Abstract
The diagnostic criteria for silent sinus syndrome (SSS) are still controversial, especially for the post-traumatic/surgery cases that are, nowadays, excluded from the diagnosis of SSS because lacking of spontaneously. We present a systematic review of the last 10 years and our case series of SSS associated to previous trauma/surgery, proposing a new interpretation of SSS. In this work, following the PRISMA guide lines for systematic reviews, we collected 86 articles published on PubMed, Cochrane Library and Medline Plus since 2013 to 2023 about SSS. We divided them in six groups forming the structure of the review: (1) epidemiology, (2) clinical presentation, (3) imaging, (4) etiopathogenesis, (5) sss and craniofacial trauma and (6) treatment. We reported two explicative clinical cases: two men of 34 and 37 years old, involved in motorcycle accident in 2020 and 2014, respectively, and underwent surgery. They came back in 2023 referring diplopia documented by Hess-Lancaster test. CT-scan reported two clear cases of SSS. Basing on what is reported in literature, and basing on our experience, the post-traumatic/surgery SSS are more frequent than the idiopathic ones. Our proposal is to considered them as two individual entities. We propose to adopt the name of Post-traumatic sinus syndrome, or CDR syndrome (Catalfamo-De Rinaldis), for all cases that respect four specific diagnostic criteria reported into the text.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
In 1964 montgomery described a case of enophthalmos associated to a mucocele of the maxillary sinus [1]. That was the first description of the entity known as “chronic maxillary atelectasis” (CMA) or “maxillary sinus hypoplasia” (MSH).
In 1994, Soparkar introduced the term “silent sinus syndrome” (SSS) to identify all clinical signs and symptoms correlated to CMA [2].
The scientific community is uncertain about diagnostic criteria of SSS. One of the main doubt is about its correlation with the chronic maxillary sinusitis even if, currently, an essential criterion for diagnosis of silent sinus syndrome is the absence of symptoms characteristic of Chronic RhinoSinusitis (CRS), as reported in the European Position Paper on Rhinosinusitis and Nasal Polyps 2020 (EPOS 2020) [3].
However, some authors disagree and suggest to include into the diagnosis of SSS also all cases of CMA associated with chronic rhinosinusitis [4].
The following criteria have been proposed for the diagnosis of Silent Sinus Syndrome [5]:
-
1.
No episodes of acute rhinosinusitis and no history of chronic rhinosinusitis;
-
2.
Remodeling and inferior bowing of the maxillary roof/orbital floor evident in a coronal CT scan;
-
3.
No history of orbital trauma or orbital/sinus surgery;
-
4.
No documented congenital deformity of sinus and/or nasal cavity.
Kass et al. [6], classified CMA in three stages based on radiological features:
-
Stage I: membranous deformity,
-
Stage II: bony deformity,
-
Stage III: clinical deformity (enophthalmos/hypoglobus/diplopia).
Still today it isn’t clear if SSS and CMA are the same pathological entity or if they are two distinct entities. In literature they are still described separately but several authors, based on the observation that the definition of the stage III of CMA meet, exactly, the same diagnostic criteria of SSS, propose to consider SSS and CMA the same entity, and propose to adopt Kass staging system to describe the natural evolution of SSS [7,8,9,10].
SSS is referred only to the involvement of the maxillary antrum but sporadic cases of “ethmoidal sinus syndrome” and “frontal sinus syndrome” are just mentioned in literature [11,12,13,14,15].
Materials and Methods
Following the rules of PRISMA guide lines, we propose a systematic review of the last 10 years, since 2013 to 2023, about the topic of Silent Sinus Syndrome and we present two of our representative clinical cases.
We used PubMed, Cochrane Library and Medline Plus as searching engines and we entered “silent sinus syndrome” as key words.
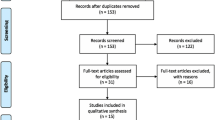
We found a total of 174 papers, forty-five of which were excluded by their title for one or more of the following reasons:
-
Duplication,
-
Different topic (ex. sick sinus syndrome),
-
Language different from English.
So, 129 papers were selected for the Abstract reading. With the following step, 98 papers were selected for the complete reading and, finally, 86 manuscripts were collected for the analysis programmed. We excluded all the articles that were only case report and that didn’t provide any further contribute more than already reported by the others just selected. After that, we divided the article in two main groups: the ones relative to SSS in adult patients (80 papers) and the others reported pediatric cases of SSS (6 papers).
Finally, we divided the articles in six subgroups basing on the main contribution each of them provided and those subgroups formed the structure of the review:
-
I.
Epidemiology.
-
II.
Clinical presentation.
-
III.
Imaging.
-
IV.
Etiopathogenesis.
-
V.
SSS and craniofacial trauma.
-
VI.
Treatment.
Each of these topics are described below.
Epidemiology
Silent Sinus Syndrome is a rare, but probably underdiagnosed, entity and data of its prevalence are still lacking [16].
An higher frequency in adult age is reported, between the 3rd and the 5th decade [17], although some pediatric cases are also reported [18,19,20,21,22,23,24].
Still today, no risk factor has been associated to SSS [25].
Sivrice et al. [8] estimated a prevalence of 0.92% for CMA, and of 0.11% for SSS.
D’Agostino et al. [26] found a prevalence of 6.17% for CMA and of 0.56% for SSS.
In conclusion, the exact prevalence of SSS isn’t still known, even if several cases report have been reported in literature [27,28,29,30,31,32,33,34], about 150 [35]. A CMA has even been find out under the wrappings of an Egyptian mummy [36].
Approximatively, the prevalence of CMA can be estimated about 0.9–6% while that one of SSS about 0.1–0.5%.
Clinical Presentation
Generally, patients with SSS first contact the ophthalmologist practitioner [37, 38]. Furthermore, the term “silent” just refers to the development of SSS which is totally without symptoms. However, in advanced cases, patients with SSS present evident facial deformities, as orbital asymmetry, enophthalmos and/or hypoglobus, sinking of the upper palpebral sulcus, palpebral retraction, and palpebral delay in the downward gaze [39].
Sometimes it’s possible to observe a “pseudopneumoortbita”, described as air trapped under the superior eyelid which gives the appearance of “air into the orbit” in CT scans [40].
Facial depression of the suborbital cutaneous area [41], laughter-induced transient vision loss [42], headache [43] and ipsilateral upper alveolar numbness [44] have been described too.
It’s known that modifications of the sinus wall and the orbital floor involve slowly and progressively and develop over years after the ostiomeatal obstruction but, sometimes, sinus collapse can be quickly progressive, so that signs and symptoms of SSS occur quickly since a known cause of an ostiomeatal obstruction [45], and some authors [46, 47] have described cases of SSS arises with acute diplopia.
Imaging
Although suspect of SSS is clinical, its confirmation must be based on radiology [48].
CT scan is considered the gold standard for diagnosis of SSS. Generally, Multi Detector Computed Tomography (MDCT) is required, however, the Cone-Beam Computed Tomography (CBCT) can produce images with sufficient high resolution but with much lower radiation burden (200–1200 μSv vs. 30 μSv) [49].
Radiographic signs of Silent Sinus Syndrome are pathognomonic [5, 50]:
-
Occlusion of the ethmoidal infundibulum,
-
Lateral retraction of the uncinate process,
-
Increase of orbital floor inward concavity,
-
Opacification of the antrum cavity,
-
Septal deviation to the affected maxillary sinus,
-
Decrease of the maxillary sinus volume,
-
Increase of the orbital cavity volume,
-
Enophthalmos and/or hypoglobus.
Opacification of the maxillary sinus cannot be considered a pathognomonic sign of SSS, because it is also present in several other sinus pathologies (for example odontogenic sinusitis) but it’s considered a consistent of SSS, as it’s present in almost all cases. However, several cases of SSS without opacification of the maxillary sinus are also reported [17, 51,52,53].
Both CT and MRI allow to obtain the diagnosis of SSS [54]. Observing the coronal plane, it is possible to recognize maxillary sinus atelectasis, orbital floor depression and the opacification of the antrum. However, CT-scan is considered the gold standard within the radiological exams for diagnosis of CMA/SSS [55].
Finally, SSS is a monolateral pathology but sporadic cases (about 5–6 cases) of bilateral SSS have been described [56,57,58,59,60] also as metachronous presentation [61].
Etiopathogenesis
The acquired obstruction of the ostiomeatal complex of Higmoro antrum is the primum movens for the onset of SSS. The obstruction results in an hypoventilation and a negative pressure into the sinus [43]. Although a chronic inflammatory process, consequent to mucosal stagnation, is inevitably present, pathogenesis of SSS is more likely due to anatomical/mechanical factors [62].
Kass et al. [63] measured the manometric pressures present into the antrum of patients affected by SSS finding an average value of − 8.4 ± 2.6 cmH2O, while the normal pressure should be isobaric.
SSS has also been associated to IgG4-related orbitopathy [64], to a mass in the deep masticatory space [65] and to a Small Lymphocytic Lymphoma [66].
SSS and Craniofacial Trauma
The traditional definition of SSS exclude the presence of a prior craniofacial trauma and/or sinus surgery. However, in literature, there are several cases report compatible with a diagnosis of SSS except for a previous trauma [67], so the recent literature suggests the possibility to include them into the traditional SSS [68,69,70,71,72,73].
Treatment
The treatment of SSS has two goals. The first is to restore the maxillary sinus aeration, the second aim is to recover the orbital architecture [74].
The ventilation of the maxillary sinus can be achieved endoscopically creating a rhinoantral access. In many cases, the orbital floor resumes spontaneously its original position as a result of the only aeration of the antrum [74] while sometimes the sinus antrostomy is not sufficient and becomes necessary an orbital floor surgical restoration [75, 76].
Some authors suggest to performe simultaneously the antrostomy and the orbital floor restoration [77, 78], others suggest to perform them deferring but some authors believe that, after antrostomy, there should be an observation period between 2 and 6 months before to procede with the correction of the orbital floor [79].
The gold standard for sinus access is FESS (Functional Endoscopic Sinus Surgery) with or without orbital floor reconstruction [80,81,82].
However, both the necessity and the timing of orbital surgery are debatable. There are three options: (1) FESS with simultaneous orbital reconstruction, (2) FESS with orbital reconstruction delayed of 2–6 months, and (3) FESS without orbital surgery [83].
Unconventional surgical procedures have also been described, for example it has been reported a case of SSS treated with balloon sinuplasty technique [84], or using a modified Foley catheter introduced into the pathological sinus and inflated [85], or with custom made prosthesis [86], or with HAG (Hyaluronic Acid Gel) intraorbital injection in extraconal position [87, 88], or by neuronavigation [89].
Our Experience
We present two explicative clinical cases, on 64 examined, on beyond 400 cases of orbital floor operated in the last 10 years.
Case 1
I.T., 34 year-old-man, white. He was involved in a motorcycle accident on 25th January 2020. After the impact, he was rescued by the passersby and suddenly conducted to G. Martino Hospital of Messina (Italy) where he underwent a Craniofacial CT scan.
The radiological examination denied the presence of brain lesion but proved the presence of multifragmentary fracture of the nasal bones, a fracture of the nasal septum, of the anterior, lateral and medial walls of the left maxillary sinus, of the left medial pteryogoid process and of the left orbital floor. It revealed, also, a plurifocal fracture of the left lamina papyracea and a fracture of the inferior orbital frame extended to the ascendent branch of the maxilla.
In Fig. 1 are reported an axial and a frontal scans and a 3-D reconstruction of the immediate post-traumatic event. In these images it’s possible to note that the volume of the maxillary sinus and of the orbital cavity involved are totally comparable to the contralateral ones, and no difference within right and left side of the skull is evident in the 3-D reconstruction too.
The patient underwent surgery 4 days after the admission. Surgery was performed under general anesthesia and, through a subciliary approach, the fracture of the orbital frame was restored and a thin matrix of alloplastic material (Medpor, microporous polyethylene high-density) was placed above the collapsed orbital floor.
The fracture of the inferior orbital frame was fixed by a 5-hole microplate and four screws of 5 mm length.
The patient was discharged 7 days and no complication occurred during the first post-operative period.
The patient hadn’t any kind of complaint for the next 3 years until, in December 2022, he came back to our clinic reported a vertical and horizontal diplopia.
The patient underwent orthotic evaluation with Hess-Lancaster test (Fig. 2). The test proved the presence of a latent hypotropia and esotropia, indeed, the patient presented a diplopia looking up and towards the left side.
Our first hypothesis was that a dislocation of the titanium plate placed in January 2020 occured, so the patient underwent a Craniofacial CT-scan.
However, no dislocation of the titanium plate was reported in the images, but they clearly showed a reduction of left maxillary sinus volume and an increase of the ipsilateral orbital cavity volume.
The left antrum was totally obliterated by hyperdense tissue until the ostioinfundibular region; the ostiomeatal complex was flared and inverted, while the infundibulum appeared medially retracted. The left orbital floor was deflected on the sinus side with a concave upper profile.
The inferior rectus muscle was stretched downwards and verticalized, with prevalence of the longitudinal axis (7–8 mm) in comparison to the transverse axis (6 mm).
Observing the patient from the submental view (Fig. 3), enophthalmos of the left eye was quite evident while, observing him from the frontal view, the hypoglobus and down dislocation of the ipsilateral globe were unequivocal. However, any alteration was evident in the 3-D reconstruction.
All the findings described seem to be an expression of a “silent sinus syndrome”, as was reported by the radiologist.
In Fig. 4 are reported the measures of the two orbital cavities and the two maxillary sinuses. It’s evident that the difference between the sagittal axis of the right and the left sinus is 7.4 mm (2.63 cm the right antrum and 1.89 cm the left one), the difference between the transversal axis of the two sinuses is 1.8 mm (2.63 cm the right antrum and 2.47 cm the left one).
Both the measures have been taken in the CT-scan slide in which the volume of the orbital cavities appeared greater.
In the same slide we measured the difference between the sagittal and the transversal axis of the right and left orbital cavity.
The difference between the left and the right sagittal axis of the orbital cavities is 7.6 mm (4.06 cm the left orbital cavity and 3.30 cm the right one), the difference between the transversal axis of the two orbital cavities is 5.4 mm (3.86 cm the left orbital cavity and 3.32 cm the right one).
We also measured the depth and the width of the antra on the axial view, considering the slide in which the two maxillary sinuses appeared greatest. The difference between the depth of the two sinuses is 2.4 mm (3.19 cm the depth of the right sinus and 2.95 cm the left one), while the difference between the width of the two sinuses is 2.1 mm (2.68 cm the width of the right sinus and 2.47 cm the left one).
After that, we measured the retrusion of the left eye, choosing the slide in which both the corneas were free from the superior eyelid. We drawn a line tangent to the most anterior point of the left and the right cornea and we measured the distance between the two lines, that is 5.62 mm, that is the measure of the left eye retrusion.
Another measure that we believed useful was the distance between the anterior wall of the maxillary sinuses and the cutaneous surface, that are 1.12 cm on the right and 1.19 cm on the left. This means that the anterior wall of the left sinus is further back of 7 mm in comparison to the left one.
Analyzing the pre-operative CT-scan we confirmed that the volume of the maxillary sinuses and of the orbital cavities of the patient were quite normal in 2020. As we can see in Fig. 1 there were any difference between the two sides of the orbital cavity and of the maxillary sinus.
Case 2
D.C., 37 years old, caucasian man. He was victim of a road accident in February 2014, when he was only 17 years old. In the incident he reported multiple fractures of the face, involving both the lower and the middle face.
The patient underwent urgent surgery during which the anatomy of the facial skull was well reconstructed (Fig. 5).
The patient was completely free of symptoms for almost 10 years, when he came back to our clinic in May 2023 referring a persistent vertical diplopia arises in the last 2 months.
The Hess-Lancaster test (Fig. 6), performed in the same May 2023, proved a mild hypotropia of the left eye.
A few days later the patient underwent a CT-scan of the facial skull that proved a reduction of the volume of the left antrum, above all in its transversal diameter, just 6.92 mm in comparison to 3.19 cm of the contralateral one (Fig. 7) while the vertical diameter was quite preserved (4.15 vs. 4.35 of the contralateral one). The CT-scan proved also an increase of the volume of the left orbital cavity whose vertical diameter was 36 mm greater in comparison to the contralateral one (3.86 cm the left orbit and 3.50 the right one) and the horizontal diameter was 20 mm greater (3.37 cm the left in comparison to 3.17 of the right one). Observing the patient in frontal view, it’s possible to note an asymmetry of the eyes position with an evident downward position of the left globe, while the CT-scan showed, in the axial view, a retroposition of the eye.
Discussion
In this work we would express the opinion that the same condition of ostiomeatal infundibulum obstruction can be idiopathic or induced by other causes, as trauma involving the nasal cavity, the orbit or, more generally, the middle face, with a clinical presentation similar to the idiopathic ones. Today they are out of diagnostic criteria of SSS but, in our opinion, they are the most frequent.
Conclusions
Based on that just exposed, we propose to keep separate the conditions of idiopathic CMA from those with previous trauma associated. We propose to continue to identify the idiopathic ones as silent sinus syndrome but to consider all the secondary cases as “Catalfamo-De Rinaldis Syndrome” (CDR Syndrome) if the following criteria are present:
-
1.
Diplopia and/or evident globe eyes asymmetries.
-
2.
Increase of horizontal and/or vertical diameters of the orbital cavity, in comparison to contralateral one, measured on the slide of a CT-scan in which the two cavities appeared greatest.
-
3.
Reduction of horizontal and/or vertical diameters of the maxillary sinus, in comparison to contralateral one, measured on the slide of a CT-scan in which the two cavities appeared greatest.
-
4.
Previous trauma involving the middle face bones.
References
Montgomery WW (1964) Mucocele of the maxillary sinus causing enophthalmus. Eye Ear Nose Throat Mon 43:41–44
Soparkar CN, Patrinely JR, Cuaycong MJ, Dailey RA, Kersten RC, Rubin PA, Linberg JV, Howard GR, Donovan DT, Matoba AY, Holds JB (1994) The silent sinus syndrome. A cause of spontaneous enophthalmos. Ophthalmology 101(4):772–778. https://doi.org/10.1016/s0161-6420(94)31267-x
Fokkens WJ, Lund VJ, Hopkins C, Hellings PW, Kern R, Reitsma S et al (2020) European position paper on rhinosinusitis and nasal polyps 2020. Rhinology 58(Suppl S29):1–464. https://doi.org/10.4193/Rhin20.600
Guillen DE, Pinargote PM, Guarderas JC (2013) The silent sinus syndrome: protean manifestations of a rare upper respiratory disorder revisited. Clin Mol Allergy 11(1):5. https://doi.org/10.1186/1476-7961-11-5
Monis PL, Parikh MH, Bhowmick H, Pai K, Shetty S, Salins PC (2021) Silent sinus syndrome: a case of sinking eyeball. J Maxillofac Oral Surg 20(4):577–580. https://doi.org/10.1007/s12663-019-01262-5
Kass ES, Salman S, Rubin PA, Weber AL, Montgomery WW (1997) Chronic maxillary atelectasis. Ann Otol Rhinol Laryngol 106(2):109–112. https://doi.org/10.1177/000348949710600204
de Dorlodot C, Collet S, Rombaux P, Horoi M, Hassid S, Eloy P (2017) Chronic maxillary atelectasis and silent sinus syndrome: two faces of the same clinical entity. Eur Arch Otorhinolaryngol 274(9):3367–3373. https://doi.org/10.1007/s00405-017-4622-8
Sivrice ME, Yasan H, Okur N, Okur E, Buyukcelik B, Kumbul YC (2022) Prevalence of chronic maxillary atelectasis: a radiological study. J Larongol Otol 136(12):1240–1244
Brandt MG, Wright ED (2008) The silent sinus syndrome is a form of chronic maxillary atelectasis: a systematic review of all reported cases. Am J Rhinol 22(1):68–73. https://doi.org/10.1017/S0022215122000056
Mangussi-Gomes J, Nakanishi M, Chalita MR, Damasco F, De Oliveira CA (2013) Stage II chronic maxillary atelectasis associated with subclinical visual field defect. Int Arch Otorhinolaryngol 17(4):409–412. https://doi.org/10.1055/s-0033-1351679
Mc Ardle B, Perry C (2010) Ethmoid silent sinus syndrome causing inward displacement of the orbit: case report. J Laryngol Otol 124(2):206–208. https://doi.org/10.1017/S0022215109990521
Brown SJ, McNab AA (2017) Ethmoid silent sinus syndrome following orbital trauma. Ophthalmic Plast Reconstr Surg 33(3):e60–e61. https://doi.org/10.1097/IOP.0000000000000746
Naik RM, Khemani S, Saleh HA (2013) Frontal silent sinus syndrome. Otolaringol Head Neck Surg 148(2):354–355. https://doi.org/10.1177/0194599812466646
Ersan M, Özdemir A, Gultam SM (2020) Silent sinus syndrome after rhinoplastic: a case report. Case Reports Plast Surg Hand Surg 7(1):73–79. https://doi.org/10.1080/23320885.2020.1788947
Ribeiro SPP, Loureiro RM, Gil JM, Dutra DL, Gomes RLE, Daniel MM (2022) Ethmoidal silent sinus syndrome after nasal swab test. Neuroradiology 64(1):205–207. https://doi.org/10.1007/s00234-021-02856-y
Magalhães C, Baptista M, Lopes G, Duarte D (2015) Silent sinus syndrome: an underdiagnosed entity. BMJ Case Rep. https://doi.org/10.1136/bcr-2015-210548
Lee DS, Murr AH, Kersten RC, Pletcher SD (2018) Silent sinus syndrome without opacification of ipsilateral maxillary sinus. Laryngoscope 128(9):2004–2007. https://doi.org/10.1002/lary.27108
Chang DT, Truong MT (2014) A child with silent sinus syndrome and spontaneous improvement after sinus surgery. Int J Pediatr Otorhinolaryngol 78(11):1993–1995. https://doi.org/10.1016/j.ijporl.2014.08.002
Leidens N, Franco A, Santos MCJ, Makeeva IM, Fernandes A (2020) Early-diagnosed silent sinus syndrome and cone-beam computed tomography in a pediatric patient: a case report. J Korean Assoc Oral Maxillofac Surg 46(2):155–159. https://doi.org/10.5125/jkaoms.2020.46.2.155
Rosa F, Figueirinhas R, Oliveira J, Sousa CAE (2018) Silent sinus syndrome in children. Acta Otorrinolaringol Esp (Engl Ed) 69(1):51–52. https://doi.org/10.1016/j.otorri.2016.11.007
Sen D, Arora V, Adlakha S, Miglani H (2016) The imploding antrum: an unusual case of nontraumatic painless enophthalmos. Indian J Ophthalmol 64(10):786–788. https://doi.org/10.4103/0301-4738.195015
Freiser ME, McCoy J, Shaffer AD, Stapleton AL (2020) Silent sinus syndrome in children. Int J Pediatr Otorhinolaryngol 134:110034. https://doi.org/10.1016/j.ijporl.2020.110034
Petraroli M, Riscassi S, Panigari A, Maltese M, Esposito S (2020) Silent sinus syndrome and williams syndrome: two rare diseases found in a pediatric patient. Front Pediatr 8:211. https://doi.org/10.3389/fped.2020.00211
Zhou S, Duncan K, Stefko ST (2018) Nonhealing orbital floor fracture in a pediatric patient: a unique presentation of pseudo-silent sinus syndrome. Orbit 37(5):375–377. https://doi.org/10.1080/01676830.2017.1423347
Sheikhi M, Faranak J (2013) The silent sinus syndrome. Dent Res J (Isfahan) 10(2):264–267. https://doi.org/10.4103/1735-3327.113369
D’Agostino Fiorenza U, Spoldi C, Nekrasova L, Pipolo C, Lozza P, Scotti A, Maccari A, Felisati G, Saibene AM (2022) Prevalence of maxillary sinus hypoplasia and silent sinus syndrome: a radiological cross-sectional retrospective cohort study. Am J Rhinol Allergy 36(1):123–128. https://doi.org/10.1177/19458924211029418
Le GK (2020) Case report: a rare case of silent sinus syndrome and vertical diplopia. Optom Vis Sci 97(7):485–488. https://doi.org/10.1097/OPX.0000000000001539
Chavez-Montoya R, Araujo-Ramìrez O, Castillo-Lòpez IY, Govea-Camacho LH (2017) Síndrome de implosión maxilar: tres casos y sus diferentes abordajes de tratamiento. Cirugía Cirujanos 85(6):529–534. https://doi.org/10.1016/j.circir.2016.08.005
Varas G, Dolman PJ (2017) Maxillary sinus wall thickening in silent sinus syndrome. JAMA Ophtalmol 135(5):e170637. https://doi.org/10.1001/jamaophthalmol.2017.0637
Gaffuri M, di Furia D, Battilocchi L, Torretta S, Accorona R, Pignataro L (2022) Unilateral silent sinus syndrome: a case report. Clin Case Rep 10(6):e05794. https://doi.org/10.1002/ccr3.5794
Gan WL (2014) Silent sinus syndrome as a recognised cause of unilateral painless enophthalmos. BMJ Case Rep. https://doi.org/10.1136/bcr-2014-203954
Eisa N, Alraiyes AH, Alraies MC (2013) Facial asymmetry: silent sinus syndrome. BMJ Case Rep. https://doi.org/10.1136/bcr-2013-010377
Bouchenna W, Delbarre M, Morfeq H, Audren F, Jani B, Froussart-Maille F (2020) A rare cause of enophthalmos: silent sinus syndrome. J Fr Ophtalmol 43(10):e371–e374. https://doi.org/10.1016/j.jfo.2020.05.007
Dumitrescu D, Fănuţă B, Stepan AE, Fronie AI, Dumitrescu CI, Mârţu MC, Şurlin P, Şurlin V, Popescu (2015) Silent sinus syndrome–report of a case. Rom J Morphol Embryol 56(1):229–237
Jovančevic L, Čanadanović V, Savović S, Zvezdin B, Komazec Z (2017) Silent sinus syndrome: One more reason for an ophthalmologist to have a rhinologist as a good friend. Vojnosanit Pregl 74(1):59–63. https://doi.org/10.2298/VSP141118141J
Michailidis G, Kyriazi S, Maravelia A, Tourna E, Couvaris CM, Kalampoukas K, Pantazis I, Lazaris P, Geroulanos S, Kalogerakou K, Bontozoglou N (2019) Chronic maxillary atelectasis under the wrappings of an Egyptian mummy. Ann Otol Rhinol Laryngol 128(12):1165–1169. https://doi.org/10.1177/0003489419879716
Keren S, Sinclair V, Mc Callum E, Martinez-Devesa P, Norris JH (2023) Silent sinus syndrome: potentially misleading features that should be recognized. Can J Ophthalmol 58(2):113–117. https://doi.org/10.1016/j.jcjo.2021.09.018
Albadr FB (2020) Silent sinus syndrome: interesting computed tomography and magnetic resonance imaging findings. J Clin Imaging Sci 10:38. https://doi.org/10.25259/JCIS_62_2020
Gòmez L, Fontàn E, Leòn JC, Garrido J (2014) Silent sinus syndrome. Clinical case. Arch Soc Esp Oftalmol 89(3):121–123. https://doi.org/10.1016/j.oftal.2012.07.029
Rullan-Oliver B, Del Toro-Diez E, Portela-Arraiza JC (2020) Natural progression of bilateral maxillary silent sinus syndrome: a metachronous case report. SAGE Open Med Case Rep. https://doi.org/10.1177/2050313X20902339
Lim BW, Jung JH, Kim ST, Kim DH, Park JW, Cha HE, Kang IG (2019) Autologous fat injection for the correction of facial depression resulting from silent sinus syndrome. J Craniofacial Surg 30(3):e191–e192
Reggie SN, Kalyam K, Holds JB, Chung SM (2018) Laughter-induced transient vision loss in a patient with silent sinus syndrome. J Neuroophthalmol 38(1):30–31. https://doi.org/10.1097/WNO.0000000000000536
Ferro A, Basyuni S, Santhanam V (2016) Not so silent sinus syndrome: a case report. Int J Surg Case Rep 23:1–3. https://doi.org/10.1016/j.ijscr.2016.04.001
Lau HT, Lim KH (2017) Isolated unilateral upper alveolar numbness in silent sinus syndrome. BMJ Case Rep. https://doi.org/10.1136/bcr-2017-219322
Jacobs JM, Chou EL, Tagg NT (2019) Rapid remodeling of the maxillary sinus in silent sinus syndrome. Orbit 38(2):166–168. https://doi.org/10.1080/01676830.2018.1473450
Singman EL, Matta NS, Silbert DI (2020) Silent sinus syndrome presenting after a roller coaster ride: a case report. J Fr Ophtalmol 43(10):e371–e374. https://doi.org/10.1016/j.jfo.2020.05.007
Saffra N, Rakhamimov A, Saint-Louis LA, Wolintz RJ (2013) Acute diplopia as the presenting sign of silent sinus syndrome. Ophthalmic Plast Reconstr Surg 29(5):e130–e131. https://doi.org/10.1097/IOP.0b013e31827bda92
AlSaloom NS, Ashri NY (2020) Silent sinus syndrome (first case report, Saudi Arabia with recommendation). Int J Surg Case Rep 74:104–108. https://doi.org/10.1016/j.ijscr.2020.08.015
Manila NG, Tahmasbi Arashlow M, Elhers S, Liang H, Nair MK (2020) Cone-beam computed tomography imaging of silent sinus syndrome: a case series and a literature review. Imaging Sci Dent 50(4):365–371. https://doi.org/10.5624/isd.2020.50.4.365
Martìnez-Capoccioni G, Varela-Martìnez E, Martìn-Martìn C (2016) Silent sinus syndrome an acquired condition and the essential role of otorhinolaryngologist consultation: a retrospective study. Eur Arch Otorhinolaryngol 273(10):3183–3188. https://doi.org/10.1007/s00405-016-3965-x
Hunt SM, Tami TA (2020) Sinusitis-induced enophthalmos: the silent sinus syndrome. Ear Nose Throat J 79(8):579–581
Stryjewska-Makuch G, Kokoszka M, Goroszkiewicz K, Karlowska-Bijak, Kolebacz B, Misiolek M (2023) What may surprise a rhinologist in everyday clinical practice: silent sinus syndrome or pneumosinus dilatans/pneumocele? Literature review and own experience. Eur Arch Oto-Rhino-Laryngol 280(2):519–527. https://doi.org/10.1007/s00405-022-07697-w
Serindere G, Belgin CA (2020) An evaluation of the relationship between maxillary sinus anterior wall depression and maxillary sinus opacity by computed tomography and panoramic radiography. Oral Radiol 36(4):383–388. https://doi.org/10.1007/s11282-020-00436-z
Eyigör H, Çekiç B, Çoban DT, Selçuk OT, Renda L, Şimşek EH, Yılmaz MD (2016) Is there a correlation between the clinical findings and the radiological findings in chronic maxillary sinus atelectasis? J Craniomaxillofac Surg 44(7):820–826. https://doi.org/10.1016/j.jcms.2016.04.004
Gaudino S, Di Lella GM, Piludu F, Martucci M, Schiarelli C, Africa E, Salvolini L, Colosimo C (2013) CT and RMI diagnosis of silent sinus syndrome. Radiol Med 118(2):265–275. https://doi.org/10.1007/s11547-012-0822-x
Vahdani K, Rose GE (2019) Bilateral silent sinus (imploding antrum) syndrome. Ophthalmic Plast Reconstr Surg 35(3):e67–e69. https://doi.org/10.1097/IOP.0000000000001350
Ho JPK, Wong E, Gunaratne DA, Singh N (2019) Chronic maxillary atelectasis (including silent sinus syndrome) can present bilaterally. J Laryngol Otol 133(3):251–255. https://doi.org/10.1017/S0022215119000252
Trope M, Schwartz JS, Tajudeen BA, Kennedy DW (2017) Bilateral silent sinus syndrome: a rare case and review of literature. Allergy Rhinol (Providence) 8(2):100–102. https://doi.org/10.2500/ar.2017.8.0197
Shieh W-S, Huggins AB, Rabinowitz MR, Rosen MR, Rabinowitz MP (2017) A case of concurrent silent sinus syndrome, thyroid eye disease, idiopathic orbital inflammatory syndrome, and dacryoadenitis. Orbit 36(6):462–464. https://doi.org/10.1080/01676830.2017.1337194
Gunaratne DA, Hasan Z, Floros P, Singh N (2016) Bilateral stage I chronic maxillary atelectasis: a case report. Int J Surg Case Rep 26:53–56. https://doi.org/10.1016/j.ijscr.2016.07.014
Farneti P, Bellusci A, Parmeggiani A, Pasquini E (2020) Metachronous bilateral silent sinus syndrome: a case report. Iran J Otorhinolaryngol 32(110):175–179. https://doi.org/10.22038/ijorl.2020.42809.2396
Zheng HD, Mecham JC, Abdel-Aty Y, Lal D, Marino MJ (2021) Microbiology, histopathology, and radiographic findings in silent sinus syndrome. Am J Rhinol Allergy 35(5):685–692. https://doi.org/10.1177/1945892421989161
Kass ES, Salman S, Montgomery WW (1996) Manometric study of complete ostial occlusion in chronic maxillary atelectasis. Laryngoscope 106(10):1255–1258. https://doi.org/10.1097/00005537-199610000-00017
Jurkov M, Olze H, Klaushen F, Bertelmann E, Schneider U, Arens P (2020) IgG4-related orbitopathy as an important differential diagnosis of advanced silent sinus syndrome. HNO 68(11):864–868. https://doi.org/10.1007/s00106-019-00798-9
Hura N, Ahmed OG, Rowan RN (2020) Atypical presentation of silent sinus syndrome: a case report and literature review. Allergy Rino (Providence) 11:2152656719899928. https://doi.org/10.1177/2152656719899928
Deekonda P, Jones HS (2022) Silent sinus syndrome secondary to lymphoma: an unusual case with radiological evidence of rapid progression. Ann Otol Rhinol Laryngol 131(8):918–922. https://doi.org/10.1177/00034894211047103
Millis MC (2021) A case of silent sinus syndrome following a history of multiple facial traumas. Clin Exp Optom 104(2):262–263. https://doi.org/10.1111/cxo.13113
Canzi G, Morganti V, Novelli G, Bozzetti A, Sozzi D (2015) Posttraumatic delayed enophthalmos: analogies with silent sinus syndrome? case report and literature review. Craniomaxillofac Trauma Reconstr 8(3):251–256. https://doi.org/10.1055/s-0034-1399799
Stryjewska-Makuch G, Goroszkiewicz K, Szymocha J, Lisowska G, Misiolek M (2022) Etiology, early diagnosis and proper treatment of silent sinus syndrome based on review of the literature and our experience. J Oral Maxillofac Surg 80(1):113.e1-118.e8. https://doi.org/10.1016/j.joms.2021.08.166
Araslanova R, Allen L, Rotenberg BW, Sowerby LJ (2017) Silent sinus syndrome after facial trauma: a case report and literature review. Laringoscope 127(7):1520–1524. https://doi.org/10.1002/lary.26527
Brown SJ, Hardy TG, McNab AA (2017) “Silent sinus syndrome” following orbital trauma: a case series and review of the literature. Ophthalmic Plast Reconstr Surg 33(3):209–212. https://doi.org/10.1097/IOP.0000000000000713
Rosso C, Saibene AM, Felisati G, Pipolo C (2022) Silent sinus syndrome: systematic review and proposal of definition, diagnosis and management. Acta Otorhinolaryngol Ital 42(4):305–316. https://doi.org/10.14639/0392-100X-N1598
Février E, Vandersteen C, Castillo L, Savoldelli C (2017) Silent sinus syndrome: a traumatic case. J Stomatol Oral Maxillofac Surg 118(3):187–190. https://doi.org/10.1016/j.jormas.2017.04.004
Cardesìn A, Escamilla Y, Romera M, Molina JA (2013) Single surgical step for endoscopic surgery and orbital reconstruction of a silent sinus syndrome. Acta Otorrinolaringol Esp 64(4):297–299. https://doi.org/10.1016/j.otorri.2011.12.004
Wladis EJ, Kersten RC, Vagefi MR, Pinheiro-Neto C, Schinder R, Kim J (2018) Clinical features and outcomes of post-traumatic silent sinus syndrome. Ophthalmic Plast Reconstr Surg 34(4):378–380. https://doi.org/10.1097/IOP.0000000000001025
Lin GC, Sedaghat AR, Bleier BS, Holbrook EH, Busaba NY, Yoon MK, Gray ST (2015) Volumetric analysis of chronic maxillary atelectasis. Am J Rhinol Allergy 29(3):166–169. https://doi.org/10.2500/ajra.2013.27.4173
Claròs P, Sobolewska AZ, Cardesa A, Lopez-Fortuny M, Claros A (2019) Silent sinus syndrome: combined sinus surgery and orbital reconstruction—report of 15 cases. Acta Otolaryngol 139(1):64–69. https://doi.org/10.1080/00016489.2018.1542161
Tieghi R, Malagutti N, Valente L, Carnevali G, Clauser LC (2017) Combined endoscopic and trans palpebral orbital reconstruction for silent sinus syndrome. J Craniofac Surg 28(4):955–958. https://doi.org/10.1097/SCS.0000000000003421
Kram YA, Pletcher SD (2014) Maxillary sinus posterior wall remodeling following surgery for silent sinus syndrome. Am J Otolaryngol 35(5):623–625. https://doi.org/10.1016/j.amjoto.2014.05.007
Hernaiz-Leonardo JC, Alqunaee M, Moghimi S, Alim BM, Javadian F, Vafaei-Nodeh S, Pascual A, Javer A (2022) Maxillary sinus volume changes after functional endoscopic sinus surgery in patients with chronic maxillary atelectasis and silent sinus syndrome. Int Forum Allergy Rhinol 12(9):1212–1215. https://doi.org/10.1002/alr.22985
Kim S-H (2016) Successful treatment of silent sinus syndrome with combined endoscopic sinus surgery and blepharoplasty without orbital floor reconstruction. J Craniofac Surg 27(6):e586–e588. https://doi.org/10.1097/SCS.0000000000002998
Mantsopoulos K, Thimsen V, Karkos P, Sievert M, Hiro H, Constantinidis J (2022) Silent sinus syndrome: reduction of surgical invasiveness in an underdiagnosed clinical entity. Am J Otolaryngol 43(5):103541. https://doi.org/10.1016/j.amjoto.2022.103541
Bhalla N, Rosenstein J, Dym H (2019) Silent sinus syndrome: interesting clinical and radiologic findings. J Oral Maxillofac Surg 77(10):2040–2043. https://doi.org/10.1016/j.joms.2019.03.042
Kilty SJ (2014) Maxillary sinus atelectasis (silent sinus syndrome): treatment with ballon sinuplasty. J Laryngol Otol 128(2):189–191. https://doi.org/10.1017/S0022215113003538
Kashima T, Goldberg RA, Kohn JC, Rootman DB (2016) One-stage bone strip reconstruction technique with balloon sinus dilatation surgery for chronic maxillary atelectasis. Clin Ophthalmol 10:2363–2368. https://doi.org/10.2147/OPTH.S103809
Baig MZ, Weber JF, Bhora F, Al Shetawi AH (2020) Surgical advances in the management of the silent sinus syndrome: our experience and review of the literature. J Oral Maxillofac Surg 78(12):2289–2295. https://doi.org/10.1016/j.joms.2020.07.026
Mavrikakis I, Detorakis ET, Yiotakis I, Kandiloros D (2012) Nonsurgical management of silent sinus syndrome with hyaluronic acid gel. Ophthalmic Plast Reconstr Surg 28(1):e6-7. https://doi.org/10.1097/IOP.0b013e31820d8840
Grusha Y, Khrovin V, Stoyukhina A, Sheptulin V (2015) Hyaluronic acid gel re-injection for enophthalmos correction in silent sinus syndrome. Orbit 34(6):351–353. https://doi.org/10.3109/01676830.2015.1078376
Chariba I, Lazard DS, Sain-Oulhen C, Lecanu JB (2014) Correlation between the rate of asymmetry volume of maxillary sinuses and clinical symptomatology in the silent sinus syndrome: a retrospective study about 13 cases. Rev Laryngol Otol Rhinol (Bord) 135(4–5):197–200
Funding
This research received no funding grant from any funding agency in the public or commercial sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Catalfamo, L., Siniscalchi, E.N., De Ponte, F.S. et al. Post-traumatic Sinus Syndrome, Proposal for a New Clinical Entity (CDR Syndrome) as Variant of the Silent Sinus Syndrome: Systematic Review and Case Series. Indian J Otolaryngol Head Neck Surg 76, 1378–1388 (2024). https://doi.org/10.1007/s12070-023-04112-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-023-04112-6