Abstract
During development, anesthetics activate neuroapoptosis and produce damage in the central nervous system that leads to several types of neurological disorders. A single dose of ketamine (40 mg/kg) during synaptogenesis in a 7-day-old rat brain activated the apoptotic cascade and caused extensive neuronal cell death in the forebrain. In this study, we investigated the protective effect of nicotinamide against ketamine-induced apoptotic neurodegeneration. After 4 h, neuronal cell death induced by ketamine was associated with the induction of Bax, release of cytochrome c into the cytosol, and activation of caspase-3. One single dose of 1 mg/g nicotinamide was administered to a developing rat and was found to inhibit ketamine-induced neuroapoptosis by downregulating Bax, inhibiting cytochrome c release from mitochondria into cytosol, and inhibiting the expression of activated caspase-3. TUNEL and immunohistochemical analyses showed that ketamine-induced cell death occurred through apoptosis and that it was inhibited by nicotinamide. Fluoro-Jade-B staining demonstrated an increased number of dead cells in the cortex and thalamus after ketamine treatment; treatment with nicotinamide reduced the number of dead cells in these brain regions. Our findings suggest that nicotinamide attenuated ketamine-induced neuronal cell loss in the developing rat brain and is a promising therapeutic and neuroprotective agent for the treatment of neurodevelopmental disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ketamine ((±)-2-(2-chlorophenyl)-2-(methylamino) cyclohexanone) is the most common agent used in emergency departments (EDs) to provide sedation/analgesia to children for painful procedures (Bhargava and Young 2007; Krauss and Green 2006). During the peak of development (i.e., synaptogenesis), transient exposure of immature developing rodent brains to anesthetic drugs including N-methyl-d-aspartate (NMDA) glutamate receptor antagonists and γ-amino butyric acid type A (GABAA)) receptor agonists, such as ethanol, which has both NMDA antagonist and GABA mimetics properties, triggered extensive apoptosis in neurons (Ikonomidou et al. 1999; Wozniak et al. 2004). Commonly used general anesthetic agents such as barbiturates, benzodiazepines, ketamine, isoflurane, and nitrous oxide, caused considerable and widespread neuronal death and learning/memory deficits (Ikonomidou et al. 1999; Jevtovic-Todorovic et al. 2003). Excessive suppression of neuronal activity by ketamine during the brain growth spurt activated apoptosis in neurons (Ikonomidou et al. 1999; Jevtovic-Todorovic et al. 2003; Olney et al. 2002).
Nicotinamide, an amide of vitamin B3, is the precursor for coenzyme β-nicotinamide adenine dinucleotide, NAD+, and is considered to be necessary for cellular functions and metabolism (Maiese and Chong 2003). Preclinical efficacy of nicotinamide is well known, but the exact molecular mechanism of neuroprotection remains to be elucidated. As a result of severe cellular insult, the activity of poly ADP-ribose polymerase, PARP-1, increased, which caused NAD+ depletion and apoptosis (Burkle 2001). In the presence of nicotinamide, NAD+ stores and DNA damage were restored (Maiese and Chong 2003; Ayoub et al. 1999). Nicotinamide improved neuronal survival during or after a variety of insults as a result of free radical exposure and oxidative stress (Mukherjee et al. 1997; Klaidman et al. 2001), and its protective function is a result of many pharmacological effects including lipid peroxidation (Klaidman et al. 2001; Chong et al. 2004) and stabilization of the mitochondrial membrane potential, which prevents cytochrome c release into the cytosol and inhibits caspase-9 and caspase-3like activity (Mukherjee et al. 1997; Chong et al. 2004; Chong et al. 2002). Furthermore, nicotinamide inhibited the activation of PARP-1 and the prevention of apoptosis (Klaidman et al. 2003; Yang et al. 2002b; Ungerstedt et al. 2003).
The removal of ketamine and other anesthetic drugs from clinical use would impair our ability to care for children in the ED, the operating room, and any other location where sedation, analgesia, and anxiolysis are needed. Therefore, caution needs to be taken during animal studies that focus on the clinical perspective, particularly the use of neuroprotective agents. To understand the precise molecular mechanisms that initiate the ketamine-induced neurodegeneration and the development of neuroprotective therapeutics, it is important to improve the neurological outcome of neonates and infants experiencing anesthesia-induced neurotoxicity. This study examined the protective role of nicotinamide on ketamine-induced neurodegeneration in developing rats. Our investigation revealed that nicotinamide effectively suppressed ketamine-induced apoptosis in developing rat brains.
Materials and Methods
Animals
Seven-day-old Sprague–Dawley rat pups (average body weight of 14–16 g) were used in all experimental paradigms and were equally distributed in four different groups, i.e., control, ketamine, nicotinamide, and ketamine + nicotinamide. The number of animals and their suffering was minimized. All the experimental procedures were approved by the local animal ethics committee of the Division of Applied Life Sciences, Department of Biology, Gyeongsang National University South Korea.
Drug Treatment
Developing rats were injected subcutaneously with 40 mg/kg ketamine and 1 mg/g of nicotinamide at different time points, i.e., (−2 h) pretreatment, (0 h) cotreatment and (+2 h) posttreatment. Animals were sacrificed 4–24 h posttreatment. Saline injection of equal volume was used as the control.
Western Blot Analysis
Equivalent amounts of protein, 30 μg per sample, were loaded onto 10–15% SDS PAGE gels under reducing conditions and transferred onto a polyvinylidene difluoride (PVDF) membrane (Santa Cruz Biotechnology, Santa Cruz, CA, USA). Prestained protein marker, broad range: 6–175 kDa (New England Biolabs, Inc., Ipswich, MA, USA), was electrophoresed in parallel to detect the molecular weights of the proteins. The membrane was blocked with 5% (w/v) skim milk to reduce the nonspecific binding, and immunoblotting was performed using rabbit-derived antiBcl2, antiBax, and anticaspase-3 and goat-derived polyclonal anticytochrome c (1:500; Santa Cruz Biotechnology, Santa Cruz, CA, USA). Antiβ-actin antibody (1:500; Sigma, St. Louis, MO, USA) was used as a control to confirm equal loading. The membrane was probed with a goat-derived horseradish peroxidase-conjugated antirabbit IgG (1:1,000; Santa Cruz Biotechnology, Santa Cruz, CA, USA), and immunocomplexes were visualized using enhanced chemiluminescence ECL-detecting reagent (Amersham Pharmacia Biotech, western blotting detection reagents). The optical densities of the western blot bands were analyzed by densitometry using the computer-based Sigma Gel, version 1.0 (Jandel Scientific, San Rafeal, Chicago, USA).
Tissue Collection and Sample Preparation
For morphological analysis, animals were sacrificed 24 h after drug treatment. The brain sections from control rats and rats injected with ketamine and nicotinamide for 24 h were analyzed. For tissue analysis (n = 3–4 per group), developing rat pups were transcardially perfused with 1× PBS followed by 4% ice-cold paraformaldehyde, and the brains were removed and postfixed in 4% paraformaldehyde overnight and then transferred to 20% sucrose until the brains sank to the bottom of the tube. Brains were frozen in O.C.T compound (A.O. USA), and 14-μm sections were sliced in the coronal plane (Leica cryostat CM 3050 C, Germany). Sections were thaw-mounted on the probe-on plus charged slide (Fisher).
Immunohistochemical Staining
Immunohistochemical analysis with some modification was performed to reveal the activation of caspase-3 as previously described by Young et al. (2005). The slides were washed in 0.01 M PBS, quenched for 10 min in methanol containing 3% hydrogen peroxide, and then incubated for 1 h in blocking solution (2% BSA/0.2% milk/0.1% Triton-X 100 in PBS) followed by incubation overnight in rabbit antiactive caspase-3 antiserum (Cell Signaling Technology, Beverly, MA) diluted 1:1,000 in blocking solution. Following incubation with primary antiserum, the sections were incubated for 90 min in secondary antiserum (goat antirabbit 1:200 in blocking solution) and then reacted in the dark with ABC reagents (standard Vectastain ABC Elite Kit; Vector Laboratories, Burlingame, CA) for 90 min. The sections were washed two times with PBS and incubated with VIP reagent (Vector VIP substrate kit for peroxidase, Vector Labs, Burlingame, CA) until the reaction turned purple. Images were viewed on a fluorescence light microscope. Active caspase-3-positive cells in the cortex and thalamus were counted by observer blinded to the treatment conditions.
Fluoro-Jade-B (FJB) Staining
Fluoro-Jade-B (FJB) staining, with some modification, was performed as previously described by Sas et al. (2008). Twenty-four hours following drug treatment, animals were deeply anesthetized and transcardially perfused with 0.9% saline followed by ice-cold 4% paraformaldehyde in 0.1 M PBS. Briefly, brain sections were mounted on slides and then air-dried over night. The slides were immersed in a solution of 1% sodium hydroxide and 80% ethanol for 5 min, 70% alcohol for 2 min, and then 2 min in distilled water. Slides were transferred to 0.06% potassium permanganate solution for 10 min. After rinsing with water, slides were immersed in 0.1% acetic acid and 0.01% FJB (Chemicon International, USA) for 20 min. Slides were washed two times in distilled water and allowed to dry for 10 min. Glass coverslips were mounted on glass slides using mounting medium. Fluoro-Jade-B was detected using an FITC filter (Green color) on a confocal laser scanning microscope (Fluoview FV 1000, Olympus, Japan). FJB-positive cells in the cortex and thalamus were counted by an observer blinded to the treatment conditions.
TUNEL and DAPI Staining
Apoptotic cell death detection was performed using terminal deoxynucleotidyl transferase (TdT)-mediated dUTP nick end labeling (TUNEL) on cryosections (14 μm) of aggregates. TUNEL staining was performed according to supplier recommendations using an In Situ Cell Death Detection Kit, Fluorescein (GenScript, USA). Aggregate cryosections (16 μm) were then incubated with DAPI (Molecular Probes, Eugene, OR, USA) for 10 min at room temperature and then rinsed with distilled water. Glass cover slips were mounted on glass slides using mounting medium. TUNEL-positive (Green, FITC filter) and DAPI (Blue, DAPI filter)-staining patterns were acquired using a confocal laser scanning microscope (Fluoview FV 1000, Olympus, Japan). TUNEL-positive cells in the cortex and thalamus were counted by observer blinded to the treatment conditions.
Data Analysis and Statistics
The bands from western blots were scanned and analyzed by densitometry using the Sigma Gel System (SPSS, Inc., Chicago, IL). Density values were expressed as mean ± SEM. Statistical difference was determined using a one-way analysis of variance (ANOVA) followed by Student’s t-test. In all experiments, the acceptance level for statistical significance was considered P < 0.05.
Results
Effects of Nicotinamide on Ketamine-induced Upregulation of Bax Protein Levels in the Developing Rat Brain
Nicotinamide prevents neuronal cell apoptosis by regulating pro- and antiapoptotic proteins (Maiese and Chong 2003; Mukherjee et al. 2005). Therefore, we measured the levels of Bax and Bcl-2 in the cortex and thalamus of young rats following 4 h of ketamine treatment in the presence and absence of nicotinamide. Bax levels in the cortex and thalamus increased following ketamine treatment as compared to the control group. Treatment with nicotinamide significantly reversed the ketamine-induced increase of Bax (Fig. 1), whereas there was no significant change in expression level of Bcl-2 (data not shown). The effect of nicotinamide on the ketamine-induced increase was observed at different time points, i.e., (−2 h) pretreated, (0 h) cotreated, and (+2 h) posttreated. At all time points, the nicotinamide effects were strongest when cotreated with ketamine (Fig. 1). These results show that treatment with ketamine for 4 h resulted in an increase in the Bax/Bcl-2 ratio that leads toward neuroapoptosis, whereas nicotinamide supplementation significantly reduced the Bax/Bcl-2 ratio that leads toward neuroprotection (Fig. 6).
Effects of nicotinamide on ketamine-induced expression of Bax protein levels after 4 h. Representative western blot analysis shows expression levels of Bax in the cortex and thalamus of 7-day-old rats treated with 40 mg/kg ketamine in the absence or presence of nicotinamide, i.e., (−2 h) pretreatment, (0 h) cotreatment and (+2 h) posttreatment of 1 mg/g nicotinamide. The protein bands from the western blot were quantified using sigma gel software, and their differences are represented in the graph. Actin was used as a protein loading control. Density values are expressed as mean ± SEM (n = 4–6 animals/group) of Bax. The density values on the Y-axis are expressed as arbitrary units (AU). (a Significantly different from CTL, b significantly different from nicotinamide, c significantly different from ketamine + nicotinamide, d significantly different from ketamine). Significance = P < 0.05
Effects of Nicotinamide on Ketamine-induced Cytosolic Cytochrome c Protein Levels in the Developing Rat Brain
Translocation of mitochondrial cytochrome c into the cytosol induces the formation of the apoptosome and, subsequently, neuronal death (Li et al. 1997). Western blot analysis showed that after 4 h of ketamine treatment, there was an increase in the levels of cytosolic cytochrome c in the cortex and thalamus, whereas treatment with nicotinamide resulted in significantly reduced cytosolic cytochrome c levels compared to the ketamine treated group. Similar to its effects on Bax levels, nicotinamide was the most effective when cotreated with ketamine (Fig. 2).
Effects of nicotinamide on ketamine-induced cytosolic cytochrome c protein levels after 4 h. Representative western blot analysis shows cytosolic cytochrome c proteins levels in the cortex and thalamus of 7-day-old rats treated with ketamine in the absence or presence of nicotinamide. The protein bands from the western blot were quantified using sigma gel software, and their differences are represented in the graph. Actin was used as a protein loading control. Density values are expressed as mean ± SEM (n = 4–5 animals/group) of cytochrome c. The density values on the Y-axis are expressed as arbitrary units (AU). (a Significantly different from CTL, b significantly different from nicotinamide, c significantly different from ketamine + nicotinamide, d significantly different from ketamine). Significance = P < 0.05
Effects of Nicotinamide on the Expression of Activated Caspase-3 after 4 h of Ketamine Treatment in the Developing Rat Brain
Caspases are cysteine proteases that play a key role in apoptosis, and its increased expression and activation contribute to neuronal cell death (Rupinder et al. 2007). Western blot analysis showed that the levels of activated caspase-3 significantly increased in the cortex and thalamus of the developing rats following 4 h of ketamine administration compared to the control group treated with saline (Fig. 3a). Nicotinamide treatment with ketamine significantly decreased the level of activated caspase-3 in both brain regions compared to animals treated with ketamine alone.
a Effects of nicotinamide on ketamine-induced expression of activated caspase-3 protein levels after 4 h. Representative western blot analysis shows expression levels of activated caspase-3 protein in the developing rat brain treated with ketamine in the absence or presence of nicotinamide. Density values of cytochrome c and activated caspases-3 are expressed as mean ± SEM (n = 4–5 animals/group). The density values on the Y-axis are expressed as arbitrary units (AU). (a Significantly different from CTL, b significantly different from nicotinamide, c significantly different from ketamine + nicotinamide, d significantly different from ketamine). Significance = P < 0.05. b Effects of nicotinamide on ketamine-induced expression of activated caspase-3 after 24 h. Representative photomicrographs of immunohistochemical analysis show neuronal cells after treatment with ketamine in the absence or presence of nicotinamide. Representative images of staining were obtained from sections prepared from at least three to four animals per group. Panels a–f show caspase-3 stained brain tissue at a higher magnification of 40× objective field (scale bar = 100 μm). (a Significantly different from saline, b significantly different from ketamine + nicotinamide, c significantly different from ketamine). Significance = P < 0.05
Effects of Nicotinamide on the Expression of Activated Caspase-3 After 24 h of Ketamine Treatment in the Developing Rat Brain
In support of the western blot results for caspase-3, immunohistochemical analysis was used to investigate the role of activated caspase-3 in the pathogenesis of neuronal death. Twenty-four hours after ketamine treatment, numerous injured and dead neurons showed strong active caspase-3 immunoreactivity in the cingulate cortex and LDN of thalamus (Fig. 3b, subpanels b and e). Active caspase-3-positive cells in the cortex and thalamus were decreased when nicotinamide was treated with ketamine (Fig. 3b, subpanels c and f).
Effects of Nicotinamide on Ketamine-induced Apoptotic Neurodegeneration in the Developing Rat Brain After 24 h
Fluoro-Jade-B (FJB) was used to stain dead neurons because it is a reliable marker for neuronal vulnerability (Anderson et al. 2005). Many dead neuronal cells in the anterior cingulate cortex and LDN of thalamus were found 24 h after ketamine treatment. There was a significant increase in the total number of FJB-positive cells in the anterior cingulate cortex and LDN of the thalamus following ketamine treatment (Fig. 4, panels b and e). In contrast, rat pups that received nicotinamide with ketamine showed a significant reduction in the number of FJB-positive cells in these brain regions (Fig. 4, panels c and f).
Effects of nicotinamide on ketamine-induced neuronal cell death after 24 h. Representative photomicrographs of FJB staining show damaged and dead neuronal cells after 40 mg/kg ketamine treatment in the absence or presence of 1 mg/g nicotinamide. Images are representative of staining obtained in sections prepared from at least three to four animals per group. a–f FJB-stained brain tissue at higher magnification of 60× objective field (scale bar = 50 μm). (a Significantly different from CTL, b significantly different from nicotinamide, c significantly different from ketamine + nicotinamide, d significantly different from ketamine). Significance = P < 0.05
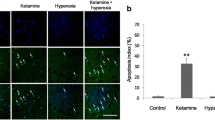
The nuclear morphology of the brain tissue was examined using TUNEL and DAPI staining to determine the ketamine-induced neuroapoptosis in the developing rat brain cortex and thalamus. Ketamine treatment increased the number of TUNEL positive cells in the cortex and thalamus (Fig. 5, panels b and f). When counterstained with DAPI, most of the TUNEL-positive cells in the cortex and thalamus showed apoptotic neuronal cell death with small multiDNA masses, which is a common feature of apoptosis (Fig. 5, panels c and g). Nicotinamide treatment with ketamine significantly reduced the number of TUNEL-positive cells in these brain regions (Fig. 5, panels d and h).
Effects of nicotinamide on ketamine-induced apoptotic neurodegeneration after 24 h. Representative photomicrographs of TUNEL staining show apoptotic dead neuronal cells following ketamine cotreated with nicotinamide. Representative images of staining were obtained from sections prepared from at least three to four animals per group. a–h TUNEL-stained brain tissue at a magnification of 60× objective field (scale bar = 20 μm). (a Significantly different from saline, b significantly different from ketamine + bicotinamide, c significantly different from ketamine). Significance = P < 0.05
Discussion
Exposure of newborn rat pups to anesthetic and anticonvulsant drugs leads to accelerated neurodegeneration and long-term behavioral, learning/memory deficits (Anand and Soriano 2004; Jevtovic-Todorovic et al. 2003). Ketamine, an NMDA receptor ion channel blocker, is a widely used anesthetic agent that was recently reported to enhance neuronal death in rats during the critical period of neuronal development, which resulted in neurotoxicity and neurodegeneration in several major brain areas (Ikonomidou et al. 1999; Scallet et al. 2004). Neurotoxicity in postnatal day 7 (PND-7) rats, presumably due to the dysregulation of NMDA receptors, has been proposed to be an important mechanism of apoptotic neurodegeneration induced by ketamine (Slikker et al. 2007; Wang et al. 2005; Wang et al. 2006). Exposure of developing brains to ketamine caused selective cell death through a compensatory upregulation of NMDA receptor subunits (Wang et al. 2005; Wang et al. 2006). Upregulation of NMDA receptors initiates a cascade that begins with Ca2+ influx, which produces an increase in reactive oxygen species (ROS), mitochondrial membrane depolarization and activation of an apoptotic cascade (Johnson et al. 1998; Slikker et al. 2005; Wang et al. 2000; Bernardi et al. 2006; O’Rourke et al. 2005).
Nicotinamide is necessary for cellular maintenance and acts as a cytoprotectant in the brain to prevent neurodegeneration induced by a variety of insults including oxidative stress (Maiese and Chong 2003; Yang et al. 2002a). Nicotinamide treatment with ketamine inhibited induction of the apoptotic cascade by blocking active caspase-3, which is responsible for the activation of PARP-1; therefore, this treatment interfered with NAD+ depletion as well as inhibited necrosis and other nonapoptotic cell death mechanisms (Ungerstedt et al. 2003; Chong et al. 2005). Our results show that nicotinamide inhibited ketamine-induced neuroapoptosis through downregulation of Bax, inhibition of cytochrome c translocation into the cytosol and inhibition of active caspase-3, which is involved in the activation of PARP-1 and formation of apoptotic bodies (Hengartner 2000; Zamzami and Kroemer 2001).
Immunohistochemical findings were consistent with the molecular results. Both western blotting and immunohistochemistry showed that ketamine treatment significantly increased the expression of active caspase-3 in the cortex and thalamus. TUNEL analysis also showed that the neuronal cell death induced by ketamine was apoptosis and was inhibited by nicotinamide. Nicotinamide can cross the blood–brain barrier (Klaidman et al. 1996) and function as a critical protective agent in various neurodegenerative diseases in which the mitochondrial apoptotic pathway is involved. Previously a similar pathway of apoptotic neurodegeneration by ethanol that share similar response to exogenous administration of nicotinamide is investigated by Laraci and Herrera (2006). In our results, we showed that at all time periods, nicotinamide showed its neuroprotective effect but the strongest effect was observed when it was cotreated with ketamine. In the present study, we found that nicotinamide cotreatment with ketamine in the developing rat brain was associated with a decrease in neuroapoptosis and improved brain histomorphological outcome.
Our results show that the protective effect of nicotinamide on ketamine-induced apoptosis involves the maintenance of mitochondrial integrity and the repression of Bax, inhibition of the mitochondrially-mediated release of cytochrome c into the cytosol, inhibition of activated caspase-3 and apoptosis (Fig. 6). This study showed the efficacy of nicotinamide in protecting against neuroapoptosis induced by ketamine and recommends it as a promising, safe neuroprotective agent for clinical use. We conclude from this study that nicotinamide treatment provides neuroprotection against ketamine in the developing rat brain, thereby preventing apoptotic neuronal cell death.
A schematic diagram showing that nicotinamide protects against ketamine-induced neurodegeneration in the brain of developing rats. Ketamine (red filled circle) that binds with GABA or NMDA receptors (blue filled rectangle) causes neurodegeneration by the production of ROS and activation of mitochondria-dependent apoptosis that is initiated by the upregulation of proapoptotic Bax, an increase in cytochrome c release from mitochondria to cytoplasm and induction of activated caspase-3. Nicotinamide, as indicated by the X sign, inhibits production of ROS by maintaining the mitochondrial membrane potential (∆Ψm) and inhibiting several key elements in the apoptotic cascade resulting in protection from ketamine-induced apoptotic cell death in the developing rat brain
References
Anand KJ, Soriano SG (2004) Anesthetic agents and the immature brain: are these toxic or therapeutic? Anesthesiology 101:527–530
Anderson KJ, Miller KM, Fugaccia I, Scheff SW (2005) Regional distribution of Fluoro-Jade B staining in the hippocampus following traumatic brain injury. Exp Neurol 193:125–130
Ayoub IA, Lee EJ, Ogilvy C, Flint BM, Maynard KI (1999) Nicotinamide reduces infarction up to two hours after the onset of permanent focal cerebral ischemia in wistar rats. Neurosci Lett 259:21–24
Bernardi P, Krauskopf A, Basso E, Petronilli V, Blachly-Dyson E, Di LF et al (2006) The mitochondrial permeability transition from in vitro artifact to disease target. FEBS J 273:2077–2099
Bhargava R, Young KD (2007) Procedural pain management patterns in academic pediatric emergency departments. Acad Emerg Med 14:479–482
Burkle A (2001) PARP-1: a regulator of genomic stability linked with mammalian longevity. Chembiochemistry 2:725–728
Chong ZZ, Lin SH, Maiese K (2002) Nicotinamide modulates mitochondrial membrane potential and cysteine protease activity during cerebral vascular endothelial cell injury. J Vasc Res 39:131–147
Chong ZZ, Lin SH, Maiese K (2004) The NAD + precursor nicotinamide governs neuronal survival during oxidative stress through protein kinase B coupled to FOXO3a and mitochondrial membrane potential. J Cereb Blood Flow Metab 24:728–743
Chong ZZ, Lin SH, Li F, Maiese K (2005) The sirtuin inhibitor nicotinamide enhances neuronal cell survival during acute anoxic injury through Akt, Bad, PARP, and mitochondrial associate “anti-apoptotic” pathways. Curr Neurovasc Res 2:271–285
Hengartner MO (2000) The biochemistry of apoptosis. Nature 407:770–776
Ikonomidou C, Bosch F, Miksa M, Bittigau P, Vockler J, Dikranian K et al (1999) Blockade of NMDA receptors and apoptotic neurodegeneration in the developing brain. Science 283:70–74
Jevtovic-Todorovic V, Hartman RE, Izumi Y, Benshoff ND, Dikranian K, Zorumski CF et al (2003) Early exposure to common anesthetic agents causes widespread neurodegeneration in the developing rat brain and persistent learning deficits. J Neurosci 23:876–882
Johnson KM, Phillips M, Wang C, Kevetter GA (1998) Chronic phencyclidine induces behavioral sensitization and apoptotic cell death in the olfactory and piriform cortex. J Neurosci Res 52:709–722
Klaidman LK, Mukherjee SK, Hutchin TP, Adams JD (1996) Nicotinamide as a precursor for NAD + prevents apoptosis in the mouse brain induced by tertiary-butylhydroperoxide. Neurosci Lett 206:5–8
Klaidman LK, Mukherjee SK, Adams JD (2001) Oxidative changes in brain pyridine nucleotides and neuroprotection using nicotinamide. Biochim Biophys Acta 1525:136–148
Klaidman L, Morales M, Kem S, Yang J, Chang ML, Adams JD (2003) Nicotinamide offers multiple protective mechanisms in stroke as a precursor for NAD+, as a PARP inhibitor and by partial restoration of mitochondrial function. Pharmacology 69:150–157
Krauss B, Green SM (2006) Procedural sedation and analgesia in children. Lancet 367:766–780
Laraci A, Herrera DG (2006) Nicotinamide protects against ethanol-induced apoptotic neurodegeneration in the developing mouse brain. PLoS Med 3:547–557
Li P, Nijhawan D, Budihardjo I, Srinivasula SM, Ahmad M, Alnemri ES et al (1997) Cytochrome c and dATP-dependent formation of Apaf-1/caspase-9 complex initiates an apoptotic protease cascade. Cell 91:479–489
Maiese K, Chong ZZ (2003) Nicotinamide: necessary nutrient emerges as a novel cytoprotectant for the brain. Trends Pharmacol Science 24:228–232
Mukherjee SK, Klaidman LK, Yasharel R, Adams JD (1997) Increased brain NAD prevents neuronal apoptosis in vivo. Eur J Pharmacol 330:27–34
Mukherjee S, Sonee M, Adams JD (2005) A review of the regulatory role of nicotinamide on pro- and anti-apoptotic proteins in neuronal cells. Lett Drug Des Discov 2:551–557
Olney JW, Tenkova T, Dikranian K, Muglia LJ, Jermakowicz WJ, D’Sa C et al (2002) Ethanol-induced caspase-3 activation in the in vivo developing mouse brain. Neurobiol Dis 9:205–219
O’Rourke B, Cortassa S, Aon MA (2005) Mitochondrial ion channels: gatekeepers of life and death. Physiology 20:303–315
Rupinder SK, Gurpreet AK, Manjeet S (2007) Cell suicide and caspases. Vascul Pharmacol 46:383–393
Sas K, Robotka H, Rozsa E, Agoston M, Szenasi G, Gigler G et al (2008) Kynurenine diminishes the ischemia-induced histological and electrophysiological deficits in the rat hippocampus. Neurobiol Dis 32:302–308
Scallet AC, Schmued LC, Slikker W, Grunberg N, Faustino PJ, Davis H et al (2004) Developmental neurotoxicity of ketamine: morphometric confirmation, exposure parameters, and multiple fluorescent labeling of apoptotic neurons. Toxicol Sci 81:364–370
Slikker W, Xu Z, Wang C (2005) Application of a systems biology approach to developmental neurotoxicology. Reprod Toxicol 19:305–319
Slikker W, Zou X, Hotchkiss CE, Divine RL, Sadovova N, Twaddle NC et al (2007) Ketamine-induced neurodegeneration in the perinatal rhesus monkey. Toxicol Sci 98:145–158
Ungerstedt JS, Blomback M, Soderdtom T (2003) Nicotinamide is a potent inhibitor of proinflammatory cytokines. Clin Exp Immunol 131:48–52
Wang C, Kaufmann JA, Sanchez-Ross MG, Johnson KM (2000) Mechanisms of N methyl-d-aspartate-induced apoptosis in phencyclidine treated cultured forebrain neurons. J Pharmacol Exp Ther 294:287–295
Wang C, Sadovova N, Fu X, Schmued L, Scallet A, Hanig J et al (2005) The role of the N-methyl-d-aspartate receptor in ketamine-induced apoptosis in rat forebrain culture. Neuroscience 132:967–977
Wang C, Sadovova N, Hotchkiss C, Fu X, Scallet AC, Patterson TA et al (2006) Blockade of N-methyl-d-aspartate receptors by ketamine produces loss of postnatal day 3 monkey frontal cortical neurons in culture. Toxicol Sci 91:192–201
Wozniak DF, Hartman RE, Boyle MP, Vogt SK, Brooks AR, Tenkova T et al (2004) Apoptotic neurodegeneration induced by ethanol in neonatal mice is associated with profound learning/memory deficits in juveniles followed by progressive functional recovery in adults. Neurobiol Dis 17:403–414
Yang J, Klaidman LK, Chang ML, Kem S, Sugawara T, Chan P et al (2002a) Nicotinamide therapy protects against both necrosis and apoptosis in a stroke model. Pharmacol Biochem Behav 73:901–910
Yang J, Klaidman LK, Nalbandian A, Oliver J, Chang ML, Chan PH et al (2002b) The effects of nicotinamide on energy metabolism following transient focal cerebral ischemia in Wistar rats. Neurosci Lett 333:91–94
Young C, Roth KA, Klocke BJ, West T, Holtzman DM, Labruyere J et al (2005) Role of caspase-3 in ethanol-induced developmental neurodegeneration. Neurobiol Dis 20:608–614
Zamzami N, Kroemer G (2001) The mitochondrion in apoptosis: how Pandora’s box opens. Nat Rev Mol Cell Biol 2:67–71
Acknowledgments
This work was supported by Rural Development Administration (Agenda: PJ007361) and Next-Generation Biogreen 21 program (PJ008075) funded by the Korean government.
Author information
Authors and Affiliations
Corresponding author
Additional information
Najeeb Ullah, Ikram Ullah and Hae Young Lee contributed equally to this work.
Rights and permissions
About this article
Cite this article
Ullah, N., Ullah, I., Lee, H.Y. et al. Protective Function of Nicotinamide Against Ketamine-induced Apoptotic Neurodegeneration in the Infant Rat Brain. J Mol Neurosci 47, 67–75 (2012). https://doi.org/10.1007/s12031-011-9685-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-011-9685-1