Summary
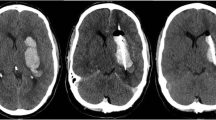
The study aimed to investigate the impact of intraclot recombinant tissue-type plasminogen activator (rt-PA) on perihematomal edema (PHE) development in patients with intracerebral hemorrhage (ICH) treated with minimally invasive surgery (MIS) and the effects of intraclot rt-PA on the 30-day survival. We reviewed the medical records of ICH patients undergoing MIS between October 2011 and July 2013. A volumetric analysis was done to assess the change in PHE and ICH volumes at pre-MIS (T1), post-MIS (T2) and day 10–16 (T3) following diagnostic computed tomographic scans (T0). Forty-three patients aged 52.8±11.1 years with (n=30) or without rt-PA (n=13) were enrolled from our institutional ICH database. The median rt-PA dose was 1.5 (1) mg, with a maximum dose of 4.0 mg. The ratio of clot evacuation was significantly increased by intraclot rt-PA as compared with controls (77.9%±20.4% vs. 64%±15%; P=0.046). From T1 to T2, reduction in PHE volume was strongly associated with the percentage of clot evacuation (ρ=0.34; P=0.027). In addition, PHE volume was positively correlated with residual ICH volume at the same day (ρ ranging from 0.39–0.56, P<0.01). There was no correlation between the cumulative dose of rt-PA and early (T2) PHE volume (ρ=0.24; P=0.12) or delayed (T3) PHE volume (ρ=0.19; P=0.16). The 30-day mortality was zero in this cohort. In the selected cohort of ICH patients treated with MIS, intraclot rt-PA accelerated clot removal and had no effects on PHE formation. MIS aspiration and low dose of rt-PA seemed to be feasible to reduce the 30-day mortality in patients with severe ICH. A large, randomized study addressing dose titration and long-term outcome is needed.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
van Asch CJ, Luitse MJ, Rinkel GJ, et al. Incidence, case fatality, and functional outcome of intracerebral haemorrhage over time, according to age, sex, and ethnic origin: a systematic review and meta-analysis. Lancet Neurol, 2010,9(2):167–176
Arima H, Wang JG, Huang Y, et al. Significance of perihematomal edema in acute intracerebral hemorrhage: the INTERACT trial. Neurology, 2009,73(23):1963–1968
Broderick JP, Brott TG, Duldner JE, et al. Volume of intracerebral hemorrhage. A powerful and easy-to-use predictor of 30-day mortality. Stroke, 1993,24(7):987–993
Staykov D, Wagner I, Volbers B, et al. Natural course of perihemorrhagic edema after intracerebral hemorrhage. Stroke, 2011,42(9):2625–2629
Zazulia AR, Diringer MN, Derdeyn CP, et al. Progression of mass effect after intracerebral hemorrhage. Stroke, 1999,30(6):1167–1173
Carhuapoma JR, Barrett RJ, Keyl PM, et al. Stereotactic aspiration-thrombolysis of intracerebral hemorrhage and its impact on perihematoma brain edema. Neurocrit Care, 2008,8(3):322–329
Mould WA, Carhuapoma JR, Muschelli J, et al. Minimally invasive surgery plus recombinant tissue-type plasminogen activator for intracerebral hemorrhage evacuation decreases perihematomal edema. Stroke, 2013,44(3):627–634
Wagner KR, Xi G, Hua Y, et al. Ultra-early clot aspiration after lysis with tissue plasminogen activator in a porcine model of intracerebral hemorrhage: edema reduction and blood-brain barrier protection. J Neurosurg, 1999,90(3):491–498
Barrett RJ, Hussain R, Coplin WM, et al. Frameless stereotactic aspiration and thrombolysis of spontaneous intracerebral hemorrhage. Neurocrit Care, 2005,3(3):237–245
Vespa P, McArthur D, Miller C, et al. Frameless stereotactic aspiration and thrombolysis of deep intracerebral hemorrhage is associated with reduction of hemorrhage volume and neurological improvement. Neurocrit Care, 2005,2(3):274–281
Figueroa BE, Keep RF, Betz AL, et al. Plasminogen activators potentiate thrombin-induced brain injury. Stroke, 1998,29(6):1202–1207
Rohde V, Rohde I, Thiex R, et al. Fibrinolysis therapy achieved with tissue plasminogen activator and aspiration of the liquefied clot after experimental intracerebral hemorrhage: rapid reduction in hematoma volume but intensification of delayed edema formation. J Neurosurg, 2002,97(4):954–962
Rohde V, Uzma N, Thiex R, et al. Management of delayed edema formation after fibrinolytic therapy for intracerebral hematomas: preliminary experimental data. Acta Neurochir Suppl, 2008,105:101–104
Thiex R, Kuker W, Muller HD, et al. The long-term effect of recombinant tissue-plasminogen-activator (rt-PA) on edema formation in a large-animal model of intracerebral hemorrhage. Neurol Res, 2003,25(3):254–262
Thiex R, Weis J, Krings T, et al. Addition of intravenous N-methyl-D-aspartate receptor antagonists to local fibrinolytic therapy for the optimal treatment of experimental intracerebral hemorrhages. J Neurosurg, 2007,106(2):314–320
Ducruet AF, Hickman ZL, Zacharia BE, et al. Exacerbation of perihematomal edema and sterile meningitis with intraventricular administration of tissue plasminogen activator in patients with intracerebral hemorrhage. Neurosurgery, 2010,66(4):648–655
Tang ZP, Shi YH, Yin XP, et al. Modifying the details of aspiration operation may contribute to the improvement of prognosis of patients with ICH. Turk Neurosurg, 2012,22(1):13–20
Xiao B, Wu FF, Zhang H, et al. A randomized study of urgent computed tomography-based hematoma puncture and aspiration in the emergency department and subsequent evacuation using craniectomy versus craniectomy only. J Neurosurg, 2012,117(3):566–573
Xu F, Tang Z, Luo X, et al. No evidence of preoperative hematoma growth representing an increased postoperative rebleeding risk for minimally invasive aspiration and thrombolysis of ICH. Br J Neurosurg, 2010,24(3):268–274
Morgenstern LB, Hemphill JC, 3rd, Anderson C, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke, 2010,41(9):2108–2129
Hemphill JC 3rd, Bonovich DC, Besmertis L, et al. The ICH score: a simple, reliable grading scale for intracerebral hemorrhage. Stroke, 2001,32(4):891–897
Keep RF, Hua Y, Xi G. Intracerebral haemorrhage: mechanisms of injury and therapeutic targets. Lancet Neurol, 2012,11(8):720–731
Mayer SA, Sacco RL, Shi T, et al. Neurologic deterioration in noncomatose patients with supratentorial intracerebral hemorrhage. Neurology, 1994,44(8):1379–1384
Naff N, Williams MA, Keyl PM, et al. Low-dose recombinant tissue-type plasminogen activator enhances clot resolution in brain hemorrhage: the intraventricular hemorrhage thrombolysis trial. Stroke, 2011,42(11):3009–3016
Staykov D, Wagner I, Volbers B, et al. Dose effect of intraventricular fibrinolysis in ventricular hemorrhage. Stroke, 2011,42(7):2061–2064
Godoy DA, Pinero G, Di Napoli M. Predicting mortality in spontaneous intracerebral hemorrhage: can modification to original score improve the prediction? Stroke, 2006,37(4):1038–1044
Wang W, Lu J, Wang C, et al. Prognostic value of ICH score and ICH-GS score in Chinese intracerebral hemorrhagepatients: analysis from the China National Stroke Registry (CNSR). PLoS One, 2013,8(10):e77421
Herrick DB, Ziai WC, Thompson CB, et al. Systemic hematologic status following intraventricular recom-binant tissue-type plasminogen activator for intra-ventricular hemorrhage: the CLEAR IVH Study Group. Stroke, 2011,42(12):3631–3633
Zimmerman RD, Maldjian JA, Brun NC, et al. Radiologic estimation of hematoma volume in intracerebral hemorrhage trial by CT scan. AJNR Am J Neuroradiol, 2006,27(3):666–670
Author information
Authors and Affiliations
Corresponding author
Additional information
This project was supported by grants from the National Natural Science Foundation of China (No. 81171089 and No. 30770751), Key Clinical Program of the Ministry of Health of China (2010), and the Future Program of New Technology and New Business in Tongji Hospital, China (2012).
Rights and permissions
About this article
Cite this article
Lian, Lf., Xu, F., Tang, Zp. et al. Intraclot recombinant tissue-type plasminogen activator reduces perihematomal edema and mortality in patients with spontaneous intracerebral hemorrhage. J. Huazhong Univ. Sci. Technol. [Med. Sci.] 34, 165–171 (2014). https://doi.org/10.1007/s11596-014-1252-x
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-014-1252-x