Abstract
mRNA encoding for the CB2 cannabinoid receptor is expressed by many subsets of human peripheral blood leukocytes (PBL), but little is known about the resulting protein expression and function. Employing clones from the A549 and 293T cell lines that were constructed to express both full-length human CB2 and GFP, we developed a flow cytometry assay for characterizing CB2 protein expression. A monoclonal antibody directed against human CB2 selectively stained the surface of transduced but not parental cell lines. When cells were fixed and permeabilized, imaging flow cytometry identified large stores of intracellular protein. Total cellular staining for CB2 corresponded closely with the level of GFP expression. When exposed to Δ9-tetrahydrocannabinol, CB2-expressing cells internalized cell surface CB2 receptors in a time- and dose-dependent manner. Applying these approaches to human PBL, CB2 protein was identified on the surface of human B cells but not on T cells or monocytes. In contrast, when PBL were fixed and permeabilized, intracellular CB2 expression was readily detected in all three subsets by both conventional and imaging flow cytometry. Similar to the protein expression pattern observed in fixed and permeabilized PBL, purified B cells, T cells, and monocytes expressed relatively equal levels of CB2 mRNA by quantitative real-time RT-PCR. Our findings confirm that human PBL express CB2 protein but that its distribution is predominantly intracellular with only B cells expressing CB2 protein at the extracellular membrane. The differential role of intracellular and extracellular CB2 receptors in mediating ligand signaling and immune function remains to be determined.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
While the use of Cannabis (marijuana) for medicinal, religious, and recreational purposes dates back 5,000 years, the identification of cannabinoids and the discovery of an endogenous cannabinoid ligand and receptor signaling pathway in human cells represents a relatively recent discovery (Mechoulam 1986; Pertwee 2006). Cannabinoid receptor subtype 1 (CB1) is highly expressed in the brain and well known for mediating the psychoactive effects of marijuana, while the highest expression of mRNA encoding for cannabinoid receptor subtype 2 (CB2) exists in peripheral tissues and particularly within cells of the immune system (Basu and Dittel 2011; Bouaboula et al. 1993; Galiègue et al. 1995; Munro et al. 1993). Both receptors are membrane-associated G-protein coupled receptors (GPCR) and bind Δ9-tetrahydrocannabinol (THC) with relatively equal affinity (Munro et al. 1993; Shire et al. 1996). However, a number of other ligands have been identified, which express high selectivity for CB2 (Pertwee 2006). Using these reagents, it has been shown that activation of CB2 receptor can regulate both innate and adaptive immunity including the ability to suppress anti-cancer responses (McKallip et al. 2005; Zhu et al. 2000) and host defenses against pneumonia (Klein et al. 2000; Newton et al. 2009; Shay et al. 2003), promote apoptosis of antigen presenting cells and T cells (Do et al. 2004; McKallip et al. 2002), alter cytokine production and antibody isotype switching (Agudelo et al. 2008; Cencioni et al. 2010; Srivastava et al. 1998; Yuan et al. 2002), modulate the infectivity and replication of HIV virus (Gorantla et al. 2010; Roth et al. 2005), regulate the inflammatory aspects of atherosclerosis (Mach and Steffens 2008), and play a role in several autoimmune diseases (Malfait et al. 2000; Sipe et al. 2005). This body of work has lead to considerable interest in understanding the role that endogenous cannabinoids have in the immune system and in developing CB2-selective therapies (Klein 2005; Mackie 2006). However, the direct examination of CB2 protein on human cells has been limited by an inability to reliably detect and quantitate receptor protein. While mRNA profiles have suggested that there is differential expression of CB2 by B cells, T cells, and other leukocyte subsets, there have been very few studies evaluating differences in protein expression or cellular distribution. The current research focuses on the development and validation of a flow cytometry approach for measuring and tracking CB2 receptor protein in human cells. The findings provide a flexible method for receptor study in primary cells and new insights regarding the differential expression of CB2 receptors at intracellular versus extracellular locations in human B cells, T cells, and monocytes.
Methods
Primary cells and cell lines
Following informed consent, peripheral blood leukocytes (PBL) were isolated by Ficoll-gradient centrifugation from the blood of healthy human donors. Cell subsets were identified by flow cytometry using fluorescent-labeled monoclonal antibodies (mAb) directed against B cells (anti-CD20, BD Biosciences, San Jose, CA), T cell subsets (anti-CD3, Invitrogen, Camarillo, CA or in combination with anti-CD4 or anti-CD8, BD Biosciences), and monocytes (anti-CD13, Invitrogen). Purified subsets were prepared from primary PBL using lineage-specific mAb and magnetic nanoparticles (StemCell Technologies, B.C., Canada). Purities for each subset were confirmed by flow cytometry.
The human embryonic kidney cell line 293T and lung cancer epithelial cell line A549 (ATCC, Manassas, VA) were maintained in culture as adherent monolayers in complete medium composed of DMEM or RPMI-1640, respectively (Cellgro, Manassas, VA), supplemented with 10 % fetal bovine serum (Omega Scientific, Tarzana, CA) and antibiotics. The 293T/CB2-GFP and A549/CB2-GFP cell lines were constructed by transducing the corresponding parental lines with a self-inactivating lentivirus expressing full-length human CB2 receptor cDNA and green fluorescent protein (GFP) as previously described (Sarafian et al. 2008). Expression of CB2 was regulated by a hCMV promoter with the expression of GFP linked through an internal ribosomal entry site. Transduced cells were sorted by flow cytometry (FACSVantage SE cell sorter, Becton Dickinson, San Jose, CA) for GFP-expressing clones, and aliquots of the expanded cell lines were cryopreserved for subsequent use.
Δ9-tetrahydrocannabinol (THC)
A 50 mg/ml stock of THC in ethanol was obtained from the National Institute on Drug Abuse (Bethesda, MD) and immediately prior to use was diluted serially in DMSO and culture medium to produce a final ethanol concentration in assays of 0.01 % (v/v) and DMSO concentration at ≤0.25 % (v/v). Diluent controls were prepared using the same dilution strategies with ethanol and DMSO that did not contain THC.
Detection of extracellular CB2 receptor
Adherent cell lines were treated with 0.1 % trypsin (Cellgro) for 1 min, quenched with 10 % fetal bovine serum, and then washed with phosphate-buffered saline (PBS) containing 0.2 mg/ml EDTA (Invitrogen, Carlsbad, CA) to produce a single cell suspension. Extracellular CB2 was detected by pre-treating with 50 μl human AB Serum (Omega Scientific) for 1 min followed by a 30 min incubation on ice with unlabeled primary mouse IgG2 mAb directed against either human CB2 (clone #352114, 0.5 μg/tube, R&D System, Minneapolis, MN) or isotype-matched mAbs against an irrelevant antigen, mouse NK1.1 (clone #PK136, 0.5 μg/tube, BD Biosciences) or mouse Thy1.2 (clone #30-H12, 0.5 μg/tube, BD Biosciences). After washing twice with PBS/2 % AB serum, cells were incubated with an APC-labeled goat anti-mouse F(ab’)2 mAb (APC-labeled GAM, 0.5 μg/tube, Invitrogen) for 30 min on ice. To identify different PBL subsets, cells were incubated with lineage-specific fluorescent-labeled mAb for 20 min and washed. All cells were then fixed and incubated with 1 % paraformaldehyde for 20 min at 4 °C and washed. The cells were covered to protect from light and stored at 4 °C until analyzed.
Detection of total cellular CB2 expression
In order to detect intracellular CB2 receptor, single cell suspensions of either PBL or indicated cell lines were fixed with 1 % paraformaldehyde (Sigma Aldrich, St. Louis, MO) and treated with permeabilizing solution (BD Biosciences). Cells were washed once with PBS/2 % AB serum, resuspended in permeabilizing solution, and blocked with 50 μl human AB serum. Staining with primary unlabeled mAb (against CB2, NK1.1, or Thy1.2) and secondary APC-labeled GAM were carried out as detailed in the extracellular staining protocol except that incubation times were prolonged to 60 min on ice. After washing, PBL were further stained with fluorescent-labeled antibodies directed against lineage-specific markers and then fixed again with 1 % paraformaldehyde prior to storage and analysis.
Conventional and imaging flow cytometry
Conventional multiparameter flow cytometry was carried out using a FACScan II-plus cytometer (BD Biosciences) with the acquisition of 5,000–30,000 events depending upon the assay conditions. Analysis of acquired data was performed using FCS Express V3 software (De Novo Software, Los Angeles, CA). Flow cytometry results are presented as histograms or two-parameter dot plots with indicated values representing the mean linear fluorescence intensity (MFI) of the gated population. Fluorescent images were acquired using an ImageStreamX® cytometer (Amnis Corporation, EMD Millipore, Seattle, WA) capable of simultaneously acquiring high resolution digital images at up to 60X magnification, in each of 12 channels, as cells pass through the cytometer’s detection chamber. Analysis was performed using IDEAS Software (Amnis Corporation) in which image display characteristics were first optimized for background and range of fluorescent intensity and then applied equally to all image within an analysis set. Gates were set to display representative cell images expressing the mean fluorescent intensity for each analysis channel. Internalization scores were derived using an eroded-pixel mask generated from the bright field image to determine the ratio of intracellular to extracellular signal for each marker of each cell.
CB2 receptor internalization assay
Single cell suspensions of 293T/CB2-GFP cells were suspended in X-VIVO media (Lonza, Walkersville, MD) and after incubating with THC or diluents alone under different conditions (of concentration and time), the reactions were quenched with ice-cold PBS. Cells were then stained to determine the residual expression of extracellular CB2 as already described. Alternatively, the trafficking of fluorescent-labeled extracellular CB2 was assessed using the imaging cytometer. 293T/CB2-GFP cells were first stained with anti-CB2 mAb and APC-labeled GAM, washed to remove excess antibodies, and then antibody-stained cells were incubated with either diluent alone or 8 μM THC at 37 °C for 40 min. At the completion of the incubation period, cells were fixed with 1 % paraformaldehyde and 3,000–5,000 cell events of interest acquired using the ImageStreamX® cytometer.
Quantitative real-time RT-PCR
cDNA was prepared directly from 2 × 105 whole PBL or purified B cell, T cell, and monocyte subsets using a FastLane cDNA kit (QIAGEN, Valencia, CA). qRT-PCR analysis was performed in batch with three replicates/sample using a StepOne real-time PCR system (Applied Biosystems, Foster City, CA) and labeled probes for CB2 and a housekeeping gene, GAPDH (both from Applied Biosystems). Relative expression of CB2 mRNA was corrected for GAPDH and represented as the average 1/Δ-CT values obtained from triplicate wells.
Statistics
Individual conditions were assayed in triplicate within an experiment and a minimum of three replicate experiments carried out for each assay. Flow cytometry histograms and dot-plots display results from a single representative tube of a single experiment. All other data are presented as means of replicate tubes or experiments as detailed. The difference between means was determined using a Student’s t-test with a p < 0.05 accepted as statistically significant.
Results
Anti-CB2 mAb detects cell membrane expression of CB2 receptor
The A549 and 293T cell lines and their transduced clones expressing human CB2 and GFP were used to optimize a flow cytometry assay for measuring cell surface CB2. Isotype-matched mAbs directed against irrelevant antigens (mouse NK1.1 and Thy1.2) were also employed to assess background staining and specificity. As demonstrated by results from a representative flow cytometry experiment in Fig. 1, no CB2-specific staining was observed when A549 cells (or 293T cells, data not shown) were stained with anti-CB2 mAb. However, there was a clear fluorescent signal when anti-CB2 mAb was used to stain the surface of A549/CB2-GFP cells (MFI = 29.6 ± 2.1 for CB2 vs 5.6 ± 2.5 for NK1.1, p < 0.05, averaged results from 3 experiments) and a much brighter signal when used to stain 293T/CB2-GFP cells (MFI = 871.2 ± 19.2 for CB2 vs 7.1 ± 0.9 for NK1.1, p < 0.05, averaged results from 3 experiments). Assessing GFP expression as an independent measure of transgene expression by these two cell lines confirmed the relatively low expression by A549/CB2-GFP cells and the much higher expression by 293T/CB2-GFP cells.
Anti-CB2 mAb detects cell membrane expression of CB2 receptor. Parental cell lines (A549 and 293T; data shown only for A549) and stable clones expressing both CB2 and GFP (A549/CB2-GFP and 293T/CB2-GFP) were incubated with a primary unlabeled mAb against CB2 protein or an isotype-matched irrelevant target (anti-mouse NK1.1 or Thy1.2) and then stained with APC-labeled GAM. Representative experiment shown, n = 3. (a) Cells were analyzed by flow cytometry for APC fluorescence and mean fluorescent intensities (MFI) for CB2-stained cells indicated for each condition. Black fill = unstained cells; white fill = isotype controls; shaded fill = CB2 stained. (b) Corresponding GFP expression with net MFI values shown
Cell permeabilization exposes intracellular CB2 protein
While GPCR are integral membrane proteins, there has been increasing interest in their expression and function at sites other than the extracellular membrane (Jean-Alphonse and Hanyaloglu 2011). Cells were therefore probed for the expression of intracellular CB2 protein by adding fixation and permeabilization steps to our standard flow cytometry protocol (Fig. 2). While surface staining of viable 293T/CB2-GFP cells revealed high levels of CB2 expression, there was a 50 to 60 % drop in fluorescent intensity when cells were stained after fixation and permeabilization suggesting an impact of the fixation process on antigen-antibody binding affinity. As a result, fluorescent intensity values could not be used to directly compare the levels of extracellular to intracellular protein. Imaging flow cytometry was therefore employed to localize antibody binding sites. As demonstrated in Fig. 2a, imaging of 293T/CB2-GFP cells that were stained with anti-CB2 mAb using the extracellular protocol revealed an intense rim of fluorescence associated with the extracellular membrane. However, when the same cells were stained following fixation and permeabilization, an entirely different CB2 expression pattern emerged (Fig. 2b). Rather than an intense rim of membrane fluorescence, the majority of the CB2 signal was associated with the cytoplasmic compartment.
Cell permeabilization exposes intracellular CB2 protein. For each condition, a representative dot-plot from conventional flow cytometry is shown (MFI indicated) followed by image sets obtained from two representative cells captured by imaging flow cytometry. Images were selected from cells expressing the mean GFP expression and mean CB2 or NK1.1 expression, respectively. Bright field (BF), GFP fluorescence, APC fluorescence, and merged fluorescence images are shown. (a) For assessing extracellular CB2 protein, viable 293T/CB2-GFP cells were incubated at 4 °C for 30 min with 0.25 μg of CB2 mAb (top panel) or 0.25 μg of an isotype control mAb, NK1.1 (bottom panel), washed, and then incubated with APC-labeled GAM for detection. (b) For assessing total cellular CB2 expression, 293T/CB2-GFP cells were fixed and permeabilized prior to staining at 4 °C for 60 min with 0.5 μg of CB2 mAb (top panel) or 0.5 μg of an isotype control, NK1.1 (bottom panel) followed by detection with APC-labeled GAM
CB2 receptor internalization and trafficking following exposure to THC
In order to assess trafficking between extracellular and intracellular CB2 receptors, we employed two complementary approaches to assess for ligand-induced receptor internalization. Using the 293T/CB2-GFP cell line as a model, we assessed changes in expression of extracellular CB2 in response to treatment with THC. Incubating cells with a 4 μM concentration of THC for up to 80 min at 37 °C was associated with a time-dependent decrease in cell surface CB2 expression (Fig. 3a). Similarly, exposing cells for 40 min (at 37 °C) to increasing concentrations of THC from 0 to 8 μM resulted in a concentration-dependent decrease in surface staining by anti-CB2 mAb (Fig. 3b). THC-dependent changes did not occur when cells were maintained at 4 °C (data not shown) confirming an energy-dependent process.
CB2 receptor internalization and trafficking following exposure to THC. Viable 293T/CB2-GFP cells were incubated in X-VIVO media at 37 °C with (a) 4 μM THC for different time intervals or (b) with increasing concentrations of THC (0–8 μM) for 40 min. After the defined incubations, reactions were quenched with excess ice-cold PBS, cells incubated with 0.25 μg of CB2 or NK1.1 mAb for 30 min on ice, and then stained with APC-labeled GAM for detection. Data for both assays are expressed as the percentage of baseline expression (MFI), which was obtained from cells maintained at 4 °C with exposure to diluent alone throughout the entire assay. Graphs display the mean (± SE) for three independent experiments, each performed in triplicate. c Imaging flow cytometry was also employed to assess CB2 receptor internalization. Cells were first incubated at 4 °C with CB2 or NK1.1 mAb, followed by APC-labeled GAM for detection, and then exposed to either diluent control (top panel) or 8 μM THC (bottom panel) for 40 min at 37 °C. Reactions were then quenched with excess cold PBS, cells fixed, and analyzed within 48 h by imaging flow cytometry. Image sets were obtained from two representative cells expressing the mean levels of GFP and CB2 expression. Bright field (BF), GFP fluorescence, APC fluorescence, and merged fluorescence images are shown
In a second approach, imaging flow cytometry was used to assess the impact of THC exposure on receptor location (Fig. 3c). Viable 293T/CB2-GFP cells were stained with anti-CB2 mAb and secondary APC-labeled GAM and then incubated at 37 °C with either 8 μM THC or diluent alone for 40 min. While conventional flow cytometry demonstrated no change in overall fluorescent signal (data not shown), fluorescent imaging demonstrated trafficking and coalescence of the fluorescent signal within the cytoplasm in response to THC. Cells labeled with anti-CB2 mAb and incubated at 37 °C, in the absence of THC, did show evidence of antibody-induced capping and early vacuolization, but extensive trafficking and coalescence of the CB2 label within the cytoplasm occurred only in the presence of THC. This visual assessment was confirmed by using quantitative measurement of the intracellular to extracellular fluorescent ratios for the two conditions, which demonstrated a significant intracellular shift in response to THC.
Distribution of CB2 expression in peripheral blood leukocytes (PBL)
Having validated the capacity for flow cytometry to assess cell surface and total cellular CB2 expression in cell lines, we assessed whether this approach could detect CB2 expression in primary human PBL. Blood samples were obtained from healthy non-smoking subjects in order to avoid any impact of exogenous THC exposure on receptor expression. As demonstrated in Fig. 4a, cell surface staining with the anti-CB2 mAb was only observed in B cells. There was no difference in fluorescence staining between the anti-NK1.1 and anti-CB2 mAb when T cells (including both the CD4 and CD8 subsets; data not shown) and monocytes were examined.
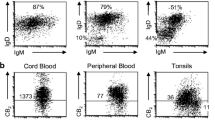
Distribution of CB2 expression in peripheral blood leukocytes (PBL). PBL were purified by density gradient centrifugation, washed, and then stained while still viable for (a) detection of extracellular CB2 +or (b) following fixation and permeabilization for detection of total cellular CB2 expression as previously described in Fig. 2, followed by counterstaining with lineage-specific fluorescent-conjugated antibodies for detection of CD20+ B cells (top), CD3+ T cells (middle), and CD13+ monocytes (bottom). MFI values for each population are listed. Representative experiment is shown, n = 4
However, the CB2 expression pattern was entirely different after fixation and permeabilization (Fig. 4b). In addition to B cells, a fluorescent signal for CB2 was detected in all T cells and monocytes. In contrast to studies with 293T/CB2-GFP cells where fixation and permeabilization was associated with a decrease in the MFI for CB2 staining, there was a marked increase in CB2 fluorescent intensity when B cells were stained after fixation and permeabilization. This finding would suggest that a much higher percentage of CB2 protein is expressed in the cytoplasm of B cells as compared to expression on the cell surface. Furthermore, while T cells failed to exhibit any CB2 expression on their cell surface, they exhibited high levels of intracellular fluorescence. Intracellular staining of monocytes was also consistently positive for cytoplasmic CB2 protein, and there were no consistent differences in the level of expression between B cells, T cells, and monocytes. The fluorescent staining intensity exhibited by these different subsets, broken down into cell surface staining and total cellular staining, are summarized in Table 1. Visual confirmation of antibody binding location was obtained using the ImageStreamX® imaging cytometer (Fig. 5). As in our cell lines, intracellular staining revealed diffuse cytoplasmic staining in B cells, T cells, and monocytes. There was no fluorescent signal when cells were stained with anti-NK1.1 mAb.
Fluorescent imaging confirms differential staining pattern in human PBL subsets. a Viable or (b) fixed and permeabilized human PBL that had been stained as detailed in Fig. 4 were fixed with 1 % paraformaldehyde and analyzed by imaging flow cytometry within 48 h. Gating was used to select for CD20+ B cells (top panels), CD3+ T cells (middle panels), and CD13+ monocytes (bottom panels) with image sets shown from two representative cells captured by imaging flow cytometry. Images were selected from cells expressing the mean GFP and mean CB2 expression for each gated population. Bright field (BF), GFP fluorescence, APC fluorescence, and merged fluorescence images are shown
As had been observed when cells from the 293T/CB2-GFP line were exposed to THC, the extracellular expression of CB2 by CD20+ B cells was also down-regulated when PBMC were exposed to THC in the range of 0.5 to 2.0 μM (results not shown). No change was observed for monocytes or T cells, which did not demonstrate extracellular CB2 staining under any conditions.
Quantitative real-time RT-PCR confirms the expression of CB2 mRNA which correlates with total cellular CB2 protein levels
Expression of CB2 protein by flow cytometry was correlated with mRNA expression using a quantitative real-time RT-PCR assay. Labeled probes for CB2 and a housekeeping gene, GAPDH, were quantitated simultaneously in the same well, allowing the relative level of CB2 expression to be described by the relative differences in cycle times (1/Δ-CT). Immunomagnetic selection was used to isolate B cell, T cell, and monocyte subsets with purity confirmed by flow cytometry at an average of 83.2 ± 5.3 % for B cells, 96.5 ± 3.5 % for T cells, and 94.5 ± 2.4 % for monocytes (Fig. 6a–b, n = 4 separations). Similar to the results for total cellular CB2 expression, all of these subsets expressed similar levels of CB2 mRNA with no statistically-significant difference noted between groups (Fig. 6c).
CB2 mRNA levels from purified human B cells, T cells, and monocytes. a Human PBL isolated by density gradient centrifugation and analyzed with lineage-specific markers to identify the B cell, T cell, and monocyte subsets, and their respective percentages within the entire PBL sample. b Each subset was then individually purified by immunomagnetic depletion with the final purity determined by flow cytometry using lineage-specific makers. Dot plots are from a representative experiment with the average purity from 5 different isolations being 83.2 ± 5.3 % for B cells, 96.5 ± 3.5 % for T cells, and 94.5 ± 2.4 % for monocytes. c cDNA was prepared from 2 × 105 PBL or the purified subsets using a FastLane cDNA kit and quantitative real-time RT-PCR for all cells isolated from a single donor carried out in triplicate using labeled probes for CB2 and GAPDH. Relative expression of CB2 between groups is displayed as 1/Δ-CT representing average data from triplicate determinations for 3 different normal donors. No significant differences were identified between groups
Discussion
The CB2 gene was cloned from a human leukemia cell line in 1993 and found to encode for a GPCR that bound cannabinoids with high affinity, but unlike CB1, it was expressed primarily in lymphoid organs by lymphocytes, monocytes, and polymorphonuclear cells (Bouaboula et al. 1993; Galiègue et al. 1995; Munro et al. 1993; Schatz et al. 1997). The functional consequences of cannabinoids on immunity have turned out to be extensive with the capacity to regulate chemotaxis, phagocytosis, bacterial killing, antigen processing and presentation, T cell activation and cytokine production, and B cell differentiation and isotype switching (Basu and Dittel 2011; Klein 2005; Klein and Cabral 2006). This has led to considerable interest in developing therapeutic drugs based on their interaction with CB2 receptor (Guindon and Hohmann 2008; Klein 2005; Mackie 2006). However, there is relatively little information regarding the expression and distribution of CB2 protein on target cells. In this study, we constructed cell lines expressing different levels of human CB2 and used a commercial anti-CB2 mAb to develop a sensitive and specific flow cytometry assay for detecting CB2 protein. This mAb was developed using gene-modified cells expressing full length human CB2 as the immunogen. It readily detects CB2 expressed on the cell membrane, and in our hands, cell staining was not blocked by pre-incubation with a 50-mer N-terminal peptide (results not shown), suggesting that it may be directed against one of the extracellular loops of the GPCR structure. With its high throughput and the capacity for multiplexing, this assay should provide an important tool for probing CB2 receptor status in cells of interest. More importantly, with the addition of cell permeabilization and imaging flow cytometry, our findings challenge the longstanding notion that CB2 functions primarily as a cell surface receptor (Basu and Dittel 2011; Dainese et al. 2010). GPCR have the capacity to traffic between different cell compartments where they can interact with different adaptor proteins and signaling pathways (Jean-Alphonse and Hanyaloglu 2011). When examining primary human B cells, our studies identified CB2 protein at both extracellular and intracellular locations. However, while B cells, T cells, and monocytes expressed similar levels of CB2 mRNA, CB2 protein expression was restricted entirely to intracellular sites in T cells and monocytes. In an analogous manner, a number of research groups have recently described a primary intracellular distribution of CB1 protein within different sets of neurons (Rozenfeld 2011). Cannabinoids are highly lipophilic molecules, and it has been shown that both extracellular and intracellular CB1 receptors can mediate signaling and biologic responses when exposed to ligands (Brailoiu et al. 2011; Rozenfeld 2011; Thomas et al. 1990). Others have also recently begun to evaluate CB2 receptor internalization and trafficking (Atwood et al. 2012; Grimsey et al. 2011). Using gene-modified cell lines and epitope-tagged CB2 molecules, a complex relationship between CB2 ligand exposure, receptor internalization, and cell signaling has been reported (Atwood et al. 2012). In this setting, our results suggest a similar paradigm for the expression of native human CB2 by PBL and make it likely that the differential expression of CB2 at extracellular and intracellular sites plays an important role in the immune responses to cannabinoids. This differential expression of CB2 may also be linked to the variety of signaling pathways that have been associated with CB2 activation (Howlett 2005).
While others have used flow cytometry to evaluate CB2 receptor expression on cells (Carayon et al. 1998; Cencioni et al. 2010; Graham et al. 2010), there are several features which distinguish our assay from past studies with human PBL. Carayon and associates (Carayon et al. 1998) generated and purified polyclonal rabbit anti-CB2 antibody directed against the C-terminal (intracellular tail portion) of human CB2. As fixation and permeabilization were required for antigen detection, their approach precluded a comparison between extracellular and intracellular staining. A fluorescent signal was detected from stained B cells and was inhibited by excess peptide, but the findings were much less convincing with respect to the staining of other cell types. More recently, Graham and coworkers (Graham et al. 2010) evaluated polyclonal antibodies from several commercial manufacturers and reported that human B cells, T cells, monocytes, NK cells, and polymorphonuclear cells all express high levels of extracellular CB2. However, the staining patterns in their report were highly-variable from manufacturer to manufacturer and from batch to batch. Furthermore, in the absence of appropriate control antibodies or the inclusion of known positive and negative controls, one cannot really draw conclusions about sensitivity and specificity. Based on these concerns we focused on a defined mAb with the ability to detect extracellular CB2 expression. In order to optimize and validate staining patterns, we constructed cell lines expressing defined levels of human CB2 (A549/CB2-GFP and 293T/CB2-GFP) and compared staining patterns to those observed with parental cells (A549 and 293T). During the optimization process, it was obvious that non-specific background staining could easily be mistaken for receptor expression if antibodies were not carefully titrated and appropriate isotype controls employed. By including the expression of a linked GFP reporter gene in our vector construct, we also possessed a mechanism for independently assessing expected CB2 staining patterns. Perhaps the most important technical advancement was the inclusion of both intracellular and extracellular staining protocols. In this respect, our studies were also aided by the use of an ImageStreamX® cytometer. Due to the impact of fixation and permeabilization on antibody staining, we could not use MFI to directly compare extracellular and intracellular protein levels by conventional flow cytometry. However, visual inspection of captured images readily identified the cytoplasmic compartment as the primary source of our CB2 signal. Imaging also allowed us to independently confirm the process of receptor internalization in response to ligand exposure. Given the controls and approaches employed, there should be little doubt regarding the performance characteristics of this flow cytometry approach.
In summary, we describe a rapid and flexible approach for detecting and localizing human CB2 protein expression in cell lines and primary human cells. This approach uses commercially available reagents and should have wide applicability. In addition, for the first time, we report that CB2 receptor is primarily located at intracellular sites in PBL and that expression is not limited to the cell membrane as previously thought. Even in B cells, which express both extracellular and intracellular CB2, the majority of receptor protein is located within the cell. Our findings and related investigations carried out with CB2 suggest that there is trafficking between receptor locations and that intracellular receptors are likely to be biologically active. Future studies focused on understanding the role of differential CB2 receptor location on cannabinoid function are warranted.
References
Agudelo M, Newton C, Widen R, Sherwood T, Nong L, Friedman H, Klein TW (2008) Cannabinoid receptor 2 (CB2) mediates immunoglobulin class switching from IgM to IgE in cultures of murine-purified B lymphocytes. J Neuroimmune Pharmacol 3:35–42
Atwood B, Wager-Miller J, Haskins C, Straiker A, Mackie K (2012) Functional selectivity in CB2 receptor signaling and regulation: implications for the therapeutic potential of CB2 ligands. Mol Pharmacol 81:250–263
Basu S, Dittel BN (2011) Unraveling the complexities of cannabinoid receptor 2 (CB2) immune regulation in health and disease. Immunol Res 51:26–38
Bouaboula M, Rinaldi M, Carayon P, Carillon C, Delpech B, Shire D, Le Fur G, Casellas P (1993) Cannabinoid-receptor expression in human leukocytes. Eur J Biochem 214:173–180
Brailoiu GC, Oprea TI, Zhao P, Abood ME, Brailoiu E (2011) Intracellular CB1 cannabinoid receptors are activated by anandamide. J Biol Chem 286:29166–29174
Carayon P, Marchand J, Dussossoy D, Derocq JM, Jbilo O, Bord A, Bouaboula M, Galiegue S, Mondiere P, Penarier G, Le Fur G, Defrance T, Casellas P (1998) Modulation and functional involvement of CB2 peripheral cannabinoid receptors during B-cell differentiation. Blood 92:3605–3615
Cencioni MT, Chiurchiù V, Catanzaro G, Borsellino G, Bernardi G, Battistini L, Maccarrone M (2010) Anandamide suppresses proliferation and cytokine release from primary human T-lymphocytes mainly via CB2 receptors. PLoS One 5:e8688
Dainese E, Oddi S, Maccarrone M (2010) Interaction of endocannabinoid receptors with biological membranes. Curr Med Chem 17:1487–1499
Do Y, McKallip RJ, Nagarkatti M, Nagarkatti PS (2004) Activation through cannabinoid receptors 1 and 2 on dendritic cells triggers NF-kappaB-dependent apoptosis: novel role for endogenous and exogenous cannabinoids in immunoregulation. J Immunol 173:2373–2382
Galiègue S, Mary S, Marchand J, Dussossoy D, Carrière D, Carayon P, Bouaboula M, Shire D, Le Fur G, Casellas P (1995) Expression of central and peripheral cannabinoid receptors in human immune tissues and leukocyte subpopulations. Eur J Biochem 232:54–61
Gorantla S, Makarov E, Roy D, Finke-Dwyer J, Murrin LC, Gendelman HE, Poluektova L (2010) Immunoregulation of a CB2 receptor agonist in a murine model of neuroAIDS. J Neuroimmune Pharm 5:456–468
Graham ES, Angel CE, Schwarcz LE, Dunbar PR, Glass M (2010) Detailed characterisation of CB2 receptor protein expression in peripheral blood immune cells from healthy human volunteers using flow cytometry. Int J Immunopathol Pharmacol 23:25–34
Grimsey NL, Goodfellow CE, Dragunow M, Glass M (2011) Cannabinoid receptor 2 undergoes Rab5-mediated internalization and recycles via a Rab11-dependent pathway. Biochim Biophys Acta 1813:1554–1560
Guindon J, Hohmann AG (2008) Cannabinoid CB2 receptors: a therapeutic target for the treatment of inflammatory and neuropathic pain. Br J Pharmacol 153:319–334
Howlett AC (2005) Cannabinoid receptor signaling. Handb Exp Pharmacol 168:53–79
Jean-Alphonse F, Hanyaloglu AC (2011) Regulation of GPCR signal networks via membrane trafficking. Mol Cell Endocrinol 331:205–214
Klein TW, Newton CA, Nakachi N, Friedman H (2000) Delta 9-tetrahydrocannabinol treatment suppresses immunity and early IFN-gamma, IL-12, and IL-12 receptor beta 2 responses to Legionella pneumophila infection. J Immunol 164:6461–6466
Klein TW (2005) Cannabinoid-based drugs as anti-inflammatory therapeutics. Nat Rev Immunol 5:400–411
Klein TW, Cabral GA (2006) Cannabinoid-induced immune suppression and modulation of antigen-presenting cells. J Neuroimmune Pharm 1:50–64
Mach F, Steffens S (2008) The role of the endocannabinoid system in atherosclerosis. J Neuroendocrinol 20:S53–S57
Mackie B (2006) Cannabinoid receptors as therapeutic targets. Annu Rev Pharmacol Toxicol 46:101–122
Malfait AM, Gallily R, Sumariwalla PF, Malik AS, Andreakos E, Mechoulam R, Feldmann M (2000) The nonpsychoactive cannabis constituent cannabidiol is an oral anti-arthritic therapeutic in murine collagen-induced arthritis. PNAS 97:9561–9566
McKallip RJ, Lombard C, Martin BR, Nagarkatti M, Nagarkatti PS (2002) Delta(9)-tetrahydrocannabinol-induced apoptosis in the thymus and spleen as a mechanism of immunosuppression in vitro and in vivo. J Pharmacol Exp Ther 302:451–465
McKallip RJ, Nagarkatti M, Nagarkatti PS (2005) Delta-9-tetrahydrocannabinol enhances breast cancer growth and metastasis by suppression of the antitumor immune response. J Immunol 174:3281–3289
Mechoulam R (1986) The pharmacohistory of Cannabis sativa. In: Mechoulam R (ed) Cannabinoids as therapeutic agents. CRC Press, Boca Raton, pp 1–19
Munro S, Thomas KL, Abu-Shaar M (1993) Molecular characterization of a peripheral receptor for cannabinoids. Nature 365:61–65
Newton CA, Chou PJ, Perkins I, Klein TW (2009) CB(1) and CB(2) cannabinoid receptors mediate different aspects of delta-9-tetrahydrocannabinol (THC)-induced T helper cell shift following immune activation by Legionella pneumophila infection. J Neuroimmune Pharm 4:92–102
Pertwee RG (2006) Cannabinoid pharmacology: the first 66 years. Br J Pharmacol 147:S163–S171
Roth MD, Tashkin DP, Whittaker KM, Choi R, Baldwin GC (2005) Tetrahydrocannabinol suppresses immune function and enhances HIV replication in the huPBL-SCID mouse. Life Sci 77:1711–1722
Rozenfeld R (2011) Type I cannabinoid receptor trafficking: all roads lead to lysosome. Traffic 12:12–18
Sarafian T, Montes C, Harui A, Beedanagari SR, Kiertscher S, Stripecke R, Hossepian D, Kitchen C, Kern R, Belperio J, Roth MD (2008) Clarifying CB2 receptor-dependent and independent effects of THC on human lung epithelial cells. Toxicol Appl Pharmacol 231:282–290
Schatz AR, Lee M, Condie RB, Pulaski JT, Kaminski NE (1997) Cannabinoid receptors CB1 and CB2: a characterization of expression and adenylate cyclase modulation within the immune system. Toxicol Appl Pharmacol 142:278–287
Shay A, Choi R, Whittaker K, Salehi K, Tashkin DP, Roth MD, Baldwin GC (2003) Impairment of antimicrobial activity and nitric oxide production in alveolar macrophages from smokers of marijuana and cocaine. J Infect Dis 187:700–704
Shire D, Calandra B, Rinaldi-Carmona M, Oustric D, Pessegue B, Bonnin-Cabanne O, Le Fur G, Caput D, Ferrara P (1996) Molecular cloning, expression and function of the murine CB2 peripheral cannabinoid receptor. Biochim Biophys Acta 1307:132–136
Sipe JC, Arbour N, Gerber A, Beutler E (2005) Reduced endocannabinoid immune modulation by a common cannabinoid 2 (CB2) receptor gene polymorphism: possible risk for autoimmune disorders. J Leukoc Biol 78:231–238
Srivastava MD, Srivastava BIS, Brouhard B (1998) Δ9 Tetrahydrocannabinol and cannabidiol alter cytokine production by human immune cells. Immunopharmacology 40:179–185
Thomas BF, Compton DR, Martin BR (1990) Characterization of the lipophilicity of natural and synthetic analogs of delta 9-tetrahydrocannabinol and its relationship to pharmacological potency. J Pharmacol Exp Ther 255:624–630
Yuan M, Kiertscher SM, Cheng Q, Zoumalan R, Tashkin DP, Roth MD (2002) Δ9-Tetrahydrocannabinol regulates Th1/Th2 cytokine balance in activated human T-cells. J Neuroimmunol 133:124–131
Zhu LX, Sharma S, Stolina M, Gardner B, Roth MD, Tashkin DP, Dubinett SM (2000) Delta-9-tetrahydrocannabinol inhibits antitumor immunity by a CB2 receptor-mediated, cytokine-dependent pathway. J Immunol 165:373–380
Acknowledgments
We thank Benjamin Alderete and Raymond Kong for their assistance with ImageStreamX® fluorescent imaging and analysis services that were graciously provided by Amnis Corporation, EMD Millipore, Seattle, WA. This work was supported by National Institutes of Health, National Institute on Drug Abuse [Grant R21-DA021813, R01-DA03018]. (M.D.R.). Flow cytometry was performed utilizing the UCLA Jonsson Comprehensive Cancer Center and Center for AIDS Research Flow Cytometry Core Facility supported by National Institutes of Health [Grant CA-16042, AI-28697]; the Jonsson Comprehensive Cancer Center, the UCLA AIDS Institute, and the David Geffen School of Medicine at UCLA. Julie T. Castaneda was supported by institutional awards through the UCLA Competitive Edge, E. Eugene Cota Robles, and Graduate Mentored Research programs. The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was presented in abstract form at the 18th Scientific Conference of the Society on NeuroImmune Pharmacology, April 26, 2012, Honolulu, HI.
Rights and permissions
About this article
Cite this article
Castaneda, J.T., Harui, A., Kiertscher, S.M. et al. Differential Expression of Intracellular and Extracellular CB2 Cannabinoid Receptor Protein by Human Peripheral Blood Leukocytes. J Neuroimmune Pharmacol 8, 323–332 (2013). https://doi.org/10.1007/s11481-012-9430-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-012-9430-8