Abstract
The phytoalexin Resveratrol (3,5,4′-trihydroxystilbene; RSV) has been related to numerous beneficial effects on health by its cytoprotection and chemoprevention activities. Liver fibrosis is characterized by the extracellular matrix accumulation after hepatic injury and can lead to cirrhosis. Hepatic stellate cells (HSC) play a crucial role during fibrogenesis and liver wound healing by changing their quiescent phenotype to an activated phenotype for protecting healthy areas from damaged areas. Strategies on promoting the activated HSC death, the quiescence return or the cellular activation stimuli decrease play an important role on reducing liver fibrosis. Here, we evaluated the RSV effects on some markers of activation in GRX, an HSC model. We further evaluated the RSV influence in the ability of GRX on releasing inflammatory mediators. RSV at 1 and 10 µM did not alter the protein content of α-SMA, collagen I and GFAP; but 50 µM increased the content of these activation-related proteins. Also, RSV did not change the myofibroblast-like morphology of GRX. Interestingly, RSV at 10 and 50 µM decreased the GRX migration and collagen-I gel contraction. Finally, we showed that RSV triggered the increase in the TNF-α and IL-10 content in culture media of GRX while the opposite occurred for the IL-6 content. Altogether, these results suggested that RSV did not decrease the activation state of GRX and oppositely, triggered a pro-activation effect at the 50 µM concentration. However, despite the increase of TNF- α in culture media, these results on IL-6 and IL-10 secretion were in accordance with the anti-inflammatory role of RSV in our model.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Resveratrol (3,5,4′-trihydroxystilbene; RSV) is a phytoalexin produced by several plant species, such as peanuts and grapes, in response to pathogenic infection and environmental stresses. This molecule is present at relevant concentrations in red wine and has been related to numerous beneficial effects on health by its cytoprotection and chemoprevention activities, which has been largely associated with its anti-inflammatory and anti-oxidant effects. Paradoxically, RSV can also exert cytotoxicity through inducing cell death and cell growth inhibition, two positive effects for treating several pathological conditions such as cancer [1, 2].
Liver fibrosis is a dynamic process characterized by the accumulation of extracellular matrix resulting from hepatic injury, including those caused by a viral infection, alcoholic liver disease (ALD), non-alcoholic steatohepatitis (NASH) and hepatic steatosis. It is a consensus that liver fibrogenesis can be reversed if the cause of injury is ceased. However, the unchecked chronic liver injury and fibrogenesis can lead to cirrhosis, which compromises the hepatic architecture leading to abnormal blood flow and eventually to portal hypertension. In addition, liver cirrhosis may lead to the onset of complications, such as hepatic encephalopathy and variceal haemorrhage, which may increase the chances of hepatocellular carcinoma (HCC) development and, thus, the mortality risk [3, 4].
Hepatic stellate cells (HSC) are known to store lipid droplets enriched in retinyl ester in their cytoplasm, a condition that characterizes their quiescent phenotype. As one of their physiological features, HSC can differentiate into an activated phenotype in response to paracrine stimulation from damaged hepatocytes after liver injury. At this condition, HSC loses their lipid droplets and becomes fibrogenic myofibroblast-like cells, playing an important role in liver wound healing through protecting healthy areas from damaged areas. Nonetheless, continuous damage to the liver results in a chronic inflammatory response in which hepatic environment may not recover its homeostatic balance. In this context, increased production/activity of cytokines may be critical for both autocrine and paracrine perpetuation of HSC activation, which contributes to the excessive extracellular matrix accumulation that leads to liver fibrosis. In this way, strategies that promote the activated HSC death, the quiescence return or the cellular activation stimuli decrease play an important role on treating chronic liver injuries, focusing in the liver fibrosis reduction [5,6,7].
Along the past years, our research group has been studying the effects of RSV treatment in the murine cell line GRX, an activated HSC model [8]. GRX cells have been an excellent tool for studying the extrinsic and intrinsic factors that could trigger or prevent liver fibrosis since these cells can be induced to display the HSC quiescent-like or a more activated-like phenotype [9,10,11,12,13]. We already found that RSV treatment (0.1–50 µM) compromised the GRX cell viability through inhibiting cell cycle at the S-phase, impaired mitochondria and induced apoptosis, especially in the cell group that received the highest dose, where the cell population was drastically reduced. However, it was interesting that these effects were attenuated by the concomitant induction of mitochondrial biogenesis and autophagy, two survival mechanism against cellular environmental toxicity, which culminated in the GRX resistance to the cytotoxic effects of RSV [14,15,16]. Further, we found that 0.1 μM of RSV was not able to restore the GRX capacity of storing lipid droplets. On the contrary, our results suggested that RSV could play a SIRT1-mediated lipolysis in GRX stimulated to store lipid droplets by Retinol treatment or by PPARγ super expression [17].
RSV treatment showed positive effects on compromising viability or reducing the number of activated HSC especially at the highest concentration (50 μM). On the other hand, RSV compromised the ability of GRX on storing lipid droplets, a characteristic of quiescent HSC. Here, we seek for evaluating the effects of RSV towards HSC activation by measuring some molecular markers and cell migration after wound induction in GRX cell culture. We further evaluated the effects of RSV in the HSC ability on releasing TNF-α, IL-6 and IL-10 in the culture media, considering the importance of these cytokines during liver fibrogenesis.
Material and methods
Cell culture
The GRX cell line was obtained from the Cell Bank of Rio de Janeiro (HUCFF, UFRJ, RJ). For most experiments, 3 × 104/cm2 cells were seeded in 24-well culture plates (Nunc, Roskilde, Denmark). For cell migration evaluation, 1.5 × 104/cm2 cells were seeded in 96-well culture plates (Nunc, Roskilde, Denmark). During culture, cells were maintained in Dulbecco’s Modified Eagle’s Medium (DMEM, Invitrogen, Carlsbad, CA, USA) supplemented with 5% foetal bovine serum (Cultilab, Campinas, SP, Brazil) and 2 g/L HEPES buffer (pH 7.4) in a humidified atmosphere containing 5% CO2 at 37 °C.
Resveratrol treatment
Resveratrol (Sigma Inc., St. Louis, MO, USA) was dissolved in 20 µL of ethanol (Merck, Darmstadt, Germany) to a stock concentration of 100 mM and sequentially diluted in DMEM to a final concentration of 1, 10 and 50 µM just before use. After reaching confluence, cells were treated for 24 h. Vehicle-treated cells were considered experimental control.
Analysis of HSC activation markers by flow cytometry
The cellular protein content for glial fibrillary acidic protein (GFAP), collagen I and smooth muscle actin-α (SMA-α) in GRX treated with RSV was measured by flow cytometry. Briefly, after 24-h treatment, cells were harvest by trypsin/EDTA (Sigma Inc.) and fixed with 4% paraformaldehyde in phosphate buffer saline (PBS) for 15 min. Sequentially, cells were overnight incubated with the primary antibodies (GFAP, n.34001, from Cell Signalling, Danvers, MA, USA; collagen I, n.8784, from Santa Cruz Biotechnology, Dallas, TX, USA; SMA-α, n.A5228, from Sigma Inc.) diluted in PBS with 5% of albumin (1:500). Then, cells were incubated with adequate secondary antibodies (1:1000, diluted in PBS with 5% of albumin) for 2 h at room temperature: GFAP and SMA-α-labelled cells were exposed to anti-mouse AlexaFluor 488 (n.A11001, from Invitrogen) while collagen I-labelled cells were exposed to anti-goat AlexaFluor 647 (n.A21447, from Invitrogen). Cells incubated only with respective fluorescence secondary antibodies were used as negative controls. A total of 20,000 events were acquired by FACSCalibur flow cytometer (BD Biosciences, San Jose, CA, USA) at FL-1 (green fluorescence) and FL-4 (red fluorescence) channels. All data analyses were performed with FCS Express 4 software (De Novo, Software, Ontario, Canada). Results were expressed as fluorescence units [Control = 1].
Analysis of HSC morphology by confocal microscopy
For analysing the cytoskeleton morphology, GRX was stained with tetramethyl-rhodamine isothiocyanate–phalloidin (Invitrogen), which specifically binds to F-actin with high affinity. Briefly, cells were cultured under coverslip, fixed in 4% paraformaldehyde for 15 min at 4 °C and permeabilized with 0.1% Triton X-100 in PBS for 5 min at room temperature. Filamentous actin was stained in accordance to the manufacturer's instructions. Images were collected using Olympus FV1000 laser‐scanning confocal microscope. Ten single confocal sections of 0.7 μM were taken parallel to the bottom plates (xy sections) with a × 60 (numeric aperture 1.35) oil-immersion objective (Olympus, U plan-super apochromat, UPLSAPO60XO). Images from six random fields were acquired and deconvolved using the interactive 3D plugin of ImageJ software (https://rsb.info.nih.gov/ij).
Analysis of HSC-induced contraction of collagen I gel
In order to evaluate the RSV effects in the HSC ability of contracting ECM, a characteristic of activated cells, a ready-to-use storable gel of collagen I was prepared after extracting it from rat tail tendon as previously described [18]. Animals were obtained from the Center for Experimental Biological Models at Pontifícia Universidade Católica do Rio Grande do Sul (PUCRS) and kept in a controlled temperature environment (24 ± 2 °C), light/dark cycle of 12 h, with free access to water and food. The experimental protocol was approved by the Ethics Research Committee of PUCRS.
Collagen I gels (constituted by 125 μl of 4 × DMEM and 125 μl of 4 mg/mL Rat Tail Tendon extracted collagen I) were impregnated with 105 cells resuspended in 250 μl of PBS and added into a 24-well plate for polymerising at 37 °C during 1 h. Then, collagen I gels and impregnated cells were detached and suspended in culture (control) and treatment (1, 10 and 50 µM of RSV) media. Images were acquired in a gel documenter (L-Pix, Loccus, Cotia, SP, Brazil) after 24 h of treatment, and the surface area for each gel was determined as percentage of well area using ImageJ software (https://rsb.info.nih.gov/ij/), a public domain Java image processing software. Cell treatment with N-acetylcysteine (NAC) at 400 μg/mL was used as a positive control [19]. Results were expressed as area of gel, considering control as 100%.
Analysis of HSC migration by in vitro scratch assay
The effect of RSV in the migration capacity of GRX was evaluated by the in vitro scratch assay as previously described [20]. Briefly, after 24-h treatment, a circular gap was created with a 200-μL pipette tip at cell-confluent monolayer. Then, 24 images for each group were acquired in the SpectraMax i3 Multi-Mode Platform (Molecular Devices, Sunnyvale, CA, USA) at 0, 6, 12 and 24 h. Wound area at the aforementioned times was measured using ImageJ software. Results were expressed as the percentage of cell migration which represents the wound area reduction (wound closure).
Analysis of HSC inflammatory release by ELISA assay
After 24-h treatment, the interleukine-6 and interleukine-10 concentrations were quantified in cell culture media using Quantikine ELISA Kit and protocol (R&D Systems, Minneapolis, MN, USA). Tumour necrosis factor-α concentration in the culture medium was determined using Sigma ELISA Kit (Sigma Inc.), accordingly to the manufacturer’s protocol. Optical density was collected in a microplate fluorimeter reader (M5, Molecular Devices, USA). For allowing a more precise estimate for the RSV effects on cytokine releasing by GRX, cell quantity had to be considered. Results were then normalized by protein content [21] at the end of RSV treatments and were expressed as pg/µg.
Statistical analysis
Data were expressed as mean ± standard deviation of the mean. Experiments were repeated at least three times (n = 3). One-way ANOVA was used to analyse the effect of RSV treatment, and Tukey post-hoc was performed. Results were considered statistically different when the p values were less than 0.05.
Results
Resveratrol induces an increase in the protein markers of activation in HSC
HSC have well-known molecular markers for activation and myofibroblast differentiation and among them, the increase in the protein content of GFAP, collagen I and SMA-α [3, 5, 22,23,24]. Thus, we sought to evaluate the content of these proteins in GRX by flow cytometry. Treatment with 1 and 10 μM of RSV did not alter the intracellular GFAP, collagen I and SMA-α protein quantity; however, 50 μM of RSV triggered an increase in the protein content of these molecular markers of activation in GRX (Fig. 1).
Resveratrol does not alter HSC cytoskeleton morphology, but the highest concentration decreases cells ability of contracting collagen I gel
The increase of cell contractibility, characterized by the F-Actin cytoskeleton rearrangement in stress fibres, is an important feature of activated HSC [25, 26]. Thus, RSV-treated cells were stained with tetramethyl-rhodamine isothiocyanate–phalloidin for evaluating cell cytoskeleton. No significant changes were observed since all groups were presented with cells with stress fibres and a myofibroblastic-like morphology with elongated cytoplasm (Fig. 2a). However, the collagen I gels containing cells treated with 50 μM of RSV were significantly less contracted (Fig. 2b).
a No significant changes were observed in GRX cytoskeleton since all-treated groups presented cells with stress fibres (white arrows) and a myofibroblastic-like morphology with elongated cytoplasm (images were pseudo-coloured in Red Hot by ImageJ; Scale bar: 10 µm); b Collagen I gels containing cells treated with RSV at 50 µM were significantly less contracted. N-acetylcysteine (400 μg/mL) was used as a positive control
Resveratrol induces a decrease in the HSC migration
The increase in the cell migration ability is also a feature of activated HSC [27]. Thus, we also evaluate GRX capacity on migrating after creating a circular gap in cultured cell at monolayer. Interestingly, after 6 and 12 h of wound creation, cells treated with 10 and 50 μM of RSV presented a decreased rate of migration. At 24 h after wound creation, only cells treated with 50 μM of RSV remained with a decreased rate of migration (Fig. 3).
Resveratrol alters the HSC capacity of releasing tumour necrosis factor-α, interleukin-6 and interleukin-10 in cellular medium
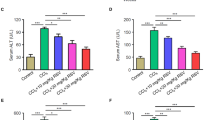
Numerous cytokines, which may be pro- or anti-fibrogenic, have been shown to play a major role in wound-healing response during liver diseases [3, 5,6,7]. Therefore, the largely discussed anti-inflammatory property RSV [1, 28,29,30] may interfere on cytokines signalling among cultured HSC. Thus, we evaluated the RSV effects in the GRX ability on releasing TNF-α, IL-6 and IL-10; three important cytokines that are involved in liver fibrogenesis [5, 22, 31, 32]. All concentrations of RSV were able to increase the release of TNF-α in culture medium by GRX (Fig. 3a) while treatment with 10 and 50 μM triggered a similar effect for IL-10 releasing (Fig. 3c). Oppositely, all concentrations of RSV triggered the decrease on IL-6 releasing by GRX in culture media (Fig. 3b).
Discussion
The phytoalexin resveratrol (RSV) has attracted a lot of researchers’ attention for being a nutraceutical compound with a large pharmacological potential for clinical treating of many diseases. In this regard, the potential health-promoting properties of RSV have been associated to its pleiotropic-like effects, which are a consequence of its interaction with a large number of signalling pathways that covers a broad range of pathologies including cancer, metabolic syndrome, cardiovascular diseases, neurodegenerative disorders, ageing and inflammation [1, 28, 33,34,35].
Understanding liver fibrosis focuses primarily on events that lead to activation and proliferation of HSC, which consists of two major phases: initiation and perpetuation. Under liver inflammatory condition, the paracrine stimuli from neighbouring cells—namely injured hepatocytes, endothelial cells, Kupffer cells and platelets—initiate HSC activation. The pathways for perpetuating the activated HSC phenotype include the acquisition of new functions such as proliferation, release of pro-inflammatory cytokines, matrix rearrangement and fibrogenesis. The HSC activation may substantially contribute for the maintenance of liver cirrhosis that can culminate in hepatocarcinoma or liver failure. Thus, the search for treating chronic liver disease, including advanced cirrhosis, shall be focusing in the liver fibrosis regression by controlling the fibrotic activity of activated HSC through inducing these cells to quiescence or apoptosis [3,4,5,6,7].
Recent studies have demonstrated the preventive and therapeutic role of RSV for many liver disorders. Among these beneficial effects, RSV was able (1) to provide liver protection against chemical, cholestatic and alcohol injury; (2) to improve glucose metabolism and lipid profile, thus decreasing liver fibrosis and steatosis; (3) to increase the survival period after liver transplantation; and (4) to decrease fat deposition, necrosis and apoptosis in hepatocytes after liver ischemia–reperfusion (I/R) injury. When focusing on HSC metabolism, previous studies had shown the RSV effects on promoting the reduction of α-SMA protein content [28, 29]. In light of the huge number of studies pointing the beneficial effects of RSV for treating numerous pathologies including liver diseases, our research group has been studying the effects of this phytoalexin in GRX cell line, seeking for evaluating its treatment effects focusing on activated HSC.
RSV was indeed cytotoxic to GRX, but these effects seemed to be dose-dependent, being attenuated along time of cell treatment. Furthermore, this phytoalexin was not able to restore the capacity of GRX cells on storing lipid droplets. Oppositely, RSV treatment promoted lipolysis in quiescent-like cells [14,15,16,17], which is an event that characterizes the early steps of HSC activation [3,4,5]. Thus, we sought to first evaluate some parameters of HSC activation in response to a 24-h treatment with RSV at 1, 10 and 50 µM. We found that RSV at lowest concentrations (1 and 10 µM) did not alter the protein content of α-SMA, collagen I and GFAP. However, treatment with 50 µM of RSV induced an increase of content for these activation-related proteins. The increase of contractibility in activated HSC is an important feature that contributes to the intrahepatic resistance and portal hypertension, which is responsible for the morbidity in liver cirrhosis. In this situation, activated HSC displays morphological changes in their cytoskeleton characterized by the presence of F-actin stress fibre [25, 26]. In this way, RSV was not able to change the myofibroblast-like morphology of GRX, which remained displaying elongated cytoplasm characterized by the presence of stress fibres. Altogether, these results suggested that RSV treatment did not decrease the activation state of GRX and, oppositely, triggered a pro-activation effect at the 50 µM concentration.
Another remarkable feature of activated HSC is their ability to migrate towards damaged areas after liver injury, a chemotactic effect that is important to wound healing and hepatic tissue remodelling. However, an increased migration of activated HSC could exacerbate the fibrotic progression, worsening organ dysfunction [3, 27]. Cells treated with 10 µM of RSV presented a decreased rate of cell migration after 6 and 12 h from wounding while this effect was observed in cells treated with 50 µM of RSV at all times of wounding evaluation. In addition, it was also notable that 50 µM of RSV apparently decreased cells ability of contracting collagen I gels. At first sight, all results regarding the RSV effects in GRX activation, contraction ability and migration were surprising and seemed to be contradictory, especially on those cells that were treated with the highest concentration. However, it is necessary to consider that RSV was cytotoxic to our model [14,15,16]. Once the HSC is activated in response to stress mediators [3,4,5], and here RSV appears to display a stressor behaviour, it seems to be a plausible hypothesis that GRX cells respond to the RSV cytotoxicity through remaining at their activation state or, in the scenario by which this phytoalexin is remarkably toxic, through increasing their activation state. Furthermore, cytotoxicity and low cell migration use to be correlated events [36,37,38], which can make sense to explain the RSV effects on impairing GRX migration regardless the fact of these cells remaining at an activated—or more activated—phenotype. In the same way, the reduction of cell population due to the cytotoxicity of RSV at 50 µM after 24-h treatment, as previously demonstrated [14], may be related to the smaller contraction of collagen I gel in this group.
Most of the new cellular functions of activated HSC are indeed sustained by an autocrine loop characterized by the enhancement of cell response to several mediators through both the upregulation of their membrane receptors and the enhancement of intracellular signalling [3,4,5]. Also, HSC-mediated inflammatory signalling may influence the function of hepatocytes and sinusoidal cells, and may favour the repair of injured tissue through promoting the restoration of hepatic homeostasis [3,4,5, 22]. Thus, we assume that the largely discussed anti-inflammatory property of RSV [1, 2, 28] would interfere on cytokines signalling mediated by HSC. Here, we showed that RSV was able to increase the release of TNF-α and IL-10 by GRX in culture media while the opposite occurred for the IL-6 releasing. Considering these results and since our model represents a restricted population of liver cells, the presence of TNF- α and IL-10 in culture media could influence the GRX itself metabolism.
Tumour necrosis factor-α (TNF-α) and interleukin-6 (IL-6) are important pro-inflammatory and pro-fibrogenic mediators that participate in the HSC activation during initiation phase. Curiously, some studies have also suggested that TNF-α can reduce liver fibrogenesis by inducing activated HSC to synthesize less collagen I during their perpetuation phase. Also, there are evidences that TNF-α mediates a pro-apoptotic pathway in which the mitochondrial potential decreases while reactive oxygen species (ROS) and caspase cascade act as downstream mediators, and this scenario is in accordance to the RSV effects on GRX, which were found in our previous studies. Similarly, IL-6 is thought to exert beneficial effects during liver chronic diseases through playing an important role for inducing the hepatocytes regeneration. These facts reveal that both TNF-α and IL-6 have, indeed, a pleiotropic function during the HSC activation process [32, 39,40,41,42,43]. Interleukin-10 (IL-10) has been regarded as one of the most important anti-inflammatory cytokines even in the presence of higher levels of pro-inflammatory cytokines [1, 2, 29, 34, 44]. Also, IL-10 may act on preventing an excessive liver fibrogenesis or an inappropriate inflammatory response through inducing activated HSC to apoptosis [45,46,47,48]. Altogether, considering that GRX is an activated HSC model, these results on the TNF- α, IL-6 and IL-10 media content may indicate an important role of RSV in our model, which may be helpful for controlling HSC activity during liver fibrosis (Fig. 4).
Several studies have demonstrated that RSV can exert contradictory effects depending on its concentration, time of treatment or model of study. Indeed, RSV studies in cell culture models have demonstrated that low concentrations of this molecule increase proliferation while high concentrations impair cell growth [1, 2, 28, 49]. Until now, we found several relevant effects on treating activated HSC with RSV (Fig. 5). However, it is relevant to point that, during liver fibrosis associated to cirrhosis, at the same time by which is expected to control the proliferation of activated HSC or to induce apoptosis or quiescence of activated HSC, the hepatocyte regeneration or survival against damage stimuli must be sought [3, 6, 7, 50]. The RSV-mediated HSC release of TNF-α and IL-10, and the decrease of IL-6 release, may influence not only HSC itself but also hepatocytes. Thus, it is undoubtedly relevant to consider the effects of RSV for other liver cells on considering this phytoalexin for treating liver fibrosis during chronic hepatic diseases and cirrhosis. In this way, more studies focusing on the HSC relationship with other liver cells, especially hepatocytes, shall be conduct for a better understanding of the RSV effects to liver as whole.
Treatment of chronic liver disease, including advanced cirrhosis, shall be focused in the liver fibrosis regression by controlling the fibrotic activity of activated HSC through inducing these cells to quiescence or apoptosis. Our previous findings showed that RSV treatment induced cell cycle arrest, cell death, and lipolysis in GRX cell line, which is an activated HSC model. Here we found that RSV at 1–10 µM did not decrease in HSC activation state; oppositely, the highest concentration induced an increase of activation markers (GFAP, collagen I, and SMA-α). However, RSV treatment decreased activated HSC migration and triggered an anti-inflammatory effect. Further studies are needed to elucidate the RSV effect on other liver cells, especially healthy or cirrhotic-injured hepatocytes
References
de la Lastra CA, Villegas I (2007) Resveratrol as an antioxidant and pro-oxidant agent: mechanisms and clinical implications. Biochem Soc Trans 35:1156–1160. https://doi.org/10.1042/BST0351156
CA Lastra de la I Villegas 2007 Resveratrol as an antioxidant and pro-oxidant agent: mechanisms and clinical implications Biochem Soc Trans 35 1156 1160 https://doi.org/10.1042/BST0351156
Signorelli P, Ghidoni R (2005) Resveratrol as an anticancer nutrient: molecular basis, open questions and promises. J Nutr Biochem 16:449–466. https://doi.org/10.1016/j.jnutbio.2005.01.017
P Signorelli R Ghidoni 2005 Resveratrol as an anticancer nutrient: molecular basis, open questions and promises J Nutr Biochem 16 449 466 https://doi.org/10.1016/j.jnutbio.2005.01.017
Tsuchida T, Friedman SL (2017) Mechanisms of hepatic stellate cell activation. Nat Rev Gastroenterol Hepatol 14:397–411. https://doi.org/10.1038/nrgastro.2017.38
T Tsuchida SL Friedman 2017 Mechanisms of hepatic stellate cell activation Nat Rev Gastroenterol Hepatol 14 397 411 https://doi.org/10.1038/nrgastro.2017.38
Puche JE, Saiman Y, Friedman SL (2013) Hepatic stellate cells and liver fibrosis. Compr Physiol 3:1473–1492. https://doi.org/10.1002/cphy.c120035
JE Puche Y Saiman SL Friedman 2013 Hepatic stellate cells and liver fibrosis Compr Physiol 3 1473 1492 https://doi.org/10.1002/cphy.c120035
Friedman SL (2008a) Hepatic stellate cells: protean, multifunctional, and enigmatic cells of the liver. Physiol Rev 88:125–172. https://doi.org/10.1152/physrev.00013.2007
SL Friedman 2008 Hepatic stellate cells: protean, multifunctional, and enigmatic cells of the liver Physiol Rev 88 125 172 https://doi.org/10.1152/physrev.00013.2007
Friedman SL (2008b) Mechanisms of hepatic fibrogenesis. Gastroenterology 134:1655–1669. https://doi.org/10.1053/j.gastro.2008.03.003
Friedman SL (2008c) Mechanisms of hepatic fibrogenesis Gastroenterology 134(1655):1669. https://doi.org/10.1053/j.gastro.2008.03.003
Lee UE, Friedman SL (2011) Mechanisms of hepatic fibrogenesis. Best Pract Res Clin Gastroenterol 25:195–206. https://doi.org/10.1016/j.bpg.2011.02.005
UE Lee SL Friedman 2011 Mechanisms of hepatic fibrogenesis Best Pract Res Clin Gastroenterol 25 195 206 https://doi.org/10.1016/j.bpg.2011.02.005
Borojevic R, Monteiro AN, Vinhas SA, Domont GB, Mourao PA, Emonard H, Grimaldi G Jr, Grimaud JA (1985) Establishment of a continuous cell line from fibrotic schistosomal granulomas in mice livers. Vitro Cell Dev Biol 21:382–390. https://doi.org/10.1007/bf02623469
R Borojevic AN Monteiro SA Vinhas GB Domont PA Mourao H Emonard G Grimaldi Jr JA Grimaud 1985 Establishment of a continuous cell line from fibrotic schistosomal granulomas in mice livers In Vitro Cell Dev Biol 21 382 390 https://doi.org/10.1007/bf02623469
Margis R, Pinheiro-Margis M, da Silva LC, Borojevic R (1992) Effects of retinol on proliferation, cell adherence and extracellular matrix synthesis in a liver myofibroblast or lipocyte cell line (GRX). Int J Exp Pathol 73:125–135
R Margis M Pinheiro-Margis LC Silva da R Borojevic 1992 Effects of retinol on proliferation, cell adherence and extracellular matrix synthesis in a liver myofibroblast or lipocyte cell line (GRX) Int J Exp Pathol 73 125 135
Pinheiro-Margis M, Margis R, Borojevic R (1992) Collagen synthesis in an established liver connective tissue cell line (GRX) during induction of the fat-storing phenotype. Exp Mol Pathol 56:108–118. https://doi.org/10.1016/0014-4800(92)90028-a
M Pinheiro-Margis R Margis R Borojevic 1992 Collagen synthesis in an established liver connective tissue cell line (GRX) during induction of the fat-storing phenotype Exp Mol Pathol 56 108 118 https://doi.org/10.1016/0014-4800(92)90028-a
Bitencourt S, de Mesquita FC, Caberlon E, da Silva GV, Basso BS, Ferreira GA, de Oliveira JR (2012) Capsaicin induces de-differentiation of activated hepatic stellate cell. Biochem Cell Biol 90:683–690. https://doi.org/10.1139/o2012-026
S Bitencourt FC Mesquita de E Caberlon GV Silva da BS Basso GA Ferreira JR Oliveira de 2012 Capsaicin induces de-differentiation of activated hepatic stellate cell Biochem Cell Biol 90 683 690 https://doi.org/10.1139/o2012-026
de Mesquita FC, Bitencourt S, Caberlon E, da Silva GV, Basso BS, Schmid J, Ferreira GA, de Oliveira FS, de Oliveira JR (2013) Fructose-1,6-bisphosphate induces phenotypic reversion of activated hepatic stellate cell. Eur J Pharmacol 720:320–325. https://doi.org/10.1016/j.ejphar.2013.09.067
FC Mesquita de S Bitencourt E Caberlon GV Silva da BS Basso J Schmid GA Ferreira FS Oliveira de JR Oliveira de 2013 Fructose-1,6-bisphosphate induces phenotypic reversion of activated hepatic stellate cell Eur J Pharmacol 720 320 325 https://doi.org/10.1016/j.ejphar.2013.09.067
Guimaraes EL, Franceschi MF, Grivicich I, Dal-Pizzol F, Moreira JC, Guaragna RM, Borojevic R, Margis R, Guma FC (2006) Relationship between oxidative stress levels and activation state on a hepatic stellate cell line. Liver Int 26:477–485. https://doi.org/10.1111/j.1478-3231.2006.01245.x
EL Guimaraes MF Franceschi I Grivicich F Dal-Pizzol JC Moreira RM Guaragna R Borojevic R Margis FC Guma 2006 Relationship between oxidative stress levels and activation state on a hepatic stellate cell line Liver Int 26 477 485 https://doi.org/10.1111/j.1478-3231.2006.01245.x
Martins LA, Coelho BP, Behr G, Pettenuzzo LF, Souza IC, Moreira JC, Borojevic R, Gottfried C, Guma FC (2014) Resveratrol induces pro-oxidant effects and time-dependent resistance to cytotoxicity in activated hepatic stellate cells. Cell Biochem Biophys 68:247–257. https://doi.org/10.1007/s12013-013-9703-8
LA Martins BP Coelho G Behr LF Pettenuzzo IC Souza JC Moreira R Borojevic C Gottfried FC Guma 2014 Resveratrol induces pro-oxidant effects and time-dependent resistance to cytotoxicity in activated hepatic stellate cells Cell Biochem Biophys 68 247 257 https://doi.org/10.1007/s12013-013-9703-8
Meira Martins LA, Vieira MQ, Ilha M, de Vasconcelos M, Biehl HB, Lima DB, Schein V, Barbe-Tuana F, Borojevic R, Guma FC (2015) The interplay between apoptosis, mitophagy and mitochondrial biogenesis induced by resveratrol can determine activated hepatic stellate cells death or survival. Cell Biochem Biophys 71:657–672. https://doi.org/10.1007/s12013-014-0245-5
LA Meira Martins MQ Vieira M Ilha M Vasconcelos de HB Biehl DB Lima V Schein F Barbe-Tuana R Borojevic FC Guma 2015 The interplay between apoptosis, mitophagy and mitochondrial biogenesis induced by resveratrol can determine activated hepatic stellate cells death or survival Cell Biochem Biophys 71 657 672 https://doi.org/10.1007/s12013-014-0245-5
Souza IC, Martins LA, Coelho BP, Grivicich I, Guaragna RM, Gottfried C, Borojevic R, Guma FC (2008) Resveratrol inhibits cell growth by inducing cell cycle arrest in activated hepatic stellate cells. Mol Cell Biochem 315:1–7. https://doi.org/10.1007/s11010-008-9781-x
IC Souza LA Martins BP Coelho I Grivicich RM Guaragna C Gottfried R Borojevic FC Guma 2008 Resveratrol inhibits cell growth by inducing cell cycle arrest in activated hepatic stellate cells Mol Cell Biochem 315 1 7 https://doi.org/10.1007/s11010-008-9781-x
de Souza IC, Martins LA, de Vasconcelos M, de Oliveira CM, Barbe-Tuana F, Andrade CB, Pettenuzzo LF, Borojevic R, Margis R, Guaragna R, Guma FC (2015) Resveratrol Regulates the Quiescence-Like Induction of Activated Stellate Cells by Modulating the PPARgamma/SIRT1 Ratio. J Cell Biochem 116:2304–2312. https://doi.org/10.1002/jcb.25181
IC Souza de LA Martins M Vasconcelos de CM Oliveira de F Barbe-Tuana CB Andrade LF Pettenuzzo R Borojevic R Margis R Guaragna FC Guma 2015 Resveratrol regulates the quiescence-like induction of activated stellate cells by modulating the PPARgamma/SIRT1 ratio J Cell Biochem 116 2304 2312 https://doi.org/10.1002/jcb.25181
Rajan N, Habermehl J, Cote MF, Doillon CJ, Mantovani D (2006) Preparation of ready-to-use, storable and reconstituted type I collagen from rat tail tendon for tissue engineering applications. Nat Protoc 1:2753–2758. https://doi.org/10.1038/nprot.2006.430
N Rajan J Habermehl MF Cote CJ Doillon D Mantovani 2006 Preparation of ready-to-use, storable and reconstituted type I collagen from rat tail tendon for tissue engineering applications Nat Protoc 1 2753 2758 https://doi.org/10.1038/nprot.2006.430
Basso BS, de Mesquita FC, Dias HB, Krause GC, Scherer M, Santarem ER, de Oliveira JR (2019) Therapeutic effect of Baccharis anomala DC. extracts on activated hepatic stellate cells. EXCLI J 18:91–105
Basso BS, Mesquita FC, de HB Dias GC Krause M Scherer ER Santarem JR Oliveira de, (2019) Therapeutic effect of Baccharis anomala DC. Extracts on activated hepatic stellate cells EXCLI J 18(91):105
Grada A, Otero-Vinas M, Prieto-Castrillo F, Obagi Z, Falanga V (2017a) Research Techniques Made Simple: Analysis of Collective Cell Migration Using the Wound Healing Assay. J Invest Dermatol 137:e11–e16. https://doi.org/10.1016/j.jid.2016.11.020
Grada A, Otero-Vinas M, Prieto-Castrillo F, Obagi Z, Falanga V (2017b) Research techniques made simple: analysis of collective cell migration using the wound healing assay. J Invest Dermatol 137(e11):e16. https://doi.org/10.1016/j.jid.2016.11.020
Peterson GL (1979a) Review of the Folin phenol protein quantitation method of Lowry, Rosebrough, Farr and Randall. Anal Biochem 100:201–220. https://doi.org/10.1016/0003-2697(79)90222-7
Peterson GL (1979b) Review of the Folin phenol protein quantitation method of Lowry. Rosebrough, Farr and Randall Anal Biochem 100(201):220. https://doi.org/10.1016/0003-2697(79)90222-7
Reeves HL, Friedman SL (2002) Activation of hepatic stellate cells–a key issue in liver fibrosis. Front Biosci 7:d808–d826. https://doi.org/10.2741/reeves
HL Reeves SL Friedman 2002 Activation of hepatic stellate cells—a key issue in liver fibrosis Front Biosci 7 d808 d826 https://doi.org/10.2741/reeves
Carotti S, Morini S, Corradini SG, Burza MA, Molinaro A, Carpino G, Merli M, De Santis A, Muda AO, Rossi M, Attili AF, Gaudio E (2008) Glial fibrillary acidic protein as an early marker of hepatic stellate cell activation in chronic and posttransplant recurrent hepatitis C. Liver Transpl 14:806–814. https://doi.org/10.1002/lt.21436
S Carotti S Morini SG Corradini MA Burza A Molinaro G Carpino M Merli A Santis De AO Muda M Rossi AF Attili E Gaudio 2008 Glial fibrillary acidic protein as an early marker of hepatic stellate cell activation in chronic and posttransplant recurrent hepatitis C Liver Transpl 14 806 814 https://doi.org/10.1002/lt.21436
Tennakoon AH, Izawa T, Wijesundera KK, Golbar HM, Tanaka M, Ichikawa C, Kuwamura M, Yamate J (2013) Characterization of glial fibrillary acidic protein (GFAP)-expressing hepatic stellate cells and myofibroblasts in thioacetamide (TAA)-induced rat liver injury. Exp Toxicol Pathol 65:1159–1171. https://doi.org/10.1016/j.etp.2013.05.008
AH Tennakoon T Izawa KK Wijesundera HM Golbar M Tanaka C Ichikawa M Kuwamura J Yamate 2013 Characterization of glial fibrillary acidic protein (GFAP)-expressing hepatic stellate cells and myofibroblasts in thioacetamide (TAA)-induced rat liver injury Exp Toxicol Pathol 65 1159 1171 https://doi.org/10.1016/j.etp.2013.05.008
Sohail MA, Hashmi AZ, Hakim W, Watanabe A, Zipprich A, Groszmann RJ, Dranoff JA, Torok NJ, Mehal WZ (2009) Adenosine induces loss of actin stress fibers and inhibits contraction in hepatic stellate cells via Rho inhibition. Hepatology 49:185–194. https://doi.org/10.1002/hep.22589
MA Sohail AZ Hashmi W Hakim A Watanabe A Zipprich RJ Groszmann JA Dranoff NJ Torok WZ Mehal 2009 Adenosine induces loss of actin stress fibers and inhibits contraction in hepatic stellate cells via Rho inhibition Hepatology 49 185 194 https://doi.org/10.1002/hep.22589
Yee HF Jr (1998) Rho directs activation-associated changes in rat hepatic stellate cell morphology via regulation of the actin cytoskeleton. Hepatology 28:843–850. https://doi.org/10.1002/hep.510280336
HF Yee Jr (1998) Rho directs activation-associated changes in rat hepatic stellate cell morphology via regulation of the actin cytoskeleton. Hepatology 28(843):850. https://doi.org/10.1002/hep.510280336
Park SY, Le CT, Sung KY, Choi DH, Cho EH (2018) Succinate induces hepatic fibrogenesis by promoting activation, proliferation, and migration, and inhibiting apoptosis of hepatic stellate cells. Biochem Biophys Res Commun 496:673–678. https://doi.org/10.1016/j.bbrc.2018.01.106
SY Park CT Le KY Sung DH Choi EH Cho 2018 Succinate induces hepatic fibrogenesis by promoting activation, proliferation, and migration, and inhibiting apoptosis of hepatic stellate cells Biochem Biophys Res Commun 496 673 678 https://doi.org/10.1016/j.bbrc.2018.01.106
Berman AY, Motechin RA, Wiesenfeld MY, Holz MK (2017) The therapeutic potential of resveratrol: a review of clinical trials. NPJ Precis Oncol. https://doi.org/10.1038/s41698-017-0038-6
AY Berman RA Motechin MY Wiesenfeld MK Holz 2017 The therapeutic potential of resveratrol: a review of clinical trials NPJ Precis Oncol https://doi.org/10.1038/s41698-017-0038-6
Faghihzadeh F, Hekmatdoost A, Adibi P (2015a) Resveratrol and liver: A systematic review. J Res Med Sci 20:797–810. https://doi.org/10.4103/1735-1995.168405
Faghihzadeh F, Hekmatdoost A, Adibi P (2015b) Resveratrol and liver: a systematic review J Res. Med Sci 20(797):810. https://doi.org/10.4103/1735-1995.168405
Kumar A, Sharma SS (2010) NF-kappaB inhibitory action of resveratrol: a probable mechanism of neuroprotection in experimental diabetic neuropathy. Biochem Biophys Res Commun 394:360–365. https://doi.org/10.1016/j.bbrc.2010.03.014
A Kumar SS Sharma 2010 NF-kappaB inhibitory action of resveratrol: a probable mechanism of neuroprotection in experimental diabetic neuropathy Biochem Biophys Res Commun 394 360 365 https://doi.org/10.1016/j.bbrc.2010.03.014
Leijas A, Reyes J, Rodríguez L (2007a) Hepatic stellate cells are a major component of liver fibrosis and a target for the treatment of chronic liver disease. Biotecnología Aplicada 24:7
Leijas A, Reyes J, Rodríguez L (2007b) Hepatic stellate cells are a major component of liver fibrosis and a target for the treatment of chronic liver disease Biotecnología Aplicada 24:7
Thirunavukkarasu C, Watkins SC, Gandhi CR (2006) Mechanisms of endotoxin-induced NO, IL-6, and TNF-alpha production in activated rat hepatic stellate cells: role of p38 MAPK. Hepatology 44:389–398. https://doi.org/10.1002/hep.21254
C Thirunavukkarasu SC Watkins CR Gandhi 2006 Mechanisms of endotoxin-induced NO, IL-6, and TNF-alpha production in activated rat hepatic stellate cells: role of p38 MAPK Hepatology 44 389 398 https://doi.org/10.1002/hep.21254
Gan Z, Wei W, Wu J, Zhao Y, Zhang L, Wang T, Zhong X (2019) Resveratrol and Curcumin Improve Intestinal Mucosal Integrity and Decrease m(6)A RNA Methylation in the Intestine of Weaning Piglets. ACS Omega 4:17438–17446. https://doi.org/10.1021/acsomega.9b02236
Z Gan W Wei J Wu Y Zhao L Zhang T Wang X Zhong 2019 Resveratrol and curcumin improve intestinal mucosal integrity and decrease m(6)A RNA methylation in the intestine of weaning piglets ACS Omega 4 17438 17446 https://doi.org/10.1021/acsomega.9b02236
Juhasz B, Varga B, Gesztelyi R, Kemeny-Beke A, Zsuga J, Tosaki A (2010) Resveratrol: a multifunctional cytoprotective molecule. Curr Pharm Biotechnol 11:810–818. https://doi.org/10.2174/138920110793262079
B Juhasz B Varga R Gesztelyi A Kemeny-Beke J Zsuga A Tosaki 2010 Resveratrol: a multifunctional cytoprotective molecule Curr Pharm Biotechnol 11 810 818 https://doi.org/10.2174/138920110793262079
Mehta J, Rayalam S, Wang X (2018a) Cytoprotective Effects of Natural Compounds against Oxidative Stress. Antioxidants (Basel). https://doi.org/10.3390/antiox7100147
Mehta J, Rayalam S, Wang X (2018b). Cytoprotective effects of natural compounds against oxidative stress Antioxidants (Basel). https://doi.org/10.3390/antiox7100147
Huang YT, Lai PC, Wu CC, Cheng CC, Chiu TH (2010) TrkB antibody elicits cytotoxicity and suppresses migration/invasion of transitional cell carcinoma cells. Int J Oncol 37:943–949. https://doi.org/10.3892/ijo_00000745
YT Huang PC Lai CC Wu CC Cheng TH Chiu 2010 TrkB antibody elicits cytotoxicity and suppresses migration/invasion of transitional cell carcinoma cells Int J Oncol 37 943 949 https://doi.org/10.3892/ijo_00000745
Lee YJ, Kim SY, Lee C (2019) Axl is a novel target of celastrol that inhibits cell proliferation and migration, and increases the cytotoxicity of gefitinib in EGFR mutant nonsmall cell lung cancer cells. Mol Med Rep 19:3230–3236. https://doi.org/10.3892/mmr.2019.9957
YJ Lee SY Kim C Lee 2019 Axl is a novel target of celastrol that inhibits cell proliferation and migration, and increases the cytotoxicity of gefitinib in EGFR mutant nonsmall cell lung cancer cells Mol Med Rep 19 3230 3236 https://doi.org/10.3892/mmr.2019.9957
Salum LB, Mascarello A, Canevarolo RR, Altei WF, Laranjeira AB, Neuenfeldt PD, Stumpf TR, Chiaradia-Delatorre LD, Vollmer LL, Daghestani HN, de Souza Melo CP, Silveira AB, Leal PC, Frederico MJ, do Nascimento LF, Santos AR, Andricopulo AD, Day BW, Yunes RA, Vogt A, Yunes JA and Nunes RJ, (2015) N-(1’-naphthyl)-3,4,5-trimethoxybenzohydrazide as microtubule destabilizer: Synthesis, cytotoxicity, inhibition of cell migration and in vivo activity against acute lymphoblastic leukemia. Eur J Med Chem 96:504–518. https://doi.org/10.1016/j.ejmech.2015.02.041
LB Salum A Mascarello RR Canevarolo WF Altei AB Laranjeira PD Neuenfeldt TR Stumpf LD Chiaradia-Delatorre LL Vollmer HN Daghestani CP Souza Melo de AB Silveira PC Leal MJ Frederico do Nascimento LF, Santos AR, Andricopulo AD, Day BW, Yunes RA, Vogt A, Yunes JA and Nunes RJ, 2015 N-(1'-naphthyl)-3,4,5-trimethoxybenzohydrazide as microtubule destabilizer: synthesis, cytotoxicity, inhibition of cell migration and in vivo activity against acute lymphoblastic leukemia Eur J Med Chem 96 504 518 https://doi.org/10.1016/j.ejmech.2015.02.041
Nieto N (2006) Oxidative-stress and IL-6 mediate the fibrogenic effects of [corrected] Kupffer cells on stellate cells. Hepatology 44:1487–1501. https://doi.org/10.1002/hep.21427
N Nieto 2006 Oxidative-stress and IL-6 mediate the fibrogenic effects of [corrected] Kupffer cells on stellate cells Hepatology 44 1487 1501 https://doi.org/10.1002/hep.21427
Yang YM, Seki E (2015) TNFalpha in liver fibrosis. Curr Pathobiol Rep 3:253–261. https://doi.org/10.1007/s40139-015-0093-z
YM Yang E Seki 2015 TNFalpha in liver fibrosis Curr Pathobiol Rep 3 253 261 https://doi.org/10.1007/s40139-015-0093-z
Kim Y, Fiel MI, Albanis E, Chou HI, Zhang W, Khitrov G, Friedman SL (2012) Anti-fibrotic activity and enhanced interleukin-6 production by hepatic stellate cells in response to imatinib mesylate. Liver Int 32:1008–1017. https://doi.org/10.1111/j.1478-3231.2012.02806.x
Y Kim MI Fiel E Albanis HI Chou W Zhang G Khitrov SL Friedman 2012 Anti-fibrotic activity and enhanced interleukin-6 production by hepatic stellate cells in response to imatinib mesylate Liver Int 32 1008 1017 https://doi.org/10.1111/j.1478-3231.2012.02806.x
Hernandez-Munoz I, de la Torre P, Sanchez-Alcazar JA, Garcia I, Santiago E, Munoz-Yague MT, Solis-Herruzo JA (1997) Tumor necrosis factor alpha inhibits collagen alpha 1(I) gene expression in rat hepatic stellate cells through a G protein. Gastroenterology 113:625–640. https://doi.org/10.1053/gast.1997.v113.pm9247485
I Hernandez-Munoz P Torre de la JA Sanchez-Alcazar I Garcia E Santiago MT Munoz-Yague JA Solis-Herruzo 1997 Tumor necrosis factor alpha inhibits collagen alpha 1(I) gene expression in rat hepatic stellate cells through a G protein Gastroenterology 113 625 640 https://doi.org/10.1053/gast.1997.v113.pm9247485
Kim JJ, Lee SB, Park JK, Yoo YD (2010) TNF-alpha-induced ROS production triggering apoptosis is directly linked to Romo1 and Bcl-X(L). Cell Death Differ 17:1420–1434. https://doi.org/10.1038/cdd.2010.19
JJ Kim SB Lee JK Park YD Yoo 2010 TNF-alpha-induced ROS production triggering apoptosis is directly linked to Romo1 and Bcl-X(L) Cell Death Differ 17 1420 1434 https://doi.org/10.1038/cdd.2010.19
Barcelos ALV, de Oliveira EA, Haute GV, Costa BP, Pedrazza L, Donadio MVF, de Oliveira JR, Bodanese LC (2019) Association of IL-10 to coronary disease severity in patients with metabolic syndrome. Clin Chim Acta 495:394–398. https://doi.org/10.1016/j.cca.2019.05.006
ALV Barcelos EA Oliveira de GV Haute BP Costa L Pedrazza MVF Donadio JR Oliveira de LC Bodanese 2019 Association of IL-10 to coronary disease severity in patients with metabolic syndrome Clin Chim Acta 495 394 398 https://doi.org/10.1016/j.cca.2019.05.006
Arnaud V, Li J, Wang Y, Fu X, Mengzhi S, Luo X, Hou X, Dessein H, Jie Z, Xin-Ling Y, He H, McManus DP, Li Y, Dessein A (2008) Regulatory role of interleukin-10 and interferon-gamma in severe hepatic central and peripheral fibrosis in humans infected with Schistosoma japonicum. J Infect Dis 198:418–426. https://doi.org/10.1086/588826
V Arnaud J Li Y Wang X Fu S Mengzhi X Luo X Hou H Dessein Z Jie Y Xin-Ling H He DP McManus Y Li A Dessein 2008 Regulatory role of interleukin-10 and interferon-gamma in severe hepatic central and peripheral fibrosis in humans infected with Schistosoma japonicum J Infect Dis 198 418 426 https://doi.org/10.1086/588826
Mathurin P, Xiong S, Kharbanda KK, Veal N, Miyahara T, Motomura K, Rippe RA, Bachem MG, Tsukamoto H (2002) IL-10 receptor and coreceptor expression in quiescent and activated hepatic stellate cells. Am J Physiol Gastrointest Liver Physiol 282:G981–G990. https://doi.org/10.1152/ajpgi.00293.2001
P Mathurin S Xiong KK Kharbanda N Veal T Miyahara K Motomura RA Rippe MG Bachem H Tsukamoto 2002 IL-10 receptor and coreceptor expression in quiescent and activated hepatic stellate cells Am J Physiol Gastrointest Liver Physiol 282 G981 G990 https://doi.org/10.1152/ajpgi.00293.2001
Mosser DM, Zhang X (2008) Interleukin-10: new perspectives on an old cytokine. Immunol Rev 226:205–218. https://doi.org/10.1111/j.1600-065X.2008.00706.x
DM Mosser X Zhang 2008 Interleukin-10: new perspectives on an old cytokine Immunol Rev 226 205 218 https://doi.org/10.1111/j.1600-065X.2008.00706.x
Zhang LJ, Zheng WD, Shi MN, Wang XZ (2006) Effects of interleukin-10 on activation and apoptosis of hepatic stellate cells in fibrotic rat liver. World J Gastroenterol 12:1918–1923. https://doi.org/10.3748/wjg.v12.i12.1918
LJ Zhang WD Zheng MN Shi XZ Wang 2006 Effects of interleukin-10 on activation and apoptosis of hepatic stellate cells in fibrotic rat liver World J Gastroenterol 12 1918 1923 https://doi.org/10.3748/wjg.v12.i12.1918
Borriello A, Bencivenga D, Caldarelli I, Tramontano A, Borgia A, Pirozzi AV, Oliva A, Della Ragione F (2013a) Resveratrol and cancer treatment: is hormesis a yet unsolved matter? Curr Pharm Des 19:5384–5393. https://doi.org/10.2174/1381612811319300007
Borriello A, Bencivenga D, Caldarelli I, Tramontano A, Borgia A, Pirozzi AV, Oliva A, Della Ragione F (2013b) Resveratrol and cancer treatment: is hormesis a yet unsolved matter? Curr Pharm Des 19(5384):5393. https://doi.org/10.2174/1381612811319300007
Tsukamoto H (2005a) Fat paradox in liver disease. Keio J Med 54:190–192. https://doi.org/10.2302/kjm.54.190
Tsukamoto H (2005b) Fat paradox in liver disease. Keio J Med 54(190):192. https://doi.org/10.2302/kjm.54.190
Acknowledgements
C.M. de Oliveira is the recipient of a fellowship from CAPES (Coordenação de Aperfeiçoamento de Pessoal de Nível Superior). This work was also supported by CNPq (Conselho Nacional de Desenvolvimento Científico e Tecnológico—Brazil), FAPERGS (Fundação de Amparo à Pesquisa do Rio Grande do Sul, PqG n°1009169) and PROPESQ-UFRGS. All authors would like to thank to Dr. Elena Bernard for the helpful comments in this study.
Author information
Authors and Affiliations
Contributions
Wrote the paper: CMO and LAMM. Establishment of GRX cell line: RB. Collected and analysed data: CMO, LAMM, ASC, KSM, BruPC, MQV, BarPC. Supervision and Contribution to the text writing: JRO and FCRG.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Oliveira, C.M., Martins, L.A.M., de Sousa, A.C. et al. Resveratrol increases the activation markers and changes the release of inflammatory cytokines of hepatic stellate cells. Mol Cell Biochem 476, 649–661 (2021). https://doi.org/10.1007/s11010-020-03933-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-020-03933-1