Abstract
Optimum but balanced food intake maintains healthy growth and disease-free lifespan. However, imbalanced and over-nutrition promotes obesity, diabetes, malignancy, osteoporosis, infectious diseases, etc. In 1936, McCay reported that calorie restriction prevents weight gain and extend lifespan in rodents. In early 1970, Dr. Good at University of Minnesota and Dr. Walford at UCLA began studies in mice by reducing protein and calorie intake and studying their impact on immune function. Dr. Good’s group (Jose, Fernandes, Kramer, Cooper, Day, etc.) reported changes in humoral and cellular immunity at present known as innate and adaptive immune function. Later, much interest was devoted by late Dr. Good on studying the role of calorie restriction (CR) and the role of zinc on immunity, particularly their role on aging, autoimmunity, and malignancy. Both functional role of T-cells, NK-cells and B-cells and their interaction during CR was studied extensively. We recently decided to pursue the beneficial effects of n-3 fatty acids (fish oil) with and without CR on controlling autoimmune-disease in NZB × NZW F1 mice. Our results indicated that n-3 FA when fed ad-libitum prolongs lifespan higher than commonly consumed n-6 FA (corn oil) in these mice. Moreover, n-3 FA + CR is found to be more effective than n-6 FA + CR. Some of the beneficial changes by n-3 FA include enhancing antioxidant enzymes and lowering Th-1/Th-2 cytokines, adhesion molecules, COX-2/PGE2 levels, pro-inflammatory cytokines (IL-1β, IL-6 and TNF-α etc. The decreased pro-inflammatory cytokines were also found to protect against bone loss in OVX mice. Further, Fat-1 transgenic mice (which make n-3 FA endogenously in vivo from n-6 FA) when fed CR revealed decreased NF-κB and AP-1 activity and increased expression of life-prolonging gene SIRT1. Also CR and n-3 FA decreases body weight and increases insulin sensitivity, as well. Thus, to prevent obesity decreased calorie intake with n-3 FA supplement is far more effective and may have protection against CVD, malignancy, autoimmunity, and osteoporosis. The CR studies undertaken in primates and recently in humans are showing very encouraging results. Inorder to understand more precisely the role of diet and nutrition, new approaches exploring the link through nutrigenomics, proteomics and metabolomics may soon provide insight into controlling age-related diseases by following a balanced food intake.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The field of nutrition and immunology was originally developed by Dr. Robert A. Good in early 1970 at the University of Minnesota along with Drs. Yunis, Fernandes, Jose, Cooper, Kramer etc [1]. Interestingly, I also studied with Ranadive in early 1960, in India, the role of nutrition, particularly the use of pharmaceutical waste products as a dietary supplements, to increase the yield of eggs and meat in chickens and to improve the breeding performance in rats and mice, primarily because at that time, commercially pelleted diets for feeding laboratory animals were not available [2–5]. Due to this prior experience in nutrition and animal studies, I was fortunate to join Yunis’s lab in 1968 and able to continue my nutrition studies with Yunis and particularly with Good and published a series of papers, studying the role of nutrition on breeding of mice and its influence on autoimmunity and renal disease in NZB and NZB × NZWF1 mice [6, 7]. However, most active work on nutrition and cellular immunity was, however, carried out by Jose and Good in early 1970, which received much attention to appreciate the protein deficiency and its relationship to cellular immunity [8–12]. Since Dr. Good is a noted pediatrician, he too immediately recognized and fostered nutrition research to study the impact of either nutrition deficiency during early growth and development or the adverse effects of excess nutrition on obesity, cancer, and particularly on aging. Soon with Yunis and Good, I also undertook a series of studies in the area of calorie restriction to prevent the development of renal disease and to reduce breast cancer in mice [13–17]. Later when Dr. Good moved to New York to head the Sloan Kettering Institute, he persuaded me to join him to continue our close and active collaborative work in the field of calorie restriction and aging. The brief summary of the impact of ad-libitum food intake on diseases of aging (Tables 1, 2) was very much in mind of Dr. Good and he was keen on studying various cellular and molecular mechanisms involved in reducing the development of autoimmune disease, cancer, and delaying the aging process by calorie restriction which he actively pursued with many of his young investigators in Oklahoma and at St. Petersburg, Tampa, Florida as well with me in San Antonio [18–34]. Dr. Good and we also studied in early years using short lived NZB × NZW F1 autoimmune prone mice fed ad-libitum (AL) were found to respond to AL feeding and found to die much earlier with kidney disease by becoming obese, whereas, CR fed mice maintain much less body weight and found to live significantly longer than AL fed high-fat or low-fat fed mice (Fig. 1).
Calorie restriction
The earliest evidence that CR retards aging and extends median and maximum lifespan in rodents was first presented in the 1930s by McCay et al. [35]. Since then similar observations have been made in several species including mice, rats, fish, etc. [36, 37]. Our own CR studies which had began over 30 years ago with Dr. Good, have investigated the role of CR on mammary cancer [13], autoimmune disease [16], and aging mice and rats [38–40]. Earlier studies undertaken in CR fed mice for changes in immune functions were also carried out at the same period by Walford and Weindruch et al. [41–43]. We also reported marked changes in IL-2 production [20, 44], Th1/Th2 subsets, changes in insulin receptors and an increased long-chain FA [45, 46]. In addition, we reported increased levels of free-radical scavenging antioxidant enzymes in CR fed mice [46]. Recently, caloric or energy restriction was shown to down regulate expression of several genes linked to inflammation by using oligonucleotide microarrays [47]. Masoro et al. has made very important observations in rats fed CR lifelong and has reviewed this subject very often [48–50]. Weindruch et al. have also made several key observations including major changes by CR in gene regulation. Due to earlier studies by both Dr. Good and Walford and their coinvestigators, and based on encouraging results seen in rodents, the CR studies were then undertaken later in primates and appear to show several benefits [51–53]. Longevity remains to be still established in these models but delayed death with CR is anticipated. CR fed monkeys have lower-body temperature and insulin concentration than AL fed monkey [54]. It is quite encouraging to note that moderate CR studies in humans are revealing quite encouraging results even with a 6 month dietary duration [55]. The precise mechanism of CR-induced lifespan extension is not fully known, yet several theories have been proposed which were recently discussed briefly by Masoro [48, 49]. Although restricting individual nutrients can extend lifespan, based on extensive studies, cutting down 20–40% macronutrients or calories but keeping same level of vitamins and micronutrients can extend maximal lifespan [48]. Several theories have been put forth for the primary mechanism involved in the extension of lifespan such as 1. The growth retardation hypothesis; 2. Reduction of body fat hypothesis; 3. Reduction of metabolic rate hypothesis; 4. Oxidative damage attenuation hypothesis; 5 Altered glucose-insulin system hypothesis; 6. Alteration of the growth hormone IGF-I Axis hypothesis; and 7. Hormesis hypothesis. However, at present based on recent supportive data the following two hypotheses 1. Oxidation damage attenuation hypothesis and; 2. Attenuation of insulin-like signaling hypotheses are both gaining much more attention for elucidating the mechanism involved in prolonging the lifespan [48, 56].
Due to our published experience with nutrition, immunity and aging we later initiated studies using n-3 FA alone AL or along with CR, we decided to pursue our recent hypotheses i.e., prevention of oxidative damage, inhibition of inflammation, and inhibition of insulin-like signaling pathway by adopting n-3 FA + CR studies. There is evidence that n-3 FA alone increases insulin sensitivity thus combining n-3 FA + CR should have a synergistic effect during aging. Most importantly, we also have pilot data to support these two hypotheses: that n-3 FA + CR decrease inflammatory mediators and that it decreases insulin and glucose and increases adiponectin in CR fed aging mice. Oxidative damage and ROS production by various immune cells follows during aging in many target tissues and are now linked to the functional loss in metabolic energetics [57]. Recent studies have shown that age-dependent increase in mitochondrial oxidative damage induces rise in ROS production [57], and their attenuation by CR [58].
Indeed, inhibition of ROS generation maybe a major cause for the reduction in the mitochondrial DNA (mtDNA) damage in CR. We strongly feel that because of upregulation of antioxidant enzymes by n-3 FA [59] and also by CR [60], it is now strongly linked to the upregulation of anti-inflammatory genes particularly those encoding ROS scavenging proteins [61]. The capability of long-term CR to induce decrease in ROS production has been shown in various tissues by various investigations such as rat mitochondrial gastrocnemius muscle [58] rat heart mitochondria [62] and rat liver mitochondria [63]. It is well-established that mitochondrial DNA plays a major role during the aging process [64]. A series of studies carried out in AL and CR fed rats have shown that long-term CR decreases the rate of mitochondrial H2O2 production and mtDNA oxidative damage in various tissues [58]. It was also shown that the quantitative reduction of mtDNA oxidative damage was closer to that found for mitochondrial free-radical generation in various tissues. We too have noticed increased antioxidant enzymes and decreased free radicals (MDA production) in CR fed animals.
Calorie restriction and SIRT1
In the field of CR and aging research many investigators were searching for life prolonging genes and were fortunate to first identify in yeast a silence information regulator 2 (Sir2) gene [65]. It was induced by CR in yeast and Drosophila and shown to have an effect in life prolonging effect of CR [66]. Deletion of this gene led to the elimination of life prolonging effect of CR. It was simultaneously shown to be a histone deacetylase. The deacetylation of histones lead to the closure of the chromatin in the nucleosome with a suppression of gene transcription. Furthermore, acetylation of histones leads to an opening-up of the chromatin in the nucleosome and an increase in gene transcription. The activity of histone acetylation is dependent upon NAD, which accumulates intracellularly in the absence of glycolysis [67, 68]. These life-prolonging genes have been further identified in mammals and have been given the name sirtuins (SIRT1-7 in humans). Among these SIRT1 is the first to have a role linking it to aging and in metabolic regulation. SIRT1 in mammals has now been shown to deacetylate proteins other than histones. They induce p65, a component of NF-κB signaling pathway and is a major mediator of the transcription of NF-κB dependent pro-inflammatory genes [69]. In addition, SIRT1 also deacetylates FOXO-1 [70] and p53 [71] and thus SIRT1 may have a role in the regulation of metabolism and cell proliferation. SIRT1 has recently been shown to have an important role in metabolic regulation [72]. In fasting or CR fed mice SIRT1 has been shown to be activated by increasing concentrations of pyruvate. SIRT1 in turn stimulates genes which regulate gluconeogenesis like PEPCK and SIRT1 suppresses glycolysis simultaneously [73]. These actions would stimulate hepatic glucose production and reduce glucose utilization. In this role it acts through a physical and functional association with PGC-1a and HNF 4a [73]. It also deacetylates PGC-1a to induce gluconeogenesis. Thus, it may have a hyperglycemia inducing effect and may play a role in the regulation of fasting state during CR. However, it appears that the role of SIRT1 is much more complex and needs more research to elucidate its role in regulation and interaction with various factors like oxidative stress and protection induced by CR during aging. We, however, would like to establish whether the expression of SIRT1 varies between n-6 FA and n-3 FA, fed AL and CR mice, and particularly in transgenic Fat-1+ mice fed CR diet. Elevated SIRT1 is quite apparent in Fat-1+ + CR mice in our pilot studies (unpublished data), and therefore we plan to measure PGC-1a and PPARγ expression along with SIRT1 to see its close interaction during aging, particularly, in mice fed n-3 FA + AL and n-3 FA + CR. We anticipate mice fed n-3 fatty acids and CR may live much longer than mice on corn oil and CR diets.
Role of n-3 fatty acids in health and disease
Since the original report of Bang et al. [74] on the diet consumed by Greenland Eskimos and the decreased incidence of cardiovascular disease (CVD), there has been considerable interest in the use of n-3 fatty acids as dietary supplements, and interest in clinical uses is receiving much attention [75, 76]. Several studies have shown promising results against inflammatory disorders including cardiovascular and autoimmune disorders [77, 78]. It is now accepted that the use of n-3 fatty acids will decrease the risk of CVD in the US population [79]. n-3 fatty acids also decreased the incidence of several chronic diseases that are closely linked particularly to the increase in saturated fat and n-6 vegetable oil consumption in the USA [80]. A recent health study in nurses revealed that higher consumption of fish and n-3 fatty acids as well as fruits and vegetables was associated with a lower risk of heart disease (HD), and particularly HD related deaths [81]. Furthermore, the blood level of n-3 fatty acids is a predictive biomarker for sudden death in men [77, 82]. Although the mechanism of n-3 fatty acid mediated inhibition of inflammation and CVD is not fully understood, a great deal of supportive evidence indicates that alterations in arachidonic acid-eicosanoid pathway intermediates, changes in lipid metabolism and/or decreases in pro-inflammatory cytokine production along with changes in expression of numerous genes and transcription factors are clearly involved [83–88]. Figure 2 shows the synthesis of higher-chain FA and lists the n-6 and n-3 FA sources [89].
The majority of studies on the effects of n-3 fatty acids have been carried out using FO or FO concentrates containing low levels of EPA and DHA. Even when purified EPA or DHA has been used there is a significant interconversion in the body in vivo, therefore, the effects of one without the other cannot be inferred with absolute certainty. However, effects on brain growth and development and visual acuity in infants are ascribed to DHA, since DHA is preferentially taken up in the brain and is found in high concentrations in brain tissue. DHA promotes neurite growth and strengthens the periventricular vascular system against hemorrhage [90].
It is widely accepted that FO, rich in n-3 polyunsaturated fatty acids, protect against several types of cardiovascular diseases such as myocardial infarction, arrhythmia, atherosclerosis, and hypertension [91, 92]. Although, the precise cellular and molecular mechanisms for these beneficial effects are still unknown, one of the mechanisms may be their direct effect on vascular smooth muscle cell functions. These n-3 PUFAs activate K+ ATP channels and inhibit certain types of Ca2+ channels [93]. There are probably at least two mechanisms for these actions: 1) n-3 PUFAs can alter the eicosanoid profile and cytokine-induced expression of inducible nitric oxide synthase and COX-2 through modulation of signaling transduction pathways, 2) n-3 PUFAs also modulate vascular smooth muscle cell proliferation, migration, and apoptosis. Recent studies strongly suggest that DHA has more potent and beneficial effects than EPA in these systems [94]. DHA has also been reported to be the most potent at decreasing plasma triglycerides, and DHA (but not EPA) supplementation significantly increased serum HDL-cholesterol [95, 96] which is associated with more efficient reverse cholesterol transport and reduced risk of coronary heart disease [97]. At least a portion of the hypotriglyceridemic effect of n-3 fatty acids has been attributed to increasing circulating apoE levels [98].
Besides, numerous beneficial effects of n-3 FA on several other chronic diseases including osteoporosis are also encouraging. Even though some earlier clinical fish oil studies did show anticipated benefits, some of the reasons for unfavorable results were the variability in the quantity and quality of FO used, variations in the oils used as controls, variability in patient selection, absence of antioxidants to prevent rancidity of oils, and lack of availability of concentrated FO early on. At present, odor-free oils highly enriched in EPA and DHA are available and only a few capsules per day are needed to produce favorable results [99]. A recent study has shown that dietary supplementation with FO may be beneficial in modifying symptomatic disease activity in SLE patients [100].
Since, n-3 fatty acids have been found to increase apoptosis [101, 102], it is quite possible that combination of various drugs with n-3 FA may increase the death of inflammatory cells, thereby further increasing the therapeutic benefits of the drugs [103]. n-3 FA initially provided beneficial effects in the control of renal disease in animal models and IgA nephropathy in humans [104–107]. Our own studies, either with CR or FO, or recently with a combination of FO and CR, have shown several beneficial effects on antioxidant enzyme mRNA levels in B/W and MRL/lpr mice [59, 99, 108–114]. When B/W mice were fed with either with 5% corn oil or 5% fish oil AL a significantly increased lifespan was noted in FO fed mice. In contrast, when a 5% corn oil diet when fed 40% CR, mice lived much longer almost double the life-span whereas when fed a diet with 5% fish oil with CR they however lived much longer than CO + CR fed mice (Fig. 3). Several recent studies have also shown numerous beneficial effects of n-3 fatty acids on normal strains of mice and rats as well as in healthy humans [115–121]. The beneficial effects of n-3 fatty acids have now been linked to changes in various genes and transcription factors including novel bioactive mediators, for example, resolvins, docosatrienes and protectins [84, 122–125]. Our ongoing studies on T-cell differentiation for Th1 and Th2 cytokine inhibition by n-3 fatty acids and down regulation of NF-κB and other transcription factors (T bet) likely to reveal new mechanistic information.
In the early years of research with n-3 FA, several adverse effects of FO were noted in humans and animals primarily because of oxidation of the oils. We, therefore, undertook detailed studies using vitamin E (vit-E) and we and others also reported much favorable results particularly, the elevated antioxidant enzymes in n-3 FA + CR fed mice which may have decreased free radicals and facilitated in increasing the life span [59] (Fig. 4). Soon afterwards the value of antioxidants on prevention of oxidation, particularly during storage of the capsules was recognized. Currently, odor-free concentrated FO with added antioxidants is regularly available at health food stores. Very recently, FDA approved OMACOR (fish oil) is available to treat hypertriglyceride in patients [126]. Our recent studies clearly showed that concentrated 5/50 DHA enriched fish oil is far more effective in controlling autoimmune disease and increasing the life-span of B/W mice (submitted for publication). Further, our recent studies using low levels of n-3 FA (5%) and CR is also not only showing increased longevity but also showed to prevent bone loss with age as well (ongoing studies).
n-3 fatty acids on bone
Nutritional supplements are compounds that are found in food material that is consumed everyday, therefore any side effects are minimal or none. One such nutritional supplement that affects the pro-inflammatory cytokines and protects bone is n-3 FA. n-3 FA decrease cytokines like IL-1β, IL-6 and TNF-α? thereby, reducing bone resorption [39, 59, 60, 101, 110, 127–129]. We have shown that n-3 FA when fed to ovariectomized young Balb/C mice downregulated the expression of RANKL and inhibits activation of NF-κB suggesting that n-3 FA can inhibit osteoclastogenesis [130]. In the case of mice fed casein and corn oil and when ovariectomized 20% bone was lost whereas casein and FO fed mice had 10% bone loss. Interestingly, mice fed soy protein and corn oil had 13% bone loss whereas, soy + FO had only 3% bone loss indicating that soy proteins + FO had far more protection against bone loss (Fig. 5). Further, the mechanism of bone loss was also linked to increased NF-κB expression. In-vitro when EPA+DHA added to bone marrow cells showed markedly less NF-κB expression, whereas, fatty acids from corn oil (LA + Arachidonic) showed high NF-κB expression (Fig. 6). In another study, long-term feeding of n-3 FA to MRL/lpr mice (6 weeks to 12 months of age) also showed that BMD increased at the end of the treatment period [131]. In other studies using young male rats, n-3 FA have been reported to increase alkaline phosphatase activity [132] and in growing rats, IGF-1 and IGFBP levels increased [133, 134] suggesting that n-3 FA may play a role in increasing bone formation as well. In Table 3 and 4 briefly the immune mechanism involved and the role of n-3 FA in preventing bone loss are listed.
It is well established that loss of body weight, seen after CR, is associated with lower-bone mass. Similarly, male F344 rats, on 40% food restricted (FR) diet also showed lower BMD. This study further reported that with age, rats fed AL lost bone whereas rats fed FR did not loose bone [135]. Middle aged female F344 rats on 40% FR diet had lower-cancellous bone mineral content in the proximal tibia, distal femur and the fourth lumbar vertebra when compared to that of AL rats [136]. In the tibia-fibula junction there was increased bone resorption in the endocortical surface thereby increasing bone marrow space [137]. In aged female Sprague Dawley rats, fed 40% energy restricted diet for 9 weeks, the bones showed reduced BMD [138]. In male Wistar rats, fed 80% food for 4 weeks, lower-bone mass and strength were reported when compared to their AL fed counterparts [139]. In male rhesus monkeys on 30% FR for 6 years, there was significantly reduced bone mineral content [140]. The mechanism by which FR reduces bone mass is not yet clear, but bone modeling in FR animals, especially in the cortical bone, seems to be envelope specific, since endocortical bone formation rates increased significantly but there was no change in the periosteal bone formation rates [137]. We strongly feel that n-3 FA when fed either AL or moderate CR will prevent bone loss during aging. In Fig. 7, we summarize also the immune and molecular mechanism involved in preventing bone loss by n-3 FA.
Fat-1 mouse
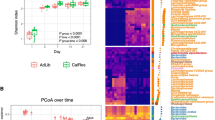
Recently, Kang et al. developed a transgenic (Tg) mouse model that can endogenously synthesize n-3 FA and lowers in vivo n-6 FA. The synthesis of n-3 FA was achieved through the expression of the Fat-1 transgene encoding for an n-3 desaturase from Caenorthabditis elegans which utilizes n-6 FA as a substrate [141, 142]. In wild type mice, the polyunsaturated FA (n-6 FA) found in the tissues are mainly (98%) the linoleic (LA, 18:2n-6) and arachidonic acids (AA, 20:4n-6) with trace amounts of n-3 FA. In contrast, in there transgenic mice, a large amount of n-3 FA including α-linoleic (ALA, 18:3n-3), EPA (20:5n-3) and DHA (22:6n-3) are found in all the tissues [143, 144]. Thus, the levels of n-6 FA LA and AA, in Tg mice tissues are significantly reduced indicating the conversion of n-6 FA to n-3 FA, and hence the ratio of n-6/n-3 is reduced from 20:1 to nearly 1:1. This reduction of n-6/n-3 FA ratio leads to an anti-inflammatory state instead of pro-inflammatory state without feeding any exogenous n-3 FA. We feel that this animal model will be useful to study the role of n-3 FA parallel to exogenously supplied n-3 FA. Last year, we obtained Fat-1 breeding pairs from Dr. Kang, and are bred in-house. We recently crossed Fat-1+ mice with B6 mice and after genotyping the progeny, mice were separated into Fat-1+ x B6 and Fat-1− X B6 mice. These mice have similar genetic background except that Fat-1 gene was found in ∼50% of the mice. This mouse model may be an invaluable tool to establish the role of n-3 FA on longevity both in the absence and in combination with CR. Our pilot data indicate that Fat-1 gene prevents bone loss in OVX mice. Moreover, elevated SIRT1 protein levels and decreased IL-6 and TNF-α cytokines were also observed in Fat-1+ + CR mice (unpublished observation). Thus, we are extremely excited to undertake our proposed CR studies both in B6 mice fed n-3 FA as well as Fat-1 mice with CR. Our recent published studies [145] indicates significantly decreased NF-κB in Fat-1+ + CR fed mice than in Fat-1− + CR fed mice indicating the anti-inflammatory role of n-3 FA particularly along with CR (Fig. 8). Thus, new studies are needed to establish whether moderate CR diet along with consumption of fish or supplementing with fish oil capsule will provide benefits in decreasing age-related on set of diseases particularly CVD and bone loss during aging.
Effect of fat-1 transgenic mice fed calorie restricted on LPS-induced NF-κB p65/p50 activity in cultured splenocytes. WT/AL = wild type ad libitum, WT/CR = wild type calorie restricted, fat-1/AL = fat-1 mice ad libitum, fat-1/CR = fat-1 mice calorie restricted. Bhattacharya et al., BBRC 349:525–530, 2006
Summary
In summary, soon after the discovery of the importance of bone marrow and the thymus in the development of B-cells and T-cells, Dr. Good also established the importance of nutritional deficiency and excess in altering the cellular and humoral immunity and later the changes in innate and adaptive immunity to prevent infection and to enhance the cellular immunity during the protein-calorie deprivation using various animal models. Further, the role of moderate caloric or food restriction in increasing life-span of short lived and long lived animals and in the reduction of mammary cancer was also unfolded by Dr. Good and his coinvestigators.
In later years the functional role of n-3 fatty acids and caloric restriction on reducing the autoimmunity and inflammation particularly the role of n-3 fatty acids on osteoclastogenesis was also established by my coinvestigators and myself. It is with great respect, we recognize the foresight of Dr. Good in pursuing the role of nutrition and diet on immunological function and its relationship on the development of diseases of aging.
References
Good RA, Fernandes G, Yunis EJ, Cooper WC, Jose DC, Kramer TR, Hansen MA. Nutritional deficiency, immunologic function, and disease. Am J Pathol 1976;84(3):599–614.
Fernandes G. Value of Penicillin mycelium residue and liver-meal residue as a supplement to chick diets. Indian J Vet Sci 1960;30:99–106.
Fernandes G, Ranadive KJ. 1962 The value of pharmaceutical waste as a supplement to poultry ration. Proc 12th World Poultry Congress, Sydney Australia:264–71.
Fernandes G, Sandbhor JK. Value of germinated pulses as a supplement to diet of breeding rats. LAIS Bull 1964;11:34–7.
Fernandes G. Some aspects of care and management of inbred strains of mice Indian. J Med Sci 1968;22(5):315–28.
Fernandes G, Yunis EJ, Jose DG, Good RA. Dietary influence on antinuclear antibodies and cell-mediated immunity in NZB mice. Int Arch Allergy Appl immunol 1973;44(6):770–82.
Fernandes G, Yunis EJ, Smith J, Good RA. Dietary influence on breeding behavior, hemolytic anemia, and longevity in NZB mice. Proc Soc Exp Biol Med 1972;139(4):1189–96.
Jose DG, Good RA. Absence of enhancing antibody in cell mediated immunity to tumour heterografts in protein deficient rats. Nature 1971;231(5301):323–5.
Jose DG, Cooper WC, Good RA. How protein deficiency enhances cellular immunity. Jama 1971;218(9):1428–9.
Jose DG, Good RA. Immune resistance and malnutrition. Lancet 1972;1(7745):314.
Jose DG, Good RA. Quantitative effects of nutritional essential amino acid deficiency upon immune responses to tumors in mice. J Exp Med 1973;137(1):1–9.
Jose DG, Good RA. Quantitative effects of nutritional protein and calorie deficiency upon immune responses to tumors in mice. Cancer Res 1973;33(4):807–12.
Fernandes G, Yunis EJ, Good RA. Influence of diet on survival of mice. Proc Natl Acad Sci USA 1976;73(4):1279–83.
Fernandes G, Yunis EJ, Good RA. Suppression of adenocarcinoma by the immunological consequences of calorie restriction. Nature 1976;263(5577):504–7.
Friend PS, Fernandes G, Good RA, Michael AF, Yunis EJ. Dietary restrictions early and late: effects on the nephropathy of the NZB × NZW mouse. Lab Invest 1978;38(6):629–32.
Fernandes G, Friend P, Yunis EJ, Good RA. Influence of dietary restriction on immunologic function and renal disease in (NZB × NZW) F1 mice. Proc Natl Acad Sci USA 1978;75(3):1500–4.
Fernandes G, Yunis EJ, Miranda M, Smith J, Good RA. Nutritional inhibition of genetically determined renal disease and autoimmunity with prolongation of life in kdkd mice. Proc Natl Acad Sci USA 1978;75(6):2888–92.
Day NK, Fernandes G, Witkin SS, Thomas ES, Sarkar NH, Good RA. The effect of diet on autogenous immunity to mouse mammary tumor virus in C3H/Bi mice. Int J Cancer 1980;26(6):813–8.
Izui S, Fernandes G, Hara I, McConahey PJ, Jensen FC, Dixon FJ, Good RA. Low-calorie diet selectively reduces expression of retroviral envelope glycoprotein gp70 in sera of NZB × NZW F1 hybrid mice. J Exp Med 1981;154(4):1116–24.
Jung LK, Palladino MA, Calvano S, Mark DA, Good RA, Fernandes G. Effect of calorie restriction on the production and responsiveness to interleukin 2 in (NZB × NZW)F1 mice. Clin Immunol Immunopathol 1982;25(2):295–301.
Fernandes G, Alonso DR, Tanaka T, Thaler HT, Yunis EJ, Good RA. Influence of diet on vascular lesions in autoimmune-prone B/W mice. Proc Natl Acad Sci USA 1983;80(3):874–7.
Good RA, West A, Day NK, Dong ZW, Fernandes G. Effects of undernutrition of host cell and organ function. Cancer Res 1982;42(2 Suppl):737s–46s.
Hansen MA, Fernandes G, Good RA. Nutrition and immunity: the influence of diet on autoimmunity and the role of zinc in the immune response. Annu Rev Nutr 1982;2:151–77.
Fernandes G, Good RA. Inhibition by restricted-calorie diet of lymphoproliferative disease and renal damage in MRL/lpr mice. Proc Natl Acad Sci USA 1984;81(19):6144–8.
Fernandes G, Chandrasekar B, Troyer DA, Venkatraman JT, Good RA. Dietary lipids and calorie restriction affect mammary tumor incidence and gene expression in mouse mammary tumor virus/v-Ha-ras transgenic mice. Proc Natl Acad Sci USA 1995;92(14):6494–8.
Johnson BC, Gajjar A, Kubo C, Good RA. Calories versus protein in onset of renal disease in NZB × NZW mice. Proc Natl Acad Sci USA 1986;83(15):5659–62.
Engelman RW, Day NK, Chen RF, Tomita Y, Bauer-Sardina I, Dao ML, Good RA. Calorie consumption level influences development of C3H/Ou breast adenocarcinoma with indifference to calorie source. Proc Soc Exp Biol Med 1990;193(1):23–30.
Cherry NN, Engelman RW, Wang BY, Kinjoh K, El-Badri NS, Good RA. Calorie restriction delays the crescentic glomerulonephritis of SCG/Kj mice. Proc Soc Exp Biol Med 1998;218(3):218–22.
Cuenca AG, Cress WD, Good RA, Marikar Y, Engelman RW. Calorie restriction influences cell cycle protein expression and DNA synthesis during liver regeneration. Exp Biol Med (Maywood) 2001;226(11):1061–7.
Patel NV, Gordon MN, Connor KE, Good RA, Engelman RW, Mason J, Morgan DG, Morgan TE, Finch CE. Caloric restriction attenuates Abeta-deposition in Alzheimer transgenic models. Neurobiol Aging 2005;26(7):995–1000.
Johnson BC, Good RA. Chronic dietary restriction and longevity. Proc Soc Exp Biol Med 1990;193(1):4–5.
Good RA, Lorenz E. Nutrition, immunity, aging, and cancer. Nutr Rev 1988;46(2):62–7.
Shao RP, Dao ML, Day NK, Good RA. Dietary manipulation of mammary tumor development in adult C3H/Bi mice. Proc Soc Exp Biol Med 1990;193(4):313–7.
Dao ML, Shao R, Risley J, Good RA. Influence of chronic energy intake restriction on intestinal alkaline phosphatase in C3H/Bi mice and autoimmune-prone MRL/lpr,lpr mice. J Nutr 1989;119(12):2017–22.
McCay CM, Cromwell MF, Maynard LA. The effect of retarded growth upon the length of lifespan and ultimate body size. J Nutr 1935;10:63–79.
Bordone L, Guarente L. Calorie restriction, SIRT1 and metabolism: understanding longevity. Nat Rev Mol Cell Biol 2005;6(4):298–305.
Sinclair DA. Toward a unified theory of caloric restriction and longevity regulation. Mech Ageing Dev 2005;126(9):987–1002.
Venkatraman J, Fernandes G. Modulation of age-related alterations in membrane composition and receptor-associated immune functions by food restriction in Fischer 344 rats. Mech Ageing Dev 1992;63(1):27–44.
Fernandes G. Dietary lipids and risk of autoimmune disease. Clin Immunol Immunopathol 1994;72(2):193–7.
Fernandes G, Venkatraman JT, Turturro A, Attwood VG, Hart RW. Effect of food restriction on life span and immune functions in long-lived Fischer-344 × Brown Norway F1 rats. J Clin Immunol 1997;17(1):85–95.
Weindruch RH, Kristie JA, Naeim F, Mullen BG, Walford RL. Influence of weaning-initiated dietary restriction on responses to T cell mitogens and on splenic T cell levels in a long-lived F1-hybrid mouse strain. Exp Gerontol 1982;17(1):49–64.
Walford RL, Liu RK, Gerbase-Delima M, Mathies M, Smith GS. Longterm dietary restriction and immune function in mice: response to sheep red blood cells and to mitogenic agents. Mech Ageing Dev 1973;2(6):447–54.
Walford R. The immunologic theory of aging. Copenhagen: Munkegaard; 1967.
Iwai H, Fernandes G. Immunological functions in food-restricted rats: enhanced expression of high-affinity interleukin-2 receptors on splenic T cells. Immunol Lett 1989;23(2):125–32.
Venkataraman J, Fernandes G. Influence of food restriction and aging on the binding of insulin to liver nuclei in Fischer 344 rats. Age 1991;14:45–51.
Byun DS, Venkatraman JT, Yu BP, Fernandes G. Modulation of antioxidant activities and immune response by food restriction in aging Fisher-344 rats. Aging (Milano) 1995;7(1):40–8.
Higami Y, Barger JL, Page GP, Allison DB, Smith SR, Prolla TA, Weindruch R. Energy restriction lowers the expression of genes linked to inflammation, the cytoskeleton, the extracellular matrix, and angiogenesis in mouse adipose tissue. J Nutr 2006;136(2):343–52.
Masoro EJ. Overview of caloric restriction and ageing. Mech Ageing Dev 2005;126(9):913–22.
Masoro EJ. Caloric restriction and aging: controversial issues. J Gerontol A Biol Sci Med Sci 2006;61(1):14–9.
Masoro EJ. Subfield history: caloric restriction, slowing aging, and extending life. Sci Aging Knowledge Environ 2003;2003(8):RE2.
Roth GS, Handy AM, Mattison JA, Tilmont EM, Ingram DK, Lane MA. Effects of dietary caloric restriction and aging on thyroid hormones of rhesus monkeys. Horm Metab Res 2002;34(7):378–82.
Lane MA, Mattison J, Ingram DK, Roth GS. Caloric restriction and aging in primates: Relevance to humans and possible CR mimetics. Microsc Res Tech 2002;59(4):335–8.
Cefalu WT, Wagner JD, Bell-Farrow AD, Edwards IJ, Terry JG, Weindruch R, Kemnitz JW. Influence of caloric restriction on the development of atherosclerosis in nonhuman primates: progress to date. Toxicol Sci 1999;52(2 Suppl):49–55.
Roth GS, Ingram DK, Lane MA. Caloric restriction in primates and relevance to humans. Ann NY Acad Sci 2001;928:305–15.
Heilbronn LK, de Jonge L, Frisard MI, DeLany JP, Larson-Meyer DE, Rood J, Nguyen T, Martin CK, Volaufova J, Most MM, Greenway FL, Smith SR, Deutsch WA, Williamson DA, Ravussin E. Effect of 6-month calorie restriction on biomarkers of longevity, metabolic adaptation, and oxidative stress in overweight individuals: a randomized controlled trial. Jama 2006;295(13):1539–48.
Masoro EJ. Caloric intake versus temporal pattern of food intake. Aging Clin Exp Res 2004;16(6):423–4.
Bevilacqua L, Ramsey JJ, Hagopian K, Weindruch R, Harper ME. Long-term caloric restriction increases UCP3 content but decreases proton leak and reactive oxygen species production in rat skeletal muscle mitochondria. Am J Physiol Endocrinol Metab 2005;289(3):E429–38.
Drew B, Phaneuf S, Dirks A, Selman C, Gredilla R, Lezza A, Barja G, Leeuwenburgh C. Effects of aging and caloric restriction on mitochondrial energy production in gastrocnemius muscle and heart. Am J Physiol Regul Integr Comp Physiol 2003;284(2):R474–80.
Venkatraman JT, Chandrasekar B, Kim JD, Fernandes G. Effects of n-3 and n-6 fatty acids on the activities and expression of hepatic antioxidant enzymes in autoimmune-prone NZBxNZW F1 mice. Lipids 1994;29(8):561–8.
Chandrasekar B, Fernandes G. Decreased pro-inflammatory cytokines and increased antioxidant enzyme gene expression by omega-3 lipids in murine lupus nephritis. Biochem Biophys Res Commun 1994;200(2):893–8.
Sreekumar R, Unnikrishnan J, Fu A, Nygren J, Short KR, Schimke J, Barazzoni R, Nair KS. Effects of caloric restriction on mitochondrial function and gene transcripts in rat muscle. Am J Physiol Endocrinol Metab 2002;283(1):E38–43.
Gredilla R, Lopez-Torres M, Barja G. Effect of time of restriction on the decrease in mitochondrial H2O2 production and oxidative DNA damage in the heart of food-restricted rats. Microsc Res Tech 2002;59(4):273–7.
Lopez-Torres M, Gredilla R, Sanz A, Barja G. Influence of aging and long-term caloric restriction on oxygen radical generation and oxidative DNA damage in rat liver mitochondria. Free Radic Biol Med 2002;32(9):882–9.
Barja G. Free radicals and aging. Trends Neurosci 2004;27(10):595–600.
Kaeberlein M, McVey M, Guarente L. The SIR2/3/4 complex and SIR2 alone promote longevity in Saccharomyces cerevisiae by two different mechanisms. Genes Dev 1999;13(19):2570–80.
Rogina B, Helfand SL. Sir2 mediates longevity in the fly through a pathway related to calorie restriction. Proc Natl Acad Sci USA 2004;101(45):15998–6003.
Imai S, Johnson FB, Marciniak RA, McVey M, Park PU, Guarente L. Sir2: an NAD-dependent histone deacetylase that connects chromatin silencing, metabolism, and aging. Cold Spring Harb Symp Quant Biol 2000;65:297–302.
Sauve AA, Schramm VL. Sir2 regulation by nicotinamide results from switching between base exchange and deacetylation chemistry. Biochemistry 2003;42(31):9249–56.
Yeung F, Hoberg JE, Ramsey CS, Keller MD, Jones DR, Frye RA, Mayo MW. Modulation of NF-kappaB-dependent transcription and cell survival by the SIRT1 deacetylase. Embo J 2004;23(12):2369–80.
Brunet A, Sweeney LB, Sturgill JF, Chua KF, Greer PL, Lin Y, Tran H, Ross SE, Mostoslavsky R, Cohen HY, Hu LS, Cheng HL, Jedrychowski MP, Gygi SP, Sinclair DA, Alt FW, Greenberg ME. Stress-dependent regulation of FOXO transcription factors by the SIRT1 deacetylase. Science 2004;303(5666):2011–5.
Vaziri H, Dessain SK, Ng Eaton E, Imai SI, Frye RA, Pandita TK, Guarente L, Weinberg RA. hSIR2(SIRT1) functions as an NAD-dependent p53 deacetylase. Cell 2001;107(2):149–59.
Guarente L, Picard F. Calorie restriction–the SIR2 connection. Cell 2005;120(4):473–82.
Rodgers JT, Lerin C, Haas W, Gygi SP, Spiegelman BM, Puigserver P. Nutrient control of glucose homeostasis through a complex of PGC-1alpha and SIRT1. Nature 2005;434(7029):113–8.
Bang HO, Dyerberg J, Hjoorne N. The composition of food consumed by Greenland Eskimos. Acta Med Scand 1976;200(1–2):69–73.
Yazawa K. Recent development of health foods enriched with DHA, EPA and DPA in Japan. World Rev Nutr Diet 2001;88:249–52.
Lands WE. Impact of daily food choices on health promotion and disease prevention. World Rev Nutr Diet 2001;88:1–5.
Albert CM, Campos H, Stampfer MJ, Ridker PM, Manson JE, Willett WC, Ma J. Blood levels of long-chain n-3 fatty acids and the risk of sudden death. N Engl J Med 2002;346(15):1113–8.
Harper CR, Jacobson TA. The fats of life: the role of omega-3 fatty acids in the prevention of coronary heart disease. Arch Intern Med 2001;161(18):2185–92.
Kris-Etherton PM, Taylor DS, Yu-Poth S, Huth P, Moriarty K, Fishell V, Hargrove RL, Zhao G, Etherton TD. Polyunsaturated fatty acids in the food chain in the United States. Am J Clin Nutr 2000;71(1 Suppl):179S–88S.
Thies F, Miles EA, Nebe-von-Caron G, Powell JR, Hurst TL, Newsholme EA, Calder PC. Influence of dietary supplementation with long-chain n-3 or n-6 polyunsaturated fatty acids on blood inflammatory cell populations and functions and on plasma soluble adhesion molecules in healthy adults. Lipids 2001;36(11):1183–93.
Fung TT, Willett WC, Stampfer MJ, Manson JE, Hu FB. Dietary patterns and the risk of coronary heart disease in women. Arch Intern Med 2001;161(15):1857–62.
Marchioli R, Barzi F, Bomba E, Chieffo C, Di Gregorio D, Di Mascio R, Franzosi MG, Geraci E, Levantesi G, Maggioni AP, Mantini L, Marfisi RM, Mastrogiuseppe G, Mininni N, Nicolosi GL, Santini M, Schweiger C, Tavazzi L, Tognoni G, Tucci C, Valagussa F. Early protection against sudden death by n-3 polyunsaturated fatty acids after myocardial infarction: time-course analysis of the results of the Gruppo Italiano per lo Studio della Sopravvivenza nell’Infarto Miocardico (GISSI)-Prevenzione. Circulation 2002;105(16):1897–903.
Uauy R, Valenzuela A. Marine oils: the health benefits of n-3 fatty acids. Nutrition 2000;16(7–8):680–4.
Hwang D. Fatty acids and immune responses–a new perspective in searching for clues to mechanism. Annu Rev Nutr 2000;20:431–56.
Denys A, Hichami A, Khan NA. Eicosapentaenoic acid and docosahexaenoic acid modulate MAP kinase enzyme activity in human T-cells. Mol Cell Biochem 2002;232(1–2):143–8.
Endres S, Meydani SN, Ghorbani R, Schindler R, Dinarello CA. Dietary supplementation with n-3 fatty acids suppresses interleukin-2 production and mononuclear cell proliferation. J Leukoc Biol 1993;54(6):599–603.
Meydani SN. Effect of (n-3) polyunsaturated fatty acids on cytokine production and their biologic function. Nutrition 1996;12(1 Suppl):S8–14.
Wu D, Meydani SN. n-3 polyunsaturated fatty acids and immune function. Proc Nutr Soc 1998;57(4):503–9.
Lerman RH. Essential fatty acids. Altern Ther Health Med 2006;12(3):20–9; quiz 30-1.
Horrocks LA, Yeo YK. Health benefits of docosahexaenoic acid (DHA). Pharmacol Res 1999;40(3):211–25.
Stark KD, Holub BJ. Differential eicosapentaenoic acid elevations and altered cardiovascular disease risk factor responses after supplementation with docosahexaenoic acid in postmenopausal women receiving and not receiving hormone replacement therapy. Am J Clin Nutr 2004;79(5):765–73.
Mata Lopez P, Ortega RM. Omega-3 fatty acids in the prevention and control of cardiovascular disease. Eur J Clin Nutr 2003;57(Suppl 1):S22–5.
Singer AL, Koretzky GA. Control of T cell function by positive and negative regulators. Science 2002;296(5573):1639–40.
Hirafuji M, Machida T, Hamaue N, Minami M. Cardiovascular protective effects of n-3 polyunsaturated fatty acids with special emphasis on docosahexaenoic acid. J Pharmacol Sci 2003;92(4):308–16.
Mori TA, Burke V, Puddey IB, Watts GF, O’Neal DN, Best JD, Beilin LJ. Purified eicosapentaenoic and docosahexaenoic acids have differential effects on serum lipids and lipoproteins, LDL particle size, glucose, and insulin in mildly hyperlipidemic men. Am J Clin Nutr 2000;71(5):1085–94.
Rambjor GS, Walen AI, Windsor SL, Harris WS. Eicosapentaenoic acid is primarily responsible for hypotriglyceridemic effect of fish oil in humans. Lipids 1996;31(Suppl):S45–9.
Alagona C, Soro A, Ylitalo K, Salonen R, Salonen JT, Taskinen MR. A low high density lipoprotein (HDL) level is associated with carotid artery intima-media thickness in asymptomatic members of low HDL families. Atherosclerosis 2002;165(2):309–16.
Buckley R, Shewring B, Turner R, Yaqoob P, Minihane AM. Circulating triacylglycerol and apoE levels in response to EPA and docosahexaenoic acid supplementation in adult human subjects. Br J Nutr 2004;92(3):477–83.
Kehn P, Fernandes G. The importance of omega-3 fatty acids in the attenuation of immune-mediated diseases. J Clin Immunol 2001;21(2):99–101.
Duffy EM, Meenagh GK, McMillan SA, Strain JJ, Hannigan BM, Bell AL. The clinical effect of dietary supplementation with omega-3 fish oils and/or copper in systemic lupus erythematosus. J Rheumatol 2004;31(8):1551–6.
Fernandes G, Chandrasekar B, Luan X, Troyer DA. Modulation of antioxidant enzymes and programmed cell death by n-3 fatty acids. Lipids 1996;31(Suppl):S91–6.
Avula CP, Zaman AK, Lawrence R, Fernandes G. Induction of apoptosis and apoptotic mediators in Balb/C splenic lymphocytes by dietary n-3 and n-6 fatty acids. Lipids 1999;34(9):921–7.
Grodzicky T, Elkon KB. Apoptosis in rheumatic diseases. Am J Med 2000;108(1):73–82.
Prickett JD, Robinson DR, Steinberg AD. Dietary enrichment with the polyunsaturated fatty acid eicosapentaenoic acid prevents proteinuria and prolongs survival in NZB × NZW F1 mice. J Clin Invest 1981;68(2):556–9.
Robinson DR, Prickett JD, Makoul GT, Steinberg AD, Colvin RB. Dietary fish oil reduces progression of established renal disease in (NZB × NZW)F1 mice and delays renal disease in BXSB and MRL/1 strains. Arthritis Rheum 1986;29(4):539–46.
Robinson DR, Tateno S, Knoell C, Olesiak W, Xu L, Hirai A, Guo M, Colvin RB. Dietary marine lipids suppress murine autoimmune disease. J Intern Med Suppl 1989;731:211–6.
Prickett JD, Trentham DE, Robinson DR. Dietary fish oil augments the induction of arthritis in rats immunized with type II collagen. J Immunol 1984;132(2):725–9.
Jeng KC, Fernandes G. Effect of fish oil diet on immune response and proteinuria in mice. Proc Natl Sci Counc Repub China B 1991;15(2):105–10.
Jolly CA, Muthukumar A, Reddy Avula CP, Fernandes G. Maintenance of NF-kappaB activation in T-lymphocytes and a naive T-cell population in autoimmune-prone (NZB/NZW)F(1) mice by feeding a food-restricted diet enriched with n-3 fatty acids. Cell Immunol 2001;213(2):122–33.
Lim BO, Jolly CA, Zaman K, Fernandes G. Dietary (n-6) and (n-3) fatty acids and energy restriction modulate mesenteric lymph node lymphocyte function in autoimmune-prone (NZB × NZW)F1 mice. J Nutr 2000;130(7):1657–64.
Muthukumar AR, Jolly CA, Zaman K, Fernandes G. Calorie restriction decreases proinflammatory cytokines and polymeric Ig receptor expression in the submandibular glands of autoimmune prone (NZB × NZW)F1 mice. J Clin Immunol 2000;20(5):354–61.
Muthukumar A, Zaman K, Lawrence R, Barnes JL, Fernandes G. Food restriction and fish oil suppress atherogenic risk factors in lupus-prone (NZB × NZW) F1 mice. J Clin Immunol 2003;23(1):23–33.
Muthukumar A, Sun D, Zaman K, Barnes JL, Haile D, Fernandes G. Age associated alterations in costimulatory and adhesion molecule expression in lupus-prone mice are attenuated by food restriction with n-6 and n-3 fatty acids. J Clin Immunol 2004;24(5):471–80.
Reddy Avula CP, Lawrence RA, Zaman K, Fernandes G. Inhibition of intracellular peroxides and apoptosis of lymphocytes in lupus-prone B/W mice by dietary n-6 and n-3 lipids with calorie restriction. J Clin Immunol 2002;22(4):206–19.
Thies F, Nebe-von-Caron G, Powell JR, Yaqoob P, Newsholme EA, Calder PC. Dietary supplementation with eicosapentaenoic acid, but not with other long-chain n-3 or n-6 polyunsaturated fatty acids, decreases natural killer cell activity in healthy subjects aged >55 y. Am J Clin Nutr 2001;73(3):539–48.
Calder PC, Yaqoob P, Thies F, Wallace FA, Miles EA. Fatty acids and lymphocyte functions. Br J Nutr 2002;87(Suppl 1):S31–48.
Calder PC. Polyunsaturated fatty acids, inflammation, and immunity. Lipids 2001;36(9):1007–24.
Wallace FA, Miles EA, Calder PC. Activation state alters the effect of dietary fatty acids on pro-inflammatory mediator production by murine macrophages. Cytokine 2000;12(9):1374–9.
Wallace FA, Miles EA, Evans C, Stock TE, Yaqoob P, Calder PC. Dietary fatty acids influence the production of Th1- but not Th2-type cytokines. J Leukoc Biol 2001;69(3):449–57.
Arrington JL, Chapkin RS, Switzer KC, Morris JS, McMurray DN. Dietary n-3 polyunsaturated fatty acids modulate purified murine T-cell subset activation. Clin Exp Immunol 2001;125(3):499–507.
Arrington JL, McMurray DN, Switzer KC, Fan YY, Chapkin RS. Docosahexaenoic acid suppresses function of the CD28 costimulatory membrane receptor in primary murine and Jurkat T cells. J Nutr 2001;131(4):1147–53.
Clarke SD. Polyunsaturated fatty acid regulation of gene transcription: a molecular mechanism to improve the metabolic syndrome. J Nutr 2001;131(4):1129–32.
Price PT, Nelson CM, Clarke SD. Omega-3 polyunsaturated fatty acid regulation of gene expression. Curr Opin Lipidol 2000;11(1):3–7.
Serhan CN, Arita M, Hong S, Gotlinger K. Resolvins, docosatrienes, and neuroprotectins, novel omega-3-derived mediators, and their endogenous aspirin-triggered epimers. Lipids 2004;39(11):1125–32.
Serhan CN. Novel eicosanoid and docosanoid mediators: resolvins, docosatrienes, and neuroprotectins. Curr Opin Clin Nutr Metab Care 2005;8(2):115–21.
Bays H. Clinical overview of Omacor: a concentrated formulation of omega-3 polyunsaturated fatty acids. Am J Cardiol 2006;98(4A):71i–6i.
Fernandes G, Bysani C, Venkatraman JT, Tomar V, Zhao W. Increased TGF-beta and decreased oncogene expression by omega-3 fatty acids in the spleen delays onset of autoimmune disease in B/W mice. J Immunol 1994;152(12):5979–87.
Chandrasekar B, Troyer DA, Venkatraman JT, Fernandes G. Dietary omega-3 lipids delay the onset and progression of autoimmune lupus nephritis by inhibiting transforming growth factor beta mRNA and protein expression. J Autoimmun 1995;8(3):381–93.
Chandrasekar B, McGuff HS, Aufdermorte TB, Troyer DA, Talal N, Fernandes G. Effects of calorie restriction on transforming growth factor beta 1 and proinflammatory cytokines in murine Sjogren’s syndrome. Clin Immunol Immunopathol 1995;76(3 Pt 1):291–6.
Sun D, Krishnan A, Zaman K, Lawrence R, Bhattacharya A, Fernandes G. Dietary n-3 fatty acids decrease osteoclastogenesis and loss of bone mass in ovariectomized mice. J Bone Miner Res 2003;18(7):1206–16.
Bhattacharya A, Rahman M, Banu J, Lawrence RA, McGuff HS, Garrett IR, Fischbach M, Fernandes G. Inhibition of osteoporosis in autoimmune disease prone MRL/Mpj-Fas(lpr) mice by N-3 fatty acids. J Am Coll Nutr 2005;24(3):200–9.
Watkins BA, Lippman HE, Le Bouteiller L, Li Y, Seifert MF. Bioactive fatty acids: role in bone biology and bone cell function. Prog Lipid Res 2001;40(1–2):125–48.
Li Y, Seifert MF, Ney DM, Grahn M, Grant AL, Allen KG, Watkins BA. Dietary conjugated linoleic acids alter serum IGF-I and IGF binding protein concentrations and reduce bone formation in rats fed (n-6) or (n-3) fatty acids. J Bone Miner Res 1999;14(7):1153–62.
Rosen CJ. Serum insulin-like growth factors and insulin-like growth factor-binding proteins: clinical implications. Clin Chem 1999;45(8 Pt 2):1384–90.
Kalu DN, Hardin RR, Cockerham R, Yu BP, Norling BK, Egan JW. Lifelong food restriction prevents senile osteopenia and hyperparathyroidism in F344 rats. Mech Ageing Dev 1984;26(1):103–12.
Banu J, Orhii PB, Okafor MC, Wang L, Kalu DN. Analysis of the effects of growth hormone, exercise and food restriction on cancellous bone in different bone sites in middle-aged female rats. Mech Ageing Dev 2001;122(8):849–64.
Banu MJ, Orhii PB, Mejia W, McCarter RJ, Mosekilde L, Thomsen JS, Kalu DN. Analysis of the effects of growth hormone, voluntary exercise, and food restriction on diaphyseal bone in female F344 rats. Bone 1999;25(4):469–80.
Talbott SM, Cifuentes M, Dunn MG, Shapses SA. Energy restriction reduces bone density and biomechanical properties in aged female rats. J Nutr 2001;131(9):2382–7.
Boyer PM, Compagnucci GE, Olivera MI, Bozzini C, Roig MC, Compagnucci CV, Alippi RM. Bone status in an animal model of chronic sub-optimal nutrition: a morphometric, densitometric and mechanical study. Br J Nutr 2005;93(5):663–9.
Lane MA, Reznick AZ, Tilmont EM, Lanir A, Ball SS, Read V, Ingram DK, Cutler RG, Roth GS. Aging and food restriction alter some indices of bone metabolism in male rhesus monkeys (Macaca mulatta). J Nutr 1995;125(6):1600–10.
Kang JX, Wang J, Wu L, Kang ZB. Transgenic mice: fat-1 mice convert n-6 to n-3 fatty acids. Nature 2004;427(6974):504.
Kang JX. From fat to fat-1: a tale of omega-3 fatty acids. J Membr Biol 2005;206(2):165–72.
Ma DW, Ngo V, Huot PS, Kang JX. N-3 polyunsaturated fatty acids endogenously synthesized in fat-1 mice are enriched in the mammary gland. Lipids 2006;41(1):35–9.
Lai L, Kang JX, Li R, Wang J, Witt WT, Yong HY, Hao Y, Wax DM, Murphy CN, Rieke A, Samuel M, Linville ML, Korte SW, Evans RW, Starzl TE, Prather RS, Dai Y. Generation of cloned transgenic pigs rich in omega-3 fatty acids. Nat Biotechnol 2006;24(4):435–6.
Bhattacharya A, Chandrasekar B, Rahman MM, Banu J, Kang JX, Fernandes G. Inhibition of inflammatory response in transgenic fat-1 mice on a calorie-restricted diet. Biochem Biophys Res Commun 2006;349(3):925–30.
Acknowledgments
The current ongoing work is supported by NIH grants AG023648 and AG 027562. Also thanks to Dr. Jameela Banu for her kind help in preparing this review paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fernandes, G. Progress in nutritional immunology. Immunol Res 40, 244–261 (2008). https://doi.org/10.1007/s12026-007-0021-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12026-007-0021-3