Abstract
Vascular dementia (VaD) is caused by the reduction of blood supply by vessel occlusion and is characterized by progressive cognitive decline. VaD incidence has been growing due to the aging population, placing greater strain on social and economic resources. However, the pathological mechanisms underlying VaD remain unclear. Many studies have used the bilateral common carotid artery occlusion (BCCAO) animal model to investigate potential therapeutics for VaD. In this study, we investigated whether bee venom (BV) improves cognitive function and reduces neuroinflammation in the hippocampus of BCCAO animals. Animals were randomly divided into three groups: a sham group (n = 15), BCCAO control group (n = 15), and BV-treated BCCAO group (n = 15). BCCAO animals were treated with 0.1 μg/g BV at ST36 (“Joksamli” acupoint) four times every other day. In order to investigate the effect of BV treatment on cognitive function, we performed a Y-maze test. In order to uncover any potential relationship between these results and neuroinflammation, we also performed Western blotting in the BCCAO group. Animals that had been treated with BV showed an improved cognitive function and a reduced expression of neuroinflammatory proteins in the hippocampus, including Iba-1, TLR4, CD14, and TNF-α. Furthermore, we demonstrated that BV treatment increased pERK and BDNF in the hippocampus. The present study thus underlines the neuroprotective effect of BV treatment against BCCAO-induced cognitive impairment and neuroinflammation. Our findings suggest that BV may be an effective complementary treatment for VaD, as it may improve cognitive function and attenuate neuroinflammation associated with dementia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vascular dementia (VaD) is caused by ischemia and/or vascular brain lesions and is characterized by progressive cognitive decline [1]. It is the second most common form of dementia after Alzheimer’s disease (AD), accounting for 20 % of all dementia cases worldwide [2]. In addition, VaD is thought to occur in 20 to 55 % of AD cases [3]. The incidence VaD has been increasing due to an aging population, and the estimated economic and societal costs for VaD treatment and care are large. However, the pathological mechanisms of VaD remain unclear, and an optimal treatment strategy therefore remains to be established.
Many studies have used the bilateral common carotid artery occlusion (BCCAO) animal model to investigate potential therapeutics for VaD. In this model, the reduction of blood flow in the cerebral cortex induces a neuroinflammatory response that is similar to that seen in VaD [4]. Neuroinflammation is an inflammation of the nervous tissue as response to injury within the central nervous system (CNS) and is associated with the pathogenesis of several neurodegenerative diseases, including AD, Parkinson’s disease (PD), and amyotrophic lateral sclerosis (ALS). In addition, neuroinflammation was considered as evidence for an inflammatory pathology in neurodegeneration, involving highly specialized brain endothelial structures composed of astrocytes and microglia. As the resident macrophages of the CNS, microglia provide the innate immune response to protect against invading pathogens, and also initiate the adaptive response through antigen presentation [5]. In the case of dementia, increasing data from non-clinical and clinical models have shown that neuroinflammation plays a key role in its pathogenesis. Activation of microglia and reactive astrocytes during neuroinflammation induces the generation of pro-inflammatory cytokines and other inflammatory mediators in dementia progression [6]. In addition, neuroinflammation has been reported to induce spatial learning and synaptic dysfunction [7, 8].
In some oriental countries, bee venom (BV) has been used for anti-inflammatory therapy such as arthritis and rheumatism [9, 10]. BV contains various active complex compound, including peptides (e.g., melittin, apamin, adolapin, and mast cell degranulating peptide), enzymes (e.g., phospholipase A2, hyaluronidase, and glucosidase), and biogenic amines (e.g., histamines, dopamine, and norepinephrine) [10]. Several research papers have demonstrated the anti-inflammatory effect of BV in several disease models such as mouse models of PD and ALS and the rat model of cholecystokinin octapeptide-induced acute pancreatitis [11–13].
Recently, Gue et al. have demonstrated that BV can attenuate neuroinflammation caused by lipopolysaccharide (LPS) administration, which prevented memory loss via the NF-kB protein [14]. Ye et al. have shown that BV phospholipase A2 treatment enhanced cognitive function and reduced neuroinflammation via microglial activation in the 3xTg-AD mouse model of AD [15]. Based on previous findings, we hypothesized that BV could be helpful for improvement of cognitive function of VaD. Therefore, we investigated whether BV improves cognitive function by the reduction of neuroinflammation in BCCAO model as an experimental animal model of VaD. We determined the effect of BV treatment on cognitive function (performance of the Y-maze test) and neuroinflammation-related signaling (using immunoblotting) in a BCCAO model.
Methods
Animals
Mongolian gerbils (7 weeks old) were purchased from the Central Lab. Animal Inc., which supplies animals from Japan SLC, Inc. (Seoul, Korea) and take care 1 week for using in animal center of Korea Institute of Oriental Medicine. Mongolian gerbils had an ad libitum access to food and water, and were maintained under a constant temperature (21 ± 2 °C) and humidity (50 ± 10 %) under a 12-h light/dark cycle (light on 07:00–19:00 h). Gerbils were randomly assigned into three groups: the sham group (n = 15), BCCAO control group (n = 15), and BV-treated BCCAO group (n = 15). All animals were handled in accordance with the animal care guidelines of the Korea Institute of Oriental Medicine and the NIH.
Surgical Procedure and BV Treatment
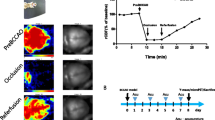
Animals were anesthetized with 2 % isoflurane in a mixture of nitrous oxide and oxygen (70:30) and subjected to BCCAO. BCCAO was induced by occluding both common carotid arteries with aneurysm clips for 5 min. Body temperature was maintained at 37 ± 0.5 °C with a heating pad during surgery (Biomed S.L., Alicante, Spain). Cerebral circulation was restored by removing the clips. Sham-operated controls underwent the same surgical operation but without clipping of the carotid arteries. Regional cerebral blood flow (rCBF) was monitored using laser Doppler flowmetry (PeriScan PIM 3 system, Perimed, Järfälla, Sweden). Gerbils that showed over an 80 % reduction of rCBF were used for further study. After reperfusion, the animals were placed in a warm incubator (32–33 °C).
BV was purchased from Sigma (St. Louis, MO, USA). According to human acupoint landmarks and a mouse anatomical reference guide [15], the ST36 acupoint (Joksamli) is located 5 mm below and lateral to the anterior tubercle of the tibia. BV (0.1 μg/g) was bilaterally injected (subcutaneously) at ST36 four times every other day after surgery. Sham animals were bilaterally injected (subcutaneously) with an equal volume of saline at the ST36 acupoint.
Y-Maze Task
After the last administration of BV or saline was completed, the behavioral test was administered. The Y-maze was a horizontal maze (40 cm long and 3 cm wide with walls 12 cm high) with three arms (labeled A, B and C) at 120° angles (Sarter et al., 1988). The maze floor and walls were constructed from dark opaque polyvinyl plastic. The gerbil was initially placed within one arm, and the sequence (e.g., ABCCAB) and the number of arm entries were recorded manually for each gerbil over an 8-min period, as has been described elsewhere (Kim et al., 2006). A spontaneous alternation was defined as consecutive entries into all three arms (i.e., ABC, CAB, or BCA, but not BAB). The maze arms were thoroughly cleaned with water spray between tests to remove residual odors. The percentage of alternation was calculated using the following equation: % Alternation = [(number of alternations)/(total arm entries − 2)] × 100. The total number of arm entries served as an indicator of locomotor activity.
Tissue Preparation
Animals were anesthetized with an intraperitoneal injection of pentobarbital, transcardially perfused with phosphate buffer (100 mM, pH 7.4). For Nissl and immunohistochemical staining, the brains were removed and postfixed in 4 % paraformaldehyde for 3 days at 4 °C prior to embedding. The paraffin-embedded brains were sectioned in the coronal plane at 5-μm thick and mounted on glass slides. Before staining, the sections were deparaffinized with xylene and rehydrated in a graded alcohol series, followed by PBS.
Nissl Staining
Following deparaffinization, brain sections were stained with 0.1 % Cresyl Violet Acetate (Sigma, St. Louis, MO) diluted with saline. Sections were then dehydrated through a graded alcohol series (70, 80, 90, and 100 %, 2×), placed in xylene, and covered with a coverslip after the addition of histomount media.
Severity of Damage
Cells were counted in three sections per animal by a person blind to the treatment group, and the average cell count per section was calculated. The degree of damage in the hippocampal region that was evident from the Nissl staining on the 8th day after ischemia was semi-quantitatively scored from 0 to 3 (0, normal; 1, <30 % of the neurons were irreversibly damaged; 2, 30–60 % of the neurons were irreversibly damaged; 3, 60–100 % of the neurons were irreversibly damaged) [16].
Immunohistochemistry and Double Immunofluorescence
For the Iba-1 immunohistochemistry staining, slides were deparaffinized and treated with 3 % H2O2 to inactivate endogenous peroxidases, and were then incubated with anti-Iba-1 (Wako, Japan). After incubation with primary antibodies, the sections were washed with PBS and incubated with a 1:1000 dilution of secondary antibodies. For visualization, an ABC kit (Vector Laboratories, Burligame, CA, USA) and a DAB peroxidase substrate kit (Vector Laboratories, Burligame, CA, USA) were used. Immunostained brain sections were observed using a light microscope (Olympus BX51, Tokyo, Japan).
For immunofluorescence staining, sections were deparaffinized and blocked in 5 % BSA for 1 h, followed by an overnight incubation with anti-NeuN antibody (Millipore Corporation, MA, USA) in 2 % BSA diluted in 0.1 % Triton-X-100 in PBS. After several washes, the sections were incubated with fluorescein isothiocyanate (FITC)-conjugated goat anti-rabbit IgG (Alexa fluor 488 1:1000 dilution, Invitrogen, CA, USA) for 1 h at room temperature and then mounted on glass slides using a mounting medium (Vector Laboratories, Burlingame, CA, USA). Slice analysis was conducted by microscopy (Olympus BX51, Tokyo, Japan). For the quantification of NeuN-positive cells and Iba-1-positive cells (the average of three sections per animal) in the CA1 of hippocampal region, NIH Image J was used (version 1.46j).
Western Blotting
Hippocampal tissues were isolated from the brain and homogenized in RIPA buffer (50 mM Tris–HCl, pH 7.4, 1 % NP-40, 0.1 % SDS, and 150 mM NaCl) containing a protease and phosphatase inhibitor cocktail. Following homogenization, a 20 μg sample of protein was quantified via the BCA assay. The samples were denatured with sodium dodecyl sulfate sampling buffer and then separated through SDS-PAGE, followed by transfer to a PVDF membrane. For the detection of target proteins, the membranes were blocked with 5 % non-fat milk in TBS (50 mM Tris–HCl, pH 7.6, 150 mM NaCl) and subsequently incubated overnight with various primary antibodies: anti-Iba-1 (diluted 1:1000, Wako, Japan), anti-TNF-α (diluted 1:1000, Abcam, MA, USA), anti-TLR4 (diluted 1:1000, Santa Cruz Biotechnology, TX, USA), anti-CD14(diluted 1:1000, BD Pharmingen, Haryana, India), anti-iNOS (diluted 1:1000, BD bioscience, CA, USA), anti-BAX (diluted 1:1000, Santa Cruz Biotechnology, TX, USA), anti-pERK (diluted 1:1000, cell signaling, MA, USA), anti-ERK (diluted 1:1000, cell signaling, MA, USA) and anti-BDNF (diluted 1:1000, Santa Cruz Biotechnology, TX, USA). Anti-α-tubulin (diluted 1:5000, Abcam, MA, USA) was used as a loading control. The blots were next probed with peroxidase-conjugated secondary antibodies (Santa Cruz Biotechnology, TX, USA) and visualized using enhanced chemiluminescence reagents (Amersham Pharmacia, NJ, USA). Protein bands were detected with the Fusion SL4-imaging system (Fusion, Eberhardzell, Germany). Quantification of the immunoblotting bands was conducted with the NIH program Image J.
Statistical Analysis
All data were analyzed using GraphPad Prism 5.0 (GraphPad Software, CA, USA) and are presented as the mean ± SEM. The results of stainings and Western blots were analyzed using a one-way analysis of variance (ANOVA) followed by Newman-Keuls post hoc test for multiple comparisons. Statistical significance was set at p < 0.05.
Results
BV Improved BCCAO-Induced Cognitive Impairment
To investigate the effect of BV on cognitive function, we tested spontaneous alternation in the Y-maze. Spontaneous alternation in the Y-maze was significantly lower (by 1.6-fold) in BCCAO animals compared with sham animals (p < 0.05) (Fig. 1a). However, BV treatment at ST36 increased spontaneous alternation by 1.2-fold compared to that at the saline-treated BCCAO animals (Fig. 1a). The number of arms entered during the test was similar between sham, BCCAO, and BV-treated BCCAO animals, which indicates that BCCAO and BV-treated animals had normal motor function and exploratory activity (Fig. 1b).
BV treatment improved cognitive function in BCCAO animals. BCCAO animals were treated with 0.1 μg/g BV at ST36 acupoint four times every other day. To determine the effect of BV at ST36 on cognitive impairment, a Y-maze test was performed. Spontaneous alternation behavior (a) and the number of total arm entries (b) during an 8-min session were recorded. Data represent the mean ± SEM. (n = 6/group). *p < 0.05, compared with the sham-operated group. #p < 0.05, compared with the BCCAO group. BCCAO + BV; BV-treated BCCAO group
BV Treatment Inhibited Neuronal Loss and Reduced the Expression of Iba-1
Occlusion induces neuronal cell death in the CA1 region, which is known to be the most vulnerable region to common carotid artery occlusion [17, 18]. We investigated the effect of BV treatment on neuronal cell death in the CA1 region using Nissl staining and immunohistochemistry. BV treatment ameliorated the severity of damage of hippocampal CA1 cells compared to saline-treated BCCAO animals (Fig. 2a). In addition, we found that the neuronal cell death by occlusion increased by 3.1-fold compared to the sham group, and BV treatment reduced neuronal loss by 2.4-fold compared to the BCCAO control group (Fig. 2b).
BV treatment reduced neuronal cell death and microglial activation in the transient BCCAO model. In the CA1 region of BCCAO animals, BV treatment significantly reduced the density of Iba1-positive cells and increased the number of NeuN-positive neuronal cells compared to BCCAO animals without BV treatment. Representative microphotograph of cells stained positive for Nissl, NeuN, and Iba-1 in the hippocampal CA1 region (bars indicate 2 mm or 200 μm) (a). The severity of neuronal damage in the CA1 region was analyzed in b. Quantification of NeuN-positive neuronal cells and Iba-1-stained microglial cells in the CA1 region of animals (b). Data are presented as the mean ± SEM (n = 5/group). *p < 0.05, compared with the sham group. #p < 0.05, compared with the BCCAO group (one-way ANOVA followed by Student Newman-Keul’s post host test)
To find the mechanism underlying the protective effect of BV, we examined neuroinflammation by assessing the expression level of Iba-1 for microglial activation in the CA1 region. Similar to the previous data, we found an 8.3-fold increase in microglial cells (detected by Iba-1) of the CA1 region in BCCAO animals compared to the sham group. However, BV treatment significantly reduced (by 4.5 fold) the expression of Iba-1 in the CA1 region compared to saline-treated BCCAO animals (Fig. 2b).
BV Treatment Reduced the Expression of Neuroinflammation-Related TLR4 Signaling in the Hippocampus of BCCAO Animals
In order to determine the neuroprotective mechanism of BV in a BCCAO model, we examined neuroinflammatory signaling-related proteins, particularly toll-like receptor 4 (TLR4). As shown in Fig. 3a, Western blot using the Iba-1 antibody confirmed there to be a 2-fold increase in microglial cells, and BV treatment reduced by 2-fold the expression of Iba-1 in the hippocampus of BCCAO animals (Fig. 3a). Next, we examined the expression of inflammatory signaling-related proteins, such as TLR4 and tumor necrosis factor—α (TNF-α), to investigate neuroinflammation caused by microglia activation. As shown in Fig. 3a, b, TLR4 expression increased by 2.6-fold in the hippocampus of BCCAO animals compared to sham animals. However, BV treatment reduced this increase by 1.4-fold compared to BCCAO animals without BV treatment. In addition, the expression of CD14 as a co-receptor with TLR4 increased by 2.1-fold in the hippocampus of BCCAO animals, but BV treatment reduced this by 1.9-fold compared to saline-treated BCCAO animals.
BV treatment modulated the expression of neuroinflammatory-related proteins in the hippocampus of BCCAO animals. Representative immunoblotting images for Iba-1, TLR4, CD14, and α-tubulin (a) (n = 3–4/each group). Tubulin was used as a loading control. Quantification of immunoblots. Each experiment was repeated at least three times. Relative expression levels of proteins were normalized to α-tubulin. Each bar represents the group mean ± SEM (b). *p < 0.05, compared with the sham group. #p < 0.05, compared with the BCCAO group
The pro-inflammatory cytokine, TNF-α, was augmented by 6-fold in the hippocampus of BCCAO animals compared to shams. However, BV treatment dramatically decreased the expression of TNF-α in the hippocampus by 2.9-fold.
BV Treatment Increased Memory-Related Proteins by the Inhibition of Oxidative Stress and Cell Death
To determine the effect of BV on oxidative stress, we examined the expression of inducible nitric oxide synthases (iNOS) in the hippocampus of BCCAO model animals. As expected, the expression level of iNOS was significantly increased by 3.2-fold compared to sham animals. However, BV treatment resulted in a significantly reduced iNOS expression level (by 1.8-fold) compared to the saline-treated BCCAO animals (Fig. 4a, b).
BV treatment increased memory-related proteins by the inhibition of oxidative stress and apoptosis. Representative images of the levels of iNOS and BAX in the hippocampus from each group (a) (n = 3–4/each group). Quantification of immunoblots (b). Each experiment was repeated at least three times. Relative expression levels of proteins were normalized to α-tubulin. Each bar represents the group mean ± SEM in b. *p < 0.001, compared with the sham group. #p < 0.001, compared with the BCCAO group. The effects of BV treatment on pERK and BDNF expression in the hippocampus from each group (c) (n = 3–4/each group). Quantification of immunoblots (d). The quantification of phospho-ERK was determined as the ratio of pERK/ERK. Each bar represents the group mean ± SEM in b. *p < 0.001, compared with the sham group. #p < 0.05, ##p < 0.001, compared with the BCCAO group
The mitochondrial apoptotic pathway is triggered by the combined action of the anti-apoptotic factor Bcl-2 and pro-apoptotic factor Bcl-2-associated X protein (BAX), which induces the Caspase-3-dependent intrinsic apoptosis pathway [19, 20]. We therefore examined the levels of BAX in the mitochondrial apoptotic pathway. In the hippocampus of BCCAO animals, the expression level of BAX was increased by 2.9-fold compared to that of sham animals. However, BV treatment decreased the expression of BAX by 2.2-fold compared to saline-treated BCCAO animals (Fig. 4a, b).
Finally, we investigated the expression of brain-derived neurotrophic factor (BDNF) because BDNF plays a critical role to the development and synaptic plasticity of brain as well as learning and memory [21]. To determine whether the BDNF/ERK signaling pathway affects the neuroprotective BV effects, we examined the expression of BDNF and activated ERK level in the hippocampus of BCCAO animals. As shown in Fig. 4c, d, the expression of phospho-ERK in the hippocampus of BCCAO animals was decreased by 3-fold compared to that of sham animals. However, BV treatment increased the levels of phospho-ERK protein by 3.6-fold compared to saline-treated BCCAO animals. In addition, BDNF expression was reduced by 1.7-fold in the hippocampus of BCCAO compared to sham animals, but BV treatment augmented BDNF expression by 1.4-fold in the hippocampus compared to BCCAO animals without BV treatment.
Discussion
In this study, we investigated the effect of BV in an animal model of BCCAO showing mild cognitive dysfunction. We found that BV treatment improved cognitive function by the inhibition of neuroinflammation.
Although dementia, including AD and VaD, is a growing global problem in the aging population, the mechanisms behind dementia and thus an effective treatment have yet to be uncovered. In order to shed light, we investigated the relationship between neuroinflammation and cognitive impairment, and did so by testing the effect of BV on cognitive function in a BCCAO animal model. We found that BV treatment improved spatial memory compared to BCCAO animals that received saline only. In addition, BV treatment reduced the severity of damage, and Iba-1 positive microglial cells, and increased the number of neuronal cells in the hippocampal CA1 of BCCAO animals. In our previous study, we observed that BV treatment decreased microglial cells and motor neuronal cell death in the spinal cord of an animal of ALS [12]. Therefore, BV treatment could be helpful for the reduction of neuroinflammation and neuronal loss in CNS diseases.
Neuroinflammation is a regular function that plays an important role in clearing pathogens and phagocytosis of apoptotic cells and debris. However, when neuroinflammation remains uncontrolled and becomes chronic, it leads to neurotoxicity by production of neurotoxic mediators/pro-inflammatory cytokines. This exacerbates neurodegenerative pathological symptom. In the CNS, microglia play an anti-inflammatory function in the active immune defense to maintain brain maintenance. However, in neurodegenerative diseases such as VaD, PD, and ALS, activated microglia can cause neurotoxicity. Products and mediators of neuroinflammation have been shown to directly affect cognition and memory, contributing to the cognitive dysfunction associated with several acute and chronic neurological conditions [22]. In the early stages of AD, for example, neuroinflammation can cause impairments in learning and memory [23]. Ways to prevent and ameliorate neuroinflammation have therefore been a topic of much interest for many researchers. Since BV has been used for the effect of ani-neuroinflammation in several diseases including arthritis and rheumatism [9, 10], we investigated the effect of BV on the neuroinflammatory signaling pathway and simultaneously looked at the effect on cognitive functioning. We found an increase of the expression levels of Iba-1 and TLR4-related signaling pathway in the hippocampus of BCCAO animals. However, BV treatment significantly reduced the expression of TLR4, CD14, and TNF-α. Microglia participate in innate and adaptive immune responses, as well as in the remodeling of neuronal circuits in the CNS. Interactions between microglia and synapses not only play an important role in the maturation of synaptic circuits during development, but continue to be vital for the regulation of synaptic plasticity and basal neurotransmission in adulthood [24]. However, in neurodegenerative diseases, activated microglia release pro-inflammatory cytokines that can induce neurotoxicity. Given that inflammatory cytokine receptors are highly concentrated in areas associated with learning and memory, particularly in hippocampal regions [25], LPS-induced neuroinflammation in the adult brain may disrupt hippocampus-dependent learning and memory [26, 27]. Moreover, recent studies have shown that peripheral LPS administration decreases the expression of BDNF in the hippocampus, which contributes to cognitive impairment [28, 29].
Toll-like receptors (TLRs) are a family of type-I trans-membrane receptors best known as sensors of microbial-associated molecular patterns (MAMPs) by cells of the immune system [30]. TLRs induce activation of signaling cascades that result in the production of inflammatory cytokines/chemokines [31]. Activation of TLRs in the CNS has been related to impairment of various aspects of learning and memory in a neuroinflammation-dependent manner [32]. Activation of TLR4 in the TLRs has been found to participate in myelin and synaptic dysfunction, as well as long-term neuroinflammatory and cognitive behavioral impairments [33]. Therefore, the effect of BV as an anti-neuroinflammatory treatment may aid synaptic plasticity by inhibition of the TLR4 signaling in BCCAO animals.
In order to confirm the effect of BV treatment on neuroinflammation, we examined the expression level of iNOS and BAX in the hippocampus of BCCAO animals. We found that BV treatment significantly reduced iNOS and BAX protein expression in BCCAO animals, which confirms our hypothesis. Furthermore, we found that BV treatment augmented the expression of BDNF by activation of ERK. As a key neurotrophic factor, BDNF plays a critical role for supporting the survival and maintenance of neurons as well as synaptic physiology in neuronal plasticity and mediating long-term potentiation and memory consolidation [34, 35]. Hritcu and Gorgan have shown that LPS-induced cognitive deficits are associated with BDNF gene expression and hippocampal function [29]. In addition, Wei et al. found that nicotine has a neuroprotective effect against LPS-induced cognitive dysfunction and neuroinflammation via an increase in BDNF in the dorsal hippocampus [36]. Furthermore, BDNF expression levels have been correlated with the severity of AD-related cognitive impairment [37]. In our study, we demonstrated that BDNF levels were significantly decreased, and TLR4-related inflammatory signaling increased in the hippocampus of BCCAO animals. However, BV treatment significantly restored BDNF levels and reduced neuroinflammation. This result indicates that BV produces its neuroprotective effect by mediating the up-regulation of BDNF and anti-neuroinflammation in BCCAO animals. However, BV therapy should consider on sensitization because it has on the risk of anaphylaxis.
Gu et al. have shown that BV ameliorates LPS-induced beta-amyloid neuroinflammation and cognitive dysfunction via the NF-kB signaling pathway [14]. Sami et al. have demonstrated that apamin attenuates the memory loss by partial hippocampal lesions [38]. Therefore, future studies should aim to determine the bioactive compound in BV that results in the improved cognitive function in BCCAO animals. In addition, one important feature of VaD is cholinergic dysfunction. Notably, the cholinergic system, which innervates the basal forebrain and projects to the cortex and hippocampus, involves brain regions important for learning and memory [39]. Another potential research avenue could therefore be to investigate the level of choline acetyltransferase (ChAT), a biosynthetic enzyme for ACh, in the hippocampus of BV-treated BCCAO animals.
References
Versijpt J (2014) Effectiveness and cost-effectiveness of the pharmacological treatment of Alzheimer’s disease and vascular dementia. J Alzheimers Dis 42(Suppl 3):S19–S25. doi:10.3233/JAD-132639
Dubois MF, Hebert R (2001) The incidence of vascular dementia in Canada: a comparison with Europe and East Asia. Neuroepidemiology 20(3):179–187
Kammoun S, Gold G, Bouras C, Giannakopoulos P, McGee W, Herrmann F, Michel JP (2000) Immediate causes of death of demented and non-demented elderly. Acta Neurol Scand Suppl 176:96–99
Yang EJ, Cai M, Lee JH (2015) Neuroprotective effects of electroacupuncture on an animal model of bilateral common carotid artery occlusion. Mol Neurobiol. doi:10.1007/s12035-015-9610-7
Nayak D, Roth TL, McGavern DB (2014) Microglia development and function. Annu Rev Immunol 32:367–402. doi:10.1146/annurev-immunol-032713-120240
Lopez-Valdes HE, Martinez-Coria H (2016) The role of neuroinflammation in age-related dementias. Rev Investig Clin 68(1):40–48
Deng X, Li M, Ai W, He L, Lu D, Patrylo PR, Cai H, Luo X et al (2014) Lipolysaccharide-induced neuroinflammation is associated with Alzheimer-like amyloidogenic axonal pathology and dendritic degeneration in rats. Adv Alzheimer Dis 3(2):78–93. doi:10.4236/aad.2014.32009
Lee YJ, Choi DY, Yun YP, Han SB, KW O, Hong JT (2013) Epigallocatechin-3-gallate prevents systemic inflammation-induced memory deficiency and amyloidogenesis via its anti-neuroinflammatory properties. J Nutr Biochem 24(1):298–310. doi:10.1016/j.jnutbio.2012.06.011
Suh SJ, Kim KS, Kim MJ, Chang YC, Lee SD, Kim MS, Kwon DY, Kim CH (2006) Effects of bee venom on protease activities and free radical damages in synovial fluid from type II collagen-induced rheumatoid arthritis rats. Toxicol in Vitro 20(8):1465–1471. doi:10.1016/j.tiv.2006.06.016
Son DJ, Lee JW, Lee YH, Song HS, Lee CK, Hong JT (2007) Therapeutic application of anti-arthritis, pain-releasing, and anti-cancer effects of bee venom and its constituent compounds. Pharmacol Ther 115(2):246–270. doi:10.1016/j.pharmthera.2007.04.004
Chung ES, Kim H, Lee G, Park S, Kim H, Bae H (2012) Neuro-protective effects of bee venom by suppression of neuroinflammatory responses in a mouse model of Parkinson’s disease: role of regulatory T cells. Brain Behav Immun 26(8):1322–1330. doi:10.1016/j.bbi.2012.08.013
Yang EJ, Jiang JH, Lee SM, Yang SC, Hwang HS, Lee MS, Choi SM (2010) Bee venom attenuates neuroinflammatory events and extends survival in amyotrophic lateral sclerosis models. J Neuroinflammation 7. doi:10.1186/1742-2094-7-69
Seo SW, Jung WS, Lee SE, Choi CM, Shin BC, Kim EK, Kwon KB, Hong SH et al (2008) Effects of bee venom on cholecystokinin octapeptide-induced acute pancreatitis in rats. Pancreas 36(2):e22–e29. doi:10.1097/MPA.0b013e31815a396b
Gu SM, Park MH, Hwang CJ, Song HS, Lee US, Han SB, Oh KW, Ham YW et al (2015) Bee venom ameliorates lipopolysaccharide-induced memory loss by preventing NF-kappaB pathway. J Neuroinflammation 12. doi:10.1186/s12974-015-0344-2
Ye M, Chung HS, Lee C, Yoon MS, Yu AR, Kim JS, Hwang DS, Shim I et al (2016) Neuroprotective effects of bee venom phospholipase A2 in the 3xTg AD mouse model of Alzheimer’s disease. J Neuroinflammation 13(10). doi:10.1186/s12974-016-0476-z
Cho KO, Kim SK, Cho YJ, Sung KW, Kim SY (2007) Regional differences in the neuroprotective effect of minocycline in a mouse model of global forebrain ischemia. Life Sci 80(22):2030–2035. doi:10.1016/j.lfs.2007.03.005
Murakami K, Kondo T, Kawase M, Chan PH (1998) The development of a new mouse model of global ischemia: focus on the relationships between ischemia duration, anesthesia, cerebral vasculature, and neuronal injury following global ischemia in mice. Brain Res 780(2):304–310
Kelly S, McCulloch J, Horsburgh K (2001) Minimal ischaemic neuronal damage and HSP70 expression in MF1 strain mice following bilateral common carotid artery occlusion. Brain Res 914(1–2):185–195
Roy S, Nicholson DW (2000) Cross-talk in cell death signaling. J Exp Med 192(8):F21–F25
Bratton SB, Cohen GM (2001) Caspase cascades in chemically-induced apoptosis. Adv Exp Med Biol 500:407–420
Jain V, Baitharu I, Prasad D, Ilavazhagan G (2013) Enriched environment prevents hypobaric hypoxia induced memory impairment and neurodegeneration: role of BDNF/PI3K/GSK3beta pathway coupled with CREB activation. PLoS One 8(5):e62235. doi:10.1371/journal.pone.0062235
Lyman M, Lloyd DG, Ji X, Vizcaychipi MP, Ma D (2014) Neuroinflammation: the role and consequences. Neurosci Res 79:1–12. doi:10.1016/j.neures.2013.10.004
Pimplikar SW (2014) Neuroinflammation in Alzheimer’s disease: from pathogenesis to a therapeutic target. J Clin Immunol 34(Suppl 1):S64–S69. doi:10.1007/s10875-014-0032-5
Schafer DP, Lehrman EK, Stevens B (2013) The “quad-partite” synapse: microglia-synapse interactions in the developing and mature CNS. Glia 61(1):24–36. doi:10.1002/glia.22389
Shaw KN, Commins S, O’Mara SM (2001) Lipopolysaccharide causes deficits in spatial learning in the watermaze but not in BDNF expression in the rat dentate gyrus. Behav Brain Res 124(1):47–54
Sparkman NL, Buchanan JB, Heyen JR, Chen J, Beverly JL, Johnson RW (2006) Interleukin-6 facilitates lipopolysaccharide-induced disruption in working memory and expression of other proinflammatory cytokines in hippocampal neuronal cell layers. J Neurosci 26(42):10709–10716. doi:10.1523/JNEUROSCI.3376-06.2006
Russo I, Barlati S, Bosetti F (2011) Effects of neuroinflammation on the regenerative capacity of brain stem cells. J Neurochem 116(6):947–956. doi:10.1111/j.1471-4159.2010.07168.x
Schnydrig S, Korner L, Landweer S, Ernst B, Walker G, Otten U, Kunz D (2007) Peripheral lipopolysaccharide administration transiently affects expression of brain-derived neurotrophic factor, corticotropin and proopiomelanocortin in mouse brain. Neurosci Lett 429(1):69–73. doi:10.1016/j.neulet.2007.09.067
Hritcu L, Gorgan LD (2014) Intranigral lipopolysaccharide induced anxiety and depression by altered BDNF mRNA expression in rat hippocampus. Prog Neuro-Psychopharmacol Biol Psychiatry 51:126–132. doi:10.1016/j.pnpbp.2014.01.016
Kawai T, Akira S (2007) Signaling to NF-kappaB by toll-like receptors. Trends Mol Med 13(11):460–469. doi:10.1016/j.molmed.2007.09.002
Takeda K, Akira S (2004) TLR signaling pathways. Semin Immunol 16(1):3–9
Okun E, Griffioen KJ, Mattson MP (2011) Toll-like receptor signaling in neural plasticity and disease. Trends Neurosci 34(5):269–281. doi:10.1016/j.tins.2011.02.005
Montesinos J, Pascual M, Pla A, Maldonado C, Rodriguez-Arias M, Minarro J, Guerri C (2015) TLR4 elimination prevents synaptic and myelin alterations and long-term cognitive dysfunctions in adolescent mice with intermittent ethanol treatment. Brain Behav Immun 45:233–244. doi:10.1016/j.bbi.2014.11.015
Andresen JH, Loberg EM, Wright M, Goverud IL, Stray-Pedersen B, Saugstad OD (2009) Nicotine affects the expression of brain-derived neurotrophic factor mRNA and protein in the hippocampus of hypoxic newborn piglets. J Perinat Med 37(5):553–560. doi:10.1515/JPM.2009.081
Numakawa T, Adachi N, Richards M, Chiba S, Kunugi H (2013) Brain-derived neurotrophic factor and glucocorticoids: reciprocal influence on the central nervous system. Neuroscience 239:157–172. doi:10.1016/j.neuroscience.2012.09.073
Wei P, Liu Q, Li D, Zheng Q, Zhou J, Li J (2015) Acute nicotine treatment attenuates lipopolysaccharide-induced cognitive dysfunction by increasing BDNF expression and inhibiting neuroinflammation in the rat hippocampus. Neurosci Lett 604:161–166. doi:10.1016/j.neulet.2015.08.008
Diogenes MJ, Costenla AR, Lopes LV, Jeronimo-Santos A, Sousa VC, Fontinha BM, Ribeiro JA, Sebastiao AM (2011) Enhancement of LTP in aged rats is dependent on endogenous BDNF. Neuropsychopharmacology 36(9):1823–1836. doi:10.1038/npp.2011.64
Ikonen S, Riekkinen P Jr (1999) Effects of apamin on memory processing of hippocampal-lesioned mice. Eur J Pharmacol 382(3):151–156
Schliebs R, Arendt T (2011) The cholinergic system in aging and neuronal degeneration. Behav Brain Res 221(2):555–563. doi:10.1016/j.bbr.2010.11.058
Acknowledgment
This work is supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT & Future Planning (No. NRF-2015R1C1A2A01053248) and the Korea Institution of Oriental Medicine (KIOM) (No. K16051).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cai, M., Lee, J.H. & Yang, E.J. Bee Venom Ameliorates Cognitive Dysfunction Caused by Neuroinflammation in an Animal Model of Vascular Dementia. Mol Neurobiol 54, 5952–5960 (2017). https://doi.org/10.1007/s12035-016-0130-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-0130-x