Abstract
Myocardial ischemia is the main cause of death in the Western societies. Therapeutic strategies aimed to protect the ischemic myocardium have been extensively studied. Reperfusion is the definitive treatment for acute coronary syndromes, especially acute myocardial infarction; however, reperfusion has the potential to exacerbate tissue injury, a process termed reperfusion injury. Ischemia/reperfusion (I/R) injury may lead to cardiac arrhythmias and contractile dysfunction that involve apoptosis and necrosis in the heart. The present review describes the mitochondrial role on cardiomyocyte death and some potential pharmacological strategies aimed at preventing the opening of the box, i.e., mitochondrial dysfunction and membrane permeabilization that result into cell death. Data in the literature suggest that mitochondrial disruption during I/R can be avoided, although uncertainties still exist, including the fact that the optimal windows of treatment are still fairly unknown. Despite this, the protection of cardiac mitochondrial function should be critical for the patient survival, and new strategies to avoid mitochondrial alterations should be designed to avoid cardiomyocyte loss.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Ischemia/Reperfusion-Induced Cardiac Damage
Heart diseases are nowadays an important health problem in our society, especially in developed countries where such diseases constitute a leading cause of death. It is known that heart diseases cause more incapacity and economic losses in industrialized countries than any other group of diseases. Myocardial ischemia is one of the most notable in this kind of diseases. A shortage of oxygen and nutrients supply to cardiac cells due to a coronary perfusion insufficiency (ischemia) followed by its reposition (reperfusion) causes serious cardiac tissue damage and can compromise survival.
Myocardial ischemia can occur under several forms and persist for a few seconds or minutes (angioplasty or angina), for hours (cardiac surgery or transplantation) or for years (chronic ischemia) [1]. Independently of the way it is manifested, myocardial ischemia is characterized by a marked imbalance between the provision of oxygen and nutrients to myocardial cells and their needs. The imbalance may arise for any of the three following reasons: (a) an increase in the myocardial demand for oxygen and nutrients (demand ischemia), (b) a decrease in the supply of oxygen and nutrients (supply ischemia) and (c) a mixed situation in which the above two factors are simultaneously present (cardiac surgery or transplantation). Whatever is the underlying mechanism, when such an imbalance of supply and demand occurs, biochemical and physiological repercussions can even result in cell death [2].
The series of biochemical phenomena by which myocardial ischemia can lead to functional depression of myocardial contractility is not yet fully understood. One possibility is that I/R is associated with increased oxidative stress in the myocardium, especially occurring during the reperfusion phase, when the affected tissue is suddenly confronted with a burst of oxygen [3, 4]. The role of cell and in particular mitochondrial oxidative stress in I/R pathophysiology [5] is demonstrated by the use of transgenic mice, which overexpress several key antioxidant enzymes, including mitochondrial glutaredoxin-2 [6], mitochondrial manganese-dependent superoxide dismutase [7], catalase [8] or glutathione peroxidase [9].
The role of mitochondria in I/R damage, including the role on the modulation of cardiomyocyte life and death has been widely explored, although several doubts still remain. In a metabolically hyperactive tissue such as the heart, mitochondria play a very important role in the energy supply for the myocyte [10]. Cardiac cells have two distinct mitochondrial populations, one beneath the plasma membrane and the other between the myofibrils, which present differences regarding calcium accumulation and respiratory activity [11–13]. Such spatial organization warrants that different needs in terms of energy of distinct cell spaces are met with proper delivery. Interestingly, it has been reported that both cardiac mitochondrial subpopulations differ in their resistance to I/R. For example, it has been described that sub-sarcolemmal mitochondria are more susceptible to ischemia-induced loss of cardiolipin [14], which explains the reported inhibition of mitochondrial complex IV [15] and the mitochondrial adenine nucleotide translocator [16] activity in that mitochondrial subpopulation during I/R.
There is evidence that multiple pathways of cell death participate simultaneously in promoting mitochondria-mediated cardiac damage (Fig. 1). Apoptosis and autophagy are considered forms of programed cell death that involve the activation of regulated pathways leading to cell death while necrosis is considered an irreversible and non-regulated process of cell killing [17]. Cardiac apoptosis is a cellular death program extremely regulated and with great efficiency, involving an interaction of innumerous factors. Loss of cardiomyocytes via apoptosis is believed to contribute to the continuous decline of ventricular function during I/R. Cardiac myocytes are terminally differentiated and are not replaced after loss. With fewer myocytes, the ability of the myocardium to sustain contractile function may be compromised [18].
Apoptotic signaling pathways involved in I/R damage. Intrinsic, extrinsic and ER stress-induced pathways are shown. ?—Caspase-12 activity induced by endoplasmic reticulum (ER) stress has not been identified in humans; therefore, its existence is controversial. Recently, Caspase-4 was considered as a gene homologous to Caspase-12 and seems to be localized predominantly to the ER and to mitochondria → Stimulatory/Activating effect;  Translocation events; ⊥ Inhibitory effect
Translocation events; ⊥ Inhibitory effect
Autophagy plays a critical and seemingly double role in cardiomyocytes, being implicated as a mechanism for both cellular survival during I/R injury and cell death when repaired of the injured myocardium is impossible [19]. Many studies have reported that autophagy is upregulated during myocardial I/R [20], while other studies reported that after cardiac I/R, many of the autophagosomes contained mitochondria [21]. Although several doubts remain, the upregulation of autophagy in response to I/R stress may serve as a protective response by removing damaged mitochondria, thus preventing activation of apoptosis.
Apoptosis and Ischemia/Reperfusion Cardiac Damage
As described earlier, apoptosis is a highly regulated, energy-requiring process that follows well-defined time-dependent signaling pathways, resulting in cell shrinkage, changes in plasma membrane, proteolysis of intracellular proteins, loss of mitochondrial function and DNA fragmentation (Fig. 2). The immediate objective of apoptotic signaling pathway is the activation of pro-caspases and the “safe” dismantling of intracellular components. Apoptosis is mediated by two central pathways: one that occurs in response to activated death receptors present in the cell surface (extrinsic pathway) and another that occurs in response to signals originated inside the cell and which involve mitochondria as either an initiator or a magnifier of apoptotic signals (intrinsic pathway) [22]. The extrinsic pathway is triggered by the linkage of specific ligands to one group of membrane receptors that belong to the tumor necrosis factor receptor family (αTNF) or Fas receptor [23].
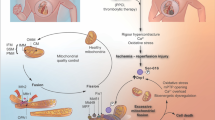
Mitochondrial mechanisms of cell dysfunction and key events in cardiac I/R injury. The fate of mitochondria determines the fate of the cell. Ischemia leads to ATP dissipation, with consequent rises in cell Ca2+ and Pi. On reperfusion, these three factors, together with oxidative stress, trigger MPTP opening. If widespread, MPTP opening results into ATP depletion and cell necrosis. If MPTP opening is more limited enabling the cell to maintain sufficient ATP, then outer membrane rupture leads to apoptosis. The degree of MPTP opening may determine the balance between necrotic and apoptotic cell death and whether it might leads to contractile dysfunction at reperfusion
Mitochondria are deeply involved in the intrinsic apoptotic signaling. As it will be discussed later on, protein release from mitochondria, including cytochrome c, may be associated with the opening of the mitochondrial permeability transition pore (MPTP) located at contact sites between the inner and outer membranes [24]. The key step in the intrinsic pathway is a disturbance in mitochondrial membrane permeability (Fig. 3) that is regulated by a variety of pro-apoptotic and anti-apoptotic Bcl-2 proteins such as Bax, Bad and Bid, or Bcl-2, respectively. The mitochondrial release of cytochrome c leads to the apoptosome formation, a macromolecular complex that includes cytochrome c itself, Apaf-1, dATP and pro-caspase-9 [25].
Mitochondrial apoptotic signaling during cardiac I/R injury. The Bcl-2 family of proteins function primarily to protect or disrupt the integrity of the mitochondrial membrane and control the mitochondrial release of pro-apoptotic proteins such as cytochrome c, AIF and Smac/DIABLO. Anti-apoptotic Bcl-2 members (Bcl-xL) protect the mitochondrial membrane. In response to ischemia injury, these anti-apoptotic proteins engage another set of pro-apoptotic proteins of the Bax subfamily (which includes Bax, Bak), normally loosely residing in the mitochondrial outer membranes or in the cytosol. The interaction between Bak and Bax proteins results in oligomerization and insertion into the mitochondrial membrane of the complete complex. Bax is located in the cytosol of healthy cardiomyocytes, although some Bax exist in mitochondria, where it is believed to be heterodimerized (and inactivated) by binding to anti-apoptotic Bcl-xL. In response to death stimulation, Bax undergoes a conformational change that triggers its translocation and insertion into the outer mitochondrial membrane, leading to the permeabilization of the outer mitochondrial membrane and release of pro-apoptotic proteins. Bcl-2 has been demonstrated to reduce the rate of ATP consumption during ischemia by inhibiting the F1Fo-ATPase. A new role for the Bcl-2 family proteins is emerging as regulators of mitochondrial energetics. During ischemia, when mitochondrial electron transport and mitochondrial ATP generation are inhibited because of lack of oxygen, the F1Fo-ATPase runs in reverse and pumps protons out of the matrix while glycolytic ATP is consumed in an attempt to restore the mitochondrial membrane potential. The functional interplay of the Bcl-2 protein family controls the induction of the intrinsic pathway of apoptosis. Transcription-dependent and transcription-independent p53 activities converge at the mitochondria. While nuclear p53 via its transcriptional activity induces expression of the BH3-only proteins PUMA, Noxa and Bid, cytosolic or mitochondrial p53 via transcription-independent mechanisms directly activates Bax/Bak and neutralizes the anti-apoptotic effect of Bcl-2/Bcl-xL. ETC.—Electron transport chain. → Stimulatory/Activating effect;  Translocation events and ⊥ Inhibitory effect
Translocation events and ⊥ Inhibitory effect
It has been described that myocardial apoptosis is dominant in the pathogenesis of cardiac I/R and in the maintenance of persistent myocardial dysfunction after reperfusion. Prolonged periods of myocardial ischemia are related with an increase in necrosis rate, whereas reperfusion leads to enhancement of apoptosis [26]. During reperfusion, the energy required for sequential apoptosis steps is supplied because oxygen and glucose supply are restored. As metabolic processes are restored, ATP becomes available and the apoptotic cascade may proceed [27]. Genetic approaches and pharmacological studies suggest that cardiomyocyte apoptosis plays a crucial role in the pathogenesis of many cardiac syndromes and pathologies. For instance, the inhibition of cardiac myocyte apoptosis reduces infarct size up to 50–70% and decreases cardiac dysfunction after I/R [28, 29].
There are very distinct published results concerning ischemia and I/R-mediated apoptosis. In various animal models of I/R, it was shown that apoptosis is not significantly active during prolonged ischemia, but it is accelerated by reperfusion [30–32]. In other studies, the first signs of apoptosis were detected as early as after 10 min of ischemia reaching maximal levels at 30–60 min of ischemia with further increase [33] or no change [34] at reperfusion. Caspase activation is detectable after 30 min ischemia, while DNA fragmentation is detectable after 60 min, while both parameters increase during reperfusion [35, 36]. Also important is the comparison between in vitro and in vivo studies. For instance, apoptosis was evident after only 50 min ischemia in isolated perfused hearts while in an in vivo preparation, apoptosis was first noted 6 h after ischemia [37].
Increased generation of free radicals without concomitant increase in antioxidant protection has been shown to induce apoptosis during I/R [38]. The resulting oxidative stress leads to peroxidation of the phospholipid cardiolipin in the inner mitochondrial membrane, which contributes to induce cytochrome c release from the inner mitochondrial membrane (IMM) to the extramitochondrial environment and trigger apoptosis [39].
In sum, cardiomyocyte injury and death following I/R injury, which can occur by apoptosis, is an important cause of morbidity and mortality. The role and clinical impact of apoptosis need to be further assessed to allow the development of more effective therapies to prevent myocardial damage during I/R. Such therapies must prevent mitochondrial dysfunction in order to preserve myocardial physiology.
The Mitochondrial Pathway in Ischemia/Reperfusion-Induced Cardiac Cell Death
Mitochondrial Dysfunction During I/R
During ischemia, an overall deterioration of cardiac cell function occurs, which is assessed by the loss of intracellular components, including proteins such as troponins and lactate dehydrogenase [40]. Intracellular levels of ATP are also reduced, while ADP, AMP and phosphate levels increase as mitochondria hydrolyzes ATP during ischemia in a futile attempt to preserve the mitochondrial membrane potential [40]. Ischemia has already been shown to damage several mitochondrial components, including proteins involved in oxidative phosphorylation and membrane lipids, which may predispose mitochondria for increased free radical generation [41] during reperfusion. Although mitochondria generate reactive oxygen species (ROS) during normal physiological conditions [42], it is accepted that during cardiac reperfusion, the production of ROS is greatly increased as a sudden supply of oxygen becomes available to the reduced components of the respiratory chain [43]. Also, a decrease in internal antioxidant defenses including superoxidase dismutase, glutathione peroxidase and reduced glutathione occurs during reperfusion, which further exacerbates oxidative stress [44]. Nevertheless, it is considered that a small amount of oxygen free radical production may also occur during ischemia, probably due to the existence of “oxygen pockets” in the cardiac tissue [45]. Several sources of free radicals during I/R include the mitochondrial respiratory chain, the oxidation of catecholamines, neutrophils or the enzyme xanthine oxidase [38]. From increased ROS production and decreased efficacy of antioxidant defenses, oxidative alterations to biomolecules occur. One consequence is protein oxidation, particularly in the respiratory chain, leading to structural alterations and consequent inhibition of mitochondrial respiration, with consequent decreased ATP synthesis [46]. Besides oxidative damage per se, reperfusion has also a negative impact on intracellular pH and Ca2+ homeostasis. Excessive influx of Ca2+ into the mitochondrion during reperfusion can also lead to inhibition of oxidative phosphorylation and increased permeability of the IMM by means of increased mitochondrial permeability transition [24].
Calcium, the Permeability Transition Pore and Cell Death
Various studies have shown that apoptosis is preceded by alterations in the mitochondrial membrane that result in the loss of the normal electrochemical gradient and lead to the phenomenon known as the mitochondrial permeability transition (MPT) [47], production of ROS and release of apoptotic factors, such as cytochrome c and the apoptosis-inducing factor (AIF), into the cytosol [48, 49]. Two mechanisms have been proposed to explain the release of cytochrome c from the mitochondrial intermembrane space. The first mechanism implies the MPT, with consequent rupture of the outer mitochondrial membrane (OMM) after mitochondrial swelling, together with loss of transmembrane potential and loss of several molecules [47]. The second mechanism is the passage of cytochrome c and other pro-apoptotic proteins through specific pores formed from complexes between pro-apoptotic proteins, such as Bax, and the voltage-dependent anion channel (VDAC), at the OMM. It is thought that some pro-apoptotic signals may induce the translocation of Bax to mitochondria and/or the activation of Bax by another pro-apoptotic protein, Bid (Fig. 1). In either case, this mechanism does not require any change in the properties of the IMM [50]. The precise nature of the MPTP is still poorly understood, but a classic model implies a complex between the VDAC, adenine nucleotide translocator (ANT) and the matrix protein cyclophilin D [51]. One important aspect of the MPT is that it may play a central role in cell death by either necrosis or apoptosis, depending on the extension of the phenomenon in the cell population, which determines the availability or unavailability of energy to activate the caspase pathway [52, 53]. It has been demonstrated that the MPT can be induced by conditions that may occur during I/R, such as the accumulation of inorganic phosphate, oxidation of pyridine nucleotides, oxidative stress, decrease/oxidation of GSH and lower matrix pH [24]. Although MPTP opening is strongly inhibited by acidosis during ischemia, it is favored by ATP depletion, oxidative stress and high intramitochondrial Ca2+ concentrations, conditions all concurrent during myocardial reperfusion [24]. Another critical agent in the induction of apoptosis is Ca2+. In the heart tissue, physiological Ca2+ spikes increase intramitochondrial Ca2+ concentration that acts as a signal for increased ATP production because of several inter-connected mechanisms [54]. However, a concerted action of the Na+/H+ (due to increase in acidosis during the ischemic period) and Ca2+/Na+ antiporters will cause cytosolic calcium overload during the reperfusion phase as acidic intracellular pH recovers toward normal values, causing a defective contractile function and mitochondrial dysfunction, though several pathways, including activation of the MPTP and calpain stimulation [55, 56]. Interestingly, a novel player involved in I/R mitochondrial dysfunction is ceramide, which emerging data pointed out to excessively accumulate in cardiac mitochondria after I/R [57].
Interaction of p53 and Bcl-2 Family Proteins with Mitochondria in the Ischemic and Reperfused Myocardium
It is known that cellular death may be directly activated by p53 translocation to mitochondria [58]. The p53 protein is capable of inducing apoptosis by a death receptor-independent pathway involving the release of mitochondrial cytochrome c. Upon stimulation that may result from nuclear damage, p53 mitochondrial translocation occurs very rapidly and precedes cytochrome c release, the collapse of the mitochondrial membrane potential and caspase-3 activation [59]. Upon mitochondrial translocation, p53 can localize to the outer membrane, which can prime mitochondria to collaborate in the cell program, once p53 transcription-dependent mechanisms are triggered [60]. Mitochondrial p53 physically interacts with the Bcl-2 family member proteins Bcl-xL and Bcl-2 and antagonizes their anti-apoptotic stabilization of the OMM [61]. Mitochondrial p53 also directly promotes the pro-apoptotic activity of Bak [60] and directly induces Bak oligomerization [62], creating a pathway through the OMM that leads to release of cytochrome c and consequently the caspases signalization activation. Hence, mitochondrial p53 has a dual action of neutralizing anti-apoptotic members as well as promoting the expression of pro-apoptotic members of Bcl-2 proteins, which results in OMM permeabilization. However, the role of p53 in heart ischemia remains somewhat controversial. Earlier studies reported that p53 is dispensable for hypoxia-induced cardiomyocyte apoptosis [63], whereas more recent studies demonstrated that p53 inhibitor pifithrin-α attenuated I/R-induced infarct size similarly to ischemic pre-conditioning [64, 65]. Another work observed a slight improvement of functional recovery upon I/R in PUMA (p53-upregulated modulator of apoptosis)—negative mice suggesting that, to some extent, p53 might contribute to I/R injury [66].
In contrast to Bak, which constitutively resides at the OMM, Bax is largely present in the cytosol in non-stressed cells [67]. p53, as a transcription factor, transactivates a large series of pro-apoptotic proteins from the Bcl-2 family, in particular Bax, Bid, Puma, Noxa, with the latter two capable of inducing the activation of Bax (Fig. 3). Upon activation, soluble Bax in the cytosol undergoes conformational changes, homo-oligomerizes and inserts into the OMM, thereby inducing membrane permeabilization, cytochrome c release and caspase-3 activation [67]. Other studies showed that cytosolic p53 can directly activate Bax and thereby induce apoptosis [68], although the exact mechanism by which p53 directly activates Bax is still under debate.
It is becoming evident that Bcl-2 family proteins play a central role in regulating apoptosis in the cardiovascular system. Pro- and anti-apoptotic Bcl-2 family proteins are both expressed in the myocardium during development and during adulthood. In the human heart, the ratio of pro- to anti-apoptotic Bcl-2 proteins has been shown to shift toward pro-apoptotic in various pathological processes such as in ischemic heart disease [67].
Pro-apoptotic Bcl-2 proteins have been implicated in the pathogenesis of various cardiac conditions, including I/R. Bax has been reported to be activated in cardiac cells in response to oxidative stress [69]. In healthy cells, Bax is localized in the cytosol and upon a cell death signal, Bax rapidly translocates to mitochondria, whereas Bak is already present in the mitochondria as an integral membrane protein (Fig. 1, 3) [70]. Interestingly, Bcl-2 is also considered to regulate the MPTP. For instance, Bcl-2 has been shown to prevent permeabilization of the OMM by inhibiting activation of Bax/Bak [71] and increase the calcium threshold for MPTP opening in heart mitochondria by blocking opening of the pore [72]. Capano and Crompton [73] showed that Bax translocation to the mitochondria during ischemia was dependent on AMP activated protein kinase and p38 MAPK in neonatal cardiac myocytes.
Anti-apoptotic Bcl-2 proteins have therapeutic potential for heart disease, since they have been shown to protect myocardial cells from several stressful events that occur during I/R [29]. Among other relevant effects, Bcl-2 has been shown to block p53-mediated apoptosis in cardiac myocytes [74] and to not only stimulate Na+/Ca2+ exchanger expression in the sarcolemma but also attenuate Na+/Ca2+ exchange in mitochondria [72].
Moreover, transgenic mice overexpressing Bcl-2 in the heart had fewer apoptotic cells, reduced infarct size, improved recovery of cardiac function after I/R [75] and attenuated phenotype in an animal model of cardiomyopathy [76]. One possible consequence of ischemia is the inhibition of electron transport and mitochondrial generation of ATP and the F1Fo-ATPase running in reverse to hydrolyze ATP, which limits the amount of energy available during I/R [77, 78]. Interestingly, Imahashi et al. [79] reported that transgenic mice overexpressing Bcl-2 in the heart showed a decreased rate of ATP decline during ischemia as well as decreased acidification, suggesting that Bcl-2 might provide myocardial protection by inhibiting mitochondrial ATP hydrolysis. In addition, Bcl-2 has been reported to play an important role in pre-conditioning. Exposure of hearts to short cycles of I/R led to significant induction of Bcl-2 expression [80], whereas reduction of Bcl-2 levels via antisense oligonucleotides eliminated delayed ischemic pre-conditioning [81].
Pharmacological Protection of Mitochondria During Ischemia/Reperfusion
Besides self-defense mechanisms, several pharmacological approaches (Fig. 4) have been developed to directly prevent myocardial injury during I/R at the mitochondrial level. Diet, exercise and other prophylactic conducts that result in stress-induced protection can also modulate I/R-induced mitochondria alterations and bring benefits during I/R, although those topics will not be discussed here.
Diagram of apoptosis and changes in mitochondrial physiology caused by cardiac I/R and reference to some drugs that can prevent the alterations. In healthy cardiomyocytes, ROS are kept at harmless levels by the activity of both non-enzymatic and enzymatic antioxidant systems. Among the former, a prominent role is played by reduced glutathione (GSH), thioredoxin (Trx) and NAD(P)H. On the other hand, glutathione- S-transferase (GST), glutathione peroxidase (GPx) and the manganese-dependent superoxide dismutase (Mn-SOD) represent redox-active enzymes. This delicate balance is disrupted when apoptosis is induced, following distinct but sometimes overlapping mechanisms. Δψm dissipation is promoted by pro-apoptotic stimuli as diverse as members of the Bcl-2 family of proteins (Bax, Bak, tBid). p53 protein can block the action of some anti-apoptotic Bcl-2 family proteins (Bcl-xL). Ca2+ and cytosolic metabolites promote the opening of the MPTP with entrance of water (H2O) and solutes and exit of H+ ions. The activation of caspases may degrade OXPHOS subunits. The progressive loss of Δψm is often accompanied by an increased generation of ROS and a decreased ATP production, inducing the functional impairment of mitochondria, by arresting oxidative phosphorylation and inducing the MPTP. This scenario of a bioenergetic crisis that progressively leads the cell to death can be prevented or moderated by some pharmacological drugs during I/R. BB—Beta-adrenergic blockers; ACE inhibitors—Angiotensin I-converting enzyme inhibitors (positive effects clearly demonstrated in chronic models; some studies appear to indicate harmful effects in acute ischemia); Ca2+ Antagonists—calcium channel antagonists; ROS—reactive oxygen species; ATP—adenosine triphosphate; MPTP—mitochondrial permeability transition pore; NO—nitric oxide; K-ATP channel—mitochondrial ATP-sensitive potassium channels. → Stimulatory/Activating effect;  Translocation events and ⊥ Inhibitory effect
Translocation events and ⊥ Inhibitory effect
The objective of the present section is to provide a few examples of strategies that can provide myocardial protection during I/R, through a mitochondrial-mediated effect. Figure 4 depicts the proposed mitochondrial mechanisms of action of the drugs here mentioned, among others also included.
Hemodynamic Drugs
Beta (β) adrenoceptor blocking agents have been shown to have cardioprotective effects on ischemic and hypoxic hearts, including attenuation of arrhythmias, and an overall decrease in mortality in patients with ischemic heart disease [82]. β-adrenoceptor blockers have also been used as an alternative to cardioplegic arrest during coronary artery bypass surgery to reduce ischemic damage [83]. β-blockers are thought to exert beneficial effects on the ischemic heart by lowering myocardial oxygen consumption as a consequence of reduced contractility and heart rate [84]. The beneficial effects are also thought to be due to their antioxidant properties [85]. Early studies demonstrated that in animal models of ischemia, the addition of propranolol to hearts previously to ischemia preserved oxidative phosphorylation and Ca2+ homeostasis [86]. Later studies showed that nebivolol exerted a protective effect on recovery of cardiac mechanical activity and on mitochondrial function during reperfusion [87]. The same study failed into finding the same protective activity for atenolol in the isolated working rabbit heart [87].
A fair amount of work has been performed by our group in one particular β-blocker, carvedilol and in its ability to provide protection of cardiac mitochondrial function.
Carvedilol is clinically used for the treatment of congestive heart failure, mild-to-moderate hypertension and myocardial infarction [88]. Carvedilol competitively blocks β1, β2 and α1-adrenoceptors, thereby showing a marked vasodilating property. Carvedilol induces a marked reduction in infarct size in animal models of myocardial ischemia, especially those in which ROS are important in the development and expansion of the infarction area [89]. Of uttermost importance are carvedilol antioxidant properties, which are responsible for the additional cardioprotection not shared by other β-adrenoceptor antagonists [90, 91]. The potential role of the antioxidant properties of carvedilol in the prevention of apoptotic cell death has been also reported [92, 93]. The protective effects of carvedilol on ischemic heart disease may be predominantly from the protection of mitochondrial function [89, 94, 95]. Several published works demonstrated the effectiveness of carvedilol as an antioxidant agent [88, 96]. Various mechanisms have been put forward to explain carvedilol antioxidant properties, including (a) direct inhibition of the cytotoxic activity of ROS, (b) blocking of ROS inhibitory effect on NO-mediated vasodilation, (c) prevention of ROS-mediated activation of transcription-regulating factors such as NFkB, of oxidative stress-activated protein kinases and (d) by indirectly preventing exhaustion of endogenous antioxidant networks [89]. However, not all authors accept that carvedilol acts through a mechanism that involves direct inactivation of ROS; some consider that carvedilol antioxidant action is due to its ability to scavenge iron ions, which can exacerbate oxidative phenomena [97]. Oliveira et al. has shown that carvedilol can prevent the MPT in rat heart by inhibiting the formation of high-conductance pores. The underlying mechanism appears to be the prevention of oxidation of membrane thiol groups, which are important in the formation of the MPTP [94, 98, 99]. Besides the cardioprotective properties described, members of our research team have reported that carvedilol inhibits the exogenous NADH dehydrogenase in rat heart mitochondria [100], which is described to play a key role in the cardiotoxicity of doxorubicin [101]. In agreement, we have published that carvedilol is able to prevent doxorubicin-induced in vivo cardiac mitochondrial toxicity [95]. Interestingly, it has also been described that carvedilol inhibits mitochondrial complex I [96], although the relevance of this effect on myocardial protection during I/R is still subject to discussion. We have also demonstrated that carvedilol behaves as a weak protonophore, which is useful to decrease the amount of ROS produced by the respiratory chain [102].
As described earlier, calcium overload contributes to I/R injury as it may induce excessive myofilament activation at the moment of reoxygenation and in addition, the rise in intracellular calcium contributes to an increase in mitochondrial calcium, which can cause the MPT, decreasing mitochondrial ability to generate ATP, limiting metabolic recovery of the myocyte. Also, a number of calcium-activated proteases may destroy critical intracellular structures and mitochondria phosphorylative capacity [103]. Verapamil, as a type l-calcium channel blocker, minimizes calcium-induced alterations, which may explain its classic cardioprotective effect [104]. HO-4038, a novel verapamil derivative, was recently described as significantly protecting against I/R-induced cardiac dysfunction and damage through the combined beneficial actions of calcium channel blocking, antioxidant and pro-survival signaling activities, which may involve mitochondria [105]. Diltiazem, another calcium antagonist, has also been shown to prevent Ca2+ uptake in mitochondria, mitochondrial swelling, as well as to preserve ATP levels in in vivo and ex vivo animal I/R models [106, 107].
Angiotensin converting enzyme (ACE) inhibitors reduce reperfusion arrhythmias and infarct size and result in improved functional recovery. One example is captopril, which exerts a protective role against I/R injury related with free radical scavenging [108]. In animal models of ischemia, captopril improves the respiratory control ratio (RCR), which may be related to protection of reduced protein thiol groups [109] or reduced ROS generation [108]. In animal models of ischemic heart failure, continuous administration of ACE inhibitors led to reduction in blood pressure and left ventricular end-diastolic pressure and limited the fall in cardiac output and ejection fraction. In these animals, ACE inhibitors (Captopril, Enalapril and Trandolapril) reversed the decrease in mitochondrial ATP levels, creatine phosphate and creatine [110]. Interestingly, in an animal model of prolonged acute ischemia, enalapril had a negative effect on the activity of complex I reducing the available energy charge [111]. These results appear to confirm clinical findings showing that in contrast to chronic ischemia, enalapril therapy started within 24 h of the onset of acute myocardial infarction does not improve survival during the 180 days after infarction [112].
A study in an ex vivo animal model submitted to global acute ischemia allowed to better understand the mechanisms of valsartan cytoprotection on mitochondrial function. Valsartan, an angiotensin II-type I receptor blocker, acts preferentially in the mitochondrial phosphorylation apparatus, increasing ATP/ADP ratios and decreasing the phosphorylative lag phase, which enables for a higher energy production in hearts submitted to acute ischemia, in which energy is critical to preserve mitochondrial function [113].
Amiodarone, which is usually used as an anti-arrhythmic, has also been shown to have cardioprotective properties based on mitochondrial effects. It has also been demonstrated that amiodarone inhibits the activity of carnitine palmitoyltransferase-1, an enzyme involved in the metabolism of fatty acids, a potentially harmful energy substrate in situations of ischemia [114]. Amiodarone was shown to prevent induction of the MPTP on heart mitochondria, while being toxic to mitochondria from other tissues [115]. The same study demonstrated protection against cardiac I/R damage in Langendorff-perfused heart [115]. The different sensitivities of the tissues toward amiodarone can be involved in the beneficial cardiac and the simultaneous non-cardiac toxic effects of the drug [115].
Metabolic and Mitochondrial Drugs
Recent advances in our understanding of cellular and molecular biology of ischemia have identified a series of molecules whose beneficial effect in ischemia is not associated with significant alterations of cardiac hemodynamics, one particular example being trimetazidine.
During ischemia, the oxidation of lipid substrates is suddenly blocked, while it sharply increases during reperfusion, leading to the accumulation of various potentially toxic metabolites that may alter Ca2+ kinetics, leading to arrhythmias, a process that can be inhibited by trimetazidine [116]. Part of trimetazidine anti-ischemic effect may be due to “metabolic shift”, i.e., the induction of preferential consumption of glucose and its metabolites in detriment of fatty acid oxidation [117]. By reducing the accumulation of acylcarnitine and lipid oxidation during reperfusion, trimetazidine reduces the quantity of harmful metabolites derived from fatty acids, which compromise cardiac function [118].
Several studies suggest that trimetazidine may also act directly on different mitochondrial targets to improve the organelle function [119]. In studies on isolated cardiac myocytes, Guarnieri et al. found an increase in Ca2+ uptake by mitochondria [120]. According to the authors, the finding suggests that one of trimetazidine mechanisms is the increase in mitochondrial Ca2+ levels, thus promoting increased ATP synthesis [120]. In other studies performed in an ex vivo animal model of prolonged acute ischemia, trimetazidine was shown to increase the activity of complex I, leading to more efficient O2 consumption in the metabolism of glucose compounds. This action in itself may lead to lower ROS production and improvement in membrane integrity, preserving electrochemical gradients [121] (Fig. 4).
Phosphodiesterase-5 (PDE-5) inhibitors, including Levitra and Viagra, may have a new utility in cardiac protection, in addition to their well-known use for the management of erectile dysfunction in men. Kukreja and his team demonstrated for the first time that pre-treatment with a clinically relevant dose of levitra, generically known as vardenafil, induces a protective effect against heart attack injury by opening mitochondrial K+-ATP channel in an animal model [122]. PDE-5 is an enzyme responsible for removing cGMP, an intracellular messenger molecule in heart cells. Sildenafil, like vardenafil, stabilizes mitochondria and protects against I/R damage of the heart by opening mitochondrial K+-ATP channels in cardiac cells. Additional studies show that sildenafil attenuates cell death resulting from necrosis and apoptosis and increases Bcl-2/Bax ratio through NO signaling in adult cardiomyocytes submitted to I/R [123, 124]. Custódio et al. concluded that sildenafil citrate concentrations of up to 50 μM do not affect either rat heart mitochondrial bioenergetics or Ca2+-induced MPT, but it depresses H2O2 generation by acting as a superoxide dismutase (SOD)-mimetic [125]. More recently, the results obtained by Wang et al. suggest that activation of mitoK (Ca) and mitoK (ATP) are both crucial for maintaining mitochondrial homeostasis and reducing cell death in sildenafil-induced pre-conditioning against I/R injury [126]. An important question was concerned the safety of PDE-5 inhibitors. Despite theoretical concerns of a reduced myocardial tolerance to ischemia or promoting cardiac arrhythmias, randomised trials and retrospective analyses do not support an increased cardiac risk with oral treatment [127].
Several studies have shown that K+-ATP channel openers such as diazoxide in moderate doses can be useful in ischemia and I/R [128–130], because it is able to induce an effect similar to ischemic pre-conditioning, attenuating intracellular acidification caused by ischemia and facilitating heart recovery. Diazoxide-mediated cardioprotection is supported by a moderate ROS production during the pre-conditioning phase that induces the opening of K+-ATP channels, preserving mitochondrial volume and the structure of the intermembrane space, which in turn leads to a reduction in ATP hydrolysis, also due to decreased disturbance of mitochondrial Ca2+ homeostasis. So, a strong decrease in oxidant generation during the subsequent ischemic and reperfusion phases is observed [131]. The combination of all these factors also prevents induction of the MPT, with release of cytochrome c, and consequent cell death [132, 133] (Fig. 4). Studies on animal models have clearly shown that nicorandil reduces infarct size [134]. By reducing oxidative stress during reperfusion [135], nicorandil preserves mitochondrial function [136] and thereby prevents ischemia-induced cell death [137].
As previously described, evidence has accumulated indicating that a sudden change in the permeability of the mitochondrial membranes by opening of a high-conductance pore (MPTP) may be another important mechanism for reperfusion-induced cell necrotic or apoptotic death [24]. Inhibition of MPTP opening is a good candidate mechanism to prevent severe heart injury from I/R. MPTP inhibition can result in prevention of cardiac cell death, limiting the loss of cardiac cells [138]. Cyclosporin-A (CsA) binds to cyclophilin-D (CyP-D), a matrix peptidyl-prolylcis-trans isomerase, [139] which is located in the mitochondrial matrix and is thought to interact with the ANT [140]. Definitive support to the role of MPTP opening inhibition through modulation of its interaction with CyP-D was recently provided by the reduced susceptibility to ischemic injury observed in mice lacking CyP-D [141, 142]. Despite the problems associated, CsA can be a mediator of protection against ischemia-triggered damage in the heart [143]. The addition of CsA as a pharmacological strategy is not free of problems because CsA also inhibits calcineurin and interfere with the maintenance of ionic gradients [144]. The future will tell whether other CyP-D ligands, preferentially not exerting immunosuppressive side effects through the inhibition of calcineurin, may achieve therapeutic responses in the clinics.
l-Carnitine facilitates the transport of fatty acids into the mitochondrial matrix in order to be used for energy production. Recent studies have shown that l-carnitine and analogous compounds are capable of protecting the heart against I/R injury [145]. The mechanism of action, however, is not yet understood. The functions of carnitine in both energy metabolism and phospholipid turnover indicate a general role of this compound in the maintenance of cardiomyocyte viability. The cytoprotective role is likely to be contributed by the inhibitory effects on ceramide synthesis [146] and caspase activities [147]. Carnitine has been shown to inhibit the activity of caspases 3 and 8 [147], which act as initiator and executioner of apoptosis, respectively.
Antioxidants
As previously described, it is widely recognized that mitochondrial oxidative stress is an important factor in I/R injury [148]. The use of antioxidants to prevent cardiac I/R injury appears to be a logic measure to improve myocyte survival.
The cardioprotective effects of edaravone, a novel free radical scavenger, were more remarkable than that of other well-known antioxidants, such as ascorbate and SOD, and were mediated by reducing intracellular generation of ROS [149]. Edaravone also alleviated the cell injury induced by exogenous oxidative stress (H2O2) [149], directly neutralizing peroxy radicals (LOO°) but not O2 − [150]. Rajesh et al. (2003) demonstrated that the MPT inhibiting property of edaravone was specific for the attenuation of cytochrome c release, thereby pathological apoptosis was decreased in rat hearts in vivo [151]. Recently, edaravone has demonstrated to be equally useful as a cardioplegic adjuvant for heart preservation [152].
Pyruvate is known for its antioxidant properties in the myocardium due to its chemical structure and the pattern of its cellular metabolism [153]. It has been shown that pyruvate also increases contractile performance in the heart and protects the organ during I/R [153, 154]. Besides being a ROS scavenger, pyruvate is considered a good mitochondrial fuel, also contributing to increase ATP production and inhibiting the induction of the MPTP [155].
Many different radical scavengers have been used both in vivo and in vitro to target the critical moment of ROS burst upon reperfusion [156]. However, the cardioprotective effects of antioxidants against I/R injury are not consistent. One reason for this discrepancy may be the differences among the drugs regarding the accessibility to myocytes during the so called “window of protection”. Furthermore, it has been reported that a small redox-dependent signal, derived from ROS and preceding ischemia, is cardioprotective, but that large bursts of oxidants contribute to cell death during I/R [157]. This paradoxical involvement of ROS may complicate the elucidation of the roles of ROS and radical scavengers in cardioprotection. It is also known that available antioxidants have not proven to be especially effective against I/R damage. It is possible that most antioxidants do not reach the relevant sites of ROS generation, especially if mitochondria are the primary source of ROS. The use of mitochondrial-targeted antioxidants is now increasing, which may be useful to prevent I/R damage to mitochondria [158–160]. One very relevant piece of work suggests that mitochondria-targeted plastoquinone derivatives maybe extremely effective in preventing reperfusion-induced damage to cardiac mitochondria [159]. In theory, by covalently attaching a tetraphenylphosphonium cation (TPP) to a desired molecule, the complex is selectively delivered to mitochondria and protects the organelle from oxidative damage more effectively than vitamin E (α-tocopherol) itself [161]. MitoQ, an analog of endogenous ubiquinone, was shown to protect against I/R-induced decrease in RCR, damage to complex I and decrease in aconitase activity [158], whereas untargeted antioxidants such as ubiquinone or TPP were ineffective.
These references point to the importance of the mitochondrial localization of the drug for its therapeutic potential. These examples suggest that it might be possible to design small molecule inhibitors of pathogenic cell death with a selective action exerted at the mitochondrial level. Melatonin, a pineal hormone, is well known as a potent antioxidant in a variety of I/R models. Giacomo et al. (2007) reported that melatonin or 5-methoxy-carbonylamino-N-acetyl-tryptamine (5-MCA-NAT), a structurally related indole compound, protects against I/R injury to the isolated rat heart [162]. Melatonin has been shown to effectively protect against I/R myocardial damage [163, 164]. The mechanism by which melatonin exerts this cardioprotective effect is not well established. Petrosillo et al. examined the effects of melatonin on various parameters of mitochondrial bioenergetics in a Langerdoff isolated perfused rat heart model and proposed that melatonin prevented the alterations induced by reperfusion on mitochondrial oxygen consumption, complex I and complex III activity, H2O2 production as well as on the degree of cardiolipin oxidation [165].
A variety of experimental models established estrogens as critical mediators of cardioprotection, which explains the evolutionary advantage of females [166]. Estrogens have been demonstrated to reduce the extent of irreversible myocardial injury, ventricular arrhythmias and infarct size after I/R [167]. Non-transcriptional actions of estrogens in myocardial I/R have been suggested to be due to stimulation of NO production, inhibition of myocardial calcium accumulation, preservation of mitochondrial structure and function and antioxidant action [168–170]. Interestingly, estrogens improve not only female but also male cardiac function after I/R [167]. Estradiol hormone in mitochondria can act on membranes directly or indirectly through estrogen receptors that have been identified in mitochondria [171]. In isolated mitochondria, exogenously added estradiol has been shown to inhibit MPTP- related release of cytochrome c from mitochondria induced by high calcium concentrations [172]. In addition, estradiol inhibits oxidative stress [173]; therefore, the protective effect of estradiol after I/R might be induced by its antioxidant action on mitochondrial membrane integrity.
Concluding Remarks
The present review points out that mitochondria are critical in the context of myocardial survival post-I/R. A wide number of publications describe strategies aimed at minimizing myocardial damage with the use of agents that recover mitochondrial function not only to provide the myocyte with increased ATP, but also to prevent mitochondrial membrane permeabilization that leads to cell death. The present review highlights some pharmacological strategies that target specific events that occur during I/R, including oxidative stress and calcium overload.
It is important to say that most experimental studies on cardioprotection have been undertaken in animal models, in which I/R is imposed in the absence of other disease processes. However, ischemic heart disease in humans is a complex disorder caused by or associated with known cardiovascular risk factors. Wanga et al. alerted to the possible interaction of risk factors on the consequences and role of I/R pharmacological protection [174], referring that the large majority of data demonstrating protection against I/R injury have been obtained in experiments on healthy animals with normal vascular function. However, most patients with an acute myocardial infarction for example have several risk factors for coronary artery disease such as hypercholesterolemia, diabetes, hypertension and atherosclerosis. It is not obvious that the pharmacological agents here discussed will afford a similar degree of cardioprotection under such conditions. It is obvious that much research remains to be done in order to understand the interactions between self-defense mechanisms, exogenous or stress-induced mitochondrial alterations in cardiac physiology, pathology and pharmacology.
Several aspects have to be taken into account when the use of a new mitochondrial protective agent is proposed. One of such aspects is the correct delivery to the heart, which in vivo may be difficult to obtain. A second important aspect is the buildup of effective concentrations in mitochondria. This is an important point in what concerns, for example, with antioxidants. We have demonstrated that α-tocopherol succinate, despite a recognized antioxidant activity in the liver, could not be accumulated in effective concentrations in cardiac mitochondria in order to prevent doxorubicin oxidative damage [175]. Also a very critical issue is the window of time in which the drug should be applied in order to rescue the heart from I/R damage.
If we add to the above described the fact there are still several unknowns in the pathophysiology of cardiac I/R, there is still a blank book to be written. The future will tell whether the protection/restoration of mitochondrial function in I/R will be the key to improve the quality of life of many patients worldwide. It is clear now that the closure of the box will protect the organ.
References
Hearse, D. J. (1990). Ischemia, reperfusion, and the determinants of tissue injury. Cardiovascular Drugs and Therapy, 4(Suppl 4), 767–776.
Holleyman, C. R., & Larson, D. F. (2001). Apoptosis in the ischemic reperfused myocardium. Perfusion, 16, 491–502.
Marczin, N., El-Habashi, N., Hoare, G. S., Bundy, R. E., & Yacoub, M. (2003). Antioxidants in myocardial ischemia–reperfusion injury: Therapeutic potential and basic mechanisms. Archives of Biochemistry and Biophysics, 420, 222–236.
Ferrari, R., Curello, S., Boffa, G. M., Condorelli, E., Pasini, E., Guarnieri, G., et al. (1989). Oxygen free radical-mediated heart injury in animal models and during bypass surgery in humans. Effects of alpha-tocopherol. Annals of the New York Academy of Sciences, 570, 237–253.
Ambrosio, G., Zweier, J. L., Duilio, C., Kuppusamy, P., Santoro, G., Elia, P. P., et al. (1993). Evidence that mitochondrial respiration is a source of potentially toxic oxygen free radicals in intact rabbit hearts subjected to ischemia and reflow. The Journal of Biological Chemistry, 268, 18532–18541.
Nagy, N., Malik, G., Tosaki, A., Ho, Y. S., Maulik, N., & Das, D. K. (2008). Overexpression of glutaredoxin-2 reduces myocardial cell death by preventing both apoptosis and necrosis. Journal of Molecular and Cellular Cardiology, 44, 252–260.
Chen, Z., Siu, B., Ho, Y. S., Vincent, R., Chua, C. C., Hamdy, R. C., et al. (1998). Overexpression of MnSOD protects against myocardial ischemia/reperfusion injury in transgenic mice. Journal of Molecular and Cellular Cardiology, 30, 2281–2289.
Li, G., Chen, Y., Saari, J. T., & Kang, Y. J. (1997). Catalase-overexpressing transgenic mouse heart is resistant to ischemia–reperfusion injury. American Journal of Physiology, 273, H1090–H1095.
Yoshida, T., Watanabe, M., Engelman, D. T., Engelman, R. M., Schley, J. A., Maulik, N., et al. (1996). Transgenic mice overexpressing glutathione peroxidase are resistant to myocardial ischemia reperfusion injury. Journal of Molecular and Cellular Cardiology, 28, 1759–1767.
Lemieux, H., & Hoppel, C. L. (2009). Mitochondria in the human heart. Journal of Bioenergetics and Biomembranes, 41, 99–106.
Riva, A., Tandler, B., Loffredo, F., Vazquez, E., & Hoppel, C. (2005). Structural differences in two biochemically defined populations of cardiac mitochondria. American Journal of Physiology Heart and circulatory Physiology, 289, H868–H872.
Palmer, J. W., Tandler, B., & Hoppel, C. L. (1977). Biochemical properties of subsarcolemmal and interfibrillar mitochondria isolated from rat cardiac muscle. The Journal of Biological Chemistry, 252, 8731–8739.
Palmer, J. W., Tandler, B., & Hoppel, C. L. (1985). Biochemical differences between subsarcolemmal and interfibrillar mitochondria from rat cardiac muscle: Effects of procedural manipulations. Archives of Biochemistry and Biophysics, 236, 691–702.
Lesnefsky, E. J., Slabe, T. J., Stoll, M. S., Minkler, P. E., & Hoppel, C. L. (2001). Myocardial ischemia selectively depletes cardiolipin in rabbit heart subsarcolemmal mitochondria. American Journal of Physiology Heart and Circulatory Physiology, 280, H2770–H2778.
Lesnefsky, E. J., Tandler, B., Ye, J., Slabe, T. J., Turkaly, J., & Hoppel, C. L. (1997). Myocardial ischemia decreases oxidative phosphorylation through cytochrome oxidase in subsarcolemmal mitochondria. American Journal of Physiology, 273, H1544–H1554.
Duan, J., & Karmazyn, M. (1989). Relationship between oxidative phosphorylation and adenine nucleotide translocase activity of two populations of cardiac mitochondria and mechanical recovery of ischemic hearts following reperfusion. Canadian Journal of Physiology and Pharmacology, 67, 704–709.
Loos, B., & Engelbrecht, A. M. (2009). Cell death: A dynamic response concept. Autophagy, 5, 590–603.
Mani, K. (2008). Programmed cell death in cardiac myocytes: Strategies to maximize post-ischemic salvage. Heart Failure Reviews, 13, 193–209.
Dhesi, P., Tehrani, F., Fuess, J., & Schwarz, E. R. (2009). How does the heart (not) die? The role of autophagy in cardiomyocyte homeostasis and cell death. Heart Failure Reviews, in press.
Gustafsson, A. B., & Gottlieb, R. A. (2008). Eat your heart out: Role of autophagy in myocardial ischemia/reperfusion. Autophagy, 4, 416–421.
Hamacher-Brady, A., Brady, N. R., & Gottlieb, R. A. (2006). The interplay between pro-death and pro-survival signaling pathways in myocardial ischemia/reperfusion injury: apoptosis meets autophagy. Cardiovascular Drugs and Therapy, 20, 445–462.
Lee, Y., & Gustafsson, A. B. (2009). Role of apoptosis in cardiovascular disease. Apoptosis, 14, 536–548.
Gupta, S. (2003). Molecular signaling in death receptor and mitochondrial pathways of apoptosis (Review). International Journal of Oncology, 22, 15–20.
Baines, C. P. (2009). The mitochondrial permeability transition pore and ischemia–reperfusion injury. Basic Research in Cardiology, 104, 181–188.
Riedl, S. J., & Salvesen, G. S. (2007). The apoptosome: Signalling platform of cell death. Nature Reviews Molecular Cell Biology, 8, 405–413.
Buja, L. M. (2005). Myocardial ischemia and reperfusion injury. Cardiovascular Pathology, 14, 170–175.
Freude, B., Masters, T. N., Robicsek, F., Fokin, A., Kostin, S., Zimmermann, R., et al. (2000). Apoptosis is initiated by myocardial ischemia and executed during reperfusion. Journal of Molecular and Cellular Cardiology, 32, 197–208.
Lee, P., Sata, M., Lefer, D. J., Factor, S. M., Walsh, K., & Kitsis, R. N. (2003). Fas pathway is a critical mediator of cardiac myocyte death and MI during ischemia–reperfusion in vivo. American Journal of Physiology Heart and Circulatory Physiology, 284, H456–H463.
Chen, Z., Chua, C. C., Ho, Y. S., Hamdy, R. C., & Chua, B. H. (2001). Overexpression of Bcl-2 attenuates apoptosis and protects against myocardial I/R injury in transgenic mice. American Journal of Physiology Heart and Circulatory Physiology, 280, H2313–H2320.
Bialik, S., Cryns, V. L., Drincic, A., Miyata, S., Wollowick, A. L., Srinivasan, A., et al. (1999). The mitochondrial apoptotic pathway is activated by serum and glucose deprivation in cardiac myocytes. Circulation Research, 85, 403–414.
Gottlieb, R. A., Burleson, K. O., Kloner, R. A., Babior, B. M., & Engler, R. L. (1994). Reperfusion injury induces apoptosis in rabbit cardiomyocytes. Journal of Clinical Investigation, 94, 1621–1628.
Zhao, Z. Q., & Vinten-Johansen, J. (2002). Myocardial apoptosis and ischemic preconditioning. Cardiovascular Research, 55, 438–455.
Black, S. C., Huang, J. Q., Rezaiefar, P., Radinovic, S., Eberhart, A., Nicholson, D. W., et al. (1998). Co-localization of the cysteine protease caspase-3 with apoptotic myocytes after in vivo myocardial ischemia and reperfusion in the rat. Journal of Molecular and Cellular Cardiology, 30, 733–742.
Chakrabarti, S., Hoque, A. N., & Karmazyn, M. (1997). A rapid ischemia-induced apoptosis in isolated rat hearts and its attenuation by the sodium-hydrogen exchange inhibitor HOE 642 (cariporide). Journal of Molecular and Cellular Cardiology, 29, 3169–3174.
Borutaite, V., Budriunaite, A., Morkuniene, R., & Brown, G. C. (2001). Release of mitochondrial cytochrome c and activation of cytosolic caspases induced by myocardial ischaemia. Biochimica et Biophysica Acta, 1537, 101–109.
Borutaite, V., Jekabsone, A., Morkuniene, R., & Brown, G. C. (2003). Inhibition of mitochondrial permeability transition prevents mitochondrial dysfunction, cytochrome c release and apoptosis induced by heart ischemia. Journal of Molecular and Cellular Cardiology, 35, 357–366.
Akiyama, K., Gluckman, T. L., Terhakopian, A., Jinadasa, P. M., Narayan, S., Singaswamy, S., et al. (1997). Apoptosis in experimental myocardial infarction in situ and in the perfused heart in vitro. Tissue and Cell, 29, 733–743.
Zhao, Z. Q. (2004). Oxidative stress-elicited myocardial apoptosis during reperfusion. Current Opinion in Pharmacology, 4, 159–165.
Kagan, V. E., Tyurina, Y. Y., Bayir, H., Chu, C. T., Kapralov, A. A., Vlasova, I. I., et al. (2006). The “pro-apoptotic genies” get out of mitochondria: Oxidative lipidomics and redox activity of cytochrome c/cardiolipin complexes. Chemico Biological Interactions, 163, 15–28.
St-Pierre, J., Brand, M. D., & Boutilier, R. G. (2000). Mitochondria as ATP consumers: Cellular treason in anoxia. Proceedings of the National Academy of Sciences of the United States of America, 97, 8670–8674.
Chen, Q., Moghaddas, S., Hoppel, C. L., & Lesnefsky, E. J. (2008). Ischemic defects in the electron transport chain increase the production of reactive oxygen species from isolated rat heart mitochondria. American Journal of Physiology Cell Physiology, 294, C460–C466.
Andreyev, A. Y., Kushnareva, Y. E., & Starkov, A. A. (2005). Mitochondrial metabolism of reactive oxygen species. Biochemistry (Mosc), 70, 200–214.
Ferrari, R., Ceconi, C., Curello, S., Cargnoni, A., De Giuli, F., & Visioli, O. (1992). Occurrence of oxidative stress during myocardial reperfusion. Molecular and Cellular Biochemistry, 111, 61–69.
Dhalla, N. S., Elmoselhi, A. B., Hata, T., & Makino, N. (2000). Status of myocardial antioxidants in ischemia–reperfusion injury. Cardiovascular Research, 47, 446–456.
Ferrari, R., Guardigli, G., Mele, D., Percoco, G. F., Ceconi, C., & Curello, S. (2004). Oxidative stress during myocardial ischaemia and heart failure. Current Pharmaceutical Design, 10, 1699–1711.
Powers, S. K., Murlasits, Z., Wu, M., & Kavazis, A. N. (2007). Ischemia–reperfusion-induced cardiac injury: A brief review. Medicine and Science in Sports and Exercise, 39, 1529–1536.
Halestrap, A. P. (2009). What is the mitochondrial permeability transition pore? Journal of Molecular and Cellular Cardiology, 46, 821–831.
Zamzami, N., Marchetti, P., Castedo, M., Hirsch, T., Susin, S. A., Masse, B., et al. (1996). Inhibitors of permeability transition interfere with the disruption of the mitochondrial transmembrane potential during apoptosis. FEBS Letters, 384, 53–57.
Skulachev, V. P. (2000). How proapoptotic proteins can escape from mitochondria? Free Radical Biology and Medicine, 29, 1056–1059.
Borutaite, V., & Brown, G. C. (2003). Mitochondria in apoptosis of ischemic heart. FEBS Letters, 541, 1–5.
Baines, C. P. (2009). The molecular composition of the mitochondrial permeability transition pore. Journal of Molecular and Cellular Cardiology, 46, 850–857.
Javadov, S., & Karmazyn, M. (2007). Mitochondrial permeability transition pore opening as an endpoint to initiate cell death and as a putative target for cardioprotection. Cellular Physiology and Biochemistry, 20, 1–22.
Kim, J. S., He, L., & Lemasters, J. J. (2003). Mitochondrial permeability transition: A common pathway to necrosis and apoptosis. Biochemical and Biophysical Research Communications, 304, 463–470.
Dedkova, E. N., & Blatter, L. A. (2008). Mitochondrial Ca2+ and the heart. Cell Calcium, 44, 77–91.
Dong, Z., Saikumar, P., Weinberg, J. M., & Venkatachalam, M. A. (2006). Calcium in cell injury and death. Annu Rev Pathol, 1, 405–434.
Chen, M., Won, D. J., Krajewski, S., & Gottlieb, R. A. (2002). Calpain and mitochondria in ischemia/reperfusion injury. The Journal of Biological Chemistry, 277, 29181–29186.
Novgorodov, S. A., & Gudz, T. I. (2009). Ceramide and mitochondria in ischemia/reperfusion. Journal of Cardiovascular Pharmacology, 53, 198–208.
Vaseva, A. V., & Moll, U. M. (2009). The mitochondrial p53 pathway. Biochimica et Biophysica Acta, 1787, 414–420.
Marchenko, N. D., Zaika, A., & Moll, U. M. (2000). Death signal-induced localization of p53 protein to mitochondria. A potential role in apoptotic signaling. The Journal of Biological Chemistry, 275, 16202–16212.
Erster, S., Mihara, M., Kim, R. H., Petrenko, O., & Moll, U. M. (2004). In vivo mitochondrial p53 translocation triggers a rapid first wave of cell death in response to DNA damage that can precede p53 target gene activation. Molecular and Cellular Biology, 24, 6728–6741.
Park, B. S., Song, Y. S., Yee, S. B., Lee, B. G., Seo, S. Y., Park, Y. C., et al. (2005). Phospho-ser 15–p53 translocates into mitochondria and interacts with Bcl-2 and Bcl-xL in eugenol-induced apoptosis. Apoptosis, 10, 193–200.
Mihara, M., Erster, S., Zaika, A., Petrenko, O., Chittenden, T., Pancoska, P., et al. (2003). p53 has a direct apoptogenic role at the mitochondria. Molecular Cell, 11, 577–590.
Webster, K. A., Discher, D. J., Kaiser, S., Hernandez, O., Sato, B., & Bishopric, N. H. (1999). Hypoxia-activated apoptosis of cardiac myocytes requires reoxygenation or a pH shift and is independent of p53. Journal of Clinical Investigation, 104, 239–252.
Mocanu, M. M., & Yellon, D. M. (2003). p53 down-regulation: A new molecular mechanism involved in ischaemic preconditioning. FEBS Letters, 555, 302–306.
Liu, P., Xu, B., Cavalieri, T. A., & Hock, C. E. (2008). Inhibition of p53 by pifithrin-alpha reduces myocyte apoptosis and leukocyte transmigration in aged rat hearts following 24 hours of reperfusion. Shock, 30, 545–551.
Toth, A., Jeffers, J. R., Nickson, P., Min, J. Y., Morgan, J. P., Zambetti, G. P., et al. (2006). Targeted deletion of Puma attenuates cardiomyocyte death and improves cardiac function during ischemia–reperfusion. American Journal of Physiology Heart and Circulatory Physiology, 291, H52–H60.
Adams, J. M., & Cory, S. (2007). Bcl-2-regulated apoptosis: Mechanism and therapeutic potential. Current Opinion in Immunology, 19, 488–496.
Chipuk, J. E., Maurer, U., Green, D. R., & Schuler, M. (2003). Pharmacologic activation of p53 elicits Bax-dependent apoptosis in the absence of transcription. Cancer Cell, 4, 371–381.
Kumar, D., & Jugdutt, B. I. (2003). Apoptosis and oxidants in the heart. Journal of Laboratory and Clinical Medicine, 142, 288–297.
Kuwana, T., Mackey, M. R., Perkins, G., Ellisman, M. H., Latterich, M., Schneiter, R., et al. (2002). Bid, Bax, and lipids cooperate to form supramolecular openings in the outer mitochondrial membrane. Cell, 111, 331–342.
Gustafsson, A. B., & Gottlieb, R. A. (2007). Bcl-2 family members and apoptosis, taken to heart. American Journal of Physiology Cell Physiology, 292, C45–C51.
Zhu, L., Yu, Y., Chua, B. H., Ho, Y. S., & Kuo, T. H. (2001). Regulation of sodium-calcium exchange and mitochondrial energetics by Bcl-2 in the heart of transgenic mice. Journal of Molecular and Cellular Cardiology, 33, 2135–2144.
Capano, M., & Crompton, M. (2006). Bax translocates to mitochondria of heart cells during simulated ischaemia: involvement of AMP-activated and p38 mitogen-activated protein kinases. Biochemical Journal, 395, 57–64.
Kirshenbaum, L. A., & de Moissac, D. (1997). The bcl-2 gene product prevents programmed cell death of ventricular myocytes. Circulation, 96, 1580–1585.
Brocheriou, V., Hagege, A. A., Oubenaissa, A., Lambert, M., Mallet, V. O., Duriez, M., et al. (2000). Cardiac functional improvement by a human Bcl-2 transgene in a mouse model of ischemia/reperfusion injury. The Journal of Gene Medicine, 2, 326–333.
Weisleder, N., Taffet, G. E., & Capetanaki, Y. (2004). Bcl-2 overexpression corrects mitochondrial defects and ameliorates inherited desmin null cardiomyopathy. Proceedings of the National Academy of Sciences of the United States of America, 101, 769–774.
Grover, G. J., Marone, P. A., Koetzner, L., & Seto-Young, D. (2008). Energetic signalling in the control of mitochondrial F1F0 ATP synthase activity in health and disease. International Journal of Biochemistry and Cell Biology, 40, 2698–2701.
Classen, J. B., Mergner, W. J., & Costa, M. (1989). ATP hydrolysis by ischemic mitochondria. Journal of Cellular Physiology, 141, 53–59.
Imahashi, K., Schneider, M. D., Steenbergen, C., & Murphy, E. (2004). Transgenic expression of Bcl-2 modulates energy metabolism, prevents cytosolic acidification during ischemia, and reduces ischemia/reperfusion injury. Circulation Research, 95, 734–741.
Maulik, N., Engelman, R. M., Rousou, J. A., Flack, J. E., 3rd, Deaton, D., & Das, D. K. (1999). Ischemic preconditioning reduces apoptosis by upregulating anti-death gene Bcl-2. Circulation, 100, II369–II375.
Hattori, R., Hernandez, T. E., Zhu, L., Maulik, N., Otani, H., Kaneda, Y., et al. (2001). An essential role of the antioxidant gene Bcl-2 in myocardial adaptation to ischemia: an insight with antisense Bcl-2 therapy. Antioxidants & Redox Signaling, 3, 403–413.
Wallace, D. C., Shoffner, J. M., Trounce, I., Brown, M. D., Ballinger, S. W., Corral-Debrinski, M., et al. (1995). Mitochondrial DNA mutations in human degenerative diseases and aging. Biochimica et Biophysica Acta, 1271, 141–151.
Yasuda, T., Kamiya, H., Tanaka, Y., & Watanabe, G. (2001). Ultra-short-acting cardioselective beta-blockade attenuates postischemic cardiac dysfunction in the isolated rat heart. European Journal of Cardio-Thoracic Surgery, 19, 647–652.
Sabbah, H. N. (1999). The cellular and physiologic effects of beta blockers in heart failure. Clinical Cardiology, 22(Suppl 5), V16–V20.
Kawai, K., Qin, F., Shite, J., Mao, W., Fukuoka, S., & Liang, C. S. (2004). Importance of antioxidant and antiapoptotic effects of beta-receptor blockers in heart failure therapy. American Journal of Physiology Heart and Circulatory Physiology, 287, H1003–H1012.
Nayler, W. G., Ferrari, R., & Williams, A. (1980). Protective effect of pretreatment with verapamil, nifedipine and propranolol on mitochondrial function in the ischemic and reperfused myocardium. American Journal of Cardiology, 46, 242–248.
Vandeplassche, G., Lu, H. R., Wouters, L., Flameng, W., & Borgers, M. (1991). Normothermic ischemic cardiac arrest in the isolated working rabbit heart: effects of dl-nebivolol and atenolol. Basic Research in Cardiology, 86, 21–31.
Carreira, R. S., Monteiro, P., Gon Alves, L. M., & Providencia, L. A. (2006). Carvedilol: Just another Beta-blocker or a powerful cardioprotector? Cardiovascular & Hematological Disorders Drug Targets, 6, 257–266.
Oliveira, P. J., Goncalves, L., Monteiro, P., Providencia, L. A., & Moreno, A. J. (2005). Are the antioxidant properties of carvedilol important for the protection of cardiac mitochondria? Current Vascular Pharmacology, 3, 147–158.
Yue, T. L., Cheng, H. Y., Lysko, P. G., McKenna, P. J., Feuerstein, R., Gu, J. L., et al. (1992). Carvedilol, a new vasodilator and beta adrenoceptor antagonist, is an antioxidant and free radical scavenger. Journal of Pharmacology and Experimental Therapeutics, 263, 92–98.
Yue, T. L., McKenna, P. J., Ruffolo, R. R., Jr., & Feuerstein, G. (1992). Carvedilol, a new beta-adrenoceptor antagonist and vasodilator antihypertensive drug, inhibits superoxide release from human neutrophils. European Journal of Pharmacology, 214, 277–280.
Spallarossa, P., Garibaldi, S., Altieri, P., Fabbi, P., Manca, V., Nasti, S., et al. (2004). Carvedilol prevents doxorubicin-induced free radical release and apoptosis in cardiomyocytes in vitro. Journal of Molecular and Cellular Cardiology, 37, 837–846.
Feuerstein, G., Yue, T. L., Ma, X., & Ruffolo, R. R. (1998). Novel mechanisms in the treatment of heart failure: Inhibition of oxygen radicals and apoptosis by carvedilol. Progress in Cardiovascular Diseases, 41, 17–24.
Oliveira, P. J., Esteves, T., Rolo, A. P., Palmeira, C. M., & Moreno, A. J. (2004). Carvedilol inhibits the mitochondrial permeability transition by an antioxidant mechanism. Cardiovascular Toxicology, 4, 11–20.
Oliveira, P. J., Bjork, J. A., Santos, M. S., Leino, R. L., Froberg, M. K., Moreno, A. J., et al. (2004). Carvedilol-mediated antioxidant protection against doxorubicin-induced cardiac mitochondrial toxicity. Toxicology and Applied Pharmacology, 200, 159–168.
Sgobbo, P., Pacelli, C., Grattagliano, I., Villani, G., & Cocco, T. (2007). Carvedilol inhibits mitochondrial complex I and induces resistance to H2O2 -mediated oxidative insult in H9C2 myocardial cells. Biochimica et Biophysica Acta, 1767, 222–232.
Noguchi, N., Nishino, K., & Niki, E. (2000). Antioxidant action of the antihypertensive drug, carvedilol, against lipid peroxidation. Biochemical Pharmacology, 59, 1069–1076.
Oliveira, P. J., Coxito, P. M., Rolo, A. P., Santos, D. L., Palmeira, C. M., & Moreno, A. J. (2001). Inhibitory effect of carvedilol in the high-conductance state of the mitochondrial permeability transition pore. European Journal of Pharmacology, 412, 231–237.
Oliveira, P. J., Rolo, A. P., Palmeira, C. M., & Moreno, A. J. (2001). Carvedilol reduces mitochondrial damage induced by hypoxanthine/xanthine oxidase: Relevance to hypoxia/reoxygenation injury. Cardiovascular Toxicology, 1, 205–213.
Oliveira, P. J., Santos, D. J., & Moreno, A. J. (2000). Carvedilol inhibits the exogenous NADH dehydrogenase in rat heart mitochondria. Archives of Biochemistry and Biophysics, 374, 279–285.
Nohl, H. (1987). Demonstration of the existence of an organo-specific NADH dehydrogenase in heart mitochondria. European Journal of Biochemistry, 169, 585–591.
Oliveira, P. J., Marques, M. P., Batista de Carvalho, L. A., & Moreno, A. J. (2000). Effects of carvedilol on isolated heart mitochondria: Evidence for a protonophoretic mechanism. Biochemical and Biophysical Research Communications, 276, 82–87.
Kristian, T., & Siesjo, B. K. (1998). Calcium in ischemic cell death. Stroke, 29, 705–718.
Ferrari, R., & Visioli, O. (1991). Calcium channel blockers and ischaemic heart disease: Theoretical expectations and clinical experience. European Heart Journal, 12(Suppl F), 18–24.
Mohan, I. K., Khan, M., Wisel, S., Selvendiran, K., Sridhar, A., Carnes, C. A., et al. (2009). Cardioprotection by HO-4038, a novel verapamil derivative, targeted against ischemia and reperfusion-mediated acute myocardial infarction. American journal of Physiology Heart and Circulatory Physiology, 296, H140–H151.
Matlib, M. A., & McFarland, K. L. (1991). Diltiazem inhibition of sodium-induced calcium release. Effects on energy metabolism of heart mitochondria. American Journal of Hypertension, 4, 435S–441S.
Tabouy, L., Chauvet-Monges, A. M., Salducci, M. D., & Crevat, A. (1994). Protective effect of some calcium antagonists against mitochondrial calcium injury. International Journal of Tissue Reactions, 16, 221–228.
Vavrinkova, H., Tutterova, M., Stopka, P., Divisova, J., Kazdova, L., & Drahota, Z. (2001). The effect of captopril on nitric oxide formation and on generation of radical forms of mitochondrial respiratory chain compounds in ischemic rat heart. Physiological Research, 50, 481–489.
Yanagishita, T., Tomita, M., Itoh, S., Mukae, S., Arata, H., Ishioka, H., et al. (1997). Protective effect of captopril on ischemic myocardium. Japanese Circulation Journal, 61, 161–169.
Sanbe, A., Tanonaka, K., Kobayasi, R., & Takeo, S. (1995). Effects of long-term therapy with ACE inhibitors, captopril, enalapril and trandolapril, on myocardial energy metabolism in rats with heart failure following myocardial infarction. Journal of Molecular and Cellular Cardiology, 27, 2209–2222.
Monteiro, P., Oliveira, P. J., Concalves, L., & Providencia, L. A. (2003). Pharmacological modulation of mitochondrial function during ischemia and reperfusion. Revista Portuguesa de Cardiologia, 22, 407–429.
Swedberg, K., Held, P., Kjekshus, J., Rasmussen, K., Ryden, L., & Wedel, H. (1992). Effects of the early administration of enalapril on mortality in patients with acute myocardial infarction. Results of the Cooperative New Scandinavian Enalapril Survival Study II (CONSENSUS II). New England Journal of Medicine, 327, 678–684.
Monteiro, P., Duarte, A. I., Goncalves, L. M., & Providencia, L. A. (2005). Valsartan improves mitochondrial function in hearts submitted to acute ischemia. European Journal of Pharmacology, 518, 158–164.
Singh, B. N. (2006). Amiodarone: A multifaceted antiarrhythmic drug. Current Cardiology Reports, 8, 349–355.
Varbiro, G., Toth, A., Tapodi, A., Veres, B., Sumegi, B., & Gallyas, F., Jr. (2003). Concentration dependent mitochondrial effect of amiodarone. Biochemical Pharmacology, 65, 1115–1128.
Spedding, M., Tillement, J. P., Morin, D., & Le Ridant, A. (1999). Medicines interacting with mitochondria: Anti-ischemic effects of trimetazidine. Therapie, 54, 627–635.
Kantor, P. F., Lucien, A., Kozak, R., & Lopaschuk, G. D. (2000). The antianginal drug trimetazidine shifts cardiac energy metabolism from fatty acid oxidation to glucose oxidation by inhibiting mitochondrial long-chain 3-ketoacyl coenzyme A thiolase. Circulation Research, 86, 580–588.
Grynberg, A., & Demaison, L. (1996). Fatty acid oxidation in the heart. Journal of Cardiovascular Pharmacology, 28(Suppl 1), S11–S17.
Morin, D., Hauet, T., Spedding, M., & Tillement, J. (2001). Mitochondria as target for antiischemic drugs. Advanced Drug Delivery Reviews, 49, 151–174.
Guarnieri, C., Finelli, C., Zini, M., & Muscari, C. (1997). Effects of trimetazidine on the calcium transport and oxidative phosphorylation of isolated rat heart mitochondria. Basic Research in Cardiology, 92, 90–95.
Veitch, K., Maisin, L., & Hue, L. (1995). Trimetazidine effects on the damage to mitochondrial functions caused by ischemia and reperfusion. American Journal of Cardiology, 76, 25B–30B.
Salloum, F. N., Ockaili, R. A., Wittkamp, M., Marwaha, V. R., & Kukreja, R. C. (2006). Vardenafil: a novel type 5 phosphodiesterase inhibitor reduces myocardial infarct size following ischemia/reperfusion injury via opening of mitochondrial K(ATP) channels in rabbits. Journal of Molecular and Cellular Cardiology, 40, 405–411.
Kukreja, R. C., Salloum, F., Das, A., Ockaili, R., Yin, C., Bremer, Y. A., et al. (2005). Pharmacological preconditioning with sildenafil: Basic mechanisms and clinical implications. Vascular Pharmacology, 42, 219–232.
Salloum, F. N., Takenoshita, Y., Ockaili, R. A., Daoud, V. P., Chou, E., Yoshida, K., et al. (2007). Sildenafil and vardenafil but not nitroglycerin limit myocardial infarction through opening of mitochondrial K(ATP) channels when administered at reperfusion following ischemia in rabbits. Journal of Molecular and Cellular Cardiology, 42, 453–458.
Fernandes, M. A., Marques, R. J., Vicente, J. A., Santos, M. S., Monteiro, P., Moreno, A. J., et al. (2008). Sildenafil citrate concentrations not affecting oxidative phosphorylation depress H2O2 generation by rat heart mitochondria. Molecular and Cellular Biochemistry, 309, 77–85.
Wang, X., Fisher, P. W., Xi, L., & Kukreja, R. C. (2008). Essential role of mitochondrial Ca2+ -activated and ATP-sensitive K+ channels in sildenafil-induced late cardioprotection. Journal of Molecular and Cellular Cardiology, 44, 105–113.
Reffelmann, T., & Kloner, R. A. (2005). Pharmacotherapy of erectile dysfunction: Focus on cardiovascular safety. Expert Opinion on Drug Safety, 4, 531–540.
Garlid, K. D., Paucek, P., Yarov-Yarovoy, V., Murray, H. N., Darbenzio, R. B., D’Alonzo, A. J., et al. (1997). Cardioprotective effect of diazoxide and its interaction with mitochondrial ATP-sensitive K+ channels. Possible mechanism of cardioprotection. Circulation Research, 81, 1072–1082.
Baines, C. P., Liu, G. S., Birincioglu, M., Critz, S. D., Cohen, M. V., & Downey, J. M. (1999). Ischemic preconditioning depends on interaction between mitochondrial KATP channels and actin cytoskeleton. American Journal of Physiology, 276, H1361–H1368.
Takashi, E., Wang, Y., & Ashraf, M. (1999). Activation of mitochondrial K(ATP) channel elicits late preconditioning against myocardial infarction via protein kinase C signaling pathway. Circulation Research, 85, 1146–1153.
Pasdois, P., Beauvoit, B., Tariosse, L., Vinassa, B., Bonoron-Adele, S., & Dos Santos, P. (2008). Effect of diazoxide on flavoprotein oxidation and reactive oxygen species generation during ischemia–reperfusion: A study on Langendorff-perfused rat hearts using optic fibers. American Journal of Physiology Heart and Circulatory Physiology, 294, H2088–H2097.
Ohnuma, Y., Miura, T., Miki, T., Tanno, M., Kuno, A., Tsuchida, A., et al. (2002). Opening of mitochondrial K(ATP) channel occurs downstream of PKC-epsilon activation in the mechanism of preconditioning. American Journal of Physiology Heart and Circulatory Physiology, 283, H440–H447.
Korge, P., Honda, H. M., & Weiss, J. N. (2002). Protection of cardiac mitochondria by diazoxide and protein kinase C: Implications for ischemic preconditioning. Proceedings of the National Academy of Sciences of the United States of America, 99, 3312–3317.
Minatoguchi, S., Wang, N., Uno, Y., Arai, M., Hashimoto, K., Hashimoto, Y., et al. (2001). Combination of miglitol, an anti-diabetic drug, and nicorandil markedly reduces myocardial infarct size through opening the mitochondrial K(ATP) channels in rabbits. British Journal of Pharmacology, 133, 1041–1046.
Ozcan, C., Bienengraeber, M., Dzeja, P. P., & Terzic, A. (2002). Potassium channel openers protect cardiac mitochondria by attenuating oxidant stress at reoxygenation. American Journal of Physiology Heart and Circulatory Physiology, 282, H531–H539.
Iwai, T., Tanonaka, K., Motegi, K., Inoue, R., Kasahara, S., & Takeo, S. (2002). Nicorandil preserves mitochondrial function during ischemia in perfused rat heart. European Journal of Pharmacology, 446, 119–127.
Sato, T., Sasaki, N., O’Rourke, B., & Marban, E. (2000). Nicorandil, a potent cardioprotective agent, acts by opening mitochondrial ATP-dependent potassium channels. Journal of the American College of Cardiology, 35, 514–518.
Halestrap, A. P., & Pasdois, P. (2009). The role of the mitochondrial permeability transition pore in heart disease. Biochimica et Biophysica Acta, 1787, 1402–1415.
Halestrap, A. P., & Davidson, A. M. (1990). Inhibition of Ca2(+)-induced large-amplitude swelling of liver and heart mitochondria by cyclosporin is probably caused by the inhibitor binding to mitochondrial-matrix peptidyl-prolyl cis–trans isomerase and preventing it interacting with the adenine nucleotide translocase. Biochemical Journal, 268, 153–160.
Halestrap, A. P., Clarke, S. J., & Javadov, S. A. (2004). Mitochondrial permeability transition pore opening during myocardial reperfusion–a target for cardioprotection. Cardiovascular Research, 61, 372–385.
Baines, C. P., Kaiser, R. A., Purcell, N. H., Blair, N. S., Osinska, H., Hambleton, M. A., et al. (2005). Loss of cyclophilin D reveals a critical role for mitochondrial permeability transition in cell death. Nature, 434, 658–662.
Nakagawa, T., Shimizu, S., Watanabe, T., Yamaguchi, O., Otsu, K., Yamagata, H., et al. (2005). Cyclophilin D-dependent mitochondrial permeability transition regulates some necrotic but not apoptotic cell death. Nature, 434, 652–658.
Halestrap, A. P., Connern, C. P., Griffiths, E. J., & Kerr, P. M. (1997). Cyclosporin A binding to mitochondrial cyclophilin inhibits the permeability transition pore and protects hearts from ischaemia/reperfusion injury. Molecular and Cellular Biochemistry, 174, 167–172.
Magnasco, A., Rossi, A., Catarsi, P., Gusmano, R., Ginevri, F., Perfumo, F., et al. (2008). Cyclosporin and organ specific toxicity: Clinical aspects, pharmacogenetics and perspectives. Current Clinical Pharmacology, 3, 166–173.
Ferrari, R., Merli, E., Cicchitelli, G., Mele, D., Fucili, A., & Ceconi, C. (2004). Therapeutic effects of l-carnitine and propionyl-l-carnitine on cardiovascular diseases: A review. Annals of the New York Academy of Sciences, 1033, 79–91.
Andrieu-Abadie, N., Jaffrezou, J. P., Hatem, S., Laurent, G., Levade, T., & Mercadier, J. J. (1999). l-carnitine prevents doxorubicin-induced apoptosis of cardiac myocytes: Role of inhibition of ceramide generation. Faseb Journal, 13, 1501–1510.
Mutomba, M. C., Yuan, H., Konyavko, M., Adachi, S., Yokoyama, C. B., Esser, V., et al. (2000). Regulation of the activity of caspases by l-carnitine and palmitoylcarnitine. FEBS Letters, 478, 19–25.
Gao, L., Laude, K., & Cai, H. (2008). Mitochondrial pathophysiology, reactive oxygen species, and cardiovascular diseases. Veterinary Clinics of North America Small Animal Practice, 38, 137–155.
Yamawaki, M., Sasaki, N., Shimoyama, M., Miake, J., Ogino, K., Igawa, O., et al. (2004). Protective effect of edaravone against hypoxia-reoxygenation injury in rabbit cardiomyocytes. British Journal of Pharmacology, 142, 618–626.
Watanabe, T., Yuki, S., Egawa, M., & Nishi, H. (1994). Protective effects of MCI-186 on cerebral ischemia: Possible involvement of free radical scavenging and antioxidant actions. Journal of Pharmacology and Experimental Therapeutics, 268, 1597–1604.
Rajesh, K. G., Sasaguri, S., Suzuki, R., & Maeda, H. (2003). Antioxidant MCI-186 inhibits mitochondrial permeability transition pore and upregulates Bcl-2 expression. American Journal of Physiology Heart and Circulatory Physiology, 285, H2171–H2178.
Yamazaki, K., Miwa, S., Toyokuni, S., Nemoto, S., Oriyanhan, W., Takaba, K., et al. (2009). Effect of edaravone, a novel free radical scavenger, supplemented to cardioplegia on myocardial function after cardioplegic arrest: in vitro study of isolated rat heart. Heart and Vessels, 24, 228–235.
Mallet, R. T., Sun, J., Knott, E. M., Sharma, A. B., & Olivencia-Yurvati, A. H. (2005). Metabolic cardioprotection by pyruvate: Recent progress. Experimental Biology and Medicine (Maywood), 230, 435–443.
Mallet, R. T., & Sun, J. (1999). Mitochondrial metabolism of pyruvate is required for its enhancement of cardiac function and energetics. Cardiovascular Research, 42, 149–161.
Kerr, P. M., Suleiman, M. S., & Halestrap, A. P. (1999). Reversal of permeability transition during recovery of hearts from ischemia and its enhancement by pyruvate. American Journal of Physiology, 276, H496–H502.
Hamilton, K. L. (2007). Antioxidants and cardioprotection. Medicine and Science in Sports and Exercise, 39, 1544–1553.
Pain, T., Yang, X. M., Critz, S. D., Yue, Y., Nakano, A., Liu, G. S., et al. (2000). Opening of mitochondrial K(ATP) channels triggers the preconditioned state by generating free radicals. Circulation Research, 87, 460–466.
Adlam, V. J., Harrison, J. C., Porteous, C. M., James, A. M., Smith, R. A., Murphy, M. P., et al. (2005). Targeting an antioxidant to mitochondria decreases cardiac ischemia–reperfusion injury. Faseb Journal, 19, 1088–1095.
Bakeeva, L. E., Barskov, I. V., Egorov, M. V., Isaev, N. K., Kapelko, V. I., Kazachenko, A. V., et al. (2008). Mitochondria-targeted plastoquinone derivatives as tools to interrupt execution of the aging program. 2. Treatment of some ROS- and age-related diseases (heart arrhythmia, heart infarctions, kidney ischemia, and stroke). Biochemistry (Mosc), 73, 1288–1299.
Fink, M. P., Macias, C. A., Xiao, J., Tyurina, Y. Y., Delude, R. L., Greenberger, J. S., et al. (2007). Hemigramicidin-TEMPO conjugates: novel mitochondria-targeted antioxidants. Critical Care Medicine, 35, S461–S467.
James, A. M., Cocheme, H. M., & Murphy, M. P. (2005). Mitochondria-targeted redox probes as tools in the study of oxidative damage and ageing. Mechanisms of Ageing and Development, 126, 982–986.
Giacomo, C. G., & Antonio, M. (2007). Melatonin in cardiac ischemia/reperfusion-induced mitochondrial adaptive changes. Cardiovascular Hematological Disorders Drug Targets, 7, 163–169.
Acuna-Castroviejo, D., Escames, G., Rodriguez, M. I., & Lopez, L. C. (2007). Melatonin role in the mitochondrial function. Front Bioscience, 12, 947–963.
Ceyran, H., Narin, F., Narin, N., Akgun, H., Ceyran, A. B., Ozturk, F., et al. (2008). The effect of high dose melatonin on cardiac ischemia- reperfusion injury. Yonsei Medical Journal, 49, 735–741.
Petrosillo, G., Di Venosa, N., Pistolese, M., Casanova, G., Tiravanti, E., Colantuono, G., et al. (2006). Protective effect of melatonin against mitochondrial dysfunction associated with cardiac ischemia- reperfusion: Role of cardiolipin. Faseb Journal, 20, 269–276.
Ostadal, B., Netuka, I., Maly, J., Besik, J., & Ostadalova, I. (2009). Gender differences in cardiac ischemic injury and protection—experimental aspects. Experimental Biology and Medicine (Maywood), 234, 1011–1019.
Booth, E. A., & Lucchesi, B. R. (2008). Estrogen-mediated protection in myocardial ischemia–reperfusion injury. Cardiovascular Toxicology, 8, 101–113.
Xu, Y., Arenas, I. A., Armstrong, S. J., Plahta, W. C., Xu, H., & Davidge, S. T. (2006). Estrogen improves cardiac recovery after ischemia/reperfusion by decreasing tumor necrosis factor-alpha. Cardiovascular Research, 69, 836–844.
Duckles, S. P., Krause, D. N., Stirone, C., & Procaccio, V. (2006). Estrogen and mitochondria: A new paradigm for vascular protection? Molecular Interventions, 6, 26–35.
Morkuniene, R., Jekabsone, A., & Borutaite, V. (2002). Estrogens prevent calcium-induced release of cytochrome c from heart mitochondria. FEBS Letters, 521, 53–56.
Yang, S. H., Liu, R., Perez, E. J., Wen, Y., Stevens, S. M., Jr., Valencia, T., et al. (2004). Mitochondrial localization of estrogen receptor beta. Proceedings of the National Academy of Sciences of the United States of America, 101, 4130–4135.
Morkuniene, R., Arandarcikaite, O., & Borutaite, V. (2006). Estradiol prevents release of cytochrome c from mitochondria and inhibits ischemia-induced apoptosis in perfused heart. Experimental Gerontology, 41, 704–708.
Sugishita, K., Li, F., Su, Z., & Barry, W. H. (2003). Anti-oxidant effects of estrogen reduce [Ca2+]i during metabolic inhibition. Journal of Molecular and Cellular Cardiology, 35, 331–336.
Wang, Q. D., Pernow, J., Sjoquist, P. O., & Ryden, L. (2002). Pharmacological possibilities for protection against myocardial reperfusion injury. Cardiovascular Research, 55, 25–37.
Berthiaume, J. M., Oliveira, P. J., Fariss, M. W., & Wallace, K. B. (2005). Dietary vitamin E decreases doxorubicin-induced oxidative stress without preventing mitochondrial dysfunction. Cardiovascular Toxicology, 5, 257–267.
Acknowledgments
The work in the authors’ laboratory is supported by the Portuguese Foundation for Science and Technology (SFRH/BD/31655/2006 to Marco G. Alves, POCI/SAU-OBS/55802/2004 to Rui A. Carvalho).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Machado, N.G., Alves, M.G., Carvalho, R.A. et al. Mitochondrial Involvement in Cardiac Apoptosis During Ischemia and Reperfusion: Can We Close the Box?. Cardiovasc Toxicol 9, 211–227 (2009). https://doi.org/10.1007/s12012-009-9055-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-009-9055-1