Abstract
Chronic NGF overexpression (OE) in the urothelium, achieved through the use of a highly urothelium-specific uroplakin II promoter, stimulates neuronal sprouting in the urinary bladder, produces increased voiding frequency and non-voiding contractions, and referred somatic sensitivity. Additional NGF-mediated pleiotropic changes might contribute to increased voiding frequency and pelvic hypersensitivity in NGF-OE mice such as neuropeptide/receptor systems including PACAP(Adcyap1) and PAC1 receptor (Adcyap1r1). Given the presence of PAC1-immunoreactive fibers and the expression of PAC1 receptor expression in bladder tissues, and PACAP-facilitated detrusor contraction, whether PACAP/receptor signaling contributes to increased voiding frequency and somatic sensitivity was evaluated in NGF-OE mice. Intravesical administration of the PAC1 receptor antagonist, PACAP(6–38) (300 nM), significantly (p ≤ 0.01) increased intercontraction interval (2.0-fold) and void volume (2.5-fold) in NGF-OE mice. Intravesical instillation of PACAP(6–38) also decreased baseline bladder pressure in NGF-OE mice. PACAP(6–38) had no effects on bladder function in WT mice. Intravesical administration of PACAP(6–38) (300 nM) significantly (p ≤ 0.01) reduced pelvic sensitivity in NGF-OE mice but was without effect in WT mice. PACAP/receptor signaling contributes to the increased voiding frequency and pelvic sensitivity observed in NGF-OE mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is a large literature detailing the importance of NGF in bladder sensory function and the development of referred hyperalgesia in response to urinary bladder inflammation (Arms and Vizzard 2011; Guerios et al. 2006, 2008; Jaggar et al. 1999). Bladder pain syndrome (BPS)/interstitial cystitis (IC) is a chronic pain syndrome characterized by pain, pressure or discomfort perceived to be bladder related with at least one urinary symptom (Clemens et al. 2014; Hanno and Sant 2001; Landis et al. 2014). In women with BPS/IC, neurotrophins are present in the urine or in the urinary bladder (Lowe et al. 1997; Okragly et al. 1999). In animal models of cystitis, the expression of neurotrophins is increased in central and peripheral micturition reflex pathways including the urinary bladder, spinal cord, and peripheral ganglia (Dmitrieva and McMahon 1996; Jaggar et al. 1999; Zvara and Vizzard 2007) (Chuang et al. 2001; Clemow et al. 1998; Guerios et al. 2006, 2008; Hu et al. 2005). Increased NGF expression may exert long-term cellular changes by activating signal transduction pathways mediated by the phosphorylation of Trk receptors and subsequent activation of the neurotrophin/Trk complex (Huang and Reichardt 2001; Pezet and McMahon 2006). Long-term cellular changes may affect neurotransmitter phenotype, synaptic reorganization and efficacy, and target organ function (Huang and Reichardt 2001; Pezet and McMahon 2006).
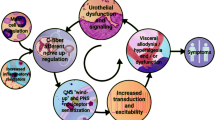
We continue to examine the role of NGF in urinary bladder dysfunction with the recent generation of a mouse model based on the hypothesis that chronic urothelial NGF overexpression induces sensory neuronal hypersensitivity and increases urinary bladder reflex function (Schnegelsberg et al. 2010). Chronic overexpression of NGF in the urothelium was achieved through the use of a highly urothelium-specific uroplakin II promoter (Liang et al. 2005; Lin et al. 1995). Our studies (Schnegelsberg et al. 2010) revealed that urothelium-specific overexpression of NGF in the urinary bladder of transgenic mice (1) stimulates neuronal sprouting in the urinary bladder; (2) produces local inflammatory changes in the urinary bladder; (3) increases voiding frequency; and (4) increases referred pelvic hypersensitivity.
An ongoing focus of our laboratory is to understand the expression and regulation of neuropeptide/receptor systems in micturition reflex pathways and their effects on urinary bladder function in the context of urinary bladder inflammation with increased NGF expression in the urinary bladder. Our previous studies (Girard et al. 2010, 2012; Merrill et al. 2013a) have examined the expression and regulation of neuropeptides (e.g., pituitary adenylate cyclase-activating polypeptide (PACAP, Adcyap1), vasoactive intestinal polypeptide (VIP), substance P (sub P), and galanin), and receptor (e.g., PAC1 (Adcyap1r1), VPAC1, and VPAC2) transcripts in the urinary bladder and lumbosacral DRG with urinary bladder inflammation induced by cyclophosphamide (CYP). In addition to PACAP binding to the PAC1 receptor (Arimura 1998; Braas and May 1996), PACAP has the capacity to bind to the primary receptors for VIP (i.e., VPAC1 and VPAC2) (Ng et al. 2012). These previous studies demonstrated that the expression and regulation of neuropeptides (e.g., PACAP, VIP, sub P, galanin) and receptors (e.g., PAC1, VPAC1, VPAC2) were dependent on the duration of CYP-induced cystitis and the tissue being studied (i.e., urothelium, detrusor, DRG) (Girard et al. 2010, 2012; Merrill et al. 2013a). Enhanced target-derived NGF availability increases PACAP expression in small nociceptive DRG cells (Jongsma et al. 2001). More recently, we have examined PACAP, VIP, and associated receptors regulation in the urinary bladder of NGF-OE and littermate wild-type (WT) mice (Girard et al. 2010, 2012; Merrill et al. 2013a). Differential regulation of PACAP, VIP, and receptors was demonstrated in NGF-OE and WT mice and in urothelium and detrusor smooth muscle (Girard et al. 2010, 2012; Merrill et al. 2013a). Exogenous administration of NGF to the detrusor smooth muscle or CYP-induced cystitis increases neuropeptide expression in spinal micturition pathways (Zvara and Vizzard 2007), voiding frequency and non-voiding bladder contractions (NVCs). PACAP or VIP null mice exhibit urinary bladder dysfunction (May and Vizzard 2010; Studeny et al. 2008). Pharmacological blockade of PACAP/PAC1 interactions reduced urinary frequency in a rat model of CYP-induced cystitis (Braas et al. 2006). The present study extends these observations by determining the effects of pharmacological blockade of PACAP/PAC1 interactions at the level of the urinary bladder on urinary bladder dysfunction in NGF-OE mice.
Materials and Methods
Animals, NGF-OE Mice
NGF-OE Mice
NGF-OE transgenic mice were generated at Roche Palo Alto (material transfer agreement with Roche Palo Alto and Dr. Debra Cockayne) in collaboration with Dr. Henry Sun at New York University Medical School as previously described (Schnegelsberg et al. 2010) (Girard et al. 2010, 2011). Animal genotype was confirmed by Southern and/or PCR analyses; all mice have the inbred genetic C57BL/6J background and were derived from F10 to F12 generations maintained through a hemizygous backcross strategy with C57BL/6J wild-type (WT) mice. Mice used in this study were bred locally at the University of Vermont College of Medicine. The litters were of normal size and weight and behaviors (feeding, drinking, activity patterns) appeared normal; adult female mice were used in these studies. As previously demonstrated (Girard et al. 2011) and confirmed in this study, urinary bladder weight was significantly (p ≤ 0.01) increased in NGF-OE mice compared to littermate WT mice (data not shown). All experimental protocols involving animal use were approved by the University of Vermont Institutional Animal Care and Use Committee (IACUC # 08–085). Animal care was under the supervision of the University of Vermont’s Office of Animal Care Management in accordance with the Association for Assessment and Accreditation of Laboratory Animal Care (AAALAC) and National Institutes of Health guidelines. All efforts were made to minimize the potential for animal pain, stress, or distress. Separate groups of female littermate WT and NGF-OE mice were used in the following experiments.
Real-Time Quantitative Reverse Transcription-Polymerase Chain Reaction (Q-PCR)
Determination of NGF transcript expression in the urinary bladder (urothelium, detrusor) of NGF-OE transgenic mice (n = 6–8) and littermate WT mice (n = 6–8) was determined using Q-PCR as previously described (Girard et al. 2011). Total RNA was extracted using the STAT-60 total RNA/mRNA isolation reagent (Tel-Test‘B’, Friendswood, TX, USA) as previously described (Girard et al. 2011). One μg of RNA per sample was used to synthesize complementary DNA using a mix of random hexamer and oligo dT primers with M-MLV reverse transcriptase (Promega Corp.) in a 25-μl final reaction volume. The quantitative PCR standards for all transcripts were prepared with the amplified cDNA products ligated directly into pCR2.1 TOPO vector using the TOPO TA cloning kit (Invitrogen). The nucleotide sequences of the inserts were verified by automated fluorescent dideoxy dye terminator sequencing (Vermont Cancer Center DNA Analysis Facility). To estimate the relative expression of the receptor transcripts, 10-fold serial dilutions of stock plasmids were prepared as quantitative standards. The range of standard concentrations was determined empirically. Complementary DNA templates, diluted 10-fold to minimize the inhibitory effects of the reverse transcription reaction components, were assayed using HotStart-IT SYBR Green qPCR Master Mix (USB, Cleveland, OH, USA) and 300 nM of each primer in a final 25 μl reaction volume.
Real-time quantitative PCR was performed on an Applied Biosystems 7500 Fast real-time PCR system (Applied Biosystems, Foster City, CA, USA) (Girard et al. 2002) using the following standard conditions: (1) serial heating at 94 °C for 2 min and (2) amplification over 45 cycles at 94 °C for 15 s and 60–64 °C depending on primers set for 30 s. The amplified product from these amplification parameters was subjected to SYBR Green I melting analysis by ramping the temperature of the reaction samples from 60 to 95 °C. A single DNA melting profile was observed under these dissociation assay conditions demonstrating the amplification of a single unique product free of primer dimers or other anomalous products. Oligonucleotide primer sequences for NGF and L32 have been previously reported (Klinger et al. 2008).
For data analyses, a standard curve was constructed by amplification of serially diluted plasmids containing the target sequence. Data were analyzed at the termination of each assay using sequence detection software (Sequence Detection Software, version 1.3.1; Applied Biosystems, Norwalk, CT, USA). In standard assays, default baseline settings were selected. The increase in SYBR Green I fluorescence intensity (ΔRn) was plotted as a function of cycle number and the threshold cycle was determined by the software as the amplification cycle at which the ΔRn first intersects the established baseline. All data are expressed as the relative quantity of the gene of interest normalized to the relative quantity of the housekeeping gene L32.
Split Bladder Preparation and Assessment of Potential Contamination of Bladder Layers
The urothelium + suburothelium was dissected from the detrusor smooth muscle using fine forceps under a dissecting microscope as previously described (Corrow et al. 2010; Schnegelsberg et al. 2010). To confirm the specificity of our split bladder preparations, urothelium + suburothelium and detrusor samples were examined for the presence of α-smooth muscle actin (1:1000; Abcam, Cambridge, MA) and uroplakin II (1:25; American Research Products, Belmont, MA) by Western blotting or reverse transcription PCR (Corrow et al. 2010; Girard et al. 2011, 2013). In urothelium + suburothelium layers, only uroplakin II was present (data not shown). Conversely, in detrusor samples, only α-smooth muscle actin was present (data not shown). In these studies, the use of the term urothelium refers to the urothelium and suburothelial layers.
Measurement of Urinary Bladder NGF
Determination of NGF protein content in the urinary bladder of NGF-OE transgenic mice (n = 8) and WT littermate controls (n = 8) was determined using enzyme-linked immunoassays (ELISAs) as previously described (Gonzalez et al. 2015; Schnegelsberg et al. 2010; Vizzard 2000a). Individual mouse bladders were dissected, weighed, and placed in Tissue Protein Extraction Reagent (1 g tissue/20 ml; Pierce Biotechnology, Woburn, MA) with Complete protease inhibitor cocktail tablets (Roche Applied Science, Mannheim, Germany) and stored at −80 °C. On the day of assay, individual bladders were disrupted with a Polytron homogenizer until homogeneous and centrifuged (10,000 rpm for 10 min) (Gonzalez et al. 2015; Schnegelsberg et al. 2010; Vizzard 2000a), and the supernatant was used for total protein estimation and CGRP and Sub P quantification. Total protein was determined by the Coomassie Plus Protein Assay Reagent Kit (Pierce) (Gonzalez et al. 2015), and NGF was quantified using standard 96-well ELISA plates (Phoenix Pharmaceuticals, Burlingame, CA) according to the manufacturer’s recommendations (Gonzalez et al. 2015). Microtiter plates (R & D Systems, Minneapolis, MN) were coated with an anti-rat NGF antibody. Sample and standard solutions were run in duplicate. A horseradish peroxidase-streptavidin conjugate was used to detect the antibody complex. Tetramethyl benzidine was the substrate and the enzyme activity was measured by the change in optical density. The NGF standard provided with this protocol generated a linear standard curve from 15 to 1000 pg/ml (R 2 = 0.998, p ≤ 0.0001) for tissue samples. The absorbance values of standards and samples were corrected by subtraction of the background absorbance due to nonspecific binding. No samples fell below the minimum detection limits of the assay and no samples were diluted prior to use. Curve fitting of standards and evaluation of NGF content of samples was performed using a least squares fit as previously described (Gonzalez et al. 2015; Schnegelsberg et al. 2010; Vizzard 2000a).
Conscious, Open Outlet, Continuous Fill Cystometry
Mice were anesthetized with isoflurane (3–4%), a lower midline abdominal incision was made, and polyethylene tubing (PE-10, Clay Adams, Parsippany, New Jersey) was inserted into the bladder dome and secured with a nylon purse-string sutures (6-zero) (Gonzalez et al. 2013; Schnegelsberg et al. 2010). The end of the PE tubing was heat flared, but the catheter did not extend into the bladder body or neck and it was not associated with inflammation or altered cystometric function (Gonzalez et al. 2013; Schnegelsberg et al. 2010). The distal end of the tubing was sealed, tunneled subcutaneously, and externalized at the back of the neck out of reach (Gonzalez et al. 2013; Schnegelsberg et al. 2010). Abdominal and neck incisions were closed with nylon sutures (6-zero). Mice recovered from survival surgery for 72 h before performing cystometry.
For cystometry in conscious mice, an unrestrained animal was placed in a Plexiglas cage with a wire bottom. Before the start of the recording, the bladder was emptied and the catheter was connected via a T-tube to a pressure transducer (Grass Model PT300, West Warwick, RI) and microinjection pump (Harvard Apparatus 22, South Natick, MA). A Small Animal Cystometry Lab Station (MED Associates, St. Albans, VT) was used for urodynamic measurements (Gonzalez et al. 2013; Schnegelsberg et al. 2010). Saline solution was infused at room temperature into the bladder at a rate of 25 μl/min to elicit repetitive bladder contractions. At least six reproducible micturition cycles were recorded after the initial stabilization period of 25–30 min (Gonzalez et al. 2013; Schnegelsberg et al. 2010). The following cystometric parameters were recorded in each animal: baseline pressure (pressure at the beginning of the bladder filling), threshold pressure (bladder pressure immediately prior to micturition), peak micturition pressure, intercontraction interval (ICI; time between micturition events), infused volume (IV), void volume (VV), and presence of non-voiding bladder contractions (NVCs) (Gonzalez et al. 2013; Schnegelsberg et al. 2010). NVCs were defined as rhythmic intravesical pressure increases 5 cm H20 above baseline, during the filling phase, without the release of fluid from the urethra. Mice in these studies had residual volume of less than 5 μl. At the conclusion of the experiment, the mouse was euthanized (5% isoflurane plus thoracotomy).
Conscious Cystometry and Effects of a PAC1 Selective Receptor Antagonist, PACAP(6–38), on Bladder Function in NGF-OE Mice
The effects of PACAP(6–38), a PAC1 selective receptor antagonist, on urinary bladder function in littermate WT and NGF-OE mice, were assessed using conscious, open outlet, cystometry with continuous instillation of intravesical saline (Gonzalez et al. 2013; Merrill et al. 2013b; Schnegelsberg et al. 2010). Two groups of mice were evaluated: WT mice receiving intravesical administration of vehicle (0.9% saline) and PACAP(6–38) (n = 8) and NGF-OE mice receiving intravesical administration of vehicle (0.9% saline) and PACAP(6–38) (n = 8). For intravesical administration of PACAP(6–38), mice were anesthetized with 2% isoflurane and PACAP(6–38) (<1.0 ml) was injected through the bladder catheter; the animals were maintained under anesthesia to prevent expulsion of PACAP(6–38) via a voiding reflex. In this procedure, PACAP(6–38) remained in the bladder for 30 min at which time, the drug was drained, the bladder washed with saline and animals recovered from anesthesia for 20 min before experimentation. These experiments were performed in the same mice before and after treatment with PACAP(6–38). The concentration (300 nM) of PACAP(6–38) (Bachem, Torrance, CA) used in these studies was based upon previous studies (Braas et al. 2006) and pilot studies. To summarize, the experimental design involves administration of a one time, intravesical infusion of PACAP(6–38) (300 nM) with cystometric data collection occurring ∼75 min after infusion. At the conclusion of the experiment, the animal was euthanized (5% isoflurane plus thoracotomy). Experiments were conducted at similar times of the day to avoid the possibility that circadian variations were responsible for changes in bladder capacity measurements. An individual blinded to genotype analyzed the cystometric data; groups were decoded after data analysis.
Exclusion Criteria
Mice were removed from the study when adverse events occurred that included a significant postoperative event, lethargy, pain, or distress not relieved by our IACUC-approved regimen of pre- and/or postoperative analgesics (Gonzalez et al. 2013; Schnegelsberg et al. 2010). In the present study, no mice were excluded from the study. In addition, behavioral movements such as grooming, standing, walking, and defecation rendered bladder pressure recordings during these events unusable.
Mechanical Sensitivity Testing
Referred (secondary) hyperalgesia was measured by testing the frequency of withdrawal responses to the application of calibrated von Frey monofilaments to the abdomen (Cheppudira et al. 2009; Schnegelsberg et al. 2010) region overlying the urinary bladder with PACAP antagonist, PACAP(6–38) (300 nM) delivered intravesically via a transurethral catheter. Four separate groups (n = 10 each) of mice were evaluated: WT mice with vehicle, NGF-OE mice with vehicle, WT mice with PACAP(6–38), and NGF-OE mice with PACAP(6–38). For these studies, a transurethral bladder catheterization method was used to avoid the need for an abdominal incision as well as due to potential confounding effects of repeated catheterization and somatic sensitivity testing. In this procedure, PACAP(6–38) (<1 ml) remained in the bladder for 30 min at which time, the drug was drained, the bladder washed with saline, the catheter removed and animals recovered from anesthesia for 20 min before experimentation. Mechanical sensitivity assessment was performed using von Frey monofilaments (Stoelting, Wood Dale, IL) with forces of 0.1–4 g applied to the pelvic region (Cheppudira et al. 2009; Schnegelsberg et al. 2010). All mice were first habituated in a clear acrylic testing chamber 20 min/day for 4 days with a fan to generate ambient noise. On day of testing, the mice were placed in the acrylic testing chamber on top of a metal mesh floor (IITC Life Science Inc., Woodland Hills, CA) and habituated again for 10 min before the application of von Frey filaments in an up-down method for 1–3 s with a minimum interstimulus interval of 2 min (Cheppudira et al. 2009; Schnegelsberg et al. 2010). Stimulation was confined to the lower abdominal area overlying the urinary bladder. The following behaviors were considered positive responses to pelvic region stimulation: sharp retraction of the abdomen, jumping, or immediate licking or scratching of the pelvic area (Cheppudira et al. 2009; Schnegelsberg et al. 2010). Separate groups of mice were used for cystometry and somatic sensitivity testing. All mechanical sensitivity testing was performed in a blinded manner. The groups were decoded after data analysis.
Statistical Analyses
All values are means ± SEM. Comparisons among experimental groups were made using ANOVA. When F ratios exceeded the critical value (p ≤ 0.05), the Newman-Keul’s post hoc test was used to compare experimental means among groups.
Results
NGF Transcript and Protein Expression Is Increased in Urothelium of NGF-OE Mice with No Changes in Detrusor
NGF-OE transgenic mice developed normally with no adverse clinical signs or altered behaviors. Consistent with our previous studies (Girard et al. 2011, 2012, 2013; Schnegelsberg et al. 2010), NGF transcript and protein expression were significantly (p ≤ 0.001) increased in urothelium of NGF-OE mice with no changes in the detrusor (data not shown).
PAC1 Receptor Blockade with Intravesical Infusion of PACAP(6–38) Using Conscious Cystometry in NGF-OE and Littermate WT Mice
Conscious cystometry was performed in NGF-OE mice before intravesical infusion of PACAP(6–38) to establish baseline voiding frequency, intercontraction interval, and void volume (Figs. 1 and 2). As previously demonstrated (Girard et al. 2012; Schnegelsberg et al. 2010), NGF-OE mice exhibit increased voiding frequency and decreased void volume (VV; 3.8-fold) and intercontraction interval (ICI; 2.5-fold) compared with littermate WT mice (Figs. 1 and 2). Following intravesical infusion of the PAC1 receptor antagonist, PACAP(6–38) (300 nM), the same NGF-OE mice exhibited significantly (p ≤ 0.01) increased ICI (2.0-fold) and VV (2.8-fold) (Figs. 1 and 2). There was also a significant (p ≤ 0.01) decrease in maximum (i.e., peak) bladder pressure (BP) following intravesical instillation with PACAP(6–38) infusion in NGF-OE mice (Fig. 3). Intravesical infusion of vehicle in NGF-OE was without effect on the cystometric parameters evaluated (Figs. 1, 2, and 3). In littermate WT mice, no effects on cystometric parameters evaluated were observed with intravesical installation of PACAP(6–38) (300 nM) or vehicle (Figs. 2 and 3). Non-voiding contractions (NVCs; increases in baseline pressure with an amplitude ≥5 cm H2O without the expulsion of urine during the filling phase) were frequently observed in NGF-OE mice (Fig. 4). Consistent with previous studies, NGF-OE mice exhibited a significant (p ≤ 0.01) increase in the number of NVCs observed per voiding cycle compared to littermate WT mice (Fig. 4). Intravesical infusion of PACAP(6–38) (300 nM) reduced the number (2.6-fold) of NVCs observed in NGF-OE (Fig. 4). Intravesical infusion of vehicle in NGF-OE was without effect on NVCs (Fig. 4). Intravesical infusion of vehicle or PACAP(6–38) (300 nM) in littermate WT mice was without effect on NVCs (Fig. 4). All changes to urinary bladder function with intravesical instillation of PACAP(6–38) persisted for the duration of the data collection period (∼75 min).
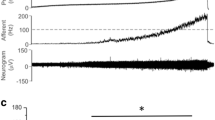
Representative bladder function recordings from the same NGF-OE mouse before and after intravesical instillation of PACAP(6–38) (300 nM). A1, A2 Prior to PACAP(6–38) instillation, NGF-OE mice exhibit greater voiding frequency and an increased number of non-voiding bladder contractions (NVCs) during the filling phase (arrows). B1, B2 After PACAP(6–38) instillation, NGF-OE mice exhibit a reduction in voiding frequency [i.e., increased intercontraction interval (ICI) and void volume (VV)], NVCs, and baseline (i.e., filling) bladder pressure
Summary histogram of void volume (VV) and intercontraction interval (ICI) measured from bladder function testing in WT (n = 8) and NGF-OE (n = 8) before and after intravesical instillation of PACAP(6–38) (300 nM). NGF-OE mice exhibited significantly (# p ≤ 0.01) reduced VV (a) and ICI (b) compared to littermate WT mice. PACAP(6–38) significantly (*p ≤ 0.01) increased VV (a) and ICI (b) in NGF-OE mice. PACAP(6–38) was without effect in WT mice
Summary histogram of bladder pressure (BP) measured from bladder function testing in WT (n = 8) and NGF-OE (n = 8) before and after intravesical instillation of PACAP(6–38) (300 nM). NGF-OE and littermate WT mice exhibit similar BP. In NGF-OE mice, intravesical instillation of PACAP(6–38) significantly (*p ≤ 0.01) reduced baseline (i.e., filling) bladder pressure with no effects on threshold pressure or maximum pressure. PACAP(6–38) was without effect on bladder pressure in WT mice
Summary histogram of the number of non-voiding contractions (NVCs) measured from bladder function testing in WT (n = 8) and NGF-OE (n = 8) before and after intravesical instillation of PACAP(6–38) (300 nM). NGF-OE mice exhibited a significantly (# p ≤ 0.01) greater number of NVCs per voiding cycle compared to littermate WT mice. PACAP(6–38) significantly (*p ≤ 0.01) reduced the number of NVCs during the filling phase. PACAP(6–38) was without effect in WT mice
Pelvic Somatic Sensitivity in NGF-OE Mice and Effects of Intravesical Infusion of the PAC1 Receptor Antagonist, PACAP(6–38)
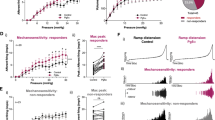
Consistent with previous studies (Schnegelsberg et al. 2010), pelvic somatic sensitivity was significantly (p ≤ 0.01) increased in NGF-OE mice compared to littermate WT mice at all monofilament forces evaluated (0.1 to 4 g) (Fig. 5). Intravesical infusion of PACAP(6–38) (300 nM) significantly (p ≤ 0.01) decreased the somatic sensitivity in the pelvic region in NGF-OE mice (Fig. 5). Intravesical infusion of vehicle was without effect on pelvic sensitivity in NGF-OE mice (Fig. 5). In littermate WT mice, intravesical infusion of PACAP(6–38) (300 nM) or vehicle produced no change in somatic sensitivity in the pelvic region (Fig. 5).
Pelvic region testing with calibrated von Frey hairs was determined in WT and NGF-OE mice. Stimulation was confined to the lower abdominal area overlying the urinary bladder. NGF-OE mice (n = 10) had a significantly (*p ≤ 0.01) increased pelvic response frequency with all von Frey hairs (0.1–4 g) tested compared with WT mice (n = 10). In NGF-OE mice, intravesical instillation of PACAP(6–38) significantly (*p ≤ 0.01) reduced pelvic response frequency with all von Frey filaments tested. No changes in pelvic sensitivity were observed in WT mice following intravesical PACAP(6–38) instillation. All somatic testing was performed in a blinded manner
Discussion
The current studies extend our understanding of the contributions of PACAP/PAC1 receptor signaling in lower urinary tract pathways in a mouse model with chronic urothelial overexpression of NGF. Intravesical administration of PACAP(6–38) (300 nM) significantly increased void volume and intercontraction interval and decreased filling pressure in NGF-OE mice with no effects on WT mice. Intravesical administration of PACAP(6–38) (300 nM) significantly reduced pelvic sensitivity in NGF-OE mice but was without effect in WT mice. PACAP/receptor signaling contributes to the increased voiding frequency and pelvic sensitivity observed in NGF-OE mice. These studies suggest that targeting PACAP/PAC1 signaling in micturition pathways may be one way to improve urinary bladder function and reduce referred pelvic sensation in urological disorders including BPS/IC.
Our previous studies have examined the expression of PACAP, VIP, and associated receptors in the urinary bladder and lumbosacral DRG of NGF-OE mice (Girard et al. 2010). We demonstrated upregulation of PAC1 receptor transcript and PAC1-immunoreactivity (IR) in urothelium of NGF-OE mice whereas PACAP transcript and PACAP-IR were decreased in urothelium (Girard et al. 2010). These data are consistent with previous studies demonstrating that NGF increases PAC1 mRNA levels in rat PC12 cells (Jamen et al. 2000, 2002) and that reduced PAC1 receptor mRNA expression is present in NGF null embryos (Andres et al. 2008). In contrast, VIP transcript and VPAC1 receptor transcript was not changed or decreased, respectively, in urothelium and detrusor smooth muscle of NGF-OE mice (Girard et al. 2010). VPAC2 receptor transcript was significantly increased in the detrusor smooth muscle in NGF-OE mice (Girard et al. 2010). No changes in VIP, PACAP, or associated receptors transcript expression were observed in lumbosacral DRG of WT or NGF-OE mice (Girard et al. 2010). In contrast, enhanced target-derived NGF availability has been shown to increase PACAP expression in small nociceptive neurons in DRG (Jongsma et al. 2001, 2003). Changes in PACAP, VIP, and associated receptors transcripts and protein expression in micturition pathways of NGF-OE mice resemble some, but not all, changes observed after CYP-induced cystitis (Girard et al. 2008) known to involve NGF production (Bjorling et al. 2001; Guerios et al. 2008; Klinger and Vizzard 2008; Vizzard 2000b). Given the presence of PAC1-IR nerve fibers (Braas et al. 2006) and PAC1 receptor expression in bladder tissues (Braas et al. 2006; Girard et al. 2010), PACAP-facilitated detrusor contractility (Braas et al. 2006), and increased PAC1-IR and transcript in the urothelium of NGF-OE mice (Girard et al. 2010), we evaluated whether blockade of PACAP/PAC1 signaling at the level of the urinary bladder could affect bladder function and pelvic sensitivity in NGF-OE mice.
PACAP peptides have diverse functions in the endocrine, nervous, gastrointestinal, and cardiovascular systems (Arimura 1998; Braas and May 1996) and differential effects on nociception (Sandor et al. 2009) through PAC1, VPAC1, and VPAC2 G protein-coupled receptors. PACAP and VIP are expressed in CNS neurons and in sensory DRG, autonomic ganglia (Arimura 1998; Arimura et al. 1991; Beaudet et al. 1998; Braas et al. 1998; May et al. 1998; Moller et al. 1997a, b; Sundler et al. 1996) and target tissues including the urinary bladder (Fahrenkrug and Hannibal 1998a, b; Mohammed et al. 2002). PACAP and VIP peptides regulate smooth muscle function, either directly or by facilitating cholinergic and nitric oxide mechanisms, in a tissue- and species-specific manner (Fox-Threlkeld et al. 1999; Mizumoto et al. 1992; Onaga et al. 1998; Seebeck et al. 2002; Zizzo et al. 2004). A number of studies have implicated PACAP/receptor expression and signaling in lower urinary tract function (Braas et al. 2006; Girard et al. 2008, 2010, 2012; Herrera et al. 2006; Vizzard 2000b; Zvara and Vizzard 2007). Our previous studies using a rat CYP-induced cystitis paradigm (Braas et al. 2006), intrathecal or intravesical administration of PAC1 receptor antagonist, PACAP(6–38), reduced cystitis-induced urinary frequency as well as the number and amplitude of NVCs. In the current study, intravesical instillation of PACAP(6–38) similarly improved urinary bladder function in NGF-OE mice. Although the site(s) of action of PACAP(6–38) is not known, PACAP(6–38) may affect PACAP/PAC1 signaling at the urothelium, in peripheral nerve terminals of DRG cells located in close proximity to the urothelium and/or detrusor smooth muscle cells each with demonstrated PAC1 expression (Braas et al. 2006). Given the high transepithelial resistance of the urothelium and the potential inability of the PAC1 receptor antagonist to reach the detrusor, a likely site of initial action is the urothelium; however, effects on nerve terminals and detrusor smooth muscle cells cannot be ruled out. In addition, subsequent to PACAP(6–38) instillation, the activation of signaling pathways from the urothelium to nerve terminals and/or detrusor is also possible. Reductions in baseline (i.e., filling) pressure after intravesical instillation of PACAP(6–38) suggest that detrusor smooth muscle cells may also be potential sites of action. The results of future studies involving protamine sulfate (to disrupt the urothelial barrier) (Greenwood-Van et al. 2015; Klinger and Vizzard 2008) plus intravesical instillation of PACAP(6–38) would be informative when compared to the data generated in this study. In addition, labeled PACAP(6–38) could also be intravesically instilled to evaluate tissue distribution within the urinary bladder under various conditions.
The improvement in urinary bladder function in NGF-OE mice demonstrated in the present study is not unique to blockade of PACAP/PAC1 receptor signaling. Recent studies (Girard et al., submitted) from our laboratory also demonstrated that intravesical instillation of a NK-1 receptor antagonist, netupitant (0.1 μg/ml), significantly increased void volume and the interval between micturition events with no effects on bladder pressure (baseline, threshold, maximum) in NGF-OE mice. However, effects on baseline (i.e., filling) pressure were only observed with intravesical PACAP(6–38) instillation. This difference suggests that some effects of blockade of PACAP/PAC1 signaling in the NGF-OE mouse may be unique to PACAP/PAC1 signaling and reflective of differential receptor distribution at the level of the bladder neck and/or urethra. Given the beneficial effects of either a PAC1 receptor antagonist or a NK-1 receptor antagonist (Girard et al., submitted) on urinary bladder function in NGF-OE mice, future studies involving intravesical instillation of both antagonists would be of interest to determine the magnitude of change in bladder function parameters compared to each antagonist alone. In addition to improvements in urinary bladder function in NGF-OE mice, intravesical instillation of PACAP(6–38) also reduced pelvic sensitivity as determined with monofilament testing. We previously demonstrated and confirmed here that NGF-OE mice exhibit increased pelvic sensitivity but demonstrated no differences in hindpaw sensitivity compared to littermate WT mice (Schnegelsberg et al. 2010). Thus, NGF-OE mice do not exhibit a generalized increased in somatic sensitivity but demonstrate increased sensitivity to the lower abdominal region overlying the urinary bladder (Schnegelsberg et al. 2010). These studies demonstrate beneficial effects of intravesical PACAP(6–38) instillation on both pelvic organ function and somatic sensation.
Although the etiology and pathogenesis of BPS/IC are unknown, numerous theories including infection, inflammation, autoimmune disorder, toxic urinary agents, urothelial dysfunction, and neurogenic causes have been proposed (Clemens et al. 2014; Hanno and Sant 2001; Landis et al. 2014). We have hypothesized that pain associated with BPS/IC involves an alteration of visceral sensation/bladder sensory physiology. Altered visceral sensations from the urinary bladder (i.e., pain at low or moderate bladder filling) that accompany BPS/IC (Clemens et al. 2014; Hanno and Sant 2001; Landis et al. 2014) may be mediated by many factors including changes in the properties of peripheral bladder afferent pathways such that bladder afferent neurons respond in an exaggerated manner to normally innocuous stimuli (allodynia). These changes may be mediated, in part, by inflammatory changes in the urinary bladder. NGF has been implicated in the peripheral sensitization of nociceptors (Guerios et al. 2006, 2008; Mendell et al. 1999). Intravenous administration of a humanized monoclonal antibody that specifically inhibits NGF (tanezumab) in patients with BPS/IC demonstrates proof of concept by improving the global response assessment and reducing the urgency episode frequency (Evans et al. 2011). However, clinical trials involving systemic anti-NGF therapies for diverse pain conditions have halted enrollment due to incidence and risk of osteonecrosis (Evans et al. 2011). The need for additional lower urinary tract targets beyond NGF is clear. The present studies suggest that blockade of PACAP/PAC1 receptor interactions at the level of the urinary bladder may be an additional approach to reducing urinary frequency and pelvic pain in BPS/IC.
These studies using NGF-OE mice may also provide important information relevant to overactive bladder (OAB) and neurogenic voiding disorders. For example, NK-1 receptor antagonists have been used to improve bladder dysfunction in adult OAB and manage neurogenic disorders of micturition (Abdel-Gawad et al. 2001; Doi et al. 1999, 2000; Frenkl et al. 2010). The present studies suggest that blockade of PACAP/PAC1 receptor interactions may be an additional approach to reducing urinary frequency in OAB. We have previously demonstrated improvement in urinary bladder function in adult rats following chronic spinal cord injury (SCI) at thoracic level 8 with intrathecal administration of the PAC1 receptor antagonist, PACAP(6–38); however, intravesical instillation was without effect. Differential success with intrathecal versus intravesical administration may reflect neuroplasticity in the expression of PACAP/receptor expression and signaling following chronic SCI.
These studies provide insight into additional NGF-mediated pleiotropic changes that may contribute to urinary bladder dysfunction and pelvic hypersensitivity in a novel transgenic mouse model with chronic urothelial NGF-OE. These studies provide new insights into (1) the contributions of PACAP/PAC1 signaling to increased voiding frequency and somatic sensitivity in NGF-OE mice and (2) additional NGF-induced lower urinary tract targets with translational relevance to BPS/IC.
References
Abdel-Gawad M, Dion SB, Elhilali MM (2001) Evidence of a peripheral role of neurokinins in detrusor hyperreflexia: a further study of selective tachykinin antagonists in chronic spinal injured rats. J Urol 165:1739–1744
Andres R, Herraez-Baranda LA, Thompson J, Wyatt S, Davies AM (2008) Regulation of sympathetic neuron differentiation by endogenous nerve growth factor and neurotrophin-3. Neurosci Lett 431:241–246
Arimura A (1998) Perspectives on pituitary adenylate cyclase activating polypeptide (PACAP) in the neuroendocrine, endocrine, and nervous systems. Jpn J Physiol 48:301–331
Arimura A, Somogyvari-Vigh A, Miyata A, Mizuno K, Coy DH, Kitada C (1991) Tissue distribution of PACAP as determined by RIA: highly abundant in the rat brain and testes. Endocrinology 129:2787–2789
Arms L, Vizzard MA (2011) Neuropeptides in lower urinary tract function. Handb Exp Pharmacol:395–423
Beaudet MM, Braas KM, May V (1998) Pituitary adenylate cyclase activating polypeptide (PACAP) expression in sympathetic preganglionic projection neurons to the superior cervical ganglion. J Neurobiol 36:325–336
Bjorling DE, Jacobsen HE, Blum JR, et al. (2001) Intravesical Escherichia coli lipopolysaccharide stimulates an increase in bladder nerve growth factor. BJU Int 87:697–702
Braas KM, May V (1996) Pituitary adenylate cyclase-activating polypeptides, PACAP-38 and PACAP-27, regulation of sympathetic neuron catecholamine, and neuropeptide Y expression through activation of type I PACAP/VIP receptor isoforms. Ann N Y Acad Sci 805:204–216 discussion 217-208
Braas KM, May V, Harakall SA, Hardwick JC, Parsons RL (1998) Pituitary adenylate cyclase-activating polypeptide expression and modulation of neuronal excitability in guinea pig cardiac ganglia. J Neurosci 18:9766–9779
Braas KM, May V, Zvara P, et al. (2006) Role for pituitary adenylate cyclase activating polypeptide in cystitis-induced plasticity of micturition reflexes. Am J Physiol Regul Integr Comp Physiol 290:R951–R962
Cheppudira BP, Girard BM, Malley SE, et al. (2009) Involvement of JAK-STAT signaling/function after cyclophosphamide-induced bladder inflammation in female rats. Am J Physiol Renal Physiol. 297:F1038–F1044
Chuang YC, Fraser MO, Yu Y, Chancellor MB, de Groat WC, Yoshimura N (2001) The role of bladder afferent pathways in bladder hyperactivity induced by the intravesical administration of nerve growth factor. J Urol 165:975–979
Clemens JQ, Mullins C, Kusek JW, et al. (2014) The MAPP research network: a novel study of urologic chronic pelvic pain syndromes. BMC Urol 14:57
Clemow DB, Steers WD, McCarty R, Tuttle JB (1998) Altered regulation of bladder nerve growth factor and neurally mediated hyperactive voiding. Am J Phys 275:R1279–R1286
Corrow K, Girard BM, Vizzard MA (2010) Expression and response of acid-sensing ion channels in urinary bladder to cyclophosphamide-induced cystitis. Am J Physiol Renal Physiol 298:F1130–F1139
Dmitrieva N, McMahon SB (1996) Sensitisation of visceral afferents by nerve growth factor in the adult rat. Pain 66:87–97
Doi T, Kamo I, Imai S, et al. (1999) Effects of TAK-637, a tachykinin receptor antagonist, on lower urinary tract function in the guinea pig. Eur J Pharmacol 383:297–303
Doi T, Kamo I, Imai S, Okanishi S, Ikeura Y, Natsugari H (2000) Effects of TAK-637, a tachykinin receptor antagonist, on the micturition reflex in guinea pigs. Eur J Pharmacol 395:241–246
Evans RJ, Moldwin RM, Cossons N, Darekar A, Mills IW, Scholfield D (2011) Proof of concept trial of tanezumab for the treatment of symptoms associated with interstitial cystitis. J Urol 185:1716–1721
Fahrenkrug J, Hannibal J (1998a) PACAP in visceral afferent nerves supplying the rat digestive and urinary tracts. Ann N Y Acad Sci 865:542–546
Fahrenkrug J, Hannibal J (1998b) Pituitary adenylate cyclase activating polypeptide immunoreactivity in capsaicin-sensitive nerve fibres supplying the rat urinary tract. Neuroscience 83:1261–1272
Fox-Threlkeld JA, McDonald TJ, Woskowska Z, Iesaki K, Daniel EE (1999) Pituitary adenylate cyclase-activating peptide as a neurotransmitter in the canine ileal circular muscle. J Pharmacol Exp Ther 290:66–75
Frenkl TL, Zhu H, Reiss T, Seltzer O, Rosenberg E, Green S (2010) A multicenter, double-blind, randomized, placebo controlled trial of a neurokinin-1 receptor antagonist for overactive bladder. J Urol 184:616–622
Girard BM, May V, Bora SH, Fina F, Braas KM (2002) Regulation of neurotrophic peptide expression in sympathetic neurons: quantitative analysis using radioimmunoassay and real-time quantitative polymerase chain reaction. Regul Pept. 109(1-3):89–101
Girard BM, Wolf-Johnston A, Braas KM, Birder LA, May V, Vizzard MA (2008) PACAP-mediated ATP release from rat urothelium and regulation of PACAP/VIP and receptor mRNA in micturition pathways after cyclophosphamide (CYP)-induced cystitis. J Mol Neurosci 36:310–320
Girard BM, Malley SE, Braas KM, May V, Vizzard MA (2010) PACAP/VIP and receptor characterization in micturition pathways in mice with overexpression of NGF in urothelium. J Mol Neurosci 42:378–389
Girard BM, Malley SE, Vizzard MA (2011) Neurotrophin/receptor expression in urinary bladder of mice with overexpression of NGF in urothelium. Am J Physiol Renal Physiol. 300:F345–F355
Girard BM, Tompkins JD, Parsons RL, May V, Vizzard MA (2012) Effects of CYP-induced cystitis on PACAP/VIP and receptor expression in micturition pathways and bladder function in mice with overexpression of NGF in urothelium. J Mol Neurosci 48:730–743
Girard BM, Merrill L, Malley S, Vizzard MA (2013) Increased TRPV4 expression in urinary bladder and lumbosacral dorsal root ganglia in mice with chronic overexpression of NGF in urothelium. J Mol Neurosci 51:602–614
Gonzalez EJ, Girard BM, Vizzard MA (2013) Expression and function of transforming growth factor-beta isoforms and cognate receptors in the rat urinary bladder following cyclophosphamide-induced cystitis. Am J Physiol Renal Physiol 305:F1265–F1276
Gonzalez EJ, Peterson A, Malley S, et al. (2015) The effects of tempol on cyclophosphamide-induced oxidative stress in rat micturition reflexes. ScientificWorldJournal 2015:545048
Greenwood-Van Meerveld B, Mohammadi E, Tyler K, et al. (2015) Mechanisms of visceral organ crosstalk: importance of alterations in permeability in rodent models. J Urol 194:804–811
Guerios SD, Wang ZY, Bjorling DE (2006) Nerve growth factor mediates peripheral mechanical hypersensitivity that accompanies experimental cystitis in mice. Neurosci Lett 392:193–197
Guerios SD, Wang ZY, Boldon K, Bushman W, Bjorling DE (2008) Blockade of NGF and trk receptors inhibits increased peripheral mechanical sensitivity accompanying cystitis in rats. Am J Physiol Regul Integr Comp Physiol. 295:R111–R122
Hanno PM, Sant GR (2001) Clinical highlights of the National Institute of Diabetes and Digestive and Kidney Diseases/Interstitial Cystitis Association scientific conference on interstitial cystitis. Urology 57:2–6
Herrera GM, Braas KM, May V, Vizzard MA (2006) PACAP enhances mouse urinary bladder contractility and is upregulated in micturition reflex pathways after cystitis. Ann N Y Acad Sci 1070:330–336
Hu VY, Zvara P, Dattilio A, et al. (2005) Decrease in bladder overactivity with REN1820 in rats with cyclophosphamide induced cystitis. J Urol 173:1016–1021
Huang EJ, Reichardt LF (2001) Neurotrophins: roles in neuronal development and function. Annu Rev Neurosci 24:677–736
Jaggar SI, Scott HC, Rice AS (1999) Inflammation of the rat urinary bladder is associated with a referred thermal hyperalgesia which is nerve growth factor dependent. Br J Anaesth 83:442–448
Jamen F, Laden JC, Bouschet T, Rodriguez-Henche N, Bockaert J, Brabet P (2000) Nerve growth factor upregulates the PAC1 promoter by activating the MAP kinase pathway in rat PC12 cells. Ann N Y Acad Sci 921:390–394
Jamen F, Bouschet T, Laden JC, Bockaert J, Brabet P (2002) Up-regulation of the PACAP type-1 receptor (PAC1) promoter by neurotrophins in rat PC12 cells and mouse cerebellar granule cells via the Ras/mitogen-activated protein kinase cascade. J Neurochem 82:1199–1207
Jongsma Wallin H, Danielsen N, Johnston JM, Gratto KA, Karchewski LA, Verge VM (2001) Exogenous NT-3 and NGF differentially modulate PACAP expression in adult sensory neurons, suggesting distinct roles in injury and inflammation. Eur J Neurosci 14:267–282
Jongsma Wallin H, Pettersson LM, Verge VM, Danielsen N (2003) Effect of anti-nerve growth factor treatment on pituitary adenylate cyclase activating polypeptide expression in adult sensory neurons exposed to adjuvant induced inflammation. Neuroscience 120:325–331
Klinger MB, Vizzard MA (2008) Role of p75NTR in female rat urinary bladder with cyclophosphamide-induced cystitis. Am J Physiol Renal Physiol 295:F1778–F1789
Klinger MB, Girard B, Vizzard MA (2008) p75NTR expression in rat urinary bladder sensory neurons and spinal cord with cyclophosphamide-induced cystitis. J Comp Neurol 507:1379–1392
Landis JR, Williams DA, Lucia MS, et al. (2014) The MAPP research network: design, patient characterization and operations. BMC Urol 14:58
Liang FX, Bosland MC, Huang H, et al. (2005) Cellular basis of urothelial squamous metaplasia: roles of lineage heterogeneity and cell replacement. J Cell Biol 171:835–844
Lin JH, Zhao H, Sun TT (1995) A tissue-specific promoter that can drive a foreign gene to express in the suprabasal urothelial cells of transgenic mice. Proc Natl Acad Sci U S A 92:679–683
Lowe EM, Anand P, Terenghi G, Williams-Chestnut RE, Sinicropi DV, Osborne JL (1997) Increased nerve growth factor levels in the urinary bladder of women with idiopathic sensory urgency and interstitial cystitis. Br J Urol 79:572–577
May V, Vizzard MA (2010) Bladder dysfunction and altered somatic sensitivity in PACAP−/− mice. J Urol 183:772–779
May V, Beaudet MM, Parsons RL, et al. (1998) Mechanisms of pituitary adenylate cyclase activating polypeptide (PACAP)-induced depolarization of sympathetic superior cervical ganglion (SCG) neurons. Ann N Y Acad Sci 865:164–175
Mendell LM, Albers KM, Davis BM (1999) Neurotrophins, nociceptors, and pain. Microsc Res Tech 45:252–261
Merrill L, Girard B, Arms L, Guertin P, Vizzard MA (2013a) Neuropeptide/Receptor expression and plasticity in micturition pathways. Curr Pharm Des 19:4411–4422
Merrill L, Malley S, Vizzard MA (2013b) Repeated variate stress in male rats induces increased voiding frequency, somatic sensitivity, and urinary bladder nerve growth factor expression. Am J Physiol Regul Integr Comp Physiol. 305:R147–R156
Mizumoto A, Fujimura M, Ohtawa M, et al. (1992) Pituitary adenylate cyclase activating polypeptide stimulates gallbladder motility in conscious dogs. Regul Pept 42:39–50
Mohammed H, Hannibal J, Fahrenkrug J, Santer R (2002) Distribution and regional variation of pituitary adenylate cyclase activating polypeptide and other neuropeptides in the rat urinary bladder and ureter: effects of age. Urol Res 30:248–255
Moller K, Reimer M, Ekblad E, et al. (1997a) The effects of axotomy and preganglionic denervation on the expression of pituitary adenylate cyclase activating peptide (PACAP), galanin and PACAP type 1 receptors in the rat superior cervical ganglion. Brain Res 775:166–182
Moller K, Reimer M, Hannibal J, Fahrenkrug J, Sundler F, Kanje M (1997b) Pituitary adenylate cyclase-activating peptide (PACAP) and PACAP type 1 receptor expression in regenerating adult mouse and rat superior cervical ganglia in vitro. Brain Res 775:156–165
Ng SY, Chow BK, Kasamatsu J, Kasahara M, Lee LT (2012) Agnathan VIP, PACAP and their receptors: ancestral origins of today’s highly diversified forms. PLoS ONE 7:e44691
Okragly AJ, Niles AL, Saban R, et al. (1999) Elevated tryptase, nerve growth factor, neurotrophin-3 and glial cell line-derived neurotrophic factor levels in the urine of interstitial cystitis and bladder cancer patients. J Urol 161:438–441 discussion 441-432
Onaga T, Harada Y, Okamoto K (1998) Pituitary adenylate cyclase-activating polypeptide (PACAP) induces duodenal phasic contractions via the vagal cholinergic nerves in sheep. Regul Pept 77:69–76
Pezet S, McMahon SB (2006) Neurotrophins: mediators and modulators of pain. Annu Rev Neurosci 29:507–538
Sandor K, Bolcskei K, McDougall JJ, et al. (2009) Divergent peripheral effects of pituitary adenylate cyclase-activating polypeptide-38 on nociception in rats and mice. Pain 141:143–150
Schnegelsberg B, Sun TT, Cain G, et al. (2010) Overexpression of NGF in mouse urothelium leads to neuronal hyperinnervation, pelvic sensitivity, and changes in urinary bladder function. Am J Physiol Regul Integr Comp Physiol. 298:R534–R547
Seebeck J, Lowe M, Kruse ML, et al. (2002) The vasorelaxant effect of pituitary adenylate cyclase activating polypeptide and vasoactive intestinal polypeptide in isolated rat basilar arteries is partially mediated by activation of nitrergic neurons. Regul Pept 107:115–123
Studeny S, Cheppudira BP, Meyers S, et al. (2008) Urinary bladder function and somatic sensitivity in vasoactive intestinal polypeptide (VIP)-/- mice. J Mol Neurosci 36:175–187
Sundler F, Ekblad E, Hannibal J, et al. (1996) Pituitary adenylate cyclase-activating peptide in sensory and autonomic ganglia: localization and regulation. Ann N Y Acad Sci 805:410–426 discussion 427-418
Vizzard MA (2000a) Changes in urinary bladder neurotrophic factor mRNA and NGF protein following urinary bladder dysfunction. Exp Neurol 161:273–284
Vizzard MA (2000b) Up-regulation of pituitary adenylate cyclase-activating polypeptide in urinary bladder pathways after chronic cystitis. J Comp Neurol 420:335–348
Zizzo MG, Mule F, Serio R (2004) Interplay between PACAP and NO in mouse ileum. Neuropharmacology 46:449–455
Zvara P, Vizzard MA (2007) Exogenous overexpression of nerve growth factor in the urinary bladder produces bladder overactivity and altered micturition circuitry in the lumbosacral spinal cord. BMC Physiol 7:9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was funded by National Institutes of Health (NIH) grants DK051369 (MAV), DK060481 (MAV), and DK065989 (MAV). This publication was also supported by grants from the National Center for Research Resources (5 P30 RR 032135) and the National Institute of General Medical Sciences (8 P30 GM 103498) from the NIH.
Conflict of Interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Girard, B.M., Malley, S.E., Mathews, M.M. et al. Intravesical PAC1 Receptor Antagonist, PACAP(6–38), Reduces Urinary Bladder Frequency and Pelvic Sensitivity in NGF-OE Mice. J Mol Neurosci 59, 290–299 (2016). https://doi.org/10.1007/s12031-016-0764-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-016-0764-1