Abstract
Animal models of copper toxicosis rarely exhibit neurological impairments and increased brain copper accumulation impeding the development of novel therapeutic approaches to treat neurodegenerative diseases having high brain Cu content. The aim of this study was to investigate the effects of intraperitoneally injected copper lactate (0.15 mg Cu/100 g body weight) daily for 90 days on copper and zinc levels in the liver and hippocampus, on biochemical parameters, and on neurobehavioral functions (by Morris water maze) of male Wistar rats. Copper-administered animals exhibited significantly decreased serum acetylcholinesterase (AChE) activity and impaired neuromuscular coordination and spatial memory compared to control rats. Copper-intoxicated rats showed significant increase in liver and hippocampus copper content (99.1 and 73 % increase, respectively), 40.7 % reduction in hepatic zinc content, and interestingly, 77.1 % increase in hippocampus zinc content with concomitant increase in copper and zinc levels in serum and urine compared to control rats. Massive grade 4 copper depositions and grade 1 copper-associated protein in hepatocytes of copper-intoxicated rats were substantiated by rhodanine and orcein stains, respectively. Copper-intoxicated rats demonstrated swelling and increase in the number of astrocytes and copper deposition in the choroid plexus, with degenerated neurons showing pyknotic nuclei and dense eosinophilic cytoplasm. In conclusion, the present study shows the first evidence in vivo that chronic copper toxicity causes impaired spatial memory and neuromuscular coordination, swelling of astrocytes, decreased serum AChE activity, copper deposition in the choroid plexus, neuronal degeneration, and augmented levels of copper and zinc in the hippocampus of male Wistar rats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Copper (Cu) is an indispensable trace element that plays a key role in the biochemistry of all organisms; but conversely, excess of Cu is highly cytotoxic as it can generate extremely damaging free hydroxyl radical production unless homeostasis is tightly regulated. Cu is present throughout the brain, being most prominent in the hippocampus, basal ganglia, cerebellum, and numerous synaptic membranes [1]. Several central nervous system enzymes such as Cu/Zn superoxide dismutase, ceruloplasmin, dopamine β-hydroxylase, and cytochrome c oxidase are dependent on Cu for their function. Recent studies have implicated alterations in Cu homeostasis, directly or indirectly, in the pathogenesis of numerous neurological and neurodegenerative diseases like Parkinson’s disease (PD), Alzheimer’s disease (AD), prion disease, and Wilson’s disease (WD) [2].
Animal models play an important role in the study of Cu homeostasis. However, animal models of Cu toxicosis rarely show any apparent neurological abnormalities and brain Cu accumulation, highlighting the urgent need of an animal model of Cu toxicosis with high brain Cu content and neurobehavioral impairments [3, 4]. Various experiments to produce a rat model of Cu toxicosis having high brain Cu levels and neurobehavioral impairments by loading a large dose of Cu have not succeeded [5, 6]; albeit, rats tend to accumulate Cu in the liver by binding to metallothionein (MT) [7]. Recently, Fujiwara et al. [8] and Leiva et al. [9] studied the effect of Cu toxicity in Wistar rats by administrating 1 ppm CuSO4 dissolved in drinking water for 6 weeks and 1 mg/kg CuSO4 dissolved in saline by intraperitoneal (i.p.) route for 30 days, respectively, and reported that there is neither any significant accumulation of Cu in the brain nor any neurobehavioral manifestations. Ozcelik et al. [10] had also reported a marginal accumulation of Cu in the brain of Wistar rats by chronic Cu administration (Cu at a dose of 1 g/L for 4 weeks in drinking water).
However, these studies had a major shortcoming in choosing either the drinking water route or adult rats for Cu administration. Drinking water uptake by individual rats can be highly variable and a single i.p. injection of Cu dose is efficient over divided smaller Cu doses for over 24 h in drinking water. Neonatal animals are more vulnerable to Cu poisoning, probably because of the immaturity of biliary excretory mechanisms (which is main route for Cu excretion from the body) and high proficiency of Cu absorption. This may describe the reason why Cu toxicity-related cirrhosis in humans, such as Indian childhood cirrhosis (ICC), is limited mainly to young kids (range, 6 months to 5 years) [11]. Further, neonates have high hepatic Cu levels, which are nearly equal to those observed in WD patients, i.e., >250 mg/kg dry weight [12, 13]. In this study, we have used the i.p. route for inducing Cu intoxication by Cu lactate solution because the lactic acid–Cu complex has a low pK (around 2 to 3), so lactic acid may function as Cu carrier to tissues.
Cu concentrations in different regions of the brain and oxidative stress in the brain upon Cu intoxication have been well documented in many studies, and the hippocampus has been shown to have the highest concentration of Cu [8, 9]. Further, the hippocampus is the region of the brain associated with learning and memory processes [14].
Acetylcholinesterase (AChE) is a crucial enzyme in the nervous system of vertebrates. AChE activity has been shown to be affected by metals viz. Cu and Zn [15], and AChE has a key role in neurophysiological and neuromodulatory functions.
Taking into account the previously mentioned facts, it was considered of interest to investigate whether chronic Cu intoxication leads to an increase in Cu content in the hippocampus region of the brain, histopathological changes, and any neurobehavioral abnormalities in Wistar rats. In this study, we have reported the effect of chronic Cu intoxication with relation to Cu and Zn levels, neurobehavioral functions, as well as histopathological changes in male Wistar rats with special reference to the brain.
Materials and Methods
Animals
Male Wistar rats in the weight range of 60–80 g (starting at 3 weeks of age) were procured from the institute animal house of PGIMER, Chandigarh, India. All the rats were housed in polypropylene cages (one animal per cage), kept in well-ventilated rooms (22 ± 2 °C), and maintained in a 12-h light–dark cycle. Neurobehavioral testing was carried out during the light cycle. The rats were fed standard rat chow (for a detailed composition of the diet, see Supplementary Table 1) and water ad libitum. All animal experiments were carried out with the approval and guidelines of the Institutional Animal Ethical Committee (IAEC-161).
Reagents
Copper chloride, histological grade formalin, dimethylaminobenzylidene rhodanine, Congo red, and Cu and Zn standard solutions assigned for atomic absorption spectrophotometry (AAS) (Sigma-Aldrich Co., Germany), S-acetylthiocholine iodide (SRL), orcein (BDH), and lactic acid (Qualigens) were purchased. All the other reagents and chemicals used in this study were of analytical grade.
Experimental Design
The LD50 for copper chloride by i.p. route in rats was reported to be 14.7 mg/kg body weight (BW) [Material Safety Data Sheet (MSDS, Sigma Aldrich)]. A previous study by Narasaki [16] reported that 36 rats intraperitoneally injected with copper lactate solution (0.15 mg Cu/100 g BW) for 6 months did not die of Cu toxicity (copper lactate solution consisted of lactic acid and copper chloride). The same study also documented that carrier mimicking the Cu lactate solution, the sodium lactate solution, when administrated intraperitoneally for 6 months, has been demonstrated to cause no major effect on Cu levels in various tissues (viz. liver, kidney, brain, and other tissues), tissue histology of various tissues, and other vital biochemical parameters in Wistar rats using a larger group of animals (n = 25); thus, ethically saving the animals in the present study. Therefore, an appropriate dose for chronic Cu intoxication at 0.15 mg Cu/100 g BW was chosen in the current study. Pregnancy and hormonal changes has been reported to elevate copper in the urine, so female Wistar rats were not chosen for the study [17].
The schematic representation of the neurobehavioral tests is depicted in Supplementary Fig. 1a. Male Wistar rats in the weight range of 60–80 g (starting at 3 weeks of age) were randomly divided into two groups having eight animals in each group:
-
Control group: i.p. injection of isotonic sodium chloride solution daily for the period of 90 days.
-
Copper intoxication group: i.p. injection of copper lactate solution (0.15 mg Cu/100 g BW) daily for the period of 90 days. The copper lactate solution was prepared by using lactic acid and copper chloride: 10 ml of 0.17 % copper chloride solution in 0.15 M HCl was combined with 3.3 ml of 75 % lactic acid. The pH of the mixture was adjusted to 7.4 with sodium carbonate [16, 18].
After 90 days of Cu intoxication, rats were used for neurobehavioral studies, as depicted in Supplementary Fig. 1a. During the course of neurobehavioral studies, neither Cu-intoxicated group rats were i.p. injected with copper lactate nor were the control group rats i.p. injected with normal saline.
Collection and Preservation of Blood, Urine, and Tissue Autopsy Samples
The serum was separated from blood obtained from animals by retrobulbar blood vessel stab with a glass capillary on the 30th, 60th, and 90th day of the study in sterile Cu-free and Zn-free containers. Urine samples were collected in sterile Cu-free and Zn-free containers containing 0.2 ml of 10 % thymol under paraffin oil by placing the animal in metabolic cage for 24 h. The collected urine was centrifuged at 4,000×g for 5 min at 4 °C to remove debris and stored at −80 °C till further processing. All the animals were weighed on an interval of 10 days throughout the study.
All the animals were sacrificed on the 99th day of the study after the completion of neurobehavioral studies under ether anesthesia, and the weight of liver and kidney tissues was recorded. Tissue autopsy samples for Cu and Zn quantifications (liver, kidney, and hippocampus) were collected in normal saline solution and stored in sterile Cu-free and Zn-free containers at −80 °C till further processing. Liver, kidney, and brain tissues were fixed in formalin for histopathological studies. All the glassware used in Cu and Zn estimations were soaked in concentrated HCl for 24 h and rinsed several times in deionized water before use. Tissues were cut with clean stainless steel scalpel blades.
Measurement of Biochemical Parameters, Serum AChE Activity, and Ceruloplasmin
Serum glutamic oxaloacetic transaminase (SGOT), serum glutamic pyruvic transaminase (SGPT), urea, creatinine, urinary creatinine, and proteinuria were determined spectroscopically using an autoanalyzer (Modular P800, Roche, Germany) on the 30th, 60th, and 90th day of the study. Serum ceruloplasmin activity was measured as Cu oxidase activity by using p-phenylenediamine dihydrochloride as a substrate as described by Ravin [19]. Serum AChE activity was determined by the Ellman method. Enzyme activity was measured spectrophotometrically at 412 nm and calculated using the molar extinction coefficient of 5-mercapto-2-nitrobenzoic acid (13.6 × 103 M−1 cm−1) [20].
Neurobehavioral Studies
Motor Function Test
Rotarod test was carried out to evaluate the muscle strength and coordination in movement of the animals [21]. As a part of the test procedure, the animals were initially trained to maintain themselves on the rotating rod at 15 rpm for a period of more than 3 min (three trials of more than 3 min each). Subsequently after a period of 24 h, the animals were again screened for their ability to remain on the rotating rod for three successive trials of 3 min each. The values were reported as mean of three trials.
Memory Function Test
Morris Water Maze Test
The Morris water maze (MWM) test was carried out to study the spatial learning and memory by the method of Morris, with slight modifications [22]. Twenty-four hours before the MWM testing, all animals were habituated to water and the MWM apparatus. The MWM apparatus was located in a room with numerous extra maze cues that remained constant throughout the experiment. The water in the tank was made opaque by the addition of powdered milk and the temperature of the water in the tank was maintained at 22 ± 2 °C throughout the study. The time and track taken to reach the platform were recorded by a video camera overhead. The data for the MWM test was analyzed by the AnyMaze™ software. At the end of each swimming trial, the animals were removed, dried off with a paper towel, and placed under a heat lamp and then back into the cages.
Acquisition Test
As a part of the MWM test procedure, the animals were trained to escape from water by swimming to a hidden platform in a dark circular water tank (180 cm in diameter) which was filled with water up to 8 cm from the top of the tank. A platform with an 8 × 8-cm top surface was placed in the middle of one quadrant about 24 cm from the side. The top surface of the platform was submerged about 2 cm below the surface of the water. The animals were allowed to swim freely and trained to find the platform, which was under the water and served as a “rescue” from the stress situation, by using visual extra maze cues. In the navigation tank, the place of the platform was the same on each day, but the starting point of the animal varied. This method requires a long-term spatial memory and learning. All animals were given four training trials per day of 60 s each trial (acquisition) on days 1 to 4. On each training trial, the animal was placed into the water with its nose facing the side of the tank at one of four randomly selected locations corresponding to each quadrant of the maze and was allowed 60 s to find the hidden platform. If the animal was unable to locate the hidden platform, it was lifted out and placed on the platform for 15 s and its escape latency was recorded as 60 s. From days 1 to 5, time taken to locate the hidden platform (escape latency) and the swimming speed were recorded.
Retrieval Test (Probe Trial)
On sixth day, the platform was removed and each animal was placed in the pool at the same randomly selected location and allowed to swim for 60 s. The number of entries and time spent in the target quadrant 1 (where the platform had been positioned on days 1 to 5) along with platform crossings (number of entries in the platform zone area; 8 × 8 cm area) was recorded. The fifth day acquisition test is considered a measure of spatial reference memory, and the retrieval (probe) test is considered a measure of the strength of spatial memory.
Measurement of Cu and Zn Ion Concentrations by Atomic Absorption Spectrophotometry
The concentrations of Cu and Zn in serum, urine, and tissue samples were measured by a flame (an air–acetylene burner) AAS (AAnalyst 400, PerkinElmer) [23]. The urine and serum samples were appropriately diluted (10 times) with ddH2O to be in the linear absorption range of the calibration curve. For tissue samples, ∼50 mg of tissue was digested with 1:1 perchloric acid and nitric acid in hot air oven and diluted five times with 10 mM HNO3 before measurement by AAS. The instrument was calibrated using the Sigma standards of Cu and Zn. Bovine liver standard reference material SRM1577 obtained from the National Bureau of Standard (Washington, DC, USA) was used as standard reference material for quality control. Each sample was measured two to three times and reported as the mean, and the concentrations of Cu and Zn were derived by comparing absorption with the calibration curve. The Cu and Zn estimations were carried out in a blinded experiment.
Histopathological Studies (Rhodanine, Orcein, H&E, and Congo Red Stain) and Grading of Cu and Cu-Associated Protein
Tissues from the liver, kidney, and brain were obtained as 5-mm-thick sections, fixed with 10 % neutral formalin for more than 12 h, dehydrated, embedded in paraffin, sectioned at 5 μm, mounted on glass slides, and stained with hematoxylin and eosin (H&E) stain, orcein stain for Cu-associated protein [24], rhodanine stain for Cu [25], and high-pH Congo red stain for amyloid formation [26]. Liver and brain sections of an ICC and AD patient, respectively (proven cases of ICC and AD patients enrolled in the histopathology department of PGIMER, Chandigarh, India), were taken as positive controls for rhodanine and Congo red stain evaluation. For all the staining studies, negative control tissues (tissues from control animals) were also stained and evaluated.
Hepatocyte copper stainability was expressed as grade 1 for absence or rare rhodanine-stained granules in the cytoplasm of an occasional hepatocytes; grade 2 for few rhodanine-stained granules in randomly distributed hepatocytes; grade 3 for variable numbers of rhodanine-stained granules in hepatocytes, predominantly in the centrilobular area of many lobules; grade 4 for presence of rhodanine-stained granules in many hepatocytes of all lobules; and grade 5 for abundant rhodanine-stained granules in most hepatocytes [27]. Cu-associated protein stainability was expressed as grade 0 for negative, grade 1 for mild staining, grade 2 for moderate staining, and grade 3 for heavy orcein staining in the cytoplasm of hepatocytes [28].
Statistical Analysis
All values were expressed as the mean ± standard error of the mean (SEM) of eight animals in each group. Unpaired Student’s t test and Mann–Whitney rank sum test were used for analysis of the data, and values with p < 0.05 were considered statistically significant. All the calculations were carried out by the SigmaStat computer software program.
Results
Body Composition Changes
Cu-intoxicated animals showed significantly lower growth rate in terms of weight gain from day 70 onwards (28.9 % less weight gain on the 90th day) when compared to control group animals (Supplementary Fig. 1b). Liver and kidney tissue weights (wet weight) expressed relative to BW did not show significant difference between control and Cu-intoxicated groups (Supplementary Table 2). The autopsies revealed fibrotic peritonitis and peripheral areas of pale hepatic tissue, swollen and slightly demarcated from adjacent tissue in liver lobes (data not given).
Biochemical Parameters in Rats Exposed to Chronic Cu Toxicity
SGOT, SGPT, and serum urea levels in the Cu-intoxicated group were markedly increased, indicating chronic hepatitis and kidney damage on the 90th day of the study (Supplementary Table 3). Importantly, serum AChE activity was significantly decreased in the Cu-intoxicated group as compared to the control group [AChE activity (in units per liter), 0.19 ± 0.01 in the control group compared to 0.08 ± 0.01 in the Cu-intoxicated group; p < 0.01 with respect to the controls]. Serum ceruloplasmin levels were considerably increased in Cu-intoxicated animals compared to control animals [serum ceruloplasmin (in milligrams per deciliter), 29.3 ± 0.5 in the control group compared to 47.9 ± 1.1 in the Cu-intoxicated group; p < 0.01 with respect to the controls].
The concentration of serum Cu was found to be significantly increased in the Cu-intoxicated group as compared to the control group [serum Cu (in micrograms per deciliter), 140.9 ± 1.1 in the control group compared to 386.3 ± 17.9 in the Cu-intoxicated group; p < 0.01 with respect to the controls]. Serum Zn levels were marginally high in the Cu-intoxicated animals as compared to the control animals [serum Zn (in micrograms per deciliter), 126.7 ± 4.8 in the control group compared to 198.1 ± 31.8 in the Cu-intoxicated group; p < 0.05 with respect to the controls]. Proteinuria and urinary Cu and Zn levels were also found to be substantially increased in the Cu-intoxicated group compared to the control group (Table 1).
A massive 99.1 % increase in hepatic Cu content along with substantial increase in hippocampus and kidney tissues Cu content (73 and 74.9 % increase, respectively) was observed in the Cu-intoxicated group compared to the control group. Interestingly, Zn levels in the hippocampus region of brain and kidney tissues were also significantly increased in the Cu-intoxicated group (77.1 and 63.4 % increase, respectively) to that of the control group. However, 40.7 % reduction in hepatic Zn levels was observed in the Cu-intoxicated group compared to the control group (Table 1).
Chronic Cu Toxicity Decreases the Neuromuscular Coordination
The rotarod test revealed a noticeable impairment in muscle strength and coordination in Cu-intoxicated rats (Fig. 1). The average retention time was reduced by 60.4 % in the Cu-intoxicated group animals as compared to the controls. None of the Cu-intoxicated rats could maintain themselves on the rotating rod for the full quota of the cutoff time (180 s).
Chronic Cu Toxicity Impairs Spatial Memory
Acquisition Test
The MWM was carried out to test memory functions. The swimming speed and time taken to locate the hidden platform (escape latency) in the water maze from days 1 to 5 are illustrated in Figs. 2 and 3, respectively. Figure 5 shows the schematic representation of the acquisition and retrieval (probe) tests conceptually divided into four quadrants. The swimming speeds of each group remained constant throughout (days 1 to 6) the water maze testing, including both acquisition and retrieval (probe) testing, with no significant difference to be found between Cu-intoxicated and control groups on each day (Fig. 2). During the 5 days of acquisition test, the performance of all animals (control as well as Cu-intoxicated animals) improved progressively, which was established by their decreased escape latencies over the trials (Fig. 3). Overall analysis showed that there was a significant effect of chronic Cu intoxication on average escape latency demonstrated by statistically increased escape latency in the Cu-intoxicated group from days 3 to 5 as compared to the control group (Fig. 3). The plot curve shows the path followed by Cu-intoxicated and control rats, which clearly shows that, with chronic Cu toxicity, rats were a little confused and took more time to locate the hidden platform (Fig. 6). The observed constant swimming speed throughout the MWM testing in both groups suggested that motor function was not the underlying determinant for the prolonged latencies. It is important here to remark that altered/impaired MWM learning is independent of locomotor deficits because land-based locomotor impairments do not affect the swimming speed and escape from water is relatively immune from body mass differences or activity of the animals [14].
Retrieval (Probe) Test
The effects of chronic Cu toxicity on the number of entries and time spent in the target quadrant where the platform had been located during the first 5 days of testing and platform zone crossings (the 8 × 8-cm area) are shown in Fig. 4. The chronic Cu intoxication in animals was associated with inferior performance in the retrieval (probe) test 24 h after the acquisition test. The chronic Cu-intoxicated group animals spent significantly less time than control animals in the target quadrant (Fig. 4a). The number of target quadrant entries in the case of Cu-treated animals was significantly reduced when compared to the controls (Fig. 4b). Cu-intoxicated animals showed a decline in their ability to recognize the area where the platform was placed; the values for the number of platform zone crossings for the Cu-intoxicated group were significantly less when compared to the control animals (Fig. 4c).
Effect of chronic copper intoxication on the a time spent in the target quadrant 1; b number of entries in the target quadrant 1; c platform crossings [number of entries in the platform zone (8 × 8 cm area)] by the rats using the retrieval (probe) test of MWM. Values are the mean ± SEM of eight animals. **p < 0.01; significantly different from the control group
Cu-Intoxicated Rats Showed Cu Deposition in the Liver and Brain Tissues and Cu-Associated Protein in Liver Tissues
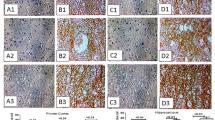
Histopathological observations of the liver and kidney tissues of the Cu-intoxicated group animals were consistent with the data on serum biochemistry analysis, indicating chronic hepatitis. H&E staining showed pigments, but no frank necrosis was observed in the liver tissues of Cu-intoxicated animals. Further, mild lymphomononuclear inflammatory infiltrate was seen in the portal tracts. Grade 4 and grade 3 Cu depositions (Fig. 8a and Supplementary Fig. 2, respectively) and grade 1 Cu-associated protein (Fig. 8b) were observed in the cytoplasm of the hepatocytes with rhodanine and orcein stain, respectively, along with Kupffer cell hyperplasia (Supplementary Fig. 2) in the liver tissue of Cu-intoxicated animals. Cu deposition was found in the choroid plexus (Fig. 7a). Astrocytes swelling (Fig. 7c, d) as well as increase in the number of astrocytes (Fig. 7b) was observed in the cerebral cortex region of the brain in the Cu-intoxicated group. In addition, neurons showed pyknotic nuclei with dense eosinophilic cytoplasm indicating neuronal degeneration (Fig. 7e). Congo red stain did not reveal any amyloid deposition in the brain sections of Cu-intoxicated rats (Supplementary Fig. 4). Renal tubular epithelial cells also demonstrated Cu deposition in the kidney sections of Cu-intoxicated animals (Supplementary Fig. 6). Liver (Supplementary Fig. 3A–C), brain (Supplementary Fig. 5), and kidney (Supplementary Fig. 7) sections of control group rats did not show any histological changes, Cu deposition, and Cu-associated protein.
Discussion
The present study demonstrated a rat model of copper toxicity by administration of copper lactate intraperitoneally for 3 months, which exhibited neurobehavioral, hepatological, and renal abnormalities corroborated by augmented levels of Cu in the hippocampus, liver, and kidney tissues of Cu-intoxicated male Wistar rats, respectively. There is growing acceptance in the scientific literature about the role of increased brain Cu content in the pathogenesis of AD, PD, and WD [29]. In particular, WD patients with neurological manifestations have significantly elevated Cu levels in cerebrospinal fluid (CSF) [30, 31] and threefold to fourfold increased concentration of Cu in the brain [32, 33]. For the first time, we demonstrated that Cu-intoxicated Wistar rats reported in the present study showed significant Cu accumulation (3.7-fold) in the hippocampus (Table 1), decreased neuromuscular coordination (Fig. 1), and impaired spatial memory (Figs. 2, 3, 4, 5, and 6) compared to control rats. These findings are of great significance because animal models of Cu toxicosis rarely develop neurological symptoms due to non-accumulation of Cu in the brain [4, 8]. Though the mechanisms for Cu transport into the brain are not fully understood, it has been shown that Cu is loosely bound to albumin in serum [34], and there is a possibility that Cu ions may be released from the albumin-bound moiety at brain barriers and these free Cu ions are then transported into the brain. The observed Cu deposition in the choroid plexus by rhodanine stain in the brain of Cu-intoxicated rats (Fig. 7a) is in accordance with the findings of Choi and Zheng [35], who have shown that, with an in situ brain perfusion technique in the rat brain, among three Cu species, i.e., free 64Cu, 64Cu-ceruloplasmin, and 64Cu-albumin, the volume of the distribution of free 64Cu in the choroid plexus is about 100 and 50 times greater than that of 64Cu-ceruloplasmin and 64Cu-albumin, respectively. Recent findings indicate that, among the cerebral capillary, CSF, choroid plexus, and brain parenchyma (neurons and glial cells), the choroid plexus shows the highest capacity in acquiring Cu from the blood circulation [35, 36].
Photomicrographs of brain sections of a rat intraperitoneally injected with copper lactate for 90 days. a Note the copper deposition in the choroid plexus (arrow). Left panel ×10 and right panel ×40. Copper is reddish brown. Rhodanine stain. b Note an increase in the number of astrocytes in the cerebral cortex section. H&E stain, ×10. c Note the swelling of astrocytes showing eosinophilic (pink) cytoplasm (Alzheimer type II cells; arrows). H&E stain, ×20. d Note the swelling of astrocytes showing eosinophilic (pink) cytoplasm (Alzheimer type II cells; arrows). H&E stain, ×40. e Note the pyknotic nuclei with dense eosinophilic cytoplasm of degenerating neurons (arrow) in the cerebral cortex section. H&E stain, ×20
It is noteworthy here to mention that rhodanine does not stain the tissue samples having Cu concentration below 0.9 mmol/kg (∼57 μg/g dry weight) [37], which indicates that Cu levels in the choroid plexus unquestionably have increased above 0.9 mmol/kg, supporting the findings of Choi and Zheng [35]. In accordance, we failed to detect Cu in the hippocampus (7.0 ± 0.6 μg Cu/g of wet tissue weight) of Cu-intoxicated animals by rhodanine stain. Zatta and Franj [38] had reported a factor of approximately 3.18 for calculating wet weight to dry weight of tissues. Further, astrocytes swelling (Fig. 7c, d; Alzheimer type II astrocytes as observed in WD patients) [39–41] and increase in number of astrocytes in the brain of Cu-intoxicated rats were also documented (Fig. 7b), which may be probably because of the neuroprotective mechanism against direct or indirect Cu-induced damage [42], supporting the astrocytes’ role as Cu depot hypothesis [43]. However, orcein staining indicated that Cu-binding protein was not detected in histopathological studies of the brain of Cu-intoxicated animals. In agreement with our observations, Haywood et al. [40] demonstrated increased immunoreactivity for MT and increased rhodanine staining for Cu in astrocytes with 343.5 μg Cu/g in the brain of North Ronaldsay sheep, which shows an abnormal sensitivity to dietary Cu. However, no Cu deposition was found in the astrocytes in our study. Astrocytes are implicated in the etiologies of many central nervous system diseases, and astrocytes are the likely sites of deposition for certain metals, especially lead (Pb) and Cu [43, 44]. The role of astrocytes in Cu toxicity warrants further studies. Degeneration of neurons has been reported in many neurodegenerative diseases [2, 29] and we have reported Cu intoxication-induced neuronal degeneration in the brain of Cu-intoxicated animals (Fig. 7e).
Chronic Cu toxicity resulted in a striking impairment of motor coordination in animals, as shown by the significant decline in retention time on the rotarod apparatus (Fig. 1). Cognitive functions are considered as sensitive markers of neurotoxicity [45]. The MWM has often been used for the confirmation of rodent models for neurocognitive disorders and evaluation of possible neurocognitive treatments [46]. Chronic Cu-intoxicated animals reported in the present study showed marked impairment to learn the spatial clues to locate the hidden platform, corroborated by significant prolongation of escape latency during the third to fifth acquisition training days compared to control animals (Fig. 3). In contrast, control animals showed progressively decreased escape latency during the third to fifth acquisition training days, suggesting that chronic Cu toxicity may produce subtle effects related with impaired ability to learn a unique task in Cu-intoxicated animals (Fig. 3). Plot curve analysis of acquisition and retrieval (probe) test (Fig. 6) suggests that the impairment of learning and memory performance are induced by Cu intoxication.
The observed impairment of learning and memory processes in Cu-intoxicated animals may be because of the neurotoxic effects of Cu toxicity on AChE activity [47–49]. Importantly, the observed decreased activity of serum AChE in Cu-intoxicated rats reported in the present study may have caused increased accumulation of acetylcholine in the synapse, causing dysfunctioning of nerve transmission, which may be accountable for the alteration in behavioral activity. Evidence from both animals and human studies has shown the significance of the central cholinergic system in learning, memory, and cognition [47]. AChE has been recently shown to be involved in the induction of neurobehavioral effects probably by affecting the “cholinergic anti-inflammatory pathway” in female Wistar rats exposed to dust from Cu smelters [48]. Recently, Cu accumulation in the hippocampus and striatum has been documented to cause behavioral changes in toxic milk mice, an animal model of WD [50].
The observed increased hippocampus Cu accumulation, degenerating neurons, and neurobehavioral and memory impairments in the Cu-intoxicated rats, along with the fact that Cu can bind to amyloid precursor protein (APP), a key regulator of neuronal Cu homeostasis [51], led us to do Congo red staining to look out for amyloid deposition in the brain sections of around 4-month-old Cu-intoxicated rats, but we found no amyloid deposition in any of the brain sections (Supplementary Fig. 4). APP potentiates the human Aβ-mediated neurotoxicity in vitro by augmenting oxidative stress [51]. In addition, it has been hypothesized that chronic Cu exposure might hasten the AD pathology, partially by upregulating APP expression in animal models of AD [52].
Zn levels were also found to be increased in conjunction with increased Cu levels in the hippocampus of Cu-intoxicated rats (Table 1). This is an interesting finding since Long-Evans Cinnamon rats (animal model of WD) exhibit age-dependent increase in Zn content in various regions of the brain [53] and an increase in brain Zn content has been reported in AD patients which too have an increased serum Cu and ceruloplasmin levels [54]. Under normal physiological conditions, a sensitive balance exists between Zn, Cu, and Aβ metabolism. The oxidative and nitrosative stress may perturb this balance which results in Zn elevation and amyloid deposition [55]. Thus, the observed increased levels of Zn documented in the hippocampus of Cu-intoxicated rats could be associated with oxidative stress caused by Cu, since Cu toxicity is known to cause oxidative stress in the brain [10]. Uncontrolled accumulation of Zn may further result in Zn-induced oxidative stress and cytotoxicity. Notwithstanding, the low levels of Zn protect against Aβ toxicity, while the excess of Zn released by oxidants could trigger neuronal death [56].
Cytoplasm of the hepatocytes stained with rhodanine and orcein stain demonstrated substantial Cu deposition along with Kupffer cell hyperplasia (Fig. 8a and Supplementary Fig. 2; corroborated by increased hepatic Cu content found by AAS studies; Table 1) and Cu-associated protein in the cytoplasm of hepatocytes of Cu-intoxicated animals (Fig. 8b). It is important here to mention that MT has been shown to be the biochemical counterpart of orcein-positive material [28] which was found in the cytoplasm of hepatocytes of Cu-intoxicated animals (Fig. 8b). The liver is a major site of Cu deposition with increased hepatic MT content following a large ingestion of Cu [7] which is corroborated with around 116-fold increase in hepatic Cu content in Cu-intoxicated rats (Table 1). In contrast to the brain, the hepatic Zn content was found to be decreased in Cu-intoxicated rats (Table 1), which is consistent with the findings of Sone et al. [57], who had also reported a reduction in hepatic Zn levels in rats upon excessive accumulation of Cu in the liver.
Photomicrograph of the histopathological study of liver tissue of Cu-intoxicated rat intraperitoneally injected with copper lactate for 90 days. a Grade 4 staining of copper deposition in the cytoplasm of hepatocytes. Copper is orange-brick red. Rhodanine stain (left panel ×10, middle panel ×20, and right panel ×40), b grade 1staining of copper-associated protein (arrow) (note the coarse dark brownish granules of copper-associated protein) in the cytoplasm of centrizonal hepatocytes. Oil immersion. Shikata’s orcein stain (left panel ×40 and right panel ×100)
SGOT and SGPT levels were significantly increased in serum of Cu-intoxicated rats, indicating widespread tissue damage (Supplementary Table 3). SGPT, a specific enzyme of the liver, was threefold higher in Cu-intoxicated rats compared to control rats. Increase in serum ceruloplasmin levels in Cu-intoxicated rats reported in this study may be attributed either to high availability of Cu for incorporation into ceruloplasmin (upregulation of ceruloplasmin gene by Cu ions) or ceruloplasmin itself is an acute phase protein, so its synthesis can be induced by Cu toxicity. The augmentation in serum Zn levels may be attributed either to the release of Zn from MT or upregulation of Zn transporters by Cu ions, leading to an increase in Zn levels in extracellular fluid and subsequent rise in serum Zn levels [58–60]. Chronic Cu intoxication also causes some toxic effects on the kidney as well, as shown by marked proteinuria (Table 1), increased serum urea (Supplementary Table 3), and around fourfold increase in Cu content in kidney tissues of these rats (Table 1). Rhodanine stain demonstrated Cu accumulation in the renal tubular epithelial cells of Cu-intoxicated rats (Supplementary Fig. 6). Cu-intoxicated rats showed 16-fold and 37-fold increase in urinary Cu and Zn levels, respectively, compared to control animals (Table 1). The observed decrease in BW of Cu-intoxicated animals (Supplementary Fig. 1b) can be explained on the basis of progressive hepatitis (Supplementary Table 3), resulting in compromised metabolism, especially lipid metabolism, due to chronic liver failure. The nonsignificant changes in liver and kidney weights expressed relative to BW in the Cu-intoxicated group compared to the control group are parallel to the observations documented by Haywood [61]. These findings are consistent with the findings of Narasaki [16] who had reported increased Cu content in the liver, brain, and kidney tissues of Wistar rats that were exposed to Cu lactate daily by i.p. route for over 160 days.
Taken together, the findings herein illustrate the first evidence in vivo that male Wistar rats chronically injected with copper lactate exhibited decreased neuromuscular coordination, impaired spatial memory, and decreased serum AChE activity along with substantial accumulation of Cu and Zn in the hippocampus, neuronal degeneration, Cu deposition in the choroid plexus, and swollen as well as increased number of astrocytes in the cerebral cortex region (Supplementary Fig. 8), which might reflect the behavioral abnormalities observed in metal dyshomeostasis-associated neurodegenerative diseases. Therefore, the reported Wistar rat model provides a new animal model of non-Wilsonian brain Cu toxicosis for studying not only hepatic and brain Cu pathology but also for studying Cu and Zn dyshomeostasis-related neurodegenerative diseases. However, more studies on the various Cu transporters like Ctr1, Ctr2, DMT1, ATP7A, and ATP7B, Cu chaperones, and mechanisms for Cu transport using molecular Cu imaging techniques especially into the brain are needed to completely elucidate the neuropathophysiological mechanisms of Cu intoxication.
References
Madsen E, Gitlin JD (2007) Copper and iron disorders of the brain. Annu Rev Neurosci 30:317–337. doi:10.1146/annurev.neuro.30.051606.094232
Desai V, Kaler SG (2008) Role of copper in human neurological disorders. Am J Clin Nutr 88(3):855S–858S
Vonk WI, Wijmenga C, van de Sluis B (2008) Relevance of animal models for understanding mammalian copper homeostasis. Am J Clin Nutr 88(3):840S–845S
Wu J, Forbes JR, Chen HS, Cox DW (1994) The LEC rat has a deletion in the copper transporting ATPase gene homologous to the Wilson disease gene. Nat Genet 7(4):541–545. doi:10.1038/ng0894-541
Howell JS (1959) Histochemical demonstration of copper in copper-fed rats and in hepatolenticular degeneration. J Pathol Bacteriol 77(2):473–484
Toyokuni S, Okada S, Hamazaki S, Fujioka M, Li JL, Midorikawa O (1989) Cirrhosis of the liver induced by cupric nitrilotriacetate in Wistar rats. An experimental model of copper toxicosis. Am J Pathol 134(6):1263–1274
Klein D, Michaelsen S, Sato S, Luz A, Stampfl A, Summer KH (1997) Binding of Cu to metallothionein in tissues of the LEC rat with inherited abnormal copper accumulation. Arch Toxicol 71(5):340–343
Fujiwara N, Iso H, Kitanaka N, Kitanaka J, Eguchi H, Ookawara T, Ozawa K, Shimoda S, Yoshihara D, Takemura M, Suzuki K (2006) Effects of copper metabolism on neurological functions in Wistar and Wilson’s disease model rats. Biochem Biophys Res Commun 349(3):1079–1086. doi:10.1016/j.bbrc.2006.08.139
Leiva J, Palestini M, Infante C, Goldschmidt A, Motles E (2009) Copper suppresses hippocampus LTP in the rat, but does not alter learning or memory in the Morris water maze. Brain Res 1256:69–75. doi:10.1016/j.brainres.2008.12.041
Ozcelik D, Uzun H (2009) Copper intoxication; antioxidant defenses and oxidative damage in rat brain. Biol Trace Elem Res 127(1):45–52. doi:10.1007/s12011-008-8219-3
Pandit A, Bhave S (1996) Present interpretation of the role of copper in Indian childhood cirrhosis. Am J Clin Nutr 63(5):830S–835S
Faa G, Liguori C, Columbano A, Diaz G (1987) Uneven copper distribution in the human newborn liver. Hepatology 7(5):838–842
Takahashi S, Takahashi I, Sato H, Kubota Y, Yoshida S, Muramatsu Y (2000) Determination of major and trace elements in the liver of Wistar rats by inductively coupled plasma-atomic emission spectrometry and mass spectrometry. Lab Anim 34(1):97–105
Vorhees CV, Williams MT (2006) Morris water maze: procedures for assessing spatial and related forms of learning and memory. Nat Protoc 1(2):848–858. doi:10.1038/nprot.2006.116
Frasco MF, Fournier D, Carvalho F, Guilhermino L (2005) Do metals inhibit acetylcholinesterase (AChE)? Implementation of assay conditions for the use of AChE activity as a biomarker of metal toxicity. Biomarkers 10(5):360–375. doi:10.1080/13547500500264660
Narasaki M (1980) Laboratory and histological similarities between Wilson’s disease and rats with copper toxicity. Acta Med Okayama 34(2):81–90
Wilken H (1961) Urinary copper excretion in pregnancy. Klin Wochenschr 39:147–149
Cefola M, Tompa AS, Celiano AV, Gentile PS (1962) Coordination compounds. II. Trends in the stability of some rare earth chelates. Inorg Chem (US) 1:290–293
Ravin HA (1961) An improved colorimetric enzymatic assay of ceruloplasmin. J Lab Clin Med 58:161–168
Ellman GL, Courtney KD, Andres V Jr, Feather-Stone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95
Dunham NW, Miya TS (1957) A note on a simple apparatus for detecting neurological deficit in rats and mice. J Am Pharm Assoc Am Pharm Assoc (Baltimore) 46(3):208–209
Morris R (1984) Developments of a water-maze procedure for studying spatial learning in the rat. J Neurosci Methods 11(1):47–60. doi:10.1016/0165-0270(84)90007-4
Prasad R, Kaur G, Walia BN (1998) A critical evaluation of copper metabolism in Indian Wilson’s disease children with special reference to their phenotypes and relatives. Biol Trace Elem Res 65(2):153–165. doi:10.1007/bf02784267
Shikata T, Uzawa T, Yoshiwara N, Akatsuka T, Yamazaki S (1974) Staining methods of Australia antigen in paraffin section—detection of cytoplasmic inclusion bodies. Jpn J Exp Med 44(1):25–36
Lindquist RR (1969) Studies on the pathogenesis of hepatolenticular degeneration. II. Cytochemical methods for the localization of copper. Arch Pathol 87(4):370–379
Bancroft JD, Gamble M (2008) Theory and practice of histological techniques. Churchill Livingstone/Elsevier, Edinburgh
Johnson GF, Gilbertson SR, Goldfischer S, Grushoff PS, Sternlieb I (1984) Cytochemical detection of inherited copper toxicosis of Bedlington terriers. Vet Pathol 21(1):57–60
Evans J, Newman SP, Sherlock S (1980) Observations on copper associated protein in childhood liver disease. Gut 21(11):970–976
Rivera-Mancia S, Perez-Neri I, Rios C, Tristan-Lopez L, Rivera-Espinosa L, Montes S (2010) The transition metals copper and iron in neurodegenerative diseases. Chem Biol Interact 186(2):184–199. doi:10.1016/j.cbi.2010.04.010
Kodama H, Okabe I, Yanagisawa M, Nomiyama H, Nomiyama K, Nose O, Kamoshita S (1988) Does CSF copper level in Wilson disease reflect copper accumulation in the brain? Pediatr Neurol 4(1):35–37
Weisner B, Hartard C, Dieu C (1987) CSF copper concentration: a new parameter for diagnosis and monitoring therapy of Wilson’s disease with cerebral manifestation. J Neurol Sci 79(1–2):229–237
Waggoner DJ, Bartnikas TB, Gitlin JD (1999) The role of copper in neurodegenerative disease. Neurobiol Dis 6(4):221–230. doi:10.1006/nbdi.1999.0250
Walshe JM, Gibbs KR (1987) Brain copper in Wilson’s disease. Lancet 2(8566):1030
Pietrangelo A, Panduro A, Chowdhury JR, Shafritz DA (1992) Albumin gene expression is down-regulated by albumin or macromolecule infusion in the rat. J Clin Invest 89(6):1755–1760. doi:10.1172/jci115778
Choi BS, Zheng W (2009) Copper transport to the brain by the blood–brain barrier and blood–CSF barrier. Brain Res 1248:14–21. doi:10.1016/j.brainres.2008.10.056
Monnot AD, Behl M, Ho S, Zheng W (2011) Regulation of brain copper homeostasis by the brain barrier systems: effects of Fe-overload and Fe-deficiency. Toxicol Appl Pharmacol 256(3):249–257. doi:10.1016/j.taap.2011.02.003
Jain S, Scheuer PJ, Archer B, Newman SP, Sherlock S (1978) Histological demonstration of copper and copper-associated protein in chronic liver diseases. J Clin Pathol 31(8):784–790
Zatta P, Frank A (2007) Copper deficiency and neurological disorders in man and animals. Brain Res Rev 54(1):19–33. doi:10.1016/j.brainresrev.2006.10.001
Gouider-Khouja N (2009) Wilson’s disease. Parkinsonism Relat Disord 15(Suppl 3):S126–S129. doi:10.1016/s1353-8020(09)70798-9
Haywood S, Paris J, Ryvar R, Botteron C (2008) Brain copper elevation and neurological changes in north ronaldsay sheep: a model for neurodegenerative disease? J Comp Pathol 139(4):252–255. doi:10.1016/j.jcpa.2008.06.008
Mikol J, Vital C, Wassef M, Chappuis P, Poupon J, Lecharpentier M, Woimant F (2005) Extensive cortico-subcortical lesions in Wilson’s disease: clinico-pathological study of two cases. Acta Neuropathol 110(5):451–458. doi:10.1007/s00401-005-1061-1
Hidalgo J, Penkowa M, Espejo C, Martinez-Caceres EM, Carrasco J, Quintana A, Molinero A, Florit S, Giralt M, Ortega-Aznar A (2006) Expression of metallothionein-I, -II, and -III in Alzheimer disease and animal models of neuroinflammation. Exp Biol Med (Maywood) 231(9):1450–1458
Tiffany-Castiglioni E, Hong S, Qian Y (2011) Copper handling by astrocytes: insights into neurodegenerative diseases. Int J Dev Neurosci 29(8):811–818. doi:10.1016/j.ijdevneu.2011.09.004
Tiffany-Castiglion E, Qian Y (2001) Astroglia as metal depots: molecular mechanisms for metal accumulation, storage and release. Neurotoxicology 22(5):577–592
White RF, Proctor SP (1992) Research and clinical criteria for development of neurobehavioral test batteries. J Occup Med 34(2):140–148
D’Hooge R, De Deyn PP (2001) Applications of the Morris water maze in the study of learning and memory. Brain Res Brain Res Rev 36(1):60–90
Alkon DL, Amaral DG, Bear MF, Black J, Carew TJ, Cohen NJ, Disterhoft JF, Eichenbaum H, Golski S, Gorman LK et al (1991) Learning and memory. FESN Study Group. Brain Res Brain Res Rev 16(2):193–220
Halatek T, Lutz P, Krajnow A, Stetkiewicz J, Domeradzka K, Swiercz R, Wasowicz W (2011) Assessment of neurobehavioral and biochemical effects in rats exposed to copper smelter dusts. J Environ Sci Health, Part A: Tox Hazard Subst Environ Eng 46(3):230–241. doi:10.1080/10934529.2011.535407
Olson DL, Christensen GM (1980) Effects of water pollutants and other chemicals on fish acetylcholinesterase (in vitro). Environ Res 21(2):327–335
Terwel D, Loschmann YN, Schmidt HH, Scholer HR, Cantz T, Heneka MT (2011) Neuroinflammatory and behavioural changes in the Atp7B mutant mouse model of Wilson’s disease. J Neurochem 118(1):105–112. doi:10.1111/j.1471-4159.2011.07278.x
Huang X, Cuajungco MP, Atwood CS, Hartshorn MA, Tyndall JD, Hanson GR, Stokes KC, Leopold M, Multhaup G, Goldstein LE, Scarpa RC, Saunders AJ, Lim J, Moir RD, Glabe C, Bowden EF, Masters CL, Fairlie DP, Tanzi RE, Bush AI (1999) Cu(II) potentiation of Alzheimer abeta neurotoxicity. Correlation with cell-free hydrogen peroxide production and metal reduction. J Biol Chem 274(52):37111–37116
Mao X, Ye J, Zhou S, Pi R, Dou J, Zang L, Chen X, Chao X, Li W, Liu M, Liu P (2012) The effects of chronic copper exposure on the amyloid protein metabolism associated genes’ expression in chronic cerebral hypoperfused rats. Neurosci Lett 518(1):14–18. doi:10.1016/j.neulet.2012.04.030
Saito T, Itoh T, Fujimura M, Saito K (1995) Age-dependent and region-specific differences in the distribution of trace elements in 7 brain regions of Long-Evans Cinnamon (LEC) rats with hereditary abnormal copper metabolism. Brain Res 695(2):240–244
Squitti R, Pasqualetti P, Dal Forno G, Moffa F, Cassetta E, Lupoi D, Vernieri F, Rossi L, Baldassini M, Rossini PM (2005) Excess of serum copper not related to ceruloplasmin in Alzheimer disease. Neurology 64(6):1040–1046. doi:10.1212/01.wnl.0000154531.79362.23
Cuajungco MP, Lees GJ (1998) Nitric oxide generators produce accumulation of chelatable zinc in hippocampal neuronal perikarya. Brain Res 799(1):118–129
Cuajungco MP, Faget KY (2003) Zinc takes the center stage: its paradoxical role in Alzheimer’s disease. Brain Res Brain Res Rev 41(1):44–56
Sone K, Maeda M, Wakabayashi K, Takeichi N, Mori M, Sugimura T, Nagao M (1996) Inhibition of hereditary hepatitis and liver tumor development in Long-Evans cinnamon rats by the copper-chelating agent trientine dihydrochloride. Hepatology 23(4):764–770. doi:10.1053/jhep.1996.v23.pm0008666330
Eide DJ (2004) The SLC39 family of metal ion transporters. Pflugers Arch 447(5):796–800. doi:10.1007/s00424-003-1074-3
Liuzzi JP, Cousins RJ (2004) Mammalian zinc transporters. Annu Rev Nutr 24:151–172. doi:10.1146/annurev.nutr.24.012003.132402
Palmiter RD, Huang L (2004) Efflux and compartmentalization of zinc by members of the SLC30 family of solute carriers. Pflugers Arch 447(5):744–751. doi:10.1007/s00424-003-1070-7
Haywood S (1980) The effect of excess dietary copper on the liver and kidney of the male rat. J Comp Pathol 90(2):217–232
Acknowledgments
The authors acknowledge the financial support provided by the Indian Council of Medical Research (I.C.M.R., New Delhi) as JRF/SRF to Mr. Amit Pal. The authors are thankful to Professor K.D. Gill for the guidance in carrying out the neurobehavioral studies and Dr. Jayagandhan J. for the suggestions and revision of the manuscript. The authors also acknowledge the support of Mr. Charan Singh (for the staining studies), Mr. Rakesh Mohindra (for the statistics), and Mrs. Minni (for the metal analysis).
Conflict of Interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pal, A., Badyal, R.K., Vasishta, R.K. et al. Biochemical, Histological, and Memory Impairment Effects of Chronic Copper Toxicity: A Model for Non-Wilsonian Brain Copper Toxicosis in Wistar Rat. Biol Trace Elem Res 153, 257–268 (2013). https://doi.org/10.1007/s12011-013-9665-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-013-9665-0