Abstract
In this report, we highlighted the clinical manifestations of obturator hernia and focused on laparoscopic views. Given its rarity and vague symptoms, the early diagnosis of obturator hernia presents a challenge. Although delays in diagnosis cause high rates of morbidity and mortality, CT with multi-planar reformations provides an excellent means of preoperative diagnosis. Despite current progress of laparoscopic surgery, its indication is believed to be limited only in elective obturator hernia repairs because of technical difficulties associated with bowel strangulation followed by a resection anastomosis. However, in selected cases, laparoscopic techniques can provide a minimally invasive option for obturator hernia repairs. These laparoscopic views, together with CT imaging, allow a better understanding of spatial anatomy and abnormality surrounding an obturator hernia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
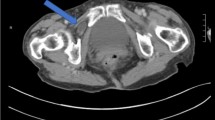
A 67-year-old woman with a body mass index of 16.6 kg/m2 presented to our department with sudden abdominal pain and vomiting. The pain occurred after urination, originated near the pubis and radiated to the left medial thigh. She obtained some relief with the affected thigh flexed. She had no history of abdominal surgery or trauma and had given birth to four children by normal vaginal delivery. Her medical history included chronic bronchiectasis and kyphoscoliosis. On examination, she had abdominal distention and tenderness to deep palpation, but no signs of peritoneal irritation and no palpable abdominal mass. Rectal examination revealed no abnormality. Blood test results were unremarkable, whereas abdominal radiographs showed dilated small bowel loops. Subsequent axial CT of the pelvis showed a fluid-filled mass between the left pectineus and external obturator muscles (Fig. 1a, arrow). On coronal imaging, this mass was seen as a loop of small intestine herniating into the left obturator canal (Fig. 1b, arrow). Because the incarcerated bowel loop had prominent wall enhancement consistent with early vascular compromise, an exploratory laparoscopy was deemed preferable. On the basis of our findings, the patient immediately underwent an exploratory laparoscopy, which did show a loop of the mid-ileum in the left obturator foramen (Fig. 2, arrow). We incidentally found bilateral femoral herniae and the contralateral obturator defect. We reduced the affected bowel loop with gentle retraction, restoring viability and rendering bowel resection unnecessary. Laparoscopic suture-repairs were carried out for bilateral obturator and femoral hernia defects. The patient recovered well and was discharged 2 days after operation. At follow-up 4 months later, she had no indication of recurrence.
Discussion
Obturator hernia is most common in multiparous, emaciated, elderly women because they have a wider pelvis with a larger obturator canal. Emaciation is an important risk factor because the loss of peritoneal fat pad overlying the obturator canal increases the risk of herniation.1 Comorbidity associated with increased intra-abdominal pressure, such as chronic constipation, chronic obstructive pulmonary disease, and kyphoscoliosis can predispose to the development of obturator hernia.2 The usual presentation is acute small-bowel obstruction with strangulation, frequently necessitating emergency bowel resection.3 A palpable groin mass in the medial thigh is uncommon because obturator hernia is externally concealed beneath the pectineus, whereas a herniated lesion is sometimes palpated on a rectal or vaginal examination.3 Obturator hernia presents less frequently on the left side because the sigmoid colon can cover the left obturator foramen, preventing herniation. About a third of patients have recurrent bowel obstruction followed by spontaneous remission.4
Because of its paucity and non-specific presentation, the early diagnosis is challenging.5 Obturator herniae produce pathognomonic signs because of compression of the obturator nerve, such as the Howship-Romberg sign (pain of the medial thigh which is exacerbated by extension, abduction, inward rotation, and relieved by flexion), and the Hannington-Kiff sign (absent thigh adductor reflex); however, its sensitivity is low, and severe abdominal symptoms can mask obturator neuropathy, causing these definitive signs to be mistaken for symptoms of degenerative arthralgia in elderly women.6 The implementation of CT including multi-planar reformations has greatly aided the preoperative diagnostic accuracy.5,6
Many possible surgical approaches including abdominal, preperitonal, inguinal, and laparoscopic exist for repairing obturator hernia although the choice depends on individual circumstances.5 Laparoscopic techniques provides a minimally invasive option and diagnostic laparoscopy can clarify the best course of action in bowel incarceration and ambiguous cases.6 It can also explore a contralateral defect, or other types of herniae. When the preoperative CT does not show severe ischemia in the affected bowel, a diagnostic laparoscopy has become our default initial approach to managing obturator hernia. Since frail, elderly women are poor candidates for surgery, delays in diagnosis cause high rates of morbidity and mortality; therefore, the timing of CT during the symptomatic period is of the utmost importance.6 Awareness of this disease process with its characteristic presentation is crucial. Heightened clinical suspicion in an emaciated, elderly woman should steer clinicians toward timely CT, prompting surgical intervention without delay.6,7
References
Yokoyama Y, Yamaguchi A, Isogai M, Hori A, Kaneoka Y. Thirty-six cases of obturator hernia: Does computed tomography contribute to postoperative outcome? World J Surg. 1999; 23(2): 214–216.
Burt BM, Cevasco M, Smink DS. Classic presentation of a type II obturator hernia. Am J Surg. 2010; 199(6): e75–e76.
Losanoff JE, Richman BW, Jones JW. Obturator hernia. J Am Coll Surg. 2002; 194(5):657–663.
Takada T, Ikusaka M, Ohira Y, Noda K, Tsukamoto T. Paroxysmal hip pain. Lancet. 2011; 377: 1464
Yip AW, AhChong AK, Lam KH. Obturator hernia: A continuing diagnostic challenge. Surgery. 1993; 119(3):266–269.
Tateno Y, Adachi K. Sudden knee pain in an underweight, older woman: obturator hernia. Lancet 2014; 384: 206.
Nasir BS, Zendejas B, Ali SM, Groenewald CB, Heller SF, Farley DR. Obturator hernia: The Mayo Clinic experience. Hernia; 2012; 16(3): 315–316.
Conflict of interest
The authors declare that they have no competing interests.
Financial support
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wada, Y., Ohtsuka, H. & Adachi, K. Laparoscopic Views of Obturator Hernia. J Gastrointest Surg 19, 1925–1926 (2015). https://doi.org/10.1007/s11605-015-2881-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2881-5