Abstract
Quetiapine, an atypical antipsychotic medication has lacked pre-clinical validation for its purported benefits in the treatment of delirium. This laboratory investigation examined the effects of quetiapine on the attentional set shifting task (ASST), a measure of cognitive flexibility and executive functioning, in a rodent model of lipopolysaccharide (LPS) mediated neuroinflammation. 19 Sprague Dawley female rats were randomly selected to receive intraperitoneal placebo (N = 5), LPS and placebo (N = 7) or LPS and quetiapine (n = 7) and performed the ASST. We measured trials to criterion, errors, non-locomotion episodes and latency to criterion, serum cortisol and tumor necrosis factor alpha (TNF-α) levels. TNF-α levels were not different between groups at 24 h. Cortisol levels in the LPS + Quetiapine group were reduced compared to LPS + Placebo (P < 0.001) and did not differ from the placebo group (P = 0.15). Analysis between LPS + Quetiapine and LPS + Placebo treated rats demonstrated improvement in the compound discrimination reversal (CD Rev1) (P = 0.016) and the intra-dimensional reversal (ID Rev2) (P = 0.007) discriminations on trials to criterion. LPS + Quetiapine treated rats had fewer errors than LPS + Placebo treated animals in the compound discrimination (CD) (P = 0.007), CD Rev1 (P = 0.005), ID Rev2 (P < 0.001) discriminations. There was no difference in non-locomotion frequency or latency to criterion between the three groups in all discriminations (P > 0.0167). We demonstrated preserved reversal learning, no effect on attentional set shifting and normalized cortisol levels in quetiapine-treated rats in this neuroinflammatory model of delirium. This suggests that quetiapine’s beneficial effects in delirium may be related to the preservation of reversal learning and potential downstream effects related to reduction in cortisol production.

Graphical Abstract
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intensive care unit (ICU) delirium is an acute condition characterized by fluctuating disturbances of consciousness, inattention, and cognitive impairment and has been associated with deleterious long-term outcomes in ICU survivors (Girard et al. 2008, 2010; Pandharipande et al. 2013). Its pathophysiology is incompletely understood, although neuroinflammation has been implicated in its development in both pre-clinical and clinical studies (Munster et al. 2011; Westhoff et al. 2013; Kawano et al. 2018; Tanaka et al. 2018). Furthermore, functional MRI studies have observed that the frontal cortex is abnormally affected by acute delirium (Choi et al. 2012). In addition, delirium may induce long-term gray and white matter abnormalities in the frontal cortex and associated areas of the brain (Shioiri et al. 2010; Morandi et al. 2012; Shioiri et al. 2016). The frontal cortex plays a critical role in executive functioning, the collection of control processes broadly responsible for complex goal-directed behavior. Its impairment likely impacts patients with both acute delirium and long-term cognitive impairment after critical illness (Inouye et al. 2016; Stollings et al. 2016; Duggan et al. 2017).
Quetiapine, an atypical antipsychotic medication with activity at dopaminergic (D2), histaminergic (H1), serotoninergic (5-HT1A, 5-HT2A), and noradrenergic (α1) receptor sites, has been utilized to manage the symptoms of delirium. Quetiapine has demonstrated clinical efficacy in the treatment of delirium (Devlin et al. 2010, 2011, 2016). Compared to haloperidol, quetiapine exerts substantial effects on the hypothalamic-pituitary axis (HPA), reducing the secretion of adrenocorticotropic hormone (ACTH) and cortisol (Cohrs et al. 2006). Increased cortisol levels have been observed in patients with delirium and other conditions associated with executive dysfunction such as major depressive disorder and schizophrenia (Carroll et al. 1976; Kazmierski et al. 2013; Girshkin et al. 2014).
The attentional set shifting task (ASST) is a task of complex cognitive processes associated with executive functioning and has been utilized across numerous species (Popik and Nikiforuk 2015; Brown and Tait 2016). A correlate for the Wisconsin Card Sorting Test (WCST), it measures the ability of the animal to learn simple rules, discriminate stimuli within a relevant dimension and update working memory in the setting of changing dimensions. These presented stimuli (odor, medium and texture) form an attentional set which are then challenged with reversal learning. The attentional set is then challenged by completely new stimuli to assess attentional set shifting performance. Published lesion studies using the ASST have demonstrated that the orbitofrontal cortex plays a major role in reversal learning and the medial prefrontal cortex in attentional set shifting in the rat (Birrell and Brown 2000; McAlonan and Brown 2003). Quetiapine has been shown to preserve ASST performance in animal models of stress and schizophrenia, conditions associated with deleterious effects on executive function (Nikiforuk and Popik 2012; Nikiforuk 2013). Lipopolysaccharide (LPS) are large molecules derived from the outer membrane of Gram-negative bacteria and are ubiquitously used as a method to induce systemic and neuroinflammation in experimental models. It has been shown that a single dose of LPS may cause chronic neuroinflammation with neurodegeneration in experimental mice (Qin et al. 2007). Treatment with LPS disrupts performance on the ASST, implicating the ASST as a useful animal model for the executive dysfunction associated with ICU delirium (Culley et al. 2014). In this study, we hypothesized that the concurrent administration of quetiapine in LPS-treated rats would preserve performance on the ASST. We utilized aged rats (12–18 months) given that advanced age has been shown to increase the risk of delirium in human populations (Kanova et al. 2017). Furthermore, we hypothesized that cortisol levels would be reduced in rats treated with LPS and quetiapine compared to LPS alone.
Methods
Animals
After approval from the Penn State College of Medicine Institutional Animal Care and Use Committee (Study Number: 47992), twenty-four Sprague-Dawley female rats aged 12–18 months (Charles River, Frederick, MD) were placed in single housing on recommendation of the institutional veterinarian (23 × 45 × 15 cm plastic cages). Animals were acclimatized over a period of seven days prior to experimental testing. Testing was performed in the dark cycle of a 12-h light/dark cycle to optimize activity. Rats were placed on a food restriction (15–20 g rat chow per day), offered water ad libitum and weighed daily. We targeted an optimal weight of 85% of free-fed weight. All procedures adhered to the guidelines in the Principles of Laboratory Animal Care (National Institutes of Health, Eighth Ed., National Academies Press 2011).
Apparatus
All rats were trained to the apparatus during the acclimatization phase (Fig. 1a). Digging bowls were white porcelain 4 oz. ramekins (diameter: 9.5 cm, depth: 4 cm). All animals were presented with the ramekins within home cages on Day 3, introduced to the attentional set shifting apparatus on Day 4–5, and trained to forage for food reward within the apparatus on days 6–7. The test apparatus was a clear plexiglass cage (40 × 70 × 18 cm) with opaque plastic dividers, a design adapted from previous authors (Birrell and Brown 2000; Popik and Nikiforuk 2015) (Fig. 1b). A removable opaque divider provided a holding area for the animal between sessions and a non-removable divider separated the reward areas. The non-removable divider was utilized to prevent animals from rapidly obtaining a reward after an error was made, allowing the experimenter to remand the animal back to the holding area to re-start the trial. A hinged lid was added to prevent the animals from exiting the apparatus and to reduce ambient noise during testing.
a The timing of acclimatization, testing and serum testing. Note that rats followed a sequential series of experimental phases with increasing complexity (simple discrimination (SD); compound discrimination (CD) compound discrimination reversal (CDRev1); Intra-dimensional Discrimination (ID); Intra-dimensional Discrimination reversal (IDRev2); Extradimensional Discrimination (ED); Extradimensional Discrimination Reversal (EDRev3)). b The Attentional Set Shifting Apparatus. Note the non-removable divider separating the reward bowls. The removable divider (black) separated the holding area from the reward areas. c Stimuli pairings for the attentional set-shifting task. Each rat performed a practice simple and complex discrimination task prior to intervention. These odors and medium were not used again. Rats were then randomized to receive one of three of the clustered pairings for experimental testing. The ED discrimination was randomized from one of the other two clusters to ensure animals were exposed to entirely new stimuli
Training
On Days 6–7, initial training was comprised of six trials during the acclimatization phase. Rats were introduced to the attentional set shifting apparatus with an uncovered food reward (Fruit Crunchie, Bio-serv, NJ) in one ramekin in trial 1. For trials 2–6, increasing amounts of sawdust were utilized to obscure the food reward and encourage foraging behavior. All animals were then trained on a simple (SD) and compound discrimination (CD) during the training phase. Nineteen animals successfully completed the training and were included in the study. Five animals were excluded as training non-responders.
Testing Paradigm
Relevant and irrelevant dimensions combinations were pre-randomized to groups (Fig. 1c). Animals were then randomized into three groups: Placebo + Placebo (0.9% saline; (n = 5)), Lipopolysaccharide (50mcg/kg; E.coli/0111:B4; Sigma-Aldrich, MO) treatment + Placebo (n = 7), and Lipopolysaccharide (50mcg/kg) + Quetiapine (2.5 mg/kg; 3.5 mg/ml buffered solution; Sigma-Aldrich, MO) treatment (n = 7). All animals received two separate intraperitoneal injections and performed neurobehavioral testing 18 h after intervention.
Testing
Each rat then performed the attentional set shifting task, a series of seven discriminations that tests attentional set acquisition, reversal learning and attentional set shifting. Simple discrimination (SD) was comprised of two stimuli from one dimension (odor). The compound discrimination (CD) added two irrelevant dimensions (medium and texture) to the relevant dimension (odor) used in the SD phase. In the intra-dimensional shift (ID) phase, all new stimuli were introduced, with the relevant dimension remaining the same. With the extra-dimensional shift (ED), all new stimuli were introduced but a previously irrelevant dimension (texture), was now relevant. The ED was performed to test attentional set shifting, a measure of executive functioning. All reversal learning stages (CD Rev1, ID Rev2, ED Rev3) demanded that the rat learn that the previously correct stimulus was now incorrect. The order of discriminations remained the same for all animals. All animals received one practice 3-min trial per discrimination that was excluded from the data analysis. During the practice trial, animals were allowed free access to the entire apparatus and allowed to explore or dig in the rewards bowls without interference.
Measurements
Each discrimination was comprised of a series of 3-min trials. Each trial started with the removal of the holding area divider. After retrieval of the reward or an error the rat was replaced in the holding area for the next trial. If, after 3 min, the rat did not complete the trial with a successful retrieval of reward, the animal was re-homed in the holding area. Subsequently, the trial was re-started. Animals attempted each discrimination until they reached trials to criterion (TTC). In this study, TTC was the number of trials needed to reach six consecutive correct trials in the discrimination. The last five consecutive trials were subtracted from the number of trials needed to reach TTC. In addition, we measured errors per discrimination (errors), defined as observer visualized food foraging behavior (digging in the medium) within the incorrect reward pot. Animals were permitted to smell and touch the pot without penalty. To measure the behavioral effects of lipopolysaccharide treatment, we measured the number of non-locomotor episodes, defined as a 3-min trial where the animal did not leave the holding area when the holding divider was removed to commence the trial.
Serum Cortisol and TnF- α Measurements
After completing the neurobehavioral testing, animals were deeply anesthetized with isoflurane (5%) and a terminal cardiac puncture procedure was performed to retrieve whole blood samples. Procured samples were immediately centrifuged (1600 rpm, 10 min) and frozen to −80 °C. For serum cortisol and TnF-α quantification, we used a competitive immunoassay (Enzo Life Sciences, NY) and a solid phase sandwich ELISA assay (R&D systems, MN), respectively. Frozen samples were thawed and run in triplicate according to the manufacturer’s instructions. Spectrophotometer OD values were quantified, and calculated results were interpolated using a four-parameter logistic (4-PL) curve-fit (Prism 7, GraphPad, CA).
Statistical Analysis
Descriptive statistics (mean, standard deviation) were calculated for the following variables: weight, serum TNF-α levels, serum cortisol levels, trials to criterion, errors to criterion, number of in phase trials of no locomotion, and latency to trials to criterion. Analysis of variance models were used to compare the treatment groups with respect to TnF-α levels and serum cortisol levels. A general linear model (GLM) with correlated errors was fit to assess the effects of group, day and the interaction of group and day on weight (Diggle et al. 2002). GLM with correlated errors also were used to assess the effects of group, discrimination, and the interaction of group and discrimination on the outcomes of trials to criterion, errors to criterion, number of trials of no locomotion, and latency to trials to criterion. The GLM with correlated errors takes into account the repeated measurement obtained per animal. Residual diagnostics were used to ensure modeling assumptions were met for normality. Pairwise comparisons among the 3 treatments are presented for individual days in Fig. 1. We were most interested in within-phase comparisons in our post-hoc analyses and we used a Bonferroni adjustment to determine significance. For our post-hoc analyses, the p value had to be less than 0.0167 to be considered significant (Bonferroni adjustment = α/R = 0.05/3 = 0.0167, where α = significance level and R = number of treatment groups per compared phase). All hypothesis tests were two-sided, and all analyses were performed using SAS software, version 9.4 (SAS Institute Inc., Cay, NC).
Results
Weight
Weight in grams did not differ between groups as measured at regular intervals (Days 0, 3, 5) during the pre-intervention time period (all P > 0.0167).
LPS and Quetiapine Effects on TnF-α and Cortisol Levels
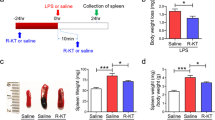
As previously demonstrated by Culley and colleagues, TNF-α levels were not significantly different between LPS-treated groups at 24 h after LPS administration and were similar to placebo animals (Fig. 2a). In contrast, values for cortisol levels were different between groups. LPS-treated animals receiving concurrent administration of quetiapine demonstrated a 5.04 ng/mL reduction in cortisol levels compared to LPS-treated animals (95% CI (−2.92, −7.15) P < 0.001). Furthermore, LPS + Quetiapine group cortisol levels did not significantly differ from Placebo group (95% CI (−0.64, 4.00) P = 0.15) (Fig. 2b).
a, b. Serum TNF-α and cortisol Levels 24 h after intervention. No difference was observed between groups with respect to TNF-α levels. The serum cortisol level of the LPS + Quetiapine group was significantly lower than the LPS + placebo group. No difference was observed between the LPS + Quetiapine and placebo groups with respect to serum cortisol levels. *denotes a p value of between group effect (p < 0.001). c Post-intervention trials to criterion between groups. The y-axis demonstrates trials to criterion (TTC), the number of trials (not including the last five) prior to reaching six consecutive trials on individual discriminations in placebo, LPS + Placebo or LPS + Quetiapine treated groups. LPS + Quetiapine treated rats displayed improved reversal learning compared to LPS + Placebo treated rats. Attentional set shifting (ED) did not differ significantly between LPS + Placebo and LPS + Quetiapine treated rats. The placebo group significantly outperformed both treatment groups in all phases of the attentional set shifting task. * denotes p value of between group effect (p < 0.0167). d Post-intervention errors to criterion between groups. The y-axis quantifies the number of errors, defined as digging behavior in the incorrect reward pot, prior to achieving TTC. LPS treated animals sharply deviated from LPS + Quetiapine treated rats in number of errors at the CD, CD Rev. 1, and ID Rev2 phases. The CD improvement may be indicative of improved discriminative learning by quetiapine treated rats. Though EDRev3 performance was not significant by Bonferroni correction, quetiapine treated rats did have improved performance. *denotes p value of between-group effect (p < 0.0167)
Behavioral Findings
Trials to Criterion between Groups
Data is presented in Fig. 2c. LPS + Quetiapine treated animals demonstrated less TTC at CD Rev1 (mean difference = −11.70; 95% CI (2.57, 20.84) P = 0.016) and ID Rev2 (95% CI (3.21, 16.64) P = 0.007 [0.137]) compared to LPS + Placebo treated animals indicative of improved performance. No difference between LPS + Quetiapine and LPS + Placebo groups was observed in the ED (95% CI (−11.55, 3.27) P = 0.248) or EDRev3 (95% CI (−7.98, 2.82) P = 0.31) phases.
Errors between Groups
Data is presented in Fig. 2d. LPS + Quetiapine treated animals had significantly fewer errors than LPS + Placebo treated animals in the CD (mean difference = −1.68; 95% CI (−2.82, −0.54) P = 0.007), CD Rev1 (mean difference = −2.17; 95% CI (−3.60, −0.73) P = 0.005), ID Rev2 (mean difference = −2.02; 95% CI (−3.07, −0.98) P < 0.001) discriminations. No significant differences in the ED (P = 0.630) or ED Rev3 (P = 0.40) discriminations were observed between these groups.
Non-locomotion between Groups
There were no observed differences in non-locomotion frequency between the LPS + Quetiapine and LPS + Placebo groups in all discriminations (all P > 0.0167). The placebo group had fewer non-locomotion periods in all discriminations compared to the other two groups however this was not statistically significant (all P > 0.0167).
Discussion
In this study of quetiapine in a model of systemic inflammation designed to simulate delirium, we were able to provide some of the first pre-clinical evidence to support the use of quetiapine for the cognitive dysfunction associated with acute delirium. LPS + Quetiapine treated rats demonstrated preserved reversal learning by trials to criterion compared to LPS + Placebo treated rats (CDRev1, IDRev2). In addition, LPS + Quetiapine treated rats compared to LPS + Placebo treated rats showed a reduction in errors to criterion in the CD, CDRev1, and IDRev2 trials. The improvement in CD between groups may demonstrate a beneficial effect on discriminative learning with Quetiapine treatment and this may have contributed to the improvement in reversal learning. Based on the aforementioned lesion studies, this may implicate the orbital prefrontal cortex in the cognitive dysfunction associated with delirium. The orbital prefrontal cortex in the rat is tasked with the integration of spatial working memory, decision making and inhibitory response control (Dalley et al. 2004; Kolb and Gibb 2015). Although primitive in rats, its function correlates with studies in primates and humans. Imaging studies in humans have demonstrated that larger orbital cortex volumes are associated with improved attentional control and reduced perseverative error on the WCST (Nestor et al. 2015; Ohtani et al. 2017) . Due to multiple neurotransmitter effects exerted by quetiapine, the pharmacological mechanism is unclear. Quetiapine demonstrates 5-HT2A antagonism and partial 5-HT1A agonism among other pharmacological properties. Previous observations in primates have demonstrated selective serotonin depletion affects reversal learning but not attentional set shifting in the ASST (Roberts et al. 2005). Quantitative in-vitro receptor autoradiography has suggested that quetiapine increases 5-HT1A, decreases 5-HT2A but exerted minimal effects on dopaminergic receptor density in the frontal cortex, implying that dopaminergic mechanisms are less likely cause of its beneficial effects (Tarazi et al. 2001).
Secondly, we observed that quetiapine exerts a strong effect on cortisol secretion. It is known that older rats demonstrate a more robust neuroinflammatory response to a peripheral immune challenge (Tanaka et al. 2018). This exaggerated and persistent response may result in prolonged cognitive impairment after surgical or systemic insult (Hovens et al. 2016; Kawano et al. 2018). We found a reduction in serum cortisol levels at 24 h in LPS + Quetiapine compared to LPS + Placebo treated rats. This observations corroborates with studies that have documented ACTH and cortisol reduction with the administration of olanzapine and quetiapine in both healthy subjects and patients with major depressive disorder (Cohrs et al. 2006; Nothdurfter et al. 2014). Given that LPS administration has been shown to cause a direct dose-dependent stimulation of cortisol secretion, these findings suggest that quetiapine may have strong inhibitory qualities on the HPA axis (Beishuizen and Thijs 2003; Vakharia and Hinson 2005). Furthermore, we surmise that the cognitive preservation demonstrated by the LPS + Quetiapine group on the ASST may be related to its salutatory effects on cortisol secretion. Clinical associations between hypercortisolemia, cognitive impairment and delirium have been previously documented (Maclullich et al. 2008; Kazmierski et al. 2013, 2014; Sun et al. 2016). The mechanism by which quetiapine exerts these beneficial effects on systemic cortisol secretion are less clear. Quetiapine is a potent noradrenaline (NE) reuptake inhibitor and increases noradrenaline release in the prefrontal cortex via inhibition of the noradrenaline transporter (Pira et al. 2004; Cross et al. 2016). It has been demonstrated that the prefrontal cortex exerts modulatory control on HPA axis activity and the sympathoadrenal system (Diorio et al. 1993; Radley et al. 2006; Myers et al. 2017). Furthermore, it has been observed that the medial prefrontal cortex may exert inhibitory effects on the sympathoadrenal system (Ondicova et al. 2012). Thus, it is reasonable to theorize that quetiapine-mediated NE release in the PFC may exert the observed cortisol suppression via this mechanism, but more evidence is required to support this theory.
Our study did have limitations. Our smaller sample size may have limited our ability to detect some potential differences although we attempted to control for this error using a post-hoc Bonferroni adjustment. Studies utilizing female compared to male animals in the ASST have not demonstrated appreciable sex-related differences, however this study should be repeated in male rats to analyze for gender-related differences (McLean et al. 2008; Alexander et al. 2013). Animals were single-housed based on the recommendation of the institutional veterinarian, we acknowledge that this may have added additional stress on the animals and potentially affected the results of a neurobehavioral study. Future research into other behavioral markers of delirium in rats would strengthen the ASST as an animal model for executive dysfunction in delirium. In addition, it is unclear how long the LPS-mediated deficits persist in the ASST, which may expand the ASST as a model for the observed long-term cognitive impairments associated with acute delirium. Quetiapine has multiple neurotransmitter binding sites therefore further testing quetiapine’s specific receptor targets may elucidate the mechanisms by which it both ameliorates cognitive dysfunction and cortisol suppression. In addition, noradrenergic modulation of the HPA axis is unclear and further studies exploring these mechanisms would improve our understanding of cortisol’s effects on reversal learning and quetiapine’s modulatory role. Finally, finding clinical associations between cortisol and measures of executive function in quetiapine-treated patients with delirium would be useful to confirm our findings.
Conclusion
To our knowledge, we have provided the first pre-clinical observation of quetiapine’s beneficial effects on cognitive flexibility in a neuroinflammatory model designed to mimic delirium. Secondly, we observed that quetiapine exerts strong inhibitory effects on the HPA axis suggesting a role for noradrenergic-mediated cortisol suppression in the treatment of acute delirium. In addition, we believe that this study confirms the utility of the ASST as a model for the study of delirium-related cognitive impairments. Finally, we believe that these findings strengthen the evidence for quetiapine in the treatment of delirium-related cognitive dysfunction.
Data Availability
All data that was generated or analyzed for this series of experiments are included in the published article.
References
Alexander KS, Pocivavsek A, Wu HQ, Pershing ML, Schwarcz R, Bruno JP (2013) Early developmental elevations of brain kynurenic acid impair cognitive flexibility in adults: reversal with galantamine. Neuroscience 238:19–28
Beishuizen A, Thijs LG (2003) Endotoxin and the hypothalamo-pituitary-adrenal (HPA) axis. J Endotoxin Res 9:3–24
Birrell JM, Brown VJ (2000) Medial frontal cortex mediates perceptual attentional set shifting in the rat. J Neurosci 20:4320–4324
Brown VJ, Tait DS (2016) Attentional set-shifting across species. Curr Top Behav Neurosci 28:363–395
Carroll BJ, Curtis GC, Mendels J (1976) Cerebrospinal fluid and plasma free cortisol concentrations in depression. Psychol Med 6:235–244
Choi SH, Lee H, Chung TS, Park KM, Jung YC, Kim SI, Kim JJ (2012) Neural network functional connectivity during and after an episode of delirium. Am J Psychiatry 169:498–507
Cohrs S, Roher C, Jordan W, Meier A, Huether G, Wuttke W, Ruther E, Rodenbeck A (2006) The atypical antipsychotics olanzapine and quetiapine, but not haloperidol, reduce ACTH and cortisol secretion in healthy subjects. Psychopharmacology 185:11–18
Cross AJ, Widzowski D, Maciag C, Zacco A, Hudzik T, Liu J, Nyberg S, Wood MW (2016) Quetiapine and its metabolite norquetiapine: translation from in vitro pharmacology to in vivo efficacy in rodent models. Br J Pharmacol 173:155–166
Culley DJ, Snayd M, Baxter MG, Xie Z, Lee IH, Rudolph J, Inouye SK, Marcantonio ER, Crosby G (2014) Systemic inflammation impairs attention and cognitive flexibility but not associative learning in aged rats: possible implications for delirium. Front Aging Neurosci 6:107
Dalley JW, Cardinal RN, Robbins TW (2004) Prefrontal executive and cognitive functions in rodents: neural and neurochemical substrates. Neurosci Biobehav Rev 28:771–784
Devlin JW, Roberts RJ, Fong JJ, Skrobik Y, Riker RR, Hill NS, Robbins T, Garpestad E (2010) Efficacy and safety of quetiapine in critically ill patients with delirium: a prospective, multicenter, randomized, double-blind, placebo-controlled pilot study. Crit Care Med 38:419–427
Devlin JW, Skrobik Y, Riker RR, Hinderleider E, Roberts RJ, Fong JJ, Ruthazer R, Hill NS, Garpestad E (2011) Impact of quetiapine on resolution of individual delirium symptoms in critically ill patients with delirium: a post-hoc analysis of a double-blind, randomized, placebo-controlled study. Crit Care 15:R215
Devlin JW, Michaud CJ, Bullard HM, Harris SA, Thomas WL (2016) Quetiapine for intensive care unit delirium: the evidence remains weak. Pharmacotherapy 36:e12-e13; discussion e13-14
Diggle P, Heagerty P, Liang K, Zeger SL (2002) Analysis of longitudinal data. Oxford University Press, Oxford
Diorio D, Viau V, Meaney MJ (1993) The role of the medial prefrontal cortex (cingulate gyrus) in the regulation of hypothalamic-pituitary-adrenal responses to stress. J Neurosci 13:3839–3847
Duggan MC, Wang L, Wilson JE, Dittus RS, Ely EW, Jackson JC (2017) The relationship between executive dysfunction, depression, and mental health-related quality of life in survivors of critical illness: results from the BRAIN-ICU investigation. J Crit Care 37:72–79
Girard TD, Pandharipande PP, Ely EW (2008) Delirium in the intensive care unit. Crit care 12(Suppl 3):S3
Girard TD, Jackson JC, Pandharipande PP, Pun BT, Thompson JL, Shintani AK, Gordon SM, Canonico AE, Dittus RS, Bernard GR, Ely EW (2010) Delirium as a predictor of long-term cognitive impairment in survivors of critical illness. Crit Care Med 38:1513–1520
Girshkin L, Matheson SL, Shepherd AM, Green MJ (2014) Morning cortisol levels in schizophrenia and bipolar disorder: a meta-analysis. Psychoneuroendocrinology 49:187–206
Hovens IB, van Leeuwen BL, Mariani MA, Kraneveld AD, Schoemaker RG (2016) Postoperative cognitive dysfunction and neuroinflammation; cardiac surgery and abdominal surgery are not the same. Brain Behav Immun 54:178–193
Inouye SK, Marcantonio ER, Kosar CM, Tommet D, Schmitt EM, Travison TG, Saczynski JS, Ngo LH, Alsop DC, Jones RN (2016) The short-term and long-term relationship between delirium and cognitive trajectory in older surgical patients. Alzheimers Dement: The Journal of the Alzheimer's Association 12:766–775
Kanova M, Sklienka P, Roman K, Burda M, Janoutova J (2017) Incidence and risk factors for delirium development in ICU patients - a prospective observational study. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 161:187–196
Kawano T, Yamanaka D, Aoyama B, Tateiwa H, Shigematsu-Locatelli M, Nishigaki A, Iwata H, Locatelli FM, Yokoyama M (2018) Involvement of acute neuroinflammation in postoperative delirium-like cognitive deficits in rats. J Anesth 32:506–517
Kazmierski J, Banys A, Latek J, Bourke J, Jaszewski R (2013) Cortisol levels and neuropsychiatric diagnosis as markers of postoperative delirium: a prospective cohort study. Crit Care 17:R38
Kazmierski J, Banys A, Latek J, Bourke J, Jaszewski R, Sobow T, Kloszewska I (2014) Mild cognitive impairment with associated inflammatory and cortisol alterations as independent risk factor for postoperative delirium. Dement Geriatr Cogn Disord 38:65–78
Kolb B, Gibb R (2015) Plasticity in the prefrontal cortex of adult rats. Front Cell Neurosci 9:15
Maclullich AM, Ferguson KJ, Miller T, de Rooij SE, Cunningham C (2008) Unravelling the pathophysiology of delirium: a focus on the role of aberrant stress responses. J Psychosom Res 65:229–238
McAlonan K, Brown VJ (2003) Orbital prefrontal cortex mediates reversal learning and not attentional set shifting in the rat. Behav Brain Res 146:97–103
McLean SL, Beck JP, Woolley ML, Neill JC (2008) A preliminary investigation into the effects of antipsychotics on sub-chronic phencyclidine-induced deficits in attentional set-shifting in female rats. Behav Brain Res 189:152–158
Morandi A, Rogers BP, Gunther ML, Merkle K, Pandharipande P, Girard TD, Jackson JC, Thompson J, Shintani AK, Geevarghese S, Miller RR 3rd, Canonico A, Cannistraci CJ, Gore JC, Ely EW, Hopkins RO (2012) The relationship between delirium duration, white matter integrity, and cognitive impairment in intensive care unit survivors as determined by diffusion tensor imaging: the VISIONS prospective cohort magnetic resonance imaging study*. Crit Care Med 40:2182–2189
Munster BC, Aronica E, Zwinderman AH, Eikelenboom P, Cunningham C, Rooij SE (2011) Neuroinflammation in delirium: a postmortem case-control study. Rejuvenation Res 14:615–622
Myers B, McKlveen JM, Morano R, Ulrich-Lai YM, Solomon MB, Wilson SP, Herman JP (2017) Vesicular glutamate transporter 1 knockdown in Infralimbic prefrontal cortex augments neuroendocrine responses to chronic stress in male rats. Endocrinology 158:3579–3591
National Research Council (US) (2011) Committee for the update of the guide for the care and Use of laboratory animals. National Academies Press (US), Washington, DC
Nestor PG, Nakamura M, Niznikiewicz M, Levitt JJ, Newell DT, Shenton ME, McCarley RW (2015) Attentional control and intelligence: MRI orbital frontal gray matter and neuropsychological correlates. Behav Neurol 2015:354186
Nikiforuk A (2013) Quetiapine ameliorates stress-induced cognitive inflexibility in rats. Neuropharmacology 64:357–364
Nikiforuk A, Popik P (2012) Effects of quetiapine and sertindole on subchronic ketamine-induced deficits in attentional set-shifting in rats. Psychopharmacology 220:65–74
Nothdurfter C, Schmotz C, Sarubin N, Baghai TC, Laenger A, Lieb M, Bondy B, Rupprecht R, Schule C (2014) Effects of escitalopram/quetiapine combination therapy versus escitalopram monotherapy on hypothalamic-pituitary-adrenal-axis activity in relation to antidepressant effectiveness. J Psychiatr Res 52:15–20
Ohtani T, Nestor PG, Bouix S, Newell D, Melonakos ED, McCarley RW, Shenton ME, Kubicki M (2017) Exploring the neural substrates of attentional control and human intelligence: diffusion tensor imaging of prefrontal white matter tractography in healthy cognition. Neuroscience 341:52–60
Ondicova K, Kvetnansky R, Mravec B (2012) Medial prefrontal cortex transection enhanced stress-induced activation of sympathoadrenal system in rats. Endocr Regul 46:129–136
Pandharipande PP, Girard TD, Jackson JC, Morandi A, Thompson JL, Pun BT, Brummel NE, Hughes CG, Vasilevskis EE, Shintani AK, Moons KG, Geevarghese SK, Canonico A, Hopkins RO, Bernard GR, Dittus RS, Ely EW (2013) Long-term cognitive impairment after critical illness. N Engl J Med 369:1306–1316
Pira L, Mongeau R, Pani L (2004) The atypical antipsychotic quetiapine increases both noradrenaline and dopamine release in the rat prefrontal cortex. Eur J Pharmacol 504:61–64
Popik P, Nikiforuk A (2015) Attentional set-shifting paradigm in the rat. Curr Protoc Neurosci 72:9.51.51–9.51.13
Qin L, Wu X, Block ML, Liu Y, Breese GR, Hong JS, Knapp DJ, Crews FT (2007) Systemic LPS causes chronic neuroinflammation and progressive neurodegeneration. Glia 55:453–462
Radley JJ, Arias CM, Sawchenko PE (2006) Regional differentiation of the medial prefrontal cortex in regulating adaptive responses to acute emotional stress. J Neurosci 26:12967–12976
Roberts HFC, Walker SC, Crofts HS, Dalley JW, Robbins TW, Roberts AC (2005) Prefrontal serotonin depletion affects reversal learning but not attentional set shifting. J Neurosci 25(2):532–538
Shioiri A, Kurumaji A, Takeuchi T, Matsuda H, Arai H, Nishikawa T (2010) White matter abnormalities as a risk factor for postoperative delirium revealed by diffusion tensor imaging. Am J Geriatr Psychiatry 18:743–753
Shioiri A, Kurumaji A, Takeuchi T, Nemoto K, Arai H, Nishikawa T (2016) A decrease in the volume of gray matter as a risk factor for postoperative delirium revealed by an atlas-based method. Am J Geriatr Psychiatry 24:528–536
Stollings JL, Wilson JE, Jackson JC, Ely EW (2016) Executive dysfunction following critical illness: exploring risk factors and management options in geriatric populations. Curr Behav Neurosci Rep 3:176–184
Sun L, Jia P, Zhang J, Zhang X, Zhang Y, Jiang H, Jiang W, Guo Y (2016) Production of inflammatory cytokines, cortisol, and Abeta1-40 in elderly oral cancer patients with postoperative delirium. Neuropsychiatr Dis Treat 12:2789–2795
Tanaka N, Cortese GP, Barrientos RM, Maier SF, Patterson SL (2018) Aging and an immune challenge interact to produce prolonged, but not permanent, reductions in Hippocampal L-LTP and mBDNF in a rodent model with features of delirium. eNeuro 5(3). https://doi.org/10.1523/ENEURO.0009-18.2018
Tarazi FI, Zhang K, Baldessarini RJ (2001) Long-term effects of olanzapine, risperidone, and quetiapine on dopamine receptor types in regions of rat brain: implications for antipsychotic drug treatment. J Pharmacol Exp Ther 297:711–717
Vakharia K, Hinson JP (2005) Lipopolysaccharide directly stimulates cortisol secretion by human adrenal cells by a cyclooxygenase-dependent mechanism. Endocrinology 146:1398–1402
Westhoff D, Witlox J, Koenderman L, Kalisvaart KJ, de Jonghe JF, van Stijn MF, Houdijk AP, Hoogland IC, Maclullich AM, van Westerloo DJ, van de Beek D, Eikelenboom P, van Gool WA (2013) Preoperative cerebrospinal fluid cytokine levels and the risk of postoperative delirium in elderly hip fracture patients. J Neuroinflammation 10:122
Funding
This work was supported by internal funding from the Penn State Health Milton S. Hershey Medical Center Department of Anesthesiology & Perioperative Medicine (Study #47992).
Author information
Authors and Affiliations
Contributions
Conceived and designed experiments: ZJC, LM, VRV.
Analysis and interpretation of the data: ZJC, ARK, VRV, KK.
Wrote the manuscript: ZJC, ARK, VRV, KK.
Data acquisition: ZJC, LM.
Corresponding author
Ethics declarations
Ethics Approval
The experimental design was approved by the Penn State College of Medicine IACUC. All procedures adhered to the guidelines in the Principles of Laboratory Animal Care (National Institutes of Health, Eighth Ed., National Academies Press, 2011).
Consent for Publication
Not applicable.
Conflict of Interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Carr, Z.J., Miller, L., Ruiz-Velasco, V. et al. In a Model of Neuroinflammation Designed to Mimic Delirium, Quetiapine Reduces Cortisol Secretion and Preserves Reversal Learning in the Attentional Set Shifting Task. J Neuroimmune Pharmacol 14, 383–390 (2019). https://doi.org/10.1007/s11481-019-09857-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-019-09857-y