Abstract
Resveratrol (RSV) is known for its antioxidant properties; however, this compound has been proposed to have cytotoxic and pro-oxidant effects depending on its concentration and time of exposure. We previously reported the cell cycle arrest effect of low doses of RSV in GRX cells, an activated hepatic stellate cell model. Here, we evaluated the effects of RSV treatment (0.1–50 μM) for 24 and 120 h on GRX viability and oxidative status. Only treatment with 50 μM of RSV reduced the amount of live cells. However, even low doses of RSV induced an increased reactive species production at both treatment times. While being diminished within 24 h, RSV induced an increase in the SOD activity in 120 h. The cellular damage was substantially increased at 24 h in the 50 μM RSV-treated group, as indicated by the high lipoperoxidation, which may be related to the significant cell death and low proliferation. Paradoxically, this cellular damage and lipoperoxidation were considerably reduced in this group after 120 h of treatment while the surviving cells proliferated. In conclusion, RSV induced a dose-dependent pro-oxidant effect in GRX cells. The highest RSV dose induced oxidative-related damage, drastically reducing cell viability; but this cytotoxicity seems to be attenuated during 120 h of treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Resveratrol (3,5,4′,-trihydroxystilbene; RSV) is a phytoalexin that responds to environmental stresses and pathogenic infections, produced by approximately 31 plant genera, including plums, peanuts, and grapes [1]. This polyphenolic compound has long been thought to be associated with the beneficial effects of red wines and the prevention of pathologies due to the nature of its molecular targets, which include cytokines, transcription factors, cell cycle proteins, and proteins associated with metastasis. Such characteristics endow RSV with important biological properties such as chemopreventive, antiproliferative, and antioxidant activities [2]. However, many studies also suggest that RSV exerts an opposite effect, acting as a pro-oxidant agent depending on its concentration, time of exposure, and cell type [3]. This dualistic behaviour characterises RSV as an active redox molecule [4]. Indeed, in different cell types, such as a fibroblast cell line and tumour human cells, RSV was found to exert its cytotoxic action at higher doses [5]. Likewise, it was already discussed that RSV induces cell cycle arrest [6, 7] and stimulates the reactive oxygen species (ROS)-activated mitochondrial pathway leading to apoptosis [8].
Hepatic stellate cells (HSC) are known to play an important role in the liver fibrogenic process. In the resting state, these cells maintain a quiescent or lipocytic phenotype characterised by the presence and storage of retinol droplets in the cytoplasm. The activation of HSC is associated with continuous damage to the liver due to virus infection, metabolic disorders, or alcohol abuse, and results mostly from paracrine stimulation due changes in the surrounding extracellular matrix (ECM). The oxidative stress as well as exposure to lipid peroxides and the products of damaged hepatocytes is a determining factor for the activation state of HSC, which ultimately leads to a chronic inflammatory process. In this context, these cells develop a myofibroblastic phenotype in which they lose their lipid droplets, proliferate more rapidly, and become the main ECM producers contributing to liver fibrosis [9, 10].
Much of our understanding on the cell and molecular mechanisms of liver fibrosis has been gained through animal models and from in vitro studies employing culture model of activated HSC [7]. The GRX cell line was established through liver fibre granulomas induced by Schistosoma mansoni experimental infection, and this cell line is the first HSC model [11, 12]. In standard cultures, GRX cells express an activated phenotype that is an intermediate of the lipocytic and myofibroblastic phenotypes [13]. GRX cells can be induced in vitro to express a lipocytic phenotype by treatment with retinoids, indomethacin, β-carotene, or capsaicin, which stimulate lipid storage and cause a decrease in cell proliferation and ECM production [14–16]. On the other hand, GRX cells can be differentiated into an activated myofibroblastic phenotype when exposed to cytokines, growth factors, or oxidative stress conditions [17].
Clearance of activated stellate cells by apoptosis remains an appealing target as an antifibrotic therapy in chronic liver diseases, using a physiological mechanism of endogenous pathway of fibrosis regression [10]. Besides the evidences that RSV induces ROS-mediated apoptosis, our earlier studies showed that even GRX treatment with low doses of RSV (0.1–1 μM) caused cell cycle arrest in the S phase [7]. In this regard, the major aim of the present study was to investigate if the cell cycle arresting effect of RSV on GRX cells found in our previous work is accompanied by ROS production. As RSV can trigger different responses depending on its dose or time of exposure, we chose to evaluate the effects of crescent concentrations (1–50 μM) on GRX cells under treatment for 24 and 120 h. Our results revealed that RSV exerts dose-dependent pro-oxidant effects in GRX under 24 and 120 h of treatment. This find may be related to the GRX cell cycle arrest at low doses. Furthermore, we found that 50 μM of RSV provoked oxidative cytotoxicity, which seems to be attenuated during 120 h of treatment.
Materials and Methods
Cell Culture
The GRX cell line was obtained from the Cell Bank of Rio de Janeiro (HUCFF, UFRJ, RJ). The cells were seeded (105/ml or 3 × 104/ml, respectively) on 6-well culture plates (for the TBARS assay) and 24-well culture plates (Nunc, Roskilde, Denmark) 24 h before treatment with RSV. The cells were maintained in Dulbecco’s Modified Eagle’s Medium (DMEM, Invitrogen, Carlsbad, CA, USA) supplemented with 5 % foetal bovine serum (FBS, Cultilab, Campinas, SP, Brazil) and 2 g/l HEPES buffer (pH 7.4) in a humidified atmosphere with 5 % CO2 at 37 °C.
Resveratrol Treatment
Resveratrol (Sigma Inc., St. Louis, MO, USA) was dissolved in 20 μl of ethanol (Merck, Darmstadt, Germany) to a stock concentration of 100 mM and diluted sequentially in DMEM to a final concentration of 0.1, 1, 10 and 50 μM just before use. The cells were treated during 24 and 120 h. Media without or with RSV at the aforementioned concentrations were changed daily during the 120-h experiments.
Viability and Cytotoxicity Analysis
MTT Assay
The cell viability was measured by quantifying the cellular dehydrogenases activities that reduce MTT (3-4,5-dimethylthiazolyl-2,5-diphenyl-2H-tetrazolium bromide, Sigma Inc.) to a purple formazan salt [18]. After RSV treatment, the cells were incubated with 1 mg/ml of MTT for 2 h at 37 °C. The cells were then lysed in dimethylsulphoxide (DMSO, Sigma Inc.) and the absorbance was quantified in a 96-well microplate spectrophotometer (Spectra Max 190, Molecular Devices, Sunnyvale, CA, USA) at 570 and 630 nm.
Sulphorhodamine B Assay
The sulphorhodamine B assay is used for cell density determination and thus, is indicative for cell survival. After RSV treatment, the cells were washed with phosphate-buffered saline (PBS) and fixed with a 4 % paraformaldehyde solution for 15 min, stained with 0.4 % sulphorhodamine B in acetic acid and finally dissolved in 1 % SDS [19]. The absorbance was measured in a 96-well microplate spectrophotometer (Spectra Max 190) at 515 nm.
The Trypan Blue Exclusion
The cell viability was also determined by the trypan blue exclusion method. Briefly, after treatment media was removed and the cells from each well were harvested by trypsin/EDTA (Sigma Inc). A 10 % solution of trypan blue (Sigma Inc.) was added and the cells were immediately counted in a haemocytometer [20]. The dead trypan blue-positive and alive negative cells were counted. Dead cells were calculated as a percentage of total cells in each group.
Oxidative Stress Analysis
Evaluation of the Intracellular Reactive Species Production
The intracellular reactive species (RS) production was analysed using the non-fluorescent and cell membrane-permeable 2′-7′-dichlorofluorescein diacetate (DCFH-DA, Sigma Inc.). DCFH-DA is hydrolysed by intracellular esterases and then oxidised by RS to a fluorescent, polar and non-permeable 2′-7′-diclorofluorescein (DCF) compound [21]. After treatment with RSV, the cells were incubated in the dark with 10 μM DCFH-DA in DMEM without serum for 30 min at 37 °C. The cells were washed and scraped with 0.2 % Triton X-100 (Sigma Inc.). The fluorescence was measured in a 96-well microplate reader (Spectra Max Gemini XPS, Molecular Devices) after exciting at 485 nm, and collecting the emission at 520 nM. The results were expressed as fluorescence units per μg of proteins, which were quantified by the Lowry’s modified assay [22].
Antioxidant Enzyme Activity Quantification: Superoxide Dismutase and Catalase
The superoxide dismutase (SOD) activity was quantified by inhibiting the superoxide-dependent adrenaline auto-oxidation, and reading the absorbance at 480 nm [23]. The results were expressed as units of SOD per mg of protein. The catalase (CAT) activity was quantified by evaluating the decrease in H2O2 absorbance and reading the absorbance at 240 nm [24]. The results were expressed as units of CAT per mg of protein. Both experiments were performed in a 96-well microplate spectrophotometer (Spectra Max 190).
Quantification of Cellular Thiol (–SH) Content
The cellular free thiols (–SH) were analysed using the sulphhydryl reagent 5,5′-dithiobis(2-nitrobenzoic acid) (DTNB), also referred as Elmann’s reagent, which estimate the oxidative alterations of proteins and non-protein peptides. This analysis is based on the reaction of free thiols with DTNB resulting in mixed disulphide and 2-nitro-5-thiobenzoic acid (TNB), which is quantified by the absorbance of TNB anion at 412 nm [25]. Briefly, after treatment with RSV for 24 and 120 h, cells were collected in 0.1 % of sodium dodecyl sulphate (SDS) and 0.01 M of DTNB diluted in ethanol, and then incubated at room temperature for 20 min. The concentration of –SH was calculated using a molar extinction coefficient of 13,600 M−1 cm−1. The absorbance was measured at 412 nm. Results were expressed as μM of –SH per mg of protein.
Quantification of Thiobarbituric Acid Reactive Species (TBARS)
Lipoperoxidation was measured as described by the TBARS method [26]. Briefly, after each treatment, the cells were washed and scraped with Tris buffer (0.05 mM, pH 7.6) and proteins were precipitated with 10 % trichloroacetic acid. The cell homogenate was mixed with 0.67 % thiobarbituric acid (TBA) and boiled at 100 °C for 30 min. The samples were centrifuged at 3,000 rpm, the lipid supernatant was extracted with butanol, and its absorbance was measured in a spectrophotometer at 512 nm. The concentration of TBARS was calculated using a molar extinction coefficient of 153,000 M−1 cm−1. The results were expressed in μM TBARS per mg of protein.
Cell Proliferation Analysis
The [3H] Thymidine Incorporation Assay
The cells were incubated during the last 24 h of each treatment with 1 μCi/ml of [6-3H] thymidine (specific activity 23.0 Ci/nmol, Amersham Biosciences, Hillerod, Denmark). Then, the cells were washed with PBS, and 10 % trichloroacetic acid was added to each well for 1 h. The pellet was dissolved with 0.1 N NaOH, and the incorporated radioactive DNA was determined by scintillation counting and expressed as cpm per mg of protein [27].
The Cell Population Doubling Calculations
After RSV treatment, the incubation media were removed, the cells were tripsinized and the viable cells were immediately counted in a haemocytometer, as described before. The population doublings were calculated for each group as follows: cell population doubling = [log (post-treatment cells number/initial cell number)]/log 2, as previously described [28].
Statistical Analysis
The data were expressed as mean ± standard error of the mean. One-way ANOVA was used to analyse the effect of RSV treatment. When necessary, two-way ANOVA was used (using the RSV doses and time of treatment as factors) and post-hoc Duncan multiple range test was performed. Results were considered statistically different when the p values were equal to or less than 0.05.
Results
The Effects of Resveratrol on the GRX Cell Viability
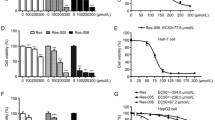
To initiate our studies, we wanted to know if different doses and times of RSV treatments would have any effect in cell viability (Fig. 1). While low doses of RSV did not affect the GRX viability, the higher dose (50 μM) significantly decreased the cell viability (Fig. 1a), reducing considerably cell survival and population density (Fig. 1b, c). However, our attention was drawn to the fact that the percentage of trypan blue-positive cells in the 50 μM RSV group was higher only at 24 h, indicating increase in cellular membrane damage only in this treatment time condition (Fig. 1d). Interestingly, treatment with doses greater than 50 μM of RSV (75–100 μM) resulted in death of all cells along the established times of treatment (Data not shown). Altogether, these results confirmed the dose-dependent effect of RSV regarding the survival/viability of GRX cells, and were in accordance with the previous studies that showed the cytotoxic effect of RSV related to the dose of treatment [3].
The effect of resveratrol on cell viability. GRX cells were treated with 0 (control), 0.1, 1, 10 and 50 μM of RSV for 24 or 120 h. The cell viability and survival were established through MTT (a) and Sulphorhodamine B (b) assays and by Trypan Blue exclusion counting (c). The percent of unviable cells was calculated (d). Asterisk indicates significant differences between groups (p ≤ 0.05). Data are expressed as mean ± SEM. (n = 4)
The Effects of Resveratrol on Reactive Species Production
Previous works had shown that hydrogen peroxide plays an important role by inducing cell cycle arrest and inhibition of cell proliferation [29, 30]. Likewise, RS may play an important role in elevating numbers of non-viable or damaged cells via the induction of oxidative stress [31]. Based on this premise and considering the fact that RSV induced GRX cell cycle arrest [6, 7], we sought to determine if RS was also present at these doses of RSV treatment. Treatment for 24 h with doses between 1 and 50 μM of RSV triggered a dose-dependent pro-oxidant effect on GRX. A similar result was found on GRX treated for 120 h, in which RSV also promoted pro-oxidant effects since the lowest dose (0.1 μM). A two-way ANOVA demonstrated that the time of treatment [F(1,38) = 248.0; p ≤ 0.05] and the RSV dose [F(4,38) = 17.3; p < 0.05] increased RS production in a dependent manner [β24h = 0.71, β120h = 0.61, p ≤ 0.05]. Also, the two-way ANOVA analysis revealed an interaction between the time of treatment and RSV dose [F(4,38) = 5.7; p ≤ 0.05] because the increase of the DCF fluorescence provoked by the RSV was higher in the 120-h treatment (Fig. 2).
The effect of resveratrol on the ROS production. GRX cells were treated with 0 (control), 0.1, 1, 10 and 50 μM of RSV for 24 or 120 h and the intracellular ROS production was detected using the non-fluorescent and cell membrane-permeable 2′-7′-dichlorofluorescein diacetate (DCFH-DA). The data were expressed as fluorescence units per μg of protein expressed as mean ± SEM. (n = 4). Single asterisk statistically significant differences from the control. Double asterisk represents significant differences between the 50 μM of RSV-treated group and the others (the control and RSV groups treated with lower doses) at 24 and 120 h (p ≤ 0.05)
The Effects of Resveratrol on the Enzymatic Antioxidant Activities: Superoxide Dismutase and Catalase
Since a significant increase in the RS production was induced by the RSV in both treatment times, we assessed the activities of the main enzymatic antioxidants defences. Interestingly, the analysis of SOD activity in each treatment period revealed an opposite effect of RSV. While cells treated for 24 h with 1–50 μM of RSV presented a decrease of SOD activity, all cells treated for 120 h presented an increase in this enzyme activity, thus revealing an interaction between the time of treatment and RSV dose [F(3,33) = 13.76; p ≤ 0.05]. The determination of the SOD activity in the untreated (control) group revealed that the SOD activity was decreased with the culture time. A two-way ANOVA demonstrated that the SOD activity was dependent on the treatment time [F(1,33) = 80.19; p ≤ 0.05] and on the RSV dose [F(4,33) = 7.73; p ≤ 0.05] (Fig. 3a). Although the highest dose of RSV has visibly decreased the CAT activity, there was no statistical difference in the enzyme activity in cells treated with all RSV concentrations for 24 h. However, compared to the control group, treatment with 50 μM of RSV for 120 h was able to significantly decrease CAT activity (p < 0.05) (Fig. 3b). Besides these effects on the SOD and CAT activities, we found a significant increase in the SOD/CAT ratio when compared with the control (control = 1) only in the cells treated with 50 μM RSV for 120 h (Fig. 3c).
The antioxidant enzyme activities. GRX cells were treated with 0 (control), 0.1, 1, 10 and 50 μM of RSV for 24 or 120 h and the SOD (a) and CAT (b) activities were determined. c The SOD/CAT ratio. Data are expressed as mean ± SEM. (n = 4). Single asterisk indicates statistically significant differences from control. Double asterisk represents significant differences between the 50 μM of RSV-treated group and the others (the control and RSV groups treated with lower doses) at 120 h (p ≤ 0.05)
The Effects of Resveratrol on the Oxidation of Protein and Non-protein Peptides
The oxidation or reduction of thiol (–SH) content of proteins or non-protein peptides, such as glutathione (GSH), cysteine and homocysteine, is a dynamic and reversible process by which cells can modulate its redox state [32, 33]. However, despite the pro-oxidant effects that were accompanied mainly by changes in SOD activity, treatment with RSV did not induce thiols oxidation in GRX. In contrast, after 24 h of treatment, only cells that received lower doses of RSV, i.e. 0.1 and 1 μM, showed an increase of reduced thiols. At 120 h, only cells that received 50 μM of RSV showed an increase of reduced thiols (Fig. 4a).
The redox status of protein and non-protein compounds and the lipid peroxidation. GRX cells were treated with 0 (control), 0.1, 1, 10 and 50 μM of RSV for 24 or 120 h. The protein or non-protein redox status was measured by the determination of these compounds’ reduced thiols, using Elmann’s reagent (a). The lipid peroxidation was measured by the determination of thiobarbituric acid reactive species (TBARS) (b). Data are expressed as mean ± SEM. (n = 4). Single asterisk indicates statistically significant differences between groups (p ≤ 0.05)
The Effects of Resveratrol on Lipid Peroxidation
Lipid peroxidation damage occurs as a consequence of ROS over-production and cell antioxidant defences failure. As such, the malondialdehyde production was quantified by the TBARS method as an index of lipid peroxidation, which is related to the cell plasma membrane damage and cell death [34]. A two-way ANOVA demonstrated that the TBARS generation was dependent on the treatment time [F(1,26) = 14.69; p ≤ 0.05] and on the RSV dose [F(3,26) = 50.34; p ≤ 0.05]. There was an interaction between time of treatment and the RSV dose [F(3,26) = 37.06; p ≤ 0.05] for the TBARS generation because 50 μM of RSV provoked a higher increase of lipid peroxidation at 24 h (Fig. 4b).
The Effects of Resveratrol on Cellular Proliferation
RSV is known to be an antiproliferative compound. We found a considerable decrease in the cell density in 50 μM-treated cells related to cytotoxicity, which may be also related to a diminished proliferation. Thus, we evaluated the RSV effects on cell proliferation. After 24 h of treatment, we observed that 50 μM of RSV promoted a decrease in the thymidine incorporation. Interestingly, in 120 h, although all groups have decreased the rate of cellular proliferation during the culture time, cells that received 50 μM of RSV continued to proliferate as indicated by the significant increase in thymidine uptake (Fig. 5a). The proliferation ratio between 120 and 24 h (Fig. 5b) and the calculation of cell population doublings (Fig. 5c) confirmed these data.
The effect of resveratrol on the GRX cell proliferation. GRX cells were treated with 0 (control), 0.1, 1, 10 and 50 μM of RSV for 24 or 120 h, and the proliferation was measured by the [3H]-thymidine incorporation assay (a). The ratio between the [3H]-thimidine uptake at 120 and 24 h indicated that GRX cells treated with 50 μM of RSV remain proliferative (b). The calculation of the rate of population doublings corroborated these data (c). Data are expressed as mean ± SEM. (n = 4). Single asterisk indicates statistically significant differences between the 50 μM of RSV-treated group and the other groups (p ≤ 0.05)
Discussion
Molecular oxygen and its reactive derivatives play an important role in several metabolic processes of aerobic organisms. Nevertheless, they are paradoxically also related to the development of several diseases, including liver fibrosis [34]. RSV is well known because of its favourable biological effects that involve its chemopreventive and antioxidant capacity; however, recent studies have demonstrated that RSV may behave as a pro-oxidising agent [3].
The GRX cells correspond to the first cell line representing activated HSC [12]. Several studies suggest oxidative stress to be one of the factors that induce liver fibrosis through HSC activation [10, 35]. In this context, RSV can interfere in the molecular mechanisms of HSC that regulate phenotypical modulation, as well as liver fibrosis development [9, 35]. On the other hand, RSV has been previously shown to trigger apoptosis [8], which is well accepted as liver fibrosis resolution [10]. In GRX cells, treatment with small doses of RSV (0.1–1 μM) resulted in growth inhibition [7]. In this work, we aimed to investigate if this cell cycle arrest effect of RSV on GRX cells is accompanied by ROS production. As RSV has been described as a cytotoxic molecule at high doses and depending on the time of exposure, we also evaluate the viability and proliferation of GRX cells under treatment with crescent doses (0.1–50 μM) for 24 and 120 h.
In our experimental model, all results regarding viability were consistent with a decrease of living cells in response to the treatment with 50 μM of RSV. Interestingly, although our two RSV treatment times resulted in increased amounts of TBARS in the groups that received 50 μM, it should be noted that at 24 h, the lipid peroxidation was about three times higher than at 120 h. It has been suggested that lipid peroxidation might proceed in the cells’ nuclear membranes close to chromosomes. The loss in the nuclear membranes integrity may make the circumstance suitable for oxygen radicals to attack chromatin and DNA. In this way, RS induce cell death by apoptosis, also providing lipid peroxidation and DNA damage. Furthermore, the increase in lipid peroxidation is also associated with the rupture of the external mitochondrial membrane and consequently, the activation of necrosis [36–39]. Considering the possible role of lipid peroxidation towards the induction of cell death, the diminished level of TBARS found in the 50 μM RSV group treated for 120 h could be directly related to the decrease in the percentage of unviable cells, thus indicating a lesser cytotoxic effect in these cells.
The imbalance between the RS production and cellular antioxidant defences may lead to lipid peroxidation and cytotoxicity, which are related to the cell damage by oxidative stress and cell death [34, 36, 37]. Indeed, the apoptotic intrinsic pathway is often activated in response to cell stress or damage due to the exposure to cytotoxic drugs such as RSV. This situation results in mitochondria dysfunction, leading to an excessive production of RS that may first damage the organelles’ membranes, which leads to the cytochrome c release into cell cytosol resulting in the caspases activation [40–43]. Interestingly, some studies also reported that the sensitivity of cells to apoptosis induction is increased upon decreasing the intracellular concentration of superoxide (O2 −), which results in the cytosol acidification [44–46]. Also, the decreased levels of intracellular O2 − could be related to an increase of hydrogen peroxide (H2O2) through SOD activity or to an increase of peroxynitrite (ONOO−) through its reaction with nitric oxide. Consequently, H2O2 can be an important source for •OH formation via the Fenton reaction or can oxidise cardiolipin, a structural mitochondrial lipid, contributing to the release of cytocrome c and the initiation of mitochondrial-mediated apoptosis. Likewise, the excessive ONOO− levels in mitochondria can also impair the MnSOD function, leading to this enzyme activity decrease [47–49].
Our results regarding the oxidative status of GRX showed that RSV triggers dose- and time-dependent increase of RS and mainly alters SOD activity. However, the two times of treatment with RSV triggered a paradoxical effect in this enzyme activity. Indeed, the imbalance between the increased RS production and the diminished SOD activity found at 24 h of treatment could be harmful to cells since that excessive O2 − can be an important source of ONOO− through reacting with nitric oxide [34]. On the other hand, another plausible explanation for this situation is that decreasing SOD activity could be owed to the consumption of this enzyme in converting O2 − to H2O2. In this context, the increased production of H2O2 along with the possible production of ONOO− in GRX could lead to a diminished level of O2 −, contributing to the decrease of SOD activity and to the increase of oxidised DCF. Interestingly, our attention was drawn to the fact that, although not statistically different, the visible decrease in the CAT activity induced by the highest dose of RSV can contribute to the high cytotoxicity found in this treated group at 24 h of treatment. On the other hand, in spite of the diminished SOD activity found in cells treated with 1 and 10 μM of RSV, the unchanged CAT activity in these groups may be important for protecting cells through regulating the possible increase on the levels of H2O2.
The increase of RS production in all cells treated with RSV for 120 h was continuous. However, in spite of the time-dependent decrease of the SOD activity in all groups including control, we found that RSV significantly prevents this decrease. In this sense, the smaller decrease in this enzyme activity, which was more significant in the 50 μM-treated cells, could be related to an increase on the O2 − production along the 120 h of treatment and could be an important cell defence mechanism, contributing to a lower cell damage in the long-term treatment. Interestingly, treatment with 0.1–10 μM of RSV did not change CAT activity, and this fact may also be important for regulating the levels of intracellular H2O2. However, the highest dose of RSV decreased the CAT activity. In this sense, the SOD/CAT ratio has also been referred to as an important factor in the establishment of the redox state of cells. Furthermore, the deleterious consequences of the overproduction or excessive activity of SOD were already reported [48]. Since we discovered an imbalance favouring SOD activity in relation to CAT activity in the cells treated with 50 μM RSV, we speculate that this situation could also be related to a possible increase of H2O2 in this group.
Thiol-based redox couples are important compounds for regulating developmental events and are closely linked to changes in the intracellular redox potential. Among these, glutathione (GSH) is the most prevalent cellular thiol that plays an essential role in preserving a reduced intracellular environment, and thus guarding cells against oxidative injury. Indeed, glutathione mostly exists in its reduced form and can be oxidised by H2O2 in a reaction catalyzed by glutathione peroxidase, producing glutathione disulphide (GSSH) and water. Furthermore, GSH can scavenge reactive nitrogen species such as peroxynitrite (ONOO−) with or without the help of glutathione peroxidase [50–53]. Interestingly, some studies reported that RSV can trigger an increase of GSH levels and an increase in the activity of glutathione reductase and glutathione peroxidise [54–56]. Curiously, our attention was drawn to the fact that RSV did not induce oxidation of thiols compounds at both treatment times. In contrast, cells treated with the lower doses of RSV for 24 h showed an increase of reduced thiols, and this fact suggests a cellular protective effect against the intracellular pro-oxidant environment induced by RSV. Interestingly, there was an increase of reduced thiols in the cells treated with 50 μM of RSV for 120 h. This situation could be important to these cells for counterattacking the more prominent pro-oxidant effects of this dose of RSV contributing to the balance between RS production and cellular antioxidant defences. In this way, the increase in the reduced intracellular thiol content could compensate the decrease in the CAT activity and could contribute to the reduction of lipid peroxidation and to the reduction of the percentage of unviable cells on this group at this treatment time.
As expected, treatment for 24 h with 50 μM RSV resulted in decreased [3H] thymidine incorporation when compared to the other groups. Paradoxically, we observed at 120 h of treatment an increase in the [3H] thymidine incorporation. The calculation of the population doubling revealed that the surviving cells of the first 24 h of treatment continued to proliferate. Interestingly, lipid peroxidation is very low or totally missing in quickly proliferating tissues such as tumours. This fact suggests that an increase of lipid peroxidation may contribute to the cell proliferation decrease [36]. Thus, these results regarding the GRX proliferation could be interrelated to that found in the TBARS assay, since the treatment with 50 μM of RSV triggered a greater lipid peroxidation at 24 h that was significantly attenuated at 120 h. In this way, the decreasing cell number showed by MTT, sulphorhodamine B, and live-trypan cell counting results found at 120 h could represent the cells that survived the significant cytotoxicity of the first 24 h of treatment, remaining viable and proliferative. Beside this, the smaller confluence after 24 h of treatment with 50 μM of RSV could also be a reason for the continuous proliferation until 120 h of treatment.
The antioxidant potential of RSV has been widely discussed because of its RS-scavenging capacity [3, 57]. However, another plausible hypothesis can be the RSV’s capacity to induce a series of signals leading to an upregulation of the cell antioxidant defence systems. Recent evidence suggests that RSV could act as a signalling molecule within tissues and cells in modulating the expression of genes and proteins through the activation of redox-sensitive intracellular pathways. In this regard, the cellular tolerance to the oxidative environment could be related to some gene expression alterations as well as to an increase in the synthesis and action of antioxidant defence systems that could result in cell survival and adaptation [58–60]. On the other hand, it was already discussed that there is an interesting correlation among the pro-oxidant activities and cytotoxicity of dietary polyphenols, such as RSV. Furthermore, it has become a consensus that every antioxidant is in fact a redox agent and thus might become a pro-oxidant, accelerating lipid peroxidation and/or inducing DNA damage under special conditions. In this way, it has been proposed that such pro-oxidant action could be an important action mechanism of RSV anti-cancer and apoptotic-inducing properties [3].
The current literature shows numerous targets for RSV; thus, the molecular actions of this phytoalexin have not yet been unequivocally determined. In this way, the possible capacity of RSV in modulating different pathways can result in several and opposite biological effects, depending on its concentration or treatment time [61, 62]. In this sense, it was already discussed that three distinct cellular responses appear to result from exposure to polyphenols such as RSV, with each response dependent upon the concentration and pro-oxidant nature of these polyphenols: (a) a mild exposure causes mild oxidative stress and thereby ignites cellular antioxidant defence systems; (b) an intermediate to high exposure gradually overwhelms the antioxidant defence systems and induces apoptotic cell death; and (c) a very high exposure quickly overwhelms the cellular antioxidant defences and causes oxidative damage leading to cell death by necrosis [63]. Furthermore, these controversial effects of RSV treatment reported by several studies were recently related to the hormesis concept [61, 64, 65], which refers to a favourable biological response to low and harmless doses of some chemical compounds that could initiate an adaptive stress response that renders cells/organism resistant against high (and normally harmful) doses of the same agent, allowing the stressed cells to avoid death or damage [61, 66].
The treatment with antioxidant molecules could be interesting as a preventative strategy for liver fibrosis development because the oxidative balance plays an important role in HSC activation [10]. Despite the wide discussion about the antioxidant properties of RSV, it was already reported that RSV can lead to DNA damage as well as a reversible or irreversible interruption of the cell cycle mediated by a pro-oxidant effect [60]. Along with the possibility that the pro-oxidant effect of RSV can trigger a reversible interruption of the cell cycle, our attention was drawn to the paradoxical effect of this phytoalexin on SOD activity. Taking into account that RSV could induce apoptosis and the role of intracellular O2 − towards this form of cell death [44, 45], we speculate that the intracellular concentration of O2 − could interfere in SOD activity. In this way, it is possible that even low doses of RSV (from 1 μM) can be more harmful to cells under 24 h of treatment since this condition can favour apoptosis. However, although RSV also triggers a pro-oxidant effect in cells treated for 120 h, the RS production at this treatment time could be more balanced and could be more effectively counterattacked by cellular antioxidant defences; thus, these facts could be important for the cell resistance against oxidative stress.
In summary, our findings showed that even low doses of RSV triggered a pro-oxidant effect in GRX cells and this fact may be related to the arrest cycle found in our previous work. However, although a dose-dependent pro-oxidative effect of RSV leading to oxidative stress in the cells treated with 50 μM was shown, the less expressive cytotoxicity found in this group at 120 h of treatment could suggest that the surviving cells seemed to be more resistant to the RSV-induced damage, which seemed to be attenuated with time of treatment. Nevertheless, more studies are necessary to better understand these paradoxical effects of RSV regarding the SOD activity and the time-dependent cell damage reduction. In the same way, the need for elucidating the additional targets of RSV in these cells, including other antioxidant defences, cell death pathways or cell pro-survival mechanisms, has become evident to evaluate the real benefit of this phytoalexin towards the prevention of HSC activation or liver fibrosis resolution through an effective induction of apoptosis in the activated HSC.
Abbreviations
- CAT:
-
Catalase
- ECM:
-
Extracellular matrix
- HSC:
-
Hepatic stellate cells
- ROS:
-
Reactive oxygen species
- RSV:
-
Resveratrol
- SOD:
-
Superoxide dismutase
References
Signorelli, P., & Ghidoni, R. (2005). Resveratrol as an anticancer nutrient: molecular basis, open questions and promises. Journal of Nutritional Biochemistry, 16(8), 449–466.
Wenzel, E., & Somoza, V. (2005). Metabolism and bioavailability of trans-resveratrol. Molecular Nutrition & Food Research, 49(5), 472–481.
De la Lastra, C. A., & Villegas, I. (2007). Resveratrol as an antioxidant and pro-oxidant agent: mechanisms and clinical implications. Biochemical Society Transactions, 35(Pt 5), 1156–1160.
Quincozes-Santos, A., Andreazza, A. C., Goncalves, C. A., & Gottfried, C. (2010). Actions of redox-active compound resveratrol under hydrogen peroxide insult in C6 astroglial cells. Toxicology in Vitro, 24(3), 916–920.
Berardi, V., Ricci, F., Castelli, M., Galati, G., & Risuleo, G. (2009). Resveratrol exhibits a strong cytotoxic activity in cultured cells and has an antiviral action against polyomavirus: Potential clinical use. Journal of Experimental & Clinical Cancer Research, 28, 96.
Joe, A. K., Liu, H., Suzui, M., Vural, M. E., Xiao, D., & Weinstein, I. B. (2002). Resveratrol induces growth inhibition, S-phase arrest, apoptosis, and changes in biomarker expression in several human cancer cell lines. Clinical Cancer Research, 8(3), 893–903.
Souza, I. C., Martins, L. A., Coelho, B. P., Grivicich, I., Guaragna, R. M., Gottfried, C., et al. (2008). Resveratrol inhibits cell growth by inducing cell cycle arrest in activated hepatic stellate cells. Molecular and Cellular Biochemistry, 315(1–2), 1–7.
Juan, M. E., Wenzel, U., Daniel, H., & Planas, J. M. (2008). Resveratrol induces apoptosis through ROS-dependent mitochondria pathway in HT-29 human colorectal carcinoma cells. Journal of Agriculture and Food Chemistry, 56(12), 4813–4818.
Lotersztajn, S., Julien, B., Teixeira-Clerc, F., Grenard, P., & Mallat, A. (2005). Hepatic fibrosis: Molecular mechanisms and drug targets. Annual Review of Pharmacology and Toxicology, 45, 605–628.
Friedman, S. L. (2008). Mechanisms of hepatic fibrogenesis. Gastroenterology, 134(6), 1655–1669.
Borojevic, R., Monteiro, A. N., Vinhas, S. A., Domont, G. B., Mourao, P. A., Emonard, H., et al. (1985). Establishment of a continuous cell line from fibrotic schistosomal granulomas in mice livers. In Vitro Cellular & Developmental Biology, 21(7), 382–390.
Geerts, A. (2001). History, heterogeneity, developmental biology, and functions of quiescent hepatic stellate cells. Seminars in Liver Disease, 21(3), 311–335.
Guma, F. C. R., Mello, T. G., Mermelstein, C. S., Fortuna, V. A., Wofchuk, S. T., Gottfried, C., et al. (2001). Intermediate filaments modulation in an in vitro model of the hepatic stellate cell activation or conversion into the lipocyte phenotype. Biochemistry and Cell Biology, 79(4), 409–417.
Borojevic, R., Guaragna, R. M., Margis, R., & Dutra, H. S. (1990). In vitro induction of the fat-storing phenotype in a liver connective tissue cell line-GRX. In Vitro Cellular & Developmental Biology, 26(4), 361–368.
Martucci, R. B., Ziulkoski, A. L., Fortuna, V. A., Guaragna, R. M., Guma, F. C., Trugo, L. C., et al. (2004). Beta-carotene storage, conversion to retinoic acid, and induction of the lipocyte phenotype in hepatic stellate cells. Journal of Cellular Biochemistry, 92(2), 414–423.
Bitencourt, S., de Mesquita, F. C., Caberlon, E., da Silva, G. V., Basso, B. S., Ferreira, G. A., et al. (2012). Capsaicin induces de-differentiation of activated hepatic stellate cell. Biochemistry and Cell Biology, 90(6), 683–690.
Guimaraes, E. L., Franceschi, M. F., Grivicich, I., Dal-Pizzol, F., Moreira, J. C., Guaragna, R. M., et al. (2006). Relationship between oxidative stress levels and activation state on a hepatic stellate cell line. Liver International, 26(4), 477–485.
Hansen, M. B., Nielsen, S. E., & Berg, K. (1989). Re-examination and further development of a precise and rapid dye method for measuring cell growth/cell kill. Journal of Immunological Methods, 119(2), 203–210.
Skehan, P., Storeng, R., Scudiero, D., Monks, A., et al. (1990). New colorimetric cytotoxicity assay for anticancer-drug screening. Journal of the National Cancer Institute, 82(13), 1107–1112.
Strober, W (2001) Trypan blue exclusion test of cell viability. Current Protocols in Immunology. Appendix 3: Appendix 3B.
Halliwell, B., & Whiteman, M. (2004). Measuring reactive species and oxidative damage in vivo and in cell culture: How should you do it and what do the results mean? British Journal of Pharmacology, 142(2), 231–255.
Peterson, G. L. (1979). Review of the Folin phenol protein quantitation method of Lowry, Rosebrough, Farr and Randall. Analytical Biochemistry, 100(2), 201–220.
Misra, H. P., & Fridovich, I. (1972). The role of superoxide anion in the autoxidation of epinephrine and a simple assay for superoxide dismutase. Journal of Biological Chemistry, 247(10), 3170–3175.
Aebi, H. (1984). Catalase in vitro. Methods in Enzymology, 105, 121–126.
Simpson, RJ (2008) Estimation of free thiols and disulfide bonds using Ellman’s reagent. CSH Protocols: pdb.prot4699.
Draper, H. H., & Hadley, M. (1990). Malondialdehyde determination as index of lipid peroxidation. Methods in Enzymology, 186, 421–431.
Kawada, N., Kuroki, T., Kobayashi, K., Inoue, M., & Kaneda, K. (1996). Inhibition of myofibroblastic transformation of cultured rat hepatic stellate cells by methylxanthines and dibutyryl cAMP. Digestive Diseases and Sciences, 41(5), 1022–1029.
Lorge, E., Hayashi, M., Albertini, S., & Kirkland, D. (2008). Comparison of different methods for an accurate assessment of cytotoxicity in the in vitro micronucleus test. I. Theoretical aspects. Mutation Research, 655(1–2), 1–3.
Li, M., Zhao, L., Liu, J., Liu, A. L., Zeng, W. S., Luo, S. Q., et al. (2009). Hydrogen peroxide induces G2 cell cycle arrest and inhibits cell proliferation in osteoblasts. Anatomical Record (Hoboken), 292(8), 1107–1113.
Chua, P. J., Yip, G. W., & Bay, B. H. (2009). Cell cycle arrest induced by hydrogen peroxide is associated with modulation of oxidative stress related genes in breast cancer cells. Experimental Biology and Medicine (Maywood), 234(9), 1086–1094.
Gong, C., Tao, G., Yang, L., Liu, J., He, H., & Zhuang, Z. (2012). The role of reactive oxygen species in silicon dioxide nanoparticle-induced cytotoxicity and DNA damage in HaCaT cells. Molecular Biology Reports, 39(4), 4915–4925.
Iciek, M., Chwatko, G., Lorenc-Koci, E., Bald, E., & Wlodek, L. (2004). Plasma levels of total, free and protein bound thiols as well as sulfane sulfur in different age groups of rats. Acta Biochimica Polonica, 51(3), 815–824.
Olas, B., Wachowicz, B., Bald, E., & Glowacki, R. (2004). The protective effects of resveratrol against changes in blood platelet thiols induced by platinum compounds. Journal of Physiology and Pharmacology, 55(2), 467–476.
Halliwell, B & Gutteridge, JMC (Eds.) (2000) Free radicals in biology and medicine 3rd ed. (p 936). Clarendon: Oxford.
Friedman, S. L. (2008). Hepatic stellate cells: protean, multifunctional, and enigmatic cells of the liver. Physiological Reviews, 88(1), 125–172.
Barrera, G., Pizzimenti, S., & Dianzani, M. U. (2008). Lipid peroxidation: control of cell proliferation, cell differentiation and cell death. Molecular Aspects of Medicine, 29(1–2), 1–8.
Baines, C. P., Kaiser, R. A., Purcell, N. H., Blair, N. S., et al. (2005). Loss of cyclophilin D reveals a critical role for mitochondrial permeability transition in cell death. Nature, 434(7033), 658–662.
Nakagawa, T., Shimizu, S., Watanabe, T., Yamaguchi, O., Otsu, K., Yamagata, H., et al. (2005). Cyclophilin D-dependent mitochondrial permeability transition regulates some necrotic but not apoptotic cell death. Nature, 434(7033), 652–658.
Barrera, G. (2012). Oxidative stress and lipid peroxidation products in cancer progression and therapy. ISRN Oncology, 2012, 137289.
Sheridan, C., & Martin, S. J. (2010). Mitochondrial fission/fusion dynamics and apoptosis. Mitochondrion, 10(6), 640–648.
Kubli, D. A., & Gustafsson, A. B. (2012). Mitochondria and mitophagy: The yin and yang of cell death control. Circulation Research, 111(9), 1208–1221.
Gottlieb, R. A., & Carreira, R. S. (2010). Autophagy in health and disease. 5. Mitophagy as a way of life. American Journal of Physiology. Cell Physiology, 299(2), C203–C210.
Kroemer, G., Galluzzi, L., & Brenner, C. (2007). Mitochondrial membrane permeabilization in cell death. Physiological Reviews, 87(1), 99–163.
Pervaiz, S., & Clement, M. V. (2002). A permissive apoptotic environment: function of a decrease in intracellular superoxide anion and cytosolic acidification. Biochemical and Biophysical Research Communications, 290(4), 1145–1150.
Teo, I. T., Tang, J. C., Chui, C. H., Cheng, G. Y., et al. (2004). Superoxide anion is involved in the early apoptosis mediated by Gleditsia sinensis fruit extract. International Journal of Molecular Medicine, 13(6), 909–913.
Ahmad, K. A., Clement, M. V., Hanif, I. M., & Pervaiz, S. (2004). Resveratrol inhibits drug-induced apoptosis in human leukemia cells by creating an intracellular milieu nonpermissive for death execution. Cancer Research, 64(4), 1452–1459.
Figueira, T. R., Barros, M. H., Camargo, A. A., Castilho, R. F., Ferreira, J. C., Kowaltowski, A. J., et al. (2013). Mitochondria as a source of reactive oxygen and nitrogen species: From molecular mechanisms to human health. Antioxidants & Redox Signaling, 18(16), 2029–2074.
Liochev, S. I., & Fridovich, I. (2007). The effects of superoxide dismutase on H2O2 formation. Free Radical Biology and Medicine, 42(10), 1465–1469.
De Oliveira, M. R., de Bittencourt Pasquali, M. A., Silvestrin, R. B., Mello, E. S. T., & Moreira, J. C. (2007). Vitamin A supplementation induces a pro-oxidative state in the striatum and impairs locomotory and exploratory activity of adult rats. Brain Research, 1169, 112–119.
Harris, C., & Hansen, J. M. (2012). Oxidative stress, thiols, and redox profiles. Methods in Molecular Biology, 889, 325–346.
Yuan, L., & Kaplowitz, N. (2009). Glutathione in liver diseases and hepatotoxicity. Molecular Aspects of Medicine, 30(1–2), 29–41.
Forman, H. J., Zhang, H., & Rinna, A. (2009). Glutathione: overview of its protective roles, measurement, and biosynthesis. Molecular Aspects of Medicine, 30(1–2), 1–12.
Biswas, S., Chida, A. S., & Rahman, I. (2006). Redox modifications of protein-thiols: Emerging roles in cell signalling. Biochemical Pharmacology, 71(5), 551–564.
Hassan-Khabbar, S., Cottart, C. H., Wendum, D., Vibert, F., Clot, J. P., Savouret, J. F., et al. (2008). Postischemic treatment by trans-resveratrol in rat liver ischemia-reperfusion: a possible strategy in liver surgery. Liver Transplantation, 14(4), 451–459.
Delmas, D., Lancon, A., Colin, D., Jannin, B., & Latruffe, N. (2006). Resveratrol as a chemopreventive agent: a promising molecule for fighting cancer. Current Drug Targets, 7(4), 423–442.
Kode, A., Rajendrasozhan, S., Caito, S., Yang, S. R., Megson, I. L., & Rahman, I. (2008). Resveratrol induces glutathione synthesis by activation of Nrf2 and protects against cigarette smoke-mediated oxidative stress in human lung epithelial cells. American Journal of Physiology. Lung Cellular and Molecular Physiology, 294(3), L478–L488.
Pervaiz, S., & Holme, A. L. (2009). Resveratrol: Its biologic targets and functional activity. Antioxidants & Redox Signaling, 11(11), 2851–2897.
Robb, E. L., Page, M. M., Wiens, B. E., & Stuart, J. A. (2008). Molecular mechanisms of oxidative stress resistance induced by resveratrol: Specific and progressive induction of MnSOD. Biochemical and Biophysical Research Communications, 367(2), 406–412.
Robb, E. L., Winkelmolen, L., Visanji, N., Brotchie, J., & Stuart, J. A. (2008). Dietary resveratrol administration increases MnSOD expression and activity in mouse brain. Biochemical and Biophysical Research Communications, 372(1), 254–259.
Ruweler, M., Gulden, M., Maser, E., Murias, M., & Seibert, H. (2009). Cytotoxic, cytoprotective and antioxidant activities of resveratrol and analogues in C6 astroglioma cells in vitro. Chemico-Biological Interactions, 182(2–3), 128–135.
Calabrese, E. J., Mattson, M. P., & Calabrese, V. (2010). Resveratrol commonly displays hormesis: Occurrence and biomedical significance. Human and Experimental Toxicology, 29(12), 980–1015.
Pirola, L., & Frojdo, S. (2008). Resveratrol: One molecule, many targets. IUBMB Life, 60(5), 323–332.
Babich, H., Schuck, A. G., Weisburg, J. H., & Zuckerbraun, H. L. (2011). Research strategies in the study of the pro-oxidant nature of polyphenol nutraceuticals. Journal of Toxicology, 2011, 467305.
Juhasz, B., Mukherjee, S., & Das, D. K. (2010). Hormetic response of resveratrol against cardioprotection. Experimental & Clinical Cardiology, 15(4), e134–e138.
Speciale, A., Chirafisi, J., Saija, A., & Cimino, F. (2011). Nutritional antioxidants and adaptive cell responses: An update. Current Molecular Medicine, 11(9), 770–789.
Martins, I., Galluzzi, L., & Kroemer, G. (2011). Hormesis, cell death and aging. Aging (Albany NY), 3(9), 821–828.
Acknowledgments
L.A.M Martins is the recipient of a fellowship from CAPES (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior—Brazil). F.C.R. Guma, J.C.F. Moreira and R. Borojevic are recipients of research fellowships from CNPq. This work was also supported by CNPq, FAPERJ, FAPERGS and PROPESQ-UFRGS.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Martins, L.A.M., Coelho, B.P., Behr, G. et al. Resveratrol Induces Pro-oxidant Effects and Time-Dependent Resistance to Cytotoxicity in Activated Hepatic Stellate Cells. Cell Biochem Biophys 68, 247–257 (2014). https://doi.org/10.1007/s12013-013-9703-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-013-9703-8