Abstract
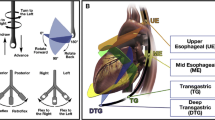
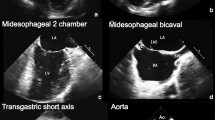
Bedside limited echocardiography, or focused cardiac ultrasound, continues to gain popularity in many emergency rooms, intensive care units, and operating rooms as a rapid method of assessing unstable patients. Effective monitoring of cardiovascular function in conditions like cardiac arrest or near-arrest is the crucial step to guide successful resuscitative efforts. Transesophageal echocardiography (TEE) has emerged as one of the preferred cardiac diagnostic and monitoring modalities in the intraoperative setting due to the fact that it is less invasive than many other monitors, is immediately accessible, and allows for continuous real-time monitoring of cardiac function. However, the minimum training requirements needed for the anesthesia provider to obtain the competency, knowledge, and skills for basic certification in perioperative TEE far exceed those developed for other medical specialties. We believe there is an urgent need to develop (1) practical guidelines for emergent perioperative TEE use for anesthesiologists and (2) a requisite educational curriculum to teach the basic skills necessary to aid in the diagnosis and treatment of cardiac arrest or near-arrest scenarios. The measures elucidated in this report summarize the efforts of the Department of Anesthesiology at the University of Florida in establishing the necessary steps to make this process not only practical, but accessible to all trainees.We hope that these collective efforts will provide more trainees the confidence in utilizing TEE to aid in establishing a diagnosis in critical situations.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Scalea TM, Rodriguez A, Chiu WC, Brenneman FD, Fallon WF Jr, Kato K, McKenney MG, Nerlich ML, Ochsner MG, Yoshii H. Focused Assessment with Sonography for Trauma (FAST): results from an international consensus conference. J Trauma 1999; 46(3): 466–472
Pershad J, Myers S, Plouman C, Rosson C, Elam K, Wan J, Chin T. Bedside limited echocardiography by the emergency physician is accurate during evaluation of the critically ill patient. Pediatrics 2004; 114(6): e667–e671
Melamed R, Hanovich S, Shapiro R, Sprenkle M, Ulstad V, Leatherman J. Limited bedside echocardiography performed in the MICU. Chest 2005; 128: 207S
Labovitz AJ, Noble VE, Bierig M, Goldstein SA, Jones R, Kort S, Porter TR, Spencer KT, Tayal VS, Wei K. Focused cardiac ultrasound in the emergent setting: a consensus statement of the American Society of Echocardiography and American College of Emergency Physicians. J Am Soc Echocardiogr 2010; 23(12): 1225–1230
ACCP Certificate of Completion Critical Care Ultrasonography Program. Available at: http://www.chestnet.org/accp/accp-certificate-completion-critical-care-ultrasonography-program (Accessed on January 9, 2012)
Lucas BP, Candotti C, Margeta B, Evans AT, Mba B, Baru J, Asbury JK, Asmar A, Kumapley R, Patel M, Borkowsky S, Fung S, Charles-Damte M. Diagnostic accuracy of hospitalist-performed hand-carried ultrasound echocardiography after a brief training program. J Hosp Med 2009; 4(6): 340–349
Razi R, Estrada JR, Doll J, Spencer KT. Bedside hand-carried ultrasound by internal medicine residents versus traditional clinical assessment for the identification of systolic dysfunction in patients admitted with decompensated heart failure. J Am Soc Echocardiogr 2011; 24(12): 1319–1324
Neumar RW, Otto CW, Link MS, Kronick SL, Shuster M, Callaway CW, Kudenchuk PJ, Ornato JP, McNally B, Silvers SM, Passman RS, White RD, Hess EP, Tang W, Davis D, Sinz E, Morrison LJ. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122(18 Suppl 3): S729–S767
Weiss SJ, Savino J. The time is ripe. J Cardiothorac Vasc Anesth 2006; 20(6): 765–767
Lin T, Chen Y, Lu C, Wang M. Use of transoesophageal echocardiography during cardiac arrest in patients undergoing elective non-cardiac surgery. Br J Anaesth 2006; 96(2): 167–170
Goins KM, May JM, Hucklenbruch C, Littlewood KE, Groves DS. Unexpected cardiovascular collapse from massive air embolism during endoscopic retrograde cholangiopancreatography. Acta Anaesthesiol Scand 2010; 54(3): 385–388
Song JE, Chun DH, Shin JH, Park C, Lee JY. Pulmonary thromboembolism after tourniquet inflation under spinal anesthesia: a case report. Korean J Anesthesiol 2010; 59(Suppl): S82–S85
Newkirk L, Vater Y, Oxorn D, Mulligan M, Conrad E. Intraoperative TEE for the management of pulmonary tumour embolism during chondroblastic osteosarcoma resection. Can J Anaesth 2003; 50(9): 886–890
Ebner FM, Paul A, Peters J, Hartmann M. Venous air embolism and intracardiac thrombus after pressurized fibrin glue during liver surgery. Br J Anaesth 2011; 106(2): 180–182
Wei J, Yang HS, Tsai SK, Hsiung MC, Chang CY, Ou CH, Chang YC, Lee KC, Sue SH, Chou YP. Emergent bedside real-time threedimensional transesophageal echocardiography in a patient with cardiac arrest following a caesarean section. Eur J Echocardiogr 2011; 12(3): E16
Blaivas M. Transesophageal echocardiography during cardiopulmonary arrest in the emergency department. Resuscitation 2008; 78(2): 135–140
Patteril M, Swaminathan M. Pro: intraoperative transesophageal echocardiography is of utility in patients at high risk of adverse cardiac events undergoing noncardiac surgery. J Cardiothorac Vasc Anesth 2004; 18(1): 107–109
Schulmeyer MC, Santelices E, Vega R, Schmied S. Impact of intraoperative transesophageal echocardiography during noncardiac surgery. J Cardiothorac Vasc Anesth 2006; 20(6): 768–771
Younker D, Reeves-Viets JL, Gopinath SP, Tsai PI, Moon TL, Cuzick LM. Cardiac arrest upon induction of general anesthesia: transesophageal echocardiography-assisted diagnosis of impending paradoxical embolus. Anesthesiology 2009; 111(3): 679–680
Vanden Hoek TL, Morrison LJ, Shuster M, Donnino M, Sinz E, Lavonas EJ, Jeejeebhoy FM, Gabrielli A. Part 12: cardiac arrest in special situations: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122(18 Suppl 3): S829–S861
Collard CD. Con: intraoperative transesophageal echocardiography is not of utility in patients at high risk of adverse cardiac events undergoing noncardiac surgery. J Cardiothorac Vasc Anesth 2004; 18(1): 110–111
Piercy M, McNicol L, Dinh DT, Story DA, Smith JA. Major complications related to the use of transesophageal echocardiography in cardiac surgery. J Cardiothorac Vasc Anesth 2009; 23(1): 62–65
Hilberath JN, Oakes DA, Shernan SK, Bulwer BE, D’Ambra MN, Eltzschig HK. Safety of transesophageal echocardiography. J Am Soc Echocardiogr 2010; 23(11): 1115–1127, quiz 1220–1221
Davis-Gomez N, Perkins GD. Safety of transoesophageal echocardiography during cardiac arrest. Resuscitation 2008; 79(1): 175
van der Wouw PA, Koster RW, Delemarre BJ, de Vos R, Lampe-Schoenmaeckers AJ, Lie KI. Diagnostic accuracy of transesophageal echocardiography during cardiopulmonary resuscitation. J Am Coll Cardiol 1997; 30(3): 780–783
Aronson S, Butler A, Subhiyah R, Buckingham RE Jr, Cahalan MK, Konstandt S, Mark J, Ramsay J, Savage R, Savino J, Shanewise JS, Smith J, Thys D. Development and analysis of a new certifying examination in perioperative transesophageal echocardiography. Anesth Analg 2002; 95(6): 1476–1482
Memtsoudis SG, Rosenberger P, Loffler M, Eltzschig HK, Mizuguchi A, Shernan SK, Fox JA. The usefulness of transesophageal echocardiography during intraoperative cardiac arrest in noncardiac surgery. Anesth Analg 2006; 102(6): 1653–1657
Hoole SP, Falter F. Evaluation of hypoxemic patients with transesophageal echocardiography. Crit Care Med 2007; 35(8 Suppl): S408–S413
Vellayappan U, Attias MD, Shulman MS. Paradoxical embolization by amniotic fluid seen on the transesophageal echocardiography. Anesth Analg 2009; 108(4): 1110–1112
Karski JM. Transesophageal echocardiography in the intensive care unit. Semin Cardiothorac Vasc Anesth 2006; 10(2): 162–166
The National Board of Echocardiography. Exams & Certifications. Available at: http://www.echoboards.org (Accessed on January 9, 2012)
American College of Emergency Physicians. Policy Statement. Emergency Ultrasound Guidelines. Approved October 2008. Appendix 3-Emergency Medicine Residency Ultrasound Education Guidelines. Available at: http://www.aium.org/publications/guidelines/acepGuidelines.pdf (Accessed on June 29, 2012)
Shanewise JS, Cheung AT, Aronson S, Stewart WJ, Weiss RL, Mark JB, Savage RM, Sears-Rogan P, Mathew JP, Quiñones MA, Cahalan MK, Savino JS. ASE/SCA guidelines for performing a comprehensive intraoperative multiplane transesophageal echocardiography examination: recommendations of the American Society of Echocardiography Council for Intraoperative Echocardiography and the Society of Cardiovascular Anesthesiologists Task Force for Certification in Perioperative Transesophageal Echocardiography. Anesth Analg 1999; 89(4): 870–884
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Peng, Y.G., Janelle, G.M. Emergent limited perioperative transesophageal echocardiography: should new guidelines exist for limited echocardiography training for anesthesiologists?. Front. Med. 6, 332–337 (2012). https://doi.org/10.1007/s11684-012-0212-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11684-012-0212-8