Abstract
Proinflammatory cytokines and chemokines have been implicated in the pathogenesis of several neurological and neurodegenerative disorders. Prominent among such factors is the pleiotropic cytokine, tumor necrosis factor (TNF)-α. Under normal physiological conditions, TNF-α orchestrates a diverse array of functions involved in immune surveillance and defense, cellular homeostasis, and protection against certain neurological insults. However, paradoxical effects of this cytokine have been observed. TNF-α is elicited in the brain following injury (ischemia, trauma), infection (HIV, meningitis), neurodegeneration (Alzheimer’s, Parkinson’s), and chemically induced neurotoxicity. The multifarious identity for this cytokine appears to be influenced by several mechanisms. Among the most prominent are the regulation of TNFα-induced NF-κB activation by adapter proteins such as TRADD and TRAF, and second, the heterogeneity of microglia and their distribution pattern across brain regions. Here, we review the differential role of TNF-α in response to brain injury, with emphasis on neurodegeneration, and discuss the possible mechanisms for such diverse and region-specific effects.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the central nervous system (CNS), the proinflammatory cytokine TNF-α is considered the principal mediator of neuroinflammation that elicits a cascade of cellular events culminating in neuronal death. At the same time, TNF-α affords neuroprotection in certain neurological conditions. Thus, TNF-α appears to exhibit a dual role in the brain, and such effects appear to vary across brain areas, thereby, complicating the understanding of this double-edged cytokine. Here, we review from literature, the neurotoxic and neuroprotective roles of this proinflammatory cytokine, survey the regional selectivity of its action, and discuss the possible mechanisms by which TNF-α mediates its conflicting effects in the CNS.
Proinflammatory responses in the brain
Brain immune and inflammatory responses occur as a consequence of microglial activation. The magnitude of the neuroinflammatory response elicited depends on the spectrum of inflammatory mediators that are produced by neural cells in response to an insult. Cytokines, chemokines, prostaglandins, free radicals, pentraxins, complement components, anaphylotoxins, proteases, and adhesion molecules are among the several factors that mediate neuroinflammation (McGeer and McGeer 2004; Minghetti 2005). Neural injury can serve both as a cause and/or a consequence of cytokine or chemokine signaling. Cytokines are a family of low molecular weight, multifunctional pleiotrophic polypeptides that regulate cell activation, proliferation, and differentiation. Chemokines (chemoattractant cytokines) are low molecular weight (8–11 kDa) glycoproteins with potent leukocyte activation and chemotactic activity. In addition, they are known to play a role in cell cycle regulation and differentiation. Both cytokines and chemokines initiate and promulgate inflammatory reactions. The actions of such proinflammatory mediators contribute to manifestation of neurological (e.g., stroke), neurodegenerative (e.g., Parkinson’s disease, Alzheimer’s disease), infectious (e.g., HIV-1, bacterial or viral meningitis, cerebral malaria), autoimmune disease (e.g., multiple sclerosis) and chemically induced (MPTP, methamphetamine, kainic acid, 6-hydroxydopamine) neurotoxic conditions (Francis et al. 1995; Bruce et al. 1996; Seilhean et al. 1997; Munoz-Fernandez and Fresno 1998; Gartner and Liu 2002; Sriram et al. 2002a; McGeer and McGeer 2004; Minghetti 2005; Sriram et al. 2006a, b).
Sources of proinflammatory factors in the brain
The CNS has for long been regarded as an immune privileged organ, with the blood–brain barrier (BBB) tightly regulating the influx of immune cells and mediators from the vascular compartment to the brain parenchyma (Perry 1998). However, recent studies have shown that immune cells do migrate across the BBB and blood–cerebrospinal fluid barrier (BCSFB), albeit at very low levels, suggesting that immune surveillance can occur in the brain (Engelhardt 2006). Under normal physiological conditions, this immune cell entry is passive, due to the lack of antigenic presentation from major histocompatibility antigen (MHC) molecules. Furthermore, the unique CNS microenvironment regulates immune responses and migration of immune cells into the brain. However, under pathological conditions, immunocompetent cells can readily migrate across the endothelial BBB and epithelial BCSFB and enter the brain parenchyma.
This immune cell influx, during local infections and neuropathological event, is thought to be elicited by glial cells, especially the microglia. Mounting evidence indicate that microglia, in addition to their phagocytic function, gain antigen-presenting capabilities through expression of MHC components (Aloisi 2001; Carson et al. 2006). Microglia and astrocytes, the major glial cell types in the brain, become “activated” or “reactive” in response to diverse insults of the CNS (Table 1) and elicit a myriad of proinflammatory cytokines, chemokines, and trophic factors to render neural immunity (Raivich et al. 1996; Ransohoff et al. 1996; Stoll and Jander 1999). Microglia function as the microsensors of the brain and play an important role in detecting subtle changes in the neuronal microenvironment (Kreutzberg 1996). Both microglia and astrocytes express and release inflammatory mediators following brain injury, as seen in neurological and neurodegenerative disorders (Dickson et al. 1993; McGeer and McGeer 1998; Masliah and LiCastro 2000; Vila et al. 2001), and following experimental brain injury (Fan et al. 1996; Sriram et al. 2002a, 2006a, b).
Tumor necrosis factor (TNF)-α
TNF-α is synthesized as a 26-kDa membrane-bound polypeptide precursor that is cleaved by proteolysis to a 17-kDa subunit. The synthesis and secretion of TNF-α is regulated by TNF-α converting enzyme (TACE), a proteinase that is responsible for cleavage of TNF-α at the membrane surface. Upon cleavage, TNF-α is released as a bioactive homotrimer, which then exerts its effects in an autocrine and/or paracrine fashion. The biological actions of TNF-α are mediated through two distinct cell surface receptors, TNFR1 (p55) and TNFR2 (p75), to which it exhibits fairly equal affinity. Despite the fact that each TNF receptor mediates distinct cellular responses, there is considerable overlap of their signaling capabilities in mediating biological effects (Hsu et al. 1996; Declercq et al. 1998; Quintana et al. 2005). The differential patterns of localization of TNF receptors on neuronal or glial cells, their expression profile and activational state on these cells, and the down-stream effectors that they activate, are thought to play a critical role in determining if TNF-α will have a protective or cytotoxic role (Dopp et al. 1997, Sairanen et al. 2001, Fontaine et al. 2002; Dziewulska and Mossakowski 2003, Akassoglou et al. 2003). TNF receptors are members of the TNF superfamily and mediate signals via recruitment and inhibition of adapter proteins. Briefly, upon receptor activation, the adapter proteins, TNFR-associated death protein (TRADD) and differentially expressed normal versus neoplastic/MAPK activating death domain (DENN/MADD) bind to TNFR through the death domains (DD). Subsequently, Fas-associated death domain (FADD), receptor-interacting protein (RIP) and/or TNFR-associated factors (TRAFs) are recruited to promote physiological actions (see recent reviews, Aggarwal 2003; Hehlgans and Pfeffer 2005).
To delineate the beneficial and detrimental effects of TNF-α in the brain and to better understand its mechanisms of action, we review from literature the neurotoxic and neuroprotective roles of this proinflammatory cytokine and discuss the factors that may potentially influence its divergent actions.
Neurotoxic effects of TNF-α
TNF-α can be potently induced following brain injury and promote neuroinflammation and neurodegeneration. Elevated levels of this cytokine have been associated with the pathological effects of a variety of infectious, neurological, neurodegenerative, and neurotoxic conditions. Infectious diseases of the CNS are of bacterial or viral origin and affect the meninges (e.g., bacterial meningitis) or the parenchyma (e.g., viral encephalitis), respectively. Increased levels of TNF-α were detected in the CSF of patients with meningitis of bacterial but not viral origin. Elevated levels of TNF-α have been observed in the brain, cerebrospinal fluid (CSF), and serum of patients with Alzheimer’s disease (AD), Parkinson’s disease (PD), multiple sclerosis (MS) and HIV-dementia, and following brain injury and chemical-induced neurotoxicity (see Table 2 for a listing of various studies documenting the neurotoxic effects of TNF-α).
In patients with AD, amyloid plaques characterized by in-filtered microglia were found to express high levels of TNF-α (Dickson et al. 1993; Eikelenboom et al. 2000). Late-onset AD is associated with three TNF polymorphisms: a-308 TNF promoter polymorphism, a-238 TNF promoter polymorphism, and a microsatellite TNF-α, which form a 2-1-2 haplotype (Collins et al. 2000). In experimental models of AD, β-amyloid triggers microglial activation and elicits the expression of TNF-α (Meda et al. 1995). Similarly, in a triple transgenic AD (3xTg-AD) mouse model, characterized by amyloid and neurofibrillary tangle deposition, neuroinflammatory responses occurred very early in the injury process, resulting in accumulation of TNF-α (Janelsins et al. 2005). These findings suggest the involvement of TNF-α-mediated inflammation in the pathogenesis of AD.
In patients with PD, significant increases in the expression of TNF-á have been reported in the caudate and putamen of postmortem brain samples (Boka et al. 1994; Mogi et al. 1994, Mogi et al. 1995). Unlike the association of TNF haplotype with late-onset AD, polymorphism of TNF gene in patients with PD has been associated with the early onset of the disease. The frequency of the −1031C allele, a high producer of TNF, increased significantly in early onset PD patients, suggesting a toxic role for TNF in PD (Nishimura et al. 2001). Increased expression of TNF-α has also been observed in several experimental models of PD (Mogi et al. 1999; Sriram et al. 2002a; Ferger et al. 2004; Sriram et al. 2006a, b).
TNF-α is implicated in the pathogenesis of MS. Increased levels of TNF-α protein were found in brain lesions, CSF, and serum of patients with MS (Hauser et al. 1990; Cannella and Raine 1995; Martino et al. 1997). In experimental allergic encephalomyelitis (EAE) animal models, increased TNF-α in the serum and CSF correlates with the peak symptoms (Villarroya et al. 1997).
In HIV-dementia, TNF-α is a predictor of neurotoxicity, and significant levels of this cytokine were found in the brains of HIV-seropositive patients with AIDS dementia, but not in non-demented patients (Wesselingh et al. 1993, Wesselingh et al. 1997). Scid mice inoculated with HIV-infected human macrophages develop HIV infection and express TNF-α (Tyor et al. 1993). Increased TNF-α expression in perivascular macrophages, microglia, and endothelial cells was detected in midfrontal cortex, subcortical and deep white matter, and basal ganglia of patients with AIDS dementia complex (Seilhean et al. 1997). Recent comprehensive reviews discuss at length the role of TNF-α in HIV-dementia (Saha and Pahan 2003; Brabers and Nottet 2006).
In ischemic brain injury, TNF-α may play a critical role in the injury process. High levels of this cytokine have been reported in ischemic stroke models (Tarkowski et al. 1999, Vila et al. 2000; Intiso et al. 2004). In experimental models of ischemia, TNF-α was induced very early in the injury process and in a region-specific fashion (Liu et al. 1994; Saito et al. 1996). Saito et al. (1996) demonstrated that following transient global ischemia, TNF-α was selectively induced in the striatum and hippocampus but not in other brain areas. Furthermore, the expression of TNF-α following ischemic brain injury appeared to occur first in neurons, and a delayed expression of this cytokine was localized to glial cells (Meistrell et al. 1997; Buttini et al. 1996). Barone et al. (1997) have reported that following permanent middle cerebral artery occlusion (MCAO), the induction of TNF-α was associated with exacerbation of neurological deficits and infarct size, implicating this cytokine as a key player in ischemic brain injury.
TNF-α is also involved in traumatic brain injury. High levels of TNF-α have been reported in serum and CSF of patients with head injury (Goodman et al. 1990; Ross et al. 1994). In experimental models of traumatic brain injury, such as the fluid percussion injury (Taupin et al. 1993, Fan et al. 1996; Kita et al. 1997) and weight-drop contusion injury (Holmin et al. 1997), elevated levels of several cytokines including TNF-α were found. Similarly, in experimental closed head injury, activation of the complement component and increased expression of TNF-α has been reported (Shohami et al. 1994; Stahel et al. 2000).
Confirmation for the neurotoxic role of TNF-α comes from studies carried out to neutralize or antagonize the actions of TNF-α. Neutralizing antibodies against TNF-α were shown to be protective against cerebral ischemia (Lavine et al. 1998). Pretreatment with monoclonal antibodies to TNF-α reduced infarct volume and improved the neurological outcome. Similarly, neutralizing TNF-α activity with a recombinant type I soluble TNF receptor (TNF-binding protein, TNFbp), protected against microvascular perfusion impairment and ischemic injury induced by permanent MCAO (Dawson et al. 1996). Intrastriatal co-injections of TNFbp with N-methyl-d-aspartic acid (NMDA) reduced striatal injury, while intrahippocampal co-injections exacerbated excitotoxic damage (Galasso et al. 2000). Neutralizing soluble TNF with a dominant-negative TNF compound XENP345 was shown to protect against dopaminergic neurotoxicity (McCoy et al. 2006). XENP345, a PEGylated form of the TNF variant A145R/I97T, reduced retrograde nigral degeneration elicited by striatal injection of the dopaminergic neurotoxicant, 6-hydroxydopamine. Pharmacological intervention with MK-801, a noncompetitive NMDA receptor antagonist or dexamethasone was shown to exert neuroprotection against permanent MCAO. Both these agents blocked TNF-α production by 70% and reduced infarct size by nearly 50%, suggesting that despite their action at distinct cellular levels, these agents can modulate cerebral injury mediated by TNF-α. The immunosuppressant drug, FK506, is neuroprotective in experimental models of cerebral ischemia. FK506-mediated neuroprotection was shown to be associated with a selective decrease in the levels of TNF-α and IL-1β in glial cells. Thus, the mechanism of action of FK-506 seems to occur through modulation of glial response and inflammation (Zawadzka and Kaminska 2005). Pentoxifylline, a phosphodiesterase inhibitor and Dexanabinol (HU-211), a synthetic cannabinoid, have been shown to improve the outcome of experimental closed head injury mediated by TNF-α, especially when administered within the early time window of brain injury (Shohami et al. 1997). Similar to pentoxifylline, the specific type IV phosphodiesterase inhibitor rolipram, protected against striatal excitotoxic injury induced by quinolinic acid (Block et al. 2001). While anti-TNF strategies have been fairly successful in experimental models, their translation to clinical conditions has been hampered by high rate of severe side effects and/or failure to demonstrate significant survival benefit.
The mechanisms by which TNF-α appears to mediate its toxic effects (Skias et al. 1987; Benveniste et al. 1989; Shrikant et al. 1994; Chao and Hu 1994; Rosenberg et al. 1995; Probert and Selmaj 1997; Lucas et al. 1997; Koller 1997; Christov et al. 2004; Brabers and Nottet 2006) include (1) endothelial cell stimulation and alteration of blood–brain barrier integrity, thus, promoting immune cell adhesion and infiltration into the injured brain, (2) stimulation of apoptosis of brain microvascular endothelial cells, (3) activation of microglial cells, thereby, triggering a “vicious cycle” of oxidative outburst and inflammatory cytokine release, (4) modulation of the expression of MHC class components on neurons and astrocytes, thereby, rendering the astrocytes vulnerable to cytotoxic T-cells, (5) potentiation of glutamate-mediated toxicity by preventing glutamate uptake, (6) increase in vasogenic brain edema, (7) modulation of ion currents and intracellular calcium homeostasis, (8) regulation of membrane potential and long-term potentiation. Thus, TNF-α appears to be a central mediator of neuroinflammation and brain injury.
Neuroprotective effects of TNF-α
While several lines of evidence point towards a neurotoxic role for TNF-α in the CNS, this cytokine does not appear to be strictly neurotoxic. Besides its key role in maintaining CNS homeostasis, TNF-α is known to influence survival, differentiation, proliferation, and growth. These features highlight a potential protective role for this cytokine. Indeed, this cytokine has been shown to afford protection against brain injury (Table 3). TNF-α has been shown to promote reparative remyelination in an experimental model of demyelination (Plant et al. 2005). In this case, TNF-α appears to promote the survival of oligodendroglia, thereby, facilitating remyelination. TNF-α protects against the neuronal cell death induced by β-amyloid peptide (Barger et al. 1995; Goodman and Mattson 1996; Kaltschmidt et al. 1999). The protective mechanism was attributed to the role of TNF-α in regulating peroxide formation, calcium accumulation, activation of NF-κB, and antioxidant pathways. In another study (Houzen et al. 1997), cerebral cortical neurons were protected against NMDA-induced neurotoxicity by TNF-mediated mechanisms. Here, TNF-α regulated the voltage-gated membrane currents, particularly the outward potassium current density (A-current). Thus, an increase of A-current density induced by TNF-α contributed to neuroprotection.
Preconditioning with TNF-α also appears to be neuroprotective in ischemic cerebral injury. Intracisternal administration of TNF-α significantly reduced infarct size and decreased microglial activation in a MCAO model of cerebral ischemia (Nawashiro et al. 1997). TNF-α-induced preconditioning mediated through ceramide, protected neurons against ischemic injury (Ginis et al. 2002). These findings suggest that TNF-α is involved in development of ischemic tolerance.
TNF-α plays a neuroprotective role against excitotoxic injury in the hippocampus (Cheng et al. 1994; Bruce et al. 1996; Gary et al. 1998). Excitotoxic death of cortical neurons mediated by NMDA was abolished by TNF-α (Carlson et al. 1998). Co-injections of TNF-α and NMDA into the hippocampus reduced excitotoxic injury; however, intrastriatal co-injections did not alter the severity of injury (Liu et al. 1999). TNF-α also mediates neuroprotection in response to acute nitric oxide excitotoxicity (Turrin and Rivest 2006). Whereas elevated levels of TNF-α are associated with neuroprotection against excitotoxic damage in hippocampus, a lack of enhanced expression of TNF-α in hippocampus is associated with significant chemically induced damage to this structure (Little et al. 2002).
The emergence of knockout and transgenic technologies has revolutionized the approach towards understanding the functional role of genes. In this regard, the availability of transgenic mice lacking TNF, TNFR1, or TNFR2 genes has greatly facilitated research towards understanding the role of this proinflammatory cytokine in the brain. Mice deficient in both TNF receptors were found to be more susceptible to hippocampal excitotoxic and ischemic injury (Bruce et al. 1996; Gary et al. 1998). Similarly, exacerbation of damage and altered NF-κB activation was observed in TNF-deficient mice after traumatic brain injury (Sullivan et al. 1999). Mice lacking TNF receptors exhibited increased oxidative stress and striatal lesion size following 3-nitropropionic acid (3-NP) administration (Bruce-Keller et al. 1999). On the other hand, we have previously shown that mice lacking both TNF receptors, but not individual receptors, were protected against the dopaminergic neurotoxicity of 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP; Sriram et al. 2002a). These paradoxical findings suggested that TNF-α was capable of mediating differential effects in specific brain areas. Indeed, we recently demonstrated that TNF-α plays a region-specific role in the brain (Sriram et al. 2006a). While deficiency of TNF receptors blocked MPTP neurotoxicity in the striatum, the lack of these receptors rendered the hippocampus, an otherwise nontarget region for MPTP effects, vulnerable to injury. Thus, TNF-α serves to promote neurodegeneration in striatum, while affording protection against neurodegeneration in the hippocampus (Fig. 1, depicts the region-specific actions of TNF-α in a neurotoxic/neurodegenerative scenario). While knockout and transgenic technologies aid understanding of the gene function, there is limited knowledge of compensatory mechanisms associated with genetically modified animals. More recent approaches such as conditional knockouts and manipulation of genes via inducible promoters may perhaps provide a better understanding of the gene function in the future.
Schematic diagram depicting a region-specific role for TNF-α in the brain: neuronal injury is associated with release of “mysterious injury factors” that activate microglia and/or astroglia. There is heterogeneity in the distribution, morphology, and activation of microglia across brain areas. Striatal dopaminergic neurotoxicity is associated with microglial activation and elaboration of microglia-derived cytokines like TNF-α. TNF-α elicits dopaminergic nerve terminal degeneration by signaling through the TNF receptors localized on dopaminergic nerve terminals. Deficiency of TNF receptors suppresses microglial activation, and as a consequence, the dopaminergic neurotoxicity. Paradoxically, lack of TNF receptors renders the hippocampus vulnerable to neuronal degeneration. Thus, TNF-α plays a dual role in brain: neurotoxic in the striatum and neurotrophic in the hippocampus.
The mechanisms by which TNF-α appears to mediate its neuroprotective effects (Grassi et al. 1994; Barger et al. 1995; Mattson et al. 1995; Bizette et al. 1996; Goodman and Mattson 1996) include (1) activation of astroglia and stimulating neurotrophic factor release, (2) activation of repair processes of peripheral nerves and cerebral microvasculature, (3) stimulation of synaptic currents and thereby mediating neuronal plasticity, (4) activation of NF-κB pathway, (5) induction of anti-apoptotic factors such as Bcl-2, (6) ceramide-mediated induction of antioxidant defense pathways, (7) regulation of extracellular calcium and the calcium binding protein calbindin-D28K.
Factors influencing the divergent actions of TNF-α
Based on the extensive evidence reviewed above in relation to the neurotoxic and neuroprotective roles for TNF-α, sufficient data exist to indicate that this cytokine has paradoxical functions that can result in simultaneous stimulation of cell survival and death pathways. How the balance between these divergent roles is maintained determines the ultimate role for this cytokine.
While basal physiological levels of TNF-α are not necessarily indicative of a neuroprotective versus a neurotoxic function (Cheng et al. 1994; Mattson et al. 1995; Uno et al. 1997), differences in the levels and activational state of the TNF receptors and related downstream effectors may serve to confer differences in its role. The type 1 (TNFR1, p55) and type 2 (TNFR2, p75) TNF receptors are members of the TNF receptor superfamily, which includes other prominent receptors like Fas, lymphotoxin β receptor, p75 nerve growth factor receptor, and CD40, among others. These receptors share substantial homology, but function in a mechanistically diverse fashion (Sprang 1990, Tartaglia et al. 1991). Constitutive expression of TNF receptors is reported to occur in neurons and blood vessels; however, these receptors are expressed on glial cells (microglia and astroglia) and macrophages following brain injury. While TNFR2 appears to be predominantly expressed by macrophages, microglia exhibit a differential pattern of immunostaining for both TNF receptors (Dziewulska and Mossakowski 2003). Thus, the differential patterns of expression of TNF receptors on neuronal and glial cells are thought to play a critical role in determining if TNF-α will have a protective or cytotoxic role (Dopp et al. 1997, Sairanen et al. 2001, Fontaine et al. 2002; Dziewulska and Mossakowski 2003, Akassoglou et al. 2003). Upon activation, the TNF receptors interact with an array of intracellular adapter proteins to mediate downstream cell signaling. TNFR1 associates with TRADD, a death domain protein that transduces signals through FADD and FADD-like interleukin-1beta-converting enzyme (FLICE), and activates intracellular proteases of the caspase family. TNFR1 and TNFR2 also associate with TRAFs, which mediate activation of the nuclear factor kappa B (NF-κB) family of transcription factors. Specifically, TRAF2 mediates NF-κB activation via NF-κB inducing kinase (NIK), which leads to IκB degradation and release of NF-κB. Activation of NF-κB promotes gene expression that can elicit either neurotoxic or neuroprotective effects. Evidence for this dual role comes from studies that show that TNF-α-mediated induction of NF-κB is associated with neuronal survival (Barger et al. 1995; Kaltschmidt et al. 1999; Albensi and Mattson 2000) or the inability of TNF-α to induce NF-κB is associated with increased neurotoxicity (Botchkina et al. 1999; Sriram et al. 2006a). One possible reason for the diverse role exhibited by TNF-α could be attributed to the differences in the activation of NF-κB, which is tightly regulated at the level of TRAF2. Three regulatory proteins (TRAF-interacting proteins), I-TRAF, TRIP, and A20, bind to TRAF2 and inhibit its ability to activate NF-κB. In addition to regulation of NF-κB by TRAF2, in the brain, NF-κB is also regulated by a novel stress response gene, brain, and reproductive organ expressed (BRE). BRE appears to be activated specifically by TNFR1 and inhibits NF-KB activation (Gu et al. 1998). Thus, the efficiency of NF-κB activation in neuronal and/or glial cells depends on the duration of NF-κB activation and the differential activity of the regulatory proteins, which eventually determine the neurotoxic or neurotrophic outcome elicited by TNF-α. Indeed, such differences in the expression of NF-κB have been known to occur in the CNS (Joseph et al. 1996; Galasso et al. 2000). TNF-α is a key player in the pathogenesis of dopaminergic neurodegeneration and is up-regulated in the striatum following MPTP and methamphetamine (Sriram et al. 2002a, Sriram et al. 2006a, b). Despite an early and large increase in the striatal expression of TNF-α, activation of NF-κB was not detectable. These findings were consistent with an earlier observation (Teismann et al. 2001) and suggest that the lack of NF-κB activation may result in increased neurotoxicity (Botchkina et al. 1999). Thus, TNF-α elicits a neurotoxic response in the striatum. Conversely, activation of NF-κB by TNF-α in the hippocampus was neuroprotective (Tamatani et al. 1999). From these findings, a multifarious identity emerges for TNF-α that is influenced not only by regulation of TNF signaling, but also by regional differences in its cellular expression across brain regions.
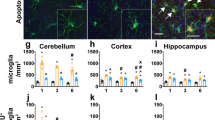
In the brain, TNF-α is predominantly produced by microglia. Microglia are localized in the vicinity of neurons and play an important role in host defense, sharing many phenotypic features with hematogenic macrophages. As the primary immune cell in the CNS, they play a dual role in cellular responses to neuronal injury: a pathogenic role that initiates inflammation and exacerbates degeneration and a neuroprotective role (Stoll and Jander 1999; Gonzalez-Scarano and Baltuch 1999; Streit et al. 1999). Under normal physiological environment, microglia reside in a quiescent state exhibiting a ramified morphology (ramified or resting microglia). In response to local injury, the ramified microglia retract their processes and acquire an amoeboid (activated microglia) or rounded (phagocytic microglia) shape. Reactive microglia express several immunological surface proteins, such as, complement type receptors (e.g., OX-42), major histocompatibility complex class II antigens (e.g., OX-6), and cytoplasmic/lysosomal antigens (e.g., ED-1, ED-2). The expression of these markers differs based on the type and extent of injury and their topographical distribution in the brain. Although microglia are abundant in the brain, the distribution and morphological heterogeneity of these cells vary across brain regions (Lawson et al. 1990). The hippocampus, basal ganglia, and substantia nigra are densely populated with microglia; moderate levels are found in cortex, thalamus, and hypothalamus, while less dense areas include the cerebellum and brain stem. The morphology of the microglia varies with their distribution, and they appear as (1) round with thick and short processes, typically localized in areas devoid of blood brain barrier, (2) longitudinally branched, as seen in fiber tracts, and (3) radially branched, distributed throughout the neuropil. Thus, the susceptibility of various brain regions to neurotoxic insults may be attributed to regional differences in microglial distribution and number, the microglial phenotype (morphology), and the repertoire of proinflammatory cytokines and chemokines they express. Marked differences in the regional expression of microglia-derived cytokines are apparent. The basal expression of proinflammatory mediators, TNF-α, MCP-1, and IL-1α were significantly higher in the hippocampus compared to striatum (Ren et al. 1999; Sriram et al. 2006a). Such regional variations in microglial distribution, morphology, and gene expression, influence cross talk with their immediate neuro-astroglial microenvironment, their response to external stimuli, and the timing and threshold of TNF-α release. A combination of these interactions ultimately define a neurotoxic or neurotrophic role for this cytokine.
One implication of such regional selectivity and dual role for microglia-derived TNF-α in the brain is that anti-TNF therapies currently in practice to treat certain auto-immune and inflammatory conditions may have negative consequences on the nervous system. It is therefore critical that a comprehensive screening of anti-TNF therapies across brain regions is performed to determine any adverse effects and evaluate the efficacy of such treatments. Overall, one has to demonstrate caution in extrapolating the results of preclinical anti-TNF studies into clinical practice.
Summary
Neurotoxicity and neurodegeneration are consequences of a shift in the subtle balance between neuronal survival and death, which is mediated by proinflammatory cytokines such as TNF-α. Enhanced expression of TNF-α can be observed in a variety of brain insults in association with other neuroinflammatory processes. Simultaneously, TNF-α possesses the ability to activate neuroprotective mechanisms. Thus, a double-edged role for this cytokine in the CNS has been documented. In reviewing the literature, a multifarious identity emerges for TNF-α that is influenced not only by the signaling pathways it activates, but also by regional differences in microglial distribution and morphology, the cells that predominantly produce this cytokine. Thus, the extent of microglial activation in specific brain regions, the timing and threshold of TNF-α expression, and the conditions that stimulate regulation of TNF signaling, eventually determine whether TNF-α plays a neurotoxic or neurotrophic role in the CNS.
Emerging concepts
Although it remains a relatively unexplored research arena, glial activation biology and drug–immune interactions may contribute to adverse neural outcomes associated with self-administration of drugs of abuse and the progression of HIV infection (Berman et al. 2006). In this context, drugs of abuse can encompass compounds as diverse as opioids and amphetamines. Methamphetamine and the HIV-1 protein Tat interact to exacerbate dopaminergic neurotoxicity (Theodore et al. 2006). It is suggested that Tat-induced expression of TNF-α may predispose striatal dopaminergic nerve terminals to subsequent damage by methamphetamine. Altered immune responses reflect stimulation of innate immune responses following the loss of adaptive immune response (Berman et al. 2006). Glial activation events that reflect stimulation of innate immunity can involve microglia and astrocytes at known targets of a given drug of abuse, e.g., the basal ganglia, but more generally, may reflect alterations at the BBB that effect enhanced entry of peripheral immune components into the brain parenchyma. Chief among proinflammatory mediators implicated in these adverse effects of drug abuse is TNF-α (see Thomas and Kuhn 2005; Sriram et al. 2006b). Of course, many other immune and nonimmune effectors may play a role in chronic adverse outcomes associated with drug abuse, but it is becoming clear that drug–neuron–glial–immune interactions up- and downstream of TNF-α are involved.
Abbreviations
- 3-NP:
-
3-nitropropionic acid
- 6-OHDA:
-
6-hydroxydopamine
- Aβ:
-
amyloid beta peptide
- AD:
-
Alzheimer’s disease
- BBB:
-
blood–brain barrier
- Bcl2:
-
B-cell CLL/lymphoma 2
- BCSFB:
-
blood–cerebrospinal fluid barrier
- BRE:
-
brain and reproductive organ expressed gene
- CER:
-
cerebellum
- CNS:
-
central nervous system
- CSF:
-
cerebrospinal fluid
- CTX:
-
cortex
- DD:
-
death domain
- DENN:
-
differentially expressed in normal versus neoplastic
- EAE:
-
experimental allergic encephalomyelitis
- FADD:
-
Fas-associated death domain
- HIP:
-
Hippocampus
- HIV:
-
human immunodeficiency virus
- MADD:
-
mitogen-activated protein kinase-activating death domain
- MCAO:
-
middle cerebral artery occlusion
- MDMA:
-
3,4-methylenedioxymethamphetamine
- METH:
-
methamphetamine
- MHC:
-
major histocompatibility complex
- MK-801:
-
(+)-5-methyl-10,11-dihydro-5H-dibenzo[a,d]cyclohepten-5,10-imine maleate
- MnSOD:
-
manganese superoxide dismutase
- MPTP:
-
1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine
- MS:
-
multiple sclerosis
- NFκB:
-
nuclear factor kappa B
- NIK:
-
nuclear factor kappa B inducing kinase
- NMDA:
-
N-methyl-d-aspartic acid
- PD:
-
Parkinson’s disease
- RIP:
-
receptor-interacting protein
- TACE:
-
TNF-α converting enzyme
- TNF:
-
tumor necrosis factor
- TNFR:
-
tumor necrosis factor receptor
- TNFR-DKO:
-
tumor necrosis factor receptor double knockout
- TRADD:
-
TNF receptor-associated death domain
- TRAF:
-
TNF receptor-associated factor
- TRIP:
-
TRAF-interacting protein
References
Achim CL, Heyes MP, Wiley CA (1993) Quantitation of human immunodeficiency virus, immune activation factors, and quinolinic acid in AIDS brains. J Clin Invest 91:2769–2775
Aggarwal BB (2003) Signalling pathways of the TNF superfamily: a double-edged sword. Nat Rev Immunol 3:745–756
Ajtai BM, Kalman M (1998) Glial fibrillary acidic protein expression but no glial demarcation follows the lesion in the molecular layer of cerebellum. Brain Res 802:285–288
Akassoglou K, Douni E, Bauer J, Lassmann H, Kollias G, Probert L (2003) Exclusive tumor necrosis factor (TNF) signaling by the p75TNF receptor triggers inflammatory ischemia in the CNS of transgenic mice. Proc Natl Acad Sci USA 100:709–714
Albensi BC, Mattson MP (2000) Evidence for the involvement of TNF and NF-kappaB in hippocampal synaptic plasticity. Synapse 35:151–159
Aloisi F (2001) Immune function of microglia. Glia 36:165–179
Aoki T, Kobayashi K, Isaki K (1999) Microglial and astrocytic change in brains of Creutzfeldt–Jakob disease: an immunocytochemical and quantitative study. Clin Neuropathol 18:51–60
Arimoto T, Bing G (2003) Up-regulation of inducible nitric oxide synthase in the substantia nigra by lipopolysaccharide causes microglial activation and neurodegeneration. Neurobiol Dis 12:35–45
Asanuma M, Tsuji T, Miyazaki I, Miyoshi K, Ogawa N (2003) Methamphetamine-induced neurotoxicity in mouse brain is attenuated by ketoprofen, a non-steroidal anti-inflammatory drug. Neurosci Lett 352:13–16
Banati RB, Daniel SF, Blunt SB (1998) Glial pathology but absence of apoptotic nigral neurons in long-standing Parkinson’s disease. Mov Disord 13:221–227
Barger SW, Horster D, Furukawa K, Goodman Y, Krieglstein J, Mattson MP (1995) Tumor necrosis factors alpha and beta protect neurons against amyloid beta-peptide toxicity: evidence for involvement of a kappa B-binding factor and attenuation of peroxide and Ca2+ accumulation. Proc Natl Acad Sci U S A 92:9328–9332
Barone FC, Arvin B, White RF, Miller A, Webb CL, Willette RN, Lysko PG, Feuerstein GZ (1997) Tumor necrosis factor-alpha. A mediator of focal ischemic brain injury. Stroke 28:1233–1244
Benkovic SA, O’Callaghan JP, Miller DB (2004) Sensitive indicators of injury reveal hippocampal damage in C57BL/6J mice treated with kainic acid in the absence of tonic–clonic seizures. Brain Res 1024:59–76
Benkovic SA, O’Callaghan JP, Miller DB (2006) Regional neuropathology following kainic acid intoxication in adult and aged C57BL/6J mice. Brain Res 1070:215–231
Benveniste EN, Sparacio SM, Bethea JR (1989) Tumor necrosis factor-alpha enhances interferon-gamma-mediated class II antigen expression on astrocytes. J Neuroimmunol 25:209–219
Berman J, Carson MJ, Chang L, Cox BM, Fox HS, Gonzalez RG, Hanson GR, Hauser KF, Ho W-Z, Maragos WF, Masliah E, McArthur JC, Miller DB, Nath A, O’Callaghan JP, Persidsky Y, Power C, Rogers TJ, Royal W (2006) NeuroAIDS, drug abuse and inflammation: building collaborative research activities. J Neuroimmune Pharmacol 1:351–399
Bizette C, Chan-Chi-Song P, Fontaine M, Tadie M (1996) Expression of mRNA, interleukin-1 beta, interleukin 6 and tumor necrosis factor-alpha during regeneration of the sciatic nerve in rats after tissue loss. Chirurg 121:474–481
Block F, Schmidt W, Nolden-Koch M, Schwarz M (2001) Rolipram reduces excitotoxic neuronal damage. NeuroReport 12:1507–1511
Bogdan I, Leib SL, Bergeron M, Chow L, Tauber MG (1997) Tumor necrosis factor-alpha contributes to apoptosis in hippocampal neurons during experimental group B streptococcal meningitis. J Infect Dis 176:693–697
Boka G, Anglade P, Wallach D, Javoy-Agid F, Agid Y, Hirsch EC (1994) Immunocytochemical analysis of tumor necrosis factor and its receptors in Parkinson’s disease. Neurosci Lett 172:151–154
Botchkina GI, Meistrell ME 3rd, Botchkina IL, Tracey KJ (1997) Expression of TNF and TNF receptors (p55 and p75) in the rat brain after focal cerebral ischemia. Mol Med 3:765–781
Botchkina GI, Geimonen E, Bilof ML, Villarreal O, Tracey KJ (1999) Loss of NF-kappaB activity during cerebral ischemia and TNF cytotoxicity. Mol Med 5:372–381
Brabers NA, Nottet HS (2006) Role of the pro-inflammatory cytokines TNF-alpha and IL-1beta in HIV-associated dementia. Eur J Clin Invest 36:447–458
Bruce AJ, Boling W, Kindy MS, Peschon J, Kraener PJ, Carpenter MK, Holtsberg FW, Mattson MP (1996) Altered neuronal and microglial responses to excitotoxic and ischemic brain injury in mice lacking TNF receptors. Nat Med 2:788–794
Bruce-Keller AJ, Geddes JW, Knapp PE, McFall RW, Keller JN, Holtsberg FW, Parthasarathy S, Steiner SM, Mattson MP (1999) Anti-death properties of TNF against metabolic poisoning: mitochondrial stabilization by MnSOD. J Neuroimmunol 93:53–71
Bruunsgaard H, Andersen-Ranberg K, Jeune B, Pedersen AN, Skinhoj P, Pedersen BK (1999) A high plasma concentration of TNF-alpha is associated with dementia in centenarians. J Gerontol Ser A Biol Sci Med Sci 54:M357–364
Butler TL, Kassed CA, Sanberg PR, Willing AE, Pennypacker KR (2002) Neurodegeneration in the rat hippocampus and striatum after middle cerebral artery occlusion. Brain Res 929:252–260
Buttini M, Appel K, Sauter A, Gebicke-Haerter PJ, Boddeke HW (1996) Expression of tumor necrosis factor alpha after focal cerebral ischaemia in the rat. Neuroscience 71:1–16
Cannella B, Raine CS (1995) The adhesion molecule and cytokine profile of multiple sclerosis lesions. Ann Neurol 37:424–435
Carbonell WS, Mandell JW (2003) Transient neuronal but persistent astroglial activation of ERK/MAP kinase after focal brain injury in mice. J Neurotrauma 20:327–336
Cardenas H, Bolin LM (2003) Compromised reactive microgliosis in MPTP-lesioned IL-6 KO mice. Brain Res 985:89–97
Carlson NG, Bacchi A, Rogers SW, Gahring LC (1998) Nicotine blocks TNF-alpha-mediated neuroprotection to NMDA by an alpha-bungarotoxin-sensitive pathway. J Neurobiol 35:29–36
Carson MJ, Doose JM, Melchior B, Schmid CD, Ploix CC (2006) CNS immune privilege: hiding in plain sight. Immunol Rev 213:48–65
Chao CC, Hu S (1994) Tumor necrosis factor-alpha potentiates glutamate neurotoxicity in human fetal brain cell cultures. Dev Neurosci 16:172–179
Cheng B, Christakos S, Mattson MP (1994) Tumor necrosis factors protect neurons against metabolic–excitotoxic insults and promote maintenance of calcium homeostasis. Neuron 12:139–153
Cheung WM, Wang CK, Kuo JS, Lin TN (1999) Changes in the level of glial fibrillary acidic protein (GFAP) after mild and severe focal cerebral ischemia. Chin J Physiol 42:227–235
Christov A, Ottman JT, Grammas P (2004) Vascular inflammatory, oxidative and protease-based processes: implications for neuronal cell death in Alzheimer’s disease. Neurol Res 26:540–546
Chung SY, Han SH (2003) Melatonin attenuates kainic acid-induced hippocampal neurodegeneration and oxidative stress through microglial inhibition. J Pineal Res 34:95–102
Collins JS, Perry RT, Watson B Jr, Harrell LE, Acton RT, Blacker D, Albert MS, Tanzi RE, Bassett SS, McInnis MG, Campbell RD, Go RC (2000) Association of a haplotype for tumor necrosis factor in siblings with late-onset Alzheimer disease: the NIMH Alzheimer Disease Genetics Initiative. Am J Med Genet 96:823–830
Dawson DA, Martin D, Hallenbeck JM (1996) Inhibition of tumor necrosis factor-alpha reduces focal cerebral ischemic injury in the spontaneously hypertensive rat. Neurosci Lett 218:41–44
De Bock F, Dornand J, Rondouin G (1996) Release of TNF alpha in the rat hippocampus following epileptic seizures and excitotoxic neuronal damage. NeuroReport 7:1125–1129
Declercq W, Denecker G, Fiers W, Vandenabeele P (1998) Cooperation of both TNF receptors in inducing apoptosis: involvement of the TNF receptor-associated factor binding domain of the TNF receptor 75. J Immunol 161:390–399
Depino AM, Earl C, Kaczmarczyk E, Ferrari C, Bededovsky H, del Rey A, Pitossi FJ, Oertel WH (2003) Microglial activation with atypical proinflammatory cytokine expression in a rat model of Parkinson’s disease. Eur J Neurosci 18:2731–2742
Dickson DW, Lee SC, Mattiace LA, Yen SH, Brosnan C (1993) Microglia and cytokines in neurological disease, with special reference to AIDS and Alzheimer’s disease. Glia 7:75–83
Dihne M, Block F (2001) Focal ischemia induces transient expression of IL-6 in the substantia nigra pars reticulata. Brain Res 889:165–173
Dihne M, Block F, Korr H, Topper R (2001) Time course of glial proliferation and glial apoptosis following excitotoxic CNS injury. Brain Res 902:178–189
Dobbs RJ, Charlett A, Purkiss AG, Dobbs SM, Weller C, Peterson DW (1999) Association of circulating TNF-alpha and IL-6 with ageing and parkinsonism. Acta Neurol Scand 100:34–41
Dopp JM, Mackenzie-Graham A, Otero GC, Merrill JE (1997) Differential expression, cytokine modulation, and specific functions of type-1 and type-2 tumor necrosis factor receptors in rat glia. J Neuroimmunol 75:104–112
Dziewulska D, Mossakowski MJ (2003) Cellular expression of tumor necrosis factor α and its receptors in human ischemic stroke. Clin Neuropathol 22:35–40
Eikelenboom P, Rozemuller AJ, Hoozemans JJ, Veerhuis R, van Gool WA (2000) Neuroinflammation and Alzheimer disease: clinical and therapeutic implications. Alzheimer Dis Assoc Disord 14(Suppl 1):S54–61
Engel S, Wehner HD, Meyermann R (1996) Expression of microglial markers in the human CNS after closed head injury. Acta Neurochir Suppl (Wien) 66:89–95
Engelhardt B (2006) Regulation of immune cell entry into the central nervous system. Results Probl Cell Differ 43:259–280
Fan L, Young PR, Barone FC, Feuerstein GZ, Smith DH, McIntosh TK (1996) Experimental brain injury induces differential expression of tumor necrosis factor-alpha mRNA in the CNS. Brain Res Mol Brain Res 36:287–291
Ferger B, Leng A, Mura A, Hengerer B, Feldon J (2004) Genetic ablation of tumor necrosis factor-alpha (TNF-alpha) and pharmacological inhibition of TNF-synthesis attenuates MPTP toxicity in mouse striatum. J Neurochem 89:822–833
Fiedorowicz A, Figiel I, Kaminska B, Zaremba M, Wilk S, Oderfeld-Nowak B (2001) Dentate granule neuron apoptosis and glia activation in murine hippocampus induced by trimethyltin exposure. Brain Res 912:116–127
Flora G, Lee YW, Nath A, Maragos W, Hennig B, Toborek M (2002) Methamphetamine-induced TNF-alpha gene expression and activation of AP-1 in discrete regions of mouse brain: potential role of reactive oxygen intermediates and lipid peroxidation. Neuromolecular Med 2:71–85
Fontaine V, Mohand-Said S, Hanoteau N, Fuchs C, Pfizenmaier K, Eisel U (2002) Neurodegenerative and neuroprotective effects of tumor necrosis factor (TNF) in retinal ischemia: opposite roles of TNF receptor 1 and TNF receptor 2. J Neurosci 22:RC216
Francis JW, Von Visger J, Markelonis GJ, Oh TH (1995) Neuroglial responses to the dopaminergic neurotoxicant, 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine in mouse striatum. Neurotoxicol Teratol 17:7–12
Galasso JM, Wang P, Martin D, Silverstein FS (2000) Inhibition of TNF-alpha can attenuate or exacerbate excitotoxic injury in neonatal rat brain. NeuroReport 7:231–235
Gartner S, Liu Y (2002) Insights into the role of immune activation in HIV neuropathogenesis. J Neurovirol 8:69–75
Gary DS, Bruce-Keller AJ, Kindy MS, Mattson MP (1998) Ischemic and excitotoxic brain injury is enhanced in mice lacking the p55 tumor necrosis factor receptor. J Cereb Blood Flow Metab 18:1283–1287
Gerber J, Bottcher T, Hahn M, Siemer A, Bunkowski S, Nau R (2004) Increased mortality and spatial memory deficits in TNF-alpha-deficient mice in ceftriaxone-treated experimental pneumococcal meningitis. Neurobiol Dis 16:133–138
Gianinazzi C, Grandgirard D, Imboden H, Egger L, Meli DN, Bifrare YD, Joss PC, Tauber MG, Borner C, Leib SL (2003) Caspase-3 mediates hippocampal apoptosis in pneumococcal meningitis. Acta Neuropathol (Berl) 105:499–507
Ginis I, Jaiswal R, Klimanis D, Liu J, Greenspon J, Hallenbeck JM (2002) TNF-alpha-induced tolerance to ischemic injury involves differential control of NF-kappaB transactivation: the role of NF-kappaB association with p300 adaptor. J Cereb Blood Flow Metab 22:142–152
Gonzalez-Scarano F, Baltuch G (1999) Microglia as mediators of inflammatory and degenerative diseases. Annu Rev Neurosci 22:219–240
Goodman Y, Mattson MP (1996) Ceramide protects hippocampal neurons against excitotoxic and oxidative insults, and amyloid beta-peptide toxicity. J Neurochem 66:869–872
Goodman JC, Robertson CS, Grossman RG, Narayan RK (1990) Elevation of tumor necrosis factor in head injury. J Neuroimmunol 30:213–217
Grassi F, Mileo AM, Monaco L, Punturieri A, Santoni A, Eusebi F (1994) TNF-alpha increases the frequency of spontaneous miniature synaptic currents in cultured rat hippocampal neurons. Brain Res 659:226–230
Gray F, Chretien F, Adle-Biassette H, Dorandeu A, Ereau T, Delisle MB, Kopp N, Ironside JW, Vital C (1999) Neuronal apoptosis in Creutzfeldt-Jakob disease. J Neuropathol Exp Neurol 58:321–328
Gu C, Castellino A, Chan JY, Chao MV (1998) BRE: a modulator of TNF-alpha action. FASEB J 12:1101–1108
Hauser SL, Doolittle TH, Lincoln R, Brown RH, Dinarello CA (1990) Cytokine accumulations in CSF of multiple sclerosis patients: frequent detection of interleukin-1 and tumor necrosis factor but not interleukin-6. Neurology 40:1735–1739
Hehlgans T, Pfeffer K (2005) The intriguing biology of the tumour necrosis factor/tumour necrosis factor receptor superfamily: players, rules and the games. Immunology 115:1–20
Hirsch EC, Breidert T, Rousselet E, Hunot S, Hartmann A, Michel PP (2003) The role of glial reaction and inflammation in Parkinson’s disease. Ann NY Acad Sci 991:214–228
Holmin S, Schalling M, Hojeberg B, Nordqvist AC, Skeftruna AK, Mathiesen T (1997) Delayed cytokine expression in rat brain following experimental contusion. J Neurosurg 86:493–504
Houzen H, Kikuchi S, Kanno M, Shinpo K, Tashiro K (1997) Tumor necrosis factor enhancement of transient outward potassium currents in cultured rat cortical neurons. J Neurosci Res 50:990–999
Hsu H, Shu HB, Pan MG, Goeddel DV (1996) TRADD-TRAF2 and TRADD-FADD interactions define two distinct TNF receptor 1 signal transduction pathways. Cell 84:299–308
Intiso D, Zarrelli MM, Lagioia G, Di Rienzo F, Checchia De Ambrosio C, Simone P, Tonali P, Cioffi Dagger RP (2004) Tumor necrosis factor alpha serum levels and inflammatory response in acute ischemic stroke patients. Neurol Sci 24:390–396
Isono M, Goda M, Kobayashi H, Wu JL (2003) TGF-alpha over-expression induces astrocytic hypertrophy after cortical stab would injury. Neurol Res 25:546–550
Janelsins MC, Mastrangelo MA, Oddo S, LaFerla FM, Federoff HJ, Bowers WJ (2005) Early correlation of microglial activation with enhanced tumor necrosis factor-alpha and monocyte chemoattractant protein-1 expression specifically within the entorhinal cortex of triple transgenic Alzheimer’s disease mice. J Neuroinflammation 2:23
Johnson EA, O’Callaghan JP, Miller DB (2002) Chronic treatment with supraphysiological levels of corticosterone enhances D-MDMA-induced dopaminergic neurotoxicity in the C57BL/6J female mouse. Brain Res 933:130–138
Joseph SA, Tassorelli C, Prasad AV, Lynd-Balta E (1996) NF-kappa B transcription factor subunits in rat brain: colocalization of p65 and alpha-MSH. Peptides 17:655–664
Kaltschmidt B, Uherek M, Wellmann H, Volk B, Kaltschmidt C (1999) Inhibition of NF-kappaB potentiates amyloid beta-mediated neuronal apoptosis. Proc Natl Acad Sci USA 96:9409–9414
Katchanov J, Waeber C, Gertz K, Gietz A, Winter B, Bruck W, Dirnagl U, Veh RW, Endres M (2003) Selective neuronal vulnerability following mild focal brain ischemia in the mouse. Brain Pathol 13:452–464
Kita T, Liu L, Tanaka N, Kinoshita Y (1997) The expression of tumor necrosis factor-alpha in the rat brain after fluid percussive injury. Int J Legal Med 110:305–311
Knoblach SM, Fan L, Faden AI (1999) Early neuronal expression of tumor necrosis factor-alpha after experimental brain injury contributes to neurological impairment. J Neuroimmunol 95:115–125
Koller H (1997) TNF alpha in cerebrospinal fluid of meningitis patients reduces astrocytes membrane potential. J Neuroimmunol 76:185–188
Kreutzberg GW (1996) Microglia: a sensor for pathological events in the CNS. Trends Neurosci 19:312–318
Krum JM, Phillips TM, Rosenstein JM (2002) Changes in astroglial GLT-1 expression after neural transplantation or stab wounds. Exp Neurol 174:137–149
Laskawi R, Rohlmann A, Landgrebe M, Wolff JR (1997) Rapid astroglial reactions in the motor cortex of adult rats following peripheral facial nerve lesions. Eur Arch Otorhinolaryngol 254:81–85
Lavine SD, Hofman FM, Zlokovic BV (1998) Circulating antibody against tumor necrosis factor-alpha protects rat brain from reperfusion injury. J Cereb Blood Flow Metab 18:52–58
Lawson LJ, Perry VH, Dri P, Gordon S (1990) Heterogeneity in the distribution and morphology of microglia in the normal adult mouse brain. Neuroscience 39:151–170
Little AR, Benkovic SA, Miller DB, O’Callaghan JP (2002) Chemically induced neuronal damage and gliosis: enhanced expression of the proinflammatory chemokine, monocyte chemoattractant protein (MCP)-1, without a corresponding increase in proinflammatory cytokines. Neuroscience 115:307–320
Liu T, Clark RK, McDonnell PC, Young PR, White RF, Barone FC, Feuerstein GZ (1994) Tumor necrosis factor-alpha expression in ischemic neurons. Stroke 25:1481–1488
Liu XH, Xu H, Barks JD (1999) Tumor necrosis factor-α attenuates N-methyl-d-aspartate-mediated neurotoxicity in neonatal rat hippocampus. Brain Res 851:94–104
Lucas R, Juillard P, Decoster E, Redard M, Burger D, Donati Y, Giroud C, Monso-Hinard C, De Kesel T, Buurman WA, Moore MW, Dayer JM, Fiers W, Bluethmann H, Grau GE (1997) Crucial role of tumor necrosis factor (TNF) receptor 2 and membrane-bound TNF in experimental cerebral malaria. Eur J Immunol 27:1719–1725
Manchester M, Eto DS, Oldstone MB (1999) Characterization of the inflammatory response during acute measles encephalitis in NSE-CD46 transgenic mice. J Neuroimmunol 96:207–217
Marquette C, Van Dam AM, Ceccaldi PE, Weber P, Haour F, Tsiang H (1996) Induction of immunoreactive interleukin-1 beta and tumor necrosis factor-alpha in the brains of rabies virus infected rats. J Neuroimmunol 68:45–51
Martino G, Consiglio A, Franciotta DM, Corti A, Filippi M, Vandenbroeck K, Sciacca FL, Comi G, Grimaldi LM (1997) Tumor necrosis factor alpha and its receptors in relapsing-remitting multiple sclerosis. J Neurol Sci 152:51–61
Masliah E, LiCastro F (2000) Neuronal and synaptic loss, reactive gliosis, microglial response, and induction of the complement cascade in Alzheimer’s disease. In: Clark CM, Trojanowski, JQ (eds) Neurodegenerative dementias, McGraw-Hill, New York, pp. 131–146
Mattson MP, Cheng B, Baldwin SA, Smith-Swintosky VL, Keller J, Geddes JW, Scheff SW, Christakos S (1995) Brain injury and tumor necrosis factors induce calbindin D-28k in astrocytes: evidence for a cytoprotective response. J Neurosci Res 42:357–370
Mattson MP, Goodman Y, Luo H, Fu W, Furukawa K (1997) Activation of NF-kappaB protects hippocampal neurons against oxidative stress-induced apoptosis: evidence for induction of manganese superoxide dismutase and suppression of peroxynitrite production and protein tyrosine nitration. J Neurosci Res 49:681–697
Matusevicius D, Navikas V, Soderstrom M, Xiao BG, Haglund M, Fredrikson S, Link H (1996) Multiple sclerosis: the proinflammatory cytokines lymphotoxin-alpha and tumour necrosis factor-alpha are upregulated in cerebrospinal fluid mononuclear cells. J Neuroimmunol 66:115–123
McCoy MK, Martinez TN, Ruhn KA, Szymkowski DE, Smith CG, Botterman BR, Tansey KE, Tansey MG (2006) Blocking soluble tumor necrosis factor signaling with dominant-negative tumor necrosis factor inhibitor attenuates loss of dopaminergic neurons in models of Parkinson’s disease. J Neurosci 26:9365–9375
McGeer PL, McGeer EG (1998) Glial cell reactions in neurodegenerative diseases: pathophysiology and therapeutic interventions. Alzheimer Dis Assoc Disord 12(Suppl 2):S1–S6
McGeer PL, McGeer EG (2004) Inflammation and the degenerative diseases of aging. Ann N Y Acad Sci 1035:104–116
McGeer PL, Schwab C, Parent A, Doudet D (2003) Presence of reactive microglia in monkey substantia nigra years after 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine administration. Ann Neurol 54:599–604
Meda L, Cassatella MA, Szendrei GI, Otvos L Jr, Baron P, Villalba M, Ferrari D, Rossi F (1995) Activation of microglial cells by beta-amyloid protein and interferon-gamma. Nature 374:647–650
Meistrell ME 3rd, Botchkina GI, Wang H, Di Santo E, Cockroft KM, Bloom O, Vishnubhakat JM, Ghezzi P, Tracey KJ (1997) Tumor necrosis factor is a brain damaging cytokine in cerebral ischemia. Shock 8:341–348
Minghetti L (2005) Role of inflammation in neurodegenerative diseases. Curr Opin Neurol 18:315–321
Mogi M, Harada M, Riederer P, Narabayashi H, Fujita K, Nagatsu T (1994) Tumor necrosis factor-alpha increases both in brain and in the cerebrospinal fluid from parkinsonian patients. Neurosci Lett 165:208–210
Mogi M, Harada M, Kondo T, Riederer P, Nagatsu T (1995) Brain beta 2-macroglobulin levels are elevated in the striatum in Parkinson’s disease. J Neural Transm 9:87–92
Mogi M, Togari A, Tanaka K, Ogawa N, Ichinose H, Nagatsu T (1999) Increase in level of tumor necrosis factor (TNF)-alpha in 6-hydroxydopamine-lesioned striatum in rats without the influence of systemic L-DOPA on the TNF-alpha induction. Neurosci Lett 268:101–104
Munoz-Fernandez MA, Fresno M (1998) The role of tumour necrosis factor, interleukin 6, interferon-gamma and inducible nitric oxide synthase in the development and pathology of the nervous system. Prog Neurobiol 56:307–340
Nawashiro H, Tasaki K, Ruetzler CA, Hallenbeck JM (1997) TNF-alpha pretreatment induces protective effects against focal cerebral ischemia in mice. J Cereb Blood Flow Metab 17:483–490
Nishimura M, Mizuta I, Mizuta E, Yamasaki S, Ohta M, Kaji R, Kuno S (2001) Tumor necrosis factor gene polymorphisms in patients with sporadic Parkinson’s disease. Neurosci Lett 311:1–4
Perry VH (1998) A revised view of the central nervous system microenvironment and major histocompatibility complex class II antigen presentation. J Neuroimmunol 90:113–121
Persidsky Y, Limoges J, Rasmussen J, Zheng J, Gearing A, Gendelman HE (2001) Reduction in glial immunity and neuropathology by a PAF antagonist and an MMP and TNFalpha inhibitor in SCID mice with HIV-1 encephalitis. J Neuroimmunol 114:57–68
Petzold A, Eikelenboom MJ, Gveric D, Keir G, Chapman M, Lazeron RH, Cuzner ML, Polman CH, Uitdehaag BM, Thompson EJ, Giovannoni G (2002) Markers for different glial cell responses in multiple sclerosis: clinical and pathological correlations. Brain 125:1462–1473
Plant SR, Arnett HA, Ting JP (2005) Astroglial-derived lymphotoxin-alpha exacerbates inflammation and demyelination, but not remyelination. Glia 49:1–14
Probert L, Selmaj K (1997) TNF and related molecules: trends in neuroscience and clinical applications. J Neuroimmunol 72:113–117
Quasney MW, Zhang Q, Sargent S, Mynatt M, Glass J, McArthur J (2001) Increased frequency of the tumor necrosis factor-alpha-308 A allele in adults with human immunodeficiency virus dementia. Ann Neurol 50:157–162
Quintana A, Giralt M, Rojas S, Penkowa M, Campbell IL, Hidalgo J, Molinero A (2005) Differential role of tumor necrosis factor receptors in mouse brain inflammatory responses in cryolesion brain injury. J Neurosci Res 82:701–716
Raivich G, Bluethmann H, Kreutzberg GW (1996) Signaling molecules and neuroglial activation in the injured central nervous system. Keio J Med 45:239–247
Ransohoff RM, Glabinski A, Tani M (1996) Chemokines in immune-mediated inflammation of the central nervous system. Cytokine Growth Factor Rev 7:35–46
Ren L, Lubrich B, Biber K, Gebicke-Haerter PJ (1999) Differential expression of inflammatory mediators in rat microglia cultured from different brain regions. Brain Res Mol Brain Res 65:198–205
Rodrigues RW, Gomide VC, Chadi G (2001) Astroglial and microglial reaction after a partial nigrostriatal degeneration induced by the striatal injection of different doses of 6-hydroxydopamine. Int J Neurosci 109:91–126
Rosenberg GA, Estrada EY, Dencoff JE, Stetler-Stevenson WG (1995) Tumor necrosis factor-alpha-induced gelatinase B causes delayed opening of the blood–brain barrier: an expanded therapeutic window. Brain Res 703:151–155
Ross SA, Halliday MI, Campbell GC, Byrnes DP, Rowlands BJ (1994) The presence of tumour necrosis factor in CSF and plasma after severe head injury. Br J Neurosurg 8:419–425
Ryu JK, Nagai A, Kim J, Lee MC, McLarnon JG, Kim SU (2003) Microglial activation and cell death induced by the mitochondrial toxin 3-nitropropionic acid: in vitro and in vivo studies. Neurobiol Dis 12:121–132
Saha RN, Pahan K (2003) Tumor necrosis factor-alpha at the crossroads of neuronal life and death during HIV-associated dementia. J Neurochem 86:1057–1071
Sairanen T, Carpen O, Karjalainen-Lindsberg ML, Paetau A, Turpeinen U, Kaste M, Lindsberg PJ (2001) Evolution of cerebral tumor necrosis factor-alpha production during human ischemic stroke. Stroke 32:1750–1758
Saito K, Suyama K, Nishida K, Sei Y, Basile AS (1996) Early increases in TNF-alpha, IL-6 and IL-1 beta levels following transient cerebral ischemia in gerbil brain. Neurosci Lett 206:149–152
Sanchez-Burgos G, Hernandez-Pando R, Campbell IL, Ramos-Castaneda J, Ramos C (2004) Cytokine production in brain of mice experimentally infected with dengue virus. Neuroreport 15:37–42
Schiefer J, Topper R, Schmidt W, Block F, Heinrich PC, Noth J, Schwarz M (1998) Expression of interleukin 6 in the rat striatum following stereotaxic injection of quinolinic acid. J Neuroimmunol 89:168–176
Seilhean D, Kobayashi K, He Y, Uchihara T, Rosenblum O, Katlama C, Bricaire F, Duyckaerts C, Hauw JJ (1997) Tumor necrosis factor-alpha, microglia and astrocytes in AIDS dementia complex. Acta Neuropathol (Berl) 93:508–517
Sherer TB, Betarbet R, Kim JH, Greenamyre JT (2003) Selective microglial activation in the rat rotenone model of Parkinson’s disease. Neurosci Lett 341:87–90
Shiozaki T, Hayakata T, Tasaki O, Hosotubo H, Fuijita K, Mouri T, Tajima G, Kajino K, Nakae H, Tanaka H, Shimazu T, Sugimoto H (2005) Cerebrospinal fluid concentrations of anti-inflammatory mediators in early-phase severe traumatic brain injury. Shock 23:406–410
Shohami E, Novikov M, Bass R, Yamin A, Gallily R (1994) Closed head injury triggers early production of TNF alpha and IL-6 by brain tissue. J Cereb Blood Flow Metab 14:615–619
Shohami E, Gallily R, Mechoulam R, Bass R, Ben-Hur T (1997) Cytokine production in the brain following closed head injury: dexanabinol (HU-211) is a novel TNF-alpha inhibitor and an effective neuroprotectant. J Neuroimmunol 72:169–177
Shrikant P, Chung IY, Ballestas ME, Benveniste EN (1994) Regulation of intercellular adhesion molecule-1 gene expression by tumor necrosis factor-alpha, interleukin-1 beta, and interferon-gamma in astrocytes. J Neuroimmunol 51:209–220
Skias DD, Kim DK, Reder AT, Antel JP, Lancki DW, Fitch FW (1987) Susceptibility of astrocytes to class I MHC antigen-specific cytotoxicity. J Immunol 138:3254–3258
Soltys Z, Janeczko K, Orzylowska-Sliwinska O, Zaremba M, Januszewski S, Oderfeld-Nowak B (2003) Morphological transformations of cells immunopositive for GFAP, TrkA or p75 in the CA1 hippocampal area following transient global ischemia in the rat: a quantitative study. Brain Res 987:186–193
Sompol P, Xu Y, Ittarat W, Daosukho C, St Clair D (2006) NF-kappaB-associated MnSOD induction protects against beta-amyloid-induced neuronal apoptosis. J Mol Neurosci 29:279–288
Sprang SR (1990) The divergent receptors for TNF. Trends Biochem Sci 15:366–368
Sriram K, Matheson JM, Benkovic SA, Miller DB, Luster MI, O’Callaghan JP (2002a) Mice deficient in TNF receptors are protected against dopaminergic neurotoxicity: implications for Parkinson’s disease. FASEB J 16:1474–1476
Sriram K, Benkovic SA, Miller DB, O’Callaghan JP (2002b) Obesity exacerbates chemically induced neurodegeneration. Neuroscience 115:1335–1346
Sriram K, Matheson JM, Benkovic SA, Miller DB, Luster MI, O’Callaghan JP (2006a) Deficiency of TNF receptors suppresses microglial activation and alters the susceptibility of brain regions to MPTP-induced neurotoxicity: role of TNF-α. FASEB J 20:670–682
Sriram K, Miller DB, O’Callaghan JP (2006b) Minocycline attenuates microglial activation but fails to mitigate striatal dopaminergic neurotoxicity: role of tumor necrosis factor-α. J Neurochem 93:706–718
Stahel PF, Kariya K, Shohami E, Barnum SR, Eugster H, Trentz O, Kossmann T, Morganti-Kossmann MC (2000) Intracerebral complement C5a receptor (CD88) expression is regulated by TNF and lymphotoxin-alpha following closed head injury in mice. J Neuroimmunol 109:164–172
Stoll G, Jander S (1999) The role of microglia and macrophages in the pathophysiology of the CNS. Prog Neurobiol 58:233–247
Streit WJ, Walter SA, Pennell NA (1999) Reactive microgliosis. Prog Neurobiol 57:563–581
Sullivan PG, Bruce-Keller AJ, Rabchevsky AG, Christakos S, Clair DK, Mattson MP, Scheff SW (1999) Exacerbation of damage and altered NF-kappaB activation in mice lacking tumor necrosis factor receptors after traumatic brain injury. J Neurosci 19:6248–6256
Tamatani M, Che YH, Matsuzaki H, Ogawa S, Okado H, Miyake S, Mizuno T, Tohyama M (1999) Tumor necrosis factor induces Bcl-2 and Bcl-x expression through NFkappaB activation in primary hippocampal neurons. J Biol Chem 274:8531–8538
Tarkowski E, Blennow K, Wallin A, Tarkowski A (1999) Intracerebral production of tumor necrosis factor-alpha, a local neuroprotective agent, in Alzheimer disease and vascular dementia. J Clin Immunol 19:223–230
Tartaglia LA, Weber RF, Figari IS, Reynolds C, Palladino MA Jr, Goeddel DV (1991) The two different receptors for tumor necrosis factor mediate distinct cellular responses. Proc Natl Acad Sci USA 88:9292–9296
Taupin V, Toulmond S, Serrano A, Benavides J, Zavala F (1993) Increase in IL-6, IL-1 and TNF levels in rat brain following traumatic lesion. Influence of pre- and post-traumatic treatment with Ro5 4864, a peripheral-type (p site) benzodiazepine ligand. J Neuroimmunol 42:177–185
Teismann P, Schwaninger M, Weih F, Ferger B (2001) Nuclear factor-kappaB activation is not involved in a MPTP model of Parkinson’s disease. NeuroReport 12:1049–1053
Teunissen CE, Steinbusch HW, Angevaren M, Appels M, de Bruijn C, Prickaerts J, de Vente J (2001) Behavioural correlates of striatal glial fibrillary acidic protein in the 3-nitropropionic acid rat model: disturbed walking pattern and spatial orientation. Neuroscience 105:153–167
Theodore S, Cass WA, Nath A, Steiner J, Young K, Maragos WF (2006) Inhibition of tumor necrosis factor-alpha signaling prevents human immunodeficiency virus-1 protein Tat and methamphetamine interaction. Neurobiol Dis 23:663–668
Thomas DM, Kuhn DM (2005) MK-801 and dextromethorphan block microglial activation and protect against methamphetamine-induced neurotoxicity. Brain Res 1050:190–198
Thomas DM, Walker PD, Benjamins JA, Geddes TJ, Kuhn DM (2004) Methamphetamine neurotoxicity in dopamine nerve endings of the striatum is associated with microglial activation. J Pharmacol Exp Ther 311:1–7
Turrin NP, Rivest S (2006) Tumor necrosis factor alpha but not interleukin 1 beta mediates neuroprotection in response to acute nitric oxide excitotoxicity. J Neurosci 26:143–151
Tyor WR, Power C, Gendelman HE, Markham RB (1993) A model of human immunodeficiency virus encephalitis in scid mice. Proc Natl Acad Sci USA 90:8658–8662
Uno H, Matsuyama T, Akita H, Nishimura H, Sugita M (1997) Induction of tumor necrosis factor-alpha in the mouse hippocampus following transient forebrain ischemia. J Cereb Blood Flow Metab 17:491–499
Vanzani MC, Iacono RF, Caccuri RL, Troncoso AR, Berria MI (2006) Regional differences in astrocyte activation in HIV-associated dementia. Medicina (B Aires) 66:108–112
Versijpt JJ, Dumont F, Van Laere KJ, Decoo D, Santens P, Audenaert K, Achten E, Slegers G, Dierckx RA, Korf J (2003) Assessment of neuroinflammation and microglial activation in Alzheimer’s disease with radiolabelled PK11195 and single photon emission computed tomography: a pilot study. Eur Neurol 50:39–47
Vila M, Jackson-Lewis V, Guegan C, Wu DC, Teismann P, Choi DK, Tieu K, Przedborski S (2001) The role of glial cells in Parkinson’s disease. Curr Opin Neurol 14:483–489
Vila N, Castillo J, Davalos A, Chamorro A (2000) Proinflammatory cytokines and early neurological worsening in ischemic stroke. Stroke 31:2325–2329
Villarroya H, Marie Y, Ouallet JC, Le Saux F, Tchelingerian JL, Baumann N (1997) Expression of TNF alpha in central neurons of Lewis rat spinal cord after EAE induction. J Neurosci Res 49:592–599
Wesselingh SL, Power C, Glass JD, Tyor WR, McArthur JC, Farber JM, Griffin JW, Griffin DE (1993) Intracerebral cytokine messenger RNA expression in acquired immunodeficiency syndrome dementia. Ann Neurol 33:576–582
Wesselingh SL, Takahashi K, Glass JD, McArthur JC, Griffin JW, Griffin DE (1997) Cellular localization of tumor necrosis factor mRNA in neurological tissue from HIV-infected patients by combined reverse transcriptase/polymerase chain reaction in situ hybridization and immunohistochemistry. J Neuroimmunol 74:1–8
Wierzba-Bobrowicz T, Gwiazda E, Kosno-Kruszewska E, Lewandowska E, Lechowicz W, Bertrand E, Szpak GM, Schmidt-Sidor B (2002) Morphological analysis of active microglia-rod and ramified microglia in human brains affected by some neurological diseases (SSPE, Alzheimer’s disease and Wilson’s disease). Folia Neuropathol 40:125–131
Wilson CM, Grace GM, Munoz DG, He BP, Strong MJ (2001) Cognitive impairment in sporadic ALS: a pathologic continuum underlying a multisystem disorder. Neurology 57:651–657
Zawadzka M, Kaminska B (2005) A novel mechanism of FK506-mediated neuroprotection: downregulation of cytokine expression in glial cells. Glia 49:36–51
Zhu W, Umegaki H, Shinkai T, Kurotani S, Suzuki Y, Endo H, Iguchi A (2003) Different glial reactions to hippocampal stab wounds in young adult and aged rats. J Gerontol A Biol Sci Med Sci 58:117–122
Author information
Authors and Affiliations
Corresponding author
Additional information
“The findings and conclusions in this report are those of the authors and do not necessarily represent the views of the National Institute for Occupational Safety and Health.”
Rights and permissions
About this article
Cite this article
Sriram, K., O’Callaghan, J.P. Divergent Roles for Tumor Necrosis Factor-α in the Brain. Jrnl Neuroimmune Pharm 2, 140–153 (2007). https://doi.org/10.1007/s11481-007-9070-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-007-9070-6