Abstract
Hyperglycemia as the major hallmark of diabetic neuropathy severely limited its therapeutic efficiency. Evidences have revealed that selenium (Se) as an essential trace element could effectively reduce the risk of neurological diseases. In the present study, 3,3′-diselenodipropionic acid (DSePA), a derivative of selenocystine, was employed to investigate its protective effect against high glucose-induced neurotoxicity in PC12 cells and evaluate the underlying mechanism. The results suggested that high glucose showed significant cytotoxicity through launching mitochondria-mediated apoptosis in PC12 cells, accompanied by poly (ADP-ribose) polymerase (PARP) cleavage, caspase activation, and mitochondrial dysfunction. Moreover, high glucose also triggered DNA damage and dysregulation of MAPKs and AKT pathways through reactive oxygen species (ROS) overproduction. p53 RNA interference partially suppressed high glucose-induced cytotoxicity and apoptosis, indicating the role of p53 in high glucose-induced signal. However, DSePA pretreatment effectively attenuated high glucose-induced cytotoxicity, inhibited the mitochondrial dysfunction through regulation of Bcl-2 family, and ultimately reversed high glucose-induced apoptotic cell death in PC12 cells. Attenuation of caspase activation, PARP cleavage, DNA damage, and ROS accumulation all confirmed its protective effects. Moreover, DSePA markedly alleviated the dysregulation of AKT and MAPKs pathways induced by high glucose. Our findings revealed that the strategy of using DSePA to antagonize high glucose-induced neurotoxicity may be a highly effective strategy in combating high glucose-mediated neurological diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetic neuropathy represents one of the most defining diabetes-related syndromes affecting up to 50 % of patients with long-standing disease, leading to sensory, motor, and autonomic dysfunction [1]. Clinical evidences report that hyperglycemia resulting from uncontrolled glucose regulation was recognized as the major hallmark of diabetic neuropathy and severely hindered its therapeutic efficiency [1–4]. The resistant mechanism of patients with diabetic neuropathy to traditional therapies was generally ascribed to high glucose-induced neurotoxicity by triggering reactive oxygen species (ROS)-mediated inflammation and oxidative damage to neuron and the connection between neuron and/or gliocyte [1–6]. Persistent hyperglycemia in the brain can affect mitochondrial membrane potential (Δψm) and trigger oxidative stress, and enhance the ROS accumulation. Overproduced ROS will harm synapse, disturb neuronal communication, and even cause neuronal cell death [5–7]. Hence, inhibition of hyperglycemia-mediated ROS generation and oxidative damage by novel antioxidants is one of the most effective strategies in combating human high glucose-mediated neurological diseases.
Selenium (Se), an essential mineral trace element, is of fundamental importance to animals and humans due to its multiple pharmacological properties [8, 9]. Epidemiological, preclinical, and clinical studies supported that many selenium-containing compounds exhibit potent antioxidant, antitumor activities, and enhancement of immunity [10, 11]. Increasing evidences also indicate that Se supplement can effectively reduce the risk of neurological diseases [12–14]. More importantly, selenium compounds display novel selectivity between cancer cells and human normal cells. 3,3′-diselenodipropionic acid (DSePA), a stable and water-soluble diselenide, exhibits robust protective potential against cell damage or apoptosis in many fields [15, 16]. Due to its high efficacy and less toxicity, DSePA has attracted much attention of many researchers, especially for its antioxidant effect [17]. Antioxidative stress currently was accepted as the critical cellular event for the protective action of DSePA. However, the exact molecular mechanism remains elusive.
Herein, we explored the possible protective effects of DSePA against high glucose-mediated neurotoxicity and the underlying molecular mechanisms. The results showed that DSePA pretreatment dramatically antagonized high glucose-induced cytotoxicity in PC12 cells by suppression of high glucose-induced apoptosis through attenuation of ROS-mediated DNA damage and mitochondrial dysfunction with involvement of modulating MAPKs and AKT pathways. Our findings revealed that the strategy of using DSePA could be a highly effective way in chemoprevention and chemotherapy of high glucose-mediated neurological diseases.
Materials and Methods
Chemicals
DSePA, glutathione (GSH), JC-1 probes, DCFH-DA probes, MTT, and other reagents were purchased from Sigma. Bicinchoninic acid (BCA) assay kit was purchased from Beyotime Institute of Biotechnology. TUNEL-DAPI co-staining kit was purchased from Roche. LY294002 were obtained from Calbiochem (San Diego, CA, USA). All antibodies used in this study were purchased from Cell Signaling Technology (Beverly, MA, USA). Dulbecco’s modification of Eagle’s medium (DMEM), fetal bovine serum (FBS), and penicillin–streptomycin were purchased from Invitrogen. All solvents used were of high-performance liquid chromatography (HPLC) grade.
Cell Culture, Drug Treatment, and Cell Viability
PC12 cells were maintained in DMEM (glucose, 25 mM, 4.5 mg/ml) supplemented with 10 % FBS, 50 U/ml streptomycin, and 100 U/ml penicillin in a humidified incubator under 5 % CO2 at 37 °C. Cytotoxicity of DSePA and high glucose was screened as follows. Briefly, PC12 cells seeded in 96-well plate (8 × 103 cells/well) were separately exposed to various concentrations of glucose 50 mM (9 mg/ml), 75 mM (13.5 mg/ml), 100 mM (18 mg/ml), 150 mM (27 mg/ml), and 200 mM (36 mg/ml) for 48 h or DSePA (2.5, 5, 10, 20, and 40 μM) for 48 h. For combined treatment, PC12 cells were pretreated with indicated concentrations of DSePA (5, 10, and 15 μM) for 6 h and co-treated with 100 mM glucose for another 48 h. Cell viability was detected by MTT assay, which based on the ability of cells to change MTT substrate into a purple formazan dye. Briefly, MTT solution (5 mg/ml) at 20 μl/well was added to cells after treatment and incubated for 5 h at 37 °C. Then, the medium was removed and replaced with DMSO (150 μl/well). Then, the color intensity reflecting the cell growth was examined at 570 nm. The data were expressed as percentages of control (as 100 %).
Cell Cycle Distribution and Cell Apoptosis
The cell cycle distribution and cell apoptosis were analyzed by flow cytometric analysis. Briefly, cells after treatment with glucose or/and DSePA were collected, washed, and fixed with 70 % ethanol at −20 °C overnight. Then, cells were stained with PI and analyzed by flow cytometry. The cell cycle distribution was analyzed using a Multi Cycle software (Phoenix Flow Systems, San Diego, CA, USA). The proportions of cells in G0/G1, S, and G2/M phases represented as DNA histograms. Apoptotic cells with hypodiploid DNA contents were measured by quantifying the sub-G1 peak. For each experiment, 10,000 events per sample were recorded.
TUNEL-DAPI Co-staining
Cell apoptosis in PC12 cells by high glucose was also detected by TUNEL-DAPI co-staining kit. Briefly, cells exposed to DSePA or/and high glucose were fixed with 4 % paraformaldehyde and permeabilized with 0.1 % Triton X-100, then incubated with 100 μl/well TUNEL reaction mixture for 1 h and 1 μg/ml DAPI for 15 min at 37 °C, respectively. Then, cells were washed with PBS for three times and examined under a fluorescence microscope (magnification, ×200). The cells stained with green fluorescence represent the TUNEL-positive cells, indicating the apoptotic cells.
Caspase Activity
Caspase activity was determined by a fluorometric method. PC12 cells after treatment were harvested by centrifugation, suspended in cell lysis buffer, and incubated on ice for 1 h. After centrifugation at 11,000 g for 15 min, supernatants were collected, normalized for protein concentration, and measured for caspase activity. Briefly, total proteins (100 μg/well) were placed in 96-well plate, then specific caspase substrates (Ac-DEVD-AMC for caspase-3, Ac-IETD-AMC for caspase-8, and Ac-LEHD-AMC for caspase-9) were added. After incubation at 37 °C for 2 h in darkness, caspase activity was detected by fluorescence intensity with the excitation and emission wavelengths set at 380 and 440 nm, respectively. The caspase-3/-8/-9 activity was expressed as percentages of control (as 100 %).
Western Blotting
Cells after treatment were collected and lysed in RIPA lysis buffer on ice for 1 h at 4 °C. Total protein was extracted and quantified by BCA assay kit strictly complying with the prospectus. Then, total protein (40 μg/lane) after denaturation was loaded and separated in 10 % SDS-PAGE (110 V, 75 min). After electrophoresis, the protein was transferred from the gel to a nitrocellulose membrane (NCM) and blocked with 5 % non-fat milk for 2 h at room temperature. Then, the NCM was incubated with primary antibodies (1:1000) overnight at 4 °C and second antibodies (1:2000) for 1 h at room temperature. Then, the target protein was scanned on X-ray film using an enhanced chemiluminescence system (Kodak). β-actin was used as the reference band. The protein expression was quantified by Quantity-One Software, and the expression rate was labeled under the bands.
Evaluation of Mitochondrial Membrane Potential (Δψm) and Structure
Mitochondrial membrane potential (Δψm) was evaluated by JC-1 assay. Briefly, PC12 cells after drug treatment were seeded in a six-well plate and incubated with JC-1 dye (5 μg/ml) for 30 min at 37 °C in darkness. Then, cells were washed with PBS and visualized by fluorescence microscopy (magnification, ×200). The fluorescence shift from red to green represents the lost of Δψm. Alternation of mitochondrial structure was detected by mito-tracker (mitochondria, green) and DAPI (nucleus, blue) co-staining. Cells after treatment were visualized under a fluorescent microscope (magnification, ×1000).
Detection of ROS and Nitric Oxide Accumulation
The intracellular ROS level was examined by DCFH-DA assay. Briefly, cells seeded in 96-well plate at 8 × 103 cells/well were pretreated with DSePA (5 and 10 μM) or GSH (5 mM) for 6 h and co-incubated with glucose (100 mM) for 2 h. Then, cells were incubated with 10 μM DCFH-DA at 37 °C for 15 min in the dark. After washing twice with PBS, ROS generation was detected with the excitation wavelength at 488 nm and emission wavelength at 525 nm, respectively. The nitric oxide (NO) production was detected by a NO detecting kit according to the manufacturer’s instructions (Beyotime, S0021). The superoxide in live cells was detected by MitoSOX specific red dye which can target mitochondria superoxide according to the manufacturer’s instructions (Invitrogen, M36008). The data are expressed as percentages of control (as 100 %).
RNA Interference
The transfection of p53 siRNA into PC12 cells was carried out according to the previous method. Cells seeded in six-well plates were incubated with 100 nM p53 siRNA and transfection reagent in serum-free DMEM medium for 24 h, and then 1 ml fresh completed medium was added to each well for another 24 h. Then, cells were administrated with DSePA or/and high glucose. Besides, cells were also transfected with a fluorescein-labeled non-targeted control siRNA to detect the transfection efficiency.
Statistical Analysis
All data were gained from three independent experiments. Statistical analysis was performed using the SPSS statistical software (SPSS 13.0, USA). Data were expressed as the means ± SD. Differences between two groups were analyzed by two-tailed Student’s t test. The significance among three or more groups was assayed by multiple comparisons. Bars with different characters represent the statistical significant at P < 0.05.
Results
DSePA Attenuates High Glucose-Induced Cytotoxicity in PC12 Cells
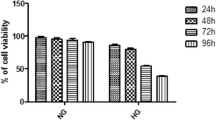
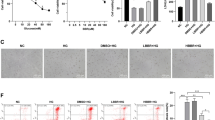
Firstly, the cytotoxicity of high glucose and DSePA was screened to ascertain the biological safe doses by MTT assay. As shown in Fig. 1a, b, glucose treatment (50–200 mM) significantly reduced the cell viability in a dose-dependent manner, with approximately 36 % cell death at 100 mM glucose (Fig. 1a). DSePA alone displayed less toxicity to PC12 cells. Subsequently, the pretreatment time of DSePA was optimized. The results showed that cells by DSePA pretreatment for 1–12 h before glucose co-treatment all exhibited prolonged cell viability (Fig. 1c, d), indicating that DSePA could inhibit glucose-induced cytotoxicity. The optimal time was observed at 6 h, therefore, pretreatment time (6 h) of DSePA was employed to evaluate the protective mechanism.
DSePA inhibits high glucose-induced cytotoxicity in PC12 cells. Cytotoxic effect of glucose (a) and DSePA (b) alone on PC12 cells. PC12 cells (8000 cells/well in 96-well plate) were treated with indicated concentrations of glucose or DSePA alone for 48 h. Cell viability was detected by MTT assay. Experimental scheme (c) and protective effect (d) induced by DSePA against high glucose in PC12 cells. PC12 cells were pretreated with 10 μM DSePA for 0, 1, 3, 6, and 12 h and then co-incubated with 100 mM glucose for another 48 h. Cell viability was measured by MTT assay. e DSePA attenuated high glucose-induced cytotoxicity in PC12 cells. For combined treatment, PC12 cells were pretreated with indicated concentrations of DSePA (5, 10, and 15 μM ) for 6 h and then exposed to 100 mM glucose for 48 h. Bars with different characters are statistically different at p < 0.05 level. f Morphological observation. Representative images were obtained by inverted light microscopy (original magnification, ×200). The images shown here are representative of four independent experiments with different treatment. All images shown here are representative of three independent experiments with similar results
As shown in Fig. 1e, pretreatment of PC12 cells with DSePA (5–15 μM) for 6 h significantly suppressed glucose-mediated cell killing in a dose-dependent manner. For instance, at concentrations of 5, 10, and 15 μM, DSePA improved the cell viability from 72.4 % (glucose 100 mM alone) to 76.2, 82.3, and 93.1 %, respectively. DSePA alone showed no toxicity to PC12 cells. To further confirm the protective effect of DSePA in the other cell lines, we repeated the Fig. 1e results with BV-2 (microglia) and HUVEC (human umbilical vein endothelial cell) cell lines. The results indicated that DSePA showed similar protective effects in BV-2 cells and HUVEC against high glucose-induced cytotoxicity (Fig. S1). The improvement of PC12 cell morphology further confirmed its protective effect (Fig. 1f). For instance, PC12 cells treated with 100 mM glucose showed cell shrinkage, reduction in attaching cell numbers, and loss of cell-to-cell contact. However, DSePA pretreatment apparently reversed this tendency. Taken together, these results clearly indicated that DSePA had the potential to inhibit high glucose-induced cytotoxicity in PC12 cells.
DSePA Suppresses High Glucose-Induced PC12 Cells Apoptosis
To elucidate the mode of cell death, flow cytometric analysis was used to detect the high glucose-induced cell death. Apoptotic cells with hypodiploid DNA content were quantified by measuring the sub-G1 peak. As shown in Fig. 2a, 100 mM glucose treatment caused significant cell apoptosis, as proven by the increase of sub-G1 peak to 23.5 %, while DSePA pretreatment apparently suppressed sub-G1 cells to 6.7 % in PC12 cells. What’s more, the control cells and cells treated with DSePA alone both showed no obvious cell apoptosis. High glucose-induced apoptosis was further confirmed by TUNEL and DAPI co-staining assay. As shown in Fig. 2b, PC12 cells after treatment with 100 mM glucose alone exhibited typical apoptotic features, such as nuclear fragmentation and chromatin condensation. However, pretreatment with DSePA effectively prevented PC12 cells from high glucose-induced apoptosis, as convinced by the weak green fluorescence. Taken together, these results all suggest that induction of apoptosis is the major mode of cell death induced by high glucose, and DSePA has the potential to antagonize high glucose-induced cytotoxicity via inhibition of cell apoptosis.
DSePA suppresses high glucose-induced apoptosis. a Flow cytometric analysis of cell cycle distribution and apoptosis. PC12 cells were pretreated with or without 10 μM DSePA for 6 h and then cultured in the presence or absence of 100 mM glucose for another 48 h. Cells after treatment were collected and stained with PI solution after fixation by 70 % ethanol. Then, the cells were analyzed by flow cytometric analysis. Apoptotic cells with hypodiploid DNA content were measured by quantifying the sub-G1 peak. b Representative images of DNA fragmentation and nuclear condensation in response to DSePA pretreatment in PC12 cells. Cells cultured in chamber slides were treated with 10 μM DSePA and/or 100 mM glucose and fixed with formaldehyde. Nuclear staining in PC12 cells was examined by TUNEL and DAPI co-staining as described in “Materials and Methods.” c Caspase activation. Analysis of caspase-3/-8/-9 activation induced by DSePA (10 μM), glucose (100 mM), and co-treatment. Cells after treatment were lysed, and caspase-3/-8/-9 activity was measured with whole cell extracts by a synthetic fluorescent substrate as described in “Materials and Methods.” d Expression levels of PARP and caspase-3/-7/-9 exposed to 10 μM DSePA and/or 100 mM glucose in PC12 cells. PC12 cells after treatment were collected and lysed, cell proteins (40 mg) were separated by SDS-PAGE and incubated with specific primary and secondary antibodies, respectively. Equal loading was confirmed by stripping immunoblots and reprobing for β-actin
The intrinsic (mitochondria-mediated) and the extrinsic (death receptor-mediated) signaling pathways both contribute to apoptotic signaling [18]. To further characterize the trait of high glucose-induced apoptotic mechanism, the status of caspases were tested using specific substrates. As shown in Fig. 2c, PC12 cells treated with high glucose showed dramatic increase in caspase-3, -8, and -9 activities, suggesting that high glucose activated both the intrinsic and extrinsic apoptosis pathways. Besides, activation of caspase-9, the predominant initiator of mitochondria-mediated apoptotic pathway, was more prominent than that of caspase-8, indicating that high glucose-induced cell apoptosis was mainly mediated by mitochondria-mediated apoptosis. However, pretreatment with DSePA distinctly inhibited the activation of caspase-3, -8, and -9. Additionally, Western blotting was employed to confirm high glucose-induced apoptosis in protein level. Figure 2d showed apparent increase of poly (ADP-ribose) polymerase (PARP) cleavage and activation of caspase-3, -8, and -9 after high glucose treatment alone. However, DSePA pretreatment significantly repressed high glucose-induced PARP cleavage and caspase activation. Taken together, these results suggested that DSePA suppressed high glucose-induced cytotoxicity by inhibiting mitochondria-mediated apoptosis.
DSePA Blocks High Glucose-Induced Mitochondrial Dysfunction Through Regulation of Bcl-2 Family
Mitochondria acts critical roles in regulating the intrinsic and extrinsic apoptosis pathways [19]. Mitochondrial membrane potential (Δψm) can affect the mitochondrial permeability transition pore (MPTP), cause the activation of caspases, and eventually trigger the apoptotic cascades [20]. Therefore, we examined the change of Δψm in PC12 cells by JC-1 molecular probe, which the fluorescence shift from red to green will reflect the depletion of Δψm. As shown in Fig. 3a, 100 mM glucose significantly decreased the Δψm, as evidenced by the shift of JC-1 fluorescence from red to green. However, DSePA pretreatment obviously reversed high glucose-induced depletion of Δψm. The statistical analysis of Δψm further quantified this protective potential (Fig. 3b). Moreover, mitochondrial morphology in living cells was examined. As shown in Fig. 3c, the mitochondrial network in healthy PC12 cells exhibits filamentous and extensively interconnected throughout the cytoplasm. Cells treated by 100 mM glucose displayed large-scale mitochondrial fragmentation (from protonema to punctiform). However, DSePA observably inhibited high glucose-induced mitochondrial fragmentation. Taken together, these findings directly revealed that DSePA blocked high glucose-induced mitochondrial dysfunction.
DSePA blocks high glucose-induced mitochondrion dysfunction through regulation of Bcl-2 family. a Representative images of PC12 cells stained with JC-1. PC12 cells after treatment were stained with JC-1 as described in “Materials and Methods” and then photographed by a fluorescence microscope. b Analysis of Δψm. The Δψm was analyzed by Image-Pro Plus 6.0. c Mitochondrial fragmentation. Alternation of mitochondrial structure was detected by mito-tracker (mitochondria, green) and DAPI (nucleus, blue) co-staining. Cells after treatment were visualized under a fluorescent microscope (magnification, ×1000). d Western blotting analysis of expression levels of Bcl-2 family proteins in PC12 cells. The protein expression was detected by Western blotting method
Bcl-2 family is thought to be important in regulation of Δψm and mitochondria-mediated apoptosis [21]. The balance between pro-apoptotic proteins (Bax, Bad, and Bid) and antiapoptotic proteins (Bcl-2 and Bcl-xL) decides the cells fate [22]. Hence, Western blotting was employed to identify whether the Bcl-2 family was involved in high glucose-induced cell apoptosis. As shown in Fig. 3d, 100 mM glucose treatment caused light changes in Bax and Bad expression, but notably decreased the expression of pro-apoptotic proteins Bcl-xL and Bcl-2. However, DSePA pretreatment effectively balanced this change, implying that DSePA blocks high glucose-induced mitochondrial dysfunction via modulating the Bcl-2 family.
DSePA Attenuates High Glucose-Induced DNA Damage and p53 Phosphorylation via Inhibiting ROS Accumulation
ROS will be mainly released from mitochondrial respiratory chain in response to various apoptotic stimulations [10]. Accumulated studies suggest that ROS overproduction and subsequent induction of oxidative damage were both involved in high glucose-induced neurotoxicity [23]. Therefore, intracellular ROS accumulation was measured by a fluorescein-labeled dye, DCFH-DA. As shown in Fig. 4a, treatment of PC12 cells with 100 mM glucose for 2 h resulted in significant intracellular ROS generation to 187.6 % of control. However, pretreatment with DSePA (5 and 10 μM) acutely hindered the intracellular ROS level to 165.3 and 123.4 % in a dose-dependent manner. Addition of glutathione (GSH) a positive ROS scavenger effectively eliminated ROS, which further confirmed DSePA’s antioxidative effect. Furthermore, the superoxide in live cells was detected by MitoSOX specific red dye which can target mitochondria superoxide. The result showed that high glucose treatment obviously induced superoxide production in mitochondria, and DSePA pretreatment significantly inhibited the superoxide production (Fig. S3). Moreover, slight NO production (not dominant) was also detected in high glucose-treated cells (Fig. S2). These results above implied that ROS and RNS both contributed to high glucose-induced cytotoxicity.
DSePA attenuates high glucose-mediated DNA damage and p53 phosphorylation. a DSePA attenuates high glucose-induced ROS accumulation in PC12 cells. PC12 cells (105 cells/well) were pretreated with DSePA (0, 5, 10 μM) or 5 mM GSH for 2 h and then cultured in the presence or absence of 100 mM glucose for another 2 h, the ROS generation was detected with a DCFH-DA probe as described in “Materials and Methods.” b DSePA supplement attenuates high glucose-mediated DNA damage. Cells after treatment were lysed, and the protein expression was examined via Western blotting methods. c Suppressive effects of p53 SiRNA on high glucose-induced p53 phosphorylation and caspase-3 activation in PC12 cells. Cells were pretreated with or without 50 nmol p53 SiRNA for 24 h and then treated with or without 100 mM glucose for another 48 h, then cells were collected and lysed and the protein expression was examined via Western blotting methods. d p53 SiRNA partially inhibits high glucose-induced cytotoxicity and apoptosis in PC12 cells. Cell viability was examined by MTT assay
Overproduced ROS may attack DNA and trigger DNA damage [24]. Therefore, high glucose-induced DNA damage was investigated by Western blotting. As shown in Fig. 4b, treatment of PC12 cells with 100 mM glucose caused obvious DNA damage, as confirmed by upregulation of the phosphorylation levels of ATM, ATR, p53 (Ser 15, Ser 9, Ser 392), and H2A, which are all the components of DNA damage axis [25]. However, DSePA pretreatment strongly inhibited high glucose-induced DNA damage, as evidenced by downregulation of phosphorylation levels of all the DNA damage markers above. Based on the importance of p53, we next examined the effect of p53 siRNA on p53 (Ser 15, Ser 9) expression. As expected, p53 siRNA treatment partly attenuated high glucose-induced DNA damage, as convinced by the decline of Ser15- and Ser 9-p53 expression (Fig. 4c). Prolonged cell viability and decreased cell apoptosis in glucose-treated cells all emphasized the role of p53 in glucose-induced apoptotic signal. Taken together, these results above observably revealed that DSePA suppressed high glucose-induced cytotoxicity and apoptosis by inhibiting ROS-mediated DNA damage and p53 phosphorylation.
Contribution of MAPKs and AKT Pathways
MAPKs and PI3K/AKT pathways both dominate kinds of cell proliferation, differentiation, and survival, including nerve cells [26]. Hence, Western blotting was employed to investigate the component changes using specific antibodies against the activated forms of kinase. Primarily, a detailed time-course examination was carried out. As shown in Fig. 5a, the p-AKT expression in PC12 cells exposed to 100 mM glucose for the indicated times showed a sustained activation from 1 to 3 h, which reached the control level after 6 h, and showed continuous inactivation thereafter. However, phosphorylated JNK and p38 were detected as a sustained activation in a time-dependent manner. Only slight down-regulation of p-ERK expression was observed after glucose treatment. These results indicate that MAPKs and PI3K/AKT pathway both contributed to glucose-induced cytotoxicity and apoptosis.
Contribution of MAPKs and AKT pathways. a Time-dependent effects of high glucose on protein expression of MAPKs and AKT pathways. Cells were treated with 100 mM glucose for indicated time, and then, temporal changes in the expression levels of proteins was detected by Western blotting. b Inhibitor of AKT (LY294002) enhanced high glucose-induced inactivation of AKT. c Inhibitor of AKT (LY294002) enhanced high glucose-induced cell death in PC12 cells. Cells were pretreated with or without 10 μM LY294002 for 1 h and then cultured in the presence or absence of 100 mM glucose for 48 h. p-AKT expression was examined via Western blotting methods, and cell viability was detected by MTT assay. d DSePA normalized MAPKs and AKT signal in high glucose-treated cells. The protein expression was detected by Western blotting method
Based on the importance of AKT pathway, LY2294002 (AKT upstream inhibitor) was used to examine its role in glucose-induced apoptotic signal. As shown in Fig. 5b, c, pretreatment of PC12 cells with LY2294002 significantly aggravated high glucose-induced AKT inactivation and cell killing. The MTT data showed that a marked decrease of cell viability was observed from 74.8 to 51.9 %, indicating that high glucose inhibited PC12 cell growth with an AKT-dependent manner. However, pretreatment with DSePA obviously up-regulated the phosphorylation level of AKT and slightly suppressed the phosphorylation of JNK and p38 (Fig. 5d). Taken together, these findings demonstrated that MAPKs and AKT pathways both contributed to DSePA-mediated protective mechanism against high glucose-induced cytotoxicity and apoptosis in PC12 cells.
Discussion
Se, an essential trace element, is of fundamental importance to humans due to its multiple pharmacological properties [8, 9]. Increasing evidences indicate that Se is essential for normal brain function, and Se supplement can effectively reduce the risk of impaired cognitive function and neurological diseases, such as Alzheimer’s disease (AD), Parkinson’s disease (PD), Huntington’s disease (HD), and epilepsy [12–14, 27]. Studies reported that Se deficiency is associated with cognitive decline, and Se supplement is helpful in preventing neurodegeneration in humans [12, 28, 29]. Evidences demonstrated that Se is potentially a beneficial agent in treating ischemia–reperfusion-induced brain injury in rats [13]. However, little information about the protective effect of Se against hyperglycemia-induced toxicity and apoptosis is available, especially the molecular mechanism.
PC12 derived from rat pheochromocytoma cells was considered as an optimal model in vitro to simulate neuron to explore the underlying mechanism [30, 31]. After all, PC12 cell line is a cancer cell line, the in vivo effect and mechanism of DSePA need further evaluation. Apoptosis, a programmed cell death, plays an essential role in maintaining the homeostasis in the brain [32, 33]. Caspase, a family of cysteine proteases, can be activated in response to apoptotic stimuli and play essential roles in launching cell apoptosis [34, 35]. Active caspase-3 could inactivate PARP and eventually lead to the occurrence of apoptotic cascade through the enzymolysis of a series of substrates [36]. In the present study, activation of caspase-8 and caspase-9 in PC12 cells treated with high glucose indicated the activation of both death receptor-mediated and mitochondria-mediated signaling pathways. The quantitative expression of caspases in protein level further verified the role of caspases in high glucose-induced apoptosis. However, pretreatment with DSePA significantly blocked the process of apoptosis as convinced by the reduction of caspase activation and PARP cleavage. These results clearly indicated that DSePA inhibited high glucose-induced apoptosis through suppressing mitochondria-mediated pathway.
Mitochondria and Δψm both play an important role in initiating mitochondria-mediated apoptosis [37–40]. Depletion of Δψm will lead to the opening of the MPTP, followed by the release of cytochrome C, apoptosis-inducing factors (AIFs), SMAC/Diablo, and endonuclease G [41, 42], which all contribute to mitochondria-mediated apoptosis. Much evidence, including oxidative stress, has established a link between various disturbances in mitochondrial functioning and diabetic neuropathy [1–4]. In the present study, DSePA pretreatment observably alleviated high glucose-induced disruption of Δψm, which is consistent with the hypothesis that the loss of Δψm as an early cellular event in response to apoptotic stimuli plays a key role in launching the mitochondria-mediated apoptosis pathway [43]. Bcl-2 family can affect and regulate the mitochondrial permeability and play critical roles in modulating mitochondria-mediated apoptosis [44, 45]. Hence, the balance between pro-apoptotic proteins (Bax, Bad, Bid, and Bim) and anti-apoptotic proteins (Bcl-2, Bcl-xL, Mcl-1, and Bcl-w) ultimately decides the fate of the cells [46]. Our results revealed that high glucose-induced apoptosis involved the unbalance of Bcl-2 family protein expression, whereas pretreatment with DSePA significantly inhibited the downregulation of Bcl-xL and Bcl-2. The findings above suggested that DSePA blocks high glucose-induced mitochondrial dysfunction through balance of Bcl-2 family expression.
Nerve dysfunction in diabetes is associated with increased oxidative stress [6]. ROS, including hydroxyl radical, hydrogen peroxide, and superoxide anion [47], all play important roles in mediating cell signaling and maintaining cell homeostasis [9, 48]. The balance of anti-antioxidant and pro-antioxidant system ultimately decides the intracellular level of ROS. Overproduced ROS is implicated in “glucose toxicity” in diabetes [3]. In fact, diabetes is typically accompanied by increased production of ROS in the onset, progression, and pathological consequences of diabetes [2, 4]. Actually, high glucose-mediated ROS accumulation was participated in the progression of various neurodegeneration, such as diabetic retinopathy [49]. Therefore, inhibition of ROS accumulation represents an important mechanism to prevent neurological disease and nerve cell injury [7]. Mitochondrial respiratory chain represents the main source of ROS [50], and ROS-mediated oxidative damage was generally accepted as the main pathogenesis in many human neurological diseases. p53, a cell cycle checkpoint protein, contributes to the preservation of genetic stability by mediating either cell cycle arrest or apoptosis in response to DNA damage [51, 52]. Activation of p53 in response to DNA damage can activate downstream signals to regulate cell apoptosis, such as Bcl-2 family proteins.
In the present study, high glucose treatment induced significant intracellular ROS accumulation and subsequently triggered PC12 cell DNA damage. The activation of DNA damage markers, including p-ATM, p-ATR, p-H2A, and p53 (Ser-15, Ser-9, Ser-392), all demonstrated this effect. ROS generation usually emerges as an early event in triggering cell apoptosis. Based on the significance of ROS, GSH (a positive ROS scavenger) was used to evaluate the role of DSePA in high glucose-induced apoptosis signal. The results indicated that GSH addition effectively prolonged the cell viability in high glucose-treated PC12 cells. Se functions in the active sites of a large number of Se-containing enzymes, such as glutathione peroxidase and thioredoxin reductase. In this study, we speculated that Se may be possibly incorporated into the peptides of Se-containing enzymes, such as glutathione peroxidase and thioredoxin reductase, which thus enhanced the antioxidant ability. Additionally, p53 siRNA supplement downregulated the expression levels of p53-inducible genes, which partially suppressed high glucose-induced cytotoxicity and apoptosis. All the results indicated that DSePA has the potential to reverse high glucose-induced apoptosis by inhibiting ROS-mediated DNA damage and p53 phosphorylation (Fig. 6).
Proposed signal pathway. High glucose directly triggered DNA damage-mediated p53 phosphorylation, disabled the MAPKs and AKT pathways, and induced PC12 cell apoptosis through induction of intracellular ROS overproduction. However, DSePA alleviated high glucose-induced dysregulation of MAPKs and AKT pathways, attenuated DNA damage-mediated p53 phosphorylation, and ultimately reversed high glucose-induced apoptosis by inhibition of ROS accumulation
Evidences have proven that ROS accumulation caused cell apoptosis involving MAPKs and AKT pathways through regulating specific phosphorylation sites [53]. Our previous studies also revealed that selenocompounds could regulate the AKT and/or ERK phosphorylation [9–11, 45]. Aberrant regulation of these two key signaling pathways was also related to the pathogenesis of diabetic neuropathy [54]. In the present study, p38 and JNK after high glucose treatment showed significant activation. However, AKT displayed continuous inactivation. Addition of specific inhibitors further confirmed their roles in high glucose-induced cytotoxicity and apoptosis in PC12 cells. These results all demonstrated that MAPKs and AKT pathways both contributed to high glucose-induced cytotoxicity and apoptosis. As expected, DSePA markedly alleviated this dysregulation of the two pathways, indicating that DSePA can act as regulator of MAPKs and AKT pathway to suppress high glucose-induced toxicity cytotoxicity and apoptosis.
In summary, our findings revealed that DSePA has the potential to antagonize high glucose-induced cytotoxicity and apoptosis in PC12 cells by suppressing ROS-mediated DNA damage and p53 phosphorylation involving regulation of MAPKs and AKT pathways. Our findings revealed that the strategy of using DSePA could be a highly effective way in chemoprevention and chemotherapy of high glucose-mediated neurological diseases.
References
Diogo CV, Suski JM, Lebiedzinska M, Karkucinska-Wieckowska A, Wojtala A, Pronicki M, Duszynski J, Pinton P et al (2013) Cardiac mitochondrial dysfunction during hyperglycemia—the role of oxidative stress and p66Shc signaling. Int J Biochem Cell Biol 45(1):114–122
Rolo AP, Palmeira CM (2006) Diabetes and mitochondrial function: role of hyperglycemia and oxidative stress. Toxicol Appl Pharmacol 212(2):167–178
Palmeira CM, Rolo AP, Berthiaume J, Bjork JA, Wallace KB (2007) Hyperglycemia decreases mitochondrial function: the regulatory role of mitochondrial biogenesis. Toxicol Appl Pharmacol 225(2):214–220
Amaral S, Oliveira PJ, Ramalho-Santos J (2008) Diabetes and the impairment of reproductive function: possible role of mitochondria and reactive oxygen species. Curr Diabetes Rev 4(1):46–54
Wang J, Li G, Wang Z, Zhang X, Yao L, Wang F, Liu S, Yin J et al (2012) High glucose-induced expression of inflammatory cytokines and reactive oxygen species in cultured astrocytes. Neuroscience 202:58–68
van Dam PS, van Asbeck BS, Bravenboer B, van Oirschot JF, Gispen WH, Marx JJ (1998) Nerve function and oxidative stress in diabetic and vitamin E-deficient rats. Free Radic Biol Med 24(1):18–26
Singh JN, Jain G, Sharma SS (2013) In vitro hyperglycemia enhances sodium currents in dorsal root ganglion neurons: an effect attenuated by carbamazepine. Neuroscience 232:64–73
Zou Y, Zhao T, Mao G, Zhang M, Zheng D, Feng W, Wang W, Wu X et al (2014) Isolation, purification and characterisation of selenium-containing polysaccharides and proteins in selenium-enriched Radix puerariae. J Sci Food Agric 94(2):349–358
Fan C, Zheng W, Fu X, Li X, Wong YS, Chen T (2014) Strategy to enhance the therapeutic effect of doxorubicin in human hepatocellular carcinoma by selenocystine, a synergistic agent that regulates the ROS-mediated signaling. Oncotarget 5(9):2853–2863
Fan C, Zheng W, Fu X, Li X, Wong YS, Chen T (2014) Enhancement of auranofin-induced lung cancer cell apoptosis by selenocystine, a natural inhibitor of TrxR1 in vitro and in vivo. Cell Death Dis 5:e1191
Fan C, Chen J, Wang Y, Wong YS, Zhang Y, Zheng W, Cao W, Chen T (2013) Selenocystine potentiates cancer cell apoptosis induced by 5-fluorouracil by triggering reactive oxygen species-mediated DNA damage and inactivation of the ERK pathway. Free Radic Biol Med 65:305–316
Pillai R, Uyehara-Lock JH, Bellinger FP (2014) Selenium and selenoprotein function in brain disorders. IUBMB Life 66(4):229–239
Ozbal S, Erbil G, Kocdor H, Tugyan K, Pekcetin C, Ozogul C (2008) The effects of selenium against cerebral ischemia-reperfusion injury in rats. Neurosci Lett 438(3):265–269
Bellinger FP, Raman AV, Reeves MA, Berry MJ (2009) Regulation and function of selenoproteins in human disease. Biochem J 422(1):11–22
Kunwar A, Bag PP, Chattopadhyay S, Jain VK, Priyadarsini KI (2011) Anti-apoptotic, anti-inflammatory, and immunomodulatory activities of 3,3′-diselenodipropionic acid in mice exposed to whole body gamma-radiation. Arch Toxicol 85(11):1395–1405
Kunwar A, Bansal P, Kumar SJ, Bag PP, Paul P, Reddy ND, Kumbhare LB, Jain VK et al (2010) In vivo radioprotection studies of 3,3′-diselenodipropionic acid, a selenocystine derivative. Free Radic Biol Med 48(3):399–410
Cao W, Li X, Zheng S, Zheng W, Wong YS, Chen T (2014) Selenocysteine derivative overcomes TRAIL resistance in melanoma cells: evidence for ROS-dependent synergism and signaling crosstalk. Oncotarget 5(17):7431–7445
Yagami T, Yamamoto Y, Koma H (2014) The role of secretory phospholipase A(2) in the central nervous system and neurological diseases. Mol Neurobiol 49(2):863–876
Cho SW, Park JS, Heo HJ, Park SW, Song S, Kim I, Han YM, Yamashita JK et al (2014) Dual modulation of the mitochondrial permeability transition pore and redox signaling synergistically promotes cardiomyocyte differentiation from pluripotent stem cells. J Am Heart Assoc 3(2):e000693
Bove J, Martinez-Vicente M, Dehay B, Perier C, Recasens A, Bombrun A, Antonsson B, Vila M (2014) BAX channel activity mediates lysosomal disruption linked to Parkinson disease. Autophagy 10(5):889–900
Gomez-Crisostomo NP, Lopez-Marure R, Zapata E, Zazueta C, Martinez-Abundis E (2013) Bax induces cytochrome c release by multiple mechanisms in mitochondria from MCF7 cells. J Bioenerg Biomembr 45(5):441–448
Simonishvili S, Jain MR, Li H, Levison SW, Wood TL (2013) Identification of Bax-interacting proteins in oligodendrocyte progenitors during glutamate excitotoxicity and perinatal hypoxia-ischemia. ASN Neuro 5(5):e00131
Liu MH, Yuan C, He J, Tan TP, Wu SJ, Fu HY, Liu J, Yu S et al (2014) Resveratrol protects PC12 cells from high glucose-induced neurotoxicity via PI3K/Akt/FoxO3a pathway. Cell Mol Neurobiol 35:513–522
Chen T, Wong YS (2008) Selenocystine induces apoptosis of A375 human melanoma cells by activating ROS-mediated mitochondrial pathway and p53 phosphorylation. Cell Mol Life Sci 65(17):2763–2775
Park JH, Lee SW, Yang SW, Yoo HM, Park JM, Seong MW, Ka SH, Oh KH et al (2014) Modification of DBC1 by SUMO2/3 is crucial for p53-mediated apoptosis in response to DNA damage. Nat Commun 5:5483
Coulpier M, Anders J, Ibanez CF (2002) Coordinated activation of autophosphorylation sites in the RET receptor tyrosine kinase: importance of tyrosine 1062 for GDNF mediated neuronal differentiation and survival. J Biol Chem 277(3):1991–1999
Pitts MW, Byrns CN, Ogawa-Wong AN, Kremer P, Berry MJ (2014) Selenoproteins in nervous system development and function. Biol Trace Elem Res 161(3):231–245
Bellinger FP, He QP, Bellinger MT, Lin Y, Raman AV, White LR, Berry MJ (2008) Association of selenoprotein p with Alzheimer’s pathology in human cortex. J Alzheimers Dis 15(3):465–472
Shahar A, Patel KV, Semba RD, Bandinelli S, Shahar DR, Ferrucci L, Guralnik JM (2010) Plasma selenium is positively related to performance in neurological tasks assessing coordination and motor speed. Mov Disord 25(12):1909–1915
Mousavi SH, Tayarani NZ, Parsaee H (2010) Protective effect of saffron extract and crocin on reactive oxygen species-mediated high glucose-induced toxicity in PC12 cells. Cell Mol Neurobiol 30(2):185–191
Eslami H, Sharifi AM, Rahimi H, Rahati M (2014) Protective effect of telmisartan against oxidative damage induced by high glucose in neuronal PC12 cell. Neurosci Lett 558:31–36
Yuan J, Huang G, Xiao Z, Lin L, Han T (2013) Overexpression of beta-NGF promotes differentiation of bone marrow mesenchymal stem cells into neurons through regulation of AKT and MAPK pathway. Mol Cell Biochem 383(1-2):201–211
Wu J, Jiang H, Luo S, Zhang M, Zhang Y, Sun F, Huang S, Li H (2013) Caspase-mediated cleavage of C53/LZAP protein causes abnormal microtubule bundling and rupture of the nuclear envelope. Cell Res 23(5):691–704
Xing S, Zhang J, Dang C, Liu G, Zhang Y, Li J, Fan Y, Pei Z et al (2014) Cerebrolysin reduces amyloid-beta deposits, apoptosis and autophagy in the thalamus and improves functional recovery after cortical infarction. J Neurol Sci 337(1-2):104–111
Vandegriff KD, Malavalli A, Lohman J, Young MA, Terraneo L, Virgili E, Bianciardi P, Caretti A et al (2014) Impact of acellular hemoglobin-based oxygen carriers on brain apoptosis in rats. Transfusion 54(8):2045–2054
Wu Q, Tang ZH, Peng J, Liao L, Pan LH, Wu CY, Jiang ZS, Wang GX et al (2014) The dual behavior of PCSK9 in the regulation of apoptosis is crucial in Alzheimer’s disease progression (Review). Biomed Rep 2(2):167–171
Kim SY, Shim MS, Kim KY, Weinreb RN, Wheeler LA, Ju WK (2014) Inhibition of cyclophilin D by cyclosporin A promotes retinal ganglion cell survival by preventing mitochondrial alteration in ischemic injury. Cell Death Dis 5:e1105
Hou Y, Ghosh P, Wan R, Ouyang X, Cheng H, Mattson MP, Cheng A (2014) Permeability transition pore-mediated mitochondrial superoxide flashes mediate an early inhibitory effect of amyloid beta1-42 on neural progenitor cell proliferation. Neurobiol Aging 35(5):975–989
Li DW, Yao M, Dong YH, Tang MN, Chen W, Li GR, Sun BQ (2014) Guanosine exerts neuroprotective effects by reversing mitochondrial dysfunction in a cellular model of Parkinson’s disease. Int J Mol Med 34(5):1358–1364
Li D, Liu M, Tao TQ, Song DD, Liu XH, Shi DZ (2014) Panax quinquefolium saponin attenuates cardiomyocyte apoptosis and opening of the mitochondrial permeability transition pore in a rat model of ischemia/reperfusion. Cell Physiol Biochem 34(4):1413–1426
Gu W, Hou X, Zhou H, Li C (2014) Protective effect of shen-fu injection on neuronal mitochondrial function in a porcine model of prolonged cardiac arrest. Evid Based Complement Alternat Med 2014:523847
Li J, Yu W, Li XT, Qi SH, Li B (2014) The effects of propofol on mitochondrial dysfunction following focal cerebral ischemia-reperfusion in rats. Neuropharmacology 77:358–368
Ge R, Ma WH, Li YL, Li QS (2013) Apoptosis induced neurotoxicity of Di-n-butyl-di-(4-chlorobenzohydroxamato) Tin (IV) via mitochondria-mediated pathway in PC12 cells. Toxicol In Vitro 27(1):92–102
Jung SY, Kim DY, Yune TY, Shin DH, Baek SB, Kim CJ (2014) Treadmill exercise reduces spinal cord injury-induced apoptosis by activating the PI3K/Akt pathway in rats. Exp Ther Med 7(3):587–593
Goncalves AC, Barbosa-Ribeiro A, Alves V, Silva T, Sarmento-Ribeiro AB (2013) Selenium compounds induced ROS-dependent apoptosis in myelodysplasia cells. Biol Trace Elem Res 154(3):440–447
Wang Y, Wu Y, Luo K, Liu Y, Zhou M, Yan S, Shi H, Cai Y (2013) The protective effects of selenium on cadmium-induced oxidative stress and apoptosis via mitochondria pathway in mice kidney. Food Chem Toxicol 58:61–67
Sun H, Leng T, Zeng Z, Gao X, Inoue K, Xiong ZG (2013) Role of TRPM7 channels in hyperglycemia-mediated injury of vascular endothelial cells. PLoS One 8(11):e79540
van Veen S, Sorensen DM, Holemans T, Holen HW, Palmgren MG, Vangheluwe P Cellular function and pathological role of ATP13A2 and related P-type transport ATPases in Parkinson’s disease and other neurological disorders. Front Mol Neurosci 7:48
Gaspar JM, Martins A, Cruz R, Rodrigues CM, Ambrosio AF, Santiago AR (2013) Tauroursodeoxycholic acid protects retinal neural cells from cell death induced by prolonged exposure to elevated glucose. Neuroscience 253:380–388
Odinokova IV, Sung KF, Mareninova OA, Hermann K, Evtodienko Y, Andreyev A, Gukovsky I, Gukovskaya AS (2009) Mechanisms regulating cytochrome c release in pancreatic mitochondria. Gut 58(3):431–442
Renaud J, Bournival J, Zottig X, Martinoli MG (2014) Resveratrol protects DAergic PC12 cells from high glucose-induced oxidative stress and apoptosis: effect on p53 and GRP75 localization. Neurotox Res 25(1):110–123
Guan L, Huang F, Li Z, Han B, Jiang Q, Ren Y, Yang Y, Xu C (2008) P53 transcription-independent activity mediates selenite-induced acute promyelocytic leukemia NB4 cell apoptosis. BMB Rep 41(10):745–750
Aminzadeh A, Dehpour AR, Safa M, Mirzamohammadi S, Sharifi AM (2014) Investigating the protective effect of lithium against high glucose-induced neurotoxicity in PC12 cells: involvements of ROS, JNK and P38 MAPKs, and apoptotic mitochondria pathway. Cell Mol Neurobiol 34(8):1143–1150
Li Q, Guo HC, Maslov LN, Qiao XW, Zhou JJ, Zhang Y (2014) Mitochondrial permeability transition pore plays a role in the cardioprotection of CB2 receptor against ischemia-reperfusion injury. Can J Physiol Pharmacol 92(3):205–214
Acknowledgments
The study was supported by the National Natural Science Foundation of China no. 81471212, 81271275, 81070947, and 30770759 to B.-L. Sun and no. 81301018 to Z.-Y Zhang; and Natural Science Foundation of Shandong no. ZR2012HZ006 to B.-L. Sun, no. ZR2015HQ009 to C.-D. Fan, and no. ZR2015PH003 to X.-Y. Fu.
Conflict of Interest
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Kun Wang and Xiao-yan Fu contributed equally to this work.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 584 kb)
Rights and permissions
About this article
Cite this article
Wang, K., Fu, Xy., Fu, Xt. et al. DSePA Antagonizes High Glucose-Induced Neurotoxicity: Evidences for DNA Damage-Mediated p53 Phosphorylation and MAPKs and AKT Pathways. Mol Neurobiol 53, 4363–4374 (2016). https://doi.org/10.1007/s12035-015-9373-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9373-1