Abstract
Angioimmunoblastic T-cell lymphoma (AILT) represents a subset of T-cell lymphomas but resembles an autoimmune disease in many of its clinical aspects. Despite the phenotype of effector T-cells and high expression of FAS and CTLA-4 receptor molecules, tumor cells fail to undergo apoptosis. We investigated single nucleotide polymorphisms (SNPs) of the FAS and CTLA-4 genes in 94 peripheral T-cell lymphomas. Although allelic frequencies of some FAS SNPs were enriched in AILT cases, none of these occurred at a different frequency compared to healthy individuals. Therefore, SNPs in these genes are not associated with the apoptotic defect and autoimmune phenomena in AILT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Angioimmunoblastic T-cell lymphoma (AILT) is characterized by a systemic lymphoproliferative disorder, generalized lymphadenopathy, and immunologic abnormalities. Originally, it was debated whether the disease should be considered a lymphoma or, alternatively, an abnormal hyperimmune reaction because the fatal outcome was mostly attributed to severe infectious complications rather than to the lymphoproliferation itself. Besides a dispersed cellular infiltrate of atypical lymphoid cells, predominant histological features of AILT include an inflammatory background of plasma cells and eosinophils as well as a proliferation of “arborizing” vessels and follicular dendritic cells. AILT patients frequently exhibit autoimmune phenomena such as cold agglutinins with hemolytic anemia, circulating immune complexes, anti-smooth muscle antibodies, and positive rheumatoid factor [1].
In recent years, clonality analysis in AILT has demonstrated a clonal expansion of T-cells in most cases. Furthermore, studies focused on the immunophenotype of the tumor cells including their correlation with normal T-cell counterparts [2], underlying cytogenetic alterations, and associations with Epstein–Barr virus (EBV) infections and EBV-driven accompanying B-cell proliferations. Based on the expression of CXCL13 and CD10, tumor cells in AILT were correlated to germinal center B-helper T-cells, which represent a population of follicular T-cells constituting a crucial checkpoint for B-cell differentiation and for the maintenance of B-cell tolerance in the periphery [3–5]. However, few approaches have been taken to explain the autoimmune features that are prominent in many AILT patients.
We could recently demonstrate that the neoplastic T-cells in AILT homogeneously correspond to effector cells [2] who are by their natural fate destined to die from apoptosis. This is in contrast to peripheral T-cell lymphomas, not otherwise specified (PTCL-NOS) which correspond to central memory T-cells, a long-living T-cell population that develops by “below threshold” antigen stimulation or when polarizing cytokines are missing [6]. The programmed cell death in effector cells is indispensable for the termination of physiological immune reactions [7], and, interestingly, the tumor cells in AILT express the two molecules FAS and CTLA-4 which are mainly regarded as mediators of apoptosis induction in lymphocytes [8]. Furthermore, the neoplastic T-cells in most of the AILTs express CD10 [9], which is a neutral peptidase expressed in reactive T-cells and some neoplastic B-cells after induction of apoptosis [10–12]. BCL-2, an anti-apoptotic molecule, has been shown to be overexpressed in different B-cell lymphomas [13], while it is consistently negative in AILT [2]. Taken together, these data raise the question, why the neoplastic T-cells in AILT do not undergo apoptosis.
In mouse models, pathological features resembling those in AILT can be induced by introducing mutations of the FAS [14], the CTLA-4 [15], or effector-caspase genes [16], respectively. Moreover, the morphological changes in lymph nodes of patients with an autoimmune lymphoproliferative syndrome (ALPS), a disease caused by hereditary mutations in the FAS gene [17, 18], can mimic the histology of AILT.
FAS, a homotrimeric transmembrane receptor, is an important mediator for the downregulation of immune responses [19] by inducing apoptosis of antigen-primed lymphocytes, including those with autoimmune potential [20]. The gene-encoding FAS contains nine exons [21], and dominant, heterozygous mutations in the FAS gene cause the above-mentioned ALPS phenotype. These patients show a defect in FAS-mediated apoptosis in lymphocytes and a pathological expansion of double negative T-cells expressing an αβ T-cell receptor [22–24]. Impairment of lymphocyte apoptosis, in general, underlies a variety of autoimmune phenomena [22, 25, 26] and predisposes to diverse lymphomas [26]. FAS mutation itself has also been suggested as contributing factor in the etiology of other diseases including autoimmune phenomena [23, 27–37] as well as malignant lymphomas [36] and solid tumors [38]. Several studies described single nucleotide polymorphisms (SNPs) of the FAS gene to be associated with susceptibility to autoimmune diseases [39–45] as well as cancer [46].
CTLA-4 is a negative regulator of T-cell activation [47] which interacts with its ligands CD80/86 and competes—albeit with a much higher affinity—against CD28 [48, 49]. The CTLA-4 gene has been a primary candidate for a genetic susceptibility to autoimmune diseases [50–54] and to a certain extent to non-Hodgkin’s lymphomas [55]. Furthermore, there are indications for a role of CTLA-4 promoter variants in cancer in general [56], and, additionally, one particular polymorphism in the promoter region has been shown to affect the gene expression level of CTLA-4 [57].
SNPs, themselves, do not cause diseases, but they can help to determine the likelihood that someone will develop a particular disease. Most SNPs are silent, i.e., they do not exert a discernible effect on gene function or phenotype. They can, however, have important consequences for the individual susceptibility to a certain disease or to reactions to certain pharmaceuticals. In addition to changes in single genes that affect disease risk, it is thought that particular combinations of SNPs located across multiple genes contribute to a predisposition for developing a certain disease [58]. Allelic variations in promoter regions could potentially affect the gene expression quantitatively or qualitatively by altering transcription factor binding sites or other regulatory domains.
Given that AILT is frequently associated with autoimmune phenomena, and given that the tumor cells of AILT show an effector phenotype but—despite their expression of FAS and CTLA-4—fail to undergo apoptosis, we investigated whether polymorphisms of the FAS and CTLA-4 genes may be responsible for these features.
Materials and methods
Subjects and SNPs
We selected 53 AILT and 41 PTCL-NOS cases from our archives based on the availability of frozen lymph node specimens or peripheral blood lymphocytes. All cases had been diagnosed according to the World Health Organization classification [1] and were characterized by an extensive immunohistochemical marker panel. All of these 94 lymphomas were analyzed for the presence of the five CTLA-4 gene polymorphisms (see below). As controls, we used data of 173 healthy blood donors that were published previously [54].
In addition, a subset of tumors (ten AILT and ten PTCL-NOS cases) was selected randomly for the analysis of the 29 FAS gene polymorphisms and three mutations (see below). As a control cohort, we used the data population PDR90 (NCBI Single Nucleotide Polymorphism Database, dbSNP; http://www.ncbi.nlm.nih.gov/sites/entrez?db=snp) which comprises SNP information in a global population of 90 individuals. To avoid false positive results due to major differences in sample numbers, ten individuals were selected randomly from this database using the “Random Function” in MS Excel. Some of the examined SNPs or mutations were not included in the PDR90 study; thus, control data were obtained from the literature (see references in Table 1). As a general approach, we preferentially chose SNPs which had already been described in correlation with relevant diseases (Table 1). Furthermore, we included one additional SNP that was detected during our sequence analyses but had not been cited in the literature previously. We compared allelic frequencies between AILT, PTCL-NOS, and healthy control samples for all 29 FAS SNPs and three mutations as well as the genotypes for 20 of these SNPs for which control data was available in the dbSNP population PDR90.
DNA extraction and genotyping
Genomic DNA was extracted from frozen lymph node tissue or from peripheral blood lymphocytes using the QIAamp DNA Mini Kit (Qiagen, Hilden, Germany).
29 FAS SNPs and three mutations (Table 1) were analyzed by polymerase chain reaction (PCR) amplification of the exon and intron sections or the promoter and 3′UTR regions, respectively. PCR products were sequenced and compared to Genbank accession numbers D31968.1 and AY450925. PCR- and sequencing-primers used were either according to the indicated literature or newly designed (Table 1). The DNA template, 50 ng in a final volume of 25 μl, was amplified in a reaction mixture containing a final concentration of 0.5 μM primer, 0.2 mM dNTPs (Fermentas, St.Leon-Rot, Germany), and 1× Taq polymerase buffer with 1.5 mM MgCl2 and 0.5 U Taq polymerase (Taq DNA polymerase, recombinant, Invitrogen, Karlsruhe, Germany). PCR reactions were run for 35 cycles in a thermocycler (Mastercycler gradient, Eppendorf, Wesseling-Berzdorf, Germany). After 3 min denaturation at 94°C, each cycle consisted of 45 s at 94°C, 30 s at the assigned annealing temperature and 1 min 30 s at 72°C followed by a final extension step of 10 min at 72°C. PCR products were purified (QIAquick PCR purification kit Qiagen, Hilden, Germany) and aliquots of 7 μl were used for sequencing analysis with 1 μM of the respective primer and 2 μl of BigDye® Terminator v3.1 Cycle Sequencing Kit (Applied Biosystems, Foster City, CA, USA) in a final volume of 10 μl. Samples were analyzed in a 3130 × l Genetic Analyzer (Applied Biosystems, Foster City, CA, USA). We investigated 6 promoter region-, 13 exon-, 10 intron- and three 3′UTR-SNPs. Sequencing peaks at the location of a SNP showed either one peak indicating homozygosity or two equal lower peaks indicating heterozygosity.
The CTLA-4 SNP genotypes and allele frequencies of three promoter-SNPs (−1722T/C, −1661A/G, and −318C/T), one exon-SNP (+49A/G), and one 3′UTR-SNP (CT60A/G) were identified following previously described polymerase chain reaction or restriction fragment length polymorphism protocols [53, 59, 60].
Different nomenclature of SNPs including their annotation is used because polymorphisms were strictly named according to the cited literature.
FAS and CTLA-4 staining by immunohistochemistry
To investigate a possible association between the respective SNPs and the FAS or CTLA-4 expression on the protein level, we performed FAS (Santa Cruz Biotechnology, Santa Cruz, CA, USA) and CTLA-4 (BD Biosciences, San Diego, CA, USA) double fluorescence stains in combination with an antibody directed against the respective T-cell receptor (TCR) Vβ-segment rearranged and expressed by the neoplastic T-cells as previously described [61]. Using this approach, 9/10 AILT and 10/10 PTCL-NOS cases analyzed for FAS SNPs were investigated. Fluorescence images were evaluated using confocal laser scanning microscopy (Leica TCS2, Leica, Bensheim, Germany). One AILT case had to be excluded from the analysis because no antibody against the respective TCRVβ-segment was available.
Statistical analysis
Allele frequencies were compared with the chi-square test. The genotype frequencies between different groups of subjects were compared with chi-square correlation calculated on 2 × 2 contingency tables. A p value less than 0.05 was considered statistically significant. Staining signal intensity was statistically compared with Spearman rank correlation to diagnoses or SNP haplotype on 2 × 2 contingency tables.
SNPs with minor allele frequencies ≥5% were estimated by the expectation maximization algorithm as determined by the Haploview program [62]. Logarithm of the odds ratio scores between 2.2 and 3.6 were considered suggestive [63].
Results
FAS gene polymorphisms
Altogether, we analyzed 29 SNPs and three mutations in the coding and flanking regions of the FAS gene (six promoter-, 13 exon-, ten intron-, three 3′UTR-SNPs; Table 1). One of the SNPs (IVS4+699T>C) was discovered during our evaluation of the data and was found in the dbSNP database; however, this SNP has not been described in the literature before. Overall, we could not detect SNPs at FAS splice sites among our sequences.
Three gene loci (−691t>c, IVS4+699T>C, IVS7+312C>T) showed differences in allelic frequencies when AILT and PTCL-NOS cases were compared; however, these SNPs did not differ statistically in their allelic frequency values when compared to the control cases. For four SNPs (IVS2+176C>T, IVS4+699T>C, A/T(735)G/C, c.699(+82)c>g), we were able to detect differences in their genotype frequencies when all three groups were compared (Tables 2 and 3, P values in bold type).
Cluster analysis of all three groups for the combined genotypes of the previously mentioned 20 SNPs revealed one subgroup with a high degree of similarities which contained 7/10 of the AILT cases (Fig. 1). The remaining three AILT cases were more closely linked to PTCL-NOS or control cases.
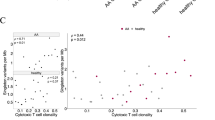
To detect a possible effect of the FAS SNP in the promoter region (−691t>c) on gene expression in AILT cases, FAS-staining was performed in 10/10 PTCL-NOS and 9/10 AILT. In general, all AILT tumors showed a significantly stronger FAS expression compared to most of the PTCL-NOS (Table 4 and Fig. 2). Performing cluster analysis of FAS expression and the −691t>c genotype, all AILT and two PTCL-NOS cases shared the same combination of parameters (data not shown).
Representative fluorescence double stainings of CTLA4/TCRVβ and FAS/TCRVβ in PTCL-NOS and AILT. Upper panel: The tumor cells in PTCL-NOS (case 10) do not coexpress CTLA4 (a: green Vβ 2, red CTLA4) and FAS (b: green Vβ 2, red FAS). Lower panel: The tumor cells in AILT (case 17) show a coexpression of CTLA4 (c: green Vβ 5.1, red CTLA4) and FAS (d: green Vβ 5.1, red FAS)
Because complex disease phenotypes including autoimmunity may be influenced by polymorphisms at multiple gene loci presumably related to expression levels or the ability of variant protein domains to interact with functional partners or substrates, we searched for a potential risk related to haplotypic differences by performing haplotype and linkage disequilibrium (LD) analysis. We found LD among several SNPs with minor allele frequency ≥5% (data not shown). However, no haplotype blocks emerged.
CTLA-4 gene polymorphisms
We found no significant association of any of the studied CTLA-4 SNPs with AILT, PTCL-NOS, and control individuals comparing allelic frequencies or genotypes (Tables 5 and 6). Likewise, cluster analysis of AILT, PTCL-NOS, and controls for the combined genotypes of the CTLA-4 SNPs revealed no subgroups (data not shown).
The eight AILT cases that could be investigated showed a significantly stronger CTLA-4 expression on the protein level compared to the six PTCL-NOS cases investigated (Table 4 and Fig. 2). Performing cluster analysis of CTLA-4 expression and the three CTLA-4 promoter SNP genotypes, no subgroups were detected that included a significant subset of one of the lymphoma entities. Comparing CTLA-4 expression with the cluster analysis performed on the basis of all CTLA-4 genotypes and all cases, a completely heterogeneous pattern emerged (data not shown).
Discussion
Tumor cells of AILT show an effector phenotype, which is—in the non-malignant counterpart—associated with a propensity to undergo apoptosis. In view of the findings that tumor cells in AILT patients highly express the proapoptotic molecules FAS and CTLA-4 and are negative for BCL2, a potent inhibitor of apoptosis, we wondered if certain SNPs and/or mutations of the FAS and CTLA-4 genes may be associated with the failure of the tumor cells to undergo apoptosis. However, no such associations could be uncovered in this study. Although six SNPs of the FAS gene showed a differential distribution between the AILT and PTCL-NOS subgroups, none of the SNPs appeared to be statistically enriched in comparison to a normal control population. These six SNPs include the SNP -691T>C, which is located in the promoter region of the FAS gene and IVS2+176C>T, which is a silent SNP in exon 2. The remaining four SNPs are located in various introns of the FAS gene. Comparing these results with data from the literature, three SNPs were associated with certain autoimmune diseases, such as multiple sclerosis (A/T(735)G/C) or Sjögren’s syndrome (c.699(+82)c>g and IVS2+176C>T) in previous reports [42, 43].
To investigate whether the SNP −691T>C located in the promoter region could potentially lead to a modified transcription factor binding site and therefore be of relevance for the expression level of the FAS gene, we analyzed the FAS expression of the neoplastic T-cells in AILT and PTCL-NOS by immunohistochemistry. As shown in Table 4 and in the representative images of Fig. 2, FAS staining in AILT and PTCL-NOS cases revealed a significant difference with a significantly higher expression of FAS among AILT cases. Moreover, cluster analysis including only the status of the promoter SNP and the expression data showed a correlation between this SNP and the FAS expression in AILT, with all AILT showing the same genotype linked to the expression pattern, while PTCL-NOS cases revealed a heterogeneous pattern regarding genotype and FAS expression. Interestingly, two of the three FAS+ PTCL-NOS cases shared the genotype characteristic of AILT, while five PTCL-NOS cases with the same genotype were FAS−. In contrast, the remaining FAS+ PTCL-NOS case revealed a completely different genotype.
We next addressed the question if the promoter SNP −691T>C could lead to changes in transcription factor binding sites. Because no reports exist in the literature to date, we compared the respective sequences with a transcription factor database (http://www.cbrc.jp/research/db/TFSEARCH.html). Potential binding sites were found for AML-1a with a score of 83.4 for allele T and for c-Myc with a score of 80.9 for binding only allele C, which could allow the speculation that in AILT, c-Myc does not interact with this location.
Are the quantitative differences in FAS expression between AILT and PTCL-NOS subgroups attributable to underlying differences in SNP genotypes? We believe that this scenario is highly unlikely. First, SNP distributions in AILT and PTCL-NOS cases did not show statistically significant differences to their occurrence in normal controls. Second, tumor cells in AILT and PTCL-NOS correspond to different subsets of normal T-cell populations [2], which show physiological variations in their FAS expression. Therefore, the difference in FAS expression likely only reflects the distinct expression levels of the physiological counterparts. Future studies will, therefore, have to address the exact quantification of the FAS expression across various physiological differentiation states of T-cells. In addition, DNA-binding studies with AML-1a and c-Myc and the different promoter variants could shed light on the question if and to what extent these transcription factors may play a role in the regulation of FAS expression.
Because certain SNPs in the CTLA-4 gene can lead to functional changes, such as modified promoter activity and lower CTLA-4 surface expression, inefficient processing led to reduced control of T-cell proliferation and a reduced soluble CTLA-4 isoform [51, 57, 64, 65], and because some of these SNPs have been associated with a broad variety of autoimmune diseases [66], we studied CTLA-4 SNPs in AILT and PTCL-NOS cases. However, the statistical evaluation of allelic frequencies and genotypes yielded no correlation between the presence of a CTLA-4 SNP with either the AILT or PTCL-NOS subgroup. Additionally, cluster analysis of genotypes also revealed no subgroups. Even though CTLA-4 expression significantly differed between AILT and PTCL-NOS cases, this again is likely to be explained by the distinct differentiation states of the normal counterparts of the neoplastic populations in AILT and PTCL-NOS. This is supported by comparing CTLA-4 expression to promoter SNP genotypes and the cluster analysis of all five genotypes, which did not show any correlation.
Interestingly, in another study, a difference in the occurrence of the +49AA genotype of the CTLA-4 gene was described between non-Hodgkin’s lymphoma patients and controls [55]. Four of 44 cases in this study were T-cell lymphomas, but, unfortunately, the authors did not provide detailed information on this subset. Thus, results between our and the previously mentioned study cannot be compared at the present time.
In summary, our study provides evidence that SNPs or mutations of the FAS and CTLA-4 genes are not responsible for the failure of the tumor cells in AILT patients to undergo apoptosis and for the accompanying autoimmune phenomena. Future studies will have to unravel the mechanism by which the neoplastic population in AILT that appears to have an effector T-cell phenotype and is equipped with high expression of the pro-apoptotic molecules FAS and CTLA-4 circumvent the induction of cell death.
References
Jaffe ES, Harris NL, Stein H et al (2001) Mature T-cell and NK-cell neoplasms. In: Tumours of Haematopoietic andLymphoid Tissues. IARC, Lyon
Geissinger E, Bonzheim I, Krenacs L et al (2006) Nodal peripheral T-cell lymphomas correspond to distinct mature T-cell populations. J Pathol 210:172–180
Grogg KL, Attygalle AD, Macon WR et al (2005) Angioimmunoblastic T-cell lymphoma: a neoplasm of germinal-center T-helper cells? Blood 106:1501–1502
Dupuis J, Boye K, Martin N et al (2006) Expression of CXCL13 by neoplastic cells in angioimmunoblastic T-cell lymphoma (AITL): a new diagnostic marker providing evidence that AITL derives from follicular helper T cells. Am J Surg Pathol 30:490–494
Vinuesa CG, Tangye SG, Moser B et al (2005) Follicular B helper T cells in antibody responses and autoimmunity. Nat Rev Immunol 5:853–865
Sallusto F, Geginat JLanzavecchia A (2004) Central memory and effector memory T cell subsets: function, generation, and maintenance. Annu Rev Immunol 22:745–763
Green DR, Droin NPinkoski M (2003) Activation-induced cell death in T cells. Immunol Rev 193:70–81
Rudin CM, Van Dongen JThompson CB (1996) Apoptotic signaling in lymphocytes. Curr Opin Hematol 3:35–40
Attygalle A, Al-Jehani R, Diss TC et al (2002) Neoplastic T cells in angioimmunoblastic T-cell lymphoma express CD10. Blood 99:627–633
Cutrona G, Leanza N, Ulivi M et al (1999) Expression of CD10 by human T cells that undergo apoptosis both in vitro and in vivo. Blood 94:3067–3076
Cutrona GFerrarini M (2001) Expression of CD10 by human T cells that undergo apoptosis both in vitro and in vivo. Blood 97:2528
Cutrona G, Tasso P, Dono M et al (2002) CD10 is a marker for cycling cells with propensity to apoptosis in childhood ALL. Br J Cancer 86:1776–1785
Lai R, Arber DA, Chang KL et al (1998) Frequency of bcl-2 expression in non-Hodgkin’s lymphoma: a study of 778 cases with comparison of marginal zone lymphoma and monocytoid B-cell hyperplasia. Mod Pathol 11:864–869
Choi Y, Ramnath VR, Eaton AS et al (1999) Expression in transgenic mice of dominant interfering Fas mutations: a model for human autoimmune lymphoproliferative syndrome. Clin Immunol 93:34–45
Masteller EL, Chuang E, Mullen AC et al (2000) Structural analysis of CTLA-4 function in vivo. J Immunol 164:5319–5327
Oliveira JBFleisher T (2004) Autoimmune lymphoproliferative syndrome. Curr Opin Allergy Clin Immunol 4:497–503
Strobel P, Nanan R, Gattenlohner S et al (1999) Reversible monoclonal lymphadenopathy in autoimmune lymphoproliferative syndrome with functional FAS (CD95/APO-1) deficiency. Am J Surg Pathol 23:829–837
Straus SE, Jaffe ES, Puck JM et al (2001) The development of lymphomas in families with autoimmune lymphoproliferative syndrome with germline Fas mutations and defective lymphocyte apoptosis. Blood 98:194–200
Depraetere VGolstein P (1997) Fas and other cell death signaling pathways. Semin Immunol 9:93–107
Lenardo MJ (1996) Fas and the art of lymphocyte maintenance. J Exp Med 183:721–724
Behrmann I, Walczak HKrammer PH (1994) Structure of the human APO-1 gene. Eur J Immunol 24:3057–3062
Fisher GH, Rosenberg FJ, Straus SE et al (1995) Dominant interfering Fas gene mutations impair apoptosis in a human autoimmune lymphoproliferative syndrome. Cell 81:935–946
Rieux-Laucat F, Le Deist F, Hivroz C et al (1995) Mutations in Fas associated with human lymphoproliferative syndrome and autoimmunity. Science 268:1347–1349
Jackson CE, Fischer RE, Hsu AP et al (1999) Autoimmune lymphoproliferative syndrome with defective Fas: genotype influences penetrance. Am J Hum Genet 64:1002–1014
Sneller MC, Straus SE, Jaffe ES et al (1992) A novel lymphoproliferative/autoimmune syndrome resembling murine lpr/gld disease. J Clin Invest 90:334–341
Puck JMSneller MC (1997) ALPS: an autoimmune human lymphoproliferative syndrome associated with abnormal lymphocyte apoptosis. Semin Immunol 9:77–84
Savinov AY, Tcherepanov A, Green EA et al (2003) Contribution of Fas to diabetes development. Proc Natl Acad Sci U S A 100:628–632
Pensati L, Costanzo A, Ianni A et al (1997) Fas/Apo1 mutations and autoimmune lymphoproliferative syndrome in a patient with type 2 autoimmune hepatitis. Gastroenterology 113:1384–1389
Giordano C, Stassi G, De Maria R et al (1997) Potential involvement of Fas and its ligand in the pathogenesis of Hashimoto’s thyroiditis. Science 275:960–963
Ma Y, Liu H, Tu-Rapp H et al (2004) Fas ligation on macrophages enhances IL-1R1-Toll-like receptor 4 signaling and promotes chronic inflammation. Nat Immunol 5:380–387
Jayaraman S, Castro M, O’Sullivan M et al (1999) Resistance to Fas-mediated T cell apoptosis in asthma. J Immunol 162:1717–1722
Maric I, Pittaluga S, Dale JK et al (2005) Histologic features of sinus histiocytosis with massive lymphadenopathy in patients with autoimmune lymphoproliferative syndrome. Am J Surg Pathol 29:903–911
Teachey DT, Manno CS, Axsom KM et al. (2005) Unmasking Evans syndrome: T-cell phenotype and apoptotic response reveal autoimmune lymphoproliferative syndrome (ALPS). Blood 105:2443–2448
Landowski TH, Qu N, Buyuksal I et al (1997) Mutations in the Fas antigen in patients with multiple myeloma. Blood 90:4266–4270
Beltinger C, Kurz E, Bohler T et al (1998) CD95 (APO-1/Fas) mutations in childhood T-lineage acute lymphoblastic leukemia. Blood 91:3943–3951
Gronbaek K, Straten PT, Ralfkiaer E et al (1998) Somatic Fas mutations in non-Hodgkin’s lymphoma: association with extranodal disease and autoimmunity. Blood 92:3018–3024
Shin MS, Park WS, Kim SY et al (1999) Alterations of Fas (Apo-1/CD95) gene in cutaneous malignant melanoma. Am J Pathol 154:1785–1791
Mullauer L, Gruber P, Sebinger D et al (2001) Mutations in apoptosis genes: a pathogenetic factor for human disease. Mutat Res 488:211–231
Kantarci OH, Hebrink DD, Achenbach SJ et al (2004) CD95 polymorphisms are associated with susceptibility to MS in women. A population-based study of CD95 and CD95L in MS. J Neuroimmunol 146:162–170
Geleijns K, Laman JD, van Rijs W et al (2005) Fas polymorphisms are associated with the presence of anti-ganglioside antibodies in Guillain–Barre syndrome. J Neuroimmunol 161:183–189
Nolsoe RL, Kelly JA, Pociot F et al (2005) Functional promoter haplotypes of the human FAS gene are associated with the phenotype of SLE characterized by thrombocytopenia. Genes Immun 6:699–706
Lucas M, Zayas MD, De Costa AF et al (2004) A study of promoter and intronic markers of ApoI/Fas gene and the interaction with Fas ligand in relapsing multiple sclerosis. Eur Neurol 52:12–17
Bolstad AI, Wargelius A, Nakken B et al (2000) Fas and Fas ligand gene polymorphisms in primary Sjogren’s syndrome. J Rheumatol 27:2397–2405
Kanemitsu S, Ihara K, Saifddin A et al (2002) A functional polymorphism in fas (CD95/APO-1) gene promoter associated with systemic lupus erythematosus. J Rheumatol 29:1183–1188
Horiuchi T, Nishizaka H, Yasunaga S et al (1999) Association of Fas/APO-1 gene polymorphism with systemic lupus erythematosus in Japanese. Rheumatology (Oxford) 38:516–520
Lai HC, Sytwu HK, Sun CA et al (2003) Single nucleotide polymorphism at Fas promoter is associated with cervical carcinogenesis. Int J Cancer 103:221–225
Carreno BM, Bennett F, Chau TA et al (2000) CTLA-4 (CD152) can inhibit T cell activation by two different mechanisms depending on its level of cell surface expression. J Immunol 165:1352–1356
Alegre ML, Frauwirth KAThompson CB (2001) T-cell regulation by CD28 and CTLA-4. Nat Rev Immunol 1:220–228
Sharpe AH, Freeman GJ (2002) The B7-CD28 superfamily. Nat Rev Immunol 2:116–126
Nistico L, Buzzetti R, Pritchard LE et al (1996) The CTLA-4 gene region of chromosome 2q33 is linked to, and associated with, type 1 diabetes. Belgian Diabetes Registry. Hum Mol Genet 5:1075–1080
Ueda H, Howson JM, Esposito L et al (2003) Association of the T-cell regulatory gene CTLA4 with susceptibility to autoimmune disease. Nature 423:506–511
Braun J, Donner H, Siegmund T et al (1998) CTLA-4 promoter variants in patients with Graves’ disease and Hashimoto’s thyroiditis. Tissue Antigens 51:563–566
Harbo HF, Celius EG, Vartdal F et al (1999) CTLA4 promoter and exon 1 dimorphisms in multiple sclerosis. Tissue Antigens 53:106–110
Chuang WY, Strobel P, Gold R et al (2005) A CTLA4 high genotype is associated with myasthenia gravis in thymoma patients. Ann Neurol 58:644–648
Monne M, Piras G, Palmas A et al (2004) Cytotoxic T-lymphocyte antigen-4 (CTLA-4) gene polymorphism and susceptibility to non-Hodgkin’s lymphoma. Am J Hematol 76:14–18
Erfani N, Razmkhah M, Talei AR et al (2006) Cytotoxic T lymphocyte antigen-4 promoter variants in breast cancer. Cancer Genet Cytogenet 165:114–120
Ligers A, Teleshova N, Masterman T et al (2001) CTLA-4 gene expression is influenced by promoter and exon 1 polymorphisms. Genes Immun 2:145–152
Shastry BS (2002) SNP alleles in human disease and evolution. J Hum Genet 47:561–566
Torres B, Aguilar F, Franco E et al (2004) Association of the CT60 marker of the CTLA4 gene with systemic lupus erythematosus. Arthritis Rheum 50:2211–2215
Hudson LL, Rocca K, Song YW et al (2002) CTLA-4 gene polymorphisms in systemic lupus erythematosus: a highly significant association with a determinant in the promoter region. Hum Genet 111:452–455
Geissinger E, Bonzheim I, Krenacs L et al (2005) Identification of the tumor cells in peripheral T-cell lymphomas by combined polymerase chain reaction-based T-cell receptor beta spectrotyping and immunohistological detection with T-cell receptor beta chain variable region segment-specific antibodies. J Mol Diagn 7:455–464
Barrett JC, Fry B, Maller J et al (2005) Haploview: analysis and visualization of LD and haplotype maps. Bioinformatics 21:263–265
Lander EKruglyak L (1995) Genetic dissection of complex traits: guidelines for interpreting and reporting linkage results. Nat Genet 11:241–247
Anjos S, Nguyen A, Ounissi-Benkalha H et al (2002) A common autoimmunity predisposing signal peptide variant of the cytotoxic T-lymphocyte antigen 4 results in inefficient glycosylation of the susceptibility allele. J Biol Chem 277:46478–46486
Kouki T, Sawai Y, Gardine CA et al (2000) CTLA-4 gene polymorphism at position 49 in exon 1 reduces the inhibitory function of CTLA-4 and contributes to the pathogenesis of Graves’ disease. J Immunol 165:6606–6611
Gough SC, Walker LSSansom DM (2005) CTLA4 gene polymorphism and autoimmunity. Immunol Rev 204:102–115
Niemela JE, Hsu AP, Fleisher TA et al (2006) Single nucleotide polymorphisms in the apoptosis receptor gene TNFRSF6. Mol Cell Probes 20:21–26
Nolsoe RL, Kristiansen OP, Sangthongpitag K et al (2000) Complete molecular scanning of the human Fas gene: mutational analysis and linkage studies in families with type I diabetes mellitus. The Danish Study Group of Diabetes in Childhood and The Danish IDDM Epidemiology and Genetics Group. Diabetologia 43:800–808
Do B, Lossos IS, Thorstenson Y et al. (2003) Analysis of FAS (CD95) gene mutations in higher-grade transformation of follicle center lymphoma. Leuk Lymphoma 44:1317–1323
Acknowledgements
We thank PD Dr. Alois Palmetshofer for critical discussion of our results.
P.S. and A.M. were supported by European Union grant LSHB-CT-2003-503410 (Euro-Thymaide) and grant 10-1740 of the Deutsche Krebshilfe.
Ethical standards
Ethics approval for the entire study was obtained from the ethics committee, Medical Faculty, University of Würzburg, Germany. In general, the procedures followed the Helsinki Declaration of 1975. Informed patient consent was not required by the ethics committee because diagnostic specimens can be used for research purposes after anonymization.
Author information
Authors and Affiliations
Corresponding author
Additional information
Irina Bonzheim and Eva Geissinger contributed equally to the work.
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License ( https://creativecommons.org/licenses/by-nc/2.0 ), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Bonzheim, I., Geissinger, E., Chuang, WY. et al. Analysis of single nucleotide polymorphisms in the FAS and CTLA-4 genes of peripheral T-cell lymphomas. J Hematopathol 1, 11–21 (2008). https://doi.org/10.1007/s12308-008-0003-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12308-008-0003-y