Abstract
Ammonia is a toxic by-product of protein catabolism and is involved in changes in glutamate metabolism. Therefore, ammonia metabolism genes may link a range of diseases involving glutamate signaling such as Alzheimer’s disease (AD), major depressive disorder (MDD), and type 2 diabetes (T2D). We analyzed data from a National Institute on Aging study with a family-based design to determine if 45 single nucleotide polymorphisms (SNPs) in glutaminase (GLS), carbamoyl phosphate synthetase 1 (CPS1), or glutamate-ammonia ligase (GLUL) genes were associated with AD, MDD, or T2D using PLINK software. HAPLOVIEW software was used to calculate linkage disequilibrium measures for the SNPs. Next, we analyzed the associated variations for potential effects on transcriptional control sites to identify possible functional effects of the SNPs. Of the SNPs that passed the quality control tests, four SNPs in the GLS gene were significantly associated with AD, two SNPs in the GLS gene were associated with T2D, and one SNP in the GLUL gene and three SNPs in the CPS1 gene were associated with MDD before Bonferroni correction. The in silico bioinformatic analysis suggested probable functional roles for six associated SNPs. Glutamate signaling pathways have been implicated in all these diseases, and other studies have detected similar brain pathologies such as cortical thinning in AD, MDD, and T2D. Taken together, these data potentially link GLS with AD, GLS with T2D, and CPS1 and GLUL with MDD and stimulate the generation of testable hypotheses that may help explain the molecular basis of pathologies shared by these disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Excess dietary protein is catabolized to release ammonia. Because of the relative toxicity of ammonia (Auron and Brophy 2012), it is removed from the body by the urea cycle and excreted as the relatively non-toxic compound urea. The urea cycle is thought to occur almost exclusively in the liver (Dimski 1994). However, certain types of ammonia metabolism such as glutamate cycling can occur in other tissues. Among the enzymes involved in ammonia metabolism are glutaminase (GLS, EC 3.5.1.2), carbamoyl phosphate synthetase 1 (CPS1, EC 6.3.4.16), and glutamate-ammonia ligase (GLUL, EC 6.3.1.2), also known as glutamine synthetase. CPS1 is the first committed step of the urea cycle. Individuals who lack a functional CPS1 gene have severe hyperammonemia resulting in cognitive impairment (Klaus et al. 2009). The majority of cells in the body (such as those in the brain) that lack a functional urea cycle rely on GLUL to locally remove ammonia by ligating it to glutamate to form glutamine (Cooper and Jeitner 2016). Glutaminase catalyzes the reverse process, releasing ammonia from glutamine to form glutamate. The human genome contains two glutaminase genes. Data from the Human Protein Atlas (www.proteinatlas.org) suggest that GLS is expressed primarily in the brain and kidney (http://www.proteinatlas.org/ENSG00000115419-GLS/tissue) (Uhlén et al. 2015). Because glutamate is an important neurotransmitter and signaling molecule, both GLUL and GLS are necessary for proper neural functioning (Cooper and Jeitner 2016).
Because (1) glutamine and glutamate are abundant and ubiquitous amino acids involved in ammonia metabolism, (2) ammonia is a by-product of protein catabolism, and (3) glutamate is an important signaling molecule, we hypothesized that the CPS1, GLUL, and GLS ammonia metabolism genes could influence various disease processes across a range of tissues. Evidence for a link between ammonia metabolism genes and type 2 diabetes (T2D) includes studies that have found changes in GLS activity in a rat model of diabetes (Ardawi 1987). In addition, a SNP in the GLUL gene has been associated with all-cause mortality in individuals with T2D (Prudente et al. 2015), and a separate study has found a transcriptomic link between T2D and GLUL (Mirza et al. 2014). Ammonia and glutamate metabolism changes have also been linked to mood disorders such as major depression. For example, glutamate signaling pathways have been shown to be altered in major depressive disorder (MDD) (Bernard et al. 2011). Furthermore, GLUL expression has been shown to be changed in individuals with MDD (Choudary et al. 2005; Miguel-Hidalgo et al. 2010; Bernard et al. 2011). However, one study reports no change in GLUL activity in astrocytes from the brains of individuals with MDD (Chandley et al. 2013). Further evidence supporting this connection is that researchers were able to induce behaviors consistent with depression in mice by inhibiting enzymes involved in ammonia and glutamate metabolism (Lee et al. 2013).
The potential link between ammonia metabolism and Alzheimer’s disease (AD) is particularly well-supported. The amyloid cascade hypothesis is the dominant hypothesis for the pathogenesis of AD (Hardy and Higgins 1992). However, increasing evidence suggests that increased amyloid-beta levels are only one facet of this complex disease (Herrup 2015). The ammonia hypothesis for the etiology of AD was first proposed in 1993 (Seiler 1993), but it has not yet been thoroughly investigated. The ammonia hypothesis suggests that ammonia toxicity plays a causal role in AD. This is supported by several observations reviewed by Seiler (2002). Briefly, individuals with AD have been found to have increased blood ammonia (Fisman et al. 1985) and cerebrospinal fluid ammonia levels. The negative effects of ammonia on cognitive functioning are well documented (Raabe 1987), and studies have suggested that there are high ammonia concentrations in AD brain (Hoyer et al. 1990). AD patients have also been shown to have increased plasma glutamate compared to controls (Miulli et al. 1993). Further studies suggest that changes in the expression of ammonia metabolism genes may be involved in AD. Researchers have found changes in GLUL expression in AD patients (Robinson 2000) as well as in mouse models of AD (Kulijewicz-Nawrot et al. 2013). Changes in GLS expression in AD brains have been found as well (Akiyama et al. 1989; McGeer et al. 1989; Burbaeva et al. 2014). The aforementioned studies suggest an association between GLUL, GLS, and CPS1 genes and disorders such as AD, T2D, and MDD. While all three of the genes of interest have not been explicitly implicated in all three diseases, there is sufficient evidence for the involvement of ammonia metabolism genes in the pathologies of these diseases to warrant further investigation.
All three of these diseases have genetic heritability; AD is estimated to have a heritability of 0.74 (Gatz et al. 1997), MDD of 0.37 (Sullivan et al. 2000), and T2D of 0.47–0.77 (Willemsen et al. 2015). There is also ample epidemiological evidence of associations among MDD, T2D, and AD. T2D has been found in several studies to be linked to the incidence of AD (Ott et al. 1999; Luchsinger et al. 2005; Gudala et al. 2013; Li et al. 2015). Two separate analyses of a GWAS data set found SNPs that were associated with both T2D and AD (Hao et al. 2015; Gao et al. 2016), suggesting the possibility of a shared genetic etiology. However, none of the hits from these studies were the genes we tested. There is also epidemiological evidence of an association between AD and MDD. Individuals with a history of depression were shown to have an increased risk for AD (Geerlings et al. 2008). Finally, T2D has been shown by several studies to nearly double the risk of developing MDD (Anderson et al. 2001; Ali et al. 2006). However, not every study supports a genetic association among these diseases. A study of 32 genetic variants identified in GWA studies of individuals with T2D found no association with AD (Chung et al. 2015). Another study also found no association between SNPs associated with T2D and risk of AD (Proitsi et al. 2014). A third study found no common genetic variants between individuals with AD and MDD (Gibson et al. 2017). Studies that continue to investigate the genetic component of these diseases could help untangle knowledge of genetic associations and elucidate targets for novel treatment strategies.
To investigate the potential association between these select ammonia metabolism genes and AD, MDD, and T2D, we used data from a family-based study of AD patients. The variations significantly associated with one or more of these diseases were interpreted considering previously published experimental results and bioinformatic analysis of possible effects of variants on gene expression. This study generates several hypotheses useful for guiding future work into mechanisms of pathogenesis of AD, MDD, and T2D and investigations into how these mechanisms may interact and overlap.
Materials and Methods
NIA-LOAD Family Study Subjects
Data for this study came from the National Institute on Aging—Late Onset Alzheimer’s Disease Family Study: Genome-Wide Association Study for Susceptibility Loci—Study Accession: phs000168.v1.p. There were 3007 individuals selected consisting of 1266 AD, 247 T2D, and 1688 MDD individuals, and 1279 non-AD individuals from 1386 pedigrees (589 nuclear families). Details on these subjects have been previously published (Lee et al. 2008). Population stratification does not apply to a family-based study design. The number of individuals in this dataset with each type of disease and combinations of co-occurrences are shown in Table 1.
Analytic Procedures
A total of 45 SNPs in GLUL (4 SNPs), GLS (8 SNPs), and CPS1 (33 SNPs) were available in the dataset for association testing. A family-based association analysis for risk of AD, T2D, and MDD was performed using the PLINK DFAM procedure. Empirical p values for single-marker analyses were calculated by 100,000 permutation tests using the Max (T) permutation procedure implemented in PLINK v1.07 software (http://zzz.bwh.harvard.edu/plink/index.shtml) (Purcell et al. 2007). Haplotype analysis was conducted in 2-SNP sliding windows using PLINK software to obtain p values, chi-square values, and haplotype frequencies for affected and unaffected individuals. HAPOVIEW v4.2 software (https://www.broadinstitute.org/haploview/haploview) (Barrett et al. 2005) was used to determine minor allele frequencies (MAFs) and to test for Hardy-Weinberg equilibrium (HWE) using all founders in the family-based dataset. The quality control cutoff values for HWE and MAF are < 0.001 and < 0.05, respectively. The linkage disequilibrium (LD) structure was constructed and r2 and D′ values were determined using HAPLOVIEW. To correct for multiple testing, the Bonferroni correction (α = 0.05/45 = 0.00111) was used.
Bioinformatic Analysis
Because the significantly associated SNPs were all intronic, the 11 SNPs associated with AD, MDD, or T2D were input into the Human Splice Finder v3.0 program (http://www.umd.be/HSF3/) (Desmet et al. 2009) to determine if any of the SNPs may affect silencing and enhancing regions of the genes. The sequence immediately surrounding the SNP was obtained from the NCBI dbSNP database (https://www.ncbi.nlm.nih.gov/snp). PERFECTOS-APE was used to predict transcription factor (TF) binding sites affected by the SNPs, and the hits were compared with the results of database searches for TF that have been experimentally determined to be associated with the genes studied. We searched the TF databases Human Transcriptional Regulation Interaction Database (http://www.lbbc.ibb.unesp.br/htri/) (Bovolenta et al. 2012) and RegNetwork (http://www.regnetworkweb.org/) (Liu et al. 2015) for TFs that have been experimentally determined to interact with the genes of interest.
Results
Single-Marker Analysis
PLINK single-marker analysis revealed several SNPs associated with AD, MDD, or T2D with an empirical p value < 0.05.
Alzheimer’s Disease
There were four SNPs significantly associated with AD before the Bonferroni correction (rs6758866, p = 0.00350; rs2355570, p = 0.03675; rs1921907, p = 0.00334; and rs883844, p = 0.00163). All four of these SNPs are located in the GLS gene on chromosome 2, and all have a HWE p > 0.001 and a MAF of p > 0.05, therefore, they passed the quality control test. These results are shown in Table 2.
Major Depressive Disorder
Five SNPs were significantly associated with MDD before the Bonferroni correction. Four of these SNPs (rs6749597, p = 0.02776; rs9789405, p = 0.01283; rs2287602, p = 0.01692; and rs2302909, p = 0.02103) are located in the CPS1 gene on chromosome 2, while one SNP (rs12735664, p = 0.03640) is located in the GLUL gene. While each of these has a MAF > 0.05, rs2302909 failed to pass the test for HWE (p = 2.0E−4). These results are shown in Table 3.
Type 2 Diabetes
As shown in Table 4, three SNPs were significantly associated with T2D before the Bonferroni correction, two in the GLS gene (rs1921915, p = 0.01794; and rs1517354, p = 0.00072) and one in the CPS1 gene (rs2302909, p = 0.00647). All of these SNPs have a MAF of > 0.05, but rs2302909 failed to pass the test for HWE (p = 2.0E−4).
Two-SNP Haplotype Analysis
PLINK two-SNP haplotype analysis revealed several haplotypes associated with AD (one haplotype), MDD (11 haplotypes), and T2D (15 haplotypes). The haplotypes with p < 0.05 are listed in Table 5 (AD), Table 6 (MDD), and Table 7 (T2D).
LD Structure
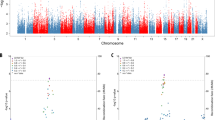
The LD structures for these genes are in shown in Fig. 1. The GLS and CPS1 genes are located on chromosome 2 (2q32.2 and 2q34, respectively), while the GLUL gene is located on chromosome 1 (1q25.3). SNP pairs with an r2 value > 0.5 and a D′ value greater than 0.8 are listed in Table 8.
Bioinformatic Analysis
All of the SNPs tested are intronic. Of the 11 SNPs with a significant association with AD, MDD, or T2D, bioinformatic analysis suggested functions for seven. Of these, only six SNPs are in HWE; the other SNP, rs2302909, will not be considered further. Three SNPs (rs6758866, rs2355570, and rs1517354) were predicted to create enhancer sites, and one SNP decreased the likelihood of the sequence binding to TFs that have been experimentally determined to interact with the gene sequences of interest (rs1921907). Another two SNPs (rs9789405 and rs2287602) both created an enhancer site and decreased the likelihood of binding with a TF. The details of these results are presented in Table 9.
Discussion
Alzheimer’s Disease
Because of the potential effect of ammonia levels on the onset and progression of AD described above (Seiler 1993), we hypothesized that SNPs in the ammonia metabolism genes GLUL, CPS1, and GLS may be associated with AD. However, single-marker analyses only found SNP markers statistically associated with AD in the GLS gene (Table 3) in this current study. Bioinformatic analysis using the Human Splice Finder software and the PERFECTOS-APE program suggested that three of these intronic SNPs may have a direct functional role in GLS regulation (Table 9). The minor alleles of SNPs rs6758866 and rs2355570 are predicted to create enhancer sites. Each of these variations may increase the expression of GLS. The minor allele of SNP rs1921907 is predicted by the PERFECTOS-APE software to decrease the likelihood of binding to the TF ETS1. ETS1 has been shown to be expressed in brain (http://www.proteinatlas.org/ENSG00000134954-ETS1/tissue) (Uhlén et al. 2015) and to interact with the GLS gene (Hollenhorst et al. 2009). Because ETS1 can be either a repressor or an activator of transcription (Dittmer 2003), it is not possible to predict the direction of regulation. The statistical association of the SNP rs883844 with AD is likely the result of an indirect association. The SNP may possibly act as a marker for a nearby unsequenced variation involved in the disease process, or its association may be due to its proximity to the other three SNPs in the GLS gene identified in this study as being associated with AD. Data in Table 8 reveal rs883844 is in LD with rs2355570 (D′ = 0.995, r2 = 0.561), rs1921907 (D′ = 0.990, r2 = 0.777), and rs6758866 (D′ = 0.987, r2 = 0.764). This may explain the significant association with AD in the absence of a predicted function.
As mentioned earlier, GLS is the isoform of glutaminase mostly found in the brain and kidneys (Uhlén et al. 2015). In contrast, GLS2 is mostly localized to the liver (http://www.proteinatlas.org/ENSG00000135423-GLS2/tissue) (Uhlén et al. 2015). GLS breaks down glutamine to ammonia and glutamate. Glutamate, an excitatory neurotransmitter, is important for synaptic transmission and memory formation (Esposito et al. 2013), but increased levels can lead to excitotoxic neuronal cell death in the brain. If the observed variants in the GLS gene or nearby unsequenced SNPs in LD affect glutaminase levels and enzyme activity, they would affect the regeneration of the glutamate used to remove neurotoxic ammonia. Changing these glutamate levels could impact cognitive function in AD (Myhrer 1998). Several studies agree that GLS levels in AD brain are decreased (Akiyama et al. 1989; McGeer et al. 1989; Burbaeva et al. 2014). Two of the three SNPs associated with AD and predicted to have a function may create an enhancer site, but enhanced expression of GLS in AD is inconsistent with the published literature. It is possible that the predicted enhancer sites created are in LD with nearby unsequenced SNPs that are more important for transcriptional regulation, or ETS1 usually acts as a relatively strong activator in this system. Experimental studies of autopsied AD patient brains have found an increase in glutamate levels (Xu et al. 2016). However, another study found decreased glutamate in the temporal cortex of AD brain (Gueli and Taibi 2013). Both increases and decreases in brain glutamate are associated with cognitive decline (Myhrer 1998). It is possible that changes in glutamate levels in AD brain are region-specific and occur because of disrupted glutamate and ammonia homeostasis.
Major Depressive Disorder
Several SNPs in the CPS1 gene were linked to MDD in this study (Table 3). CPS1 is critically important in ammonia metabolism as evidenced by the devastating effects of hyperammonemia in CPS1-deficient individuals (Suzuki et al. 1986; Finckh et al. 1998). Therefore, the variations identified in this study could potentially have major effects on blood ammonia levels if the variations are linked to changes in CPS1 activity. As previously mentioned, CPS1 is mainly found in the liver (http://www.proteinatlas.org/ENSG00000021826-CPS1/tissue) (Uhlén et al. 2015), and it catalyzes the incorporation of ammonia into carbamoyl phosphate in the urea cycle. The clinical observations described above suggest that changes in CPS1 activity may have an impact on blood ammonia levels, and changes in blood ammonia levels may also impact glutamate levels in the brain, affecting cognition (Suárez et al. 2002). Several studies suggest that changes in glutamate levels in several areas of the brain could be linked to mood disorders through disruption of the levels of glutamate and glutamine (Sanacora et al. 2012).
Bioinformatic analyses suggested that two SNPs in HWE analyzed in this study may have a functional role in MDD (Table 9). The minor allele of the SNP rs9789405 is predicted by the Human Splice Finder program to create an enhancer site. The same SNP variant is predicted by PERFECTOS-APE to decrease the likelihood of binding by the TF E2F4. E2F4 is mainly a transcriptional repressor (Crosby and Almasan 2004) and has been experimentally demonstrated to interact with the CPS1 gene (Litovchick et al. 2007). The minor allele of the SNP rs2287602 is predicted by Human Splice Finder to create an enhancer site and by PERFECTOS-APE to decrease the likelihood of association with the TF FOXP3. This TF mainly plays a role in regulatory T cell function (Vent-Schmidt et al. 2014), but it has recently been found to play a role in promoting mitochondrial oxidative metabolism (Angelin et al. 2017) and can even localize to mitochondria in hepatocytes (Rojas et al. 2016). FOXP3 is known to either increase or decrease gene expression depending upon the other TFs with which it associates (Szylberg et al. 2016). The Human Protein Atlas reports mRNA for both E2F4 (http://www.proteinatlas.org/ENSG00000205250-E2F4/tissue) and FOXP3 (http://www.proteinatlas.org/ENSG00000049768-FOXP3/tissue) in human liver (Uhlén et al. 2015). Based on the predicted functions of these variants, we predict that there may be altered expression of CPS1 in the liver of some MDD subjects. Altered CPS1 expression may change the levels of ammonia in the blood, therefore changing the glutamate levels in the brains of individuals with MDD. A SNP in CPS1 significantly associated with MDD that was not assigned a function by our bioinformatic analysis, rs6749597, is in LD with the predicted functional SNPs (rs6749597:rs9789405, D′ = 1, r2 = 0.941; rs6749597:rs2287602, D′ = 1, r2 = 0.937). All variations in CPS1 that passed the quality control tests are in the same haplotype block (Fig. 1).
Type 2 Diabetes
SNPs in the GLS and CPS1 genes were associated with T2D (Table 4). The SNP in the CPS1 gene (rs2302909) is not in HWE, so it will not be further considered. The liver is the major hub of ammonia metabolism and gluconeogenesis, so it is not surprising that ammonia metabolism genes are linked to T2D. Excess glutamate in the liver can be deaminated, fed into the citric acid cycle, and then used for gluconeogenesis, contributing to the high blood glucose levels observed in T2D. Although T2D is traditionally associated with insulin resistance in the liver and peripheral tissues, one of the hallmarks of the later stages of T2D is the inability of β cells in the pancreas to secrete enough insulin to activate insulin signaling pathways in insulin-resistant tissues (Cantley and Ashcroft 2015). The incretin pathway is involved in insulin secretion in the pancreas (Yokoi et al. 2016). Several experimental drugs for the treatment of T2D have been designed to increase the effectiveness of the incretin pathway (Drucker et al. 2010). Glutamate has been found to increase insulin excretion by amplifying the incretin pathway in beta cells (Gheni et al. 2014). Therefore, changes in glutamate levels in the pancreas may affect the response to glucose signaling in T2D. As discussed above, CPS1, GLUL, and GLS may all affect the levels of glutamate available for signaling. GLS is expressed in pancreatic tissue (http://www.proteinatlas.org/ENSG00000115419-GLS/tissue) (Uhlén et al. 2015), so changes in expression of these genes could affect pancreatic function. These changes may play a role in the disease processes of T2D.
One SNP in HWE in the GLS gene is predicted to have a functional role that may be associated with T2D (Table 9). The SNP rs1517354 was predicted by Human Splice Finder to create an enhancer site (Table 9), possibly leading to an increase in GLS gene expression in T2D. This variation may lead to an increase in the rate at which glutamine is catabolized to glutamate and ammonia. When released from neurons, increased glutamate levels in the synaptic cleft can lead to excitotoxicity (Zhou and Danbolt 2014). A recent study suggests that some of the pathology of T2D may be due to increased activity of pancreatic receptors for glutamate (Huang et al. 2017). Glutamate excitotoxicity in the brain is mainly mediated by the NMDA receptor (NMDAR) (Lau and Tymianski 2010). A functional role for NMDARs has also been found in pancreatic beta cells (Inagaki et al. 1995; Marquard et al. 2015). The NMDAR agonist, glutamate, was found to be increased in the plasma of diabetic patients and in a rat model of diabetes (Huang et al. 2017). In vitro studies have shown that blocking NMDAR activation reduces glucose-mediated damage to pancreatic beta cells and improves beta cell function (Huang et al. 2017). These results suggest that changes in the expression of genes involved in glutamate metabolism may play a role in T2D by affecting the function of pancreatic beta cells.
Changes in Expression of Ammonia Metabolism Genes: an Explanation for Some Common Pathologies in AD, MDD, and T2D?
Cortical thinning is a feature of AD (Du et al. 2007), MDD (Tu et al. 2012), and T2D (Yoon et al. 2017). The temporal cortex appears to be specifically affected. Cortical thinning may be caused by cell death due to glutamate excitotoxicity. As previously discussed, the epidemiology of these diseases seems to be linked. For example, a study found that individuals with AD are at increased risk for T2D (Janson et al. 2004). A more recent study concluded that comorbidity of MDD and T2D increased the risk of dementia (Katon et al. 2012).
Memantine, an NMDAR antagonist, is a drug used to reduce glutamate excitotoxicity for the treatment of AD. Memantine was also found to have protective effects on pancreatic beta cells and to reduce blood glucose levels in a mouse model of diabetes (Huang et al. 2017), and it improved some measures of cognitive functioning in a mouse model of T2D (Iwanami et al. 2014). Double-blind studies suggest that memantine may also be an effective treatment for MDD (Amidfar et al. 2017). The efficacy of this drug for the treatment of several different diseases suggests clinically significant commonalities in the disease mechanisms. Because glutamate signaling is so tightly tied to ammonia metabolism, changes in the expression of ammonia metabolism genes may be at least partially responsible for the observed cortical thinning and disease phenotypes in all three of these disorders.
Testable Hypotheses Generated and Study Limitations
This study generates several testable hypotheses: (1) Individuals with the minor allele variants of rs6758866, rs2355570, and rs1517354 have altered GLS gene expression and glutaminase enzyme activity. (2) Individuals with abnormal GLS gene expression are at greater risk for AD or T2D. (3) Individuals with the minor allele variants rs9789405 and rs2287602 have altered expression of the CPS1 gene and altered CPS1 enzyme activity. (4) Individuals with altered CPS1 gene expression are at higher risk for MDD. (5) Individuals with abnormal blood ammonia levels are at higher risk for MDD, and reducing blood ammonia may alleviate some of the symptoms of MDD. (6) Changes in glutamate levels in the brain due to changes in the expression of GLS, GLUL, or CPS1 are common to AD, MDD, and T2D, and these changes contribute to the common tissue pathology observed in these diseases. (7) Drugs that regulate glutamate signaling may alleviate some symptoms of AD, MDD, and T2D.
While this study’s results generate many hypotheses consistent with the published literature, the study also has several limitations. We report a genetic association from just one dataset; to decrease the risk of a type 1 error, other datasets with similar and different study designs should also be examined for comparable associations. Only rs1517354, the C-C haplotype from rs1517354 and rs883844, and the C-A haplotype from rs12468557 and rs2302909 with T2D (Tables 4 and 7) showed significant associations after a Bonferroni correction (p < 0.00111). Thus, our current findings might be subject to type 1 error, and the results need to be supported by additional large samples in a future study. Second, it was not possible to predict the direction of change in gene expression of the SNPs rs2287602 and rs1921907 because they were predicted to interact with TFs that can be either activators or repressors. Third, GWAS have largely not indicated ammonia metabolism gene associations with AD, T2D, or MDD. This may be because the associations are weak or because of incomplete genomic coverage in GWAS datasets. Lastly, the bioinformatic results of this study need to be supported by experimentation to verify these predictions. Even with these limitations, the findings of this study are potentially clinically relevant and warrant further investigation due to their high explanatory power and their general consistency with experimental results.
Conclusion
This study used data from a family-based study design and found a novel epidemiological association of select ammonia metabolism genes with AD, MDD, and T2D. Bioinformatic analyses suggested a functional role for many of the identified SNPs. These functional roles generally fit with previously published experimental results. The associations found in this study should be confirmed by other genetic epidemiological studies to increase confidence in our conclusions. One dataset which may replicate the current results is from the Columbia University Study of Caribbean Hispanics with Familial and Sporadic Late Onset Alzheimer’s Disease, dbGaP Study Accession: phs000496.v1.p1. The next step would be to experimentally verify the effects of these SNPs on gene expression and protein levels. This study is a step toward understanding the genetic and metabolic underpinnings of complex diseases with heritable components.
References
Akiyama H, McGeer PL, Itagaki S et al (1989) Loss of glutaminase-positive cortical neurons in Alzheimer’s disease. Neurochem Res 14(4):353–358. https://doi.org/10.1007/BF01000038
Ali S, Stone MA, Peters JL, Davies MJ, Khunti K (2006) The prevalence of co-morbid depression in adults with type 2 diabetes: a systematic review and meta-analysis. Diabet Med 23(11):1165–1173. https://doi.org/10.1111/j.1464-5491.2006.01943.x
Amidfar M, Khiabany M, Kohi A, Salardini E, Arbabi M, Roohi Azizi M, Zarrindast MR, Mohammadinejad P, Zeinoddini A, Akhondzadeh S (2017) Effect of memantine combination therapy on symptoms in patients with moderate-to-severe depressive disorder: randomized, double-blind, placebo-controlled study. J Clin Pharm Ther 42(1):44–50. https://doi.org/10.1111/jcpt.12469
Anderson RJ, Freedland KE, Clouse RE, Lustman PJ (2001) The prevalence of comorbid depression in adults with diabetes: a meta-analysis. Diabetes Care 24(6):1069–1078. https://doi.org/10.2337/diacare.24.6.1069
Angelin A, Gil-de-Gómez L, Dahiya S, Jiao J, Guo L, Levine MH, Wang Z, Quinn WJ III, Kopinski PK, Wang L, Akimova T, Liu Y, Bhatti TR, Han R, Laskin BL, Baur JA, Blair IA, Wallace DC, Hancock WW, Beier UH (2017) Foxp3 reprograms T cell metabolism to function in low-glucose, high-lactate environments. Cell Metab 25(6):1282–1293.e7. https://doi.org/10.1016/j.cmet.2016.12.018
Ardawi MSM (1987) The maximal activity of phosphate-dependent glutaminase and glutamine metabolism in the colon and the small intestine of streptozotocin-diabetic rats. Diabetologia 30(2):109–114. https://doi.org/10.1007/bf00274581
Auron A, Brophy PD (2012) Hyperammonemia in review: pathophysiology, diagnosis, and treatment. Pediatr Nephrol 27(2):207–222. https://doi.org/10.1007/s00467-011-1838-5
Barrett JC, Fry B, Maller J, Daly MJ (2005) Haploview: analysis and visualization of LD and haplotype maps. Bioinformatics 21(2):263–265. https://doi.org/10.1093/bioinformatics/bth457
Bernard R, Kerman IA, Thompson RC, Jones EG, Bunney WE, Barchas JD, Schatzberg AF, Myers RM, Akil H, Watson SJ (2011) Altered expression of glutamate signaling, growth factor, and glia genes in the locus coeruleus of patients with major depression. Mol Psychiatry 16(6):634–646. https://doi.org/10.1038/mp.2010.44
Bovolenta LA, Acencio ML, Lemke N (2012) HTRIdb: an open-access database for experimentally verified human transcriptional regulation interactions. BMC Genomics 13(1):405. https://doi.org/10.1186/1471-2164-13-405
Burbaeva GS, Boksha IS, Tereshkina EB, Savushkina OK, Prokhorova TA, Vorobyeva EA (2014) Glutamate and GABA-metabolizing enzymes in post-mortem cerebellum in Alzheimer’s disease: phosphate-activated glutaminase and glutamic acid decarboxylase. Cerebellum 13(5):607–615. https://doi.org/10.1007/s12311-014-0573-4
Cantley J, Ashcroft FM (2015) Q&A: insulin secretion and type 2 diabetes: why do β-cells fail? BMC Biol 13(1):33. https://doi.org/10.1186/s12915-015-0140-6
Chandley MJ, Szebeni K, Szebeni A, Crawford J, Stockmeier A, Turecki G, Miguel-Hidalgo J, Ordway G (2013) Gene expression deficits in pontine locus coeruleus astrocytes in men with major depressive disorder. J Psychiatry Neurosci 38(4):276–284. https://doi.org/10.1503/jpn.120110
Choudary PV, Molnar M, Evans SJ, Tomita H, Li JZ, Vawter MP, Myers RM, Bunney WE, Akil H, Watson SJ, Jones EG (2005) Altered cortical glutamatergic and GABAergic signal transmission with glial involvement in depression. Proc Natl Acad Sci U S A 102(43):15653–15658. https://doi.org/10.1073/pnas.0507901102
Chung SJ, Kim M-J, Kim J, Ryu HS, Kim YJ, Kim SY, Lee JH (2015) Association of type 2 diabetes GWAS loci and the risk of Parkinson’s and Alzheimer’s diseases. Parkinsonism Relat Disord 21(12):1435–1440. https://doi.org/10.1016/j.parkreldis.2015.10.010
Cooper AJL, Jeitner TM (2016) Central role of glutamate metabolism in the maintenance of nitrogen homeostasis in normal and hyperammonemic brain. Biomol Ther 6(2). https://doi.org/10.3390/biom6020016
Crosby ME, Almasan A (2004) Opposing roles of E2Fs in cell proliferation and death. Cancer Biol Ther 3(12):1208–1211. https://doi.org/10.4161/cbt.3.12.1494
Desmet F-O, Hamroun D, Lalande M, Collod-Béroud G, Claustres M, Béroud C (2009) Human Splicing Finder: an online bioinformatics tool to predict splicing signals. Nucleic Acids Res 37(9):e67–e67. https://doi.org/10.1093/nar/gkp215
Dimski DS (1994) Ammonia metabolism and the urea cycle: function and clinical implications. J Vet Intern Med 8(2):73–78. https://doi.org/10.1111/j.1939-1676.1994.tb03201.x
Dittmer J (2003) The biology of the Ets1 proto-oncogene. Mol Cancer 2(1):29. https://doi.org/10.1186/1476-4598-2-29
Drucker DJ, Sherman SI, Gorelick FS, Bergenstal RM, Sherwin RS, Buse JB (2010) Incretin-based therapies for the treatment of type 2 diabetes: evaluation of the risks and benefits. Diabetes Care 33(2):428–433. https://doi.org/10.2337/dc09-1499
Du A-T, Schuff N, Kramer JH et al (2007) Different regional patterns of cortical thinning in Alzheimer’s disease and frontotemporal dementia. Brain 130(4):1159–1166. https://doi.org/10.1093/brain/awm016
Esposito Z, Belli L, Toniolo S, Sancesario G, Bianconi C, Martorana A (2013) Amyloid B, glutamate, excitotoxicity in Alzheimer’s disease: are we on the right track? CNS Neurosci Ther 19(8):549–555. https://doi.org/10.1111/cns.12095
Finckh U, Kohlschütter A, Schäfer H, Sperhake K, Colombo JP, Gal A (1998) Prenatal diagnosis of carbamoyl phosphate synthetase I deficiency by identification of a missense mutation in CPS1. Hum Mutat 12(3):206–211. https://doi.org/10.1002/(SICI)1098-1004(1998)12:3<206::AID-HUMU8>3.0.CO;2-E
Fisman M, Gordon B, Feleki V, Helmes E, Appell J, Rabheru K (1985) Hyperammonemia in Alzheimer’s disease. Am J Psychiatry 142(1):71–73. https://doi.org/10.1176/ajp.142.1.71
Gao L, Cui Z, Shen L, Ji H-F (2016) Shared genetic etiology between type 2 diabetes and Alzheimer’s disease identified by bioinformatics analysis. J Alzheimers Dis 50(1):13–17. https://doi.org/10.3233/JAD-150580
Gatz M, Pedersen NL, Berg S, et al (1997) Heritability for Alzheimer’s disease: the study of dementia in Swedish twins. J Gerontol 52:117–125
Geerlings MI, den Heijer T, Koudstaal PJ, Hofman A, Breteler MMB (2008) History of depression, depressive symptoms, and medial temporal lobe atrophy and the risk of Alzheimer disease. Neurology 70(15):1258–1264. https://doi.org/10.1212/01.wnl.0000308937.30473.d1
Gheni G, Ogura M, Iwasaki M, Yokoi N, Minami K, Nakayama Y, Harada K, Hastoy B, Wu X, Takahashi H, Kimura K, Matsubara T, Hoshikawa R, Hatano N, Sugawara K, Shibasaki T, Inagaki N, Bamba T, Mizoguchi A, Fukusaki E, Rorsman P, Seino S (2014) Glutamate acts as a key signal linking glucose metabolism to incretin/cAMP action to amplify insulin secretion. Cell Rep 9(2):661–673. https://doi.org/10.1016/j.celrep.2014.09.030
Gibson J, Russ TC, Adams MJ, Clarke TK, Howard DM, Hall LS, Fernandez-Pujals AM, Wigmore EM, Hayward C, Davies G, Murray AD, Smith BH, Porteous DJ, Deary IJ, McIntosh AM (2017) Assessing the presence of shared genetic architecture between Alzheimer’s disease and major depressive disorder using genome-wide association data. Transl Psychiatry 7(4):e1094. https://doi.org/10.1038/tp.2017.49
Gudala K, Bansal D, Schifano F, Bhansali A (2013) Diabetes mellitus and risk of dementia: a meta-analysis of prospective observational studies. J Diabetes Investig 4(6):640–650. https://doi.org/10.1111/jdi.12087
Gueli MC, Taibi G (2013) Alzheimer’s disease: amino acid levels and brain metabolic status. Neurol Sci 34(9):1575–1579. https://doi.org/10.1007/s10072-013-1289-9
Hao K, Di Narzo AF, Ho L et al (2015) Shared genetic etiology underlying Alzheimer’s disease and type 2 diabetes. Mol Asp Med 43–44:66–76. https://doi.org/10.1016/j.mam.2015.06.006
Hardy JA, Higgins GA (1992) Alzheimer’s disease: the amyloid cascade hypothesis. Science (80) 256:184–185
Herrup K (2015) The case for rejecting the amyloid cascade hypothesis. Nat Neurosci 18(6):794–799. https://doi.org/10.1038/nn.4017
Hollenhorst PC, Chandler KJ, Poulsen RL, Johnson WE, Speck NA, Graves BJ (2009) DNA specificity determinants associate with distinct transcription factor functions. PLoS Genet 5(12):e1000778. https://doi.org/10.1371/journal.pgen.1000778
Hoyer S, Nitsch R, Oesterreich K (1990) Ammonia is endogenously generated in the brain in the presence of presumed and verified dementia of Alzheimer type. Neurosci Lett 117(3):358–362. https://doi.org/10.1016/0304-3940(90)90691-2
Huang X-T, Li C, Peng X-P, Guo J, Yue SJ, Liu W, Zhao FY, Han JZ, Huang YH, Yang-Li, Cheng QM, Zhou ZG, Chen C, Feng DD, Luo ZQ (2017) An excessive increase in glutamate contributes to glucose-toxicity in β-cells via activation of pancreatic NMDA receptors in rodent diabetes. Sci Rep 7:44120. https://doi.org/10.1038/srep44120
Inagaki N, Kuromi H, Gonoi T, Okamoto Y, Ishida H, Seino Y, Kaneko T, Iwanaga T, Seino S (1995) Expression and role of ionotropic glutamate receptors in pancreatic islet cells. FASEB 9(8):686–691. https://doi.org/10.1096/fasebj.9.8.7768362
Iwanami J, Mogi M, Tsukuda K, Jing F, Ohshima K, Wang XL, Nakaoka H, Kan-no H, Chisaka T, Bai HY, Min LJ, Horiuchi M (2014) Possible synergistic effect of direct angiotensin II type 2 receptor stimulation by compound 21 with memantine on prevention of cognitive decline in type 2 diabetic mice. Eur J Pharmacol 724:9–15. https://doi.org/10.1016/j.ejphar.2013.12.015
Janson J, Laedtke T, Parisi JE, et al (2004) Increased risk of type 2 diabetes in Alzheimer disease
Katon W, Lyles CR, Parker MM, Karter AJ, Huang ES, Whitmer RA (2012) Association of depression with increased risk of dementia in patients with type 2 diabetes. Arch Gen Psychiatry 69(4):410–417. https://doi.org/10.1001/archgenpsychiatry.2011.154
Klaus V, Vermeulen T, Minassian B, Israelian N, Engel K, Lund AM, Roebrock K, Christensen E, Häberle J (2009) Highly variable clinical phenotype of carbamylphosphate synthetase 1 deficiency in one family: an effect of allelic variation in gene expression? Clin Genet 76(3):263–269. https://doi.org/10.1111/j.1399-0004.2009.01216.x
Kulijewicz-Nawrot M, Syková E, Chvátal A, Verkhratsky A, Rodríguez JJ (2013) Astrocytes and glutamate homoeostasis in Alzheimer’s disease: a decrease in glutamine synthetase, but not in glutamate transporter-1, in the prefrontal cortex. ASN Neuro 5(4):273–282. https://doi.org/10.1042/AN20130017
Lau A, Tymianski M (2010) Glutamate receptors, neurotoxicity and neurodegeneration. Eur J Phys 460(2):525–542. https://doi.org/10.1007/s00424-010-0809-1
Lee JH, Cheng R, Graff-Radford N, Foroud T, Mayeux R, National Institute on Aging Late-Onset Alzheimer’s Disease Family Study Group (2008) Analyses of the National Institute on Aging Late-Onset Alzheimer’s Disease Family Study: implication of additional loci. Arch Neurol 65(11):1518–1526. https://doi.org/10.1001/archneur.65.11.1518
Lee Y, Son H, Kim G, Kim S, Lee DH, Roh GS, Kang SS, Cho GJ, Choi WS, Kim HJ (2013) Glutamine deficiency in the prefrontal cortex increases depressive-like behaviours in male mice. J Psychiatry Neurosci 38(3):183–191. https://doi.org/10.1503/jpn.120024
Li X, Song D, Leng SX (2015) Link between type 2 diabetes and Alzheimer’s disease: from epidemiology to mechanism and treatment. Clin Interv Aging 10:549–560. https://doi.org/10.2147/CIA.S74042
Litovchick L, Sadasivam S, Florens L, Zhu X, Swanson SK, Velmurugan S, Chen R, Washburn MP, Liu XS, DeCaprio JA (2007) Evolutionarily conserved multisubunit RBL2/p130 and E2F4 protein complex represses human cell cycle-dependent genes in quiescence. Mol Cell 26(4):539–551. https://doi.org/10.1016/j.molcel.2007.04.015
Liu Z-P, Wu C, Miao H, Wu H (2015) RegNetwork: an integrated database of transcriptional and post-transcriptional regulatory networks in human and mouse. Database 2015:bav095. https://doi.org/10.1093/database/bav095
Luchsinger JA, Reitz C, Honig LS, Tang MX, Shea S, Mayeux R (2005) Aggregation of vascular risk factors and risk of incident Alzheimer disease. Neurology 65(4):545–551. https://doi.org/10.1212/01.wnl.0000172914.08967.dc
Marquard J, Otter S, Welters A, Stirban A, Fischer A, Eglinger J, Herebian D, Kletke O, Klemen MS, Stožer A, Wnendt S, Piemonti L, Köhler M, Ferrer J, Thorens B, Schliess F, Rupnik MS, Heise T, Berggren PO, Klöcker N, Meissner T, Mayatepek E, Eberhard D, Kragl M, Lammert E (2015) Characterization of pancreatic NMDA receptors as possible drug targets for diabetes treatment. Nat Med 21(4):363–372. https://doi.org/10.1038/nm.3822
McGeer EG, McGeer PL, Akiyama H, Harrop R (1989) Cortical glutaminase, beta-glucuronidase and glucose utilization in Alzheimer’s disease. Can J Neurol Sci 16(S4):511–515. https://doi.org/10.1017/S0317167100029851
Miguel-Hidalgo JJ, Waltzer R, Whittom AA, Austin MC, Rajkowska G, Stockmeier CA (2010) Glial and glutamatergic markers in depression, alcoholism, and their comorbidity. J Affect Disord 127(1-3):230–240. https://doi.org/10.1016/j.jad.2010.06.003
Mirza Z, Kamal MA, Buzenadah AM et al (2014) Establishing genomic/transcriptomic links between Alzheimer’s disease and type 2 diabetes mellitus by meta-analysis approach. CNS Neurol Disord Drug Targets 13(3):501–516. https://doi.org/10.2174/18715273113126660154
Miulli DE, Norwell DY, Schwartz FN (1993) Plasma concentrations of glutamate and its metabolites in patients with Alzheimer’s disease. J Am Osteopath Assoc 93(6):670–676
Myhrer T (1998) Adverse psychological impact, glutamatergic dysfunction, and risk factors for Alzheimer’s disease. Neurosci Biobehav Rev 23(1):131–139. https://doi.org/10.1016/S0149-7634(98)00039-6
Ott A, Stolk RP, van Harskamp F, Pols HAP, Hofman A, Breteler MMB (1999) Diabetes mellitus and the risk of dementia: the Rotterdam Study. Neurology 53(9):1937–1942. https://doi.org/10.1212/WNL.53.9.1937
Proitsi P, Lupton MK, Velayudhan L, Hunter G, Newhouse S, Lin K, Fogh I, Tsolaki M, Daniilidou M, Pritchard M, Craig D, Todd S, Johnston JA, McGuinness B, Kloszewska I, Soininen H, Mecocci P, Vellas B, Passmore PA, Sims R, Williams J, Brayne C, Stewart R, Sham P, Lovestone S, Powell JF (2014) Alleles that increase risk for type 2 diabetes mellitus are not associated with increased risk for Alzheimer’s disease. Neurobiol Aging 35:2883.e3–2882883.e10. doi: https://doi.org/10.1016/j.neurobiolaging.2014.07.023, 12
Prudente S, Shah H, Bailetti D, Pezzolesi M, Buranasupkajorn P, Mercuri L, Mendonca C, de Cosmo S, Niewczas M, Trischitta V, Doria A (2015) Genetic variant at the GLUL locus predicts all-cause mortality in patients with type 2 diabetes. Diabetes 64(7):2658–2663. https://doi.org/10.2337/db14-1653
Purcell S, Neale B, Todd-Brown K, Thomas L, Ferreira MAR, Bender D, Maller J, Sklar P, de Bakker PIW, Daly MJ, Sham PC (2007) PLINK: a tool set for whole-genome association and population-based linkage analyses. Am J Hum Genet 81(3):559–575. https://doi.org/10.1086/519795
Raabe W (1987) Synaptic transmission in ammonia intoxication. Neurochem Pathol 6(1-2):145–166. https://doi.org/10.1007/BF02833604
Robinson SR (2000) Neuronal expression of glutamine synthetase in Alzheimer’s disease indicates a profound impairment of metabolic interactions with astrocytes. Neurochem Int 36(4-5):471–482. https://doi.org/10.1016/S0197-0186(99)00150-3
Rojas J, Teran-Angel G, Barbosa L, Peterson DL, Berrueta L, Salmen S (2016) Activation-dependent mitochondrial translocation of Foxp3 in human hepatocytes. Exp Cell Res 343(2):159–167. https://doi.org/10.1016/j.yexcr.2016.04.008
Sanacora G, Treccani G, Popoli M (2012) Towards a glutamate hypothesis of depression: an emerging frontier of neuropsychopharmacology for mood disorders. Neuropharmacology 62(1):63–77. https://doi.org/10.1016/j.neuropharm.2011.07.036
Seiler N (1993) Is ammonia a pathogenetic factor in Alzheimer’s disease? Neurochem Res 18(3):235–245. https://doi.org/10.1007/BF00969079
Seiler N (2002) Ammonia and Alzheimer’s disease. Neurochem Int 41(2-3):189–207. https://doi.org/10.1016/S0197-0186(02)00041-4
Suárez I, Bodega G, Fernández B (2002) Glutamine synthetase in brain: effect of ammonia. Neurochem Int 41(2-3):123–142. https://doi.org/10.1016/S0197-0186(02)00033-5
Sullivan PF, Neale MC, Kendler KS (2000) Genetic epidemiology of major depression: review and meta-analysis. Am J Psychiatry 157:1552–1562. https://doi.org/10.1176/appi.ajp.157.10.1552
Suzuki Y, Matsushima A, Ohtake A, Mori M, Tatibana M, Orii T (1986) Carbamyl phosphate synthetase I deficiency with no detectable mRNA activity. Eur J Pediatr 145(5):406–408. https://doi.org/10.1007/BF00439249
Szylberg Ł, Karbownik D, Marszałek A (2016) The role of FOXP3 in human cancers. Anticancer Res 36(8):3789–3794
Tu P-C, Chen L-F, Hsieh J-C, Bai YM, Li CT, Su TP (2012) Regional cortical thinning in patients with major depressive disorder: a surface-based morphometry study. Psychiatry Res Neuroimaging 202(3):206–213. https://doi.org/10.1016/j.pscychresns.2011.07.011
Uhlén M, Fagerberg L, Hallström BM, et al (2015) Tissue-based map of the human proteome
Vent-Schmidt J, Han JM, MacDonald KG, Levings MK (2014) The role of FOXP3 in regulating immune responses. Int Rev Immunol 33(2):110–128. https://doi.org/10.3109/08830185.2013.811657
Willemsen G, Ward KJ, Bell CG, et al (2015) The concordance and heritability of type 2 diabetes in 34,166 twin pairs from international twin registers: the Discordant Twin (DISCOTWIN) Consortium. Twin Res Hum Genet 18:762–771. https://doi.org/10.1017/thg.2015.83
Xu J, Begley P, Church SJ, Patassini S, Hollywood KA, Jüllig M, Curtis MA, Waldvogel HJ, Faull RLM, Unwin RD, Cooper GJS (2016) Graded perturbations of metabolism in multiple regions of human brain in Alzheimer’s disease: snapshot of a pervasive metabolic disorder. Biochim Biophys Acta - Mol Basis Dis 1862(6):1084–1092. https://doi.org/10.1016/j.bbadis.2016.03.001
Yokoi N, Gheni G, Takahashi H, Seino S (2016) β-Cell glutamate signaling: its role in incretin-induced insulin secretion. J Diabetes Investig 7(Suppl 1):38–43. https://doi.org/10.1111/jdi.12468
Yoon S, Cho H, Kim J, Lee DW, Kim GH, Hong YS, Moon S, Park S, Lee S, Lee S, Bae S, Simonson DC, Lyoo IK (2017) Brain changes in overweight/obese and normal-weight adults with type 2 diabetes mellitus. Diabetologia 60(7):1–11. https://doi.org/10.1007/s00125-017-4266-7
Zhou Y, Danbolt NC (2014) Glutamate as a neurotransmitter in the healthy brain. J Neural Transm 121(8):799–817. https://doi.org/10.1007/s00702-014-1180-8
Acknowledgments
We acknowledge the NIH GWAS Data Repository, the Contributing Investigator(s) who contributed the phenotype data and DNA samples from his/her original study, and the primary funding organization that supported the contributing study “National Institute on Aging—Late Onset Alzheimer’s Disease Family Study: Genome-Wide Association Study for Susceptibility Loci.” The datasets used for analyses described in this manuscript were obtained from dbGaP at http://www.ncbi.nlm.nih.gov/gap through dbGaP accession number phs000219.v1.p1. Funding support for the “Genetic Consortium for Late Onset Alzheimer’s Disease” was provided through the Division of Neuroscience, NIA. The Genetic Consortium for Late Onset Alzheimer’s Disease includes a genome-wide association study funded as part of the Division of Neuroscience, NIA. Assistance with phenotype harmonization and genotype cleaning, as well as with general study coordination, was provided by the Genetic Consortium for Late Onset Alzheimer’s Disease. In addition, JG would like to thank Wayne C. Birchfield for directing his attention to the role of ammonia metabolism in cognitive functioning.
Funding
This study was funded by East Tennessee State University.
Author information
Authors and Affiliations
Contributions
JG and KW performed the research, and JG wrote the first draft of the manuscript. PB, KW, and YL contributed to the content of the manuscript. All authors have approved the final version of this article.
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Griffin, J.W.D., Liu, Y., Bradshaw, P.C. et al. In Silico Preliminary Association of Ammonia Metabolism Genes GLS, CPS1, and GLUL with Risk of Alzheimer’s Disease, Major Depressive Disorder, and Type 2 Diabetes. J Mol Neurosci 64, 385–396 (2018). https://doi.org/10.1007/s12031-018-1035-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-018-1035-0