Abstract
Background
Detection of common bile duct (CBD) stones in patients with acute biliary pancreatitis (ABP) proves challenging. We hypothesized that grouping clinically significant predictors would increase reliability of detection.
Methods
A retrospective review was performed of 144 consecutive patients who presented to a single tertiary care institution from 2002 to 2007 with ABP.
Results
Of the 144 patients, 32 had a persistent CBD stone. Following multivariate analysis, admission CBD size on ultrasound, gamma glutamyl transferase (GGT), alkaline phosphatase (AP), total bilirubin (TB), and direct bilirubin (DB) significantly correlated with persistent CBD stone. Receiver operator curve analysis and linear regression were applied to obtain optimal and equitable predictive values, and variables combined. Optimal values were: CBD ≥ 9 mm; AP ≥ 250 U/l; GGT ≥ 350 U/l; TB ≥ 3 mg/dl; and DB ≥ 2 mg/dl. Presence of five variables had an associated odds ratio (OR) of 53.1 (p < 0.001) and four variables an OR of 8.97 (p = 0.004) for presence of persistent CBD stone. Zero variables conferred a significantly decreased probability of CBD stone, OR 0.15 (p < 0.001). Presence of one to three variables did not predict presence of CBD stone.
Conclusion
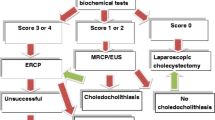
Presence of four or five variables significantly correlated with persistent CBD stone. Biliary evaluation by endoscopic retrograde cholangiopancreatography is suggested, as initial magnetic resonance cholangiopancreatography (MRCP) may only increase cost and delay time to intervention. In the absence of any variable, biliary evaluation by intraoperative cholangiogram may be sufficient. Decisions regarding patients with one to three variables should occur on a case-to-case basis. Initial biliary evaluation by MRCP is likely preferable, however, as no increased probability of CBD stone was identified, thus not warranting risks associated with intervention.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Acute biliary pancreatitis (ABP) accounts for 40% of pancreatitis cases diagnosed worldwide.1,2 Proposed mechanisms for ABP pathogenesis include reflux of bile into the pancreatic duct or transient obstruction of the ampulla of Vater by biliary sludge or stone.2,3 The majority of biliary stones pass spontaneously; however, risk of persistent ampullary obstruction increases with advanced patient age and stone size less than 5 mm.3 Complications of persistent common bile duct (CBD) stone include sepsis, hemorrhage, and necrotizing pancreatitis, and occur with increased frequency when duct obstruction persists greater than 48 h.3–6 Persistent CBD stones may also increase ABP mortality rate. Autopsy studies demonstrate CBD stones in up to 60% of patients with mortality secondary to ABP.5
Detection of persistent CBD stones in patients presenting with ABP remains challenging, as no reliable predictive parameters exist.7–9 Proper identification of ABP patients with CBD stone is central for selective biliary evaluation, prevention of disease progression, and assistance with perioperative planning.10–16 The purpose of this study was to increase reliability of CBD stone detection in patients presenting with ABP. We hypothesized that grouping clinically significant predictors, as opposed to individual values, would increase reliability of detection. Identifying the subset of patients with a high probability of persistent stone will facilitate appropriate selection of biliary evaluation modality, potentially decreasing negative imaging and intervention.
Methods
Following approval by the Mount Sinai School of Medicine Institutional Review Board, a retrospective review was performed of 144 consecutive patients with ABP who presented to The Mount Sinai Medical Center from 2002 to 2007. Patients were identified through an administrative database by use of ICD-9 577.0 identification code for acute pancreatitis alone and in conjunction with ICD-9 codes for cholecystectomy (51.2, 51.21, 51.22, 52.23, and 51.24). Clinical diagnosis of ABP was confirmed by elevated pancreatic enzymes and ultrasound findings of cholelithiasis at time of hospital admission. Minors, patients with history of alcohol abuse, known history of pancreatitis secondary to hereditary or medical factors, patients with cholangitis, and patients with history of cholecystectomy were excluded from the study. Standard of care at our institution is performance of cholecystectomy during same hospital admission for ABP when feasible.
Patient demographics, medical, social, and surgical history, and physical exam on admission were assessed. Ranson’s score was determined from presentation laboratory values. Hospital course including laboratory values, radiographic studies (ultrasound, computed tomography scan, and magnetic resonance cholangiopancreatography [MRCP]), interventions (endoscopic retrograde cholangiopancreatography [ERCP] and cholecystectomy), pathology report, length of hospital stay, morbidity, and mortality were reviewed. Laboratory values were trended daily from admission to discharge. Decisions regarding preoperative biliary evaluation, choice of ERCP versus MRCP for biliary assessment, and time to laparoscopic cholecystectomy were determined by the individual physician.
Statistical Evaluation
Univariate analysis by unpaired Student t test with two-tail distribution was used for quantitative variables and chi-square test for categorical variables. Multivariate logistic regression models were used to estimate odds ratios and an associated 95% confidence interval. Final multivariate models were created by elimination of non-significant variables from univariate analysis. Once significant values were identified, “cut-off” points were determined. Receiver operator curves (ROC) were plotted and linear regression applied to obtain optimum predictive values. Optimum values were determined as data points that provided the most favorable and equitable combination of sensitivity and specificity between variables. Significant variables were grouped and odds ratio with 95% confidence interval calculated for patients based on total variables present on admission. PRISM 2.0 software (San Diego, CA, USA; 2003) was used for all analysis and statistics were reviewed with a statistician.
Results
From 2002 to 2007, 144 patients with ABP qualified for the study. Analysis of initial management demonstrated 69 (48%) patients underwent biliary evaluation, 29 patients by MRCP, and 40 ERCP. All biliary evaluation occurred within 72 h of admission. Of the 29 patients who underwent MRCP, 11 (38%) patients had CBD stone. Of the 11 patients with positive MRCP, 100% had CBD stone on subsequent ERCP. One subsequent ERCP failed secondary to anatomical difficulty and the patient required CBD exploration. Forty patients underwent initial ERCP of which 16 (40%) were positive for CBD stone. All ERCP were successful. Twelve patients underwent sole sphincterotomy, two sole stent placement, two both sphincterotomy and stent placed, and three patients had neither.
Of the 144 patients, 100 (69%) underwent cholecystectomy on same admission. Mean time to cholecystectomy was 7.6 days (range 4–22 days). Sixty-one (61%) patients underwent cholangiogram at time of cholecystectomy, of which five patients had incidental discovery of CBD stone. All five patients did not undergo preoperative biliary evaluation and were successfully managed by postoperative ERCP.
A total of 32 patients (22%) were identified with a CBD stone. Table 1 demonstrates univariate comparison of patients with and without persistent CBD stone. Patients were well matched by age, gender, comorbidity, history of pancreatitis, and severity of ABP as assessed by Ranson’s score on presentation. Following univariate analysis of admission variables, multivariate logistic regression models were created by elimination of non-significant univariate variables. Increased CBD size on admission ultrasound (US), increased admission alkaline phosphatase (AP), total bilirubin (TB), direct bilirubin (DB), and gamma glutamyl transferase (GGT) significantly correlated with presence of persistent stone. Significant variables with associated odds ratio (OR) and 95% confidence interval (CI) are presented in Table 2.
Receiver operator curves were plotted and linear regression applied to determine optimum cut-off values. Optimal values were those that maintained the most equitable and favorable balance of sensitivity and specificity between variables and are demonstrated by Fig. 1 and Table 3. Optimal values were determined as admission ultrasound CBD ≥ 9 mm, AP ≥ 250 U/l, GGT ≥ 350 U/l, TB ≥ 3 mg/dl, and DB ≥ 2 mg/dl. Selected cut-off points had comparable sensitivity and specificity for correlation with CBD stone, which allowed for equal weighting when variables were grouped. Table 4 demonstrates results after variable grouping and application to our patient population. Patients with five clinical variables present on admission had an OR of 53.1 (p < 0.001) for presence of persistent CBD stone. Patients with any four clinical variables had an OR of 8.97 (p = 0.004) for presence of CBD stone. No increased correlation with persistent CBD stone was demonstrated in patients with any combination of one to three variables.
Retroactive application of grouped variables to the 69 patients who underwent preoperative biliary evaluation demonstrated 78% of patients with one to three variables had negative biliary evaluation (variables present [negative evaluation] = 0 [78%], 1 [71%], 2 [57%], 3 [63%]). For patients with four to five variables, 92% had CBD stone on biliary evaluation.
Discussion
Our study identified five clinical variables on hospital presentation: CBD size on ultrasound, AP, GGT, TB, and DB, which significantly correlated with presence of persistent CBD stone. Several studies have also identified individual clinical parameters that correlate with persistent CBD stone.7–9,17 Lin et al. identified initial CBD size on ultrasound and AST as significant predictors of CBD stone in patients with ABP.18 A study by Chang et al. demonstrated TB, ALT, and AP as significant clinical variables, with hospital day 2 TB as the most accurate predictor.7 Cohen et al. demonstrated rise in any serum chemistry within 24–48 h of hospital admission correlated with a persistent CBD stone in 31% of patients.8 To date, however, no individual laboratory value or trend has proven to reliably identify ABP patients at high risk of persistent CBD stone. As the majority of CBD stones pass spontaneously within 48 h, it is not surprising that a significant proportion of biliary evaluation in patients with abnormal liver function tests result in negative studies. We hypothesized that the combined predictive ability of significant admission clinical variables would be more reliable at identifying patients with persistent, rather than passed, CBD stone.
Based on this hypothesis, cut-off points with comparable sensitivity and specificity were selected to allow variables to be equally weighted and grouped. Assessment of our study population demonstrated that patients with four or five clinical variables were at significantly increased risk for persistent CBD stone. Patients with five variables had an OR of 53.1 (p < 0.001) with 100% PPV for presence of CBD stone and for those with four variables, a calculated OR of 8.97 (p = 0.004) with 71% PPV. In addition, 92% of patients with four or five variables on admission who underwent preoperative biliary evaluation were found to have persistent CBD stone. While the retrospective nature of this paper precludes definitive recommendations, this finding strongly supports biliary evaluation by ERCP for patients in whom four or five variables are present, as MRCP may only delay time to intervention. Endoscopic ultrasound (EUS) is recommended prior to ERCP where available. Within the past several years, EUS has emerged as a highly sensitive and specific modality for detection of biliary stones.19 Studies demonstrate that the use of EUS prior to ERCP decreases negative ERCP rates in up to 75% of patients with ABP.20,21 Performance of EUS prior to ERCP adds minimal procedural time and precludes performance of unnecessary intervention.19–21
Patients in whom any one to three clinical variables were present demonstrated no significantly increased probability of persistent CBD stone. However, when retroactively assessed, 22% of patients were found to have persistent CBD stone on biliary evaluation. While decisions regarding biliary evaluation for this patient subset should occur on a case-to-case basis, preoperative biliary imaging by MRCP is likely preferable with subsequent ERCP in patients with positive imaging. MRCP has a 91% sensitivity and 98% specificity for detection of choledocholithiasis and is advantageous as it is a non-invasive procedure with negligible complication rate.22,23 MRCP is preferential as many studies will likely be negative, not warranting the 5–10% morbidity rate associated with ERCP.10,15
Of note, patients with zero clinical variables were at significantly decreased risk for persistent CBD stone. For this subset of patients, our study suggests biliary evaluation by cholangiogram (IOC) at time of cholecystectomy may be sufficient. Although debated within the literature, at our institution biliary, evaluation with IOC at time of cholecystectomy in patients with ABP remains the standard of care.9 The authors strongly recommend performance of cholangiogram, in the absence of preoperative biliary imaging, as a means to ensure patients with asymptomatic choledocholithiasis are identified.
The necessity for improved reliability of persistent CBD stone detection in patients with ABP is emphasized by the significant rate of negative MRCP and ERCP reported within literature, varying from 50% to 80% and 40% to 70%, respectively.8,17,18,21 Our institution is no exception. Sixty-two percent of patients underwent negative MRCP and 60% negative ERCP which is disconcerting as biliary evaluation for ABP patients is not standard and based on physician assessment. This finding further highlights the inaccuracy of current evaluation criteria utilized to identify persistent CBD stones in patients with ABP. Grouping clinical variables may facilitate appropriate selection of initial biliary evaluation in patients presenting with ABP. While future prospective application is necessary, this study identified a combination of clinical variables which significantly correlated with presence of persistent CBD stone. In addition, we identified a subset of patients with a significantly negligible risk. Although methodological limitations preclude conclusive recommendations, this study suggests that evaluation by ERCP for patients with four or five clinical variables and cholangiogram for patients with zero variables is appropriate. For patients presenting with one to three variables, individual assessment is necessary; however, initial evaluation by MRCP, rather than ERCP, appears preferable.
References
Riela A, Zinsmeister AR, Melton LJ, DiMagno EP. Etiology, incidence, and survival of acute pancreatitis in Olmsted County, Minnesota. Gastroenterology 1991;100:A296.
Frossard JL, Steer ML, Pastor CM. Acute pancreatitis. Lancet 2008;371(9607):143–152.
Wilson C, Imrie CW, Carter DC. Fatal acute pancreatitis. Gut 1988;29(6):782–788.
Corfield AP, Cooper MJ, Williamson RC. Acute pancreatitis: a lethal disease of increasing incidence. Gut 1985;26(7):724–729.
Wilson C, Imrie CW, Carter DC. Fatal acute pancreatitis. Gut 1988;29(6):782–788.
Acosta JM, Rubio Galli OM, Rossi R, Chinellato AV, Pellegrini CA. Effect of duration of ampullary biliary obstruction on severity of lesions of acute pancreatitis. J Am Coll Surg 1997;184(5):499–505.
Chang L, Lo SK, Stabile BE, Lewis RJ, de Virgilio C. Biliary pancreatitis: a prospective study on the incidence of cholangitis and clinical predictors of retained common bile duct stones. Am J Gastroenterol 1998;93(4):527–531.
Cohen ME, Slezak L, Wells CK, Andersen DK, Topazian M. Prediction of bile duct stones and complications in biliary pancreatitis using early laboratory trends. Am J Gastroenterol 2001;96(12):3305–3311.
Roston AD, Jacobson IM. Evaluation of the pattern of liver tests and yield of cholangiography in symptomatic choledocholithiasis: a prospective study. Gastrointest Endosc 1997;45(5):394–399.
Moretti A, Papi C, Aratari A, Festa V, Tanga M, Koch M, et al. Is early endoscopic retrograde cholangiopancreatography useful in the management of acute biliary pancreatitis? A meta-analysis of randomized controlled trials. Dig Liver Dis 2008;40(5):379–385.
Petrov MS, van Santvoort HC, Besselink MG, van der Heijden GJ, van Erpecum KJ, Gooszen HG. Early endoscopic retrograde cholangiopancreatography versus conservative management in acute biliary pancreatitis without cholangitis: a meta-analysis of randomized trials. Ann Surg 2008;247(2):250–257.
Diagnosis and treatment of common bile duct stones (CBDS). Results of a consensus development conference. Scientific Committee of the European Association for Endoscopic Surgery (E.A.E.S.). Surg Endosc 1998;12(6):856–864.
Vitale GC. Early management of acute biliary pancreatitis. Ann Surg 2007;245(1):18–19.
Folsch UR, Nitsche R, Lüdtke R, Hilgers RA, Creutzfeld W. Early ERCP and papillotomy compared with conservative treatment for acute biliary pancreatitis. N Engl J Med 1997;336:237–242.
de Virgilio C, Verbin C, Chang L, Linder S, Stabile BE, Klein S. Biliary pancreatitis. The role of preoperative endoscopic retrograde cholangiopancreatography. Arch Surg 1994;129(9):90912.
Acosta JM, Katkhouda N, Debian KA, Groshen SG, Tsao-Wei DD, Berne TV. Early ductal decompression versus conservative management for biliary pancreatitis with ampullary obstruction: a prospective randomized clinical trial. Ann Surg 2006;243(1):33–40.
Chan T, Yaghoubian A, Rosing D, Lee E, Lewis RJ, Stabile BE, De Virgilio C. Total bilirubin is a useful predictor of persisting common bile duct stone in gallstone pancreatitis. Am Surg 2008;74(10):977–980.
Lin G, Halevy A, Girtler O, Gold-Deutch R, Zisman A, Scapa E. The role of endoscopic retrograde cholangiopancreatography in management of patients recovering from acute biliary pancreatitis in the laparoscopic era. Surg Endosc 1997;11(4):371–375.
Chak A, Hawes R, Cooper GS, et al. Prospective assessment of the utility of EUS in the evaluation of gallstone pancreatitis. Gastrointest Endosc 1999;49:599–604.
Liu CL, Fan ST, Lo CM, et al. Comparison of early endoscopic ultrasonography and endoscopic retrograde cholangiopancreatography in the management of acute biliary pancreatitis: a prospective randomized study. Clin Gastroenterol Hepatol 2005;3:1238–1244.
Moon JH, Cho YD, Cha SW, et al. The detection of bile duct stones in suspected biliary pancreatitis: comparison of MRCP, ERCP, and intraductal US. Am J Gastroenterol 2005;100:1051–1057.
Varghese JC, Liddell RP, Farrell MA, Murray FE, Osborne H, Lee MJ. The diagnostic accuracy of magnetic resonance cholangiopancreatography and ultrasound compared with direct cholangiography in the detection of choledocholithiasis. Clin Radiol 2000;55(7):579.
Mofidi R, Lee AC, Madhavan KK, Garden OJ, Parks RW. The selective use of magnetic resonance cholangiopancreatography in the imaging of the axial biliary tree in patients with acute biliary pancreatitis. Pancreatology 2008;8(1):55–60.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Telem, D.A., Bowman, K., Hwang, J. et al. Selective Management of Patients with Acute Biliary Pancreatitis. J Gastrointest Surg 13, 2183–2188 (2009). https://doi.org/10.1007/s11605-009-1041-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-009-1041-1