Abstract
Purpose of Review
Ethnicity has long been described as a major risk factor for the development of gestational diabetes mellitus (GDM), and it is widely recognised that women from ethnicities other than Europids are at higher risk of developing GDM. There are also described differences between ethnicities in key GDM pregnancy outcomes. This review describes some of the factors that relate to the ethnic disparities in GDM.
Recent Findings
The global prevalence of GDM has been steadily increasing and estimated to be 16.2% from the International Diabetes Federation extrapolation. Reported prevalence rates may understate the true prevalence, due to factors of access and attitudes to GDM diagnosis and screening in low resource settings for foreign-born women and indigenous populations. Other factors may relate to genes associated with specific ethnicities, obesity, body composition and gestational weight gain.
Summary
Various factors such as access to screening, body composition, genetics and gestational weight gain may result in ethnic disparities in the prevalence and outcomes of GDM.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gestational diabetes mellitus (GDM) has traditionally been defined as “any degree of glucose intolerance with onset or first recognition in pregnancy” [1, 2]. The World Health Organisation (WHO) now designates GDM as a subset of and distinct from the broader term hyperglycaemia in pregnancy (HIP) [3, 4, 5••]. GDM is said to occur late in pregnancy as a transient condition with less severe hyperglycaemia, differing from diabetes in pregnancy (DIP) where diabetes is overt in pregnancy and likely to continue after birth. However, recent literature suggests there may also be an entity related to early-onset GDM which may be distinct from DIP and a separate subset of HIP [6], as GDM typically appears in the second or third trimester. GDM exhibits a large proportion of HIP, with estimates that it represents 75–90% of all HIP cases [7]. The term GDM in this review will imply cases of hyperglycaemia that exclude DIP, unless such a delineation is not evident.
Ethnicity has long been recognised as a major risk factor to the development of GDM [8], and women from many ethnic groups have been recommended to be screened as soon as feasible, and have the screening repeated at 24–28 weeks of gestation [1, 2]. Specific ethnicities of high risk cited include Hispanic, African, Native American, South or East Asian, Pacific Islands or Indigenous Australians [1, 9, 10]. However, in reality, this is all ethnic groups besides those of Anglo-European descent (“Europids”) [11].
The Concept of Ethnicity
The Oxford Dictionary defines ethnic as “relating to a population subgroup (within a larger or dominant national or cultural group) with a common national or cultural tradition” [12]. It is felt to be a social construct to group individuals who share a similar sense of traits and potentially outlook on healthcare. However, the word is problematic as it often has variable meanings, and the boundaries of ethnic groups have become more narrowly defined for research purposes [13]. For example, in 1997, the United States’ Office of Management and Budget released a directive recommending the classification of data into five racial (American Indian or Alaska Native, Asian, Black or African American, Native Hawaiian or Pacific Islander, White) and two ethnic categories (Hispanic or Latino, or Not Hispanic or Latino) [14]. Prior to this, the terms American Indian or Alaskan Native, Asian or Pacific Islander, Black not of Hispanic origin, Hispanic and White not of Hispanic (NHW) origin were the broad categories. When looking at the epidemiology data around GDM, many large US-based studies have used broad classifications such as “Black not Hispanic” or “White not Hispanic”, despite obvious heterogeneity within groups [15,16,17,18]. Despite this, commentators recognise that it is still useful to use ethnic classifications in medical research, as they represent the social history which potentially underpins a person’s health [19,20,21].
Beyond ethnic differences in GDM, pregnant women from one ethnic group who live in a country outside of their country of birth may further predispose them to developing GDM [22,23,24]. For example, Kim et al. showed that the relative risk of developing GDM was higher among foreign-born mothers compared to US-born women, across almost all ethnic groups aside from East Asian (Chinese, Japanese and Korean), both in adjusted and unadjusted models for BMI, age and parity [16].
Prevalence and Screening
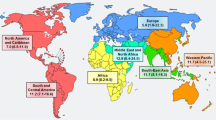
The prevalence of GDM relating to various ethnic groups varies considerably. The International Diabetes Federation (IDF) Atlas 8th edition estimates that the global prevalence of HIP between 20 and 49 years of age to be 16.2%, affecting 21.3 million births [7]. Of these, 86.4% are predicted to be due to GDM with 7.4% due to DIP and 6.2% due to diabetes detected prior to pregnancy. Regional prevalence ranges from 10.4% in Africa to 24.2% in South East Asia (comprising of seven countries—India, Bangladesh, Nepal, Sri Lanka, Mauritius, Bhutan and the Maldives) [25]. However, these groupings hide substantial variation within ethnic groups. For example, a large retrospective study in New Jersey differentiating between South Asians showed that Bangladeshi women had the highest rate of GDM, followed by Indians, Sri Lankans and Pakistanis [18].
The landmark Hyperglycaemia and Adverse Pregnancy Outcomes (HAPO) study was published in 2008, and the International Association of Diabetes and Pregnancy Study Groups (IADPSG) developed screening strategy based on the HAPO study outcomes [2, 26]. Based on this, the World Health Organisation has updated its diagnostic criteria for classification of GDM [5••]. Prior to HAPO, there was no standard agreement on which screening strategy was to be used, and even within a country, it was not uncommon for varying screening strategies to be used [27]. Since then, there has been an explosion of GDM-related literature, particularly around the impact of the changed diagnostic criteria and increased prevalence [28, 29]. Several large epidemiological studies have also highlighted the range of differences in GDM between ethnic groups. Table 1 summarises the largest epidemiological studies in the past 5 years since the widespread adoption of the HAPO recommendations through the IADPSG diagnostic criteria.
HAPO also highlighted the varying patterns of hyperglycaemia in different ethnic groups. Overall 55% of women were diagnosed based on the fasting plasma glucose (FPG), 33% were diagnosed on the 1-h value and only 12% at 2 h. However, among the various ethnic groups, GDM was diagnosed on the FPG in 24% of women in Bangkok but 74% of women in Barbados, this pattern was reversed at the 1-h value (76 v 32%); however, women from Belfast had the lowest (25%) and Hong Kong had the highest (65%) diagnostic rate at the 2-h value [39].
The widespread uptake of the IADPSG and WHO recommendations has meant comprehensive screening programs have been implemented with increased diagnosis and improved access to perinatal care for women with GDM [27, 38, 40]. Most GDM prevalence studies applying these recommendations describe an increase in prevalence, with studies in North India and United Arab Emirates reporting as much as a fourfold increase to representing over one-third of the population [41, 42]. However, when looking at data recorded in Table 1, it appears that the crude prevalence rates, even for the high-risk ethnicities, are below that of the estimated 16.2% by the IDF. This is due in part to a gradual adoption of the IADPSG criteria, with only 4 of the 11 studies mentioned applying the newer criteria, or variants thereof. There are however many other factors influencing prevalence estimates and Fig. 1 summaries the various factors that influence the prevalence estimates of GDM.
Difficulties in comparing prevalence data in GDM with different approaches. GDM: gestational diabetes mellitus; OGTT: oral glucose tolerance testing. (From Simmons D. Epidemiology of Diabetes in Pregnancy. In: McCance D, Maresh M, Sacks DA, editors. A Practical Manual of Diabetes in Pregnancy. 2nd Edition. Copyright © 2018 by John Wiley & Sons, Inc. Reprinted by permission of John Wiley & Sons, Inc.) [11]
Most of the large prevalence studies are focused in the geographic regions of North America, Europe and Asia Pacific, and hence there are inaccuracies when estimating GDM in ethnicities outside of these regions. Many factors impact on the ability of low or limited-resource settings to be able to implement the IADPSG and NICE screening guidelines [2, 29, 43, 44•]. For example, some West African and Sub-Saharan African countries which have no estimation of GDM as screening is not systematically performed due to resource limitations and selective screening strategies are used [45,46,47]. Many limited-resource countries use risk factor-based screening, and Ogu et al. describe an underestimation of GDM prevalence in the Niger Delta due to using selective risk-based screening compared with universal screening [47]. Similarly, Nakabuye et al. reported that 23.8% of GDM cases were missed through the current selective screening strategy employed in Nsambaya Uganda [48]. Other authors from Asian cohorts have suggested the use of alternate strategies such as fasting plasma glucose [49] or the “two-step” [50] approaches as being more appropriate in developing countries.
Authors of studies in high-resource settings have also questioned the benefits of using a comprehensive screening strategy with recent studies in Finland and Denmark reporting that use of comprehensive screening over risk factor-based screening increased the rate of diagnosis of mild GDM with little consequence in health outcomes while placing substantial demands on hospitals and healthcare resources [40, 51, 52].
Utz and De Brouwere reported barriers to GDM screening and management in the low and lower-middle income countries of Africa, South Asian and Latin America include lack of standard comprehensible guidelines; lack of knowledge and training in screening and managing GDM; limited access to care with some settings only having 15% women attending public facilities; prohibitive costs in relation to testing, equipment, medication and hospitalisation; and unavailability of specific equipment, medications and health care providers [44•]. Compounding the problem is the lack of awareness of patients, providers and the general community to GDM and inertia to change established behaviours. This often results in non-adherence to dietary modifications, medications, performance of regular blood glucose monitoring and attendance of appointments [53]. The prevalence estimates of indigenous populations of Australian and Canadian Aborigines, American Indian and Inuit are likely understated due to low screening rates and similar factors discussed above [54,55,56].
Genetic Predisposition
There has been a growing interest in the genetics of GDM. A number of gene variants were identified that may predispose to GDM, largely based on their known association with type 2 diabetes (T2D). To date, candidate studies and genome-wide association analysis (GWAS) have identified eight genes associated with development of GDM–CDK5 regulatory subunit associated protein 1 like 1(CDKAL1), glucokinase (GCK), insulin-like growth factor 2 mRNA binding protein 2 (IGF2BP2), insulin receptor substrate 1 (IRS1), potassium voltage-gated channel subfamily J member 11 (KCNJ11), potassium voltage-gated channel subfamily Q member 1 (KCNQ1), melatonin receptor 1B (MTNR1B) and transcription factor 7 like 2 (TCF7L2) [57,58,59]. Of these, using the unbiased approach of GWAS, only CDKALI (odds ratio 1.518; p = 6.65 × 10−16) and MTNR1B (odds ratio 1.454; p = 2.49 × 10−13) have been shown to have strong GDM association in a study of Korean women with 468 affected and 1242 controls [60].
The methylthiotransferase CDKALI rs7754580 has been associated in a study of 1146 Han Chinese women with reduced gestational insulin sensitivity (p = 0.011) and increased disposition (p = 0.0002) [61]. Another hypothesis exploring the genetic susceptibility of GDM is that abnormal changes in the melatonin signalling pathway occur in patients with GDM, as melatonin receptors are expressed in pancreatic beta-cells and are part of a signalling system that may reduce insulin secretion. Variants in the single-nucleotide polymorphism rs10830963 in MTNR1B have been associated with GDM susceptibility [62]. Li investigated 350 GDM patients and 480 controls concluded that both MTNR1B (genotype OR 1.22, padjusted = 0.039; allele OR 1.21, padjusted = 0.032) and MTNR1A (genotype OR 1.36; padjusted = 0.011; allele OR 1.45, padjusted = 0.003) were associated with women of Han Chinese ethnicity who had GDM [63]. Whereas a study of 750 Mexican women (408 cases and 342 controls) showed that MTNR1B rs1387153 was associated with GDM (p = 0.00022) [64].
Lin et al.’s meta-analysis of 16 studies involving 4853 cases and 10,631 controls showed that the TCF7L2 rs7903146 polymorphism was associated with increased risk of GDM in Europid, Hispanic and Asian subgroups, with Asians who are TT allele homozygous having the highest risk (OR 3.08, p = 0.002) [65]. Another large recent analysis conducted using DNA collected from offspring of predominantly Europid ethnicity from three large cohort studies (1160 DNA trios) including 1367 HAPO participants, demonstrated that the polymorphic variation in foetal paternally transmitted genes IGF2 rs10770125 (p = 3.2 × 10−8) and INS rs2582 (p = 3.6 × 10−5) may result in elevated glucose intolerance in the mother in late pregnancy [58]. Studies in non-pregnant populations have shown there is substantial overlap between genetic variations association with T2D and metabolic quantitative traits [66]. In the GDM literature to date, there have been two genes identified through GWAS, HKDC1 (pmeta-analysis = 1.022 × 10−22) that has been associated with 2 h-glucose post oral glucose tolerance test and BACE2 (pmeta-analysis = 6.30 × 10−16) associated with fasting c-peptide in a meta-analysis of HAPO sample and two other cohorts [67].
Body Composition and Gestational Weight Gain
Obesity is on the rise across the world, with the rates nearly tripling since 1975 and an estimated 40% of adult women aged 18 and over are reported as being overweight or obese [68]. Studies show that the absolute risk of having GDM was more than two times higher among mothers who had a body mass index (BMI) of ≥ 25 kg/m2and the risk of women rising to eightfold if severely obese [16, 69]. However, Makgoba et al. demonstrated the influential role ethnicity plays in stratifying risk according to BMI, where women of a normal BMI from African, Caribbean and South Asian ethnicities had a 2.52, 1.21 and 3.0 odds ratio of developing GDM compared with Europids. This trend increased exponentially with increasing body mass levels [70]. Although obesity is strongly associated with risk of developing GDM, it is not a reliable predictor of developing GDM in East Asian women. A large study conducted in London showed that only 13% of East Asian women who develop GDM were in the obese range when BMI was measured and calculated at the first booking appointment, compared with one-third of White and South Asian, and half of the Black women [32].
Widespread immigration of Asian and African ethnicities, which traditionally have a greater proportion of women who are underweight or normal weight [71] to countries with higher rates of overweight and obese weight such as the US, has meant obesity rates among those (migrated) ethnic groups are rising dramatically [72], placing pregnant women in these groups at greater risk of GDM [73]. The ethnicities with the highest average female adult weight were those from Polynesia and Micronesia, averaging above 30 kg/m2 [71].
Maternal obesity, excessive gestational weight gain (GWG) and presence of GDM all contribute to a metabolic state during pregnancy that can have lasting sequelae for the child, long into adulthood. This adverse metabolic state caused by obesity and GDM in utero may have effect on the central nervous regulatory centres of metabolism and weight control, and lead to increased insulin, glucose, protein and/or leptin levels during the early critical stages of a child’s development [74].
Both maternal undernutrition and overweight conditions have been implicated in foetal programming, with long-term health implications for the child [75]. Being underweight is also associated with poor pregnancy outcomes, including increased mortality, delivery complications, preterm birth and intrauterine growth retardation [76, 77]. East Asian women have some of the highest rates of moderate or severely underweight [71]. In Japan, 1 in 5 women of childbearing age (20–30s) are underweight, defined by BMI < 18.5 kg/m2 [78]. However, the risk of GDM occurs at a much lower BMI in Asian women compared to women of other ethnicities, as seen in the Kaiser Permanente cohort analysis [73]. In fact, being underweight at age 20 was found to be positively associated with GDM in Japanese women [79].
Aside from obvious ethnic differences in BMI and weight, the parameters of subcutaneous fat and serum leptin levels have been described to be more likely retained after delivery in South Asians compared with Europeans. These likely contribute to the increase risk of GDM in subsequent pregnancies as they increase the risk of retaining weight and subcutaneous fat which leads to excess adiposity and obesity when entering the next pregnancy [80].
Treatment
Treatment of GDM has traditionally consisted of lifestyle measures aimed at reducing hyperglycaemia of women through dietary counselling, physical activity and glucose monitoring, prior to the initiation of medical management [81].
Medical Nutritional Therapy (MNT) or diet has been associated in GDM with improved foetal outcomes, and prevention of macrosomia [82]. The standard nutritional advice for pregnant women is largely based on the Institute of Medicine (IOM) reports on “Nutrition During Pregnancy” published in 1990 [83], the 2009 report on weight gain in pregnancy [84] and the 2006 “Dietary Reference Intakes: The Essential Guide to Nutrient Requirements” [85]. These guidelines recommend the appropriate amount of gestational weight gain (GWG) should be calculated for each woman based on prepregnancy weight and height. Modern recommendations recommend a balanced approach to macro and micronutrient intake and a modest increment in daily caloric intake of 340 to 450 kcal/day in the latter two trimesters [86].
Despite MNT being the main treatment option for GDM, there are substantial differences in the knowledge or way this is applied in various cultures. Ali et al. showed that women with GDM from the United Arab Emirates (UAE) had no significant difference in food knowledge compared to women without GDM, and overall had poor awareness of the carbohydrate content in food and drink [87]. Paradoxically, a study in Japan noted that high carbohydrate intake was associated with a lower risk of glucose intolerance as seen with a positive glucose challenge test (GCT). They also noted that rice accounted for only 30.3% of the carbohydrate intake of Japanese women, and a 60% total energy intake from carbohydrates was associated with a halving of the risk of a positive GCT compared with those who had a carbohydrate intake of 49% [88]. In Singapore, the Growing Up in Singapore Toward Healthy Outcomes (GUSTO) trial showed that a higher dietary protein intake was associated with a higher risk of GDM [89].
A challenge in the prescription and adherence to MNT is the impact of cultural traditions that surround food and meal times [90]. For example, many women of the Islamic faith will observe fasting during the month of Ramadan, despite being excused by their faith from participating while pregnant [91]. Furthermore, there are large variations in the amount of carbohydrate intake between cultural groups, for instance South Asians and Pacific Islanders will traditionally consume large amounts of carbohydrates in different forms at each meal. This poses a challenge for clinicians in trying to limit the carbohydrate intake for women in these ethnic groups [92].
GWG has been a topical issue, as many women are gaining excess weight during pregnancy resulting in adverse pregnancy outcomes and there are ethnic differences in the amount of weight gained during pregnancy [93]. Recently, there has been a push for women with GDM to gain less weight than the recommended by the 2009 IOM guidelines [84, 94]. Previously, a large multi-ethnic population study in Washington State concluded that the IOM recommendations decreased adverse maternal outcomes, and decreased the odds ratio of small for gestational age and large for gestational age (LGA) infants [95]. This was echoed in a Korean study where the BMI cut-offs were lower [96]. However, a recent randomised control trial of 606 women in Norway aimed at limiting GWG through lifestyle intervention showed no measurable benefit in obstetric or neonatal outcomes despite a small decrease in GWG [97]. A large systematic review of over 1.3 million pregnancies published in 2017 concluded that weight gain above and below the IOM recommendations were associated with adverse maternal and infant outcomes [98].
The recommendations of physical activity for GDM treatment are likely based on assumptions that physical activity has a direct impact on insulin sensitivity and glucose homeostasis [99, 100], as well as the WHO guidelines for physical activity for the general adult population [101]. However, few studies have defined specific recommendations for physical activity in the treatment of GDM women and its effect on varying ethnicities [102]. The GUSTO trial in Singapore in fact showed that sedentary behaviour was not associated with increased risk of GDM, but that high levels of physical activity had a protective effect against women developing GDM but specifically in women with BMI ≥ 23 kg/m2 [103].
Outcomes
GDM is recognised to be associated with poor perinatal and foetal outcomes such as macrosomia, LGA infants, preeclampsia, hypertensive disorders in pregnancy, shoulder dystocia and caesarean section [5]. Pregnant mothers with GDM are also at risk postpartum complications of developing overt diabetes and having GDM in subsequent pregnancies [104]. As described above, the epigenetic environment is often unfavourable for the child who is at risk of developing obesity, diabetes and metabolic syndrome in adulthood [105, 106]. Appropriate treatment of GDM has been shown to reduce the incidence of adverse foetal outcomes of macrosomia, preeclampsia and shoulder dystocia [107].
Ethnic differences in perinatal outcomes have been reported in the past by several authors [108, 109]. More recently, Sanchalika and Teresa reported that Bangladeshi, Indian and Pakistani women with GDM had a lower rate of preterm birth and LGA than Non-Hispanic white females, but higher small for gestational age (SGA) infants [18].
Development of diabetes post GDM has been quoted as occurring in between 2.6% in Europid and 70% in the Sioux in a 2002 meta-analysis [110], and 9.6 times the general population at 25.8% at 25 years [111]. Moses et al. found that the Australian prevalence of diabetes in a predominantly Europid population followed for up to 25 years after GDM pregnancy was twice the general prevalence at 10.3% [112]. A systematic review showed that overall there was a 48% rate of GDM recurrence, but that the NHW recurrence rate of 39% which was significantly lower than that of other ethnicities at 56% [113].
Interestingly, Khan et al. recently published a cohort study of more than 40,000 Ontario singleton pregnancies who had GDM and showed a lower rate of GDM-associated adverse outcomes in 2106 refugees and 16,232 immigrants from various countries were compared with 22,564 non-immigrant women [114]. Overall, they had lower rates of preeclampsia, preterm birth, macrosomia, respiratory distress syndrome and neonatal hyperbilirubinaemia, despite being of significantly lower socio-economic status than the non-immigrant group. The authors put this down to a “healthy immigrant effect” and are self-selected to be healthy individuals, but were somewhat surprised that this effect applied to refugee women [114].
Conclusion
There appear to be many factors which contribute to the ethnic differences in prevalence and outcomes in GDM including screening strategies in different countries, genetics, body composition, gestational weight gain and cultural attitudes and practices. With a move toward global adoption of the IADPSG guidelines, low-resourced countries are not currently able to meet the increased demands placed on them through the lowered screening OGTT thresholds, nor the follow-up required to manage the increased prevalence of GDM. A deeper understanding of these factors and focusing further research on strategies that may help narrow the gap between how GDM can be managed among different ethnicities will likely result in lower prevalence rates and better outcomes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major Importance
Metzger BE, Coustan DR. Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. The Organizing Committee. Diabetes Care. 1998;21(Suppl 2):B161–7.
International Association of Diabetes Pregnancy Study Groups Consensus Panel, Metzger BE, Gabbe SG, Persson B, Buchanan TA, Catalano PA, et al. International association of diabetes and pregnancy study groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care. 2010;33(3):676–82. https://doi.org/10.2337/dc09-1848.
Guariguata L, Linnenkamp U, Beagley J, Whiting DR, Cho NH. Global estimates of the prevalence of hyperglycaemia in pregnancy. Diabetes Res Clin Pract. 2014;103(2):176–85. https://doi.org/10.1016/j.diabres.2013.11.003.
Hod M, Kapur A, Sacks DA, Hadar E, Agarwal M, Di Renzo GC, et al. The International Federation of Gynecology and Obstetrics (FIGO) initiative on gestational diabetes mellitus: a pragmatic guide for diagnosis, management, and care. Int J Gynecol Obstet. 2015;131:S173–211. https://doi.org/10.1016/S0020-7292(15)30007-2.
•• World Health Organization. Diagnostic criteria and classification of hyperglycaemia first detected in pregnancy. 2013. This report formally adopted the IADPSG and HAPO guidelines and clarified the differences between diabetes in pregnancy and gestational diabetes mellitus.
Immanuel J, Simmons D. Screening and treatment for early-onset gestational diabetes mellitus: a systematic review and meta-analysis. Curr Diab Rep. 2017;17(11). https://doi.org/10.1007/s11892-017-0943-7.
International Diabetes Federation. IDF Diabetes Atlas. Brussels, Belgium: International Diabetes Federation 2017.
Yue DK, Molyneaux LM, Ross GP, Constantino MI, Child AG, Turtle JR. Why does ethnicity affect prevalence of gestational diabetes? The underwater volcano theory. Diabet Med :J Br Diabet Assoc. 1996;13(8):748–52. https://doi.org/10.1002/(SICI)1096-9136(199608)13:8<748::AID-DIA164>3.0.CO;2-I.
Berkowitz GS, Lapinski RH, Wein R, Lee D. Race/ethnicity and other risk factors for gestational diabetes. Am J Epidemiol. 1992;135(9):965–73. https://doi.org/10.1093/oxfordjournals.aje.a116408.
Dornhorst A, Paterson CM, Nicholls JS, Wadsworth J, Chiu DC, Elkeles RS, et al. High prevalence of gestational diabetes in women from ethnic minority groups. Diabet Med: J Br Diabet Assoc. 1992;9(9):820–5.
Simmons D. Epidemiology of Diabetes in Pregnancy. In: McCance D, Maresh M, Sacks DA, editors. A practical manual of diabetes in pregnancy. Newark, UNITED KINGDOM: John Wiley & Sons, Incorporated; 2017. p. 3–16.
Stevenson A. Oxford dictionary of English. 3rd ed. Oxford England; New York: Oxford University Press, 2010.
Kaplan JB, Bennett T. Use of race and ethnicity in biomedical publication. JAMA. 2003;289(20):2709–16. https://doi.org/10.1001/jama.289.20.2709.
Office of Management and Budget (US). Revisions to the standards for classification of federal data on race and ethnicity. In: Budget OoMa, editor.: 62 Federal Register 58781; 1997.
Avilés-Santa ML, Colón-Ramos U, Lindberg NM, Mattei J, Pasquel FJ, Pérez CM. From sea to shining sea and the great plains to patagonia: a review on current knowledge of diabetes mellitus in hispanics/Latinos in the US and Latin America. Front Endocrinol. 2017;8(NOV). https://doi.org/10.3389/fendo.2017.00298.
Kim SY, Sappenfield W, Sharma AJ, Wilson HG, Bish CL, Salihu HM, et al. Racial/ethnic differences in the prevalence of gestational diabetes mellitus and maternal overweight and obesity, by nativity, Florida, 2004–2007. Obesity (Silver Spring, Md). 2013;21(1):E33–40. https://doi.org/10.1002/oby.20025.
Thorpe L, Berger D, Ellis J, Bettegowda V. Trends and racial/ethnic disparities in gestational diabetes among pregnant women in New York City, 1990-2001. Am J Public Health. 2005;95(9):1536–9.
Sanchalika A, Teresa J. Risk of gestational diabetes among South Asian immigrants living in New Jersey—a retrospective data review. J Racial Ethn Health Disparities. 2015;2(4):510–6. https://doi.org/10.1007/s40615-015-0099-6.
Caldwell SH, Popenoe R. Perceptions and misperceptions of skin color. Ann Intern Med. 1995;122(8):614–7.
Huth EJ. Identifying ethnicity in medical papers. Ann Intern Med. 1995;122(8):619–21.
Williams DR. Race and health: basic questions, emerging directions. Ann Epidemiol. 1997;7(5):322–33.
Piffer S, Pertile R, Romanelli T. The prevalence of gestational diabetes in the province of trento, trend 2010-2015 and adverse neonatal outcomes. Diabetes. 2017;66(Supplement 1):A646.
Jeppesen C, Maindal HT, Kristensen JK, Ovesen PG, Witte DR. National study of the prevalence of gestational diabetes mellitus among Danish women from 2004 to 2012. Scand J Public Health. 2017;45(8):811–7. https://doi.org/10.1177/1403494817736943.
Yallampalli C, Golla C, Banadakoppa M, Espinoza AF, Espinoza J. Migrant status is a risk factor for gestational diabetes, independent from maternal obesity in hispanic populations. Am J Obstet Gynecol. 2018;218(1 Supplement 1):S592.
Ogurtsova K, da Rocha Fernandes JD, Huang Y, Linnenkamp U, Guariguata L, Cho NH, et al. IDF diabetes atlas: global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Res Clin Pract. 2017;128:40–50. https://doi.org/10.1016/j.diabres.2017.03.024.
HAPO Study Cooperative Research Group, Metzger BE, Lowe LP, Dyer AR, Trimble ER, Chaovarindr U et al. Hyperglycemia and adverse pregnancy outcomes, . N Engl J Med. 2008;358(19):1991–2002. doi:https://doi.org/10.1056/NEJMoa0707943.
Yan Y, Liu Z, Liu D. Heterogeneity of glycometabolism in patients with gestational diabetes mellitus: retrospective study of 1,683 pregnant women. J Diabetes Investig. 2017;8(4):554–9. https://doi.org/10.1111/jdi.12595.
Colagiuri S, Falavigna M, Agarwal MM, Boulvain M, Coetzee E, Hod M, et al. Strategies for implementing the WHO diagnostic criteria and classification of hyperglycaemia first detected in pregnancy. Diabetes Res Clin Pract. 2014;103(3):364–72. https://doi.org/10.1016/j.diabres.2014.02.012.
Jenum AK, Morkrid K, Sletner L, Vangen S, Torper JL, Nakstad B, et al. Impact of ethnicity on gestational diabetes identified with the WHO and the modified International Association of Diabetes and Pregnancy Study Groups criteria: a population-based cohort study. Eur J Endocrinol. 2012;166(2):317–24. https://doi.org/10.1530/eje-11-0866.
Bardenheier BH, Imperatore G, Gilboa SM, Geiss LS, Saydah SH, Devlin HM, et al. Trends in gestational diabetes among hospital deliveries in 19 U.S. states, 2000-2010. Am J Prev Med. 2015;49(1):12–9. https://doi.org/10.1016/j.amepre.2015.01.026.
Yeung RO, Savu A, Kinniburgh B, Lee L, Dzakpasu S, Nelson C, et al. Prevalence of gestational diabetes among Chinese and South Asians: a Canadian population-based analysis. J Diabetes Complicat. 2017;31(3):529–36. https://doi.org/10.1016/j.jdiacomp.2016.10.016.
Nishikawa E, Oakley L, Seed PT, Doyle P, Oteng-Ntim E. Maternal BMI and diabetes in pregnancy: investigating variations between ethnic groups using routine maternity data from London, UK. PLoS One. 2017;12(6):e0179332. https://doi.org/10.1371/journal.pone.0179332.
Kim SY, Saraiva C, Curtis M, Wilson HG, Troyan J, Sharma AJ. Fraction of gestational diabetes mellitus attributable to overweight and obesity by race/ethnicity, California, 2007-2009. Am J Public Health. 2013;103(10):e65–72. https://doi.org/10.2105/ajph.2013.301469.
Pu J, Zhao B, Wang EJ, Nimbal V, Osmundson S, Kunz L, et al. Racial/ethnic differences in gestational diabetes prevalence and contribution of common risk factors. Paediatr Perinat Epidemiol. 2015;29(5):436–43. https://doi.org/10.1111/ppe.12209.
Tsai PJ, Roberson E, Dye T. Gestational diabetes and macrosomia by race/ethnicity in Hawaii. BMC Res Notes. 2013;6:395. https://doi.org/10.1186/1756-0500-6-395.
Chang AL, Hurwitz E, Miyamura J, Kaneshiro B, Sentell T. Maternal risk factors and perinatal outcomes among Pacific Islander groups in Hawaii: a retrospective cohort study using statewide hospital data. BMC Pregnancy Childbirth. 2015;15:239. https://doi.org/10.1186/s12884-015-0671-4.
McDonald R, Karahalios A, Le T, Said J. A retrospective analysis of the relationship between ethnicity, body mass index, and the diagnosis of gestational diabetes in women attending an Australian antenatal clinic. Int J Endocrinol. 2015;2015:297420. https://doi.org/10.1155/2015/297420.
Wong VW, Lin A, Russell H. Adopting the new World Health Organization diagnostic criteria for gestational diabetes: how the prevalence changes in a high-risk region in Australia. Diabetes Res Clin Pract. 2017;129:148–53. https://doi.org/10.1016/j.diabres.2017.04.018.
Sacks DA, Coustan DR, Hadden DR, Hod M, Maresh M, Oats JJN, et al. Frequency of gestational diabetes mellitus at collaborating centers based on IADPSG consensus panel-recommended criteria: the hyperglycemia and adverse pregnancy outcome (HAPO) study. Diabetes Care. 2012;35(3):526–8. https://doi.org/10.2337/dc11-1641.
Koivunen S, Torkki A, Bloigu A, Gissler M, Pouta A, Kajantie E, et al. Towards national comprehensive gestational diabetes screening—consequences for neonatal outcome and care. Acta Obstet Gynecol Scand. 2017;96(1):106–13. https://doi.org/10.1111/aogs.13030.
Arora GP, Thaman RG, Prasad RB, Almgren P, Brons C, Groop LC, et al. Prevalence and risk factors of gestational diabetes in Punjab, North India: results from a population screening program. Eur J Endocrinol. 2015;173(2):257–67. https://doi.org/10.1530/eje-14-0428.
Agarwal MM, Dhatt GS, Othman Y. Gestational diabetes: differences between the current international diagnostic criteria and implications of switching to IADPSG. J Diabetes Complicat. 2015;29(4):544–9. https://doi.org/10.1016/j.jdiacomp.2015.03.006.
National Institute for Health and Care Excellence. Diabetes in Pregnancy: Management of diabetes and its complications from preconception to the postnatal period. In: guideline N, editor. Diabetes in pregnancy: management of diabetes and its complications from preconception to the postnatal period. National Institute for Health and Care Excellence: Clinical Guidelines. London: National Institue for Health and Care Excellence; 2015.
• Utz B, De Brouwere V. Why screen if we cannot follow-up and manage? Challenges for gestational diabetes screening and management in low and lower-middle income countries: results of a cross-sectional survey. BMC Pregnancy and Childbirth. 2016;16(1):341. https://doi.org/10.1186/s12884-016-1143-1. This study presented a survey that illustrated specific challenges in adopting GDM screening and management guidelines in 40 countries in Africa, South-Asia and Latin-America
Sagna Y, Yanogo DAR, Bagbila A, Saloukou E, Zombre TY, Guira O, et al. Prevalence, associated factors and evolution of gestational diabetes mellitus in Ouagadougou. Trop Med Int Health. 2017;22(Supplement 1):333. https://doi.org/10.1111/%28ISSN%291365-3156.
Pastakia SD, Njuguna B, Onyango BA, Washington S, Christoffersen-Deb A, Kosgei WK, et al. Prevalence of gestational diabetes mellitus based on various screening strategies in western Kenya: a prospective comparison of point of care diagnostic methods. BMC Pregnancy Childbirth. 2017;17(1):226. https://doi.org/10.1186/s12884-017-1415-4.
Ogu RN, John OC, Maduka O, Chinenye S. Assessing the outcome of universal vs. risk-based screening for GDM in resource limited setting of the Niger-delta. Diabetes. 2017;66(Supplement 1):A647.
Nakabuye B, Bahendeka S, Byaruhanga R. Prevalence of hyperglycaemia first detected during pregnancy and subsequent obstetric outcomes at St. Francis Hospital Nsambya BMC research notes 2017;10(1):174. https://doi.org/10.1186/s13104-017-2493-0.
Shen S, Lu J, Zhang L, He J, Li W, Chen N, et al. Single fasting plasma glucose versus 75-g oral glucose-tolerance test in prediction of adverse perinatal outcomes: a cohort study. EBioMedicine. 2017;16:284–91. https://doi.org/10.1016/j.ebiom.2017.01.025.
Luewan S, Bootchaingam P, Tongsong T. Comparison of the screening tests for gestational diabetes mellitus between “one-step” and “two-step” methods among Thai pregnant women. Obstet Gynecol Int. 2018;2018:1521794–5. https://doi.org/10.1155/2018/1521794.
Lencioni C, Gualdani E, Lacaria E, Francesconi P, Di Cianni G, Seghieri G. Identification of gestational diabetes and pregnancy outcomes: a population study. Diabetologia 2017;60 (1 Supplement 1):S293-S4. https://doi.org/10.1007/s00125-017-4350-z.
McIntyre HD, Jensen DM, Jensen RC, Kyhl HB, Jensen TK, Glintborg D, et al. Gestational diabetes mellitus: does one size fit all? A challenge to uniform worldwide diagnostic thresholds. Diabetes Care. 2018;41:1339–42. https://doi.org/10.2337/dc17-2393.
Utz B, Assarag B, Essolbi A, Barkat A, El Ansari N, Fakhir B, et al. Improving detection and initial management of gestational diabetes through the primary level of care in Morocco: protocol for a cluster randomized controlled trial. Reprod Health. 2017;14(1):75. https://doi.org/10.1186/s12978-017-0336-z.
Saad N, Wilson D, Donovan LE. Solving the mystery: the true prevalence of gestational diabetes in indigenous women. Diabetes Metab Res Rev. 2015;31(5):476–8. https://doi.org/10.1002/dmrr.2648.
Chamberlain C, Joshy G, Li H, Oats J, Eades S, Banks E. The prevalence of gestational diabetes mellitus among Aboriginal and Torres Strait islander women in Australia: a systematic review and meta-analysis. Diabetes Metab Res Rev. 2015;31(3):234–47. https://doi.org/10.1002/dmrr.2570.
Kirkham R, Whitbread C, Connors C, Moore E, Boyle JA, Richa R, Barzi F, Li S, Dowden M, Oats J, Inglis C, Cotter M, McIntyre HD, Kirkwood M, van Dokkum P, Svenson S, Zimmet P, Shaw JE, O’Dea K, Brown A, Maple-Brown L, on behalf of the Northern Territory Diabetes in Pregnancy Partnership Implementation of a diabetes in pregnancy clinical register in a complex setting: findings from a process evaluation. PLoS One 2017;12 (8) (no pagination)(e0179487). https://doi.org/10.1371/journal.pone.0179487.
U.S. National Library of Medicine. Gestational diabetes. In: Your Guide to Understanding Genetic Conditions. National Institutes of Health, Lister Hill National Center for Biomedical Communications. 2018. https://ghr.nlm.nih.gov/condition/gestational-diabetes-diagnosis-diagnosis. Accessed 10 May 2018 2018.
Petry CJ, Mooslehner K, Prentice P, Hayes MG, Nodzenski M, Scholtens DM, et al. Associations between a fetal imprinted gene allele score and late pregnancy maternal glucose concentrations. Diabetes Metab. 2017;43:323–31. https://doi.org/10.1016/j.diabet.2017.03.002.
Lowe WL Jr, Scholtens DM, Sandler V, Hayes MG. Genetics of gestational diabetes mellitus and maternal metabolism. Curr Diab Rep. 2016;16(2):15. https://doi.org/10.1007/s11892-015-0709-z.
Kwak SH, Kim S-H, Cho YM, Go MJ, Cho YS, Choi SH, et al. A genome-wide association study of gestational diabetes mellitus in Korean women. Diabetes. 2012;61(2):531–41. https://doi.org/10.2337/db11-1034.
Jie M, Shunyao L, Yunqiang L, Yuande T, Hailian W, Yaming L, et al. Association of variants in CDKN2A/2B and CDKAL1 genes with gestational insulin sensitivity and disposition in pregnant Han Chinese women. J Diabetes Investig. 2015;6(3):295–301. https://doi.org/10.1111/jdi.12315.
Tarnowski M, Malinowski D, Safranow K, Dziedziejko V, Pawlik A. MTNR1A and MTNR1B gene polymorphisms in women with gestational diabetes. Gynecol Endocrinol : Off J Int Soc Gynecol Endocrinol 2017;33(5):395–398. https://doi.org/10.1080/09513590.2016.1276556.
Li C, Qiao B, Zhan Y, Peng W, Chen ZJ, Sun L, et al. Association between genetic variations in MTNR1A and MTNR1B genes and gestational diabetes mellitus in Han Chinese women. Gynecol Obstet Investig. 2013;76(4):221–7. https://doi.org/10.1159/000355521.
Huerta-Chagoya A, Vazquez-Cardenas P, Moreno-Macias H, Tapia-Maruri L, Rodriguez-Guillen R, Lopez-Vite E, et al. Genetic determinants for gestational diabetes mellitus and related metabolic traits in Mexican women. PLoS One. 2015;10(5):e0126408. https://doi.org/10.1371/journal.pone.0126408.
Lin PC, Lin WT, Yeh YH, Wung SF. Transcription factor 7-like 2 (TCF7L2) rs7903146 polymorphism as a risk factor for gestational diabetes mellitus: a meta-analysis. PLoS One. 2016;11(4):e0153044. https://doi.org/10.1371/journal.pone.0153044.
Marullo L, El-Sayed Moustafa JS, Prokopenko I. Insights into the genetic susceptibility to type 2 diabetes from genome-wide association studies of glycaemic traits. Curr Diab Rep. 2014;14(11):551. https://doi.org/10.1007/s11892-014-0551-8.
Hayes MG, Urbanek M, Hivert MF, Armstrong LL, Morrison J, Guo C, et al. Identification of HKDC1 and BACE2 as genes influencing glycemic traits during pregnancy through genome-wide association studies. Diabetes. 2013;62(9):3282–91. https://doi.org/10.2337/db12-1692.
World Health Organization. Obesity and overweight. 2016. http://www.who.int/en/news-room/fact-sheets/detail/obesity-and-overweight.
Chu SY, Callaghan WM, Kim SY, Schmid CH, Lau J, England LJ, et al. Maternal obesity and risk of gestational diabetes mellitus. Diabetes Care. 2007;30(8):2070–6. https://doi.org/10.2337/dc06-2559a.
Makgoba M, Savvidou MD, Steer PJ. An analysis of the interrelationship between maternal age, body mass index and racial origin in the development of gestational diabetes mellitus. BJOG : Int J Obstet Gynaecol. 2012;119(3):276–82. https://doi.org/10.1111/j.1471-0528.2011.03156.x.
NCD Risk Factor Collaboration. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: a pooled analysis of 2416 population-based measurement studies in 128.9 million children, adolescents, and adults. Lancet. 2017;390(10113):2627–42. https://doi.org/10.1016/S0140-6736(17)32129-3.
Goel MS, McCarthy EP, Phillips RS, Wee CC. Obesity among US immigrant subgroups by duration of residence. JAMA. 2004;292(23):2860–7. https://doi.org/10.1001/jama.292.23.2860.
Hedderson M, Ehrlich S, Sridhar S, Darbinian J, Moore S, Ferrara A. Racial/ethnic disparities in the prevalence of gestational diabetes mellitus by BMI. Diabetes Care. 2012;35(7):1492–8. https://doi.org/10.2337/dc11-2267.
Stupin JH. Current aspects of perinatal programming. J Perinat Med. 2017;45(Supplement 2):245.
Marciniak A, Patro-Malysza J, Kimber-Trojnar Z, Marciniak B, Oleszczuk J, Leszczynska-Gorzelak B. Fetal programming of the metabolic syndrome. Taiwan J Obstet Gynecol. 2017;56(2):133–8. https://doi.org/10.1016/j.tjog.2017.01.001.
Han Z, Lutsiv O, Mulla S, Rosen A, Beyene J, McDonald SD, et al. Low gestational weight gain and the risk of preterm birth and low birthweight: a systematic review and meta-analyses. Acta Obstet Gynecol Scand. 2011;90(9):935–54. https://doi.org/10.1111/j.1600-0412.2011.01185.x.
Black RE, Victora CG, Walker SP, Bhutta ZA, Christian P, de Onis M, et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet. 2013;382(9890):427–51. https://doi.org/10.1016/S0140-6736(13)60937-X.
Ministry of Health Labour and Welfare of Japan. The national health and nutrition survey in Japan. In: Welfare MoHLa, editor; 2011.
Yachi Y, Tanaka Y, Nishibata I, Sugawara A, Kodama S, Saito K, et al. Low BMI at age 20 years predicts gestational diabetes independent of BMI in early pregnancy in Japan: Tanaka Women’s Clinic Study. DiabMed: J Brit Diabetic Assoc. 2013;30(1):70–3. https://doi.org/10.1111/j.1464-5491.2012.03712.x.
Sommer C, Jenum AK, Waage CW, Morkrid K, Sletner L, Birkeland KI. Ethnic differences in BMI, subcutaneous fat, and serum leptin levels during and after pregnancy and risk of gestational diabetes. Eur J Endocrinol. 2015;172(6):649–56. https://doi.org/10.1530/eje-15-0060.
Crowther CA, Hiller JE, Moss JR, McPhee AJ, Jeffries WS, Robinson JS, et al. Effect of treatment of gestational diabetes mellitus on pregnancy outcomes. N Engl J Med. 2005;352(24):2477–86. https://doi.org/10.1056/NEJMoa042973.
Vestgaard M, Christensen AS, Viggers L, Lauszus FF. Birth weight and its relation with medical nutrition therapy in gestational diabetes. Arch Gynecol Obstet. 2017;296(1):35–41. https://doi.org/10.1007/s00404-017-4396-7.
Food and Nutritional Board. Part II Dietary Intake and Nutrient Supplements. In: Institute of Medicine, editor. Nutrition during pregnancy: part I weight gain: part II nutrient supplements. Washington (DC): National Academy of Science; 1990.
National Research Council, Rasmussen KM, Yaktine AL, Institute of Medicine (U.S.). Committee to reexamine IOM pregnancy weight guidelines. Weight gain during pregnancy : reexamining the guidelines. 2009.
Institute of Medicine. Dietary reference intakes: the essential guide to nutrient requirements. Washington, DC: the National Academies Press; 2006.
Garner CD. Nutrition in pregnancy. In: UpToDate. UpToDate. 2018. www.uptodate.com. Accessed 11 May 2018.
Ali HI, Jarrar AH, El Sadig M, Yeatts B, Diet K. Carbohydrate food knowledge of multi-ethnic women: a comparative analysis of pregnant women with and without gestational diabetes mellitus. PLoS One. 2013;8(9):e73486. https://doi.org/10.1371/journal.pone.0073486.
Tajima R, Yachi Y, Tanaka Y, Kawasaki YA, Nishibata I, Hirose AS, et al. Carbohydrate intake during early pregnancy is inversely associated with abnormal glucose challenge test results in Japanese pregnant women. Diabetes Metab Res Rev. 2017;33 https://doi.org/10.1002/dmrr.2898.
Pang WW, Colega M, Cai S, Chan YH, Padmapriya N, Chen LW, et al. Higher maternal dietary protein intake is associated with a higher risk of gestational diabetes mellitus in a multiethnic Asian cohort. J Nutr. 2017;147(4):653–60. https://doi.org/10.3945/jn.116.243881.
Yuen L, Wong VW. Gestational diabetes mellitus: challenges for different ethnic groups. World J Diabetes. 2015;6(8):1024–32. https://doi.org/10.4239/wjd.v6.i8.1024.
Okunoye G, Konje J, Lindow S, Perva S. Gestational diabetes in the Gulf region: streamlining care to optimise outcome. Journal of Local and Global Health Science. 2015;2015(1):1–6. https://doi.org/10.5339/jlghs.2015.2.
Major AC, Henry JM, De Veciana AM, Morgan AM. The effects of carbohydrate restriction in patients with diet-controlled gestational diabetes. Obstet Gynecol. 1998;91(4):600–4. https://doi.org/10.1016/S0029-7844(98)00003-9.
Kinnunen TI, Waage CW, Sommer C, Sletner L, Raitanen J, Jenum AK. Ethnic differences in gestational weight gain: a population-based cohort study in Norway. Matern Child Health J. 2016;20(7):1485–96. https://doi.org/10.1007/s10995-016-1947-7.
Viecceli C, Remonti LR, Hirakata VN, Mastella LS, Gnielka V, Oppermann MLR, et al. Weight gain adequacy and pregnancy outcomes in gestational diabetes: a meta-analysis. Obes Rev. 2017;18(5):567–80. https://doi.org/10.1111/obr.12521.
Khanolkar AR, Hanley GE, Koupil I, Janssen PA. 2009 IOM guidelines for gestational weight gain: how well do they predict outcomes across ethnic groups? Ethn Health. 2017:1–16. https://doi.org/10.1080/13557858.2017.1398312.
Wie JH, Park IY, Namkung J, Seo HW, Jeong MJ, Kwon JY. Is it appropriate for Korean women to adopt the 2009 Institute of Medicine recommendations for gestational weight gain? PLoS One. 2017;12(7):e0181164. https://doi.org/10.1371/journal.pone.0181164.
Sagedal LR, Overby NC, Bere E, Torstveit MK, Lohne-Seiler H, Smastuen M, et al. Lifestyle intervention to limit gestational weight gain: the Norwegian fit for delivery randomised controlled trial. BJOG : Int J Obstet Gynaecol. 2017;124(1):97–109. https://doi.org/10.1111/1471-0528.13862.
Goldstein RF, Abell SK, Ranasinha S, Misso M, Boyle JA, Black MH, et al. Association of gestational weight gain with maternal and infant outcomes: a systematic review and meta-analysis. JAMA. 2017;317(21):2207–25. https://doi.org/10.1001/jama.2017.3635.
Retnakaran R, Qi Y, Sermer M, Connelly PW, Zinman B, Hanley AJ. Pre-gravid physical activity and reduced risk of glucose intolerance in pregnancy: the role of insulin sensitivity. Clin Endocrinol. 2009;70(4):615–22. https://doi.org/10.1111/j.1365-2265.2008.03393.x.
Tobias DK, Zhang C, van Dam RM, Bowers K, Hu FB. Physical activity before and during pregnancy and risk of gestational diabetes mellitus: a meta-analysis. Diabetes Care. 2011;34(1):223–9. https://doi.org/10.2337/dc10-1368.
World Health Organization. Global recommendations on physical activity for health. Switzerland: WHO Library Cataloguing-in-Publication Data; 2010.
Reader DM. Medical nutrition therapy and lifestyle interventions. Diabetes Care. 2007;30(Suppl 2):S188–93. https://doi.org/10.2337/dc07-s214.
Padmapriya N, Bernard JY, Liang S, Loy SL, Cai S, Zhe IS, et al. Associations of physical activity and sedentary behavior during pregnancy with gestational diabetes mellitus among Asian women in Singapore. BMC pregnancy and childbirth. 2017;17(1):364. https://doi.org/10.1186/s12884-017-1537-8.
Catalano PM, McIntyre HD, Cruickshank JK, McCance DR, Dyer AR, Metzger BE, et al. The hyperglycemia and adverse pregnancy outcome study: associations of GDM and obesity with pregnancy outcomes. Diabetes Care. 2012;35(4):780–6. https://doi.org/10.2337/dc11-1790.
Hammoud NM, Visser GHA, van Rossem L, Biesma DH, Wit JM, de Valk HW. Long-term BMI and growth profiles in offspring of women with gestational diabetes. Diabetologia 2018;61(5):1037–1045. https://doi.org/10.1007/s00125-018-4584-4.
Sellers EA, Dean HJ, Shafer LA, Martens PJ, Phillips-Beck W, Heaman M, et al. Exposure to gestational diabetes mellitus: impact on the development of early-onset type 2 diabetes in Canadian first nations and non-first nations offspring. Diabetes Care. 2016;39(12):2240–6. https://doi.org/10.2337/dc16-1148.
Falavigna M, Schmidt MI, Trujillo J, Alves LF, Wendland ER, Torloni MR, et al. Effectiveness of gestational diabetes treatment: a systematic review with quality of evidence assessment. Diabetes Res Clin Pract. 2012;98(3):396–405. https://doi.org/10.1016/j.diabres.2012.09.002.
Silva JK, Kaholokula JK, Ratner R, Mau M. Ethnic differences in perinatal outcome of gestational diabetes mellitus. Diabetes Care. 2006;29(9):2058–63. https://doi.org/10.2337/dc06-0458.
Rao AK, Cheng YW, Caughey AB. Perinatal complications among different Asian-American subgroups. Am J Obstet Gynecol. 2006;194(5):e39–41. https://doi.org/10.1016/j.ajog.2006.01.027.
Kim C, Newton KM, Knopp RH. Gestational diabetes and the incidence of type 2 diabetes: a systematic review. Diabetes Care. 2002;25(10):1862–8.
Lee AJ, Hiscock RJ, Wein P, Walker SP, Permezel M. Gestational diabetes mellitus: clinical predictors and long-term risk of developing type 2 diabetes: a retrospective cohort study using survival analysis. Diabetes Care. 2007;30(4):878–83. https://doi.org/10.2337/dc06-1816.
Moses RG, Goluza I, Borchard JP, Harman A, Dunning A, Milosavljevic M. The prevalence of diabetes after gestational diabetes—an Australian perspective. Aust N Z J Obstet Gynaecol. 2017;57(2):157–61. https://doi.org/10.1111/ajo.12581.
Schwartz N, Nachum Z, Green MS. The prevalence of gestational diabetes mellitus recurrence—effect of ethnicity and parity: a metaanalysis. Am J Obstet Gynecol. 2015;213(3):310–7. https://doi.org/10.1016/j.ajog.2015.03.011.
Khan S, Yao Z, Shah BR. Gestational diabetes care and outcomes for refugee women: a population-based cohort study. Diabet Med. 2017;34(11):1608–14. https://doi.org/10.1111/dme.13440.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Lili Yuen, Vincent W. Wong, and David Simmons declare they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Diabetes and Pregnancy
Rights and permissions
About this article
Cite this article
Yuen, L., Wong, V.W. & Simmons, D. Ethnic Disparities in Gestational Diabetes. Curr Diab Rep 18, 68 (2018). https://doi.org/10.1007/s11892-018-1040-2
Published:
DOI: https://doi.org/10.1007/s11892-018-1040-2