Abstract
Association between fruit intake and risk of type 2 diabetes is inconsistent. In this study, we performed a meta-analysis of all prospective cohort studies to clarify the association between fruit intake and risk of type 2 diabetes. Relevant studies were identified by searches of the PubMed and Embase databases up to November 2013. The summary relative risks of association were obtained using a fixed- or random-effects model. A total of nine prospective studies (403,259 participants, including 27,940 with incident type 2 diabetes) from seven publications were included in the meta-analysis of fruit intake and risk of type 2 diabetes. We found that individuals in the highest category of fruit intake had a reduced risk of type 2 diabetes (relative risk 0.92, 95 % confidence interval 0.86–0.97, p = 0.003) compared to those in the lowest category, with moderate evidence of between-study heterogeneity (I 2 = 37.6 %, p = 0.12). There was an evident non-linear association of fruit intake with type 2 diabetes (P for nonlinearity <0.001). A non-linear threshold of 200 g/day of fruit intake was identified and the risk of type 2 diabetes reduced by about 13 % at this cut-off. Our findings are consistent with diet recommendations to consume about 200 g/day of fruits to prevent type 2 diabetes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes is one of the most common chronic diseases worldwide, which is expected to increase to at least 366 million by 2030 [1]. Since type 2 diabetes is one of the main causes of morbidity and premature mortality, the prevention of this disease should be an important public health priority. Results from lifestyle intervention trials have shown dietary modifications as an effective strategy in the prevention of type 2 diabetes [2]. However, the contributions of various foods to the development of type 2 diabetes are not clear.
As is known, fruits contain antioxidants, fibers, vitamins, minerals, and other unidentified phytochemicals that may have beneficial effects on health. Higher intake of fruit has been associated with a reduced risk of several chronic diseases including coronary heart disease [3], stroke [4], and various cancers [5, 6]. To date, several prospective cohort studies have investigated the association between fruit intake and incidence of type 2 diabetes. However, the results are not entirely consistent [7–13]. Two previous meta-analyses suggested that higher intake of fruit was not associated with incident type 2 diabetes [14, 15]. This result is somewhat unexpected given the beneficial effect of fruit intake on several other chronic diseases [3–6]. However, it should be noted that the two meta-analyses mentioned above were based on a limited number of studies [7–10], and the majority of included studies had short follow-up duration (<10 years) [7, 8, 10]. A recent meta-analysis by Cooper et al. [11] involved six studies and the authors did not find any association between fruit intake and type 2 diabetes risk although there was an inverse association in population with longer follow-up (≥10 years). Since publication of the three meta-analyses, results from four new prospective studies have become available [12, 13] which will contribute to greater statistical power for an updated meta-analysis.
Thus, in this study, we propose to conduct a systematic review and an updated meta-analysis to clarify the association of fruit intake with incidence of type 2 diabetes.
Materials and methods
Literature and search strategy
The Meta-analysis of Observational Studies in Epidemiology (MOOSE) guidelines were followed for the current study [16]. The literature databases including PubMed and Embase were searched. Search terms were “fruit” and “type 2 diabetes” or “T2DM”. The reference lists of retrieved articles were also screened. The literature search was limited to the English language. If more than one article was published on the same cohort, only the study with the largest sample size was included. The literature search was updated on November 4, 2013.
Inclusion criteria and data extraction
Studies included in the meta-analysis met the following inclusion criteria: (1) evaluation of the association between fruit intake and incidence of type 2 diabetes, (2) a prospective study design; and (3) covariate adjusted relative risks (RRs) or hazard ratios (HRs) with 95 % confidence intervals (CIs) for highest versus lowest category of fruit. Studies on association between fruit juice or dried fruit and type 2 diabetes were excluded. The following information was extracted from each study: (1) name of the first author; (2) year of publication; (3) country of study; (4) number of incident cases and study population; (5) age distribution of the study population at baseline; (6) sex of the participants; (7) average duration of follow-up; (8) the covariates included in the regression models; and (9) RRs or HRs with 95 % CIs for highest versus lowest category of fruit. Two investigators (SL and ZL) independently assessed the articles for compliance with the inclusion/exclusion criteria and resolved disagreements through discussion.
The quality of each study was assessed by the Newcastle–Ottawa quality scale (NOS) [17], which is a validated scale for non-randomized studies in meta-analyses. This scale assigned a maximum of nine points for each study. Three broad perspectives were considered: the selection of the cohorts (4 points); the comparability of cohorts (2 points); and the ascertainment of the exposure and outcome of interest (3 points).
Statistical analysis
Fixed [18] or random [19] effects model, based on whether there was heterogeneity between studies, was used to calculate pooled RRs with 95 % CIs for highest versus lowest category of fruit. Heterogeneity was assessed by the Q test and the I 2 statistic [20]. The significance for the Q test was defined as p < 0.10. The I 2 statistic represents the amount of total variation attributed to heterogeneity. Low, moderate, and high degrees of heterogeneity correspond to I 2 values of 25, 50, and 75 %, respectively.
For the dose–response analysis, the generalized least square for trend estimation (GLST) method reported by Greenland et al. [21] and Orsini et al. [22] was used to calculate study-specific slopes (linear trends) and 95 % CIs based on the results across categories of fruit intake. The method requires the amount of fruit intake, distributions of cases and person years, and RRs or HRs with 95 % CIs for at least three exposure categories. The median or mean level of fruit intake in each category was assigned to the corresponding RR or HR with 95 % CI for each study. When fruit intake was reported by ranges of intakes, the midpoint of the range was used. When the highest category was open-ended, we assumed the width of the category to be the same as the adjacent category. When the lowest category was open-ended, we set the lower boundary to zero [23, 24]. If studies reported intakes as frequency, we used 100 g as a serving size for recalculation of the intake to a common scale (g/day) [25]. A two-stage GLST model was used to synthesize the study-specific linear component and the non-linear fractional polynomials component generated by the restricted cubic spline model. The potential nonlinearity was to test whether the coefficient of the fractional polynomials component is equal to zero [26].
Sensitivity analysis was performed to assess the stability of the results. Publication bias was assessed by Egger’s test [27] (p < 0.05 was considered statistically significant). Statistical analysis was conducted using STATA version 11 (StataCorp LP, College Station, TX, USA).
Results
Study characteristics
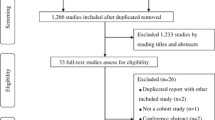
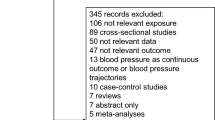
Figure 1 shows the process of study selection for the meta-analyses of fruit intake and risk of incident type 2 diabetes. A total of nine studies from seven publications were included in the meta-analysis. In the publication by Muraki et al. [13], results were reported for the three studies: the Nurses’ Health Study, the Nurses’ Health II Study, and the Health Professionals Follow-up Study, and treated as three separate studies in the current analysis. The characteristics of the studies included in the meta-analyses are summarized in Table 1. Five studies were from the USA, two studies from Europe, and two studies from East Asia; the duration of follow-up ranged from 4.6 to 25 years.
Meta-analysis of fruit intake and risk of developing type 2 diabetes
Highest versus lowest
A total of 403,259 participants, including 27,940 with incident type 2 diabetes were included in the meta-analysis. The pooled result suggested that individuals with a higher intake of fruit had a lower risk of developing type 2 diabetes (highest vs. lowest level: RR = 0.92, 95 % CI 0.86–0.97, p = 0.003, Fig. 2), with moderate evidence of between-study heterogeneity (I 2 = 37.6 %, p = 0.12). The association was significant with and without adjustment for BMI (Table 2).
In subgroup analyses (Table 2), the association was significant in women only (RR = 0.92, 95 % CI 0.86–0.99, p = 0.03), studies with follow-up longer than 10 years (RR = 0.86, 95 % CI 0.79–0.93, p < 0.001), and studies with high quality (RR = 0.87, 95 % CI 0.81–0.94, p = 0.001). However, there was no significant association in men (RR = 0.97, 95 % CI 0.83–1.14, p = 0.75), studies with short duration of follow-up (RR = 0.98, 95 % CI 0.90–1.07, p = 0.65), and studies with relatively low quality (RR = 0.98, 95 % CI 0.89–1.08, p = 0.68).
Dose–response analysis
There was an evident non-linear association of fruit intake with type 2 diabetes (P for nonlinearity < 0.001, Fig. 3). A non-linear threshold of 200 g/day fruit intake was identified and the risk of type 2 diabetes reduced by about 13 % at this cut-off (Fig. 3).
Sensitivity analysis
To examine the stability of the observed significant association, we performed sensitivity analyses after excluding the study by Cooper et al. [11] with the largest number of individuals with type 2 diabetes and the study by Montonen et al. [9] with the smallest number of individuals with type 2 diabetes. The pooled RRs and 95 % CIs for the remaining studies were 0.92 (0.86–0.98, p = 0.01) and 0.93 (0.87–0.98, p = 0.01), respectively.
Potential publication bias
No publication bias was detected (p = 0.47 for Egger’s test).
Discussion
Based on the present meta-analysis, individuals in the top category of fruit intake had an 8 % lower risk of incident of type 2 diabetes compared to those in the bottom category. Previous epidemiological studies have reported inconsistent findings for an association between fruit intake and risk of developing type 2 diabetes [7–13]. Two previous independent meta-analyses showed no association between fruit intake and risk of incident type 2 diabetes [14, 15]. It should be noted that compared with our current updated meta-analysis, several limitations exist in both previous meta-analyses. First, both meta-analyses were based on a limited number of studies. That is, the first meta-analysis included four studies [7–9, 28] and the second one included five studies [7–10, 29]. However, the current meta-analysis includes nine studies [7–13]. Second, the majority of studies included in both previous meta-analyses had short duration of follow-up (<10 years). However, nearly half of the studies included in the current meta-analysis had greater than 10 years of follow-up (long duration). Third, significant between-study heterogeneity existed in both previous meta-analyses, with p for heterogeneity being 0.009 and 0.07, respectively. However, nine studies included in the current meta-analysis were homogeneous (p = 0.16). Thus, based on this evidence, it is not surprising that a protective effect was observed in the present study with sufficient sample size for fruit intake on risk of developing type 2 diabetes, while previous meta-analyses did not. The two previous meta-analyses obtained a risk reduction of type 2 diabetes with increasing fruit intake ranging between 7 and 10 %. The present meta-analysis reported an estimate of reduced risk of 8 %, not being different from that of the two previous meta-analyses. However, the risk reduction of type 2 diabetes was small and lower than that obtained with healthy dietary patterns having reduction of type 2 diabetes ranging from 15 to 83 % [30–32].
Several biological mechanisms might explain the inverse association between fruit intake and risk of type 2 diabetes. First, the inverse association may be mediated through weight gain or obesity which is an established risk factor for type 2 diabetes. Fruits are low in energy, but high in fiber, which would promote the feeling of fullness and prevent over consumption of energy-dense foods; potentially, resulting in weight loss [33]. It should be noted that adjustment for BMI would be an over correction. However, results of studies included in the current meta-analysis that were adjusted for BMI did not change the significantly inverse association between fruit intake and risk of type 2 diabetes (Table 2). Second, fruits are rich in polyphenols, such as flavonoids and antioxidant compounds including carotenoids, vitamin C and E. These compounds may decrease risk of type 2 diabetes by mitigating the oxidative stress that interferes with the glucose uptake by cells [34]. Intake of antioxidants has reportedly improved endothelial function in individuals with non-obese type 2 diabetes [35] as well as lowered the risk of incident type 2 diabetes [14]. Third, fruits are rich in fiber, which has also been related to improved insulin sensitivity [36]. In addition, fiber from fruits may delay the absorption of carbohydrates and then inhibit the postprandial glucose load [9].
Our study has several strengths, including the prospective study design, large sample size, long follow-up duration, and relatively precise RRs (95 % CIs) adjusted for potential confounders in the studies included in the current meta-analysis. However, several limitations should be considered. First, although most known confounding factors have been controlled for, residual confounding or confounding from unmeasured factors cannot be ruled out. Second, the majority of included studies assessed dietary intake data at baseline, but change in dietary intake pattern over time was not considered. However, the non-differential misclassification tends to attenuate the observed association toward the null. In other words, the inverse association between fruit and risk of type 2 diabetes may potentially be stronger than reported presently. Third, although several studies included in the meta-analysis used validated self-reported method to identify type 2 diabetes, the potential misclassification of individuals with undiagnosed type 2 diabetes may also have attenuated our findings.
In conclusions, findings from the current meta-analysis support dietary recommendations to consume about 200 g/day of fruits to prevent the development of type 2 diabetes. However, large randomized controlled trials are warranted to confirm the observed study finding.
Abbreviations
- CI:
-
Confidence interval
- HR:
-
Hazard ratio
- RR:
-
Relative risk
References
J.E. Shaw, R.A. Sicree, P.Z. Zimmet, Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res. Clin. Pract. 87, 4–14 (2010)
C.L. Gillies, K.R. Abrams, P.C. Lambert, N.J. Cooper, A.J. Sutton, R.T. Hsu, K. Khunti, Pharmacological and lifestyle interventions to prevent or delay type 2 diabetes in people with impaired glucose tolerance: systematic review and meta-analysis. BMJ. 334, 299 (2007)
L. Dauchet, P. Amouyel, S. Hercberg, J. Dallongeville, Fruit and vegetable consumption and risk of coronary heart disease: a meta-analysis of cohort studies. J. Nutr. 136, 2588–2593 (2006)
F.J. He, C.A. Nowson, G.A. MacGregor, Fruit and vegetable consumption and stroke: meta-analysis of cohort studies. Lancet. 367, 320–326 (2006)
D. Aune, D.S. Chan, A.R. Vieira, D.A. Rosenblatt, R. Vieira, D.C. Greenwood, T. Norat, Fruits, vegetables and breast cancer risk: a systematic review and meta-analysis of prospective studies. Breast Cancer Res. Treat. 134, 479–493 (2012)
J. Liu, J. Wang, Y. Leng, C. Lv, Intake of fruit and vegetables and risk of esophageal squamous cell carcinoma: a meta-analysis of observational studies. Int. J. Cancer 133, 473–485 (2013)
K.A. Meyer, L.H. Kushi, D.R. Jacobs Jr, J. Slavin, T.A. Sellers, A.R. Folsom, Carbohydrates, dietary fiber, and incident type 2 diabetes in older women. Am. J. Clin. Nutr. 71, 921–930 (2000)
S. Liu, M. Serdula, S.J. Janket, N.R. Cook, H.D. Sesso, W.C. Willett, J.E. Manson, J.E. Buring, A prospective study of fruit and vegetable intake and the risk of type 2 diabetes in women. Diabetes Care 27, 2993–2996 (2004)
J. Montonen, R. Järvinen, M. Heliövaara, A. Reunanen, A. Aromaa, P. Knekt, Food consumption and the incidence of type II diabetes mellitus. Eur. J. Clin. Nutr. 59, 441–448 (2005)
R. Villegas, X.O. Shu, Y.T. Gao, G. Yang, T. Elasy, H. Li, W. Zheng, Vegetable but not fruit consumption reduces the risk of type 2 diabetes in Chinese women. J. Nutr. 138, 574–580 (2008)
A.J. Cooper, N.G. Forouhi, Z. Ye, B. Buijsse, L. Arriola, B. Balkau, A. Barricarte, J.W. Beulens, H. Boeing, F.L. Büchner, C.C. Dahm, B. de Lauzon-Guillain, G. Fagherazzi, P.W. Franks, C. Gonzalez, S. Grioni, R. Kaaks, T.J. Key, G. Masala, C. Navarro, P. Nilsson, K. Overvad, S. Panico, J. Ramón Quirós, O. Rolandsson, N. Roswall, C. Sacerdote, M.J. Sánchez, N. Slimani, I. Sluijs, A.M. Spijkerman, B. Teucher, A. Tjonneland, R. Tumino, S.J. Sharp, C. Langenberg, E.J. Feskens, E. Riboli, N.J. Wareham, InterAct consortium. Fruit and vegetable intake and type 2 diabetes: EPIC-InterAct prospective study and meta-analysis. Eur. J. Clin. Nutr. 66, 1082–1092 (2012)
K. Kurotani, A. Nanri, A. Goto, T. Mizoue, M. Noda, M. Kato, M. Inoue, S. Tsugane, Japan Public Health Center-based Prospective Study Group. Vegetable and fruit intake and risk of type 2 diabetes: Japan Public Health Center-based Prospective Study. Br. J. Nutr. 109, 709–717 (2013)
I. Muraki, F. Imamura, J.E. Manson, F.B. Hu, W.C. Willett, R.M. van Dam, Q. Sun, Fruit consumption and risk of type 2 diabetes: results from three prospective longitudinal cohort studies. BMJ. 347, f5001 (2013)
M. Hamer, Y. Chida, Intake of fruit, vegetables, and antioxidants and risk of type 2 diabetes: systematic review and meta-analysis. J. Hypertens. 25, 2361–2369 (2007)
P. Carter, L.J. Gray, J. Troughton, K. Khunti, M.J. Davies, Fruit and vegetable intake and incidence of type 2 diabetes mellitus: systematic review and meta-analysis. BMJ. 341, c4229 (2010)
D.F. Stroup, J.A. Berlin, S.C. Morton, I. Olkin, G.D. Williamson, D. Rennie, D. Moher, B.J. Becker, T.A. Sipe, S.B. Thacker, Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA. 283, 2008–2012 (2000)
Wells GA, Shea B, O’connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed October 2013
R. DerSimonian, N. Laird, Meta-analysis in clinical trials. Control. Clin. Trials 7, 177–188 (1986)
N. Mantel, W. Haenszel, Statistical aspects of the analysis of data from retrospective studies of disease. J. Natl. Cancer Inst. 22, 719–748 (1959)
J.P. Higgins, S.G. Thompson, J.J. Deeks, D.G. Altman, Measuring inconsistency in meta-analyses. BMJ. 327, 557–560 (2003)
S. Greenland, M.P. Longnecker, Methods for trend estimation from summarized dose–response data, with applications to meta-analysis. Am. J. Epidemiol. 135, 1301–1309 (1992)
N. Orsini, R. Bellocco, S. Greenland, Generalized least squares for trend estimation of summarized dose–response data. Stata J. 6, 40–57 (2006)
Y. Rong, L. Chen, T. Zhu, Y. Song, M. Yu, Z. Shan, A. Sands, F.B. Hu, L. Liu, Egg consumption and risk of coronary heart disease and stroke: dose–response meta-analysis of prospective cohort studies. BMJ. 346, e8539 (2013)
D.E. Threapleton, D.C. Greenwood, C.E. Evans, C.L. Cleghorn, C. Nykjaer, C. Woodhead, J.E. Cade, C.P. Gale, V.J. Burley, Dietary fibre intake and risk of cardiovascular disease: systematic review and meta-analysis. BMJ. 347, f6879 (2013)
E. Riboli, T. Norat, Epidemiologic evidence of the protective effect of fruit and vegetables on cancer risk. Am. J. Clin. Nutr. 78, 559S–569S (2003)
P. Royston, A strategy for modelling the effect of a continuous covariate in medicine and epidemiology. Stat. Med. 19, 1831–1847 (2000)
M. Egger, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 315, 629–634 (1997)
G.A. Colditz, J.E. Manson, M.J. Stampfer, B. Rosner, W.C. Willett, F.E. Speizer, Diet and risk of clinical diabetes in women. Am. J. Clin. Nutr. 55, 1018–1023 (1992)
L.A. Bazzano, T.Y. Li, K.J. Joshipura, F.B. Hu, Intake of fruit, vegetables, and fruit juices and risk of diabetes in women. Diabetes Care 31, 1311–1317 (2008)
K. Esposito, C.M. Kastorini, D.B. Panagiotakos, D. Giugliano, Prevention of type 2 diabetes by dietary patterns: a systematic review of prospective studies and meta-analysis. Metab. Syndr. Relat. Disord. 8, 471–476 (2010)
Esposito K, Chiodini P, Maiorino MI, Bellastella G, Panagiotakos D, Giugliano D. Which diet for prevention of type 2 diabetes? A meta-analysis of prospective studies. Endocrine:1-10 (2014)
K. Hodgson, B. Govan, N. Ketheesan, J. Morris, Dietary composition of carbohydrates contributes to the development of experimental type 2 diabetes. Endocrine 43, 447–451 (2013)
A.H. Harding, N.J. Wareham, S.A. Bingham, K. Khaw, R. Luben, A. Welch, N.G. Forouhi, Plasma vitamin C level, fruit and vegetable consumption, and the risk of new-onset type 2 diabetes mellitus: the European prospective investigation of cancer—Norfolk prospective study. Arch. Intern. Med. 168, 1493–1499 (2008)
M. Gordon, Dietary antioxidants in disease prevention. Nat. Prod. Rep. 13, 265–273 (1996)
D. Montero, G. Walther, C.D. Stehouwer, A.J. Houben, J.A. Beckman, A. Vinet, Effect of antioxidant vitamin supplementation on endothelial function in type 2 diabetes mellitus: a systematic review and meta-analysis of randomized controlled trials. Obes. Rev. (2013). doi:10.1111/obr.12114
A.D. Liese, A.K. Roach, K.C. Sparks, L. Marquart, R.B. D’Agostino Jr, E.J. Mayer-Davis, Whole-grain intake and insulin sensitivity: the insulin resistance atherosclerosis study. Am. J. Clin. Nutr. 78, 965–971 (2003)
Conflict of interest
None
Author information
Authors and Affiliations
Corresponding authors
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, S., Miao, S., Huang, Y. et al. Fruit intake decreases risk of incident type 2 diabetes: an updated meta-analysis. Endocrine 48, 454–460 (2015). https://doi.org/10.1007/s12020-014-0351-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-014-0351-6