Abstract
Infection with HIV-1 frequently affects the brain and causes NeuroAIDS prior to the development of overt AIDS. The HIV-1 envelope protein gp120 interacts with host CD4 and chemokine co-receptors to initiate infection of macrophages and lymphocytes. In addition, the virus or fragments of it, such as gp120, cause macrophages to produce neurotoxins and trigger neuronal injury and apoptosis. Moreover, the two major HIV co-receptors, the chemokine receptors CCR5 and CXCR4, serve numerous physiological functions and are widely expressed beyond immune cells, including cells in the brain. Therefore, HIV co-receptors are poised to play a direct and indirect part in the development of NeuroAIDS. Although rodents are not permissive to infection with wild type HIV-1, viral co-receptors - more than CD4 - are highly conserved between species, suggesting the animals can be suitable models for mechanistic studies addressing effects of receptor-ligand interaction other than infection. Of note, transgenic mice expressing HIV gp120 in the brain share several pathological hallmarks with NeuroAIDS brains. Against this background, we will discuss recently completed or initiated, ongoing studies that utilize HIV co-receptor knockout and viral gp120-transgenic mice as models for in vitro and in vivo experimentation in order to address the potential roles of HIV gp120 and its co-receptors in the development of NeuroAIDS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Infection with the human immunodeficiency virus-1 (HIV-1) and acquired immunodeficiency syndrome (AIDS) remain 30 years into the epidemic a persistent public health problem worldwide. In addition to a progressive destruction of the immune system, HIV-1 also initiates a spectrum of neurological problems and neurocognitive impairments that historically have been described as NeuroAIDS but are now also comprehensively categorized under the term HIV-associated neurocognitive disorders (HAND) (Antinori et al. 2007). While much information has been gained over the years regarding HIV-1 infection of the periphery and the central nervous system (CNS) in general, the pathological, cellular and molecular mechanisms leading to HAND, NeuroAIDS and AIDS remain incompletely understood.
An important step in AIDS and NeuroAIDS research occurred in the mid 1990s, when it was discovered by several groups that HIV-1 infection required, in addition to CD4, one or two chemokine receptors as co-receptors. The most prominent HIV co-receptors are CCR5 (CD195) (Alkhatib et al. 1996; Dragic et al. 1996; Choe et al. 1996; Doranz et al. 1996) and CXCR4 (CD184) (Bleul et al. 1996), and together with CD4 they provide the preferred binding site for the HIV-1 envelope protein gp120 on the virus’ target cells.
Furthermore, several lines of evidence based on work of numerous investigators over many years strongly suggest that NeuroAIDS, HIV-1 associated neurodegeneration and consequent HAND may occur via at least two major mechanisms (reviewed in (Kaul 2008)). The first is neurotoxicity as a consequence of either direct exposure to HIV-1 and its fragments or indirect injury through neurotoxins released by infected or immune-stimulated, inflammatory microglia and macrophages (MΦ) in the brain (Giulian et al. 1990; Kaul et al. 2001; Gonzalez-Scarano and Martin-Garcia 2005; Lindl et al. 2010). The second assault of HIV on the brain comprises the impairment of neurogenesis (Krathwohl and Kaiser 2004; Tran et al. 2005; Poluektova et al. 2005; Okamoto et al. 2007).
Since HIV-1 was discovered and linked to the development of AIDS (Barre-Sinoussi et al. 1983; Hahn et al. 1984), multiple approaches have been taken to generate suitable animal models for studying HIV disease, including NeuroAIDS (Gardner and Luciw 1989; Klotman and Notkins 1996; Toggas and Mucke 1996; Ambrose et al. 2007; Nath et al. 2000; Van Duyne et al. 2009).
Animal models in AIDS and neuroAIDS research
The variety of model systems employed in AIDS research includes chimpanzees and other non-human primates, cats and rodents (rats and mice) (Nath et al. 2000; Ambrose et al. 2007; Gardner and Luciw 1989; Reid et al. 2001; Keppler et al. 2002; Klotman and Notkins 1996; Toggas and Mucke 1996; Van Duyne et al. 2009). Chimpanzees can be infected with some HIV-1 groups but rarely develop AIDS and are primarily employed in vaccine research (Nath et al. 2000). Other non-human primates, cats and rodents are not permissive to wild type HIV-1. However, several non-human primate species are susceptible to Simian Immunodeficiency virus (SIV) and cats can be infected by Feline Immunodeficiency virus (FIV) (Ambrose et al. 2007; Clements et al. 1994; Olmsted et al. 1989). Both viruses can cause in a species-specific fashion an AIDS-like disease and neuropathological changes or even encephalitis, and macaques and cats are therefore used for studies of the pathogenesis of AIDS and NeuroAIDS (Ambrose et al. 2007; Clements et al. 1994; Olmsted et al. 1989; Meeker et al. 1997; Jacobson et al. 1997; Clements et al. 2008). While SIV is considered to be the animal virus most closely related to HIV-1, significant differences exist between the viruses. Therefore, several SIV-HIV hybrid viruses have been generated in order to better adapt the SIV model for HIV research (Ambrose et al. 2007).
Among the various model systems, rodents have turned out to be useful in spite of the fact that they cannot be productively infected with wild type HIV-1. Interestingly however, two recently generated chimeric HIV mutants in which the envelope protein gp120 was replaced by the gp80 of ecotropic murine leukemia virus (EcoHIV) allowed for the first time to establish in mice a lasting lentiviral infection that also triggered an immune response (Potash et al. 2005). Furthermore, one of the chimeric viruses was shown to be neuroinvasive, suggesting its potential suitability for NeuroAIDS research.
Other approaches to generate small animal models for AIDS and NeuroAIDS research took advantage of the fact that certain mouse strains can be reconstituted with a human hematopoietic system which is permissive to HIV infection (Van Duyne et al. 2009; Dash et al. 2011). Numerous other studies have employed the intracranial injection of HIV-infected human monocyte-derived macrophages into the brains of mice with severe combined immunodeficiency (SCID). This model demonstrated that HIV-infected macrophages can cause a neuropathology that shares key features with post mortem brains from NeuroAIDS patients (Persidsky et al. 1996; Limoges et al. 2000; Poluektova et al. 2002; Sas et al. 2007). Furthermore, these studies indicated that HIV-infected cells in the brain can trigger a peripheral immune response.
Another important advantage of rodents, both mice and rats, is that they can be genetically modified (Klotman and Notkins 1996; Toggas and Mucke 1996; Van Duyne et al. 2009; Reid et al. 2001). Several transgenic mice and a rat have been generated that express an entire HIV genome and develop AIDS-like diseases (Leonard et al. 1988; Iwakura et al. 1992; Hanna et al. 1998a; Hanna et al. 1998b; Reid et al. 2001). Furthermore, transgenic mouse microglia carrying the provirus of a macrophage-tropic HIV-1 were shown to release infectious virus (Wang et al. 2003). Transgenic mice expressing the entire HIV genome or distinct components of the virus, such as gp120, Tat or Vpr, in the brain show various degrees of neuropathology, including pruning of neuronal dendrites, loss of synapses and neurons as well as glial activation, and also behavioral alterations that recapitulate several features observed in NeuroAIDS patients (Thomas et al. 1994; Toggas et al. 1994; Berrada et al. 1995; Toneatto et al. 1999; Kim et al. 2003; Bruce-Keller et al. 2008; Jones et al. 2007; D’hooge et al. 1999). Overall, the exact spectrum of pathological features with resemblance to AIDS and NeuroAIDS depends on the specific animal model and ranges from depletion of CD4+ T-cells to immunodeficiency to wasting disease to failure-to-thrive to neuronal injury and loss to behavioral impairment to shortened life span. Of note, studies employing injection of HIV-infected macrophages in the brain or HIV-infected humanized mice or transgenic expression of entire viral genomes are useful to investigate the sum of the pathological effects of all viral components, but do not allow to discern the potential contribution of a single viral factor. Therefore, approaches that use injection or transgenic expression of one viral component at a time appear very useful as well. A number of such studies have addressed the pathological potential of HIV-1 gp120, Tat and Vpr, and indeed suggested that isolated viral factors can produce some of the pathological characteristics of HIV disease and NeuroAIDS (Toggas et al. 1994; Berrada et al. 1995; Toneatto et al. 1999; Kim et al. 2003; Bruce-Keller et al. 2008; Jones et al. 2007; Bachis et al. 2006; Hauser et al. 2009). Mice have in comparison to all other animal models one additional advantage, the availability of many specific genetic knockout mutants. Thus, transgenic and genetic knockout mice allow studying the effect of viral and host factors in a way that is not possible in any other model.
The remainder of this article will discuss recent studies in the field of NeuroAIDS research that employed transgenic mice expressing HIV-1 gp120 in the brain and mouse strains deficient in the major HIV coreceptors CCR5 and CXCR4. As such this review will primarily focus on a selection from a variety of model systems that are available to investigate aspects of NeuroAIDS and in particular the potential role of viral gp120. Several other animal models for NeuroAIDS research will be presented in more detail elsewhere in this journal, and we encourage the reader to consider the here discussed findings in the context of data obtained in other models. Like all investigations using animal models, our studies served at least one of two purposes: either improving our understanding of the neuropathological mechanism(s) of HIV infection, or suggesting potential future therapies for NeuroAIDS.
Chemokine receptors, HIV-1 infection and neuroAIDS
Several excellent reviews extensively discuss the currently recognized 20 chemokine receptors and over 50 chemokines (Locati and Murphy 1999; Zlotnik and Yoshie 2000; Rot and von Andrian 2004; Cartier et al. 2005; Biber et al. 2006; Domanska et al. 2011). Chemokines are mostly small, ~7 to 14 kD, proteins that have been categorized into four subfamilies based on different cysteine-containing sequence motifs near their N-terminus, α or CXC, β or CC, γ or XC and δ or CX3C ligands (L). Chemokine receptors have been named in analogy, such as α or CXCR and β or CCR, and belong to the large family of seven transmembrane domain G protein-coupled receptors (Zlotnik and Yoshie 2000). Interestingly, chemokine receptors and their ligands are expressed in a wide variety of cell types in both the periphery as well as the central nervous system (CNS) (Locati and Murphy 1999; Rot and von Andrian 2004; Bajetto et al. 2001; Cartier et al. 2005; Biber et al. 2006; Miller et al. 2008; Domanska et al. 2011; Gorry and Ancuta 2011). Chemokines and their receptors were historically described as a biological system that controls cell migration, mostly as part of the immune defense system. However, it has become clear over time that this complex receptor-ligand network contributes to many more biological processes, including organ development, vascularization, cell proliferation and apoptosis, in both health and disease. Chemokine receptors play well recognized pathological roles in diseases such as asthma, cancer and, most prominently, HIV infection (Locati and Murphy 1999; Bisset and Schmid-Grendelmeier 2005; Durig et al. 2001; Domanska et al. 2011; Gorry and Ancuta 2011).
In HIV-1 infection, CD4 and the chemokine receptors CCR5 (CD195) and CXCR4 (CD184) likely provide the first sites of host-virus interaction. The virus binds via its envelope protein gp120 first to CD4 receptors, which are only located on cells of immune lineage, in order to then efficiently engage chemokine co-receptors and eventually infect its primary target cells, macrophages/microglia and CD4+ T-lymphocytes (Bleul et al. 1996; Alkhatib et al. 1996; Dragic et al. 1996; Kaul et al. 2001; Gonzalez-Scarano and Martin-Garcia 2005). Besides CCR5, CCR3 possibly also facilitates HIV infection of microglia in the brain (He et al. 1997). While most macrophage/microglia-tropic (M-tropic) HIV are CCR5-preferring (R5) and most CD4+ T-lymphocyte-infecting HIV (T-tropic) are CXCR4-preferring virus strains (X4), many R5 viruses can readily infect CCR5-expressing T cell populations and several X4 viruses can spread among macrophages(Alkhatib et al. 1996; Dragic et al. 1996; Choe et al. 1996; Bleul et al. 1996). In addition, numerous HIV-1 strains exist that can use both CCR5 and CXCR4 (R5X4) and can propagate in macrophages and T cells (dual tropic) (Doranz et al. 1996). Therefore HIV tropism seems to be determined by more factors than co-receptor usage (Gorry and Ancuta 2011). CCR5, however, plays a crucial role in HIV-1 infection and disease. In fact, most sexually transmitted viral strains prefer CCR5, and a congenital deletion mutation, named CCR5Δ32, causes the absence of this chemokine receptor from the cell surface and offers significant protection from infection (Dean et al. 1996). Most interestingly, a recent transplantation of CCR5Δ32 hematopoietic stem cells into a HIV patient with acute myeloid leukemia allowed survival for already more than 20 month without detectable viral titer in the absence of anti-retroviral therapy (Hutter et al. 2009). In the presence of CCR5, its endogenous ligands, namely ‘macrophage inflammatory protein’ (MIP)-1α (CCL3), MIP-1β (CCL4) and ‘regulated-and-normal-T cell-expressed-and-secreted’ (RANTES, CCL5), can slow progression to AIDS (Cocchi et al. 1995). However, once HIV infection is established, dual tropic and X4-preferring viruses can evolve, and these viruses usually herald progression to AIDS (Michael and Moore 1999). Interestingly, CD4+ T-lymphocytes seem to be more efficient propagators of HIV-1 than macrophages, but also rapidly die from apoptosis, except for a certain number of memory cells that constitute a quiescent, latent reservoir (Pantaleo and Fauci 1995; Chun and Fauci 1999; Alexaki et al. 2008). Macrophages infected with HIV-1, on the other hand, appear to produce less virus but constitute a long-lived reservoir and are the primary suspects for trafficking HIV into the brain where the virus may then spread to local macrophages and microglia (Koenig et al. 1986; Kaul et al. 2001; Gonzalez-Scarano and Martin-Garcia 2005; Kraft-Terry et al. 2009).
Interestingly, expression of CCR5 and CXCR4 is not restricted to cells of immune lineages, such as macrophages and microglia. Neurons and astrocytes, which lack CD4, readily express the two major HIV co-receptors (Lavi et al. 1997; Halks-Miller et al. 1997; Rottman et al. 1997; Kaul et al. 2007). Of note, interaction between HIV-1 gp120 and CXCR4, independent of CD4, has been reported to trigger intracellular Ca2+ accumulation and signaling (Hesselgesser et al. 1997). Furthermore, the virus seems to be able to enter astrocytes via a process that requires a mannose receptor and leads to a non-productive infection (Liu et al. 2004). While neurons appear to resist HIV infection, direct interaction of gp120 with neuronal chemokine receptors may nevertheless contribute to neuronal injury (Hesselgesser et al. 1997; Hesselgesser et al. 1998; Wang et al. 2009). In any case, several lines of evidence suggest that activation of HIV co-receptors on CD4+ macrophages, with or without resultant HIV infection, and subsequent release of neurotoxins, including excitotoxins, chemokines and pro-inflammatory cytokines, provide the predominant trigger for neuronal injury and death (Giulian et al. 1990; Giulian et al. 1993; Kaul and Lipton 1999; Porcheray et al. 2006; O’Donnell et al. 2006; Cheung et al. 2008; Eggert et al. 2010; Medders et al. 2010; Kaul et al. 2001; Gonzalez-Scarano and Martin-Garcia 2005; Kraft-Terry et al. 2009). In line with this hypothesis two recent studies observed that the amount of pro-viral HIV DNA in peripherally circulating monocytes and macrophages correlates well with HAND (Shiramizu et al. 2005; Shiramizu et al. 2006).
Development of NeuroAIDS in patients during life time is believed to underlie the neurological and neurocognitive complications subsumed under the term HAND. HIV-associated dementia (HAD) represents the most severe manifestation of HAND (Antinori et al. 2007) and has been correlated to a range of post mortem diagnosed neuropathological features that are often referred to as HIV encephalitis (HIVE). The neuropathological hallmarks include infiltration predominantly by monocytes and macrophages entering from the blood stream, activated resident microglia, microglial nodules, multinucleated giant cells, widespread reactive astrocytosis, myelin pallor, and decreased synaptic and dendritic density, combined with selective neuronal loss (Petito et al. 1986; Masliah et al. 1997a). Interestingly, cognitive dysfunction and HAND during life seem to correlate with evidence of excitatory neurotoxins in cerebrospinal fluid (CSF) and serum (Heyes et al. 1991) and the amount of pro-viral HIV DNA in peripherally circulating monocytes and macrophages (Shiramizu et al. 2005; Shiramizu et al. 2006). In contrast, HAND is not necessarily reflected by the numbers of HIV-positive cells, multinucleated giant cells or the abundance of viral antigens in brain tissue found at autopsy (Glass et al. 1995; Achim et al. 1994; Wiley et al. 1994; Masliah et al. 1997a). Instead, clinical signs of HAND coincide best with post mortem findings of decreased synaptic and dendritic density, selective neuronal loss (Masliah et al. 1997a; Achim et al. 1994; Wiley et al. 1994), increased counts of microglia (Glass et al. 1995), and elevated tumor necrosis factor (TNF)-α mRNA in microglia and astrocytes (Wesselingh et al. 1997).
The genome of HIV-1 encodes nine proteins with structural, regulatory or accessory functions (reviewed in (Ellis et al. 2007)). Most of these viral factors have been implicated in the process of infection and in the HIV life cycle; six of the proteins have been reported to directly or indirectly affect neurons and glia (Ellis et al. 2007). Beyond establishing the first virus-host interaction and initiating infection, the envelope protein gp120 seems to be a major inducer of apoptosis in infected and uninfected bystander lymphocytes (Perfettini et al. 2005a; Perfettini et al. 2005b) and has been implicated in brain injury underlying HAND (Brenneman et al. 1988; Giulian et al. 1993; Meucci and Miller 1996; Kaul and Lipton 1999; Liu et al. 2000; Kaul et al. 2001; Mattson et al. 2005). In fact, the envelope glycoprotein gp120s of various HIV-1 strains produce in vitro and in vivo injury and apoptosis in both primary human and rodent neurons (Brenneman et al. 1988; Lannuzel et al. 1995; Meucci and Miller 1996; Singh et al. 2005; Giulian et al. 1993; Toggas et al. 1994; Meucci et al. 1998; Kaul and Lipton 1999; Kaul et al. 2007; Hesselgesser et al. 1998). These observations may not be completely surprising considering the high degree of conservation between human, mouse and rat for the two major HIV-co-receptors and CD4. Homology in percent at the level of protein sequence between the various species is: hu CXCR4: 91% with rat CXCR4, 89% with mouse; 96% between mouse and rat; hu CCR5: 82% each with rat and mouse CCR5; 92% between mouse and rat CCR5; hu CD4: 56% with mouse CD4 (L3T4), 53% with rat CD4; 74% between mouse and rat (Maung et al. 2011).
Chemokine receptor knockout-mice in neuroAIDS research
In order to investigate the role of CCR5 and CXCR4 in neuronal injury and death as it can be induced by HIV-1 gp120, we employed mice deficient in either one or both of the viral co-receptors (Kaul et al. 2007). Mice expressing both alleles of both chemokine receptors served as wild type controls. Of note, embryos derived from murine chemokine receptor wild type between days E14.5 and E16 and rat embryos at days E16 to E17 give rise to cerebrocortical cell cultures that respond in an almost identical fashion to recombinant HIV gp120s from R5-, X4- and R5X4 viral strains in neurotoxicity experiments (Kaul et al. 2007). Mixed cerebrocortical cell cultures, containing neurons, astrocytes and microglia were prepared from mouse embryos of all four genotypes between days E14.5 and E16 and allowed to differentiate in vitro for 17 days before neurotoxicity studies. Interestingly, based on immunostaining with cell type-specific markers for neurons, astrocytes and microglia and with regard to the percentage of the different cell types, wild type and chemokine receptor-deficient cerebrocortical cell cultures appeared indistinguishable (Kaul et al. 2007). However, while the in vitro approach appears helpful by leveling the field for survival, growth and development of cerebrocortical cells with and without HIV co-receptors, a look at the in vivo situation reveals important peripheral and central differences between the genotypes.
CXCR4 knockout (KO) mice have been generated by three different groups (Ma et al. 1998; Zou et al. 1998; Tachibana et al. 1998). Mice heterozygous for CXCR4 gene deficiency are viable, fertile and appear indistinguishable from wild type littermates. In contrast, homozygous CXCR4-deficient animals die in utero or at the first day after birth (Ma et al. 1998). Although it has been estimated that about one third of CXCR4 KO embryos are dead at day E18.5, we found that they seem to stay alive throughout E14.5 to E16 (Kaul et al. 2007). The most prominent pathology of CXCR4-deficient mice revealed by histological analysis presented itself as severe alterations in bone marrow and cerebellum (Ma et al. 1998; Zou et al. 1998; Tachibana et al. 1998). All other organs appeared grossly and microscopically normal, although the lungs were collapsed, the kidneys showed vascular congestion and pronounced interstitial hemorrhage, and intestinal vascularization seemed to be abnormal (Tachibana et al. 1998). Interestingly, contrary to other CXCR4 mutant mouse strains generated in two different laboratories (Zou et al. 1998; Tachibana et al. 1998), no septal defects were observed in the CXCR4 mutant strains described by a third group (Ma et al. 1998).
Hematopoiesis in CXCR4-deficient mice is also affected. At E15.5, the bone marrow is hypocellular with remarkably reduced hematopoiesis compared to wild type littermates, and comprises primarily stromal cells and osteoclasts with severe reduction in all hematopoietic lineages. While surviving E18.5 KO embryos show cellularity comparable with wild type and normal numbers of maturing erythrocytes and megakaryocytes, hematopoiesis remains underdeveloped (Ma et al. 1998; Zou et al. 1998; Tachibana et al. 1998).
While B-lymphopoiesis in CXCR4-KO liver at E18.5 is strongly reduced compared to wild type and heterozygotes, T-lymphopoiesis appears undisturbed in CXCR4-deficient thymus. Myelopoiesis, however, is also defect in CXCR4 deficiency, with virtual absence of myeloid forms at day E18.5 (Ma et al. 1998; Zou et al. 1998; Tachibana et al. 1998).
Regarding the central nervous system, the cerebellum of CXCR4-deficient (and SDF-1 KO) mice displays a highly abnormal structure while cerebrum, basal ganglia, midbrain, and spinal cord appear normal. In the cerebellum, the external granular layer (EGL) seems diminished and chromophilic cell clumps are visible after H&E staining. Furthermore, the EGL is irregular, the overall shape of cerebellum is altered, and foliation is absent. Purkinje cells which are normally located immediately underneath the EGL, are located ectopically in the absence of CXCR4 (Ma et al. 1998; Zou et al. 1998). In addition, CXCR4 KO mice display significant defects in the formation of the hippocampus, in particular the dentate gyrus (Lu et al. 2002). A reduction in the number of neural precursors and cells in the rostral migratory stream indicate a severe disturbance of hippocampal neurogenesis. CXCR4 also plays a crucial role in the correct placement of interneurons in the neocortex during brain development (Stumm et al. 2003).
CCR5 KO mice have been generated independently by two groups (Zhou et al. 1998; Huffnagle et al. 1999). CCR5-deficient mice are viable, fertile and at birth indistinguishable from wild type or heterozygous littermates. Histopathological analysis of major organs does not indicate any abnormalities in gross morphology. No differences between CCR5 KO and wild type mice were found in cells from thymus, spleen, lymph nodes, and bone marrow using markers for T-, B-, granulocyte, and monocyte/macrophage type cell populations. Also, there was no significant change observed in macrophage recruitment in a disease model of glucan-induced granuloma. However, CCR5-deficient macrophages display reduced cytokine production compared to their wild type counterparts (GM-CSF, IL-1ß, IL-6 = 50%), although production of TNF-α and IL-10 appear to be normal. In the T cell compartment, the lack of CCR5 goes along with enhanced cytokine production (IFNy: 5-fold, GM-CSF: 2.5-fold, IL-4: 2-fold). Interestingly, peripheral production of chemokines, namely CCR5 ligands CCL5/RANTES, CCL3/MIP-1α, or CCL4/MIP-1ß, seems to be not different between CCR5-expressing and deficient mice. On the other hand, depending on the antigen trigger CCR5 KO show enhanced cell-mediated or humoral immune responses compared to wild type controls (Zhou et al. 1998).
Over time, several studies have revealed that with regard to infections and inflammation, CCR5 plays important roles in the resolution of some diseases but exerts an aggravating effect in other pathological circumstances. As such, CCR5 KO mice present with more severe disease outcome in the case of infection with L. monocytogenes (Zhou et al. 1998), Cryptococcus neoformans (Huffnagle et al. 1999), Toxoplasma gondii (Luangsay et al. 2003; Khan et al. 2006), Trypanosoma cruzi (Machado et al. 2005), Influenza A virus (Dawson et al. 2000), Herpes Simplex Virus (HSV)-2 (Thapa et al. 2007), HSV-1 (Teixeira et al. 2010), and lethality in West Nile virus (WNV) infection (Glass et al. 2005).
In contrast, CCR5 KO mice show less severe disease or protection during Lipopolysaccharide (LPS)-induced endotoxemia (Zhou et al. 1998), IFNγ-induced pulmonary emphysema (Ma et al. 2005; Bracke et al. 2007), atherosclerosis due to high fat diet (Potteaux et al. 2006; Zernecke et al. 2006; Braunersreuther et al. 2007), inflammation-associated hepatic fibrosis (Seki et al. 2009) and in a model of cerebral malaria triggered by infection with Plasmodium berghei (Belnoue et al. 2003; Nitcheu et al. 2003)
Overall, the above reports suggest that differences due to the absence of the β-chemokine receptor emerge primarily with a challenge of the immune response. Still, a recent study of 12 to 18 month old CCR5 KO mice found in comparison to age-matched controls memory impairment, astrocytosis and increased β-amyloid deposition in the brain (Lee et al. 2009). As a note of caution, the controls in this study did not completely match the genetic background of the CCR5 KO animals. In contrast, our group has been studying the consequences of CCR5-deficiency for the CNS in a different mixed genetic background using a breeding strategy that allows for production of CCR5-expressing and –lacking animals as littermates. Thus, the animals in our investigations share a common genetic background. Interestingly, we found in a genome-wide gene expression analysis using RNA from whole brain tissue significant differential regulation between CCR5 KO and wild type mice for more than 250 genes (Maung et al. 2011).
CCR5-CXCR4 Double KO (DKO) mice were generated by our group through cross-breeding of animals first described by Ma and colleagues (CXCR4KO) and Huffnagle and collaborators (CCR5KO) (Ma et al. 1998; Huffnagle et al. 1999; Kaul et al. 2007). The new mouse line is maintained using viable CXCR4+/−CCR5+/− and CXCR4+/−CCR5−/− animals which allow for production of homozygous, single and double chemokine receptor KO embryos as well as wild type controls.
Cerebrocortical cultures with the various chemokine receptor deficiencies (CCR5 KO, CXCR4 KO, CCR5-CXCR4 double KO and wild type as control) enabled us to show that both CCR5 and CXCR4 can separately mediate the neurotoxic effect of gp120 depending on the co-receptor usage of the virus strain from which the envelope protein was originally isolated (Kaul et al. 2007). The fact that the absence of CCR5 or CXCR4 in mixed neuronal-glial cerebrocortical cells from mouse abrogates or significantly decreases neurotoxicity by CCR5- or CXCR4-preferring gp120s, respectively, resembles the specificity of HIV co-receptor usage in human cells. Thus, the murine system provides a suitable model for these functional studies of the two major HIV co-receptors. Moreover, only cerebrocortical cells of CCR5-CXCR4 DKOs were resistant to the neurotoxicity of any tested viral gp120. Interestingly, however, when we replaced microglia in CCR5-CXCR4 DKO cerebrocortical cell cultures with human monocytic THP-1 cells, which express both HIV co-receptors, neurotoxicity of gp120 was restored (Medders et al. 2010). This finding indicates that activation by HIV gp120 of viral co-receptors in macrophages and microglia may suffice to indirectly produce neuronal injury and death, and that CXCR4−/−CCR5−/− neurons are still susceptible to macrophage toxins induced by HIV-1 envelope protein.
HIV-1 gp120-transgenic mice as animal model in neuroAIDS research
Three different genetically engineered mouse lines have been reported so far that express either HIV-1 gp120 or its precursor gp160 as transgene in the absence of other viral proteins. Of note, two of these transgenic mice have been specifically generated for NeuroAIDS research (Toggas et al. 1994; Berrada et al. 1995) while a third line was designed to study the effect of the viral envelope on CD4+ T lymphocytes (Finco et al. 1997).
The HIV gp120-transgenic mouse aimed at investigating the demise of T-cells in AIDS is a viral gp120-human CD4-doubly transgenic animal expressing both proteins in lymphocytes (Finco et al. 1997). The viral gp120 is derived from HIV-1 SF2 and is expressed under the control of a modified Thy1.2 promotor containing an immunoglobulin heavy chain enhancer (Thy-1Eμ) which leads to transgene expression in most peripheral T-cells and thymocytes, but also the central nervous system. Therefore, it may not seem surprising that these animals develop besides antibody-dependent T-cell depletion also pathological changes in the blood–brain-barrier (BBB) (Toneatto et al. 1999). However, it remains unknown whether or not these animals display any additional neuropathological changes.
A transgenic mouse that expresses viral gp160 of the HIV-1 strain IIIB under the control of the human neurofilament light chain promotor in neurons shows expression of viral envelope in brain stem and anterior horns of the spinal cord and dendritic swellings in motor neurons and other fibers of the spinal cord (Berrada et al. 1995). Surprisingly, however, no expression is detected in cerebral cortex.
The first HIV gp120-transgenic mouse reported is apparently so far also the most studied model and expresses a soluble viral envelope gp120 of HIV-1 LAV in the brain in astrocytes under the control of the promoter of glial fibrillary acidic protein (GFAP-gp120-transgenic mouse) (Toggas et al. 1994). The expression of transgene is the highest in neocortex, olfactory bulb, hippocampus, tectum, selected white matter tracts, and along the glia limitans. Although this transgenic mouse only expresses viral gp120, it develops a neuropathology that is strikingly similar to human AIDS brains, including decreased synaptic and dendritic density, frank neuronal loss, increased numbers of activated microglia and pronounced astrocytosis (Toggas et al. 1994). The potential relevance of this model is supported by a comparable neuropathology that results when HIV-infected human macrophages are intracerebrally administered into SCID mice, an experimental approach that also closely recapitulates the above mentioned features of the neuropathology in human AIDS brains (Persidsky et al. 1996). The founder lines described in the first study of GFAP-gp120-transgenic mice also suggested that neuropathology required a sufficiently high expression of gp120 RNA while unfortunately at the time, due to a lack of suitable antibodies, the protein itself was not detected. However, a peripheral immune challenge with recombinant gp160 triggered a strong lymphocyte-mediated immune response and infiltration of the brain only in gp120-transgenic animals, but not non-transgenic littermate controls or in GFAP-LacZ transgenic mice, thus providing indirect evidence for the presence of envelope protein in the CNS of gp120-transgenic mice (Toggas and Mucke 1998). Several subsequent studies included an additional GFAP-gp120-transgenic founder line that expresses more easily detectable envelope protein levels and therefore is called gp120-transgenic High Protein Expressor, (HPX) line (Toggas and Mucke 1996; Garden et al. 2002; Lee et al. 2011; Maung et al. 2011).
The neuropathological features that have so far been described for the GFAP-gp120-transgenic mouse comprise: 1) Loss of neuronal dendrites at 3, 6, 10 and 12 months of age (Toggas et al. 1994), (Garden et al. 2002; Kang et al. 2010; Maung et al. 2011), (see Fig. 1 for immunofluorescence staining of neocortex of 6 months-old mice); 2) loss of synapses at 3 and 6 months (Toggas et al. 1994; Maung et al. 2011); 3) activated microglia at 3, 6, 10 months (Toggas et al. 1994; Kang et al. 2010; Maung et al. 2011); 4) astrocytosis at 3 and 6 months (Toggas et al. 1994; Maung et al. 2011), and 5) compromised neurogenesis at 2 and 4 to 5 months (Okamoto et al. 2007; Lee et al. 2011).
Immunofluorescence staining of MAP-2-positive neuronal dendrites in cerebral cortex of HIV gp120-transgenic and non-transgenic, wild type control mice. Sagittal brain sections of 6 months-old gp120-transgenic and WT littermate controls were immunostained for neuronal MAP-2 (red). In the upper panel Synaptophysin (green) and DNA (blue) is shown in addition to indicate pre-synaptic terminals and nuclei, respectively. Fluorescence-labeled sections were analyzed using a Zeiss Axiovert 100 M inverted microscope and Slidebook software (Intelligent Imaging Innovations, Denver, CO) to record Z-stacks for 3D reconstruction (upper panel, 3 color fluorescence of WT brain) and deconvolution (lower panels, MAP-2 only). Representative images of mid-frontal cortex, layer 3, are shown. Note the blood vessel on the left side of the upper panel and the diminished MAP-2-positive structural features of gp120-transgenic in comparison to WT brain in the lower panel
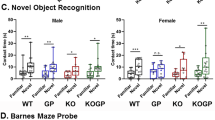
In addition, GFAP-gp120-transgenic mice display in comparison to non-transgenic littermate controls behavioral changes or impairment at 12 months, such as reduced escape latency, swimming velocity, and spatial retention (D’hooge et al. 1999) as well as reduced contextual but not cued fear conditioning at 9 to 13 months (Maung et al. 2011). In line with these findings, electrophysiological studies detect abnormalities in short- and long-term potentiation in the CA1 region of the hippocampus in gp120-transgenic mice (~53 day and 10.5 month-old mice) (Krucker et al. 1998), (Piña-Crespo et al, unpublished observations). Moreover, gp120-transgenic mice present with an altered acute response to Methamphetamine that manifests as changes in stereotypic behavior (Roberts et al. 2009).
Several studies have aimed at unraveling the potential pathological mechanisms underlying the neuropathological and behavioral features of GFAP-gp120-transgenic mice. Compared to non-transgenic controls, only young but not 6 months-old gp120-transgenic animals were found to have increased plasma corticosterone, and plasma and pituitary adreno-corticotropic hormone (ACTH) levels, indicating activation of the hypothalamic-pituitary axis (HPA) (Raber et al. 1996). This endocrine activation depended on activation of N-methyl-D-asparate-type glutamate receptors (NMDAR), neuronal nitric oxide synthase (nNOS) and reactive oxygen species (ROS) as it was inhibited by the non-competitive NMDAR inhibitor memantine, the nNOS blocker N G-methyl-L-arginine (LNMA) and a superoxide dismutase (SOD)-transgene (Raber et al. 1996). Hence, excitotoxic and oxidative stress are suspected as major contributors to the development of gp120-induced brain injury and possibly NeuroAIDS.
On the other hand, activation of protein kinase C (PKC) may contribute to astrocytosis and potentially HIV gp120-associated neuronal injury (Wyss-Coray et al. 1996). Also, compared to non-transgenic littermate controls, gp120-transgenic animals show increased expression of matrix metalloproteinase (MMP)-2 (Marshall et al. 1998) and accumulation of phosphorylated protein Tau (pTau) (Kang et al. 2010), but it remains to be elucidated if these factors are contributing causes or mere consequences of gp120-initiated CNS insult. However, increased immunostaining for pTau was also found in brain specimen of NeuroAIDS patients in comparison to age-matched healthy controls, thus revealing another pathological feature of HIV-infected brains that is present in the transgenic mouse model (Kang et al. 2010).
Besides the investigation of putative mechanisms contributing to the development of NeuroAIDS, GFAP-gp120-transgenic mice have been used to explore potential strategies for protection of the CNS against damage associated with the expression of gp120 or HIV infection. Memantine, which acts as a non-competitive inhibitor of NMDARs and thus ameliorates excitotoxicity protected 1 to 6 weeks-old gp120-transgenic mice from loss of neuronal dendrites and pre-synaptic terminals (Toggas et al. 1996). Interestingly, human amyloid precursor protein expressed as transgene also protected neurons of gp120-transgenic and control mice at ~5 months of age against acute or chronic excitotoxic injury (Mucke et al. 1995; Masliah et al. 1997b). Another recent study found that voluntary exercise or a selective serotonin re-uptake inhibitor (Paroxetine) rescued hippocampal neurogenesis in gp120-transgenic mice (Lee et al. 2011), but it remained unclear if the protective effects extended into the cerebral cortex. On the other hand, we found in a collaborative study that erythropoietin (EPO) in combination with insulin-like growth factor-1 (IGF-1) abrogated neuronal injury and pTau accumulation, but not astrocytosis, in both cerebral cortex and hippocampus of gp120-transgenic mice (Kang et al. 2010).
Ongoing and future neuroAIDS-related studies utilizing chemokine receptor deficient and HIV gp120-transgenic mouse models
In order to extent our above mentioned in vitro studies on the potential role of HIV envelope gp120 and chemokine receptors in the development of NeuroAIDS into an in vivo model, we have crossed HIV gp120-transgenic with CCR5 KO mice (Maung et al. 2011). Investigating the role of CCR5 in gp120-transgenic mice seems most interesting because this chemokine receptor and its physiological ligands influence HIV disease beyond a role in the initial HIV-target interaction leading to viral entry (Dolan et al. 2007; Ahuja et al. 2008). In fact, we previously found that CCR5-ligands, such as CCL4/MIP-1β and CCL5/RANTES prevent neurotoxicity of gp120 from R5-, X4-, and R5X4-viruses (Kaul et al. 2007). Thus, a clear rationale exists to hypothesize that CCR5 can affect the neuropathology of gp120-transgenic mice, even though the viral envelope in this model is derived from HIV-1 LAV (Toggas et al. 1994), a virus generally considered to be of the less frequent CXCR4-preferring variety that can infect macrophages (Valentin et al. 2000).
Cross-breeding of HIV gp120-transgenic with CCR5 KO mice produces viable and fertile offspring with all expected genotypes. Following an established approach, we first estimated the percentage of MAP-2 or Synaptophysin-positive neuropil by quantitative fluorescence and deconvolution microscopy in sagittal brain sections of 6 months-old gp120transgenic mice both expressing and lacking CCR5, using CCR5KO and wild type (wt)/non-transgenic animals as control. Interestingly, only CCR5wt/gp120-transgenic mice displayed a significant reduction in the percentage of MAP-2 positive neuropil and Synaptophysin immunoreactivity in comparison to all of the other three genotypes. Surprisingly, quantification of GFAP immunofluorescence revealed that astrocytosis occurred in brains of gp120-transgenic animals regardless of CCR5-deficiency. Thus, CCR5 is necessary to produce neuronal injury but not astrocytosis (Maung et al. 2011).
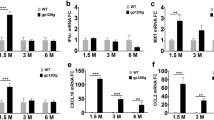
Microarray analysis of brain tissue from 6 months-old mice revealed that HIV-1 gp120 caused differential expression of about 800 genes in the presence of CCR5 but of only about 50 genes in the absence of the HIV co-receptor. Differentially expressed genes in CCR5wt/gp120tg mice suggested alterations in the function of the nervous system, immune response, cell trafficking, endocrine system, metabolism and cell death pathways compared to non-transgenic controls. Gene expression between CCR5KO/gp120tg and non-transgenic CCR5KO control mice differed mostly for GFAP and factors of the innate immune system. Interestingly, a database analysis showed that numerous genes differentially expressed in CCR5wt/gp120tg mice have also been reported for the brains of neurocognitively impaired AIDS patients and SIV-infected non-human primates, including the chemokines CCL2/MCP-1 and CXCL10/IP-10 (Maung et al. manuscript in preparation).
Ongoing and future studies will expand the characterization of the combined chemokine receptor knockout and transgenic mouse model and address questions regarding the mechanism of CCR5 function under in vivo conditions. Altogether, we propose that an in depth analysis of existing models for HIV disease of the CNS, including the one described here, will generate invaluable information. Because only if we learn what the currently existing models do or do not provide can we design the next generation of new and better animal models. Given the apparent limitations of all current animal models, new and improved in vivo models will be necessary for a better understanding and future treatment of NeuroAIDS.
References
Achim CL, Wang R, Miners DK, Wiley CA (1994) Brain viral burden in HIV infection. J Neuropathol Exp Neurol 53:284–294
Ahuja SK, Kulkarni H, Catano G, Agan BK, Camargo JF, He W, O’connell RJ, Marconi VC, Delmar J, Eron J, Clark RA, Frost S, Martin J, Ahuja SS, Deeks SG, Little S, Richman D, Hecht FM, Dolan MJ (2008) CCL3L1-CCR5 genotype influences durability of immune recovery during antiretroviral therapy of HIV-1-infected individuals. Nat Med 14:413–420
Alexaki A, Liu Y, Wigdahl B (2008) Cellular reservoirs of HIV-1 and their role in viral persistence. Curr HIV Res 6:388–400
Alkhatib G, Combadiere C, Broder CC, Feng Y, Kennedy PE, Murphy PM, Berger EA (1996) CC CKR5: a RANTES, MIP-1alpha, MIP-1beta receptor as a fusion cofactor for macrophage-tropic HIV-1. Science 272:1955–1958
Ambrose Z, Kewalramani VN, Bieniasz PD, Hatziioannou T (2007) HIV/AIDS: in search of an animal model. Trends Biotechnol 25:333–337
Antinori A, Arendt G, Becker JT, Brew BJ, Byrd DA, Cherner M, Clifford DB, Cinque P, Epstein LG, Goodkin K, Gisslen M, Grant I, Heaton RK, Joseph J, Marder K, Marra CM, McArthur JC, Nunn M, Price RW, Pulliam L, Robertson KR, Sacktor N, Valcour V, Wojna VE (2007) Updated research nosology for HIV-associated neurocognitive disorders. Neurology 69:1789–1799
Bachis A, Aden SA, Nosheny RL, Andrews PM, Mocchetti I (2006) Axonal transport of human immunodeficiency virus type 1 envelope protein glycoprotein 120 is found in association with neuronal apoptosis. J Neurosci 26:6771–6780
Bajetto A, Bonavia R, Barbero S, Florio T, Schettini G (2001) Chemokines and their receptors in the central nervous system. Front Neuroendocrinol 22:147–184
Barre-Sinoussi F, Chermann JC, Rey F, Nugeyre MT, Chamaret S, Gruest J, Dauguet C, Axler-Blin C, Vezinet-Brun F, Rouzioux C, Rozenbaum W, Montagnier L (1983) Isolation of a T-lymphotropic retrovirus from a patient at risk for acquired immune deficiency syndrome (AIDS). Science 220:868–871
Belnoue E, Kayibanda M, Deschemin JC, Viguier M, Mack M, Kuziel WA, Renia L (2003) CCR5 deficiency decreases susceptibility to experimental cerebral malaria. Blood 101:4253–4259
Berrada F, Ma D, Michaud J, Doucet G, Giroux L, Kessous-Elbaz A (1995) Neuronal expression of human immunodeficiency virus type 1 env proteins in transgenic mice: distribution in the central nervous system and pathological alterations. J Virol 69:6770–6778
Biber K, de Jong EK, van Weering HR, Boddeke HW (2006) Chemokines and their receptors in central nervous system disease. Curr Drug Targets 7:29–46
Bisset LR, Schmid-Grendelmeier P (2005) Chemokines and their receptors in the pathogenesis of allergic asthma: progress and perspective. Curr Opin Pulm Med 11:35–42
Bleul CC, Farzan M, Choe H, Parolin C, Clark-Lewis I, Sodroski J, Springer TA (1996) The lymphocyte chemoattractant SDF-1 is a ligand for LESTR/fusin and blocks HIV-1 entry. Nature 382:829–833
Bracke KR, D’hulst AI, Maes T, Demedts IK, Moerloose KB, Kuziel WA, Joos GF, Brusselle GG (2007) Cigarette smoke-induced pulmonary inflammation, but not airway remodelling, is attenuated in chemokine receptor 5-deficient mice. Clin Exp Allergy 37:1467–1479
Braunersreuther V, Zernecke A, Arnaud C, Liehn EA, Steffens S, Shagdarsuren E, Bidzhekov K, Burger F, Pelli G, Luckow B, Mach F, Weber C (2007) Ccr5 but not Ccr1 deficiency reduces development of diet-induced atherosclerosis in mice. Arterioscler Thromb Vasc Biol 27:373–379
Brenneman DE, Westbrook GL, Fitzgerald SP, Ennist DL, Elkins KL, Ruff MR, Pert CB (1988) Neuronal cell killing by the envelope protein of HIV and its prevention by vasoactive intestinal peptide. Nature 335:639–642
Bruce-Keller AJ, Turchan-Cholewo J, Smart EJ, Geurin T, Chauhan A, Reid R, Xu R, Nath A, Knapp PE, Hauser KF (2008) Morphine causes rapid increases in glial activation and neuronal injury in the striatum of inducible HIV-1 Tat transgenic mice. Glia 56:1414–1427
Cartier L, Hartley O, Dubois-Dauphin M, Krause KH (2005) Chemokine receptors in the central nervous system: role in brain inflammation and neurodegenerative diseases. Brain Res Brain Res Rev 48:16–42
Cheung R, Ravyn V, Wang L, Ptasznik A, Collman RG (2008) Signaling mechanism of HIV-1 gp120 and virion-induced IL-1beta release in primary human macrophages. J Immunol 180:6675–6684
Choe H, Farzan M, Sun Y, Sullivan N, Rollins B, Ponath PD, Wu L, Mackay CR, LaRosa G, Newman W, Gerard N, Gerard C, Sodroski J (1996) The beta-chemokine receptors CCR3 and CCR5 facilitate infection by primary HIV-1 isolates. Cell 85:1135–1148
Chun TW, Fauci AS (1999) Latent reservoirs of HIV: obstacles to the eradication of virus. Proc Natl Acad Sci U S A 96:10958–10961
Clements JE, Anderson MG, Zink MC, Joag SV, Narayan O (1994) The SIV model of AIDS encephalopathy. Role of neurotropic viruses in diseases. Res Publ Assoc Res Nerv Ment Dis 72:147–157
Clements JE, Mankowski JL, Gama L, Zink MC (2008) The accelerated simian immunodeficiency virus macaque model of human immunodeficiency virus-associated neurological disease: from mechanism to treatment. J Neurovirol 14:309–317
Cocchi F, Devico AL, Garzino-Demo A, Arya SK, Gallo RC, Lusso P (1995) Identification of RANTES, MIP-1 alpha, and MIP-1 beta as the major HIV- suppressive factors produced by CD8+ T cells. Science 270:1811–1815
D’hooge R, Franck F, Mucke L, De Deyn PP (1999) Age-related behavioural deficits in transgenic mice expressing the HIV-1 coat protein gp120. Eur J Neurosci 11:4398–4402
Dash PK, Gorantla S, Gendelman HE, Knibbe J, Casale GP, Makarov E, Epstein AA, Gelbard HA, Boska MD, Poluektova LY (2011) Loss of neuronal integrity during progressive HIV-1 infection of humanized mice. J Neurosci 31:3148–3157
Dawson TC, Beck MA, Kuziel WA, Henderson F, Maeda N (2000) Contrasting effects of CCR5 and CCR2 deficiency in the pulmonary inflammatory response to influenza A virus. Am J Pathol 156:1951–1959
Dean M, Carrington M, Winkler C, Huttley GA, Smith MW, Allikmets R, Goedert JJ, Buchbinder SP, Vittinghoff E, Gomperts E, Donfield S, Vlahov D, Kaslow R, Saah A, Rinaldo C, Detels R, O’Brien SJ (1996) Genetic restriction of HIV-1 infection and progression to AIDS by a deletion allele of the CKR5 structural gene. Hemophilia Growth and Development Study, Multicenter AIDS Cohort Study, Multicenter Hemophilia Cohort Study, San Francisco City Cohort, ALIVE Study. Science 273:1856–1862
Dolan MJ, Kulkarni H, Camargo JF, He W, Smith A, Anaya JM, Miura T, Hecht FM, Mamtani M, Pereyra F, Marconi V, Mangano A, Sen L, Bologna R, Clark RA, Anderson SA, Delmar J, O’connell RJ, Lloyd A, Martin J, Ahuja SS, Agan BK, Walker BD, Deeks SG, Ahuja SK (2007) CCL3L1 and CCR5 influence cell-mediated immunity and affect HIV-AIDS pathogenesis via viral entry-independent mechanisms. Nat Immunol 8:1324–1336
Domanska UM, Kruizinga RC, den Dunnen WF, Timmer-Bosscha H, de Vries EG, Walenkamp AM (2011) The chemokine network, a newly discovered target in high grade gliomas. Crit Rev Oncol Hematol 79:154–163
Doranz BJ, Rucker J, Yi Y, Smyth RJ, Samson M, Peiper SC, Parmentier M, Collman RG, Doms RW (1996) A dual-tropic primary HIV-1 isolate that uses fusin and the beta- chemokine receptors CKR5, CKR3, and CKR2b as fusion cofactors. Cell 85:1149–1158
Dragic T, Litwin V, Allaway GP, Martin SR, Huang Y, Nagashima KA, Cayanan C, Maddon PJ, Koup RA, Moore JP, Paxton WA (1996) HIV-1 entry into CD4+ cells is mediated by the chemokine receptor CC-CKR-5. Nature 381:667–673
Durig J, Schmucker U, Duhrsen U (2001) Differential expression of chemokine receptors in B cell malignancies. Leukemia 15:752–756
Eggert D, Dash PK, Gorantla S, Dou H, Schifitto G, Maggirwar SB, Dewhurst S, Poluektova L, Gelbard HA, Gendelman HE (2010) Neuroprotective activities of CEP-1347 in models of neuroAIDS. J Immunol 184:746–756
Ellis R, Langford D, Masliah E (2007) HIV and antiretroviral therapy in the brain: neuronal injury and repair. Nat Rev Neurosci 8:33–44
Finco O, Nuti S, De Magistris MT, Mangiavacchi L, Aiuti A, Forte P, Fantoni A, van der Putten H, Abrignani S (1997) Induction of CD4+ T cell depletion in mice doubly transgenic for HIV gp120 and human CD4. Eur J Immunol 27:1319–1324
Garden GA, Budd SL, Tsai E, Hanson L, Kaul M, D’Emilia DM, Friedlander RM, Yuan J, Masliah E, Lipton SA (2002) Caspase cascades in human immunodeficiency virus-associated neurodegeneration. J Neurosci 22:4015–4024
Gardner MB, Luciw PA (1989) Animal models of AIDS. FASEB J 3:2593–2606
Giulian D, Vaca K, Noonan CA (1990) Secretion of neurotoxins by mononuclear phagocytes infected with HIV-1. Science 250:1593–1596
Giulian D, Wendt E, Vaca K, Noonan CA (1993) The envelope glycoprotein of human immunodeficiency virus type 1 stimulates release of neurotoxins from monocytes. Proc Natl Acad Sci U S A 90:2769–2773
Glass JD, Fedor H, Wesselingh SL, McArthur JC (1995) Immunocytochemical quantitation of human immunodeficiency virus in the brain: correlations with dementia. Ann Neurol 38:755–762
Glass WG, Lim JK, Cholera R, Pletnev AG, Gao JL, Murphy PM (2005) Chemokine receptor CCR5 promotes leukocyte trafficking to the brain and survival in West Nile virus infection. J Exp Med 202:1087–1098
Gonzalez-Scarano F, Martin-Garcia J (2005) The neuropathogenesis of AIDS. Nat Rev Immunol 5:69–81
Gorry PR, Ancuta P (2011) Coreceptors and HIV-1 pathogenesis. Curr HIV/AIDS Rep 8:45–53
Hahn BH, Shaw GM, Arya SK, Popovic M, Gallo RC, Wong-Staal F (1984) Molecular cloning and characterization of the HTLV-III virus associated with AIDS. Nature 312:166–169
Halks-Miller M, Hesselgesser J, Miko IJ, Horuk R (1997) Chemokine receptors in developing human brain. Methods Enzymol 288:27–38
Hanna Z, Kay DG, Cool M, Jothy S, Rebai N, Jolicoeur P (1998a) Transgenic mice expressing human immunodeficiency virus type 1 in immune cells develop a severe AIDS-like disease. J Virol 72:121–132
Hanna Z, Kay DG, Rebai N, Guimond A, Jothy S, Jolicoeur P (1998b) Nef harbors a major determinant of pathogenicity for an AIDS-like disease induced by HIV-1 in transgenic mice. Cell 95:163–175
Hauser KF, Hahn YK, Adjan VV, Zou S, Buch SK, Nath A, Bruce-Keller AJ, Knapp PE (2009) HIV-1 Tat and morphine have interactive effects on oligodendrocyte survival and morphology. Glia 57:194–206
He J, Chen Y, Farzan M, Choe H, Ohagen A, Gartner S, Busciglio J, Yang X, Hofmann W, Newman W, Mackay CR, Sodroski J, Gabuzda D (1997) CCR3 and CCR5 are co-receptors for HIV-1 infection of microglia. Nature 385:645–649
Hesselgesser J, Halks-Miller M, DelVecchio V, Peiper SC, Hoxie J, Kolson DL, Taub D, Horuk R (1997) CD4-independent association between HIV-1 gp120 and CXCR4: functional chemokine receptors are expressed in human neurons. Curr Biol 7:112–121
Hesselgesser J, Taub D, Baskar P, Greenberg M, Hoxie J, Kolson DL, Horuk R (1998) Neuronal apoptosis induced by HIV-1 gp120 and the chemokine SDF-1 alpha is mediated by the chemokine receptor CXCR4. Curr Biol 8:595–598
Heyes MP, Brew BJ, Martin A, Price RW, Salazar AM, Sidtis JJ, Yergey JA, Mouradian MM, Sadler AE, Keilp J (1991) Quinolinic acid in cerebrospinal fluid and serum in HIV-1 infection: relationship to clinical and neurological status. Ann Neurol 29:202–209
Huffnagle GB, McNeil LK, McDonald RA, Murphy JW, Toews GB, Maeda N, Kuziel WA (1999) Cutting edge: role of C-C chemokine receptor 5 in organ-specific and innate immunity to Cryptococcus neoformans. J Immunol 163:4642–4646
Hutter G, Nowak D, Mossner M, Ganepola S, Mussig A, Allers K, Schneider T, Hofmann J, Kucherer C, Blau O, Blau IW, Hofmann WK, Thiel E (2009) Long-term control of HIV by CCR5 Delta32/Delta32 stem-cell transplantation. N Engl J Med 360:692–698
Iwakura Y, Shioda T, Tosu M, Yoshida E, Hayashi M, Nagata T, Shibuta H (1992) The induction of cataracts by HIV-1 in transgenic mice. AIDS 6:1069–1075
Jacobson S, Henriksen SJ, Prospero-Garcia O, Phillips TR, Elder JH, Young WG, Bloom FE, Fox HS (1997) Cortical neuronal cytoskeletal changes associated with FIV infection. J Neurovirol 3:283–289
Jones GJ, Barsby NL, Cohen EA, Holden J, Harris K, Dickie P, Jhamandas J, Power C (2007) HIV-1 Vpr causes neuronal apoptosis and in vivo neurodegeneration. J Neurosci 27:3703–3711
Kang YJ, Digicaylioglu M, Russo R, Kaul M, Achim CL, Fletcher L, Masliah E, Lipton SA (2010) Erythropoietin plus insulin-like growth factor-I protects against neuronal damage in a murine model of human immunodeficiency virus-associated neurocognitive disorders. Ann Neurol 68:342–352
Kaul M (2008) HIV’s double strike at the brain: neuronal toxicity and compromised neurogenesis. Front Biosci 13:2484–2494
Kaul M, Lipton SA (1999) Chemokines and activated macrophages in HIV gp120-induced neuronal apoptosis. Proc Natl Acad Sci U S A 96:8212–8216
Kaul M, Garden GA, Lipton SA (2001) Pathways to neuronal injury and apoptosis in HIV-associated dementia. Nature 410:988–994
Kaul M, Ma Q, Medders KE, Desai MK, Lipton SA (2007) HIV-1 coreceptors CCR5 and CXCR4 both mediate neuronal cell death but CCR5 paradoxically can also contribute to protection. Cell Death Differ 14:296–305
Keppler OT, Welte FJ, Ngo TA, Chin PS, Patton KS, Tsou CL, Abbey NW, Sharkey ME, Grant RM, You Y, Scarborough JD, Ellmeier W, Littman DR, Stevenson M, Charo IF, Herndier BG, Speck RF, Goldsmith MA (2002) Progress toward a human CD4/CCR5 transgenic rat model for de novo infection by human immunodeficiency virus type 1. J Exp Med 195:719–736
Khan IA, Thomas SY, Moretto MM, Lee FS, Islam SA, Combe C, Schwartzman JD, Luster AD (2006) CCR5 is essential for NK cell trafficking and host survival following Toxoplasma gondii infection. PLoS Pathog 2:e49
Kim BO, Liu Y, Ruan Y, Xu ZC, Schantz L, He JJ (2003) Neuropathologies in transgenic mice expressing human immunodeficiency virus type 1 Tat protein under the regulation of the astrocyte-specific glial fibrillary acidic protein promoter and doxycycline. Am J Pathol 162:1693–1707
Klotman PE, Notkins AL (1996) Transgenic models of human immunodeficiency virus type-1. Curr Top Microbiol Immunol 206:197–222
Koenig S, Gendelman HE, Orenstein JM, Dal Canto MC, Pezeshkpour GH, Yungbluth M, Janotta F, Aksamit A, Martin MA, Fauci AS (1986) Detection of AIDS virus in macrophages in brain tissue from AIDS patients with encephalopathy. Science 233:1089–1093
Kraft-Terry SD, Buch SJ, Fox HS, Gendelman HE (2009) A coat of many colors: neuroimmune crosstalk in human immunodeficiency virus infection. Neuron 64:133–145
Krathwohl MD, Kaiser JL (2004) HIV-1 promotes quiescence in human neural progenitor cells. J Infect Dis 190:216–226
Krucker T, Toggas SM, Mucke L, Siggins GR (1998) Transgenic mice with cerebral expression of human immunodeficiency virus type-1 coat protein gp120 show divergent changes in short- and long-term potentiation in CA1 hippocampus. Neuroscience 83:691–700
Lannuzel A, Lledo PM, Lamghitnia HO, Vincent JD, Tardieu M (1995) HIV-1 envelope proteins gp120 and gp160 potentiate NMDA [Ca2+]i increase, alter [Ca2+]i homeostasis and induce neurotoxicity in human embryonic neurons. Eur J Neurosci 7:2285–2293
Lavi E, Strizki JM, Ulrich AM, Zhang W, Fu L, Wang Q, O’Connor M, Hoxie JA, Gonzalez-Scarano F (1997) CXCR-4 (fusin), a co-receptor for the type 1 human immunodeficiency virus (HIV-1), is expressed in the human brain in a variety of cell types, including microglia and neurons. Am J Pathol 151:1035–1042
Lee YK, Kwak DH, Oh KW, Nam SY, Lee BJ, Yun YW, Kim YB, Han SB, Hong JT (2009) CCR5 deficiency induces astrocyte activation, Abeta deposit and impaired memory function. Neurobiol Learn Mem 92:356–363
Lee MH, Wang T, Jang MH, Steiner J, Haughey N, Ming GL, Song H, Nath A, Venkatesan A (2011) Rescue of adult hippocampal neurogenesis in a mouse model of HIV neurologic disease. Neurobiol Dis 41:678–687
Leonard JM, Abramczuk JW, Pezen DS, Rutledge R, Belcher JH, Hakim F, Shearer G, Lamperth L, Travis W, Fredrickson T (1988) Development of disease and virus recovery in transgenic mice containing HIV proviral DNA. Science 242:1665–1670
Limoges J, Persidsky Y, Poluektova L, Rasmussen J, Ratanasuwan W, Zelivyanskaya M, McClernon DR, Lanier ER, Gendelman HE (2000) Evaluation of antiretroviral drug efficacy for HIV-1 encephalitis in SCID mice. Neurology 54:379–389
Lindl KA, Marks DR, Kolson DL, Jordan-Sciutto KL (2010) HIV-associated neurocognitive disorder: pathogenesis and therapeutic opportunities. J Neuroimmune Pharmacol 5:294–309
Liu Y, Jones M, Hingtgen CM, Bu G, Laribee N, Tanzi RE, Moir RD, Nath A, He JJ (2000) Uptake of HIV-1 Tat protein mediated by low-density lipoprotein receptor-related protein disrupts the neuronal metabolic balance of the receptor ligands. Nat Med 6:1380–1387
Liu Y, Liu H, Kim BO, Gattone VH, Li J, Nath A, Blum J, He JJ (2004) CD4-independent infection of astrocytes by human immunodeficiency virus type 1: requirement for the human mannose receptor. J Virol 78:4120–4133
Locati M, Murphy PM (1999) Chemokines and chemokine receptors: biology and clinical relevance in inflammation and AIDS. Annu Rev Med 50:425–440
Lu M, Grove EA, Miller RJ (2002) Abnormal development of the hippocampal dentate gyrus in mice lacking the CXCR4 chemokine receptor. Proc Natl Acad Sci U S A 99:7090–7095
Luangsay S, Kasper LH, Rachinel N, Minns LA, Mennechet FJ, Vandewalle A, Buzoni-Gatel D (2003) CCR5 mediates specific migration of Toxoplasma gondii-primed CD8 lymphocytes to inflammatory intestinal epithelial cells. Gastroenterology 125:491–500
Ma Q, Jones D, Borghesani PR, Segal RA, Nagasawa T, Kishimoto T, Bronson RT, Springer TA (1998) Impaired B-lymphopoiesis, myelopoiesis, and derailed cerebellar neuron migration in CXCR4- and SDF-1-deficient mice. Proc Natl Acad Sci U S A 95:9448–9453
Ma B, Kang MJ, Lee CG, Chapoval S, Liu W, Chen Q, Coyle AJ, Lora JM, Picarella D, Homer RJ, Elias JA (2005) Role of CCR5 in IFN-gamma-induced and cigarette smoke-induced emphysema. J Clin Invest 115:3460–3472
Machado FS, Koyama NS, Carregaro V, Ferreira BR, Milanezi CM, Teixeira MM, Rossi MA, Silva JS (2005) CCR5 plays a critical role in the development of myocarditis and host protection in mice infected with Trypanosoma cruzi. J Infect Dis 191:627–636
Marshall DC, Wyss-Coray T, Abraham CR (1998) Induction of matrix metalloproteinase-2 in human immunodeficiency virus-1 glycoprotein 120 transgenic mouse brains. Neurosci Lett 254:97–100
Masliah E, Heaton RK, Marcotte TD, Ellis RJ, Wiley CA, Mallory M, Achim CL, McCutchan JA, Nelson JA, Atkinson JH, Grant I (1997a) Dendritic injury is a pathological substrate for human immunodeficiency virus-related cognitive disorders. HNRC group. The HIV Neurobehavioral Research Center. Ann Neurol 42:963–972
Masliah E, Westland CE, Rockenstein EM, Abraham CR, Mallory M, Veinberg I, Sheldon E, Mucke L (1997b) Amyloid precursor proteins protect neurons of transgenic mice against acute and chronic excitotoxic injuries in vivo. Neuroscience 78:135–146
Mattson MP, Haughey NJ, Nath A (2005) Cell death in HIV dementia. Cell Death Differ 12:893–904
Maung R, Sejbuk NE, Russo R, Hoefer MM, Sanchez AB, Medders KE, Desai MK, Catalan IC, Cox CJ, DeRozieres CM, Garden GA, Roberts AJ, Williams R, Kaul M (2011) CCR5 controls brain injury in a transgenic mice expressing HIV-1 envelope glycoprotein 120 (manuscript in preparation)
Medders KE, Sejbuk NE, Maung R, Desai MK, Kaul M (2010) Activation of p38 MAPK is required in monocytic and neuronal cells for HIV glycoprotein 120-induced neurotoxicity. J Immunol 185:4883–4895
Meeker RB, Thiede BA, Hall C, English R, Tompkins M (1997) Cortical cell loss in asymptomatic cats experimentally infected with feline immunodeficiency virus. AIDS Res Hum Retrovir 13:1131–1140
Meucci O, Miller RJ (1996) Gp120-induced neurotoxicity in hippocampal pyramidal neuron cultures: protective action of TGF-beta1. J Neurosci 16:4080–4088
Meucci O, Fatatis A, Simen AA, Bushell TJ, Gray PW, Miller RJ (1998) Chemokines regulate hippocampal neuronal signaling and gp120 neurotoxicity. Proc Natl Acad Sci U S A 95:14500–14505
Michael NL, Moore JP (1999) HIV-1 entry inhibitors: evading the issue. Nat Med 5:740–742
Miller RJ, Rostene W, Apartis E, Banisadr G, Biber K, Milligan ED, White FA, Zhang J (2008) Chemokine action in the nervous system. J Neurosci 28:11792–11795
Mucke L, Abraham CR, Ruppe MD, Rockenstein EM, Toggas SM, Mallory M, Alford M, Masliah E (1995) Protection against HIV-1 gp120-induced brain damage by neuronal expression of human amyloid precursor protein. J Exp Med 181:1551–1556
Nath BM, Schumann KE, Boyer JD (2000) The chimpanzee and other non-human-primate models in HIV-1 vaccine research. Trends Microbiol 8:426–431
Nitcheu J, Bonduelle O, Combadiere C, Tefit M, Seilhean D, Mazier D, Combadiere B (2003) Perforin-dependent brain-infiltrating cytotoxic CD8+ T lymphocytes mediate experimental cerebral malaria pathogenesis. J Immunol 170:2221–2228
O’Donnell LA, Agrawal A, Jordan-Sciutto KL, Dichter MA, Lynch DR, Kolson DL (2006) Human immunodeficiency virus (HIV)-induced neurotoxicity: roles for the NMDA receptor subtypes. J Neurosci 26:981–990
Okamoto S, Kang YJ, Brechtel CW, Siviglia E, Russo R, Clemente A, Harrop A, McKercher S, Kaul M, Lipton SA (2007) HIV/gp120 decreases adult neural progenitor cell proliferation via checkpoint kinase-mediated cell-cycle withdrawal and G1 arrest. Cell Stem Cell 1:230–236
Olmsted RA, Barnes AK, Yamamoto JK, Hirsch VM, Purcell RH, Johnson PR (1989) Molecular cloning of feline immunodeficiency virus. Proc Natl Acad Sci U S A 86:2448–2452
Pantaleo G, Fauci AS (1995) Apoptosis in HIV infection. Nat Med 1:118–120
Perfettini JL, Castedo M, Nardacci R, Ciccosanti F, Boya P, Roumier T, Larochette N, Piacentini M, Kroemer G (2005a) Essential role of p53 phosphorylation by p38 MAPK in apoptosis induction by the HIV-1 envelope. J Exp Med 201:279–289
Perfettini JL, Castedo M, Roumier T, Andreau K, Nardacci R, Piacentini M, Kroemer G (2005b) Mechanisms of apoptosis induction by the HIV-1 envelope. Cell Death Differ 12(Suppl 1):916–923
Persidsky Y, Limoges J, McComb R, Bock P, Baldwin T, Tyor W, Patil A, Nottet HS, Epstein L, Gelbard H, Flanagan E, Reinhard J, Pirruccello SJ, Gendelman HE (1996) Human immunodeficiency virus encephalitis in SCID mice. Am J Pathol 149:1027–1053
Petito CK, Cho ES, Lemann W, Navia BA, Price RW (1986) Neuropathology of acquired immunodeficiency syndrome (AIDS): an autopsy review. J Neuropathol Exp Neurol 45:635–646
Poluektova LY, Munn DH, Persidsky Y, Gendelman HE (2002) Generation of cytotoxic T cells against virus-infected human brain macrophages in a murine model of HIV-1 encephalitis. J Immunol 168:3941–3949
Poluektova L, Meyer V, Walters L, Paez X, Gendelman HE (2005) Macrophage-induced inflammation affects hippocampal plasticity and neuronal development in a murine model of HIV-1 encephalitis. Glia 52:344–353
Porcheray F, Samah B, Leone C, Dereuddre-Bosquet N, Gras G (2006) Macrophage activation and human immunodeficiency virus infection: HIV replication directs macrophages towards a pro-inflammatory phenotype while previous activation modulates macrophage susceptibility to infection and viral production. Virology 349:112–120
Potash MJ, Chao W, Bentsman G, Paris N, Saini M, Nitkiewicz J, Belem P, Sharer L, Brooks AI, Volsky DJ (2005) A mouse model for study of systemic HIV-1 infection, antiviral immune responses, and neuroinvasiveness. Proc Natl Acad Sci U S A 102:3760–3765
Potteaux S, Combadiere C, Esposito B, Lecureuil C, it-Oufella H, Merval R, Ardouin P, Tedgui A, Mallat Z (2006) Role of bone marrow-derived CC-chemokine receptor 5 in the development of atherosclerosis of low-density lipoprotein receptor knockout mice. Arterioscler Thromb Vasc Biol 26:1858–1863
Raber J, Toggas SM, Lee S, Bloom FE, Epstein CJ, Mucke L (1996) Central nervous system expression of HIV-1 Gp120 activates the hypothalamic-pituitary-adrenal axis: evidence for involvement of NMDA receptors and nitric oxide synthase. Virology 226:362–373
Reid W, Sadowska M, Denaro F, Rao S, Foulke J Jr, Hayes N, Jones O, Doodnauth D, Davis H, Sill A, O’Driscoll P, Huso D, Fouts T, Lewis G, Hill M, Kamin-Lewis R, Wei C, Ray P, Gallo RC, Reitz M, Bryant J (2001) An HIV-1 transgenic rat that develops HIV-related pathology and immunologic dysfunction. Proc Natl Acad Sci U S A 98:9271–9276
Roberts AJ, Maung R, Sejbuk NE, Ake C, Kaul M (2009) Alteration of Methamphetamine-induced stereotypic behaviour in transgenic mice expressing HIV-1 envelope protein gp120. J Neurosci Methods 186:222–225. doi:10.1016/j.jneumeth.2009.11.007
Rot A, von Andrian UH (2004) Chemokines in innate and adaptive host defense: basic chemokinese grammar for immune cells. Annu Rev Immunol 22:891–928
Rottman JB, Ganley KP, Williams K, Wu L, Mackay CR, Ringler DJ (1997) Cellular localization of the chemokine receptor CCR5. Correlation to cellular targets of HIV-1 infection. Am J Pathol 151:1341–1351
Sas AR, Bimonte-Nelson HA, Tyor WR (2007) Cognitive dysfunction in HIV encephalitic SCID mice correlates with levels of Interferon-alpha in the brain. AIDS 21:2151–2159
Seki E, De MS, Gwak GY, Kluwe J, Inokuchi S, Bursill CA, Llovet JM, Brenner DA, Schwabe RF (2009) CCR1 and CCR5 promote hepatic fibrosis in mice. J Clin Invest 119:1858–1870
Shiramizu B, Gartner S, Williams A, Shikuma C, Ratto-Kim S, Watters M, Aguon J, Valcour V (2005) Circulating proviral HIV DNA and HIV-associated dementia. AIDS 19:45–52
Shiramizu B, Ratto-Kim S, Sithinamsuwan P, Nidhinandana S, Thitivichianlert S, Watt G, Desouza M, Chuenchitra T, Sukwit S, Chitpatima S, Robertson K, Paul R, Shikuma C, Valcour V (2006) HIV DNA and dementia in treatment-Naive HIV-1-infected individuals in Bangkok, Thailand. Int J Med Sci 4:13–18
Singh IN, El-Hage N, Campbell ME, Lutz SE, Knapp PE, Nath A, Hauser KF (2005) Differential involvement of p38 and JNK MAP kinases in HIV-1 Tat and gp120-induced apoptosis and neurite degeneration in striatal neurons. Neuroscience 135:781–790
Stumm RK, Zhou C, Ara T, Lazarini F, Dubois-Dalcq M, Nagasawa T, Hollt V, Schulz S (2003) CXCR4 regulates interneuron migration in the developing neocortex. J Neurosci 23:5123–5130
Tachibana K, Hirota S, Iizasa H, Yoshida H, Kawabata K, Kataoka Y, Kitamura Y, Matsushima K, Yoshida N, Nishikawa S, Kishimoto T, Nagasawa T (1998) The chemokine receptor CXCR4 is essential for vascularization of the gastrointestinal tract. Nature 393:591–594
Teixeira MM, Vilela MC, Soriani FM, Rodrigues DH, Teixeira AL (2010) Using intravital microscopy to study the role of chemokines during infection and inflammation in the central nervous system. J Neuroimmunol 224:62–65
Thapa M, Kuziel WA, Carr DJ (2007) Susceptibility of CCR5-deficient mice to genital herpes simplex virus type 2 is linked to NK cell mobilization. J Virol 81:3704–3713
Thomas FP, Chalk C, Lalonde R, Robitaille Y, Jolicoeur P (1994) Expression of human immunodeficiency virus type 1 in the nervous system of transgenic mice leads to neurological disease. J Virol 68:7099–7107
Toggas SM, Mucke L (1996) Transgenic models in the study of AIDS dementia complex. Curr Top Microbiol Immunol 206:223–241
Toggas SM, Mucke L (1998) Transgenic models to assess the pathogenic potential of viral products in HIV-1-associated CNS disease. In: Gendelman HE, Lipton SA, Epstein L, Swindells S (eds) The neurology of AIDS. Chapman & Hall, New York, pp 156–167
Toggas SM, Masliah E, Rockenstein EM, Rall GF, Abraham CR, Mucke L (1994) Central nervous system damage produced by expression of the HIV-1 coat protein gp120 in transgenic mice. Nature 367:188–193
Toggas SM, Masliah E, Mucke L (1996) Prevention of HIV-1 gp120-induced neuronal damage in the central nervous system of transgenic mice by the NMDA receptor antagonist memantine. Brain Res 706:303–307
Toneatto S, Finco O, van der Putten H, Abrignani S, Annunziata P (1999) Evidence of blood–brain barrier alteration and activation in HIV-1 gp120 transgenic mice. AIDS 13:2343–2348
Tran PB, Ren D, Miller RJ (2005) The HIV-1 coat protein gp120 regulates CXCR4-mediated signaling in neural progenitor cells. J Neuroimmunol 160:68–76
Valentin A, Trivedi H, Lu W, Kostrikis LG, Pavlakis GN (2000) CXCR4 mediates entry and productive infection of syncytia-inducing (X4) HIV-1 strains in primary macrophages. Virology 269:294–304
Van Duyne R, Pedati C, Guendel I, Carpio L, Kehn-Hall K, Saifuddin M, Kashanchi F (2009) The utilization of humanized mouse models for the study of human retroviral infections. Retrovirology 6:76
Wang EJ, Sun J, Pettoello-Mantovani M, Anderson CM, Osiecki K, Zhao ML, Lopez L, Lee SC, Berman JW, Goldstein H (2003) Microglia from mice transgenic for a provirus encoding a monocyte-tropic HIV type 1 isolate produce infectious virus and display in vitro and in vivo upregulation of lipopolysaccharide-induced chemokine gene expression. AIDS Res Hum Retrovir 19:755–765
Wang YJ, Wang X, Zhang H, Zhou L, Liu S, Kolson DL, Song L, Ye L, Ho WZ (2009) Expression and regulation of antiviral protein APOBEC3G in human neuronal cells. J Neuroimmunol 206:14–21
Wesselingh SL, Takahashi K, Glass JD, McArthur JC, Griffin JW, Griffin DE (1997) Cellular localization of tumor necrosis factor mRNA in neurological tissue from HIV-infected patients by combined reverse transcriptase/polymerase chain reaction in situ hybridization and immunohistochemistry. J Neuroimmunol 74:1–8
Wiley CA, Masliah E, Achim CL (1994) Measurement of CNS HIV burden and its association with neurologic damage. Adv Neuroimmunol 4:319–325
Wyss-Coray T, Masliah E, Toggas SM, Rockenstein EM, Brooker MJ, Lee HS, Mucke L (1996) Dysregulation of signal transduction pathways as a potential mechanism of nervous system alterations in HIV-1 gp120 transgenic mice and humans with HIV-1 encephalitis. J Clin Invest 97:789–798
Zernecke A, Liehn EA, Gao JL, Kuziel WA, Murphy PM, Weber C (2006) Deficiency in CCR5 but not CCR1 protects against neointima formation in atherosclerosis-prone mice: involvement of IL-10. Blood 107:4240–4243
Zhou Y, Kurihara T, Ryseck RP, Yang Y, Ryan C, Loy J, Warr G, Bravo R (1998) Impaired macrophage function and enhanced T cell-dependent immune response in mice lacking CCR5 the mouse homologue of the major HIV-1 coreceptor. J Immunol 160:4018–4025
Zlotnik A, Yoshie O (2000) Chemokines: a new classification system and their role in immunity. Immunity 12:121–127
Zou YR, Kottmann AH, Kuroda M, Taniuchi I, Littman DR (1998) Function of the chemokine receptor CXCR4 in haematopoiesis and in cerebellar development. Nature 393:595–599
Acknowledgments
M.K. is supported by grants from the National Institutes of Health, MH087332, DA026306 and DA029480.
Conflict of interest disclosure
The authors state that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maung, R., Medders, K.E., Sejbuk, N.E. et al. Genetic Knockouts Suggest a Critical Role for HIV Co-Receptors in Models of HIV gp120-Induced Brain Injury. J Neuroimmune Pharmacol 7, 306–318 (2012). https://doi.org/10.1007/s11481-011-9328-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-011-9328-x