Abstract
Background and aims
As the prevalence of nonalcoholic fatty liver disease (NAFLD) is approximately 30% in the general population, it is important to develop a non-invasive biomarker for the diagnosis of nonalcoholic steatohepatitis (NASH). This prospective cross-sectional study aimed to develop a scoring system for NASH diagnosis through multiparametric magnetic resonance (MR) and clinical indicators.
Methods
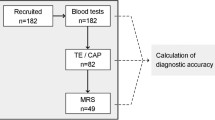
Medical history, laboratory tests, and MR parameters of patients with NAFLD were assessed. A scoring system was developed using a logistic regression model. In total, 127 patients (58 with nonalcoholic fatty liver [NAFL] and 69 with NASH) were enrolled. After evaluating 23 clinical characteristics of the patients (4 categorical and 19 numeric variables) for the NASH diagnostic model, an equation for MR elastography (MRE)-based NASH score was obtained using 3 demographic factors, 2 laboratory variables, and MRE.
Results
The MRE-based NASH score showed a satisfactory accuracy for NASH diagnosis (c-statistics, 0.841; 95% CI 0.772–0.910). At a cut-off MRE-based NASH score of 0.68 for NASH diagnosis, its sensitivity was 0.68 and specificity was 0.91. When an MRE-based NASH score of 0.37 was used as a cut-off for NASH exclusion, the sensitivity was 0.91 and specificity was 0.55. Overall, 35% (44/127) of patients were in the gray zone (between 0.37 and 0.68). Internal validation via bootstrapping also indicated the satisfactory accuracy of NASH diagnosis (optimism-corrected statistics, 0.811).
Conclusion
MRE-based NASH score is a useful and accurate non-invasive biomarker for diagnosis of NASH in patients with NAFLD.
Graphical abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Nonalcoholic steatohepatitis (NASH) is the progressive form of nonalcoholic fatty liver disease (NAFLD), defined as the presence of ≥ 5% hepatic steatosis with inflammation and ballooning of hepatocytes, regardless of hepatic fibrosis [1]. NASH account for 20–25% of NAFLD patients [2], and its diagnosis is important owing to its poor prognosis compared with nonalcoholic fatty liver (NAFL). As NAFLD affects approximately 30% of the global population [3], it is difficult to perform liver biopsy in whole NAFLD patients. Besides, liver biopsy carries several limitations such as high cost, high risk of bleeding and infection, and longer time to obtain results [4]. Therefore, development of a non-invasive method for the evaluation of NAFLD severity is emerging.
Non-invasive biomarkers have been studied, including serologic biomarkers, combination panels, and imaging biomarkers in the diagnosis of NASH [5, 6]. Cytokeratin 18 (CK18) is one of the most investigated markers for NAFLD severity [7]. However, its intermediate accuracy and uncertain optimal cut-off value limit its clinical use. Transient elastography (TE) and magnetic resonance elastography (MRE), which can measure liver stiffness, exhibited a modest accuracy for the diagnosis of NASH [8]. NASH is a highly complex disease, and it is difficult to develop a non-invasive biomarker for it with a single parameter. Combined panels, including NASH Test and NASH Diagnostics Panel were developed, but exhibited poor accuracy and were expensive [9]. The FibroScan-AST (FAST) score calculated using the controlled attenuation parameter (CAP), liver stiffness measurement, and aspartate transaminase (AST) had been developed as a prediction model to identify patients with significant activity and fibrosis [10]. Although the FAST score showed satisfactory performance (c-statistic, 0.80; 95% CI 0.76–0.85) and was validated with another external cohort (c-statistic range 0.74–0.95), this scoring system is not intended for diagnosing NASH.
Multiparametric magnetic resonance (MR) is a valuable modality for evaluating the severity of NAFLD [11]. Magnetic resonance imaging (MRI), proton density fat fraction (PDFF), and MRE exhibited superior performances than other non-invasive modalities in detecting steatosis and fibrosis and grading their severity [12]. We previously reported that the non-invasive MR index, comprising magnetic resonance spectroscopy (MRS), MRE, and T1 relaxation time, can effectively diagnose NASH [13]. Moreover, MRI can effectively detect pathologic lesions in the liver, whereas ultrasonography does not facilitate the visualization of lesions in a fatty liver. Thus, multiparametric MR could be a useful replacement or supplement of liver biopsy.
Although the use of multiparametric MR for evaluating NASH has been reported previously, we aimed to develop a diagnostic scoring system that could improve the accuracy, sensitivity, and specificity of diagnosis of NASH by combining MR parameter and clinical indicators.
Patients and methods
Study population
To develop a scoring system, we included NAFLD patients from a biopsy-confirmed NAFLD cohort from Korea University Guro hospital [8]. All the patients underwent liver biopsy when they were suspected NAFLD in sonography, needed exclusion of other liver diseases, or required accurate assessment of disease severity of NAFLD. All patients had no other chronic liver disease, such as chronic hepatitis B or C infection, or autoimmune liver disease. Alcohol abusers, defined as men and women who consumed more than 140 g and 70 g of alcohol per week, respectively, patients with decompensated liver cirrhosis, those with contraindications to MRI, and those with other severe systemic disease or malignancy were excluded. All patients underwent laboratory tests and MRI within 6 months after liver biopsy. Diabetes was diagnosed based on previous medical history and diagnostic criteria [14]. Impaired fasting glucose (IFG) was defined as a fasting plasma glucose level between 100 and 125 mg/dL. Laboratory tests included white blood cell count, platelet count, hemoglobin, aspartate aminotransferase (AST), alanine aminotransferase, alkaline phosphatase, gamma-glutamyl transferase, total bilirubin, albumin, prothrombin time, blood urea nitrogen, creatinine, and c-reactive protein.
This study was approved by the institutional review board of the Korea University Guro Hospital (2016GR0302). All patients who agreed to participate in the study provided written informed consent. This study was done according to the Declaration of Helsinki.
Histopathologic evaluation
Liver biopsy was performed by a skilled radiologist via the intercostal space with an 18-gauge Tru-cut needle (TSK Laboratory, Tochigi, Japan). Two liver specimens were fixed in formalin and paraffin block was made. The sliced sections were stained using hematoxylin and eosin. NAFLD was diagnosed by two experienced pathologists, and its severity was evaluated according to the NASH Clinical Research Network histologic score [15]. NASH was diagnosed when hepatic steatosis was ≥ 5%, along with inflammation and ballooning of hepatocytes, regardless of fibrosis [1].
Multiparametric magnetic resonance imaging
All patients underwent MRI using a 3 T MR scanner (MAGNETOM Skyra; Siemens Healthcare, Erlangen, Germany). Multiparametric MR sequences consisted of seven sequences, namely MRI-PDFF, MRS, T1 relaxation time, MRE, T1-weighted image, T2-weighted image, and diffusion-weighted image. The image parameters are summarized in Supplementary Table 1. Modified Dixon techniques were used to measure the MRI-PDFF [16]. MRS data was obtained from a single voxel measuring 20 × 20 × 20 mm, and data were analyzed using an online program from the MR scanner vendor, described in our previous study [13]. T1 relaxation time was measured using a shortened Modified Look Locker Inversion recovery sequence based on fast low-angle shot (FLASH) [17]. Images were acquired at three different levels, namely the point where the hepatic veins join the inferior vena cava, hilum of the liver, and gallbladder fossa. T1 relaxation time was measured by applying a non-selective inversion recovery pulse and low-flip angle FLASH acquisitions for 16 inversion contrasts. Three regions of interest (ROIs) from different images were measured and their mean values were represented as T1 relaxation time (milliseconds). Liver stiffness was measured by MRE using a pneumatic driver system (Resoundant, Inc., Rochester, MN, USA) attached to the right anterior chest wall and the liver of the patients. A 60-Hz shear wave was generated from the driver and delivered through a flexible vinyl tube. Four MRE images were acquired during the expiratory phase of respiration. The acquired images were processed by elastograms, and the liver stiffness was measured using ROIs drawn on the elastograms. Four ROIs from different images were measured, and the mean values of MRE-liver stiffness measurement (MRE-LSM) were represented in kilopascals (kPa).
Score development
The score was developed using demographics, laboratory data, and MRI parameters of the 127 enrolled patients. The selection of parameters was based on the − 2 log likelihood test statistic. The parameters which have ΔAIC and ΔBIC with negative value were selected. The selected parameters were used to build a second-order multiple logistic regression model. The statistical significance of each predictor was also evaluated using the − 2 log likelihood test statistic, which is − 2 times the difference of log likelihood values between logistic regression models with and without the predictor when the other predictors are adjusted. The internal validation of a developed model was performed using 1,000 bootstrap samples to the performance of the model and tenfold cross validation. The performance was assessed in terms of c-statistic.
Statistics
The patients’ demographic and laboratory characteristics are summarized as numbers with percentages for categorical variables or medians with interquartile ranges for numerical variables. Pearson’s chi-squared test and Mann–Whitney U test were used to compare the baseline characteristics between patients with NAFL and NASH. Multiple logistic regression analysis was performed to develop a prediction model for the diagnosis of NASH. The model was built using SAS software version 9.4 (SAS Institute, Cary, NC, USA), and the bootstrapping for the internal validation of the developed model was conducted using R language version 3.6.2 (R Foundation for Statistical Computing, Vienna, Austria). p values < 0.05 were considered statistically significant, except for a variable selection that used a value of 0.1.
Results
Baseline characteristics
In total, 127 patients diagnosed with NAFLD were enrolled at the Korea University Guro Hospital between September 2016 and March 2019. The demographic and laboratory characteristics of patients with NAFL and NASH are summarized in Table 1. Patients with NASH were older (p < 0.001) and showed a lower body mass index (BMI) (p = 0.015) compared with NAFL patients. The prevalence of diabetes/IFG, hypertension, and dyslipidemia was higher in patients with NASH than in patients with NAFL, but diabetes/IFG was only significant (p = 0.002). Compared with patients with NAFL, those with NASH had a lower hemoglobin (p = 0.011) and platelet count (p < 0.001) and a higher AST level (p < 0.001). Among multiparametric MR sequences, MRE-liver stiffness measurement (MRE-LSM) was higher in NASH patients comparing with NAFL patients (p < 0.001). The histopathologic findings are summarized in Supplementary Table 2. Steatosis did not significantly differ between patients with NAFL and NASH, whereas more patients with NASH exhibited higher grade inflammation and more advanced stage of fibrosis than those with NAFL. Representative histopathological features are shown in Supplementary Fig. 1.
Data inspection
No evidence of multicollinearity was observed in terms of a variable inflation factor among the variables used to develop the prediction model (Supplementary Table 3). No influential observation was identified through regression model diagnostics (data not shown).
Model building
We summarized flow chart for developing MRE-based NASH scoring system in Supplementary Fig. 2. Four categorical variables and 19 continuous variables were examined for the NASH diagnostic model (Supplementary Table 4). Total six parameters, comprising three clinical (age, BMI, and diabetes/IFG) and two laboratory parameters (hemoglobin and platelet count), and MRE-LSM were chosen as candidate parameters for the diagnostic model. A model consisting of three clinical and two laboratory parameters provided a c-statistic of 0.784 (95% CI 0.702–0.852). When the MRE-LSM parameters were added to the model, the c-statistic increased to 0.841 (95% CI 0.772–0.910), which was statistically significant (p = 0.049 by DeLong test) (Supplementary Fig. 3). This implies that MR parameters significantly increased the diagnostic accuracy of the model. There was no significant effect of interactions among the six selected parameters for the diagnosis of NASH (Supplementary Table 5).
The final MRE-based NASH score prediction model is as follows;
These six parameters that were used in MRE-based NASH score were significantly correlated with ballooning but not inflammation (Supplementary table 6).
Diagnostic accuracy
The MRE-based NASH score showed a satisfactory diagnostic accuracy for diagnosis of NASH (c-statistic, 0.841; 95% CI 0.772–0.910) (Fig. 1). To establish an exclusion cut-off value for a sensitivity greater than 0.9, while compensating for a low specificity and ensuring a diagnostic cut-off value for specificity larger than 0.9, we suggested a cut-off value of 0.37 for exclusion of NASH (sensitivity, 0.91; specificity, 0.55; negative predictive value 0.84) and a predicted score of 0.68 for diagnosis of NASH (sensitivity, 0.57; specificity, 0.91; positive predictive value 0.89). We found that 35% of patients (44 out of 127 patients) remained in the so-called “gray zone” between 0.37 and 0.68 (Table 2). The overall sensitivity, specificity, positive predictive value, and negative predictive value are shown in Fig. 2.
We compared c-statistics between the MRE-LSM and the TE-LSM, while adjusting the other five clinical and laboratory parameters (age, BMI, diabetes/IFG, hemoglobin, and platelet count). Although the difference was not significant (p = 0.2054 by Delong test), the AUC of the MRE-LSM (c-statistics = 0.841) was higher than that of the TE-LSM (c-statistics = 0.809).
Internal validation of MRE-based NASH Score using bootstrapping
Our MRE-based NASH score model was internally validated through bootstrapping and tenfold cross validation. Based on 1000 bootstrap samples, the optimism-corrected c-statistic, 0.811 was obtained. Also, through tenfold cross validation the optimism-corrected c-statistic, 0.821 was obtained. The Brier score, another measure for the accuracy of probabilistic predictions that ranges between 0 and 1, was 0.163. Lower Brier scores indicated better calibrated predictions. Meanwhile, the discrimination slope, defined as the slope of a linear regression of predicted probabilities of events derived from a prognostic model on the binary event status, was 0.295. Overall, the internal validity of the MRE-based NASH score model was satisfactory.
Discussion
As NASH is a progressive form of NAFLD and liver biopsy is essential for its diagnosis [1], non-invasive biomarkers are urgently required. In the present study, we developed the MRE-based NASH score by combining age, diabetes/IFG, BMI, hemoglobin, platelet count, and MRE-LSM.
The diagnosis of NASH is important, as it has a poor prognosis compared with NAFL and as only patients with NASH are indicated for drug therapy [3]. Although liver biopsy is required to diagnose NASH, it carries limitations such as complication risks, high cost, and inconvenience [18]. To overcome these limitations, non-invasive diagnostic biomarkers for NASH have been developed. Early NASH biomarkers were single markers targeting NASH disease pathways such as apoptosis, inflammation, and oxidative stress [5]. However, most of them could not be applied in the clinical setting because of their unsatisfactory accuracy. As complex pathologic processes are involved in the progression of NASH, biomarkers with single parameters exhibit limited efficacy in discriminating NASH from NAFL. Therefore, the NASH test, NASH diagnostic panel, and a combination of CK-18 and surface antigen Fas has been developed as a combined biomarker [9]. Although these combined panels showed an elevated accuracy, they included parameters that are not routinely checked including CK-18, apolipoprotein, adiponectin, and resistin. Except MRE, the MRE-based NASH score consists of easily accessible demographic parameters including age, status of diabetes/IFG, BMI, and easy to measure laboratory parameters, such as hemoglobin and platelet count. Moreover, the MRE-based NASH score showed a high accuracy of 0.841.
Diabetes/IFG are metabolic diseases related to the development and progression of NAFLD [19]. Diabetes and a family history of diabetes are significantly associated with NASH [20]. In diabetes, insulin resistance and adipose tissue dysfunction induce lipotoxicity in hepatocytes and activate the pro-inflammatory pathway [21]. Glucotoxicity in diabetes is also associated with lipotoxicity and insulin resistance promotes NASH [21]. Diabetes/IFG showed a positive correlation with the MRE-based NASH score. Increasing age was also associated with NASH in this scoring system. Older patients with NAFLD showed more severe histologic changes [22] and cellular senescence was correlated with hepatic steatosis and the severity of NAFLD [23]. Meanwhile, BMI was inversely correlated with NASH in the MRE-based NASH score. Obesity and higher BMI increase the risk of NAFLD and NASH [24]. However, Hagström et.al. reported that lean patients with NAFLD have a higher risk of severe liver disease than NALFD patients with higher BMI [25]. Another study reported that lean patients with NAFLD presented a poor clinical course with a higher overall mortality than did overweight or obese patients with NAFLD [26]. Sarcopenia, a significant risk factor for NASH, is a cause of lean body mass [27] and could be the reason for the negative correlation between NASH and BMI in this study. Laboratory examination revealed that hemoglobin and platelet count were significantly lower in patients with NASH than in patients with NAFLD. Chronic inflammation is one of the causes of anemia, and patients with NASH showed a lower hemoglobin level than that of patients with NAFLD [28]. Platelet count is a known biomarker for liver fibrosis in various kinds of liver diseases, and thrombocytopenia is associated with disease severity in NAFLD [29].
The major difference between the MRE-based NASH score and other scoring systems in evaluating the disease severity of NAFLD is the use of MRE-LSM. Multiparametric MR could predict the NAFLD activity score in a mouse NAFLD model [30], and it showed good correlation with inflammation, fibrosis, and ballooning [31]. Our previous study had also reported that the multiparametric MR index showed a good accuracy to diagnose NASH according to the steatosis-activity-fibrosis score [13]. The difference in the results arising from different equipment used can raise a concern regarding validation. Previously, higher technical failure rates were observed at 3 T than at 1.5 T. However, spin-echo echo-planar imaging (SE-EPI) was introduced for 3 T MRE allowing the advancement of techniques; after which no difference was found in the analysis of the magnetic field subgroup (3 T vs. 1.5 T) using the SE-EPI sequence [32]. We used the SE-EPI sequence with a 3 T MRI in this study, which will not lead to any notable problem in the validation. Recent advances in radiomics will probably contribute to the early and non-invasive diagnosis of liver diseases [33, 34]. A recent study found that the radiomics approach could predict liver fibrosis [35]. Further studies applying radiomics to NASH diagnosis would be interesting.
Our MRE-based NASH score focused on the diagnosis of NASH in patients with NAFLD. Meanwhile, the FAST score, composed of AST, CAP, and TE, has been developed to discriminate NASH with a NAS ≥ 4 and fibrosis stage ≥ 2, which is an advanced form of NAFLD, and a potential target for the clinical trial of treatment of NASH [10]. These scoring systems showed a good performance (c-statistic 0.80, 95% CI 0.76–0.85) with satisfactory validation in several external cohorts (c-statistic range, 0.74–0.95). Our previous study also showed that MRE-LSM had a good performance in diagnosing NASH or advanced stage of fibrosis (stage 3 or 4) with good accuracy (AUC 0.86) [8]. Although diagnosing more severe forms of NASH is important, NASH with early fibrosis or without fibrosis could be ignored in this setting. According to the MRE-based NASH score, patients with NASH could be discriminated from those with NAFL. When we compared c-statistics between model with MRE-LSM and model with TE-LSM, model with MRE-LSM showed better AUC than model with TE-LSM (c-statics 0.841 vs. 0809). Moreover, the diagnostic accuracy of our scoring system was not influenced by the fibrosis stage when comparing between the non-advanced and advanced fibrosis groups.
We established diagnostic and exclusion cut-off values to maximize the accuracy of the MRE-based NASH score, granting it a negative predictive value of 0.84 and a positive predictive value of 0.89. Additional diagnostic evaluations, including liver biopsy, are required for patients located in the gray zone (44/127, 35%). Further studies are needed to determine the time interval for follow-up.
This study has several limitations. First, the MRE-based NASH score has not been validated in other cohorts. Although we conducted bootstrapping, an external validation study is essential for evaluating its clinical application. Further external validation from other groups will help generalize the MRE-based NASH score after this study. Second, the MRE-based NASH score included multiparametric MR, which has limited use in primary clinics. Therefore, the MRE-based NASH score would be useful only in tertiary clinics where multiparametric MR is available. Finally, this study included a relatively small number of patients. Further validation studies that include a larger number of patients would help strengthen the accuracy of the MRE-based NASH score.
In conclusion, we developed a novel non-invasive biomarker—the MRE-based NASH score—to diagnose NASH in patients with NAFLD. This scoring system improves the accuracy, sensitivity, and specificity of diagnosis of NASH by combining multiparametric MR and clinical indicators. Further external validation to evaluate its clinical application is warranted.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Abbreviations
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate transaminase
- AUC:
-
Area under the ROC curve
- BMI:
-
Body Mass Index
- CAP:
-
Controlled attenuation parameter
- CK18:
-
Cytokeratin 18
- FAST:
-
FibroScan-AST
- FLASH:
-
Fast low-angle shot
- IFG:
-
Impaired fasting glucose
- kPa:
-
Kilopascal
- MR:
-
Magnetic resonance
- MRE:
-
Magnetic resonance elastography
- MRI:
-
Magnetic resonance imaging
- MRS:
-
Magnetic resonance spectroscopy
- NAFLD:
-
Nonalcoholic fatty liver disease
- NASH:
-
Nonalcoholic steatohepatitis
- PDFF:
-
Proton density fat fraction
- PT:
-
Prothrombin time
- ROI:
-
Regions-of-interest
- TE:
-
Transient elastography
References
Chalasani N, Younossi Z, Lavine JE, Charlton M, Cusi K, Rinella M, et al. The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology 2018;67:328–357. https://doi.org/10.1002/hep.29367
Rinella ME. Nonalcoholic fatty liver disease: a systematic review. JAMA 2015;313:2263–2273. https://doi.org/10.1001/jama.2015.5370
Younossi ZM, Koenig AB, Abdelatif D, Fazel Y, Henry L, Wymer M. Global epidemiology of nonalcoholic fatty liver disease—meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 2016;64:73–84. https://doi.org/10.1002/hep.28431
Thampanitchawong P, Piratvisuth T. Liver biopsy: complications and risk factors. World J Gastroenterol 1999;5:301–304. https://doi.org/10.3748/wjg.v5.i4.301
Wong VW, Adams LA, de Lédinghen V, Wong GL, Sookoian S. Noninvasive biomarkers in NAFLD and NASH—current progress and future promise. Nat Rev Gastroenterol Hepatol 2018;15:461–478. https://doi.org/10.1038/s41575-018-0014-9
Kim TH, Lee Y, Lee YS, Gim JA, Ko E, Yim SY, et al. Circulating miRNA is a useful diagnostic biomarker for nonalcoholic steatohepatitis in nonalcoholic fatty liver disease. Sci Rep 2021;11:14639. https://doi.org/10.1038/s41598-021-94115-6
Amacher DE. Progress in the search for circulating biomarkers of nonalcoholic fatty liver disease. Biomarkers 2014;19:541–552. https://doi.org/10.3109/1354750x.2014.958535
Lee YS, Yoo YJ, Jung YK, Kim JH, Seo YS, Yim HJ, et al. Multiparametric MR is a valuable modality for evaluating disease severity of nonalcoholic fatty liver disease. Clin Transl Gastroenterol 2020;11:e00157. https://doi.org/10.14309/ctg.0000000000000157
Younossi ZM, Jarrar M, Nugent C, Randhawa M, Afendy M, Stepanova M, et al. A novel diagnostic biomarker panel for obesity-related nonalcoholic steatohepatitis (NASH). Obes Surg 2008;18:1430–1437. https://doi.org/10.1007/s11695-008-9506-y
Newsome PN, Sasso M, Deeks JJ, Paredes A, Boursier J, Chan WK, et al. FibroScan-AST (FAST) score for the non-invasive identification of patients with non-alcoholic steatohepatitis with significant activity and fibrosis: a prospective derivation and global validation study. Lancet Gastroenterol Hepatol 2020;5:362–373. https://doi.org/10.1016/s2468-1253(19)30383-8
Yoo JJ, Kim W, Kim MY, Jun DW, Kim SG, Yeon JE, et al. Recent research trends and updates on nonalcoholic fatty liver disease. Clin Mol Hepatol 2019;25:1–11. https://doi.org/10.3350/cmh.2018.0037
Park CC, Nguyen P, Hernandez C, Bettencourt R, Ramirez K, Fortney L, et al. Magnetic resonance elastography vs transient elastography in detection of fibrosis and noninvasive measurement of steatosis in patients with biopsy-proven nonalcoholic fatty liver disease. Gastroenterology 2017;152:598–607. https://doi.org/10.1053/j.gastro.2016.10.026 (e592)
Kim JW, Lee YS, Park YS, Kim BH, Lee SY, Yeon JE, et al. Multiparametric MR Index for the diagnosis of non-alcoholic steatohepatitis in patients with non-alcoholic fatty liver disease. Sci Rep 2020;10:2671. https://doi.org/10.1038/s41598-020-59601-3
American Diabetes Association. 2. Classification and diagnosis of diabetes: standards of medical care in diabetes—2021. Diabetes Care 2021;44(Suppl 1):S15–S33. https://doi.org/10.2337/dc21-S002
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 2005;41:1313–1321. https://doi.org/10.1002/hep.20701
Grimm A, Meyer H, Nickel MD, Nittka M, Raithel E, Chaudry O, et al. Evaluation of 2-point, 3-point, and 6-point Dixon magnetic resonance imaging with flexible echo timing for muscle fat quantification. Eur J Radiol 2018;103:57–64. https://doi.org/10.1016/j.ejrad.2018.04.011
Taylor AJ, Salerno M, Dharmakumar R, Jerosch-Herold M. T1 mapping: basic techniques and clinical applications. JACC Cardiovasc Imaging 2016;9:67–81. https://doi.org/10.1016/j.jcmg.2015.11.005
Chang Y, Kim JI, Lee B, Kim SG, Jung MJ, Kim YS, et al. Clinical application of ultrasonography-guided percutaneous liver biopsy and its safety over 18 years. Clin Mol Hepatol 2020;26:318–327. https://doi.org/10.3350/cmh.2019.0019n
Lee YH, Bang H, Park YM, Bae JC, Lee BW, Kang ES, et al. Non-laboratory-based self-assessment screening score for non-alcoholic fatty liver disease: development, validation and comparison with other scores. PLoS ONE 2014;9: e107584. https://doi.org/10.1371/journal.pone.0107584
Loomba R, Abraham M, Unalp A, Wilson L, Lavine J, Doo E, et al. Association between diabetes, family history of diabetes, and risk of nonalcoholic steatohepatitis and fibrosis. Hepatology 2012;56:943–951. https://doi.org/10.1002/hep.25772
Gastaldelli A, Cusi K. From NASH to diabetes and from diabetes to NASH: mechanisms and treatment options. JHEP Rep 2019;1:312–328. https://doi.org/10.1016/j.jhepr.2019.07.002
Frith J, Day CP, Henderson E, Burt AD, Newton JL. Non-alcoholic fatty liver disease in older people. Gerontology 2009;55:607–613. https://doi.org/10.1159/000235677
Ogrodnik M, Miwa S, Tchkonia T, Tiniakos D, Wilson CL, Lahat A, et al. Cellular senescence drives age-dependent hepatic steatosis. Nat Commun 2017;8:15691. https://doi.org/10.1038/ncomms15691
Loomis AK, Kabadi S, Preiss D, Hyde C, Bonato V, St Louis M, et al. Body Mass Index and risk of nonalcoholic fatty liver disease: two electronic health record prospective studies. J Clin Endocrinol Metab 2016;101:945–952. https://doi.org/10.1210/jc.2015-3444
Hagström H, Nasr P, Ekstedt M, Hammar U, Stål P, Hultcrantz R, et al. Risk for development of severe liver disease in lean patients with nonalcoholic fatty liver disease: a long-term follow-up study. Hepatol Commun 2018;2:48–57. https://doi.org/10.1002/hep4.1124
Younes R, Bugianesi E. NASH in lean individuals. Semin Liver Dis 2019;39:86–95. https://doi.org/10.1055/s-0038-1677517
Koo BK, Kim D, Joo SK, Kim JH, Chang MS, Kim BG, et al. Sarcopenia is an independent risk factor for non-alcoholic steatohepatitis and significant fibrosis. J Hepatol 2017;66:123–131. https://doi.org/10.1016/j.jhep.2016.08.019
Moya D, Baker SS, Liu W, Garrick M, Kozielski R, Baker RD, et al. Novel pathway for iron deficiency in pediatric non-alcoholic steatohepatitis. Clin Nutr 2015;34:549–556. https://doi.org/10.1016/j.clnu.2014.06.011
Panke CL, Tovo CV, Villela-Nogueira CA, Cravo CM, Ferreira FC, Rezende GFM, et al. Evaluation of thrombocytopenia in patients with non-alcoholic fatty liver disease without cirrhosis. Ann Hepatol 2020;19:88–91. https://doi.org/10.1016/j.aohep.2019.05.011
Yin Z, Murphy MC, Li J, Glaser KJ, Mauer AS, Mounajjed T, et al. Prediction of nonalcoholic fatty liver disease (NAFLD) activity score (NAS) with multiparametric hepatic magnetic resonance imaging and elastography. Eur Radiol 2019;29:5823–5831. https://doi.org/10.1007/s00330-019-06076-0
Pavlides M, Banerjee R, Sellwood J, Kelly CJ, Robson MD, Booth JC, et al. Multiparametric magnetic resonance imaging predicts clinical outcomes in patients with chronic liver disease. J Hepatol 2016;64:308–315. https://doi.org/10.1016/j.jhep.2015.10.009
Kim DW, Kim SY, Yoon HM, Kim KW, Byun JH. Comparison of technical failure of MR elastography for measuring liver stiffness between gradient-recalled echo and spin-echo echo-planar imaging: a systematic review and meta-analysis. J Magn Reson Imaging 2020;51:1086–1102. https://doi.org/10.1002/jmri.26918
Hu W, Yang H, Xu H, Mao Y. Radiomics based on artificial intelligence in liver diseases: where we are? Gastroenterol Rep (Oxf) 2020;8:90–97. https://doi.org/10.1093/gastro/goaa011
Jeong WK, Jamshidi N, Felker ER, Raman SS, Lu DS. Radiomics and radiogenomics of primary liver cancers. Clin Mol Hepatol 2019;25:21–29. https://doi.org/10.3350/cmh.2018.1007
Ni M, Wang L, Yu H, Wen X, Yang Y, Liu G, et al. Radiomics approaches for predicting liver fibrosis with nonenhanced T1-weighted imaging: comparison of different radiomics models. J Magn Reson Imaging 2021;53:1080–1089. https://doi.org/10.1002/jmri.27391
Funding
This study was supported by a National Research Foundation of Korea grant from the Korean government (the Ministry of Education, Science and Technology 2021R1C1C1009445 and 2018R1A2B2006183).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare no potential conflicts of interest.
Ethical approval
This study had been approved by the institutional review board from Korea University Guro Hospital (2016GR0302).
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lee, YS., Lee, J.E., Yi, HS. et al. MRE-based NASH score for diagnosis of nonalcoholic steatohepatitis in patients with nonalcoholic fatty liver disease. Hepatol Int 16, 316–324 (2022). https://doi.org/10.1007/s12072-022-10300-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-022-10300-3