3 litters, 15 females. Data are presented as mean ± SEM. The levels of 3NT were significantly (*p < 0.05) decreased in both SHR male (a; 34.7 %) and SHR female (b) exposed to LPS. Exposure to LPS in SD rats resulted in a trend (+ p = 0.09) towards increase in 3-NT levels in male (c; 16.2 % increase) and in female (d; 21.2 % increase) pups, but the difference was not found to be statistically significant
LPS Challenge Alters Cerebellar D2 Activity in a Strain- and Sex-Dependent Manner
The levels of D2 activity were quantified in cerebellar tissue from control and LPS-challenged P21 male and female SHR and SD rat neonates (Fig. 4). Perinatal challenge with LPS resulted in a significant (p < 0.05) decrease in cerebellar D2 activity in male (40.3 %; Fig. 4a), while the decrease in female SHR pups (Fig. 4b) was not found to be significant. In SD pups, LPS challenge did not affect D2 activity in males (Fig. 4c), but resulted in a significant (p < 0.05) reduction (47.4 %; Fig. 4d) in D2 activity in female SD pups.
LPS exposure results in altered cerebellar D2 activity. Cerebellar D2 activity is presented in femtomoles per minute per milligram of tissue. a C, 3 litters, 5 males; LPS, 3 litters, 14 males. b C, 3 litters, 8 females; LPS, 3 litters, 7 females. c C, 3 litters, 4 males; LPS, 6 litters, 8 males. d C, 3 litters, 4 females; LPS, 6 litters, 5 females. Data are expressed as mean ± SEM. Perinatal exposure to LPS resulted in a significant (a; *p < 0.05) decrease (40.3 %) in cerebellar levels of D2 in SHR male, while the decrease in SHR female pups (b) was not found to be significant. In SD rats, D2 was not affected in LPS-exposed SD males (c) but was significantly decreased in SD female pups (d; *p < 0.05)
LPS Exposure Disrupts Cerebellar Gene Expression
The decrease in D2 activity observed in SHR male (Fig. 4a) and SD female (Fig. 4b) neonates suggests that there may be less local T4 to T3 conversion in the cerebellum of these animals, resulting in a decreased T3 content within this tissue. To assess if this affects downstream T3-regulated gene expression, we determined the mRNA levels of several genes negatively regulated by T3 [39, 40]. A number of genes negatively regulated by T3 have been found to be significantly increased in D2KO mice [41]. Consistent with this hypothesis, we observed a small increase in SWAP gene expression in SHR male pups, which was not found to be significant, while SWAP expression in female pups (Fig. 5a, b) was not affected. Interestingly, we observed a significant (p < 0.05) increase in DIO2 gene expression in SHR female pups (Fig. 5b) although the activity of D2 enzyme was not altered. However, the expression of the T3-responsive genes Odf4, Cirbp, and TTR remained unchanged in LPS challenged SHR males and females (Fig. 5a, b). In SD rats, we observed a significant decrease (p < 0.05) in TTR expression in both male (Fig. 5c) and female (Fig. 5d) pups.
The effect of LPS exposure on cerebellar gene expression. Cerebellar gene expression was measured by quantitative RT-PCR and was normalized to cyclophilin A expression. a SHR males, b SHR females, c SD males, d SD females. CycloA gene was used as a housekeeper gene for normalization, and data are presented as a relative gene expression (mean ± SEM; *p < 0.05)
We also examined the expression of several genes positively regulated by TH and/or which are critically involved in cerebellar development. The expression of the Pcp2 gene was not changed in SHR male or female pups (Fig. 5a, b). The expression of BDNF was significantly (p < 0.05) upregulated in SHR females (Fig. 5b). The expression of DIO3 showed a small decrease only in females (Fig. 5b), which was not found to be significant. The expression of RELN and FoxP4 genes was not affected by LPS challenge in SHR pups, while in SD rats there was a small decrease in RELN gene expression in females (Fig. 5d), but again this difference was not found to be significant.
Effect of Chronic Versus Acute LPS Exposure on the Cerebellar Cultures
We next assessed the effects of LPS exposure on Purkinje cell development in primary mixed cerebellar cultures. Chronic LPS exposure of cultures for 17 days resulted in a significant decrease (p < 0.05) in Purkinje cell arborization by approximately 40–60 % beginning at concentrations of 10−8 M LPS, with an additional decrease in dendritic area at LPS concentrations of 10−6 M (Fig. 6a, b). Treatment with 10−8 to 10−5 M LPS for 24 h significantly increased D2 activity in these cultures from 1.5- to 2-fold (p < 0.05) (Fig. 6c). However, no increase in D2 activity was found after 17 days of continuous LPS treatment (data not shown).
The effect of chronic LPS treatment on Purkinje cell arborization. a Primary mixed cerebellar cultures were treated with either vehicle or 10−9–10−5 LPS as indicated and representative samples stained with α-calbindin-28K. b Relative dendritic tree—mean ± SEM. c D2 activity measured in primary mixed cerebellar cultures treated with the indicated LPS concentration for 24 h; values represent the mean ± SEM of triplicate wells. Each portion of experiment was repeated twice with similar results
Discussion
Maternal infection during pregnancy affects the health of both the mother and the unborn child, has been associated with both the developmental disorders such as autism [7], and has been identified as a major risk factor in schizophrenia [4, 5] and cerebral palsy [1, 2]. It has been hypothesized that maternal infection affects the developing brain and several studies have confirmed the developmental impact of LPS challenge on brain and behavior [42]. LPS challenge has been reported to be associated with decreased neurogenesis [43], increased apoptosis [44], and disruption of the blood–brain barrier [45].
LPS is a major component of the outer membrane of Gram-negative bacteria that triggers the infectious response; the challenge of experimental animals with LPS is a common model of infection. LPS is transferred to the fetus through the placenta, as shown by the presence of radioactive LPS in the fetus following the administration to the dams [8], and also acts indirectly via the cytokines present in amniotic fluid [9, 10]. Although the presence of LPS has not been reported in milk, following maternal bacterial infection there is an increased level of cytokines present in the milk [11]. LPS accumulates in the fetal brain [9] and thus can affect both fetal and neonatal CNS development and behavior.
In the present study, we used several parameters, such as surface righting (rollover time), auditory maturation, and motor learning, to assess the consequences of LPS challenge on the neurobehavioral development of the offspring. Our studies indicate that the rollover time, an early index of motor maturation, was not significantly changed by LPS challenge in either strain or gender. This contrasts with a previously reported study of LPS effect in Fischer 344 rats where the surface righting response was accelerated in the LPS-exposed pups [46].
LPS-treated SHR pups, both male and female, showed a tendency towards delayed auditory maturation, while only SD female pups showed a similar tendency; it has been previously reported that an LPS challenge reduced the startle response in adult Long–Evans rats [47]. Furthermore, a congenital hearing loss has been linked to inflammation caused by bacterial infection [48].
Our results indicate that a perinatal LPS challenge did not affect the spontaneous motor coordination needed for balancing on a rotarod in pups of either strain or sex. Spontaneous motor coordination increased with age in both strains and sexes and was further improved with training in SD, but not SHR, rats. In the SHR pups, which appear to be less coordinated overall, LPS exposure did not affect motor learning in SHR male or female pups. On the other hand, in SD rats, LPS challenge led to significantly impaired motor learning in both male and female pups. While comparative studies on the effect of LPS on motor learning are lacking, the LPS-induced deficit in learning and memory in SD rat pups [49] and memory acquisition [50] have been previously reported. Tests including the beam walking, the pole test, the passive avoidance test, and the elevated plus-maze test were used to assess LPS-induced hippocampal injury in SD rats; LPS impaired learning on the beam walking test, the pole test, the passive avoidance test, and the elevated plus-maze test. Interestingly, no difference was found between the male and female rats [49]. Impaired learning on the passive avoidance test was observed in Wistar rats, although sex of the animals was not indicated in these experiments [50].
Our results indicate that the perinatal LPS challenge reduced cerebellar levels of the oxidative stress marker, 3-NT in female SHR pups, which are characterized by high endogenous levels of 3-NT. On the other hand, 3-NT levels showed a trend towards increased levels in SD pups of both sexes. LPS is a known potent trigger of oxidative stress [12–14, 16] and also a disruptor of antioxidant defenses [12]. In response to maternal infection, there is an increase in brain oxidative stress [17], including lipid peroxidation [14] and reduced GSH [51].
While the effects of maternal challenge with LPS during pregnancy on brain biochemistry and behavior of offspring have been examined, little is known about its effect on thyroid hormone (TH) metabolism. D2, a selenoenzyme that converts the pro-hormone thyroxine (T4) to the active hormone, 3′,3,5-triiodothyronine (T3), is responsible for most of the T3 supply within the brain [20]. Acute LPS exposure in rats increases D2 activity in the mediobasal hypothalamus, anterior pituitary, and cerebral cortex [21]. Chronic exposure to LPS, examined in the present study, took place during G10 through G15, a period corresponding to the beginning of the second trimester of pregnancy in humans and a period of Purkinje cell birth, and P5–P10, corresponding to the critical period of brain development and granule cell proliferation [52]. It has been previously observed that deficiency of T3 during early postnatal periods impacts the migration of granule cells [53]; thus, changes in D2 activity and consequently T3 levels in LPS-exposed rat pups may impact the developing brain.
Alternatively, oxidative stress has been found to decrease D2 activity in several cellular models both through transcriptional and post-transcriptional mechanisms [23, 54]. Thus, LPS-mediated effects that result in changes in oxidative stress levels could also modulate D2 activity. We observed that the LPS challenge significantly decreased cerebellar D2 activity in the SHR male pups and showed a tendency to deceased D2 activity in female SHR pups. In the SD strain, LPS challenge did not affect D2 activity in male pups, but resulted in a significant reduction of D2 activity in female pups. However, these changes only correlate with increased 3-NT in female SD pups, thus indicating that there may be other factors that can regulate D2 activity under these conditions. While the mechanism by which D2 activity is decreased in LPS-challenged pups is unclear, it is possible that it could be modulated by low selenium levels accompanying sepsis both in terms of a direct effect on the production of the D2, a selenoenzyme, and also in terms of susceptibility of the cell to oxidative stress [55].
A decrease in D2 activity within the cerebella of LPS-challenged SHR male and SD female neonates could result in local cerebellar “hypothyroidism” and significant changes in the pattern of gene expression. Consistent with this, the impairment of auditory and the motor functions is also observed in propylthiouracil (PTU)-induced hypothyroid conditions in rats [39]. Furthermore, mice with a global targeted disruption of the Dio2 gene (D2KO mice) have ∼50 % less T3 content in their cerebral cortex, cerebellum, and hypothalamus. Neurological functions in D2-deficient D2KO mice were examined using a rotarod apparatus (with learning over time component), vertical pole, the Morris water maze, the elevated plus maze, and the open field [40]. Compared to WT mice, no differences were observed in D2KO except for small difference in performance on a vertical pole. Interestingly, no differences in either spontaneous or learned performance on a rotarod were observed in D2KO mice [40]. On the other hand, performance on a rotarod in the hypothyroid Crl(CD)SD P30 male rats was significantly impaired [56]. Similarly, performance on a rotarod was significantly impaired in hypothyroid (hyt/hyt ) as compared to phenotypically normal mice; both male and female (hyt/hyt )mice showed a more gradual improvement in their ability over time and overall lower level of their performance on the rod [57]. Auditory impairment can be observed in D2 knockout mice; however, this is due to defects in cochlear development [58].
It has been previously reported that the immune activation by LPS selectively alters the expression of specific genes involved in interneuronal migration and oxidative stress [59]. It has also been shown that the expression of genes negatively regulated by T3 was preferentially upregulated in D2KO mice [41]. Thus, we assumed that that LPS-induced changes in D2 expression resulting in decreased cerebellar T3 levels would result in an activation of genes negatively regulated by TH. Contrary to our expectations, we found limited LPS-associated changes in the expression of these genes. We did find that expression of SWAP, a gene negatively regulated by T3, showed a tendency to be increased in SHR males. Elevated SWAP expression during critical developmental periods in the hypothyroid brain may be reflected downstream by increased pre-mRNA splicing and generation of additional neural-specific transcripts [60]. Elevation in SWAP expression following LPS exposure may thus contribute to increased splicing and possibly lead to distinctive splicing patterns during the development of rat cerebellum [61].
TTR gene is also negatively regulated by TH expression and upregulated in PTU-treated mouse cortex [62]; however, paradoxically, we observed a decrease in TTR expression in SD male and female pups. TTR protein is a T4 carrier protein both in plasma and the cerebrospinal fluid; however, TTR KO mice do not have decreased T3 content in their brains [63], and thus, this mechanism is unlikely to contribute to the observed neurodevelopmental changes in LPS-exposed pups. TTR protein also has neuroprotective properties [64]; thus, LPS treatment could be affecting neuronal survival.
We have also examined several genes positively regulated by TH and of special relevance to cerebellar development. Pcp2 is involved in neuronal differentiation [65], and T3 upregulates the expression of Pcp2 gene during the first 2 weeks of rat neonatal life [66]; however, we saw no significant changes in the expression of this gene. Cerebellar BDNF expression is decreased in PTU-treated hyperthyroid mice during postnatal development [67] and increased by TH in several regions of the developing brain [68]. However, we did not find decreased expression of BDNF in any of the conditions we studied, and in fact, BDNF was upregulated in LPS-challenged SHR female pups. Expression of the Dio3 gene that encodes the T3 inactivating enzyme type 3 deiodinase (D3) is also positively regulated by T3 [69]; it showed a tendency towards inhibition only in LPS-challenged SHR female pups. Interestingly, Dio2 gene expression was significantly elevated in SHR female pups, suggesting that a compensatory mechanism might be in play. RELN is a gene involved in neuronal migration that is downregulated by methiamazole-induced hypothyroidism [70], and this gene was found to be decreased in SD female pups. However, while the pattern of expression of some T3-regulated genes is consistent with intra-cerebellar D2 deficiency and a local hypothyroidism, when our data are taken together as a whole, it appears to be unlikely that local hypothyroidism in the cerebellum provides exclusive mechanism responsible for neurological impairments observed in LPS rats on P21. On the other hand, due to nature of our experimental design, we cannot discount an early transient increase in D2 activity and T3 levels immediately following the periods of LPS exposure that may contribute to the observed neurodevelopmental changes. In this regard, previous studies in rats have also shown that maternal hyperthyroidism results in changes in offspring that suggest accelerated neuronal development [71].
In vitro, chronic exposure to LPS resulted in decreased Purkinje cell arborization. However, while acute LPS exposure in cerebellar cultures in vitro resulted in an increase in D2 activity, as has also been previously reported for astrocytes [22], this increase appears to be transient, observed within the first 24 h following LPS exposure, and was not observed after chronic LPS exposure. Previous work using a co-culture system has shown that an LPS-mediated induction of D2 in glial cells in the presence of T4 can increase neuronal T3-dependent gene expression [24]. Further, induction of hyperthyroidism in pregnant rats leads to accelerated differentiation of neurons [71]. Taken together, this indicates that the transient increase in D2, along with other factors to be yet defined, could play a role in the decreased arborization of Purkinje cells after chronic LPS exposure.
The effect of the LPS challenge is clearly different in SHR and SD rat strains, consistent with other studies that have reported strain differences in response to LPS challenge [72]. This difference may be attributed to the individual, genetically determined specificity of inflammatory response and sensitivity to environmental triggers. Our results show higher levels of the brain oxidative stress marker 3-NT in SHR than in SD rats, as others have reported [73–75], that may be due, at least in part, to a different degree of activation of inflammatory processes between the two strains [76]. In addition to strain specificity of LPS effect, our behavioral and biochemical data indicate that the consequences of perinatal LPS challenge are sex-dependent, in agreement with earlier observations of sex-dependent response to inflammatory challenge [77].
Conclusions
Our data suggest that maternal infection exerts a negative neurodevelopmental impact in the offspring and that the effect appears to be both strain and sex dependent. Impaired motor learning, but not spontaneous motor skills, is most consistently observed following the maternal LPS challenge. Factors that may contribute to altered neonatal behavior include changes in cerebellar oxidative stress, D2 activity, and alterations in gene expression that could be, in part, the result of local changes in thyroid hormone availability. LPS exposure affects Purkinje cell arborization through mechanism(s) yet to be defined that may involve transient, but not chronic, alterations in D2. However, additional studies will be needed to further address the link between perinatal infection and neurodevelopmental abnormalities.
References
Schendel DE, Schuchat A, Thorsen P. Public health issues related to infection in pregnancy and cerebral palsy. Ment Retard Dev Disabilit Res Rev. 2001;8:39–45.
Schendel DE. Infection in pregnancy and cerebral palsy. J Am Med Womens Assooc. 2002;56:105–8.
Ferriero DM. Neonatal brain injury. N Engl J Med. 2004;351:1985–95.
Watson JB, Mednick SA, Huttunen M, Wang X. Prenatal teratogens and the development of adult mental illness. Dev Psychopathol. 1999;11:457–66.
Pearce BD. Schizophrenia and viral infection during neurodevelopment: a focus on mechanisms. Mol Psychiatry. 2001;6:634–46.
Carvey PM, Chang Q, Lipton JW, Ling Z. Prenatal exposure to the bacteritoxin lipopolysaccharide leads to long-term losses of dopamine neurons in offspring: a potential, new model of Parkinson’s disease. Front Biosci. 2003;8:s826–37.
Patterson PH. Maternal infection: window on neuroimmune interactions in fetal brain development and mental illness. Curr Opin Neurobiol. 2002;12:115–8.
Kohmura Y, Kirikae T, Kirikae F, Nakano M, Sato I. Lipopolysaccharide (LPS)-induced intra-uterine fetal death (IUFD) in mice is principally due to maternal cause but not fetal sensitivity to LPS. Microbiol Immunol. 2000;44:897–904.
Urakubo A, Jarskog LF, Lieberman JA, Gilmore JH. Prenatal exposure to maternal infection alters cytokine expression in the placenta, amniotic fluid, and fetal brain. Schizophr Res. 2001;47:27–36.
Gayle DA, Beloosesky R, Desai M, Amidi F, Nunez SE, Ross MG. Maternal LPS induces cytokines in the amniotic fluid and corticotrophin releasing hormone in the fetal rat brain. Am J Regul Integr Comp Physiol. 2004;286:R1024–9.
Bannerman DD, Paape MJ, Hare WR, Sohn EJ. Increased levels of LPS-binding protein in bovine blood and milk following bacterial lipopolysaccharide challenge. J Dairy Sci. 2003;86:312–3137.
Cambonie G, Hirbec H, Michaud M, Kamenka JM, Barnabel G. Prenatal infection obliterates glutamate-related protection against hydroxyl radicals in neonatal rat brain. J Neurosci Res. 2004;75:125–32.
Gayle DA, Ling Z, Tong C, Landers T, Lipton JW, Carvey PM. Lipopolysaccharide (LPS)-induced dopamine cell loss in culture: roles of tumor necrosis factor-alpha, interleukin-1beta, and nitric oxide. Brain Res Dev Brain Res. 2002;133:27–35.
Rohl C, Armbrust E, Herbst E, Jess A, Gulden M, Maser E, et al. Mechanisms involved in the modulation of astroglial resistance to oxidative stress induced by activated microglia: antioxidaive systems, peroxide elimination, radical generation, lipid peroxidation. Neurotox Res. 2010;17:317–31.
Davies KJA. An overview of oxidative stress. IUMB Life. 2000;50:241–4.
Gaillard PJ, de Boer AB, Breimer DD. Pharmacological investigations on LPS-induced permeability changes in the blood–brain barrier in vitro. Microvasc Res. 2003;65:24–31.
Sebai H, Gadacha W, Sani M, Aouani E, Ghanem-Boughanmi N, Ben-Attia M. Protective effect of resveratrol against lipopolysaccharide-induced oxidative stress in rat brain. Brain Inj. 2009;23:1089–94.
McNaught KS, Jenner P. Extracellular accumulation of nitric oxide, hydrogen peroxide, and glutamate in astrocytic cultures following glutathione depletion, complex I inhibition, and/or lipopolysaccharide-induced activation. Biochem Pharmacol. 2000;60:979–88.
Saura J. Microglial cells in astroglial culture; a cautionary note. J Neuroinflammation. 2007;4:26.
Silva JE. Role of circulating thyroid hormones and local mechanisms in determining the concentration of T3 in various tissues. Prog Clin Biol Res. 1983;116:23–44.
Fekete C, Gereben B, Doleschall M, Harney JW, Dora JM, Bianco AC, et al. Lipopolysaccharide induces type 2 iodothyronine deiodinase in the mediobasal hypothalamus: implications for the nonthyroidal illness syndrome. Endocrinology. 2004;145:1649–55.
Lamirand A, Ramauge M, Pierre M, Courtin F. Bacterial lipopolysaccharide induced type 2 deiodinase in cultured rat astrocytes. J Endocrinol. 2011;208:183–92.
Lamirand A, Palud-Mothré S, Ramaugé M, Pierre M, Courtin F. Oxidative stress regulates type 3 deiodinase and type 2 deiodinase in cultured rat astrocytes. Endocrinology. 2008;149:3713–21.
Freitas BC, Gereben B, Castillo M, Kallo I, Zeold A, Egri P, et al. Paracrine signaling by glial cell-derived triiodothyronine activates neuronal gene expression in the rodent brain and human cells. J Clin Invest. 2010;120:2206–17.
Engeland CG, Kavaliers M, Ossenkopp KP. Sex differences in the effects of muramyl dipeptide and lipopolysaccharide on locomotor activity and the development of behavioral tolerance in rats. Pharmacol Biochem Behav. 2003;74:433–47.
Nguyen LT, Ramanathan M, Weinstock-Guttman B, Baier M, Brownscheidle C, Jacobs LD. Sex differences in vitro pro-inflammatory cytokine production from peripheral blood of multiple sclerosis patients. J Neurol Sci. 2009;2003:93–9.
Gourdy P, Araujo LM, Zhu R, Garmy-Susini B, Diem S, Laurell H, et al. Relevance of sexual dimorphism to regulatory T cells; estradiol promotes IFN-(gamma) production by invariant natural killer T cells. Blood. 2005;105:2015–420.
Theas MS, De Laurentis A, Lasaga M, Pisera D, Duvilanski BH, Seilcovich A. Effect of lipopolysaccharide on tumor necrosis factor and prolactin release from rat anterior pituitary cells. Endocrine. 1998;8:241–5.
Candolfi M, Jaita G, Zaldivar V, Zarate S, Pisera D, Seilicovich A. Tumor necrosis factor-alpha-induced nitric oxide restrains the apoptotic response of anterior pituitary cells. Neuroendocrinology. 2004;80:83–91.
Ospina JA, Brevig HN, Krause DN, Duckles SP. Estrogen suppresses IL-1beta-mediated induction of COX-2 pathway in rat cereberal blood vessels. Am J Physiol Heart Circ Physiol. 2004;286:H2010–9.
Nguon K, Baxter MG, Sajdel-Sulkowska EM. Perinatal exposure to polychlorinated biphenyls differentially affects cerebellar development and motor functions in male and female rat neonates. Cerebellum. 2005;4:112–22.
Sajdel-Sulkowska EM, Nguon K, Sulkowski ZL, Rosen GD, Baxter MG. Purkinje cell loss accompanies motor impairment in rats developing at altered gravity. Neuroreport. 2005;16:2037–40.
Sajdel-Sulkowska EM, Lipinski B, Windom H, Audhya T, McGinnis W. Oxidative stress in autism: cerebellar 3-nitrotyrosine levels. Am J Biochem Biotechnol. 2008;4:73–84.
Zavacki AM, Ying H, Christoffolete MA, Aerts G, So E, Harney JW, et al. Type 1 iodothyronine deiodinase is a sensitive marker of peripheral thyroid status in the mouse. Endocrinology. 2005;146:1568–75.
Ibhazehiebo K, Iwasaki T, Shimokawa N, Koibuchi N. 1,2,5,6,9,10-αHexabromocyclododecane (HBCD) impairs thyroid hormone-induced dendrite arborization of Purkinje cells and suppresses thyroid hormone receptor-mediated transcription. Cerebellum. 2011;10:22–31.
Bangalore S, Messerli FH. Of statistical difference: “Trends” towards significance and optimism bias free. J Am Coll Cardiol. 2006;48:1471.
Maier SE, Cramer JA, West JR, Sohrabji F. Alcohol exposure during the first two trimesters equivalent alters granule cell number and neurotropin expression in the developing rat olfactory bulb. J Neurobiol. 1999;41:414–23.
Bellinger FP, Bedi KS, Wilson P, Wilce PA. Ethanol exposure during the third trimester equivalent results in long-lasting decreased synaptic efficacy but not plasticity in the CA1 region of the rat hippocampus. Synapse. 1999;31:51–8.
Goldey ES, Kehn LS, Rehnberg GL, Crofton KM. Effects of developmental hypothyroidism on auditory and motor function in the rat. Toxicol Appl Pharmacol. 1995;135:67–76.
Galton VA, Wood ET, St Germain EA, Withrow CA, Aldrich G, St. Germain GM, et al. Thyroid hormone homeostasis and action in the type 2 deiodinase-deficient rodent brain during development. Endocrinology. 2007;148:3080–8.
Morte B, Ceballos A, Diez D, Grijota-Martinez C, Dumitrescu AM, Di Cosmo C, et al. Thyroid hormone-regulated mouse cerebral cortex genes are differentially dependent on the source of the hormone: a study in monocarboxylate transporter-8- and deiodinase-2-deficient mice. Endocrinology. 2010;151:2381–7.
Ghiani CA, Mattan NS, Nobuta H, Malvar JS, Boles J, Ross MG, Waschek JA, Carpenter EM, Fisher RS, de Vellis J. Early effects of lipopolysaccharide-induced inflammation on foetal brain development in rat. ASN Neuro 2011;3 pii:e00068.
Cui K, Ashdown H, Luheshi GN, Boksa P. Effects of prenatal immune activation on hippocampal neurogenesis in the rat. Schizophr Res. 2009;113:288–97.
Sharangpani A, Takanohashi A, Bell MJ. Caspase activation in fetal rat brain following experimental intrauterine inflammation. Brain Res. 2008;1200:138–45.
Stolp HB, Dziegielewska KM, Ek CJ, Potter AM, Saunders NR. Long-term changes in blood–brain barrier permeability and white matter following prolonged systemic inflammation in early development in the rat. Eur J Neurosci. 2005;22:2805–16.
Poggi SH, Park J, Toso L, Abebe D, Roberson R, Woodard JE, et al. No phenotype associated with established lipopolysaccharide model of cerebral palsy. Am J Obstet Gynecol. 2005;192:727–33.
Lockey AJ, Kavaliers M, Ossenkopp KP. Lipopolysacchaide produces dose-dependent reduction of the acoustic startle response without impairing prepulse inhibition in male rats. Brain Behav Immun. 2009;23:101–7.
Li L, Kosugi I, Han GP, Kawasaki H, Arai Y, Takeshita T, et al. Induction of cytomegalovirus-infected labyrinthitis in newborn mice by lipopolysaccharide: a model for hearing loss in congenital CMV infection. Lab Invest. 2008;88:722–30.
Fan LW, Tien LT, Mitchell HJ, Rhodes PG, Cai Z. Alpha-phenyl-n-tert-butyl-nitrone ameliorates hippocampal injury and improves learning and memory in juvenile rats following neonatal exposure to lipopolysaccharide. Eur J Neurosci. 2008;27:1475–84.
Tanaka S, Ide M, Shibutani T, Ohtaki H, Numazawa S, Shioda S, et al. Lipopolysaccharide-induced microglial activation induces learning and memory deficits without neuronal cell death in rats. J Neurosci Res. 2006;83:557–66.
Abd El-Gawad HM, Khalifa AE. Quercetin, coenzyme Q10, and l-canavanine as protective agents against lipid peroxidation and nitric oxide generation in endotoxin-induced shock in rat brain. Pharmacol Res. 2001;43:257–63.
Li GH, Post J, Koibuchi N, Sajdel-Sulkowska EM. Impact of thyroid hormone deficiency on the developing CNS: cerebellar glial and neuronal protein expression in rat neonates exposed to antithyroid drug propylthiouracil. Cerebellum. 2004;3(2):100–6.
Rabié A, Favre C, Clavel MC, Legrand J. Sequential effects of thyroxine on the developing cerebellum of rats made hypothyroid by propylthiouracil. Brain Res. 1979;161:469–79.
Wajner SM, Goemann IM, Bueno AL, Larsen PR, Maia AL. IL-6 promotes nonthyroidal illness syndrome by blocking thyroxine activation while promoting thyroid hormone inactivation in human cells. J Clin Invest. 2011;121:1834–45.
Forceville X. Effects of high doses of selenium, as sodium selenite, in septic shock patients a placebo-controlled, randomized, double-blind, multi-center phase II study - selenium and sepsis. J Trace Elem Med Biol. 2007;21 Suppl 1:62–5.
Hasebe M, Matsumoto I, Imagawa T, Uehara M. Effects of an anti-thyroid drug, methimazole, administration to rat dams on the cerebellar cortex development in their pups. Int J Devl Neuroscience. 2008;26:409–14.
Laffan EW, Lisciotto CA, Gapp DA, Weldon DA. Development of rotorod performance in normal and congenitally hypothyroid mutant mice. Behavioral and Neural Biology. 1989;52:411–6.
Ng L, Goodyear RJ, Woods CA, Schneider MJ, Diamond E, Richardson GP, et al. Hearing loss and retarded cochlear development in mice lacking type 2 iodothyronine deiodinase. Proc Natl Acad Sci U S A. 2004;101:3474–9.
Oskvig DB, Elkahloun AG, Johnson KR, Phillips TM, Herkenham M. Maternal immune activation by LPS selectively alters specific expression profiles of interneuron migration and oxidative stress in the fetus without triggering a fetal immune response. Brain Behav Immun. 2012;26:623–34.
Cuadrado A, Bernal J, Munoz A. Identification of the mammalian homolog of the splicing regulator suppressor-of-white-apricot as a thyroid hormone regulated gene. Brain Res Mol Brain Res. 1999;71:332–40.
Donai H, Murakami T, Amano T, Sogawa Y, Yamauchi T. Induction and alternative splicing of delta isoform of Ca(2+)/calmodulin-dependent protein kinase II during neural differentiation of P19 embryonal carcinoma cells and during brain development. Brain Res Mol Brain Res. 2000;85:189–99.
Padhi BK, Pelletier G, Williams A, Berndt-Weis L, Yauk C, Bowers WJ, et al. Gene expression profiling in rat cerebellum following in utero and lactational exposure to mixture of methylmercury, polychlorinated biphenyls and organochlorine pesticides. Toxicol Lett. 2008;176:93–103.
Sousa JC, de Escobar GM, Oliveira P, Saraiva MJ, Palha JA. Transthyretin is not necessary for thyroid hormone metabolism in conditions of increased hormone demand. J Endocrinol. 2005;187:257–66.
Richardson SJ. Cell and molecular biology of transthyretin and thyroid hormones. Int Rev Cytol. 2007;258:137–93.
Guan J, Luo Y, Denker BM. Purkinje cell protein-2 (Pcp2) stimulates differentiation in PC12 cells by G-betagamma-mediated activation of Ras and p38 MAPK. Biochem J. 2005;392:389–97.
Anderson GW, Hagen SG, Larson RJ, Strait KA, Schwartz HL, Mariash CN, et al. Purkinje cell protein-2 cis elements mediate repression of T3-dependent transcriptional activation. Mol Cell Endocrinol. 1997;131:79–87.
Koibuchi N, Yamaoka S, Chin WW. Effect of altered thyroid status on neurotrophin gene expression during postnatal development of mouse cerebellum. Thyroid. 2001;11:205–10.
Camboni D, Roskoden T, Schwegler H. Effect of early thyroxine on brain-derived neurotrophic factor mRNA expression and protein amount in the rat medial septum/diagonal band of Broca. Neurosci Lett. 2003;350:141–4.
Tu HM, Legradi G, Bartha T, Salvatore D, Lechan RM, Larsen PR. Regional expression of the 3 iodothyronine deiodinase messenger ribonucleic acid in the rat central nervous system and its regulation by thyroid hormone. Endocrinology. 1999;140:784–90.
Pathak A, Sinha RA, Mohan V, Mitra K, Godbole MM. Maternal thyroid hormone before the onset of fetal thyroid function regulated reelin and downstream signaling affecting neocortical neuronal migration. Cereb Cortex. 2011;21:11–21.
Evans IM, Pickard MR, Sinha AK, Leonard AJ, Sampson DC, Ekins RP. Influence of maternal hyperthyroidism in the rat on the expression of neuronal and astrocytic cytoskeletal proteins in fetal brain. J Endocrinol. 2002;175:597–604.
Zhang Y, Lin X, Koga K, Takahashi K, Linge HM, Mello A, et al. Strain differences in alveolar neutrophil infiltration and macrophage phenotypes in an acute lung inflammation model. Mol Med. 2011;17:780–9.
Kodavanti UP, Schladweiler MC, Ledbetter AD, Ortuno RV, Suffia M, Evansky P, et al. The spontaneously hypertensive rat: an experimental model of sulfur dioxide-induced airways disease. Toxicol Sci. 2006;94:193–205.
Wang X, Desai K, Juurlink BH, de Champlain J, Wu L. Gender-related differences in advanced glycation end products, oxidative stress markers and nitric oxide synthases in rats. Kidney Int. 2006;69:281–7.
Saiki R, Okazaki M, Iwai S, Kumai T, Kobayashi S, Oguchi K. Effects of pioglitazone on increases in visceral fat accumulation and oxidative stress in spontaneously hypertensive hyperlipidemic rats fed a high-fat diet and sucrose solution. J Pharmacol Sci. 2007;105:157–67.
Ballerio R, Gianazza E, Mussoni L, Miller I, Gelosa P, Guerrini U, et al. Gender differences in endothelial function and inflammatory markers along the occurrence of pathological events in stroke-prone rats. Exp Mol Pathol. 2007;82:33–41.
Santos-Galindo M, Acaz-Fonseca E, Bellini MJ, Garcia-Segura LM. Sex differences in the inflammatory response of primary astrocytes to lipopolysaccharide. Biol Sex Differ. 2011;11:2–7.
Acknowledgments
We would like to thank SafeMinds for grants awarded to Dr. Sajdel-Sulkowska and the NIDDK-DK76117 grant awarded to A.M. Zavacki.
Conflict of interest
The authors declare that there are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, M., Sulkowski, Z.L., Parekh, P. et al. Effects of Perinatal Lipopolysaccharide (LPS) Exposure on the Developing Rat Brain; Modeling the Effect of Maternal Infection on the Developing Human CNS. Cerebellum 12, 572–586 (2013). https://doi.org/10.1007/s12311-013-0465-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-013-0465-z