Abstract
Background
Large hemispheric infarction (LHI) is an ischemic stroke affecting at least two-thirds of the middle cerebral artery territory, with or without involvement of the anterior cerebral artery or posterior cerebral artery, and approximately 77% of LHI patients have early consciousness disorder (ECD). We constructed a functional brain network for LHI patients with an acute consciousness disorder to identify new diagnostic markers related to ECDs by analyzing brain network characteristics and mechanisms.
Methods
Between August 1, 2017, and September 30, 2018, patients with acute (< 1 month) LHI were admitted to the neurocritical care unit at Xuanwu Hospital of Capital Medical University. Electroencephalography (EEG) data were recorded, and the MATLAB platform (2017b) was used to calculate spectral power, entropy, coherence and phase synchronization. The quantitative EEG and brain network characteristics of different consciousness states and different frequency bands were analyzed (α = 0.05). EEG data were recorded 38 times in 30 patients, 25 of whom were in the ECD group, while 13 patients were in the conscious group.
Results
(1) Spectral power analysis: The conscious group had higher beta relative spectral power across the whole brain, higher alpha spectral power in the frontal-parietal lobe on the infarction contralateral side, and lower theta and delta spectral power in the central-occipital lobe on the infarction contralateral side than the ECD group. (2) Entropy analysis: The conscious group had higher approximate entropy (ApEn) and permutation entropy (PeEn) across the whole brain than the ECD group. (3) Coherence: The conscious group had higher alpha coherence in nearly the whole brain and higher beta coherence in the bilateral frontal-parietal and parietal-occipital lobes than the ECD group. (4) Phase synchronization: The conscious group had higher alpha and beta synchronization in nearly the whole brain, particularly in the frontal-parietal and parietal-occipital lobes, than the ECD group. (5) Graph theory: The conscious group had higher small-worldness in each frequency band than the ECD group.
Conclusion
In patients with LHI, higher levels of consciousness were associated with more alpha and beta oscillations and fewer delta and theta oscillations. Higher ApEn, PeEn, total brain connectivity, and small-worldness and a wider signal distribution range corresponded to a higher consciousness level.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Impairment of consciousness results from pathologies capable of interfering with or abolishing the capacity to be awake and aware, which encompass a spectrum of conditions ranging from somnolence, stupor, coma, confusion, and delirium in the acute stage and vegetative state/unresponsive wakefulness syndrome (VS/UWS) and minimally conscious state (MCS) in the chronic stage. Many patients in early stages of acute ischemic stroke show acute disorder of consciousness, a condition known as early consciousness disorder (ECD). Large hemispheric infarction (LHI), which is primarily caused by an occlusion of either the internal carotid or the proximal middle cerebral artery, is the most malignant type of supratentorial ischemic stroke [1], and approximately 77% of LHI patients have ECD [2]. ECD is associated with higher frequencies of stroke-related complications and 3-month death/disability.
Recent functional magnetic resonance imaging (fMRI) functional network studies in consciousness disorder patients at rest have provided promising but divergent accounts about the spatial extent and topography of functional brain changes. For patients in the acute phase of disorders of consciousness, fundamental network characteristics were preserved, but a restructuring of hubs was noted [3]. The varying degrees of preservation of intrinsic default mode network (DMN) connectivity accurately discriminated comatose patients who regained consciousness from those who did not [4, 5]. Moreover, Fisher et al. [6] reported that injury to a small region in the pontine tegmentum is significantly associated with coma. For patients in the chronic stage of consciousness disorders, the DMN is somewhat stronger in an MCS than in VS/UWS but is severely impaired compared to that in healthy subjects [7, 8]. However, fMRI is associated with considerable expenses and difficulty, limiting the possibility of wider clinical application in patients. Meanwhile, the time resolution of most fMRI techniques does not enable detection of fast neural oscillations, which are involved in conscious perception and information transfer between regions [9], limiting possibilities to study synchronization-based communication with fMRI.
Electroencephalography (EEG) has been widely used in studies of consciousness disorders as a portable, cost-effective, convenient bedside and objective monitoring and analysis technique [10]. Traditional EEG analysis techniques have been able to accurately predict poor outcomes (brain death or vegetative state) [11,12,13], while prediction of awakening is still difficult. In the past 5 years, the construction of a functional brain network based on resting-state EEG has achieved some progress. EEG has a high time resolution and precision and allows dynamic analysis [14], enabling prediction of consciousness recovery. Studies have found that brain network connectivity analysis can differentiate different consciousness states; in particular, compared with patients in a persistent vegetative state (PVS) or with UWS, MCS patients and healthy controls had higher alpha frequency coherence in the parietal-occipital cortex, lower theta frequency coherence in the frontal and frontal-parietal cortices [15,16,17], and enhanced approximate entropy (ApEn) in the whole brain and permutation entropy (PeEn) in the central and temporal cortices [18,19,20]. However, these studies mainly focused on chronic consciousness disorders, while functional brain network studies for acute consciousness disorders have been rare. Therefore, we constructed a functional brain network for LHI patients with an acute consciousness disorder to identify new diagnostic markers related to ECD by analyzing brain network characteristics and mechanisms.
Materials and Methods
Materials
Between August 1, 2017, and September 30, 2018, patients with acute LHI were admitted to the neurocritical care unit (NCU) at Xuanwu Hospital of Capital Medical University. The inclusion criteria were as follows: (1) 18–80 years of age; (2) within 1 month of symptom onset; and (3) unilateral LHI with a volume of at least 2/3 of the territory of the middle cerebral artery as determined neuroradiologically by computed tomography (CT) or magnetic resonance imaging (MRI). The exclusion criteria were as follows: (1) brainstem involvement of the responsible lesion; (2) premorbid conditions such as neurological or psychological disease, brain trauma or surgery; (3) treatment with central nervous system suppressive drugs (such as anesthetics, sedatives and antipsychotics) within 24 h before data collection; and (4) simultaneous multiple organ dysfunction with unstable vital signs. The study observed the principles of the Helsinki Declaration and was approved by the Ethics Committee of Xuanwu Hospital, Capital Medical University, Beijing. Informed consent was obtained from the family members or designated surrogates of all participants.
Methods
The trial was designed as a prospective, blinded cohort study. Participants were dichotomized as the ECD group or the conscious group according to assessments by two experienced neurologists according to Adams and Victor’s Principles of Neurology (9th edition) [21] by evaluating the patient’s wakefulness, verbal and motor response, orientation to person, place and time, and other physical examinations. The Glasgow Coma Scale (GCS) was used to assess the degree of consciousness impairment. To avoid the effect of aphasia, dysarthria and airway management, we adopted a 10-point scale for the GCS (language items removed). The NCU physicians who recorded the clinical data, including age, sex, infarction side, consciousness level, GCS score and the time between onset and EEG recording, were blinded to the EEG results. The researchers who analyzed the EEG results were blinded to the clinical conditions.
EEG Recording
EEG data were recorded at the bedside within 1 month of illness onset (not during the period of hypothermia treatment) with NicoletOne software (Nicolet, America) using a 64-electrode EEG wireless 64A system. For each patient, EEG was recorded at least once and lasted for 30 to 60 min. Electrodes were placed according to the international 10–20 system. The data were referenced to the Cpz electrode. Impedances were maintained at less than 5 kΩ. The continuous EEG data were recorded online at a sampling rate of 512 Hz with a bandpass filter in the range of 0.5–70 Hz as well as a 50-Hz notch filter. Frequency bands were divided into delta (0.5–4 Hz), theta (4–8 Hz), alpha (8–13 Hz), and beta (13–30 Hz). During the period of EEG acquisition, all instruments and equipment that might interfere with EEG signals were switched off to ensure that the surroundings were quiet and stable and to avoid signal fluctuations and artifact interference.
Preprocessing
Researchers (State Key Laboratory of Cognitive Neuroscience and Learning, Beijing Normal University) quantitatively analyzed the EEG data, including a frequency spectral analysis (power spectrum analysis), nonlinear analysis (entropy analysis), brain network connectivity analysis (coherence and phase synchronization) and graph theory.
The MATLAB platform (2017b) was used to write programs. First, a 0.5–45-Hz bandpass digital filter was used to attenuate frequency artifacts. Noise caused by eye movement was removed using FastICA. Then, the superfast spherical interpolation method was used to interpolate the bad channels. Next, the continuous EEG data were cut into epochs with a length of 4 s such that we could remove bad signals by visual assessment. Finally, all of the signals were converted to average references after downsampling to 128 Hz, and every channel signal was transformed by the standardized z score procedure before calculating the EEG features.
Quantitative EEG Analysis
Power Spectrum Analysis
The power spectrum is the abbreviation for the power spectral density function and is defined as the signal power per unit frequency band, namely the distribution of signal power in the frequency domain [22]. Processed time-series data were transformed into the frequency domain by a 1024-point fast Fourier transform with Welch’s method. Specifically, data were analyzed with a 512-point moving window with a 256-point overlap. Windowed data were extended to 1024 points by zero-padding to calculate power spectra, yielding an estimation of the power spectra ranging from 0.5 to 30 Hz (frequency resolution: 0.125 Hz). The power spectra of these windows were averaged. After obtaining the power spectral density estimate, frequency bands were divided into delta (δ: 0.5– 4 Hz), theta (θ: 4–8 Hz), alpha (α: 8–13 Hz), and beta (β: 13–30 Hz) to calculate the power spectrum. Finally, each frequency band’s relative power was computed by dividing by the total power of the frequency band into 0.5–30 Hz.
Entropy Analysis
Entropy studies the law of change in EEG activity complexity, which is a nonlinear analysis method. ApEn and PeEn were calculated in our study. ApEn describes the complexity or irregularity of the time sequence. The algorithm of ApEn is based on the phase-space reconstruction method, where the embedded dimension is m, and the time delay is r. Pincus increased the dimension of the phase space from m to m + 1 in the definition of ApEn [23]. The max distance between two vector quantities is used to describe the model. ApEn is obviously related to the values of m and r. According to Pincus’s experience, we usually take r = 0.1–0.2 * SD(u) (SD represents the standard deviation of the sequence {u(i)}). In this paper, ApEn has more reasonable statistical characteristics. Therefore, we take m = 3 and r = 0.2 * SD. A higher ApEn corresponds to a more irregular signal [24, 25]. Similar to ApEn, PeEn is another method used to estimate signal regularity and is based on the phase-space reconstruction method [26]. In the PeEn algorithm, the data of the vector quantity \(X_{i}^{m}\) is mapped to a sequence of a symbol, the probability density function is determined, and the value of PeEn is calculated. PeEn has better noise resistance and a faster operation speed than ApEn [27, 28]. The calculation procedures for ApEn and PeEn are shown in the supplementary materials.
Brain Network Connectivity Analysis
Coherence
Coherence is the spectral cross-correlation between two signals normalized by their power spectra [29]. Coherence was calculated according to the equations in the supplementary materials. Coherence is between 0 and 1, which represent out of synchronization and the higher degree of synchronization, respectively. When the autopower spectral density and cross-power spectral density were calculated, 50 overlapping 4-s epochs were averaged. Then, these values were used in the equations to acquire the coherence function and mean coherence under in the delta, theta, alpha and beta frequency bands.
Phase Synchronization
Phase synchronization is used to measure the dynamic synchronization of two signals by calculating the phase of two signals in the same frequency band [30]. It has two advantages: (1) the information extracted by coherence and phase synchronization is different, and sometimes no correlation exists between spectral power of signals, but a correlation exists between phases; and (2) phase synchronization is suitable for EEG analysis because it requires little signal stationarity [31]. The calculation steps are shown in the supplementary materials online. If the phase difference is uniformly or randomly distributed, then γ moves to zero. If the phase difference is synchronous, then γ tends to move to one.
Graph Theory
Graph theory is a branch of discrete mathematics that has been applied in numerous studies of both structural and functional brain networks. A graph is a collection of objects, called vertices or nodes; the pairwise relationships among nodes are called edges or links [32]. Many calculation methods exist for graph theory. We face one big problem: how to transform the connection matrix to a binary connection matrix by selecting the threshold value r. However, no theory is available to help us ensure this transformation. Additionally, many studies always select its value by testing many times, ranging from the smallest value to the largest value in the matrix. Therefore, in our study, a weighted undirected connection matrix was used to calculate the graph index, and the codes are provided in the Brain Connectivity Toolbox (BCT, Version 2017-15-01, https://sites.google.com/site/bctnet/Home) [33]. In this work, we select small-worldness to estimate the affected brain networks. Thus, we should consider three parameters: the clustering coefficient, average path length and small-worldness. The average path length represents the shortest path through which nodes are related to each other [34]. The clustering coefficient of a node is calculated as the number of existing connections between the node’s neighbors divided by all their possible connections [35]. In 1998, Watts and Strogatz algorithmically defined for the first time a class of networks with topological properties similar to social networks, demonstrating both the high clustering of a lattice and the short path length of a random graph, which they called small-world networks. The ratio of the normalized average clustering coefficient to the normalized characteristic path length is called the small-worldness [36]. The specific calculation equations for the three parameters are shown in the supplementary materials online.
Statistical Analysis
Brain network connectivity data were calculated using MATLAB software. The permutation test was used for statistical analyses and is suitable for small sample data with an unknown population distribution and for hypothesis-testing problems that are difficult to analyze by conventional methods. By replacing the sample order, the statistical test quantity is recalculated to construct the distribution probability of the mean value, and then the P value is calculated and inferred on this basis. P < 0.05 was considered statistically significant.
Results
Patient Baseline Data
Thirty LHI patients were enrolled in the study (Fig. 1). For each participant, EEG was recorded at least once, and 38 recordings were taken in total. Among the 30 patients, 22 patients were in the ECD group and had 25 EEG recordings (11 left infarction, 14 right infarction), and 8 patients were in the conscious group and had 13 EEG recordings (9 left infarction, 4 right infarction) (Tables 1, 2).
Quantitative EEG Analysis
Spectral Power Analysis
Left LHI patients: The conscious group had higher beta relative spectral power in the whole brain and alpha spectral power in the frontal-occipital lobe on the infarction contralateral side than the ECD group; among these areas, the increase in the beta frequency band relative spectral power in the parietal-occipital lobe on the infarction side was significantly different. The conscious group had lower theta and delta spectral power than the ECD group in the central-parietal lobe on the infarction contralateral side (Fig. 2a). Right LHI patients: The conscious group had higher beta relative spectral power in the whole brain and alpha spectral power in the parietal-occipital lobe on the infarction contralateral side than the ECD group; among these areas, the increase in the beta frequency band relative spectral power in the temporal-occipital lobe on the infarction side and frontal–temporal lobe on the infarction contralateral side were significantly different. The conscious group had lower theta frequency band spectral power in the whole brain and delta spectral power in the parietal-occipital lobe on the infarction contralateral side than the ECD group. The decrease in the theta frequency band relative spectral power in the temporal lobe on the infarction side was significantly different (Fig. 2b).
Topography based on relative spectral power: a left LHI patients; b right LHI patients; ECD group was compared with conscious group, significance represents the channel with statistical difference, the greater the absolute value of significance, the greater the difference. ECD early consciousness disorder, LHI large hemispheric infarction
Entropy Analysis
Left LHI patients: The conscious group had higher ApEn and PeEn in the whole brain than the ECD group; the increase in entropy in the central-parietal lobe was significantly different (Fig. 3a, c). Right LHI patients: The conscious group had higher ApEn in nearly the whole brain and higher PeEn in the whole brain than the ECD group; the increase in PeEn in the temporal lobe was significantly different (Fig. 3b, d).
Topography based on ApEn and PeEn: a, b are ApEn topographic maps of LHI patients on the left and right, respectively, c, d are PeEn topographic maps of LHI patients on the left and right, respectively; ECD group was compared with conscious group, the color scale represents the entropy value. The more red the higher the entropy value, and the more blue the lower the entropy value. Significance is the statistical P value, the greater the absolute value of P, the greater the difference. ApEn approximate entropy, ECD early consciousness disorder, LHI large hemispheric infarction, PeEn permutation entropy (Color figure online)
Brain Network Analysis
Coherence
Left LHI patients: The conscious group had higher alpha and beta frequency band coherence in the bilateral frontal-parietal, frontal-occipital and parietal-occipital lobes than the ECD group (Fig. 4a). Right LHI patients: The conscious group had higher alpha coherence in nearly the whole brain, higher beta coherence in the bilateral parietal lobes, higher theta coherence in the bilateral parietal-occipital and frontal-parietal lobes, and higher delta coherence in the bilateral parietal-occipital lobes than the ECD group (Fig. 4b).
Brain connectivity map based on coherence and phase synchronization: a, b are coherence based brain connectivity maps of LHI patients on the left and right, respectively, c, d are phase synchronization-based brain connectivity maps of LHI patients on the left and right, respectively. Early consciousness disorder group was compared with conscious group, the red line means stronger connections and the blue line means weaker connections. LHI large hemispheric infarction (Color figure online)
Phase Synchronization
Left LHI patients: The conscious group had higher alpha and beta frequency band synchronization in the bilateral frontal-central, frontal-parietal and parietal-occipital lobes than the ECD group (Fig. 4c). Right LHI patients: The conscious group had higher alpha synchronization in nearly the whole brain and higher beta, theta and delta synchronization in the bilateral parietal lobes than the ECD group (Fig. 4d).
Graph Theory
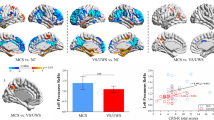
Small-world properties: Regardless of whether the connectivity network was constructed based on coherence or phase synchronization, the conscious group had higher small-worldness in each frequency band than the ECD group, and the differences were statistically significant (Fig. 5a, b). On the infarction side, the small-worldness in the conscious group was not significantly different from that in the ECD group. On the infarction contralateral side, the conscious group had higher small-worldness in each frequency band than the ECD group, and the differences in delta and theta frequency bands were statistically significant (Fig. 6). Clustering coefficient: The conscious group had a higher beta frequency band clustering coefficient than the ECD group (Fig. 5c, d). Average path length: In the functional network constructed based on two kinds of connectivity, the average path lengths in the conscious group in each frequency band were not significantly different from those in the ECD group (Fig. 5e, f).
Graph theoretical analysis using EEG data: a, b represent the differences in the results of small-worldness between the ECD group and the conscious group under the brain functional network constructed based on coherence and phase synchronization, respectively; c, d are the comparison of clustering coefficient between two groups, e, f are the comparison of average path length. Error bars are standard deviations. “*” means the difference is statistically significant. ECD early consciousness disorder
Graph theoretical analysis using EEG data: a, b represent the differences in the results of small-worldness on the infarction side between the ECD group and the conscious group under the brain functional network constructed based on coherence and phase synchronization, respectively; c, d are the comparison of small-worldness on the infarction contralateral side between two groups. Error bars are standard deviations. “*” means the difference is statistically significant. ECD early consciousness disorder
Discussion
Consciousness can be divided into two components: arousal and awareness. The traditional view has been that arousal is maintained by the ascending reticular activating system in the brainstem and thalamus, whereas awareness depends on extensive cortico-cortical connectivity [37]. However, anatomy alone cannot explain all impaired consciousness processes. EEG has high temporal resolution and the sensitivity and specificity to evaluate disturbance of consciousness severity and prognosis [10]. Previous studies have found that EEG patterns and reactivity can predict consciousness recovery [16, 38, 39], but some subjectivity and limitations remain in these analyses, and the mechanisms of consciousness recovery cannot be fully explained.
The spectrum power analysis revealed that conscious group patients had higher alpha and beta frequency band relative spectral power and lower theta and delta spectral power across the whole brain. Matousek et al. [40] found that the amount of EEG slow wave power is significantly correlated with the coma degree. Similar results have been found in studies of patients with chronic consciousness disorders; that is, healthy controls had higher alpha spectral power and lower delta and theta spectral power than VS/UWS and MCS patients [16, 41]. Alpha activity and beta activity have been related to higher brain activities such as cognition, attention and consciousness [42]. Normal people have alpha rhythms in the occipital region when they are awake with their eyes closed. Alpha activity results from the interaction of the thalamus with specific areas of the cortex. Pacemaker neurons distributed in the thalamic region oscillate in the alpha band to regulate and synchronize the excitability of thalamic-cortical pathway cells [43]. Meanwhile, the reticulum nucleus neurons in the brainstem inhibit thalamic pacemaker neurons through gamma-aminobutyric acid (GABA)-ergic action, hyperpolarizing the pacemaker cells and reducing the transmission of relay nucleus neurons to cortical receptors, thereby reducing the average frequency of oscillation and thus converting alpha rhythms into theta rhythms or delta rhythms. In the awake state, delta oscillation is inhibited by ARAS [44], and delta frequency activity is evident only in a pathological state. Therefore, increased alpha and beta band oscillations and decreased delta and theta band oscillations are associated with wakefulness and may be indicators of wakefulness prediction.
As a parameter for analyzing the complexity or irregularity of time series, entropy can provide clues and evidence for the degree of brain function activity. Our ApEn and PeEn analyses found that ApEn and PeEn across the whole brain were higher in conscious group patients. Previous studies have reported that ApEn and PeEn are positively related to the GCS in patients with acute disorders of consciousness [45, 46]. In studies on the chronic stage of consciousness disorders, some researchers also found that the ApEn across the whole brain and PeEn in the central cortex and temporal lobe of UWS patients were significantly lower than those of healthy controls [19, 20]. The reception and processing of information in patients with consciousness disorders have been suggested to be impaired to varying degrees, thus reducing the complexity of brain function activities, and EEG has shown a decrease in information content and information flow [18]. Consciousness is possible only when the network of cortical information can be integrated on a large scale, which is a prerequisite for awakening [47, 48]. Our research found higher ApEn and PeEn and a wider signal distribution range corresponded to a higher the level of consciousness. Therefore, ApEn and PeEn may also be indicators for predicting awakening.
Our brain network connectivity analysis based on coherence and phase synchronization found that compared with the group with ECD, the conscious group showed increased synchronization in nearly the whole brain, but particularly in the frontal-parietal and parietal-occipital lobes, which is consistent with previous studies reporting that disorders of consciousness at early stages of coma are accompanied by a decrease in the levels of EEG coherence of alpha rhythms [49, 50]. For chronic stages, studies also have found that compared with VS/UWS patients, MCS patients and healthy controls have higher alpha band coherence in the parietal-occipital region and lower theta band coherence in the frontal and frontal-parietal regions [15,16,17]. We speculate that LHI patients with ECD have lost the beta and alpha band connectivity between bilateral cerebral hemispheres due to severe infarction in one hemisphere. The connectivity of complex cortical–cortical and thalamo-cortical networks is an important parameter for assessing the level of consciousness [8, 51, 52]. As a parameter of brain connectivity, coherence can measure the coupling degree of the spectrum in different time series. Higher coherence of EEG signals between scalp regions corresponded to stronger functional interactions of the potential neural networks [17]. Phase synchronization is another index that measures the dynamic synchronization of two signals, which is calculated by the phase of two signals in the same frequency band [30]. Regardless of whether a coherence analysis or phase synchronization analysis was used, higher whole-brain connectivity corresponded to a higher level of consciousness. Subsequent graph theory analyses were carried out on the constructed functional network. We found that the small-world properties of the conscious group were significantly higher than those of the ECD group regardless of the network constructed by any method. The clustering coefficient and average path length were not significantly different between the groups. Our finding is comparable to those in previous literature indicating that the number of significant connections in the graphs of coma patients was significantly lower compared to that of healthy controls [53]. Further, most of the latest studies related to graph theory focus on chronic consciousness disorder, and the results are similar to those in our patients with acute consciousness disorder; that is, the brain networks of both the healthy controls and the MCS/UWS patients had efficient and economical small-world properties, the clustering coefficient of the MCS/UWS patients was reduced, the average path length was not significantly different between the MCS/UWS group and the healthy control group, and the large-scale functional brain networks had decreasing integration with lower levels of consciousness [54,55,56]. The small-world structure of neural networks is hypothesized to reflect an optimal configuration associated with rapid synchronization and information transfer, minimal wiring costs, resilience to certain types of damage, as well as a balance between local processing and global integration [57]. We complement this finding by comparing the small-worldness of the stroke-affected and non-affected brains separately in the conscious and ECD groups. We found no significant difference between the two groups on the infarction side, while the small-worldness of the conscious group patients was significantly higher than that of the ECD patients on the infarction contralateral side. These findings suggested that the non-affected brain plays a more important role in determining the consciousness level of LHI patients.
Emerging evidence supports that impaired consciousness is characterized by disruptions of brain networks that sustain arousal and awareness. Our article provides an overview of existing functional connectivity methods used to construct the brain network in LHI patients with ECD and sets a foundation for future studies investigating potential clinical implications of such an approach. Future research should include more patients with accurate long-term longitudinal follow-ups to validate the value of predicting these metrics and provide further guidance for clinical medical decision-making.
The limitations of the study are as follows: (1) due to the small analyzed sample sizes, the representativeness of the results is limited; (2) imaging data were lacking; (3) adding multiple EEGs from the same subjects can also be a confounding factor; (4) EEG signals are corrupted by volume conduction due to the head electrical conduction properties; and (5) graph theory relies on arbitrarily fixing a threshold to retain the strongest connections proportionally equal across subjects, which risks the inclusion of false-positive and therefore spurious connections, especially in the context of brain disorders.
Conclusion
Our study found that in patients with LHI, higher levels of consciousness were associated with more alpha and beta oscillations and fewer delta and theta oscillations. Higher ApEn, PeEn and a wider distribution range corresponded to a higher consciousness level. Higher total brain connectivity and small-worldness also corresponded to a higher level of consciousness. These characteristics may be indicators of recovery. However, considering the limitation of the small sample size in this study, future research should expand the sample size to further confirm the present findings.
References
Torbey MT, Bösel J, Rhoney DH, et al. Evidence-based guidelines for the management of large hemispheric infarction. Neurocrit Care. 2015;22(1):146–64.
Li J, Wang D, Tao W, et al. Early consciousness disorder in acute ischemic stroke: incidence, risk factors and outcome. BMC Neurol. 2016;16(1):140.
Achard S, Delon-Martin C, Vertes PE, et al. Hubs of brain functional networks are radically reorganized in comatose patients. Proc Natl Acad Sci USA. 2012;109:20608–13.
Sair HI, Hannawi Y, Li S, et al. Early functional connectome integrity and 1-year recovery in comatose, survivors of cardiac arrest. Radiology. 2018;287(1):247–55.
Norton L, Hutchison RM, Young GB, et al. Disruptions of functional connectivity in the default mode network of comatose patients. Neurology. 2012;78(3):175–81.
Fischer DB, Boes AD, Demertzi A, et al. A human brain network derived from coma-causing brainstem lesions. Neurology. 2016;87(23):2427–34.
Di Perri C, Bastianello S, Bartsch AJ, et al. Limbic hyperconnectivity in the vegetative state. Neurology. 2013;81(16):1417–24.
Vanhaudenhuyse A, Noirhomme Q, Tshibanda LJF, et al. Default network connectivity reflects the level of consciousness in non-communicative brain-damaged patients. Brain. 2010;133(1):161–71.
Fries P. Rhythms for cognition: communication through coherence. Neuron. 2015;88(1):220–35.
Young GB. The EEG in coma. J Clin Neurophysiol. 2000;17(5):473–85.
Liu G, Su Y, Jiang M, et al. Electroencephalography reactivity for prognostication of post-anoxic coma after cardiopulmonary resuscitation: a comparison of quantitative analysis and visual analysis. Neurosci Lett. 2016;626:74–8.
Yang Q, Su Y, Hussain M, et al. Poor outcome prediction by burst suppression ratio in adults with post-anoxic coma without hypothermia. Neuro Res. 2014;36(5):453–60.
Jiang M, Su Y, Liu G, et al. Predicting the non-survival outcome of large hemispheric infarction patients via quantitative electroencephalography: superiority to visual electroencephalography and the Glasgow Coma Scale. Neurosci Lett. 2019;706:88–92.
Park HJ, Friston K. Structural and functional brain networks: from connections to cognition. Science. 2013;342(6158):1238411.
Ller Y, Thomschewski A, Bergmann, et al. Connectivity biomarkers can differentiate patients with different levels of consciousness. Clin Neurophysiol. 2014;125(8):1545–55.
Lehembre R, MarieAurélie B, Vanhaudenhuyse A, et al. Resting-state EEG study of comatose patients: a connectivity and frequency analysis to find differences between vegetative and minimally conscious states. Funct Neurol. 2012;27(1):41–7.
Cavinato M, Genna C, Manganotti P, et al. Coherence and consciousness: study of fronto-parietal gamma synchrony in patients with disorders of consciousness. Brain Topogr. 2015;28(4):570–9.
Sarà M, Pistoia F. Complexity loss in physiological time series of patients in a vegetative state. Nonlinear Dyn Psychol Life Sci. 2010;14(1):1–13.
Sarà M, Pistoia F, Pasqualetti P, et al. Functional isolation within the cerebral cortex in the vegetative state. Neurorehabil Neural Repair. 2011;25(1):35–42.
Thul A, Lechinger J, Donis J, et al. EEG entropy measures indicate decrease of cortical information processing in disorders of consciousness. Clin Neurophysiol. 2016;127(2):1419–27.
Ropper AH, Samuels MA. Adams and victor’s principles of neurology. 9th ed. New York: McGraw-Hill professional; 2009.
Nuwer MR. Quantitative EEG: I. Techniques and problems of frequency analysis and topographic mapping. J Clin Neurophysiol. 1988;5(1):1–43.
Pincus S. Approximate entropy (ApEn) as a complexity measure. Chaos. 1995;5(1):110–7.
Pincus SM. Approximate entropy as a measure of irregularity for psychiatric serial metrics. Bipolar Disord. 2006;8(5 Pt 1):430–40.
Stam CJ. Nonlinear dynamical analysis of EEG and MEG: review of an emerging field. Clin Neurophysiol. 2005;116(10):2266–301.
Bandt C, Pompe B. Permutation entropy: a natural complexity measure for time series. Phys Rev Lett. 2002;88(17):174102.
Ferlazzo E, Mammone N, Cianci V, et al. Permutation entropy of scalp EEG: a tool to investigate epilepsies. Clin Neurophysiol. 2014;125(1):13–20.
Kaufmann A, Kraft B, Michaleksauberer A, et al. Using permutation entropy to measure the electroencephalographic effects of sevoflurane. Anesthesiology. 2008;109(3):448–56.
Shaw JC, Ongley C. The measurement of synchronization. Synchronization of EEG activity in epilepsies; 1972.
Ito J, Nikolaev AR, Leeuwen CV. Spatial and temporal structure of phase synchronization of spontaneous alpha EEG activity. Biol Cybern. 2005;92(1):54–60.
Le M, Quyen V, Foucher J, et al. Comparison of Hilbert transform and wavelet methods for the analysis of neuronal synchrony. J Neurosci Methods. 2001;111(2):83–98.
Hallquist MN, Hillary FG. Graph theory approaches to functional network organization in brain disorders: a critique for a brave new small-world. Netw Neurosci. 2018;3:1–58.
Rubinov M, Sporns O. Complex network measures of brain connectivity: uses and interpretations. Neuroimage. 2010;52(3):1059–69.
Stam CJ, de Haan W, Daffertshofer A, et al. Graph theoretical analysis of magnetoencephalographic functional connectivity in Alzheimer”s disease. Brain. 2008;132(1):213–24.
Onnela JP, Saramaki J, Kertesz J, Kaski K. Intensity and coherence of motifs in weighted complex networks. Phys Rev E Stat Nonlinear Soft Matter Phys. 2005;71(6 Pt 2):065103.
Watts DJ, Strogatz SH. Collective dynamics of small world networks. Nature. 1998;393(6684):440–2.
George A, Richard B, Elizabeth M, et al. Medical aspects of the persistent vegetative state. N Engl J Med. 1994;330(21):1499–508.
Claassen J, Doyle K, Matory A, et al. Detection of brain activation in unresponsive patients with acute brain injury. N Engl J Med. 2019;380(26):2497–505.
Young GB, McLachlan RS, Kreeft JH, et al. An electroencephalographic classification for coma. Can J Neurol Sci. 1997;24(4):320–5.
Matousek M, Takeuchi E, Starmark JE, Stalhammar D. Quantitative EEG analysis as a supplement to the clinical coma scale RLS85. Acta Anaesthesiol Scand. 1996;40(7):824–31.
Lechinger J, Bothe K, Pichler G, et al. CRS-R score in disorders of consciousness is strongly related to spectral EEG at rest. J Neurol. 2013;260(9):2348–56.
Ward LM. Synchronous neural oscillations and cognitive processes. Trends Cogn Sci. 2003;7(12):553–9.
Piarulli A, Bergamasco M, Thibaut A, et al. EEG ultradian rhythmicity differences in disorders of consciousness during wakefulness. J Neurol. 2016;263(9):1746–60.
John ER, Prichep LS. The anesthetic cascade-A theory of how anesthesia suppresses consciousness. Anesthesiology. 2005;102(2):447–71.
Lin M, Chan H, Fang S. Linear and nonlinear EEG indexes in relation to the severity of coma. Conf Proc IEEE Eng Med Biol Soc. 2005;2005:4580–3.
Gosseries O, Schnakers C, Ledoux D, et al. Automated EEG entropy measurements in coma, vegetative state/unresponsive wakefulness syndrome and minimally conscious state. Funct Neurol. 2011;26(1):25–30.
Dehaene S, Changeux JP. Experimental and theoretical approaches to conscious processing. Neuron. 2011;70(2):200–27.
Alkire MT, Hudetz AG, Tononi G. Consciousness and anesthesia. Science. 2008;322(5903):876–80.
Grindel’ OM. Optimal level of EEG coherence and its importance in evaluating the functional state of the human brain. Zh Vyssh Nerv Deiat Im I P Pavlova. 1980;30(1):62–70.
Grindel’ OM. Intercentral correlations in the cerebral cortex according to the EEG coherence index after restoration of consciousness and speech following prolonged coma. Zh Vyssh Nerv Deiat Im I P Pavlova. 1985;35(1):60–7.
Fernández-Espejo D, Soddu A, Cruse D, et al. A role for the default mode network in the bases of disorders of consciousness. Ann Neurol. 2012;72(3):335–43.
Thibaut A, Bruno M, Chatelle C, et al. Metabolic activity in external and internal awareness networks in severely brain-damaged patients. J Rehabil Med. 2012;44(6):487–94.
Malagurski B, Peran P, Sarton B, et al. Topological disintegration of resting state functional connectomes in coma. Neuroimage. 2019;195:354–61.
Crone JS, Soddu A, Holler Y, et al. Altered network properties of the fronto-parietal network and the thalamus in impaired consciousness. NeuroImage Clin. 2014;4:240–8.
Chennu S, Annen J, Wannez S, et al. Brain networks predict metabolism, diagnosis and prognosis at the bedside in disorders of consciousness. Brain. 2017;140(8):2120–32.
Rizkallah J, Annen J, Modolo J, et al. Decreased integration of EEG source-space networks in disorders of consciousness. Neuroimage Clin. 2019;23:101841.
Reijneveld JC, Ponten SC, Berendse HW, Stam CJ. The application of graph theoretical analysis to complex networks in the brain. Clin Neurophysiol. 2007;118(11):2317–31.
Funding
This study was supported by the National Natural Science Foundation Of China (No. 81671037).
Author information
Authors and Affiliations
Contributions
Yingying Su, Gang Liu and Huijin Huang are responsible for conception and design of the study. Acquisition of data was done by Huijin Huang, Mengdi Jiang and Qingxia Jia. Xiaoli Li and Zikang Niu are reponsible for analysis and interpretation of data. Yingying Su, Xiaoli Li, Huijin Huang and Zikang Niu involved in drafting the article or revising it critically for important intellectual content. All authors approved the fnal version of this manuscript for publication.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval/informed consent
The study observed the principles of the Helsinki Declaration and was approved by the Ethics Committee of Xuanwu Hospital, Capital Medical University, Beijing. Informed consent was obtained from the family members or designated surrogates of all participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Huang, H., Niu, Z., Liu, G. et al. Early Consciousness Disorder in Acute Large Hemispheric Infarction: An Analysis Based on Quantitative EEG and Brain Network Characteristics. Neurocrit Care 33, 376–388 (2020). https://doi.org/10.1007/s12028-020-01051-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-020-01051-w