Abstract
Background
Photopolymerizable poly(ethylene glycol) (PEG) hydrogels offer a platform to deliver cells in vivo and support three-dimensional cell culture but should be designed to degrade in sync with neotissue development and endure the physiologic environment.
Questions/purposes
We asked whether (1) incorporation of degradation into PEG hydrogels facilitates tissue development comprised of essential cartilage macromolecules; (2) with early loading before pericellular matrix formation, the duration of load affects matrix production; and (3) dynamic loading in general influences macroscopic tissue development.
Methods
Primary bovine chondrocytes were encapsulated in hydrogels (n = 3 for each condition). The independent variables were hydrogel degradation (nondegrading PEG and degrading oligo(lactic acid)-b-PEG-b-oligo(lactic acid) [PEG-LA]), culture condition (free swelling, unconfined dynamic compressive loading applied intermittently for 1 or 4 weeks), and time (up to 28 days). The dependent variables were neotissue deposition through biochemical contents, immunohistochemistry, and compressive modulus.
Results
Degradation led to 2.3- and 2.9-fold greater glycosaminoglycan and collagen contents, respectively; macroscopic cartilage-like tissue formation comprised of aggrecan, collagen II and VI, link protein, and decorin; but decreased moduli. Loading, applied early or throughout culture, did not affect neotissue content in either hydrogel but affected neotissue spatial distribution in degrading hydrogels where 4 weeks of loading appeared to enhance hydrogel degradation resulting in tissue defects.
Conclusions
PEG-LA hydrogels led to macroscopic tissue development comprised of key cartilage macromolecules under loading, but hydrogel degradation requires further tuning.
Clinical Relevance
PEG-LA hydrogels have potential for delivering chondrocytes in vivo to replace damaged cartilage with a tissue-engineered native equivalent, overcoming many limitations associated with current clinical treatments.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Despite a variety of clinical treatments for articular cartilage damage, including joint débridement [24], microfracture [35, 36], and autologous chondrocyte implantation [11], none has led to regenerated tissue similar in structure and function to native articular cartilage [3]. An alternative is tissue engineering, which commonly uses cells placed within scaffolds to facilitate regeneration [14]. However, scaffold structure and its degradation rate will influence tissue development [28]. Because cartilage is composed of extracellular matrix (ECM) reaching micrometer dimensions [22], ample space is required for its deposition and organization into a structured matrix, thus necessitating degradable scaffolds. Scaffold degradation must be synchronous with ECM synthesis because if degradation is too fast or too slow, defects may develop or tissue development may be hindered. Appropriate degradation times are likely to be on the order of weeks but will depend on factors such as donor age, external stimuli, etc.
In addition to scaffold degradation, cell-laden scaffolds placed in situ will experience a dynamic mechanical environment. Mechanical loading reportedly enhances scaffold degradation [30], regulates chondrocyte behavior [12], and leads to loss of newly synthesized matrix as a result of increased transport [16]. Depending on strain, frequency, temporal distribution of loading (eg, intermittent or continuous daily loading), and overall duration of loading, loading enhances [14, 16, 20] or inhibits [15, 17, 19] tissue synthesis. Loading applied intermittently, early [38], or throughout the duration of culture [14] has enhanced neotissue development, whereas loading applied later has had minimal effects on neotissue synthesis [29]. Loading applied before pericellular matrix (PCM) development [18, 38] may provide critical biomechanical cues for tissue synthesis, in part as a mechanism to protect chondrocytes from deformation. Furthermore, cells are capable of selectively responding to mechanical stimulation, in which cells may only respond to short bouts of loading, thus requiring periods of recovery [32]. Taken together, these findings and others illustrate cellular responses to mechanical stimulation are complex, which will further be impacted by scaffold chemistry and structure [2].
One possible scaffold for cartilage tissue engineering is photopolymerizable poly(ethylene glycol) (PEG) hydrogels, whereby incorporating oligomers of lactic acid (LA) into the crosslinks offers a hydrolytically labile platform for formation and delivery of chondrocytes in vivo [1, 5, 6, 8, 9]. Degradation of oligo(LA)-b-PEG-b-oligo(LA) (PEG-LA) hydrogels can be tuned through several mechanisms, including changes in the number of LA units and hydrogel crosslinking density [25–27]. PEG-LA hydrogels are promising scaffolds for cartilage regeneration because they retain the chondrocyte phenotype and promote synthesis and deposition of proteoglycans and collagen type II [4, 9].
To further realize the potential of PEG-LA hydrogels, we addressed three research questions: (1) Does incorporation of degradation into PEG-based hydrogels facilitate macroscopic development of tissue comprised of essential matrix molecules that make up the PCM and ECM of cartilage? (2) When loading is applied early and before PCM formation, does the duration of load affect matrix production in the long term? (3) Does dynamic mechanical loading in general impact macroscopic tissue development in PEG-based hydrogels?
Materials and Methods
To address each research question, three subsequent studies were developed (Fig. 1). In Study 1, the impact of hydrogel degradation on macroscopic tissue formation was assessed as a function of time in which the independent variables were nondegrading PEG hydrogels, degrading PEG-LA hydrogels, and culture time. In Study 2, the impact of loading duration (1 week versus 4 weeks) on tissue synthesis and deposition was investigated in nondegrading and degrading hydrogels as a function of time. In Study 3, matrix synthesis and deposition in mechanically stimulated nondegrading and degrading hydrogels were compared with their free-swelling counterparts. For Studies 2 and 3, the independent variables included a 1-week loading duration, 4-week loading duration, nondegrading hydrogels, degrading hydrogels, and culture time. For each study, the dependent variables investigated were compressive moduli, biochemical content (sulfated glycosaminoglycan [GAG] and collagen), and spatial distribution of matrix molecules.
A diagram of the experimental design shows the independent variables (nondegrading PEG versus degrading PEG-LA, culture conditions [free swelling, 1-week loading duration, and 4-week loading duration] and culture time) and the dependent variables (biochemical content, mechanical properties, and immunohistochemistry).
A sample size of three was chosen based on prior data [6, unpublished data], in which the variable was degradation. If the desired effect is a 50% difference in GAG content (micrograms of GAG/milligrams of dry weight) by 4 weeks in PEG-LA hydrogels with different degradation rates, prior data having a variance of 550 indicate a sample size of three will give a statistical power of 80% with an error probability of 0.05. For the other variables, loading and load duration, this study serves as a preliminary study.
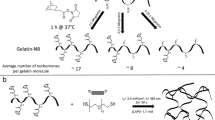
PEG-LA and PEG were synthesized to produce degradable and nondegradable macromolecular monomers (macromers), respectively. L-Lactic acid (PolySciences, Warrington, PA) was reacted with PEG (4600 g/mol; Sigma-Aldrich Corp, St Louis, MO) in the presence of stannous octoate at 70°C for 6 hours [34] resulting in 2.4 LA units per side determined by 1H-nuclear magnetic resonance (NMR). The polymers were end-capped with methacrylates following established procedures [21] and purified by repeated precipitations in diethyl ether. Degree of methacrylate functionalization, determined by 1H-NMR, was 0.85 and 0.87 for PEG and PEG-LA macromers, respectively.
Full-depth articular cartilage was harvested from the patellar-femoral groove of 1- to 3-week-old calves (Research 87, Boylston, MA). Cartilage was digested in 500 U collagenase II per mL in Dulbecco’s Minimum Essential Medium (DMEM) supplemented with 5% fetal bovine serum (FBS) for 16 hours at 37°C on an infinity shaker (40 rpm). The digest was passed through a 100-μm cell strainer, pelleted, and rinsed 3× with phosphate-buffered saline (PBS) containing 1% penicillin/streptomycin, 0.5 μg fungizone/mL, and 20 μg gentamicin/mL (PBS + antibiotics). Chondrocytes (50 million cells/mL) were mixed with 10% (w/w) macromer and 0.05% (w/w) photoinitiator (Irgacure I2959; Ciba Specialty Chemical, Newport, DE) in PBS and photopolymerized (365 nm, 6 mW/cm2, 10 minutes). Resulting hydrogels (5- × 5-mm cylinders) were rinsed in PBS + antibiotics and individually placed into wells of a 24-well plate with 2 mL chondrocyte medium (DMEM supplemented with 10% FBS [v/v], 0.04 mmol L-proline per L, 50 mg L-ascorbic acid per L, 10 mmol HEPES per L, 0.1 mol Minimum Essential Medium with nonessential amino acids/L, 1% penicillin/streptomycin, 0.5 μg fungizone/mL, and 20 μg gentamicin/mL).
Gels were cultured at 37°C in 5% CO2 and allowed to equilibrate for 24 hours. After 24 hours, gels were removed from culture (time = 0 days), placed under free-swelling conditions, or placed into bioreactors [37]. Free-swelling gels were placed on a figure-of-eight shaker (40 rpm). Loaded gels were placed between permeable bases and platens (Porex 40–70 μm) [30] and subjected to intermittent loading (eight cycles/day of 30 minutes on/90 minutes off followed by 8 hours off) applied by a sinusoidal dynamic unconfined compression at 0.3 Hz with a 15% peak-to-peak strain. Displacement control was verified using the on-board linear variable differential transformer sensor, which showed less than 0.01% deviation. Cell viability before loading was semiqualitatively assessed using a LIVE/DEAD® assay, indicating viability was 76% ± 7% and 87% ± 3% for PEG and PEG-LA hydrogels, respectively, 24 hours postencapsulation (based on three separate hydrogels acquired at 100×). Media were replaced every 2 to 3 days and stored at −20°C for subsequent analysis. At specified time points, gels were removed from culture, weighed, and processed.
The compressive moduli were obtained from the linear region of stress-strain curves generated on a mechanical tester (Synergie 100, 10 N; MTS, Eden Prairie, MN). Hydrated constructs were strained to 20% under unconfined compression at 0.5 mm/minute.
At specified time points, one half of the hydrogel construct was lyophilized and digested with papain (125 mg/mL) for 18 hours at 60°C. Sulfated GAG (sGAG) content was measured using dimethylmethylene blue [10] referenced to chondroitin-6-sulfate standards. Collagen content was determined by assaying for hydroxyproline, which is approximately 10% of total collagen [13, 39] against known standards.
At specified time points, the remaining construct halves were fixed for 24 hours in 4% paraformaldehyde, dehydrated, paraffin-embedded, and sectioned (10 μm). Samples were treated with chondroitinase ABC and/or hyaluronidase for 1 hour at 37°C. For antigen retrieval of the link protein, samples were reduced and alkylated. All samples were blocked using 1% bovine serum albumin. Primary antibodies were used against aggrecan (1:10), collagen II (1:100) (US Biologicals, Swampscott, MA), collagen VI (1:100) (Abcam, Cambridge, MA), chondroitin-6-sulfate (1:100) (Chemicon, Billerica, MA), link protein (1:5), or decorin (1:5) (University of Iowa Developmental Studies Hybridoma Bank, Iowa City, IA). Fluorescent detection was achieved using secondary goat antirabbit IgG Alexa Fluor® 488 or goat antimouse IgG Alexa Fluor® 546 antibodies (1:200) and nuclei counterstained using 4’,6-diamidino-2-phenylindole (DAPI) (1:1000). Sections were mounted using VectaMount™ (Vector Laboratories, Burlingame, CA). Laser scanning confocal microscopy (Zeiss LSM 5 Pascal; Carl Zeiss, Thornwood, NY) was used to acquire images.
For Study 1, a two-way ANOVA with Tukey’s post hoc was performed in which hydrogel composition (PEG versus PEG-LA) and time were factors. For Study 2 and Study 3, a two-way ANOVA with Tukey’s post hoc was performed in which hydrogel composition (PEG versus PEG-LA), time, and loading duration (1 week versus 4 weeks) were factors. Statistical analyses were used to determine differences in the dependent variables (compressive moduli, sGAG content, sGAG loss to the culture medium, and collagen content) between the independent variables (hydrogel composition, time, and loading duration).
Results
Incorporating degradation into PEG hydrogels enhanced neotissue deposition and its spatial distribution. Both hydrogel environments promoted deposition of sGAGs (Fig. 2A) and collagen (Fig. 2C), which increased (p < 0.001) with culture time in PEG-LA hydrogels for sGAG and collagen and increased (p = 0.013) in PEG hydrogels but only for sGAG. However, degradation led to improved matrix content. For example, after 28 days, the engineered neotissue within PEG-LA hydrogels was comprised of 2.3-fold greater (p = 0.004) sGAG and 2.9-fold greater (p = 0.031) total collagen contents over PEG hydrogels. Matrix loss was detected from the constructs as measured by sGAGs released into the culture medium (Fig. 2B). Although neotissue deposition was greater in PEG-LA hydrogels, construct mechanical properties, measured by compressive modulus (Fig. 2D), were lowest (p ≤ 0.014) in degrading hydrogels and decreased (p < 0.001) with culture time but remained constant for nondegrading hydrogels. Immunohistochemistry revealed chondrocytes cultured in nondegrading and degrading hydrogels synthesized the major structural matrix molecules found in articular cartilage, but their spatial deposition was enhanced in degrading gels (Figs. 3, 4). Specifically, chondrocytes in PEG gels exhibited a PCM rich in chondroitin-6-sulfate, aggrecan core protein and link protein, collagen II, collagen VI, and decorin. In contrast, the engineered tissue formed from PEG-LA hydrogels was comprised of chondroitin-6-sulfate, aggrecan, collagen II, and decorin depositions in the extracellular space and of collagen VI within the pericellular regions, similar to that observed in native cartilage.
Graphs show the matrix content and mechanical properties of nondegradable PEG (dark gray) and degradable PEG-LA (light gray) hydrogels cultured up to 28 days under free-swelling conditions: (A) accumulation of sGAG in the construct; (B) cumulative sGAG released into the culture medium; (C) accumulation of total collagen in the construct; and (D) compressive modulus. ECM content within the hydrogel and media, as represented by sGAG and collagen, increases for both material types over time, whereas the mechanical properties are maintained for PEG but decrease for PEG-LA. This indicates matrix formation; however, at 4 weeks, it is not a mature, mechanically functional ECM. Data are represented as mean ± SD.
Gross examination of proteoglycan matrix deposition by immunohistochemical evaluation for chondrocytes encapsulated in nondegradable PEG or degradable PEG-LA hydrogels and cultured up to 28 days is shown. PEG hydrogels have staining largely in the pericellular region, whereas the incorporation of degradation through PEG-LA allows for matrix deposition that more closely approximates the articular cartilage. Sections were stained using antibodies against chondroitin-6-sulfate (red), aggrecan (red), and link protein (red). Cell nuclei (blue) were counterstained using DAPI. Bovine articular cartilage explants were also stained. Images were acquired by laser scanning confocal microscopy. Scale bars represent 50 μm.
Gross examination of collagen matrix deposition by immunohistochemical evaluation for chondrocytes encapsulated in nondegradable PEG or degradable PEG-LA hydrogels and cultured up to 28 days is shown. PEG hydrogels have staining largely in the pericellular region, whereas the incorporation of degradation through PEG-LA allows for matrix deposition that more closely approximates the articular cartilage. Sections were stained using antibodies against collagen II (green), collagen VI (green), and decorin (red). Cell nuclei (blue) were counterstained using DAPI. Bovine articular cartilage explants were also stained. Images were acquired by laser scanning confocal microscopy. Scale bars represent 50 μm.
The duration of loading (1 week versus 4 weeks) had minimal effects on neotissue deposition for each hydrogel formulation. In nondegrading hydrogels, loading duration did not affect sGAG content (Fig. 5A), but the higher loading duration led to increased (p = 0.064) collagen content (Fig. 5C). Degradation led to reduced sGAG content when subjected to either loading duration but increased collagen content, by 9.7-fold (p = 0.021), when subjected to 1-week loading duration. There was detectable matrix loss from the loaded constructs as measured by sGAGs released into the culture medium (Fig. 5B), which was accentuated by hydrogel degradation. Compressive modulus (Table 1) was lowest (p ≤ 0.003) in degrading hydrogels. In addition, the major cartilage components, chondoritin-6-suflate, aggrecan, and collagens II and VI (Fig. 6), were present in loaded hydrogels and were largely restricted to the PCM in nondegrading hydrogels but were located throughout in degrading hydrogels. Increased loading duration, however, led to more defects and a localized presence of collagen II in the PCM in degradable hydrogels.
Graphs show the matrix content of nondegradable PEG (dark gray) and degradable PEG-LA (light gray) hydrogels cultured up to 28 days under 1-week intermittent dynamic compressive loading followed by 3 weeks free swelling (stripes) or 4 weeks of intermittent dynamic compressive loading (solid): (A) accumulation of sGAG in the construct normalized to Day 0; (B) cumulative sGAG released into the culture medium; and (C) accumulation of total collagen in the construct normalized to Day 0. Day 0 correlates to the 24-hour preconditioning time point and immediately before loading. Loading duration did not affect the sGAG or collagen contents; however, degradable hydrogels had decreased sGAG within the hydrogel and enhanced sGAG lost to the medium but enhanced collagen within the hydrogel. Data are represented as mean ± SD.
Gross examination of cartilage matrix deposition by immunohistochemical evaluation for chondrocytes encapsulated in nondegradable PEG or degradable PEG-LA hydrogels and cultured up to 28 days is shown. PEG-LA hydrogels had defects, whereas the PEG hydrogels did not. Additionally, longer loading durations (4 weeks) enhanced the formation of defects in PEG-LA hydrogels compared with those loaded for 1 week and free swelling for 3 weeks. Sections were stained using antibodies against chondroitin-6-sulfate (red), aggrecan (red), collagen II (green), and collagen VI (green). Cell nuclei (blue) were counterstained using DAPI. Images were acquired by laser scanning confocal microscopy. Scale bars represent 50 μm.
The application of dynamic mechanical loading did not affect matrix deposition within nondegrading PEG hydrogels but negatively impacted matrix deposition within degrading PEG-LA hydrogels at early culture times (14 days) (Fig. 7). For example, after 14 days, the percent change in sGAG and collagen contents was −40% (p = 0.057) and −85% (p = 0.011), respectively, for degrading hydrogels subjected to a 4-week load duration. However, by 28 days, sGAG and collagen contents were similar to their free-swelling counterparts. Degradation resulted in higher (p = 0.018 and 0.036) sGAG loss at 14 days and 28 days, respectively, for the 1-week loading duration.
Graphs show the matrix content of nondegradable PEG (dark gray) and degradable PEG-LA (light gray) hydrogels cultured up to 28 days under 1-week intermittent dynamic compressive loading followed by 3 weeks free swelling (stripes) or 4 weeks of intermittent dynamic compressive loading (solid): (A) accumulation of sGAG in the construct, (B) cumulative sGAG released into the culture medium normalized to the amount of sGAG in the construct, and (C) accumulation of total collagen in the construct, all expressed as % change from free swelling. Loaded nondegradable constructs had increased sGAG within the construct and less sGAG lost to the medium, whereas degradation increased loss of sGAG from the construct to the medium when compared with free-swelling counterparts after 28 days. Data are represented as mean ± SD. *p values above a column indicate differences from free-swelling constructs.
Discussion
In designing scaffolds for delivering chondrocytes in situ, several factors should be considered, including the roles that scaffold degradation and the dynamic mechanical environment have on neotissue development. Because PEG-based hydrogels are promising cell carriers for in vivo cartilage regeneration, we addressed three important questions regarding how tissue development is impacted: (1) by hydrogel degradation in the absence of loading; (2) by the type of loading, specifically load duration, as a function of hydrogel degradation; and (3) in general by loading when compared with tissue developed without loading.
We acknowledge several limitations. First, findings from this study are limited to one PEG-LA formulation and one loading regime (frequency, strain, intermittent loading pattern). This formulation was chosen based on previous studies, which showed that faster degrading PEG-LA hydrogels led to cartilage-like engineered tissue that contained large defects, indicating degradation was too fast [6]. The loading regime was selected because it falls within physiologic ranges [33] and reportedly enhances cartilage ECM mRNA levels over unloaded nondegrading PEG hydrogels [31]. Although the conditions chosen resulted in fewer defects, slower degrading hydrogels and/or different loading regimes may better match neotissue development. Second, adolescent bovine chondrocytes were used because they are easily obtained in large quantities. However, adolescent chondrocytes have higher metabolic rates and synthesize greater amounts of ECM over adult chondrocytes [23] and cell response may be species-specific. Thus, hydrogels may require redesigning to regenerate human cartilage for clinical applications. Nonetheless, these limitations do not jeopardize our overall conclusions but instead underscore the importance of scaffold selection and degradation in a loading environment.
Our findings demonstrate scaffold degradation is essential for macroscopic tissue formation when using PEG-based hydrogels where cells are encapsulated. One of the challenges in regenerating cartilage is supporting deposition of collagen II and aggrecan, which can reach dimensions of a few micrometers [14, 22]. A crosslinked hydrogel inherently creates a mesh-like structure with dimensions approximately 150 to 200 Å for similar hydrogels [5], which hindered matrix evolution. Degradation permitted matrix diffusion, leading to immature neocartilage comprised of approximately 11% to 12% sGAGs and approximately 14% to 32% total collagens by dry weight with a compressive modulus that was twofold lower than native cartilage. For collagen to diffuse, near-complete degradation must occur [8], which may account for the low collagen content (approximately 20% of native cartilage). Longer culture times may be required to develop a mature and mechanically strong cartilage. Although findings from this study agree with previous reports regarding macroscopic deposition of sGAGs and collagen [4, 9], we demonstrate the main building blocks of cartilage ECM (aggrecan and collagen II), primary matrix molecules found in the PCM (collagen VI), and matrix molecules associated with assembly (link protein and decorin) are also present. Overall, these findings demonstrate a cartilage-like matrix is developing comprised of key macromolecules necessary for forming functional cartilage.
The data also demonstrate load duration applied to PEG-based hydrogels had minimal effects on matrix content but affected spatial distribution of matrix. Loading was applied early in culture based on previous studies [29, 38], indicating chondrocytes are more responsive when loading is applied before a protective PCM forms. Chondrocytes when encapsulated in PEG-based hydrogels generally synthesized neotissue with similar matrix contents regardless of load duration, suggesting cells are less sensitive to loading in the long term. This observation may be partly the result of the formation of a stiff PCM, which occurs within 1 week, preventing cells from deforming under applied strains [7], especially when surrounded by a hydrogel or neotissue that is 10- to 100-fold less stiff than native cartilage. It is possible, with the development of mechanically strong engineered cartilage, cells may become more responsive to loading in the long term [14]. However, load duration impacted spatial development of neotissue. Although mechanically stimulated degradable hydrogels were capable of promoting neotissue comprised of cartilage-specific matrix, the higher loading duration led to large tissue defects and a more localized tissue surrounding the cells, indicating load-induced degradation. These findings suggest the duration of loading may be less critical to matrix content but critical to spatial distribution of matrix.
Dynamic loading generally had no effect on matrix content in nondegrading hydrogels but had a negative impact on matrix contents in degrading hydrogels, although this observation was only temporary. Because changes in the hydrogel structure and mechanical properties occur during degradation, the mechanical cues sensed by the cells will inevitably change, which may have altered mechanotransduction events and led to decreased matrix synthesis. Alternatively, there may have been load-induced matrix loss, although sGAG loss was not higher in loaded versus free-swelling constructs. However, by 4 weeks, loading led to increases in matrix deposition whereby matrix content of the engineered tissue reached similar contents to the tissue developed under free-swelling conditions. This finding suggests loading may have stimulated matrix synthesis in chondrocytes once some tissue had been deposited. Longer culture times may provide more insights into whether loading has long-term positive effects on tissue development [14]. Nonetheless, these findings suggest loading does not have a large impact on tissue content for two distinctly different PEG-based hydrogels (ie, nondegrading and fast degrading) at least for the loading conditions and culture times investigated.
The ability to incorporate degradation into PEG-based hydrogels and control degradation through simple formulation changes makes these materials promising for tissue engineering [1, 5, 6, 8, 9]. The appropriate degradation rate required to align scaffold degradation with neotissue development is still under investigation but will be impacted by dynamic mechanical loading, especially when degrading hydrogels are used. Loading appears to have a greater impact on the spatial composition of neotissue, resulting in tissue defects and to a lesser degree on neotissue content. Overall, these findings are promising in that PEG-LA hydrogels lead to macroscopic development of tissue comprised of key cartilage matrix molecules but underscore scaffold degradation should be further tuned when loading is present.
References
Anseth KS, Metters AT, Bryant SJ, Martens PJ, Elisseeff JH, Bowman CN. In situ forming degradable networks and their application in tissue engineering and drug delivery. J Control Release. 2002;78:199–209.
Babalola OM, Bonassar LJ. Parametric finite element analysis of physical stimuli resulting from mechanical stimulation of tissue engineered cartilage. J Biomech Eng. 2009;131:061014.
Bhosale AM, Richardson JB. Articular cartilage: structure, injuries and review of management. Br Med Bull. 2008;87:77–95.
Bryant SJ. Photocrosslinkable Hydrogels as Cell-scaffolds for Tissue Engineering Cartilage: A Study Examining Gel Properties, Degradation, Mechanical Loading, and Clinical Relevance. Boulder, CO: Chemical Engineering, University of Colorado-Boulder; 2002.
Bryant SJ, Anseth KS. Hydrogel properties influence ECM production by chondrocytes photoencapsulated in poly(ethylene glycol) hydrogels. J Biomed Mater Res. 2002;59:63–72.
Bryant SJ, Anseth KS. Controlling the spatial distribution of ECM components in degradable PEG hydrogels for tissue engineering cartilage. J Biomed Mater Res A. 2003;64:70–79.
Bryant SJ, Anseth KS, Lee DA, Bader DL. Crosslinking density influences the morphology of chondrocytes photoencapsulated in PEG hydrogels during the application of compressive strain. J Orthop Res. 2004;22:1143–1149.
Bryant SJ, Bender RJ, Durand KL, Anseth KS. Encapsulating chondrocytes in degrading PEG hydrogels with high modulus: engineering gel structural changes to facilitate cartilaginous tissue production. Biotechnol Bioeng. 2004;86:747–755.
Bryant SJ, Durand KL, Anseth KS. Manipulations in hydrogel chemistry control photoencapsulated chondrocyte behavior and their extracellular matrix production. J Biomed Mater Res A. 2003;67:1430–1436.
Farndale RW, Buttle DJ, Barrett AJ. Improved quantitation and discrimination of sulfated glycosaminoglycans by use of dimethylmethylene blue. Biochim Biophys Acta. 1986;883:173–177.
Gillogly SD, Voight M, Blackburn T. Treatment of articular cartilage defects of the knee with autologous chondrocyte implantation. J Orthop Sports Phys Ther. 1998;28:241–251.
Grodzinsky AJ, Levenston ME, Jin M, Frank EH. Cartilage tissue remodeling in response to mechanical forces. Annu Rev Biomed Eng. 2000;2:691–713.
Hollander AP, Heathfield TF, Webber C, Iwata Y, Bourne R, Rorabeck C, Poole AR. Increased damage to type II collagen in osteoarthritic articular cartilage detected by a new immunoassay. J Clin Invest. 1994;93:1722–1732.
Hung CT, Mauck RL, Wang CCB, Lima EG, Ateshian GA. A paradigm for functional tissue engineering of articular cartilage via applied physiologic deformational loading. Ann Biomed Eng. 2004;32:35–49.
Hunter CJ, Mouw JK, Levenston ME. Dynamic compression of chondrocyte-seeded fibrin gels: effects on matrix accumulation and mechanical stiffness. Osteoarthritis Cartilage. 2004;12:117–130.
Kisiday JD, Jin MS, DiMicco MA, Kurz B, Grodzinsky AJ. Effects of dynamic compressive loading on chondrocyte biosynthesis in self-assembling peptide scaffolds. J Biomech. 2004;37:595–604.
Kisiday JD, Lee JH, Siparsky PN, Frisbie DD, Flannery CR, Sandy JD, Grodzinsky AJ. Catabolic responses of chondrocyte-seeded peptide hydrogel to dynamic compression. Ann Biomed Eng. 2009;37:1368–1375.
Knight MM, Lee DA, Bader DL. The influence of elaborated pericellular matrix on the deformation of isolated articular chondrocytes cultured in agarose. Biochim Biophys Acta. 1998;1405:67–77.
Lee CR, Grodzinsky AJ, Spector M. Biosynthetic response of passaged chondrocytes in a type II collagen scaffold to mechanical compression. J Biomed Mater Res A. 2003;64:560–569.
Lee DA, Bader DL. Compressive strains at physiological frequencies influence the metabolism of chondrocytes seeded in agarose. J Orthop Res. 1997;15:181–188.
Lin-Gibson S, Bencherif S, Cooper JA, Wetzel SJ, Antonucci JM, Vogel BM, Horkay F, Washburn NR. Synthesis and characterization of PEG dimethacrylates and their hydrogels. Biomacromolecules. 2004;5:1280–1287.
Mark KVD. Structure, biosynthesis, and gene regulation of collagens in cartilage and bones. In: Seibel MJ, Robins SP, Bilezikian JP, eds. Dynamics of Bone and Cartilage Metabolism. Vol 1. 2nd ed. Burlington, VT: Elsevier; 2006:3–40.
Martin JA, Buckwalter JA. Roles of articular cartilage aging and chondrocyte senescence in the pathogenesis of osteoarthritis. Iowa Orthop J. 2001;21:1–7.
McLaren AC, Blokker CP, Fowler PJ, Roth JN, Rock MG. Arthroscopic débridement of the knee for osteoarthrosis. Can J Surg. 1991;34:595–598.
Metters AT, Anseth KS, Bowman CN. Fundamental studies of a novel, biodegradable PEG-b-PLA hydrogel. Polymer. 2000;41:3993–4004.
Metters AT, Bowman CN, Anseth KS. A statistical kinetic model for the bulk degradation of PLA-b-PEG-b-PLA hydrogel networks. J Phys Chem B. 2000;104:7043–7049.
Metters AT, Bowman CN, Anseth KS. Verification of scaling laws for degrading PLA-b-PEG-b-PLA hydrogels. AIChE J. 2001;47:1432–1437.
Nicodemus GD, Bryant SJ. Cell encapsulation in biodegradable hydrogels for tissue engineering applications. Tissue Eng Part B Rev. 2008;14:149–165.
Nicodemus GD, Bryant SJ. Mechanical loading regimes affect the anabolic and catabolic activities by chondrocytes encapsulated in PEG hydrogels. Osteoarthritis Cartilage. 2010;18:126–137.
Nicodemus GD, Shiplet KA, Kaltz SR, Bryant SJ. Dynamic compressive loading influences degradation behavior of PEG-PLA hydrogels. Biotechnol Bioeng. 2009;102:948–959.
Nicodemus GD, Villanueva I, Bryant SJ. Mechanical stimulation of TMJ condylar chondrocytes encapsulated in PEG hydrogels. J Biomed Mater Res A. 2007;83:323–331.
Robling AG, Burr DB, Turner CH. Partitioning a daily mechanical stimulus into discrete loading bouts improves the osteogenic response to loading. J Bone Miner Res. 2000;15:1596–1602.
Sah RL, Kim YJ, Doong JYH, Grodzinsky AJ, Plaas AH, Sandy JD. Biosynthetic response of cartilage explants to dynamic compression. J Orthop Res. 1989;7:619–636.
Sawhney AS, Pathak CP, Hubbell JA. Bioerodible hydrogels based on photopolymerized poly(ethylene glycol)-co-poly(alpha-hydroxy acid) diacrylate macromers. Macromolecules. 1993;26:581–587.
Sledge SL. Microfracture techniques in the treatment of osteochondral injuries. Clin Sports Med. 2001;20:365–377.
Steadman JR, Rodkey WG, Briggs KK, Rodrigo JJ. The microfracture technic in the management of complete cartilage defects in the knee joint [in German]. Orthopade. 1999;28:26–32.
Villanueva I, Hauschulz DS, Mejic D, Bryant SJ. Static and dynamic compressive strains influence nitric oxide production and chondrocyte bioactivity when encapsulated in PEG hydrogels of different crosslinking densities. Osteoarthritis Cartilage. 2008;16:909–918.
Waldman SD, Couto DC, Grynpas MD, Pilliar RM, Kandel RA. A single application of cyclic loading can accelerate matrix deposition and enhance the properties of tissue-engineered cartilage. Osteoarthritis Cartilage. 2006;14:323–330.
Woessner JF. Determination of hydroxyproline in tissue and protein samples containing small proportions of this amino acid. Arch Biochem Biophys. 1961;93:440–447.
Acknowledgments
The antibodies developed by B. Caterson (link protein) and G. A. Pringle (decorin) used here were obtained from the Developmental Studies Hybridoma Bank developed under the auspices of the NICHD and maintained by the Department of Biology, University of Iowa, Iowa City, IA.
Author information
Authors and Affiliations
Corresponding author
Additional information
The institution of the authors has received funding from the NIH/NIDCR (K22DE016608) and the NIH/NIAMS (R01AR053126); one of the authors (JJR) has received funding from the National Institute of Health’s Leadership Training in Pharmaceutical Biotechnology Program; two of the authors (JJR, GDN) have received funding from the Department of Education’s Graduate Assistantships in Areas of National Need (GAANN) fellowships.
About this article
Cite this article
Roberts, J.J., Nicodemus, G.D., Greenwald, E.C. et al. Degradation Improves Tissue Formation in (Un)Loaded Chondrocyte-laden Hydrogels. Clin Orthop Relat Res 469, 2725–2734 (2011). https://doi.org/10.1007/s11999-011-1823-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-011-1823-0