Abstract
There appears to be no unique mechanically sensitive pathway by which changes in bone loading regulate bone mass and architecture to ensure adequate structural strength. Rather, strain-derived changes in bone cells activate a number of nonspecific strain-sensitive pathways (including calcium fluxes, prostanoids, nitric oxide, extracellular signal-regulated kinase, and sclerostin), the activities of which are modified by a number of factors (including estrogen receptors) for which this contribution is subsidiary to other purposes. The strain-sensitive pathways modified by these factors interact with a number of other pathways, some of which appear to have specific osteoregulatory potential (eg, the parathyroid hormone pathway), whereas others such as the Wnt pathway appear to be associated primarily with the response mechanisms of proliferation, differentiation, and apoptosis. The outcome of these multiple interactions are stimuli for local bone formation, resorption, or maintenance of the status quo, to maintain existing bone architecture or adapt it to a new mechanical regimen.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mechanical loading is the major functional influence on bone mass and architecture and thus the ability of the skeleton to withstand the loads of everyday activity without fracture. The continued importance of this influence in preserving skeletal fracture resistance is evident from the rapid bone loss that occurs with bed rest, disuse, or microgravity. This bone loss when functional loading is reduced is mirrored by bone gain when loading is increased as in adoption of higher levels of athletic activity or manual occupation [1]. Because both the increase in bone mass with increased loading and the decrease with decreased loading are local phenomena directly related to local loading conditions, it has been generally accepted that this functionally adaptive response is locally controlled [2]. It has also been accepted that the controlling stimulus, as far as the bone cells responsible are concerned, is derived from mechanical strain (proportional change in dimension) within the bone tissue under load. These assumptions are supported by a considerable amount of experimental evidence, primarily derived from animal experiments in vivo and experiments on bone cells in vitro [3].
In general, the consensus from animal experiments is that bone architecture is preferentially influenced by loading which generates high strains imposed in unaccustomed distributions at high strain rates, and that the maximum effect of such stimulation can be achieved by very short bursts of activity [4]. Although such a definition of the “active ingredient” of a loading regimen is useful in prescribing “osteogenic” exercise, the potential to use exercise to prevent or treat osteoporosis is limited by a number of factors including 1) lack of compliance; 2) the contraindication of applying vigorous loading to fragile skeletons; 3) the fact that the endocrine/paracrine environment in which loading operates may not always be conducive to an effective osteoregulatory response; and 4) the signaling pathways required for mechanotransduction may be attenuated as a result of aging. The aim of this review is to briefly discuss recent advances regarding selected endocrine and paracrine factors in the adaptation of bone to mechanical loading.
Parathyroid Hormone
The skeleton acts both as a means of providing rigid structural support and a store for calcium. The former requires bone tissue to remain in place to bear loads, whereas the latter requires its removal for metabolic purposes. These two opposing requirements are principally mediated respectively by mechanical loading and calcium-regulating hormones. For many years parathyroid hormone (PTH) was regarded as being almost exclusively involved in the removal of calcium from the skeleton by stimulating resorption. More recently, it has been shown that intermittent doses of PTH are strongly osteogenic. At present, intermittently administered PTH is the only drug licensed for the anabolic treatment of osteoporosis.
PTH acts by binding to the type 1 PTH/PTH-related peptide receptor (PTH1R), a seven-transmembrane receptor highly expressed in bone cells, and activates the Gs-mediated adenylate cyclase–adenosine 3′,5′-monophosphate (cAMP)–protein kinase A (PKA) and Gq/11-mediated phospholipase C–β (PLC-β)–inositol 1,4,5-trisphosphate (IP3)–protein kinase C (PKC) signaling pathways. Additionally, PTH activates the MEK-ERK mitogen-activated protein kinase cascade through both G-protein–dependent and –independent mechanisms [5].
There is some experimental evidence that PTH enhances the osteogenic effects of mechanical loading. Combining loading with intermittent PTH (1–34) synergistically increases cortical bone volume in adult female mice [6]. Therefore, exercise that involves significant loading could be clinically employed as a useful adjunct to support the anabolic effect of intermittent PTH. However, the mechanisms by which PTH acts to enhance the effects of loading remain unclear and require further investigation. Recent evidence suggests that this may involve PTH influencing the “activation state” of the Wingless (Wnt) and AKT signaling pathways [7], both of which are known to be regulated by loading. For example, PTH1R is involved in mediating transduction of mechanical events into biochemical responses in bone cells [8] and activation of PTH1R signaling in osteocytes, the main mechanosensing cells in bone, is associated with increases in bone mass through the Wnt coreceptor low-density lipoprotein receptor–related protein 5 (LRP5) [9]. PTH1R also physically interacts with LRP6 and facilitates its recruitment of intracellular Wnt pathway components [10]. In addition, PTH may promote Wnt signaling by phosphorylating glycogen synthase kinase 3β through a cAMP/PKA-dependent mechanism [11].
Wnts and Sclerostin
Although established as a key developmental pathway in Drosophila, the importance of the Wnt pathway in the regulation of bone mass only became evident when separate mutations of the Lrp5/Frizzled receptor were associated with radically different levels of bone mass in two human families [12]. These receptors are used by locally secreted Wnt proteins to activate canonical and non-canonical Wnt signaling pathways. A major feature of canonical Wnt signaling is the translocation of the second messenger protein β-catenin to the nucleus and it is now established that β-catenin is a key regulator of bone mass acquisition [13]. There is a significant body of evidence to show that β-catenin signaling in bone cells is activated by mechanical stimulation [14–16, 17••, 18] and recent work has shown that this is Wnt/Lrp5 receptor independent [15, 17••]. Mechanical stimulation has also been shown to regulate osteoblast cell fate in a process that involves both non-canonical Wnt signaling and N-cadherin–related β-catenin signaling [16].
One of the ways in which the Wnt pathway is activated is by association of one of the Wnt proteins with the Lrp5/Frizzled receptor. However, this interaction is antagonized by the protein sclerostin. Sclerostin is secreted predominantly by osteocytes, and was first identified as the product of the Sclerosteosis (Sost) gene that is mutated in Sclerosteosis and van Buchem high bone mass disease patients. Sclerostin expression is regulated by multiple factors including PTH [19] and mechanical loading [20] and sclerostin knockout mice do not suffer bone loss due to mechanical unloading caused by tail suspension [21••]. This has led to the idea that sclerostin may be the long-postulated osteocyte-secreted factor that relates osteoblast activity (and thus bone mass) to local strain. To date, little work has been done on the link between sclerostin expression, the bones’ mechanical environment, and exercise/loading in humans. However, stroke patients with immobilization-induced bone loss develop “hypersclerostinemia” [22], and there is evidence of an association between sclerostin expression in osteocytes and fracture risk [23].
Imitation of sclerostin downregulation by a sclerostin-neutralizing antibody increases bone formation, bone mass, and bone strength in nonhuman primates [24] and use of this antibody is a promising anabolic treatment for osteoporosis [25]. One potential feature of using an antibody that neutralizes sclerostin to treat osteoporosis is that by imitating, and adding to, natural strain-related downregulation of sclerostin it may direct the formation of bone to structurally relevant sites, in a way that does not necessarily occur with systemic factors such as PTH.
The relationship between strain-related regulation of sclerostin and other established contributors to bone cells’ early strain-related response remains unclear. Periostin is a matricellular protein that appears to be important, as periostin knockout mice have a high level of sclerostin expression and are unable to downregulate its expression following mechanical loading [26•]. Sex steroids are also potentially important in regulating sclerostin expression as there is accumulating evidence that in women circulating sclerostin levels are influenced by estrogen [27], and in vitro estrogen has been shown to downregulate sclerostin expression in osteocyte-like cells [28]. The nature of the link between sex steroid receptors, mechanical loading, and sclerostin expression has yet to be fully demonstrated; however, as will be discussed in the next section, the role of the estrogen and androgen receptors (ERs and ARs) in mediating bone’s response to mechanical strain gives clues as to the gender-related nature of the structurally deleterious bone loss associated with osteoporosis.
Estrogen Receptor-α
The obvious association between bone loss and the menopause in women has always suggested a causal relationship between regulation of bone mass and declining levels of estrogen. This has been supported by studies associating levels of bioavailable estrogen with levels of bone loss in both women and men. Despite this obvious association, establishing the role of estrogen itself in the regulation of bone mass has proved problematic. More promising has been the involvement of the estrogen receptor (ER).
There is accumulating evidence [3] indicating that ERα is involved in loading-related osteogenesis in animals in vivo [29, 30••] as well as osteoblasts’ and osteocytes’ responses to mechanical stimulation in vitro [14, 17••, 31]. Its potential role in estrogen deficiency–related bone loss in humans is, as yet, hypothetical but could involve ER downregulation, as a consequence of reduced estrogen concentrations, to an extent that there are insufficient ERs in the bone cells to facilitate those mechanically related signaling pathways in which it is involved. This suggests the possibility that targeting specific ER actions with selective estrogen receptor modulators (SERMs) could stimulate bone gain, in a structurally relevant manner, without unwanted effects on other estrogen target tissues.
The effects of tamoxifen and fulvestrant, drugs used clinically for breast cancer patients, on bone’s responses to mechanical loading have recently been investigated in ovariectomized adult mice [32•]. Fulvestrant, considered to be a pure estrogen antagonist, does not modify the effects of mechanical loading on either trabecular or cortical bone whereas a clinically relevant dose of tamoxifen, the first SERM, has a profound osteogenic effect on trabecular bone and synergistically enhances loading-related increase in trabecular bone mass through an ER-mediated mechanism [32•]. This supports the hypothesis that appropriate modulation of ER activity to enhance loading-related regulation of bone mass could not only mitigate the effects of potentially reduced ER numbers, but also enhance the osteoregulatory effects of loading thus stimulating the maintenance or restitution of structurally appropriate bone architecture.
Although the ER does not appear to be essential for bone cells to be able to respond to mechanical strain, it does appear to contribute to a range of signaling pathways activated by mechanical stimulation. The range of this effect has been shown quite dramatically in a microarray study in which the transcriptional response of mouse bones to loading was markedly reduced and delayed in ERα knockout mice compared with wild-type littermates [33]. In contrast to the 642 genes differentially transcribed in the tibiae of wild-type mice 3 h after being subjected to a single brief episode of loading, the expression of only 26 genes was altered in the tibiae of ERα knockout mice at this time point. Of particular interest is that Sost expression was significantly reduced by loading in wild-type mice but did not occur in those lacking ERα [33].
ERα is believed to contribute to bone cells’ response to mechanical strain through both genomic and nongenomic actions. Nongenomic contributions of ERα include its sensitization of insulin-like growth factor 1 receptor (IGF-1R) signaling through a direct interaction with this receptor [17••] facilitating upregulation of early strain target genes such as cyclooxygenase-2 (COX-2) [34]. Although there is compelling evidence that signaling by IGF-1 is a key component of the early stages of the adaptive response of bone to loading [17••], the actual source of the IGF-1 remains controversial. The time frame in which IGF-1 signaling appears to act is not associated with any autocrine or paracrine synthesis. Similarly, long-term exercise also does not correlate with elevated serum IGF-1 levels [35]. Our experiments have shown that mechanical strain sensitizes the osteoblastic response to endogenous IGF-1 levels [17••], which would suggest that risk factors for osteoporosis capable of reducing basal IGF-1 levels could well attenuate the IGF-1 component of the adaptive response. It has also recently been shown that β1 integrin, which is required for loading-related bone formation in vivo [36] as well as bone loss caused by disuse [37], can be regulated by ERα and that this is a mechanism by which estrogen can augment the expression of target genes [38].
In contrast to its effect in female mice, in males ERα seems to have no significant effect on bone’s response to mechanical loading in vivo. In these animals AR signaling appears to be important, as male AR knockout mice show higher cortical bone response to mechanical loading compared with wild-type littermates, and in male AR knockout mice the suppression of sclerostin expression in osteocytes was greater following loading than in wild-types [30••]. In the same study it was shown that testosterone appears to blunt fluid flow-induced production of nitric oxide, a known modulator of bone mechanotransduction, in osteoblastic cells. Nevertheless, another study has shown that mechanical loading prevented cancellous bone loss in male mice after orchidectomy [39]. Clearly many questions remain unanswered as to the role of sex steroids in mediating bone’s adaptive response to loading. This is not surprising since recent experiments in mice targeting the deletion of ERs and ARs to different bone cell types are now revealing the complexity of the role(s) of sex steroid receptors in regulating bone metabolism [40].
Other Factors
Within the past few years it has become evident that there is no unique mechanically sensitive transduction pathway by which changes in bone strain regulate bone mass and architecture to ensure that bones are able to withstand customary loads without fracture or accumulation of structurally deleterious levels of microdamage. Rather, changes in bone strain, which involve changes in the dimension of the cells as well as fluid flow past them and tension on their attachments to their matrix, activate a large number of nonspecific pathways that interact with one another and are modified by multiple factors, many of which (eg, ERα) have traditionally been associated exclusively with other specific processes under endocrine or paracrine control (Fig. 1). The outcomes of these multiple activations and interactions are presumably signals for adaptive remodeling or maintenance of the structural status quo. The upside of this is that there are presumably multiple opportunities for therapeutic interference to produce a beneficial remodeling result. The downsides include the complexity of a system, which makes it difficult to identify such opportunities by logical systematic experiment, and that the system itself provides many opportunities for compensatory regulation. Below we list a number of areas that are being investigated and may prove of future benefit as therapeutic targets.
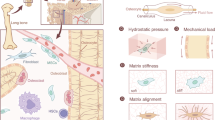
Schematic representation of signaling pathways activated by mechanical stimuli in osteoblastic cells. Stimuli engendered by increased loading are sensed by a variety of receptors including integrin-mediated connections to the extracellular matrix (ECM) and membrane structures sensitive to physical forces such as the stretch-activated cation (Ca2+) channels. These in turn activate a number of signaling pathways, resulting in reduced expression of anti-osteogenic factors, such as sclerostin, and increased signaling by pro-osteogenic molecules such as Wnts, prostanoids (PGE2) acting via EP2/4 receptors, and insulin-like growth factors (IGFs) that act through the IGF-1 receptor (IGF-1R). These extracellular signaling molecules, together with changes in the activity of intracellular mediators such as β-catenin and estrogen receptor-α (ERα), provide an environment conducive to structurally appropriate osteogenesis. These local processes are influenced by systemic hormones such as parathyroid hormone and leptin, acting through their specific membrane receptors, PTH1R and Lepr, respectively. AR androgen receptor; COX-2 cyclooxygenase-2; Cx43 connexin 43; eNOS endothelial nitric oxide synthase; ERK extracellular signal-regulated kinase; GSK-3 glycogen synthase kinase 3; LRP lipoprotein receptor–related protein; NFAT nuclear factor of activated T cells; PI3-K phosphotidylinositol 3-kinase; PKA protein kinase A; PKC protein kinase C
Leptin
It is known that an increase in body weight is associated with bone gain in the weight-bearing regions. However, gain in body fat, rather than lean body mass, actually leads to bone resorption, and a link between fat and bone has been suggested via the adipocyte-secreted hormone leptin. Although it remains controversial whether leptin exerts its effect on bone mass mainly through central or peripheral mechanisms, a recent study has demonstrated a role for the leptin receptor (Lepr) as a direct negative modulator of bones’ osteogenic response to mechanical loading [41]. This study showed that the response of bone to loading in vivo and of osteoblastic cells to fluid flow in vitro was both enhanced in leptin or Lepr knockout mice compared with their wild-type littermates. Furthermore, the enhanced response to fluid flow in osteoblastic cells from leptin knockout mice was abrogated by the addition of leptin. Removal of leptin or Lepr also enhanced mechanically induced increases in Wnt and ERα signaling.
Prostanoids
Nonselective and selective COX-2 inhibitors (NSAIDs), widely used to treat pain and inflammation in humans, are thought to influence bone metabolism by blocking the production of prostaglandin E2 (PGE2), and a number of studies have reported a role for COX-2 expression in bone’s adaptation to loading. Among four PGE2 G-protein–coupled receptors, EP1-4, EP2, and EP4 appear to exert primary skeletal effects. For example, in osteocytes subjected to fluid flow, PGE2 signaling through EP2/EP4 receptors appears to protect against dexamethasone-induced apoptosis in vitro [42]. However, in a recent randomized controlled trial, administration of ibuprofen, a commonly used nonselective COX inhibitor, before exercise did not significantly reduce exercise-related increase in hip and femoral shaft areal bone mineral density in healthy premenopausal women [43].
Connexin 43
Connexin 43 (Cx43) is emerging as a key factor in mediating mechanotransduction in bone. In vivo mechanical loading of Cx43 knockout mice showed that these mice had a significant reduction in their loading-related increase in bone formation [44]. This is in agreement with an in vitro study showing increased Cx43 expression in osteocytes subjected to fluid flow [45]. The role of Cx43 in loading involves, at least in part, its ability to form hemi-channels through which PGE2 is released into the extracellular space [46].
Nuclear factor of activated T cells
Nuclear factor of activated T cells (NFAT) is activated in osteoblast progenitor-like cells by fluid flow [47] and fluid flow–induced activation of NFAT plays a role in COX-2 upregulation in osteoblastic cells [48]. NFAT activation may hold potential benefits to augmenting reduced responses to loading in the senescent skeleton as treatment of aged mice with a low dose of cyclosporine A augmented loading-related bone formation to the level seen in young controls [49].
Interleukin-11
Interleukin-11 is a factor that has recently been shown to play a potentially important role in bone cells’ response to mechanical stimulation [50]. Its expression is upregulated following mechanical stimulation and enhances the differentiation of osteoblastic cells. The enhancement of interleukin-11 gene transcription was shown to result from activation of the Smad pathway through PKCδ.
Conclusions
It is becoming increasingly evident that there is no unique mechanically sensitive pathway by which bone loading regulates bone mass and architecture to ensure resistance to fracture. Rather, changes in bone strain activate a number of nonspecific strain-sensitive pathways that can be modified by a number of factors such as ERα whose contribution is subsidiary to other purposes. These strain-sensitive pathways interact with other osteoregulatory pathways including the PTH and Wnt signaling pathways. The outcomes of these multiple interactions are stimuli for local changes in bone formation and resorption to either maintain existing bone architecture or adapt it to a new mechanical regimen. A challenge for the future is to translate this increased knowledge of the complex portfolio of strain-responsive pathways into novel therapeutic strategies and to gain a better understanding of the influence of aging on this complex system.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Lanyon LE, Sugiyama T, Price JS. Regulation of bone mass: local control or systemic influence or both? IBMS BoneKEy. 2009;6:218–26.
Sugiyama T, Price JS, Lanyon LE. Functional adaptation to mechanical loading in both cortical and cancellous bone is controlled locally and is confined to the loaded bones. Bone. 2010;46:314–21.
Lanyon LE, Armstrong VJ, Saxon LK, et al. Estrogen receptors critically regulate bone's adaptive responses to loading. Clinic Rev Bone Miner Metab. 2007;5:234–48.
Skerry TM. The response of bone to mechanical loading and disuse: fundamental principles and influences on osteoblast/osteocyte homeostasis. Arch Biochem Biophys. 2008;473:117–23.
Datta NS, Abou-Samra AB. PTH and PTHrP signaling in osteoblasts. Cell Signal. 2009;21:1245–54.
Sugiyama T, Saxon LK, Zaman G, et al. Mechanical loading enhances the anabolic effects of intermittent parathyroid hormone (1–34) on trabecular and cortical bone in mice. Bone. 2008;43:238–48.
Weinstein RS, Jilka RL, Almeida M, et al. Intermittent parathyroid hormone administration counteracts the adverse effects of glucocorticoids on osteoblast and osteocyte viability, bone formation, and strength in mice. Endocrinology. 2010;151:2641–9.
Zhang YL, Frangos JA, Chachisvilis M. Mechanical stimulus alters conformation of type 1 parathyroid hormone receptor in bone cells. Am J Physiol Cell Physiol. 2009;296:C1391–1399.
O'Brien CA, Plotkin LI, Galli C, et al. Control of bone mass and remodeling by PTH receptor signaling in osteocytes. PLoS One. 2008;3:e2942.
Wan M, Yang C, Li J, et al. Parathyroid hormone signaling through low-density lipoprotein-related protein 6. Genes Dev. 2008;22:2968–79.
Suzuki A, Ozono K, Kubota T, et al. PTH/cAMP/PKA signaling facilitates canonical Wnt signaling via inactivation of glycogen synthase kinase-3β in osteoblastic Saos-2 cells. J Cell Biochem. 2008;104:304–17.
Baron R, Rawadi G. Wnt signaling and the regulation of bone mass. Curr Osteoporos Rep. 2007;5:73–80.
Kramer I, Halleux C, Keller H, et al. Osteocyte Wnt/β-catenin signaling is required for normal bone homeostasis. Mol Cell Biol. 2010;30:3071–85.
Armstrong VJ, Muzylak M, Sunters A, et al. Wnt/β-catenin signaling is a component of osteoblastic bone cell early responses to load-bearing and requires estrogen receptor α. J Biol Chem. 2007;282:20715–27.
Case N, Ma M, Sen B, et al. β-catenin levels influence rapid mechanical responses in osteoblasts. J Biol Chem. 2008;283:29196–205.
Arnsdorf EJ, Tummala P, Jacobs CR. Non-canonical Wnt signaling and N-cadherin related β-catenin signaling play a role in mechanically induced osteogenic cell fate. PLoS One. 2009;4:e5388.
•• Sunters A, Armstrong VJ, Zaman G, et al.: Mechano-transduction in osteoblastic cells involves strain-regulated estrogen receptor α-mediated control of insulin-like growth factor (IGF) I receptor sensitivity to ambient IGF, leading to phosphatidylinositol 3-kinase/AKT-dependent Wnt/LRP5 receptor-independent activation of β-catenin signaling. J Biol Chem 2010, 285:8743–8758. Whereas β-catenin signaling is recognized to be a key regulator of bone’s adaptation to loading, the mechanisms by which it is activated in osteoblastic cells following mechanical strain are less clearly understood. This paper shows that β-catenin may be activated through a mechanism involving the IGF/AKT axis independently of canonical Wnts or LRP5 but involving ERα.
Kamel MA, Picconi JL, Lara-Castillo N, Johnson ML. Activation of β-catenin signaling in MLO-Y4 osteocytic cells versus 2T3 osteoblastic cells by fluid flow shear stress and PGE2: Implications for the study of mechanosensation in bone. Bone. 2010;47:872–81.
Kramer I, Loots GG, Studer A, et al. Parathyroid hormone (PTH)-induced bone gain is blunted in SOST overexpressing and deficient mice. J Bone Miner Res. 2010;25:178–89.
Robling AG, Niziolek PJ, Baldridge LA, et al. Mechanical stimulation of bone in vivo reduces osteocyte expression of Sost/sclerostin. J Biol Chem. 2008;283:5866–75.
•• Lin C, Jiang X, Dai Z, et al.: Sclerostin mediates bone response to mechanical unloading through antagonizing Wnt/β-catenin signaling. J Bone Miner Res 2009, 24:1651–1661. While sclerostin expression had previously been demonstrated to be mechanically regulated, this paper attributes functional importance to this process by showing lack of unloading-induced bone loss in the absence of sclerostin expression. Furthermore, lack of unloading-induced changes in Wnt signaling in sclerostin knockout mice supports the supposition that sclerostin exerts its effects as an antagonist of Wnt signaling in vivo.
Gaudio A, Pennisi P, Bratengeier C, et al. Increased sclerostin serum levels associated with bone formation and resorption markers in patients with immobilization-induced bone loss. J Clin Endocrinol Metab. 2010;95:2248–53.
Power J, Poole KE, van Bezooijen R, et al. Sclerostin and the regulation of bone formation: effects in hip osteoarthritis and femoral neck fracture. J Bone Miner Res. 2010;25:1867–76.
Ominsky MS, Vlasseros F, Jolette J, et al. Two doses of sclerostin antibody in cynomolgus monkeys increases bone formation, bone mineral density, and bone strength. J Bone Miner Res. 2010;25:948–59.
Padhi D, Jang G, Stouch B, et al. Single-dose, placebo-controlled, randomized study of AMG 785, a sclerostin monoclonal antibody. J Bone Miner Res. 2011;26:19–26.
• Bonnet N, Standley KN, Bianchi EN, et al.: The matricellular protein periostin is required for sost inhibition and the anabolic response to mechanical loading and physical activity. J Biol Chem 2009, 284:35939–35950. This study shows that mechanical loading increases periostin expression, which is involved in the inhibition of Sost expression thereby up-regulating osteoblast function.
Modder UI, Clowes JA, Hoey K, et al. Regulation of circulating sclerostin levels by sex steroids in women and in men. J Bone Miner Res. 2011;26:27–34.
Mabilleau G, Mieczkowska A, Edmonds ME. Thiazolidinediones induce osteocyte apoptosis and increase sclerostin expression. Diabet Med. 2010;27:925–32.
Lee K, Jessop H, Suswillo R, et al. Bone adaptation requires oestrogen receptor-α. Nature. 2003;424:389.
•• Callewaert F, Bakker A, Schrooten J, et al.: Androgen receptor disruption increases the osteogenic response to mechanical loading in male mice. J Bone Miner Res 2010, 25:124–131. This study shows that AR activation limits the periosteal bone response to in vivo mechanical loading whereas testosterone administration and subsequent AR activation block the in vitro fluid flow-induced NO production. In addition, AR signaling following mechanical loading appears to be associated with changes in SOST/sclerostin signaling.
Aguirre JI, Plotkin LI, Gortazar AR, et al. A novel ligand-independent function of the estrogen receptor is essential for osteocyte and osteoblast mechanotransduction. J Biol Chem. 2007;282:25501–8.
• Sugiyama T, Galea GL, Lanyon LE, Price JS: Mechanical loading-related bone gain is enhanced by tamoxifen but unaffected by fulvestrant in female mice. Endocrinology 2010, 151:5582–5590. This study provides experimental evidence to support the hypothesis that targeting specific ER actions with SERMs may stimulate bone gain, in a structurally appropriate manner, without adverse effects on other estrogen target tissues.
Zaman G, Saxon LK, Sunters A, et al. Loading-related regulation of gene expression in bone in the contexts of estrogen deficiency, lack of estrogen receptor α and disuse. Bone. 2010;46:628–42.
Liedert A, Wagner L, Seefried L, et al. Estrogen receptor and Wnt signaling interact to regulate early gene expression in response to mechanical strain in osteoblastic cells. Biochem Biophys Res Commun. 2010;394:755–9.
Pomerants T, Tillmann V, Karelson K, et al. Impact of acute exercise on bone turnover and growth hormone/insulin-like growth factor axis in boys. J Sports Med Phys Fitness. 2008;48:266–71.
Litzenberger JB, Tang WJ, Castillo AB, Jacobs CR. Deletion of β1 integrins from cortical osteocytes reduces load-induced bone formation. Cell Mol Bioeng. 2009;2:416–24.
Phillips JA, Almeida EA, Hill EL, et al. Role for β1 integrins in cortical osteocytes during acute musculoskeletal disuse. Matrix Biol. 2008;27:609–18.
Yeh CR, Chiu JJ, Lee CI, et al. Estrogen augments shear stress-induced signaling and gene expression in osteoblast-like cells via estrogen receptor-mediated expression of β1-integrin. J Bone Miner Res. 2010;25:627–39.
Fritton JC, Myers ER, Wright TM, van der Meulen MC. Bone mass is preserved and cancellous architecture altered due to cyclic loading of the mouse tibia after orchidectomy. J Bone Miner Res. 2008;23:663–71.
Imai Y, Kondoh S, Kouzmenko A, Kato S. Regulation of bone metabolism by nuclear receptors. Mol Cell Endocrinol. 2009;310:3–10.
Kapur S, Amoui M, Kesavan C, et al. Leptin receptor (Lepr) is a negative modulator of bone mechanosensitivity and genetic variations in Lepr may contribute to the differential osteogenic response to mechanical stimulation in the C57BL/6J and C3H/HeJ pair of mouse strains. J Biol Chem. 2010;285:37607–18.
Kitase Y, Barragan L, Qing H, et al. Mechanical induction of PGE2 in osteocytes blocks glucocorticoid-induced apoptosis through both the β-catenin and PKA pathways. J Bone Miner Res. 2010;25:2381–92.
Kohrt WM, Barry DW, Van Pelt RE, et al. Timing of ibuprofen use and bone mineral density adaptations to exercise training. J Bone Miner Res. 2010;25:1415–22.
Grimston SK, Brodt MD, Silva MJ, Civitelli R. Attenuated response to in vivo mechanical loading in mice with conditional osteoblast ablation of the connexin43 gene (Gja1). J Bone Miner Res. 2008;23:879–86.
Xia X, Batra N, Shi Q, et al. Prostaglandin promotion of osteocyte gap junction function through transcriptional regulation of connexin 43 by glycogen synthase kinase 3/β-catenin signaling. Mol Cell Biol. 2010;30:206–19.
Siller-Jackson AJ, Burra S, Gu S, et al. Adaptation of connexin 43-hemichannel prostaglandin release to mechanical loading. J Biol Chem. 2008;283:26374–82.
Sen B, Styner M, Xie Z, et al. Mechanical loading regulates NFATc1 and β-catenin signaling through a GSK3β control node. J Biol Chem. 2009;284:34607–17.
Celil Aydemir AB, Minematsu H, Gardner TR, et al. Nuclear factor of activated T cells mediates fluid shear stress- and tensile strain-induced Cox2 in human and murine bone cells. Bone. 2010;46:167–75.
Srinivasan S, Ausk BJ, Prasad J, et al. Rescuing loading induced bone formation at senescence. PLoS Comput Biol. 2010;6:e1000924.
Kido S, Kuriwaka-Kido R, Umino-Miyatani Y, et al. Mechanical stress activates Smad pathway through PKCδ to enhance interleukin-11 gene transcription in osteoblasts. PLoS One. 2010;5:e13090.
Acknowledgments
This work was supported by the Wellcome Trust. G.L. Galea and L.B. Meakin are recipients of Integrated Training Fellowships for Veterinarians from the Wellcome Trust.
Disclosure
No potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Price, J.S., Sugiyama, T., Galea, G.L. et al. Role of Endocrine and Paracrine Factors in the Adaptation of Bone to Mechanical Loading. Curr Osteoporos Rep 9, 76–82 (2011). https://doi.org/10.1007/s11914-011-0050-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-011-0050-7