Abstract
Purpose of Review
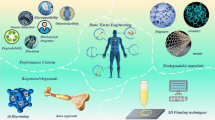
The purpose of this review is to illustrate the current state of 3D printing (3DP) technology used in biomedical industry towards bone regeneration. We have focused our efforts towards correlating materials and structural design aspects of 3DP with biological response from host tissue upon implantation. The primary question that we have tried to address is—can 3DP be a viable technology platform for bone regeneration devices?
Recent Findings
Recent findings show that 3DP is a versatile technology platform for numerous materials for mass customizable bone regeneration devices that are also getting approval from different regulatory bodies worldwide.
Summary
After a brief introduction of different 3DP technologies, this review elaborates 3DP of different materials and devices for bone regeneration. From cell-based bioprinting to acellular patient-matched metallic or ceramic devices, 3DP has tremendous potential to improve the quality of human life through bone regeneration among patients of all ages.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Three-dimensional printing (3DP) or additive manufacturing (AM) has transformed the manufacturing world in the past three decades—from product design/concept models to rapid prototyping and functional part manufacturing. 3DP is a layer-by-layer process that allows us to manufacture complex structures without any part-specific tooling. The first commercial 3DP technology, called “stereolithography,” was introduced by Charles Hull in 1988. Since then, different 3DP processes have been introduced commercially for a variety of materials and applications [1, 2••]. The American Society for Testing and Materials (ASTM) has classified 3DP into seven broad categories based on part manufacturing approaches, summarized in Table 1. The following section briefly describes some of the 3DP processes that are relevant for treatment options for bone disorders.
Vat Photopolymerization
This is the first commercial process, also known as “stereolithography (SLA).” In SLA, a photopolymer resin is cured on a build plate using an ultraviolet (UV) light. The UV beam moves based on the part design, one layer at a time. Later, this process was modified for area curing for each layer, called digital light processing (DLP) or continuous DLP (cDLP) which is faster than standard SLA. Since the printed part is immersed in a monomer liquid, the surface finish of the printed part is better than other polymer 3DP techniques. Vat photopolymerization can be used to print ceramic parts by forming a uniform suspension of ceramic powder in the photopolymer resin, which acts as a binder, followed by binder removal and sintering process. However, sedimentation of ceramics in the suspension can be a major issue, which can cause nonuniform density in the final part [1, 2••, 3].
Materials Extrusion
Materials extrusion or “fused deposition modeling (FDM)” is one of the most popular AM techniques because of its simplicity and ease of use. In most systems, a thermoplastic filament is fed into a heated nozzle, softened, and extruded out, while the printhead is moving in the x-y plane. Other systems may utilize pellets and an auger extrusion concept. Extruded material is then deposited on a build plate that can move along the z direction. Apart from the polymers, metals and ceramic parts can also be printed using FDM. In those cases, metal or ceramic powders are premixed with polymers and extruded in feedstock filament form for 3DP. FDM-processed metal or ceramic parts require binder/polymer removal at high temperature followed by sintering. Relative to other techniques, the resolution offered by an FDM machine is low (layer thickness ~ 50–250 μm), however it is easy to use, maintain, and customize, with machine and filament material at low cost [1, 2••, 4].
Binder Jetting
Binder jetting is a technique developed by researchers at the Massachusetts Institute of Technology in 1993. In this technique, a roller rolls a metal or a ceramic, or a polymeric powder from a powder bed onto a build plate forming a uniform thin layer of powder, followed by liquid binder deposition from an inkjet head based on the CAD file. The binder acts as a glue and provides temporary strength to the printed part. Further heating of the powder bed is carried out at the curing temperature of the binder to obtain substantial green strength, thus allowing powder removal without damaging the part, followed by binder removal and sintering in case of metallic and ceramic parts. Binder jetting offers tight tolerances and is the most appropriate technique to print complex geometries, especially for ceramics. Sintering step can cause cracking due to nonuniform shrinkage. Optimization of binder droplet size and binder composition are the most important factors to ensure good part quality. Binder jetting is not suitable for large part size [1, 2••, 5].
Powder Bed Fusion
Powder bed fusion was invented at the University of Texas at Austin based on the similar principle of binder jetting where the inkjet head is replaced by a focused laser beam or an electron beam (e-beam) to sinter (selective laser sintering, SLS) or melt (selective laser melting or SLM; or electron beam melting) the powder. While SLS is primarily used for polymers, SLM or e-beam processes are used for metallic parts. Powder bed fusion can be used to print complex designs where unused powders act as a support material, or support structures designed to support thermal strain caused during the high-temperature process. Factors such as laser power, scan speed, and layer thickness need to be optimized to acquire the required physical and mechanical properties in a printed part. Printing demands an enclosed environment to minimize oxidation of liquid metals (vacuum for e-beam, argon or nitrogen for SLM) primarily when using reactive metals such as titanium or aluminum [1, 2••, 6]. E-beam (in vacuum) is popular in the titanium medical implant industry owing to lower oxygen pickup in the final printed part relative to an environmentally controlled SLM process, resulting in better mechanical properties.
Directed Energy Deposition
Directed energy deposition (DED) uses a focused high-energy laser beam to melt or sinter metal or ceramic powders as soon as they are deposited from coaxial nozzles focused towards the build plate. Since no powder bed is used, multi-material structures can be easily printed along with compositional gradient using DED, to tailor the properties of components along multiple directions. As in the case of powder bed fusion, the laser power, scan speed, and powder flow rate are some parameters that need to be optimized for various materials depending on their laser absorptivity and thermal conductivity. DED offers poor part resolution and tolerances (layer thicknesses ~ 250–500 μm). DED is widely used for surface modification on existing components, structures with varying compositions, and repair of high value parts. Figure 1 summarizes the schematic of all of these five 3DP processes [1, 2••, 7].
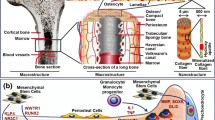
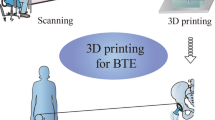
The application of 3DP in biomaterials is increasing rapidly. Apart from a large number of metallic implant manufacturing or producing resorbable polymer or ceramic scaffolds, 3DP is also being used for printing materials with live cells, or bioprinting. Moreover, not only 3DP can use a variety of materials, it can also create innovative structures with interconnected porosity suitable for tissue integration in vivo. Finally, using 3DP, patient-matched devices can be created based on the computed tomography (CT) or magnetic resonance imaging (MRI) of an anatomical defect. This approach is also becoming popular for defect-specific surgical models to aid physicians for complex surgeries. Both bioresorbable and non-resorbable materials have been processed using 3DP particularly for bone defects based on the location of the injury. For low load-bearing applications such as craniomaxillofacial areas, polymers, ceramics, or ceramic-polymer composites have been used via 3DP. However, in load-bearing applications such as hip or knee or spinal defects, 3D-printed metallic implants are common today that have received clearance from a variety of regulatory bodies worldwide including the U.S. Food and Drug Administration (FDA) [8].
Bioprinting
Bioprinting is essentially 3DP of structures using acellular materials in combination with living cells to replace tissues to restore their lost function. Bioprinting uses similar principle as any other 3DP operation by layerwise deposition of bioink, i.e., cell/tissue laden biopolymeric material, to develop 3-dimensional anatomical structures from a 3D digital model [9, 10]. Bioprinting requires extensive optimization of the process in addition to maintaining a sterile environment to ensure cellular viability while taking care of adequate printing resolution. During bioprinting, function-specific bioink preparation through a combination of cells and a suitable scaffolding medium such as collagen, gelatin, and nanocellulose are needed to provide nutrition to the cells to grow and multiply. Curing the polymeric material using UV light helps crosslink the scaffolding medium and entrapping the cells to make the 3D structure. Several thermoresponsive polymers such as poly(N-isopropylacrylamide) (PNIPAm), pluronics, elastin polypeptides, and polycaprolactone (PCL) have found their applications in printing cell sheets for bioprinting operations. Several studies have been conducted over the years towards feasibility of thermoresponsive polymers for bioprinting operations and have found that PNIPAm is probably the most extensively used polymer. PNIPAm biomedical grafts are most typically prepared by electron beam irradiation and have been already commercialized as a tool for cell sheet engineering [11]. The application of materials such as nanocellulose can be twofold: (1) it can serve as bioink where the nanocellulose is used as a scaffolding nutrient medium for living cells to be incorporated prior to printing, and also, (2) growth factors and other acellular biologics can be incorporated into the nanocellulose matrix followed by subsequent cell seeding [12]. Figure 2 shows inspired bioprinted cartilage constructs fabricated using stem cells in alginate bioink and PCL crosslink exhibiting protein adhesion on the surface of the constructs.
3D bioprinting of stem cells-alginate-PCL structures for cartilage bioprints and biological assessment of protein adhesion on the material [13••]. a 1, CAD image outline of the vertebral structure; 2, PCL deposition to form a crosslinked network; 3, bioink deposition; and 4, composite printing. b μCT image of the composite PCL/alginate/MSC laden vertebrae structure. c Live/dead cell imaging of MSC laden PCL network. Used with permission from John Wiley and Sons
3DP of Bioceramics
3D-printed porous ceramics have introduced several benefits towards development of lightweight multifunctional materials that are tailored to the patient’s needs. 3D-printed porous ceramic scaffolds show superior performance than traditionally manufactured structures [14]. Ceramics used for 3DP operations are either biodegradable ceramics such as calcium phosphates (CaPs) and calcium silicates or nonbiodegradable ceramics such as alumina and zirconia. Based on the application site, these ceramics are typically functionalized by drugs, dopants, and growth factors or structurally modified to perform a specific function. CaPs are the most common ceramics used in bone regeneration. Typically fabricated using powder bed 3DP techniques such as binder jetting, CaPs can achieve very high structural resolution. 3D-printed CaP scaffolds for biomedical applications can be broadly classified into two major categories based on processing parameters: (1) high-temperature 3D-printed CaP scaffolds for bone regeneration and (2) low-temperature 3D-printed scaffolds for drug and growth factor delivery. The former involves either powder bed fusion or thermal material extrusion techniques followed by high-temperature post-processing such as sintering. These scaffolds have good mechanical strength but are incapable of drugs or biologics incorporation during fabrication. The only way these scaffolds can be characterized for biocompatibility is external in vitro cell seeding on the surface and in vivo osseointegration studies. Extensive research has been performed with a variety of cells to assess biocompatibility of these scaffolds [15,16,17,18,19]. Additionally, a number of studies have evaluated the printability and biocompatibility of these CaP scaffolds with different dopant systems [20, 21, 22••] at low temperatures using binder jetting. Low-temperature processes render the possibility of in situ printing of CaP parts together with growth factors, drugs, and dopants.
Biological performance of 3D-printed CaP scaffolds incorporated with dopant systems such as strontium (Sr), magnesium (Mg), iron (Fe), and silicon (Si) showed enhanced osteogenic ability of these materials as a combined function of the chemistry of the dopants as well as structural design through 3DP [21, 22••] (Fig. 3). In vivo results observed over periods of 4, 8, and 12 weeks on rat distal femur models showed accelerated bone ingrowth through interconnected open porous channels in the scaffolds, which promote cellular migration and thereafter osseous tissue integration. Dopants such as Fe and Si are found naturally in human physiological systems and hence deemed to be nontoxic. This elemental incorporation into ceramic scaffolds increases the chances of osteogenesis and eventually leads to complete bone regeneration, while simultaneously the scaffolding materials biodegrade in vivo. The combined osteogenic effect of CaP and Fe/Si/Sr/Mg suggests that such combinations are not only feasible for fabrication but also can be effective towards being a comprehensive bone regenerative scaffolding device.
a, b Schematic of 3D printing of ceramics using inkjet printing technique and images of fabricated parts, c 3D-printed porous ceramic scaffold structure, d in vitro cell-material interaction, e, f histological micrograph for in vivo bone formation on Sr, Mg-doped CaP scaffolds and subsequent histomorphometric quantification, and g, h in vivo bone section images from decalcified bone/scaffold system with Fe and Si dopants. Used with permission from Springer [21] and Elsevier [22••]
Alumina and zirconia are used in dental and musculoskeletal bone regeneration due to their toughness and high mechanical strength [23,24,25,26]. Alumina parts fabricated using stereolithography with added infiltration of liquid phase zirconium by in situ precipitation have been studied [27]. The enhanced strength was observed compared with parts without liquid infiltration. However, these structures exhibited lower fracture toughness. Dehurtevent et al. [28] studied the effect of particle size on flexural strength and shrinkage of printed alumina dental crown to prove that flexural strength does not depend on particle size. Additionally, research has shown bimodally distributed particle size (micro and nano) can contribute towards higher part density compared with uniform single-sized alumina particles [29]. However direct ceramic stereolithography can be expensive, and only a limited number of materials are available so far for this technique [30].
3DP of Ceramic-Polymer Composites
The ability to 3D print polymeric composites has been explored extensively in medical field especially for non-load-bearing applications such as craniomaxillofacial and dental. Several bone mimetic models and soft tissue mimetic models have been developed using polymer-ceramic composite 3DP [31]. PCL finds an extensive application in such fields due to its lower degradation rate in physiological environment as well as higher mechanical strength compared with other polymers such as polylactic acid (PLA) or polylactide glycolic acid (PLGA). Very high bone regenerative response has been observed for such 3D-printed scaffolds in non-load-bearing application [32]. Porous structures with very high-resolution and patient-matched designs can be fabricated using FDM which leads to the onset of effective bone regeneration and ingrowth. These scaffolds are eventually degraded in the physiological environment. Bone mimetic scaffolds have been independently fabricated with a combination of decellularized extracellular matrix (ECM) and PCL [33, 34].
More recently, starch-based structures have been 3D-printed as bone regenerative scaffolds with added advantage of drug elution from pores. Koski et al. have utilized solid freeform fabrication to fabricate bone scaffolds from calcium phosphate and starch-based composites. The integration of calcium phosphate, PCL, and starch improved the mechanical properties as well as resulted in better biological performance. These scaffolds were later studied as drug-eluting vehicles for chemopreventive measures [35] (Fig. 4). While polymers have been shown to effectively enhance mechanical properties of ceramic scaffolds, they are also extensively used as coatings on drug delivery ceramic systems. Polymeric coatings (PCL, PLGA) can regulate the rate of drug release from scaffolds based on the pH of the environment and hence effectively sustain the therapeutic efficacy of the drug. Several studies have been performed with polymer coatings on CaP scaffolds which are targeted towards sustained delivery natural medicinal compounds [36].
Ceramic scaffolds structures with polymer coatings aiding in sustained direct drug delivery as well as from liposomal encapsulation [37••]. a Turmeric rhizomes, source of curcumin. b SEM morphology of 3DP ceramic scaffold. c SEM micrograph HA structure with and without curcumin encapsulation. d In vitro cell osteoblast morphology on porous 3DP TCP scaffold with and without curcumin encapsulated liposome. e Osteoblast proliferation on curcumin loaded HA-coated Ti implants. f In vivo histology staining for tissue-material interaction through collagen, blood vessel formation, and new bone growth into porous implants. Used with permission from Elsevier
3DP of Metals and Alloys
Numerous common orthopedic diseases in load-bearing anatomical sites need metal implants to restore function of that part. There are two major factors that determine the suitability of a load-bearing metallic implant: (1) mechanical stability which can be better achieved through 3DP of customized part based on the CT scan or MRI of the patient’s defect site and (2) biological response towards host bone which is often achieved by bulk or surface modification of such implants. 3DP of metals primarily comprised of melting of metal powder feedstock using either a laser source or electron beam and follows similar principle as any other 3DP operation. The most common techniques are powder bed fusion (SLM), directed energy deposition (laser or electron beam), and fairly newly binder jetting.
3D-printed titanium (Ti) alloys have been extensively used in biomedical devices for total knee arthroplasty (TKA) and total hip arthroplasty (THA) due to their excellent biocompatibility, initial stability due to lower modulus, and low cost of production. Dumas et al. fabricated a novel porosity-graded diamond-type lattice structures via powder bed fusion 3DP technology and evaluated the stiffness and yield strength of the Ti64 structures with varying porosities (80, 58, and 40%) towards mechanical stability at the implantation site [38]. The porous structures were shown to have modulus ranging from 1.6 to 20.3 GPa which were comparable with that of trabecular and cortical bone. On the other hand, Sheydaeian et al. used binder jet multi-scale 3DP to analyze porosity deviation in functionally graded commercially pure Ti (CpTi) cellular structures using different layer thicknesses [39]. Apart from a 5% variation in porosity of the fabricated parts, no significant variation in Young’s modulus (2.9 ± 0.5–3.5 ± 0.4) GPa as well as yield stress (158 ± 10–175 ± 27) MPa was observed. Other Ti alloys have been studied for structural dependence of mechanical properties based on 3DP fabrication, for example, solid and porous lattice structures of Ti-25Ta alloys have been fabricated by Soro et al. using selective laser melting (SLM) and have been shown to exhibit identical mechanical compatibility as Ti64 but with a lower elastic modulus and higher strength [41]. This is particularly useful in a bone repair application since a lower elastic modulus of the material or design suggests a reduction in the probability of stress shielding due to mismatch in modulus. However, when it comes to the biological compatibility of Ti alloys in physiological implantation, poor bonding on the surface of these bioinert implants is their primary disadvantage. Several coating techniques such as ceramics on Ti, tantalum (Ta) on Ti, and titania nanotubes have been implemented to overcome the drawback [40,41,42].
Tantalum (Ta) is a newly implemented metallic biomaterial that has seen popularity over the last decade. It has attracted the attention of the biomedical industry due to its excellent corrosion resistance and biocompatibility. However, high density and melting temperature of Ta make it difficult to process using conventional techniques in addition to its high inventory cost. 3DP techniques such as directed energy deposition make it feasible to process Ta [43]. Recently, Bandyopadhyay et al. showed the processing feasibility of porous Ta structures using laser engineered net shaping (LENS™) keeping processing parameters close to that of Ti64. The 30% porous Ta structures showed similar in vivo biological performance as 30% porous Ti64 with nanotube surface modifications [44]. In vivo studies carried out over periods of 5 and 12 weeks in rat distal femur model suggested 3D-designed volume fraction porosity to play a key role in early-stage osseointegration ability of these implants. This was achieved through enhanced bone ingrowth through bulk porosity. In addition, higher and continued osteoid or new bone formation at the interface of these implants and host bone was observed for extended time periods as a function of surface chemistry (titania nanotubes) (Fig. 5). Bone regenerative capability of these 3D-printed implants suggests their candidacy as effective bone replacement biomedical devices.
a, b In vivo biological response from tantalum parts fabricated using direct energy deposition (DED) showing early-stage osseointegration as a function of designed porosities and extended new bone formation at 5- and 12-weeks post-implantation, respectively. c, d Histomorphometric quantification of new bone formation at the implant-bone interface at 5 and 12 weeks, respectively. e In vitro cellular response of 3D-printed Ta coatings evaluated through confocal microscopy (image courtesy: Bandyopadhyay et al. [44, 45]). Used with permission from Elsevier
Recently, among metallic orthopedic implants, biodegradation profile has been of emerging importance. Biodegradable metallic bone implants are therefore fabricated from either soft metal such as magnesium or iron which is found naturally in physiological system. Magnesium implants have mechanical properties close to that of bone, and magnesium has been reported to stimulate new bone formation [46] because it is an essential mineral in nutrition intake. However, magnesium has a fast degradation rate because it is a soft metal and corrodes faster than other inert metals such as Ti or cobalt-chrome alloys. Iron, on the other hand, has a slower degradation rate which can be disadvantageous for its use in orthopedic applications. 3DP techniques provide solutions to overcome both these drawbacks and successfully fabricate implantable parts with moderate degradation rates and comparable mechanical properties to that of human bone. Li et al. have extensively studied the contribution of additively manufactured magnesium and iron implant structures towards optimized effective performance [47]. The magnesium scaffolds were fabricated using SLM, while the iron porous lattice structures were fabricated using direct metal printing (DMP). Both the implants showed a structural or design dependence on mechanical properties as well as biological activity. Magnesium scaffolds showed continued mechanical stability as trabecular bone even after 4 weeks of biodegradation and revealed less than 25% cytotoxicity in vitro. On the other hand, porous iron structures also revealed mechanical stability even after 28 days of biodegradation. The biodegradation behavior of iron scaffolds was found to be faster on the periphery compared with the center which suggests an important role of topology or design on the additively manufactured porous iron.
Nickel-titanium alloys also known as Nitinol (NiTi) have been of importance in biomedical applications such as vascular stents, orthodontic wires, and bone implants due to their shape-memory properties, super elasticity, and corrosion resistance by spontaneous formation of titanium oxide layer on the surface. However, conventional manufacturing of NiTi is difficult mainly because of machining issues, hardening characteristic, and martensitic transformation due to stress. 3DP techniques for fabrication of NiTi structures have been developed to circumvent the difficulties of conventional manufacturing while providing ease of fabricating complex geometries and porous structures. Although 3DP has provided a way to successfully fabricate these structures, porosity led to higher surface area which in turn resulted in higher rate of corrosion and Ni ion release [48]. Therefore, coating techniques in 3DP are suggested for effective implementation of NiTi in biomedical applications. Similarly, other studies suggest biofunctionalization of NiTi surfaces using biologics to reduce Ni ion release and enhance cell-material interactions [49].
3DP of metals makes it easier for part fabrication with complex geometries for expensive materials or materials that are difficult to work with. This field for metals is rapidly growing with numerous advances in newer methods, alloys, and part improvement. Metal 3DP provides us the advantages of reduced cost of tooling, design versatility, and complex geometry fabrication in addition to one-step part consolidation.
Summary and Future Direction
3D printing provides the end user with design freedom, part customization, and the ability to print complex parts on demand. A review on the main techniques of 3D printing in bone regeneration, methods, and materials is presented here. Some of the challenges related to specific 3D printing operations are also discussed. 3D printing has contributed to ongoing research and advancement of biomedical materials with customized structures and patient specificity. However, challenges such as regulatory issues pose concerns with the use of 3D printing. Although 3D printing of metallic materials for implants is becoming common, over 100,000 implants have been printed in 2019 for human use and it is still not common for ceramics in clinical applications due to challenges in process optimization and quality control. Void formation between layers during printing operations is one of the major concerns that can compromise mechanical properties of the printed parts. Additionally, anisotropic properties in 3D-printed parts are also difficult to avoid. Current research on the development of materials and methods has helped overcome some of these challenges. 3D printing is expected to be a part of mainstream medicine, not just in orthopedics but also in other areas of health care. 3D printing will serve as a great tool for surgical training to young physicians for better visualization of different anatomical structures. It is also becoming common for physicians to use surgical models for pre-surgical planning. The innovation of next generation of biomaterials to treat various diseases and large-scale on-demand manufacturing of implants will be possible in the coming days with the help of 3D printing. Overall, the evolution of 3D printing over the past decades has been phenomenal, and this trend is expected to continue in the next decade.
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
Bandyopadhyay A, Bose S. Additive Manufacturing, Second Edition [Internet]. 2nd ed. CRC Press; 2019 [cited 2020 Jan 14]. Available from: https://www.crcpress.com/Additive-Manufacturing-Second-Edition/Bandyopadhyay-Bose/p/book/9781138609259
•• Bose S, Ke D, Sahasrabudhe H, Bandyopadhyay A. Additive manufacturing of biomaterials. Progress in Materials Science. 2018;93:45–111. This recent review provides a thorough understanding of different AM technologies, their compatibility with manufacturing biomaterials for clinical applications, and subsequent challenges that need to be addressed in the coming days. It covers a broad area of biomedical industry concerned with 3DP of biomedical electronic devices to pharmaceutical drug delivery vehicles to bone regenerative implants.
Billiet T, Vandenhaute M, Schelfhout J, Van Vlierberghe S, Dubruel P. A review of trends and limitations in hydrogel-rapid prototyping for tissue engineering. Biomaterials. 2012;33:6020–41.
Peng F, Vogt BD, Cakmak M. Complex flow and temperature history during melt extrusion in material extrusion additive manufacturing. Addit Manuf. 2018;22:197–206.
Gonzalez JA, Mireles J, Lin Y, Wicker RB. Characterization of ceramic components fabricated using binder jetting additive manufacturing technology. Ceram Int. 2016;42:10559–64.
Hossain MS, Gonzalez JA, Hernandez RM, Shuvo MAI, Mireles J, Choudhuri A, et al. Fabrication of smart parts using powder bed fusion additive manufacturing technology. Addit Manuf. 2016;10:58–66.
Bandyopadhyay A, Traxel KD. Invited review article: metal-additive manufacturing—modeling strategies for application-optimized designs. Addit Manuf. 2018;22:758–74.
Bose S, Traxel KD, Vu AA, Bandyopadhyay A. Clinical significance of three-dimensional printed biomaterials and biomedical devices. MRS Bull. 2019;44:494–504.
Kolesky DB, Truby RL, Gladman AS, Busbee TA, Homan KA, Lewis JA. 3D bioprinting of vascularized, Heterogeneous Cell-Laden Tissue Constructs. Adv Mater. 2014;26:3124–30.
Murphy SV, Atala A. 3D bioprinting of tissues and organs. Nat Biotechnol. 2014;32:773–85.
Doberenz F, Zeng K, Willems C, Zhang K, Groth T. Thermoresponsive polymers and their biomedical application in tissue engineering. J Mater Chemist B [Internet]. 2020 [cited 2020 Jan 11]; Available from: https://pubs.rsc.org/en/content/articlelanding/2020/tb/c9tb02052g
Sultan S, Siqueira G, Zimmermann T, Mathew AP. 3D printing of nano-cellulosic biomaterials for medical applications. Curr Opin Biomed Eng. 2017;2:29–34.
•• Daly AC, Cunniffe GM, Sathy BN, Jeon O, Alsberg E, Kelly DJ. 3D Bioprinting of Developmentally Inspired Templates for Whole Bone Organ Engineering. Advanced Healthcare Materials. 2016;5:2353–62. Bioprinting is still in its infancy but recent developments have been made to successfully implement this technology in bone regeneration. This article illustrates inspired cartilage printing using alternative novel system comprised of stem cells-alginate bioink and PCL crosslinking towards enhanced protein adhesion.
Wen Y, Xun S, Haoye M, Baichuan S, Peng C, Xuejian L, et al. 3D printed porous ceramic scaffolds for bone tissue engineering: a review. Biomater Sci. 2017;5:1690–8.
Trombetta R, Inzana JA, Schwarz EM, Kates SL, Awad HA. 3D printing of calcium phosphate ceramics for bone tissue engineering and drug delivery. Ann Biomed Eng. 2017;45:23–44.
Comesaña R, Lusquiños F, Del Val J, Quintero F, Riveiro A, Boutinguiza M, et al. Toward smart implant synthesis: bonding bioceramics of different resorbability to match bone growth rates.
Bergemann C, Cornelsen M, Quade A, Laube T, Schnabelrauch M, Rebl H, et al. Continuous cellularization of calcium phosphate hybrid scaffolds induced by plasma polymer activation. Mater Sci Eng C Biomimet Mater Sens Syst. 2016;59:514–23.
Zhang Y, Xia L, Zhai D, Shi M, Luo Y, Feng C, et al. Mesoporous bioactive glass nanolayer-functionalized 3D-printed scaffolds for accelerating osteogenesis and angiogenesis. Nanoscale. 2015;7:19207–21.
Sweet L, Kang Y, Czisch C, Witek L, Shi Y, Smay J, et al. Geometrical versus random beta-TCP scaffolds: exploring the effects on Schwann cell growth and behavior. PLoS One. 2015;10:e0139820.
Bose S, Tarafder S, Bandyopadhyay A. Effect of chemistry on Osteogenesis and angiogenesis towards bone tissue engineering using 3D printed scaffolds. Ann Biomed Eng. 2017;45:261–72.
Bose S, Banerjee D, Robertson S, Vahabzadeh S. Enhanced in vivo bone and blood vessel formation by Iron oxide and silica doped 3D printed tricalcium phosphate scaffolds. Ann Biomed Eng. 2018;46:1241–53.
•• Bose S, Vahabzadeh S, Bandyopadhyay A. Bone tissue engineering using 3D printing. Materials today. 2013;16:496–504. This review brings 3D printed ceramic scaffolds to the forefront of bone tissue engineering devices. It illustrates how porous ceramic structures can be designed using 3DP technology and hence can be beneficial in securing successful tissue ingrowth and subsequent bone regeneration.
Baino F, Minguella-Canela J, Korkusuz F, Korkusuz P, Kankılıç B, Montealegre MÁ, et al. In vitro assessment of bioactive glass coatings on alumina/zirconia composite implants for potential use in prosthetic applications. Int J Mol Sci. 2019;20:722.
Baino F, Montealegre MA, Minguella-Canela J, Vitale-Brovarone C. Laser surface texturing of alumina/zirconia composite ceramics for potential use in hip joint prosthesis. Coatings. 2019;9:369.
Rodriguez CA, Lara-Padilla H, Dean D. Bioceramics for musculoskeletal regenerative medicine: materials and manufacturing process compatibility for synthetic bone grafts and medical devices. In: Ovsianikov a, Yoo J, Mironov V, editors. 3D printing and biofabrication [internet]. Cham: springer international publishing; 2018 [cited 2020 Jan 11]. p. 161–93. Available from: https://doi.org/10.1007/978-3-319-45444-3_22.
Mussano F, Genova T, Serra FG, Carossa M, Munaron L, Carossa S. Nano-pore size of alumina affects Osteoblastic response. Int J Mol Sci. 2018;19:528.
Liu W, Wu H, Zhou M, He R, Jiang Q, Wu Z, et al. Fabrication of fine-grained alumina ceramics by a novel process integrating stereolithography and liquid precursor infiltration processing. Ceram Int. 2016;15:17736–41.
Dehurtevent M, Robberecht L, Hornez JC, Thuault A, Deveaux E, Béhin P. Stereolithography: a new method for processing dental ceramics by additive computer-aided manufacturing. Dental Mater. 2017;33:477–85.
Wu H, Cheng Y, Liu W, He R, Zhou M, Wu S, et al. Effect of the particle size and the debinding process on the density of alumina ceramics fabricated by 3D printing based on stereolithography. Ceram Int. 2016;15:17290–4.
Travitzky N, Bonet A, Dermeik B, Fey T, Filbert-Demut I, Schlier L, et al. Additive manufacturing of ceramic-based materials. Adv Eng Mater. 2014;16:729–54.
Placone JK, Engler AJ. Recent advances in extrusion-based 3D printing for biomedical applications. Adv Healthcare Mater 2019;1701161.
Bose S, Sarkar N, Vahabzadeh S. Sustained release of vitamin C from PCL coated TCP induces proliferation and differentiation of osteoblast cells and suppresses osteosarcoma cell growth. Mater Sci Eng C. 2019;105:110096.
Hung BP, Naved BA, Nyberg EL, Dias M, Holmes CA, Elisseeff JH, et al. Three-Dimensional Printing of Bone Extracellular Matrix for Craniofacial Regeneration.
Nyberg E, Rindone A, Dorafshar A, Grayson WL. Comparison of 3D-printed poly-ɛ-caprolactone scaffolds functionalized with tricalcium phosphate, hydroxyapatite, bio-Oss, or decellularized bone matrix. Tissue Eng A. 2017;23:503–14.
Koski C, Onuike B, Bandyopadhyay A, Bose S. Starch-hydroxyapatite composite bone scaffold fabrication utilizing a slurry extrusion-based solid freeform fabricator. Addit Manuf. 2018;24:47–59.
Sarkar N, Bose S. Liposome-encapsulated Curcumin-loaded 3D printed scaffold for bone tissue engineering. ACS Appl Mater Interfaces. 2019;11:17184–92.
•• Bose S, Sarkar N. Natural medicinal compounds in bone tissue engineering. Trends in Biotechnology. This paper provides detailed insight on the beneficial role of combining 3DP ceramic scaffolds and natural medicinal compounds that have osteogenic effects. This kind of novel combinations can provide more efficient and faster bone healing due to augmented effects of porous ceramic scaffolding together with chemical/pharmacological contributions of the natural medicinal compounds.
Dumas M, Terriault P, Brailovski V. Modelling and characterization of a porosity graded lattice structure for additively manufactured biomaterials. Mater Des. 2017;121:383–92.
Sheydaeian E, Fishman Z, Vlasea M, Toyserkani E. On the effect of throughout layer thickness variation on properties of additively manufactured cellular titanium structures. Addit Manuf. 2017;18:40–7.
Kuo T-Y, Chin W-H, Chien C-S, Hsieh Y-H. Mechanical and biological properties of graded porous tantalum coatings deposited on titanium alloy implants by vacuum plasma spraying. Surf Coat Technol. 2019;372:399–409.
Hee AC. Wear and corrosion resistance of tantalum coating on titanium alloys for biomedical implant applications. 2017;
Campanelli LC, Bortolan CC, da Silva PSCP, Bolfarini C, Oliveira NTC. Effect of an amorphous titania nanotubes coating on the fatigue and corrosion behaviors of the biomedical Ti-6Al-4V and Ti-6Al-7Nb alloys. J Mech Behav Biomed Mater. 2017;100:542–51.
Balla VK, Bose S, Davies NM, Bandyopadhyay A. Tantalum—a bioactive metal for implants. Jom. 2010;62:61–4.
Bandyopadhyay A, Mitra I, Shivaram A, Dasgupta N, Bose S. Direct comparison of additively manufactured porous titanium and tantalum implants towards in vivo osseointegration. Addit Manuf. 2019;28:259–66.
Balla VK, Banerjee S, Bose S, Bandyopadhyay A. Direct laser processing of a tantalum coating on titanium for bone replacement structures. Acta Biomater. 2010;6:2329–34.
Staiger MP, Pietak AM, Huadmai J, Dias G. Magnesium and its alloys as orthopedic biomaterials: a review. Biomaterials. 2006;9:1728–34.
Li Y, Zhou J, Pavanram P, Leeflang MA, Fockaert LI, Pouran B, et al. Additively manufactured biodegradable porous magnesium. Acta Biomater. 2018;67:378–92.
Ibrahim H, Jahadakbar A, Dehghan A, Moghaddam NS, Amerinatanzi A, Elahinia M. In vitro corrosion assessment of additively manufactured porous NiTi structures for bone fixation applications. Metals. 2018;8:164.
Gorgin Karaji Z, Speirs M, Dadbakhsh S, Kruth J-P, Weinans H, Zadpoor AA, et al. Additively manufactured and surface biofunctionalized porous Nitinol. ACS Appl Mater Interfaces. 2017;9:1293–304.
Funding
We would like to acknowledge financial support from the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the National Institutes of Health under Award Nos. R01 AR066361–01 and R01 AR067306–01. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Regenerative Biology and Medicine in Osteoporosis
Rights and permissions
About this article
Cite this article
Bandyopadhyay, A., Mitra, I. & Bose, S. 3D Printing for Bone Regeneration. Curr Osteoporos Rep 18, 505–514 (2020). https://doi.org/10.1007/s11914-020-00606-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-020-00606-2