Abstract
First described in the 1800s, glioblastoma multiforme (GBM), a class IV neoplasm with astrocytic differentiation, as per the revised 2016 World Health Organization classification of tumors of the central nervous system (CNS) is the most common malignant tumor of the CNS. GBM has an extremely wide set of alterations, both genetic and epigenetic, which yield a great number of mutation subgroups, some of which have an established role in independent patient survival and treatment response. All of those components not only represent a closed cycle but are also relevant to the tumor biological behavior and resistance to treatment as they form the pathobiological behavior and clinical course. The presence of different triggering mutations on the background of the presence of key mutations in the GBM stem cells (GBMsc) further separates GBM as primary arising de novo from neural stem cell precursors developing into GBMsc and secondary, by means of aggregated mutations. Some of the change in cellular biology in GBM can be observed via light microscope as they form the cellular and tissue hallmarks of the condition. Changes in genetic information, resulting in alteration, suppression and expression of genes compared to their physiological levels in healthy astrocytes lead to not only cellular, but also extracellular matrix reorganization. These changes result in a multiform number of micromorphological and purely immunological/biochemical forms. Therefore, in the twenty-first century the term multiforme, previously outcast from nomenclatures, has gained new popularity on the background of genotypic diversity in this neoplastic entry.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glioblastoma multiforme (GBM), a class IV neoplasm with astrocytic differentiation, as per the revised 2016 and prior World Health Organization (WHO) classification of tumors of the central nervous system (CNS), is the most common malignant tumor of the CNS, being even more commonly encountered than CNS metastasis (Fig. 1) [1,2,3,4]. Clinically, GBM is an entry encountered in its late stages of biological evolution, requiring intensive multidisciplinary diagnostic and treatment strategies. Even so, the survival prognosis of patients with GBM is one of the dimmest, as the survival rate is one of the worst encountered in modern day oncology [5,6,7,8].
Cellular contrast between healthy brain tissue and GBM. a Healthy brain tissue, H&E, original magnification ×400. b Healthy astrocytes, IHC stain with GFAP, original magnification ×400. c Hypercellularity and cellular atypism of GBM, H&E, original magnification ×400. d Neoplastic astrocytes of GBM, IHC stain with GFAP, original magnification ×400
First described in 1800s, GBM is a unique entry into cancer pathology, as it behaves in a unique way bringing its biological behavior closer to extracranial tumors than to intracranial [9, 10]. Unlike other neoplastic entries, where in the past 50 years the prognosis and quality of life have increased drastically due to investigations into cellular and tumor biology, such investigations into GBM have opened up more questions than they have answered [5, 11,12,13].
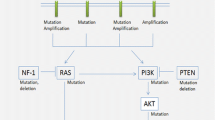
GBM has an extremely wide set of alterations, both genetic and epigenetic, which yield a great number of mutation subgroups (MSG), some of which have an established role in independent patient survival and treatment response (Fig. 2) [10, 14,15,16,17,18]. However, most of the encountered mutations either have a limited, disputed or unestablished role in patient survival. Hence, in the present day the term multiforme, originally introduced due to the multiform appearance of tumors cells within the same biopsy sample and in-between samples of the same overall entry, has widely been reintroduced due to the genotypical multiformity of this neoplastic entry [19, 20].
A subset of mutations, most of which are widely unidentified or their impact on diagnosis has yet been unestablished, have widely been forgotten, placing a gap in the diagnostic process [1, 16, 21,22,23]. Only a few studies focus on the different phenotypic appearance of the varying genotypic subgroups of GBM.
Alterations in basic cellular biology
Based on the present genetic and epigenetic changes, there are substantial mutations, leading to cytoplasmic and extracellular matrix reorganization. These changes present the morphological tissue hallmarks—monstrous cells, based on the multiformity of the genetic and epigenetic alterations within the cells of the same tumor sample, pseudopalicadic necrosis, formed both from areas of cellular death and nearby cells migrating away from the necrotic bead, and neovascular pseudoglumerlar formations, formed from the released growth factors from the tumor cell, which also auto-stimulate the cells themselves (Fig. 3) [9, 24].
All of these components not only represent a closed cycle but are also relevant to the tumor biological behavior and resistance to treatment as these tissue hallmarks form the pathobiological behavior and clinical course. The presence of GBM cancer stem cells (GBMsc) within the tissue sample also provides everlasting replenishing supply of new mature GBM cancer cells (GBMmc) with further mutations and treatment resistant behavior [14, 15, 25]. These GBMsc can be identified by the presence of CD24, CD44, CD133 and Hes3 positivity and are highly resistant to treatment due to active mechanisms of DNA repair and self-regeneration [10, 15, 25,26,27].
The presence of different triggering mutations on the background of the presence of key mutations in the GBMsc further separates GBM as primary (pGBM) arising de novo from neural stem cell precursors (NscP) developing into GBMsc and secondary (sGBM) arising from NscP by means of aggregated mutations, different from the triggering mutations in GBMsc of pGBM [28,29,30].
These two forms of biological evolution of GBM were first identified by the father of modern pathology and the cellular theory Rudolf Virchow and nearly a century later by the most prominent researcher in the field of CNS glial tumors—Joachim Scherer, after whom the pseudopalisadic necrosis has trivially been named Scherer formations (Fig. 3) [9, 19, 20, 24, 31, 32]. Both of these prominent researchers postulated the biological behavior of GBM based on their observations of both biopsy and autopsy samples and clinical observation of patients.
Only recently with the advances of molecular biology, pathology and genetics on the background of multidisciplinary approach with neurologists and neurosurgeons have we been able to understand the train of thought of these prominent figures.
Alterations in cellular biology with relevance to pathological verification
Some of the change in cellular biology in GBMmc can be observed via light microscope as they form the cellular and tissue hallmarks of the condition. Changes in genetic information, resulting in alteration, suppression and expression of genes compared to their physiological levels in healthy astrocytes lead to not only cellular, but also extracellular matrix reorganization (Fig. 1). These features are used as the diagnostic medium, by which GBM is verified pathologically [1].
Glial fibrillary acidic protein (GFAP) is a class III intermediate cytoskeletal filament with a 50kD molecular weight, found in all astrocytes, other glial cells and some pericytes (Fig. 1). Although used as a cornerstone for the immunohistochemical (IHC) verification of CNS tumor samples, more often than not, GFAP is relied upon too much (Fig. 4). Some studies state lack of GFAP IHC expression in some GBM tumor specimens, misleading untrained neuropathologists into other diagnostic categories. Therefore, this once cornerstone of CNS tumor verification, although highly specific, is now only part of a wider testing panel. So far there has been no confirmed report of GFAP IHC negativity correlating with GBM presentation, clinical course or treatment. However, changes in GFAP coding deoxyribonucleic acid (DNA) and subsequent loss of IHC reactivity may be key to identifying new mutations in genes adjacent to the GFAP coding ones on 17q21.31 and perhaps associating with loss of heterozygosity (LOH) 17p [33, 34].
Vimentin is also a class III intermediate cytoskeletal filament with a 57kD molecular weight, found in all cells with a mesenchymal origin. Due to its wide set of tissue samples with a positive IHC reaction, Vimentin is mostly used as a positive IHC control, when verifying CNS tumor samples (Fig. 5). There, however, have been conflicting reports of GBM tumor samples losing their IHC reaction with Vimentin, while remaining GFAP positive, while on the other hand samples which have lost their GFAP IHC positivity remain Vimentin positive. This, likewise with GFAP, may, in the future, lead to the discovery of new GBM or tumor-associated mutation, adjacent to the Vimentin coding gene on 10p13 and its association with LOH 10p [34,35,36,37].
S-100 is a family of more than 21 different cytoplasmic regulatory proteins with distinctive regulatory and cell cycle functions. The most pronounced type found in glial cells and GBMmc is S-100B, an astrocyte specific marker (Fig. 6). Despite this, IHC reactions for S-100 are very unspecific, unlike GFAP, due to most commercial antibody kits being an antibody cocktail for the S-100 family altogether and S-100 family members being present in a number of tissues and tumor types, including melanoma, different types of sarcoma and histiocytoma. However, so far there have been no reports of GBM tumor samples with negative IHC expression for S-100B. Yet wieldy unresearched, S-100B is coded on 21q22.3, a locus commonly associated with epigenetic encasement in cancer stem cells [38,39,40].
The most common differential diagnosis for morphological verification of GBM, based both on its classical hallmarks and its multiform appearance, is CNS metastatic tumors, primarily of epithelial origin [3, 10]. Diagnosis is carried out predominantly with IHC, especially when there is an overlap of histological hallmarks, unspecific hallmarks or variants of GBM, especially giant cell GBM and epitheloid GBM. Two such IHC markers are the pan-keratin AE1/AE3 antibody cocktail and epithelial membrane antigen (EMA), both of whom, despite wide positivity across tissues, do not react in healthy brain tissue.
Cytokeratin (CK) AE1/AE3 is a pan-cytokeratin antibody cocktail, reacting with unspecific epitomes, preset in the protein chain of most cytokeratin filaments. Cytokeratins are a diverse group comprised of acidic (type I) and alkaline/basic (type II) intermediate cytoskeletal filaments. The AE1 fraction of the antibody cocktail detects the type I fraction, represented with the high molecular weights 10, 14, 15, 16 and the low molecular weight 19, while the AE3 fraction detects type II cytokeratins—the high molecular weights 1, 2, 3, 4, 5, 6 and the low molecular weights 7 and 8. Widely reported GBM tumor samples react positively with CK AE1/AE3, with some studies reporting an excess of 96% of GBM giving a positive IHC reaction (Fig. 7) [41,42,43]. This has given background the claim of keratin production in GBM, explained with the anaplastic cells regaining their neuroepithelial hallmarks [41]. However, since GBM originates from NscP, such dedifferentiation cannot take place. As proven by a set of studies, CK AE1/AE3 positivity is not based on the production of keratin filaments by GBMmc, but rather on the AE3 fraction of the mixture reacting with a similar epitome of another intermediate filament, highly likely being GFAP (Fig. 8) [44,45,46,47]. These claims were further supported by electrophoresis and immunoblot tests, proving that no molecules with the characteristics and molecular weight of keratin filaments were present in GBMmc reacting with CK AE1/AE3 in IHC [47].
EMA is a surface glycoprotein found on the outer cellular membrane of most epithelial cell types and some hematopoietic cells, taking place in cellular interactions. Again, widely accepted as a standard phenomenon, but yet unresearched specifically, EMA IHC positivity is yet another candidate for false IHC positivity like CK AE1/AE3, as the reaction is both weak and unspecific of the antibody (Fig. 9) [48]. There are, however, some claims that this type of reaction may not be due to antigen and epitome mimicry, such as the CK AE1/AE3 reaction, but due to slide contamination during preparation [48].
Other classical epithelial markers such as CAM5.2, CK20, CK7 and others have also been reported with positive reactions in GBMmc, although this phenomenon is much rarer when compared to CK AE1/AE3 and EMA [41, 46, 47]. Though considered falsely positive as presented in some studies, it remains widely accepted as a standard phenomenon explained by the neuroepithelial origin of glial cells. However, the immunoblot studies carried out, together with the highly unspecific reactions uncharacteristic of the antibodies, give ample field for future research and antibody refinement.
All of these alterations in the cellular biology of intermediate filament structure, rearranging and the alteration of other cytoplasmic component, inevitably contribute to the morphological changes observed in GBMmc, and different combinations may even attribute to the widely diverse morphological variants.
Uncharacteristic of other CNS and ICTs, GBM is a tumor that is reportedly able to metastasize. Although rare, this phenomenon gives rise to several very important questions about the cellular biology processes diverging GBM from these other tumors and the factors contributing to this rare event [49,50,51,52,53]. Furthermore, there are two distinct patterns of GBM metastasis—metastasis within the CNS, predominantly spinal cord and contralateral hemisphere prior to butterfly pattern formation and metastasis outside of the CNS, observed both after subsequent craniotomies for treatment and prior to them [54,55,56]. CNS metastasis can be attributed to both pseudopodic migration of GBMsc and their dissemination through the cerebrospinal fluid, while extracranial metastases are a yet widely unexplained phenomenon attributed both to the damaging of the blood–brain barrier and immature tumor blood vessels, tissue trauma due to surgical and non-surgical intervention and the presence of newly discovered lymph vessels in the CNS. These phenomena give rise to the discussion whether GBM naturally has the ability to metastasize, and these events are rare and far in between due to the short patient survival period, or are they triggered by a rare specific, yet unidentified mutation.
A key fact of notice is the presence of GBM outside of the limits of the CNS. Paradoxically this phenomenon can occur in teratomas, predominantly in the mediastinal space, although occurrences in ovarian and testicular teratoma are also common [57, 58]. This phenomenon develops on the background of NscP, as reportedly up to 30% of teratomas have neural tissue as their component [59, 60]. Further worth noticing is that most malignant tumors developing on the background of teratomas develop on the background of already malignant immature teratomas, while GBM can develop from mature teratomas, further underlining the value of GBMsc arising from NscP [58].
Specific alterations in cellular biology
Complementary, however, to the great variety of genetic changes with a visible morphological or IHC manifestation, there are a greater number of micromorphological and purely immunological/biochemical forms. Therefore, in the twenty-first century the term multiforme, previously outcast from nomenclatures, has gained new popularity on the background of genotypic diversity in this neoplastic entry [61].
These genetic multiformities are not observed in unison, but form distinct MSG, which in modern times are key, outlining not only the biological behavior and aggression of the tumor, but also the response to different treatment strategies. MSG are also a pivotal point in the development of new diagnostic and curative modalities for GBM.
Based on the current WHO classifications of tumors of the CNS, mutations with an integrated treatment include isocitrate dehydrogenases mutations (IDH) and the presence of an MGMT mutation, purely genetic or epigenetic, as IDH status is an independent prognostic factor and MGMT status is representative of treatment response to Temozolomide [1].
The MGMT mutation status on its own has no value comparative to clinical manifestation and progression [16, 23]. However, when MGMT levels in GBMmc are decreased, this makes them more susceptible to DNA alkalization and therefore therapeutic eradication. The already aforementioned alkalizing agent Temozolomide can actively alkylate the guanin portions of DNA at the N-7 and O-6 portions, which in turn promotes cell death, allowing for a median postoperative survival amounting to more than 13 months [8, 21].
Another key finding, not considered a mutation as it is a physiological component of cellular division cycle, is the percentage of positive nuclei for Ki-67 (MIB-1) [6, 62,63,64]. This finding has recently lost its value due to conflicting reports on its possibility to predict tumor malignancy class, patient survival and response to therapy, unlike in some other oncological entries [62, 65]. However, as a component of the physiological process of cell division, Ki-67, although not key, is a component of cellular biology inevitably impacted by other mutations in GBMmc and GBMsc.
Considered key cellular alterations in modern times, micro-RNAs (miR) have provided another multiform background to GBM [10, 66, 67]. Currently there are more than 300 miR with either a confirmed or disputed role in GBM development, progression, GBMsc and GBMmc resistance to treatment of disease progression [10].
Currently, the best studied miR with a role in GBM oncogenesis is miR-21 [10, 68,69,70]. Its associated overexpression in GBM tumor samples increases with the anaplasticity of GBMmc and is a negative prognostic factor. Increased levels of miR-21 lead to overexpression of ANP32A, HNRPK, LRRFIR1, PDCD4, PTEN, SMARCA4, SPRY2 and TAp63, thus resulting in an increase in caspase levels, which themselves decrease apoptotic activity pathways in GBMmc [70]. miR-21 also aids the invasion of surrounding tissues by suppressing TIMP-3 and RECK, without changing the levels of matrix metalloproteases. Missense miR-21 transfection in laboratory conditions, in turn, leads to increased sensitivity to radio and chemotherapeutics.
Interestingly, however, on the background of so many disrupted processes and alteration in the cell biology of GBMmc, the autocrine and paracrine processes of cellular stimulation remain intact, that is purely in function, however, since all of them seem to be overstimulated in either autocrine overproduction of ligands, overexpression of receptors or overreaction when stimulated. Remarkably GBM is perhaps the only neoplastic entry in which there is not a single downregulated pathway for proliferation.
Further underlining the importance of the growth factor systems is the fact that when NscP are overstimulated with growth factor, specifically PDGF, they develop into GBM-like tumors, even after stimulation is withdrawn and the samples are implanted in experimental animals [71]. Some studies even go so far as to suggest that growth factor overstimulation is the reason for development of GBM and suggest specific genotypes arising in different areas of the CNS, depending on the growth factor presented in these areas. These claims, however, seem to be not representative, as the recently suggested molecular classifications of GBM do not report a corresponding subtype from a specific area of the CNS [10, 18, 72].
Individual specific alterations in cellular biology
GBM is observed across all age groups, including prenatally, with a spike in the age group 20–35 and an even more pronoun spike in the age groups above 60 years of age [3, 4, 73].
Often described as independent risk factors, age, gender and race are currently up for debate. Historically, it has been established that the male-to-female ratio in GBM is between 1.3:1 and 2:1 depending on the population [3, 74, 75]. Another recently challenged statement is that of ethnicity. While some statistical reports give data for wide incidence gap between different ethnicities in the same population, other studies give nearly identical figures in different, ethnically diverse and contrasting populations widely isolated from one another. It would seem that ethnicity itself is not a risk factor, as mush as yet unidentified life factors for different populations [3, 4, 76]. Irradiation to the CNS has also been described as a risk factor for development of GBM, although low doses of environmental radiation seem to be of no effect, while direct irradiation to the CNS is a severe risk factor for rapid development and progression of the condition [77].
More well-established risk factors are the presence of genetic syndromes such as neurofibromatosis, von Hippel-Lindo disease and others, which are closely associated with increased risk for many other neural and non-neural benign and malignant tumors [78, 79].
A directive for future research is the effects of glucose metabolism on the development and progression of GBM as well as its effect on survival and therapy [80]. GBM is a yet unresearched entry and should yield some interesting research both based on data from other neoplastic entries and the unique metabolism of glucose in the CNS and the specifics of the blood–brain barrier [81,82,83,84].
Conclusion
Although the triggering mutation(s) in gliomagenesis are still unidentified and the relevant mutations to treatment strategies are still few and yield limited results, the progress in the understandings of disruption of cell biology in the development and progression of this condition yield an ever-narrowing field toward the key mutations. While current cytoreduction by means of surgery is still key not only to the diagnostic process, but also to patient survival and quality of life when optimal with limited damage to nearby structures and optimized therapy to the MSG, patient survival and quality of life are still among the worst encountered in oncology.
References
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, et al. The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol. 2016;131(6):803–20.
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, Jouvet A, et al. The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol. 2007;114(2):97–109.
Stoyanov GS, Dzhenkov DL, Kitanova M, Ghenev P, Tonchev AB. Demographics and incidence of histologically confirmed intracranial tumors: a five-year, two-center prospective study. Cureus. 2017;9(7):e1476.
de Carvalho LEW, Sarraf JS, Semblano AAP, Moreira MA, de Lemos MN, de Mello VJ, et al. Central nervous system tumours profile at a referral center in the Brazilian Amazon region, 1997–2014. PLoS One. 2017;12(4):e0174439.
Yeung JT, Hamilton RL, Ohnishi K, Ikeura M, Potter DM, Nikiforova MN, et al. LOH in the HLA class I region at 6p21 is associated with shorter survival in newly diagnosed adult glioblastoma. Clin Cancer Res. 2013;19(7):1816–26.
Stoyanov GS, Dzhenkov DL, Kitanova M, Donev IS, Ghenev P. Correlation Between Ki-67 Index, World Health Organization grade and patient survival in glial tumors with astrocytic differentiation. Cureus. 2017;9(6):e1396.
Krex D, Klink B, Hartmann C, Von Deimling A, Pietsch T, Simon M, et al. Long-term survival with glioblastoma multiforme. Brain. 2007;130(10):2596–606.
Darefsky AS, King JT, Dubrow R. Adult glioblastoma multiforme survival in the temozolomide era: a population-based analysis of surveillance, epidemiology, and end results registries. Cancer. 2012;118(8):2163–72.
Scherer HJ. A critical review: the pathology of cerebral gliomas. J Neurol Neurosurg Psychiatry. 1940;3(2):147–77.
Stoyanov GS, Dzhenkov DL. On the concepts and history of glioblastoma multiforme—morphology, genetics and epigenetics. Folia Med (Plovdiv). 2017; online ahead of print.
Nakayama K, Nakayama N, Wang TL, Shih IM. NAC-1 controls cell growth and survival by repressing transcription of Gadd45GIP1, a candidate tumor suppressor. Cancer Res. 2007;67(17):8058–64.
Costa PM, Cardoso AL, Mano M, de Lima MCP. MicroRNAs in glioblastoma: role in pathogenesis and opportunities for targeted therapies. CNS Neurol Disord Drug Targets. 2015;14(2):222–38.
Kwak Y, Kim SI, Park CK, Paek SH, Lee ST, Park SH. C-MET overexpression and amplification in gliomas. Int J Clin Exp Pathol. 2015;8(11):14932–8.
De Almeida Sassi F, Lunardi Brunetto A, Schwartsmann G, Roesler R, Abujamra AL. Glioma revisited: from neurogenesis and cancer stem cells to the epigenetic regulation of the niche. J Oncol. 2012;2012:1–20.
Safa AR, Saadatzadeh MR, Cohen-Gadol AA, Pollok KE, Bijangi-Vishehsaraei K. Glioblastoma stem cells (GSCs) epigenetic plasticity and interconversion between differentiated non-GSCs and GSCs. Genes Dis. 2015;2(2):152–63.
Zhang J, Yang JH, Quan J, Kang X, Wang HJ, Dai PG. Identification of MGMT promoter methylation sites correlating with gene expression and IDH1 mutation in gliomas. Tumor Biol. 2016;37(10):13571–9.
Stancheva G, Goranova T, Laleva M, Kamenova M, Mitkova A, Velinov N, et al. IDH1/IDH2 but not TP53 mutations predict prognosis in Bulgarian glioblastoma patients. Biomed Res Int. 2014;2014:654727.
Crespo I, Vital AL, Nieto AB, Rebelo O, Tão H, Lopes MC, et al. Detailed characterization of alterations of chromosomes 7, 9, and 10 in glioblastomas as assessed by single-nucleotide polymorphism arrays. J Mol Diagn. 2011;13(6):634–47.
Kettenmann H, Verkhratsky A. Neuroglia: the 150 years after. Trends Neurosci. 2008;31(12):653–9.
De Angelis LM, Mellinghoff IK. Virchow 2011 or how to ID(H) human glioblastoma. J Clin Oncol. 2011;29(34):4473–4.
Yang P, Zhang W, Wang Y, Peng XJ, Chen B, Qiu X, et al. IDH mutation and MGMT promoter methylation in glioblastoma: results of a prospective registry. Oncotarget. 2015;6(38):40896.
Kramář F, Minárik M, Benešová L, Halková T, Netuka D, Bradáč O, et al. IDH1/2 mutation and MGMT promoter methylation—the relevant survival predictors in Czech patients with brain Gliomas. Folia Biol (Czech Republic). 2016;62(5):194–202.
Combs SE, Rieken S, Wick W, Abdollahi A, von Deimling A, Debus J, et al. Prognostic significance of IDH-1 and MGMT in patients with glioblastoma: One step forward, and one step back? Radiat Oncol. 2011;6(1):115.
Virchow R. Cellular pathology as based upon physiological and pathological histology; twenty lectures delivered in the Pathological Institute of Berlin during the months of February, March, and April, 1858. New York: Robert M. De Witt; 1860.
Liu G, Yuan X, Zeng Z, Tunici P, Ng H, Abdulkadir IR, et al. Analysis of gene expression and chemoresistance of CD133+ cancer stem cells in glioblastoma. Mol Cancer. 2006;5(1):67.
Altaner C. Glioblastoma and stem cells—minireview. Neoplasma. 2008;55(5):369–74.
Park DM, Jung J, Masjkur J, Makrogkikas S, Ebermann D, Saha S, et al. Hes3 regulates cell number in cultures from glioblastoma multiforme with stem cell characteristics. Sci Rep. 2013;3(1):1095.
Ohgaki H, Kleihues P. Genetic pathways to primary and secondary glioblastoma. Am J Pathol. 2007;170(5):1445–53.
Fujisawa H, Reis RM, Nakamura M, Colella S, Yonekawa Y, Kleihues P, et al. Loss of heterozygosity on chromosome 10 is more extensive in primary (de novo) than in secondary glioblastomas. Lab Investig. 2000;80(1):65–72.
Nakamura M, Yang F, Fujisawa H, Yonekawa Y, Kleihues P, Ohgaki H. Loss of heterozygosity on chromosome 19 in secondary glioblastomas. J Neuropathol Exp Neurol. 2000;59(6):539–43.
Peiffer J, Kleihues P. Hans-Joachim Scherer (1906–1945), pioneer in glioma research. Brain Pathol. 1999;9(2):241–5.
Scherer M. Some comments on the paper: Hans-Joachim Scherer (1906–1945), pioneer in glioma research. Brain Pathol. 2013;23(4):485–7.
Gene: GFAP (ENSG00000131095)—Summary—Homo sapiens—Ensembl genome browser 91. http://www.ensembl.org/Homo_sapiens/Gene/Summary?g=ENSG00000131095;r=17:44903161-44916937.
Zainuddin N, Jaafar H, Isa MN, Abdullah JM. Loss of heterozygosity on chromosomes 10q, 9p, 17p and 13q in Malays with malignant glioma. Neurol Res. 2004;26(1):88–92.
Gene: VIM (ENSG00000026025)—Summary—Homo sapiens—Ensembl genome browser 91. http://www.ensembl.org/Homo_sapiens/Gene/Summary?g=ENSG00000026025;r=10:17228259-17237593.
Kakkar A, Suri V, Jha P, Srivastava A, Sharma V, Pathak P, et al. Loss of heterozygosity on chromosome 10q in glioblastomas, and its association with other genetic alterations and survival in Indian patients. Neurol India. 2011;59(2):254–61.
Kuga D, Mizoguchi M, Guan Y, Hata N, Yoshimoto K, Shono T, et al. Prevalence of copy-number neutral LOH in glioblastomas revealed by genomewide analysis of laser-microdissected tissues. Neuro Oncol. 2008;10(6):995–1003.
Gene: S100B (ENSG00000160307)—Summary—Homo sapiens—Ensembl genome browser 91. Available from: http://www.ensembl.org/Homo_sapiens/Gene/Summary?g=ENSG00000160307;r=21:46598962-46605208.
Mathews LA, Crea F, Farrar WL. Epigenetic gene regulation in stem cells and correlation to cancer. Differentiation. 2009;78(1):1–17.
Guo Y, Su ZY, Kong ANT. Current perspectives on epigenetic modifications by dietary chemopreventive and herbal phytochemicals. Curr Pharmacol Rep. 2015;1(4):245–57.
Terada T. Expression of cytokeratins in glioblastoma multiforme. Pathol Oncol Res. 2015;21(3):817–9.
Goswami C, Chatterjee U, Sen S, Chatterjee S, Sarkar S. Expression of cytokeratins in gliomas. Indian J Pathol Microbiol. 2007;50(3):478–81.
Cosgrove MM, Rich KA, Kunin SA, Sherrod AE, Martin SE. Keratin intermediate filament expression in astrocytic neoplasms: analysis by immunocytochemistry, western blot, and northern hybridization. Mod Pathol. 1993;6(3):342–7.
Stoyanov GS, Dzhenkov D, Ghenev P. Cytokeratin AE1/AE3 mimicry in Glioblastoma. Scr Sci Medica. 2017;49(1):47–52.
Stoyanov G, Kitanova M, Dzhenkov D, Ghenev P. The diagnostic dilemma of epithelial marker expression in glioblastoma. Pathol Oncol Res. 2017; online ahead of print.
Oh D, Prayson RA. Evaluation of epithelial and keratin markers in glioblastoma multiforme: an immunohistochemical study. Arch Pathol Lab Med. 1999;123(10):917–20.
Kriho VK, Yang HY, Moskal JR, Skalli O. Keratin expression in astrocytomas: an immunofluorescent and biochemical reassessment. Virchows Arch. 1997;431(2):139–47.
Stoyanov GS, Dzhenkov D, Ghenev P. The great imitator—EMA positive glioblastoma multiforme. Scr Sci Medica. 2017;49(1):21–5.
Moon K-S, Jung S, Lee M-C, Kim I-Y, Kim H-W, Lee J-K, et al. Metastatic glioblastoma in cervical lymph node after repeated craniotomies: report of a case with diagnosis by fine needle aspiration. J Korean Med Sci. 2004;19(6):911–4.
Forsyth PA, Laing TD, Gibson AW, Rewcastle NB, Brasher P, Sutherland G, et al. High levels of gelatinase-B and active gelatinase-A in metastatic glioblastoma. J Neurooncol. 1998;36(1):21–9.
Zappia JJ, Wolf GT. Cervical metastatic glioblastoma multiforme. Arch Otolaryngol Head Neck Surg. 1992;118(7):755–6.
Kalokhe G, Grimm SA, Chandler JP, Helenowski I, Rademaker A, Raizer JJ. Metastatic glioblastoma: case presentations and a review of the literature. J Neurooncol. 2012;107(1):21–7.
González Cámpora R, Otal Salaverri C, Vázquez Ramirez F, Salguero Villadiego M, Galera Davidson H. Metastatic glioblastoma multiforme in cervical lymph nodes. Report of a case with diagnosis by fine needle aspiration. Acta Cytol. 1993;37(6):938–42.
Agrawal A. Butterfly glioma of the corpus callosum. J Cancer Res Ther. 2009;5(1):43–5.
Dziurzynski K, Blas-Boria D, Suki D, Cahill DP, Prabhu SS, Puduvalli V, et al. Butterfly glioblastomas: a retrospective review and qualitative assessment of outcomes. J Neurooncol. 2012;109(3):555–63.
Stark AM, Nabavi A, Mehdorn HM, Blömer U. Glioblastoma multiforme—report of 267 cases treated at a single institution. Surg Neurol. 2005;63(2):162–9.
Trabelsi A, Conan-Charlet V, Lhomme C, Morice P, Duvillard P, Sabourin JC. Peritoneal glioblastoma: recurrence of ovarian immature teratoma (report of a case). Ann Pathol. 2002;22(2):130–3.
Yadav A, Lellouch-Tubiana A, Fournet JC, Quazza JE, Kalifa C, Sainte-Rose C, et al. Glioblastoma multiforme in a mature ovarian teratoma with recurring brain tumours. Histopathology. 1999;35(2):170–3.
Thompson S, Stern PL, Webb M, Walsh FS, Engstrom W, Evans EP, et al. Cloned human teratoma cells differentiate into neuron-like cells and other cell types in retinoic acid. J Cell Sci. 1984;72(1):37–64.
Nogales FF, Aguilar D. Neural tissues in human teratomas. In: Damjanov I, Knowles BB, Solter D, editors. The human teratomas. Contemporary biomedicine, vol. 3. New York: Humana Press; 1983. p. 173–90.
Martínez R. Beyond genetics in glioma pathways: the ever-increasing crosstalk between epigenomic and genomic events. J Signal Transduct. 2012;2012:1–9.
Thangarajah F, Enninga I, Malter W, Hamacher S, Markiefka B, Richters L, et al. A retrospective analysis of Ki-67 index and its prognostic significance in over 800 primary breast cancer cases. Anticancer Res. 2017;37(4):1957–64.
Shibata T, Burger PC, Kleihues P. Ki-67 immunoperoxidase stain as marker for the histological grading of nervous system tumours. Acta Neurochir Suppl (Wien). 1988;43:103–6.
Litofsky NS, Mix TCH, Baker SP, Recht LD, Smith TW. Ki-67 (clone MIB-1) proliferation index in recurrent glial neoplasms: no prognostic significance. Surg Neurol. 1998;50(6):579–85.
Yábar A, Meléndez R, Muñoz S, Deneo H, Freire J, Domínguez V, et al. Effect of Ki-67 assessment in the distribution of breast cancer subtypes: evaluation in a cohort of Latin American patients. Mol Clin Oncol. 2017;6(4):503–9.
Sarkar SH, Ahmad A, Mittal S. The therapeutic role of microRNAs in human gliomas. In: Sarkar FH, editor. MicroRNA targeted cancer therapy. Cham: Springer International Publishing; 2014. p. 1–27.
Silber J, James CD, Hodgson JG. MicroRNAs in gliomas: small regulators of a big problem. NeuroMolecular Med. 2009;11(3):208–22.
Li S-J, Zhou J, Zhang L, Xiang W, Hu Q, He Y-Y, et al. The effect of miR-21 on SWOZ2 glioma cells and its biological mechanism. J BUON. 2017;22(2):468–73.
Zhou X, Zhang J, Jia Q, Ren Y, Wang Y, Shi L, et al. Reduction of miR-21 induces glioma cell apoptosis via activating caspase 9 and 3. Oncol Rep. 2010;24(1):195–201.
Becker Buscaglia LE, Li Y. Apoptosis and the target genes of miR-21. Chin J Cancer. 2011;30(6):371–80.
Jackson EL, Garcia-Verdugo JM, Gil-Perotin S, Roy M, Quinones-Hinojosa A, VandenBerg S, et al. PDGFRβ-positive B cells are neural stem cells in the adult SVZ that form glioma-like growths in response to increased PDGF signaling. Neuron. 2006;51(2):187–99.
Crespo I, Vital AL, Gonzalez-Tablas M, Patino MDC, Otero A, Lopes MC, et al. Molecular and genomic alterations in glioblastoma multiforme. Am J Pathol. 2015;185(7):1820–33.
Geraghty AV, Knott PD, Hanna HM. Prenatal diagnosis of fetal glioblastoma multiforme. Prenat Diagn. 1989;9(9):613–6.
Sun T, Plutynski A, Ward S, Rubin JB. An integrative view on sex differences in brain tumors. Cell Mol Life Sci. 2015;72(17):3323–42.
Ahmadloo N, Kani AA, Mohammadianpanah M, Nasrolahi H, Omidvari S, Mosalaei A, et al. Treatment outcome and prognostic factors of adult glioblastoma multiforme. J Egypt Natl Canc Inst. 2013;25(1):21–30.
Ostrom QT, Gittleman H, Liao P, Rouse C, Chen Y, Dowling J, et al. CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2007–2011. Neuro Oncol. 2014;16(suppl 4):iv1–63.
Enchev Y, Ferdinandov D, Kounin G, Encheva E, Bussarsky V. Radiation-induced gliomas following radiotherapy for craniopharyngiomas: a case report and review of the literature. Clin Neurol Neurosurg. 2009;111(7):591–6.
Abadin SS, Zoellner NL, Schaeffer M, Porcelli B, Gutmann DH, Johnson KJ. Racial/ethnic differences in pediatric brain tumor diagnoses in patients with neurofibromatosis type 1. J Pediatr. 2015;167(3):613–20.
Karajannis MA, Ferner RE. Neurofibromatosis-related tumors. Curr Opin Pediatr. 2015;27(1):26–33.
Vander Heiden MG, Cantley LC, Thompson CB. Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science. 2009;324(5930):1029–33.
Hay N. Reprogramming glucose metabolism in cancer: Can it be exploited for cancer therapy? Nat Rev Cancer. 2016;16(10):635–49.
Fadaka A, Ajiboye B, Ojo O, Adewale O, Olayide I, Emuowhochere R. Biology of glucose metabolization in cancer cells. J Oncol Sci. 2017;3(2):45–51.
Sarraf JS, Puty TC, de Brito GSA, Cunha RDPC, Lira GSA, de Carvalho LEW, et al. Glucose variations and their impact on the treatment response in advanced colorectal cancer. Scr Sci Vox Studentium. 2017;1(1):23–7.
Deeken JF, Löscher W. The blood-brain barrier and cancer: transporters, treatment, and trojan horses. Clin Cancer Res. 2007;13(6):1663–74.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Stoyanov, G.S., Dzhenkov, D., Ghenev, P. et al. Cell biology of glioblastoma multiforme: from basic science to diagnosis and treatment. Med Oncol 35, 27 (2018). https://doi.org/10.1007/s12032-018-1083-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12032-018-1083-x