Abstract
(−)-Epigallocatechin-3‑gallate (EGCG), the predominant constituent of green tea, has been demonstrated to be neuroprotective against acute ischemic stroke. However, the long-term actions of EGCG on neurogenesis and functional recovery after ischemic stroke have not been identified. In this study, C57BL/6 mice underwent middle cerebral artery occlusion (60 min) followed by reperfusion for 28 days. Neural progenitor cells (NPCs) were isolated from ipsilateral subventricular zone (SVZ) at 14 days post-ischemia (dpi). The effects of EGCG on the proliferation and differentiation of NPCs were examined in vivo and in vitro. Behavioral assessments were made 3 days before MCAO and at 28 dpi. SVZ NPCs were stimulated with lipopolysaccharide (LPS) in vitro to mimic the inflammatory response after ischemic stroke. We found that 14 days treatment with EGCG significantly increased the proliferation of SVZ NPCs and the migration of SVZ neuroblasts, as well as functional recovery, perhaps through M2 phenotype induction in microglia. LPS stimulation promoted the neuronal differentiation in cultured NPCs from the ischemic SVZ. EGCG treatment (20 or 40 μM) further significantly increased the neuronal differentiation of LPS-stimulated SVZ NPCs. After screening for multiple signaling pathways, the AKT signaling pathway was found to be involved in EGCG-mediated proliferation and neuronal differentiation of NPCs in vitro. Taken together, our results reveal a previously uncharacterized role of EGCG in the augment of proliferation and neuronal differentiation of SVZ NPCs and subsequent spontaneous recovery after ischemic stroke. Thus, the beneficial effects of EGCG on neurogenesis and stroke recovery should be considered in developing therapeutic approaches.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stroke is the second most common cause of death and the major cause of permanent disability in adults worldwide [1, 2]. Recombinant tissue plasminogen activator (tPA) is the only FDA-approved thrombolytic therapy for clinical stroke treatment, but the efficacy and safety of its therapeutic application are limited by its narrow therapeutic window and side effects [3]. Thus, there is a compelling need to expand the narrow repertoire of therapeutic opportunities for stroke. Clinical and research efforts have focused on promoting post-ischemic neurovascular remodeling and functional recovery in the later phases of stroke recovery.
Green tea is an extremely popular beverage worldwide and is next to water, and its habitual consumption has long been associated with health benefits [4]. (−)-Epigallocatechin-3‑gallate (EGCG), the most abundant and bioactive polyphenol in green tea [5], displays strong preventive effects against diabetes, Parkinson’s disease, Alzheimer’s disease, obesity, aging, cancer, and stroke [6–8]. Our and other previous studies have shown that EGCG exerts strong neuroprotective effects against ischemic damage in the acute phase of ischemic stroke [8, 9]. However, the long-term effects of EGCG on the post-stroke neurogenesis and functional recovery in the later phases of stroke recovery remain unclear. Increasing evidences have indicated that EGCG could confer various neurological benefits. EGCG promotes neuronal plasticity in the hippocampus of mice [10]. Long-term oral administration of green tea polyphenol EGCG promoted spatial cognition learning ability of animals, which may be associated with the increasing angiogenesis and neuronal spine density in the dentate gyrus of the hippocampus [11]. EGCG has also been demonstrated to promote the proliferation of adult hippocampal neural progenitor cells (NPCs) and thus improve spatial cognition in mice [12]. In addition, EGCG treatment promotes neural stem cells (NSCs) proliferation and inhibits free radical-induced degradation of NSCs, which have the potential to differentiate into neurons and glias around the damaged area following traumatic brain injury [13]. Taken together, all these studies indicate that EGCG is closely related to the proliferation and differentiation of NSCs/NPCs. Therefore, we speculate that consistent administration of EGCG during stroke recovery could promote the proliferation and differentiation of NPCs in the adult subventricular zone (SVZ) and thus promote functional recovery.
In an in vivo study, we found that EGCG treatment during stroke recovery significantly promoted functional recovery via enhancement of the proliferation of SVZ NPCs and the migration of SVZ neuroblasts, which could be associated with the microglial response toward a neuroprotective M2 phenotype. Our in vitro study demonstrated that EGCG treatment (20 or 40 μM) significantly increased the proliferation and neuronal differentiation of lipopolysaccharide (LPS)-stimulated SVZ NPCs dissociated from the ischemic ipsilateral SVZ at 14 days post-ischemia (dpi), all of which were through the activation of AKT signaling pathway.
Methods
Animals and Middle Cerebral Artery Occlusion (MCAO) Model
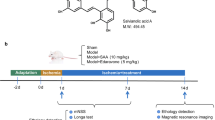
Male wild-type (WT) C57BL/6 mice were purchased from the Wuhan University Laboratory Animal Center. The mice used for all experiments were 8–10 weeks old and were housed under specific pathogen-free conditions at the Animal Laboratory Center of Tongji Medical College. All experiments with the mice were performed in accordance with the protocols approved by the Animal Care and Use Committee of Tongji Medical College, Huazhong University of Science and Technology. The C57BL/6 mice (24–25 g) were anesthetized intraperitoneally (i.p.) with ketamine (100 mg/kg) and xylazine (8 mg/kg). Focal cerebral ischemia was induced by MCAO with a 6–0 silicone-coated nylon monofilament for 1 h, to block the origin of the MCA as previously described [14]. Occlusion was confirmed by laser Doppler flowmeter (Periflux system 5000, PERIMED, Stockholm, Sweden) with a probe placed on the thinned skull over the lateral parietal cortex [14]. The blood flow was restored by withdrawal of the monofilament. Body temperature was maintained at 37 ± 0.5 °C with a feedback temperature control unit until the mice had recovered from surgery. Our previous studies showed no physiological differences between groups [14, 15].
In Vivo Drug Treatments
Treatment groups were assigned in a randomized and blinded manner. The mice intracerebroventricular (ICV) injection was performed under anesthesia using a stereotaxic instrument (RWD Life Science Co., Ltd.) with a sterile 26-G Hamilton microsyringe (80330; Hamilton Company, Reno, NV). EGCG was dissolved in dimethyl sulfoxide (DMSO) (all obtained from Sigma-Aldrich, St. Louis, MO, USA). EGCG (1 mg/ml; 2 μl) or 1 % DMSO (2 μl) was injected slowly (0.5 μl/min) into the left ventricle (0.9 mm laterally, 0.1 mm posteriorly, 3.1 mm deep from the bregma). EGCG was repeated every 24 h for 2 weeks starting at 14 dpi. Drug treatments were performed by an investigator blinded to the experimental protocol.
5-Bromo-2′-deoxyuridine (BrdU) Labeling
We assessed cell proliferation by treating the mice i.p. twice with BrdU (dissolved at 10 mg/ml in saline, 50 mg/kg per injection; Sigma, St. Louis, MO, USA) with an 8-h interval between injections at 27 dpi; on the following day, the mice were humanely killed to analyze BrdU labeling of dividing cells.
Functional Assays
The elevated body swing test (EBST) was performed to evaluate the symmetry of motor behavior at 28 dpi [16]. The mice (n = 12/group) were examined for lateral movements/turning when their bodies were suspended 10 cm above the testing table by lifting their tails. A swing was recorded when mice moved their head away from the vertical axis (angle >10°) in three sets of 10 trials, performed over 5 min. Results are expressed as the ratio of the total number of the contralateral swings.
The rotarod test provided an index of the forelimb and hindlimb motor coordination and balance [16]. The mice (n = 12/group) were trained daily on an accelerating (5 to 40 rpm) rotating rod for 3 days before MCAO; only those mice able to remain on the rod for 20 s at 40 rpm were subjected to MCAO. Test sessions consisting of three trials at 40 rpm were carried out just before focal ischemia, at 28 dpi, by an investigator who was blinded to the experimental groups. The final score was expressed as the mean time that a mouse was able to remain on the rod over three trials.
The pole test was used to assess forelimb strength, ability to grasp, and balance performed in a blinded fashion at 28 dpi [17]. The mice (n = 12/group) were placed head upward near the top of a vertical steel pole (60-cm high with a rough surface). Thereafter, both times taken to orientate the body completely downward and to reach the floor with all four paws were recorded.
Neurosphere Cultures
Ipsilateral SVZ cells were dissociated from ischemic hemispheric brains at 14 dpi. After digestion, the cells were cultured in cell proliferation medium (DMEM/F-12 medium (Thermo Scientific HyClone, Beijing, China) supplemented with 1 % penicillin plus streptomycin (Solarbio Science & Technology, Beijing, China), 2 μg/ml heparin (StemCell Technologies, Vancouver, Canada), 1 % insulin-transferrin-selenium (ITS; Sigma, St. Louis, MO, USA), 2 % B27 supplement (Invitrogen/Gibco, Carlsbad, CA, USA), 20 ng/ml epidermal growth factor (EGF; PeproTech, Rocky Hill, NJ, USA), and 20 ng/ml basic fibroblast growth factor (bFGF; PeproTech, Rocky Hill, NJ, USA)) at a concentration of 5 × 104 cells/ml. The cells were maintained at 37 °C with 5 % CO2 in an incubator with high humidity. The medium was changed twice per week. After 7–10 days of culture, primary neurospheres of 100–150 μm in diameter could be collected without disturbing the attached cells and were passaged into a fresh cell proliferation medium. Passage 2 SVZ neurospheres were dissociated from single cells and placed onto a poly-l-ornithine (Sigma, St. Louis, MO, USA)- and laminin (Invitrogen, Carlsbad, CA, USA)-coated coverslip in a cell proliferation medium. At 18 h post-plating, the medium was changed into a differentiation medium (DMEM/F-12 medium supplemented with 1 % penicillin plus streptomycin, 1 % ITS, 2 % B27 supplement, 1 % FBS (Gibco, Carlsbad, CA, USA)) and differentiated for 7 days.
Assessment of Neurosphere Formation and Proliferation
Passage 2 neurospheres were dissociated from single cells and were passaged into 24-well plates and cultured in a fresh cell proliferation medium. Two hours after the passage, LPS (10 ng/ml) was added to the proliferation medium to mimic the inflammation conditions that were induced by cerebral ischemia [18]. At 2 h after LPS treatment (10 ng/ml), the proliferation medium was supplemented with EGCG (10, 20, or 40 μM) or 1 % DMSO every 24 h for 7 days. The neurosphere number was counted on day 8. Then, the primary neurospheres were dissociated from single cells and placed onto a poly-l-ornithine- and laminin-coated coverslip in a cell proliferation medium. At 18 h post-plating, the medium was changed into a differentiation medium and BrdU was added to the cells for 16 h, followed by fixation using 4 % paraformaldehyde.
The phosphatidylinositol 3-kinase (PI3K)/Akt inhibitor LY294002 (25 μM; Sigma, St. Louis, MO, USA) was added to the cultures 30 min prior to EGCG treatment.
Assessment of Neural Precursor Cells Differentiation
At 2 h after LPS (10 ng/ml) treatment, the differentiation medium of passage 2 NPCs was supplemented with EGCG (10, 20, or 40 μM) or 1 % DMSO every 24 h for 7 days. Differentiated cells were collected by either direct cell lysis for Western blotting analysis or by fixation using 4 % paraformaldehyde for immunohistochemical staining using cell lineage-specific antibodies. LY294002 was also added to the cultures 30 min prior to EGCG treatment.
Real-Time PCR Analysis
Total RNA was isolated using Trizol Reagent (Invitrogen, Carlsbad, CA). Complementary DNA (cDNA) was synthesized from total RNA with Taqman reverse transcriptase (Applied Biosystems, Foster City, CA). cDNA were amplified using Power SYBR Green (Applied Biosystems, Foster City, CA). Two-step real-time PCR was performed (95 °C for 15 s, 60 °C for 60 s extension and detection, 40 cycles) with specific primers. The PCR primers are shown in Table 1. The relative quantitation value is expressed as 2−ΔCt, where ΔCt is the difference between the mean ΔCt value of duplicate measurements of the sample and β-actin control.
Western Blotting
Western blotting was done according to our previously established protocols [14, 15]. The primary cells were lysed in RIPA buffer containing protease and phosphatase inhibitors (KeyGen Biotech Co., Ltd., Nanjing, China). Equal amounts of protein were subjected to SDS-PAGE analysis, transferred onto a PVDF membrane and probed with primary antibodies against phospho-AKT (p-AKT), total-AKT (t-AKT), p-ERK, t-ERK, p-JNK, t-JNK, p-p38, t-p38, or β-actin (all obtained from Cell Signaling Technology, Danvers, MA, USA). After washing, the membranes were treated with the corresponding horseradish peroxidase (HRP)-conjugated secondary antibody. Chemiluminescence detection was carried out with ECL Western Blotting Detection Reagents (Millipore, Billerica, MA, USA) plus BioWest enhanced chemiluminescence (UVP, Upland, CA). Band intensity was quantified with ImageJ software (NIH, Bethesda, MD, USA).
Immunocytochemistry
The mice were transcardially perfused with 4 % paraformaldehyde, and the brains were embedded with paraffin. The brains were cut into 4-μm-thick coronal sections. Cell cultures were fixed using 4 % paraformaldehyde for 15 min. For both sections and cells, nonspecific binding was blocked using normal goat serum. Immunoassays were performed using the following antibodies at concentrations (and using protocols) recommended by the respective manufacturers: BrdU, doublecortin (DCX), Ki67, beta-3-tubulin (Tuj-1), glial fibrillary acidic protein (GFAP) (all obtained from Cell Signaling Technology, Danvers, MA, USA), or Iba1 (Wako Pure Chemical Industries, Osaka, Japan). The primary antibodies were detected with cy3-conjugated goat anti-rabbit, DyLight 488-conjugated goat anti-mouse secondary antibody. The nuclei were counterstained by DAPI.
Statistical Analyses
Multiple comparisons were performed by one-way analysis of variance (ANOVA) followed by Newman-Keuls multiple comparison tests for multiple comparisons (GraphPad Prism statistics software version 5.0, La Jolla, CA, USA). Two groups were compared by two-tailed Student’s t test. Behavioral data were analyzed by two-way ANOVA with repeated measures, followed by post hoc multiple comparison tests. All data are presented as mean ± SEM. A P value of <0.05 was considered statistically significant.
Results
EGCG Enhances the NPCs Proliferation and Neuroblasts Migration During Stroke Recovery
We assessed cell proliferation by treating 27 dpi mice twice with S-phase marker BrdU with an 8-h interval between injections; on the following day, the animals were humanely killed to analyze BrdU labeling of dividing cells. Results showed that the mice treated with EGCG had a significantly higher number of BrdU+ cells in the ischemic SVZ to the mice treated with 1 % DMSO at 28 dpi (Fig. 1a, b; P < 0.05). Consistently, the number of cell proliferation marker Ki67+ cells in the ischemic SVZ was also significantly increased in the mice treated with EGCG (Fig. 1c, d; P < 0.05).
EGCG promotes the proliferation of neural progenitor cells (NPCs) in the adult subventricular zone (SVZ) and the migration of neuroblasts after ischemic stroke. a Immunofluorescence imaging for BrdU+ (red) cells coexpressing DCX (green) in the ischemic SVZ and striatum at 28 days post-ischemia (dpi). Bar = 50 μm. b Quantitative comparison of BrdU-labeled and BrdU/DCX double-labeled cells in the ischemic SVZ and striatum for each group. Data represent mean ± SEM, n = 5; # P < 0.05. c Representative micrographs of Ki67 labeling in the ischemic SVZ at 28 dpi. Bar = 100 μm. d Quantitative determination of Ki67-labeled cells in the ischemic SVZ for each group. Data represent mean ± SEM, n = 5; *P < 0.05, significantly different from the DMSO-treated sham group; # P < 0.05. LV lateral ventricles, Str striatum
Next, we evaluated DCX expression because DCX as a marker for neuronal precursors and neurogenesis is expressed by virtually all neuroblasts. The migration of newly generated neuroblasts and SVZ neurogenesis was detected with BrdU and DCX double marker. We observed more BrdU+/DCX+ cells in EGCG-treated mice in the ischemic striatum (Fig. 1a, b; P < 0.05).
Promoting Effects of EGCG on Post-Stroke Functional Recovery
Improving functional outcome after stroke is the ultimate goal of stroke treatment. It is essential to detect the functional recovery after the intervention. We found that deficits in the EBST (P < 0.05), rotarod test (P < 0.05), and pole test (P < 0.05 and P < 0.01, respectively) were better in EGCG-treated mice tested at 28 dpi (Fig. 2a–d).
EGCG improves post-ischemic functional recovery. Behavioral tests were assessed at 28 days post-ischemia (dpi), including the elevated body swing test (EBST) (a), rotarod test (b), pole test (time to turn completely head down (c) and time to reach the floor (d)). Data represent mean ± SEM, n = 12; # P < 0.05, ## P < 0.01
EGCG Enhanced Microglial Activation
Recent studies suggest that activated microglia contribute to post-stroke neurogenesis and functional recovery [19]. Therefore, to test the effects of EGCG on microglia, we used immunofluorescence staining of Iba1 in the peri-infarct striatum at 28 dpi. Microglia were classified into ramified, intermediate, amoeboid, or round phenotypes (Fig. 3a), which is correlated with distinct functional states, ramified microglia signifying resting, and round microglia, typically the most activated ones [20, 21]. In the peri-infarct striatum, there was a dramatic decrease of ramified microglia, whereas a significant increase of round microglia was observed 28 days after the treatment with EGCG (Fig. 3b, c; P < 0.05).
EGCG enhances microglial activation in the peri-infarct striatum at 28 days after ischemia. a Photomicrographs showing examples of microglia classified into four different morphological phenotypes: ramified, intermediate, amoeboid, and round in striatal peri-infarct area. b Representative micrographs of Iba1-labeling in the peri-infarct striatum at 28 days after 60 min MCAO or sham surgery. Bar = 50 μm. c Percentage of microglia with different morphological phenotypes of the total number of Iba1+ cells in the peri-infarct striatum. Data represent mean ± SEM, n = 5; # P < 0.05
EGCG Treatment Promoted the Polarization of the Microglia Toward the M2 Phenotype in the Ischemic Brain
Activated microglia are classified as either classically activated (M1) or alternatively activated (M2) microglia, which are characterized by the expression of the signature genes that are associated with the M1 or M2 phenotype [22]. The M1 phenotype is involved in tissue injury whereas the M2 phenotype has a role in neurogenesis and functional recovery [22, 23]. To further understand the EGCG-induced increase in activated microglia, we examined markers of activated microglia phenotypes in the ischemic brain. We found that EGCG treatment significantly decreased M1 markers (CD16, CD11b, CD32, inducible nitric oxide synthase (iNOS), and tumor necrosis factor-α (TNF-α)) and increased M2 markers (IL-10, arginase-1 (Arg-1), transforming growth factor-β (TGF-β), CD206, and YM1) of activated microglia (Fig. 4; all changes P < 0.05), suggesting a shift from M1 to M2 phenotypes at 28 dpi.
EGCG inhibits the M1 phenotype and promotes the M2 phenotype in microglia after ischemic stroke. a M1 marker (CD16, CD11b, CD32, iNOS, and TNF-α) mRNA levels. Data represent mean ± SEM, n = 5; # P < 0.05, ## P < 0.01. b M2 marker (IL-10, Arg-1, TGF-β, CD206, and YM1) mRNA levels. Data represent mean ± SEM, n = 5; # P < 0.05, ## P < 0.01. Real-time polymerase chain reaction was performed using total RNA extracted from ischemic brains at 28 days after transient MCAO or from sham-operated brains. iNOS inducible nitric oxide synthase; TNF-α tumor necrosis factor-α; Arg-1 arginase-1; and TGF-β transforming growth factor-β
EGCG Promotes the Proliferation of NPCs Through AKT In Vitro
To further investigate the direct function of EGCG in NPCs, we prepared neurosphere cultures from the SVZ of ischemic mice at 14 dpi. LPS (10 ng/ml) was added to the medium to mimic the inflammation conditions that were induced by cerebral ischemia [18]. Bright-field microscope images showed that LPS treatment of NPCs decreased the size and the number of the neurosphere compared with the control group (Fig. 5a, b; P < 0.05), and the percentage of cells that incorporated BrdU was significantly decreased by the treatment with LPS (Fig. 5c, d; P < 0.05).
EGCG directly promotes the proliferation of neural progenitor cells (NPCs) in vitro. a Representative images of neurospheres treated with 10, 20, or 40 μM EGCG or DMSO. Bar = 50 μm. b Quantification of the numbers of neurospheres for each group. Data represent mean ± SEM from three experiments. *P < 0.05, significantly different from the control group; # P < 0.05, significantly different from the DMSO-treated group stimulated by LPS. c Representative micrographs of BrdU labeling. BrdU was added to NPCs at the time of differentiation induction for 16 h and then subjected to immunofluorescence analysis. DAPI was used to label the nucleus. Bar = 20 μm. d Quantification of the percentage of BrdU-positive cells for each group. Data represent mean ± SEM from three experiments. *P < 0.05, significantly different from the control group; # P < 0.05, significantly different from the DMSO-treated group stimulated by LPS
We next investigate the effects of EGCG on neurosphere formation and proliferation of LPS-stimulated NPCs, the neurosphere number and the percentage of cells that incorporated BrdU was measured 7 days after the treatment of EGCG at different concentrations (10, 20, 40 μM). The neurosphere formation (Fig. 5a, b; P < 0.05 and P < 0.05, respectively) and proliferation (Fig. 5c, d; P < 0.05 and P < 0.05, respectively) of LPS-stimulated NPCs were significantly increased by EGCG (20 or 40 μM).
We then explored the potential underlying mechanisms in vitro. Mitogen-activated protein kinase (MAPK) and PI3K/AKT are major signaling pathways implicated in NPCs proliferation and differentiation [24–28]. The expression of p-AKT was significantly increased after EGCG treatment in the LPS-treated group compared with the LPS-only treatment group (P < 0.05), without altering the levels of p-ERK, p-JNK, and p-38 (Fig. 6a). LY294002 pretreatment effectively inhibited the protein level of p-AKT (Fig. 6b; P < 0.05), which significantly reduced the neurosphere number (Fig. 6c; P < 0.05) and the percentage of cells that incorporated BrdU (Fig. 6d; P < 0.05).
AKT signaling is involved in the promoting effects of EGCG on the proliferation of neural progenitor cells (NPCs) in vitro. a Western blotting and quantitative data for p-Akt, p-ERK, p-JNK, and p-p38 in passage 2 NPCs treated with EGCG after 7 days of proliferation. Data represent mean ± SEM from three experiments; # P < 0.05. b Western blotting and quantitative data for p-AKT in passage 2 NPCs treated with EGCG with or without the addition of LY294002 to cell proliferation medium. Data represent mean ± SEM from three experiments; # P < 0.05. c Representative images and quantification of neurospheres treated with 20 μM EGCG with or without the addition of LY294002 to cell proliferation medium. Bar = 50 μm. Data represent mean ± SEM from three experiments; # P < 0.05. d Representative micrographs of BrdU labeling, and quantification of the percentage of BrdU-positive cells for each group. Bar = 20 μm. Data represent mean ± SEM from three experiments; # P < 0.05
EGCG Promotes the Neuronal Differentiation of NPCs Through AKT In Vitro
We analyzed the role of EGCG in NPC differentiation, and immunofluorescent staining with antibodies against Tuj-1 and GFAP was performed on NPCs after 7 days of differentiation. LPS, which is added to the medium to mimic the inflammation conditions after ischemic stroke, significantly increased the percentage of Tuj-1+ neurons and reduced the percentage of GFAP+ astrocytes (Fig. 7a, b; P < 0.05 and P < 0.05, respectively). The percentage of Tuj-1+ neurons was further significantly increased after 20 μM EGCG (P < 0.05 and P < 0.05, respectively) or 40 μM EGCG (P < 0.05 and P < 0.05, respectively) treatment in the LPS-treated group compared with the LPS-only treatment group (Fig. 7a, b).
EGCG directly promotes the neuronal differentiation of neural progenitor cells (NPCs) in vitro. Double immunofluorescence labeling (a) and quantitative analyses (b) for Tuj-1 (red) and GFAP (green) in passage 2 NPCs treated with 10, 20, or 40 μM EGCG or DMSO. Bar = 50 μm. Data represent mean ± SEM from three experiments; *P < 0.05, significantly different from the control group; # P < 0.05, significantly different from the DMSO-treated group stimulated by LPS
The levels of p-AKT were significantly increased after EGCG treatment in the LPS-treated group compared with the LPS-only treatment group, without altering the expression of p-ERK, p-JNK, and p-38 (Fig. 8a; P < 0.05). LY294002 pretreatment effectively inhibited the protein level of p-AKT (Fig. 8b; P < 0.05), which significantly decreased the percentage of Tuj-1+ neurons (Fig. 8c, d; P < 0.05).
AKT signaling is involved in the promoting effects of EGCG on the neuronal differentiation of neural progenitor cells (NPCs) in vitro. a Western blotting and quantitative data for p-Akt, p-ERK, p-JNK, and p-p38 in passage 2 NPCs treated with EGCG after 7 days of differentiation. Data represent mean ± SEM from three experiments; # P < 0.05. b Western blotting and quantitative data for p-AKT in passage 2 NPCs treated with EGCG with or without the addition of LY294002 to differentiation medium. Data represent mean ± SEM from three experiments; # P < 0.05. Double immunofluorescence labeling (c) and quantitative analyses (d) for Tuj-1 (red) and GFAP (green) in passage 2 NPCs treated with 20 μM EGCG with or without the addition of LY294002 to differentiation medium. Bar = 50 μm. Data represent mean ± SEM from three experiments; # P < 0.05
Discussion
Stroke treatment is constrained by narrow therapeutic windows and the clinical inefficacy of agents that showed preclinical promise. Yet, animal and clinical studies suggest considerable post-stroke neurovascular remodeling, which could allow treatment with recovery-modulating agents. Our in vivo results revealed that chronic treatment with green tea polyphenol EGCG could promote neurogenesis and functional recovery in the later phases of stroke recovery. The clinical and theoretical significance of our findings is twofold. First, it suggests that post-stroke recovery can be enhanced without the stringent time-dependency of neuroprotective strategies. Second, it suggests a treatment for post-stroke functional recovery that is also neuroprotective in acute ischemic brain injury [8, 9].
Accumulating evidence suggests that M2-polarized microglia resolve the over-activation of inflammation and promote tissue repair following cerebral ischemic injury [19, 22, 23]. We present in vivo evidence that the promoting effects of EGCG on the neurogenesis and long-term recovery could be associated with increased activation of an M2 phenotype of microglia in the ischemic brain. In this study, we assessed the cerebral polarization of the microglia by analyzing the expression of signature genes associated with M1 or M2 polarization in the ischemic brain. We observed an increase in M2 signature gene expression and a decrease in M1 gene expression in the ischemic brain. Therefore, we suggest that the predominant M2 phenotype of microglia after EGCG treatment could provide a better environment for neurogenesis by resolving inflammation via the secretion of anti-inflammatory cytokines after ischemic stroke, such as IL-10, TGF-β, and Arg-1. However, the mechanism by which EGCG activates microglia and polarizes activated microglia to M2 phenotypes remains to be defined.
The promoting effects of EGCG on the neurogenesis and long-term recovery could also be corrected with the direct promotion of the proliferation and neuronal differentiation of SVZ NPCs, as further demonstrated in vitro by our results. To mimic the inflammatory conditions observed in vivo experimental ischemic stroke, we incubated NPCs with LPS in vitro, which is due to its similar effects with ischemic stimulation on the proliferation and differentiation of NPCs in vivo [18]. The proliferation rate was evaluated through neurosphere formation assays. The size and the number of the neurosphere reflect the state of proliferation. LPS was shown to be capable of causing the size of the neurosphere to decrease [18]. In our present study, we found that LPS treatment markedly decreased the number of the neurosphere and the percentage of cells that incorporated S-phase marker BrdU, both indicating that LPS inhibits the proliferation rate of NPCs. One explanation is that LPS stimulation may inhibit proliferation but promote neuronal differentiation of NPCs. More DCX-positive NSCs and microtubule associated protein-2 (MAP-2)-positive mature neuronal cells were detected after the stimulation of LPS [18]. Our present results further substantiate the promoting effect of LPS on the neuronal differentiation of NPCs, which is similar to the post-ischemic stimulation after stroke. Stroke, induced by MCAO, triggers increased generation of neuroblasts in SVZ, which migrate toward the damaged striatum where they differentiate to mature striatal neurons [29, 30]. Endogenous neurogenesis may be one of the mechanisms underlying the spontaneous recovery after stroke, but its contribution is probably minor [31]. We found that EGCG, which is the main polyphenolic constituent in green tea, markedly enhanced endogenous neurogenesis and long-term functional recovery after cerebral ischemia. When studied in vitro, EGCG could obviously promote the proliferation and neuronal differentiation of SVZ NPCs under LPS-stimulated inflammatory conditions that mimicking the in vivo microenvironment after ischemic stroke.
Our in vitro results showed that AKT signaling pathway played an important role in EGCG-mediated proliferation and neuronal differentiation of SVZ NPCs after screening for PI3K/AKT and MAPK signaling pathways, which are major signaling pathways implicated in the proliferation and differentiation of NPCs [24–28]. Subsequently, we showed that the effects of EGCG appear not to be associated with the ERK, JNK, or p38 pathways as these were not different between EGCG- and DMSO-treated mice. The serine/threonine protein kinase AKT is shown to play a critical role in stroke-induced NPC proliferation [26, 32–34]. Depletion of PTEN, a negative regulator of the PI3K/AKT signaling pathway, leads to persistently enhanced self-renewal of NPCs [35]. Inactivation of AKT is indeed required for the inhibitory effects of caspase-3 on NPCs proliferation [34]. Our data revealed that AKT signaling plays an important role in the promoting effects of EGCG on the neurogenesis. However, in addition to AKT, multiple other signaling pathways may also contribute to the proneurogenesis effects of EGCG during stroke recovery. Future studies are needed to study how AKT signal may modulate EGCG-induced neurogenesis after stroke.
Conclusions
Neurogenesis holds promise for brain repair and long-term functional recovery after ischemic stroke. Thus, proneurogenesis and recovery-modulating agents are needed. Our data here suggests that delayed treatment with EGCG improves stroke outcomes in an apparently proneurogenesis manner involving increased SVZ NPCs proliferation, enhanced migration of neuroblasts, and elevated neuronal differentiation, associated with improved recovery of sensory and motor cortical function. Increased activation of an M2 phenotype of microglia in the ischemic brain could provide a better environment for EGCG-induced neurogenesis. Considering that EGCG also exerts neuroprotective effects against neuronal death during acute stroke, our data suggest that EGCG could be used for the treatment of ischemic stroke throughout all phases from acute to chronic. However, additional evaluation of EGCG in the clinical setting may be warranted.
References
Donnan GA, Fisher M, Macleod M, Davis SM (2008) Stroke. Lancet 371:1612–1623
Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Blaha MJ, Dai S, Ford ES et al (2014) Heart disease and stroke statistics—2014 update: a report from the American Heart Association. Circulation 129:e28–e292
Schwamm LH, Ali SF, Reeves MJ, Smith EE, Saver JL, Messe S, Bhatt DL, Grau-Sepulveda MV et al (2013) Temporal trends in patient characteristics and treatment with intravenous thrombolysis among acute ischemic stroke patients at Get With The Guidelines-Stroke hospitals. Circ Cardiovasc Qual Outcomes 6:543–549
Suzuki Y, Miyoshi N, Isemura M (2012) Health-promoting effects of green tea. Proc Jpn Acad Ser B Phys Biol Sci 88:88–101
Graham HN (1992) Green tea composition, consumption, and polyphenol chemistry. Prev Med 21:334–350
Singh BN, Shankar S, Srivastava RK (2011) Green tea catechin, epigallocatechin-3-gallate (EGCG): mechanisms, perspectives and clinical applications. Biochem Pharmacol 82:1807–1821
Afzal M, Safer AM, Menon M (2015) Green tea polyphenols and their potential role in health and disease. Inflammopharmacology 23:151–161
Yao C, Zhang J, Liu G, Chen F, Lin Y (2014) Neuroprotection by (−)-epigallocatechin-3-gallate in a rat model of stroke is mediated through inhibition of endoplasmic reticulum stress. Mol Med Rep 9:69–76
Zhang F, Li N, Jiang L, Chen L, Huang M (2015) Neuroprotective effects of (−)-epigallocatechin-3-gallate against focal cerebral ischemia/reperfusion injury in rats through attenuation of inflammation. Neurochem Res 40:1691–1698
Xie W, Ramakrishna N, Wieraszko A, Hwang YW (2008) Promotion of neuronal plasticity by (−)-epigallocatechin-3-gallate. Neurochem Res 33:776–783
van Praag H, Lucero MJ, Yeo GW, Stecker K, Heivand N, Zhao C, Yip E, Afanador M et al (2007) Plant-derived flavanol (−)epicatechin enhances angiogenesis and retention of spatial memory in mice. J Neurosci 27:5869–5878
Wang Y, Li M, Xu X, Song M, Tao H, Bai Y (2012) Green tea epigallocatechin-3-gallate (EGCG) promotes neural progenitor cell proliferation and sonic hedgehog pathway activation during adult hippocampal neurogenesis. Mol Nutr Food Res 56:1292–1303
Itoh T, Imano M, Nishida S, Tsubaki M, Mizuguchi N, Hashimoto S, Ito A, Satou T (2012) (−)-Epigallocatechin-3-gallate increases the number of neural stem cells around the damaged area after rat traumatic brain injury. J Neural Transm (Vienna) 119:877–890
Zhang J, Mao X, Zhou T, Cheng X, Lin Y (2014) IL-17A contributes to brain ischemia reperfusion injury through calpain-TRPC6 pathway in mice. Neuroscience 274:419–428
Zhang J, Wu Y, Weng Z, Zhou T, Feng T, Lin Y (2014) Glycyrrhizin protects brain against ischemia-reperfusion injury in mice through HMGB1-TLR4-IL-17A signaling pathway. Brain Res 1582:176–186
Sun F, Wang X, Mao X, Xie L, Jin K (2012) Ablation of neurogenesis attenuates recovery of motor function after focal cerebral ischemia in middle-aged mice. PLoS One 7:e46326
Gertz K, Kronenberg G, Kalin RE, Baldinger T, Werner C, Balkaya M, Eom GD, Hellmann-Regen J et al (2012) Essential role of interleukin-6 in post-stroke angiogenesis. Brain 135:1964–1980
Song J, Cho KJ, Cheon SY, Kim SH, Park KA, Lee WT, Lee JE (2013) Apoptosis signal-regulating kinase 1 (ASK1) is linked to neural stem cell differentiation after ischemic brain injury. Exp Mol Med 45:e69
Shin JA, Lim SM, Jeong SI, Kang JL, Park EM (2014) Noggin improves ischemic brain tissue repair and promotes alternative activation of microglia in mice. Brain Behav Immun 40:143–154
Ransohoff RM, Brown MA (2012) Innate immunity in the central nervous system. J Clin Invest 122:1164–1171
Thored P, Heldmann U, Gomes-Leal W, Gisler R, Darsalia V, Taneera J, Nygren JM, Jacobsen SE et al (2009) Long-term accumulation of microglia with proneurogenic phenotype concomitant with persistent neurogenesis in adult subventricular zone after stroke. Glia 57:835–849
Hu X, Li P, Guo Y, Wang H, Leak RK, Chen S, Gao Y, Chen J (2012) Microglia/macrophage polarization dynamics reveal novel mechanism of injury expansion after focal cerebral ischemia. Stroke 43:3063–3070
Brifault C, Gras M, Liot D, May V, Vaudry D, Wurtz O (2015) Delayed pituitary adenylate cyclase-activating polypeptide delivery after brain stroke improves functional recovery by inducing m2 microglia/macrophage polarization. Stroke 46:520–528
Xu D, Zhang F, Wang Y, Sun Y, Xu Z (2014) Microcephaly-associated protein WDR62 regulates neurogenesis through JNK1 in the developing neocortex. Cell Rep 6:104–116
Zhang D, Guo M, Zhang W, Lu XY (2011) Adiponectin stimulates proliferation of adult hippocampal neural stem/progenitor cells through activation of p38 mitogen-activated protein kinase (p38MAPK)/glycogen synthase kinase 3beta (GSK-3beta)/beta-catenin signaling cascade. J Biol Chem 286:44913–44920
Zhang C, Chopp M, Cui Y, Wang L, Zhang R, Zhang L, Lu M, Szalad A et al (2010) Cerebrolysin enhances neurogenesis in the ischemic brain and improves functional outcome after stroke. J Neurosci Res 88:3275–3281
Rosa AI, Goncalves J, Cortes L, Bernardino L, Malva JO, Agasse F (2010) The angiogenic factor angiopoietin-1 is a proneurogenic peptide on subventricular zone stem/progenitor cells. J Neurosci 30:4573–4584
Nicoleau C, Benzakour O, Agasse F, Thiriet N, Petit J, Prestoz L, Roger M, Jaber M et al (2009) Endogenous hepatocyte growth factor is a niche signal for subventricular zone neural stem cell amplification and self-renewal. Stem Cells 27:408–419
Arvidsson A, Collin T, Kirik D, Kokaia Z, Lindvall O (2002) Neuronal replacement from endogenous precursors in the adult brain after stroke. Nat Med 8:963–970
Parent JM, Vexler ZS, Gong C, Derugin N, Ferriero DM (2002) Rat forebrain neurogenesis and striatal neuron replacement after focal stroke. Ann Neurol 52:802–813
Thored P, Arvidsson A, Cacci E, Ahlenius H, Kallur T, Darsalia V, Ekdahl CT, Kokaia Z et al (2006) Persistent production of neurons from adult brain stem cells during recovery after stroke. Stem Cells 24:739–747
Chen J, Zhang ZG, Li Y, Wang Y, Wang L, Jiang H, Zhang C, Lu M et al (2003) Statins induce angiogenesis, neurogenesis, and synaptogenesis after stroke. Ann Neurol 53:743–751
Shioda N, Han F, Morioka M, Fukunaga K (2008) Bis(1-oxy-2-pyridinethiolato)oxovanadium(IV) enhances neurogenesis via phosphatidylinositol 3-kinase/Akt and extracellular signal regulated kinase activation in the hippocampal subgranular zone after mouse focal cerebral ischemia. Neuroscience 155:876–887
Fan W, Dai Y, Xu H, Zhu X, Cai P, Wang L, Sun C, Hu C et al (2014) Caspase-3 modulates regenerative response after stroke. Stem Cells 32:473–486
Gregorian C, Nakashima J, Le Belle J, Ohab J, Kim R, Liu A, Smith KB, Groszer M et al (2009) Pten deletion in adult neural stem/progenitor cells enhances constitutive neurogenesis. J Neurosci 29:1874–1886
Authors’ Contributions
SYY, YL, and JCZ contributed in the experimental design. JCZ, HX, and YY contributed in the stroke model, functional assays, and Western blotting. JCZ, YY, JYC, and YJZ helped in the immunocytochemistry and functional assays. JCZ helped in the neurosphere cultures. JCZ contributed in the imaging tools. SYY, YL, and JCZ contributed in the data analysis. JCZ wrote the article
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Sources of Funding
This work was supported by the Huazhong University of Science and Technology Innovation fund (0118530238) and the National Natural Science Foundation of China (Grant Nos. 81571138, 81571286).
Disclosures
None.
Additional information
Jian-Cheng Zhang and Hang Xu are joint first authors.
Yun Lin and Shiying Yuan are joint last authors.
Rights and permissions
About this article
Cite this article
Zhang, JC., Xu, H., Yuan, Y. et al. Delayed Treatment with Green Tea Polyphenol EGCG Promotes Neurogenesis After Ischemic Stroke in Adult Mice. Mol Neurobiol 54, 3652–3664 (2017). https://doi.org/10.1007/s12035-016-9924-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-9924-0