Abstract
Purpose
Immunotherapy, such as checkpoint inhibitors against anti-programmed death-ligand 1 (PD-L1), has not been successful in treating patients with pancreatic ductal adenocarcinoma (PDAC). Tumor-associated macrophages (TAMs), myeloid-derived suppressor cells (MDSCs), dendritic cells (DCs), and the TGF-β cytokine are critical in anti-cancer immunity. We hypothesized that TGF-β enhances the immunosuppressive effects of TAM, MDSC, and DC presence in tumors.
Methods
Using a murine PDAC cell line derived from a genetically engineered mouse model, we orthotopically implanted treated cells plus drug embedded in Matrigel into immunocompetent mice. Treatments included saline control, TGF-β1, or a TGF-β receptor 1 small molecule inhibitor, galunisertib. We investigated TAM, MDSC, DC, and TAM PD-L1 expression with flow cytometry in tumors. Separately, we used the TIMER2.0 database to analyze TAM and PD-L1 gene expression in human PDAC tumors in TCGA database.
Results
TGF-β did not alter MDSC or DC frequencies in the primary tumors. However, in PDAC metastases to the liver, TGF-β decreased the proportion of MDSCs (P=0.022) and DCs (P=0.005). TGF-β significantly increased the percent of high PD-L1 expressing TAMs (32 ± 6 % vs. 12 ± 5%, P=0.013) but not the proportion of TAMs in primary and metastatic tumors. TAM PD-L1 gene expression in TCGA PDAC database was significantly correlated with tgb1 and tgfbr1 gene expression (P<0.01).
Conclusions
TGF-β is important in PDAC anti-tumor immunity, demonstrating context-dependent impact on immune cells. TGF-β has an overall immunosuppressive effect mediated by TAM PD-L1 expression and decreased presence of DCs. Future investigations will focus on enhancing anti-cancer immune effects of TGF-β receptor inhibition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Approximately 10% of patients diagnosed with pancreatic ductal adenocarcinoma (PDAC) will be alive 5 years after diagnosis,1 and PDAC is projected to become the second leading cause of cancer-related deaths in the next decade.2 The two current mainstay chemotherapies—FOLFIRINOX (5-FU/leucovorin/oxaliplatin/irinotecan) or gemcitabine/paclitaxel—have limited efficacy with significant adverse effects3,4,5 and nearly universal development of therapeutic resistance.6, 7 A glaring failure in the development of PDAC therapeutics remains the lack of targeted therapies that have changed the landscape in many other cancers with small molecule inhibitors and immunotherapy.8,9,10 Checkpoint inhibitors, perhaps the most effective immune-based approach for targeted therapies for cancer, have not resulted in success for patients with PDAC.11
Over the last decade, immunotherapy has revolutionized the treatment of many malignancies.12 Specifically, the family of drugs called immune checkpoint inhibitors targeting cytotoxic T lymphocyte–associated protein 4 (anti-CTLA-4), the programmed cell death 1 receptor, and its ligand programmed cell death-ligand 1 (anti-PD-1 and anti-PD-L1, respectively) have emerged as frontline therapy for advanced cancers such as melanoma, non-small cell lung cancer, renal cell, and bladder cancer.13 Since FDA approval of the first checkpoint inhibitor ipilimumab for treatment of metastatic melanoma, 14 the number of immunotherapies has increased significantly.15 Despite some early promise for immune therapy against PDAC, the overall enthusiasm has waned due to overall ineffectiveness.16,17,18,19,20,21,22
Transforming growth factor-beta (TGF-β) has been shown to play a dual role in the development of PDAC and can act both as a promoter and tumor suppressor depending on the context.23,24,25 TGF-β is a protein involved in numerous normal and abnormal cellular process 10, 24, 26 and ubiquitous in PDAC tumors.10, 24,25,26,27,28,29 TGF-β demonstrates a striking paradox as a tumor suppressor in patients with primary-site PDAC (i.e., non-metastatic) but a tumor promoter in metastatic PDAC.23, 25, 28,29,30,31 The TGF-β receptor (TGFβR) family 32, 33 is a large family of cell membrane proteins that perform intracellular SMAD protein phosphorylation upon activation that require an extracellular ligand. While there are 3 gene products for receptors specific to TGF-β, tgfbr1, tgfbr2, and tgfbr3, type 1 and type 2 TGFβR represent the most common and biologically relevant TGFβRs composed of gene products of tgfbr1 and tgfbr2. Recent work by Zhong et al.34 reported that TGF-β receptor superfamily can induce p38MAPK, which is the first step of non-SMAD TGF-β signaling as demonstrated by our group and others.25, 35 Published data has also demonstrated that TGFβR inhibition (TGFβRi) still allows for phosphorylation of p38MAPK and subsequent non-SMAD intracellular signaling36 implying that in some cells, it may be possible to induce intracellular molecular signaling while blocking a receptor.
There are a number of immune cells found in the PDAC tumor microenvironment (TME) as well as a number of mechanisms in which PDAC is resistant to immunotherapy including through TGF-β signaling.37,38,39,40 However, in many cases, there are some tumors that do in fact elicit a T cell–mediated anti-tumor response, suggesting a potential mechanism to target.37 The immune TME is composed of tumor-associated macrophages (TAMs) which are frequently found in close proximity to PDAC cells.38, 41 In addition, recent work by Hegde et al. found that a paucity of dendritic cells (DCs) in the PDAC TME inhibited potent anti-tumor immune activity as well.42 Myeloid-derived suppressor cells (MDSCs) are a group of cells often found in the PDAC TME43, 44 consisting of myeloid-MDSC (M-MDSC) and granulocyte (polymorphonuclear)-MDSC (PMN-MDSC). Interestingly, the presence of MDSC in the PDAC TME is almost mutually exclusive with the presence of tumor-infiltrating lymphocytes44, suggesting a potential mechanism for the failure of T cell lymphocyte–based immune therapy.
Given the near ubiquitous presence of TGF-β in the PDAC TME and its well-known role in modulating normal and abnormal immune cell function, we theorized that TGF-β may affect the immune TME by impacting the proportion of immune cells as well as activation of TAMs, a central immune cell mediator. We utilized a model to measure the direct immune cell effects of therapy in the TME rather than systemic therapy to understand early tumor biology. We hypothesized that TGF-β enhances the immunosuppressive effects of TAM, MDSC, and DC presence in tumors.
Methods
All animal procedures were approved by the Institutional Animal Care and Use Committee at the University of Tennessee Health Science Center in accordance with the American Association for Accreditation of Laboratory Animal Care and the National Institutes of Health (NIH) Guide for the Care and Use of Laboratory Animals.
Mice and Cell Lines
C57BL/6J “B6” mice were purchased from The Jackson Laboratory (Bar Harbor, ME) and implanted with 106 cells from a syngeneic murine PDAC cell line derived from KPC mice. KPC (KrasLSL.G12D/+; p53R172H/+; PdxCretg/+, authenticated by LabCorp Cell Line Authentication Service via short tandem repeat (STR) profiling, Burlington, NC) is a genetically engineered mouse model that spontaneously forms murine PDAC similar to human PDAC with KRAS and TP53 mutations selective induced in the pancreas. By orthotopically implanting KPC cells into syngeneic mice (N=5 per treatment group), we can ensure an intact immune system and control the identical tumor inoculum at the same time. The KPC cell line was maintained in standard conditions in DMEM media with 10% fetal bovine serum and 1% penicillin-streptomycin.
Orthotopic Tumor Implantation and Treatment
KPC cells were pre-treated in vitro with the assigned treatment for 24 h and orthotopically implanted (106 cells/50μL; 1:1, v/v with Matrigel with the assigned treatment embedded within the Matrigel in order to limit off target effects of treatment and sustain treatment in the PDAC TME). Orthotopic implantation was performed as previously described.29 Briefly, 50,000 KPC cells (provided as a kind gift from Dr. Williams Hawkins at Washington University in St. Louis) were implanted into the pancreatic tail of C57BL/6J mice (The Jackson Laboratory, Bar Harbor, ME) according to our approved protocol (University of Tennessee Health Science Center Institutional Animal Care and Use Committee) after induction of general anesthesia. A left abdominal incision was made; the spleen was identified and brought into the field which also brought the pancreas into the field. A total of 50 μL of Matrigel was injected into the pancreas with the KPC cells and treatment (see below). The spleen and pancreas were placed back into their anatomic position. The abdominal muscle was closed with absorbable suture. The skin was closed with titanium clips (which were removed after 10 days). Mice were placed into their cage on a warming pad until fully awake. Groups were in replicates of 5. All experiments were performed in accordance with relevant guidelines and regulations as approved by UTHSC.
The treatments were equal volume of PBS control, recombinant murine TGF-β1 (10 ng/mL, BioLegend, San Diego, CA ), or galunisertib (10 μM, Selleckchem/Thermo Fisher, Pittsburgh, PA) as indicated. The cell lines were cultured and maintained in complete media with 10% fetal bovine serum (FBS) and penicillin-streptomycin at 37°C with 5% CO2 as recommended by the supplier. Two weeks after implantation, tumors were collected from the pancreas and liver and analyzed as below. One to two mice per group did not develop tumors. We verified that TGF-β1 treatment activated the SMAD pathways with phosphorylation of SMAD2 (Ser465, Ser467) as measured by immunohistochemistry of the tumors (Thermo Fisher) at sacrifice (Supplemental Figure 1). GAL treatment diminished endogenous TGF-β homodimer expression as measured by immunohistochemistry of the tumors at sacrifice (Supplemental Figure 2).
Flow Cytometric Analysis of Immune Cells in TME
Tumor single cell suspensions were obtained using Mouse Tumor Dissociation Kit (Miltenyi Biotec). Single cell suspensions were incubated with Ghost dye (Tonbo, San Diego, CA) to assess cell viability, FcR-blocking reagent (Tonbo), and fluorescently labeled antibodies and incubated for 30 min as previously described45. Controls consisted of single color UltraComp Beads (Invitrogen)–positive and Fluorescence Minus One (FMO)–negative controls. Data were acquired using high-performance Bio-Rad ZE5 flow cytometer (Bio-Rad) and analyzed using the flow cytometry analysis program FlowJo (Treestar/BD Bio Sciences, Ashland, OR). Gating strategy for immune cell populations is detailed in Fig. 1.
Experimental design and TME immune cell gating strategy. A KPC cells were treated with PBS control, galunisertib (GAL), TGF-β, or combined TGF-β + GAL. B Single cell suspensions were created by harvesting tumors from mice and underwent flow cytometric analysis for quantification of immune cells in the TME. The gating strategy identified PDAC myeloid-derived suppressor cells (MDSCs), tumor-associated macrophages (TAMs), and dendritic cells (DCs)
After gating total cells by plotting forward scatter versus side scatter areas, single cells by plotting side scatter height versus side scatter area, and live CD45+ cells by plotting CD45 versus Ghost viability dye, immune cells were gated as follows: myeloid cells (CD45+ CD11b+); M-MDSC (CD45+ CD11b+ Ly6C-high Ly6G-); PMN-MDSC (CD45+ CD11b+ Ly6C-low Ly6G+); macrophages (TAM) (CD45+ CD11b+ Ly6C- Ly6G- F4/80+); and dendritic cells (DCs) (CD45-high CD11b + CD11c+). Given the importance of PD-L1 on PDAC TAMs38, 46, the proportion of TAMs with high expression of PD-L1 was determined (CD274) thereafter.
Validation of Gene Expression of PDAC TAMs With the TIMER Data Set
Tumor IMmune Estimation Resource (TIMER2.0), a comprehensive tool to explore tumor immunological, clinical, and genomic features across diverse cancer types (https://cistrome.shinyapps.io/timer/),47 was used to analyze TGF-β and TAM gene correlations. The TIMER database48, 49 includes more than ten thousand samples across thirty-two cancer types from The Cancer Genome Atlas (TCGA) and applies an established algorithm to estimate the abundance of immune infiltrates from their gene expression profiles. In order to explore the relationship between TGF-β, TAMs, and PD-L1 in pancreatic cancer, the TIMER database was interrogated to find gene correlations between TGFB1, TGFBR1, and TAM genes (CD68, CD163, CD206) and CD274 (PD-L1) in human PDAC samples from TCGA.
Results
Galunisertib Abrogates Differences in DC Frequencies between Metastatic (Liver) and Primary (Pancreas) PDAC Tumors in Mice
DCs are important for an effective tumor-specific T cell response.50 Dysregulation of DCs occurs through a number of mechanisms, including decreased levels of IL-6, that lead to ineffective antigen presentation among other immunologic defects.51 Since loss of DCs would allow tumor growth, we investigated proportion of DCs in the TME. We found that DCs, as a percent of CD45+ cells in the TME, are less common in metastatic PDAC in the liver compared to primary tumors in the pancreas (P=0.0063, Fig. 2). TGF-β exacerbates the targeting of DCs with greater DCs in primary pancreatic tumors compared to liver metastases (P=0.0209, Fig. 2) which is not ablated when TGF-β is co-administered with GAL. DCs in the liver and pancreas were similar when GAL treatment occurred alone (Fig. 2).
Galunisertib (GAL) abrogates differences in dendritic cell (DC) content between metastatic (liver) and primary (pancreas) PDAC tumors in mice. DC frequencies were calculated as a percent of CD45+ cells in the TME in mice treated with control (PBS), TGF-β receptor small molecule inhibitor GAL, TGFβ, or combined TGF β + GAL. Median and range are shown as violin plot. Two-way ANOVA with Fisher’s least square difference (LSD) was used to determine significance of < 0.05. P values are indicated in the figure. N=3–4 mice per treatment
TGF-β Increases PMN-Myeloid-Derived Suppressor Cell (PMN-MDSC) Frequencies in Primary PDAC but not Metastatic Tumors
PMN-MDSCs have a similar frequency (percent of CD45+ cells in the TME) in primary PDAC and metastases to the liver (Fig. 3). GAL had no effect on the density of PMN-MDSCs in these tumors. TGF-β increased the density of PMN-MDSCs in the pancreas compared to PBS-treated mice, while significantly decreased the density in the metastases (P=0.0493, Fig. 3). Upon combined treatment with TGF-β and GAL, the effect of TGF-β was maintained and was not blunted by TGF-β1 receptor inhibition (P=0.0336).
TGF-β significantly increases PMN-myeloid-derived suppressor cell (PMN-MDSC) density differences between metastatic (liver) and primary (pancreas) PDAC tumors which could not be abrogated with inhibition of TGFβR1. PMN-MDSCs were calculated as a percent of CD45+ cells in the TME in mice treated with control (PBS), TGF-β receptor small molecule inhibitor galunisertib (GAL), TGF-β, or combined TGF-β + GAL. Median and range are shown as violin plot. Two-way ANOVA with Fisher’s least square difference (LSD) was used to determine significance of < 0.05. P values are indicated in the figure. N=3–4 mice per treatment
Primary Pancreatic PDAC Tumors Contain Greater M-MDSC than Liver Metastatic Tumors
Metastatic liver PDAC tumors had fewer M-MDSCs compared to pancreatic tumors (P=0.0221). Overall, GAL was not associated with changes in M-MDSC proportions (P>0.05), while this difference was abrogated by TGF-β treatment but not by GAL treatment (P=0.0198, Fig. 4). Combined treatment with TGF-β + GAL decreased the proportion of M-MDSCs (P=0.0075) without a difference between primary-site pancreatic and metastatic liver PDAC tumors.
Primary PDAC tumors (pancreas) contain greater M-MDSC which may be downregulated by TGF-β. The percent of M-MDSCs in the pancreatic tumor or liver metastases is presented as % of CD45+ cells in mice treated with control (PBS), TGF-β receptor small molecule inhibitor Galunisertib (GAL), TGF-β, or combined TGF-β + GAL. Median and range are shown as violin plot. Two-way ANOVA with Fisher’s least square difference (LSD) was used to determine significance of < 0.05. P values are indicated in the figure. N=3–4 mice per treatment
The Proportion of TAMs Did not Vary with Treatment or Location
Primary and metastatic tumors did not have significant differences in the proportion of TAMs (Fig. 5A). TGF-β increased overall TAM PD-L1 surface expression in PDAC tumors, suggesting a more immunosuppressed phenotype (P=0.013, Fig. 5B) which was not found in the other treatment groups.
The proportion of TAMs did not vary with treatment or location. A The percent of TAMs in the pancreatic tumor or liver metastases is presented as % of CD45+ cells in mice treated with control (PBS), TGF-β receptor small molecule inhibitor galunisertib (GAL), TGF-β, or combined TGF-β + GAL. Median and range are shown as violin plot. B Pancreatic tumors treated with TGF-β showed higher percentage of PD-L1–positive TAMs compared to PBS-treated mice
TGFB1 and TGFBR1 Gene Expression Positively Correlate with TAM Signature and PD-L1 (CD274) Gene Expression in Human PDAC Samples from TCGA
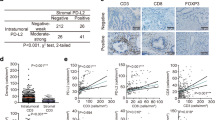
Since TGF-β ultimately regulates gene expression, we investigated TAM gene expression signature associated with gene expression of TGF-β and its receptor. Using the Tumor IMmune Estimation Resource (TIMER, https://cistrome.shinyapps.io/timer/) version 2.0, we identified that genes comprising the TAM signature (CD68-macrophage marker, CD163-scavenger receptor, or CD206-mannose receptor) significantly correlated with the expression of TGFB1 or TGFBR1 in TAMs (Fig. 6). In addition, TGFB1 gene expression significantly correlated with tumoral CD274/PD-L1 (r = 0.28, P<0.0002, Fig. 6) as well as each gene in the TAM signature (each correlation r>0.26, P<.0004, Fig. 6). Finally, TGFBR1 gene expression also significantly correlated with CD274/PD-L1 (r = 0.45, P<0.0001, Fig. 6) as well as each gene comprising the TAM signature (each correlation r >0.36, P<.0001, Fig. 6).
TGFB1 and TGFBR1 gene expression positively correlates with markers of TAMs and PD-L1 (CD274) gene expression in human PDAC samples from TCGA. Using Tumor IMmune Estimation Resource (TIMER, https://cistrome.shinyapps.io/timer/) informatics, expression of genes from the TAM signature (CD68/CD163/CD206) correlate to expression of TGFB1 and TGFBR1
Discussion
A complex set of immunosuppressive cells in the PDAC TME are likely the primary diver for the failure of immunotherapy in patients.52 Among the many cells in the immune TME, TAMs represent a fundamental cell in the immune TME that affects not only other immune cells but also cancer-associated fibroblasts (CAFs) that serve as regulators of the immune milieu as well.40 Both TAMs and CAF may be sources of TGF-β.46, 53,54,55
Given the ubiquitous presence of the TGF-β cytokine in the PDAC TME, the ongoing clinical trials designed to harness anti-TGF-β receptor are exciting.56 However, from our work and others, it is apparent that off-target effects of TGFβRi may undermine this therapy if not addressed a priori. For example, a recent phase 1 clinical trial found that gemcitabine plus GAL was associated with a 43% rate of stable disease, but the median progression-free survival was only 64 days suggesting limited clinical utility.57 Given the broad effect of TGF-β on multiple types of immune cells,24 it is not surprising that gemcitabine plus GAL has limited efficacy in isolation. Aberrant activation of Akt, p38MAPK, and ERK in PDAC tumors, especially in the setting of KRAS or SMAD4 mutation, contributes to the confusion in understanding non-SMAD (non-canonical) TGF-β signaling.24, 25, 32, 33
In order to identify potential mechanisms of immune cell escape from TGFβRi, we studied critical changes between metastatic-site and primary-site PDAC in an immunocompetent murine model using pre-treatment to prime cells and treatments embedded in the TME. Unlike other scenarios where the whole mouse is treated, we focused our treatments in the PDAC TME by embedding the treatment in Matrigel and collecting tumors after 2 weeks—relatively early in tumorigenesis.
DC tissue content suggests that DCs are more prevalent in the primary pancreatic tumor site which is dependent upon TGF-β signaling. Given the antigen presentation function of DCs, we theorized that decreased presence of DCs would impair effective anti-tumor immunity leading to accelerated tumor growth. Namely, fewer DCs would be expected in the liver compared to the pancreas after orthotopic implantation which was in fact found (Fig. 2, P<0.05). However, upon GAL treatment, we found that the difference between DC proportions in each site dramatically decreased but was exacerbated by TGF-β treatment. The lack of DCs would be expected to allow for metastatic (liver) tumor growth. Given the ability for DCs to activate cytotoxic cells,58 the paucity of DCs in the liver may be one mechanism by which PDAC and TGF-β induce immunosuppression.
The importance of MDSCs in regulating PDAC anti-tumor immunity is an area of growing research.40, 59 Of the two subtypes of MDSC, PMN-MDSC are the most prevalent subtype in both pancreas and liver at about 20–50% of CD45+ cells compared to M-MDSCs, comprising just 5–15% of CD45+ cells, as is similar to other cancers.60 While both types of MDSCs are highly immunosuppressive, the effects of PMN-MDSC are more tumor promotive.60 In control mice, there is not a significant difference in PMN-MDSC content. TGF-β increases pancreatic tumor PMN-MDSC content relative to liver metastasis (P=0.0087). This differential expression was not ablated by the addition of GAL to TGF-β therapy (P=0.0336). Like DCs, pancreas primary tumor has significantly greater M-MDSC compared to liver metastases. TGF-β reduced this content and this reduction was not reversed by TGF-β + GAL coadministration.
Recently, Mota Reyes et al. found that neoadjuvant chemotherapy in PDAC patients remodeled the pancreatic TME by decreasing the proportion of MDSC cells, suggesting transition to an anti-cancer, inflammatory TME.61 Interestingly, this was found in multiple types of chemotherapeutic regimens, suggesting a biologic effect, not therapy-specific phenomenon. While we did not identify any changes in M-MDSC, we did unexpectedly find that TGF-β decreased the proportion of MDSC in the liver (metastases) but not the pancreas compared to control-treated mice. This difference was maintained with TGF-β and GAL co-treatment. This data, in isolation, could suggest that reduced immunosuppression was ongoing in liver metastases. However, the same tumors also had lower levels of DCs. Taken together, our findings suggest a complex picture of immune modulation where the balance is likely still favoring overall immune suppression.
We next investigated the effects of TGF-β and GAL on the proportion of TAMs and expression of PD-L1 on them. Recent work by Strauss et al demonstrated that selective deletion of PD-L1 from TAMs and M-MDSCs differentiated to TAMs resulted in enhanced anti-tumor immune activity.59 Our previous work and others have found that the TAM-TGF-β axis is critical for tumor immunosuppressive phenotype in PDAC.22, 28, 29, 46 Here, we did not identify significant differences between the proportion of TAMs in pancreas or liver tumors. Likewise, treatments did not significantly alter the frequencies in total TAMs. However, we found that across both disease sites, the number of PD-L1 expressing TAMs was significantly increased with TGF-β administration compared to controls (Fig. 5B). Increased PD-L1 expression would be expected to directly induce an immunosuppressive TME via induction of an exhausted phenotype in cytotoxic T cells and DC dysfunction.6, 22, 40, 52, 62 This observation in conjunction with the reduction in DCs in liver metastases implicates a mechanism of action for TGF-β–induced loss of immune cell surveillance.
Based on the results found in the mouse model, we investigated gene correlations in the TCGA data set. Unlike genetic expression22, 38 markers for DC and MDSC which are not well characterized, gene expression markers of TAMs are much better defined. We identified that gene expression of early markers of TGF-β signaling (the receptor, specifically) are well-correlated with PD-L1 expression in the tumors as well as markers of TAM phenotype (Fig. 6), demonstrating activation of a TAM immunosuppressive gene expression profile due to TGF-β receptor activation. While this data is only correlative, it is supportive that early changes in the immune TME take place due to TGF-β signaling and these mechanisms ensue through tumor progression. It is supportive that this interaction induces a novel cellular program with long-term effects on immune cells in both the primary- and metastatic-site immune TME.
Our novel finding that TGF-β both exacerbates the differences in the proportion of DCs that present antigen in metastatic PDAC and increases TAMs with high PD-L1 expression implies an immune TME is much more complex than our model describes. It supports that that TGF-β paradox exists as a balance between inflammatory, anti-tumor immune TME (i.e., loss of MDSCs), and immunosuppressed, pro-cancer immune TME (i.e., increased PD-L1+ TAMs and loss of DCs). Given that TGF-β is released from PDACs and CAFs in the TME, it is likely that the TGF-β paradox is a balance between the quantity of TGF-β and the proportion and function of immune cells in the TME.
There are a number of limitations to our work. While the immunocompetent mouse implanted with murine PDAC cells model recapitulates the human PDAC TME well, it is only a model, and in this case, we focused on the early effects of molecules in the TME, not the host. Patient-derived primary and metastatic samples would be more advantageous for us to examine the TME and TGF-β concentrations directly, but since PDAC metastasectomy is not routinely performed, there are limited patient-derived specimens available with a complete immune TME. Thus, we utilized a large publicly available database to interrogate existing gene expression and immune cell populations. Importantly, TGF-β and its receptor expression significantly correlated with TAMs in human PDAC samples. Likewise, both TGF-β and its receptor also correlated with the potent immune checkpoint ligand PD-L1, which was in line with findings from our KPC transplants treated with TGF-β. Therefore, using the power of informatics in the large TCGA database, we provide supportive translational evidence of the potential for TGF-β in creating immunosuppressive, dysfunctional TAMs. The specific role of TGF-β and its receptor in TAM immunosuppression in the TME is under active investigation. Reprogramming the myeloid compartment in PDAC and other cancers is an area of intense research.12 Finally, we focused our work on liver metastases as these were the most common in our model (and in patients). However, among other sites, patients have peritoneal and lung metastases that are clinically important, molecular unique,3 but not well recapitulated in our system.
Overall, TGF-β which is highly present in TME drives greater accumulation of DCs in pancreatic tumors, but this is potentially overshadowed by great increases in PMN-MDSCs. Inhibition of the TGFβR did not improve this differential, thus emphasizing that both anti-tumor and immunosuppressive immune cells must be examined in the TME to best understand how TGF-β or inhibition of this pathway impacts the tumor immune TME.
Conclusion
Anti-tumor immune cells, such as DCs, and pro-tumor TAMs are detected in PDAC tumors in the pancreas and liver. While TAMs do not display dynamic regulation between tissue sites or with varied therapies targeting the TGF-β pathway, our results suggest that an immunosuppressive effect mediated by PD-L1+ TAMs may be initiated by TGF-β. Furthermore, DCs are highly variably regulated between sites and in response to therapies. DCs are significantly greater in pancreatic site tumors compared to liver metastases; this difference is lost with GAL treatment. Interestingly, TGF-β administration parallels control-treated mice, wherein the differential between pancreatic site and liver metastases is significant with nearly 5-fold greater DCs in tumors in the pancreas compared to the liver. Of note, this difference cannot be reversed with dual TGF-β + GAL therapy.
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2018. CA Cancer J Clin. 2018;68(1):7-30.
Giovannetti E, van der Borden CL, Frampton AE, Ali A, Firuzi O, Peters GJ. Never let it go: Stopping key mechanisms underlying metastasis to fight pancreatic cancer. Semin Cancer Biol. 2017;44:43-59.
Ferguson MD, Dong L, Wan J, et al. Molecular Alterations Associated with DNA Repair in Pancreatic Adenocarcinoma Are Associated with Sites of Recurrence. J Gastrointest Cancer. 2018.
Von Hoff DD, Ervin T, Arena FP, et al. Increased survival in pancreatic cancer with nab-paclitaxel plus gemcitabine. N Engl J Med. 2013;369(18):1691-1703.
Conroy T, Desseigne F, Ychou M, et al. FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. N Engl J Med. 2011;364(19):1817-1825.
Huang H, Brekken RA. Recent advances in understanding cancer-associated fibroblasts in pancreatic cancer. Am J Physiol Cell Physiol. 2020.
Neumann CCM, von Horschelmann E, Reutzel-Selke A, et al. Tumor-stromal cross-talk modulating the therapeutic response in pancreatic cancer. Hepatobiliary Pancreat Dis Int. 2018;17(5):461-472.
Duraiswamy J, Freeman GJ, Coukos G. Therapeutic PD-1 pathway blockade augments with other modalities of immunotherapy T-cell function to prevent immune decline in ovarian cancer. Cancer Res. 2013;73(23):6900-6912.
Gajewski TF, Corrales L, Williams J, Horton B, Sivan A, Spranger S. Cancer Immunotherapy Targets Based on Understanding the T Cell-Inflamed Versus Non-T Cell-Inflamed Tumor Microenvironment. Adv Exp Med Biol. 2017;1036:19-31.
de Gramont A, Faivre S, Raymond E. Novel TGF-beta inhibitors ready for prime time in onco-immunology. Oncoimmunology. 2017;6(1):e1257453.
Feng M, Xiong G, Cao Z, et al. PD-1/PD-L1 and immunotherapy for pancreatic cancer. Cancer Lett. 2017;407:57-65.
Chaib M, Chauhan SC, Makowski L. Friend or Foe? Recent Strategies to Target Myeloid Cells in Cancer. Front Cell Dev Biol. 2020;8:351.
Ribas A, Wolchok JD. Cancer immunotherapy using checkpoint blockade. Science. 2018;359(6382):1350-1355.
Hodi FS, O'Day SJ, McDermott DF, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010;363(8):711-723.
Tang J, Yu JX, Hubbard-Lucey VM, Neftelinov ST, Hodge JP, Lin Y. Trial watch: The clinical trial landscape for PD1/PDL1 immune checkpoint inhibitors. Nat Rev Drug Discov. 2018;17(12):854-855.
Royal RE, Levy C, Turner K, et al. Phase 2 trial of single agent Ipilimumab (anti-CTLA-4) for locally advanced or metastatic pancreatic adenocarcinoma. J Immunother. 2010;33(8):828-833.
Le DT, Lutz E, Uram JN, et al. Evaluation of ipilimumab in combination with allogeneic pancreatic tumor cells transfected with a GM-CSF gene in previously treated pancreatic cancer. J Immunother. 2013;36(7):382-389.
Brahmer JR, Tykodi SS, Chow LQ, et al. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med. 2012;366(26):2455-2465.
Henriksen A, Dyhl-Polk A, Chen I, Nielsen D. Checkpoint inhibitors in pancreatic cancer. Cancer Treat Rev. 2019;78:17-30.
Schmitz-Winnenthal FH, Escobedo LV, Beckhove P, et al. Specific immune recognition of pancreatic carcinoma by patient-derived CD4 and CD8 T cells and its improvement by interferon-gamma. Int J Oncol. 2006;28(6):1419-1428.
Zhu Y, Herndon JM, Sojka DK, et al. Tissue-Resident Macrophages in Pancreatic Ductal Adenocarcinoma Originate from Embryonic Hematopoiesis and Promote Tumor Progression. Immunity. 2017;47(2):323-338 e326.
Quaranta V, Schmid MC. Macrophage-Mediated Subversion of Anti-Tumour Immunity. Cells. 2019;8(7).
Principe DR, Doll JA, Bauer J, et al. TGF-beta: duality of function between tumor prevention and carcinogenesis. J Natl Cancer Inst. 2014;106(2):djt369.
Akhurst RJ, Hata A. Targeting the TGF beta signalling pathway in disease. Nature Reviews Drug Discovery. 2012;11(10):790-811.
Alvarez MA, Freitas JP, Mazher Hussain S, Glazer ES. TGF-beta Inhibitors in Metastatic Pancreatic Ductal Adenocarcinoma. J Gastrointest Cancer. 2019;50(2):207-213.
Yu L, Hebert MC, Zhang YE. TGF-beta receptor-activated p38 MAP kinase mediates Smad-independent TGF-beta responses. The EMBO journal. 2002;21(14):3749-3759.
Yeh HW, Lee SS, Chang CY, Lang YD, Jou YS. A New Switch for TGFbeta in Cancer. Cancer Res. 2019;79(15):3797-3805.
Glazer ES, Welsh E, Pimiento JM, Teer JK, Malafa MP. TGFbeta1 overexpression is associated with improved survival and low tumor cell proliferation in patients with early-stage pancreatic ductal adenocarcinoma. Oncotarget. 2017;8(1):999-1006.
Hussain SM, Reed LF, Krasnick BA, et al. IL23 and TGF-β diminish macrophage associated metastasis in pancreatic carcinoma. Sci Rep. 2018;8(1):5808.
Katz LH, Likhter M, Jogunoori W, Belkin M, Ohshiro K, Mishra L. TGF-beta signaling in liver and gastrointestinal cancers. Cancer Lett. 2016;379(2):166-172.
Massague J. TGFbeta in Cancer. Cell. 2008;134(2):215-230.
Vander Ark A, Cao J, Li X. TGF-beta receptors: In and beyond TGF-beta signaling. Cell Signal. 2018;52:112-120.
Huang F, Chen YG. Regulation of TGF-beta receptor activity. Cell Biosci. 2012;2:9.
Zhong X, Pons M, Poirier C, et al. The systemic activin response to pancreatic cancer: implications for effective cancer cachexia therapy. J Cachexia Sarcopenia Muscle. 2019;10(5):1083-1101.
Bakkebo M, Huse K, Hilden VI, Smeland EB, Oksvold MP. TGF-beta-induced growth inhibition in B-cell lymphoma correlates with Smad1/5 signalling and constitutively active p38 MAPK. BMC Immunol. 2010;11:57.
Wang L, Bai YY, Yang Y, et al. Diabetes mellitus stimulates pancreatic cancer growth and epithelial-mesenchymal transition-mediated metastasis via a p38 MAPK pathway. Oncotarget. 2016;7(25):38539-38550.
Leinwand J, Miller G. Regulation and modulation of antitumor immunity in pancreatic cancer. Nat Immunol. 2020.
Chen Y, Song Y, Du W, Gong L, Chang H, Zou Z. Tumor-associated macrophages: an accomplice in solid tumor progression. J Biomed Sci. 2019;26(1):78.
Fuxe J, Karlsson MC. TGF-beta-induced epithelial-mesenchymal transition: a link between cancer and inflammation. Semin Cancer Biol. 2012;22(5-6):455-461.
Zhang Y, Lazarus J, Steele NG, et al. Regulatory T cell depletion alters the tumor microenvironment and accelerates pancreatic carcinogenesis. Cancer Discov. 2020.
Sanford DE, Belt BA, Panni RZ, et al. Inflammatory monocyte mobilization decreases patient survival in pancreatic cancer: a role for targeting the CCL2/CCR2 axis. Clin Cancer Res. 2013;19(13):3404-3415.
Hegde S, Krisnawan VE, Herzog BH, et al. Dendritic Cell Paucity Leads to Dysfunctional Immune Surveillance in Pancreatic Cancer. Cancer Cell. 2020;37(3):289-307 e289.
Bayne LJ, Beatty GL, Jhala N, et al. Tumor-derived granulocyte-macrophage colony-stimulating factor regulates myeloid inflammation and T cell immunity in pancreatic cancer. Cancer Cell. 2012;21(6):822-835.
Clark CE, Hingorani SR, Mick R, Combs C, Tuveson DA, Vonderheide RH. Dynamics of the immune reaction to pancreatic cancer from inception to invasion. Cancer Res. 2007;67(19):9518-9527.
Schmid MC, Khan SQ, Kaneda MM, et al. Integrin CD11b activation drives anti-tumor innate immunity. Nature Communications. 2018;9(1):5379.
Sahai E, Astsaturov I, Cukierman E, et al. A framework for advancing our understanding of cancer-associated fibroblasts. Nat Rev Cancer. 2020;20(3):174-186.
Li T, Fu J, Zeng Z, et al. TIMER2.0 for analysis of tumor-infiltrating immune cells. Nucleic Acids Res. 2020;48(W1):W509-W514.
Li T, Fan J, Wang B, et al. TIMER: A Web Server for Comprehensive Analysis of Tumor-Infiltrating Immune Cells. Cancer Res. 2017;77(21):e108-e110.
Li B, Severson E, Pignon JC, et al. Comprehensive analyses of tumor immunity: implications for cancer immunotherapy. Genome Biol. 2016;17(1):174.
Gajewski TF, Cron KR. cDC1 dysregulation in cancer: An opportunity for intervention. J Exp Med. 2020;217(8).
Lin JH, Huffman AP, Wattenberg MM, et al. Type 1 conventional dendritic cells are systemically dysregulated early in pancreatic carcinogenesis. J Exp Med. 2020;217(8).
Seo YD, Pillarisetty VG. T-cell programming in pancreatic adenocarcinoma: a review. Cancer Gene Ther. 2017;24(3):106-113.
Mantovani A, Sica A, Sozzani S, Allavena P, Vecchi A, Locati M. The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol. 2004;25(12):677-686.
Wolff RA, Tomas JJ, Hullett DA, Stark VE, van Rooijen N, Hoch JR. Macrophage depletion reduces monocyte chemotactic protein-1 and transforming growth factor-beta1 in healing rat vein grafts. J Vasc Surg. 2004;39(4):878-888.
Mitchem JB, Brennan DJ, Knolhoff BL, et al. Targeting tumor-infiltrating macrophages decreases tumor-initiating cells, relieves immunosuppression, and improves chemotherapeutic responses. Cancer Res. 2013;73(3):1128-1141.
Gromisch C, Qadan M, Albuquerque Machado M, Liu K, Colson Y, Grinstaff MW. Pancreatic Adenocarcinoma: Unconventional Approaches for an Unconventional Disease. Cancer Res. 2020.
Ikeda M, Takahashi H, Kondo S, et al. Phase 1b study of galunisertib in combination with gemcitabine in Japanese patients with metastatic or locally advanced pancreatic cancer. Cancer Chemother Pharmacol. 2017;79(6):1169-1177.
Tchekneva EE, Goruganthu MUL, Uzhachenko RV, et al. Determinant roles of dendritic cell-expressed Notch Delta-like and Jagged ligands on anti-tumor T cell immunity. J Immunother Cancer. 2019;7(1):95.
Strauss L, Mahmoud MAA, Weaver JD, et al. Targeted deletion of PD-1 in myeloid cells induces antitumor immunity. Sci Immunol. 2020;5(43).
Metzger P, Kirchleitner SV, Kluge M, et al. Immunostimulatory RNA leads to functional reprogramming of myeloid-derived suppressor cells in pancreatic cancer. J Immunother Cancer. 2019;7(1):288.
Mota Reyes C, Teller S, Muckenhuber A, et al. Neoadjuvant Therapy Remodels the Pancreatic Cancer Microenvironment via Depletion of Protumorigenic Immune Cells. Clin Cancer Res. 2020;26(1):220-231.
Takeuchi Y, Nishikawa H. Roles of regulatory T cells in cancer immunity. Int Immunol. 2016;28(8):401-409.
Acknowledgements
Small portions of this work were presented at the 2020 Society of Surgical Oncology Annual Meeting-International Conference on Surgical Cancer Care.
Funding
Dr. Glazer receives support from the Society for Surgery of the Alimentary Tract in the form of the 2019–2021 Career Development Award.
Author information
Authors and Affiliations
Contributions
Conception and design: ESG and LM
Provision of study materials: all authors
Experiments: MAA, RK, MC, AKP
Manuscript writing and reviewing: all authors
Final approval: all authors
Corresponding author
Ethics declarations
Ethics Approval
All animal procedures were approved by the Institutional Animal Care and Use Committee at the University of Tennessee Health Science Center in accordance with the American Association for Accreditation of Laboratory Animal Care and the National Institutes of Health (NIH) Guide for the Care and Use of Laboratory Animals.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 5328 kb)
Rights and permissions
About this article
Cite this article
Trebska-McGowan, K., Chaib, M., Alvarez, M.A. et al. TGF-β Alters the Proportion of Infiltrating Immune Cells in a Pancreatic Ductal Adenocarcinoma. J Gastrointest Surg 26, 113–121 (2022). https://doi.org/10.1007/s11605-021-05087-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-021-05087-x