Abstract
Osteoarthritis (OA) is a major chronic disease of the joints, affecting mostly the articular cartilage but also all the surrounding tissues including the subchondral bone, synovium, meniscus, tendons, and ligaments. Despite the availability in the clinic of a variety of therapeutic approaches, there is crucial need for improved treatment to protect and regenerate the cartilage with full integrity and function. In this regard, combining gene, cell, and tissue engineering-based procedures is an attractive concept for novel, effective therapy against AO, a slow, progressive, and irreversible disease. Here, we provide an overview of the treatment available for management of the progression of the OA phenotype and discuss current progress and remaining challenges for potential future treatment of patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
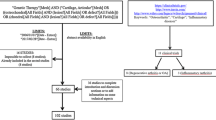
Osteoarthritis (OA) is a highly prevalent, critical cause of physical disability without a definitive cure. On onset OA is mainly characterized by gradual loss of articular cartilage because of impaired anabolic and/or catabolic balance; the disease then further affects all other joint tissues (subchondral bone, synovial membrane, capsule, menisci, tendons, ligaments and periarticular muscles) [1, 2]. For patients who are too young to undergo joint replacement or for individuals at earlier stages of OA, in particular, there is a significant need to develop novel therapy to protect the cartilage, inhibiting further loss or even re-establishing its structural integrity. Such approaches as structure and/or disease-modifying drugs have not yet been successful, leaving joint arthroplasty as unmatched therapy for restoration of function and alleviation of pain. A better understanding of the factors and mechanisms leading to OA has enabled significant advances in the design of novel treatment for OA that has been tested in preclinical models. OA is a highly complex, multifactorial disease with a substantial genetic background [1, 3]. OA may be also caused by secondary issues, for example axial malalignment, loss of meniscal tissue, or repetitive stress injury. Pathological loading is another critical factor in OA [1, 4], because the response of cells in the joint to mechanical signals is impaired during OA. Obesity and production of adipokines also alter cartilage homeostasis in the joint and lead to OA [4]. OA is also strongly linked to aging processes, including mitochondrial dysfunction and changes in signaling pathways [5, 6]. Epigenetic events controlling a large group of disease-related genes have also been reported to be critically important in OA [7]. On the basis of this new knowledge, strategies using gene therapy and tissue engineering have become very attractive for developing treatments that could enable durable restoration of such joint tissues as cartilage when OA becomes irreversible (Fig. 1).
Strategies Used to Treat OA
Target Cells
Although articular chondrocytes are the primary targets of viral gene transfer approaches to treatment of OA, other cells relevant to the pathogenesis of OA may be genetically modified to target different cellular processes or specific tissue types (Table 1). The many cell types present in subchondral bone are important targets for correcting the disrupted physiological relationship between the bone and the articular cartilage [2]. Pathological subchondral bone changes in OA that must be addressed include, for example, increased bone formation and turnover, changes in its microstructure, and the formation of osteophytes [2].
Target Pathways
Reproduction of the native, structural, and functional cartilage may be achieved by targeting different levels in the affected cells via:
-
1.
inhibition of inflammatory and catabolic pathways that lead to joint surface degeneration;
-
2.
stimulation of anabolic pathways for restoration of the damaged cartilage by promoting the production of essential components of the extracellular matrix (ECM);
-
3.
activation of cell proliferation and survival, while preventing apoptosis and aging, to revitalize the resident cells in cartilage in the early stages of OA disease, or in the setting of transplantation;
-
4.
prevention of endochondral ossification processes involved in osteophyte formation, vascular invasion of the cartilage at the subchondral bone junction, and cartilage calcification;
-
5.
modulation of OA-related epigenetic events that control OA disease-related gene expression and post-translational modifications;
-
6.
modification of the multiple genetic, or hereditary, components of OA; and
-
7.
combination of strategies that by themselves do not enable complete reproduction of the original chondrocyte phenotype and cartilage structure.
Choice of a Gene Transfer Vector
A variety of viral vectors are available to achieve this objective, each of which has advantages and limitations because of the biology of the viruses from which they are derived (Table 2).
Adenoviral Vectors
Adenoviral vectors enable very high transduction efficiencies and levels of transgene expression in vitro (more than 80 % and close to 100 %) [8–41], but serious concerns remain about their safety because of immunogenicity in vivo and short-term efficacy (1 to 2 weeks maximum), which are critical issues in the context of a slow, progressive disease such as OA.
Retroviral Vectors
These vectors can become integrated into the host genome, enabling long-term maintenance of the transgenes delivered. However, integration may lead to insertional mutagenesis and activation of tumorigenic genes. Furthermore, retroviral vectors can only transduce dividing cells and at relatively low efficacy (<20 % before cell selection) [12–14, 24, 28, 42–44, 45•, 46–52], making them unsuitable for targeting adult chondrocytes with low proliferative activity.
Lentiviral Vectors
Lentiviral vectors are good alternatives, because they can become integrated into the genome of nondividing cells, and have higher levels of transduction (at least 70 %) [53•, 54, 55•, 56], although concerns remain about their potential for insertional mutagenesis.
Recombinant Adeno-Associated Virus (rAAV) Vectors
rAAV are derived from a nonpathogenic, replication-defective human parvovirus and are much less immunogenic than adenoviruses. Stable, episomal rAAV transgenes are expressed with high efficiency (>65 %) in dividing and nondividing cells for extended periods of time (at least 150 days in situ) and can access the cells via dense ECM [33, 57–87]. The use of self-complementary AAV (scAAV) has enabled, at least in part, circumvention of the step-limiting conversion of single-stranded into double-stranded DNA [64, 66, 67, 69, 70, 86]. Trans-splicing systems have also been used successfully to improve the size capacity of the vectors [88]. For these various reasons, rAAV has become the vector of choice for clinical applications.
Use of Biocompatible Materials
The advantage of using a biomaterial to treat joint disorders is that it enables spatially and temporarily controlled delivery and expression of the candidate therapeutic gene to the sites of injury. Interestingly, despite the availability of many biocompatible materials in research on this topic, relatively few have been used for treatment of OA as opposed to focal articular cartilage defects. They mostly include collagen gels [89, 90] and hyaluronic acid [91].
Evidence in Vitro
Whereas most of the vectors mentioned above have been used successfully to transduce most, if not all, of the cells relevant to the pathogenesis of OA in experimental systems in vitro, thus far, only rAAV vectors are capable of modifying the cells in situ when they are located in their natural ECM environment. Table 3 gives an overview of the combined strategies currently used in vitro.
Inhibition of Inflammatory and Catabolic Pathways
Many studies focusing on limiting or blocking cartilage loss have been performed in vitro or in vivo, using viral vectors to drive expression of inhibitors of matrix-degrading enzymes and of inflammatory pathways (IL-1Ra, sIL-1R, IL-1-specific shRNA, sTNFR, TIMPs, IκBα, NF-κBp65-specific siRNA, kallistatin, thrombospondin-1, pro-opiomelanocortin, Dkk-1, ADAMTS-5-specific siRNA, heme oxygenase-1) [8, 11, 17, 19, 20, 35, 49, 52, 54, 55•, 66, 69, 71, 77, 79, 80, 86]. Their effects may be enhanced by using a three-dimensionally woven, porous, biomimetic poly(ε-caprolactone) (PCL) scaffold [55•]. Alternatively, such chondroprotective cytokines as IL-4 and IL-10 can be delivered in viral vectors [52].
Stimulation of Anabolic Pathways
Successful activation of anabolic processes has been reported upon viral delivery of enzymes that produce or process ECM components [15], growth factors, including IGF-I, FGF-2, BMPs, TGF-β, GDF-5, HGF, PTHrP, Indian hedgehog (IHH), scleraxis [16–18, 22, 25, 26, 29–32, 36–38, 40, 41, 43, 47, 48, 53•, 58, 60, 64, 78, 83, 87, 92]. Because many of these are involved in endochondral ossification during skeletal development, osteophyte formation, cartilage calcification, and abnormal bone changes may occur in vivo. Scaffolds such as PCL scaffold [53•], or tissue-specific transcription factors (SOX5, SOX6, SOX9) [9, 21, 23, 24, 45•, 51, 59, 63, 85] have been used to enhance anabolism.
Activation of Cell Proliferation and Survival—Prevention of Apoptosis and Aging
The restoration or activation of cell vitality and proliferation can be achieved by application of IGF-I, FGF-2, BMPs, TGF-β [58, 60–62, 72, 87, 92], telomerase (hTERT) [44, 50, 56], or inhibitors of apoptosis (kallistatin) [20].
Prevention of Osteophyte Formation and Cartilage Vascular Invasion
Studies in vivo have provided antagonists of the TGF-β/BMP pathway, for example latency-associated peptide and inhibitory Smads, which inhibit osteophyte formation [34]. Inhibition of vascular invasion has been attempted using sFlt-1, a soluble receptor that acts a vascular endothelial growth factor antagonist, preventing angiogenesis and cartilage resorption and resulting in persistent cartilage regeneration and repair in a rat model of OA [48]. Similar results were obtained when applying other types of inhibitor of angiogenesis, for example thrombospondin-1, leading to reduced microvessel density, inflammation, and suppression of the progression of OA in a model of anterior cruciate ligament transection (ACLT) in rats [19]. Gene transfer of chondromodulin has also been reported to inhibit the invasion of vessel structures, endochondral ossification, and terminal chondrocyte hypertrophy in porcine cartilage lesions while stimulating chondrogenic differentiation and the formation of hyaline-like matrix in the lesions [70]. Also, remarkably, application of pro-opiomelanocortin (POMC), a precursor of neuropeptides with potent anti-inflammatory activity, has been shown to suppress microvessel density, reduce NF-κB activity, and prevent the progression and severity of ACLT-induced OA in rats [35].
Modulation of OA-Related Epigenetic Events
With the identification of functional miRNAs, new molecular therapy can be envisaged, for example delivery of miRNAs to modulate the production of proinflammatory cytokines [93], down-regulate the expression of matrix-degrading enzymes [94], or up-regulate type-II collagen expression [95]. Also, remarkably, gene transfer of sirtuin 1, a histone deacetylase, has been shown to protect chondrocytes under stress conditions [96, 97]; it thus has strong promise as a new therapeutic approach.
Modification of Genetic Factors in OA
Therapy compensating for loss of function or inhibiting undesirable gene overexpression in OA might be envisaged but, so far, little work has been performed to address this crucial issue.
Combined Approaches
Successful co-transfer of different factors has been achieved by providing combinations of activators of anabolic and proliferative processes [21, 61], inhibitors of catabolic pathways [52], or inhibitors of catabolism with activators of anabolic and proliferative pathways [17, 27, 30]. Another interesting approach has been developed recently on the basis of co-application of anabolic factors with specific silencers of potentially undesirable cellular processes, for example a combination of TGF-β with a small hairpin RNA to silence type-I collagen expression and thus minimize the formation of fibrocartilage [98].
Evidence in Vivo
Gene engineering and tissue engineering-based treatment of OA in vivo might, in theory, be achieved either by providing a biomaterial coated with a gene-transfer vector (direct approach) or by using a scaffold carrying or seeded with genetically modified cells (indirect approach). Direct procedures are simpler and more convenient, because they are less invasive, yet indirect strategies might be desirable in cases of advanced, severe OA in which little cartilage surface and few chondrocytes remain and when cell repopulation is required.
In contrast with the literature on focal cartilage defects [9, 45•, 99–103], few studies have examined the benefits of applying viral gene transfer methods concomitantly with a biocompatible material (hydrogel compounds or solid scaffolds) to treat experimental models reflective of the complex pathology of OA. So far, only Lee et al. [45•] have demonstrated the benefits of injecting adipose-derived stem cells that had been retrovirally-co-transduced with the SOX trio and suspended in fibrin glue to prevent the progression of degenerative changes in surgically induced OA in rats (Table 3). Therapeutic approaches for OA in vivo have, instead, focused on administration of gene transfer vectors [11, 19, 20, 34, 35, 66, 80, 104] and of genetically modified cells [48, 52, 105] in the absence of supportive matrices.
Conclusions
Because of the remarkable advances in experimental research in cell biology, molecular biology (therapeutic candidate factors and genes), biomaterials, and translational science, gene engineering and tissue engineering-based strategies are attractive approaches to repair of joint tissues in OA. There is a large body of evidence showing the benefits of gene therapy for OA, including two clinical trials of indirect administration of retrovirally-modified, TGF-β-expressing chondrocytes [106] and direct delivery of IL-1Ra via rAAV [107]. However, little is known about the value of combining such a methods with use of biocompatible materials both in vitro and in experimental models of the disease in vivo compared with current knowledge on the advantages of this approach for focal cartilage defects. Among unanswered questions, the choice of an appropriate scaffold for treatment of large OA lesions compared with defined focal defects may be the most complex to address, because such issues as the best source of cells, candidate gene, and vector (most likely rAAV) have been, in general, well investigated. It will also be important to keep in mind that the products used to generate a new treatment will need challenging approval by the regulatory organizations before use in a clinical procedure. Only a combined effort among scientists, clinicians, industry, and regulatory organizations will enable us to address the crucial issue of treating the slow, progressive disease in OA patients.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Goldring MB. Chondrogenesis, chondrocyte differentiation, and articular cartilage metabolism in health and osteoarthritis. Ther Adv Musculoskelet Dis. 2012;4(4):269–85.
Loeser RF, Goldring SR, Scanzello CR, Goldring MB. Osteoarthritis: a disease of the joint as an organ. Arthritis Rheum. 2012;64(6):1697–707.
Sandell LJ. Etiology of osteoarthritis: genetics and synovial joint development. Nat Rev Rheumatol. 2012;8(2):77–89.
Guilak F. Biomechanical factors in osteoarthritis. Best Pract Res Clin Rheumatol. 2011;25(6):815–23.
Lotz M, Loeser RF. Effects of aging on articular cartilage homeostasis. Bone. 2012;51(2):241–8.
van den Berg WB. Osteoarthritis year 2010 in review: pathomechanisms. Osteoarthr Cartil. 2011;19(4):338–41.
Goldring MB, Marcu KB. Epigenomic and microRNA-mediated regulation in cartilage development, homeostasis, and osteoarthritis. Trends Mol Med. 2012;18(2):109–18.
Baragi VM, Renkiewicz RR, Jordan H, Bonadio J, Hartman JW, Roessler BJ. Transplantation of transduced chondrocytes protects articular cartilage from interleukin 1-induced extracellular matrix degradation. J Clin Invest. 1995;96(5):2454–60.
Cao L, Yang F, Liu G, Yu D, Li H, Fan Q, et al. The promotion of cartilage defect repair using adenovirus mediated Sox9 gene transfer of rabbit bone marrow mesenchymal stem cells. Biomaterials. 2011;32(16):3910–20.
Doherty PJ, Zhang H, Tremblay L, Manolopoulos V, Marshall KW. Resurfacing of articular cartilage explants with genetically-modified human chondrocytes in vitro. Osteoarthr Cartil. 1998;6(3):153–9.
Frisbie DD, Ghivizzani SC, Robbins PD, Evans CH, McIlwraith CW. Treatment of experimental equine osteoarthritis by in vivo delivery of the equine interleukin-1 receptor antagonist gene. Gene Ther. 2002;9(1):12–20.
Gerich TG, Ghivizani S, Fu FH, Robbins PD, Evans CH. Gene transfer into the patellar tendon of rabbits: a preliminary study of locoregional expression of growth factors. Wien Klin Wochenschr. 1997;109(11):384–9.
Gerich TG, Lobenhoffer HP, Fu FH, Robbins PD, Evans CH. Virally mediated gene transfer in the patellar tendon. An experimental study in rabbits. Unfallchirurg. 1997;100(5):354–62.
Goto H, Shuler FD, Lamsam C, Moller HD, Niyibizi C, Fu FH, et al. Transfer of lacZ marker gene to the meniscus. J Bone Joint Surg Am. 1999;81(7):918–25.
Gouze JN, Gouze E, Palmer GD, Kaneto H, Ghivizzani SC, Grodzinsky AJ, et al. Adenovirus-mediated gene transfer of glutamine: fructose-6-phosphate amidotransferase antagonizes the effects of interleukin-1beta on rat chondrocytes. Osteoarthr Cartil. 2004;12(3):217–24.
Hao J, Yao Y, Varshney RR, Wang L, Prakash C, Li H, et al. Gene transfer and living release of transforming growth factor-beta3 for cartilage tissue engineering applications. Tissue Eng Part C. 2008;14(4):273–80.
Haupt JL, Frisbie DD, McIlwraith CW, Robbins PD, Ghivizzani S, Evans CH, et al. Dual transduction of insulin-like growth factor-I and interleukin-1 receptor antagonist protein controls cartilage degradation in an osteoarthritic culture model. J Orthop Res. 2005;23(1):118–26.
Hidaka C, Ibarra C, Hannafin JA, Torzilli PA, Quitoriano M, Jen SS, et al. Formation of vascularized meniscal tissue by combining gene therapy with tissue engineering. Tissue Eng. 2002;8(1):93–105.
Hsieh JL, Shen PC, Shiau AL, Jou IM, Lee CH, Wang CR, et al. Intraarticular gene transfer of thrombospondin-1 suppresses the disease progression of experimental osteoarthritis. J Orthop Res. 2010;28(10):1300–6.
Hsieh JL, Shen PC, Shiau AL, Jou IM, Lee CH, Teo ML, et al. Adenovirus-mediated kallistatin gene transfer ameliorates disease progression in a rat model of osteoarthritis induced by anterior cruciate ligament transection. Hum Gene Ther. 2009;20(2):147–58.
Ikeda T, Kamekura S, Mabuchi A, Kou I, Seki S, Takato T, et al. The combination of SOX5, SOX6, and SOX9 (the SOX trio) provides signals sufficient for induction of permanent cartilage. Arthritis Rheum. 2004;50(11):3561–73.
Kawamura K, Chu CR, Sobajima S, Robbins PD, Fu FH, Izzo NJ, et al. Adenoviral-mediated transfer of TGF-beta1 but not IGF-1 induces chondrogenic differentiation of human mesenchymal stem cells in pellet cultures. Exp Hematol. 2005;33(8):865–72.
Kupcsik L, Stoddart MJ, Li Z, Benneker LM, Alini M. Improving chondrogenesis: potential and limitations of SOX9 gene transfer and mechanical stimulation for cartilage tissue engineering. Tissue Eng Part A. 2010;16(6):1845–55.
Li Y, Tew SR, Russell AM, Gonzalez KR, Hardingham TE, Hawkins RE. Transduction of passaged human articular chondrocytes with adenoviral, retroviral, and lentiviral vectors and the effects of enhanced expression of SOX9. Tissue Eng. 2004;10(3–4):575–84.
Menendez MI, Clark DJ, Carlton M, Flanigan DC, Jia G, Sammet S, et al. Direct delayed human adenoviral BMP-2 or BMP-6 gene therapy for bone and cartilage regeneration in a pony osteochondral model. Osteoarthr Cartil. 2011;19(8):1066–75.
Mi Z, Ghivizzani SC, Lechman ER, Jaffurs D, Glorioso JC, Evans CH, et al. Adenovirus-mediated gene transfer of insulin-like growth factor 1 stimulates proteoglycan synthesis in rabbit joints. Arthritis Rheum. 2000;43(11):2563–70.
Morisset S, Frisbie DD, Robbins PD, Nixon AJ, McIlwraith CW. IL-1ra/IGF-1 gene therapy modulates repair of microfractured chondral defects. Clin Orthop Relat Res. 2007;462:221–8.
Nita I, Ghivizzani SC, Galea-Lauri J, Bandara G, Georgescu HI, Robbins PD, et al. Direct gene delivery to synovium. An evaluation of potential vectors in vitro and in vivo. Arthritis Rheum. 1996;39(5):820–8.
Nixon AJ, Brower-Toland BD, Bent SJ, Saxer RA, Wilke MJ, Robbins PD, et al. Insulin-like growth factor-I gene therapy applications for cartilage repair. Clin Orthop. 2000;379(Suppl):S201–13.
Nixon AJ, Haupt JL, Frisbie DD, Morisset SS, McIlwraith CW, Robbins PD, et al. Gene-mediated restoration of cartilage matrix by combination insulin-like growth factor-I/interleukin-1 receptor antagonist therapy. Gene Ther. 2005;12(2):177–86.
Palmer GD, Steinert A, Pascher A, Gouze E, Gouze JN, Betz O, et al. Gene-induced chondrogenesis of primary mesenchymal stem cells in vitro. Mol Ther. 2005;12(2):219–28.
Park J, Gelse K, Frank S, von der Mark K, Aigner T, Schneider H. Transgene-activated mesenchymal cells for articular cartilage repair: a comparison of primary bone marrow-, perichondrium/periosteum- and fat-derived cells. J Gene Med. 2006;8(1):112–25.
Santangelo KS, Bertone AL. Effective reduction of the interleukin-1beta transcript in osteoarthritis-prone guinea pig chondrocytes via short hairpin RNA mediated RNA interference influences gene expression of mediators implicated in disease pathogenesis. Osteoarthr Cartil. 2011;19(12):1449–57.
Scharstuhl A, Diepens R, Lensen J, Vitters E, van Beuningen H, van der Kraan P, et al. Adenoviral overexpression of Smad-7 and Smad-6 differentially regulates TGF-beta-mediated chondrocyte proliferation and proteoglycan synthesis. Osteoarthr Cartil. 2003;11(11):773–82.
Shen PC, Shiau AL, Jou IM, Lee CH, Tai MH, Juan HY, et al. Inhibition of cartilage damage by pro-opiomelanocortin prohormone overexpression in a rat model of osteoarthritis. Exp Biol Med (Maywood). 2011;236(3):334–40.
Shuler FD, Georgescu HI, Niyibizi C, Studer RK, Mi Z, Johnstone B, et al. Increased matrix synthesis following adenoviral transfer of a transforming growth factor beta1 gene into articular chondrocytes. J Orthop Res. 2000;18(4):585–92.
Smith P, Shuler FD, Georgescu HI, Ghivizzani SC, Johnstone B, Niyibizi C, et al. Genetic enhancement of matrix synthesis by articular chondrocytes: comparison of different growth factor genes in the presence and absence of interleukin-1. Arthritis Rheum. 2000;43(5):1156–64.
Steinert AF, Ghivizzani SC, Rethwilm A, Tuan RS, Evans CH, Noth U. Major biological obstacles for persistent cell-based regeneration of articular cartilage. Arthritis Res Ther. 2007;9(3):213–27.
Steinert AF, Noth U, Tuan RS. Concepts in gene therapy for cartilage repair. Injury. 2008;39 Suppl 1:S97–113.
Steinert AF, Palmer GD, Pilapil C, Noth U, Evans CH, Ghivizzani SC. Enhanced in vitro chondrogenesis of primary mesenchymal stem cells by combined gene transfer. Tissue Eng Part A. 2009;15(5):1127–39.
Steinert AF, Proffen B, Kunz M, Hendrich C, Ghivizzani SC, Noth U, et al. Hypertrophy is induced during the in vitro chondrogenic differentiation of human mesenchymal stem cells by bone morphogenetic protein-2 and bone morphogenetic protein-4 gene transfer. Arthritis Res Ther. 2009;11(5):R148–62.
Allay JA, Dennis JE, Haynesworth SE, Majumdar MK, Clapp DW, Shultz LD, et al. LacZ and interleukin-3 expression in vivo after retroviral transduction of marrow-derived human osteogenic mesenchymal progenitors. Hum Gene Ther. 1997;8(12):1417–27.
Goto H, Shuler FD, Niyibizi C, Fu FH, Robbins PD, Evans CH. Gene therapy for meniscal injury: enhanced synthesis of proteoglycan and collagen by meniscal cells transduced with a TGFbeta(1)gene. Osteoarthr Cartil. 2000;8(4):266–71.
Huang G, Zheng Q, Sun J, Guo C, Yang J, Chen R, et al. Stabilization of cellular properties and differentiation mutilpotential of human mesenchymal stem cells transduced with hTERT gene in a long-term culture. J Cell Biochem. 2008;103(4):1256–69.
Lee JM, Im GI. SOX trio-co-transduced adipose stem cells in fibrin gel to enhance cartilage repair and delay the progression of osteoarthritis in the rat. Biomaterials. 2012;33(7):2016–24. This study indicates the feasibility of combining cell engineering, gene engineering, and tissue engineering-based strategies (retrovirally-transduced adipose-derived stem cells to overexpress SOX9 in fibrin glue) as a means of significantly improving the healing of cartilage lesions in OA in vivo.
Martinek V, Usas A, Pelinkovic D, Robbins P, Fu FH, Huard J. Genetic engineering of meniscal allografts. Tissue Eng. 2002;8(1):107–17.
Mason JM, Breitbart AS, Barcia M, Porti D, Pergolizzi RG, Grande DA. Cartilage and bone regeneration using gene-enhanced tissue engineering. Clin Orthop Relat Res. 2000;379(Suppl):S171–8.
Matsumoto T, Cooper GM, Gharaibeh B, Meszaros LB, Li G, Usas A, et al. Cartilage repair in a rat model of osteoarthritis through intraarticular transplantation of muscle-derived stem cells expressing bone morphogenetic protein 4 and soluble Flt-1. Arthritis Rheum. 2009;60(5):1390–405.
Pelletier JP, Caron JP, Evans C, Robbins PD, Georgescu HI, Jovanovic D, et al. In vivo suppression of early experimental osteoarthritis by interleukin-1 receptor antagonist using gene therapy. Arthritis Rheum. 1997;40(6):1012–9.
Simonsen JL, Rosada C, Serakinci N, Justesen J, Stenderup K, Rattan SI, et al. Telomerase expression extends the proliferative life-span and maintains the osteogenic potential of human bone marrow stromal cells. Nat Biotechnol. 2002;20(6):592–6.
Tew SR, Li Y, Pothacharoen P, Tweats LM, Hawkins RE, Hardingham TE. Retroviral transduction with SOX9 enhances re-expression of the chondrocyte phenotype in passaged osteoarthritic human articular chondrocytes. Osteoarthr Cartil. 2005;13(1):80–9.
Zhang X, Mao Z, Yu C. Suppression of early experimental osteoarthritis by gene transfer of interleukin-1 receptor antagonist and interleukin-10. J Orthop Res. 2004;22(4):742–50.
Brunger JM, Huynh NP, Guenther CM, Perez-Pinera P, Moutos FT, Sanchez-Adams J, et al. Scaffold-mediated lentiviral transduction for functional tissue engineering of cartilage. Proc Natl Acad Sci U S A. 2014;111(9):E798–806. This study indicates the feasibility of combining cell engineering, gene engineering, and tissue engineering-based strategies (lentiviral-mediated transduction of TGF-b in bone marrow-derived mesenchymal stem cells seeded in PCL scaffolds) to promote chondrogenesis in vitro.
Chu X, You H, Yuan X, Zhao W, Li W, Guo X. Protective effect of lentivirus-mediated siRNA targeting ADAMTS-5 on cartilage degradation in a rat model of osteoarthritis. Int J Mol Med. 2013;31(5):1222–8.
Glass KA, Link JM, Brunger JM, Moutos FT, Gersbach CA, Guilak F. Tissue-engineered cartilage with inducible and tunable immunomodulatory properties. Biomaterials. 2014;35(22):5921–31. This study indicates the feasibility of combining cell engineering, gene engineering, and tissue engineering-based strategies (lentivirus-mediated transduction IL-1Ra of in bone marrow-derived mesenchymal stem cells seeded in PCL scaffolds) to reduce the inflammatory responses to IL-1 treatment in vitro.
Liu TM, Ng WM, Tan HS, Vinitha D, Yang Z, Fan JB, et al. Molecular basis of immortalization of human mesenchymal stem cells by combination of p53 knockdown and human telomerase reverse transcriptase overexpression. Stem Cells Dev. 2013;22(2):268–78.
Arai Y, Kubo T, Fushiki S, Mazda O, Nakai H, Iwaki Y, et al. Gene delivery to human chondrocytes by an adeno associated virus vector. J Rheumatol. 2000;27(4):979–82.
Cucchiarini M, Madry H, Ma C, Thurn T, Zurakowski D, Menger MD, et al. Improved tissue repair in articular cartilage defects in vivo by rAAV-mediated overexpression of human fibroblast growth factor 2. Mol Ther. 2005;12(2):229–38.
Cucchiarini M, Thurn T, Weimer A, Kohn D, Terwilliger EF, Madry H. Restoration of the extracellular matrix in human osteoarthritic articular cartilage by overexpression of the transcription factor SOX9. Arthritis Rheum. 2007;56(1):158–67.
Cucchiarini M, Schetting S, Terwilliger EF, Kohn D, Madry H. rAAV-mediated overexpression of FGF-2 promotes cell proliferation, survival, and alpha-SMA expression in human meniscal lesions. Gene Ther. 2009;16(11):1363–72.
Cucchiarini M, Terwilliger EF, Kohn D, Madry H. Remodelling of human osteoarthritic cartilage by FGF-2, alone or combined with Sox9 via rAAV gene transfer. J Cell Mol Med. 2009;13(8B):2476–88.
Cucchiarini M, Ekici M, Schetting S, Kohn D, Madry H. Metabolic activities and chondrogenic differentiation of human mesenchymal stem cells following recombinant adeno-associated virus-mediated gene transfer and overexpression of fibroblast growth factor 2. Tissue Eng Part A. 2011;17(15–16):1921–33.
Cucchiarini M, Orth P, Madry H. Direct rAAV SOX9 administration for durable articular cartilage repair with delayed terminal differentiation and hypertrophy in vivo. J Mol Med (Berl). 2013;91(5):625–36.
Dupont KM, Boerckel JD, Stevens HY, Diab T, Kolambkar YM, Takahata M, et al. Synthetic scaffold coating with adeno-associated virus encoding BMP2 to promote endogenous bone repair. Cell Tissue Res. 2012;347(3):575–88.
Goater J, Muller R, Kollias G, Firestein GS, Sanz I, O’Keefe RJ, et al. Empirical advantages of adeno associated viral vectors in vivo gene therapy for arthritis. J Rheumatol. 2000;27(4):983–9.
Goodrich LR, Phillips JN, McIlwraith CW, Foti SB, Grieger JC, Gray SJ, et al. Optimization of scAAVIL-1ra in vitro and in vivo to deliver high levels of therapeutic protein for treatment of osteoarthritis. Mol Ther Nucleic Acids. 2013;2:e70–9.
Goodrich LR, Choi VW, Carbone BA, McIlwraith CW, Samulski RJ. Ex vivo serotype-specific transduction of equine joint tissue by self-complementary adeno-associated viral vectors. Hum Gene Ther. 2009;20(12):1697–702.
Ito H, Goater JJ, Tiyapatanaputi P, Rubery PT, O’Keefe RJ, Schwarz EM. Light-activated gene transduction of recombinant adeno-associated virus in human mesenchymal stem cells. Gene Ther. 2004;11(1):34–41.
Kay JD, Gouze E, Oligino TJ, Gouze JN, Watson RS, Levings PP, et al. Intra-articular gene delivery and expression of interleukin-1Ra mediated by self-complementary adeno-associated virus. J Gene Med. 2009;11(7):605–14.
Klinger P, Surmann-Schmitt C, Brem M, Swoboda B, Distler JH, Carl HD, et al. Chondromodulin 1 stabilizes the chondrocyte phenotype and inhibits endochondral ossification of porcine cartilage repair tissue. Arthritis Rheum. 2011;63(9):2721–31.
Kyostio-Moore S, Bangari DS, Ewing P, Nambiar B, Berthelette P, Sookdeo C, et al. Local gene delivery of heme oxygenase-1 by adeno-associated virus into osteoarthritic mouse joints exhibiting synovial oxidative stress. Osteoarthr Cartil. 2013;21(2):358–67.
Madry H, Kohn D, Cucchiarini M. Direct FGF-2 gene transfer via recombinant adeno-associated virus vectors stimulates cell proliferation, collagen production, and the repair of experimental lesions in the human ACL. Am J Sports Med. 2013;41(1):194–202.
Madry H, Cucchiarini M, Terwilliger EF, Trippel SB. Recombinant adeno-associated virus vectors efficiently and persistently transduce chondrocytes in normal and osteoarthritic human articular cartilage. Hum Gene Ther. 2003;14(4):393–402.
Madry H, Cucchiarini M, Kaul G, Kohn D, Terwilliger EF, Trippel SB. Menisci are efficiently transduced by recombinant adeno-associated virus vectors in vitro and in vivo. Am J Sports Med. 2004;32(8):1860–5.
Mason JB, Vandenberghe LH, Xiao R, Wilson JM, Richardson DW. Influence of serotype, cell type, tissue composition, and time after inoculation on gene expression in recombinant adeno-associated viral vector-transduced equine joint tissues. Am J Vet Res. 2012;73(8):1178–85.
Mason JB, Gurda BL, Engiles JB, Hankenson KD, Wilson JM, Richardson DW. Multiple recombinant adeno-associated viral vector serotypes display persistent in vivo gene expression in vector-transduced rat stifle joints. Hum Gene Ther Methods. 2013;24(3):185–94.
Mease PJ, Wei N, Fudman EJ, Kivitz AJ, Schechtman J, Trapp RG, et al. Safety, tolerability, and clinical outcomes after intraarticular injection of a recombinant adeno-associated vector containing a tumor necrosis factor antagonist gene: results of a phase 1/2 study. J Rheumatol. 2010;37(4):692–703.
Pagnotto MR, Wang Z, Karpie JC, Ferretti M, Xiao X, Chu CR. Adeno-associated viral gene transfer of transforming growth factor-beta1 to human mesenchymal stem cells improves cartilage repair. Gene Ther. 2007;14(10):804–13.
Santangelo KS, Baker SA, Nuovo G, Dyce J, Bartlett JS, Bertone AL. Detectable reporter gene expression following transduction of adenovirus and adeno-associated virus serotype 2 vectors within full-thickness osteoarthritic and unaffected canine cartilage in vitro and unaffected guinea pig cartilage in vivo. J Orthop Res. 2010;28(2):149–55.
Santangelo KS, Nuovo GJ, Bertone AL. In vivo reduction or blockade of interleukin-1beta in primary osteoarthritis influences expression of mediators implicated in pathogenesis. Osteoarthr Cartil. 2012;20(12):1610–8.
Stender S, Murphy M, O’Brien T, Stengaard C, Ulrich-Vinther M, Soballe K, et al. Adeno-associated viral vector transduction of human mesenchymal stem cells. Eur Cell Mater. 2007;13:93–9.
Ulrich-Vinther M, Duch MR, Soballe K, O’Keefe RJ, Schwarz EM, Pedersen FS. In vivo gene delivery to articular chondrocytes mediated by an adeno-associated virus vector. J Orthop Res. 2004;22(4):726–34.
Ulrich-Vinther M, Stengaard C, Schwarz EM, Goldring MB, Soballe K. Adeno-associated vector mediated gene transfer of transforming growth factor-beta1 to normal and osteoarthritic human chondrocytes stimulates cartilage anabolism. Eur Cell Mater. 2005;10:40–59.
Venkatesan N, Barre L, Benani A, Netter P, Magdalou J, Fournel-Gigleux S, et al. Stimulation of proteoglycan synthesis by glucuronosyltransferase-I gene delivery: a strategy to promote cartilage repair. Proc Natl Acad Sci U S A. 2004;101(52):18087–92.
Venkatesan JK, Ekici M, Madry H, Schmitt G, Kohn D, Cucchiarini M. SOX9 gene transfer via safe, stable, replication-defective recombinant adeno-associated virus vectors as a novel, powerful tool to enhance the chondrogenic potential of human mesenchymal stem cells. Stem Cell Res Ther. 2012;3(3):22–36.
Watson RS, Broome TA, Levings PP, Rice BL, Kay JD, Smith AD, et al. scAAV-mediated gene transfer of interleukin-1-receptor antagonist to synovium and articular cartilage in large mammalian joints. Gene Ther. 2013;20(6):670–7.
Weimer A, Madry H, Venkatesan JK, Schmitt G, Frisch J, Wezel A, et al. Benefits of rAAV-mediated IGF-I overexpression for the long-term reconstruction of human osteoarthritic cartilage by modulation of the IGF-I axis. Mol Med. 2012;18:346–58.
McCarty DM, Monahan PE, Samulski RJ. Self-complementary recombinant adeno-associated virus (scAAV) vectors promote efficient transduction independently of DNA synthesis. Gene Ther. 2001;8(16):1248–54.
Centeno CJ, Busse D, Kisiday J, Keohan C, Freeman M, Karli D. Increased knee cartilage volume in degenerative joint disease using percutaneously implanted, autologous mesenchymal stem cells. Pain Phys. 2008;11(3):343–53.
Wakitani S, Imoto K, Yamamoto T, Saito M, Murata N, Yoneda M. Human autologous culture expanded bone marrow mesenchymal cell transplantation for repair of cartilage defects in osteoarthritic knees. Osteoarthr Cartil. 2002;10(3):199–206.
Pak J. Regeneration of human bones in hip osteonecrosis and human cartilage in knee osteoarthritis with autologous adipose-tissue-derived stem cells: a case series. J Med Case Rep. 2011;5:296–303.
Venkatesan JK, Rey-Rico A, Schmitt G, Wezel A, Madry H, Cucchiarini M. rAAV-mediated overexpression of TGF-beta stably restructures human osteoarthritic articular cartilage in situ. J Transl Med. 2013;11:211–24.
Jones SW, Watkins G, Le Good N, Roberts S, Murphy CL, Brockbank SM, et al. The identification of differentially expressed microRNA in osteoarthritic tissue that modulate the production of TNF-alpha and MMP13. Osteoarthr Cartil. 2009;17(4):464–72.
Tardif G, Hum D, Pelletier JP, Duval N, Martel-Pelletier J. Regulation of the IGFBP-5 and MMP-13 genes by the microRNAs miR-140 and miR-27a in human osteoarthritic chondrocytes. BMC Musculoskelet Disord. 2009;10:148–58.
Dudek KA, Lafont JE, Martinez-Sanchez A, Murphy CL. Type II collagen expression is regulated by tissue-specific miR-675 in human articular chondrocytes. J Biol Chem. 2010;285(32):24381–7.
Dvir-Ginzberg M, Gagarina V, Lee EJ, Hall DJ. Regulation of cartilage-specific gene expression in human chondrocytes by SirT1 and nicotinamide phosphoribosyltransferase. J Biol Chem. 2008;283(52):36300–10.
Matsushita T, Sasaki H, Takayama K, Ishida K, Matsumoto T, Kubo S, et al. The overexpression of SIRT1 inhibited osteoarthritic gene expression changes induced by interleukin-1beta in human chondrocytes. J Orthop Res. 2013;31(4):531–7.
Zhang F, Yao Y, Su K, Fang Y, Citra F, Wang DA. Co-transduction of lentiviral and adenoviral vectors for co-delivery of growth factor and shRNA genes in mesenchymal stem cells-based chondrogenic system. J Tissue Eng Regen Med. 2012. doi:10.1002/term.1656.
Gelse K, von der Mark K, Aigner T, Park J, Schneider H. Articular cartilage repair by gene therapy using growth factor-producing mesenchymal cells. Arthritis Rheum. 2003;48(2):430–41.
Gelse K, Muhle C, Franke O, Park J, Jehle M, Durst K, et al. Cell-based resurfacing of large cartilage defects: long-term evaluation of grafts from autologous transgene-activated periosteal cells in a porcine model of osteoarthritis. Arthritis Rheum. 2008;58(2):475–88.
Mason JM, Grande DA, Barcia M, Grant R, Pergolizzi RG, Breitbart AS. Expression of human bone morphogenic protein 7 in primary rabbit periosteal cells: potential utility in gene therapy for osteochondral repair. Gene Ther. 1998;5(8):1098–104.
Ueblacker P, Wagner B, Vogt S, Salzmann G, Wexel G, Kruger A, et al. In vivo analysis of retroviral gene transfer to chondrocytes within collagen scaffolds for the treatment of osteochondral defects. Biomaterials. 2007;28(30):4480–7.
Vogt S, Wexel G, Tischer T, Schillinger U, Ueblacker P, Wagner B, et al. The influence of the stable expression of BMP2 in fibrin clots on the remodelling and repair of osteochondral defects. Biomaterials. 2009;30(12):2385–92.
Blaney Davidson EN, Vitters EL, van den Berg WB, van der Kraan PM. TGF beta-induced cartilage repair is maintained but fibrosis is blocked in the presence of Smad7. Arthritis Res Ther. 2006;8(3):R65–72.
Bandara G, Mueller GM, Galea-Lauri J, Tindal MH, Georgescu HI, Suchanek MK, et al. Intraarticular expression of biologically active interleukin 1-receptor-antagonist protein by ex vivo gene transfer. Proc Natl Acad Sci U S A. 1993;90(22):10764–8.
Ha CW, Noh MJ, Choi KB, Lee KH. Initial phase I safety of retrovirally transduced human chondrocytes expressing transforming growth factor-beta-1 in degenerative arthritis patients. Cytotherapy. 2012;14(2):247–56.
Evans CH, Ghivizzani SC, Robbins PD. Arthritis gene therapy and its tortuous path into the clinic. Transl Res. 2013;161(4):205–16.
Compliance with Ethics Guidelines
ᅟ
Conflict of Interest
Magali Cucchiarini and Henning Madry declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Osteoarthritis
Rights and permissions
About this article
Cite this article
Cucchiarini, M., Madry, H. Use of Tissue Engineering Strategies to Repair Joint Tissues in Osteoarthritis: Viral Gene Transfer Approaches. Curr Rheumatol Rep 16, 449 (2014). https://doi.org/10.1007/s11926-014-0449-0
Published:
DOI: https://doi.org/10.1007/s11926-014-0449-0