Abstract
Ketamine, a noncompetitive N-methyl D-aspartate (NMDA) receptor antagonist, is widely used in pediatric clinical practice. The neuroprotective and neurotoxic effects of ketamine on brain neurons during development remain controversial. The reason may be related to the different concentrations of ketamine used in practice and the small range of concentrations used in previous studies. In this study, cultured hippocampal neurons were treated with ketamine in a wide range of concentrations to comprehensively observe the effects of different concentrations of ketamine on neurons. We demonstrated that low concentrations of ketamine (10 μM, 100 μM and 1000 μM) promoted neuronal survival (p < 0.05) and reduced neuronal apoptosis (p < 0.05) compared with those of the control group. High concentrations of ketamine (2000 μM, 2500 μM and 3000 μM) reduced neuronal survival (p < 0.05) and promoted neuronal apoptosis (p < 0.05). The p38 MAPK inhibitor SB203580 reduced neuronal apoptosis induced by high concentrations of ketamine (2500 μM) (p < 0.05). Our findings indicate that ketamine exerts a dual effect on the apoptosis of primary cultured fetal rat hippocampal neurons in vitro and that the neurotoxic effects of ketamine are related to activation of the p38 MAPK signaling pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ketamine is a noncompetitive antagonist of the N-methyl-D-aspartate receptor (NMDA) and has been widely used in pediatric patients and critically ill patients due to its advantageous sedative and analgesic effects, low number of side effects involving hemodynamics and respiration, and short half-life (Fang et al. 2020; Li et al. 2021; Biliškov et al. 2021; Pansini et al. 2021; Marinello et al. 2020). However, in infancy, the development of the nervous system is very sensitive to changes in both internal and external environments. Overexcitation or inhibition can impair the morphology and function of neurons and affect the normal development of neurons. Studies have shown that ketamine exhibits a certain level of neurotoxicity in the early developing brain and induces neuronal apoptosis, leading to learning, memory and cognitive defects later in brain development (Huang et al. 2012; Paule et al. 2011; Huang et al. 2021; Zhang et al. 2021; Ye et al. 2018; Meng et al. 2020). The p38 MAPK signaling pathway is considered the possible mechanism of ketamine neurotoxicity (Guo et al. 2018). Other studies have also found that ketamine reduces neuronal apoptosis and exerts a certain neuroprotective effect (Rovnaghi et al. 2008; Anand et al. 2007; Tannich et al. 2020; Wang et al. 2021; Yang et al. 2018). Thus, the effects of ketamine on early brain development remain controversial. The reason for these controversies may be related to the small range of ketamine concentrations used in previous studies. Based on the pharmacokinetics and pharmacodynamics of ketamine, the clinically relevant concentration of ketamine was 10 μM. After intravenous injection, the concentration in the brain can be 6.5 times higher than that in the plasma. The concentration of ketamine used by researchers may be closely related to the findings. Based on this information, hippocampal neurons of fetal rats were used in our study to explore the effects of ketamine on hippocampal neuron apoptosis and the role of the p38 MAPK signaling pathway ; furthermore, these results will provide an experimental basis for further clinical research on the effects of ketamine on infant brain development.
Materials and methods
Chemicals and reagents
Ketamine hydrochloride (batch number KH080401, Fujian, China), MTT (Abcam, ab211091), Hoechst 33342 (Sigma, CAS: 875756-97-1), rabbit anti-rat phospho-p38 MAPK monoclonal antibody (CST, 9215s), and rabbit anti-rat p38 MAPK polyclonal antibody (CST, 9212s) were used in this study. The 10 mM ketamine storage solution was prepared as follows: 0.274 mL of ketamine stock solution (182.36 mmol/l) was diluted to 5 mL with Dulbecco’s modified Eagle's medium (DMEM), filtered, sterilized, packaged and stored at 4 °C. Each concentration of ketamine was prepared by the multiple ratio gradient dilution method. The pH of solutions at each concentration was measured and adjusted prior to application.
Experimental methods
Experimental animals
Clean grade 17–19–day pregnant Sprague–Dawley (SD) rats (provided by Shanghai Slack Laboratory Animal Co., Ltd., Production License No. SCXK (Shanghai) ) were bred in specific pathogen-free conditions and housed in air-conditioned, temperature-controlled rooms with a 12–h light/dark cycle (lights on, 08:00 am), 22-25 °C ambient temperature, and ad libitum access to food and water in the Laboratory Animal Center of Fujian Medical University. All procedures and the use of the animals were approved by the Institutional Animal Care and Use Committee of Fujian Medical University.
Harvest and culture of hippocampal neurons
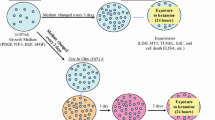
According to a previously reported method (Fath et al. 2009), embryonic hippocampal neurons were harvested from embryonic/gestational day 17–19 SD rats. In brief, timed pregnant rats were euthanized by cervical dislocation under an overdose of isoflurane. The uterus was dissected, and the whole fetal brain was removed and placed in a large plate containing DMEM in an ice bath. Hippocampal tissue was dissected and chopped into small, 1 mm3 pieces, and 0.125% pancreatic enzyme was added in an equal volume. After trituration with Barts pipette, the samples were digested for 15 min in a 5% CO2 incubator at 37 °C. An equal volume of 20% fetal bovine serum was added to stop digestion, and the mixture was triturated several times, filtered through a 200-mesh filter, and centrifuged for 3 min at a speed of 1000 rpm. The precipitate was collected and added to the inoculation solution to prepare a cell suspension. After the cell viability was measured and the cells were counted, they were diluted with high-glucose medium containing 10% fetal calf serum (FBS) according to the results of the live cell count. The inoculation density was 0.5×106 cells/mL, and 1.5 mL was seeded in each well of a 6-well plate, placed in an incubator containing 5% CO2 at 37 °C and incubated for 24 h. The implant solution was completely replaced with maintenance medium (97% neurobasal medium, 2% B27 and 1% glutamine). Afterward, half of the culture medium was changed once every two days. The neurons were observed under an inverted phase contrast microscope and photographed every day. After 7 days of culture, hippocampal neurons were removed for fluorescence staining and identification of β-tubulin III; the neurons were observed and photographed under a laser confocal microscope. Five fields were randomly selected under high magnification, and the number of positive cells among 100 cells was counted. The mean percentage of positive neurons ± standard deviation was reported.
MTT assay
Hippocampal neurons were collected at a final density of 0.8×106 cells/ mL and inoculated into a 96-well culture plate at 200 μL per well. On the 7th day of culture, ketamine was added at final concentrations of 0 μM (control), 0.1 μM, 1 μM, 10 μM, 100 μM, 1000 μM, 1500 μM, 2000 μM, 2500 μM, or 3000 μM. Six replicate wells were utilized for each concentration, and the culture was continued for 24 h. Then, 20 μL of MTT (5 mg/mL) was added to each well and the neurons were incubated for 4 h. Next, 150 μL of DMSO was added to each well, the plates were incubated for 10 min, and the absorption value was measured at 570 nm with a microplate reader. The results are presented as the mean of six well replicates of each ketamine concentration on the same plate. The OD result of the control without ketamine (ODC) was taken as 100%, and the percentages of MTT reductions at other concentrations were calculated as [(ODS - OD0)/(ODC - OD0)] ×100%, where ODS is the OD result of wells with different ketamine concentrations, and OD0 is the OD result of the eight MTT blank cell wells without MTT added. The experiment was repeated five times.
Nuclear staining
Twenty-four hours after ketamine intervention, neurons were washed with PBS, fixed with 4% paraformaldehyde for 15 min, rinsed, and labeled with 5 μg/mL Hoechst 33342 at room temperature for 10 min. The cells were then immersed in 1% PBST, fixed with anti-fluorescence quenching agent, excited with ultraviolet light at wavelengths of 350-460 nm, observed and photographed at high magnification under a fluorescence microscope.
Apoptosis rate based on flow cytometry (Annexin V/PI double staining)
Twenty-four hours after the ketamine intervention, neurons were digested with 0.25% trypsin, washed with PBS, and centrifuged at 1000 rpm for 5 min. The supernatant was discarded, and an appropriate amount of buffer was added to suspend the cells such that the number of cells per tube was not less than 1×106/mL. Then, 100 μL of the cell suspension was placed in a 5 mL flow tube and mixed with 2 μL of Annexin V (20 μg/mL) and 2 μL of propidium iodide (50 μg/mL). The reaction lasted for 15 min, and the cells were detected using a flow cytometer.
Western blotting
Western blotting was performed in three steps as follows.
-
Step1: To detect the influence of ketamine on the expression of p-p38 MAPK and t-p38 MAPK protein at different periods of time, hippocampal neurons were obtained at DIV 7 and treated with ketamine. The duration of ketamine intervention was 0 min, 1 min, 5 min, 15 min, 30 min and 60 min. After intervention, the protein expression levels of p-p38 MAPK and t-p38 MAPK were detected, and the p-p38 MAPK/t-p38 MAPK ratio was used to reflect phosphorylation of the p38 MAPK signaling pathway.
-
Step2: To determine the influence of different concentrations of ketamine on the expression of the p-p38 MAPK and the t-p38 MAPK protein at the same time, hippocampal neurons were obtained at DIV 7, and different concentrations of ketamine were used for intervention. The ketamine concentrations were 0 μM (control), 1 μM, 10 μM, 100 μM, 1000 μM, 1500 μM, 2000 μM and 2500 μM. The peak phosphorylation of p38 MAPK was achieved at 15 min (based on the experimental results of step 1); therefore, this was used as the duration to measure the action of ketamine. After the intervention, the protein expression levels of p-p38 MAPK and t-p38 MAPK were detected, and the p-p38 MAPK/t-p38 MAPK ratio reflected the phosphorylation of the p38 MAPK signaling pathway.
-
Step3: To investigate the relationship between the apoptosis of hippocampal neurons induced by high concentrations of ketamine and the activity of the p38 MAPK signaling pathway, hippocampal neurons were obtained at DIV 7 and randomly divided into the following four groups: the control group, ketamine group, SB203580 group and SB203580+ ketamine group. The SB203580+ ketamine group was pretreated with SB203580 (10 μM) for 30 min and then was treated with ketamine. Each group was treated for 24 hours. After the intervention, the apoptosis rate of each group was detected by flow cytometry.
Briefly, after the intervention, neurons were washed with PBS twice and lysed in RIPA buffer with PMSF. After incubating on ice for 30 min, the lysates were centrifuged at 12,000 rpm for 15 min. The protein concentration was then determined using the BCA method. After sample loading and resolution on gels, the membrane was subjected to 120 V constant voltage electrophoresis for 90 min and 300 mA constant current flow for 1.5 h. The PVDF membrane was removed, placed in 20 mL of blocking solution, and incubated for 2 h. A rabbit anti-rat phospho- p38 MAPK monoclonal antibody and rabbit anti-rat p38 MAPK polyclonal antibody were diluted with primary antibody diluent (1:1000). The mouse anti-rat GAPDH monoclonal antibody was diluted with primary antibody diluent (1:500). Then, the PVDF membrane was completely immersed in the prepared primary antibody incubation solution and incubated at 4 °C overnight. The PVDF membrane was washed to remove nonspecifically bound primary antibody, fully immersed in a specific secondary antibody (HRP-labeled goat anti-rabbit IgG 1:6000; HRP-labeled sheep anti-mouse IgG 1:3000) and incubated at room temperature for 1.5 h. The nonspecifically bound secondary antibody on the PVDF membrane was fully removed by washing with 1% PBST. Substrate reaction, exposure, development, fixing, scanning and analysis were performed. ImageJ software (National Institutes of Health) was used to determine the band intensities, which reflected the expression of each protein. Data are presented as the mean ± SD. A probability of *p < 0.05 was considered significant (one-way ANOVA with the Holm–Sidak test). The experiment was repeated three times.
Statistical analysis
All experimental data were tested for homogeneity of variance and normality and are reported as the mean ± standard deviation(\(\overline{\textrm{x}}\pm \textrm{s}\)). SPSS 22.0 software was used for statistical analyses. One-way ANOVA was used for comparisons between groups, and the LSD test was used for pairwise comparisons of means between samples. P<0.05 indicated that the difference was statistically significant.
Results
Morphological observation and determination of the purity of hippocampal neurons.
Under an inverted phase contrast microscope, the neurons that were cultured for 24 h showed a spindle shape with protrusions (Fig. 1a). The neurons that were cultured for 7 days had plump cell bodies, obvious surrounding halos and longer protrusions due to the formation of neural fiber networks (Fig. 1b). Vacuoles appeared in the cell bodies of neurons cultured for 14 days, and the cells were degenerated and deformed (Fig. 1c). The neurons that had been cultured for 21 days displayed obvious nuclear pyknosis, nuclear fragmentation and protrusion fractures (Fig. 1d). Using a β-tubulin III monoclonal antibody and Hoechst 33342 immunofluorescence staining, the cytoplasm and neuronal processes of positive cells were red, and the nucleus was blue (Fig. 1e). The purity of the neurons was 91.5±2.8%.
The morphology of hippocampal neurons in culture. (a). After 24 hours in vitro (1 DIV), the cells acquired an evenly rounded and phase-bright appearance, and several neurites formed. (b). After 7 DIV, neurons developed axons, as well as several dendrites, and a network of mature neurons developed. (c). After 14 DIV, neuronal aggregation was obvious, vacuoles began to appear in the cell body, and the cells began to deform. (d). After 21 DIV, the degeneration of neurons was obvious, there was obvious nucleolysis and nuclear fragmentation, neurite receding and breaking, and the halo around the cells became faint or disappeared. (e). Using β-tubulin III monoclonal antibody and Hoechst 33342 immunofluorescence staining, the plasma and neurite of the positive cells were red, and the nucleus was blue under laser confocal microscopy. Scale bar = 50 μm.
Effect of ketamine on hippocampal neuron cell activity.
The MTT results showed that ketamine exerted bidirectional effects on neuronal survival. Low concentrations of ketamine (10 μM, 100 μM, and 1000 μM) promoted neuronal survival (p < 0.01), and high concentrations of ketamine (2000 μM, 2500 μM, and 3000 μM) decreased neuronal survival (p < 0.01) (Fig. 2).
The effect of ketamine on the neuron survival rate. An MTT assay was used to evaluate the effect of ketamine on neuron viability. Compared with the control group, no significant effects were observed when the ketamine concentrations were 0.1 μM and 1 μM. With increasing ketamine concentration, the cell survival rates increased significantly in the 10 μM (p < 0.01), 100 μM (p < 0.01) and 1000 μM (p < 0.05) ketamine-treated groups. There were no significant differences between the results of the 1500 μM ketamine-treated and control groups. With a further increase in ketamine concentration, the cell survival rates of the 2000 μM, 2500 μM, and 3000 μM ketamine-treated groups were significantly decreased (p < 0.01). The results are presented as the mean ± standard error of the mean. The experiments were repeated five times. *p< 0.05; **p< 0.01, n = 5.
Effect of ketamine on hippocampal neuron apoptosis.
Hoechst 33342 staining showed that nuclear enrichment and fragmentation were reduced at low concentrations (10 μM, 100 μM, and 1000 μM). At high concentrations (2000 μM, 2500 μM, and 3000 μM), the nuclei were concentrated, and the number of nuclear fragments increased (Fig. 3). A subsequent flow cytometry analysis showed that low concentrations of ketamine (10 μM, 100 μM, and 1000 μM) inhibited neuronal apoptosis (p < 0.05). High concentrations of ketamine (2000 μM, 2500 μM, and 3000 μM) promoted neuronal apoptosis (p < 0.01) (Fig. 4).
Flow cytometry was used to examine cell apoptosis. (a). Typical representative diagram. (b). Compared with the control group, no significant effects were observed when the ketamine concentrations were 0.1 μM and 1 μM. With increasing ketamine concentration, the cell apoptosis rates decreased significantly in the 10 μM (p < 0.05) , 100 μM (p < 0.01) and 1000 μM (p < 0.05) ketamine-treated groups, but the rate was not significantly different in the 1500 μM ketamine-treated group. With a further increase in ketamine concentration, the cell apoptosis rates showed a concentration-dependent increase in the 2000 μM, 2500 μM, and 3000 μM ketamine-treated groups. The results are presented as the mean ± standard error of the mean. The experiments were repeated three times. *p < 0.05; **p < 0.01, n = 3.
High concentrations of ketamine activate the p38 MAPK signaling pathway.
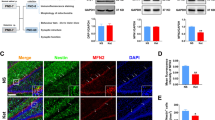
We detected and analyzed the level of phosphorylated p38 MAPK, a key molecule in the p38 MAPK signaling pathway, to further study the mechanism by which high ketamine concentrations induced apoptosis in hippocampal neurons. The activation of the p38 MAPK signaling pathway was related to the duration and concentration of ketamine treatment. After treatment with ketamine (2500 μM), the level of phosphorylated p38 MAPK peaked at 15 min and gradually decreased to the baseline level (Fig. 5a). Low concentrations of ketamine (1 μM, 10 μM, 100 μM, and 1000 μM) did not activate the p38 MAPK signaling pathway, and only high concentrations of ketamine (1500 μM, 2000 μM, and 2500 μM) promoted p38 MAPK phosphorylation in a concentration-dependent manner (Fig. 5c).
The influence of ketamine on the p38 MAPK pathway. (a). The relative p-p38 MAPK level after treatment with 2500 μM ketamine for different time periods (0 to 60 min); (b). Differences between control group values and 5, 15 and 30 min (p < 0.01); differences between 5 and 15 min (p < 0.01); differences between 15 and 30 min (p < 0.01). The results are presented as the mean ± standard error of the mean. The experiments were repeated three times. **p < 0.01, ## p < 0.01, n = 3. (c). The relative p-p38 MAPK level after treatment with different concentrations of ketamine for 15 min; (d). Differences between the control group values and 1500 μM, 2000 μM and 2500 μM ketamine-treated groups (p < 0.01); differences between 1500 and 2000 μM ketamine-treated groups (p < 0.01); differences between 2000 and 2500 μM ketamine-treated groups (p < 0.01). The results are presented as the mean ± standard error of the mean. The experiments were repeated three times. **p < 0.01, ## p < 0.01, n = 3.
The role of the p38 MAPK signaling pathway in hippocampal neuron apoptosis.
The flow cytometry analysis showed that compared with the control group, the apoptosis rate of the group treated with the p38 MAPK inhibitor SB203580 was not significantly different (p > 0.05), and the apoptosis rate of neurons in the ketamine (2500 μM) group and the SB203580+ ketamine group was significantly increased (p < 0.01). Compared with the ketamine (2500 μM) group, the apoptosis rate of the SB203580+ketamine (2500 μM) group was significantly decreased (p < 0.01) (Fig. 6).
The effect of SB203580 on cell apoptosis induced by high concentrations (2500 μM) of ketamine. Flow cytometry was used to examine apoptosis after treatment with SB203580. (a). A typical representative diagram of cell apoptosis. (b). Differences between the control group values and the SB203580 group (p > 0.05), the 2500 μM ketamine-treated group and the SB203580+ ketamine-treated group (p < 0.01); differences between the ketamine-treated group and the SB203580+ ketamine-treated groups (p < 0.01). The results are presented as the mean ± standard error of the mean. The experiments were repeated three times. **p < 0.01, ## p < 0.01, n = 3.
Discussion
The aim of this study was to investigate the effects of ketamine on the developing brain. Our results suggest that ketamine has a dual effect on apoptosis in primary fetal rat hippocampal neurons cultured in vitro and that activation of the p38 MAPK signaling pathway plays an important role in the neurotoxic effects of ketamine.
Currently, research on the effects of ketamine on neuronal development remains controversial. Dong et al. (2012) found that a clinical concentration of ketamine does not induce the death of nerve stem progenitor cells through apoptosis or necrosis, and ketamine can even promote the differentiation of nerve stem progenitor cells and alters cell proliferation. However, some studies have shown that ketamine is neurotoxic (Yang et al. 2021; Liu et al. 2021; Fan et al. 2021). The reason for these controversies may be related to the small range of ketamine concentrations used in these studies. Therefore, in this study, we selected a wide range of concentrations of ketamine for administration to hippocampal neurons from fetal rats and found that low concentrations of ketamine inhibited neuronal apoptosis and promoted neuronal survival. High concentrations promoted neuronal apoptosis and reduced neuronal survival. Based on these results, different concentrations of ketamine exert different effects on neuronal development, which explains the controversy over the effect of ketamine on neuronal development to a certain extent.
Ketamine is an antagonist of the NMDA receptor, and p38 MAPK is an important intracellular signal transduction protein downstream of the NMDA receptor. p38 MAPK is one of the important members of the MAPK family, which mainly mediates inflammatory signaling, stress and injury. It is widely believed that the p38MAPK signaling pathway plays an important role in regulating learning memory processes (Wang et al. 2020). Wang et al. (2014) found that elevated levels of peripheral blood phosphorylated p38 MAPK expression were associated with Alzheimer's disease (AD) and Parkinson's disease (PD). Another study also found that activation of p38 MAPK plays a key role in the pathophysiology of Alzheimer's disease (AD) and that selective degradation of phosphorylated p38 MAPK may provide an attractive therapeutic option for the treatment of AD (Son et al. 2023). Interestingly, there is also some literature discussing the potential of ketamine for the treatment of Alzheimer's disease (Lozupone et al. 2018; Smalheiser et al. 2019). Recent studies have found that activation or inhibition of the p38 MAPK signaling pathway affects neuronal apoptosis (Li et al. 2020; Zhou et al. 2020; Lyu et al. 2018). In the present study, the phosphorylation of p38 MAPK, a key molecule in the p38 MAPK signaling pathway, was significantly increased by intervention with a high concentration of ketamine, and ketamine promoted the phosphorylation of p38 MAPK in a concentration-dependent manner when the concentration of ketamine was greater than 1500 μM. Combined with the previous results, we speculated that the neurotoxic effects of ketamine may be related to the activation of the p38 MAPK signaling pathway. Previous studies have shown that inhibiting the activation of the p38 MAPK signaling pathway alleviates neuronal damage caused by hypoxia (Lan et al. 2011; He et al. 2021). SB203580, a p38 MAPK inhibitor, was used to further verify our hypothesis. SB203580 significantly reduced the rate of neuronal apoptosis induced by high concentrations of ketamine. This result confirms that the p38 MAPK signaling pathway is involved in the neurotoxic effects of high concentrations of ketamine. Liu et al. found that NMDA could mediate the apoptosis of primary cortical neurons by activating the p38 signaling pathway. SB203580 has a neuroprotective effect on NMDA-induced apoptosis, and this finding is similar to the results of this study (Liu et al. 2014).
However, we found that low concentrations of ketamine did not cause neuronal apoptosis but instead promoted neuronal survival. Further experiments showed that the p38 MAPK signaling pathway was not activated by low ketamine concentrations. Based on this phenomenon, we speculate that other signal transduction pathways are involved and exert an anti-apoptotic effect when the concentration of ketamine is relatively low; this finding requires further investigation.
On the other hand, ketamine has been used as an antidepressant in addition to anesthesia (Hirota and Lambert 2018). At subanesthetic doses, a single ketamine infusion has been reported to promote not only a rapid-acting antidepressant effect (usually within hours) but also in patients resistant to prior treatment (Chang et al. 2009). The mechanisms by which ketamine improves depressive symptoms are not fully understood, but a growing body of evidence suggests that the rapid antidepressant-like effects of ketamine are associated with reductions in pro-inflammatory cytokines (e.g., interleukin (IL)-1β, tumor necrosis factor (TNF)-α, IL-6) in serum and brain tissue (Yang et al. 2013a, 2013b; Wang et al. 2015; Tan et al. 2017; Xie et al. 2017; Clarke et al. 2017). The optimal dose of ketamine for the treatment of depression is not yet clear. However, according to the literature, the peak blood levels of ketamine hydrochloride during surgical anesthesia are 2000 ~ 3000 ng/mL (7.29 ~ 10.94 μM), and the peak blood levels associated with anesthetic awakening are 500 ~ 1000 ng/mL (1.82 ~ 3.65 μM). A typical antidepressant dose of 0.5 mg/kg, administered intravenously for 40 minutes, produces peak plasma concentrations of 70 to 200 ng/mL (0.26 to 0.73 μM) of ketamine hydrochloride without general anesthesia (Sanacora et al. 2017). Due to its high lipid solubility and ease of crossing the blood-brain barrier, the concentration of ketamine in rat cerebrospinal fluid is approximately 6.5 times higher than the blood concentration (Cohen et al. 1973), so that 47.41 ~ 71.12 μM in cerebrospinal fluid corresponds to concentrations relevant to clinical anesthesia and 1.66 ~ 4.74 μM in cerebrospinal fluid corresponds to concentrations relevant to antidepressant treatment. Previous studies have found that ketamine exerts antidepressant effects by inhibiting PC12 cell apoptosis (Zhang et al. 2021). The results of the present study showed that 10 μM ketamine promoted neuronal cell survival and reduced apoptosis, whereas 1 μM ketamine had no effect on neuronal cell survival and apoptosis. Since 1 μM ~ 10 μM ketamine was not used in this study, the effect of ketamine in this concentration range (antidepressant concentration) on neuronal cell survival and apoptosis is unknown and needs to be further investigated.
In summary, ketamine exerts a dual effect on the apoptosis of primary cultured fetal rat hippocampal neurons in vitro. It exerts neuroprotective effects at low concentrations and neurotoxic effects at high concentrations. The neurotoxic effects of ketamine are related to the activation of the p38 MAPK signaling pathway.
There are also some limitations for this study. After all, this is just an in vitro study. Moreover, rodents and primates are different species, and their neurons must respond differently to the effects of ketamine. Therefore, the results of this study can only provide a certain reference for clinical practice. The protective mechanism of low concentration ketamine and whether there are other signaling pathways involved in the neuroprotective or neurotoxic effects of ketamine also need to be further explored. Another limitation of the present study is that the experiments were performed on a single cell line only. Further studies, particularly animal and other cell culture models are required to obtain a more definite answer regarding the effects of ketamine on the developing brain.
Data availability
The datasets are available from the corresponding author upon reasonable request.
Code availability
Not applicable.
References
Anand KJ, Garg S, Rovnaghi CR, Narsinghani U, Bhutta AT, Hall RW (2007) Ketamine reduces the cell death following inflammatory pain in newborn rat brain. Pediatr Res 62(3):283–290. https://doi.org/10.1203/PDR.0b013e3180986d2f
Biliškov AN, Ivančev B, Pogorelić Z (2021) Effects on Recovery of Pediatric Patients Undergoing Total Intravenous Anesthesia with Propofol versus Ketofol for Short-Lasting Laparoscopic Procedures. Children (Basel, Switzerland) 8(7):610. https://doi.org/10.3390/children8070610
Cohen ML, Chan SL, Way WL, Trevor AJ (1973) Distribution in the brain and metabolism of ketamine in the rat after intravenous administration. Anesthesiology 39(4):370–376. https://doi.org/10.1097/00000542-197310000-00003
Clarke M, Razmjou S, Prowse N, Dwyer Z, Litteljohn D, Pentz R, Anisman H, Hayley S (2017) Ketamine modulates hippocampal neurogenesis and pro-inflammatory cytokines but not stressor induced neurochemical changes. Neuropharmacology 112:210–220. https://doi.org/10.1016/j.neuropharm.2016.04.021
Chang Y, Lee JJ, Hsieh CY, Hsiao G, Chou DS, Sheu JR (2009) Inhibitory effects of ketamine on lipopolysaccharide-induced microglial activation. Mediators of Inflammation 705379. https://doi.org/10.1155/2009/705379
Dong C, Rovnaghi CR, Anand KJ (2012) Ketamine alters the neurogenesis of rat cortical neural stem progenitor cells. Crit Care Med 40(8):2407–2416. https://doi.org/10.1097/CCM.0b013e318253563c
Fang H, Li HF, Yang M, Zhang FX, Liao R, Wang RR, Wang QY, Zheng PC, Zhang JP (2020) Effect of ketamine combined with lidocaine in pediatric anesthesia. J Clin Lab Anal 34(4):e23115. https://doi.org/10.1002/jcla.23115
Fan X, Bian W, Liu M, Li J, Wang Y (2021) MiRNA-429 alleviates ketamine-induced neurotoxicity through targeting BAG5. Environ Toxicol 36(4):620–627. https://doi.org/10.1002/tox.23066
Fath T, Ke YD, Gunning P, Götz J, Ittner LM (2009) Primary support cultures of hippocampal and substantia nigra neurons. Nat Protoc 4(1):78–85. https://doi.org/10.1038/nprot.2008.199
Guo XQ, Cao YL, Zhao L, Zhang X, Yan ZR, Chen WM (2018) p38 mitogen-activated protein kinase gene silencing rescues rat hippocampal neurons from ketamine-induced apoptosis: An in vitro study. Int J Mol Med 42(3):1401–1410. https://doi.org/10.3892/ijmm.2018.3750
He Y, Liu Z, Huang Y, Li B (2021) Role of the p38MAPK signaling pathway in hippocampal neuron autophagy in rats with chronic intermittent hypoxia. J Neurophysiol 126(4):1112–1121. https://doi.org/10.1152/jn.00240.2021
Huang H, Zhao C, Hu Q, Liu Q, Sun YM, Chen C, Huang H, Zhou CH, Wu YQ (2021) Neonatal anesthesia by ketamine in neonatal rats inhibits the proliferation and differentiation of hippocampal neural stem cells and decreases neurocognitive function in adulthood via inhibition of the notch1 signaling pathway. Mol Neurobiol 58(12):6272–6289. https://doi.org/10.1007/s12035-021-02550-3
Hirota K, Lambert DG (2018) Ketamine and depression. Br J Anaesth 121(6):1198–1202. https://doi.org/10.1016/j.bja.2018.08.020
Huang L, Liu Y, Jin W, Ji X, Dong Z (2012) Ketamine potentiates hippocampal neurodegeneration and persistent learning and memory impairment through the PKCγ-ERK signaling pathway in the developing brain. Brain Res 1476:164–171. https://doi.org/10.1016/j.brainres.2012.07.059
Lan A, Liao X, Mo L, Yang C, Yang Z, Wang X, Hu F, Chen P, Feng J, Zheng D, Xiao L (2011) Hydrogen sulfide protects against chemical hypoxia-induced injury by inhibiting ROS-activated ERK1/2 and p38MAPK signaling pathways in PC12 cells. PLoS One 6(10):e25921. https://doi.org/10.1371/journal.pone.0025921
Li HP, Liu KP, Yao L (2021) Dexmedetomidine in combination with ketamine for pediatric procedural sedation or premedication: A meta-analysis. Am J Emerg Med 50:442–448. https://doi.org/10.1016/j.ajem.2021.08.073
Li L, Li Y, Miao C, Liu Y, Liu R (2020) Coriolus versicolor polysaccharides (CVP) regulates neuronal apoptosis in cerebral ischemia-reperfusion injury via the p38MAPK signaling pathway. Annals of translational medicine 8(18):1168. https://doi.org/10.21037/atm-20-5759
Lozupone M, La Montagna M, D'Urso F, Piccininni C, Sardone R, Dibello V, Giannelli G, Solfrizzi V, Greco A, Daniele A, Quaranta N, Seripa D, Bellomo A, Logroscino G, Panza F (2018) Pharmacotherapy for the treatment of depression in patients with alzheimer's disease: a treatment-resistant depressive disorder. Expert Opin Pharmacother 19(8):823–842. https://doi.org/10.1080/14656566.2018.1471136
Liu S, Tao G, Zhou C, Wang Q, Wang W, Fei X (2021) Ketamine inhibits neuronal differentiation by regulating brain-derived neurotrophic factor (BDNF) signaling. Toxicology in vitro : an international journal published in association with BIBRA 72:105091. https://doi.org/10.1016/j.tiv.2021.105091
Liu XW, Ji EF, He P, Xing RX, Tian BX, Li XD (2014) Protective effects of the p38 MAPK inhibitor SB203580 on NMDA-induced injury in primary cerebral cortical neurons. Mol Med Rep 10(4):1942–1948. https://doi.org/10.3892/mmr.2014.2402
Lyu Z, Cao J, Wang J, Lian H (2018) Protective effect of vitexin reduces sevoflurane-induced neuronal apoptosis through HIF-1α, VEGF and p38 MAPK signaling pathway in vitro and in newborn rats. Exp Ther Med 15(3):3117–3123. https://doi.org/10.3892/etm.2018.5758
Marinello L, Zanotti G, Spinelli A, Zarantonello M, De Santis D, Zotti F, Iurlaro A, Alberti C, Zangani A, Capocasale G, Bertajola A, Donadello D, Finotti M (2020) Ketamine in dentistry: a useful way for non-compliant pediatric patients. J Biol Regul Homeost Agents 34(6 Suppl. 2):63–68
Meng C, Yao XQ, Chang RJ, Wang SL, Wang X, Ma DQ, Li Q, Wang XY (2020) Exogenous GM1 Ganglioside Attenuates Ketamine-Induced Neurocognitive Impairment in the Developing Rat Brain. Anesth Analg 130(2):505–517. https://doi.org/10.1213/ANE.0000000000004570
Pansini V, Curatola A, Gatto A, Lazzareschi I, Ruggiero A, Chiaretti A (2021) Intranasal drugs for analgesia and sedation in children admitted to pediatric emergency department: a narrative review. Ann Trans Med 9(2):189. https://doi.org/10.21037/atm-20-5177
Paule MG, Li M, Allen RR, Liu F, Zou X, Hotchkiss C, Hanig JP, Patterson TA, Slikker W Jr, Wang C (2011) Ketamine anesthesia during the first week of life can cause long-lasting cognitive deficits in rhesus monkeys. Neurotoxicol Teratol 33(2):220–230. https://doi.org/10.1016/j.ntt.2011.01.001
Rovnaghi CR, Garg S, Hall RW, Bhutta AT, Anand KJ (2008) Ketamine analgesia for inflammatory pain in neonatal rats: a factorial randomized trial examining long-term effects. Behav Brain Funct 4:35. https://doi.org/10.1186/1744-9081-4-35
Tannich F, Barhoumi K, Rejeb A, Aouichri M, Souilem O (2020) Ketamine, at low dose, decrease behavioural alterations in epileptic diseases induced by pilocarpine in mice. Intl J Neurosci 130(11):1118–1124. https://doi.org/10.1080/00207454.2020.1730363
Tan SJ, Wang Y, Chen K, Long ZF, Zou J (2017) Ketamine Alleviates Depressive-Like Behaviors via Down-Regulating Inflammatory Cytokines Induced by Chronic Restraint Stress in Mice. Biol Pharm Bull 40(8):1260–1267. https://doi.org/10.1248/bpb.b17-00131
Sanacora G, Frye MA, McDonald W, Mathew SJ, Turner MS, Schatzberg AF, Summergrad P, Nemeroff CB; American Psychiatric Association (APA) Council of Research Task Force on Novel Biomarkers and Treatments. (2017) A Consensus Statement on the Use of Ketamine in the Treatment of Mood Disorders. JAMA Psychiatry 74(4):399-405. https://doi.org/10.1001/jamapsychiatry.2017.0080
Smalheiser NR (2019) Ketamine: A Neglected Therapy for Alzheimer Disease. Front Aging Neurosci 11:186. https://doi.org/10.3389/fnagi.2019.00186
Son SH, Lee NR, Gee MS, Song CW, Lee SJ, Lee SK, Lee Y, Kim HJ, Lee JK, Inn KS, Kim NJ. (2023) Chemical Knockdown of Phosphorylated p38 Mitogen-Activated Protein Kinase (MAPK) as a Novel Approach for the Treatment of Alzheimer's Disease. ACS Centr Sci 9(3):417-426. https://doi.org/10.1021/acscentsci2c01369
Wang L, Deng B, Yan P, Wu H, Li C, Zhu H, Du J, Hou L (2021) Neuroprotective effect of ketamine against TNF-α-induced necroptosis in hippocampal neurons. J Cell Mol Med 25(7):3449–3459. https://doi.org/10.1111/jcmm.16426
Wang N, Yu HY, Shen XF, Gao ZQ, Yang C, Yang JJ, Zhang GF (2015) The rapid antidepressant effect of ketamine in rats is associated with down-regulation of pro-inflammatory cytokines in the hippocampus. Ups J Med Sci 120(4):241–248. https://doi.org/10.3109/03009734.2015.1060281
Wang S, Zhang C, Sheng XN, Zhang XW, Wang BB, Zhang GH (2014) Peripheral expression of MAPK pathways in Alzheimer's and Parkinson's diseases. J Clin Neurosci 21(5):810–814. https://doi.org/10.1016/j.jocn.2013.08.017
Wang Y, Wang Q, Ren B, Guo T, Qiang J, Cao H, Gao YJ, L ZB, Gao XY, Zhu B (2020) "Olfactory Three-Needle" Enhances Spatial Learning and Memory Ability in SAMP8 Mice. Behav Neurol 2020:2893289. https://doi.org/10.1155/2020/2893289
Xie ZM, Wang XM, Xu N, Wang J, Pan W, Tang XH, Zhou ZQ, Kenji H, Yang JJ (2017) Alterations in the inflammatory cytokines and brain-derived neurotrophic factor contribute to depression-like phenotype after spared nerve injury: improvement by ketamine. Sci Rep 7(1):3124. https://doi.org/10.1038/s41598-017-03590-3
Yang C, Hong T, Shen J, Ding J, Dai XW, Zhou ZQ, Yang JJ (2013a) Ketamine exerts antidepressant effects and reduces IL-1β and IL-6 levels in rat prefrontal cortex and hippocampus. Exp Ther Med 5(4):1093–1096. https://doi.org/10.3892/etm.2013.930
Yang C, Si M, Zhou J (2021) Silencing TRPV4 partially reverses the neurotoxic effects caused by excess Ketamine. J Toxicol Sci 46(2):69–81. https://doi.org/10.2131/jts.46.69
Yang C, Shen J, Hong T, Hu TT, Li ZJ, Zhang HT, Zhang YJ, Zhou ZQ, Yang JJ (2013b) Effects of ketamine on lipopolysaccharide-induced depressive-like behavior and the expression of inflammatory cytokines in the rat prefrontal cortex. Mol Med Rep 8(3):887–890. https://doi.org/10.3892/mmr.2013.1600
Yang J, Li X, Yang C, Bu XX, Shen J, Hong T (2018) Research on ketamine in mediating autophagy and inhibiting apoptosis of astrocytes in cerebral cortex of rats through NF-κB pathway. European review for medical and pharmacological sciences 22(16):5385–5393. https://doi.org/10.26355/eurrev_201808_15741
Ye Z, Li Q, Guo Q, Xiong Y, Guo D, Yang H, Shu Y (2018) Ketamine induces hippocampal apoptosis through a mechanism associated with the caspase-1 dependent pyroptosis. Neuropharmacology 128:63–75. https://doi.org/10.1016/j.neuropharm.2017.09.035
Zhang WF, Sun Q, Jia LL, Li M (2020) Ketamine exerts a protective role in a cell-based model of major depressive disorder via the inhibition of apoptosis and inflammation and activation of the Krebs cycle. Biomolecules and Biomedicine 20(1):44-55. https://doi.org/10.17305/bjbms.2019.4222
Zhang Z, Liu W, Shen M, Ma X, Li R, Jin X, Bai H, Gao L (2021) Protective effect of GM1 attenuates hippocampus and cortex apoptosis after ketamine exposure in neonatal rat via PI3K/AKT/GSK3β pathway. Mol Neurobiol 58(7):3471–3483. https://doi.org/10.1007/s12035-021-02346-5
Zhou RX, Li YY, Qu Y, Huang Q, Sun XM, Mu DZ, Li XH (2020) Regulation of hippocampal neuronal apoptosis and autophagy in mice with sepsis-associated encephalopathy by immunity-related GTPase M1. CNS Neurosci Ther 26(2):177–188. https://doi.org/10.1111/cns.13229
Funding
This work was supported by the Joint Fund for the innovation of science and Technology, Fujian province [Grant number: 2018Y9024].
Author information
Authors and Affiliations
Contributions
Conceptualization: Guo-Hua Wu, Que-Hui Guo, Liang-Cheng Zhang, and Cai-Hou Lin. Data curation: Guo-Hua Wu, Que-Hui Guo, Xiao-Dong Xu, Jian-Chang Lin, and Gui-Ting You ; formal analysis: Guo-Hua Wu, Que-Hui Guo, Xiao-Dong Xu, Jian-Chang Lin, Liang-Cheng Zhang, and Cai-Hou Lin. Funding acquisition: Cai-Hou Lin. Investigation: Guo-Hua Wu, Xiao-Dong Xu, Jian-Chang Lin, Gui-Ting You , and Cai-Hou Lin. Methodology: Guo-Hua Wu, Que-Hui Guo, Xiao-Dong Xu, Liang-Cheng Zhang, and Cai-Hou Lin. Project administration: Guo-Hua Wu, and Liang-Cheng Zhang. Supervision: Que-Hui Guo, and Cai-Hou Lin. Visualization: Guo-Hua Wu, Que-Hui Guo, Liang-Cheng Zhang, and Cai-Hou Lin. Writing - original draft; writing - review & editing: Guo-Hua Wu, Que-Hui Guo, Xiao-Dong Xu, Jian-Chang Lin, Gui-Ting You , Liang-Cheng Zhang, and Cai-Hou Lin.
Corresponding authors
Ethics declarations
Ethics approval
The use of animals was approved by the Institutional Animal Care and Use Committee of Fujian Medical University.
Consent to participate
Not applicable.
Consent for publication
All authors agree to the publication.
Conflicts of interest
There are no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Guo-Hua Wu handles correspondence at all stages of the review and publication process.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, GH., Guo, QH., Xu, XD. et al. Ketamine exerts dual effects on the apoptosis of primary cultured hippocampal neurons from fetal rats in vitro. Metab Brain Dis 38, 2417–2426 (2023). https://doi.org/10.1007/s11011-023-01236-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-023-01236-0