Abstract
Vascular dementia (VD) is a degenerative cerebrovascular disorder associated with progressive cognitive decline. Previous reports have shown that 7,8-dihydroxyflavone (7,8-DHF), a well-known TrkB agonist, effectively ameliorates cognitive deficits in several disease models. Therefore, this study investigated the protective effects of 7,8-DHF against 2-VO-induced VD. VD was established in rats using the permanent bilateral carotid arteries occlusion (two-vessel occlusion, 2-VO) model. 7,8-DHF (5, 10, and 20 mg/kg) and Donepezil (10 mg/kg) were administered for 4 weeks. Memory function was assessed by the novel objective recognition task (NOR) and Morris water maze (MWM) tests. Inflammatory (TNF-α, IL-1β, and NF-kβ), oxidative stress, and apoptotic (BAX, BCL-2, caspase-3) markers, along with the activity of choline acetylcholinesterase (AChE) was assessed. p-AKT, p-CREB, BDNF, and neurotransmitter (NT) (GLU, GABA, and ACh) levels were also analyzed in the hippocampus of 2-VO rats. Our results show that 7,8-DHF effectively improved memory performance and cholinergic dysfunction in 2-VO model rats. Furthermore, 7,8-DHF treatment also increased p-AKT, p-CREB, and BDNF levels, suppressed oxidative, inflammatory, and apoptotic markers, and restored altered NT levels in the hippocampus. These findings imply that 7, 8-DHF may act via multiple mechanisms and as such serve as a promising neuroprotective agent in the context of VD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Vascular dementia (VD) is a progressive neurodegenerative disease that is known to account for 20% of all cases of dementia [1]. In older adults, it is the second most prevalent type of dementia after AD [2]. VD is known to be associated with impairment of executive functions such as working memory, planning, thinking, reasoning, problem-solving, judgment, and the execution of tasks [3]. Advanced age, smoking, hypertension, diabetes, generalized atherosclerosis, and atrial fibrillation are important risk factors for VD [4]. Chronic cerebral hypoperfusion (CCH) represents an important cause of VD. Neuronal energy failure secondary to reduced blood flow may promote the production of reactive oxygen species, initiating neuronal apoptosis and ultimately leading to functional deficits associated with VD [5]. Presently, cholinergic agents, including acetylcholinesterase (AChE) inhibitors, calcium channel blockers, N-methyl-d-aspartate receptor antagonists, anti-thrombotics, statins, nootropics, thyrotropin-releasing hormone analogues, vasoactive agents, serotonin and histamine receptor antagonists, ginkgo biloba extracts, hyperbaric oxygen, and antioxidants have been purported to be useful in the treatment of VD [6, 7]. However, most of these therapeutic agents have largely yielded negative results thereby highlighting the need for developing new effective treatment strategies for tackling VD.
Brain-derived neurotrophic factor (BDNF) is one of the most widely studied growth factors known to promote neuronal survival and differentiation [8]. BDNF regulates synaptic transmission and hippocampal neuroplasticity which is crucial for cognitive function [9]. It is known to promote neuronal survival and prevent apoptosis by activating various signalling pathways such as phospholipase C-γ, PI3K, and MAPK through its receptor tropomyosin-related kinase B (TrkB). Furthermore, previous studies have reported CCH inhibits BDNF signalling whereas its enhancement may prevent CCH-induced hippocampus neuronal damage and cognitive impairment [10, 11]. In clinical trials, recombinant BDNF has yielded disappointing results [12]. As a result, various small-molecule ligands that can stimulate the TrkB receptor are being pursued as alternative agents for treating neurological diseases [13].
7,8-Dihydroxyflavone (7,8-DHF), a flavone derivative, is a potent and selective TrkB agonist known to penetrate the brain-blood barrier [14]. 7,8-DHF is known to mimic the physiological actions of BDNF by binding to the extracellular domain of the TrkB receptor [15]. As a result, 7,8-DHF has demonstrated its therapeutic efficacy in several animal disease models linked to deficient BDNF signalling [13]. It has shown anti-apoptotic, anti-oxidant, anti-inflammatory, anti-depressant, and neuroprotective activity along with efficacy in neurodegenerative diseases, traumatic brain injury, and glutamate-induced neurotoxicity [16]. Moreover, treatment with 7,8-DHF has also been proven to reverse cognitive deficits in various disease models via multiple mechanisms [17,18,19]. Regarding the rationale of using donepezil as a positive control in this study, it has been extensively reported that cholinergic deficits are known to exist in VD patients, and as such acetylcholinesterase (AChE) inhibitors may be beneficial in the treatment of this disorder. In earlier studies, donepezil has been shown to protect against neuronal cell death, attenuate cognitive deficits following traumatic brain injury, and enhance adult hippocampal neurogenesis [20]. To date, no study has reported the role of 7,8-DHF in VD. Therefore, the present study was undertaken to investigate the therapeutic effects of 7,8-DHF on learning and memory function in a rat model of VD.
Materials and Methods
Animals
Male Sprague-Dawley rats (200–250 gm) bred at the central animal house, Panjab University, Chandigarh were used. Animals were kept under standard laboratory conditions (25 ± 2 °C, 60–70% humidity, and 12-h light and dark cycle). Standard rodent food pellets and water were available ad libitum throughout the study. All experiments were performed in agreement with the guidelines of the committee for the purpose of control and supervision of experiments on animals (CPCSEA). The experimental protocols were approved by the Institutional Animal Ethical Committee (PU/45/99/CPCSEA/IAEC/2018/78).
Drugs and Reagents
7,8-DHF and donepezil (DNPZ) were purchased from TCI Chemicals, India. NF-kβ, BAX, BCL-2 (Elabscience, Wuhan, China), TNF-α, IL-1β (PeproTech, Rocky Hill, NJ, USA), p-AKT, p-CREB (Bioassay Technology Laboratory, China) and BDNF (Merck Millipore, Billerica, MA, USA) levels were measured using ELISA kits. Furthermore, Caspase-3 activity was estimated using a commercially available colorimetric assay kit (BioVision, Inc., Milpitas, CA, USA).
Surgical Procedure and Drug Treatment
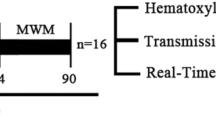
In the present study, CCH was induced by the permanent, bilateral occlusion of the common carotid arteries (2-VO) method. Briefly, rats were anesthetized with ketamine (80 mg/kg) and xylazine (5 mg/kg). Thereafter, a midline cervical incision was made and the bilateral carotid arteries were carefully separated from the vagus nerve and carotid sheath. Thereafter, each carotid artery was ligated with a 5–0 silk suture. In sham-operated rats, an identical surgical procedure was carried out, but without carotid artery ligation. A heating lamp was used during the surgery to prevent hypothermia [21]. After surgery, all rats were randomly divided into seven different groups (n = 8–10) as follows: a sham group, a sham + 7,8-DHF (20 mg/kg) group, a 2-VO or group, a DNPZ (10 mg/kg) group and 7,8-DHF (5,10 and 20 mg/kg) groups. 7,8-DHF (5,10 and 20 mg/kg) was prepared in phosphate-buffered saline (PBS) containing 17% DMSO and administered through the intraperitoneal (i.p.) route. DNPZ (10 mg/kg) was dissolved in 0.5% CMC-Na and administered orally. Both drugs were daily administered for 4 weeks (Fig. 1). Doses for DNPZ and 7,8-DHF were selected based on earlier studies [22, 23].
Schematic representation of the experimental design ACM Actophotometer, MWM Morris water maze, NOR novel object recognition test, LPO Lipid peroxidation, PCO protein carbonylation, AChE acetylcholinesterase, GSH Reduced Glutathione, SOD Superoxide dismutase, CAT catalase, GPx glutathione peroxidase, TNF-α Tumor necrosis factor alpha, IL-1β interleukin 1β, NF-kβ Nuclear Factor kappa-light-chain-enhancer of activated B cells, p-AKT phosphorylated AKT, p-CREB phosphorylated cAMP-responsive element binding protein, BDNF brain-derived neurotrophic factor, Bcl-2 B-cell lymphoma 2, Bax BCL-2 associated X protein GLU glutamate, Ach acetylcholine, GABA Gamma-aminobutyric acid
Behavioural Assessments
Closed Field Activity
Closed field activity was performed on day 29. The apparatus consisted of a squared closed arena (30 × 24 × 22 cm3) which was equipped with 16 infrared light-sensitive photocells that were present in two rows. During the habituation phase, each animal was kept for at least 2–3 min in the chamber. Thereafter, locomotor activity was measured for 5-min during which rearing and ambulatory scores of each rat were recorded [22].
Morris Water Maze Test
The MWM test was performed from day 32 to 36 [24]. The test was conducted in a black circular tank (diameter,180 cm; depth, 60 cm) that was filled to a depth of 40 cm with water (28.5 ± 2 °C). At the center of one of the quadrants, a hidden platform (diameter, 12.5; height 38 cm) was placed 2 cm below the surface of the water. Several prominent cues whose position remained unchanged throughout the experiment were placed external to the pool. The rats were given training for 5 consecutive days. The time taken for the rat to reach the platform (latency period) was noted during each training trial. Rats that failed to find the platform within 90 s cut-off period time were guided to the platform and were allowed to sit on the platform for 20 s. A probe trial was conducted after the training period during which no platform was present. The escape latency, swimming speed, frequency of entries into the target quadrant (FATQ), and time spent in the target quadrant (TSTQ) were recorded using the Ethovision-XT tracking system (Noldus Information Technology, Wageningen, The Netherlands).
Novel Object Recognition (NOR) Test
The NOR test was performed as described previously [21]. Briefly, on day one, during the habituation phase animals were familiarized for some time of 5 min by placing them in a circular open field arena (50 cm in diameter and height 40 cm) without any objects. During the training phase, two identical objects were placed in the arena and rats were allowed to investigate them for 5 min. Twenty-four hours after the training phase, one familiar object was substituted by a novel object, and the exploration time was recorded. The discrimination index was calculated using the formula: (TN–TF)/(TN+TF) where TF: Time spent exploring the familiar object; TN: Time spent exploring the novel object.
Tissue Sampling
After the behavioral tests, animals were anesthetized with diethyl ether and sacrificed by cervical dislocation. The brains of the rats were taken out carefully and divided into two equal halves. One half was used for assessing oxidative stress markers, AChE, ChAT, Ach, and ELISA assays, and the other half was used for BDNF measurement. The hippocampus was dissected quickly and homogenized in 10% (w/v) of 0.1 M of PBS. Homogenates obtained were centrifuged at 10,000×g for 20 min at 4 °C. For the BDNF assay, hippocampus tissues were homogenized in an ice-cold buffer (100 mM Tris/HCl containing 1 M NaCl, 0.1% sodium azide, 2% bovine serum albumin (BSA), 2% Triton X-100, 4 mM EDTA, and protease inhibitors).
Estimation of Lipid Peroxidation (LPO)
The extent of lipid peroxidation in the hippocampus was measured quantitatively in the form of thiobarbituric acid-reactive substances by the method described by Wills [25]. Briefly, a reaction mixture involving Tris-HCL and supernatant (0.5 ml) was incubated for 2 h at 37 °C. Thereafter, 1 ml of 10% TCA (10% w/v) was added to the incubated mixture and this was followed by centrifugation for 10 min at 1000×g. To the supernatant obtained 1 ml of thiobarbituric acid (0.67% w/v) was added and this mixture was kept in boiling water for 10 min. On cooling, distilled water (1 ml) was added to the samples. Absorbance was measured at 532 nm and results were expressed as a nanomole of malondialdehyde per milligram protein.
Estimation of Protein Carbonyl (PCO) Levels
Protein carbonyl levels were measured by incubating 20 mM of 2, 4-dinitrophenylhydrazine (DNPH) solution and 100 µl of homogenate for 1 h. Thereafter, 120 µl of 20% (w/v) TCA was added and centrifuged at 10,000×g for 10 min after keeping it on ice for 10 min. An ethyl acetate-ethanol–mixture (1:1) was used to wash the pellets obtained which were subsequently dissolved in 6 M guanidine–HCl solution (1 ml). Absorbance was determined spectrophotometrically at 370 nm and the protein carbonyl content was expressed as nmol/mg protein [26].
Estimation of Reduced Glutathione Levels (GSH)
For estimating reduced glutathione levels,1 ml of sulphosalicylic acid(4%w/v) was added to tissue homogenate which was kept at 4 °C for 1 h and centrifuged for 15 min at 1200×g. Thereafter, 0.2 ml of 0.01 M DTNB and 2.7 ml of phosphate buffer (0.1 M, pH 8) were added to the supernatant (0.1 ml), and absorbance was measured at 412 nm. GSH levels were expressed as µM per mg protein [27].
Estimation of Superoxide Dismutase Activity
SOD activity was determined by adding homogenate (0.05 ml) to an assay mixture consisting of 50 mM sodium carbonate, 0.05 ml hydroxylamine hydrochloride (pH 6.0), 0.1 mM ethylenediaminetetraacetic acid (EDTA), and 96 mM of nitro blue tetrazolium (NBT). Thereafter, a change in absorbance was observed at 560 nm for 2 min at 30/60s intervals and SOD activity was expressed as units per milligram protein [28].
Estimation of Catalase Activity
The activity of catalase was determined according to a previously described method [22]. Briefly, to an assay mixture consisting of 1.0 ml hydrogen peroxide (0.019 M) and 1.95 ml phosphate buffer (0.05 M, pH 7.0), 0.05 ml homogenate was added. The change in absorbance was measured at 240 nm. Catalase activity was expressed as µM of H2O2 decomposed per minute per milligram protein.
Estimation of Glutathione Peroxidase (GSH-Px) Activity
GSH-Px was estimated by a previously described method [29]. Briefly, to the sample (0.1 ml), 10 µl of 0.25 mM hydrogen peroxide, 100 µl of 1 mM sodium azide, 1.44 ml of 50 mM potassium phosphate buffer (pH 7.0), 100 µl of 0.2 mM NADPH, 50 mm potassium phosphate buffer, 100 µl of 1 mM EDTA, and 50 µl of glutathione reductase was added. Absorbance was measured spectrophotometrically at 340 nm at 37 °C for 2 min at each 60 sand GSH-Px activity was expressed as nmol/min/mg protein.
Estimation of Acetylcholinesterase (AChE) Activity
A reaction mixture consisting of 50 µl of tissue homogenate, 3 ml of 0.01 M sodium phosphate buffer (pH 8.0), 100 µl of acetylthiocholine iodide, and 100 µl 5,5, dithiobis-(2-nitro benzoic acid) was taken. AChE activity was measured using molar extinction co-efficient 1.36 × 104 M−1 cm−1 at 412 nm and measured as nmol of acetylthiocholine iodide hydrolysed/min/mg protein [30].
Neurotransmitter Analysis
Glutamate (Glu), acetylcholine (ACh), and γ-aminobutyric acid (GABA), levels were measured in the hippocampus of 2-VO rats. For Glu estimation, the hippocampus was homogenized in perchloric acid and centrifuged for 10 min at 3000×g. An assay system consisting of 10 µl of 33.5 m M ADP, 20 µl of 27 mM NAD, and 200 µl of glycine-hydrazine buffer was taken to which 100 µl of tissue homogenate was added. Extinction E1 was read at 340 nm. Thereafter, 5 µl of glutamate dehydrogenase (GlDH) was added and extinction E2 was measured. The difference between E1 and E2 was calculated for sample and blank and ∆Esam-Eblk = ∆Eglu was subsequently used for the calculations. Glu content in the hippocampus was expressed as µmol/g [31]. Regarding the ACh assay, a reaction mixture consisting of 0.2 ml of supernatant, 0.25 ml of 2 M calabarine sulfate, 0.2 ml of 1.85 M TCA, and 0.375 ml of pure water was incubated at room temperature and subsequently centrifuged for 10 min at 2000×g. The supernatant obtained was mixed with 2 M hydroxylamine for 10 min. An equal amount (0.125 ml) of 0.37 M ferric chloride and 4 M HCl was added to stop the reaction. Absorbance was measured at 540 nm and ACh was expressed as µM per mg protein. GABA levels were measured as previously described [32]. Briefly, hippocampus tissues were homogenized in 0.01 M HCl. Thereafter, 0.2 ml of 0.14 M ninhydrin solution prepared in 0.5 M carbonate bicarbonate buffer was added to 0.1 ml of tissue homogenate. The solution was heated (60 °C) for 30 min and cooled. Thereafter, 5 ml of copper tartrate reagent (0.0329% tartaric acid, 0.16% sodium carbonate, 0.03% copper sulfate) was added. After 10 min fluorescence emission was noted at 377/455 nm.
Enzyme-Linked Immunosorbent Assay (ELISA)
TNF-α and IL-1β Estimations
The levels of TNF-α and IL-1β were measured according to the manufacturer’s instructions. Briefly, 100 µl of Capture Antibody (anti-TNF-α and anti-IL-1β) was used to coat the ELISA plates overnight. Thereafter, plates were repeatedly washed and tissue homogenate (100 µl) was added and incubated for 2 h. To each well Avidin-HRP Conjugate (100 µl) was added after washing followed by incubation for 30 min at room temperature. The washing step was subsequently repeated and 100 µl of Avidin-horseradish peroxidase conjugate was added. Finally, after washing each well ABTS Liquid Substrate was added and the color development was measured at 405 nm.
p-AKT (S473) and p-CREB (S133) Estimations
Briefly, hippocampus homogenate (100 µl) was added to pre-coated antibody-specific wells for p-AKT (S473) and p-CREB (S133) for 60 min at 37 °C. The plate was washed subsequently. Thereafter, 50 µl of substrate solutions were added and incubated for 10 min at 37 °Cin the dark. Finally, to each well 50 µl of stop solution was added and the plate was read using a microplate reader set to 450 nm.
BDNF Estimation
The hippocampus tissues were homogenized in an ice-cold buffer (1 M NaCl, 100 mM Tris/HCl (pH 7), 2% Triton X-100, 2% bovine serum albumin (BSA), 4 mM EDTA, 0.1% sodium azide, and protease inhibitors) followed by centrifugation at 14,000×g for 30 min (Eppendorf, model 5430R). The tissue homogenate (100 µl) was added to each well and incubated at a 2–8° overnight. This was followed by repetitive washing and the addition of a biotinylated detection antibody and incubation for 2–3 h. After that, streptavidin-HRP conjugate solution was added, followed by 100 µl 3,3′,5,5′-Tetramethylbenzidine (TMB) after an hour. A stop solution was added and absorbance was recorded at 450 nm.
NF-kβ, Bcl-2, and Bax Estimations
To assess BCL-2, BAX, and NF-kβ levels tissue homogenate (100 µl) was added to an ELISA plate, pre-coated with monoclonal antibodies specific for Bcl-2, Bax, and NF-kβ for 90 min. Thereafter, a biotinylated detection antibody was added followed by incubation for 1 h at 37 °C. The plate was repetitively washed followed by the addition of HRP Conjugate for 30 min. The washing step was subsequently repeated and the substrate reagent was added and incubated for 15–30 min Finally, stop solution (50 µL) was added to each well. The absorbance of samples was read at 450 nm using a microplate reader (Bio-Rad Model 550; CA, USA).
Estimation of Caspase-3 Activity
To assess caspase-3 enzymatic activity, 50 µl of 2X Reaction Buffer containing 10 mM of DTT was added to 50 µl of the sample. Thereafter, 5 µl of 4 mM caspase-3 substrate (DEVD-pNA) was added to each reaction well and the reaction mixtures were incubated for 2 h at 37 °C. The absorbance was measured at a wavelength of 405 nm.
Statistical Analysis
All experimental data were analysed using Graph Pad Prism 6.0 software (Graph Pad, San Diego, USA) and results were presented as mean ± SEM. The escape latency data in the MMW was assessed using the two-way repeated-measures analysis of variance (ANOVA) followed by the Bonferroni multiple comparison post hoc test. For the rest of the data, a statistical comparison was made by one-way ANOVA followed by Tukey’s post hoc test. Results were considered to be statistically significant if p < 0.05 was considered.
Results
Effect of 7, 8 DHF on Locomotor Activity in 2-VO Rats
Regarding locomotor activity, no statistically significant difference was observed in the number of ambulations (p = 0.6946) and rearings (p = 0.4251) among various groups during the study (Fig. 2a and b).
Effect of 7, 8 DHF on Cognitive Function in 2-VO Rats
In MWM, the escape latency is measured as the time taken to reach a hidden platform and in repeated trials, a decrease in retention latency time indicates intact learning and memory function [33]. As shown in Fig. 3a, significantly longer escape latency was observed in 2-VO rats from day 3 onwards when compared to the sham group. A two-way ANOVA analysis detected a significant effect of both treatment [F (6, 175) = 8.26, p < 0.001) and time [F (4, 175) = 103.7, p < 0.001] while the interaction between these factors was not significant [F (24, 175) = 1.069, p = 0.3883]. Furthermore, we found that on days 4 and 5, 7,8-DHF (20 mg/kg) treatment significantly decreased escape latencies (p < 0.05, p < 0.01). 7, 8-DHF (10 mg/kg) and DNPZ group had a shorter escape latency on day 5 (p < 0.05). In addition, fewer crossings [F (6, 35) = 8.318, p < 0.001] and less time F (6, 35) = 7.723, p < 0.001] was spent by the 2-VO rats during the probe trial (Fig. 3b and c). However, both probe trial parameters were significantly improved on treatment with 7, 8-DHF (20 mg/kg), and DNPZ. Furthermore, no significant difference was observed in swimming speeds (p = 0.1093) among the groups (Fig. 3d). In the NOR test, the discrimination index was significantly decreased [F (6, 35) = 4.875, p < 0.01, Fig. 3e] in the 2 -VO group. 7, 8-DHF (10 and 20 mg/kg) and DNPZ treatment attenuated impairment in recognition memory reflected by improvement in discrimination index (p < 0.05).
Effect of 7,8-DHF on a escape latency b time spent in the target quadrant c platform crossings d swimming speed and e discrimination ratio in 2-VO rats. Data values are expressed as mean ± SEM. n = 6 in each group. *p < 0.05 as compared to sham group, #p < 0.05 as compared to 2-VO group. 7,8-DHF: 7,8-dihydroflavone, DNPZ: donepezil
Effect of 7,8 DHF on Hippocampal Cholinergic Activity in 2-VO Rats
Disruption in cholinergic signalling has been observed in VD. AChE is an enzyme that is responsible for catalyzing the hydrolysis of ACh into acetate and choline leading to a reduction in the neurotransmitter levels in the brain. As shown in Fig. 4, a significant increase in AChE activity [F (6, 35) = 10.58, p < 0.001] was observed in the hippocampus of 2-VO rats when compared to the sham group. In contrast, the administration of 7,8-DHF (10 and 20 mg/kg) and DNPZ were able to reduce AChE activity.
Effect of 7, 8 DHF on Hippocampal Oxidative Stress and Anti-oxidant Status
As shown in Table 1, hippocampal malondialdehyde (MDA) [F (6, 35) = 10.82, p < 0.001] and PCO [F (6, 35) = 8.752, p < 0.001] levels were significantly increased in 2-VO rats. Treatment with 7,8-DHF dose-dependently reduced MDA levels. Also, 7, 8-DHF (10 and 20 mg/kg) reduced PCO (p < 0.05, p < 0.01) levels in the hippocampus. Furthermore, the SOD [F (6, 35) = 10.02, p < 0.001], GSH-PX [F (6, 35) = 9.301, p < 0.001], and CAT [F (6,35) = 7.984, p < 0.01] enzymatic activities along with GSH [F (6, 35) = 10.79, p < 0.001] levels were also reduced in the hippocampus of 2-VO rats. However, treatment with 7,8-DHF (10 and 20 mg/kg) increased CAT and GSH-Px activity and GSH levels. 7, 8-DHF (20 mg/kg) treatment also enhanced hippocampal SOD activity (p < 0.05).
Effect of 7, 8-DHF on Hippocampal TNF-α, IL-1β, and NF-kβ Levels
As shown in Fig. 5a–c, TNF-α [F (6, 28) = 17.2, p < 0.001, Fig. 5a], IL-1β [F (6, 28) = 11.18, p < 0.001, Fig. 5b] and NF-kβ [F (6, 28) = 7.781, p < 0.001, Fig. 5c] levels were significantly elevated in the hippocampus of 2-VO rats. Treatment with 7,8-DHF (10 and 20 mg/kg) inhibited hippocampal TNF-α and IL-1β levels in 2-VO rats. Moreover, treatment with 7,8-DHF (10 & 20 mg/kg) also attenuated elevated hippocampal NF-kβ (p < 0.05) levels in 2-VO rats.
Effect of 7,8-DHF on hippocampal a TNF-α, b IL-1β, and c NF-kβ levels in 2-VO rats. Data values are expressed as mean ± SEM. n = 5 in each group. *p < 0.05 as compared to sham group, #p < 0.05 as compared to 2-VO group, βp < 0.05 as compared to DNPZ group. 7,8-DHF : 7,8-dihydroflavone, DNPZ: donepezil
Effect of 7, 8-DHF on Hippocampal p-AKT, p-CREB, and BDNF Levels in 2-VO Rats
A marked reduction in p-AKT [F (6, 28) = 18.28, p < 0.001, Fig. 6a], p-CREB [F (6, 28) = 11.08, p < 0.001, Fig. 6b], and BDNF [F (6, 28) = 13.67, p < 0.001, Fig. 6c] levels was observed in the hippocampus of 2-VO rats. However, 7,8-DHF (20 mg/kg) treatments significantly increased hippocampal p-AKT, p-CREB, and BDNF levels (p < 0.001, p < 0.05, p < 0.01). Furthermore, 7,8-DHF (10 mg/kg) also enhanced BDNF levels in the hippocampus although the results were statistically non-significant.
Effect of 7,8-DHF on hippocampal a p-AKT, b p-CREB, and c BDNF levels in 2-VO rats. Data values are expressed as mean ± SEM. n = 5 in each group. *p < 0.05 as compared to sham group, #p < 0.05 as compared to 2-VO group, αp < 0.05 as compared to 7,8-DHF (5 mg/kg). 7,8-DHF:7,8-dihydroflavone, DNPZ: donepezil
Effect of 7, 8-DHF on Hippocampal BCL-2, BAX and caspase-3 Levels in 2-VO Rats
Our results showed that the BCL-2 [F (6, 28) = 9.137, p < 0.001, Fig. 7a] levels were significantly decreased whereas BAX [F (6, 28) = 16.42, p < 0.001, Fig. 7b] levels were significantly higher in the hippocampus of 2-VO rats. Moreover, hippocampal caspase-3 [F (6, 28) = 11.25, p < 0.001, Fig. 7c) activity was also elevated in 2-VO rats. However, 7,8-DHF (10 and 20 mg/kg) and DNPZ treatments significantly reduced BAX levels and caspase-3 activity. In contrast, 7, 8-DHF (20 mg/kg) significantly increased hippocampal BCL-2 (p < 0.01) levels in 2-VO rats.
Effect of 7,8-DHF on hippocampal a BCL-2, b BAX, and c caspase-3 levels in 2-VO rats. Data values are expressed as mean ± SEM. n = 5 in each group. *p < 0.05 as compared to sham group, #p < 0.05 as compared to 2-VO group, αp < 0.05 as compared to 7,8-DHF (5 mg/kg). 7,8-DHF: 7,8-dihydroflavone, DNPZ: donepezil
Effect of 7, 8 DHF on Hippocampal ACh, GABA, and GLU Levels in 2-VO Rats
A significant increase in GLU [F (6, 28) = 11.59, p < 0.001] levels and reduction in ACh [F (6, 28) = 20.59, p < 0.001] levels was observed in the hippocampus of 2-VO rats when compared to the control group (Table 2). Hippocampal GABA levels were also decreased although the results were not statistically significant (p = 0.1638). Nevertheless, treatment with 7,8-DHF (10 and 20 mg/kg) and DNPZ increased ACh levels compared to vehicle-treated 2-VO rats. Moreover, 7,8-DHF (10 & 20 mg/kg) treatment also significantly reduced hippocampal GLU levels (p < 0.01, p < 0.001).
Discussion
VD is caused by a persistent but moderate reduction in cerebral blood flow (CBF) to distinct brain regions causing the deprivation of oxygen and nutrients to the brain and leading to cell death [34]. Over the years, the biochemical mechanisms involved in hypoperfusion-induced cognitive decline have been studied using the 2-VO model. This model is known to exhibit memory or cognitive impairment in various animal behavioral tests along with inflammatory reactions, blood–brain barrier disruption, and neuronal damage in the brain [35]. As such, potential neuroprotective strategies may be developed for VD and related neurodegenerative diseases using the 2-VO rat model. Therefore, in the present study, CCH induced by 2-VO was used to investigate the neuroprotective effects of 7, 8-DHF on cognitive impairment.
In the current study, 2-VO rats showed longer escape latency along with a reduction in the number of entries and time spent in the target quadrant. Moreover, the discrimination index a measure of cognitive dysfunction was also significantly decreased in 2-VO rats. These results are consistent with previous studies that show that CCH secondary to 2-VO results in impairment in spatial and recognition memory [36, 37]. Interestingly, results from our study illustrated that administration of 7,8-DHF alleviates cognitive decline in 2-VO rats. Indeed, in earlier studies, 7,8-DHF has been shown to reverse memory deficit in AD, schizophrenia, and Fragile X syndrome [17]. Moreover, 7,8-DHF is also known to counteract age-related decline in synaptic plasticity and spatial memory [18].
In addition, to behavioral changes, we also observed neurotransmitter alterations following CCH which are consistent with earlier experimental studies [38]. CCH caused a significant elevation in hippocampal glutamate levels whereas GABA levels were reduced. Interestingly, 2-VO rats treated with 7, 8-DHF significantly reduced hippocampal glutamate levels. Glutamate is an excitatory neurotransmitter that is responsible for synaptic transmission and long-term potentiation (LTP) process. However, excessive glutamate accumulation in the synaptic cleft leads to neuronal damage, a phenomenon known as excitotoxicity. It is well known that under ischemic conditions the activity of glial glutamate transporters ceases. Moreover, the pro-inflammatory cytokine TNF-α is also known to increase the expression of astrocytic glutaminase, which is known to convert glutamine to glutamate [39]. These events may lead to increased accumulation of glutamate in the extracellular space promoting neuronal excitotoxicity.
In the present study, we also observed a reduction in ACh levels in 2-VO rats. This could be attributed to the enhanced degradation of ACh into acetate and choline by AChE. Loss of cholinergic neurons along with reduced AChE activity has been observed in VD patients in the hippocampus, striatum cortex, and CSF. On this basis, numerous clinical studies have reported the benefits of AChE inhibitors, in improving cognitive function in mild to moderate VD [40]. Our results showed that AChE activity was elevated whereas ACh levels were reduced in the hippocampus of 2 VO rats. Treatment with 7,8-DHF effectively attenuated central cholinergic dysfunction. It has been reported earlier that 7,8-DHF treatment improved cognitive function by decreasing elevated hippocampal AChE activity in alcohol and HFD-fed animals and sporadic Alzheimer’s disease (SAD) model rats [16, 22]. These findings indicate the potential of 7,8-DHF as a cholinergic agent for VD treatment.
Oxidative stress and neuroinflammation are important mechanisms of neuronal injury and cognitive impairment induced by CCH. Reactive oxygen species (ROS) generated during CCH are known to oxidize intracellular molecules, such as membrane proteins, lipids, and DNA, and promote cellular apoptosis. Consistent with previous reports, the present findings indicated that MDA and PCO levels were increased in the hippocampus of CCH rats, indicative of oxidative damage to lipids and proteins [21, 36]. Moreover, reduced GSH levels and GPx, CAT, and SOD activities indicated compromised anti-oxidative machinery. In addition to oxidative stress, we also observed elevated levels of TNF-α, IL-1β, and NF-kβ in the hippocampus of VD rats. It has been found that following CCH the number of microglial cells is increased, and activated microglia release pro-inflammatory cytokines that mediate secondary brain damage [41]. Elevated TNF-α concentration can promote glutamate neurotoxicity, eventually leading to neuronal and oligodendrocyte cell death. Increased levels of IL-1β in the hippocampus may affect long-term potentiation, resulting in impaired learning and memory [42, 43]. Moreover, it also has been reported that in response to ROS, CCH induces activation of NF-kB, which is known to be involved in astrocyte inflammatory cascades, axonal loss, oligodendrocyte death, demyelination, and loss of white matter integrity [44]. 7,8-DHF treatment reversed hippocampal MDA and PCO levels and boosted anti-oxidative defences. Furthermore, 7,8-DHF treatment also significantly reduced the levels of TNF-α and IL-1β which is most likely mediated by its ability to suppress hippocampal NF-κβ levels. Previous studies have reported that 7,8-DHF possesses potent antioxidant, anti-inflammatory and anti-apoptotic properties. The presence of two adjacent hydroxyl groups as electron donors has led to the notion that 7,8-DHF may be a direct free radical scavenger [45]. Furthermore, 7,8-DHF reduced ROS production and enhanced cellular GSH levels caused by glutamate in a hippocampal HT-22 cell line [46]. Similarly, 7,8-DHF increased SOD activity and demonstrated direct free radical scavenging against 6-OHDA-induced cytotoxicity [47]. 7,8-DHF has also been shown to protect cortical neurons and RGC (retinal ganglion cells) and PC12 cells from oxidative stress and excitotoxic and induced apoptosis and cell death [13]. Regarding its anti-apoptotic actions in earlier studies, 7,8-DHF has been shown to increase AKT phosphorylation which is known to prevent the inhibition of anti-apoptotic BCL-2 by inactivating pro-apoptotic factors [14]. Moreover, in a recent study Ahmed, Kwatra [48] reported that 7,8-DHF upregulated the PI3K-AKT pathway leading to AKT phosphorylation which inhibited apoptosis by phosphorylating Bad at serine-136.
The upregulation of BDNF expression may be another possible mechanism for the neuroprotective action of 7, 8 DHF. BDNF is a major neurotrophic factor that is involved in various neurophysiological processes such as neuronal differentiation, maturation and survival, and neurogenesis [49, 50]. BDNF has been detected in the cerebral cortex, hippocampus, cerebellum, and amygdala, in both rodents and humans, with the highest levels found in hippocampal neurons [8]. It is also known to exert a neuroprotective effect under adverse conditions, such as cerebral ischemia, hypoglycemia, glutamatergic stimulation, and neurotoxicity [50]. BDNF is also known to induce long-term potentiation (LTP) that is linked to synaptic plasticity and learning and memory abilities [9]. In the present study, CCH reduced the hippocampal p-AKT, p-CREB, and BDNF, and this effect was reduced in treatment with 7,8-DHF. It has been reported that CREB becomes active and up-regulates BDNF expression when protein kinases such as AKT phosphorylate it at the serine-133 residue [51]. CREB is also involved in the transcription of various genes that are essential for learning and memory. Moreover, previous studies have shown that the maintenance of long-term potentiation is impaired due to a diminished level of CREB in hippocampus slices [52]. In the current study, it is possible that treatment with 7,8-DHF enhanced BDNF synthesis and release through phosphorylation of CREB which led to the reduction in 2-VO-induced cognitive decline. Indeed, in earlier studies, 7,8-DHF treatment is known to upregulate BDNF mRNA by enhancing neuronal CREB activation in experimental models of intracerebral haemorrhage, traumatic brain, and spinal cord injuries [14, 53].
Donepezil, an AChE inhibitor, is clinically used for the management of Alzheimer’s dementia. It is known to improve cognitive function in patients as well as in animal models of VD [37, 54]. Moreover, donepezil has also been shown to boost SVZ neurogenesis and BDNF expression in the cortex in CCH rat models [23, 55]. In the present study, donepezil improved memory performance in VD rats possibly via its actions on cholinergic neurotransmission and anti-apoptotic effects. However, it did not exhibit any significant effects on hippocampal BDNF levels, antioxidant machinery, inflammatory mediators, and glutamate levels as shown by 7,8-DHF. As multiple pathological pathways are involved in VD it appears that 7,8-DHF pleiotropic effects may provide additional pathways with therapeutic benefit in VD.
Conclusion
In conclusion, our study demonstrated that 7,8-DHF mitigates CCH-induced cognitive impairments and exerts neuroprotective effects by the inhibition of oxidative stress, inflammatory responses, and apoptosis as well as the regulation of the cholinergic system. Moreover, the mechanism of 7,8-DHFon memory impairment may also be related to the activation of the hippocampal AKT/CREB/BDNF signalling pathway and the amelioration of neurochemical alterations. These results indicate that 7,8-DHF could be a promising treatment against aging-related diseases, such as VD.
Data Availability
All data generated and/ or analysed during this study are included in this article.
References
Luo X-Q, Li A, Yang X, Xiao X, Hu R, Wang T-W, Dou X-Y, Yang D-J, Dong Z (2018) Paeoniflorin exerts neuroprotective effects by modulating the M1/M2 subset polarization of microglia/macrophages in the hippocampal CA1 region of vascular Dementia rats via cannabinoid receptor 2. Chin Med 13:1–17
Eyileten C, Kaplon-Cieslicka A, Mirowska-Guzel D, Malek L, Postula M (2017) Antidiabetic effect of brain-derived neurotrophic factor and its association with inflammation in type 2 diabetes mellitus. J Diabetes Res 2017:2823671
Venkat P, Culmone L, Chopp M, Landschoot-Ward J, Wang F, Zacharek A, Chen J (2020) HUCBC Treatment improves cognitive outcome in rats with vascular Dementia. Front Aging Neurosci 12:258
Zhang Z-Y, Liu Z, Deng H-H, Chen Q (2018) Effects of acupuncture on vascular Dementia (VD) animal models: a systematic review and meta-analysis. BMC Complement Altern Med 18:1–10
Zhang Y, Wang LL, Wu Y, Wang N, Wang SM, Zhang B, Shi CG, Zhang SC (2016) Paeoniflorin attenuates hippocampal damage in a rat model of vascular Dementia. Exp Ther Med 12:3729–3734
Erkinjuntti T, Roman G, Gauthier S, Feldman H, Rockwood K (2004) Emerging therapies for vascular Dementia and vascular cognitive impairment. Stroke 35:1010–1017
Baskys A, Cheng J-x (2012) Pharmacological prevention and treatment of vascular Dementia: approaches and perspectives. Exp Gerontol 47:887–891
Miranda M, Morici JF, Zanoni MB, Bekinschtein P (2019) Brain-derived neurotrophic factor: a key molecule for memory in the healthy and the pathological brain. Front Cell Neurosci 13:363
Zhen Y-F, Liu X-Y, Zhou D-H, Du X, Yin G, Zhang Y, Fang H, Xu G, Soares JC, Zhang XY (2018) Cognition, serum BDNF levels, and BDNF Val66Met polymorphism in type 2 Diabetes patients and healthy controls. Oncotarget 9:3653
Wang D-P, Yin H, Lin Q, Fang S-P, Shen J-H, Wu Y-F, Su S-H, Hai J (2019) Andrographolide enhances hippocampal BDNF signaling and suppresses neuronal apoptosis, astroglial activation, neuroinflammation, and spatial memory deficits in a rat model of chronic cerebral hypoperfusion. Naunyn-Schmiedeberg Arch Pharmacol 392:1277–1284
Wan Q, Ma X, Zhang Z-J, Sun T, Xia F, Zhao G, Wu Y-M (2017) Ginsenoside reduces cognitive impairment during chronic cerebral hypoperfusion through brain-derived neurotrophic factor regulated by epigenetic modulation. Mol Neurobiol 54:2889–2900
Weissmiller AM, Wu C (2012) Current advances in using neurotrophic factors to treat neurodegenerative disorders. Transl Neurodegen 1:1–9
Liu C, Chan CB, Ye K (2016) 7, 8-dihydroxyflavone, a small molecular TrkB agonist, is useful for treating various BDNF-implicated human disorders. Transl Neurodegen 5:1–9
Wu C-H, Hung T-H, Chen C-C, Ke C-H, Lee C-Y, Wang P-Y, Chen S-F (2014) Post-injury treatment with 7, 8-dihydroxyflavone, a TrkB receptor agonist, protects against experimental traumatic brain injury via PI3K/Akt signaling. PLoS ONE 9:e113397
Agrawal R, Noble E, Tyagi E, Zhuang Y, Ying Z, Gomez-Pinilla F (2015) Flavonoid derivative 7, 8-DHF attenuates TBI pathology via TrkB activation. Biochim Biophys Acta Mol Basis Dis 1852:862–872
Pandey SN, Mohit K, Dwivedi DK, Priyansha C, Mangala L, Ashok J (2020) 7, 8-Dihydroxyflavone alleviated the high-fat diet and alcohol-induced memory impairment: behavioral, biochemical and molecular evidence. Psychopharmacology 237:1827–1840
Tan Y, Nie S, Zhu W, Liu F, Guo H, Chu J, Cao XB, Jiang X, Zhang Y, Li Y (2016) 7, 8-dihydroxyflavone ameliorates cognitive impairment by inhibiting expression of tau pathology in ApoE-knockout mice. Front Aging Neurosci 8:287
Zeng Y, Lv F, Li L, Yu H, Dong M, Fu Q (2012) 7, 8-dihydroxyflavone rescues spatial memory and synaptic plasticity in cognitively impaired aged rats. J Neurochem 122:800–811
Castello NA, Nguyen MH, Tran JD, Cheng D, Green KN, LaFerla FM (2014) 7, 8-Dihydroxyflavone, a small molecule TrkB agonist, improves spatial memory and increases thin spine density in a mouse model of Alzheimer disease-like neuronal loss. PLoS ONE 9:e91453
Kwon KJ, Kim MK, Lee EJ, Kim JN, Choi B-R, Kim SY, Cho KS, Han J-S, Kim HY, Shin CY (2014) Effects of Donepezil, an acetylcholinesterase inhibitor, on neurogenesis in a rat model of vascular Dementia. J Neurol Sci 347:66–77
Dhaliwal N, Dhaliwal J, Singh A, Chopra K (2021) Dimethyl fumarate attenuates 2-VO-induced vascular Dementia via activating the Nrf2 signaling pathway in rats. Inflammopharmacology 29:537–547
Akhtar A, Dhaliwal J, Sah SP (2021) 7, 8-Dihydroxyflavone improves cognitive functions in ICV-STZ rat model of sporadic Alzheimer’s disease by reversing oxidative stress, mitochondrial dysfunction, and insulin resistance. Psychopharmacology 238:1–19
Jian W-x, Zhang Z, Zhan J-h, Chu S-f, Peng Y, Zhao M, Wang Q, Chen N-h (2020) Donepezil attenuates vascular Dementia in rats through increasing BDNF induced by reducing HDAC6 nuclear translocation. Acta Pharmacol Sin 41:588–598
Sachdeva AK, Chopra K (2015) Lycopene abrogates Aβ (1–42)-mediated neuroinflammatory cascade in an experimental model of Alzheimer’s Disease. J Nutr Biochem 26:736–744
Wills E (1965) Mechanisms of lipid peroxide formation in tissues role of metals and haematin proteins in the catalysis of the oxidation of unsaturated fatty acids. Biochim Biophys Acta Lipids Lipid Metab 98:238–251
Levine RL, Garland D, Oliver CN, Amici A, Climent I, Lenz A-G, Ahn B-W, Shaltiel S, Stadtman ER (1990) Determination of carbonyl content in oxidatively modified proteins. Methods in enzymology. Elsevier, Amsterdam, pp 464–478
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82:70–77
Kono Y (1978) Generation of superoxide radical during autoxidation of hydroxylamine and an assay for superoxide dismutase. Arch Biochem Biophys 186:189–195
Lawrence RA, Burk RF (1976) Glutathione peroxidase activity in selenium-deficient rat liver. Biochem Biophys Res Commun 71:952–958
Ellman GL, Courtney KD, Andres V Jr, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95
Bernt E, Bergmeyer HU (1974) l-Glutamate UV-assay with gutamate dehydrogenase and NAD. Methods of enzymatic analysis. Elsevier, Amsterdam, pp 1704–1715
Yadav M, Parle M, Jindal DK, Sharma N (2018) Potential effect of spermidine on GABA, dopamine, acetylcholinesterase, oxidative stress and proinflammatory cytokines to diminish ketamine-induced psychotic symptoms in rats. Biomed Pharmacother 98:207–213
Naik B, Nirwane A, Majumdar A (2017) Pterostilbene ameliorates intracerebroventricular streptozotocin induced memory decline in rats. Cog Neurodyn 11:35–49
Liu D-d, Yuan X, Chu S-f, Chen C, Ren Q, Luo P, Lin M-y, Wang S-s, Zhu T-b, Zhang D-m (2019) CZ-7, a new derivative of Claulansine F, ameliorates 2VO-induced vascular Dementia in rats through a Nrf2-mediated antioxidant responses. Acta Pharmacol Sin 40:425–440
Sohn E, Kim YJ, Lim H-S, Kim B-Y, Jeong S-J (2019) Hwangryunhaedok-Tang exerts neuropreventive effect on memory impairment by reducing cholinergic system dysfunction and inflammatory response in a vascular Dementia rat model. Molecules 24:343
Hu Y, Yang Y, Zhang M, Deng M, Zhang J-J (2017) Intermittent fasting pretreatment prevents cognitive impairment in a rat model of chronic cerebral hypoperfusion. J Nutr 147:1437–1445
Zhu X, Tian J, Sun S, Dong Q, Zhang F, Zhang X (2016) (-)-SCR1693 protects against memory impairment and hippocampal damage in a chronic cerebral hypoperfusion rat model. Sci Rep 6:28908
Bhuvanendran S, Bakar SNS, Kumari Y, Othman I, Shaikh MF, Hassan Z (2019) Embelin improves the spatial memory and hippocampal long-term potentiation in a rat model of chronic cerebral hypoperfusion. Sci Rep 9:1–11
Belov Kirdajova D, Kriska J, Tureckova J, Anderova M (2020) Ischemia-triggered glutamate excitotoxicity from the perspective of glial cells. Front Cell Neurosci 14:51
Wang J, Zhang H-Y, Tang X-c (2009) Cholinergic deficiency involved in vascular Dementia: possible mechanism and strategy of treatment. Acta Pharmacol Sin 30:879–888
Zhao Y, Zhang J, Zheng Y, Zhang Y, Zhang X, Wang H, Du Y, Guan J, Wang X, Fu J (2021) NAD + improves cognitive function and reduces Neuroinflammation by ameliorating mitochondrial damage and decreasing ROS Production in Chronic Cerebral Hypoperfusion models through Sirt1/PGC-1α pathway. J Neuroinflamm 18:207
Chen N, Chen X, Xie J, Wu C, Qian J (2019) Dexmedetomidine protects aged rats from postoperative cognitive dysfunction by alleviating hippocampal inflammation. Mol Med Rep 20:2119–2126
Bourgognon J-M, Cavanagh J (2020) The role of cytokines in modulating learning and memory and brain plasticity. Brain Neurosci Adv 4:2398212820979802
Saggu R, Schumacher T, Gerich F, Rakers C, Tai K, Delekate A, Petzold GC (2016) Astroglial NF-kB contributes to white matter damage and cognitive impairment in a mouse model of vascular Dementia. Acta Neuropathol Commun 4:1–10
Kang JS, Choi I-W, Han MH, Kim G-Y, Hong SH, Park C, Hwang HJ, Kim CM, Kim BW, Choi YH (2015) The cytoprotective effects of 7, 8-dihydroxyflavone against oxidative stress are mediated by the upregulation of Nrf2-dependent HO-1 expression through the activation of the PI3K/Akt and ERK pathways in C2C12 myoblasts. Int J Mol Med 36:501–510
Chen J, Chua K-W, Chua CC, Yu H, Pei A, Chua BH, Hamdy RC, Xu X, Liu C-F (2011) Antioxidant activity of 7, 8-dihydroxyflavone provides neuroprotection against glutamate-induced toxicity. Neurosci Lett 499:181–185
Han X, Zhu S, Wang B, Chen L, Li R, Yao W, Qu Z (2014) Antioxidant action of 7, 8-dihydroxyflavone protects PC12 cells against 6-hydroxydopamine-induced cytotoxicity. Neurochem Int 64:18–23
Ahmed S, Kwatra M, Gawali B, Panda SR, Naidu V (2021) Potential role of TrkB agonist in neuronal survival by promoting CREB/BDNF and PI3K/Akt signaling in vitro and in vivo model of 3-nitropropionic acid (3-NP)-induced neuronal death. Apoptosis 26:52–70
Kowiański P, Lietzau G, Czuba E, Waśkow M, Steliga A, Moryś J (2018) BDNF: a key factor with multipotent impact on brain signaling and synaptic plasticity. Cell Mol Neurobiol 38:579–593
Bathina S, Das UN (2015) Brain-derived neurotrophic factor and its clinical implications. Arch Med Sci: AMS 11:1164
Yu X, Guan Q, Wang Y, Shen H, Zhai L, Lu X, Jin Y (2019) Anticonvulsant and anti-apoptosis effects of salvianolic acid B on pentylenetetrazole-kindled rats via AKT/CREB/BDNF signaling. Epilepsy Res 154:90–96
Kalivarathan J, Kalaivanan K, Chandrasekaran SP, Nanda D, Ramachandran V, Venkatraman AC (2020) Apigenin modulates hippocampal CREB-BDNF signaling in high fat, high fructose diet-fed rats. J Funct Foods 68:103898
Wu C-H, Chen C-C, Hung T-H, Chuang Y-C, Chao M, Shyue S-K, Chen S-F (2019) Activation of TrkB/Akt signaling by a TrkB receptor agonist improves long-term histological and functional outcomes in experimental intracerebral Hemorrhage. J Biomed Sci 26:1–16
Wilkinson D, Doody R, Helme R, Taubman K, Mintzer J, Kertesz A, Pratt R (2003) Donepezil in vascular Dementia: a randomized, placebo-controlled study. Neurology 61:479–486
Man J, Cui K, Fu X, Zhang D, Lu Z, Gao Y, Yu L, Li N, Wang J (2020) Donepezil promotes neurogenesis via Src signaling pathway in a rat model of chronic cerebral hypoperfusion. Brain Res 1736:146782
Funding
This experimental work did not receive any specific grant from any funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
KC and ND conceived and designed the present study. JD and ND carried out the experiments and analysed and interpreted the data. ND wrote and edited the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dhaliwal, N., Dhaliwal, J. & Chopra, K. 7, 8-dihydroxyflavone Ameliorates Cholinergic Dysfunction, Inflammation, Oxidative Stress, and Apoptosis in a Rat Model of Vascular Dementia. Neurochem Res 49, 1137–1149 (2024). https://doi.org/10.1007/s11064-023-04090-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-023-04090-9