Abstract
Type 1 diabetes mellitus (T1DM) is a T cell-mediated autoimmune disease characterized by the destruction of pancreatic β cells. Numerous studies have demonstrated the key role of CD4+CD25+FoxP3+ regulatory T cells (Tregs) in the development of T1DM. However, the changes in Treg expression and function as well as the regulation of these activities are not clearly elucidated. Most studies on the role of Tregs in T1DM were performed on peripheral blood rather than pancreas or pancreatic lymph nodes. Tissue-based studies are more difficult to perform, and there is a lack of histological data to support the role of Tregs in T1DM. In spite of this, strategies to increase Treg cell number and/or function have been viewed as potential therapeutic approaches in treating T1DM, and several clinical trials using these strategies have already emerged. Notably, many trials fail to demonstrate clinical response even when Treg treatment successfully boosts Tregs. In view of this, whether a failure of Tregs does exist and contribute to the development of T1DM and whether more Tregs would be clinically beneficial to patients should be carefully taken into consideration before applying Tregs as treatments in T1DM.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The Immune Basis of T1DM
Type 1 diabetes mellitus (T1DM) is a chronic, T cell-mediated autoimmune disease. The immune system attacks the insulin-producing β cells of the pancreatic islet, eventually resulting in insulin deficiency [1, 2]. Under normal conditions, the vast majority of self-reactive T cells are eliminated in the thymus through a mechanism called “central tolerance induction.” This is part of the process which ensures immune tolerance to self-antigens. Nevertheless, a few remaining autoreactive T cells escape thymic elimination and are released to the peripheral circulation [3]. Normally, these autoreactive T cells are actively suppressed by regulatory T cells (Tregs). Therefore, impaired thymic deletion and defective Treg function may both contribute to the onset and development of autoimmune T1DM [4].
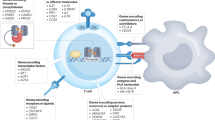
In animal models of T1DM, islet-reactive T cells are primed in the pancreatic lymph nodes [5] and then infiltrate into islets causing damage to β cells. Abnormal autoreactive T cell responses, together with effect of other immune cells, including macrophages, dendritic cells (DCs), natural killer T (NKT) cells, and B cells, eventually induce the onset of autoimmune diabetes. Specifically, the destruction of β cells is mediated by granzyme and perforin produced by CD8+ T cells, cytokines such as interferon gamma (IFN-γ), and interleukin-17 (IL-17) [6]. Fas/Fas and tumor necrosis factor-α (TNF-α)-dependent pathway also contribute to the pathogenesis of T1DM [3] (Fig. 1).
The Immunological Properties of Tregs
Tregs are a diverse population of lymphocytes that exhibit inhibitory or regulatory effects on immune responses by influencing the activity of other cells. A dysfunction in Treg cells has been implicated in the pathogenesis of many autoimmune diseases [7–9]. Tregs suppress autoreactive T cells and induce immune tolerance, resulting in a dampening of inflammation [10]. Cell-to-cell contact, secretion of immunosuppressive cytokines, killing or modification of antigen-presenting cells (APCs), and competition for growth factors are the four main regulatory mechanisms Tregs exert their regulatory effects on T cells, natural killer (NK) and NKT cells, B cells, and antigen-presenting cells (APCs) [11, 12]. Types of Tregs include CD4+CD25+FoxP3+ Tregs, interleukin-10 (IL-10)-secreting TR1 cells, transforming growth factor-β (TGF-β)-secreting T helper 3 (TH3) cells, CD8+ Tregs, CD8+CD28-FoxP3-Tregs, CD3+CD4-CD8-(DN) Tregs, CD4+Vα14+ NKTregs, and γδ-T-cells [10, 13, 14]. A comprehensive review of all the various subsets of Tregs is beyond the scope of this article. CD4+CD25+FoxP3+ Treg cells have been one of the more extensively studied types of Treg cells, and the effect of this subset of Treg cells on T1DM is the main focus of this paper.
Among the various characteristic markers of Treg cells, the most specific and important one is foxhead box P3(FoxP3), which is constitutively expressed by Tregs and acts as a master regulator [15, 16]. CD4+CD25+FoxP3+ Tregs consist of two major subsets with different origins: thymus-derived natural Treg (nTreg) and peripheral-induced Treg (iTreg). Though there exist some differences between the two subsets, nTreg and iTreg share many similar phenotypes and show comparable suppressive function [17].
Treg Cell Interactions
Animal Models
The existence of suppressor T cells has been recognized for almost two decades [18–21]. However, inconsistent data obtained from different laboratories have delayed our understanding of the mechanism of action of these cells. It was not until 1995 that several laboratories [22–25] demonstrated that a distinct subset of CD4+ T cells expressing CD25 possesses regulatory properties. When CD4+ T cells depleted of this CD25+ population were transferred into the immunodeficient nude mice, various forms of autoimmunity [22, 23] including autoimmune diabetes [26] ensued. Later, FoxP3 [15, 16, 27] was found to be the master regulator of Treg development as well as function [28], directly demonstrated by the observation that FoxP3 point mutations lead to fatal autoimmune disease in mice [27, 28]. Data obtained from animal models of T1DM clearly demonstrate that CD4+CD25+FoxP3+ Tregs are crucial for bridling T1DM. Elimination of Tregs in non-obese diabetic (NOD) mice led to the spontaneous development of autoimmune diabetes. In contrast, reconstitution or transfer of Tregs could prevent the development of autoimmune diabetes in murine models [29–31]. As islet-reactive T cell priming takes place in the pancreatic lymph nodes, and then primed effector T (Teff) cells migrate to the islets to destroy β cells, the protective effect of Tregs can occur both in the secondary lymphoid organs and the inflammatory pancreas, respectively.
Treg Cell Effects on T Effector Cells
Tregs regulate the activity of autoreactive T cells via several different mechanisms. In pancreatic lymph nodes (PLNs), Teff proliferation is inhibited by Tregs, demonstrated by the inverse correlation between the level of Tregs and proliferation of Teffs [30]. Attracted to sites of inflammation, Tregs co-localize with Teffs and dampen the activity of Teffs. Direct cell-to-cell contact is required as demonstrated in in vitro experiments [32]. For example, in lymphoid tissues, Tregs impaired the survival of T helper type 1 (Th1) cells via FasL-dependent cytotoxicity [33]. It should be noted that the elimination of Teffs is only one of the many regulatory mechanisms of Treg cells. Van et al. found that Tregs in the PLNs of NOD mice suppress the activation as well as IFN-γ secretion of both CD4+ and CD8+ T cells [34]. In addition, Tregs block Teffs migration to the T–B cell boundary in the lymph node where antigen-loaded DCs are present [35, 36], thus impinging upon the proper priming of autoreactive T cells. By suppressing CXCR3 expression in Teffs, Tregs reduce their migration to the PLNs [30].
Tregs may also interfere with the interaction between Teffs and antigen-presenting cells (APCs). Tang et al. [37] showed that Tregs and DCs form persistent conjugation, possibly preventing stable associations between Teffs and these APCs. Tregs thus use a variety of mechanisms to restrict DCs activity, consequently suppressing the activation and differentiation of Teffs in the PLNs [38]. Furthermore, it has been proposed that the suppressive function of Tregs involves the ability of Tregs to “educate” other T cells to adopt a regulatory phenotype [39]. In combination with TGF-βand IL-10, Tregs induce CD4+CD25− cells to become suppressor cells [39].
Treg Cell Effects on Dendritic Cells (DCs)
It has also been observed that Tregs cluster around DCs in the PLNs of NOD mice and the engagement of Tregs with DCs blocks the activation of Teffs [41]. CLTA4 expressed by Tregs downregulates DC’s expression of CD80 and CD86 and thereby inhibits the activation of Teffs [42, 43]. Lee et al. [44] showed that nTreg depletion resulted in accelerated autoimmune diabetes characterized by a large number of DCs infiltrating the pancreas. They further proposed that Tregs can inhibit DC’s infiltration by regulating chemotaxis of DCs toward islets-produced CCL19/21 [44].
Cytokines play an important role in the interaction between Treg cells and DCs. Secreted by Tregs, TGF-β and IL-10 affect the function of Teffs and DCs in a number of ways. TGF-β1 reduces the production of inflammatory cytokines from CD4+ T cells [39]. Furthermore, TGF-β1 also induces the production of IL-10 in Th1 cells and hence attenuates Th1 cell function [45]. Reciprocally, IL-10 enhances the response of Teffs to TGF-β1 [45]. Thus, TGF-β and IL-10 work in combination to suppress the function of Teffs. IL-10 also downregulates IL-12 production in DCs and inhibits the function of Th1 cells [46, 47]. IL-2 is a key factor in the activation of T cells. Tregs avidly capture and exhaust IL-2, leading to IL-2 deprivation of Teffs [48]. The inhibition of IL-2-dependent MHC/protein interactions has been postulated to be a potential mechanism by which to shut down autoreactivity and treat autoimmunity [49].
Other Cellular Interactions
Tregs can also regulate pancreatic autoimmune activity through the control of other types of immune cells in addition to autoreactive T cells. Transfer of Tregs resulted in a decrease in the number of macrophages in the pancreas and inhibition of deleterious cytokine production [40]. Natural killer (NK) cells may also be targets of Tregs [50], demonstrated by the observation that NK cells are activated in the islets in Treg-deficient mice [38].
Another NOD-related observation involves the role of a protein CD137, which is a Treg-derived natural immunosuppressive protein. It has been found that NOD mice are deficient in CD137+_Treg cells. An APC independent assay showed that soluble CD137 suppresses highly purified CD4 T cells through its interaction with CD137 ligand on APCs. CD137 is postulated to act via a negative feedback mechanism to suppress hyperactive immune responses. A deficiency in this population of CD137+ Treg cells may play a role in the pathogenesis of NOD mouse T1DM [51].
Alteration of Peripheral Tregs in T1DM Patients
Methods
Because of the important regulatory role that Tregs play in the pathogenesis of T1DM, the number and/or function of Tregs in T1DM patients have been investigated in the recent years. We searched the PubMed for all potentially relevant articles. The key search terms were “diabetes mellitus, type 1”; “diabetes mellitus”; “T-lymphocytes, regulatory”; and ‘T-lymphocytes.” We focused on studies which investigated the number/frequency and/or function of Tregs in patients with type 1 diabetes. The search was restricted to cross-sectional or longitudinal studies conducted in humans. In addition, we manually reviewed references from important review articles for relevant articles.
Results
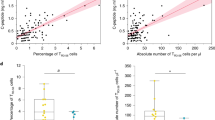
The search identified 24 relevant references that investigated the frequency and/or number of Tregs in T1DM patients. Sixteen studies reported the frequency of Tregs in T1DM patients. Twelve studies investigated the suppressive function of Tregs in patients with type 1 diabetes. The main results of the included studies are summarized in Table 1.
As shown in Table 1, conflicting results have been obtained thus far. Peripheral Treg number and frequency have been shown to be slightly increased, significantly decreased, or normal in T1DM patients (Table 1). Functional assessments have also demonstrated lower or normal suppressive function of Tregs in T1DM patients.
The lack of a general consensus on the role of Treg cells is not unexpected for the reasons outlined below.
-
1.
Currently, there is no precise definition of Tregs. Different experiments use different markers to define Tregs, making comparison of the results almost impossible. Most work [52–63] utilized CD4+CD25+/high to define Tregs, but after the identification of FoxP3, researchers [64–70] preferred to use this more specific marker to differentiate Tregs from other T cells. More recently, studies by Badami et al. [71], Ferraro et al. [72], and Liu et al. [73] exploited lower expression of CD127 in combination with the expression of CD4 and CD25 as more precise markers for live Tregs, allowing for flow cytometry-based cell sorting.
-
2.
Nearly all of the studies in Table 1 used Tregs from peripheral blood. Most of their conclusions were based on the hypothesis that T cell population in the peripheral at least partly parallels the one infiltrating various tissues including the pancreas. However, it has been suggested that Tregs exert their function within the target organ undergoing autoimmune attack as well as in draining lymph nodes (DLN) [35, 37, 38, 40, 44]. Consequently, it is possible that the frequency or function of Treg population in the local immune sites does not parallel to the one in the peripheral blood. Preferably, Tregs in T1DM patients should be assessed in the context of the organ where the autoimmune process takes place in addition to the peripheral blood.
-
3.
Though most Tregs retained FoxP3 expression after adoptive transfer under physiological conditions [74, 75], a minority of Tregs were found to have lost FoxP3 expression following transfer into lymphopenic hosts in animal models [74]. Likewise, diminished maintenance of FOXP3 expression in Tregs has been shown to occur in T1DM patients [76]. Thus, under particular inflammatory conditions, the environment may impact on the frequency and/or function of Treg cells.
-
4.
The discrepancies between various studies may also result from the complexity of the in vitro systems. Since tools for the identification of Tregs in vivo are limited, in vitro assays are widely used, despite the fact that they are of limited relevance to the physiological or pathological conditions in vivo. Furthermore, different systems may clamp cell behavior to different artificial environment.
-
5.
The disparities of characteristics between patients and healthy subjects recruited by each study should also be taken into consideration. Various factors including age, gender, and disease duration can all influence the immune status of the patients and possibly change Treg number or function to some extent. For example, the majority of studies [53, 54, 62, 65, 66, 68, 72] in Table 1 used age-matched controls to avoid the potential confounding effect of age. Moreover, in several studies [52, 61, 63, 65, 67], the researchers divided T1DM patients into two subgroups, namely the new-onset T1DM patients and established T1DM patients (6).
Recently, it has been reported that the effector T cell population in T1DM can resist the regulatory activity of Tregs [57, 59]. Thereby, it is tempting to contemplate that instead of defects in Tregs, the refractory nature of hyperactivated effector T cells to the control of Tregs mimics the defect in Treg function. Taken collectively, current published data suggests that the frequency of Tregs in the peripheral blood of T1DM patients may appear normal. However, it is still unclear whether Treg cells from T1DM patients have intrinsic defective function or whether the responder T cells are resistant to suppression. To answer this question, with certainty, further studies are urgently needed.
Tregs in the Pancreas and Peripheral Lymph Nodes
The characterization of Treg population in the pancreas and PLNs remains poorly addressed in clinical settings. One study mentioned in Table 1 compared PLNs-derived Tregs from T1DM patients and controls, reporting that PLN-derived Treg functions were impaired in T1DM subjects [72]. Willcox [77] analyzed postmortem pancreatic samples from 29 T1DM patients. FoxP3+ Tregs were only found in islets from a single patient, suggesting that the lack of Treg cells may play a role in autoimmune pathogenesis in T1DM patients.
Compared to the void of studies in human subjects, several animal studies have focused on Tregs in the pancreas and PLNs. Tonkin [40] generated TGF-β-induced islet-specific Tregs and demonstrated their ability to suppress the transfer of diabetes into NOD.scid mice using diabetic spleen cells. Infiltration of both Teffs and Tregs were observed in the pancreas, suggesting the active role that Tregs play in the inflammatory site. By the induction of hemopoietic chimerism, antea-diabetic mice were restored to adequate pancreatic islet function even after they had been rendered hyperglycemic. Compared to the antea-diabetic mice, the numbers of Tregs in the PLNS were significantly decreased in NOD mice, indicating that Tregs in the PLNs had a potential role in ameliorating disease progression in the model [78]. The accumulation of Treg cells that was observed in the islets and PLNs in mice models likely played a significant role in controlling anti-islet inflammation [79].
Mechanistically, local production of CCL22 in islets recruits Tregs to the islets and leads to protection from T1DM in the NOD model [80]. In parallel, pDCs [81] was shown to take a critical role in recruiting Tregs to the pancreas and preventing the progression of T1DM. After entering the pancreas and PLNs, Tregs function to prevent islet destruction via a variety of mechanisms, including the blocking of interactions between Teffs and DCs [37]. Further studies are needed to establish whether or not clinical effects in human subjects parallel those results seen in animal models of T1DM.
Antigen-Specific Tregs in T1DM
Studies on the impairment in the function of Tregs specific to islet antigen are sparse. In most of these studies, the Tregs under investigation are not truly antigen-specific Tregs but are polycolonal in nature. However, it has been demonstrated that antigen-specific Tregs are much more potent in suppressing autoimmunity in T1DM than polyclonal Tregs [29]. In the NOD model, β cell peptide-pulsed DCs can lead to the differentiation of islet-specific Tregs, which are capable of preventing the development of diabetes when co-transferred with diabetogenic cells [82, 83]. NKG2D, an immune-activating receptor found on NK cells and CD8 cells, has been shown to be increased in virus-induced T1DM. Treatment with antibody to NKG2D in combination with antigen-specific Treg cells was able to prevent the development of T1DM in 75 % of mice belonging to a rat insulin promotor (RIP) lymphocytic choriomeningitis virus (LCMV) mouse model. On the other hand, NKG2D blockade by itself was unable to prevent the development of T1DM in a NOD mouse model, even in the presence of the downregulation of NKG2D in NK and CD8+ T cells. The authors concluded that while NKG2D can help maintain Treg cell functionality during ongoing inflammation, it is insufficient by itself to protect against T1DM in the face of strong inflammatory signals [84].
Similarly, in several clinical trials, islet-specific Tregs have been generated and deemed as one of the mechanism contributing to the control of disease progression. For example, in a phase I clinical trial [85], insulin B-chain immunotherapy induced the generation of insulin B-chain-specific Tregs. GAD65-specific Tregs are also generated during treatment with a GAD-alum moiety [86]. However, the existence of naturally occurring islet-specific has not yet been investigated. It is also possible that even if levels of polyclonal Tregs are unaltered in T1DM patients, islet-specific Tregs may be deficient in number or function in these subjects with T1DM.
Treg Cell-Based Therapy for T1DM
Several clinical trials aiming to re-establish immune tolerance via Treg induction or direct infusion of Treg cells have emerged (Table 2), including anti-CD3 therapy [87, 88], glutamic acid decarboxylase (GAD) injection [89, 90], hematopoietic stem cell transplantation (HSCT) [91, 92], autologous umbilical cord blood transfusion [93–95], and stem cell educator therapy [96]. Some of these therapies have shown efficacy, as demonstrated by increased C-peptide levels and decreased daily dose of insulin requirement, while the others failed in meeting their primary goals.
Anti-CD3 Therapy
Anti-CD3 monoclonal antibody effectively blocks T effector cell activation and, hence, inhibits the development of T1DM in animal models [97, 98]. In addition, anti-CD3 therapies lead to the depletion of pathogenic T cells, but preserve or even boost Treg cell numbers [99]. In general, clinical trials of anti-CD3 therapy have shown improvement in islet function in patients with T1DM [88, 100, 101].
Antigen-Specific Therapy
Administration of GAD [89, 102, 103], insulin [104, 105], and DiaPep277 [106] all fall within the realm of antigen-specific therapy. The mechanism of these therapies involves the induction of antigen-specific Tregs [107]. Such Tregs then potently regulate autoimmune responses. However, there are pitfalls to the success of antigen-specific therapies in the clinical settings, and most trials brought about no clinical benefit.
Direct Infusion of Treg Cells
Direct infusion of Tregs is also a promising strategy in the treatment of T1DM. Stem cells from bone marrow and umbilical cord blood are abundant with Tregs and may be utilized for Treg cell transplant. In addition, stem cells have been shown to inhibit immune activation triggered by antigen-presenting cells (APCs), recruit immunosuppressive cells including Tregs, and support islet function and regeneration. Though proven to be effective in reversing autoimmunity in NOD mice [108] and reducing the levels of islet autoantibodies as well as the level of blood glucose in a clinical trial [109], most stem cell therapies did not bring about improvement in metabolic parameters. The exceptions to this include two HSCT therapy trials [91, 92].
Conclusions
The evidence supports a defect in the regulation of effector T cell activity by Tregs, either due to intrinsic defects of Treg function or resistance of Teff to Treg modulation. Nevertheless, a definitive answer to the question as to whether the frequency/function of Tregs is different between T1DM patients and healthy controls needs to be further explored, perhaps by larger clinical surveys.
Animal models clearly demonstrate that CD4+CD25+FoxP3+ Treg cells play a pivotal role in modulating the outcome of autoimmunity. Early clinical trials affecting the number of function of Treg cells have produced encouraging results that indicate the development of Treg cell-based treatments should be a strategy that should be pursued. However, the lack of specific markers, imperfect systems for testing Treg function, the plasticity of Tregs as well as varying clinical manifestations across studies as a function of age or disease duration all contribute to the mixed results reported from these clinical studies. Future studies of Treg number and function in local sites of inflammation and the effects of antigen-specific Tregs in T1DM patients will bring new insights into the precise role of Treg cells in T1DM. Moreover, the definition of the specific defects in Treg regulation in autoimmune diabetes will lead to improved diagnosis as well as possible cure for the disease. Ultimately, a more thorough understanding of T1DM and the role of Tregs will contribute to the development of safe and effective novel treatment strategies of T1DM.
References
van Belle TL, Coppieters KT, von Herrath MG (2011) Type 1 diabetes: etiology, immunology, and therapeutic strategies. Physiol Rev 91:79–118
Eisenbarth GS (1986) Type I, diabetes mellitus. A chronic autoimmune disease. N Engl J Med 314:1360–1368
Chen W, Xie A, Chan L (2013) Mechanistic basis of immunotherapies for type 1 diabetes mellitus. Transl Res : J Lab Clin Med 161:217–229
Askenasy EM, Askenasy N (2013) Is autoimmune diabetes caused by aberrant immune activity or defective suppression of physiological self-reactivity? Autoimmun Rev 12:633–637
Gagnerault MC, Luan JJ, Lotton C, Lepault F (2002) Pancreatic lymph nodes are required for priming of beta cell reactive T cells in NOD mice. J Exp Med 196:369–377
Xiao J, Liu C, Li G, Peng S, Hu J, Qu L et al (2013) PDCD5 negatively regulates autoimmunity by upregulating FOXP3(+) regulatory T cells and suppressing Th17 and Th1 responses. J Autoimmun 47:34–44
Selmi C (2013) Autoimmunity in 2012. Clin Rev Allergy Immunol 45:290–301
Walker LS (2013) Treg and CTLA-4: two intertwining pathways to immune tolerance. J Autoimmun 45:49–57
Longhi MS, Ma Y, Grant CR, Samyn M, Gordon P, Mieli-Vergani G et al (2013) T-regs in autoimmune hepatitis-systemic lupus erythematosus/mixed connective tissue disease overlap syndrome are functionally defective and display a Th1 cytokine profile. J Autoimmun 41:146–151
Peterson RA (2012) Regulatory T-cells: diverse phenotypes integral to immune homeostasis and suppression. Toxicol Pathol 40:186–204
Sakaguchi S, Miyara M, Costantino CM, Hafler DA (2010) FOXP3+ regulatory T cells in the human immune system. Nat Rev Immunol 10:490–500
Battaglia M, Roncarolo MG (2011) Immune intervention with T regulatory cells: past lessons and future perspectives for type 1 diabetes. Semin Immunol 23:182–194
Tang Q, Bluestone JA (2008) The Foxp3+ regulatory T cell: a jack of all trades, master of regulation. Nat Immunol 9:239–244
Venigalla RK, Guttikonda PJ, Eckstein V, Ho AD, Sertel S, Lorenz HM et al (2012) Identification of a human Th1-like IFNgamma-secreting Treg subtype deriving from effector T cells. J Autoimmun 39:377–387
Fontenot JD, Gavin MA, Rudensky AY (2003) Foxp3 programs the development and function of CD4+CD25+ regulatory T cells. Nat Immunol 4:330–336
Hori S, Nomura T, Sakaguchi S (2003) Control of regulatory T cell development by the transcription factor Foxp3. Science (New York, NY) 299:1057–1061
You S, Thieblemont N, Alyanakian MA, Bach JF, Chatenoud L (2006) Transforming growth factor-beta and T-cell-mediated immunoregulation in the control of autoimmune diabetes. Immunol Rev 212:185–202
Gershon RK, Kondo K (1970) Cell interactions in the induction of tolerance: the role of thymic lymphocytes. Immunology 18:723–737
Benacerraf B, Kapp JA, Debre P, Pierce CW, de la Croix F (1975) The stimulation of specific suppressor T cells in genetic non-responder mice by linear random copolymers of L-amino acids. Transplant Rev 26:21–38
Bach JF, Boitard C, Yasunami R, Dardenne M (1990) Control of diabetes in NOD mice by suppressor cells. J Autoimmun 3(Suppl 1):97–100
Boitard C, Yasunami R, Dardenne M, Bach JF (1989) T cell-mediated inhibition of the transfer of autoimmune diabetes in NOD mice. J Exp Med 169:1669–1680
Sakaguchi S, Sakaguchi N, Asano M, Itoh M, Toda M (2011) Pillars article: immunologic self-tolerance maintained by activated T cells expressing IL-2 receptor alpha-chains (CD25). Breakdown of a single mechanism of self-tolerance causes various autoimmune diseases. J. Immunol. 1995. J Immunol (Baltimore, Md: 1950), 186:3808–3821
Takahashi T, Tagami T, Yamazaki S, Uede T, Shimizu J, Sakaguchi N et al (2000) Immunologic self-tolerance maintained by CD25(+)CD4(+) regulatory T cells constitutively expressing cytotoxic T lymphocyte-associated antigen 4. J Exp Med 192:303–310
Thornton AM, Shevach EM (1998) CD4+CD25+ immunoregulatory T cells suppress polyclonal T cell activation in vitro by inhibiting interleukin 2 production. J Exp Med 188:287–296
Thornton AM, Shevach EM (2000) Suppressor effector function of CD4+CD25+ immunoregulatory T cells is antigen nonspecific. J Immunol (Baltimore, Md: 1950) 164:183–190
Piccirillo CA, Tritt M, Sgouroudis E, Albanese A, Pyzik M, Hay V (2005) Control of type 1 autoimmune diabetes by naturally occurring CD4+CD25+ regulatory T lymphocytes in neonatal NOD mice. Ann N Y Acad Sci 1051:72–87
Khattri R, Cox T, Yasayko SA, Ramsdell F (2003) An essential role for Scurfin in CD4+CD25+ T regulatory cells. Nat Immunol 4:337–342
Katoh H, Zheng P, Liu Y (2013) FOXP3: genetic and epigenetic implications for autoimmunity. J Autoimmun 41:72–78
Tang Q, Henriksen KJ, Bi M, Finger EB, Szot G, Ye J et al (2004) In vitro-expanded antigen-specific regulatory T cells suppress autoimmune diabetes. J Exp Med 199:1455–1465
Sarween N, Chodos A, Raykundalia C, Khan M, Abbas AK, Walker LS (2004) CD4+CD25+ cells controlling a pathogenic CD4 response inhibit cytokine differentiation, CXCR-3 expression, and tissue invasion. J Immunol (Baltimore, Md: 1950) 173:2942–2951
Jaeckel E, von Boehmer H, Manns MP (2005) Antigen-specific FoxP3-transduced T-cells can control established type 1 diabetes. Diabetes 54:306–310
Piccirillo CA, Letterio JJ, Thornton AM, McHugh RS, Mamura M, Mizuhara H et al (2002) CD4(+)CD25(+) regulatory T cells can mediate suppressor function in the absence of transforming growth factor beta1 production and responsiveness. J Exp Med 196:237–246
Weber SE, Harbertson J, Godebu E, Mros GA, Padrick RC, Carson BD et al (2006) Adaptive islet-specific regulatory CD4 T cells control autoimmune diabetes and mediate the disappearance of pathogenic Th1 cells in vivo. J Immunol (Baltimore, Md: 1950) 176:4730–4739
Van YH, Lee WH, Ortiz S, Lee MH, Qin HJ, Liu CP (2009) All-trans retinoic acid inhibits type 1 diabetes by T regulatory (Treg)-dependent suppression of interferon-gamma-producing T-cells without affecting Th17 cells. Diabetes 58:146–155
Bluestone JA (2005) Regulatory T-cell therapy: is it ready for the clinic? Nat Rev Immunol 5:343–349
Tritt M, Sgouroudis E (2008) d’Hennezel E, Albanese A, Piccirillo CA. Functional waning of naturally occurring CD4+ regulatory T-cells contributes to the onset of autoimmune diabetes. Diabetes 57:113–123
Tang Q, Adams JY, Tooley AJ, Bi M, Fife BT, Serra P et al (2006) Visualizing regulatory T cell control of autoimmune responses in nonobese diabetic mice. Nat Immunol 7:83–92
Feuerer M, Shen Y, Littman DR, Benoist C, Mathis D (2009) How punctual ablation of regulatory T cells unleashes an autoimmune lesion within the pancreatic islets. Immunity 31:654–664
Zheng SG, Wang JH, Gray JD, Soucier H, Horwitz DA (2004) Natural and induced CD4+CD25+ cells educate CD4+CD25- cells to develop suppressive activity: the role of IL-2, TGF-beta, and IL-10. J Immunol (Baltimore, Md: 1950) 172:5213–5221
Tonkin DR, Haskins K (2009) Regulatory T cells enter the pancreas during suppression of type 1 diabetes and inhibit effector T cells and macrophages in a TGF-beta-dependent manner. Eur J Immunol 39:1313–1322
Bluestone JA, Tang Q (2005) How do CD4+CD25+ regulatory T cells control autoimmunity? Curr Opin Immunol 17:638–642
Wing K, Onishi Y, Prieto-Martin P, Yamaguchi T, Miyara M, Fehervari Z et al (2008) CTLA-4 control over Foxp3+ regulatory T cell function. Science (New York, NY) 322:271–275
Romo-Tena J, Gomez-Martin D, Alcocer-Varela J (2013) CTLA-4 and autoimmunity: new insights into the dual regulator of tolerance. Autoimmun Rev 12:1171–1176
Lee MH, Lee WH, Todorov I, Liu CP (2010) CD4+ CD25+ regulatory T cells prevent type 1 diabetes preceded by dendritic cell-dominant invasive insulitis by affecting chemotaxis and local invasiveness of dendritic cells. J Immunol (Baltimore, Md: 1950) 185:2493–2501
Cottrez F, Groux H (2001) Regulation of TGF-beta response during T cell activation is modulated by IL-10. J Immunol (Baltimore, Md: 1950) 167:773–778
Moore KW, de Waal MR, Coffman RL, O’Garra A (2001) Interleukin-10 and the interleukin-10 receptor. Annu Rev Immunol 19:683–765
Zhang J, Huang Z, Sun R, Tian Z, Wei H (2012) IFN-gamma induced by IL-12 administration prevents diabetes by inhibiting pathogenic IL-17 production in NOD mice. J Autoimmun 38:20–28
Scheffold A, Huhn J, Hofer T (2005) Regulation of CD4+CD25+ regulatory T cell activity: it takes (IL-)two to tango. Eur J Immunol 35:1336–1341
Edwards LJ, Evavold BD (2013) Destabilization of peptide:MHC interaction induces IL-2 resistant anergy in diabetogenic T cells. J Autoimmun 44:82–90
Peng H, Tian Z. NK (2013) Cell trafficking in health and autoimmunity: a comprehensive review. Clin Rev Allergy Immunol
Kachapati K, Bednar KJ, Adams DE, Wu Y, Mittler RS, Jordan MB et al (2013) Recombinant soluble CD137 prevents type one diabetes in nonobese diabetic mice. J Autoimmun 47:94–103
Kukreja A, Cost G, Marker J, Zhang C, Sun Z, Lin-Su K et al (2002) Multiple immuno-regulatory defects in type-1 diabetes. J Clin Invest 109:131–140
Ryba M, Rybarczyk-Kapturska K, Zorena K, Mysliwiec M, Mysliwska J (2011) Lower frequency of CD62L(high) and higher frequency of TNFR2(+) Tregs are associated with inflammatory conditions in type 1 diabetic patients. Mediat Inflamm 2011:645643
Lindley S, Dayan CM, Bishop A, Roep BO, Peakman M, Tree TI (2005) Defective suppressor function in CD4(+)CD25(+) T-cells from patients with type 1 diabetes. Diabetes 54:92–99
Putnam AL, Vendrame F, Dotta F, Gottlieb PA (2005) CD4+CD25high regulatory T cells in human autoimmune diabetes. J Autoimmun 24:55–62
Luczynski W, Wawrusiewicz-Kurylonek N, Stasiak-Barmuta A, Urban R, Ilendo E, Urban M et al (2009) Diminished expression of ICOS, GITR and CTLA-4 at the mRNA level in T regulatory cells of children with newly diagnosed type 1 diabetes. Acta Biochim Pol 56:361–370
Lawson JM, Tremble J, Dayan C, Beyan H, Leslie RD, Peakman M et al (2008) Increased resistance to CD4+CD25hi regulatory T cell-mediated suppression in patients with type 1 diabetes. Clin Exp Immunol 154:353–359
Brusko TM, Wasserfall CH, Clare-Salzler MJ, Schatz DA, Atkinson MA (2005) Functional defects and the influence of age on the frequency of CD4+ CD25+ T-cells in type 1 diabetes. Diabetes 54:1407–1414
Schneider A, Rieck M, Sanda S, Pihoker C, Greenbaum C, Buckner JH (2008) The effector T cells of diabetic subjects are resistant to regulation via CD4+ FOXP3+ regulatory T cells. J Immunol (Baltimore, Md: 1950) 181:7350–7355
Monti P, Scirpoli M, Maffi P, Piemonti L, Secchi A, Bonifacio E et al (2008) Rapamycin monotherapy in patients with type 1 diabetes modifies CD4+CD25+FOXP3+ regulatory T-cells. Diabetes 57:2341–2347
Glisic-Milosavljevic S, Waukau J, Jailwala P, Jana S, Khoo HJ, Albertz H et al (2007) At-risk and recent-onset type 1 diabetic subjects have increased apoptosis in the CD4+CD25+ T-cell fraction. PLoS One 2:e146
Hughson A, Bromberg I, Johnson B, Quataert S, Jospe N, Fowell DJ (2011) Uncoupling of proliferation and cytokines from suppression within the CD4+CD25+Foxp3+ T-cell compartment in the 1st year of human type 1 diabetes. Diabetes 60:2125–2133
Glisic S, Ehlenbach S, Jailwala P, Waukau J, Jana S, Ghosh S (2010) Inducible regulatory T cells (iTregs) from recent-onset type 1 diabetes subjects show increased in vitro suppression and higher ITCH levels compared with controls. Cell Tissue Res 339:585–595
Ryba-Stanislawowska M, Skrzypkowska M, Mysliwska J, Mysliwiec M (2013) The serum IL-6 profile and Treg/Th17 peripheral cell populations in patients with type 1 diabetes. Mediat Inflamm 2013:205284
McClymont SA, Putnam AL, Lee MR, Esensten JH, Liu W, Hulme MA et al (2011) Plasticity of human regulatory T cells in healthy subjects and patients with type 1 diabetes. J Immunol (Baltimore, Md: 1950) 186:3918–3926
Du W, Shen YW, Lee WH, Wang D, Paz S, Kandeel F et al (2013) Foxp3+ Treg expanded from patients with established diabetes reduce Helios expression while retaining normal function compared to healthy individuals. PLoS One 8:e56209
Brusko T, Wasserfall C, McGrail K, Schatz R, Viener HL, Schatz D et al (2007) No alterations in the frequency of FOXP3+ regulatory T-cells in type 1 diabetes. Diabetes 56:604–612
Marwaha AK, Crome SQ, Panagiotopoulos C, Berg KB, Qin H, Ouyang Q et al (2010) Cutting edge: increased IL-17-secreting T cells in children with new-onset type 1 diabetes. J Immunol (Baltimore, Md: 1950) 185:3814–3818
Alonso N, Martinez-Arconada MJ, Granada ML, Soldevila B, Canton A, Mate JL et al (2009) Regulatory T cells in type 1 diabetic patients with autoimmune chronic atrophic gastritis. Endocrine 35:420–428
Haseda F, Imagawa A, Murase-Mishiba Y, Terasaki J, Hanafusa T (2013) CD4(+) CD45RA(-) FoxP3high activated regulatory T cells are functionally impaired and related to residual insulin-secreting capacity in patients with type 1 diabetes. Clin Exp Immunol 173:207–216
Badami E, Sorini C, Coccia M, Usuelli V, Molteni L, Bolla AM et al (2011) Defective differentiation of regulatory FoxP3+ T cells by small-intestinal dendritic cells in patients with type 1 diabetes. Diabetes 60:2120–2124
Ferraro A, Socci C, Stabilini A, Valle A, Monti P, Piemonti L et al (2011) Expansion of Th17 cells and functional defects in T regulatory cells are key features of the pancreatic lymph nodes in patients with type 1 diabetes. Diabetes 60:2903–2913
Liu W, Putnam AL, Xu-Yu Z, Szot GL, Lee MR, Zhu S et al (2006) CD127 expression inversely correlates with FoxP3 and suppressive function of human CD4+ T reg cells. J Exp Med 203:1701–1711
Komatsu N, Mariotti-Ferrandiz ME, Wang Y, Malissen B, Waldmann H, Hori S (2009) Heterogeneity of natural Foxp3+ T cells: a committed regulatory T-cell lineage and an uncommitted minor population retaining plasticity. Proc Natl Acad Sci U S A 106:1903–1908
Yang XO, Nurieva R, Martinez GJ, Kang HS, Chung Y, Pappu BP et al (2008) Molecular antagonism and plasticity of regulatory and inflammatory T cell programs. Immunity 29:44–56
Long SA, Cerosaletti K, Bollyky PL, Tatum M, Shilling H, Zhang S et al (2010) Defects in IL-2R signaling contribute to diminished maintenance of FOXP3 expression in CD4(+)CD25(+) regulatory T-cells of type 1 diabetic subjects. Diabetes 59:407–415
Willcox A, Richardson SJ, Bone AJ, Foulis AK, Morgan NG (2009) Analysis of islet inflammation in human type 1 diabetes. Clin Exp Immunol 155:173–181
Nti BK, Markman JL, Bertera S, Styche AJ, Lakomy RJ, Subbotin VM et al (2012) Treg cells in pancreatic lymph nodes: the possible role in diabetogenesis and beta cell regeneration in a T1D model. Cell Mol Immunol 9:455–463
Green EA, Choi Y, Flavell RA (2002) Pancreatic lymph node-derived CD4(+)CD25(+) Treg cells: highly potent regulators of diabetes that require TRANCE-RANK signals. Immunity 16:183–191
Montane J, Bischoff L, Soukhatcheva G, Dai DL, Hardenberg G, Levings MK et al (2011) Prevention of murine autoimmune diabetes by CCL22-mediated Treg recruitment to the pancreatic islets. J Clin Invest 121:3024–3028
Beaudoin L, Diana J, Ghazarian L, Simoni Y, Boitard C, Lehuen A. (2014) Plasmacytoid dendritic cells license regulatory T cells, upon iNKT-cell stimulation, to prevent autoimmune diabetes. European journal of immunology
Luo X, Tarbell KV, Yang H, Pothoven K, Bailey SL, Ding R et al (2007) Dendritic cells with TGF-beta1 differentiate naive CD4+CD25− T cells into islet-protective Foxp3+ regulatory T cells. Proc Natl Acad Sci U S A 104:2821–2826
Tarbell KV, Petit L, Zuo X, Toy P, Luo X, Mqadmi A et al (2007) Dendritic cell-expanded, islet-specific CD4+ CD25+ CD62L+ regulatory T cells restore normoglycemia in diabetic NOD mice. J Exp Med 204:191–201
Van Belle TL, Ling E, Haase C, Bresson D, Urso B, von Herrath MG (2013) NKG2D blockade facilitates diabetes prevention by antigen-specific Tregs in a virus-induced model of diabetes. J Autoimmun 40:66–73
Orban T, Farkas K, Jalahej H, Kis J, Treszl A, Falk B et al (2010) Autoantigen-specific regulatory T cells induced in patients with type 1 diabetes mellitus by insulin B-chain immunotherapy. J Autoimmun 34:408–415
Hjorth M, Axelsson S, Ryden A, Faresjo M, Ludvigsson J, Casas R (2011) GAD-alum treatment induces GAD65-specific CD4+CD25highFOXP3+ cells in type 1 diabetic patients. Clin Immunol (Orlando, Fla) 138:117–126
Herold KC, Gitelman SE, Masharani U, Hagopian W, Bisikirska B, Donaldson D et al (2005) A single course of anti-CD3 monoclonal antibody hOKT3gamma1(Ala-Ala) results in improvement in C-peptide responses and clinical parameters for at least 2 years after onset of type 1 diabetes. Diabetes 54:1763–1769
Keymeulen B, Vandemeulebroucke E, Ziegler AG, Mathieu C, Kaufman L, Hale G et al (2005) Insulin needs after CD3-antibody therapy in new-onset type 1 diabetes. N Engl J Med 352:2598–2608
Ludvigsson J, Faresjo M, Hjorth M, Axelsson S, Cheramy M, Pihl M et al (2008) GAD treatment and insulin secretion in recent-onset type 1 diabetes. N Engl J Med 359:1909–1920
Axelsson S, Cheramy M, Hjorth M, Pihl M, Akerman L, Martinuzzi E et al (2011) Long-lasting immune responses 4 years after GAD-alum treatment in children with type 1 diabetes. PLoS One 6:e29008
Couri CE, Oliveira MC, Stracieri AB, Moraes DA, Pieroni F, Barros GM et al (2009) C-peptide levels and insulin independence following autologous nonmyeloablative hematopoietic stem cell transplantation in newly diagnosed type 1 diabetes mellitus. JAMA : J Am Med Assoc 301:1573–1579
Voltarelli JC, Couri CE, Stracieri AB, Oliveira MC, Moraes DA, Pieroni F et al (2007) Autologous nonmyeloablative hematopoietic stem cell transplantation in newly diagnosed type 1 diabetes mellitus. JAMA : J Am Med Assoc 297:1568–1576
Haller MJ, Wasserfall CH, Hulme MA, Cintron M, Brusko TM, McGrail KM et al (2011) Autologous umbilical cord blood transfusion in young children with type 1 diabetes fails to preserve C-peptide. Diabetes Care 34:2567–2569
Haller MJ, Wasserfall CH, Hulme MA, Cintron M, Brusko TM, McGrail KM et al (2013) Autologous umbilical cord blood infusion followed by oral docosahexaenoic acid and vitamin D supplementation for C-peptide preservation in children with Type 1 diabetes. Biol Blood Marrow Transplant : J Am Soc Blood Marrow Transplant 19:1126–1129
Giannopoulou EZ, Puff R, Beyerlein A, von Luettichau I, Boerschmann H, Schatz D et al (2014) Effect of a single autologous cord blood infusion on beta-cell and immune function in children with new onset type 1 diabetes: a non-randomized, controlled trial. Pediatr Diabetes 15:100–109
Zhao Y, Jiang Z, Zhao T, Ye M, Hu C, Yin Z et al (2012) Reversal of type 1 diabetes via islet beta cell regeneration following immune modulation by cord blood-derived multipotent stem cells. BMC Med 10:3
Ishikawa H, Ochi H, Chen ML, Frenkel D, Maron R, Weiner HL (2007) Inhibition of autoimmune diabetes by oral administration of anti-CD3 monoclonal antibody. Diabetes 56:2103–2109
Chatenoud L, Primo J, Bach JF (1997) CD3 antibody-induced dominant self tolerance in overtly diabetic NOD mice. J Immunol (Baltimore, Md: 1950) 158:2947–2954
Daifotis AG, Koenig S, Chatenoud L, Herold KC (2013) Anti-CD3 clinical trials in type 1 diabetes mellitus. Clin Immunol (Orlando, Fla) 149:268–278
Herold KC, Gitelman SE, Ehlers MR, Gottlieb PA, Greenbaum CJ, Hagopian W et al (2013) Teplizumab (anti-CD3 mAb) treatment preserves C-peptide responses in patients with new-onset type 1 diabetes in a randomized controlled trial: metabolic and immunologic features at baseline identify a subgroup of responders. Diabetes 62:3766–3774
Keymeulen B, Walter M, Mathieu C, Kaufman L, Gorus F, Hilbrands R et al (2010) Four-year metabolic outcome of a randomised controlled CD3-antibody trial in recent-onset type 1 diabetic patients depends on their age and baseline residual beta cell mass. Diabetologia 53:614–623
Ludvigsson J, Krisky D, Casas R, Battelino T, Castano L, Greening J et al (2012) GAD65 antigen therapy in recently diagnosed type 1 diabetes mellitus. N Engl J Med 366:433–442
Wherrett DK, Bundy B, Becker DJ, DiMeglio LA, Gitelman SE, Goland R et al (2011) Antigen-based therapy with glutamic acid decarboxylase (GAD) vaccine in patients with recent-onset type 1 diabetes: a randomised double-blind trial. Lancet 378:319–327
Chaillous L, Lefevre H, Thivolet C, Boitard C, Lahlou N, Atlan-Gepner C et al (2000) Oral insulin administration and residual beta-cell function in recent-onset type 1 diabetes: a multicentre randomised controlled trial. Diabete Insuline Orale group. Lancet 356:545–549
Ergun-Longmire B, Marker J, Zeidler A, Rapaport R, Raskin P, Bode B et al (2004) Oral insulin therapy to prevent progression of immune-mediated (type 1) diabetes. Ann N Y Acad Sci 1029:260–277
Huurman VA, van der Meide PE, Duinkerken G, Willemen S, Cohen IR, Elias D et al (2008) Immunological efficacy of heat shock protein 60 peptide DiaPep277 therapy in clinical type I diabetes. Clin Exp Immunol 152:488–497
Dahan R, Gebe JA, Preisinger A, James EA, Tendler M, Nepom GT et al (2013) Antigen-specific immunomodulation for type 1 diabetes by novel recombinant antibodies directed against diabetes-associates auto-reactive T cell epitope. J Autoimmun 47:83–93
Zhao Y, Lin B, Darflinger R, Zhang Y, Holterman MJ, Skidgel RA (2009) Human cord blood stem cell-modulated regulatory T lymphocytes reverse the autoimmune-caused type 1 diabetes in nonobese diabetic (NOD) mice. PLoS One 4:e4226
Mesples A, Majeed N, Zhang Y, Hu X (2013) Early immunotherapy using autologous adult stem cells reversed the effect of anti-pancreatic islets in recently diagnosed type 1 diabetes mellitus: preliminary results. Med Sci Monit:Int Med J Exp Clin Res 19:852–857
Ambery P, Donner TW, Biswas N, Donaldson J, Parkin J, Dayan CM (2014) Efficacy and safety of low-dose otelixizumab anti-CD3 monoclonal antibody in preserving C-peptide secretion in adolescent type 1 diabetes: DEFEND-2, a randomized, placebo-controlled, double-blind, multi-centre study. DiabetMed:J Br Diabet Assoc 31:399–402
Lazar L, Ofan R, Weintrob N, Avron A, Tamir M, Elias D et al (2007) Heat-shock protein peptide DiaPep277 treatment in children with newly diagnosed type 1 diabetes: a randomised, double-blind phase II study. Diabetes Metab Res Rev 23:286–291
Buzzetti R, Cernea S, Petrone A, Capizzi M, Spoletini M, Zampetti S et al (2011) C-peptide response and HLA genotypes in subjects with recent-onset type 1 diabetes after immunotherapy with DiaPep277: an exploratory study. Diabetes 60:3067–3072
Gu W, Hu J, Wang W, Li L, Tang W, Sun S et al (2012) Diabetic ketoacidosis at diagnosis influences complete remission after treatment with hematopoietic stem cell transplantation in adolescents with type 1 diabetes. Diabetes Care 35:1413–1419
Acknowledgments
This work was supported by the National Natural Science Foundation of China (Grant No.81170725, 81070672), Program for Changjiang Scholars and Innovative Research Team in University (IRT1195), the National key technology R&D program (2012BAI02B04), Research Fund for the Doctoral Program of Higher Education of China 20120162110044; Yufei Xiang is supposed by a European Foundation for the Study of Diabetes-China Diabetes Society (EFSD-CDS) fellowship (2013).
Conflict of Interest
All authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tan, T., Xiang, Y., Chang, C. et al. Alteration of Regulatory T Cells in Type 1 Diabetes Mellitus: A Comprehensive Review. Clinic Rev Allerg Immunol 47, 234–243 (2014). https://doi.org/10.1007/s12016-014-8440-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12016-014-8440-0