Abstract
The objective of this study was to determine the role of Hsp90α in regulating the migration of mesenchymal stem cells (MSCs) and to investigate the underlying mechanisms of this effect. MSCs migration was assessed by wound healing assay and transwell migration assay. Hsp90α expression was silenced in MSC by siRNA (sirHsp90α). The activity of secreted metalloproteases MMP-2 and MMP-9, and their expression levels in MSC were evaluated using gelatin zymography, Western blot analysis and real-time PCR. Gene expression of VCAM-1 and CXCR4 cytokines was evaluated by real-time PCR. Akt and ERK activity were analyzed by Western blotting using antibodies against phosphorylated forms of these proteins. Treatment with Hsp90α significantly enhanced MSC migration, and this effect was blocked by transfecting MSC with sirHsp90α. Treating the cells with recombinant human Hsp90α (rhHsp90α) enhanced gene expression and protein levels of MMP-2 and MMP-9, as well as their secretion and activity. MSC incubated with rhHsp90α exhibited increased gene expression of CXCR4 and VCAM-1. Finally, the levels of phosphorylated Akt and Erk were markedly increased by rhHsp90α treatment. These findings indicate that Hsp90α promotes MSCs migration via PI3K/Akt and ERK signaling pathways, and that this effect is possibly mediated by MMPs, SDF-1/CXCR4 pathway, and VCAM-1.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bone marrow mesenchymal stem cells (MSCs) are pluripotent stem cells that localize in the stromal compartment of the bone marrow, where they support hematopoiesis and differentiate into mesenchymal lineages such as bone, cartilage, muscle, ligament, tendon, and adipose tissues [1–6]. MSCs possess migratory capacity, and are attractive candidates for cardiovascular therapy because of their ability to facilitate myocardial repair and neovascularization in animal models of cardiac injury [7]. MSCs are able to migrate into the injured myocardium from the circulation and contribute to cardiac repair post myocardial infarction (MI) [8].
Recent clinical studies showed that the main benefit of stem cell therapy is due primarily to the ability of stem cells to secrete paracrine factors [9]. The appropriate homing of these cells, therefore, is the first and essential step to enable paracrine factors to function in tissue repair, since relatively high local concentrations of these factors are required to enhance their short-range activity. The efficiency of engrafted cells migration into the infarcted myocardium is no more than 1.5 % [10], therefore, there is a great need for further researching the ways to enhance MSC migration efficiency in order to improve clinical application of stem cell research.
Heat shock protein 90 (Hsp90) is a highly conserved, constitutively expressed chaperone that accounts for 1–2 % of total protein in unstressed cells, rising to 4–6 % when cells are stressed [11]. There are two predominant Hsp90 isoforms in eukaryotic cells: Hsp90α and Hsp90β, both essential for cell viability. The function of Hsp90 is to maintain the stability and activity of numerous proteins referred to as client proteins which include the oncogenic tyrosine kinase v-Src [12], the mutated oncogene Bcr/Abl [13], the receptor tyrosine kinases ErbB2 [14] and c-Met [15], and the serine/threonine kinase Raf-1 [16]. Sidera et al. [17] reported that treating human breast cancer cells with a function-blocking monoclonal antibody against Hsp90 (mAb 4C5) altered actin dynamics, inhibited cell invasion by disrupting surface Hsp90/Her-2 interactions, inhibited heregulin-induced Her-2/Her-3 heterodimer formation, and reduced Her-2 phosphorylation. Tsutsumi et al. [18] reported using a specific Hsp90 inhibitor, DMAG-N-oxide, to significantly attenuate tumor cell migration and integrin/extracellular matrix-dependent cytoskeletal reorganization. Our previous study showed that Hsp90 protects rat MSCs against hypoxia and serum deprivation-induced apoptosis via the PI3K/Akt and ERK1/2 pathways [19]. However, whether Hsp90 plays an important role in regulating MSCs migration is still unclear.
In the present study, we hypothesized that Hsp90 may be involved in the migration of MSCs in vitro. Our data provides new mechanistic insights into the Hsp90-mediated migration of MSCs. Furthermore, we also elucidated new perspectives in the development of MSCs therapeutic strategies by showing that Hsp90 preconditioning enhances cell migration.
Methods
Reagents and Chemicals
All the reagents and chemicals were purchased from Sigma (St. Louis, CA, USA) unless specified otherwise.
Animals and Cell Preparations
Male Sprague–Dawley rats (80–100 g) were purchased from the Experimental Animal Center of Zhejiang Academy of Medical Sciences (Hangzhou, China). All studies were performed with the approval of Zhejiang University Institutional Animal Care and Use Committee. Rat bone marrow-derived MSCs were harvested from femora and tibiae by density gradient centrifugation. MSCs were then purified and cultured in Dulbecco’s modified Eagle’s medium (DMEM) supplemented with 10 % (v/v) heat-inactivated fetal calf serum (FCS), 100 U/ml penicillin, and 100 µg/ml streptomycin (Gibco, USA). Cells at passages 3–5 were labeled with FITC conjugated anti-rat CD44, anti-rat CD45, anti-rat CD90 antibodies (Caltag Laboratories Inc, USA) and characterized by fluorescence activated cell sorting (FACSCalibur, Becton-Dickinson, USA) [20].
Wound Healing Assay
The MSCs (1.5 × 105) were seeded in a six-well plate and cultured to at least 95 % confluence. Monolayers of cells were washed with PBS twice, scraped with a plastic 200 μl pipette tip to simulate wound formation, and returned to a 5 %CO2 incubator at 37 °C. When required, cells were preincubated with Hsp90 inhibitor 17-(allylamino)-17-demethoxygeldanamycin (17-AAG, Sigma, USA Cat#A8476, 40 nmol/l), PI3K inhibitor wortmannin (Alexis Pharmaceuticals, USA Cat#350-020, 10 μm), or MEK1/2 inhibitor U0126 (CST, USA Cat#9904, 10 μm) for 1 h, and cell migration was documented by digital time-lapse microscopy at various time points (0 and 24 h after the treatment). Results are expressed as the mean ± SD. Experiments were repeated at least three times.
Transfection of sirHsp90α
The MSCs were cultured as described above. Small-interfering RNA to Hsp90α (sirHsp90α) was obtained from Guangzhou RiboBio Co Ltd (Guangzhou, China). Cells were grown to 60–70 % confluency on six-well tissue culture plates and transfected with 100 nM of sirHsp90α or control siRNA using siPORT™ NeoFX™ Transfection Agents (Ambion, Austin, TX, USA), according to the manufacturer’s instructions. After transfection cells were grown for additional for 24–48 h, and total RNA was extracted from transfected cells and assessed for expression levels of Hsp90α using real-time PCR as described below. Primers for sirHsp90α were purchased from Guangzhou RiboBio Co. Ltd. China and are as listed as follows:
-
sense: 5′ GCUGCACAUUAAUCUCAUU dTdT 3′
-
antisense: 3′ dTdT CGACGUGUAAUUAGAGUAA 5′
-
GAPDH as control:
-
sense: 5′ TGAAGGTCGGAGTCAACGG 3′
-
antisense: 3′ TAGGGTAGTGGTAGAAGGT 5′
The PCR products were resolved on agarose gel.
Transwell Migration Assay
The assay for cell migration was performed in transwell chambers (Costar, MA, USA). Briefly, 200 μl of medium (DMEM + 1 %FCS) containing MSCs (2 × 104), or MSCs transfected with sirHsp90α, was seeded on the upper chamber of a porous polycarbonate membrane (pore size: 8 μm). 500 μl of DMEM + 1 %FCS containing recombinant human Hsp90α (rhHsp90α 10 μmol/l Assay Designs, USA), or medium alone (as control), was then added to the lower chamber. The chambers were incubated at 37 °C in 5 % CO2 for 24 h. When indicated, cells were pre-treated with 17-AAG (40 nmol/L), wortmannin (10 μm), or U0126 (10 μm) [19] for 1 h before the incubation with rhHsp90. At the end of the incubation, the cells on the upper side of the membrane were mechanically removed. Cells that had migrated to the lower side of the membrane were fixed for 30 min with 11 % glutaraldehyde and stained with Wright’s stain. Five to ten random fields were counted for each membrane.
Gelatin Zymography
To detect the activity of MMP-2 and MMP-9 from the supernatant of the cells, gelatin zymography was performed as described by Heussen and Dowdle [21]. In brief, medium samples underwent electrophoresis on 10 % polyacrylamide gels containing 0.1 % gelatin. The volume of each sample applied was normalized by the cell number (1.5 × 105). After electrophoresis, the gels were washed twice for 30 min each time in washing buffer containing 2.5 % Triton X-100 at room temperature, and then incubated in substrate reaction buffer (50 mM Tris–HCl, 5 mM CaCl2, 0.02 % NaN3, pH 8.0 at 25 °C) for 16–20 h at 37 °C with gentle shaking. The gels were then fixed and stained with 30 % methanol, 10 % acetic acid, and 0.5 % Coomassie brilliant blue for 1–2 h, destained briefly in 30 % methanol with 10 % acetic acid, and fully destained in water overnight. Proteolytic activity was detected by the appearance of clear bands that indicated lysis of the gelatin substrate. Quantitation of the bands was carried out using a Molecular Dynamics Inc. scanning laser densitometer (Sunnyvale, CA, USA) and ImageJ software (version 1.17, NIH Bethesda, USA).
Western Blot Analysis
Proteins were extracted from the cells with ice-cold lysis buffer (1 % Triton X-100, 20 mM HEPES, 5 mM MgCl2, 1 mM EDTA, 1 mM EGTA, 1 mM DTT, 1 mM phenylmethane-sulfonylfluoride, and 1 mg/ml each of leupeptin, aprotinin, and pepstatin), followed by centrifugation at 13,000×g at 4 °C for 25 min. Samples were subjected to 10 % SDS-PAGE and transferred to polyvinylidene difluoride membranes (PVDF). Filters were then blocked in 5 % non-fat milk-Tris buffered saline (TBS)-0.05 % Tween 20 for 1 h and incubated with the following primary antibodies overnight: mouse polyclonal antibody to MMP-2, rabbit polyclonal antibody against MMP-9 (1:1,000 Abcam, Cambridge, MA, USA), ERK1/2, phospho-ERK1/2, Akt, and phospho-Akt monoclonal antibodies (1:1,000 Cell Signaling technology, Danvers, MA, USA). Membranes were washed four times in TBS-Tween 20 and incubated for 2 h with the appropriate horseradish peroxidase-conjugated goat anti-rabbit or anti-mouse IgG (1:5,000 Santa Cruz Biotechnology, CA, USA) antibody. Bands were visualized using an enhanced chemiluminescence kit (Biological industries, Israel), exposed to Kodak radiographic film, and then analyzed by densitometry using Image J. 17-AAG, Wortmannin, and U0126 inhibitors were used where indicated. β-Actin was used as an internal control.
Reverse Transcription-PCR (RT-PCR)
Total RNA was extracted from frozen specimens using Trizol reagent (Invitrogen, Gaithersburg, MD, USA), and first strand cDNA was synthesized using a PrimeScript II 1st Strand cDNA Synthesis Kit Oligo d (T) 18 (TaKaRa, Dalian, China). Real-time PCR was conducted using a BioEasy SYBR green I RT-PCR kit (Bioer Technology, Hangzhou, China). Primers used were as listed:
-
MMP-2f: 5′AGCTCCCGGAAAAGATTGAT3′
-
MMP-2r: 5′TCCAGTTAAAGGCAGCGTCT3′
-
MMP-9f: 5′CCACCGAGCTATCCACTCAT3′
-
MMP-9r: 5′GTCCGGTTTCAGCATGTTTT3′
-
CXCR4f: 5′GCTGAGGAGCATGACAGACA3′
-
CXCR4r: 5′GATGAAGGCCAGGATGAGAA3′
-
VCAM-1f: 5′TGACATCTCCCCTGGATCTC3′
-
VCAM-1r: 5′CTCCAGTTTCCTTCGCTGAC3′
-
GAPDHf: 5′TGAAGGTCGGAGTCAACGG3′
-
GAPDHr: 5′TGGAAGATGGTGATGGGAT3′
GAPDH was used as an internal control. Relative quantification was calculated using the ΔΔCt method
Statistical Analysis
All data were expressed as mean ± SEM. For analysis of differences between two groups, Student’s t test was performed. For multiple group comparisons, one-way ANOVA of variance followed by Bonferroni post hoc test was carried out using SPSS version 13.0 (Chicago, IL, USA). P < 0.05 was considered statistically significant.
Results
RhHsp90α Treatment Enhanced Rat MSC Migration In Vitro
We first evaluated the ability of Hsp90α to enhance MSC motility. We used wound healing and transwell migration assays to evaluate the migration potential of MSCs. MSCs treated with RhHsp90α for 24 h exhibited over 4.5-fold increase in the amount of cells migrated to the wound and to the lower compartment (Fig. 1c, g, i) as compared to the untreated control cells (Fig. 1a, b, g, h; **P < 0.01). Addition of 17-(allylamino)-17-demethoxygeldanamycin (17-AAG, 40 nmol/l), a specific inhibitor of Hsp90, resulted in the reduction of migration to a level similar to the control (Fig. 1d, g, j), indicating that the inhibitor blocked the effect of RhHsp90 on cell migration (## P < 0.01). Similarly, treatment with wortmannin (10 μm), an inhibitor of PI3K/Akt, or with U0126 (10 μm), an inhibitor of ERK, also blocked the stimulation effect of RhHsp90 on cell migration (Fig. 1). Together these data suggest that RhHsp90α can enhance MSC migration, a process that can be blocked by inhibiting Hsp90, as well as PI3K/Akt and ERK signaling pathways.
RhHsp90α treatment enhances rat MSCs migration in vitro. Rat MSCs migration was evaluated by healing assay (a–f) and transwell migration assay (h–l). Cells were cultured for 24 h on six-well tissue cultures plates or in transwell plates as described in “Methods” section, and were either left untreated (control, a, h), treated with 1 %FCS (b), incubated with rhHsp90α, or pre-treated with 17-AAG (d, j), wortmannin (e, k), and U0126 (f, l), respectively. After 24 h, migrated cells were quantified using microscopy, three wells were counted for each condition and three independent experiments were performed (g). Data represent mean ± SD of a single representative experiment; n = 3; **P < 0.01; ## P < 0.01
SiRNA Hsp90α Decreased Rat MSCs Migration
To further investigate the role of Hsp90α in MSC migration, we silenced Hsp90 expression in MSC by transfecting the cells with siRNA for Hsp90α. Knocking down Hsp90α resulted in 88.1 ± 3.5 % decrease in Hsp90 mRNA levels as comparing to non-specific siRNA control (Fig. 2a, b). As indicated by the transwell migration assay, Hsp90α silencing resulted in a significant decrease in the number of migrating MSC as compared to control cells (**P < 0.01; Fig. 3a, b).
Knock-down of Hsp90α expression in MSC. Cells at 60–70 % confluency were transfected with 100 nM of siRNA Hsp90α (sirHsp90) and control siRNA using siPORT™ NeoFX™ transfection agents, accordingly to the manufacturer’s instructions. The expression level of Hsp90α was assessed by real-time PCR (a), and agarose gel electrophoresis (b). GAPDH was used as a normalizer. **P < 0.01
Hsp90 Increased MMP-2 and MMP-9 Expression and Activity
The ability of cells to migration requires the activity of matrix-degrading enzymes, especially matrix metalloproteinases MMP-2 and MMP-9. To investigate whether MMPs are involved in Hsp90α-induced MSC migration, we evaluated the expression of MMP-2 and MMP-9 in MSC, treated with rhHsp90, by Western blot analysis and real-time PCR, and assessed their secretion and activity by gelatin zymography of the cell supernatant, a simple method to analyze proteolytic activity of enzymes, capable of degrading gelatin.
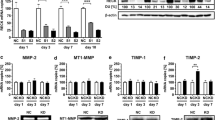
Treating the cells with rhHsp90α significantly up-regulated activity of both MMP-2 and MMP-9 secreted into cell supernatant (Fig. 4). Pre-treating the cells with 17-AAG, wortmannin or U0126 completely abolished the effect of rhHsp90 on the activity of MMP-9 but failed to bring down the activity of MMP-2 (Fig. 4). rhHsp90α treatment led to increase in the protein levels of MMPs in MSC (Fig. 5a). This effect coincided with over 1.5-fold increase in the levels of MMP-2 and twofold increase in the levels of MMP-9 mRNA expression (Fig. 5b; P < 0.01) as compared to control. In MSC pre-treated with 17-AAG, there was a significant decrease in MMP-9 and MMP-2 expression comparing to rhHsp90α group (Fig. 5b; P < 0.01 and P < 0.05, respectively). U0126 had a similar effect on MMP-9 and MMP-2 expression, with expression levels of metaloproteases significantly lower than in rhHsp90α group (Fig. 5b; P < 0.01). On the other hand, pre-treating the cells with wortmannin prior to incubation with rhHsp90α resulted in markedly decreased MMP-9 expression levels (P < 0.01) but had no effect on MMP-2 expression comparing to rhHsp90α treatment group (Fig. 5b). Pre-treatment of MSC with 17-AAG, wortmannin or U0126 was not enough to reduce MMP-2 expression, elevated by rhHsp90 α, to the levels detected in control cells (Fig. 5b; P < 0.01, P < 0.05, P < 0.01, respectively).
The effect of rhHsp90 on the proteolytic activity of MMPs in MSC. Cells were either left untreated (control), or pre-treated with 17-AAG, wortmannin or U0126 where required, and treated with rhHsp90 as described above. Proteolitic activity of secreted MMP-2 and MMP-9 in the growth medium was analyzed by gelatin zymography
RhHsp90α enhances the protein expression of MMP-2 and MMP-9. Cells were treated as in Fig. 4. Protein expression levels of MMP-2 and MMP-9 were detected using Western blot (a). β-Actin was used as a loading control. Expression levels of MMP-9 and MMP-2 mRNA were assessed by real-time PCR as described in “Methods” section and normalized to GAPDH expression (b). Data represent mean ± SD; n = 3; **P < 0.01, ## P ≤ 0.01, # P < 0.05, and + P < 0.01
RhHsp90α Up-Regulates mRNA Expression of VCAM-1 and CXCR4
The SDF-1/CXCR4 axis plays a pivotal role in cell migration. Vascular cell adhesion molecule 1 (VCAM-1) also modulate cell adhesion and motility. We next investigated whether rhHsp90α is able to affect gene expression of VCAM-1 and CXCR4 in MSC. Cells were incubated with rhHsp90α with or without inhibitors 17-AAG, wortmannin, or U0126 for 24 h, and expression levels of VCAM-1 and CXCR4 mRNA were evaluated using real-time PCR. Exposure to rhHsp90α significantly increased the expression of VCAM-1 and CXCR4 (over 1.5- and 3-fold increase, respectively; P < 0.01) as compared with the control group (Fig. 6). As shown in Fig. 6, rhHsp90-induced up-regulation of VCAM-1 expression was markedly reduced following pre-treatment with 17-AAG and wortmannin to the levels below the untreated control (P < 0.01) as compared to cells treated directly with rhHsp90 α (P < 0.01). While pre-treating the cells with 17-AAG and wortmannin was able to slightly decrease the levels of CXCR4 expression, it remained significantly elevated as compared to control cells (P < 0.05; Fig. 6). On the other hand, U0126 efficiently suppressed rhHsp90-induced up-regulation of VCAM-1 and CXCR4 in MSC to the levels similar to untreated control (P < 0.05; Fig. 6).
RhHsp90α causes up-regulation of the VCAM-1 and CXCR4 gene expression. Expression levels of VCAM-1 and CXCR4 in MSC, treated with rhHsp90 in the presence/absence of 17-AAG, wortmannin or U0126 were analyzed by real-time PCR, and normalized to GAPDH expression. Data represent mean ± SD, n = 3. P values are specified above
PI3K/Akt Pathways and ERK Pathways Mediated rhHsp90α-Induced Cell Migration
We further explored the mechanisms involved in Hsp90α regulation of MSC migration by analyzing the phosphorylation of Akt and ERK1/2, an indicator of the activity of PI3K/Akt and ERK signaling pathways. MSC, treated with rhHsp90α for 24 h, exhibited markedly increased levels of Akt phosphorylation compared with control group (Fig. 7a; *P < 0.05). This increase was significantly attenuated by pre-treating the cells with 17-AAG and wortmannin (*P < 0.05) (Fig. 7a). Similarly, RhHsp90α treatment resulted in the increase in the levels of the ERK1/2 phosphorylation as compared to control group (Fig. 7b; *P < 0.05). ERK1/2 phosphorylation was specifically inhibited by pre-treating the cells with 17-AAG and U0126 (P < 0.05 compared to rhHsp90α treatment group), while wortmannin had no effect on ERK1/2 phosphorylation levels (Fig. 7b).
The effect of rhHsp90α on PI3K/Akt and ERK pathways in MSC. MSC were pre-treated with 17-AAG, wortmannin, and U0126 when required, and incubated with rhHspα for 24 h. Levels of p-Akt (a) and p-ERK1/2 (b) were measured by Western blotting and normalized for total Akt and ERK1/2, respectively. β-Actin was used as a loading control
Discussion
The aim of this study was to investigate the mechanisms by which recombinant human Hsp90α regulates rat MSC migration in vitro. We demonstrated that in MSC rhHsp90α stimulated PI3K/Akt and ERK1/2 signaling pathways, leading to increased cell migration. Activation of the PI3K/Akt and ERK1/2 pathways by rhHsp90α correlated with increased expression, secretion, and activity of MMP-9 and MMP-2 metalloproteases. The use of specific inhibitors and silencing Hsp90 expression in MSC with siRNA confirmed that the effect of rhHsp90α on cell migration was dependent on PI3K/Akt and ERK1/2 signaling.
Homing and engraftment of MSCs into damaged tissue are presumably a multistep process, sharing some common features with leukocyte migration to inflammatory sites, and the homing of lymphocytes into lymph nodes [22]. Transplanted MSCs, which migrate through the blood circulation, interact with endothelial cells, and these interactions are mediated by the coordinated action of activated adhesive molecules. Adhesive activation processes are triggered specifically by chemokines, such as SDF-1, and vascular ligands, such as VCAM-1 and ICAM-1. Transendothelial migration of cells requires degradation of basement membrane, which is dependent on the production of matrix-degrading enzymes capable of degrading type IV collagen, especially MMP-2 and MMP-9. In this study, we provide first evidence that Hsp90 can enhance MSC migration in vitro.
Hsp90 is a chaperone protein, highly expressed in the G0 phase of cells during neuroectoderm differentiation, suggesting that it is required to maintain cells in this phase [23]. Lesko et al. reported that inhibiting Hsp90 with geldanamycin (GA) decreased the expression of MET receptor in rhabdomyosarcoma (RMS) cell lines in vitro, and inhibited the chemotaxis of RMS cells toward the hepatocyte growth factor gradient. Treatment with GA also blocked the homing of RMS cells into the bone marrow of mice with severe combined immune deficiency [24].
Hsp90 exists mainly as a constitutive homodimer, consisting of α and β isoforms, or as a higher molecular weight oligomer in mammalian cells [25, 26], and its dimerization domain resides mainly within the 90 carboxyl-terminal amino acids. Both Hsp90α and β have a highly conserved 25 kDa N-terminal domain that is the ATP-binding pocket and a binding site for GA [27, 28]. ATP binding assists in the dimerization of Hsp90 by changing its conformation and stabilizing Hsp90 client proteins [29]. Substrate binding at the N-terminal site is affected by nucleotides (ATP and ADP) and by drugs such as GA, which binds to Hsp90 and disrupts the complex between Hsp90 and certain client proteins such as the protein kinase Akt [30].
Stromal cell derived factor 1 (SDF-1) is constitutively expressed on the bone marrow endothelium, and is a ligand of C-X-C chemokine receptor type 4 (CXCR4) that is expressed on the surface of many different cell types such as monocytes, B-lymphocytes, and most T cells. SDF-1 expression is increased in atherosclerotic plaques, while unstable coronary syndromes are associated with decreased SDF-1 expression [31]. SDF-1 mediates several different activities such as chemotaxis, adhesion, proliferation, survival, and apoptosis [32, 33]. Activation of CXCR4 on the surface of lymphocytes and monocytes through binding SDF-1 stimulates chemotaxis, resulting in recruitment to sites of immune and inflammatory reactions. Hematopoietic and endothelial precursor cells (EPC) express CXCR4, and the release of SDF-1 by bone marrow (BM) stromal cells mediates sequestration and homing of these progenitor cells to BM [34]. SDF-1 and CXCR4 contribute to the involvement of bone marrow-derived cells and collaborate with VEGF in the development of several types of ocular neovascularization [35]. Abbott et al. reported that, after 48 h intravenous infusion of donor-lineage bone marrow-derived stem cells (BMDCs), about 80.5 % BDMCs had migrated within the infracted hearts compared with sham-operated controls. Treatment with AMD3100 (a specific blocker of CXCR4) diminished BMDC recruitment after MI, whereas expression of SDF-1 in the heart by adenoviral gene delivery 48 h after MI doubled BMDC recruitment over MI alone. Also, levels of VEGF, MMP-9, and VCAM-1 were increased after MI, which suggest that these proteins may act in concert with SDF-1 to recruit BMDCs to the injured heart [36]. SDF-1/CXCL12 induced chemotaxis of ESCs, which was enhanced by diprotin A inhibition of CD26/dipeptidylpeptidase IV. Endogenous and exogenous SDF-1/CXCL12 enhanced embryoid body production of primitive and definitive erythroid, granulocyte–macrophage, and multipotential progenitors [37]. Combined use of Statins and SDF-1 further improved the reperfusion ratio (0.62 ± 0.08, P < 0.05). More cell proliferation, less apoptosis, enhanced EPC incorporation, and higher capillary density were observed in ischemic tissues treated with both statin and SDF-1. In vitro mono-treatment with either fluvastatin or SDF-1 facilitated EPC proliferation and migration, inhibited EPC apoptosis, enhanced the expression of MMP-2 and MMP-9, and increased Akt phosphorylation and nitric oxide production [38].
VCAM-1 plays a role in the migration of human T lymphocytes [39] and in the mouse cardiac endothelium [40]. VCAM-1 induced migration of endothelial cells and CPCs and prevented cardiomyocyte death from oxidative stress through activation of Akt, ERK, and p38 MAPK. Treatment with a specific antibody for very late antigen-4 (VLA-4), a receptor of VCAM-1, abolished the effects of CPC-derived conditioned medium on cardiomyocytes and CPCs in vitro, and inhibited angiogenesis, CPC migration, and survival in vivo [41]. Lu et al. [42] reported that on the third and seventh day post MI, the activity of ICAM-l and chemoattractant cytokines (MCP-1) were enhanced, which facilitate the homing, chemotaxis, and migration of circulating cells into the infarct site. Our results clearly show that RhHsp90α causes the up-regulation of VCAM-1 and CXCR4 expression in MSCs, suggesting the role of VCAM-1 and CXCR4 in modulating rat MSC migration.
Conclusions
In this study, we addressed the role of AKT and ERK1/2 pathways in the effect of rhHsp90α on the migration of rat MSCs. Stimulation of Akt and ERK1/2 phosphorylation and activity by Hsp90α was attenuated by wortmannin, a PI3K/Akt inhibitor, and U0126, an inhibitor of MEK1/2. Wortmannin and U0126 also inhibited rhHsp90α-induced MMP-2 and MMP-9 mRNA expression, and the activities of these secreted proteases in rat MSCs. RhHsp90α enhanced gene expression of VCAM-1 and CXCR4 in MSCs, which implies that VCAM-1 and CXCR4 are involved in regulating the migration of MSC.
To our knowledge, this is the first study that explains the involvement of Hsp90 in enhancing the migration of rat MSCs. Our results conclude that Hsp90-induced MSCs migration is mediated at least in part by the activation of MMP-2, MMP-9, SDF-1/CXCR4 pathways, and VCAM-1 through AKT and ERK1/2 signaling. Understanding the mechanisms by which Hsp90 induces MSCs migration may lead to improved therapies for treating ischemia heart diseases.
Change history
15 June 2019
An amendment to this paper has been published and can be accessed via a link at the top of the paper.
15 June 2019
An amendment to this paper has been published and can be accessed via a link at the top of the paper.
References
Majumdar, M. K., Thiede, M. A., Haynesworth, S. E., Bruder, S. P., & Gerson, S. L. (2000). Human marrow-derived mesenchymal stem cells (MSCs) express hematopoietic cytokines and support long-term hematopoiesis when differentiated toward stromal and osteogenic lineages. Journal of Hematotherapy & Stem Cell Research, 9(6), 841–848.
Wright, V., Peng, H., Usas, A., et al. (2002). BMP4-expressing muscle-derived stem cells differentiate into osteogenic lineage and improve bone healing in immunocompetent mice. Molecular Therapy, 6(2), 169–178.
Mizuno, K., Muneta, T., Morito, T., et al. (2008). Exogenous synovial stem cells adhere to defect of meniscus and differentiate into cartilage cells. Journal of Medical and Dental Sciences, 55(1), 101–111.
Li, Y., Yu, J., Li, M., Qu, Z., & Ruan, Q. (2011). Mouse mesenchymal stem cells from bone marrow differentiate into smooth muscle cells by induction of plaque-derived smooth muscle cells. Life Sciences, 88(3–4), 130–140.
Wang, Q. W., Chen, Z. L., & Piao, Y. J. (2005). Mesenchymal stem cells differentiate into tenocytes by bone morphogenetic protein (BMP) 12 gene transfer. Journal of Bioscience and Bioengineering, 100(4), 418–422.
Elabd, C., Chiellini, C., Carmona, M., et al. (2009). Human multipotent adipose-derived stem cells differentiate into functional brown adipocytes. Stem Cells, 27(11), 2753–2760.
Psaltis, P. J., Zannettino, A. C., Worthley, S. G., & Gronthos, S. (2008). Concise review: Mesenchymal stromal cells: potential for cardiovascular repair. Stem Cells, 26(9), 2201–2210.
Marenzi, G., & Bartorelli, A. L. (2007). Improved clinical outcome after intracoronary administration of bone marrow-derived progenitor cells in acute myocardial infarction: final 1-year results of the REPAIR-AMI trial. European Heart Journal, 28(17), 2172–2173. author reply 2173–2174.
Fuh, E., & Brinton, T. J. (2009). Bone marrow stem cells for the treatment of ischemic heart disease: A clinical trial review. Journal of Cardiovascular Translational Research, 2(2), 202–218.
Barbash, I. M., Chouraqui, P., Baron, J., et al. (2003). Systemic delivery of bone marrow-derived mesenchymal stem cells to the infarcted myocardium: feasibility, cell migration, and body distribution. Circulation, 108(7), 863–868.
Langer, T., Rosmus, S., & Fasold, H. (2003). Intracellular localization of the 90 kDA heat shock protein (HSP90alpha) determined by expression of a EGFP-HSP90alpha-fusion protein in unstressed and heat stressed 3T3 cells. Cell Biology International, 27(1), 47–52.
Yano, A., Tsutsumi, S., Soga, S., et al. (2008). Inhibition of Hsp90 activates osteoclast c-Src signaling and promotes growth of prostate carcinoma cells in bone. Proceedings of the National Academy of Sciences of the United States of America, 105(40), 15541–15546.
Wu, L. X., Xu, J. H., Huang, X. W., Zhang, K. Z., Wen, C. X., & Chen, Y. Z. (2006). Down-regulation of p210(bcr/abl) by curcumin involves disrupting molecular chaperone functions of Hsp90. Acta Pharmacologica Sinica, 27(6), 694–699.
Zsebik, B., Citri, A., Isola, J., Yarden, Y., Szollosi, J., & Vereb, G. (2006). Hsp90 inhibitor 17-AAG reduces ErbB2 levels and inhibits proliferation of the trastuzumab resistant breast tumor cell line JIMT-1. Immunology Letters, 104(1–2), 146–155.
Giaccone, G., & Rajan, A. (2009). Met amplification and HSP90 inhibitors. Cell Cycle, 8(17), 2682.
Grammatikakis, N., Lin, J. H., Grammatikakis, A., Tsichlis, P. N., & Cochran, B. H. (1999). p50(cdc37) acting in concert with Hsp90 is required for Raf-1 function. Molecular and Cellular Biology, 19(3), 1661–1672.
Sidera, K., Gaitanou, M., Stellas, D., Matsas, R., & Patsavoudi, E. (2008). A critical role for HSP90 in cancer cell invasion involves interaction with the extracellular domain of HER-2. Journal of Biological Chemistry, 283(4), 2031–2041.
Tsutsumi, S., Scroggins, B., Koga, F., et al. (2008). A small molecule cell-impermeant Hsp90 antagonist inhibits tumor cell motility and invasion. Oncogene, 27(17), 2478–2487.
Gao, F., Hu, X. Y., Xie, X. J., et al. (2010). Heat shock protein 90 protects rat mesenchymal stem cells against hypoxia and serum deprivation-induced apoptosis via the PI3K/Akt and ERK1/2 pathways. Journal of Zhejiang University-Science B, 11(8), 608–617.
Xie, X. J., Wang, J. A., Cao, J., & Zhang, X. (2006). Differentiation of bone marrow mesenchymal stem cells induced by myocardial medium under hypoxic conditions. Acta Pharmacologica Sinica, 27(9), 1153–1158.
Heussen, C., & Dowdle, E. B. (1980). Electrophoretic analysis of plasminogen activators in polyacrylamide gels containing sodium dodecyl sulfate and copolymerized substrates. Analytical Biochemistry, 102(1), 196–202.
Baer, P. C., & Geiger, H. (2010). Mesenchymal stem cell interactions with growth factors on kidney repair. Current Opinion in Nephrology and Hypertension, 19(1), 1–6.
Walsh, D., Li, Z., Wu, Y., & Nagata, K. (1997). Heat shock and the role of the HSPs during neural plate induction in early mammalian CNS and brain development. Cellular and Molecular Life Sciences, 53(2), 198–211.
Lesko, E., Gozdzik, J., Kijowski, J., Jenner, B., Wiecha, O., & Majka, M. (2007). HSP90 antagonist, geldanamycin, inhibits proliferation, induces apoptosis and blocks migration of rhabdomyosarcoma cells in vitro and seeding into bone marrow in vivo. Anti-Cancer Drugs, 18(10), 1173–1181.
Minami, Y., Kawasaki, H., Miyata, Y., Suzuki, K., & Yahara, I. (1991). Analysis of native forms and isoform compositions of the mouse 90-kDa heat shock protein, HSP90. Journal of Biological Chemistry, 266(16), 10099–10103.
Nemoto, T., & Sato, N. (1998). Oligomeric forms of the 90-kDa heat shock protein. Biochemical Journal, 330(Pt 2), 989–995.
Grenert, J. P., Sullivan, W. P., Fadden, P., et al. (1997). The amino-terminal domain of heat shock protein 90 (hsp90) that binds geldanamycin is an ATP/ADP switch domain that regulates hsp90 conformation. Journal of Biological Chemistry, 272(38), 23843–23850.
Basso, A. D., Solit, D. B., Chiosis, G., Giri, B., Tsichlis, P., & Rosen, N. (2002). Akt forms an intracellular complex with heat shock protein 90 (Hsp90) and Cdc37 and is destabilized by inhibitors of Hsp90 function. Journal of Biological Chemistry, 277(42), 39858–39866.
Roe, S. M., Ali, M. M., Meyer, P., et al. (2004). The mechanism of Hsp90 regulation by the protein kinase-specific cochaperone p50(cdc37). Cell, 116(1), 87–98.
Sato, S., Fujita, N., & Tsuruo, T. (2000). Modulation of Akt kinase activity by binding to Hsp90. Proceedings of the National Academy of Sciences of the United States of America, 97(20), 10832–10837.
Abi-Younes, S., Sauty, A., et al. (2000). The stromal cell-derived factor-1 chemokine is a potent platelet agonist highly expressed in atherosclerotic plaques. Circulation Research, 86(2), 131–138.
Yamaguchi, J., Kusano, K. F., et al. (2003). Stromal cell-derived factor-1 effects on ex vivo expanded endothelial progenitor cell recruitment for ischemic neovascularization. Circulation, 107(9), 1322–1328.
Oberlin, E., Amara, A., et al. (1996). The CXC chemokine SDF-1 is the ligand for LESTR/fusin and prevents infection by T-cell-line-adapted HIV-1. Nature, 382(6594), 833–835.
Jo, D. Y., Rafii, S., et al. (2000). Chemotaxis of primitive hematopoietic cells in response to stromal cell-derived factor-1. Journal of Clinical Investigation, 105(1), 101–111.
Lima e Silva, R., Shen, J., et al. (2007). The SDF-1/CXCR4 ligand/receptor pair is an important contributor to several types of ocular neovascularization. FASEB Journal, 21(12), 3219–3230.
Abbott, J. D., Huang, Y., et al. (2004). Stromal cell-derived factor-1alpha plays a critical role in stem cell recruitment to the heart after myocardial infarction but is not sufficient to induce homing in the absence of injury. Circulation, 110(21), 3300–3305.
Guo, Y., Hangoc, G., et al. (2005). SDF-1/CXCL12 enhances survival and chemotaxis of murine embryonic stem cells and production of primitive and definitive hematopoietic progenitor cells. Stem Cells, 23(9), 1324–1332.
Shao, H., Tan, Y., et al. (2008). Statin and stromal cell-derived factor-1 additively promote angiogenesis by enhancement of progenitor cells incorporation into new vessels. Stem Cells, 26(5), 1376–1384.
Hyun, Y. M., Chung, H. L., et al. (2009). Activated integrin VLA-4 localizes to the lamellipodia and mediates T cell migration on VCAM-1. The Journal of Immunology, 183(1), 359–369.
Bowden, R. A., Ding, Z. M., et al. (2002). Role of alpha4 integrin and VCAM-1 in CD18-independent neutrophil migration across mouse cardiac endothelium. Circulation Research, 90(5), 562–569.
Matsuura, K., Honda, A., et al. (2009). Transplantation of cardiac progenitor cells ameliorates cardiac dysfunction after myocardial infarction in mice. Journal of Clinical Investigation, 119(8), 2204–2217.
Lu, L., Zhang, J. Q., et al. (2004). Molecular and cellular events at the site of myocardial infarction: from the perspective of rebuilding myocardial tissue. Biochemical and Biophysical Research Communications, 320(3), 907–913.
Acknowledgments
This project was supported by the National Natural Science Foundation of China (Nos. 30670868, 30770887, and 30770887/H0220), the Traditional Chinese Medicine of Zhejiang Province (No. 2014ZA005), and the Zhejiang Provincial Natural Science foundation of China (Y2100362) and Science Technology Department of Zhejiang Province (2010R10G2010160). China.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gao, F., Hu, X., Xie, X. et al. Heat Shock Protein 90 Stimulates Rat Mesenchymal Stem Cell Migration via PI3K/Akt and ERK1/2 Pathways. Cell Biochem Biophys 71, 481–489 (2015). https://doi.org/10.1007/s12013-014-0228-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-014-0228-6