Abstract
Chronic cerebrovascular hypoperfusion is a high-risk factor for Alzheimer’s disease (AD) as it is conducive to beta amyloid (Aβ) over-production. Brain-derived neurotrophic factor (BDNF) is a member of the neurotrophin family widely expressed in the central nervous system. The structure of the rat BDNF gene is complex, consisting of eight non-coding exons (I–VIII) and one coding exon (IX). The BDNF gene is transcribed from multiple promoters located upstream of different 5′ non-coding exons to produce a heterogeneous population of BDNF mRNAs. S-adenosylmethionine (SAM) produced in the methionine cycle is the primary methyl donor and the precursor of glutathione. In this study, a cerebrovascular hypoperfusion rat model and an Aβ intrahippocampal injection rat model were used to explore the expression profiles of all BDNF transcripts in the hippocampus with chronic cerebrovascular hypoperfusion or Aβ injection as well as with SAM treatment. We found that the BDNF mRNAs and protein were down-regulated in the hippocampus undergoing chronic cerebrovascular hypoperfusion as well as Aβ treatment, and BDNF exons IV and VI played key roles. SAM improved the low BDNF expression following these insults mainly through exons IV and VI. These results suggest that SAM plays a neuroprotective role by increasing the expression of endogenous BDNF and could be a potential target for AD therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is the most common neurodegenerative disease of the central nervous system and the causes are not very clear. It is well known that beta amyloid (Aβ) is the main component of senile plaques, one of the pathological features of AD. Aβ, derived from beta amyloid precursor protein, is a strong inducer of oxidative stress that results in oxidative damage of membranes, proteins, lipids, and nucleic acids [1]. Meanwhile, glial cells can be activated by Aβ to release various inflammatory mediators, leading to neuronal degeneration and necrosis [2, 3]. Although this amyloid hypothesis has recently been challenged, the fact that Aβ plays important roles in neuronal damage, especially in the early stage of AD, cannot be ignored. A persistent decline of cerebral blood flow due to neurovascular dysfunction is associated with cognitive decline, and is a high-risk factor for AD. Evidence from epidemiological, neuroimaging, and clinical studies suggests that sporadic AD is a vascular disorder caused by impaired cerebral perfusion [4]. Overproduction of Aβ, progressive spatial memory deficits, and hyperphosphorylation of tau, as well as dysregulation of synaptic proteins are also found in rat brains undergoing cerebral hypoperfusion [5, 6].
Brain derived neurotrophic factor (BDNF) is an important member of the neurotrophin family, and is widely expressed in the central nervous system. It plays important roles in learning and memory, maintaining the functions of neurons and protecting them from diverse injuries such as cerebrovascular hypoperfusion or Aβ accumulation. The structure of the rat BDNF gene is complex. It consists of at least eight 5′ non-coding exons (I–VIII) and one 3′ coding exon (IX), each of which has an individual promoter region [7, 8]. This special gene structure determines that different promoters may affect its transcription. External stimulation can regulate the different promoters of BDNF non-coding exons, causing alterations in the expression of BDNF mRNAs and protein [9, 10]. Accumulating evidence has demonstrated that BDNF is down-regulated in AD patients and rodent models of AD. In vivo and in vitro studies have shown that Aβ can inhibit the expression of BDNF and intracellular transport through the oxidative stress-related signaling pathway [11]. Our previous studies revealed that chronic cerebrovascular hypoperfusion can reduce BDNF expression in cortex and the hippocampus [5].
S-adenosylmethionine (SAM) produced in homocysteine metabolism is the primary methyl donor and the precursor of glutathione (GSH). As a critical antioxidant, SAM is mainly used in the treatment of liver disease and arthritis [12, 13]. Animal experiments and clinical studies suggest that SAM can be used for the treatment of nervous system diseases, since it can pass through the blood-brain barrier (BBB). Recently, curative effects of SAM on depression, drug addiction, and cognitive dysfunction have been reported [14–16]. Significantly low SAM has been found in the cerebrospinal fluid of AD patients [17]. SAM may be beneficial for improving spatial memory in patients suffering from many types of dementia, including AD. Furthermore, SAM supplementation reduces the progress of AD-like features induced by a vitamin B-deficient diet in mice by preventing oxidative stress and regulating GSH metabolism [18, 19]. SAM can improve spatial learning and memory through the up-regulation of BDNF in the hippocampus of rats undergoing chronic cerebral hypoperfusion [5, 18].
In the present study, rat models of cerebrovascular hypoperfusion (bilateral carotid occlusion) and the intrahippocampal injection of Aβ were used to explore their effects on the expression profiles of all BDNF transcripts.
Materials and Methods
Animals
Adult (12 weeks old) male Sprague-Dawley rats (Beijing Vital River Experimental Animal Technology Co., Ltd, Beijing, China) were used for all experiments. All the animals were housed under standard conditions in the Experimental Animal Center of Capital Medical University. All experimental procedures were approved by the Animal Care and Use Committee of Capital Medical University and complied with the Guide for the Care and Use of Laboratory Animals formulated by the Ministry of Science and Technology of China.
Two-Vessel Occlusion Surgery and SAM Treatment
The rats were randomly divided into sham, experimental, and SAM-treated groups. Animals in the experimental group were subjected to permanent bilateral common carotid occlusion (two-vessel occlusion, 2-VO) carried out as previously described [20]. The animals in the sham group received the same surgery except for carotid artery ligation. Two days after 2-VO surgery, the rats received an intraperitoneal injection of either SAM (10 mg/kg, Yuanye Bio, Shanghai, China) or saline every other day for 90 days.
Intrahippocampal Aβ Injection and SAM Treatment
Aβ1-42 (China Peptides Co., Ltd, Shanghai, China) was aggregated by incubation in distilled water (20 mg/mL) at 37 °C for 72 h, and diluted to the final concentration with saline immediately before surgery. The rats were anaesthetized by intraperitoneal injection of chloral hydrate (350 mg/kg) and microcannulae were stereotaxically implanted into the bilateral hippocampus (4.3 mm posterior to bregma; 3.5 mm lateral to midline; and 3.3 mm ventral to bregma). Aβ1-42 (20 μg/5 μL) or the same volume of saline was injected using a 10 μL stepper-motorized micro-syringe (Pigeon, Shanghai, China) at a rate of 1 μL/min. Then the rats received an intraperitoneal injection of either SAM (10 mg/kg, Yuanye Bio, Shanghai, China) or saline each day for 6 weeks after surgery.
RT-PCR
Total RNA was extracted from the hippocampus using an RNAsimple Total RNA kit (TIANGEN, Beijing, China) and cDNA was generated from 2 μg of total RNA using a FastQuant RT kit (Tiangen, Beijing, China). The RT-PCR reaction was performed at 95 °C for 5 min, followed by 45 cycles of 95 °C for 30 s, 60 °C for 30 s and 72 °C for 60 s, and the products were analyzed in 1.5% agarose gel containing ethidium bromide. DNA bands were photographed using Alpha FluorChem FC3 (ProteinSimple, CA). The optical density of DNA bands was quantified using ImageJ 16.0 (NIH, Bethesda, MD). The primer sequences are listed in Table 1.
Quantitative Real-Time PCR (q-PCR)
RNA was extracted from the hippocampus with an RNAsimple Total RNA kit (Tiangen, Beijing, China). Reverse transcription was performed using a FastQuant RT kit (Tiangen, Beijing, China). The q-PCR reaction was performed at 95 °C for 15 min, followed by 45 cycles of 95 °C for 10 s, 55 °C for 20 s and 72 °C for 20 s, and the melting curve was analyzed. Each q-PCR was conducted in triplicate in a CFX96 Touch system (Bio-Rad, CA). Data were analyzed using the 2−△△Ct method with glyceraldehyde-3-phosphate dehydrogenase (GAPDH) as normalization control. The primer sequences are listed in Table 2.
Western Blot Analysis
Hippocampal tissues were dissected out from each group and homogenized in lysis buffer containing 50 mmol/L Tris-HCl (pH 7.5), 150 mmol/L NaCl, 1% NP-40, 0.1% SDS, and protease inhibitor cocktail (Pplygen, Beijing, China). Routine procedures were carried out as described previously [21]. Primary rabbit polyclonal BDNF antibody (1:1000, Abcam, Cambridge, MA) and mouse monoclonal β-actin (1:500, ZSGB-BIO, Beijing, China) were used. Second peroxidase-conjugated AffiniPure goat anti-mouse IgG antibody (1:5000, ZSGB-BIO) and peroxidase-conjugated AffiniPure goat anti-rabbit IgG antibody (1:5000, ZSGB-BIO) were used. Imaging of bands was carried out using Alpha FluorChem FC3 (ProteinSimple, CA) and quantified with ImageJ 16.0 (NIH, Bethesda, MD).
Statistical Analysis
Statistical analysis was performed using SPSS software, version 16.0 (SPSS Inc., Chicago, IL). Two-tailed, independent samples t-tests or variance (ANOVA) tests with LSD post hoc tests were used. P <0.05 was considered as statistically significant.
Results
Expression Profiles of All BDNF Transcripts in Rat Hippocampus
The rat BDNF transcripts contained exons I–IX. We first tested the expression profiles of all BDNF transcripts in rat hippocampus by semi-quantitative RT-PCR, and found low mRNA levels of exons I, II, III, and VIII (Fig. 1). BDNF exon II mRNA splice variants A, B, and C were expressed at similar levels. The mRNA levels of exons IV and VI were 4–6-fold those of exons I, II, III, and VIII. Since exons V and VII were expressed at rather low levels, we were unable to detect their mRNAs by RT-PCR.
Expression Profiles of All BDNF mRNAs in the Hippocampus of Rats undergoing Chronic Cerebrovascular Hypoperfusion
To explore the effect of chronic cerebrovascular hypoperfusion on BDNF transcripts, we examined the expression of BDNF exon mRNAs by q-PCR in rat hippocampus after surgery (Fig. 2A–D). Only exon IIC mRNA was increased by 21% 1 day after surgery (Fig. 2A). Exon IIB mRNA increased by 53%, exon IV mRNA by 36%, and exon IX mRNA by 43% compared with the sham group on day 7 after surgery (Fig. 2B). However, on day 30 after surgery, exon I mRNA had increased by 41%, while exon IV mRNA had decreased by 31%. No significant change of exon IX mRNA was found (Fig. 2C). In the late stage of cerebrovascular hypoperfusion, most exons showed significantly reduced mRNA levels on day 90 after surgery [exon I (−47%), exon IIB (−41%), exon IIC (−42%), exon III (−43%), exon IV (−36%), exon VI (−44%), and exon IX (−45%)] (Fig. 2D). These q-PCR results indicated that the expression of BDNF mRNAs increased at the early stage of acute ischemia and then gradually decreased. Meanwhile, this result was confirmed by BDNF protein expression tested by western blot (Fig. 2E). Among all BDNF exons, the IV transcript seemed to be the most strongly induced in response to cerebrovascular hypoperfusion.
Expression of BDNF exon mRNAs and protein in rat hippocampus after 2-VO surgery. A–D q-PCR analysis of all BDNF exon mRNA levels 1 (A), 7 (B), 30 (C), and 90 days (D) after surgery. E BDNF protein assessed by western blot. The data were normalized to β-actin and are expressed as mean ± SD (n = 3–6). *P <0.05; **P <0.01 vs sham group.
SAM Improves the Expression of BDNF in the Hippocampus of Rats undergoing Chronic Cerebrovascular Hypoperfusion
Our previous study revealed that SAM improves spatial memory deficits in rats 90 days after 2-VO surgery [5], so the time-point of 90 days was selected to test the effect of SAM treatment on the expression of BDNF exon mRNAs. SAM treatment reversed the low mRNA expression of several BDNF exons induced by chronic cerebrovascular hypoperfusion. Compared with the 2-VO group, exon I mRNA was increased by 47%, exon IIC by 46%, exon IV by 107%, exon VI by 52%, and exon IX by 92% after SAM treatment (Fig. 3A). Western blot analysis also confirmed this effect (Fig. 3B). These results suggested that SAM can enhance the expression of BDNF mRNAs that are inhibited during chronic cerebrovascular hypoperfusion, and BDNF exon IV might play an important role.
Effects of SAM on the expression of BDNF exon mRNAs and protein in the hippocampus of rats undergoing chronic cerebrovascular hypoperfusion. A q-PCR analysis of BDNF mRNAs 90 days after SAM treatment. B Western blot analysis of BDNF. The data, normalized to β-actin, are shown as mean ± SD (n = 3–6). *P <0.05, **P <0.01 vs sham group; # P <0.05, ## P <0.01 vs 2-VO group.
SAM Reversed the Reduction of BDNF Exon mRNAs Caused by Aβ
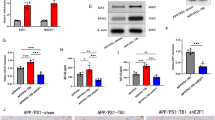
Chronic cerebrovascular hypoperfusion can cause progressive spatial memory deficits and Aβ accumulation in the brain is accompanied by BDNF down-regulation [22]. It is thus necessary to explore how Aβ affects the expression of BDNF exon transcripts. In this study, down-regulation of almost all the BDNF exon mRNAs was found in rat hippocampus injected with Aβ [exon I (−51%), exon IIB (−60%), exon IIC (−56%), exon IV (−74%), exon VI (−58%), exon IX (−50%)] compared with the sham group (Fig. 4A). Similarly, SAM improved the low expression of BDNF mRNAs caused by Aβ. Compared with the Aβ injection group, exon I mRNA was increased by 110%, exon IIB by 252%, exon IIC by 125%, exon III by 164%, exon IV by 137%, exon V by 139%, exon VI by 264%, exon VII by 202%, and exon IX by 158% after SAM treatment (Fig. 4A). Moreover, SAM reversed the low expression of BDNF protein induced by Aβ (Fig. 4B). These results implied that BDNF exons IV and VI play critical roles both in the down-regulation of BDNF by Aβ and its reversal by SAM in rat hippocampus.
Effects of SAM on the expression of BDNF exon mRNAs and protein in hippocampus from rats injected with Aβ. A q-PCR analysis of BDNF mRNA levels. B Western blot analysis of BDNF. The data, normalized to β-actin, are expressed as mean ± SD (n = 3–6). *P <0.05, **P <0.01 vs sham group; # P <0.05, ## P <0.01 vs Aβ group.
Discussion
In recent decades, numerous studies have demonstrated the complexity of BDNF gene structure in rodents and humans. According to the report by Aid et al. [7], the rat BDNF gene consists of eight 5′ untranslated exons and one protein-coding 3′ exon. Transcription of the gene results in BDNF transcripts containing one of the eight 5′ exons spliced to the protein-coding exon and in a transcript containing only the 3′ extended protein-coding exon. The present study revealed different expression levels of BDNF exon mRNAs in rat hippocampus. Among them, exons IV and VI were expressed at higher levels than other non-coding exons, consistent with previous reports [8]. The high expression of exon IV and VI mRNAs implied that the changes in these two exon mRNAs might play key roles in BDNF translation in response to various stimuli.
A series of reports has demonstrated a significant elevation of BDNF expression soon after ischemic stroke [23]. Using irreversible occlusion of multiple arterioles in the left hemisphere and left common carotid artery, Béjot et al. [24] showed that BDNF expression sustained high levels from 24 h to 8 days later. Chronic cerebral ischemia caused by blood flow insufficiency is a group of diseases manifested by progressive cognitive dysfunction associated with BDNF down-regulation. The 2-VO rat model used in the current study is a well-established model to investigate the effects of chronic cerebrovascular hypoperfusion on neurodegenerative diseases [20]. In 2-VO rats, the cerebral hypoperfusion is global and long-lasting, as the blood vessels are permanently ligated [25]. After occlusion of the bilateral common carotid arteries, the blood flow in the brain decreases quickly and notably in the acute phase (2–7 days), then a chronic phase (2–3 months) follows and this closely resembles the condition of reduced cerebral blood flow in human aging and dementia. The results of this study revealed different regulation patterns of BDNF transcripts in different periods of ischemia. In the early stage of the acute phase, no evident changes in BDNF expression were found, while in the late stage of the acute phase, BDNF expression was increased in association with high expression of exon IV mRNA. In the early stage of the chronic phase, BDNF expression almost returned to normal levels with low exon IV mRNA expression. In the late stage of the chronic phase, the BDNF expression was significantly decreased and almost all the BDNF exons contributed to this low expression. Although the degree of reduced expression of all BDNF exons mRNAs was similar, exons IV and VI played major roles, as their original expression was high. As to the transient increase of BDNF expression in the acute stage, we speculate that this might be due to endogenous compensation in response to the acute stimulation.
Our previous studies suggested that chronic cerebrovascular hypoperfusion leads to progressive spatial memory deficits, increased Aβ levels associated with increased production, decreased neprilysin, and impaired clearance of Aβ from the brain [22]. In rats injected with amyloid fibrils, BDNF mRNA exon VI and protein significantly decrease in the hippocampal CA1 area [27]. Shin et al. [28] have reported that the expression of BDNF mRNA and protein are decreased in SH-SY5Y cells and primary cultured neurons treated with Aβ. Our data are consistent with the previous studies, and q-PCR revealed that exons IV and VI play crucial roles. Chronic cerebral hypoperfusion could reduce BDNF expression and increase Aβ production, while Aβ could further aggravate the down-regulation of BDNF.
As a member of the neurotrophin family, BDNF is involved in neuronal survival, development, and synaptic plasticity. A series of studies have demonstrated that it acts as an endogenous repair agent after stroke [29]. However, BDNF is hardly able to pass through the BBB, raising difficulties for exogenous administration. Fortunately, studies have demonstrated that SAM can cross the BBB [16]. In this study, we showed that SAM improved endogenous BDNF expression in both the 2-VO and Aβ-injection rat models. Fuso et al. [18, 19] reported that SAM supplementation can improve spatial memory deficits of TgCRND8 mice induced by vitamin B deficiency via several mechanisms: it affects presenilin 1 and BACE1 (β-Amyloid precursor protein cleavage enzyme 1) expression, inhibits amyloid production and tau hyperphosphorylation, increases GSH, and influences oxidative metabolism. Recently a meta-analysis of the effect of SAM on cognitive performance in mice suggested that it may be useful in improving spatial memory in patients suffering from many types of dementia, including AD [30]. The promotion of BDNF expression by SAM shown in this study supports this claim.
SAM is the primary methyl donor and the precursor of GSH. As the precursor of GSH, SAM acts as the major endogenous antioxidant protecting cells against injury in alcoholic liver disease [13]. SAM treatment is beneficial for inflammation-induced colon cancer by inhibiting inflammatory factors [31]. SAM administration can also affect the intracellular methylation of DNA; SAM pretreatment can alter cocaine-induced gene expression in mice by affecting the epigenome [15]. In this study, we reported that SAM reversed the low BDNF expression induced by hypoxia and Aβ, and this was mainly dependent on BDNF exons IV and VI. The expression profiles of all BDNF transcripts revealed high levels of expression of exon IV and VI mRNAs, indicating that the changes of BDNF mRNA and protein largely depend on these two exons. Meanwhile, the transcripts of these two exons were sensitive to the insults in this study, changing dramatically compared with other exons. In recent years, many studies on the regulation of the BDNF gene have revealed that epigenetic modification plays an important role. Multiple BDNF exon promoter regions are rich in CpG islands, which are potential sites of epigenetic modification [32]. Early-life adversity, prenatal stress, and exercise regulate the methylation of exon IV promoter DNA and BDNF expression [33–35]. Methylation of exon VI promoter DNA increases after fear conditioning [26]. The expression of exons IV and VI is regulated by modification of H3K9 methylation in the early stress response of rats [9]. Anier and collogues [15] have reported that SAM pretreatment modifies cocaine-induced gene expression and this is associated with reduced DNA methyltransferase-3a and -3b expression in the nucleus accumbens. All these data suggest that exons IV and VI are key exons in BDNF protein expression in the processes of BDNF transcription and translation. The exact regulatory mechanisms acting on BDNF expression need further investigation.
In summary, BDNF exons IV and VI may play key roles in the BDNF protein down-regulation caused both by chronic cerebrovascular hypoperfusion and Aβ in rat hippocampus. SAM can improve the low BDNF expression caused by these insults mainly via BDNF exons IV and VI. SAM may play a neuroprotective role by increasing the expression of the endogenous BDNF gene and be a potential target for AD therapy.
References
Hardy J, Selkoe DJ. The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 2002, 297: 353–356.
Apelt J, Schliebs R. Beta-amyloid-induced glial expression of both pro- and anti-inflammatory cytokines in cerebral cortex of aged transgenic Tg2576 mice with Alzheimer plaque pathology. Brain Res 2001, 894: 21–30.
Orellana JA, Shoji KF, Abudara V, Ezan P, Amigou E, Saez PJ, et al. Amyloid beta-induced death in neurons involves glial and neuronal hemichannels. J Neurosci 2011, 31: 4962–4977.
de la Torre JC. Is Alzheimer’s disease a neurodegenerative or a vascular disorder? Data, dogma, and dialectics. Lancet Neurol 2004, 3: 184–190.
Wu X, Sun J, Zhang X, Li X, Liu Z, Yang Q, et al. Epigenetic Signature of Chronic Cerebral Hypoperfusion and Beneficial Effects of S-adenosylmethionine in Rats. Mol Neurobiol 2014, 50:839–851.
Yao ZH, Zhang JJ, Xie XF. Enriched environment prevents cognitive impairment and tau hyperphosphorylation after chronic cerebral hypoperfusion. Curr Neurovasc Res 2012, 9: 176–184.
Aid T, Kazantseva A, Piirsoo M, Palm K, Timmusk T. Mouse and ratBDNF gene structure and expression revisited. Journal of Neuroscience Research 2007, 85: 525–535.
Liu QR, Lu L, Zhu XG, Gong JP, Shaham Y, Uhl GR. Rodent BDNF genes, novel promoters, novel splice variants, and regulation by cocaine. Brain Res 2006, 1067: 1–12.
Suri D, Veenit V, Sarkar A, Thiagarajan D, Kumar A, Nestler EJ, et al. Early stress evokes age-dependent biphasic changes in hippocampal neurogenesis, BDNF expression, and cognition. Biol Psychiatry 2013, 73: 658–666.
Koo JW, Mazei-Robison MS, LaPlant Q, Egervari G, Braunscheidel KM, Adank DN, et al. Epigenetic basis of opiate suppression of Bdnf gene expression in the ventral tegmental area. Nat Neurosci 2015, 18: 415–422.
Song JH, Yu JT, Tan L. Brain-Derived Neurotrophic Factor in Alzheimer’s Disease: Risk, Mechanisms, and Therapy. Mol Neurobiol 2014.
Martinez-Una M, Varela-Rey M, Mestre D, Fernandez-Ares L, Fresnedo O, Fernandez-Ramos D, et al. S-Adenosylmethionine increases circulating very-low density lipoprotein clearance in non-alcoholic fatty liver disease. J Hepatol 2015, 62: 673–681.
Anstee QM, Day CP. S-adenosylmethionine (SAMe) therapy in liver disease: a review of current evidence and clinical utility. J Hepatol 2012, 57: 1097–1109.
Papakostas GI, Cassiello CF, Iovieno N. Folates and S-adenosylmethionine for major depressive disorder. Can J Psychiatry 2012, 57: 406–413.
Anier K, Zharkovsky A, Kalda A. S-adenosylmethionine modifies cocaine-induced DNA methylation and increases locomotor sensitization in mice. Int J Neuropsychopharmacol 2013, 16: 2053–2066.
Bottiglieri T, Godfrey P, Flynn T, Carney MW, Toone BK, Reynolds EH. Cerebrospinal fluid S-adenosylmethionine in depression and dementia: effects of treatment with parenteral and oral S-adenosylmethionine. J Neurol Neurosurg Psychiatry 1990, 53: 1096–1098.
Linnebank M, Popp J, Smulders Y, Smith D, Semmler A, Farkas M, et al. S-adenosylmethionine is decreased in the cerebrospinal fluid of patients with Alzheimer’s disease. Neurodegener Dis 2010, 7: 373–378.
Fuso A, Nicolia V, Ricceri L, Cavallaro RA, Isopi E, Mangia F, et al. S-adenosylmethionine reduces the progress of the Alzheimer-like features induced by B-vitamin deficiency in mice. Neurobiol Aging 2012, 33: 1482 e1481–1416.
Cavallaro RA, Fuso A, Nicolia V, Scarpa S. S-adenosylmethionine prevents oxidative stress and modulates glutathione metabolism in TgCRND8 mice fed a B-vitamin deficient diet. J Alzheimers Dis 2010, 20: 997–1002.
Farkas E, Luiten PG, Bari F. Permanent, bilateral common carotid artery occlusion in the rat: a model for chronic cerebral hypoperfusion-related neurodegenerative diseases. Brain Res Rev 2007, 54: 162–180.
Gu X, Sun J, Li S, Wu X, Li L. Oxidative stress induces DNA demethylation and histone acetylation in SH-SY5Y cells: potential epigenetic mechanisms in gene transcription in Abeta production. Neurobiol Aging 2013, 34: 1069–1079.
Liu H, Xing A, Wang X, Liu G, Li L. Regulation of beta-amyloid level in the brain of rats with cerebrovascular hypoperfusion. Neurobiol Aging 2012, 33: 826 e831–842.
Yang L, Zhang Z, Sun D, Xu Z, Yuan Y, Zhang X, et al. Low serum BDNF may indicate the development of PSD in patients with acute ischemic stroke. Int J Geriatr Psychiatry 2011, 26: 495–502.
Bejot Y, Prigent-Tessier A, Cachia C, Giroud M, Mossiat C, Bertrand N, et al. Time-dependent contribution of non neuronal cells to BDNF production after ischemic stroke in rats. Neurochem Int 2011, 58: 102–111.
Choy M, Ganesan V, Thomas DL, Thornton JS, Proctor E, King MD, et al. The chronic vascular and haemodynamic response after permanent bilateral common carotid occlusion in newborn and adult rats. J Cereb Blood Flow Metab 2006, 26: 1066–1075.
Lubin FD, Roth TL, Sweatt JD. Epigenetic regulation of BDNF gene transcription in the consolidation of fear memory. J Neurosci 2008, 28: 10576–10586.
Wang BY, Zhong Y, Zhao Z, Miao Y. Epigenetic suppression of hippocampal BDNF mediates the memory deficiency induced by amyloid fibrils. Pharmacol Biochem Behav 2014, 126C: 83–89.
Shin MK, Kim HG, Baek SH, Jung WR, Park DI, Park JS, et al. Neuropep-1 ameliorates learning and memory deficits in an Alzheimer’s disease mouse model, increases brain-derived neurotrophic factor expression in the brain, and causes reduction of amyloid beta plaques. Neurobiol Aging 2014, 35: 990–1001.
Berretta A, Tzeng YC, Clarkson AN. Post-stroke recovery: the role of activity-dependent release of brain-derived neurotrophic factor. Expert Rev Neurother 2014, 14: 1335–1344.
Montgomery SE, Sepehry AA, Wangsgaard JD, Koenig JE. The effect of S-adenosylmethionine on cognitive performance in mice: an animal model meta-analysis. PLoS One 2014, 9: e107756.
Li TW, Yang H, Peng H, Xia M, Mato JM, Lu SC. Effects of S-adenosylmethionine and methylthioadenosine on inflammation-induced colon cancer in mice. Carcinogenesis 2012, 33: 427–435.
Bennett MR, Lagopoulos J. Stress and trauma: BDNF control of dendritic-spine formation and regression. Prog Neurobiol 2014, 112: 80–99.
Roth TL, Lubin FD, Funk AJ, Sweatt JD. Lasting Epigenetic Influence of Early-Life Adversity on the BDNF Gene. Biological Psychiatry 2009, 65: 760–769.
Boersma GJ, Lee RS, Cordner ZA, Ewald ER, Purcell RH, Moghadam AA, et al. Prenatal stress decreases Bdnf expression and increases methylation of Bdnf exon IV in rats. Epigenetics 2014, 9: 437–447.
Gomez-Pinilla F, Zhuang Y, Feng J, Ying Z, Fan G. Exercise impacts brain-derived neurotrophic factor plasticity by engaging mechanisms of epigenetic regulation. Eur J Neurosci 2011, 33: 383–390.
Acknowledgments
This work was supported by the National Natural Science Foundation of China (81070926 and 81571281).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, Q., Cui, J., Fang, C. et al. S-adenosylmethionine Administration Attenuates Low Brain-Derived Neurotrophic Factor Expression Induced by Chronic Cerebrovascular Hypoperfusion or Beta Amyloid Treatment. Neurosci. Bull. 32, 153–161 (2016). https://doi.org/10.1007/s12264-016-0023-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12264-016-0023-z